7445d871ae401254428ebe6f2435762c.ppt
- Количество слайдов: 40

WHO – Lausanne University Seminar on Non Communicable Diseases Geneva, 7 January 2010 Multisectoral action to improve nutrition throughout the life course for the prevention of NCD F. Branca Director, Department of Nutrition for Health and Development WHO

The multifaceted challenge of malnutrition Malnutrition should be dealt in all its forms (underweight, wasting, stunting and overweight, as well as micronutrient deficiencies and nutrition-related chronic diseases)
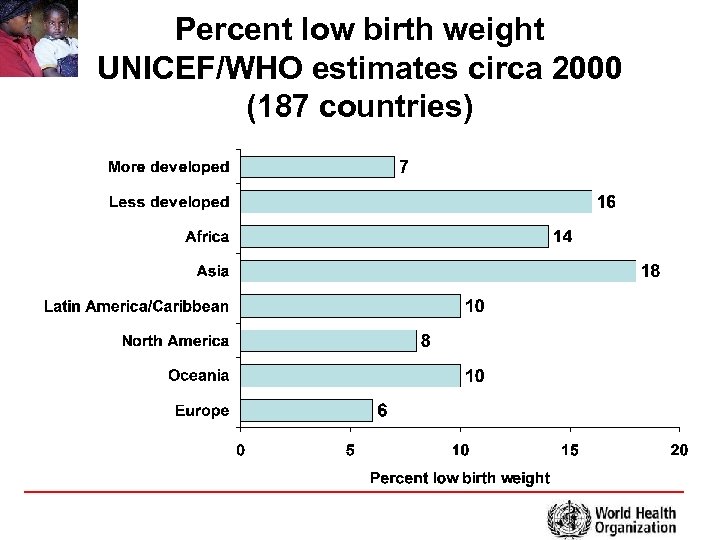
Percent low birth weight UNICEF/WHO estimates circa 2000 (187 countries)

178 million children under 5 are stunted Prevalence of Stunting

293 million children under 5 are anemic Category of public health significance (anaemia prevalence) Normal (<5. 0%) Mild (5. 0 -19. 9%) Moderate (20. 0 -39. 9%) Severe (≥ 40. 0%) No Data Source: WHO Global database on Anaemia, 2006

Over 500 million adults are obese

The double burden of malnutrition Source: WHO Global Database on Child Growth and Malnutrition
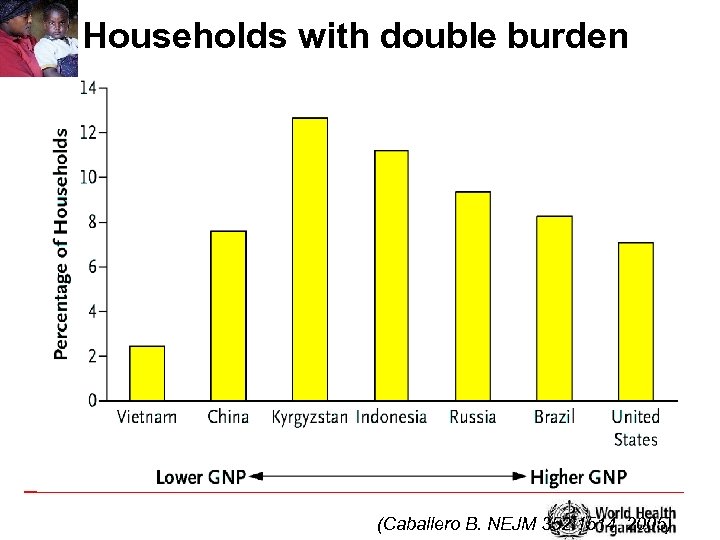
Households with double burden (Caballero B. NEJM 352: 1514 2005)

