8694df7a3ef091a48891eaba950d677f.ppt
- Количество слайдов: 55

Treatment strategies for metastatic prostate cancer Oliver Hakenberg Department of Urology, Rostock University
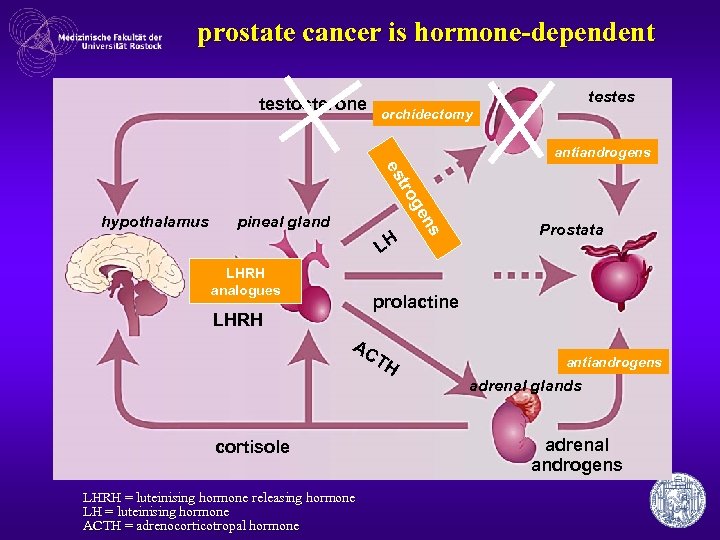
prostate cancer is hormone-dependent testosterone testes orchidectomy antiandrogens pineal gland LH LHRH analogues ns ge tro es hypothalamus Prostata prolactine LHRH AC TH antiandrogens adrenal glands cortisole LHRH = luteinising hormone releasing hormone LH = luteinising hormone ACTH = adrenocorticotropal hormone adrenal androgens
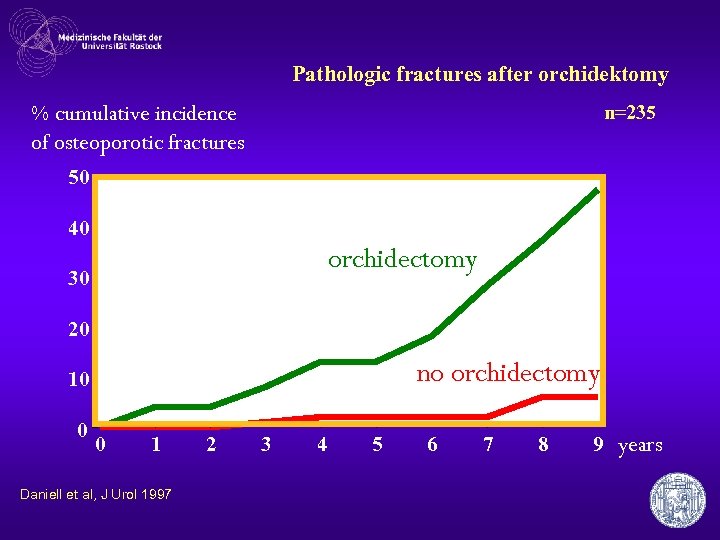
Pathologic fractures after orchidektomy % cumulative incidence of osteoporotic fractures n=235 50 40 orchidectomy 30 20 no orchidectomy 10 0 0 1 Daniell et al, J Urol 1997 2 3 4 5 6 7 8 9 years

Immediate androgen ablation • permanent – advanced metastatic disease M+ – locally advanced, if androgen ablation is the only treatment option • adjuvant/temporary – radical prostatectomy with positive nodes (p. N+) – adjuvant with radiotherapy in intermediate and high risk disease
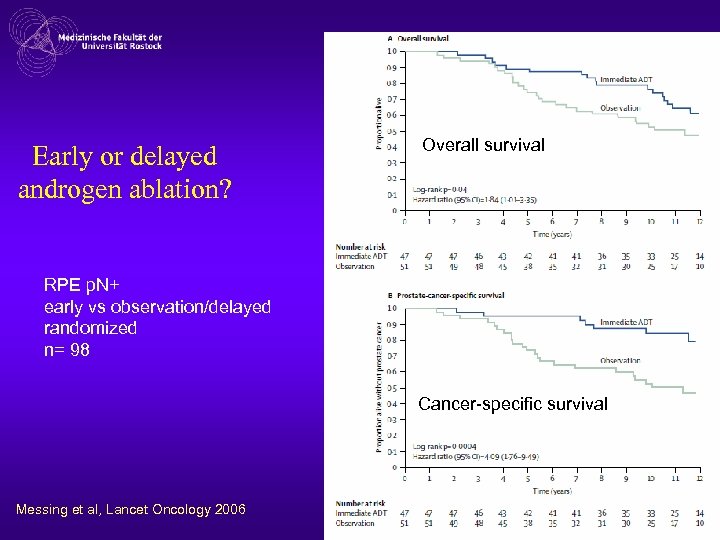
Early or delayed androgen ablation? Overall survival RPE p. N+ early vs observation/delayed randomized n= 98 Cancer-specific survival Messing et al, Lancet Oncology 2006

androgen ablation • ↓ gonadal testosterone • 10 -30% serum androgens from other sources • Adrenal cortex: DHEA + androstendione → transformed to testosterone in periphery (including prostate) • progression after xx months → hormone resistant

hormone resistance? • de novo intratumoral androgen synthesis in progressive CRPC • → maintenance of intracellular andogen levels • → androgen receptor (AR) stimulation despite low serume testosterone • „castration-resistant prostate cancer“ = CRPC Locke et al, Cancer Res 2008

