9761f455360b30e5b9e53889360b4cd6.ppt
- Количество слайдов: 52
 Whack a Mole and Other Approaches to Health Care Cost Containment Merton D. Finkler, Ph. D Lawrence University
Whack a Mole and Other Approaches to Health Care Cost Containment Merton D. Finkler, Ph. D Lawrence University
 The Agenda l l A Brief History of Health Care Cost Containment Efforts Strategies That Don’t Work Three Potentially Successful Strategies Guidelines for Selecting the Right Cost Containment Strategy
The Agenda l l A Brief History of Health Care Cost Containment Efforts Strategies That Don’t Work Three Potentially Successful Strategies Guidelines for Selecting the Right Cost Containment Strategy
 Whack a Mole Game
Whack a Mole Game
 Points to Remember l l l Component-based cost containment is temporary. The burden of health care cost falls mostly on labor. Value-based purchasing requires leaping many barriers. All sustainable strategies involve sacrifice. Each organization needs to find the tradeoff that best matches its mission.
Points to Remember l l l Component-based cost containment is temporary. The burden of health care cost falls mostly on labor. Value-based purchasing requires leaping many barriers. All sustainable strategies involve sacrifice. Each organization needs to find the tradeoff that best matches its mission.
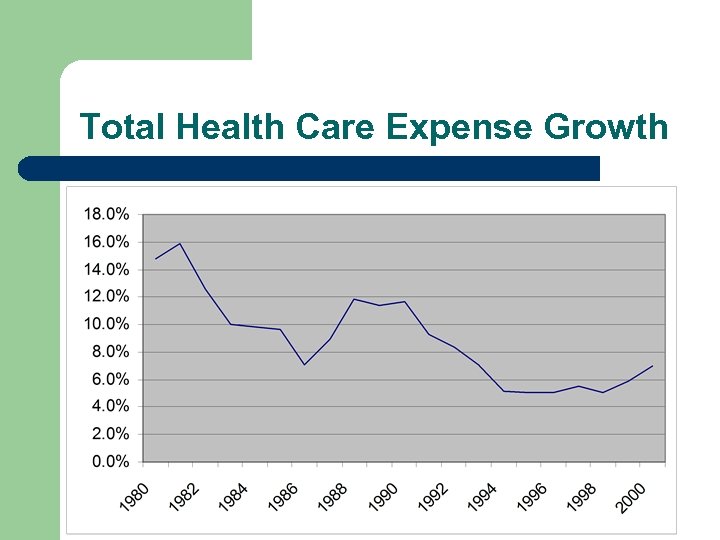 Total Health Care Expense Growth
Total Health Care Expense Growth
 Cost Containment 1980 to the Present l l Health care expenditures increased at double digit rates in the early and late eighties Health care expenditures are again approaching double digit rates Insurance premiums have featured double-digit growth for the past two years. Each health care service component has had its turn at leading the rise in costs
Cost Containment 1980 to the Present l l Health care expenditures increased at double digit rates in the early and late eighties Health care expenditures are again approaching double digit rates Insurance premiums have featured double-digit growth for the past two years. Each health care service component has had its turn at leading the rise in costs
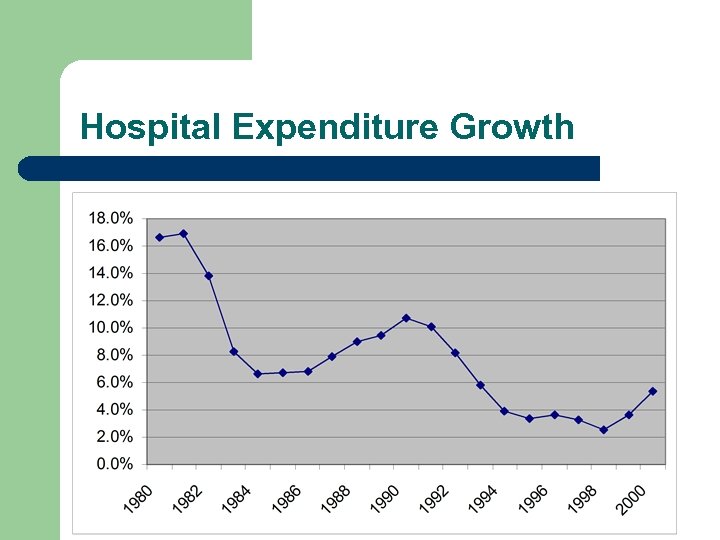 Hospital Expenditure Growth
Hospital Expenditure Growth
 Hospital Cost l l l l 14% or greater expenditure growth in 1980 -82 DRGs led to stabilized expenditure growth. Movement to outpatient services, ambulatory surgery, and clinics since the mid 1980 s Early 1980 s, 80% of all surgeries was inpatient hospital event and 20% outpatient or ambulatory surgery center Now close to reversed Hospital costs share declined from 42% of total to 32%. Yet spending on hospital services accounted for over 50% of health care expenditure growth in 2001. Hospitals continue to build.
