0769641aab73611fd8b01d0d79963edc.ppt
- Количество слайдов: 28

Violence/ Abuse: Role of Dental Education in Identification/Intervention Leslie R. Halpern, DDS, MD, Ph. D, MPH Assistant Professor, Harvard School of Dental Medicine , Massachusetts General Hospital, Liaison for AAOMS, AMA National Advisory Council on Violence and Abuse

Family Violence (V/A) and Dentistry 1. As much as 75% of physical abuse involves injuries to the head , face, or neck 2. Abusers often avoid the same physician, BUT return to the same dental office 3. The dental professional often has established trust with the patient. 4. Dentists may be the first or only point of contact for domestic violence victims in a health care setting, and they may be the most capable of recognizing the signs of abuse.
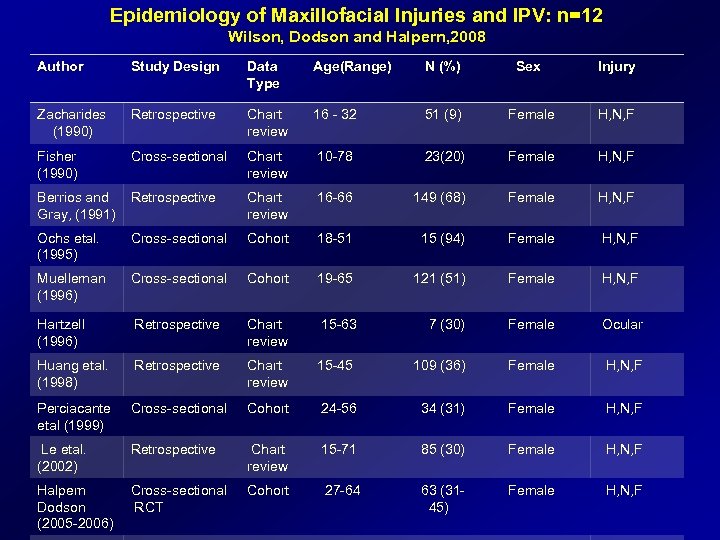
Epidemiology of Maxillofacial Injuries and IPV: n=12 Wilson, Dodson and Halpern, 2008 Author Study Design Data Type Age(Range) N (%) Sex Injury Zacharides (1990) Retrospective Chart review 16 - 32 51 (9) Female H, N, F Fisher (1990) Cross-sectional Chart review 10 -78 23(20) Female H, N, F Berrios and Gray, (1991) Retrospective Chart review 16 -66 149 (68) Female H, N, F Ochs etal. (1995) Cross-sectional Cohort 18 -51 15 (94) Female H, N, F Muelleman (1996) Cross-sectional Cohort 19 -65 121 (51) Female H, N, F Hartzell (1996) Retrospective Chart review 15 -63 7 (30) Female Ocular Huang etal. (1998) Retrospective Chart review 15 -45 109 (36) Female H, N, F Perciacante etal (1999) Cross-sectional Cohort 24 -56 34 (31) Female H, N, F Le etal. (2002) Retrospective Chart review 15 -71 85 (30) Female H, N, F Halpern Dodson (2005 -2006) Cross-sectional RCT Cohort 27 -64 63 (31 45) Female H, N, F

Family Violence and Dentistry • A 1998 national survey revealed that 16. 7 percent of women who sought health care for rape injuries visited dentists * • 9. 2 percent of women who sought care for physical assault by a partner saw a dentist ** • Routine dental visits may alert dental professionals to evidence that patients are being abused and lead to early intervention * Love etal. 2001 ** Tjaden and Thoennes, 1998

Studies : Identification/Intervention • “……. dentists and dental hygienists least likely…to suspect abuse in children, elders or young adults…. . if so are not responsible. . ” * • “ 87% never screened pts with head, and facial injuries…. . ” ** • “ 18% did not screen even when there were visible signs of head and neck injury” ** • “<1% of all child abuse reports are made by dental staff even though they are mandated so…” *** * Tilden etal 1994; **Love etal 2001; ***Mouden and Smedstad, 2002

