01438a25c02b877dcb91bea9fc8bac7b.ppt
- Количество слайдов: 47
 University of Minnesota The Healthcare Marketplace Medical Industry Leadership Institute Course: MILI 6990/5990 Spring Semester A, 2015 Stephen T. Parente, Ph. D. Carlson School of Management Department of Finance sparente@umn. edu
University of Minnesota The Healthcare Marketplace Medical Industry Leadership Institute Course: MILI 6990/5990 Spring Semester A, 2015 Stephen T. Parente, Ph. D. Carlson School of Management Department of Finance sparente@umn. edu
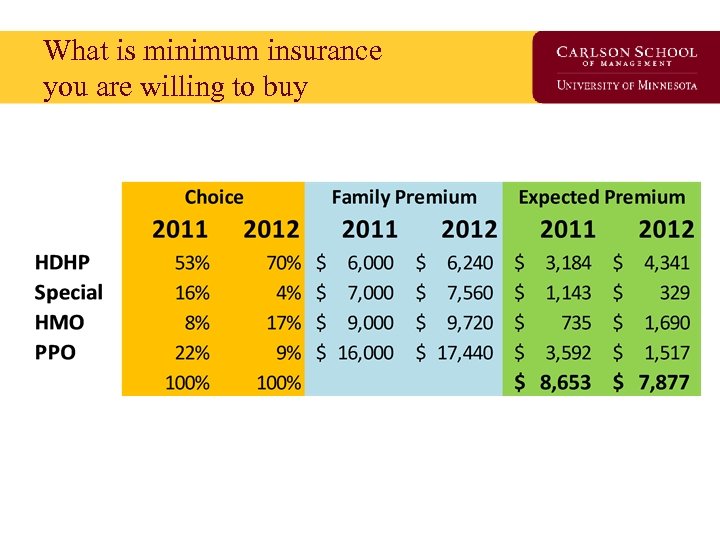 What is minimum insurance you are willing to buy
What is minimum insurance you are willing to buy
 Information Technology Overview • • Goals of Health IT Econ Background Value of Health IT – IOM Report Health IT Pyramid – Hardware – Data • Vision Quest – Integrating Clinical & Insurance Data for Management • Health IT & Health Reform – Options
Information Technology Overview • • Goals of Health IT Econ Background Value of Health IT – IOM Report Health IT Pyramid – Hardware – Data • Vision Quest – Integrating Clinical & Insurance Data for Management • Health IT & Health Reform – Options
 What are the Goals of Information Technology? • Make life easier – Easier to obtain products & services • Improve quality of life • Save Money – Labor-savings $$$ – Less costly mistakes • Make Money – Focused Marketing
What are the Goals of Information Technology? • Make life easier – Easier to obtain products & services • Improve quality of life • Save Money – Labor-savings $$$ – Less costly mistakes • Make Money – Focused Marketing
 Economic Theory of IT • Good work by: Erik Brynjolfsson and Lorin Hitt (2000) from MIT Sloan School • Three Different Measure’s of IT Value: – Productivity – Profit – Consumer Welfare
Economic Theory of IT • Good work by: Erik Brynjolfsson and Lorin Hitt (2000) from MIT Sloan School • Three Different Measure’s of IT Value: – Productivity – Profit – Consumer Welfare
 Unique Features of Health IT Economics • Standard assumption is that IT can not yield profits only reduce costs. • Assumption is not true if an industry has high barriers to entry. • Health care has many barriers to entry, so providers & insurers should buy IT not just as a tool to control cost but to profit as well.
Unique Features of Health IT Economics • Standard assumption is that IT can not yield profits only reduce costs. • Assumption is not true if an industry has high barriers to entry. • Health care has many barriers to entry, so providers & insurers should buy IT not just as a tool to control cost but to profit as well.
 Econometric Application - 3 Consumer Surplus • Consumer surplus is derived from consumers purchasing a good at a market price lower than what they would have been willing to pay. • IT is full of these examples in the PC market today. What about Health IT? • Want to plot a demand curve to measure CS: – Could obtain data from insurers and providers to see whether consumer surplus exists. – May need a patient survey for Internet applications related to health.
Econometric Application - 3 Consumer Surplus • Consumer surplus is derived from consumers purchasing a good at a market price lower than what they would have been willing to pay. • IT is full of these examples in the PC market today. What about Health IT? • Want to plot a demand curve to measure CS: – Could obtain data from insurers and providers to see whether consumer surplus exists. – May need a patient survey for Internet applications related to health.
 What is the ‘Value’ of Information? • Hard to Express……. • A proxy valuation is the ‘opportunity cost’ of not having the information. • Opportunity cost is defined as the cost you would pay to obtain one unit of information in exchange for one unit of another good. • Health example: An insurer not having a diabetes care tracking system by 2010 will lead to employer with 5, 000 beneficiaries to leave the plan, which would decrease profits by $2 million.
What is the ‘Value’ of Information? • Hard to Express……. • A proxy valuation is the ‘opportunity cost’ of not having the information. • Opportunity cost is defined as the cost you would pay to obtain one unit of information in exchange for one unit of another good. • Health example: An insurer not having a diabetes care tracking system by 2010 will lead to employer with 5, 000 beneficiaries to leave the plan, which would decrease profits by $2 million.
 The IOM Quality Chasm Report: Health IT Diffusion Catalyst?
