a2bc9cf14bc5ae23bbe593b24647f7b4.ppt
- Количество слайдов: 30

Use Of Mobile Phones To Promote Physical Activity In A Rural Population Of Delhi, India Dr. Malvika Sharma, Dr. B Banerjee, Dr. G. K Ingle, Dr. S. Garg Department of Community Medicine, Maulana Azad Medical College, New Delhi, India

BURDEN OF NON-COMMUNCABLE DISEASES (NCD) NCDs are the leading cause of adult mortality and morbidity worldwide. (About 67% of all deaths) 82% of NCD deaths- CVD, Cancer, Diabetes, Chronic respiratory disease. Nearly 75% of NCD deaths- LAMI countries 42% of all NCD deaths globally- before 70 years age (48% in LAMI countries) India: NCDs account for 53% deaths and 44% DALYs (2004), estimated to cause 75% of all deaths in India by 2030. Dual Burden SDG Target 3. 4 Page 2
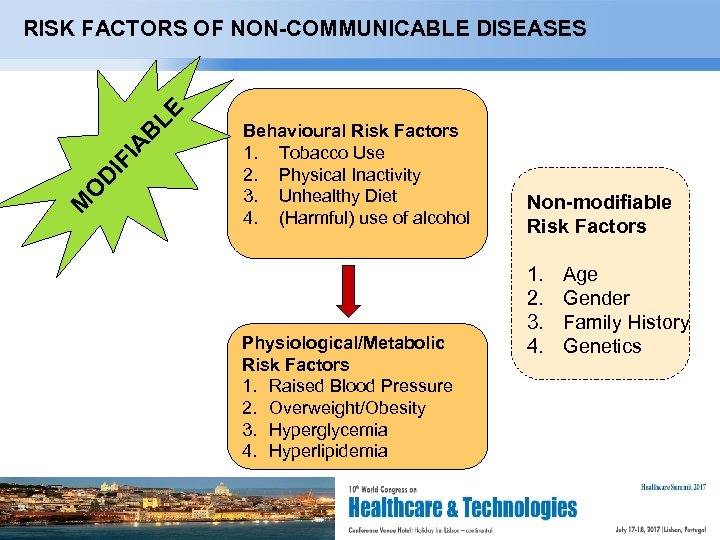
M O D IF IA B LE RISK FACTORS OF NON-COMMUNICABLE DISEASES Behavioural Risk Factors 1. Tobacco Use 2. Physical Inactivity 3. Unhealthy Diet 4. (Harmful) use of alcohol Physiological/Metabolic Risk Factors 1. Raised Blood Pressure 2. Overweight/Obesity 3. Hyperglycemia 4. Hyperlipidemia Page 3 Non-modifiable Risk Factors 1. 2. 3. 4. Age Gender Family History Genetics

m. HEALTH FOR HEALTH PROMOTION/LIFESTYLE MODIFICATION? Most common NCDs share common pool of risk factors High prevalence of these risk factors in the community- health promotion messages need to reach large population m. Health delivered to large number of individuals through one-to-one communication in cost-effective manner and shorter time. Automated system-generated SMS- dissemination of health messages (also for surveillance, management and treatment compliance) Page 4

PROMISE OF m. HEALTH IN INDIA Second largest mobile-phone user base in the world- 1. 12 million users (2016). Low priced phones. Among the lowest mobile tariffs in the world. Steady increase in geographical coverage of mobile networks. Rural tele-density increased from 5. 89% in 2007 to 52. 3% in 2016 (Oct) m. Health currently used in various health programs- Mother and Child Tracking System, Dengue outbreak control, Adherence to TB medication etc. Page 5