Consensus Statements : (ADA)/(AAOMS) 1996: “ADA developed an educational policy…conflicting histories, behavioral changes, multiple injuries at variable stages of healing” 1999: “In all 50 states , physicians and dentists are required to report suspected cases of child abuse…to Social Service or law enforcement agencies…. and to collaborate in order to increase the prevention, detection and treatment of these conditions” * 2006: “ADA ran a commentary …. . importance of educating the dental community and obligation to recognize signs and symptoms of family violence/abuse” 2008: “ Oral and maxillofacial surgeons are dedicated to the health and well-being of all our patients, including those affected by violence and abuse, post traumatic stress disorders or traumatic brain injury” * *American Academy of Pediatrics and American Academy of Pediatric Dentistry, 1999 * American Association of Oral/Maxillofacial Surgeons (AAOMS)

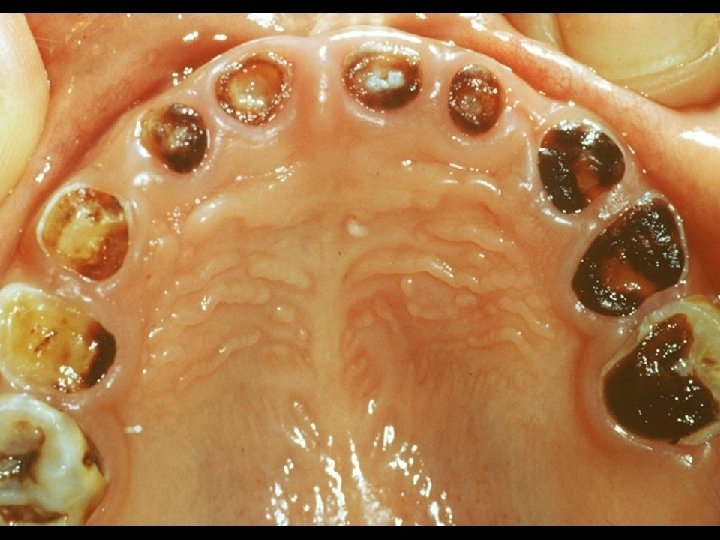
DV/IPV and Oral Health

Barriers for Identification • Education: – The training of healthcare providers has been insufficient even when the signs of abuse are present. – Inadequate education on the approach to identify victims. – Barriers to questioning that include patients accompanied by their partners, family members, cultural norms, and personal embarrassment by the doctor. – Fear of litigation if mistaken – Risk Predictors for victims: Physical vs. Psychological: What are they? ? ? ? ?

Oral /Maxillofacial Surgeons and Dentistry; P. A. N. D. A. TM ** • • • P: Prevent A: Abuse N: Neglect D: Dental A: Awareness • * Artwork and acronym used by permission of the P. A. N. D. A. TM Coalition developed by Delta Dental of Missouri, copyright 1992 * L Mouden, with permission
The P. A. N. D. A. Explosion Alaska Ontario IHS Finland Romania HI Guam Mexico Peru US Army Dental Command Israel

Curricula in Pre-doctoral Programs • Medical Schools: – “medical educators have emphasized the need to identify/intervene …. . victims of DV, IPV” * • Dental Schools: – “ dental educators. . Instruction on the familiarity with signs and symptoms…. monitoring regulations…” ** – Do Dental Professionals face the same challenges and barriers to addressing violence and abuse in their training programs? *** "There is recognition in both dentistry and medicine that oral health directly impacts systemic health, ……each profession's academic community should address the role that oral health education ultimately plays in patient care quality. " • Alpert etal. 1998; ** ADEA/ADA, 2007 ; ***AVA Blueprint; Halpern, 2008 * AAMC Medical Education Director Alexis L. Ruffin.

