ad9395c647ea6f1c116a7cd264824d2b.ppt
- Количество слайдов: 78

working with a disability in California World Institute on Disability Copyright © 2006

“Medicare, the Parts and the Players” And Medicare Part D 2

Medicare Training 1. 2. 3. 4. 5. 6. 7. 8. Medicare Parts and Supplements New Prescription Drug Benefit 2006 Financial Subsidy for New Drug Plan Costs What’s in a Medicare Prescription Drug Plan? Special Needs Plans Beneficiary Protections and Appeals State of California Involvement Resources and References 3

Medicare >Caution Ahead< New rules and new programs … The Gold Standard: know your customer. þ What is their current benefits status, their needs, their plans? þ Work from this vantage point when explaining new rules and new options. þ Avoid information overload, if possible. þ Share practical info for customer needs, wants, plans. 4

Medicare Training 1. Medicare Parts and Supplements 5

Medicare • • • Covers most age 65 or older Some younger than 65 with disabilities, mostly Social Security Disability Insurance (SSDI) beneficiaries People with end stage renal diseases (ESRD) 6

Medicare Today Ü The Parts Not full coverage or comprehensive insurance by itself New parts and supplements make for many new rules Leave your logic and common sense at the door. 7

Medicare Key Terms, or Terms of Art • • Part A, Part B, Part C, and Part D Medicare Supplements • Medigap Plans, or Medigap: private insurance plans • Medicare Savings Programs: government support to supplement Medicare costs for low income beneficiaries • • Medicare Advantage Plans (HMOs, were called Medicare + Choice), what is now Medicare Part C Premiums, Deductibles, Coinsurance, Co-payments (copays) Dual eligible(s), or Medi-Medi(s) Formulary 8

Medicare Key Terms or Terms of Art Courtesy: California Legislative Analyst Office, www. lao. ca. gov Key Insurance Terms — Definitions • Premium • An amount paid often in monthly installments to purchase an insurance policy • Deductible • An initial specified amount that an enrollee has to pay before the insurer begins to contribute towards medical costs • Coinsurance • A set percentage of medical costs that enrollees must pay towards the cost of their medical care • Co-payment • A fixed fee that enrollees of a medical insurance plan must pay for their use of specific medical services provided by the plan, for example, prescription drugs 9

Medicare Eligibility For most SSDI beneficiaries: • Eligibility begins in the 25 th month of SSDI cash benefits, which is 29 months after the date Social Security determines that the disability began. 10

Medicare in 2006 • • Part A: Hospital Insurance Part B: Medical Insurance Part C: Medicare Advantage (HMOs) formerly Medicare + Choice, in some but not all CA counties Part D: Prescription Drug Benefit 11

Medicare Part A • Pays for most inpatient hospital care • some inpatient skilled nursing home care • some health care, and hospice care, blood transfusions • SSDI qualify automatically for Medicare, no monthly premium for Part A coverage 12

Medicare Part A • Has deductibles and copayments 13

Medicare Part B • • • Pays for doctors' services Outpatient hospital care Outpatient physical and speech therapy Some health care but not long term services Ambulance services, and some medical equipment and supplies 14

Medicare Part B • • • Part B coverage is voluntary, about 95 percent of Part A folks voluntarily stay enrolled in Part B. Monthly premium ($88. 50 in 2006) automatically deducted from Social Security benefit check every month, higher premiums with incomes above $80, 000/yr. starting in 2007 If you don't receive Social Security benefits, 15 you are billed for Part B.

Medigap Insurance Private insurance q Covers co-payments, deductibles, and some services for Original Medicare beneficiaries only q Details at www. calmedicare. org 16

Medicare Savings Programs Government help with Medicare deductibles, premiums, copays, or coinsurance. Apply for at CA county welfare offices. q Details at www. calmedicare. org 1. 2. 3. 4. q Qualified Medicare Beneficiary-QMB Specified Low-Income Medicare Beneficiary-SLMB Qualified Individual-QI-1 Qualified Disabled Working Individual-QDWI Also see Medi-Cal on www. db 101. org and in training manual 17

MMA The Medicare Prescription Drug, Improvement, and Modernization Act of 2003 18

Medicare Training 1. 2. Medicare Parts and Supplements New Prescription Drug Benefit 2006 19

New Drug Benefit Overview ü Standard and enhanced benefits delivered through private plans, Prescription Drug Plans, PDPs, Medicare’s new Part D, and Medicare Advantage Prescription Drug Plans, MA-PD, to be found in Medicare’s Part C ü Market driven model of competing private plans in terms of benefits and costs, with a minimum choice of at least two plans for every Medicare beneficiary, one of which must be a stand-alone Prescription Drug Plan, a PDP ü Each PDP negotiates with drug makers for drug prices, not Medicare or the government. Drug Benefit Cost slides with permission the Kaiser Family Foundation, 2004 20

