21a31214661daaabdc2738b32fb7dbdc.ppt
- Количество слайдов: 58

 This slide presentation will review data from a study conducted by the Los Angeles County HIV Epidemiology Program to examine HIV prevalence, incidence, and risk behaviors among men seeking HIV testing and prevention services in two bathhouses in Los Angeles county. For the sake of brevity, we call this project the Bathhouse Study. This project was funded by the Centers for Disease Control and Prevention through their Prevention Services Research Branch. The Principal Investigator in charge of this study Trista Bingham. Trista is an Epidemiologist and she is Chief of the Seroepidemiology Unit at the HIV Epidemiology Program.
This slide presentation will review data from a study conducted by the Los Angeles County HIV Epidemiology Program to examine HIV prevalence, incidence, and risk behaviors among men seeking HIV testing and prevention services in two bathhouses in Los Angeles county. For the sake of brevity, we call this project the Bathhouse Study. This project was funded by the Centers for Disease Control and Prevention through their Prevention Services Research Branch. The Principal Investigator in charge of this study Trista Bingham. Trista is an Epidemiologist and she is Chief of the Seroepidemiology Unit at the HIV Epidemiology Program.

 To provide some background and context as a framework for the Bathhouse Study, a few facts should be noted before describing this project. Early on in the HIV/AIDS epidemic, some jurisdictions that had commercial sex venues such as bathhouses forced those establishments out of business. However, bathhouses were never forced to close in Los Angeles County. In lieu of closing local bathhouses, certain conditions of operation were established and bathhouses were monitored for compliance with these conditions. In short, bathhouse owners were to ensure that patrons had adequate access to free condoms and safer sex messages were to be posted in common areas.
To provide some background and context as a framework for the Bathhouse Study, a few facts should be noted before describing this project. Early on in the HIV/AIDS epidemic, some jurisdictions that had commercial sex venues such as bathhouses forced those establishments out of business. However, bathhouses were never forced to close in Los Angeles County. In lieu of closing local bathhouses, certain conditions of operation were established and bathhouses were monitored for compliance with these conditions. In short, bathhouse owners were to ensure that patrons had adequate access to free condoms and safer sex messages were to be posted in common areas.
 Two surveys conducted prior to the Bathhouse Study, one by Van Beneden in 2002 and Richwald, et al. in 1988, indicated that 10% to 11% of bathhouse patrons reported engaging in unprotected anal sex when having sex with other bathhouse patrons. Both studies were conducted as exit surveys in which patrons were questioned about their behaviors as they left the bathhouse premises. Also, there was considerable anecdotal evidence that after the widespread availability and use of highly active antiretroviral therapies, safer sex behaviors were waning. Finally, the syphilis outbreak in Los Angeles county in 2000, in which some cases reported frequenting commercial sex venues, lent credence to the anecdotal reports of waning safer sex practices.
Two surveys conducted prior to the Bathhouse Study, one by Van Beneden in 2002 and Richwald, et al. in 1988, indicated that 10% to 11% of bathhouse patrons reported engaging in unprotected anal sex when having sex with other bathhouse patrons. Both studies were conducted as exit surveys in which patrons were questioned about their behaviors as they left the bathhouse premises. Also, there was considerable anecdotal evidence that after the widespread availability and use of highly active antiretroviral therapies, safer sex behaviors were waning. Finally, the syphilis outbreak in Los Angeles county in 2000, in which some cases reported frequenting commercial sex venues, lent credence to the anecdotal reports of waning safer sex practices.