The IOM Quality Chasm Report: Health IT Diffusion Catalyst?
 The Problem of Health IT From the IOM Quality Chasm Report • “Health care delivery has been relatively untouched by the revolution information technology that has been transforming nearly every other aspect of society. ” • “The challenges of applying information technology to health care should not be underestimated…. do to the complexity of the industry. ”
The Problem of Health IT From the IOM Quality Chasm Report • “Health care delivery has been relatively untouched by the revolution information technology that has been transforming nearly every other aspect of society. ” • “The challenges of applying information technology to health care should not be underestimated…. do to the complexity of the industry. ”
 The Opportunity of Health IT “The Internet has enormous potential to transform health care through information technology applications in such as areas as consumer health, clinical care, administrative and financial transactions, public health, professional education, and biomedical and health services research (National Research Council, 2000). ”
The Opportunity of Health IT “The Internet has enormous potential to transform health care through information technology applications in such as areas as consumer health, clinical care, administrative and financial transactions, public health, professional education, and biomedical and health services research (National Research Council, 2000). ”
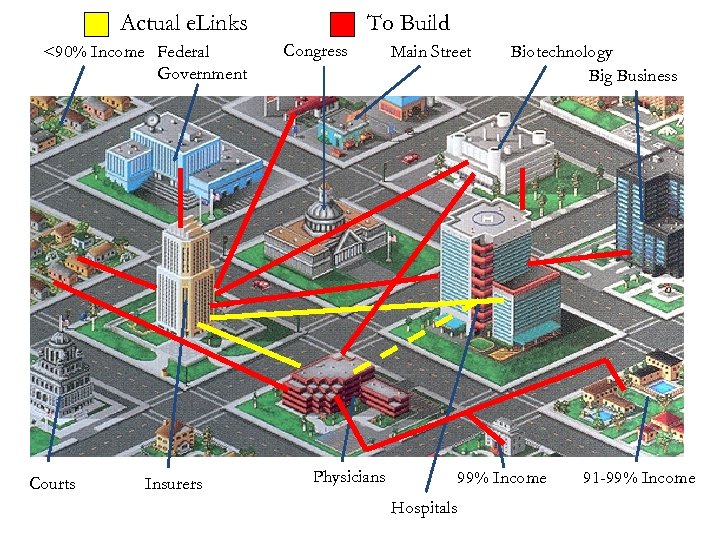 Actual e. Links <90% Income Federal Government Courts Insurers To Build Congress Main Street Physicians Biotechnology Big Business 99% Income Hospitals 91 -99% Income
Actual e. Links <90% Income Federal Government Courts Insurers To Build Congress Main Street Physicians Biotechnology Big Business 99% Income Hospitals 91 -99% Income
 Chasm Recommendation #9 • “Congress, the executive branch, leaders of health care organizations, public and private purchasers, and health informatics associations and vendors should make a renewed national commitment to building an information infrastructure to support health care delivery, consumer health, quality measurement and improvement, public accountability, clinical and health services research, and clinical education. This commitment should lead to the elimination of most handwritten clinical data by the end of the decade. ” • In short, Health IT is good. • IT is a necessary, but not sufficient asset for a 21 st century delivery system.
Chasm Recommendation #9 • “Congress, the executive branch, leaders of health care organizations, public and private purchasers, and health informatics associations and vendors should make a renewed national commitment to building an information infrastructure to support health care delivery, consumer health, quality measurement and improvement, public accountability, clinical and health services research, and clinical education. This commitment should lead to the elimination of most handwritten clinical data by the end of the decade. ” • In short, Health IT is good. • IT is a necessary, but not sufficient asset for a 21 st century delivery system.
 Insurer’s IT Paradox • They are being held accountable for an insured patient’s total care. • Best breadth of data – Most all places of service – ‘Standardized’ data • Worst detail – No clinical info on patient health status and outcomes.
Insurer’s IT Paradox • They are being held accountable for an insured patient’s total care. • Best breadth of data – Most all places of service – ‘Standardized’ data • Worst detail – No clinical info on patient health status and outcomes.
