bdc6da333e0b98ebebcb2bde0044d2c3.ppt
- Количество слайдов: 52
![TRAINING FOR THE HEALTH SECTOR [Date …Place …Event…Sponsor…Organizer] CHILDREN AND CANCER Children's Health and TRAINING FOR THE HEALTH SECTOR [Date …Place …Event…Sponsor…Organizer] CHILDREN AND CANCER Children's Health and](https://present5.com/presentation/bdc6da333e0b98ebebcb2bde0044d2c3/image-1.jpg) TRAINING FOR THE HEALTH SECTOR [Date …Place …Event…Sponsor…Organizer] CHILDREN AND CANCER Children's Health and the Environment WHO Training Package for the Health Sector World Health Organization www. who. int/ceh 1
TRAINING FOR THE HEALTH SECTOR [Date …Place …Event…Sponsor…Organizer] CHILDREN AND CANCER Children's Health and the Environment WHO Training Package for the Health Sector World Health Organization www. who. int/ceh 1
 Children and Cancer CHILDHOOD CANCER OBJECTIVES v To discuss childhood cancer v To address the links between childhood environments and adult onset of cancer v To present current knowledge of causation and environmental risk factors v To discuss cancer clusters v To present educational and preventive measures 2
Children and Cancer CHILDHOOD CANCER OBJECTIVES v To discuss childhood cancer v To address the links between childhood environments and adult onset of cancer v To present current knowledge of causation and environmental risk factors v To discuss cancer clusters v To present educational and preventive measures 2
 Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 3
Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 3
 Children and Cancer TEN LEADING CAUSES OF DEATH (Children aged under 15 years) U. S. 2006 * Rates are per 100, 000 population and age adjusted to the 2000 US standard population. Based on US Mortality Data, 2006, National Center for Health Statistics, Centers for Disease Control and Prevention, 2009 4
Children and Cancer TEN LEADING CAUSES OF DEATH (Children aged under 15 years) U. S. 2006 * Rates are per 100, 000 population and age adjusted to the 2000 US standard population. Based on US Mortality Data, 2006, National Center for Health Statistics, Centers for Disease Control and Prevention, 2009 4
 Children and Cancer INCIDENCE CHILDHOOD CANCER (Globally) v Childhood 160, 000 new cases/year < 15 years of age 90, 000 deaths/year < 15 years of age Ferlay J, IARC Cancer Base N° 5, 2004 INCIDENCE CHILDHOOD CANCER v Childhood (U. S. 2006) 14. 9 per 100, 000 < 15 years of age 16. 4 per 100, 000 < 20 years of age v Adult 470. 1 per 100, 000 Ries LAG, SEER U. S. 2000 -2004 5
Children and Cancer INCIDENCE CHILDHOOD CANCER (Globally) v Childhood 160, 000 new cases/year < 15 years of age 90, 000 deaths/year < 15 years of age Ferlay J, IARC Cancer Base N° 5, 2004 INCIDENCE CHILDHOOD CANCER v Childhood (U. S. 2006) 14. 9 per 100, 000 < 15 years of age 16. 4 per 100, 000 < 20 years of age v Adult 470. 1 per 100, 000 Ries LAG, SEER U. S. 2000 -2004 5
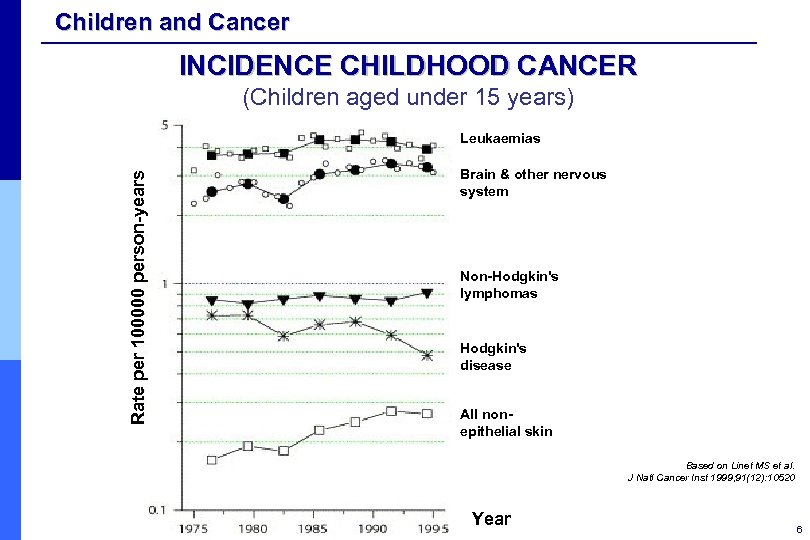 Children and Cancer INCIDENCE CHILDHOOD CANCER (Children aged under 15 years) Rate per 100000 person-years Leukaemias Brain & other nervous system Non-Hodgkin's lymphomas Hodgkin's disease All nonepithelial skin Based on Linet MS et al. J Natl Cancer Inst 1999; 91(12): 10520 Year 6
Children and Cancer INCIDENCE CHILDHOOD CANCER (Children aged under 15 years) Rate per 100000 person-years Leukaemias Brain & other nervous system Non-Hodgkin's lymphomas Hodgkin's disease All nonepithelial skin Based on Linet MS et al. J Natl Cancer Inst 1999; 91(12): 10520 Year 6
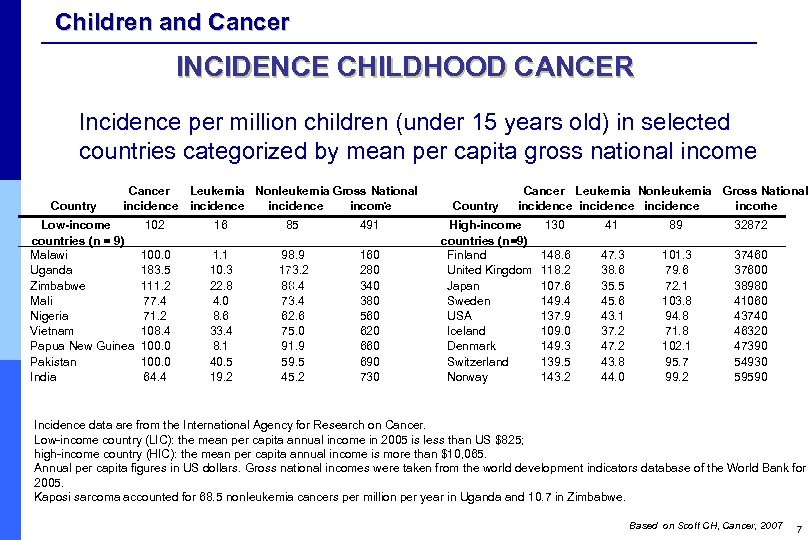 Children and Cancer INCIDENCE CHILDHOOD CANCER Incidence per million children (under 15 years old) in selected countries categorized by mean per capita gross national income Country Cancer Leukemia Nonleukemia Gross National * incidence income Low-income countries (n = 9) Malawi Uganda Zimbabwe Mali Nigeria Vietnam Papua New Guinea Pakistan India 102 16 85 491 100. 0 183. 5 111. 2 77. 4 71. 2 108. 4 100. 0 64. 4 1. 1 10. 3 22. 8 4. 0 8. 6 33. 4 8. 1 40. 5 19. 2 98. 9 173. 2 88. 4 73. 4 62. 6 75. 0 91. 9 59. 5 45. 2 160 280 340 380 560 620 660 690 730 Country Cancer Leukemia Nonleukemia Gross National * incidence income High-income countries (n=9) Finland United Kingdom Japan Sweden USA Iceland Denmark Switzerland Norway 130 41 89 32872 148. 6 118. 2 107. 6 149. 4 137. 9 109. 0 149. 3 139. 5 143. 2 47. 3 38. 6 35. 5 45. 6 43. 1 37. 2 43. 8 44. 0 101. 3 79. 6 72. 1 103. 8 94. 8 71. 8 102. 1 95. 7 99. 2 37460 37600 38980 41060 43740 46320 47390 54930 59590 Incidence data are from the International Agency for Research on Cancer. Low-income country (LIC): the mean per capita annual income in 2005 is less than US $825; high-income country (HIC): the mean per capita annual income is more than $10, 065. Annual per capita figures in US dollars. Gross national incomes were taken from the world development indicators database of the World Bank for 2005. Kaposi sarcoma accounted for 68. 5 nonleukemia cancers per million per year in Uganda and 10. 7 in Zimbabwe. Based on Scott CH, Cancer, 2007 7