Hospital Cost l l l l 14% or greater expenditure growth in 1980 -82 DRGs led to stabilized expenditure growth. Movement to outpatient services, ambulatory surgery, and clinics since the mid 1980 s Early 1980 s, 80% of all surgeries was inpatient hospital event and 20% outpatient or ambulatory surgery center Now close to reversed Hospital costs share declined from 42% of total to 32%. Yet spending on hospital services accounted for over 50% of health care expenditure growth in 2001. Hospitals continue to build.
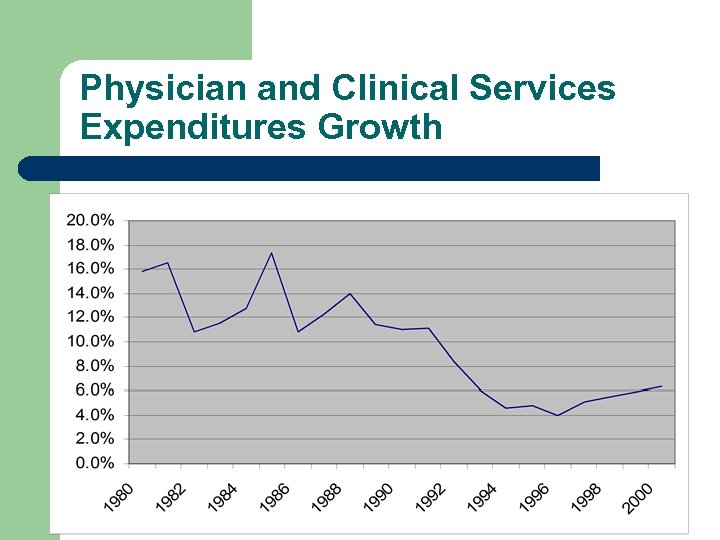 Physician and Clinical Services Expenditures Growth
Physician and Clinical Services Expenditures Growth
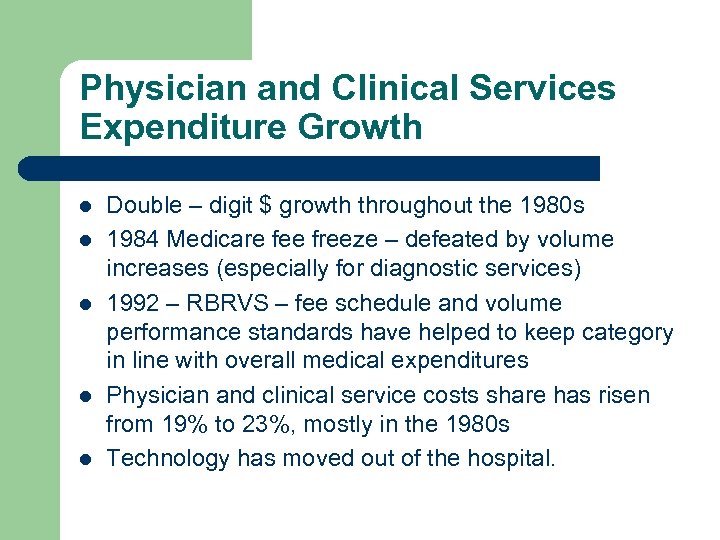 Physician and Clinical Services Expenditure Growth l l l Double – digit $ growth throughout the 1980 s 1984 Medicare fee freeze – defeated by volume increases (especially for diagnostic services) 1992 – RBRVS – fee schedule and volume performance standards have helped to keep category in line with overall medical expenditures Physician and clinical service costs share has risen from 19% to 23%, mostly in the 1980 s Technology has moved out of the hospital.
Physician and Clinical Services Expenditure Growth l l l Double – digit $ growth throughout the 1980 s 1984 Medicare fee freeze – defeated by volume increases (especially for diagnostic services) 1992 – RBRVS – fee schedule and volume performance standards have helped to keep category in line with overall medical expenditures Physician and clinical service costs share has risen from 19% to 23%, mostly in the 1980 s Technology has moved out of the hospital.