 Insurers’ Role in Health Information Technology • They are the ‘links’ that connect to everything about a patient in an electronic form. – Employers – Providers – Patients – Government agencies – Researchers
Insurers’ Role in Health Information Technology • They are the ‘links’ that connect to everything about a patient in an electronic form. – Employers – Providers – Patients – Government agencies – Researchers
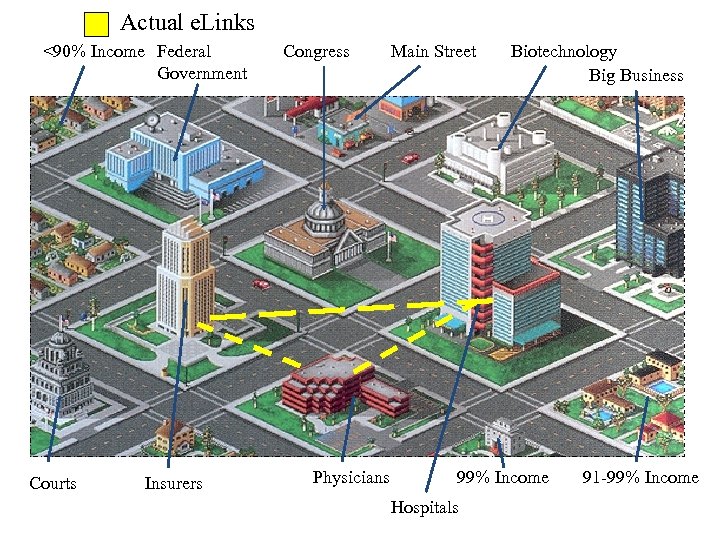 Actual e. Links <90% Income Federal Government Courts Insurers Congress Physicians Main Street Biotechnology Big Business 99% Income Hospitals 91 -99% Income
Actual e. Links <90% Income Federal Government Courts Insurers Congress Physicians Main Street Biotechnology Big Business 99% Income Hospitals 91 -99% Income
 HEALTH INSURANCE CLAIM FORM
HEALTH INSURANCE CLAIM FORM
 Insurance Database Architecture • • Claims Membership Provider files Case management Utilization review / Demand Management Decision-support databases Analytic / Financial data
Insurance Database Architecture • • Claims Membership Provider files Case management Utilization review / Demand Management Decision-support databases Analytic / Financial data
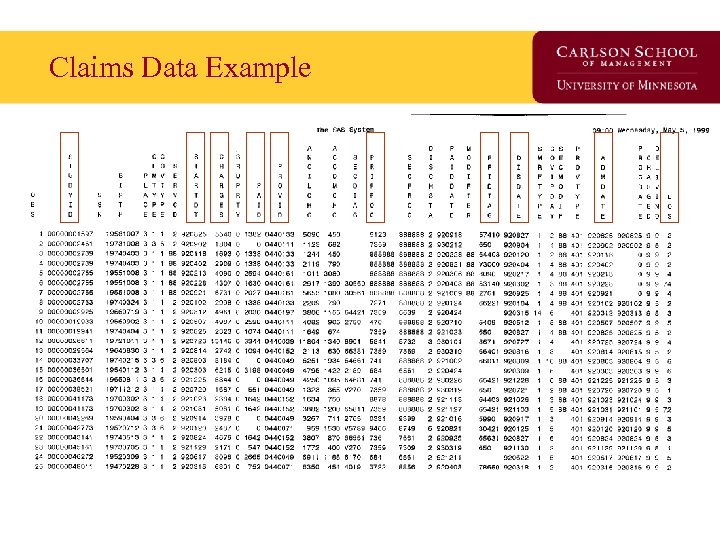 Claims Data Example
Claims Data Example
 Medical Data Collection - 1 • Operational data: Transaction-oriented – Hospital pharmacies – Laboratories – Radiology departments – Critical care units – Order-processing units
Medical Data Collection - 1 • Operational data: Transaction-oriented – Hospital pharmacies – Laboratories – Radiology departments – Critical care units – Order-processing units
 Code Systems Standards - 1 • HL 7 - American National Standards Institute Health Level – Patient registration data – Patient orders – Clinical information (e. g. , vital signs) – Referral information – Clinical trial data – Other operational transactions
Code Systems Standards - 1 • HL 7 - American National Standards Institute Health Level – Patient registration data – Patient orders – Clinical information (e. g. , vital signs) – Referral information – Clinical trial data – Other operational transactions
 Code Systems Standards - 2 • Diagnoses: International Classification of Diseases, Version 9 (ICD 9) • Procedures: Current Procedural Terminology, Version 4 (CPT 4) • Drugs: Food and Drug Administration’s Nation Drug Code (NDC) directory