 The objectives of the Bathhouse Study were as follows: The first phase of this project was a formative research phase design to conducted qualitative data to describe thinks like: 1) a typical bathhouse visit; 2) patron characteristics; and 3) sexual practices. The study was also designed to estimate the incidence of HIV among patrons using a specific methodology to distinguish between a new and a longstanding HIV infection. In general, HIV incident cases are those new cases of HIV that occur within a 12 month period. The testing methodology used to estimate HIV incidence will be described in a later slide. Another key component of the study was the effort to describe the HIV risk profiles of bathhouse patrons and examine attitudes that may impact their likelihood of engaging in or refraining from HIV risk behaviors. Also, a primary objective was to set up an infrastructure for on-site HIV/STD testing in participating bathhouse venues that could be transferred to community -based organizations (CBO) after completion of the study.
The objectives of the Bathhouse Study were as follows: The first phase of this project was a formative research phase design to conducted qualitative data to describe thinks like: 1) a typical bathhouse visit; 2) patron characteristics; and 3) sexual practices. The study was also designed to estimate the incidence of HIV among patrons using a specific methodology to distinguish between a new and a longstanding HIV infection. In general, HIV incident cases are those new cases of HIV that occur within a 12 month period. The testing methodology used to estimate HIV incidence will be described in a later slide. Another key component of the study was the effort to describe the HIV risk profiles of bathhouse patrons and examine attitudes that may impact their likelihood of engaging in or refraining from HIV risk behaviors. Also, a primary objective was to set up an infrastructure for on-site HIV/STD testing in participating bathhouse venues that could be transferred to community -based organizations (CBO) after completion of the study.

 In this presentation, the following objectives will be met. First, the formative research methods and findings will be reviewed. Second, findings from the Epidemiologic, or quantitative research phase will be presented. These findings represent a subset of 676 participants out of 916 total participants in the epidemiologic research phase. Lastly, implications of the findings for future intervention and prevention work in commerical sex venues will be reviewed.
In this presentation, the following objectives will be met. First, the formative research methods and findings will be reviewed. Second, findings from the Epidemiologic, or quantitative research phase will be presented. These findings represent a subset of 676 participants out of 916 total participants in the epidemiologic research phase. Lastly, implications of the findings for future intervention and prevention work in commerical sex venues will be reviewed.

 In the formative research phase, two distinct groups were selected for interview. Sixteen systems interviews were conducted. In these, bathhouse staff, bathhouse management, and prevention outreach workers assigned to bathhouses were interviewed. Additionally, 23 key participant interviews were conducted. Bathhouse patrons participated in the key participant interviews. The study instrument used in the formative research phase was a semi -structured questionnaire. As such, most questions in this qualitative phase of the study are open-ended to allow for broad responses from the participants. For analysis of the qualitative data obtained during this phase, EZText software was used for data coding. This software was designed by the Centers for Disease Control and Prevention.
In the formative research phase, two distinct groups were selected for interview. Sixteen systems interviews were conducted. In these, bathhouse staff, bathhouse management, and prevention outreach workers assigned to bathhouses were interviewed. Additionally, 23 key participant interviews were conducted. Bathhouse patrons participated in the key participant interviews. The study instrument used in the formative research phase was a semi -structured questionnaire. As such, most questions in this qualitative phase of the study are open-ended to allow for broad responses from the participants. For analysis of the qualitative data obtained during this phase, EZText software was used for data coding. This software was designed by the Centers for Disease Control and Prevention.

 Several key interview topics were covered during each formative interview. Participants were asked to describe a typical bathhouse visit, describe their observations of the sexual behavior and condom use of bathhouse patrons, and comment on sexual communication between patrons. Participants were asked to comment on the extent to which patrons engaged in disclosure regarding serostatus and assumptions about the serostatus of other patrons. Also, participants were asked about their perceptions of alcohol and drug use among patrons and participants were asked to reveal their attitudes and beliefs about having a HIV/STD testing clinic located in the bathhouse.
Several key interview topics were covered during each formative interview. Participants were asked to describe a typical bathhouse visit, describe their observations of the sexual behavior and condom use of bathhouse patrons, and comment on sexual communication between patrons. Participants were asked to comment on the extent to which patrons engaged in disclosure regarding serostatus and assumptions about the serostatus of other patrons. Also, participants were asked about their perceptions of alcohol and drug use among patrons and participants were asked to reveal their attitudes and beliefs about having a HIV/STD testing clinic located in the bathhouse.