Nutritional influences throughout the life course
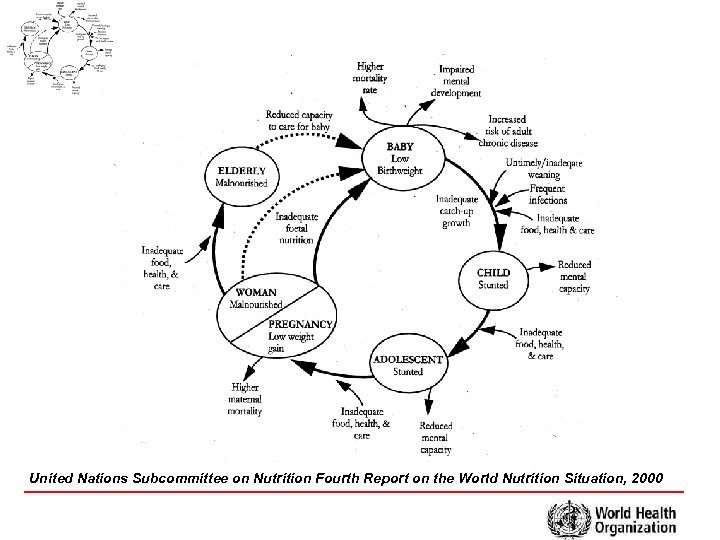
United Nations Subcommittee on Nutrition Fourth Report on the World Nutrition Situation, 2000
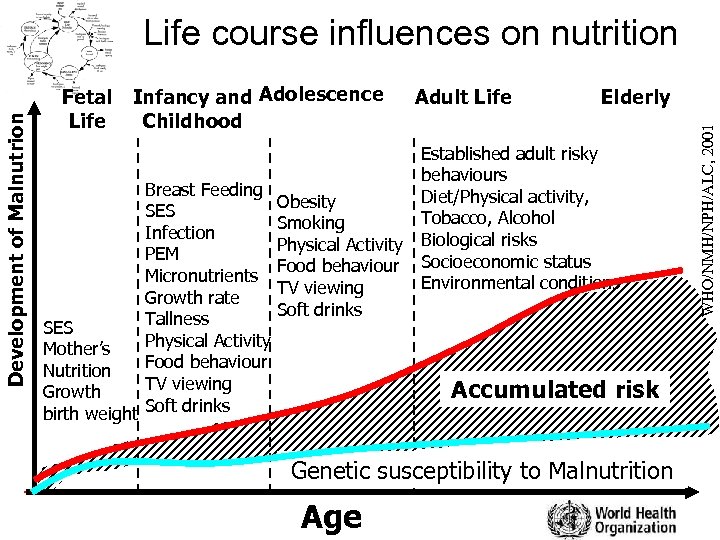
Fetal Life Infancy and Adolescence Childhood Breast Feeding SES Infection PEM Micronutrients Growth rate Tallness SES Physical Activity Mother’s Food behaviour Nutrition TV viewing Growth birth weight Soft drinks Obesity Smoking Physical Activity Food behaviour TV viewing Soft drinks Adult Life Elderly Established adult risky behaviours Diet/Physical activity, Tobacco, Alcohol Biological risks Socioeconomic status Environmental conditions Accumulated risk Genetic susceptibility to Malnutrition Age WHO/NMH/NPH/ALC, 2001 Development of Malnutrion Life course influences on nutrition
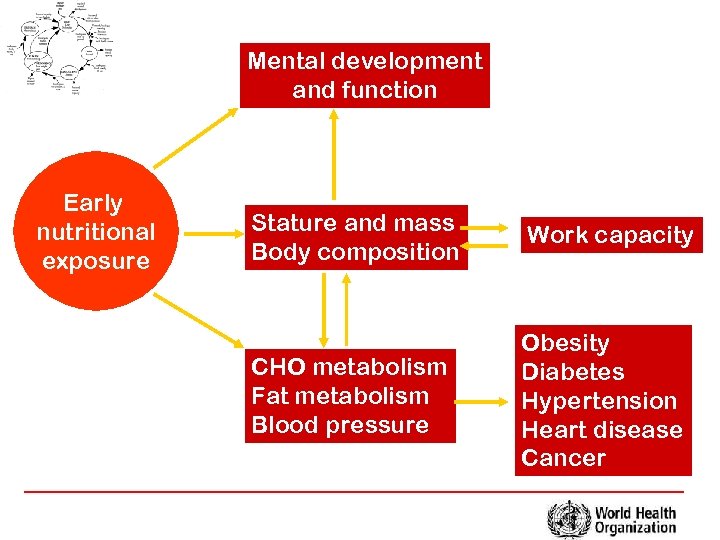
Mental development and function Early nutritional exposure Stature and mass Body composition Work capacity CHO metabolism Fat metabolism Blood pressure Obesity Diabetes Hypertension Heart disease Cancer
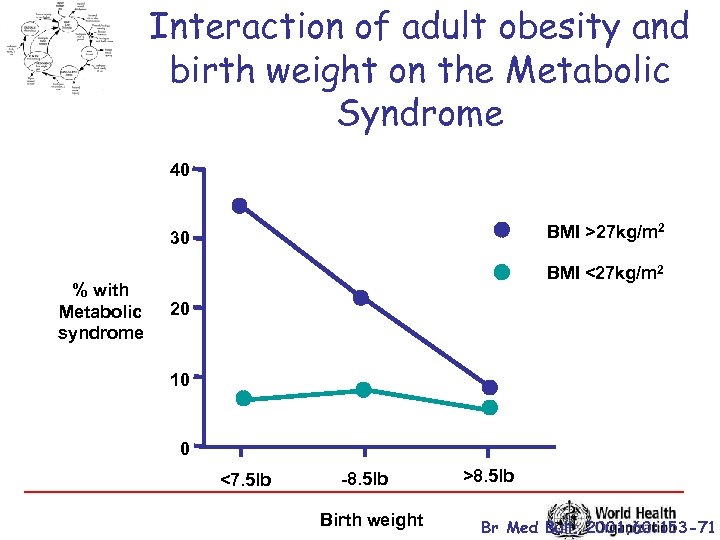
Interaction of adult obesity and birth weight on the Metabolic Syndrome 40 BMI >27 kg/m 2 30 % with Metabolic syndrome BMI <27 kg/m 2 20 10 0 <7. 5 lb -8. 5 lb Birth weight >8. 5 lb Br Med Bull. 2001; 60: 153 -71