Code Systems Standards - 2 • Diagnoses: International Classification of Diseases, Version 9 (ICD 9) • Procedures: Current Procedural Terminology, Version 4 (CPT 4) • Drugs: Food and Drug Administration’s Nation Drug Code (NDC) directory
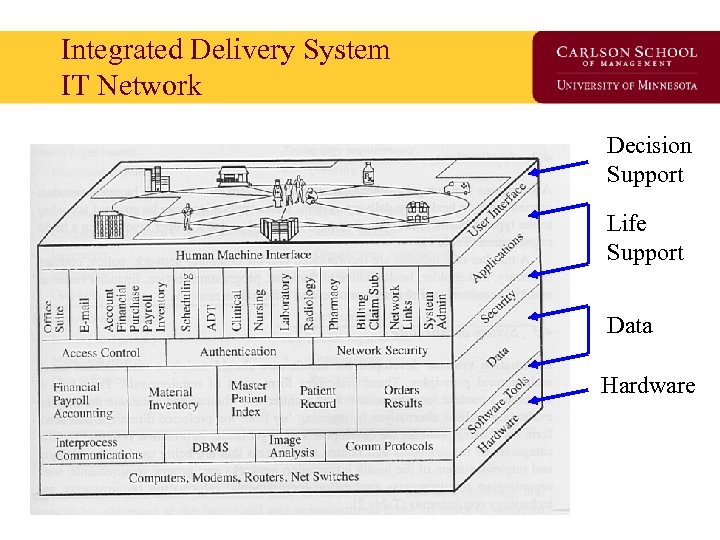 Integrated Delivery System IT Network Decision Support Life Support Data Hardware
Integrated Delivery System IT Network Decision Support Life Support Data Hardware
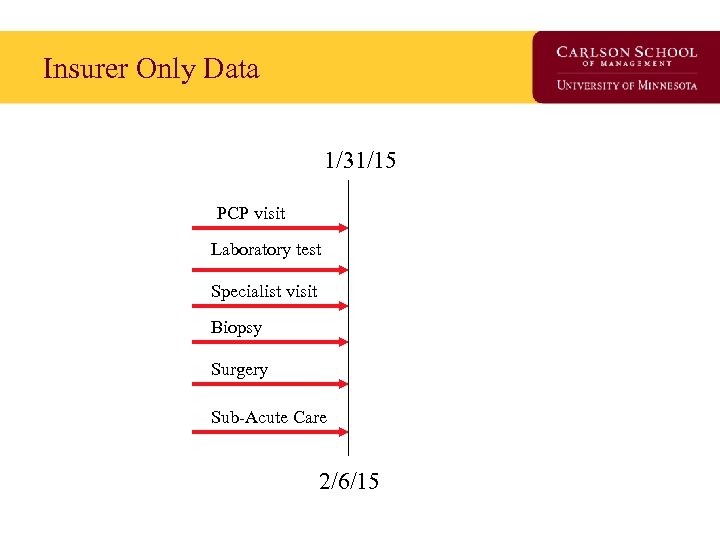 Insurer Only Data 1/31/15 PCP visit Laboratory test Specialist visit Biopsy Surgery Sub-Acute Care 2/6/15
Insurer Only Data 1/31/15 PCP visit Laboratory test Specialist visit Biopsy Surgery Sub-Acute Care 2/6/15
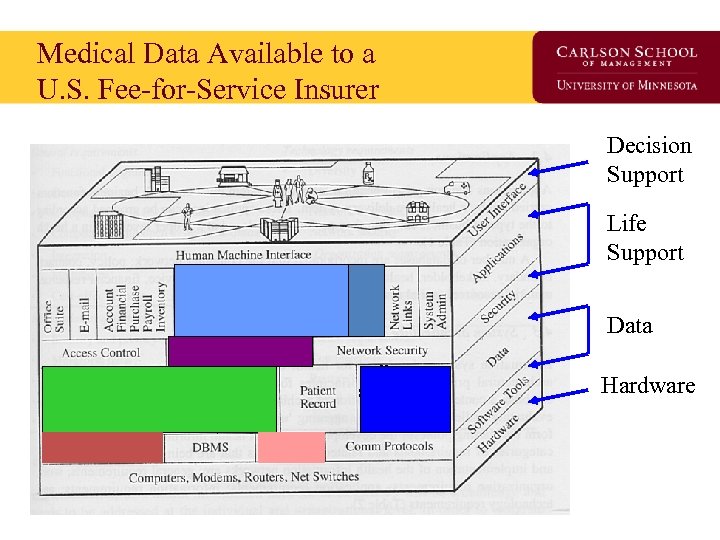 Medical Data Available to a U. S. Fee-for-Service Insurer Decision Support Life Support Data Hardware
Medical Data Available to a U. S. Fee-for-Service Insurer Decision Support Life Support Data Hardware
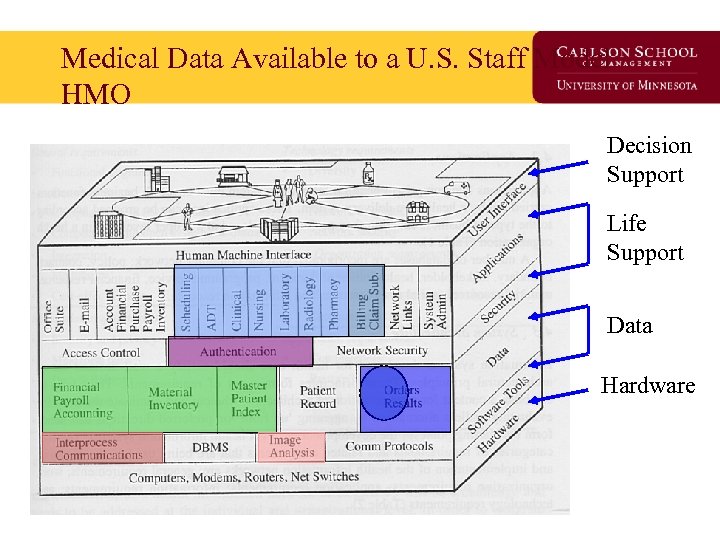 Medical Data Available to a U. S. Staff Model HMO Decision Support Life Support Data Hardware
Medical Data Available to a U. S. Staff Model HMO Decision Support Life Support Data Hardware
 Provider Only Data 1/31/15 Referral to specialist White blood cell count high Cancer metastasized Malignant cancer remains 2/6/15
Provider Only Data 1/31/15 Referral to specialist White blood cell count high Cancer metastasized Malignant cancer remains 2/6/15
 Data Available to the Average Medical Provider About a Patient’s Care 10% of Care 25% of Care 15% of Care 35% of Care
Data Available to the Average Medical Provider About a Patient’s Care 10% of Care 25% of Care 15% of Care 35% of Care
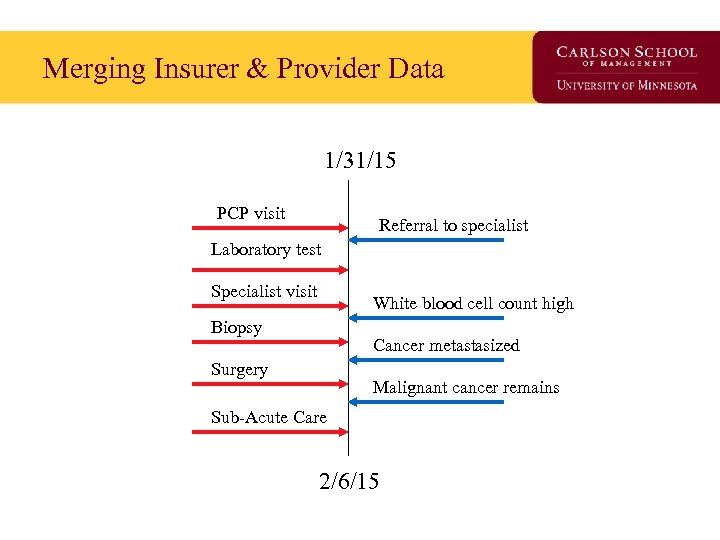 Merging Insurer & Provider Data 1/31/15 PCP visit Referral to specialist Laboratory test Specialist visit White blood cell count high Biopsy Cancer metastasized Surgery Malignant cancer remains Sub-Acute Care 2/6/15
Merging Insurer & Provider Data 1/31/15 PCP visit Referral to specialist Laboratory test Specialist visit White blood cell count high Biopsy Cancer metastasized Surgery Malignant cancer remains Sub-Acute Care 2/6/15
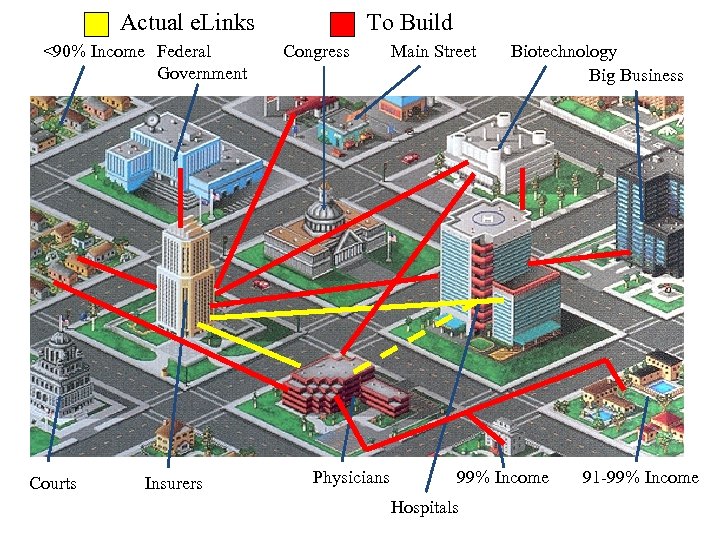 Actual e. Links <90% Income Federal Government Courts Insurers To Build Congress Physicians Main Street Biotechnology Big Business 99% Income Hospitals 91 -99% Income