Dental Curricula in the US * • Inclusion of DV curricula in dental school/ dental hygiene : – Dental School: 96%, CA; unknown for IPV/EA – Dental Hygiene school: 70%, CA; 54. 9%, EA; 46%, IPV • Surveys: – 1996 : 53 US and 11 Canadian Dental Schools (N=55) – 2007: 55 US Dental Schools (N=25) • Topics relevant to DV: – – – – Responsibility of healthcare professional Physical and behavioral indicators Referral protocol Reporting protocol Prevalence Documentation Characteristics Interviewing skills * Gibson-Howell etal 2008

Results of Survey: 1996 -2007* • Dental Curriculum: – Responsibility of healthcare provider – Physical/behavioral variables – Prevalence • Critical questions: – Translation of above into daily practice patterns – Comfort zone of exam – Impact of IPV/DV on society • Direct costs • Indirect costs – Do cultural norms influence ethics of care * Gibson-Howell etal 2008

Pre-doctoral Dental Education Model: 1. University of MN 1. 1997: School of Dentistry/ Program Against Sexual Violence : Family Violence: An Intervention Model for Dental Professionals *www. ojp. usdoj. gov/ovc/publications/bulletins/dentalproviders/welco me. html – – – Ethical and legal responsibilities of dental professionals. Definitions and dynamics of family violence. The impact of abuse on victims. Intervention skills and techniques. Methods for creating a safe office environment. • Videos: – Clinical implications : 6 minutes – Healing Voices : 11 minutes – Comprehensive curriculum: » Images of injuries of abuse » Effective intervention strategies

Pre-doctoral Dental Education Model: 2. UCSF School of Dentistry • 2001: (Gerbert etal): – Survey: “dentists in UCSF study have major barriers to screening for domestic violence …a partner during the office visit; …. lack of training and the dentist's own embarrassment “ – AVDR: to help patients without imposing unreasonable expectations that dentists solve the problem of family violence. • 2004: JADA: – RCT with a multimedia Tutorial on preparing dental students to recognize/respond to DV • 2006: JADA: Ask: Asking patients about abuse Validate: Providing validating messages that acknowledge that battering is wrong while confirming patient’s worth Document: signs, symptoms , disclosures in the patient’s dental record in writing and with photographs Refer: to DV specialists and resources in the community – “the intervention effectively improved dentists’ intentions to practice ADVR intervention……. . perceived knowledge both of DV and of how to help victims…after taking the tutorial, dentists reported that they would be more likely to inquire about a patient’s safety after recognizing injuries to the head or neck”.