New Drug Benefit Overview ü Most dual eligibles now get most of their drug benefits from Medicare or other insurance, not Medi-Cal drug services which use federal funds, effective January 1, 2006. ü Monthly penalty for late enrollment, which is 1% of base premium for each month of delay Important exception applies for those who already have prescription drug coverage at least as good as Medicare Part D drug plans (CMS 3/05). This is called “creditable” coverage. Drug Benefit Cost slides with permission the Kaiser Family Foundation, 2004 21
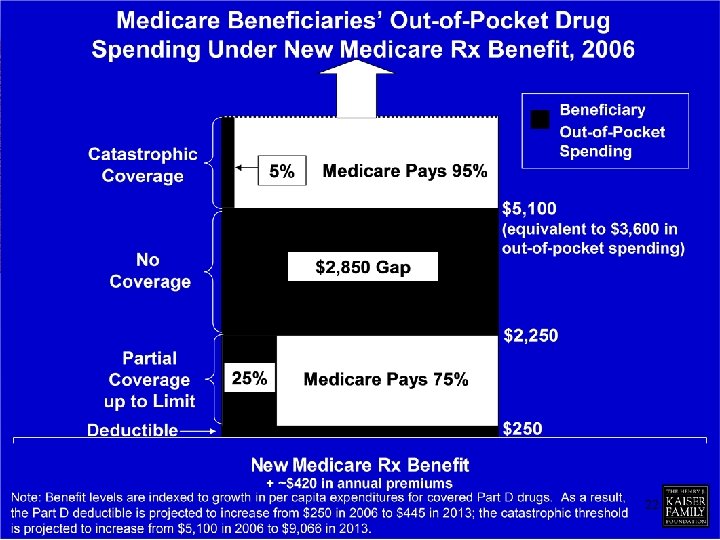
22

2006 Prescription Drug Benefit Important General Information ÜEntitled to Part A or enrolled in Part B = eligible for a Medicare PDP ÜEntitled to Part A and enrolled in Part B = also eligible for a Medicare Advantage PD plan ÜVoluntary benefit, for all except duals and with an understanding of the late enrollment rules 23

Medicare Training 1. 2. 3. Medicare Parts and Supplements New Prescription Drug Benefit 2006 Financial Subsidy for New Drug Plan Costs 24

The Players • • • 43 million Medicare beneficiaries nationwide 6. 8 million are dual eligible for Medicaid and Medicare California Players Statewide and Select Counties 25
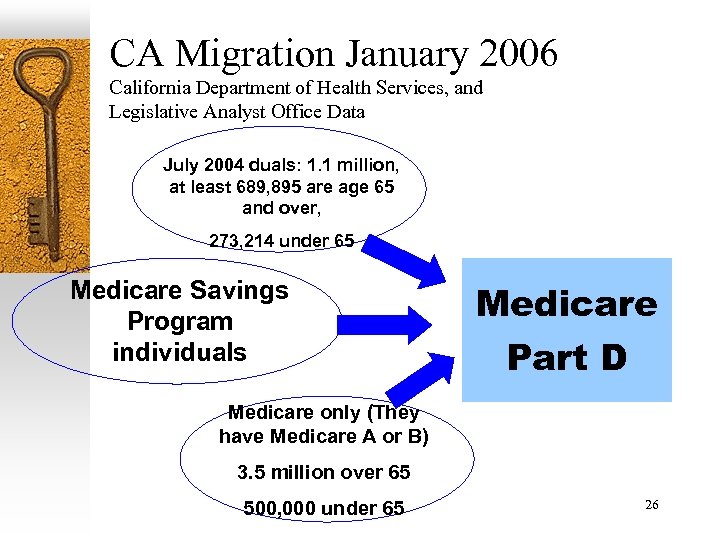
CA Migration January 2006 California Department of Health Services, and Legislative Analyst Office Data July 2004 duals: 1. 1 million, at least 689, 895 are age 65 and over, 273, 214 under 65 Medicare Savings Program individuals Medicare Part D Medicare only (They have Medicare A or B) 3. 5 million over 65 500, 000 under 65 26