Maternal obesity in Early Pregnancy and Obesity in the Offspring Odds Ratio (95% CI) Childhood obesity 2. 3 (2. 0 -2. 6) at 4 yrs of age (Whitaker 2004)
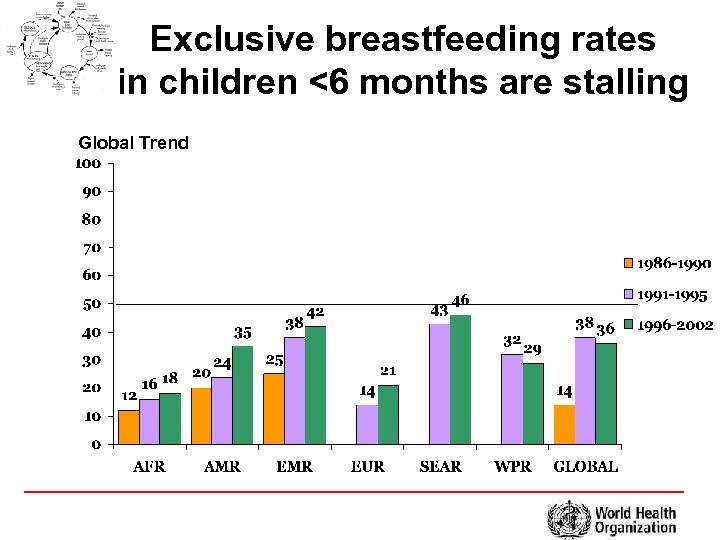
Exclusive breastfeeding rates in children <6 months are stalling Global Trend
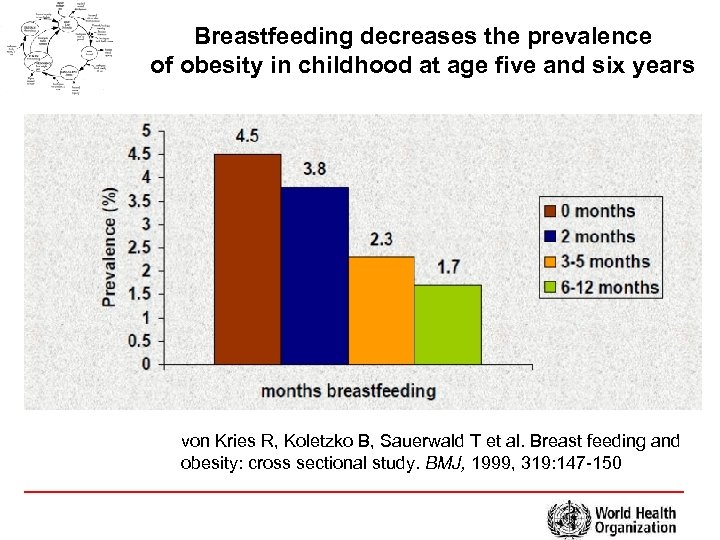
Breastfeeding decreases the prevalence of obesity in childhood at age five and six years von Kries R, Koletzko B, Sauerwald T et al. Breast feeding and obesity: cross sectional study. BMJ, 1999, 319: 147 -150
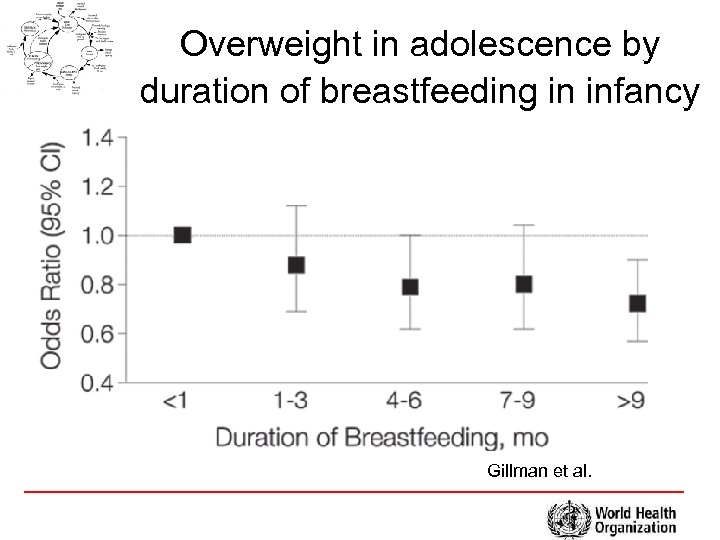
Overweight in adolescence by duration of breastfeeding in infancy Gillman et al.
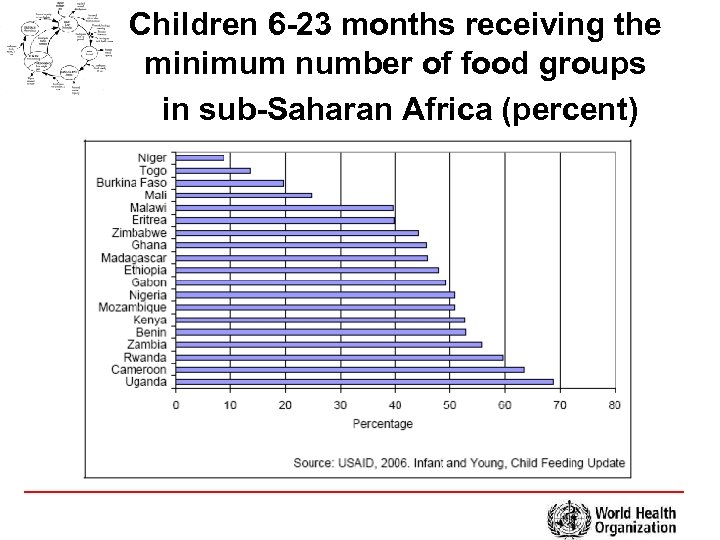
Children 6 -23 months receiving the minimum number of food groups in sub-Saharan Africa (percent)