3 new developments • autologous vaccine sipuleucel-T (IMPACT) – m. CRPC docetaxel-naive (85%) – improved OS vs placebo • cabazitaxel (TROPIC) – m. CRPC doxetaxel-refractory – improved OS vs mitoxantrone • arbiraterone – hormonal principle in CPRC Kantoff et al, N Engl J Med 2010 De Bono et al, Lancet 2010

Arbiraterone inhibition of testosterone biosynthesis • arbiraterone acetate inhibits – C 17, 20 lyase – 17 hydroxylase – Inhibition selective & irreversible • • adrenals, testes, prostate cancer cells arbiraterone acetate: prodrug good oral bioavailability Development of resistance
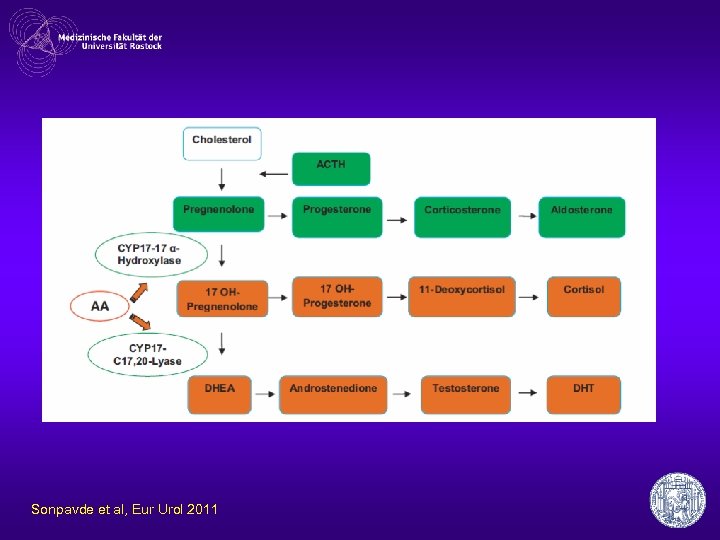
Sonpavde et al, Eur Urol 2011
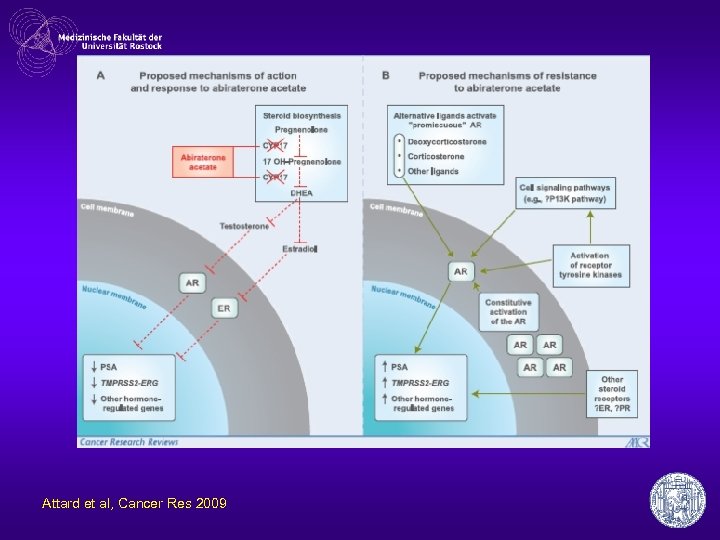
Attard et al, Cancer Res 2009

Study data: arbiraterone in CRPC • phase I – chemotherapy-naive CRPC patients • phase-II NCT 00474383 – progression after docetaxel • phase-III NCT 00638690 – progression after docetaxel • phase III NCT 00887198 – asymptomatic, low metastatic load in chemotherapy-naive patients

phase I • n=21 • chemo-naive, CRPC – 12/21 with PSA↓>50% and > 3 months – of which in 6/12 PSA↓ > 90% – PR (RESIST) in 5/8 patients and ↓analgesic medication – no grade 3/4 toxicity Attard et al, J Clin Oncol 2008

phase II a • • • chemotherapy-naive CRPC patients PSA↓> 50% in 70 -80% of patients RESIST response 37. 5% median time to PSA-rise 225 days dexamethasone at progression with arbiraterone: further PSA↓>50% in 33% Attard et al, J Clin Oncol 2009