CA Migration January 2006 California Department of Health Services, and Legislative Analyst Office Data 937, 000 in Medi-Cal fee for service More than twice as likely to be in fair or poor health, 25% are in long-term care facilities, 40% have a cognitive impairment Medicare Part D 137, 00 in Medi-Cal managed care 27
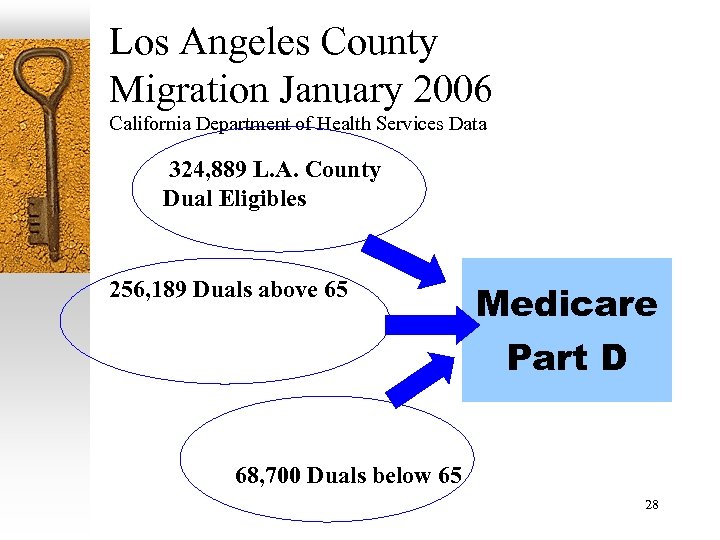
Los Angeles County Migration January 2006 California Department of Health Services Data 324, 889 L. A. County Dual Eligibles 256, 189 Duals above 65 Medicare Part D 68, 700 Duals below 65 28
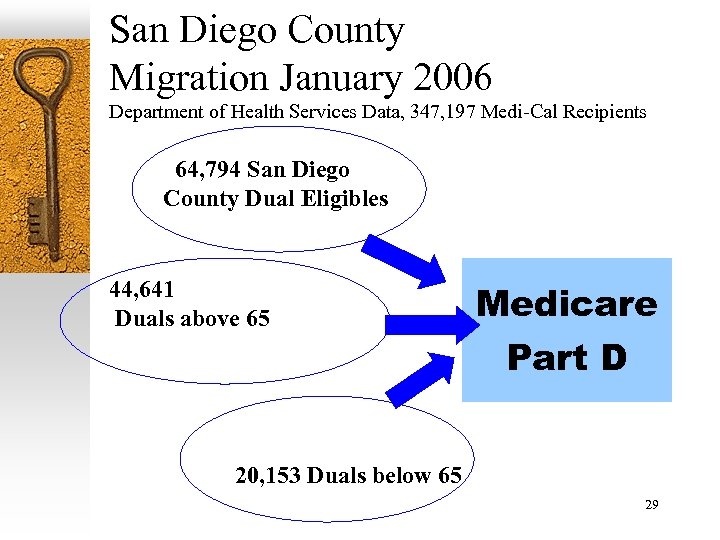
San Diego County Migration January 2006 Department of Health Services Data, 347, 197 Medi-Cal Recipients 64, 794 San Diego County Dual Eligibles 44, 641 Duals above 65 Medicare Part D 20, 153 Duals below 65 29
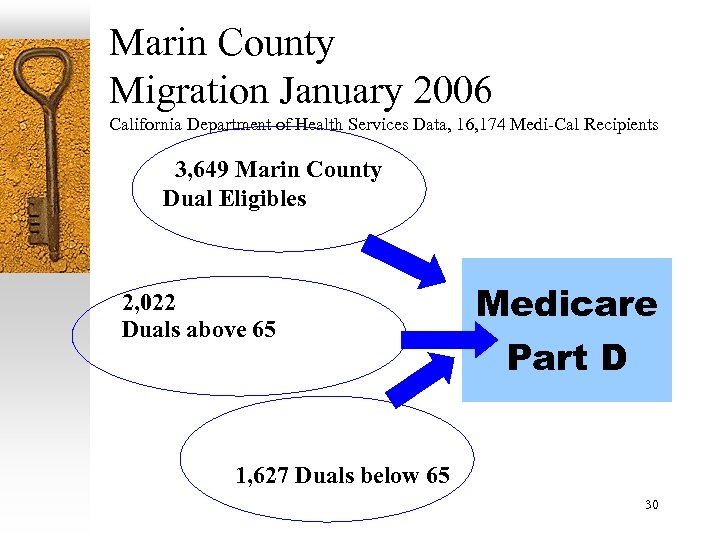
Marin County Migration January 2006 California Department of Health Services Data, 16, 174 Medi-Cal Recipients 3, 649 Marin County Dual Eligibles 2, 022 Duals above 65 Medicare Part D 1, 627 Duals below 65 30
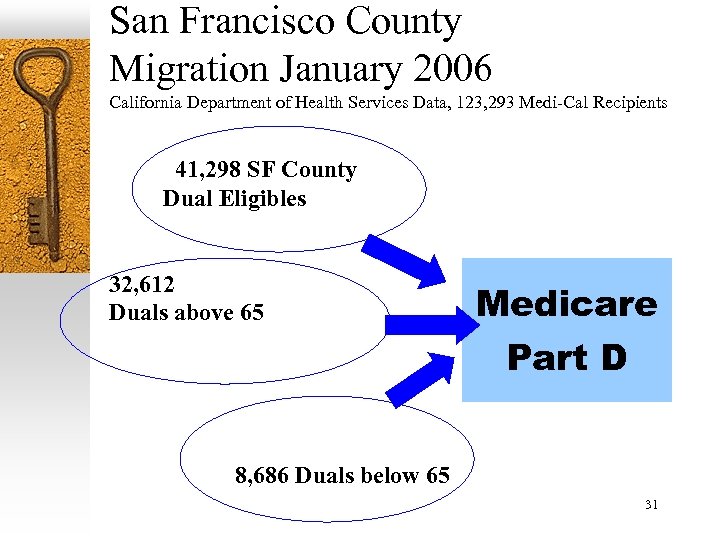
San Francisco County Migration January 2006 California Department of Health Services Data, 123, 293 Medi-Cal Recipients 41, 298 SF County Dual Eligibles 32, 612 Duals above 65 Medicare Part D 8, 686 Duals below 65 31

