0b76e39bdb89a4d1b78c7ef272e5f2d5.ppt
- Количество слайдов: 55
 TTN vs. TTT (Time to Transport): Assessment of Neonatal Respiratory Distress Children’s/March of Dimes Neonatal Conference May 17, 2010 Mark Bergeron, MD, MPH Associates in Newborn Medicine, PA, St. Paul Assistant Professor, Pediatrics, University of Minnesota Medical School
TTN vs. TTT (Time to Transport): Assessment of Neonatal Respiratory Distress Children’s/March of Dimes Neonatal Conference May 17, 2010 Mark Bergeron, MD, MPH Associates in Newborn Medicine, PA, St. Paul Assistant Professor, Pediatrics, University of Minnesota Medical School
 Disclosures • I will not be discussing any experimental or off-label uses for any therapies during this presentation. • I have no relevant financial relationships to declare.
Disclosures • I will not be discussing any experimental or off-label uses for any therapies during this presentation. • I have no relevant financial relationships to declare.
 Objectives 1. Formulate a differential diagnosis for the infant in respiratory distress. 2. Describe initial stabilization measures for the infant in respiratory distress. 3. Describe situations where ongoing respiratory distress requires transfer to a NICU for further management.
Objectives 1. Formulate a differential diagnosis for the infant in respiratory distress. 2. Describe initial stabilization measures for the infant in respiratory distress. 3. Describe situations where ongoing respiratory distress requires transfer to a NICU for further management.

 Introduction • Respiratory distress is a frequent problem in the newborn period. – Most common indication for evaluation or reevaluation of the newborn infant – Affects as many as 7% of newborns – Potentially life-threatening – Must be promptly assessed and managed by an on-site provider in the delivery room or newborn nursery
Introduction • Respiratory distress is a frequent problem in the newborn period. – Most common indication for evaluation or reevaluation of the newborn infant – Affects as many as 7% of newborns – Potentially life-threatening – Must be promptly assessed and managed by an on-site provider in the delivery room or newborn nursery
 Clinical Presentation • • • apnea cyanosis grunting stridor nasal flaring • retractions – subcostal – intercostal – suprasternal • tachypnea – (> 60/min) • gasping • choking
Clinical Presentation • • • apnea cyanosis grunting stridor nasal flaring • retractions – subcostal – intercostal – suprasternal • tachypnea – (> 60/min) • gasping • choking
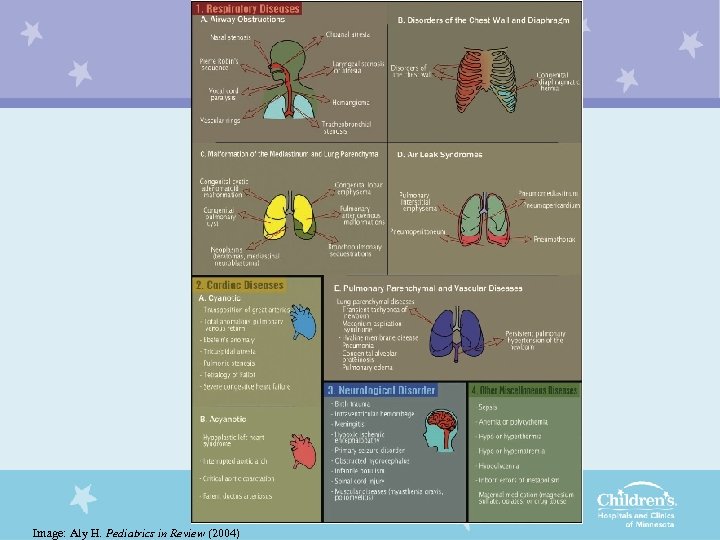 Image: Aly H. Pediatrics in Review (2004)
Image: Aly H. Pediatrics in Review (2004)
 Narrowing the Differential • Pulmonary – Transient Tachypnea of the Newborn (TTN) – Respiratory Distress Syndrome (RDS) – Meconium aspiration syndrome – Pneumonia/sepsis – Pneumothorax – Persistent pulmonary hypertension (PPHN) • Non-pulmonary – Congenital cyanotic heart disease – Congenital airway anomalies – Other (neurologic, hematologic, metabolic, endocrine, maternal, etc. )
Narrowing the Differential • Pulmonary – Transient Tachypnea of the Newborn (TTN) – Respiratory Distress Syndrome (RDS) – Meconium aspiration syndrome – Pneumonia/sepsis – Pneumothorax – Persistent pulmonary hypertension (PPHN) • Non-pulmonary – Congenital cyanotic heart disease – Congenital airway anomalies – Other (neurologic, hematologic, metabolic, endocrine, maternal, etc. )
 Case Studies
Case Studies
 Case #1 • 3. 6 -kg term newborn female (20 minutes old) has tachypnea and acrocyanosis. She is 40 weeks EGA delivered by scheduled repeat c-section and Apgar scores were 7 and 8 at 1 and 5 minutes, respectively. • Vitals are normal with the exception of a respiratory rate of 84 and exam is notable for slight subcostal retractions but otherwise normal. Over the next several hours, her respiratory rate steadily improves to the 40 s and her acrocyanosis resolves.