 This slide shows some of the findings from the formative research. First, formative research participants felt that, on average, 85% of bathhouse patrons never discuss HIV status with partners before engaging in sex with those partners. Formative research participants indicated that a prevailing assumption about healthy looking men is that those men are HIV negative. Also, men who engage in anal receptive sex (bottoms) are assumed to be HIV positive and men who engage in insertive anal sex (tops) are assumed to be HIV negative.
This slide shows some of the findings from the formative research. First, formative research participants felt that, on average, 85% of bathhouse patrons never discuss HIV status with partners before engaging in sex with those partners. Formative research participants indicated that a prevailing assumption about healthy looking men is that those men are HIV negative. Also, men who engage in anal receptive sex (bottoms) are assumed to be HIV positive and men who engage in insertive anal sex (tops) are assumed to be HIV negative.

 When asked about their views regarding the planned HIV testing clinic in the bathhouses, participants expressed several key structural concerns and several key concerns regarding incentives and marketing. Structural concerns were such things as ensuring that clinic services were provided in a manner that maximized privacy and anonymity. Additionally, participants felt that the clinic should be comfortable and casual and they felt strongly that disclosures of positive laboratory findings should occur off-site. Formative research participants also felt that additional incentives would increase clinic use [ADDITIONAL SUCH AS? ? ? ] and additional services such as STD testing would increase patron visits to the clinic. Lastly, participants felt that the addition of promotional cards, ads, flyers, and signage would increase patron awareness of the clinic and clinic services.
When asked about their views regarding the planned HIV testing clinic in the bathhouses, participants expressed several key structural concerns and several key concerns regarding incentives and marketing. Structural concerns were such things as ensuring that clinic services were provided in a manner that maximized privacy and anonymity. Additionally, participants felt that the clinic should be comfortable and casual and they felt strongly that disclosures of positive laboratory findings should occur off-site. Formative research participants also felt that additional incentives would increase clinic use [ADDITIONAL SUCH AS? ? ? ] and additional services such as STD testing would increase patron visits to the clinic. Lastly, participants felt that the addition of promotional cards, ads, flyers, and signage would increase patron awareness of the clinic and clinic services.