Full Benefit Dual Eligibles • Medicare offers better premium and costsharing rates for certain “subsidy eligible” individuals. • Eligibility for a subsidy depends on an enrollee’s Medi-Cal status and income. 32

Full Benefit Dual Eligibles Medicare enrollees eligible for Medicaid “under any eligibility category covered under the State Plan” are deemed “FULL BENEFIT DUAL ELIGIBLE” individuals (MMA/CMS regulation Section 423. 772), or Section 1860 D and 1935 C-6, Social Security Act. Ü Includes ü 2, 400 Medi-Cal Working Disabled Program enrollees. 88% today are employed dual eligibles (November 2006) ü Medically Needy categories, special rules apply here. ü Home and community based waiver folks who are eligible for some services in a Medicaid state plan 33

Low Income Subsidy, or LIS Ü For those with limited income Ü For those with limited assets or resources Ü Medicare Part D LIS rules are based on SSI income and asset rules, not identical to all of them Ü POMS Citations, updated regularly HI 03000. 000: Eligibility for Subsidized Medicare Prescription Drug Coverage 34

LIS Application in English and Spanish: How to apply: Ü LIS Application via the Internet, www. socialsecurity. gov Ü Social Security Field Office application Ü LIS phone application with Social Security 1 -800 -772 -1213 Ü LIS paper application via the US Mail, scannable, do not photo copy Ü State Welfare or Medi-Cal Office will take application for the LIS 35

LIS Benefit Analysis, Frank Ü Is Frank on Medicare? YES Ü Is Frank on Medi-Cal? NO Ü Is Frank in a Medicare Savings Program, an MSP? NO Ü Does Frank have limited income? YES Ü Does Frank have limited assets? YES Ü Explain the LIS and assist with LIS if Frank chooses to apply. 36

LIS Benefit Analysis, Frank Ü Does Frank have all the information needed for the LIS? NO Consider using and mailing the paper application, the SSA-1020 form, Social Security will contact Frank. Ü Does Frank have all the information needed for the LIS? YES Consider the Internet Application Ü Is Frank working and not on Medi-Cal? YES Consider Medi-Cal Working Disabled Program. Explain Medi-Cal estate recovery rules if Frank is 55 and does not know about these Medi-Cal rules. 37

LIS Benefit Analysis, Frank Ü Is Frank on Medi-Cal using the Medically Needy category, with a Share of Cost (SOC)? YES Explain the special LIS rules for this situation and that he can be eligible for the LIS. Ü Is Frank married? Are they living together? YES SSI deeming rules apply, as in SSI or Medi-Cal. LIS information is checked against the data Social Security has on file for the spouse. Ü Frank’s exempt assets: The house he lives in, his car, $1, 500 in savings for burial 38

LIS Benefit Analysis, Frank Ü If Frank appears to be eligible for MSP or Medi-Cal, or both, explain the differences between applying for the LIS with Social Security, or with the local welfare or Medi. Cal offices. Social Security will not screen and enroll for MSP and Medi-Cal. CA welfare and Medi-Cal offices will screen and enroll for MSP and Medi-Cal. 39

Common Medi-Cal Categories Eligible for Low Income Subsidy (LIS) 40

Medi-Cal Working Disabled Program Eligible person: • • Can be working when applying for Medi-Cal Social Security disability rules apply Does not need to be on SSI or SSDI IHSS personal assistance services available: • • • In the program At the workplace Dual status rules apply with respect to Medicare Part D eligibility 41