Complementary feeding and obesity • size at birth and childhood growth in height, weight and BMI • Greater consumption of protein in earlier life has been suggested to predispose people to later adiposity ?
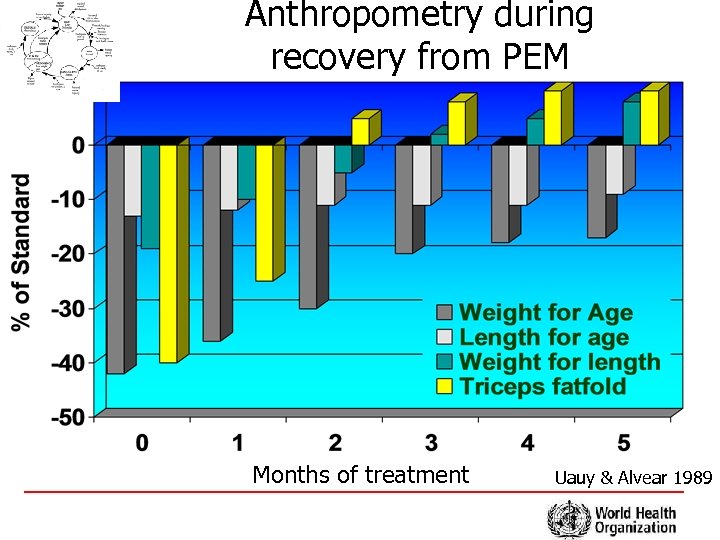
Anthropometry during recovery from PEM Months of treatment Uauy & Alvear 1989