 A cross-sectional HIV incidence study design was used. In a cross-sectional study, subjects are not followed over time but are interviewed at one point in time. This cross-sectional study is a convenience sample of men who sought HIV testing at one of two on-site HIV testing centers at the bathhouses. Participants were tested for HIV, syphilis, and Hepatitis B. Participants had the option to decline testing for syphilis and Hepatitis B. Participants were given pre- and post-test counseling using the Project RESPECT counseling methods. After completion of the quantitative interview, participants were given an entertainment voucher valued at $15 for completing the survey. Vouchers were redeemable at local fast food restaurants. Participants were tested for gonorrhea and chlamydia using urine-based tests. Subjects were given the option to elect to return in person for their test results or call-in for their results a week later.
A cross-sectional HIV incidence study design was used. In a cross-sectional study, subjects are not followed over time but are interviewed at one point in time. This cross-sectional study is a convenience sample of men who sought HIV testing at one of two on-site HIV testing centers at the bathhouses. Participants were tested for HIV, syphilis, and Hepatitis B. Participants had the option to decline testing for syphilis and Hepatitis B. Participants were given pre- and post-test counseling using the Project RESPECT counseling methods. After completion of the quantitative interview, participants were given an entertainment voucher valued at $15 for completing the survey. Vouchers were redeemable at local fast food restaurants. Participants were tested for gonorrhea and chlamydia using urine-based tests. Subjects were given the option to elect to return in person for their test results or call-in for their results a week later.
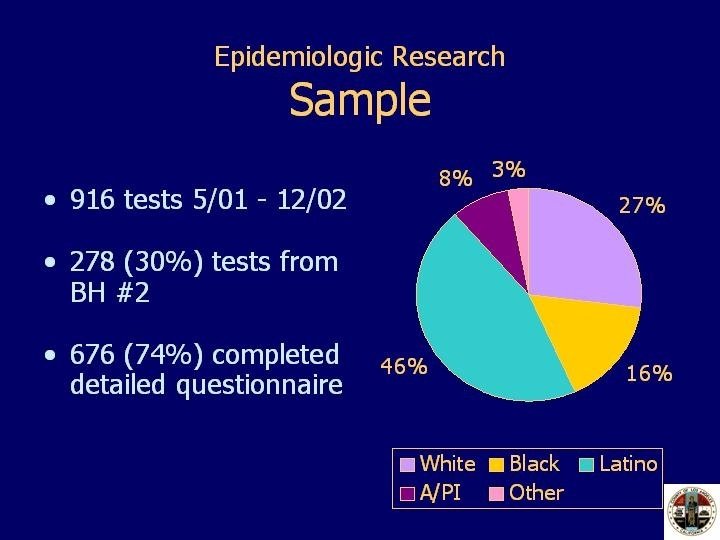
 916 HIV tests were administered during 19 months of subject recruitment. 278 of 916 (30%) were recruited from Bathhouse #2. Due to problems with completing the construction of the counseling and testing rooms, recruitment at this site didn’t begin until much later in the project. Of all subjects tested, 676 (74%) completed the detailed quantitative questionnaire. Latinos made up the majority of the sample, 46%. Of all Latino participants, 76% were of Mexican origin, another 11% were of Central American origin and yet another 7% were South American. A couple were Puerto Rican and a couple were Cuban. Twenty-seven percent of the sample were White, 16% were Black, 8% were Asian/Pacific-Islander, and three percent were classified as Other usually included persons of mixed-race.
916 HIV tests were administered during 19 months of subject recruitment. 278 of 916 (30%) were recruited from Bathhouse #2. Due to problems with completing the construction of the counseling and testing rooms, recruitment at this site didn’t begin until much later in the project. Of all subjects tested, 676 (74%) completed the detailed quantitative questionnaire. Latinos made up the majority of the sample, 46%. Of all Latino participants, 76% were of Mexican origin, another 11% were of Central American origin and yet another 7% were South American. A couple were Puerto Rican and a couple were Cuban. Twenty-seven percent of the sample were White, 16% were Black, 8% were Asian/Pacific-Islander, and three percent were classified as Other usually included persons of mixed-race.
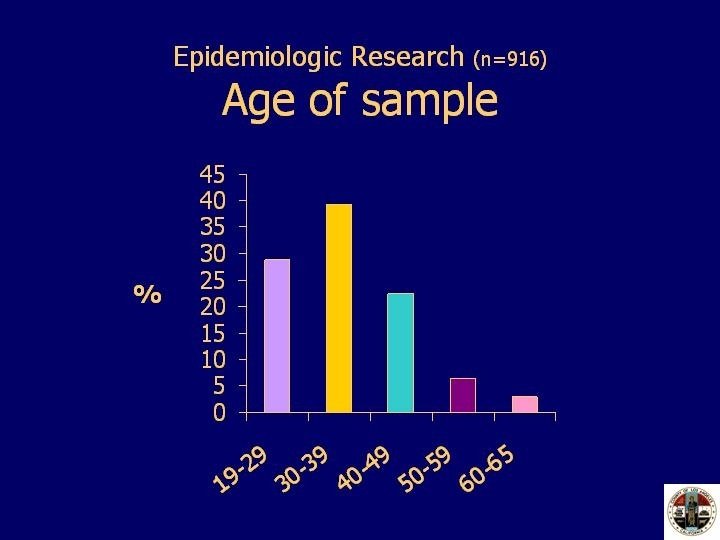
 This slide illustrates the age of the study sample, including those who did not participate in the quantitative survey. The majority of the participants were between the ages of 19 and 39. Twenty-nine percent were between the ages of 19 to 29, and 39% were between the ages of 30 to 39. Twenty-two percent of the sample were 40 to 49, 6% were 50 to 59, and 3% were 60 to 65 years of age.
This slide illustrates the age of the study sample, including those who did not participate in the quantitative survey. The majority of the participants were between the ages of 19 and 39. Twenty-nine percent were between the ages of 19 to 29, and 39% were between the ages of 30 to 39. Twenty-two percent of the sample were 40 to 49, 6% were 50 to 59, and 3% were 60 to 65 years of age.