Case #1 • 3. 6 -kg term newborn female (20 minutes old) has tachypnea and acrocyanosis. She is 40 weeks EGA delivered by scheduled repeat c-section and Apgar scores were 7 and 8 at 1 and 5 minutes, respectively. • Vitals are normal with the exception of a respiratory rate of 84 and exam is notable for slight subcostal retractions but otherwise normal. Over the next several hours, her respiratory rate steadily improves to the 40 s and her acrocyanosis resolves.
 Transient Tachypnea of the Newborn (TTN) • Most common etiology of newborn respiratory distress. – 11/1000 live births – Represents 40% of cases of newborn respiratory distress. • Caused by delayed clearance of fetal lung fluid in both term and preterm infants
Transient Tachypnea of the Newborn (TTN) • Most common etiology of newborn respiratory distress. – 11/1000 live births – Represents 40% of cases of newborn respiratory distress. • Caused by delayed clearance of fetal lung fluid in both term and preterm infants
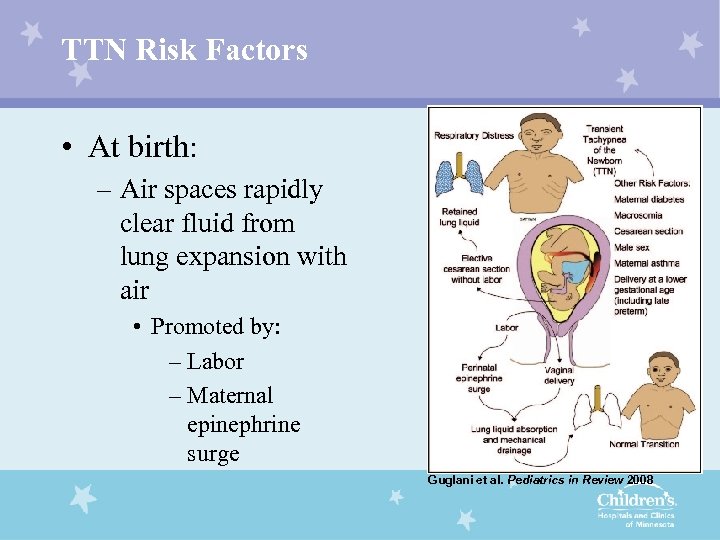 TTN Risk Factors • At birth: – Air spaces rapidly clear fluid from lung expansion with air • Promoted by: – Labor – Maternal epinephrine surge Guglani et al. Pediatrics in Review 2008
TTN Risk Factors • At birth: – Air spaces rapidly clear fluid from lung expansion with air • Promoted by: – Labor – Maternal epinephrine surge Guglani et al. Pediatrics in Review 2008
 TTN: Clinical Findings • History: – C/S > NSVD • Exam: – Tachypnea +/ • Grunting • Nasal flaring • Retractions • Transient oxygen need • Lab: – Mild respiratory acidosis or normal blood gas
TTN: Clinical Findings • History: – C/S > NSVD • Exam: – Tachypnea +/ • Grunting • Nasal flaring • Retractions • Transient oxygen need • Lab: – Mild respiratory acidosis or normal blood gas
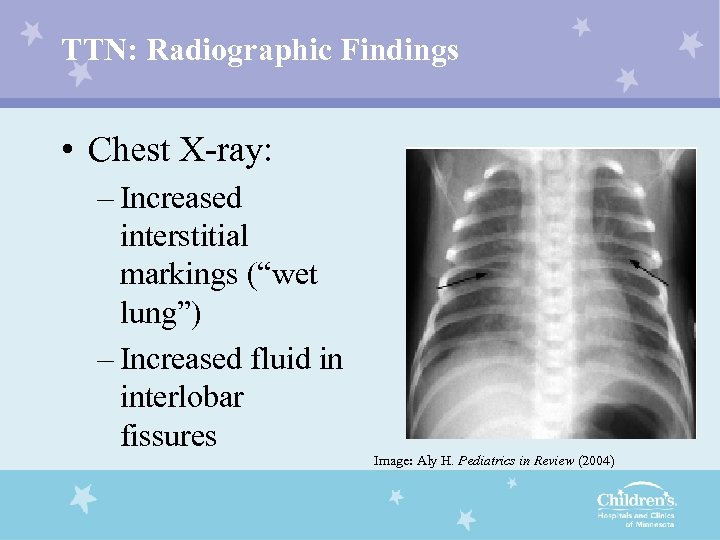 TTN: Radiographic Findings • Chest X-ray: – Increased interstitial markings (“wet lung”) – Increased fluid in interlobar fissures Image: Aly H. Pediatrics in Review (2004)
TTN: Radiographic Findings • Chest X-ray: – Increased interstitial markings (“wet lung”) – Increased fluid in interlobar fissures Image: Aly H. Pediatrics in Review (2004)
 TTN: Typical Course • Usually benign, self • Diuretics not -limited effective • Occasionally – i. e. Lasix requires therapy: • Typically resolves – Oxygen by 2 days of age – n. CPAP • No lasting sequalae – Mechanical ventilation
TTN: Typical Course • Usually benign, self • Diuretics not -limited effective • Occasionally – i. e. Lasix requires therapy: • Typically resolves – Oxygen by 2 days of age – n. CPAP • No lasting sequalae – Mechanical ventilation
 Case #2 • 1. 2 -kg male infant born vaginally at 32 weeks EGA • Apgars 6, 8 • Required bulb suctioning, brief PPV. • Grunting, retractions, nasal flaring, acrocyanosis immediately after birth. • VS: HR 178, RR 79, Mean BP 39 mm. Hg. O 2 sat 74 -78% in room air.