phase II b • n= 47 docetaxele-pretreated CRPC • PSA↓> 50% in 51% of patients • 35 with RESIST – PR 17% – SD 66% • 23% ECOG improvement Reid et al, J Clin Oncol 2009
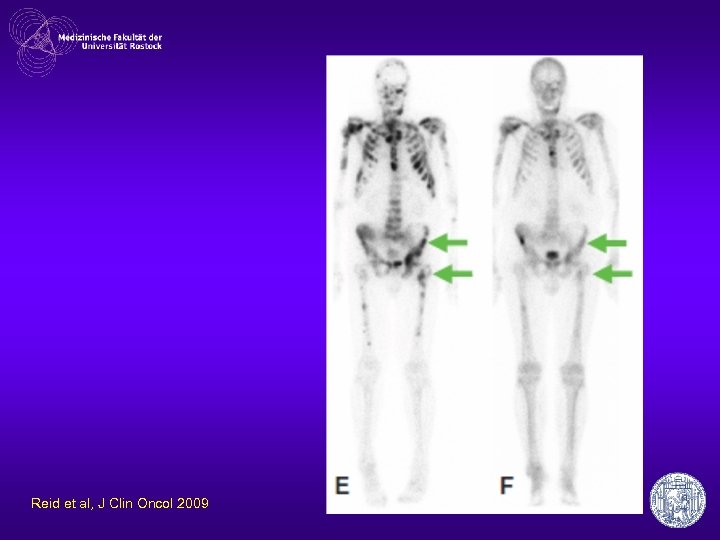
Reid et al, J Clin Oncol 2009
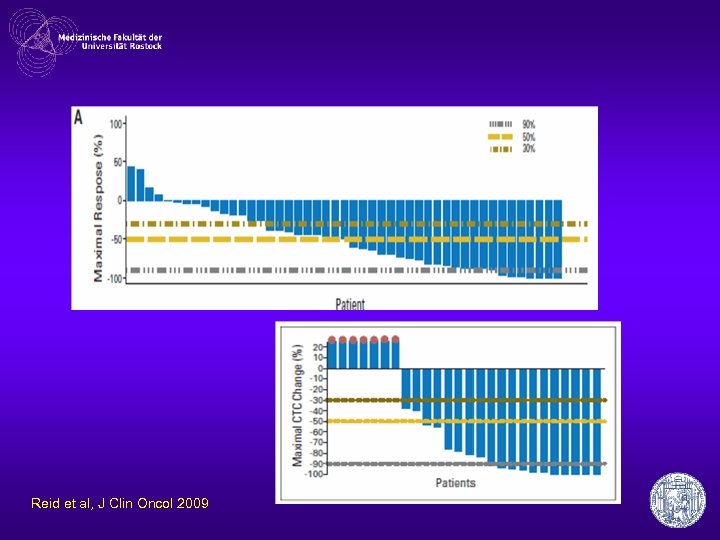
Reid et al, J Clin Oncol 2009

Phase II c • docetaxele-pretreated CRPC • better efficacy without ketoconazole pretreatment – 53% vs 33% PSA-response without/with – 31% vs 4% PSA↓>90% without/with ketoconazole – median time to progression 198 vs 99 days with/without ketoconazole Danila et al, J Clin Oncol 2009

phase III (COU-AA-301) • n=1195 docetaxel-refractory CRPC • arbiraterone vs placebo 2: 1 randomisation • stratification – ECOG 0 -1 vs 2 – prior chemotherapy schedules 1 vs 2 – pain score – type of progression: PSA vs XR

phase III (COU-AA-301) 1. interim analysis 2010 • • • OS 14. 8 vs 10. 4 months TTP 10. 2 vs 6. 6 months r. PFS 5. 6 vs 3. 6 months PSA RR 29. 1% vs 5. 5% toxicity – – hyperhydration 2. 3% vs 1. 0% hypokalaemia 3. 8% vs 0. 8% hypertension 1. 3% vs 0. 3% cardiopulmonary 4. 1% vs 2. 3% De Bono et al, ESMO 2010
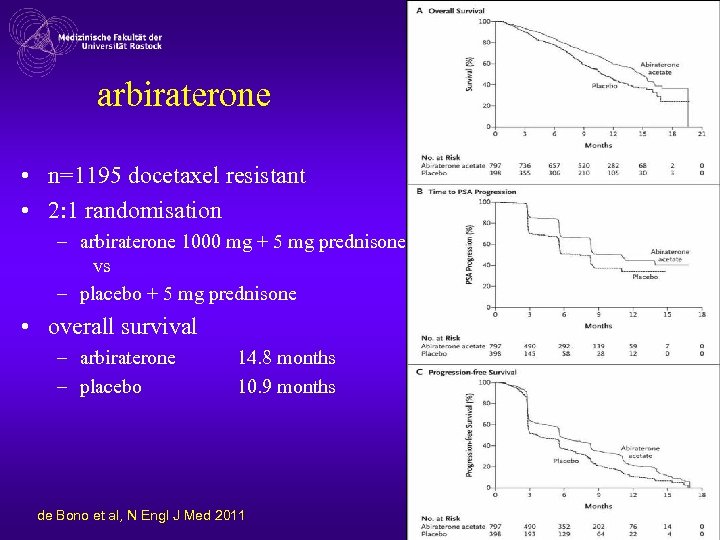
arbiraterone • n=1195 docetaxel resistant • 2: 1 randomisation – arbiraterone 1000 mg + 5 mg prednisone vs – placebo + 5 mg prednisone • overall survival – arbiraterone – placebo 14. 8 months 10. 9 months de Bono et al, N Engl J Med 2011

treatment options for metastatic prostate cancer • hormonal – androgen ablation • orchidectomy • LHRH-antagonists or –agonists • androgen blockers – androgen conversion blocker • arbiraterone • chemotherapy – docetaxel – cabazitaxel • • bisphonates pain treatment nuclear medical tretament: samarium, strontium best supportive care