CAN m. HEALTH BE EFFECTIVELY UTILIZED TO REDUCE BEHAVIOURAL RISK FACTORS OF NON-COMMUNICABLE DISEASES? Page 6

Literature Review for m. Health interventions for NCD risk-factor modification in Low and Middle Income countries Systematic review by Muller et al, published in 2016 (Int J Behav Nutr Phys Act) reviewed 15 studies evaluating m. Health and e. Health interventions for promoting healthy diet and physical activity in LAMI countries: – 50% of the interventions were effective in increasing physical activity and 70% were effective in improving diet quality – BUT, none of the included studies were conducted in general population. Studies in India: – Pfammatter A et al (J Med Internet Res), 2016: parallel-group cohort study to determine effectiveness of m. Diabetes, a text messaging programme to improve diabetes risk behaviours. – Shetty et al (J Assoc Physicians India), 2011: RCT to study feasibility of using SMS to ensure adherence to management prescriptions by diabetic patients. Limited data on such interventions in apparently healthy, general population Page 7

Aim of the current study was to assess the effect of telephone-delivered communication on behavioural risk-factors of Non-Communicable Diseases. Page 8

MATERIALS AND METHODS STUDY DESIGN: Community-based “Before and After” Intervention study with control. Registered with Clinical Trials Registry of India: CTRI/2017/03/008264 STUDY AREA: Barwala Village located in noth-west district of Delhi The population of the village was 4500 with 639 households as per a demographic survey conducted on 2014. The village is catered by the Rural Health Training Centre (RHTC), Department of Community Medicine, Maulana Azad Medical College. Page 9

INCLUSION CRITERIA: – Adults aged 18 -64 years – Resident of the village for at least 6 months – Having access to mobile phone with SMS facility in Hindi – Ability to read SMS EXCLUSION CRITERIA: – Individuals with impaired hearing, inability to talk and severe mental retardation – Individuals who could not be contacted after 3 successive visits – Pregant women Page 10

Sample Size The sample size was calculated using the formula: Sample size= 2 (Zα+Z 1 -β)2 pq d 2 Where, Zα is type 1 error, Z 1 -β is power p = (p 1+p 2)/2; p 1= proportion before intervention, p 2= proportion after intervention q is (1 -p) d is absolute difference expected after intervention. Value of p was calculated as 0. 1 using prevalence estimate from a study done by Garg et al in Delhi in 2014. With p=0. 1, q=0. 9, d=0. 1, Zα =1. 96 at 95% confidence, Z 1 -β = 0. 84 at 80% power, calculated sample size was 144 in each group. Adding 20% for attrition and rounding up, our target sample size was 200 in each group. Page 11

Sampling Method Two stage sampling was done: STAGE 1: Systematic random sampling at household level using household list available at RHTC as sampling frame. STAGE 2: One adult fulfilling inclusion criteria was selected from each selected household using simple random sampling by lottery method. Page 12

Methodology Study was conducted for a period of one year from January 2016 to December 2016, in 3 phases: 1. Pre-Intervention Phase: – 2 months (January-February 2016) – Baseline data was collected from selected individuals after obtaining written, informed consent. – Pre-tested schedule (in Hindi) based on WHO STEPS approach was used to collect data. • Step 1: Questions on behavioural risk factors, history of raised BP, history of diabetes • Step 2: Physical examination: Height, Waist circumference, Hip circumference, Blood Pressure • Step 3: Investigations: Fasting blood sugar and Lipid Profile. Page 13

2. Intervention Phase: – 8 months (March-October 2016) – m. Health package: weekly SMS (pre-prepared roster) + monthly phone call – Content: importance of modification of behavioural risk factors, addressing queries, positive reinforcement – No such intervention given in control group 3. Post-Intervention Phase: – 2 months (November-December 2016) – Post-intervention data collected from both groups using the same schedule as in baseline. Page 14