Case #2 • 1. 2 -kg male infant born vaginally at 32 weeks EGA • Apgars 6, 8 • Required bulb suctioning, brief PPV. • Grunting, retractions, nasal flaring, acrocyanosis immediately after birth. • VS: HR 178, RR 79, Mean BP 39 mm. Hg. O 2 sat 74 -78% in room air.
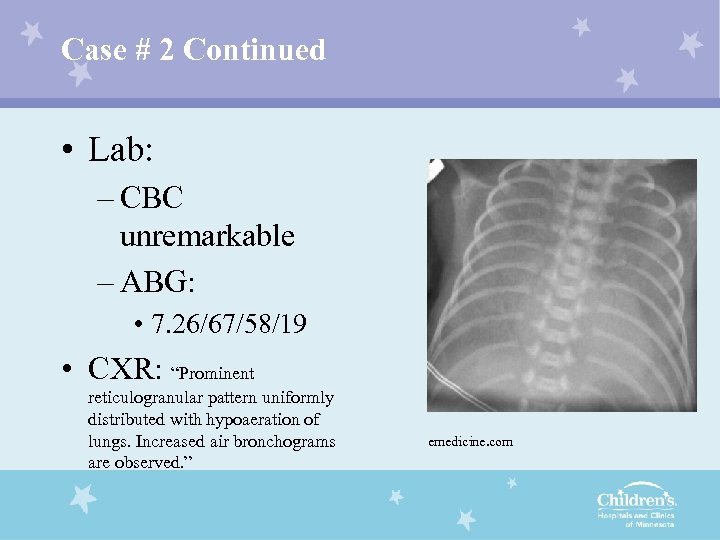 Case # 2 Continued • Lab: – CBC unremarkable – ABG: • 7. 26/67/58/19 • CXR: “Prominent reticulogranular pattern uniformly distributed with hypoaeration of lungs. Increased air bronchograms are observed. ” emedicine. com
Case # 2 Continued • Lab: – CBC unremarkable – ABG: • 7. 26/67/58/19 • CXR: “Prominent reticulogranular pattern uniformly distributed with hypoaeration of lungs. Increased air bronchograms are observed. ” emedicine. com
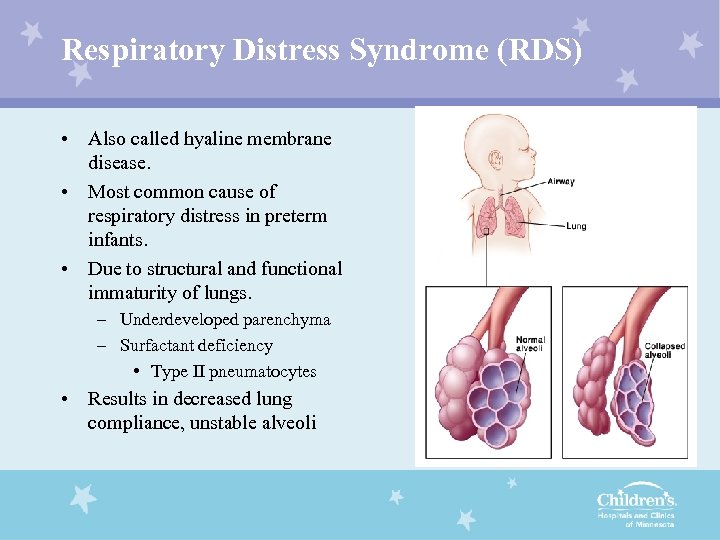 Respiratory Distress Syndrome (RDS) • Also called hyaline membrane disease. • Most common cause of respiratory distress in preterm infants. • Due to structural and functional immaturity of lungs. – Underdeveloped parenchyma – Surfactant deficiency • Type II pneumatocytes • Results in decreased lung compliance, unstable alveoli
Respiratory Distress Syndrome (RDS) • Also called hyaline membrane disease. • Most common cause of respiratory distress in preterm infants. • Due to structural and functional immaturity of lungs. – Underdeveloped parenchyma – Surfactant deficiency • Type II pneumatocytes • Results in decreased lung compliance, unstable alveoli
 RDS Continued • Risk factors – Prematurity • <28 weeks GA (≈100%) • 28 -34 weeks GA (33%) • >34 weeks GA (5%) – Perinatal depression – Male predominance – Maternal diabetes – C-section – Multiple birth
RDS Continued • Risk factors – Prematurity • <28 weeks GA (≈100%) • 28 -34 weeks GA (33%) • >34 weeks GA (5%) – Perinatal depression – Male predominance – Maternal diabetes – C-section – Multiple birth
 Respiratory Distress Syndrome: Clinical Finings • • Exam: – Moderate to severe respiratory distress • Tachypnea • Grunting • Apnea • Retractions • Nasal flaring • Cyanosis Lab: – Moderate hypoxia – Respiratory acidosis – Metabolic acidosis (delayed) • X-ray: – Low lung volumes – Diffuse atelectasis: “ground glass opacities” – Air bronchograms – Difficult to distinguish from pneumonia emedicine. com
Respiratory Distress Syndrome: Clinical Finings • • Exam: – Moderate to severe respiratory distress • Tachypnea • Grunting • Apnea • Retractions • Nasal flaring • Cyanosis Lab: – Moderate hypoxia – Respiratory acidosis – Metabolic acidosis (delayed) • X-ray: – Low lung volumes – Diffuse atelectasis: “ground glass opacities” – Air bronchograms – Difficult to distinguish from pneumonia emedicine. com