 As mentioned earlier 676 participants completed a quantitative interview. Participants were asked whether they identified as homosexual/gay, heterosexual, bisexual, or don’t identify. Four-hundred-sixty-eight (69%) self-identified as homosexual/gay. Seven (1%) identified as heterosexual, 189 (28%) identified as bisexual, and 10 (1%) did not selfidentify. Two subjects did not answer. Participants were also asked about the extent to which they had disclosed their sexual identify to friends, family, co-workers, etc. Thirty-nine percent said they were out to half of those they know, 36% said they were out to everyone they know, and 25% said they were out to only a few or to none of those they know.
As mentioned earlier 676 participants completed a quantitative interview. Participants were asked whether they identified as homosexual/gay, heterosexual, bisexual, or don’t identify. Four-hundred-sixty-eight (69%) self-identified as homosexual/gay. Seven (1%) identified as heterosexual, 189 (28%) identified as bisexual, and 10 (1%) did not selfidentify. Two subjects did not answer. Participants were also asked about the extent to which they had disclosed their sexual identify to friends, family, co-workers, etc. Thirty-nine percent said they were out to half of those they know, 36% said they were out to everyone they know, and 25% said they were out to only a few or to none of those they know.

 Interview participants were also asked about their reasons for frequenting bathhouses. Subjects were allowed to indicate all reasons that applied to them. Ninety-one percent indicated that they went to bathhouses for the sex, 71% said that they went specifically to engage in anonymous sex, 50% said they went to see other patrons or be seen by other patrons and 49% said they went to bathhouses because of boredom. Some of the less frequent reasons for going to the bathhouse were to blow off steam (26%), out of habit (26%) and to see friends (20%).
Interview participants were also asked about their reasons for frequenting bathhouses. Subjects were allowed to indicate all reasons that applied to them. Ninety-one percent indicated that they went to bathhouses for the sex, 71% said that they went specifically to engage in anonymous sex, 50% said they went to see other patrons or be seen by other patrons and 49% said they went to bathhouses because of boredom. Some of the less frequent reasons for going to the bathhouse were to blow off steam (26%), out of habit (26%) and to see friends (20%).

 Participants were also asked how often the frequent the bathhouse and they were asked to compare the level of HIV risk behaviors in which they engage when in the bathhouse to the level of HIV risk behaviors in which they engage in other places where they have sex. Thirty-eight percent stated that they visit the bathhouse more than twice per month. Compared to other places were they have sex, 35% say their sex habits in the bathhouse are riskier than in other places where they have sex. Forty-nine percent say their risk behaviors are the same regardless of where they have sex, and 12% say they take less risk when having sex with bathhouse patrons compared to sex partners in other venues. Subjects were also queried regarding their level of concern about contracting HIV. Thirty-nine percent said they were somewhat concerned about getting HIV and 49% said they were very concerned about getting HIV.
Participants were also asked how often the frequent the bathhouse and they were asked to compare the level of HIV risk behaviors in which they engage when in the bathhouse to the level of HIV risk behaviors in which they engage in other places where they have sex. Thirty-eight percent stated that they visit the bathhouse more than twice per month. Compared to other places were they have sex, 35% say their sex habits in the bathhouse are riskier than in other places where they have sex. Forty-nine percent say their risk behaviors are the same regardless of where they have sex, and 12% say they take less risk when having sex with bathhouse patrons compared to sex partners in other venues. Subjects were also queried regarding their level of concern about contracting HIV. Thirty-nine percent said they were somewhat concerned about getting HIV and 49% said they were very concerned about getting HIV.