Medi-Cal Working Disabled Program • • • Individual can earn $48, 870 in 2005 Affordable premiums, $20 - $175. 00 for a single person Any IRS approved retirement products, Individual Retirement Accounts are allowed, “IRAs” Disability income not counted See Medi-Cal on www. db 101. org or in 42 training manual

Medically Needy Medi-Cal, MN Common name: Share of Cost (SOC) Medi-Cal • Apply for Low Income Subsidy (LIS). Result: • In the first month the share of cost is met, the recipient is eligible for the LIS in the Group 2 levels of cost sharing. • Eligible for LIS for remainder of that calendar year. • See Medi-Cal on www. db 101. org and in training manual 43

Other Subsidy Eligible Folks Ü Medicare • • Savings Program Eligibles Qualified Medicare Beneficiary, QMB Specified Low Income Medicare Beneficiary, SLMB Qualified Individual, QI 1 Qualified Disabled Working Individual, QDWI, • QDWI must apply for subsidy 44

Subsidy Eligibles Ü Medicare Benefits Planning Tips ü Assess if a Medicare only beneficiary may be eligible for Medi Cal, or a Medicare Savings Program (MSP). ü If so, Medicare, and Medicare drug benefit may become more affordable. ØFile Subsidy application at CA Medi-Cal for processing, not at Social Security. ØCounties encouraged to take Medi-Cal and MSP applications ØSubsidy application filed with Social Security will not be screened for MSP or Medi-Cal eligibility. ØCA All County Welfare Directors Letter ACWDL 05 -23 (August 4, 2005)Medicare Part D Prescription Drug Program 45

Other Subsidy Eligibles Ü Duals living in institutions have no cost sharing or copays during those months. ÜSpecial rules apply for these plans and their participating pharmacies 46

Subsidy Help Groups • Group 1 • Full-benefit dual eligibles with incomes at or below 100% of the Federal Poverty Level (FPL), $9, 570 • Group 2 • Full-benefit dual eligibles above 100% of FPL, $9, 570 • Medicare Savings Programs eligibles or enrollees: QMB, SLMB, QI, or non-dual eligible beneficiaries with incomes below 135% FPL, $12, 920 and limited resources ($6, 000 per individual and $9, 000 for a married couple) • Group 3 • Medicare beneficiaries with incomes below 150% FPL, $14, 355 and limited resources ($10, 000 individual and $20, 000 married couple) (CMS March 2005) 47
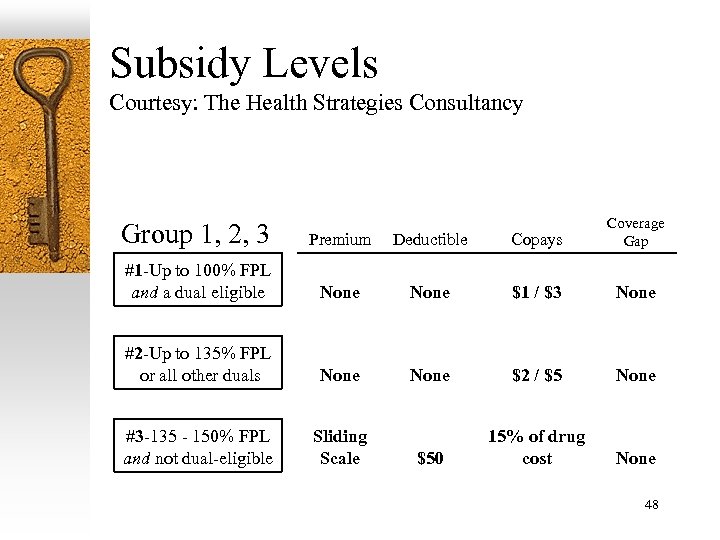
Subsidy Levels Courtesy: The Health Strategies Consultancy Group 1, 2, 3 Premium Deductible Copays Coverage Gap #1 -Up to 100% FPL and a dual eligible None $1 / $3 None #2 -Up to 135% FPL or all other duals None $2 / $5 None $50 15% of drug cost None #3 -135 - 150% FPL and not dual-eligible Sliding Scale 48
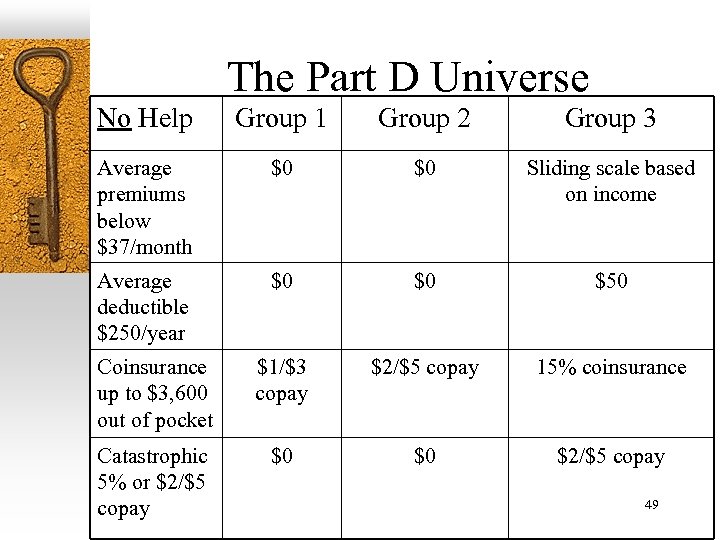
The Part D Universe No Help Group 1 Group 2 Group 3 Average premiums below $37/month $0 $0 Sliding scale based on income Average deductible $250/year $0 $0 $50 Coinsurance up to $3, 600 out of pocket $1/$3 copay $2/$5 copay 15% coinsurance Catastrophic 5% or $2/$5 copay $0 $0 $2/$5 copay 49