 RDS: Typical Course • • Prevention: – Antenatal bethamethasone – Arrest of preterm labor Treatment – Oxygen supplementation – Assisted ventilation • n. CPAP • mechanical ventilation – Fi. O 2 >. 40 – Exogenous surfactant replacement – Fluid restriction • Outcome – Peak severity 1 -3 days – Recovery coincides with diuresis beginning at 72 hrs – Severe cases evolve into bronchopulmonary dysplasia (chronic lung disease) • Extreme prematurity • Prolonged mechanical ventilation • Sepsis
RDS: Typical Course • • Prevention: – Antenatal bethamethasone – Arrest of preterm labor Treatment – Oxygen supplementation – Assisted ventilation • n. CPAP • mechanical ventilation – Fi. O 2 >. 40 – Exogenous surfactant replacement – Fluid restriction • Outcome – Peak severity 1 -3 days – Recovery coincides with diuresis beginning at 72 hrs – Severe cases evolve into bronchopulmonary dysplasia (chronic lung disease) • Extreme prematurity • Prolonged mechanical ventilation • Sepsis
 Case #3 • 4. 2 -kg female infant is cyanotic and tachypneic at 30 minutes of age following a vaginal delivery through meconium-stained amniotic fluid. Apgar scores were 3 and 6. She had a spontaneous but weak cry at birth and received some positive pressure ventilation followed by suctioning. • Vitals signs reveal a pulse of 169, respiratory rate of 115, and a mean BP of 55. Sats are 76% despite 100% O 2 by headbox. She is barrelchested, retracting, grunting, and has diminished coarse breath sounds bilaterally. • She is electively intubated, lines placed and labs sent.
Case #3 • 4. 2 -kg female infant is cyanotic and tachypneic at 30 minutes of age following a vaginal delivery through meconium-stained amniotic fluid. Apgar scores were 3 and 6. She had a spontaneous but weak cry at birth and received some positive pressure ventilation followed by suctioning. • Vitals signs reveal a pulse of 169, respiratory rate of 115, and a mean BP of 55. Sats are 76% despite 100% O 2 by headbox. She is barrelchested, retracting, grunting, and has diminished coarse breath sounds bilaterally. • She is electively intubated, lines placed and labs sent.
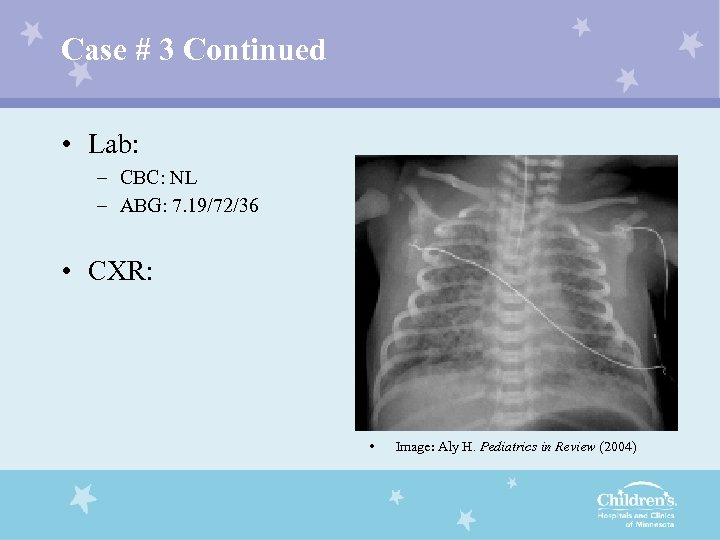 Case # 3 Continued • Lab: – CBC: NL – ABG: 7. 19/72/36 • CXR: • Image: Aly H. Pediatrics in Review (2004)
Case # 3 Continued • Lab: – CBC: NL – ABG: 7. 19/72/36 • CXR: • Image: Aly H. Pediatrics in Review (2004)
 Meconium Aspiration Syndrome (MAS) • Meconium staining of amniotic fluid complicates nearly 15% of all deliveries. – Fetal distress – Primarily term and post-term • Meconium can be aspirated before, during or after delivery. • Once aspirated, meconium causes – Chemical pneumonitis – Mechanical obstruction (“ball-valve”) with severe air-trapping • Pneumothoraces (10 -20%) – Surfactant inactivation – Severe hypoxemia and hypoventilation • V/Q mismatch
Meconium Aspiration Syndrome (MAS) • Meconium staining of amniotic fluid complicates nearly 15% of all deliveries. – Fetal distress – Primarily term and post-term • Meconium can be aspirated before, during or after delivery. • Once aspirated, meconium causes – Chemical pneumonitis – Mechanical obstruction (“ball-valve”) with severe air-trapping • Pneumothoraces (10 -20%) – Surfactant inactivation – Severe hypoxemia and hypoventilation • V/Q mismatch