The interventions

Integrated food and nutrition action • • Inadequate foetal development Lack of breastfeeding Inappropriate complementary feeding Child under nutrition • • Low fruit and vegetable intake High salt (Na. Cl) intake Saturated fat and trans fatty acid intake High blood pressure High cholesterol Overweight and obesity Physical inactivity

Effective actions to improve fetal development ? Strength of evidence Strong Some Limited ↓ Adolescent pregnancies ↓ Occupational hazards Social support Improved nutrition in girls and women Safe water and sanitation Self-esteem ↓ Infectious and other diseases Pregnancy complications Sleep duration ↓ Life style risk factors (smoking, alcohol, workload) ↓ Environmental toxins Number of partners/duration of cohabitation Other nutritional factors Protection including food supplementation of pregnant women in humanitarian crisis

Evidence based maternal nutrition interventions All Countries Specific Situational Contexts • Iron folate supplementation • Maternal supplements of multiple micronutrients • Maternal iodine through iodization of salt • Maternal calcium supplementation • Interventions to reduce tobacco consumption or indoor air pollution • Maternal supplements of balanced energy and protein • Maternal iodine supplements • Maternal deworming in pregnancy • Intermittent preventative treatment for malaria • Insecticide-treated bednets

Infant and Young Child Feeding • Protection, promotion and support of appropriate IYCF – Exclusive breast feeding for 6 months – Complementary feeding (need strengthening and support for use of local foods, food fortification, micronutrient supplementation) – Feeding of IYC in difficult circumstances (HIV, malnutrition, emergencies, LBW) • Health services – Baby Friendly Hospital Initiative – Pre-service education and in-service training • • • Maternity protection Code of marketing of breastmilk substitutes Monitoring and evaluation

The European Food And Nutrition Action Plan HEALTH CHALLENGES Diet related noncommunicable diseases Obesity in children and adolescents Micronutrient deficiencies Foodborne diseases ACTION AREAS 1. Supporting a healthy start 2. Ensuring safe, healthy and sustainable food supply 3. Providing comprehensive information and education to consumers 4. Implementing integrated actions 5. Strengthening nutrition and food safety in the health sector 6. Monitoring and evaluation

Action area 1 Supporting a healthy start 1. Promote maternal nutrition and safe dietary habits 2. Protect, promote and support breastfeeding and timely, adequate and safe complementary feeding of infants and young children 3. Promote the development of school and pre-school nutrition and food safety policies

Action area 2 Ensuring safe, healthy and sustainable food supply 1. Improve the availability of fruit and vegetables 2. Promote the reformulation of mainstream food products 3. Improve food supply and food safety in public institutions 4. Explore the use of economic tools (taxes, subsidies)

Action area 2 Ensuring safe, healthy and sustainable food supply 5. 6. 7. Ensure that the commercial offer of food products is aligned to food-based dietary guidelines Establish targeted programmes for the protection of vulnerable groups Establish intersectoral food safety systems with a farm to fork approach

Action area 3 Providing comprehensive information and education to consumers 1. Food-based dietary guidelines and food safety guidelines, complemented by physical activity guidelines 2. Public campaigns aimed at informing consumers 3. Appropriate marketing practices 4. Adequate labelling of food products