RESULTS Page 15
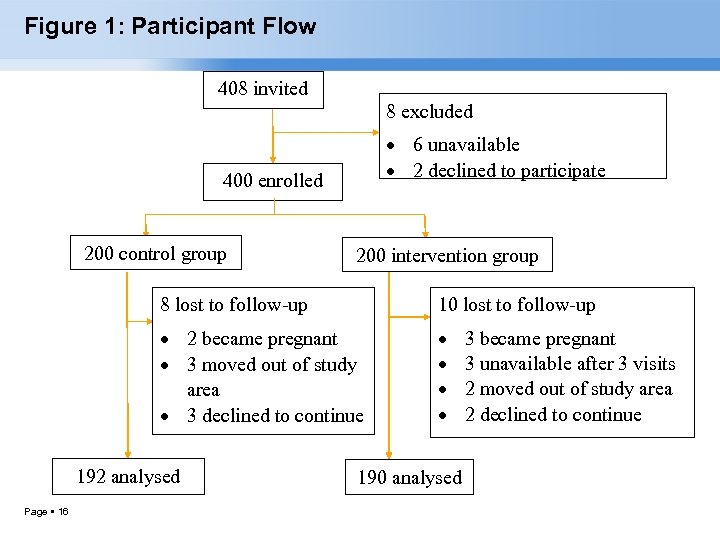
Figure 1: Participant Flow 408 invited 8 excluded 6 unavailable 2 declined to participate 400 enrolled 200 control group 200 intervention group 8 lost to follow-up 10 lost to follow-up 2 became pregnant 3 moved out of study area 3 declined to continue 192 analysed Page 16 190 analysed 3 became pregnant 3 unavailable after 3 visits 2 moved out of study area 2 declined to continue