 Meconium Aspiration Syndrome: Clinical Presentation • Exam: – Air trapping with barrel chest – Moderate to severe respiratory distress – Rales and/or rhonchi – Hypoxia with cyanosis – Hypoperfusion • Lab: – Acidosis • Respiratory and metabolic • CXR: – Hyperinflation/overdistensi on – Diffuse, patchy intraparenchymal opacities
Meconium Aspiration Syndrome: Clinical Presentation • Exam: – Air trapping with barrel chest – Moderate to severe respiratory distress – Rales and/or rhonchi – Hypoxia with cyanosis – Hypoperfusion • Lab: – Acidosis • Respiratory and metabolic • CXR: – Hyperinflation/overdistensi on – Diffuse, patchy intraparenchymal opacities
 Meconium Aspiration Syndrome: Typical Course • Prevention? – NRP • Treatment: – Oxygen – Mechanical ventilation • High-Frequency – Jet – Oscillator – Surfactant replacement • Complications – Sepsis/pneumonia – Airleaks • Pneumothorax/pneum opericardium – Persistent pulmonary hypertension (PPHN) • Treated with inhaled Nitric Oxide (i. NO) • ECMO • Resolution – Days to weeks – Mortality 10 -12%
Meconium Aspiration Syndrome: Typical Course • Prevention? – NRP • Treatment: – Oxygen – Mechanical ventilation • High-Frequency – Jet – Oscillator – Surfactant replacement • Complications – Sepsis/pneumonia – Airleaks • Pneumothorax/pneum opericardium – Persistent pulmonary hypertension (PPHN) • Treated with inhaled Nitric Oxide (i. NO) • ECMO • Resolution – Days to weeks – Mortality 10 -12%
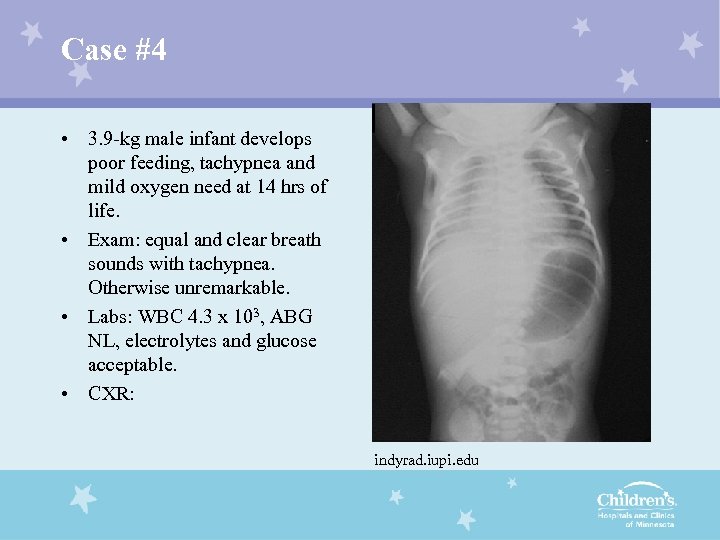 Case #4 • 3. 9 -kg male infant develops poor feeding, tachypnea and mild oxygen need at 14 hrs of life. • Exam: equal and clear breath sounds with tachypnea. Otherwise unremarkable. • Labs: WBC 4. 3 x 103, ABG NL, electrolytes and glucose acceptable. • CXR: indyrad. iupi. edu
Case #4 • 3. 9 -kg male infant develops poor feeding, tachypnea and mild oxygen need at 14 hrs of life. • Exam: equal and clear breath sounds with tachypnea. Otherwise unremarkable. • Labs: WBC 4. 3 x 103, ABG NL, electrolytes and glucose acceptable. • CXR: indyrad. iupi. edu
 Congenital Pneumonia: Clinical Presentation • Most common neonatal infection • Wide variety of presenting signs – Varying degree of respiratory distress – Lethargy, poor feeding – Apnea – Temperature instability • High or low • CXR: “Can look like anything!” – Mild focal opacities – Pleural effusion(s) – Complete white-out – Normal
Congenital Pneumonia: Clinical Presentation • Most common neonatal infection • Wide variety of presenting signs – Varying degree of respiratory distress – Lethargy, poor feeding – Apnea – Temperature instability • High or low • CXR: “Can look like anything!” – Mild focal opacities – Pleural effusion(s) – Complete white-out – Normal