Prognosis of metastatic prostate cancer • • initial response to androgen ablation > 80% progression in 50 -60% of patients within 2 years after that median survival 23 -37 months 5 year survival rate with M+oss 20%

androgen antagonists • steroidal – cyproterone acetate • non-steroidal – bicalutamide – flutamide – nilutamide
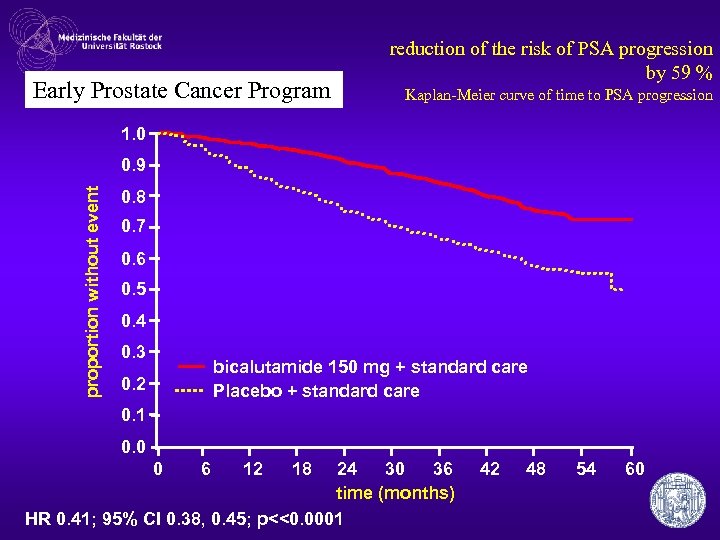
Early Prostate Cancer Program reduction of the risk of PSA progression by 59 % Kaplan-Meier curve of time to PSA progression 1. 0 proportion without event 0. 9 0. 8 0. 7 0. 6 0. 5 0. 4 0. 3 bicalutamide 150 mg + standard care Placebo + standard care 0. 2 0. 1 0. 0 0 6 12 18 24 30 36 time (months) HR 0. 41; 95% CI 0. 38, 0. 45; p<<0. 0001 42 48 54 60
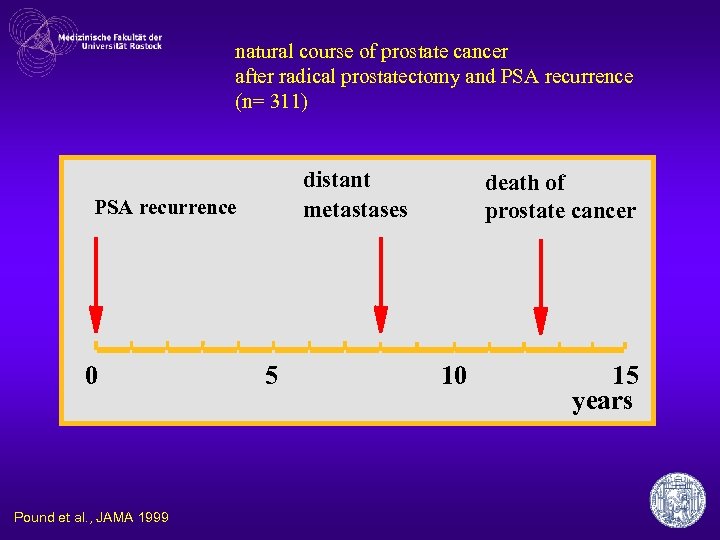
natural course of prostate cancer after radical prostatectomy and PSA recurrence (n= 311) distant metastases PSA recurrence 0 Pound et al. , JAMA 1999 5 death of prostate cancer 10 15 years
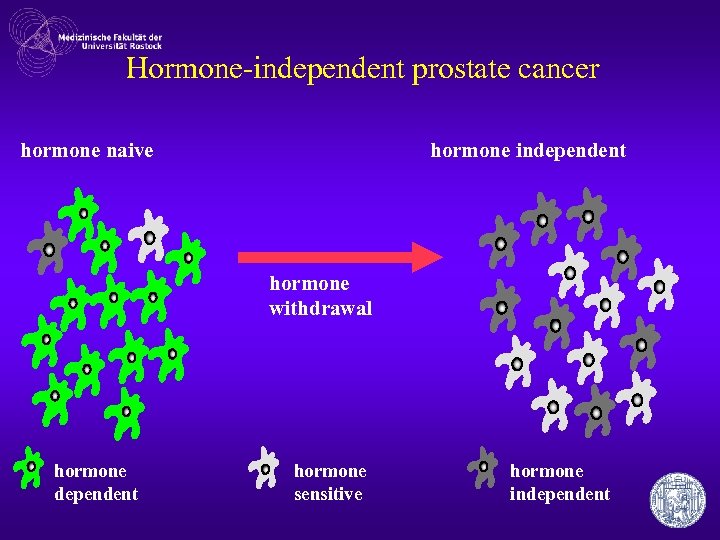
Hormone-independent prostate cancer hormone independent hormone naive hormone withdrawal hormone dependent hormone sensitive hormone independent

definition of castration-resistant prostate hormonerefractory prostate cancer (HRPC) • serume testosteron at castration level • secondary hormonal treatment without effect • ketoconazole • estrogens • rising PSA at 3 consecutive measurements at intervals of 1 week at leastt • with continued LHRH – blockade and after witrhdrawal of androgen blocker • lowest PSA limit: 0. 4 ng/ml