Children and Cancer INCIDENCE CHILDHOOD CANCER Incidence per million children (under 15 years old) in selected countries categorized by mean per capita gross national income Country Cancer Leukemia Nonleukemia Gross National * incidence income Low-income countries (n = 9) Malawi Uganda Zimbabwe Mali Nigeria Vietnam Papua New Guinea Pakistan India 102 16 85 491 100. 0 183. 5 111. 2 77. 4 71. 2 108. 4 100. 0 64. 4 1. 1 10. 3 22. 8 4. 0 8. 6 33. 4 8. 1 40. 5 19. 2 98. 9 173. 2 88. 4 73. 4 62. 6 75. 0 91. 9 59. 5 45. 2 160 280 340 380 560 620 660 690 730 Country Cancer Leukemia Nonleukemia Gross National * incidence income High-income countries (n=9) Finland United Kingdom Japan Sweden USA Iceland Denmark Switzerland Norway 130 41 89 32872 148. 6 118. 2 107. 6 149. 4 137. 9 109. 0 149. 3 139. 5 143. 2 47. 3 38. 6 35. 5 45. 6 43. 1 37. 2 43. 8 44. 0 101. 3 79. 6 72. 1 103. 8 94. 8 71. 8 102. 1 95. 7 99. 2 37460 37600 38980 41060 43740 46320 47390 54930 59590 Incidence data are from the International Agency for Research on Cancer. Low-income country (LIC): the mean per capita annual income in 2005 is less than US $825; high-income country (HIC): the mean per capita annual income is more than $10, 065. Annual per capita figures in US dollars. Gross national incomes were taken from the world development indicators database of the World Bank for 2005. Kaposi sarcoma accounted for 68. 5 nonleukemia cancers per million per year in Uganda and 10. 7 in Zimbabwe. Based on Scott CH, Cancer, 2007 7
 Children and Cancer CAUSES OF CHILDHOOD CANCERS 1. Identified familial and genetic factors l 2. Known Environmental exposures & exogenous factors l 3. (5 -15%) (<5 -10%) UNKNOWN l 75 -90% 8
Children and Cancer CAUSES OF CHILDHOOD CANCERS 1. Identified familial and genetic factors l 2. Known Environmental exposures & exogenous factors l 3. (5 -15%) (<5 -10%) UNKNOWN l 75 -90% 8
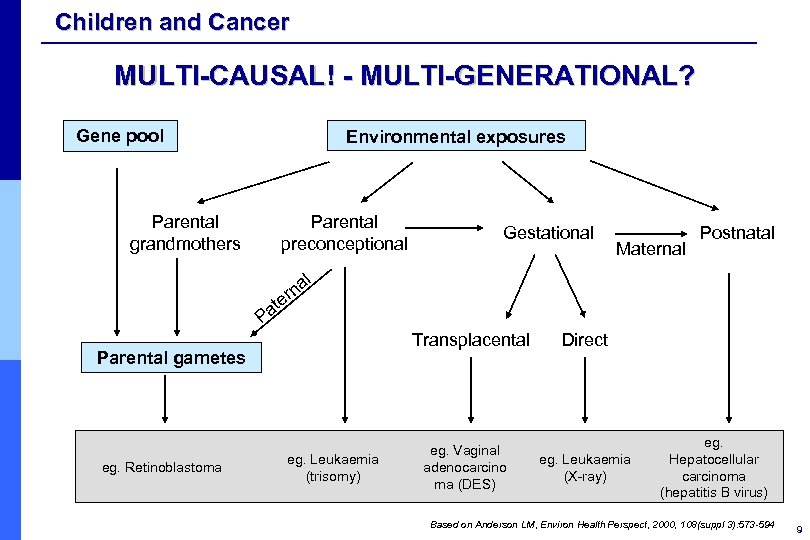 Children and Cancer MULTI-CAUSAL! - MULTI-GENERATIONAL? Gene pool Environmental exposures Parental grandmothers Parental preconceptional r te a Gestational Maternal Postnatal al n P Transplacental Parental gametes eg. Retinoblastoma eg. Leukaemia (trisomy) eg. Vaginal adenocarcino ma (DES) Direct eg. Leukaemia (X-ray) eg. Hepatocellular carcinoma (hepatitis B virus) Based on Anderson LM, Environ Health Perspect, 2000, 108(suppl 3): 573 -594 9
Children and Cancer MULTI-CAUSAL! - MULTI-GENERATIONAL? Gene pool Environmental exposures Parental grandmothers Parental preconceptional r te a Gestational Maternal Postnatal al n P Transplacental Parental gametes eg. Retinoblastoma eg. Leukaemia (trisomy) eg. Vaginal adenocarcino ma (DES) Direct eg. Leukaemia (X-ray) eg. Hepatocellular carcinoma (hepatitis B virus) Based on Anderson LM, Environ Health Perspect, 2000, 108(suppl 3): 573 -594 9
 Children and Cancer CHILDREN ARE NOT LITTLE ADULTS 1. Different and unique exposures 2. Dynamic developmental physiology 3. Longer life expectancy 4. Politically powerless Raphael, National Gallery of Art, Washington, DC 10
Children and Cancer CHILDREN ARE NOT LITTLE ADULTS 1. Different and unique exposures 2. Dynamic developmental physiology 3. Longer life expectancy 4. Politically powerless Raphael, National Gallery of Art, Washington, DC 10
 Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 11
Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 11
 Children and Cancer RISK FACTORS Definition : Specific agent statistically associated with a disease either positively or negatively Increasing levels of exposure or incidence of disease causation more likely 12
Children and Cancer RISK FACTORS Definition : Specific agent statistically associated with a disease either positively or negatively Increasing levels of exposure or incidence of disease causation more likely 12
 Children and Cancer RISK FACTORS Carcinogenic Agents identified as Risk Factors 1. EXTERNAL AGENTS: v Physical carcinogens: § ionizing radiation (X-ray) § non-ionizing radiation (electromagnetic fields, UV) v Biological carcinogens: § infections from viruses (Epstein Barr virus: Burkitt's lymphoma and Hodgkin's disease; Hepatitis B: liver carcinoma; and HHV 8 and HIV: Kaposi's sarcoma) 13
Children and Cancer RISK FACTORS Carcinogenic Agents identified as Risk Factors 1. EXTERNAL AGENTS: v Physical carcinogens: § ionizing radiation (X-ray) § non-ionizing radiation (electromagnetic fields, UV) v Biological carcinogens: § infections from viruses (Epstein Barr virus: Burkitt's lymphoma and Hodgkin's disease; Hepatitis B: liver carcinoma; and HHV 8 and HIV: Kaposi's sarcoma) 13
 Children and Cancer v Chemical carcinogens: § tobacco: mothers who smoke during pregnancy § pesticides, asbestos: parental occupation § aflatoxin, arsenic: food and drinking water contaminants § drugs and medication: pregnant women treatment (diethylstilboestrol: cell adenocarcinoma of the vagina or cervix ) v Dietary constituents 2. INTERNAL AGENTS: v Inherited factors § predisposition to particular familial diseases § genetically determined features 14
Children and Cancer v Chemical carcinogens: § tobacco: mothers who smoke during pregnancy § pesticides, asbestos: parental occupation § aflatoxin, arsenic: food and drinking water contaminants § drugs and medication: pregnant women treatment (diethylstilboestrol: cell adenocarcinoma of the vagina or cervix ) v Dietary constituents 2. INTERNAL AGENTS: v Inherited factors § predisposition to particular familial diseases § genetically determined features 14
 Children and Cancer RISK FACTORS Weight of evidence may be 1) Known 2) Suggestive 3) Limited according to extent to which evidence of causality supports a relationship between a risk factor and a disease 15
Children and Cancer RISK FACTORS Weight of evidence may be 1) Known 2) Suggestive 3) Limited according to extent to which evidence of causality supports a relationship between a risk factor and a disease 15