 Insurance and Administrative Cost Inflation
Insurance and Administrative Cost Inflation
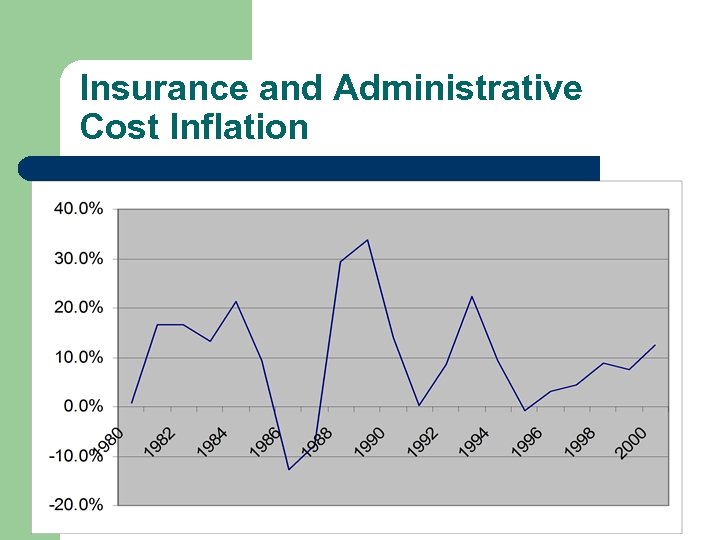
 Insurance and Administrative Cost l l The insurance and administrative portion (load factor) of the premium has been most volatile cost component. Insurance pricing cycle features market share chasing followed by bouts of profit margin expansion and reserve replenishment Average growth above 20% for 1988 -1990 led to movement for major health care policy reform It failed but managed care (pricing) boomed.
Insurance and Administrative Cost l l The insurance and administrative portion (load factor) of the premium has been most volatile cost component. Insurance pricing cycle features market share chasing followed by bouts of profit margin expansion and reserve replenishment Average growth above 20% for 1988 -1990 led to movement for major health care policy reform It failed but managed care (pricing) boomed.
 Pharmaceutical Cost Inflation
Pharmaceutical Cost Inflation
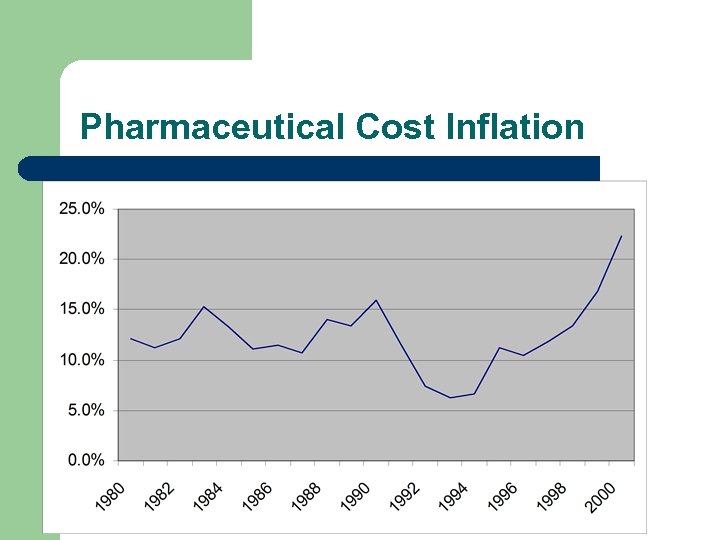
 Pharmaceutical Cost l l l l Double-digit growth since 1980 except for 1992 -94 The most rapidly rising component of expenditures since 1995. Some argue increased Rx has been the key ingredient in keeping total expenditures down. Mix of rising usage, new products & rising prices Public policy response varies; some states act as large purchaser and/or price fixer (Maine). Three tiered programs drive private purchasing. Expenditure share has risen from 5% to 9. 7%
Pharmaceutical Cost l l l l Double-digit growth since 1980 except for 1992 -94 The most rapidly rising component of expenditures since 1995. Some argue increased Rx has been the key ingredient in keeping total expenditures down. Mix of rising usage, new products & rising prices Public policy response varies; some states act as large purchaser and/or price fixer (Maine). Three tiered programs drive private purchasing. Expenditure share has risen from 5% to 9. 7%
 Back to the Future
Back to the Future
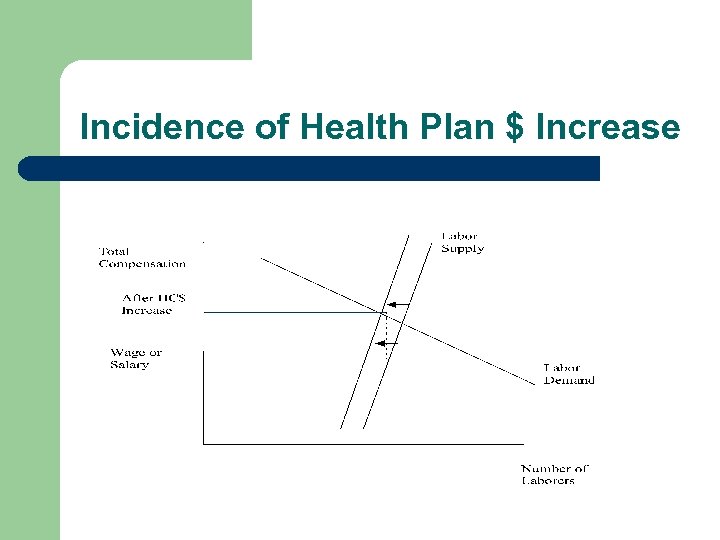
 Who Bears the Burden? l Two Central Facts – – l Consequence: Labor bears most of the burden even if employers pay the bill – l Employer arranged health care plans are a cost of labor Management is more responsive to changes in the cost of labor than laborers are to changes in pay (80% - median estimate among economists) Common Perception: businesses or consumers bear the burden
Who Bears the Burden? l Two Central Facts – – l Consequence: Labor bears most of the burden even if employers pay the bill – l Employer arranged health care plans are a cost of labor Management is more responsive to changes in the cost of labor than laborers are to changes in pay (80% - median estimate among economists) Common Perception: businesses or consumers bear the burden
 Incidence of Health Plan $ Increase
Incidence of Health Plan $ Increase
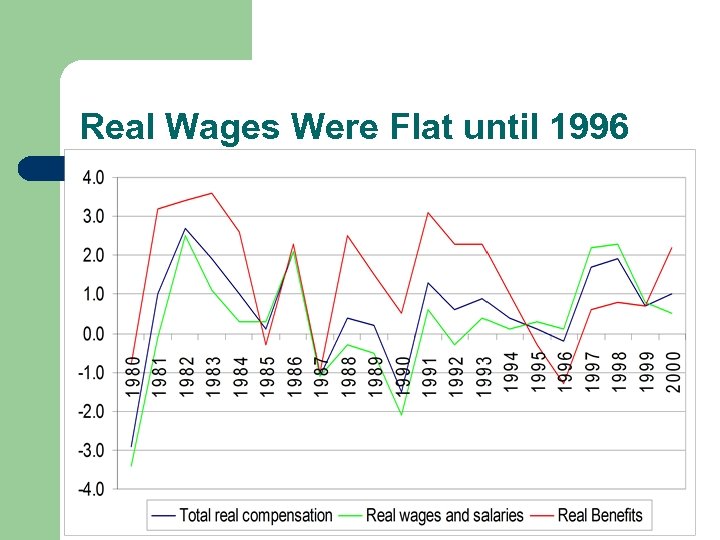 Real Wages Were Flat until 1996
Real Wages Were Flat until 1996
 Real Wages and Sales did not grow between 1980 and 1995 l l l Total real compensation grew by 0. 5% per year Real wages grew by 0. 0% per year Real benefits grew by 1. 6% per year For 2000, TC 1%; Ben 2. 2%; Wages 0. 5% Conclusion: Increases in productivity (1. 5%) consumed by health insurance and pension Conclusion: Laborers bear the burden of health insurance cost even if employer pays
Real Wages and Sales did not grow between 1980 and 1995 l l l Total real compensation grew by 0. 5% per year Real wages grew by 0. 0% per year Real benefits grew by 1. 6% per year For 2000, TC 1%; Ben 2. 2%; Wages 0. 5% Conclusion: Increases in productivity (1. 5%) consumed by health insurance and pension Conclusion: Laborers bear the burden of health insurance cost even if employer pays