Chemotherapy for prostate cancer? Reviews response rates P. Walsh 1995: 1985: (17 to be an extremely short 6, 5 % „This is going Studien) discussion. Not only does it fail to cure the cancer, it doesn’t. M. Eisenberger, J Clinsurvival to any even prolong Oncol 1985 significant degree, and its side effects only add to the unpleasantness of having prostate cancer. “ 1992: (26 Studien) 8, 7 % Yagoda & Petrylak, Cancer 1993

chemotherapy for prostate cancer – mitoxantrone for HRPC? • phase III: mitoxantrone (12 mg/m²) + prednisone (10 mg/d) vs. FDA – 161 patients. (80 M+P; 81 P) d by (40 mg/d) vs. • phase III: mitoxantrone (14 mg/m²) + hydrocortisone in rove apy app hydrocortisone (40 mg/d)e ther ron – 242 patients n xa t d chemo mito ndar results s sta in pain. HRPC a – improvement in quality of life – duration of response 5 -7 months – no influence on survival Tannock et al. 1996 Kantoff et al. 1999

docetaxel • TAX 327 • SWOG 9916 • both studies showed overall survival advantage for docetaxel Petrylak, N Engl J Med 2004 Tannock, N Engl J Med 2004
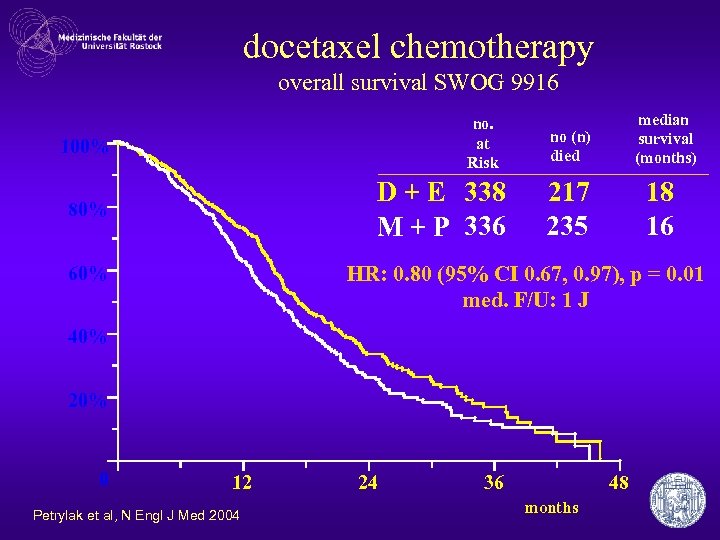
docetaxel chemotherapy overall survival SWOG 9916 no. at Risk 100% D + E 338 M + P 336 80% median survival (months) no (n) died 217 235 18 16 HR: 0. 80 (95% CI 0. 67, 0. 97), p = 0. 01 med. F/U: 1 J 60% 40% 20% 0 12 Petrylak et al, N Engl J Med 2004 24 36 48 months
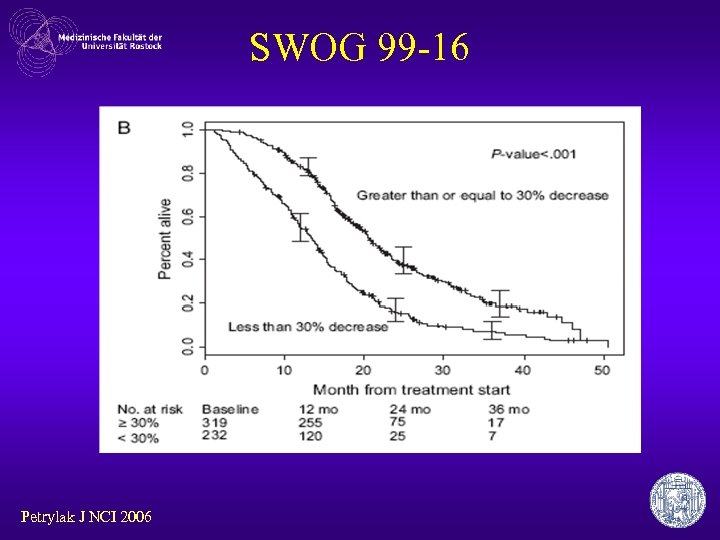
SWOG 99 -16 Petrylak J NCI 2006
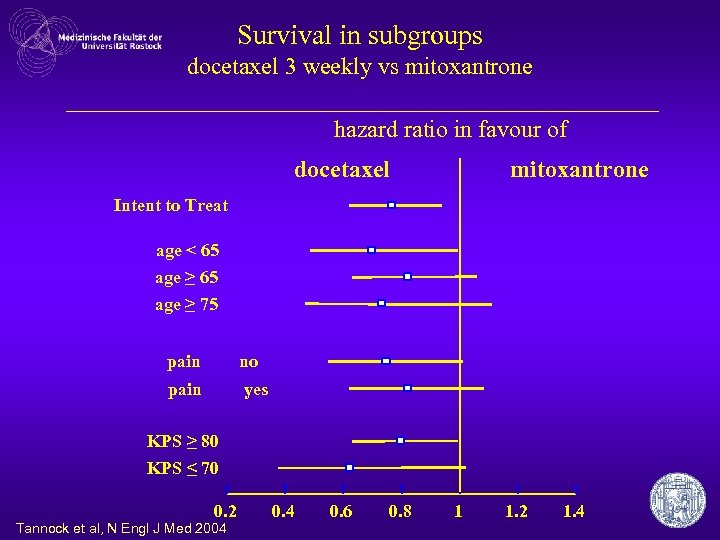
Survival in subgroups docetaxel 3 weekly vs mitoxantrone hazard ratio in favour of docetaxel mitoxantrone Intent to Treat age < 65 age ≥ 75 pain no pain yes KPS ≥ 80 KPS ≤ 70 0. 2 Tannock et al, N Engl J Med 2004 0. 6 0. 8 1 1. 2 1. 4