Pre-doctoral Dental Education: Model: 3. Tufts Univ. (TUSDM): * VVIP *: A Public Health Approach to Domestic Violence In An Academic Dental Setting Mission: 1. To develop an interdisciplinary group of healthcare providers that will identify and treat victims of violence and abuse. 2. To educate / train future dentists at both the pre-doctoral and post-doctoral levels on the diagnoses of oral disease as a predictive risk factor. 3. To care treat and follow up with populations at risk for violence, abuse, neglect : Child, Adult, Elders. 4. To educate future dental care providers in an academic dental care setting, through classroom trainings, clinical dental practice, outcomes assessment, and community outreach. * Victims of Violence Intervention Program ; * Gul etal. 2004
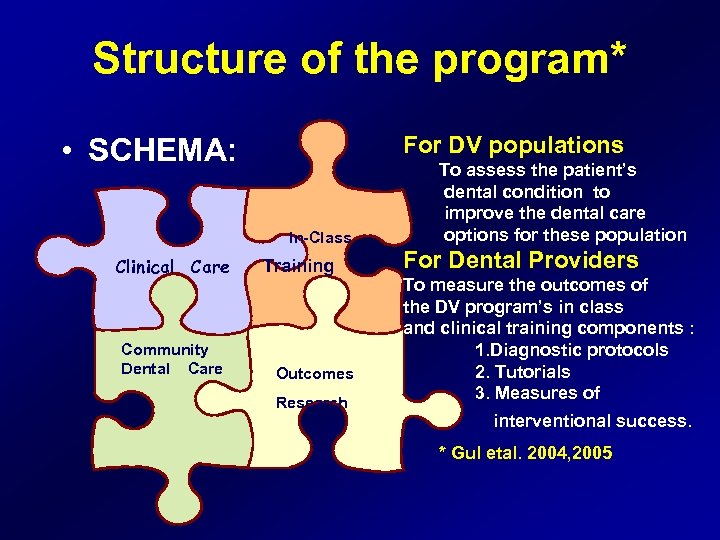
Structure of the program* • SCHEMA: Clinical Care For DV populations To assess the patient’s dental condition to improve the dental care options for these population In-Class Training Community Dental Care Outcomes Research For Dental Providers To measure the outcomes of the DV program’s in class and clinical training components : 1. Diagnostic protocols 2. Tutorials 3. Measures of interventional success. * Gul etal. 2004, 2005
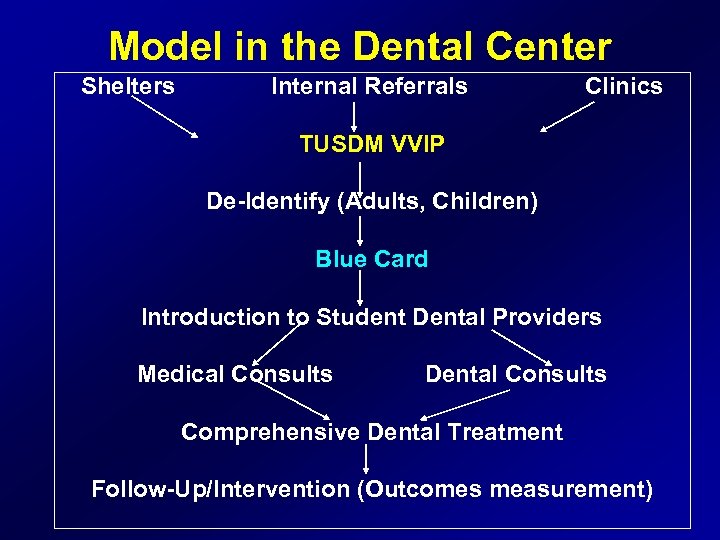
Model in the Dental Center Shelters Internal Referrals Clinics TUSDM VVIP De-Identify (Adults, Children) Blue Card Introduction to Student Dental Providers Medical Consults Dental Consults Comprehensive Dental Treatment Follow-Up/Intervention (Outcomes measurement)
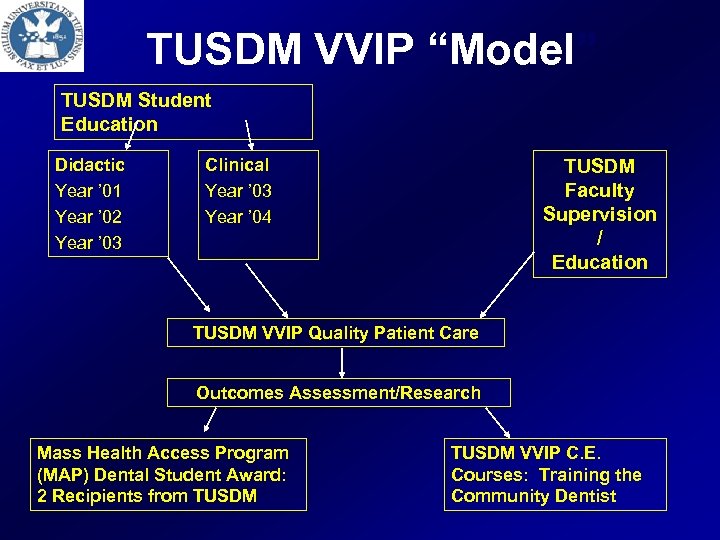
TUSDM VVIP “Model” TUSDM Student Education Didactic Year ’ 01 Year ’ 02 Year ’ 03 Clinical Year ’ 03 Year ’ 04 TUSDM Faculty Supervision / Education TUSDM VVIP Quality Patient Care Outcomes Assessment/Research Mass Health Access Program (MAP) Dental Student Award: 2 Recipients from TUSDM VVIP C. E. Courses: Training the Community Dentist