Actual e. Links <90% Income Federal Government Courts Insurers To Build Congress Physicians Main Street Biotechnology Big Business 99% Income Hospitals 91 -99% Income
 Harnessing Health Information in Real Time Stephen T. Parente, Ph. D. Professor, Department of Finance Director, Medical Industry Leadership Institute Adjunct Scholar, AEI
Harnessing Health Information in Real Time Stephen T. Parente, Ph. D. Professor, Department of Finance Director, Medical Industry Leadership Institute Adjunct Scholar, AEI
 Harnessing Health Information in Real Time: Back to the Future for a More Practical and Effective Infrastructure • • • The Road to the Current Health IT initiative The Fable of the Trojan Rabbit EMR Parallel Universes & Flux Capacitors Cheaper than Bribery: Retool current infrastructure How Real Time Health IT may affect care & insurance • Short List of Pragmatic Health IT Policy Prescriptions
Harnessing Health Information in Real Time: Back to the Future for a More Practical and Effective Infrastructure • • • The Road to the Current Health IT initiative The Fable of the Trojan Rabbit EMR Parallel Universes & Flux Capacitors Cheaper than Bribery: Retool current infrastructure How Real Time Health IT may affect care & insurance • Short List of Pragmatic Health IT Policy Prescriptions
 The Road to ARRA Funded Health IT-1 • 1991: HHS Secretary Sullivan proposes Health IT infrastructure improvements. • 1993: Health Security Act includes provisions for modernized Health IT infrastructure: TBD • 1996: HIPAA – Kennedy-Kassenbaum mandates health insurance standard and advocates for electronic medical record standard by next decade • 1998: David Brailer, Ph. D, MD starts Care Science, Inc. and proposes health IT data ‘interoperability’ between medical practices using financial services firms as paradigm.
The Road to ARRA Funded Health IT-1 • 1991: HHS Secretary Sullivan proposes Health IT infrastructure improvements. • 1993: Health Security Act includes provisions for modernized Health IT infrastructure: TBD • 1996: HIPAA – Kennedy-Kassenbaum mandates health insurance standard and advocates for electronic medical record standard by next decade • 1998: David Brailer, Ph. D, MD starts Care Science, Inc. and proposes health IT data ‘interoperability’ between medical practices using financial services firms as paradigm.