BASELINE DATA Page 17
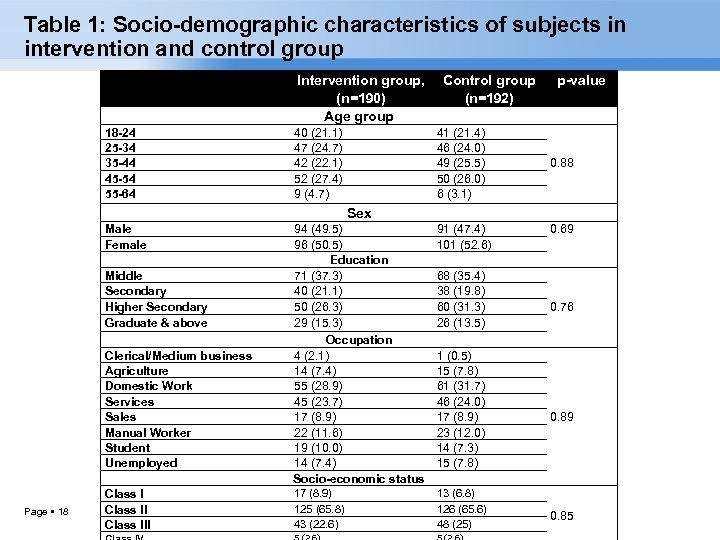
Table 1: Socio-demographic characteristics of subjects in intervention and control group Intervention group, Control group (n=190) (n=192) Age group 18 -24 25 -34 35 -44 45 -54 55 -64 40 (21. 1) 47 (24. 7) 42 (22. 1) 52 (27. 4) 9 (4. 7) p-value 41 (21. 4) 46 (24. 0) 49 (25. 5) 50 (26. 0) 6 (3. 1) 0. 88 94 (49. 5) 96 (50. 5) Education 71 (37. 3) 40 (21. 1) 50 (26. 3) 29 (15. 3) Occupation 4 (2. 1) 14 (7. 4) 55 (28. 9) 45 (23. 7) 17 (8. 9) 22 (11. 6) 19 (10. 0) 14 (7. 4) Socio-economic status 91 (47. 4) 101 (52. 6) 0. 69 68 (35. 4) 38 (19. 8) 60 (31. 3) 26 (13. 5) 0. 76 1 (0. 5) 15 (7. 8) 61 (31. 7) 46 (24. 0) 17 (8. 9) 23 (12. 0) 14 (7. 3) 15 (7. 8) 0. 89 17 (8. 9) 125 (65. 8) 43 (22. 6) 13 (6. 8) 126 (65. 6) 48 (25) Sex Male Female Middle Secondary Higher Secondary Graduate & above Clerical/Medium business Agriculture Domestic Work Services Sales Manual Worker Student Unemployed Page 18 Class III 0. 85
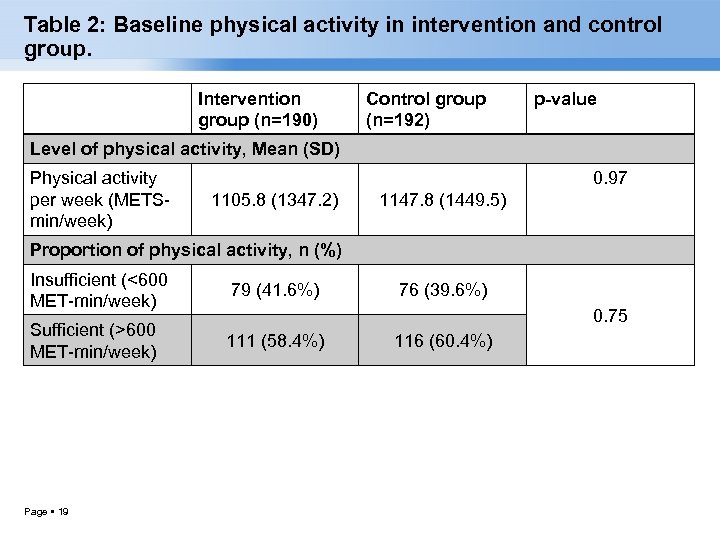
Table 2: Baseline physical activity in intervention and control group. Intervention group (n=190) Control group (n=192) p-value Level of physical activity, Mean (SD) Physical activity per week (METSmin/week) 0. 97 1105. 8 (1347. 2) 1147. 8 (1449. 5) Proportion of physical activity, n (%) Insufficient (<600 MET-min/week) 79 (41. 6%) Sufficient (>600 MET-min/week) 111 (58. 4%) Page 19 76 (39. 6%) 0. 75 116 (60. 4%)
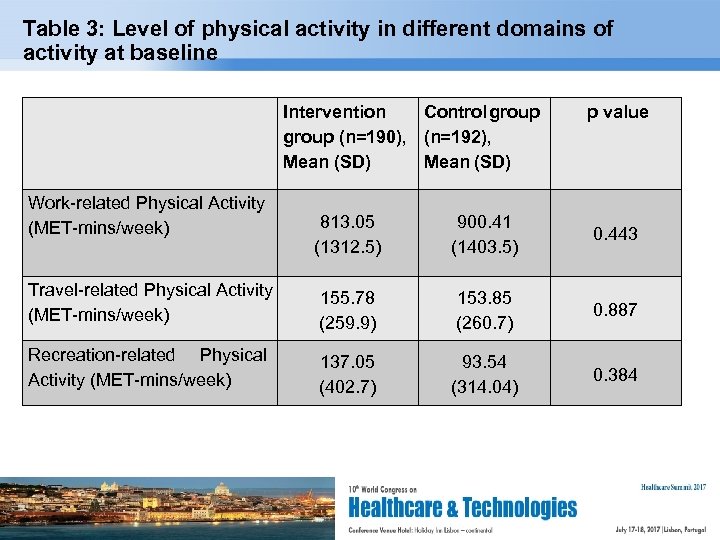
Table 3: Level of physical activity in different domains of activity at baseline Intervention Control group (n=190), (n=192), Mean (SD) Work-related Physical Activity (MET-mins/week) p value 813. 05 (1312. 5) 900. 41 (1403. 5) 0. 443 Travel-related Physical Activity (MET-mins/week) 155. 78 (259. 9) 153. 85 (260. 7) 0. 887 Recreation-related Physical Activity (MET-mins/week) 137. 05 (402. 7) 93. 54 (314. 04) 0. 384 Page 20