Pre-doctoral Dental Education: Model: 4. Harvard School DM/MGH: A Diagnostic protocol to diagnose IPV: • Injury location as a marker for IPV: Head, Neck and/or Facial * • Responses to a questionnaire (Partner Violence Screen : PVS)* * as markers for IPV – Have you been kicked, punched, hit in a relationship? – Do you feel unsafe in a relationship? – Past feelings of being unsafe? • An affirmative response to any of the above questions was considered positive as a marker for IPV * Ochs etal. 1995; Perciaccante etal. 1999; 2002; Halpern etal. 2005; 2006 * Feldhaus etal. 1997

Schema: Diagnostic Protocol for IPV Females with non-verifiable injuries presenting to ED for evaluation and treatment Injury location HNF Other Questionnaire Positive Negative High Risk Low Risk
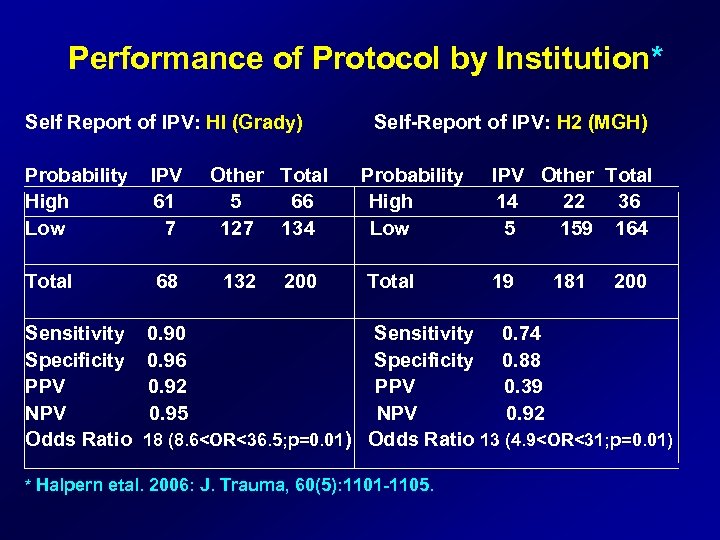
Performance of Protocol by Institution* Self Report of IPV: HI (Grady) Self-Report of IPV: H 2 (MGH) Probability IPV Other Total Probability IPV Other Total High 61 5 66 High 14 22 36 Low 7 127 134 Low 5 159 164 Total 68 132 200 Total 19 181 200 Sensitivity 0. 90 Sensitivity 0. 74 Specificity 0. 96 Specificity 0. 88 PPV 0. 92 PPV 0. 39 NPV 0. 95 NPV 0. 92 Odds Ratio 18 (8. 6<OR<36. 5; p=0. 01) Odds Ratio 13 (4. 9<OR<31; p=0. 01) * Halpern etal. 2006: J. Trauma, 60(5): 1101 -1105.
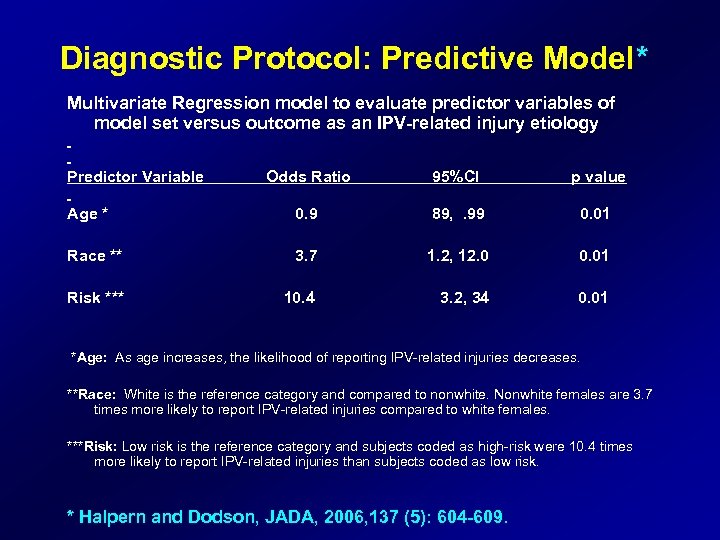
Diagnostic Protocol: Predictive Model* Multivariate Regression model to evaluate predictor variables of model set versus outcome as an IPV-related injury etiology Predictor Variable Odds Ratio 95%CI p value Age * 0. 9 89, . 99 0. 01 Race ** 3. 7 1. 2, 12. 0 0. 01 Risk *** 10. 4 3. 2, 34 0. 01 *Age: As age increases, the likelihood of reporting IPV-related injuries decreases. **Race: White is the reference category and compared to nonwhite. Nonwhite females are 3. 7 times more likely to report IPV-related injuries compared to white females. ***Risk: Low risk is the reference category and subjects coded as high-risk were 10. 4 times more likely to report IPV-related injuries than subjects coded as low risk. * Halpern and Dodson, JADA, 2006, 137 (5): 604 -609.