Cochrane Review chemotherapy of HRPC • n=6929 patients; 47 studies • investigated substances: – – – – EMP docetaxel 5 -FU cyclophosphamide doxorubicine mitoxantrone vinorelbine Shelley M, Harrison C et al. Cochrane Database Syst Rev 2006

Cochrane Review • PSA response (>50%): – EMP – docetaxel – 5 -FU – cyclophosphamide – doxorubicine – mitoxantrone – vinorelbine Shelley M, Harrison C et al. Cochrane Database Syst Rev 2006 48% 52% 20% n. d. 50% (CAVE: only 1 study!) 33% n. d.

results • only DOC => months) • pain ↓ • quality of life ↑ overall survival ↑ (<2. 5 DOC > Mit + Pred authors‘ conclusion: „At the present time this* probably represents the best chemotherapeutic regime available for men with HRPC“ *- docetaxel q 3 w Shelley M, Harrison C et al. Cochrane Database Syst Rev 2006
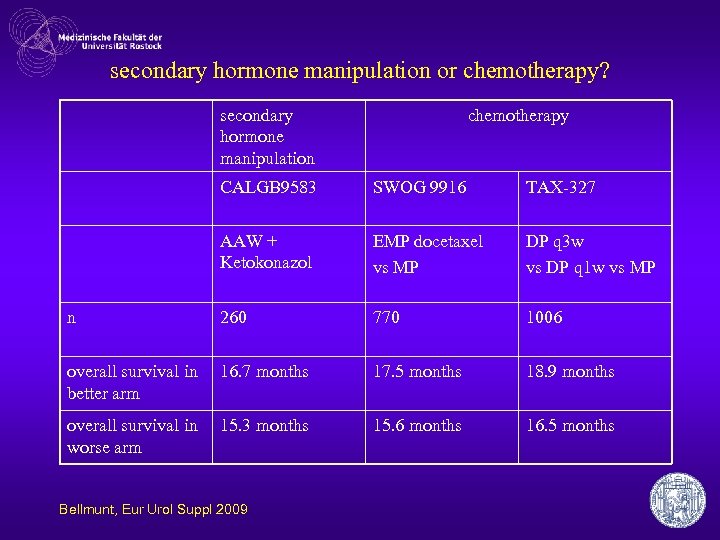
secondary hormone manipulation or chemotherapy? secondary hormone manipulation chemotherapy CALGB 9583 SWOG 9916 TAX-327 AAW + Ketokonazol EMP docetaxel vs MP DP q 3 w vs DP q 1 w vs MP n 260 770 1006 overall survival in better arm 16. 7 months 17. 5 months 18. 9 months overall survival in worse arm 15. 3 months 15. 6 months 16. 5 months Bellmunt, Eur Urol Suppl 2009

open questions • • • when to start with chemotherapy? should asymptomatic M+ patients be treated? how long to continue treatment? secondary treatment? intermittent chemotherapy? re-exposition?

Early vs late chemotherapy? • for – benefit established for other entities (breast cancer, colorectal cancer) – lower tumour mass – treatment prolongs survival • against – toxicity vs unreliable response – early induction of chemotherapy-refractory state – outcome is not influenced since no difference in survival between symptomatic vs asymptomatic patients (TAX 327)