 Pneumonia: Epidemiology • Hematogenous vs. aspiration acquisition • Antenatal, perinatal, or postnatally acquired • Common organisms: – Antenatal: rubella, CMV, HSV, adenovirus, Toxoplasma gondii, Treponema pallidum, Mycobacterium tuberculosis, Listeria monocytogenes, Varicella zoster and others – Perinatal: GBS, E. coli, Klebsiella, Chlamydia trachomatis – Postnatal: adenovirus, RSV, Streptococcus, Staphylococcus, gram negative enterics
Pneumonia: Epidemiology • Hematogenous vs. aspiration acquisition • Antenatal, perinatal, or postnatally acquired • Common organisms: – Antenatal: rubella, CMV, HSV, adenovirus, Toxoplasma gondii, Treponema pallidum, Mycobacterium tuberculosis, Listeria monocytogenes, Varicella zoster and others – Perinatal: GBS, E. coli, Klebsiella, Chlamydia trachomatis – Postnatal: adenovirus, RSV, Streptococcus, Staphylococcus, gram negative enterics
 Congenital Pneumonia: Typical Course • Transient oxygen need • Gradual resolution of tachypnea • Antibiotic (ampicillin, gentamicin) therapy 5 -7 days unless complicated by sepsis or for specific organism requiring longer courses of therapy
Congenital Pneumonia: Typical Course • Transient oxygen need • Gradual resolution of tachypnea • Antibiotic (ampicillin, gentamicin) therapy 5 -7 days unless complicated by sepsis or for specific organism requiring longer courses of therapy

 Other Pulmonary Causes of Respiratory Distress
Other Pulmonary Causes of Respiratory Distress
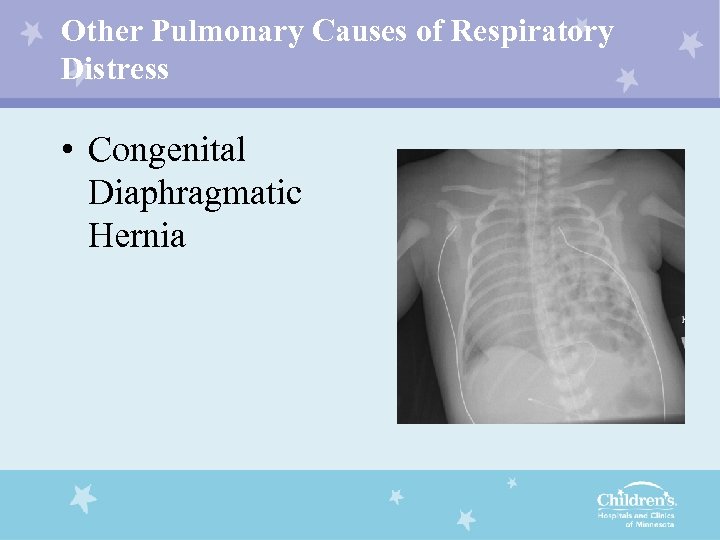 Other Pulmonary Causes of Respiratory Distress • Congenital Diaphragmatic Hernia
Other Pulmonary Causes of Respiratory Distress • Congenital Diaphragmatic Hernia
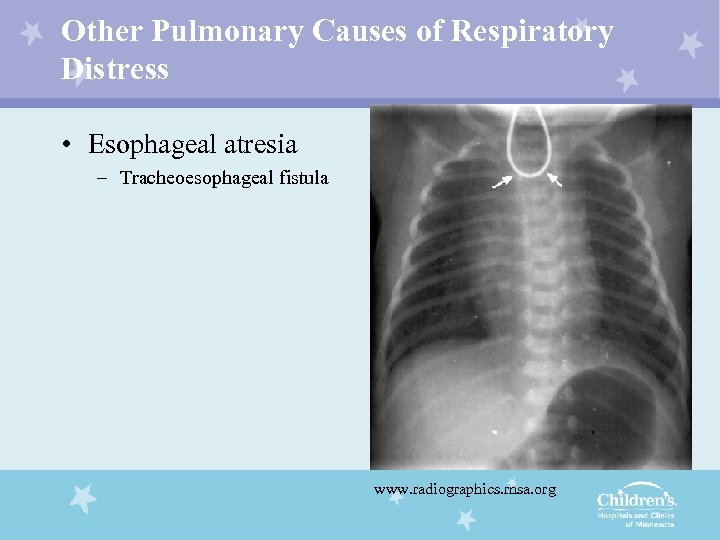 Other Pulmonary Causes of Respiratory Distress • Esophageal atresia – Tracheoesophageal fistula www. radiographics. rnsa. org
Other Pulmonary Causes of Respiratory Distress • Esophageal atresia – Tracheoesophageal fistula www. radiographics. rnsa. org
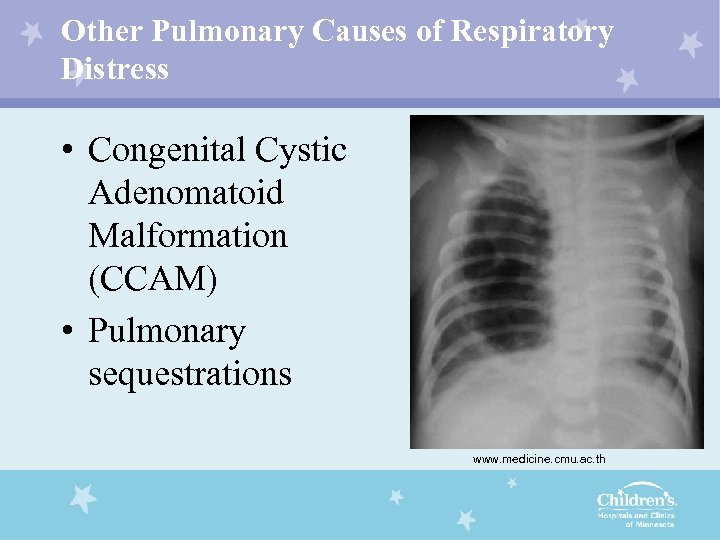 Other Pulmonary Causes of Respiratory Distress • Congenital Cystic Adenomatoid Malformation (CCAM) • Pulmonary sequestrations www. medicine. cmu. ac. th
Other Pulmonary Causes of Respiratory Distress • Congenital Cystic Adenomatoid Malformation (CCAM) • Pulmonary sequestrations www. medicine. cmu. ac. th
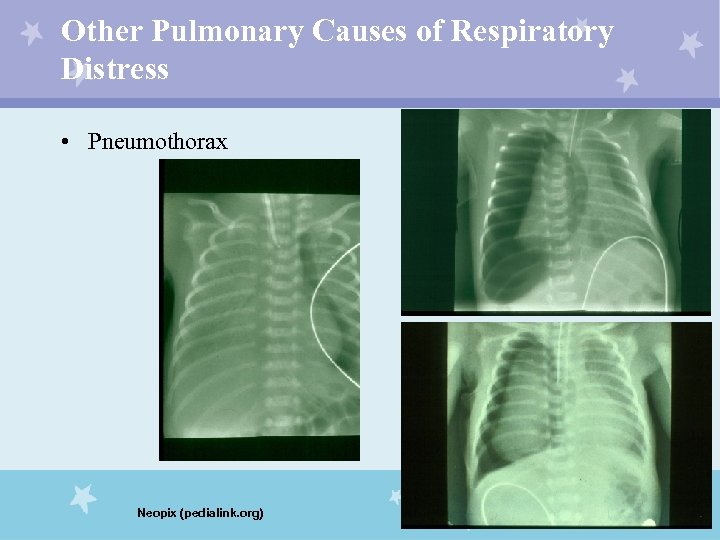 Other Pulmonary Causes of Respiratory Distress • Pneumothorax Neopix (pedialink. org)
Other Pulmonary Causes of Respiratory Distress • Pneumothorax Neopix (pedialink. org)
 Non-Pulmonary Causes of Respiratory Distress: Congenital Heart Disease
Non-Pulmonary Causes of Respiratory Distress: Congenital Heart Disease