 Children and Cancer RISK FACTORS Associated with each type of Childhood Cancer 1) Known a) Genetic/congenital disorders b) Age peak c) Ethnics d) Gender e) Environmental 2) Suggestive a) Family history b) Reproductive factors c) Environmental 3) Limited a) Family History b) Environmental 16
Children and Cancer RISK FACTORS Associated with each type of Childhood Cancer 1) Known a) Genetic/congenital disorders b) Age peak c) Ethnics d) Gender e) Environmental 2) Suggestive a) Family history b) Reproductive factors c) Environmental 3) Limited a) Family History b) Environmental 16
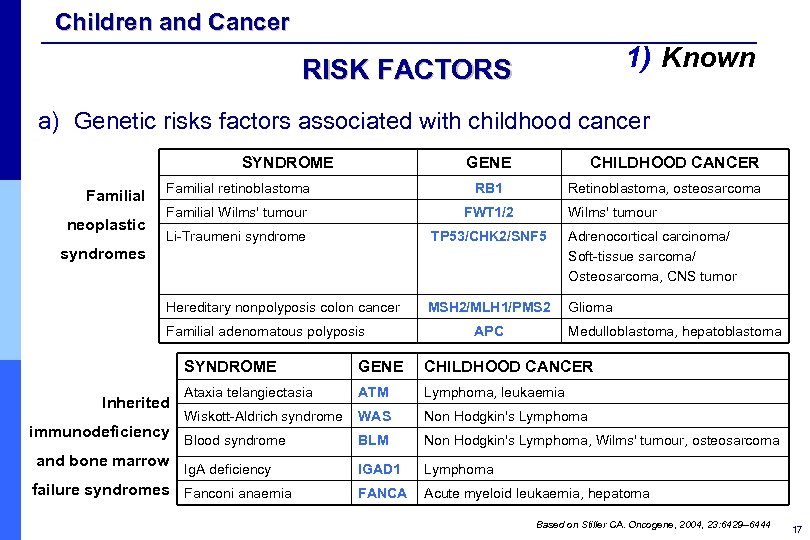 Children and Cancer 1) Known RISK FACTORS a) Genetic risks factors associated with childhood cancer SYNDROME GENE CHILDHOOD CANCER neoplastic Familial retinoblastoma RB 1 Familial Wilms' tumour FWT 1/2 Li-Traumeni syndrome TP 53/CHK 2/SNF 5 Adrenocortical carcinoma/ Soft-tissue sarcoma/ Osteosarcoma, CNS tumor Hereditary nonpolyposis colon cancer Familial Retinoblastoma, osteosarcoma MSH 2/MLH 1/PMS 2 Glioma Wilms' tumour syndromes Familial adenomatous polyposis APC Medulloblastoma, hepatoblastoma SYNDROME Inherited GENE CHILDHOOD CANCER Ataxia telangiectasia ATM Lymphoma, leukaemia Wiskott-Aldrich syndrome WAS Non Hodgkin's Lymphoma BLM Non Hodgkin's Lymphoma, Wilms' tumour, osteosarcoma IGAD 1 Lymphoma FANCA Acute myeloid leukaemia, hepatoma immunodeficiency Blood syndrome and bone marrow Ig. A deficiency failure syndromes Fanconi anaemia Based on Stiller CA. Oncogene, 2004, 23: 6429– 6444 17
Children and Cancer 1) Known RISK FACTORS a) Genetic risks factors associated with childhood cancer SYNDROME GENE CHILDHOOD CANCER neoplastic Familial retinoblastoma RB 1 Familial Wilms' tumour FWT 1/2 Li-Traumeni syndrome TP 53/CHK 2/SNF 5 Adrenocortical carcinoma/ Soft-tissue sarcoma/ Osteosarcoma, CNS tumor Hereditary nonpolyposis colon cancer Familial Retinoblastoma, osteosarcoma MSH 2/MLH 1/PMS 2 Glioma Wilms' tumour syndromes Familial adenomatous polyposis APC Medulloblastoma, hepatoblastoma SYNDROME Inherited GENE CHILDHOOD CANCER Ataxia telangiectasia ATM Lymphoma, leukaemia Wiskott-Aldrich syndrome WAS Non Hodgkin's Lymphoma BLM Non Hodgkin's Lymphoma, Wilms' tumour, osteosarcoma IGAD 1 Lymphoma FANCA Acute myeloid leukaemia, hepatoma immunodeficiency Blood syndrome and bone marrow Ig. A deficiency failure syndromes Fanconi anaemia Based on Stiller CA. Oncogene, 2004, 23: 6429– 6444 17
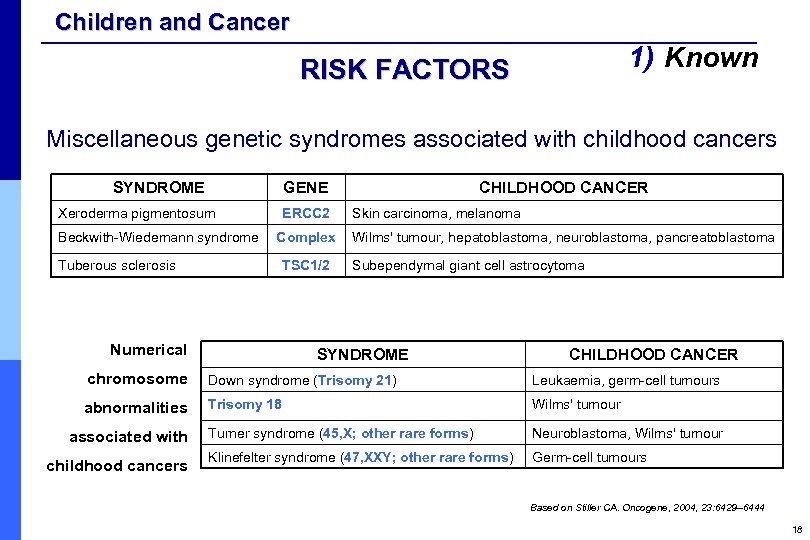 Children and Cancer 1) Known RISK FACTORS Miscellaneous genetic syndromes associated with childhood cancers SYNDROME GENE Xeroderma pigmentosum Beckwith-Wiedemann syndrome ERCC 2 Complex Tuberous sclerosis TSC 1/2 Numerical CHILDHOOD CANCER Skin carcinoma, melanoma Wilms' tumour, hepatoblastoma, neuroblastoma, pancreatoblastoma Subependymal giant cell astrocytoma SYNDROME CHILDHOOD CANCER chromosome Down syndrome (Trisomy 21) Leukaemia, germ-cell tumours abnormalities Trisomy 18 Wilms' tumour Turner syndrome (45, X; other rare forms) Neuroblastoma, Wilms' tumour Klinefelter syndrome (47, XXY; other rare forms) Germ-cell tumours associated with childhood cancers Based on Stiller CA. Oncogene, 2004, 23: 6429– 6444 18
Children and Cancer 1) Known RISK FACTORS Miscellaneous genetic syndromes associated with childhood cancers SYNDROME GENE Xeroderma pigmentosum Beckwith-Wiedemann syndrome ERCC 2 Complex Tuberous sclerosis TSC 1/2 Numerical CHILDHOOD CANCER Skin carcinoma, melanoma Wilms' tumour, hepatoblastoma, neuroblastoma, pancreatoblastoma Subependymal giant cell astrocytoma SYNDROME CHILDHOOD CANCER chromosome Down syndrome (Trisomy 21) Leukaemia, germ-cell tumours abnormalities Trisomy 18 Wilms' tumour Turner syndrome (45, X; other rare forms) Neuroblastoma, Wilms' tumour Klinefelter syndrome (47, XXY; other rare forms) Germ-cell tumours associated with childhood cancers Based on Stiller CA. Oncogene, 2004, 23: 6429– 6444 18
 Children and Cancer RISK FACTORS 1) Known b) Age peak v Age at onset: § Age-related exposures § Some prenatal exposures (see: e) Environmental exposures) § Hormonal influences of adolescence v Age peak: § infancy: sympathetic nervous system tumors, rhabdomyosarcoma, Wilm’s tumor § adolescent: malignant bone tumors, soft tissue sarcomas, renal cell carcinoma 19
Children and Cancer RISK FACTORS 1) Known b) Age peak v Age at onset: § Age-related exposures § Some prenatal exposures (see: e) Environmental exposures) § Hormonal influences of adolescence v Age peak: § infancy: sympathetic nervous system tumors, rhabdomyosarcoma, Wilm’s tumor § adolescent: malignant bone tumors, soft tissue sarcomas, renal cell carcinoma 19
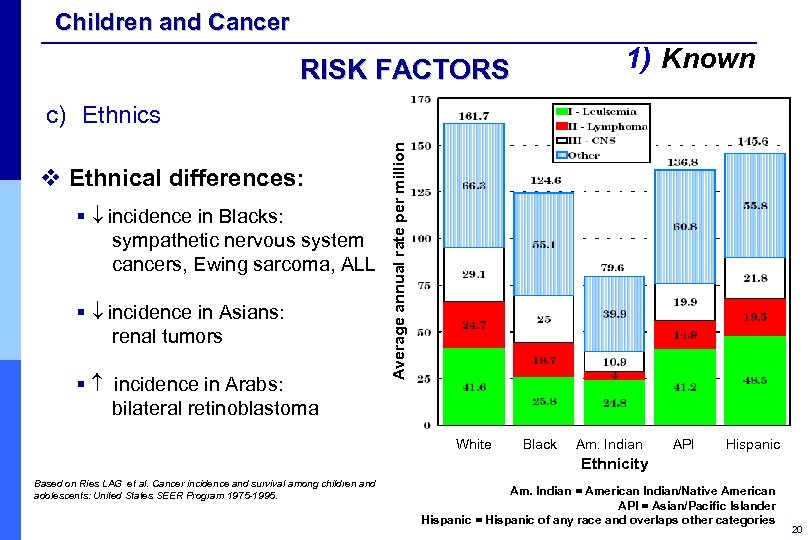 Children and Cancer 1) Known RISK FACTORS v Ethnical differences: § incidence in Blacks: sympathetic nervous system cancers, Ewing sarcoma, ALL § incidence in Asians: renal tumors § incidence in Arabs: bilateral retinoblastoma Average annual rate per million c) Ethnics White Black Am. Indian API Hispanic Ethnicity Based on Ries LAG et al. Cancer incidence and survival among children and adolescents: United States SEER Program 1975 -1995. Am. Indian = American Indian/Native American API = Asian/Pacific Islander Hispanic = Hispanic of any race and overlaps other categories 20