Lower Subsidies for Medicare Enrollees who are not Medi-Cal Eligible • Medicare only enrollees are eligible for a subsidy based on income levels • Individuals with income below 135% FPL and resources at or below $6, 000 ($9, 000 couple) receive full subsidy with $2/$5 co-pays, or Group 2 • Individuals with income below 150% FPL and resources at or below $10, 000 ($20, 000 couple), or Group 3: • Sliding scale premium • $50 deductible • 15% cost-sharing up to $3, 600 out-of-pocket limit (OOP) • $2/$5 co-pay after OOP limit is reached 50

Subsidy Eligibility Data Courtesy: ©The Health Strategies Consultancy The Federal Poverty Level, or “the FPL” 2005 - 100% of FPL: $9, 570 for one-person household, $12, 830 for two-person household; 135% of FPL: $12, 920, and $17, 321 respectively; 150% of FPL: $14, 355, and $19, 245 respectively Sliding scale premium defined for individuals between 135 -150% FPL • 135%-140% FPL, CMS will cover 75% of premium • 140%-145% FPL, CMS will cover 50% of premium • 145%-150% FPL, CMS will cover 25% of premium Subsidy Income and Resource Calculations generally based on SSI countable income and asset rules, with some changes. Note: Institutionalized dual eligibles pay NO cost-sharing. 51

Medicare Training 1. 2. 3. 4. Medicare Parts and Supplements New Prescription Drug Benefit 2006 Financial Subsidy for New Drug Plan Costs What’s in a Medicare Prescription Drug Plan? 52

2006 Prescription Drug Benefit Drug Plan Formularies Contain: 1. 2. Broad categories, for example, drugs for depression With classes of drugs in each category grouped according to chemical nature of the drugs, for example antineoplastics (cancer drugs) 53

2006 Prescription Drug Benefit Drug Plan Formularies • • • Must provide 2 drugs for each of 146 drug therapy categories. Brand name and generic drugs will be in each formulary (CMS 3/05). Provide prescription drugs, biologicals, insulin and medical supplies for injection of insulin Allowed to change drug formulary at any time with 60 days written notice to doctors, pharmacists and beneficiaries using that drug 54

2006 Prescription Drug Benefit Drug Plan Formularies • • • Cannot provide Barbiturates, Benzodiazepines, valium, xanax, non prescription drugs, or agents used for anorexia, weight loss, fertility, hair loss Cannot provide drugs available in Medicare Part A or Part B regardless of whether beneficiary has Part A or Part B. CMS will ensure formularies do not discourage enrollment among certain groups of people (CMS 3/05). The PDP not Medicare makes the determination of what is medically necessary. Formulary review requirements are posted on www. cms. hhs. gov/pdps 55

2006 Prescription Drug Benefit Drug Plan Formularies CMS Administrator Mark Mc. Clellan recently announced that there will be 6 categories of drugs for which all Part D plans must provide a: 1. Majority of antidepressants 2. Majority of antipsychotics 3. Majority of anticonvulsants 4. Majority of antiretrovirals 5. Majority of immunosuppressants 6. Majority of antineoplastics (cancer drugs) If a Part D plan does not cover “all or substantially all” of the drugs in each class, the plan must provide justification to CMS why not. 56

Plans can have tiered formularies Preferred Drug Levels • • Tier 1 has the lowest cost sharing. Subsequent tiers have higher cost sharing in ascending order. CMS will review to identify drug categories that may discourage enrollment of certain people with Medicare by placing drugs in non-preferred tiers Plan must have procedures so beneficiaries can request exceptions for tiered formularies (CMS March 2005) 57

Drug Transition Planning – Plan “Requirements” 423. 120 (b)(3)) CMS MMA regulation Prescription Drug Plans are required to have an approved drug "transition process" for new enrollees. http: //www. cms. hhs. gov/medicarereform/issuepapers/title 1 and 2/ ü Expected to have procedures for medical review of non-formulary drug requests by the beneficiary 58