 Congenital Heart Disease • Cyanotic – Transposition of the great arteries – Total anomalous pulmonary venous return – Tricuspid atresia – Tetralogy of Fallot – Truncus arteriosus – Pulmonary atresia – Severe CHF – Ebstein’s anomaly – Double outlet right ventricle • Acyanotic – Hypoplastic left heart syndrome – Interrupted aortic arch – Critical aortic stenosis – Patent ductus arteriosus – VSD/ASD – AV canal defect – Coarctation of the aorta* – Valvular defects * May present as cyanotic or acyanotic
Congenital Heart Disease • Cyanotic – Transposition of the great arteries – Total anomalous pulmonary venous return – Tricuspid atresia – Tetralogy of Fallot – Truncus arteriosus – Pulmonary atresia – Severe CHF – Ebstein’s anomaly – Double outlet right ventricle • Acyanotic – Hypoplastic left heart syndrome – Interrupted aortic arch – Critical aortic stenosis – Patent ductus arteriosus – VSD/ASD – AV canal defect – Coarctation of the aorta* – Valvular defects * May present as cyanotic or acyanotic
 Congenital Heart Disease • Presenting features – Murmur +/ – Tachypnea – Cyanosis – Active precordium – Gallop rhythm – Hypoperfusion • Acidosis? – Weak pulses – Hepatomegaly • CXR – Heart size/shape • Ebstein’s anomaly • Tetralogy of Fallot • CHF – Abnormal lung vascularity • Increased • Decreased • Echocardiogram • EKG
Congenital Heart Disease • Presenting features – Murmur +/ – Tachypnea – Cyanosis – Active precordium – Gallop rhythm – Hypoperfusion • Acidosis? – Weak pulses – Hepatomegaly • CXR – Heart size/shape • Ebstein’s anomaly • Tetralogy of Fallot • CHF – Abnormal lung vascularity • Increased • Decreased • Echocardiogram • EKG
 Differentiating CHD from Pulmonary Disease Aly H. Pediatrics in Review (2004)
Differentiating CHD from Pulmonary Disease Aly H. Pediatrics in Review (2004)
 Management of the Newborn with Respiratory Distress
Management of the Newborn with Respiratory Distress
 Initial Assessment: “ABCs” • First: – Airway – Breathing – Circulation • Next: – Stabilize – Gather data – Generate DDx • Finally: – Consult? – Manage or Transfer
Initial Assessment: “ABCs” • First: – Airway – Breathing – Circulation • Next: – Stabilize – Gather data – Generate DDx • Finally: – Consult? – Manage or Transfer
 Initial Assessment, continued • Identify life-threatening conditions that require prompt support – Inadequate or obstructed airway • Gasping • Choking • Stridor – Inadequate oxygenation • Cyanosis – Central vs. peripheral – Inadequate ventilation • Tachypnea • Grunting • Nasal flaring • Retractions – Inadequate perfusion • Pallor • Capillary refill
Initial Assessment, continued • Identify life-threatening conditions that require prompt support – Inadequate or obstructed airway • Gasping • Choking • Stridor – Inadequate oxygenation • Cyanosis – Central vs. peripheral – Inadequate ventilation • Tachypnea • Grunting • Nasal flaring • Retractions – Inadequate perfusion • Pallor • Capillary refill
 Clues from the History? • • • Prolonged maternal rupture of membranes? Maternal GBS status? Maternal fever? Fetal distress? Meconium? Onset of respiratory distress? – Immediate? – Delayed?