Action area 4 Integrated actions to address related determinants 1. Increase opportunities to perform physical activity 2. Reduce the consumption of alcohol 3. Ensure the provision of safe drinking water 4. Reduce environmental contamination of the food chain

Action area 5 Strengthening nutrition and food safety in the health sector 1. 2. 3. Engage primary care staff in nutrition assessment and in the provision of diet, food safety and physical activity counselling Improve the standards of service delivery for the prevention, diagnosis and treatment of nutrition related diseases Improve the quality of nutrition services and food safety in hospitals

Action area 6 Monitoring and evaluation 1. 2. 3. 4. Establish national and international surveillance systems on nutritional status and food consumption Establish monitoring and surveillance systems for microbial and chemical hazards in the food chain and foodborne diseases Evaluate the impact of programmes and policies Improve public and private research establishments

Why little progress? • Inadequate investments • Inadequate coordination among players • Inadequate coverage • Inadequate responses • Life course not addressed • Social determinants not considered
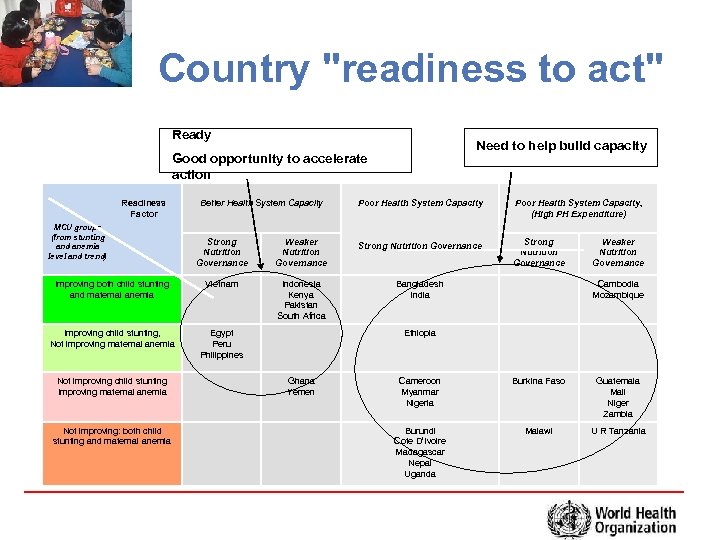
Country "readiness to act" Ready Need to help build capacity Good opportunity to accelerate action Readiness Factor MCU groups (from stunting and anemia level and trend) Better Health System Capacity Poor Health System Capacity, (High PH Expenditure) Strong Nutrition Governance Weaker Nutrition Governance Strong Nutrition Governance Improving both child stunting and maternal anemia Vietnam Indonesia Kenya Pakistan South Africa Bangladesh India Improving child stunting, Not improving maternal anemia Egypt Peru Philippines Not improving child stunting Improving maternal anemia Not improving: both child stunting and maternal anemia Weaker Nutrition Governance Cambodia Mozambique Ethiopia Ghana Yemen Cameroon Myanmar Nigeria Burkina Faso Guatemala Mali Niger Zambia Burundi Cote D’Ivoire Madagascar Nepal Uganda Malawi U R Tanzania

Country level support in nutrition THE FUNCTIONS ♦ ♦ ♦ Analysing the needs : nutrition surveillance Analysing the responses and the capacities : policy analysis Supporting the development of integrated food and nutrition policies Strengthening the delivery of essential nutrition actions through the health system Guidance on programme design and implementation Assisting in emergency responses THE PROGRAMMES ♥ Landscape analysis ♥ Growth standards ♥ Micronutrients supplements in antenatal care and in child care ♥ Micronutrient fortification of staple food ♥ Nutritional support of people living with HIV and TB ♥ Integrated treatment of malnutrition ♥ Promotion of breastfeeding, safe and adequate complementary feeding