CHANGE AFTER INTERVENTION Page 21
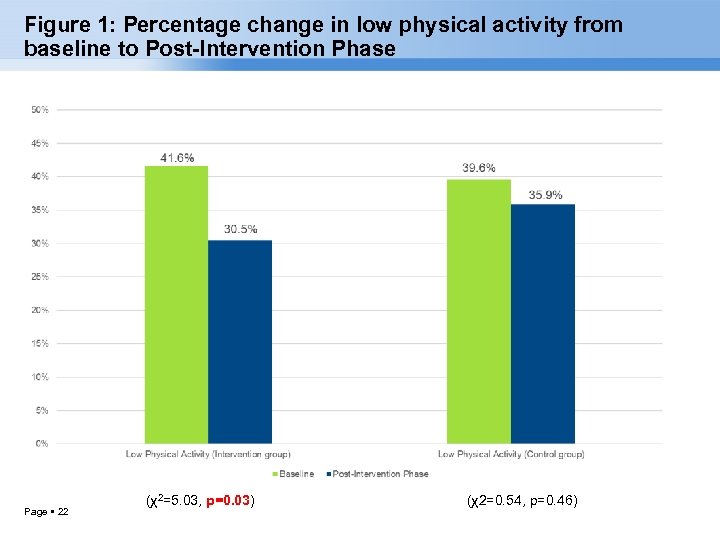
Figure 1: Percentage change in low physical activity from baseline to Post-Intervention Phase Page 22 (χ2=5. 03, p=0. 03) (χ2=0. 54, p=0. 46)
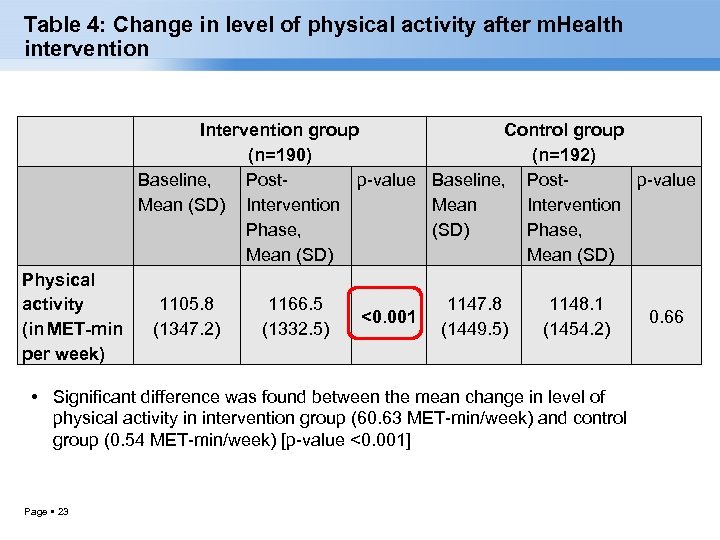
Table 4: Change in level of physical activity after m. Health intervention Intervention group Control group (n=190) (n=192) Baseline, Postp-value Mean (SD) Intervention Mean Intervention Phase, (SD) Phase, Mean (SD) Physical activity (in MET-min per week) 1105. 8 (1347. 2) 1166. 5 (1332. 5) <0. 001 1147. 8 (1449. 5) 1148. 1 (1454. 2) • Significant difference was found between the mean change in level of physical activity in intervention group (60. 63 MET-min/week) and control group (0. 54 MET-min/week) [p-value <0. 001] Page 23 0. 66
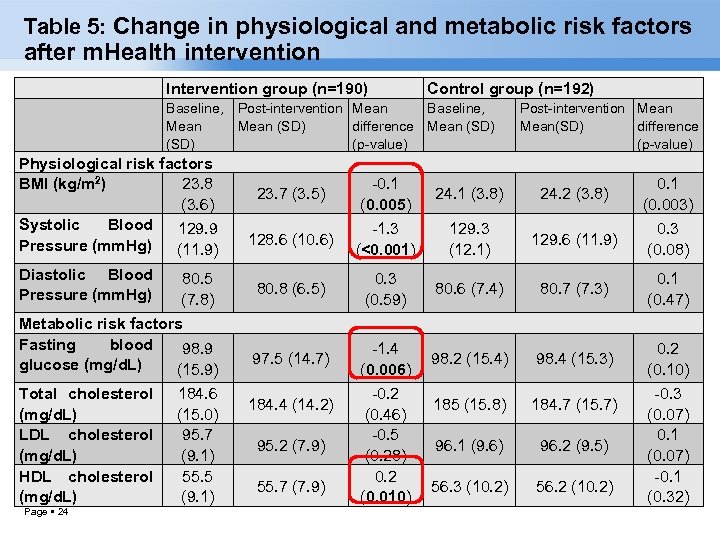
Table 5: Change in physiological and metabolic risk factors after m. Health intervention Intervention group (n=190) Control group (n=192) Baseline, Post-intervention Mean Baseline, Post-intervention Mean (SD) difference Mean (SD) Mean(SD) difference (SD) (p-value) Physiological risk factors BMI (kg/m 2) 23. 8 (3. 6) Systolic Blood 129. 9 Pressure (mm. Hg) (11. 9) Diastolic Blood Pressure (mm. Hg) 80. 5 (7. 8) Metabolic risk factors Fasting blood 98. 9 glucose (mg/d. L) (15. 9) Total cholesterol (mg/d. L) LDL cholesterol (mg/d. L) HDL cholesterol (mg/d. L) Page 24 184. 6 (15. 0) 95. 7 (9. 1) 55. 5 (9. 1) 23. 7 (3. 5) -0. 1 (0. 005) 24. 1 (3. 8) 24. 2 (3. 8) 0. 1 (0. 003) 128. 6 (10. 6) -1. 3 (<0. 001) 129. 3 (12. 1) 129. 6 (11. 9) 0. 3 (0. 08) 80. 8 (6. 5) 0. 3 (0. 59) 80. 6 (7. 4) 80. 7 (7. 3) 0. 1 (0. 47) 97. 5 (14. 7) -1. 4 (0. 006) 98. 2 (15. 4) 98. 4 (15. 3) 0. 2 (0. 10) 185 (15. 8) 184. 7 (15. 7) 96. 1 (9. 6) 96. 2 (9. 5) 56. 3 (10. 2) 56. 2 (10. 2) 184. 4 (14. 2) 95. 2 (7. 9) 55. 7 (7. 9) -0. 2 (0. 46) -0. 5 (0. 28) 0. 2 (0. 010) -0. 3 (0. 07) 0. 1 (0. 07) -0. 1 (0. 32)