 The Whack a Mole Response to Rising Health Care Costs l Short-sighted benefit redesign: – l Cost Accountant’s Revenge – l Target the fastest growing component (e. g. , ER use, RX use) If policy slows the fastest growing component, a new fastest grower emerges Only attempts to address total expenditures have the potential for sustainable success
The Whack a Mole Response to Rising Health Care Costs l Short-sighted benefit redesign: – l Cost Accountant’s Revenge – l Target the fastest growing component (e. g. , ER use, RX use) If policy slows the fastest growing component, a new fastest grower emerges Only attempts to address total expenditures have the potential for sustainable success
 Capital Expenditures Control l l Duplication of services and reduction of excess capacity have often led to calls for controlled entry – Certificate of Need (CON) laws Common practice – 1970 s & 80 s, the results: barriers to new entrants and no changes in expenditure growth Solutions are dictated by political power, not market success CON insulates existing providers from attempts to increase quality or reduce cost
Capital Expenditures Control l l Duplication of services and reduction of excess capacity have often led to calls for controlled entry – Certificate of Need (CON) laws Common practice – 1970 s & 80 s, the results: barriers to new entrants and no changes in expenditure growth Solutions are dictated by political power, not market success CON insulates existing providers from attempts to increase quality or reduce cost
 Which Costs Should Be Contained? l l Those paid by third parties Total payments to the industry (including out-ofpocket) Those related to diseases and their burdens Politicians, employers, and individuals have different answers
Which Costs Should Be Contained? l l Those paid by third parties Total payments to the industry (including out-ofpocket) Those related to diseases and their burdens Politicians, employers, and individuals have different answers
 Managed Care in the 1990 s l l 1990 s version featured insurance companies trading patient volume for provider network discounts or capitated payment Most insurers focused on discounts and major utilization trends – “the low hanging fruit” Employers selected 1 plan (an insurance carrier HMO) to reduce administrative cost HMO plans offered comprehensive benefits
Managed Care in the 1990 s l l 1990 s version featured insurance companies trading patient volume for provider network discounts or capitated payment Most insurers focused on discounts and major utilization trends – “the low hanging fruit” Employers selected 1 plan (an insurance carrier HMO) to reduce administrative cost HMO plans offered comprehensive benefits
 Managed Care and its Backlash l l l Comprehensive benefits with employer-chosen restricted access infuriated virtually everyone. Low unemployment rates and income tax exemption encouraged expanded benefits and networks ; thus, less management & higher $ Further reductions in hospital length of stay not cost-effective but contentious
Managed Care and its Backlash l l l Comprehensive benefits with employer-chosen restricted access infuriated virtually everyone. Low unemployment rates and income tax exemption encouraged expanded benefits and networks ; thus, less management & higher $ Further reductions in hospital length of stay not cost-effective but contentious
 3 Potentially Sustainable Strategies l Make health care a consumer responsibility – l Cap payments to the health care sector – l Nationalize insurance or employ global budgets Encourage primary and secondary prevention – – l Encourage patients to be efficient consumers Disease management for chronic disease Changes in life style for the rest of us Ideally, seek to add value
3 Potentially Sustainable Strategies l Make health care a consumer responsibility – l Cap payments to the health care sector – l Nationalize insurance or employ global budgets Encourage primary and secondary prevention – – l Encourage patients to be efficient consumers Disease management for chronic disease Changes in life style for the rest of us Ideally, seek to add value