2006 Prescription Drug Benefit CA Dual Eligible LIS covered Drug Plans Stand-Alone Drug Plans Ü 10 PDPs approved statewide with LIS coverage (CMS as of 10/10/05) Medicare Advantage Drug Plans ÜMA-PDs approved and with LIS coverage are listed county by county Keep Checking www. Medicare. gov þ þ Landscape of Local Plans 1 -800 -MEDICARE will mail detailed responses to caller inquiries 59

Drug Transition Planning Requirements 423. 120 (b)(3)) CMS MMA regulation Special Enrollment Period Allows a full-benefit dual eligible individual to change PD plans to better accommodate his/her pharmaceutical needs and pharmacy affiliations at any time because of a Special Enrollment Period afforded to them. (SEP) Special Enrollment Period allows full benefit dual eligibles to switch from one MA-PD plan to another, from one PD plan to another, or from original Medicare and a PD plan into an MA-PD plan and vice versa. Special Enrollment Period extends beyond December 31 st indefinitely. There is no known termination date for duals eligible for the SEP. 60

Medicare Training 1. 2. 3. 4. 5. 6. Medicare Today, Parts and Supplements Temporary Prescription Drug Discount Card New Prescription Drug Benefit 2006 Financial Subsidy for New Drug Plan Costs What’s in a Medicare Prescription Drug Plan? Special Needs Plans 61

Special Needs Plans - SNPs • SNPs by design cover all services for SNP enrolled beneficiaries • SNPs running now or soon: • Evercare • Cal Optima One. Care, Orange County: 55, 000 Orange County duals would be eligible to enroll. 62

Cal Optima One. Care Discussion A single system responsible for providing access to a full continuum of services • • Primary and specialty physician care Acute inpatient care Prescription drugs Medical supplies and equipment Home and community based care (future) Long-term care Coordinate care and help members get the services they need 63

Medicare Training 3. Medicare Parts and Supplements New Prescription Drug Benefit 2006 Financial Subsidy for New Drug Plan Costs 4. What’s in a Medicare Prescription Drug Plan? 5. Special Needs Plans Beneficiary Protections, Appeals and Exceptions in New Drug Plans 1. 2. 64

Plan Information Dissemination • Plans must provide information about • • • Service areas Benefits Cost sharing Formulary Pharmacy access Other aspects of coverage available through the plan 65

Exceptions Process • • Ensures access to medically necessary Medicare covered prescription drugs Provides process for enrollee to • Obtain a covered Medicare prescription drug at a more favorable cost-sharing level • Obtain a covered Medicare prescription drug not on the formulary 66

Protections and Appeal Process • • ALL beneficiaries protected by the same process, no population receives special or different formulary access Some protections: • CMS oversight of formularies to prevent discrimination to Medicare sub-populations • PDP drug transition process 67

A Coverage Determination The Appeals and Exceptions Process 5 steps for an exception or an appeal to a PDP Appeal rights are provided to beneficiaries by all PDPs. ü ü The beneficiary, not others, appeals or files an exception to the plan, not to the pharmacy. A Coverage Determination comes from the PDP or MAPDP to the beneficiary. Beneficiary files a Redetermination request of an unfavorable Coverage Determination to the PDP using this process. A Redetermination is performed by the PDP. If a negative result: 1. Beneficiary files a Request for Reconsideration to an Independent Review Entity, IRE, a CMS contractor. IRE decisions based on and have capacity for medical appropriateness. Unfavorable PDP Redeterminations above are not auto referred to an IRE. 2. Further appeal allowable to an Administrative Law Judge (ALJ) 3. Further appeal allowable to the Medicare Appeals Council (MAC), and finally to 4. Federal Court Process builds on the current Medicare Part C (MA) Appeals Process 68