Children and Cancer 1) Known RISK FACTORS v Ethnical differences: § incidence in Blacks: sympathetic nervous system cancers, Ewing sarcoma, ALL § incidence in Asians: renal tumors § incidence in Arabs: bilateral retinoblastoma Average annual rate per million c) Ethnics White Black Am. Indian API Hispanic Ethnicity Based on Ries LAG et al. Cancer incidence and survival among children and adolescents: United States SEER Program 1975 -1995. Am. Indian = American Indian/Native American API = Asian/Pacific Islander Hispanic = Hispanic of any race and overlaps other categories 20
 Children and Cancer RISK FACTORS 1) Known d) Gender v Gender: § Exposures differing by gender § Effects of hormonal influences § Gender related genetic differences v Male / female ratio: WHO § males: Hodgkin’s and Non-Hodgkin’s lymphomas, ALL, ependymomas, primitive neuroectodermal tumours § females: thyroid carcinoma, malignant melanoma 21
Children and Cancer RISK FACTORS 1) Known d) Gender v Gender: § Exposures differing by gender § Effects of hormonal influences § Gender related genetic differences v Male / female ratio: WHO § males: Hodgkin’s and Non-Hodgkin’s lymphomas, ALL, ependymomas, primitive neuroectodermal tumours § females: thyroid carcinoma, malignant melanoma 21
 Children and Cancer RISK FACTORS 1) Known e) Environmental exposures v Ionizing radiation: § Diagnostic x-ray in utero acute lymphoblastic leukaemia § Chernobyl radiation fallout thyroid cancer § Radiation therapy malignant bone tumours, leukaemia v Immunosuppressive therapy: Non-Hodgkin’s lymphoma v Treatment with diethylstilboestrol: adenocarcinoma of vagina v Infections: § HIV/AIDS Kaposi’s sarcoma § Malaria and Epstein Barr virus Burkitt’s lymphoma 22
Children and Cancer RISK FACTORS 1) Known e) Environmental exposures v Ionizing radiation: § Diagnostic x-ray in utero acute lymphoblastic leukaemia § Chernobyl radiation fallout thyroid cancer § Radiation therapy malignant bone tumours, leukaemia v Immunosuppressive therapy: Non-Hodgkin’s lymphoma v Treatment with diethylstilboestrol: adenocarcinoma of vagina v Infections: § HIV/AIDS Kaposi’s sarcoma § Malaria and Epstein Barr virus Burkitt’s lymphoma 22
 Children and Cancer RISK FACTORS 2) Suggestive b) Maternal reproductive factors v Fetal loss, first born and age > 35 years: acute lymphoblastic leukaemia v Diet (cured meats): brain tumours v Preterm birth: germ cell tumours v Alcohol, tobacco: sympathetic nervous system tumours 23
Children and Cancer RISK FACTORS 2) Suggestive b) Maternal reproductive factors v Fetal loss, first born and age > 35 years: acute lymphoblastic leukaemia v Diet (cured meats): brain tumours v Preterm birth: germ cell tumours v Alcohol, tobacco: sympathetic nervous system tumours 23
 Children and Cancer RISK FACTORS 2) Suggestive c) Environmental exposures v Parental smoking: neuroblastoma, acute lymphoblastic leukaemia, acute myeloid leukaemia v Residential pesticides: § Prenatal maternal & paternal exposures brain, bone, kidney tumours, acute myeloid leukaemia, Hodgkin’s disease WHO § Postnatal exposures brain, bone, kidney tumours, acute myeloid leukaemia, Hodgkin’s disease 24
Children and Cancer RISK FACTORS 2) Suggestive c) Environmental exposures v Parental smoking: neuroblastoma, acute lymphoblastic leukaemia, acute myeloid leukaemia v Residential pesticides: § Prenatal maternal & paternal exposures brain, bone, kidney tumours, acute myeloid leukaemia, Hodgkin’s disease WHO § Postnatal exposures brain, bone, kidney tumours, acute myeloid leukaemia, Hodgkin’s disease 24
 Children and Cancer RISK FACTORS 2) Suggestive v Parental occupational exposures: § Agriculture brain, CNS, renal tumours § Paint, solvents germ cell tumours, hepatic tumours, brain and CNS tumours, acute lymphoblastic leukaemia § Welder renal tumours, retinoblastoma § Petroleum acute lymphoblastic leukaemia, brain and CNS tumours, hepatic tumours § Paper or pulp mill brain tumours WHO § High fluoride exposure osteosarcoma 25
Children and Cancer RISK FACTORS 2) Suggestive v Parental occupational exposures: § Agriculture brain, CNS, renal tumours § Paint, solvents germ cell tumours, hepatic tumours, brain and CNS tumours, acute lymphoblastic leukaemia § Welder renal tumours, retinoblastoma § Petroleum acute lymphoblastic leukaemia, brain and CNS tumours, hepatic tumours § Paper or pulp mill brain tumours WHO § High fluoride exposure osteosarcoma 25
 Children and Cancer RISK FACTORS Example: Acute Lymphoblastic Leukaemia 1) Known v Genetic/congenital disorders: ataxia telangiectasia, v Age peak: v Age-adjusted incidence: v Race: v Gender: v Environmental: Fanconi syndrome, Bloom syndrome, neurofibromatosis 2 -4 years 26. 3 per million W: B = 2. 0 M: F = 1. 3 Ionizing Radiation (diagnostic-in utero, therapeutic-postnatal) 26
Children and Cancer RISK FACTORS Example: Acute Lymphoblastic Leukaemia 1) Known v Genetic/congenital disorders: ataxia telangiectasia, v Age peak: v Age-adjusted incidence: v Race: v Gender: v Environmental: Fanconi syndrome, Bloom syndrome, neurofibromatosis 2 -4 years 26. 3 per million W: B = 2. 0 M: F = 1. 3 Ionizing Radiation (diagnostic-in utero, therapeutic-postnatal) 26
 Children and Cancer RISK FACTORS Example: Acute Lymphoblastic Leukaemia 2) Suggestive v Reproductive factors: maternal fetal loss, mother older than 35 years at pregnancy, first born 3) Limited v Environmental: Paternal smoking before conception Parental occupational exposures (hydrocarbons, paints, motor vehicle exhaust) 60 -Hz magnetic fields >0. 4ųT Postnatal chloramphenicol use v Other: Decreased risk associated with breastfeeding 27