Clues from the History? • • • Prolonged maternal rupture of membranes? Maternal GBS status? Maternal fever? Fetal distress? Meconium? Onset of respiratory distress? – Immediate? – Delayed?
 Objective Data • Physical exam findings: – Breath sounds – Stridor – Severity • Laboratory data: – CBC w/ differential – Glucose – Blood gas – Blood culture – CXR – Hyperoxia test?
Objective Data • Physical exam findings: – Breath sounds – Stridor – Severity • Laboratory data: – CBC w/ differential – Glucose – Blood gas – Blood culture – CXR – Hyperoxia test?
 Management • Supplemental oxygen: – Blow by – Head box – Nasal cannula – Face mask • Monitoring – HR, RR – Pulse ox • How long? – 2 hrs? – 4 hrs? – Longer? • NPO
Management • Supplemental oxygen: – Blow by – Head box – Nasal cannula – Face mask • Monitoring – HR, RR – Pulse ox • How long? – 2 hrs? – 4 hrs? – Longer? • NPO
 Hermansen CL, Lorah KN. American Family Physician. 2007.
Hermansen CL, Lorah KN. American Family Physician. 2007.
 Management • Infants with TTN and no sepsis risk factors likely just need support and observation. • Infants with possible meconium aspiration, RDS, sepsis or pneumonia require a sepsis evaluation with blood culture, cbc and IV antibiotics x 48 hrs and repeat CXR(s). • Unclear risk factors or presentation? – Undertake sepsis evaluation
Management • Infants with TTN and no sepsis risk factors likely just need support and observation. • Infants with possible meconium aspiration, RDS, sepsis or pneumonia require a sepsis evaluation with blood culture, cbc and IV antibiotics x 48 hrs and repeat CXR(s). • Unclear risk factors or presentation? – Undertake sepsis evaluation
 So when to transport? ! • It depends… – Failure to resolve in 2 -4 hrs – Worsening condition • Perfusion • Oxygen needs • Distress – Staff ability/comfort/availability • IV access • Airway – Any suspicion of cardiac disease
So when to transport? ! • It depends… – Failure to resolve in 2 -4 hrs – Worsening condition • Perfusion • Oxygen needs • Distress – Staff ability/comfort/availability • IV access • Airway – Any suspicion of cardiac disease
 Take-Home Points • • Respiratory distress is common! Most do well with little intervention. Short differential dx When to transport is up to you! – Every situation is unique • Help is just a phone call away!
Take-Home Points • • Respiratory distress is common! Most do well with little intervention. Short differential dx When to transport is up to you! – Every situation is unique • Help is just a phone call away!
 How to Arrange Transport? • • Neonatologist on-call (In-house 24/7) – St. Paul NICU: • (800) 869 -1350 • (651) 220 -6210 – Minneapolis NICU: • (800) 636 -6283 • (612) 813 -6295 Transport team – Centralized Children’s Neonatal Transport Team in 2010 • Air – Helicopter – Fixed-wing plane • Ground
How to Arrange Transport? • • Neonatologist on-call (In-house 24/7) – St. Paul NICU: • (800) 869 -1350 • (651) 220 -6210 – Minneapolis NICU: • (800) 636 -6283 • (612) 813 -6295 Transport team – Centralized Children’s Neonatal Transport Team in 2010 • Air – Helicopter – Fixed-wing plane • Ground
 References • • • Aly H. Respiratory disorders in the newborn: Identification and diagnosis. Pediatrics in Review 2004; 25: 201 -207. Guglani L, Lakshminrusimha S, Ryan RM. Transient tachypnea of the newborn. Pediatrics in Review 2008; 29: e 59 -e 65. Hermansen CL, Lorah KN. Respiratory distress in the newborn. American Family Physician 2007; 76: 98 -994. Additional suggested reading: • Fidel-Rimon O, Shinwell ES. Respiratory distress in the term and near-term infant. Neo. Reviews 2005; 6: e 289 -e 296. Suggested resources: • NRP Program, AAP/AHA • S. T. A. B. L. E. Program
References • • • Aly H. Respiratory disorders in the newborn: Identification and diagnosis. Pediatrics in Review 2004; 25: 201 -207. Guglani L, Lakshminrusimha S, Ryan RM. Transient tachypnea of the newborn. Pediatrics in Review 2008; 29: e 59 -e 65. Hermansen CL, Lorah KN. Respiratory distress in the newborn. American Family Physician 2007; 76: 98 -994. Additional suggested reading: • Fidel-Rimon O, Shinwell ES. Respiratory distress in the term and near-term infant. Neo. Reviews 2005; 6: e 289 -e 296. Suggested resources: • NRP Program, AAP/AHA • S. T. A. B. L. E. Program
 We’re online! www. newbornmed. com • Provider resources • Family resources • Meet our neonatologists • Articles • NICU profiles
We’re online! www. newbornmed. com • Provider resources • Family resources • Meet our neonatologists • Articles • NICU profiles
 Thank You!
Thank You!