 Consumer Responsibility to the Rescue l l l A response to OPM (Other People’s Money) Increased cost sharing – it’s your money, you decide how to spend it Benefit Shift: from comprehensive coverage with restricted choice to partial subsidy for broad choice Medical Savings Accounts feature the extreme version – only catastrophic insurance Many new (untested) options exist Consumer income and preferences drive choices
Consumer Responsibility to the Rescue l l l A response to OPM (Other People’s Money) Increased cost sharing – it’s your money, you decide how to spend it Benefit Shift: from comprehensive coverage with restricted choice to partial subsidy for broad choice Medical Savings Accounts feature the extreme version – only catastrophic insurance Many new (untested) options exist Consumer income and preferences drive choices
 The Costs of Shifting the Burden l l l Some employers abandon health care Risk segmentation increases Reduced incentives to join comprehensive benefit plans (HMOs) Incentives to postpone treatment and ignore prevention are increased “Out of the managed care frying pan into the cost sharing fire”
The Costs of Shifting the Burden l l l Some employers abandon health care Risk segmentation increases Reduced incentives to join comprehensive benefit plans (HMOs) Incentives to postpone treatment and ignore prevention are increased “Out of the managed care frying pan into the cost sharing fire”
 The Ultimate: Cheap Insurance
The Ultimate: Cheap Insurance
 Single Payer Rises Again l l l Expenditures can be contained by politically set budgets or global caps Canada and UK have successfully controlled the health care line item Priorities in these systems set politically or by providers
Single Payer Rises Again l l l Expenditures can be contained by politically set budgets or global caps Canada and UK have successfully controlled the health care line item Priorities in these systems set politically or by providers
 The Costs of Single Payer l l l Individual preferences play limited role Burdens of illness not addressed, only gov’t budgets Technology limited: both that which adds value and that which does not – – l l Fewer MRIs means more surgery Fewer new drugs means more intensive medicine If enrollees can choose a capped plan (or not), individual preferences can served Gov’t. systems run out of money before fiscal year ends
The Costs of Single Payer l l l Individual preferences play limited role Burdens of illness not addressed, only gov’t budgets Technology limited: both that which adds value and that which does not – – l l Fewer MRIs means more surgery Fewer new drugs means more intensive medicine If enrollees can choose a capped plan (or not), individual preferences can served Gov’t. systems run out of money before fiscal year ends
 The Budget Cake is Only So Big
The Budget Cake is Only So Big
 Chronic Disease Burdens are Huge l The burden of illness far exceeds documented paid claims – l Total burden approximates $10 k per year per worker with only 47% from group health $ (Goetzel) Chronic disease burdens cost > $1 trillion per year – – CDC/RWJ report estimates that 125 million American suffer from a chronic condition (Anderson) Average annual medical cost of $6, 032 for those with vs. $1, 105 for those without a chronic disease (Anderson) Chronic disease a/c 67. 5% of medical $ for working age adults Ave. work impairment is ranges from 2. 3 to 10. 9 days per 30 day work period (Kessler)