Children and Cancer RISK FACTORS Example: Acute Lymphoblastic Leukaemia 2) Suggestive v Reproductive factors: maternal fetal loss, mother older than 35 years at pregnancy, first born 3) Limited v Environmental: Paternal smoking before conception Parental occupational exposures (hydrocarbons, paints, motor vehicle exhaust) 60 -Hz magnetic fields >0. 4ųT Postnatal chloramphenicol use v Other: Decreased risk associated with breastfeeding 27
 Children and Cancer RISK FACTORS 3) Limited: Infection (hypothesis) 1. Areas of rapid population growth 2. Areas of increased population commuting 3. Influences of population war, disasters, tourism 4. Maternal infection in pregnancy 5. Immunization or risks 6. Exposure to infection in infancy or early childhood - child care, spacing of siblings 28
Children and Cancer RISK FACTORS 3) Limited: Infection (hypothesis) 1. Areas of rapid population growth 2. Areas of increased population commuting 3. Influences of population war, disasters, tourism 4. Maternal infection in pregnancy 5. Immunization or risks 6. Exposure to infection in infancy or early childhood - child care, spacing of siblings 28
 Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 29
Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 29
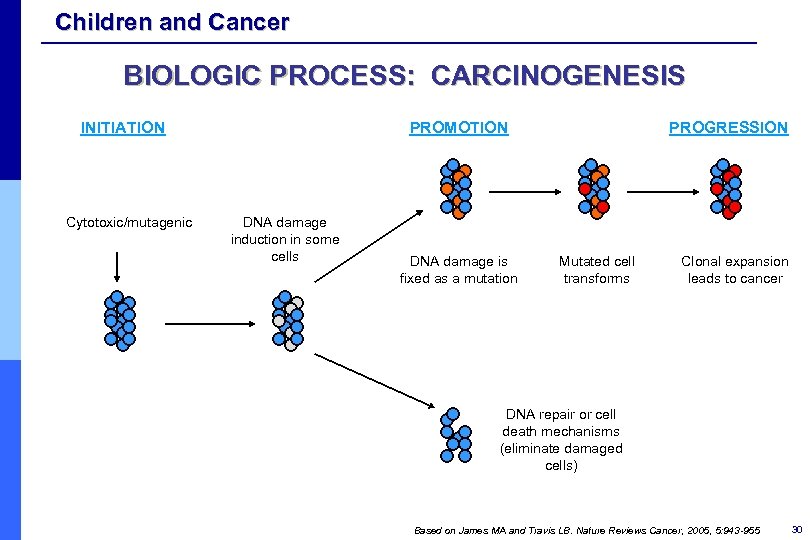 Children and Cancer BIOLOGIC PROCESS: CARCINOGENESIS INITIATION Cytotoxic/mutagenic PROMOTION DNA damage induction in some cells DNA damage is fixed as a mutation PROGRESSION Mutated cell transforms Clonal expansion leads to cancer DNA repair or cell death mechanisms (eliminate damaged cells) Based on James MA and Travis LB. Nature Reviews Cancer, 2005, 5: 943 -955 30
Children and Cancer BIOLOGIC PROCESS: CARCINOGENESIS INITIATION Cytotoxic/mutagenic PROMOTION DNA damage induction in some cells DNA damage is fixed as a mutation PROGRESSION Mutated cell transforms Clonal expansion leads to cancer DNA repair or cell death mechanisms (eliminate damaged cells) Based on James MA and Travis LB. Nature Reviews Cancer, 2005, 5: 943 -955 30
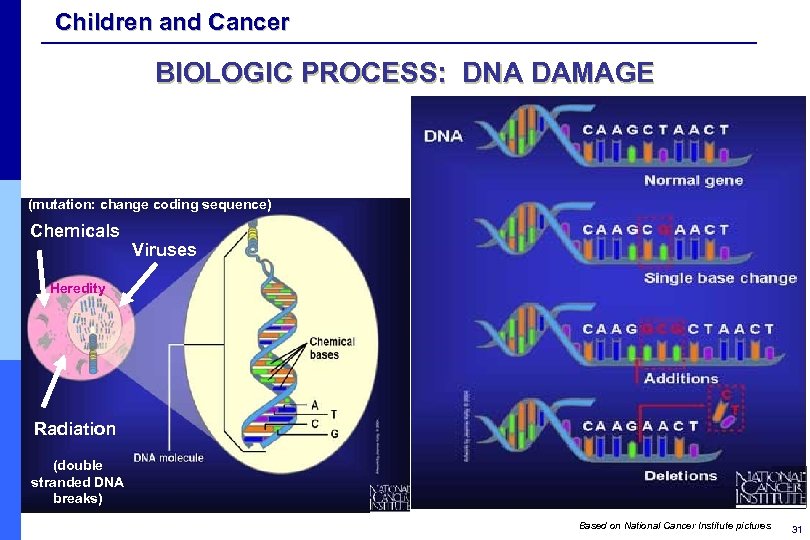 Children and Cancer BIOLOGIC PROCESS: DNA DAMAGE (mutation: change coding sequence) Chemicals Viruses Heredity Radiation (double stranded DNA breaks) Based on National Cancer Institute pictures 31
Children and Cancer BIOLOGIC PROCESS: DNA DAMAGE (mutation: change coding sequence) Chemicals Viruses Heredity Radiation (double stranded DNA breaks) Based on National Cancer Institute pictures 31
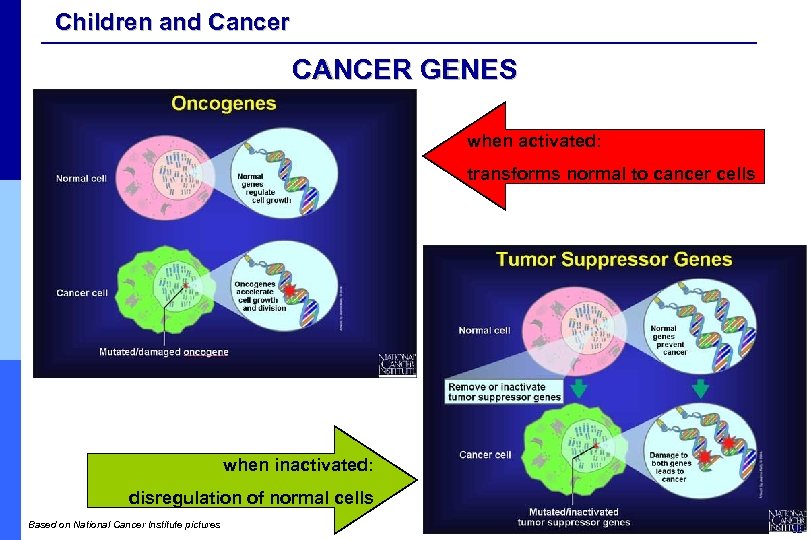 Children and Cancer CANCER GENES when activated: transforms normal to cancer cells when inactivated: disregulation of normal cells Based on National Cancer Institute pictures 32
Children and Cancer CANCER GENES when activated: transforms normal to cancer cells when inactivated: disregulation of normal cells Based on National Cancer Institute pictures 32
 Children and Cancer BIOMARKERS AND OTHER MARKERS v Biomarkers: indicators that measure a physiological, biochemical, or pharmacological event. § Diagnostic (screening) biomarker: for diagnosis and classification i. e. Bence–Jones protein in urine indicator of multiple myeloma § Prognostic biomarker: for refining staging § Stratification (predictive) biomarker: for predicting or monitoring response to treatment v Circulating tumour markers for cancer testing and noninvasive prenatal diagnosis: § nucleic acids : detection of gene mutations, chromosomal rearrangements, microsatellite alterations, viral sequences, gene promoter hypermethylation and changes in microarray-generated profiles (genetic signatures) § hormones, enzymes, glycoproteins, oncofoetal antigens and receptors 33
Children and Cancer BIOMARKERS AND OTHER MARKERS v Biomarkers: indicators that measure a physiological, biochemical, or pharmacological event. § Diagnostic (screening) biomarker: for diagnosis and classification i. e. Bence–Jones protein in urine indicator of multiple myeloma § Prognostic biomarker: for refining staging § Stratification (predictive) biomarker: for predicting or monitoring response to treatment v Circulating tumour markers for cancer testing and noninvasive prenatal diagnosis: § nucleic acids : detection of gene mutations, chromosomal rearrangements, microsatellite alterations, viral sequences, gene promoter hypermethylation and changes in microarray-generated profiles (genetic signatures) § hormones, enzymes, glycoproteins, oncofoetal antigens and receptors 33
 Children and Cancer v Proteomics: promising for the analysis of biological fluids and biomarker identification. v Fetal-derived epigenetic markers in maternal plasma: differences between the maternal and the fetal DNA. v Ideal factors for a serological tumour biomarker: § Produced by the tumour cells and can also enter the circulation § Present at low levels in the serum of healthy individuals and those with benign disease but increases substantially in cancer (preferably in one cancer type only) § Easily quantifiable with an inexpensive assay § Present in detectable (or higher than normal) quantities at early or preclinical stages § Quantitative levels of the tumour marker reflect the tumour burden § High diagnostic sensitivity (few false negatives) and specificity (few false positives) 34