Coverage Determination and the Appeals www. medicareadvocacy. org Appeals Process Resource Expedited Review (faster) is available when and if Medicare Part C (MA) due process standards are in place and being met. Continued drug coverage pending an appeal (as in current Medi-Cal protections) is not included. Pharmacy is allowed to not fill a prescription if beneficiary does not have the copay, but is also allowed to waive the copay. 69
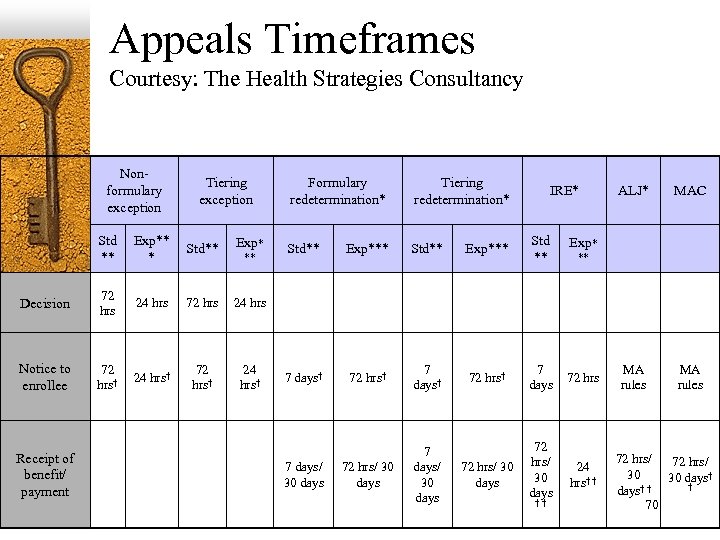
Appeals Timeframes Courtesy: The Health Strategies Consultancy Nonformulary exception Tiering exception Std ** Exp** * Std** Decision 72 hrs 24 hrs 72 hrs† 24 hrs† Tiering redetermination* Std** Exp*** Std ** 7 days† 72 hrs† 7 days 72 hrs/ 30 days 7 days/ 30 days 72 72 hrs/ 30 days IRE* ALJ* MAC 72 hrs MA rules 24 hrs† † 72 hrs/ 30 days† 24 hrs Notice to enrollee Formulary redetermination* Receipt of benefit/ payment Exp* ** 7 days/ 30 days † † Exp* ** 70 †

Due Process PDPs are required to send written Notice of a formulary change or cost sharing change at least 60 days in advance of the changes to those enrolled using that drug; and, The Notice must be sent to CMS, SPAPs, pharmacies and prescribing providers. http: //www. cms. hhs. gov/medicarereform/issuepapers/title 1 and 2/ - Issue Paper #33 71

Medicare Training 1. 2. 3. 4. 5. 6. 7. Medicare Parts and Supplements New Prescription Drug Benefit 2006 Financial Subsidy for New Drug Plan Costs What’s in a Medicare Prescription Drug Plan? Special Needs Plans Beneficiary Protections and Appeals State of California Involvement 72

Medi-Cal, Dept. of Health Services • Medi-Cal “wrap-around” coverage to Part D • CA new budget contains $94 million for current Medi. Cal drugs not available in Medicare Part D and which will continue to receive federal match funds • No CA funds available for Part D covered drugs, co-pay assistance, or premium assistance for higher cost plans. • CA is required to help CMS identify duals. • State is required to take subsidy applications, along with Social Security, the lead agency for subsidy applications for those who must apply for a subsidy • Those who are not already deemed and/or notified by CMS. 73

Medicare Training 1. 2. 3. 4. 5. 6. 7. 8. Medicare Today, Parts and Supplements New Prescription Drug Benefit 2006 Financial Subsidy for New Drug Plan Costs What’s in a Medicare Prescription Drug Plan? Special Needs Plans Beneficiary Protections and Appeals State of California Involvement Resources, Citations and References 74

www. Medicare. gov þ þ Landscape of Local Plans Compare Medicare Prescription Drug Plans Formulary Finder Medicare & You 2007 75

Resources For individual counseling and assistance HICAP: Health Insurance Counseling and Advocacy Program Statewide program, state and federally funded counseling Call 1 -800 -434 -0222 for individual appointments For technical information and assistance California Health Advocates 916 -231 -5110 (Sacramento office) Medicare fact sheets, updated information for CA www. cahealthadvocates. org and www. calmedicare. org California Benefits Planners www. db 101. org working with a disability in California 76

Resources Center for Medicare and Medicaid Services, CMS www. medicare. gov 1 -800 -MEDICARE, TTY 1 -877 -486 -2048 www. cms. hhs. gov/medicarereform/ Center for Medicare Advocacy, Inc. www. medicareadvocacy. org Kaiser Family Foundation www. kff. org Families USA http: //www. familiesusa. org/site/Page. Server? pagen ame=Medicare_Drug_Law_Materials 77

Citations and Legal References • Medicare Part D Statute and Regulation(s) • • • 42 USC § 1395, Tit. XVIII. 70 Fed. Reg. 4194 (January 28, 2005). 42 CFR Parts 400, 403, 411, 417 and 423. www. cms. gov Low Income Subsidy • 70 Fed Reg 10558 (March 4, 2005). • 20 CFR Part 418. • POMS Section HI 03001. 000 et seq • Dept. of Health Services Index: All County Welfare Director Letters: • http: //www. dhs. ca. gov/mcs/mcpd/MEB/ACLs/ © Copyright 2006 by World Institute on Disability, permission to copy will be granted to non profit entities with appropriate acknowledgement of credit. 78
ad9395c647ea6f1c116a7cd264824d2b.ppt