Chronic Disease Burdens are Huge l The burden of illness far exceeds documented paid claims – l Total burden approximates $10 k per year per worker with only 47% from group health $ (Goetzel) Chronic disease burdens cost > $1 trillion per year – – CDC/RWJ report estimates that 125 million American suffer from a chronic condition (Anderson) Average annual medical cost of $6, 032 for those with vs. $1, 105 for those without a chronic disease (Anderson) Chronic disease a/c 67. 5% of medical $ for working age adults Ave. work impairment is ranges from 2. 3 to 10. 9 days per 30 day work period (Kessler)
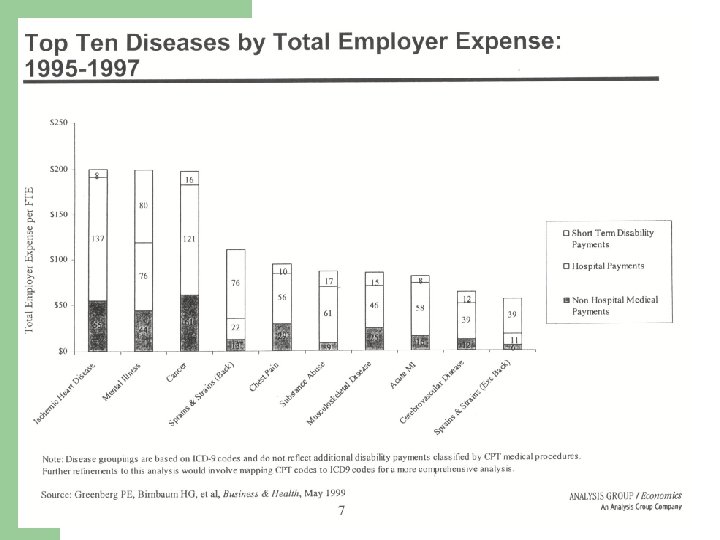 Top 10 Diseases by Employer Expense
Top 10 Diseases by Employer Expense
 Chronic Disease Management l l Use evidence-based medicine Well conceived disease management programs yield $5 - $10 of benefit per $ spent Successful programs integrate care, emphasize communication, and reduce barriers to compliance Success requires compliance with evidencebased guidelines
Chronic Disease Management l l Use evidence-based medicine Well conceived disease management programs yield $5 - $10 of benefit per $ spent Successful programs integrate care, emphasize communication, and reduce barriers to compliance Success requires compliance with evidencebased guidelines
 Primary Prevention l l l The prevalence of chronic disease and the impact of risk increases with age Pick prevention programs that match risks Wellness programs – Goetzel AJHP – medical costs dropped for 28 /32 corporate programs reviewed
Primary Prevention l l l The prevalence of chronic disease and the impact of risk increases with age Pick prevention programs that match risks Wellness programs – Goetzel AJHP – medical costs dropped for 28 /32 corporate programs reviewed
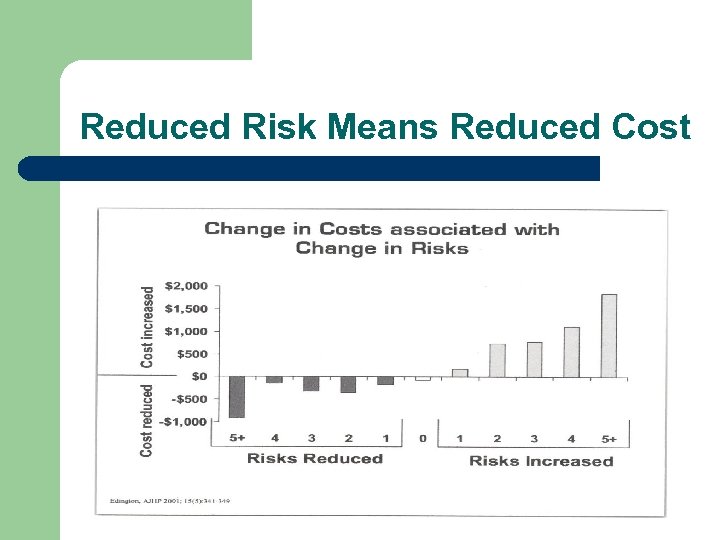 Reduced Risk Means Reduced Cost
Reduced Risk Means Reduced Cost
 Some Costs of Prevention l l Payment comes before savings and, thus, may not make sense with annual enrollment switching Each program has a different payback period Each population faces a different set of risks Compliance (medical community and patient/consumers) does not happen without education and compatible incentives
Some Costs of Prevention l l Payment comes before savings and, thus, may not make sense with annual enrollment switching Each program has a different payback period Each population faces a different set of risks Compliance (medical community and patient/consumers) does not happen without education and compatible incentives
 Pay Me Now or Pay Me Later
Pay Me Now or Pay Me Later
 Seek to Add Value l l Determine services that add the most improvement in health status or consumer satisfaction per $ spent Employ evidence-based medicine – that based on the most valid and reliable scientific information available Reward evidence-based “best” practice Recognize there may not be one “best” way.
Seek to Add Value l l Determine services that add the most improvement in health status or consumer satisfaction per $ spent Employ evidence-based medicine – that based on the most valid and reliable scientific information available Reward evidence-based “best” practice Recognize there may not be one “best” way.
 Value-Based Purchasing: No Mean Feat l l l No common definition of value or quality; hence hard to implement Multiple reporting requirements and data validity mean extra expense to implement Public sector purchasers face legislative and administrative restrictions on options Purchasers must have market power Providers resist quality performance comparisons
Value-Based Purchasing: No Mean Feat l l l No common definition of value or quality; hence hard to implement Multiple reporting requirements and data validity mean extra expense to implement Public sector purchasers face legislative and administrative restrictions on options Purchasers must have market power Providers resist quality performance comparisons
 Join a Purchasing Coalition l l Increased bargaining power if in same market Shared benefits and administrative responsibility is essential for success Mixed results since each pool represents an unique mix of risks, benefits, and incentives California HIPC aggressively negotiated prices with plans; most others had very limited effect