Children and Cancer v Proteomics: promising for the analysis of biological fluids and biomarker identification. v Fetal-derived epigenetic markers in maternal plasma: differences between the maternal and the fetal DNA. v Ideal factors for a serological tumour biomarker: § Produced by the tumour cells and can also enter the circulation § Present at low levels in the serum of healthy individuals and those with benign disease but increases substantially in cancer (preferably in one cancer type only) § Easily quantifiable with an inexpensive assay § Present in detectable (or higher than normal) quantities at early or preclinical stages § Quantitative levels of the tumour marker reflect the tumour burden § High diagnostic sensitivity (few false negatives) and specificity (few false positives) 34
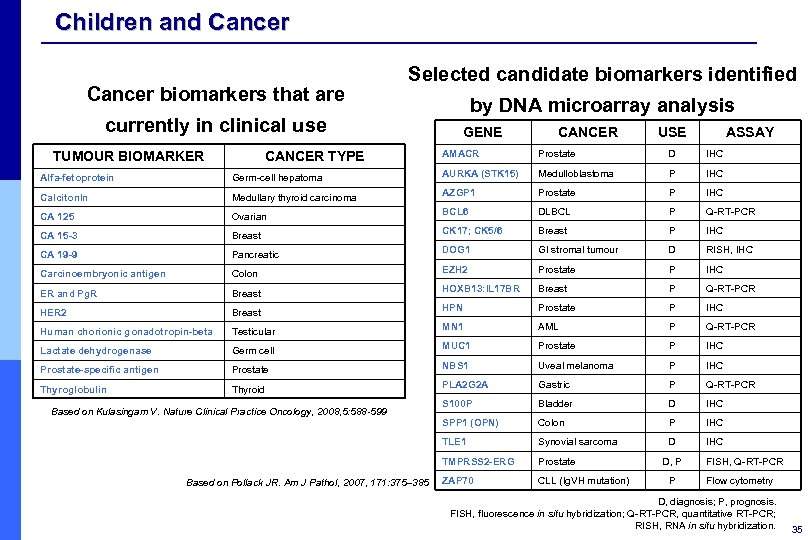 Children and Cancer biomarkers that are Selected candidate biomarkers identified currently in clinical use TUMOUR BIOMARKER CANCER TYPE by DNA microarray analysis GENE CANCER USE ASSAY AMACR Prostate D IHC Alfa-fetoprotein Germ-cell hepatoma AURKA (STK 15) Medulloblastoma P IHC Calciton. In Medullary thyroid carcinoma AZGP 1 Prostate P IHC CA 125 Ovarian BCL 6 DLBCL P Q-RT-PCR CA 15 -3 Breast CK 17; CK 5/6 Breast P IHC CA 19 -9 Pancreatic DOG 1 GI stromal tumour D RISH, IHC Carcinoembryonic antigen Colon EZH 2 Prostate P IHC ER and Pg. R Breast HOXB 13: IL 17 BR Breast P Q-RT-PCR HER 2 Breast HPN Prostate P IHC Human chorionic gonadotropin-beta Testicular MN 1 AML P Q-RT-PCR Lactate dehydrogenase Germ cell MUC 1 Prostate P IHC Prostate-specific antigen Prostate NBS 1 Uveal melanoma P IHC Thyroglobulin Thyroid PLA 2 G 2 A Gastric P Q-RT-PCR S 100 P Bladder D IHC SPP 1 (OPN) Colon P IHC TLE 1 Synovial sarcoma D IHC TMPRSS 2 -ERG Prostate ZAP 70 CLL (Ig. VH mutation) Based on Kulasingam V. Nature Clinical Practice Oncology, 2008, 5: 588 -599 Based on Pollack JR. Am J Pathol, 2007, 171: 375– 385 D, P P FISH, Q-RT-PCR Flow cytometry D, diagnosis; P, prognosis. FISH, fluorescence in situ hybridization; Q-RT-PCR, quantitative RT-PCR; RISH, RNA in situ hybridization. 35
Children and Cancer biomarkers that are Selected candidate biomarkers identified currently in clinical use TUMOUR BIOMARKER CANCER TYPE by DNA microarray analysis GENE CANCER USE ASSAY AMACR Prostate D IHC Alfa-fetoprotein Germ-cell hepatoma AURKA (STK 15) Medulloblastoma P IHC Calciton. In Medullary thyroid carcinoma AZGP 1 Prostate P IHC CA 125 Ovarian BCL 6 DLBCL P Q-RT-PCR CA 15 -3 Breast CK 17; CK 5/6 Breast P IHC CA 19 -9 Pancreatic DOG 1 GI stromal tumour D RISH, IHC Carcinoembryonic antigen Colon EZH 2 Prostate P IHC ER and Pg. R Breast HOXB 13: IL 17 BR Breast P Q-RT-PCR HER 2 Breast HPN Prostate P IHC Human chorionic gonadotropin-beta Testicular MN 1 AML P Q-RT-PCR Lactate dehydrogenase Germ cell MUC 1 Prostate P IHC Prostate-specific antigen Prostate NBS 1 Uveal melanoma P IHC Thyroglobulin Thyroid PLA 2 G 2 A Gastric P Q-RT-PCR S 100 P Bladder D IHC SPP 1 (OPN) Colon P IHC TLE 1 Synovial sarcoma D IHC TMPRSS 2 -ERG Prostate ZAP 70 CLL (Ig. VH mutation) Based on Kulasingam V. Nature Clinical Practice Oncology, 2008, 5: 588 -599 Based on Pollack JR. Am J Pathol, 2007, 171: 375– 385 D, P P FISH, Q-RT-PCR Flow cytometry D, diagnosis; P, prognosis. FISH, fluorescence in situ hybridization; Q-RT-PCR, quantitative RT-PCR; RISH, RNA in situ hybridization. 35
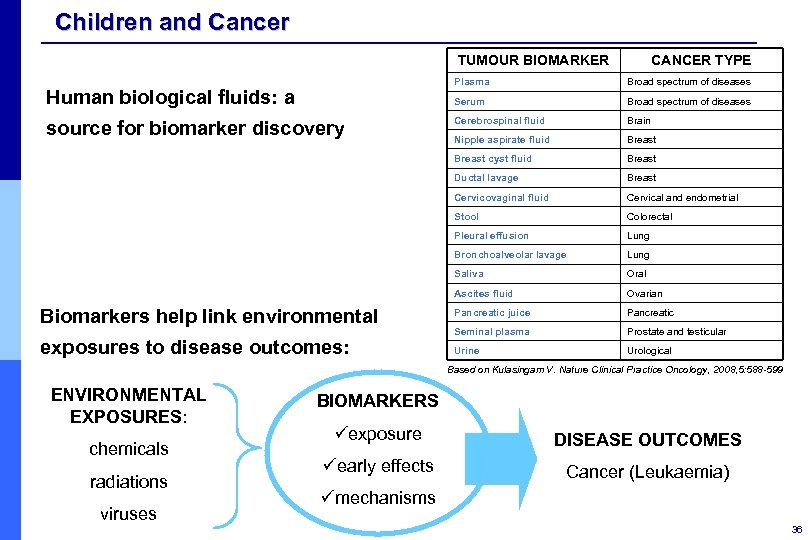 Children and Cancer TUMOUR BIOMARKER CANCER TYPE Plasma Broad spectrum of diseases Serum Broad spectrum of diseases Cerebrospinal fluid Brain Nipple aspirate fluid Breast cyst fluid Breast Ductal lavage Breast Cervicovaginal fluid Cervical and endometrial Stool Colorectal Pleural effusion Lung Bronchoalveolar lavage Lung Saliva Oral Ascites fluid Ovarian Biomarkers help link environmental Pancreatic juice Pancreatic exposures to disease outcomes: Seminal plasma Prostate and testicular Urine Urological Human biological fluids: a source for biomarker discovery Based on Kulasingam V. Nature Clinical Practice Oncology, 2008, 5: 588 -599 ENVIRONMENTAL EXPOSURES: chemicals radiations viruses BIOMARKERS üexposure DISEASE OUTCOMES üearly effects Cancer (Leukaemia) ümechanisms 36
Children and Cancer TUMOUR BIOMARKER CANCER TYPE Plasma Broad spectrum of diseases Serum Broad spectrum of diseases Cerebrospinal fluid Brain Nipple aspirate fluid Breast cyst fluid Breast Ductal lavage Breast Cervicovaginal fluid Cervical and endometrial Stool Colorectal Pleural effusion Lung Bronchoalveolar lavage Lung Saliva Oral Ascites fluid Ovarian Biomarkers help link environmental Pancreatic juice Pancreatic exposures to disease outcomes: Seminal plasma Prostate and testicular Urine Urological Human biological fluids: a source for biomarker discovery Based on Kulasingam V. Nature Clinical Practice Oncology, 2008, 5: 588 -599 ENVIRONMENTAL EXPOSURES: chemicals radiations viruses BIOMARKERS üexposure DISEASE OUTCOMES üearly effects Cancer (Leukaemia) ümechanisms 36
 Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 37
Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 37
 Children and Cancer EXPOSURE ASSESSMENT Objective: obtaining measurements quantifying effects a) Environmental b) Occupational c) Biological 38
Children and Cancer EXPOSURE ASSESSMENT Objective: obtaining measurements quantifying effects a) Environmental b) Occupational c) Biological 38
 Children and Cancer EXPOSURE ASSESSMENT Approaches v Questionnaire data v Laboratory measurement § Environmental § Biological § Molecular genetic evidence 39
Children and Cancer EXPOSURE ASSESSMENT Approaches v Questionnaire data v Laboratory measurement § Environmental § Biological § Molecular genetic evidence 39