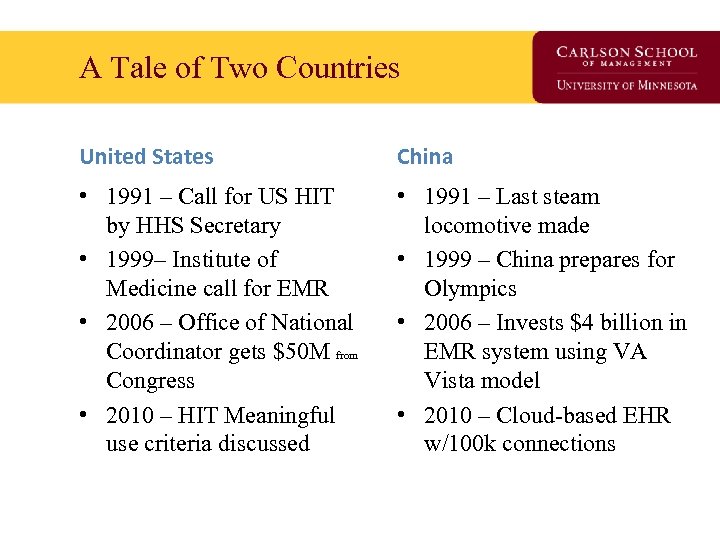 A Tale of Two Countries United States China • 1991 – Call for US HIT by HHS Secretary • 1999– Institute of Medicine call for EMR • 2006 – Office of National Coordinator gets $50 M from Congress • 2010 – HIT Meaningful use criteria discussed • 1991 – Last steam locomotive made • 1999 – China prepares for Olympics • 2006 – Invests $4 billion in EMR system using VA Vista model • 2010 – Cloud-based EHR w/100 k connections
A Tale of Two Countries United States China • 1991 – Call for US HIT by HHS Secretary • 1999– Institute of Medicine call for EMR • 2006 – Office of National Coordinator gets $50 M from Congress • 2010 – HIT Meaningful use criteria discussed • 1991 – Last steam locomotive made • 1999 – China prepares for Olympics • 2006 – Invests $4 billion in EMR system using VA Vista model • 2010 – Cloud-based EHR w/100 k connections
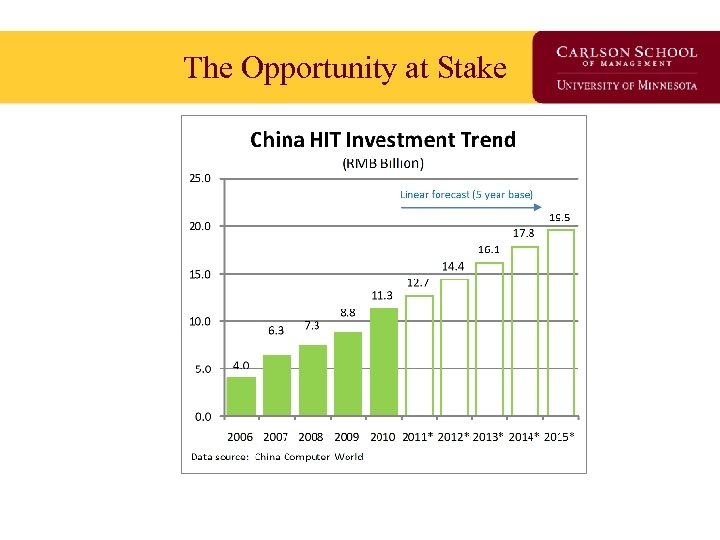 The Opportunity at Stake
The Opportunity at Stake
 What if No One Wants a Trojan Rabbit? • Sir Bedivere the Wise: “Now once we have gotten all the physicians to buy a ARRA-financed Dell computers from Wal Mart for an EMR/EHR install, we can distribute the software to them to place more data entry onto their existing workflow and then pay them less when we use the Meaningful Use criteria to tell them they are under-performing in their new medical home or Accountable Care Organization CMS Pilot. ”
What if No One Wants a Trojan Rabbit? • Sir Bedivere the Wise: “Now once we have gotten all the physicians to buy a ARRA-financed Dell computers from Wal Mart for an EMR/EHR install, we can distribute the software to them to place more data entry onto their existing workflow and then pay them less when we use the Meaningful Use criteria to tell them they are under-performing in their new medical home or Accountable Care Organization CMS Pilot. ”
 Some Napkin Calculations • Assume $34 billion ARRA HIT funds goes only to doctors: – $68, 000 per physician • Buy hardware & software • Offset training and indirect cost learning expense • Compared to cost of malpractice premiums: – In 2002 in Dade County, FL (granted – higher then ave. ): • $56, 153 (internal medicine) • $174, 268 (general surgery) • $201, 376 (OB/GYN) • Bonus from HIT!!! EMR produces terabytes of discoverable data for medical malpractice.
Some Napkin Calculations • Assume $34 billion ARRA HIT funds goes only to doctors: – $68, 000 per physician • Buy hardware & software • Offset training and indirect cost learning expense • Compared to cost of malpractice premiums: – In 2002 in Dade County, FL (granted – higher then ave. ): • $56, 153 (internal medicine) • $174, 268 (general surgery) • $201, 376 (OB/GYN) • Bonus from HIT!!! EMR produces terabytes of discoverable data for medical malpractice.