Join a Purchasing Coalition l l Increased bargaining power if in same market Shared benefits and administrative responsibility is essential for success Mixed results since each pool represents an unique mix of risks, benefits, and incentives California HIPC aggressively negotiated prices with plans; most others had very limited effect
 Central Florida Health Care Coalition l l 1 million covered lives – 1/3 of the market Started in mid 1980 s, spent millions Focus: good quality is cost-effective Identify evidence-based best practices – – – Over-use, under-use, and inappropriate use MBGH estimates at $1, 350 per employee per year + $350 indirect costs for poor quality care Estimate: 30% of direct hc $ related to poor quality
Central Florida Health Care Coalition l l 1 million covered lives – 1/3 of the market Started in mid 1980 s, spent millions Focus: good quality is cost-effective Identify evidence-based best practices – – – Over-use, under-use, and inappropriate use MBGH estimates at $1, 350 per employee per year + $350 indirect costs for poor quality care Estimate: 30% of direct hc $ related to poor quality
 Pay for Performance l l Central Florida Coalition spent $1 million – 5 year implementation plan Measure and communicate best practices – Establish platinum, gold, and silver payment l l l – l 50% based on clinical quality 25% based on cost 25% based on patient satisfaction Silver level: pay 65% of Medicare Also reward platinum consumers – – Make consumers aware of cost Reward compliance and risk reduction
Pay for Performance l l Central Florida Coalition spent $1 million – 5 year implementation plan Measure and communicate best practices – Establish platinum, gold, and silver payment l l l – l 50% based on clinical quality 25% based on cost 25% based on patient satisfaction Silver level: pay 65% of Medicare Also reward platinum consumers – – Make consumers aware of cost Reward compliance and risk reduction
 Trade-offs to be faced–all options l Increased life expectancy means increased cost but increased healthy years – – l Demographic factors suggest that health burdens will rise dramatically in the future; thus need to determine – – l Success in acute care increases life expectancy. Chronic disease increases with age, and, thus, life expectancy. Which services to provide Who will pay the bill Health care resources are scarce; thus, priority setting, not new entitlements, is needed
Trade-offs to be faced–all options l Increased life expectancy means increased cost but increased healthy years – – l Demographic factors suggest that health burdens will rise dramatically in the future; thus need to determine – – l Success in acute care increases life expectancy. Chronic disease increases with age, and, thus, life expectancy. Which services to provide Who will pay the bill Health care resources are scarce; thus, priority setting, not new entitlements, is needed
 Fundamental Choice for Purchasers l Patients / customers must choose either broad choice or increased integration – A broad network of providers l l – A narrow network of integrated providers l l l with high cost or external rationing fragmented care with lower costs and internal rationing more care coordination IBM helps its enrollees evaluate tradeoffs in terms of their own preferences
Fundamental Choice for Purchasers l Patients / customers must choose either broad choice or increased integration – A broad network of providers l l – A narrow network of integrated providers l l l with high cost or external rationing fragmented care with lower costs and internal rationing more care coordination IBM helps its enrollees evaluate tradeoffs in terms of their own preferences
 The Big Tradeoff
The Big Tradeoff