 Children and Cancer EXPOSURE ASSESSMENT Challenges v Relevant past exposures v Recall variation in affected vs. healthy v Varying levels of exposures v Relation with growth, development, behaviour 40
Children and Cancer EXPOSURE ASSESSMENT Challenges v Relevant past exposures v Recall variation in affected vs. healthy v Varying levels of exposures v Relation with growth, development, behaviour 40
 Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 41
Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 41
 Children and Cancer CHILDHOOD CANCER CLUSTERS Cluster definition: notable aggregations of cases in v. Geographic proximity v. Similar temporal onset seemingly statistically higher incidence than expected 42
Children and Cancer CHILDHOOD CANCER CLUSTERS Cluster definition: notable aggregations of cases in v. Geographic proximity v. Similar temporal onset seemingly statistically higher incidence than expected 42
 Children and Cancer CHILDHOOD CANCER CLUSTERS Residential/school proximity v Manufacturing facilities/waste sites v Underground storage tanks v Environmental/industrial accidents 43
Children and Cancer CHILDHOOD CANCER CLUSTERS Residential/school proximity v Manufacturing facilities/waste sites v Underground storage tanks v Environmental/industrial accidents 43
 Children and Cancer CHILDHOOD CANCER CLUSTERS Analysis of clusters v Define the minimum number of cases (rare disease small number of cases) v Type of cluster: § Transient: occurring in given period and disappearing § Prolonged: persisting, new cases developing v Define: § Homogeneous/heterogeneous types of cancer § Designate temporal and geographic boundaries (latency periods may be long) 44
Children and Cancer CHILDHOOD CANCER CLUSTERS Analysis of clusters v Define the minimum number of cases (rare disease small number of cases) v Type of cluster: § Transient: occurring in given period and disappearing § Prolonged: persisting, new cases developing v Define: § Homogeneous/heterogeneous types of cancer § Designate temporal and geographic boundaries (latency periods may be long) 44
 Children and Cancer CHILDHOOD CANCER CLUSTERS Reporting cancer clusters 1. Logical time sequence (i. e. cause preceded effect) 2. Specificity of effect (i. e. same type of cancer) 3. Dose-response relationship 4. Biologic plausibility 5. Consistency with other observations 6. Exclusion of concomitant variables 7. Disappearance of effect when cause removed 45
Children and Cancer CHILDHOOD CANCER CLUSTERS Reporting cancer clusters 1. Logical time sequence (i. e. cause preceded effect) 2. Specificity of effect (i. e. same type of cancer) 3. Dose-response relationship 4. Biologic plausibility 5. Consistency with other observations 6. Exclusion of concomitant variables 7. Disappearance of effect when cause removed 45
 Children and Cancer CHILDHOOD CANCER CLUSTERS Chernobyl childhood thyroid cluster April 26, 1986 - nuclear reactor 4 releases 1311 § Total numbers reported § Mainly papillary thyroid cancer (aggressive) Num. cases 1986 2 1987 4 1988 Incidence thyroid cancer in Belarus (0 -15 yrs age) Year 5 1989 6 1990 29 1991 30 1992 50 46
Children and Cancer CHILDHOOD CANCER CLUSTERS Chernobyl childhood thyroid cluster April 26, 1986 - nuclear reactor 4 releases 1311 § Total numbers reported § Mainly papillary thyroid cancer (aggressive) Num. cases 1986 2 1987 4 1988 Incidence thyroid cancer in Belarus (0 -15 yrs age) Year 5 1989 6 1990 29 1991 30 1992 50 46
 Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 47
Children and Cancer OVERVIEW 1. INCIDENCE AND TYPES OF CHILDHOOD CANCER 2. CAUSES, RISK FACTORS AND HYPOTHESES 3. BIOLOGICAL PROCESSES LEADING TO CANCER DEVELOPMENT 4. EXPOSURE ASSESSMENT AND ITS CHALLENGES 5. INVESTIGATING POTENTIAL CANCER CLUSTERS 6. QUESTIONS FROM PARENTS 47
 Children and Cancer PREVENTION 1. Avoid smoking/SHTS, chewing tobacco 2. Sun protection 3. Diet § § fibre fat salt / smoke, cured food carotenoids aflatoxins 4. Test for radon, asbestos (mitigate risks) 48
Children and Cancer PREVENTION 1. Avoid smoking/SHTS, chewing tobacco 2. Sun protection 3. Diet § § fibre fat salt / smoke, cured food carotenoids aflatoxins 4. Test for radon, asbestos (mitigate risks) 48
 Children and Cancer EARLY CHILDHOOD EXPOSURES Predisposing to adult cancer 1. Ionising radiation breast cancer, ALL, thyroid cancer 2. Radiotherapy for Hodgkin’s disease osteosarcoma, leukaemia, skin cancer, breast cancer, soft tissue sarcoma 3. UV sunlight melanoma, basal and squamous cell carcinomas 4. Tobacco 5. Asbestos 6. Diet - fats and aflatoxins cancer colon, breast, and Liver 49
Children and Cancer EARLY CHILDHOOD EXPOSURES Predisposing to adult cancer 1. Ionising radiation breast cancer, ALL, thyroid cancer 2. Radiotherapy for Hodgkin’s disease osteosarcoma, leukaemia, skin cancer, breast cancer, soft tissue sarcoma 3. UV sunlight melanoma, basal and squamous cell carcinomas 4. Tobacco 5. Asbestos 6. Diet - fats and aflatoxins cancer colon, breast, and Liver 49
 Children and Cancer We hold our future in our hands and it is our children. Poster Contest by HRIDAY with support from WHO SEARO 50
Children and Cancer We hold our future in our hands and it is our children. Poster Contest by HRIDAY with support from WHO SEARO 50