 Let’s Rev Up the Flux Capacitor “When the Medicare Debt Hits $88 trillion you’re going to see some serious…debt reduction commissions”
Let’s Rev Up the Flux Capacitor “When the Medicare Debt Hits $88 trillion you’re going to see some serious…debt reduction commissions”
 Parallel Universe Number One • Veteran Administration (Vist. A) System • Started 25+ years ago • Has received $8 billion • Links 153 hospitals • Links 768 outpatient clinics & pharmacy • Real-time access • Add-ins: Indian Health Service, DOD military hospitals
Parallel Universe Number One • Veteran Administration (Vist. A) System • Started 25+ years ago • Has received $8 billion • Links 153 hospitals • Links 768 outpatient clinics & pharmacy • Real-time access • Add-ins: Indian Health Service, DOD military hospitals
 Parallel Universe Number Two • Financial Services industry – Started 25 years ago too – ATM transfers was key – Electronic credits cards were rife with fraud by early 1990 s – Created fraud scoring technologies & data to flag suspicious transactions in real-time – Data was siloed like HIT – Led to FOUR near-time repositories of all financial services data.
Parallel Universe Number Two • Financial Services industry – Started 25 years ago too – ATM transfers was key – Electronic credits cards were rife with fraud by early 1990 s – Created fraud scoring technologies & data to flag suspicious transactions in real-time – Data was siloed like HIT – Led to FOUR near-time repositories of all financial services data.
 Applying Financials Services Lessons to Stop Health Care Fraud B 4 Payment Terra. Medica’ fraud and abuse identification and prevention solutions can be plugged into virtually any point in the healthcare value chain P a g e 4 Need to identify fraud and abuse and stop payment. This is the only way to get the savings from fraud & abuse prevention activities at an industrial scale with verifiable outcomes. Can plug in intervention before or after payment by an insurer / Medicare / Medicaid. Ideally, you want to not pay a fraudulent claim.
Applying Financials Services Lessons to Stop Health Care Fraud B 4 Payment Terra. Medica’ fraud and abuse identification and prevention solutions can be plugged into virtually any point in the healthcare value chain P a g e 4 Need to identify fraud and abuse and stop payment. This is the only way to get the savings from fraud & abuse prevention activities at an industrial scale with verifiable outcomes. Can plug in intervention before or after payment by an insurer / Medicare / Medicaid. Ideally, you want to not pay a fraudulent claim.
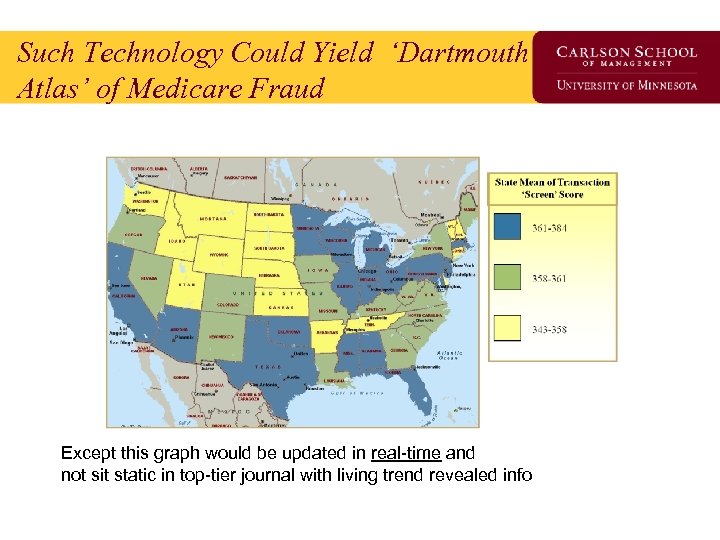 Such Technology Could Yield ‘Dartmouth Atlas’ of Medicare Fraud Except this graph would be updated in real-time and not sit static in top-tier journal with living trend revealed info Page 42
Such Technology Could Yield ‘Dartmouth Atlas’ of Medicare Fraud Except this graph would be updated in real-time and not sit static in top-tier journal with living trend revealed info Page 42
 Instead of Bribery Tap Existing Tech Infrastructure for Health Reform 1) Get actuarially certified risk profiles for all insured based on existing data. Let people get them like a they would a credit report. Equifax and Experian are standing by and waiting for the go-switch. 2) Government and private federal exchanges portals. Take risk profiles from (1) and provide a ‘lock in’ by Internet click. Target the younger population not buying coverage today through the web. Have brokers handle the rest. Gives brokers time to get a Plan B. 3) Where the market fails from (2), auction off the high risk Given (1) and (2), who are the vulnerable and why Target resources to fill the insurance gaps using federal and state resources. 4) Let the Employer-sponsored market evolve; it’s not broken.
Instead of Bribery Tap Existing Tech Infrastructure for Health Reform 1) Get actuarially certified risk profiles for all insured based on existing data. Let people get them like a they would a credit report. Equifax and Experian are standing by and waiting for the go-switch. 2) Government and private federal exchanges portals. Take risk profiles from (1) and provide a ‘lock in’ by Internet click. Target the younger population not buying coverage today through the web. Have brokers handle the rest. Gives brokers time to get a Plan B. 3) Where the market fails from (2), auction off the high risk Given (1) and (2), who are the vulnerable and why Target resources to fill the insurance gaps using federal and state resources. 4) Let the Employer-sponsored market evolve; it’s not broken.