 Fundamental Choice for Medical Community l Physicians must choose between – Independent practice with l l – Oversight from third parties Some ability to bill for extra services Limited financial risk Continuous need to market services Group practice with l l Assumption of financial risk Some clinical independence Group practice decision-making and oversight Opportunity for cost-effective integrated programs
Fundamental Choice for Medical Community l Physicians must choose between – Independent practice with l l – Oversight from third parties Some ability to bill for extra services Limited financial risk Continuous need to market services Group practice with l l Assumption of financial risk Some clinical independence Group practice decision-making and oversight Opportunity for cost-effective integrated programs
 Guidelines for Purchaser Choice of a Cost Containment Strategy l l l Focus on the total burden of illness, not component cost control Develop and nurture long term partnerships among patients, providers, and payers. (Structure the system for all to win) Identify health risk factors and choose health programs and benefit designs to reduce them
Guidelines for Purchaser Choice of a Cost Containment Strategy l l l Focus on the total burden of illness, not component cost control Develop and nurture long term partnerships among patients, providers, and payers. (Structure the system for all to win) Identify health risk factors and choose health programs and benefit designs to reduce them
 Guidelines continued l l l Invest in the information (including evidencebased guidelines) and communication infrastructure for prevention Provide incentives for enrollees, providers, and payers to reward performance consistent with reduced risks and illness burdens Success requires strong leaders who seek value from health services & human capital.
Guidelines continued l l l Invest in the information (including evidencebased guidelines) and communication infrastructure for prevention Provide incentives for enrollees, providers, and payers to reward performance consistent with reduced risks and illness burdens Success requires strong leaders who seek value from health services & human capital.
 Editorial views l l l “…So far, health care has no Toyota…” –Molly Coye JD Kleine – Oxymoron: The Myth of a U. S. Health Care System “Knowing is not enough; we must apply. Willing is not enough; we must do” - Goethe
Editorial views l l l “…So far, health care has no Toyota…” –Molly Coye JD Kleine – Oxymoron: The Myth of a U. S. Health Care System “Knowing is not enough; we must apply. Willing is not enough; we must do” - Goethe
 American Values l l “You can always count on Americans to do the right thing - after they’ve tried everything else. ” – W. Churchill “When faced with second-best trade-off between cost-conscious choice and no choice at all, however, Americans may grumble but select the former. ” – J. Robinson
American Values l l “You can always count on Americans to do the right thing - after they’ve tried everything else. ” – W. Churchill “When faced with second-best trade-off between cost-conscious choice and no choice at all, however, Americans may grumble but select the former. ” – J. Robinson
 One Solution: Value + Choice l l l Find value and support it. Fixed contribution by employers to a flexible spending account (Enthoven) Provide two options for coverage – – A focused narrow network that encourages prevention and chronic disease management Broad choice with consumers determining how to spend their money
One Solution: Value + Choice l l l Find value and support it. Fixed contribution by employers to a flexible spending account (Enthoven) Provide two options for coverage – – A focused narrow network that encourages prevention and chronic disease management Broad choice with consumers determining how to spend their money