STRENGTHS OF THE STUDY Evaluated behavioural, physiological as well as biochemical risk-factors: anthropometric measurement and measurement of BP, Blood sugar and Cholesterol provides objectivity. m. Health package consisted of a monthly phone call that provided opportunity for two way communication. Study conducted at community level in a randomly selected sample- enhances external validity. Page 25

LIMITATIONS OF THE STUDY Allocation was non-random. Blinding was not possible. Self reported behavioural risk factors- prone to recall and selfdesirability bias. Sample size was calculated based on primary outcome (change in behavioural risk factor)- might be underpowered to detect changes in physiological and biochemical risk factors. The intervention and control group were both served by the same health centre and were thus both exposed to ongoing health promotion activities and preventive services provided by the centre. Might lead to dilution of results. Page 26

CONCLUSION At baseline, proportion of insufficient physical activity in intervention and control group was 41. 6% and 39. 6% respectively. After m. Health intervention, insufficient physical activity reduced significantly by about 27% compared to baseline in intervention group. There was no significant change in control group. Change observed only in the Recreation Domain. Page 27

CONCLUSION Significant reduction in physiological risk factors- Mean BMI and Systolic BP in intervention group. Among metabolic risk-factors: significant reduction was seen in fasting blood glucose and rise in HDL Cholesterol in intervention group. Page 28

RECOMMENDATIONS Deployment of innovative measures such as m. Health to increase awareness of risk factors of NCDs- rapid, cheap, can reach large number of people with limited manpower. m. Health for health promotion and lifestyle modification should be scaled up- incorporated in the national programme for NCDs. Multipronged approach required for awareness creation and behaviour change- IEC activities through other media such as mass media and mid media, in addition to m. Health services. Page 29

THANK YOU
a2bc9cf14bc5ae23bbe593b24647f7b4.ppt