 Instead of Bribery Tap Existing Technology and Infrastructure Insurers Providers • Let your systems be the conduits and record locators of clinical data. • Sell/spin off or lease too data marts and sell retail insurance services in exchanges. • Use coming ANSI X 12 standard with ICD 10 to harmonize all platforms • Attach clinical data to billing records in return for prompt (<3 day to seconds) pay for ambulatory care. • Stop customizing and get your data on an ICD 10 compliant cloud. • Walk away from ACO mutually assured destruction
Instead of Bribery Tap Existing Technology and Infrastructure Insurers Providers • Let your systems be the conduits and record locators of clinical data. • Sell/spin off or lease too data marts and sell retail insurance services in exchanges. • Use coming ANSI X 12 standard with ICD 10 to harmonize all platforms • Attach clinical data to billing records in return for prompt (<3 day to seconds) pay for ambulatory care. • Stop customizing and get your data on an ICD 10 compliant cloud. • Walk away from ACO mutually assured destruction
 How might this Real Time HIT operate in the ideal world? Consider Anna a consumer with a diabetes. 1. On January 1, 2016, she begins health coverage in a new health plan with Real Time HIT technology, an Integrated Health Card (IHC). 2. The IHC web site provides a list of endocrinologists accepting patients in her area and quality scores for providers as well as those accepting IHC. 3. Prior to the visit, the Anna logs onto a secure IHC web site from the health plan to verify her eligibility and requests her previous pharmacy history from a different health plan. 4. When she visits the endocrinologist, the physician’s assistant swipes the health card using a USB swipe card machine connected to the Internet. 5. The physician sees on the IHC web site that the patient has already authorized the provider to review her past history. The physician reviews all prior drug history and proceeds to conduct an initial evaluation with some sense of patient compliance with medications for a chronic illness as well as prior dosing. 6. During the visit, the physician orders tests for Glycosylated Hemoglobin, blood sugar, and creatinine - records blood pressure, weight and height.
How might this Real Time HIT operate in the ideal world? Consider Anna a consumer with a diabetes. 1. On January 1, 2016, she begins health coverage in a new health plan with Real Time HIT technology, an Integrated Health Card (IHC). 2. The IHC web site provides a list of endocrinologists accepting patients in her area and quality scores for providers as well as those accepting IHC. 3. Prior to the visit, the Anna logs onto a secure IHC web site from the health plan to verify her eligibility and requests her previous pharmacy history from a different health plan. 4. When she visits the endocrinologist, the physician’s assistant swipes the health card using a USB swipe card machine connected to the Internet. 5. The physician sees on the IHC web site that the patient has already authorized the provider to review her past history. The physician reviews all prior drug history and proceeds to conduct an initial evaluation with some sense of patient compliance with medications for a chronic illness as well as prior dosing. 6. During the visit, the physician orders tests for Glycosylated Hemoglobin, blood sugar, and creatinine - records blood pressure, weight and height.
 Anna’s Story - 2 7. 8. 9. 10. 11. 12. The physician’s assistant bills for an initial evaluation on the IHC web site which requests standard claims data as well as the patient’s height, weight and blood pressure Since the patient’s eligibility information is already known the allowed amount for the initial consultation is transferred directly to the physician’s practice business account. The patient sees the endocrinologist four more times during the year and keeps recording stable or improving lab values. At the end of year, the health plan invites the patient to comment on quality of care she has received since her Hb. A 1 c scores improved. If she comments, she will receive either a reduction in her co-insurance rate or a credit to her health savings/reimbursement account if she is enrolled in a consumer directed health plan. Anna decides to shop for a new health plan using her IHC data with clinical information, preferences and comments, and lab values. She finds she can get a 15% discount from another plan because of her healthy habits as a diabetic patient. She decides to take the new plan and keeps her IHC. The only changes are the designation of her health plan and eligibility criteria as well as the plan’s provider panel.
Anna’s Story - 2 7. 8. 9. 10. 11. 12. The physician’s assistant bills for an initial evaluation on the IHC web site which requests standard claims data as well as the patient’s height, weight and blood pressure Since the patient’s eligibility information is already known the allowed amount for the initial consultation is transferred directly to the physician’s practice business account. The patient sees the endocrinologist four more times during the year and keeps recording stable or improving lab values. At the end of year, the health plan invites the patient to comment on quality of care she has received since her Hb. A 1 c scores improved. If she comments, she will receive either a reduction in her co-insurance rate or a credit to her health savings/reimbursement account if she is enrolled in a consumer directed health plan. Anna decides to shop for a new health plan using her IHC data with clinical information, preferences and comments, and lab values. She finds she can get a 15% discount from another plan because of her healthy habits as a diabetic patient. She decides to take the new plan and keeps her IHC. The only changes are the designation of her health plan and eligibility criteria as well as the plan’s provider panel.
 Closing Thoughts • Other than official deadlines when providers will be penalized for not having purchased the right health IT solution, little transparent and measurable progress is being made right now. • Currently, there is no proactive sophisticated, effective, and efficient fraud-prevention solution in the health care industry. • To succeed with health IT, we need to go back to the future before “bribed interoperability” became the latest policy prescription. • Real-time health IT, if widespread, could break the oligopolistic control of health data by providers and insurers.
Closing Thoughts • Other than official deadlines when providers will be penalized for not having purchased the right health IT solution, little transparent and measurable progress is being made right now. • Currently, there is no proactive sophisticated, effective, and efficient fraud-prevention solution in the health care industry. • To succeed with health IT, we need to go back to the future before “bribed interoperability” became the latest policy prescription. • Real-time health IT, if widespread, could break the oligopolistic control of health data by providers and insurers.