Scaling up on WHO strategic priorities WHO has a major responsibility for promoting healthy nutrition for all the world's people, through collaborative support to Member States, particularly in their national nutrition programmes, in partnership with other intergovernmental and nongovernmental organizations, and their related sectoral approaches. 1. Development and operationalization of integrated food and nutrition policies 2. Intelligence of needs and response 3. Development of evidence based programme guidance 4. Country-level advocacy and technical assistance
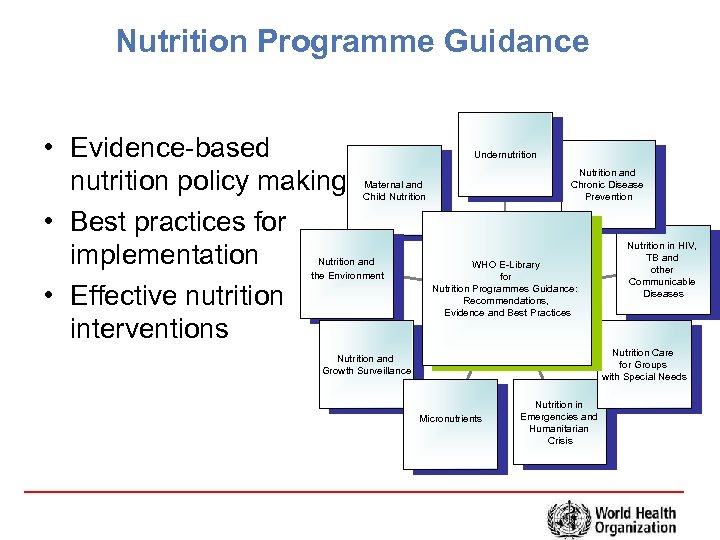
Nutrition Programme Guidance • Evidence-based nutrition policy making • Best practices for implementation • Effective nutrition interventions Undernutrition Nutrition and Chronic Disease Prevention Maternal and Child Nutrition and the Environment WHO E-Library for Nutrition Programmes Guidance: Recommendations, Evidence and Best Practices Nutrition in HIV, TB and other Communicable Diseases Nutrition Care for Groups with Special Needs Nutrition and Growth Surveillance Micronutrients Nutrition in Emergencies and Humanitarian Crisis
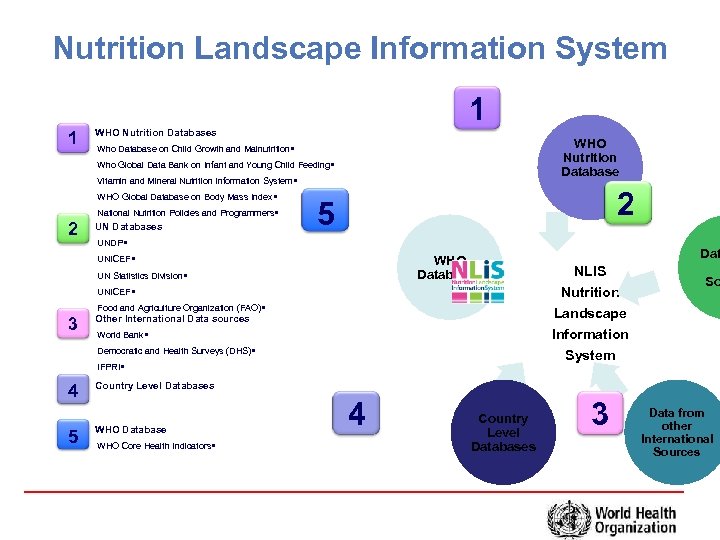
Nutrition Landscape Information System 1 1 WHO Nutrition Databases WHO Nutrition Database Who Database on Child Growth and Malnutrition§ Who Global Data Bank on Infant and Young Child Feeding§ Vitamin and Mineral Nutrition Information System§ WHO Global Database on Body Mass Index§ National Nutrition Policies and Programmers§ 2 UN Databases 2 5 UNDP§ WHO Databases UNICEF§ UN Statistics Division§ Food and Agriculture Organization (FAO)§ World Bank§ IFPRI§ 5 So Landscape Information System Other International Data sources Democratic and Health Surveys (DHS)§ 4 NLIS Nutrition UNICEF§ 3 Dat Country Level Databases WHO Database WHO Core Health Indicators§ 4 Country Level Databases 3 Data from other International Sources

http: //www. who. int/nutrition/en/index. html
7445d871ae401254428ebe6f2435762c.ppt