 Interview subjects were asked about their risk behaviors during their most recent bathhouse visit. * Thirty-four percent admitted to substance use either just before or during their most recent bathhouse visit. * Sixteen percent indicated that they engaged in group sex during their last bathhouse visit. Group sex was defined as having two or more men at the same time. * Seventy-three percent said they engaged in oral sex without using a condom. With regard to anal sex, 47% of participants said they engaged in insertive anal sex (as a Top) during their last bathhouse visit, and 7% said that while having insertive anal sex during their last visit, they did not use a condom. Twenty-five percent of participants said they engaged in receptive anal sex (as a Bottom) during their last bathhouse visit, and 4% said that while having receptive anal sex during their last visit, they did not use a condom.
Interview subjects were asked about their risk behaviors during their most recent bathhouse visit. * Thirty-four percent admitted to substance use either just before or during their most recent bathhouse visit. * Sixteen percent indicated that they engaged in group sex during their last bathhouse visit. Group sex was defined as having two or more men at the same time. * Seventy-three percent said they engaged in oral sex without using a condom. With regard to anal sex, 47% of participants said they engaged in insertive anal sex (as a Top) during their last bathhouse visit, and 7% said that while having insertive anal sex during their last visit, they did not use a condom. Twenty-five percent of participants said they engaged in receptive anal sex (as a Bottom) during their last bathhouse visit, and 4% said that while having receptive anal sex during their last visit, they did not use a condom.

 One of the variables we wanted to address in this study was the frequency with which bathhouse patrons sought HIV testing. This was particularly relevant for assessing the utility and acceptability of having HIV counseling and testing services available in this venue after the close of this study. Ninety-one percent of participants reported testing for HIV in the past and of those who had tested before, 77% indicated that they received an HIV test within the past two years. Of those had tested previously, 67% said they sought testing from either an anonymous or confidential alternative test site, 36% said they sought HIVtesting from their primary medical doctor, and 24% said they had one or more prior HIV tests through an STD clinic. Sixty (9%) of the participants reported that they had never tested for HIV prior to participating in this study. When they were asked to give their primary reason for testing at this visit, 57% said they just wanted to know, 14% said they were testing because they have had risky sex, 14% said it was for reasons other than those provided on the questionnaire, and 10% said they sought testing at the bathhouse primarily because the on-site testing center is convenient.
One of the variables we wanted to address in this study was the frequency with which bathhouse patrons sought HIV testing. This was particularly relevant for assessing the utility and acceptability of having HIV counseling and testing services available in this venue after the close of this study. Ninety-one percent of participants reported testing for HIV in the past and of those who had tested before, 77% indicated that they received an HIV test within the past two years. Of those had tested previously, 67% said they sought testing from either an anonymous or confidential alternative test site, 36% said they sought HIVtesting from their primary medical doctor, and 24% said they had one or more prior HIV tests through an STD clinic. Sixty (9%) of the participants reported that they had never tested for HIV prior to participating in this study. When they were asked to give their primary reason for testing at this visit, 57% said they just wanted to know, 14% said they were testing because they have had risky sex, 14% said it was for reasons other than those provided on the questionnaire, and 10% said they sought testing at the bathhouse primarily because the on-site testing center is convenient.

 This slide reviews the mean and median number of oral or anal sex partners in the six months prior to interview. Mean is the another term for an average. Median is the middle observation among all numerically ordered observations for a particular variable. The median is a better statistic when there are extreme values on either side, because extreme high or low values can significantly impact the mean, but they have no impact on the median because it is simply the middle value. The mean number of sex partners in the six months prior to interview was 31 and the median, 15. The mean number of sex partner contacts within the bathhouse setting during the past six months was 25 and the median 8 and the mean number of sex partner contacts outside the bathhouse setting was 9 and the median 3. For each category above, there were some participants who had a large number of sex partners, thereby elevating the mean value. Therefore, the median is a better statistic for interpreting these results. Overall, these findings suggest a high level of sexual activity overall, with more sexual contacts in the bathhouse setting than in other settings. It is important to note data from a previous slide which demonstrates that most of the sexual partnering was restricted to oral sex.
This slide reviews the mean and median number of oral or anal sex partners in the six months prior to interview. Mean is the another term for an average. Median is the middle observation among all numerically ordered observations for a particular variable. The median is a better statistic when there are extreme values on either side, because extreme high or low values can significantly impact the mean, but they have no impact on the median because it is simply the middle value. The mean number of sex partners in the six months prior to interview was 31 and the median, 15. The mean number of sex partner contacts within the bathhouse setting during the past six months was 25 and the median 8 and the mean number of sex partner contacts outside the bathhouse setting was 9 and the median 3. For each category above, there were some participants who had a large number of sex partners, thereby elevating the mean value. Therefore, the median is a better statistic for interpreting these results. Overall, these findings suggest a high level of sexual activity overall, with more sexual contacts in the bathhouse setting than in other settings. It is important to note data from a previous slide which demonstrates that most of the sexual partnering was restricted to oral sex.