 Children and Cancer ACKNOWLEDGEMENTS WHO is grateful to the US EPA Office of Children’s Health Protection for the financial support that made this project possible and for some of the data, graphics and text used in preparing these materials. First draft prepared by Irena Buka, MD, Canada With the advice of the Working Group Members on Training Package for the Health Sector: Cristina Alonzo, MD (Uruguay); Yona Amitai, MD, MPH (Israel); Stephan Boese-O’Reilly, MD, MPH (Germany); Stephania Borgo, MD (ISDE, Italy); Irena Buka, MD (Canada); Lilian Corra, MD (Argentina); Ligia Fruchtengarten, MD (Brazil); Amalia Laborde, MD (Uruguay); Leda Nemer, TO (WHO/EURO); R. Romizzi, MD (ISDE, Italy); Katherine M. Shea, MD, MPH (USA). Reviewer: Carolina Espina, Ph. D (Spain) WHO CEH Training Project Coordination: Jenny Pronczuk, MD Medical Consultant: Ruth A. Etzel, MD, Ph. D Technical Assistance: Marie-Noël Bruné, MSc Latest update: December 2009 51
Children and Cancer ACKNOWLEDGEMENTS WHO is grateful to the US EPA Office of Children’s Health Protection for the financial support that made this project possible and for some of the data, graphics and text used in preparing these materials. First draft prepared by Irena Buka, MD, Canada With the advice of the Working Group Members on Training Package for the Health Sector: Cristina Alonzo, MD (Uruguay); Yona Amitai, MD, MPH (Israel); Stephan Boese-O’Reilly, MD, MPH (Germany); Stephania Borgo, MD (ISDE, Italy); Irena Buka, MD (Canada); Lilian Corra, MD (Argentina); Ligia Fruchtengarten, MD (Brazil); Amalia Laborde, MD (Uruguay); Leda Nemer, TO (WHO/EURO); R. Romizzi, MD (ISDE, Italy); Katherine M. Shea, MD, MPH (USA). Reviewer: Carolina Espina, Ph. D (Spain) WHO CEH Training Project Coordination: Jenny Pronczuk, MD Medical Consultant: Ruth A. Etzel, MD, Ph. D Technical Assistance: Marie-Noël Bruné, MSc Latest update: December 2009 51
 Children and Cancer DISCLAIMER p p p The designations employed and the presentation of the material in this publication do not imply the expression of any opinion whatsoever on the part of the World Health Organization concerning the legal status of any country, territory, city or area or of its authorities, or concerning the delimitation of its frontiers or boundaries. Dotted lines on maps represent approximate border lines for which there may not yet be full agreement. The mention of specific companies or of certain manufacturers’ products does not imply that they are endorsed or recommended by the World Health Organization in preference to others of a similar nature that are not mentioned. Errors and omissions excepted, the names of proprietary products are distinguished by initial capital letters. The opinions and conclusions expressed do not necessarily represent the official position of the World Health Organization. This publication is being distributed without warranty of any kind, either express or implied. In no event shall the World Health Organization be liable for damages, including any general, special, incidental, or consequential damages, arising out of the use of this publication The contents of this training module are based upon references available in the published literature as of its last update. Users are encouraged to search standard medical databases for updates in the science for issues of particular interest or sensitivity in their regions and areas of specific concern. If users of this training module should find it necessary to make any modifications (abridgement, addition or deletion) to the presentation, the adaptor shall be responsible for all modifications made. The World Health Organization disclaims all responsibility for adaptations made by others. All modifications shall be clearly distinguished from the original WHO material. 52
Children and Cancer DISCLAIMER p p p The designations employed and the presentation of the material in this publication do not imply the expression of any opinion whatsoever on the part of the World Health Organization concerning the legal status of any country, territory, city or area or of its authorities, or concerning the delimitation of its frontiers or boundaries. Dotted lines on maps represent approximate border lines for which there may not yet be full agreement. The mention of specific companies or of certain manufacturers’ products does not imply that they are endorsed or recommended by the World Health Organization in preference to others of a similar nature that are not mentioned. Errors and omissions excepted, the names of proprietary products are distinguished by initial capital letters. The opinions and conclusions expressed do not necessarily represent the official position of the World Health Organization. This publication is being distributed without warranty of any kind, either express or implied. In no event shall the World Health Organization be liable for damages, including any general, special, incidental, or consequential damages, arising out of the use of this publication The contents of this training module are based upon references available in the published literature as of its last update. Users are encouraged to search standard medical databases for updates in the science for issues of particular interest or sensitivity in their regions and areas of specific concern. If users of this training module should find it necessary to make any modifications (abridgement, addition or deletion) to the presentation, the adaptor shall be responsible for all modifications made. The World Health Organization disclaims all responsibility for adaptations made by others. All modifications shall be clearly distinguished from the original WHO material. 52