forms of HRPC indications for starting with chemotherapy • only rising PSA • asymptomatic, low metastatic load no indication PSA doubling time? individual decision inclusion in study? • asymptomatic, large metastatic load yes • symptomatic metastases yes
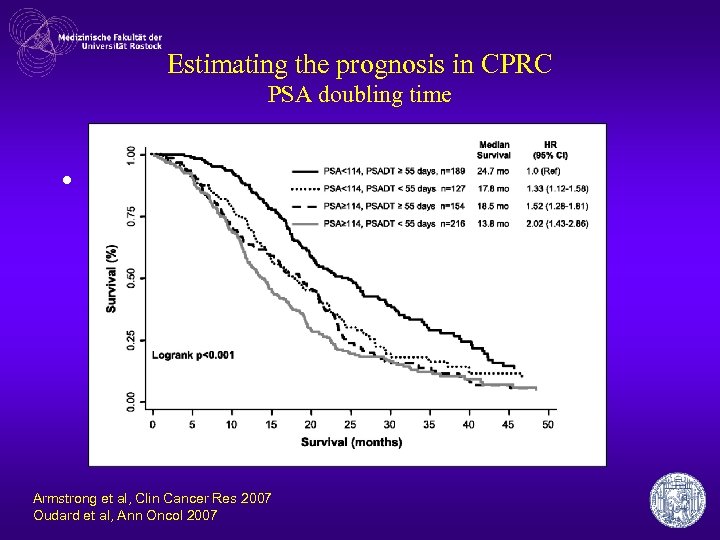
Estimating the prognosis in CPRC PSA doubling time • günstig – TAX 327: PSA-DT > 55 Tage – Oudard et al: PSA-DT > 45 Tage Armstrong et al, Clin Cancer Res 2007 Oudard et al, Ann Oncol 2007
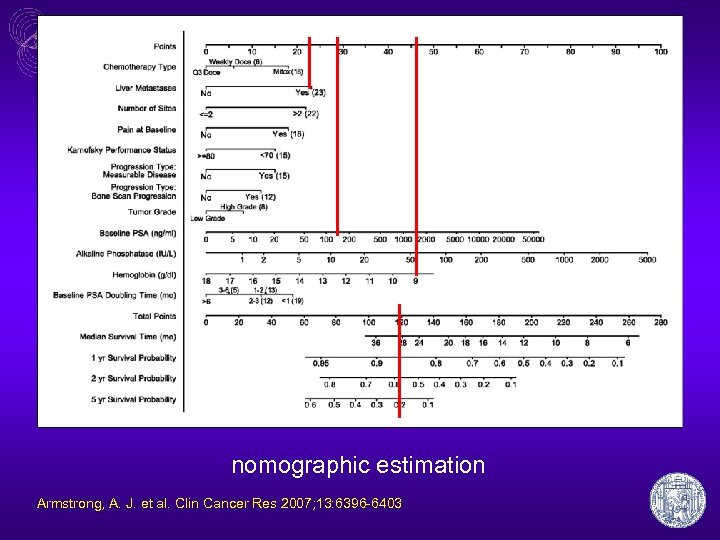
nomographic estimation Armstrong, A. J. et al. Clin Cancer Res 2007; 13: 6396 -6403

rising PSA under chemotherapy… • often initiial PSA flare-up • no negative influence on survival, unless there are signs of clinical progression => minimum of 8 weeks treatment before deciding to discontinue ! Olbert Anticancer Drugs 2006
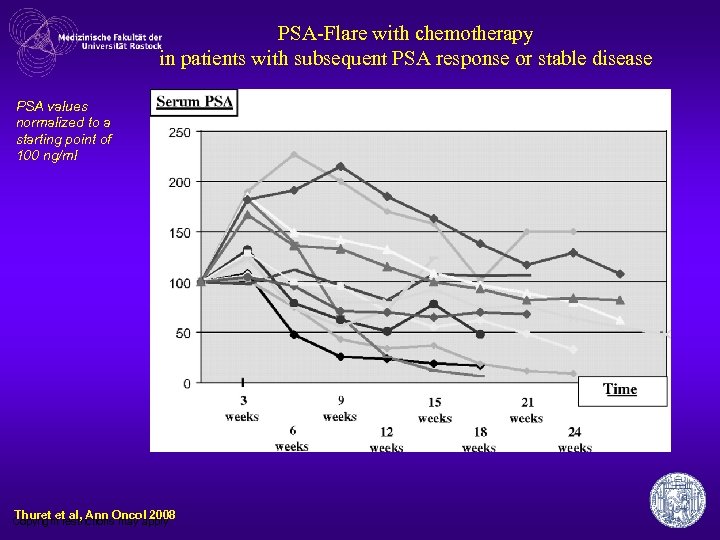
PSA-Flare with chemotherapy in patients with subsequent PSA response or stable disease PSA values normalized to a starting point of 100 ng/ml Thuret et al, Ann Oncol 2008 Copyright restrictions may apply.

Chemotherapy until… • best number of cycles unknown • TAX 327: mean of 8 cycles • but: chronic toxicity increases with no of cycles • intermittend chemotherapy?

When to discontinue chemotherapy…? • definite worsening of physical state • PSA doubling time < 3 Monate • slow PSA increase: - discontinue if clinically progressive Miller et al. Akt Urol 2006

