ddd465ee10ea98aebddfaa7e5a8186b2.ppt
- Количество слайдов: 32

Wii-Fit for Activity, Balance and Gait in Assisted Living Kalpana P. Padala, MD, MS Research Geriatrician, Assistant Professor Department of Family Medicine University of Nebraska Medical Center Omaha, NE

Faculty Disclosures: The presenter’s have disclosed that they have no relevant financial relationship(s).

Funding source • 2009 AMDA foundation / Pfizer Quality Improvement Award

Learning Objectives: By the end of the session, participants will be able to: • Objective 1: Appreciate the impact of balance and gait problems in AD • Objective 2: Recognize barriers to exercise in this population • Objective 3: Evaluate the feasibility of Wii-Fit to improve balance and gait in AD

Falls in AD • Three fold higher in AD compared to cognitively intact older adults • Impact – rate of injuries and fractures – rate of institutionalization – Older adults who wander and fall their life span by more than 3 years

Gait in AD • Shortened step length • double support time • stride length variability - proven risk factor falls in AD • gait speed

Importance of Exercise & Barriers • Exercise is known to improve gait and balance in elderly • Barriers to Exercise: – Difficulty in engaging subjects – Lack of motivation – Cost – Transportation issues – Availability of coach or physical therapist – Lack of facilities in rural areas

Wii-Fit • A Nintendo gaming console • Includes a balance board that senses weight, movement and balance • Virtual trainers talk the user through the activity while tracking progress • Exercise Components – Yoga – Strength training – Aerobics – Balance games

Wii- Fit Component

* Creating Mii * Calculating BMI and Wii-Fit Age

* Yoga * Strength Training

Aerobics
Balance Games

Balance Games

Specific Aims • To compare the effect of the Wii-Fit program to a walking program, on measures of balance, in subjects with mild AD residing in an assisted living facility • To compare the effect of the Wii-Fit program to a walking program, on measures of activity, gait, and quality of life in the same population

Methods • Study design: – 8 -week prospective randomized parallel-group study
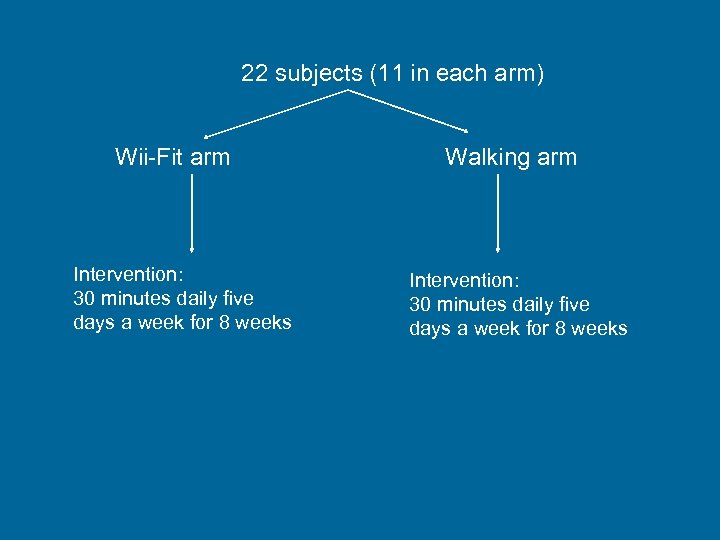
22 subjects (11 in each arm) Wii-Fit arm Intervention: 30 minutes daily five days a week for 8 weeks Walking arm Intervention: 30 minutes daily five days a week for 8 weeks
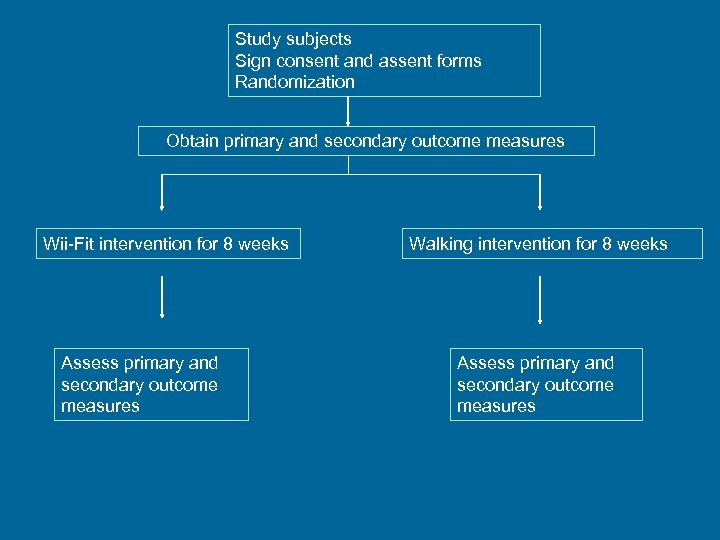
Study subjects Sign consent and assent forms Randomization Obtain primary and secondary outcome measures Wii-Fit intervention for 8 weeks Assess primary and secondary outcome measures Walking intervention for 8 weeks Assess primary and secondary outcome measures

Primary Outcome Measures • Berg Balance Scale (BBS) – 14 subsets of tasks performed in a standard order – Each task is scored on a five-point scale (0 -4) – The maximum score for this assessment is 56 – A score of < 45 is predictive of falls – Good inter-rater reliability of 0. 98