Future Directions/Conclusions: Strategies/Approaches 1. Change the learning environment: - Minimize a formal lecture format to one that invites speakers from the community 2. Convert lecture format to student –centered – Role play and “real-life” scenario • Mock interviews • Community service/ shelter clinic environment • Outreach vans 3. Develop a standard template/protocol/Web/DVD – Risk predictors • Injury location • Other; i. e. ; health risk predictors 4. Asking is an intervention – Studies demonstrate that abused women want their providers to query them about IPV/ and “side effects”.

Future Directions/Conclusions: Successful Intervention 5. Making a connection between their health history, previously incomprehensible symptoms and h/o V/A may have a significant therapeutic effect. – Long term negative health consequences • i. e. Chronic illnesses : New Risk Predictors? ? • a paucity of data exists to measure the consequences of these physiologic responses. 6. Education on domestic violence needs to be “standardized and incorporated into dental school and continuing education curricula, thus normalizing intervention with victims and making it a standard part of a dentist’s/oral healthcare providers professional responsibility”. * *OVC; Dep’t Justice, 2004

Acknowledgments/Funding • • • American Association of Oral and Maxillofacial Surgeons AMA National Advisory Council on Violence and Abuse Thomas B. Dodson, DMD, MPH – Director, Center of Clinical Investigation, MGH, HSDM Lynn D. Mouden, DDS, MPH – Director, Office of Oral Health, Arkansas Department of Health and Human Services; Professor, UAMS College of Public Health – Founder of P. A. N. D. A. TM David Mc. Cullum, MD, MPH, – Former Chair, AMA, National Advisory Council on Violence and Abuse (NACVA) – President of Academy on Violence and Abuse (AVA) Megan Gerber, MD, MPH, – – Assistant Clinical Professor, Harvard Medical School Women’s Health Center, Veteran’s Administration , Boston, MA • Funding • Oral and Maxillofacial Surgery Foundation • Harvard Medical School, Center of Excellence in Women’s Health • Dep’t Oral/Maxillofacial Surgery, Massachusetts General Hospital/Harvard School of Dental Medicine • Harvard Vanguard Medical Associates , ATRIUS HEALTH, MA.

Thank you
0769641aab73611fd8b01d0d79963edc.ppt