First line chemotherapy docetaxel Mono (75 mg/m² KO d 1, q 21 d) Second line chemotherapy options: – docetaxel (M D) – docetaxel weekly – mitoxantrone (D M) – satraplatin (SPARC) – cabazitaxel PR: 44 -85% PR: 72% PR: 6 -15%
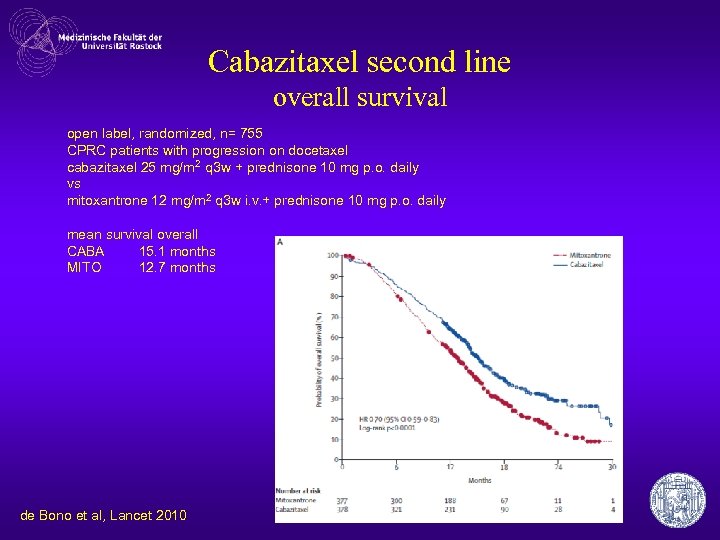
Cabazitaxel second line overall survival open label, randomized, n= 755 CPRC patients with progression on docetaxel cabazitaxel 25 mg/m 2 q 3 w + prednisone 10 mg p. o. daily vs mitoxantrone 12 mg/m 2 q 3 w i. v. + prednisone 10 mg p. o. daily mean survival overall CABA 15. 1 months MITO 12. 7 months de Bono et al, Lancet 2010
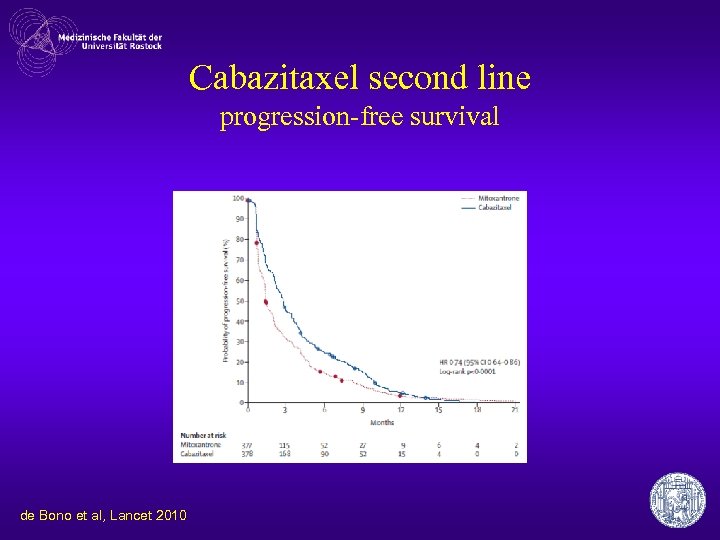
Cabazitaxel second line progression-free survival de Bono et al, Lancet 2010
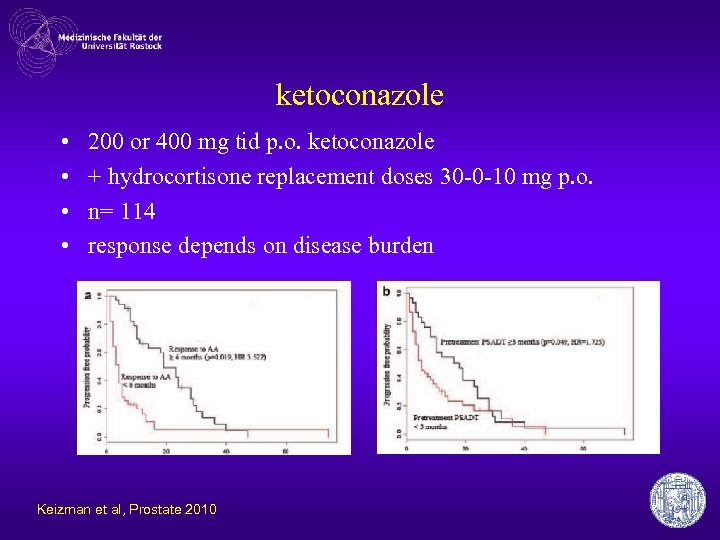
ketoconazole • • 200 or 400 mg tid p. o. ketoconazole + hydrocortisone replacement doses 30 -0 -10 mg p. o. n= 114 response depends on disease burden Keizman et al, Prostate 2010
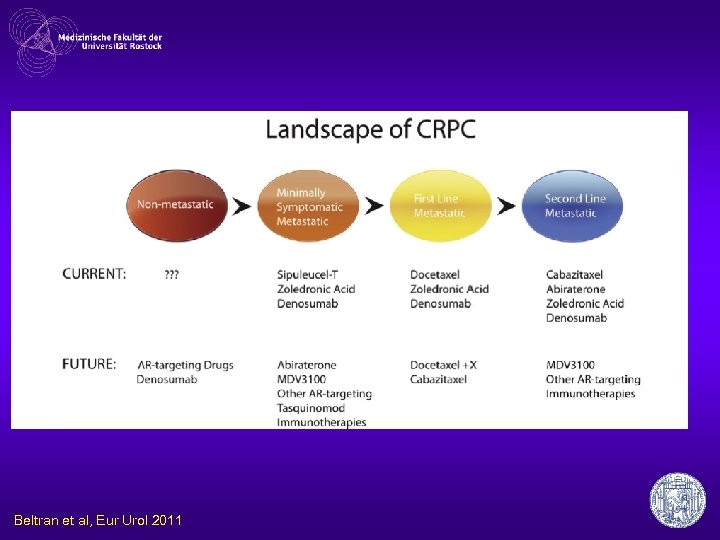
Beltran et al, Eur Urol 2011

Hypothetical calculation Future prognosis of metastatic prostate cancer? • • • initial response to androgen ablation > 80% progression in 50 -60% of patients within 2 years after that median survival 23 -37 months + 4 months with docetaxel + 4 months with cabazitaxel + 4 months with arbiraterone

„This will buy you three months“

Rostock
8694df7a3ef091a48891eaba950d677f.ppt