Secondary Outcome Measures • • Timed Up and Go (TUG) Tinetti’s Test Activities of daily living (ADL) Instrumental Activities of daily Living (IADL) Quality Of Life-AD (QOL-AD) Mini Mental State Exam (MMSE) Executive Function tests (Trails A & B and Exit -25) • Apathy Evaluation Scale (AES) • Actigraphs (advanced pedometers - measure physical function)
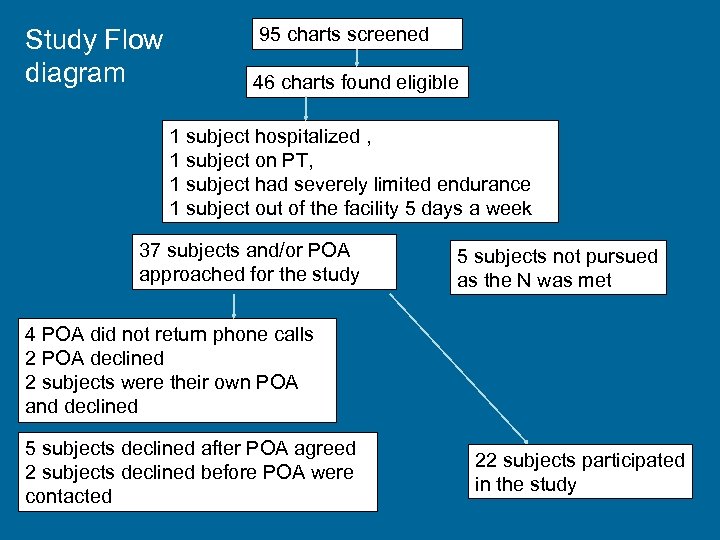
Study Flow diagram 95 charts screened 46 charts found eligible 1 subject hospitalized , 1 subject on PT, 1 subject had severely limited endurance 1 subject out of the facility 5 days a week 37 subjects and/or POA approached for the study 5 subjects not pursued as the N was met 4 POA did not return phone calls 2 POA declined 2 subjects were their own POA and declined 5 subjects declined after POA agreed 2 subjects declined before POA were contacted 22 subjects participated in the study

Results • 22 subjects enrolled, 11 in each arm • One subject in each arm did not complete the study • The subject in Wii-Fit arm did not want to continue after completing 4 weeks • The subject from Walking arm was discharged to his home after 4 weeks • Data was analyzed with intent to treat analysis • RM-ANOVA was used to analyze the continuous variables

Demographics & baseline variables • • • Mean age: 80. 4 (± 7. 8) years Gender: 8 females in each group Race: All subjects were Caucasians Mean BMI: 25. 4 (± 4. 05) kg/m 2 Mean Years of education: 13. 9 (± 2. 1) years No baseline differences among the two groups with regards to demographics, primary and secondary outcome variables

Results • There was a significant improvement in BBS across the entire study subjects (p<0. 001) • There was also significant improvement in TUG (p=0. 036) and Tinetti’s (p<0. 001)
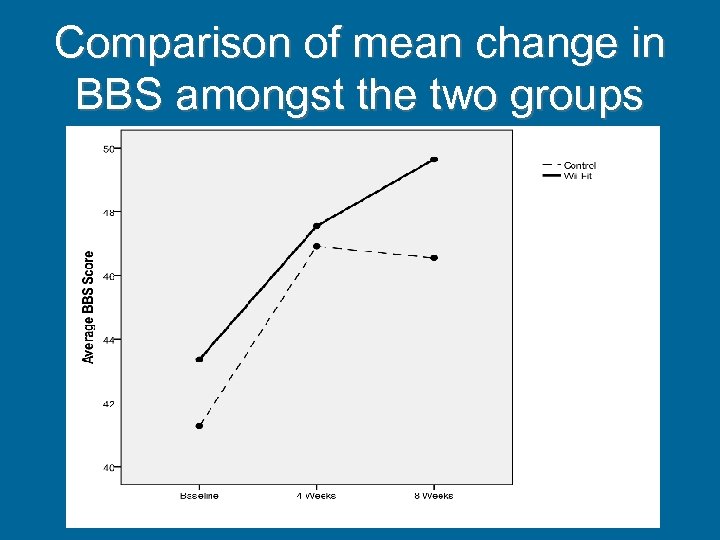
Comparison of mean change in BBS amongst the two groups

Results (contd) • There was significant improvement in the balance and gait in both groups but within group differences were not statistically significant • There was no significant improvement in the ADL, IADL, QOL, MMSE in both groups and within group differences were not statistically significant

Conclusion • Both Wii-Fit and walking are feasible in an Assisted living facility • Balance and Gait improved significantly with both interventions • Both groups had good adherence

Limitations • Conducted in an Assisted living, so not generalizeable to community dwellers • Small sample size • Study intervention was investigator driven than patient’s self motivation • The study intervention was not aimed towards the primary outcome variable

Acknowledgements • • William J. Burke, MD: Primary Mentor Timothy Malloy, MD, CMD: Medical Director Sarah Frost, PT, Physical Therapist Jenenne Geske, Ph. D: Statistician Marie Bissell, BSN, RN: Graduate assistant Penny Schweitzer, RN, Administrator Chris Stungis’, RN, QMA/Director of Health care Services • Facility: Parson’s House on Eagle Run

Questions

Inclusion criteria • • Age ≥ 60 Alzheimer’s Dementia, mild(MMSE ≥ 18) Residing in assisted living facility Presence of legal surrogate

Exclusion criteria • History of myocardial infarction, TIA or stroke in last 6 months • Presence of serious mental illness impacting memory • Active cancer except skin cancer • Medical conditions likely to compromise survival (e. g. severe CHF) • Severe sensory and musculoskeletal impairments • Using wheel-chair
ddd465ee10ea98aebddfaa7e5a8186b2.ppt