 Forty-eight percent of participants indicated that they frequent other venues for sex. Twenty percent indicated that they visit sex clubs in addition to bathhouses, 20% visit bookstores and pornographic video arcades where sexual contacts can be made, and 14% indicated that they frequent parks for sexual contacts. Six percent indicated that they have sex in public restrooms and 5% indicated they attend circuit parties for the purpose of engaging in sex with other men.
Forty-eight percent of participants indicated that they frequent other venues for sex. Twenty percent indicated that they visit sex clubs in addition to bathhouses, 20% visit bookstores and pornographic video arcades where sexual contacts can be made, and 14% indicated that they frequent parks for sexual contacts. Six percent indicated that they have sex in public restrooms and 5% indicated they attend circuit parties for the purpose of engaging in sex with other men.

 Seven-hundred-ninety-one syphilis screenings were done and of these 18 (2. 2%) were reactive. Eight of the participants who tested positive for syphilis indicated that they had a previous syphilis infection. One-hundred-two of 910 HIV antibody tests were positive, yielding a seroprevalence of 11%.
Seven-hundred-ninety-one syphilis screenings were done and of these 18 (2. 2%) were reactive. Eight of the participants who tested positive for syphilis indicated that they had a previous syphilis infection. One-hundred-two of 910 HIV antibody tests were positive, yielding a seroprevalence of 11%.
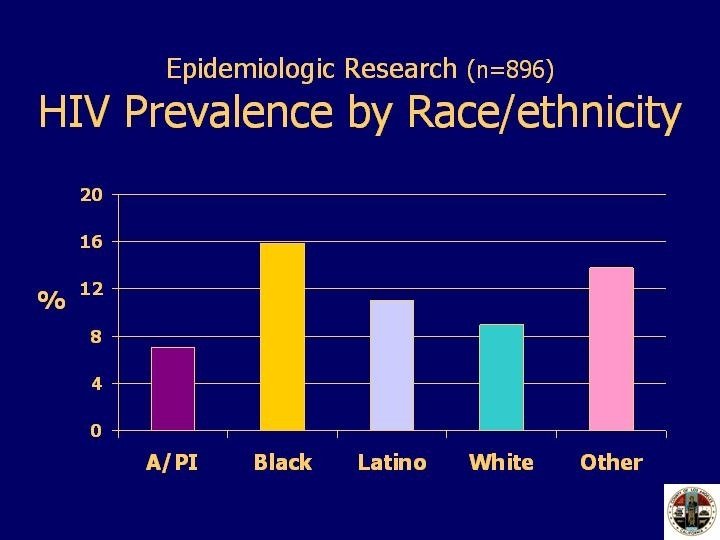
 HIV prevalence varied considerably by race/ethnicity. With the exception of Asian/Pacific Islanders, non-Whites had the highest HIV prevalence. Consistent with data from other seroprevalence studies conducted in recent years by HIV Epidemiology Program, the seroprevalence is highest among Blacks, followed by Latinos and Whites. HIV prevalence for Asian/Pacific Islanders is 7%, Blacks 16%, Latinos 11%, Whites 9% and Other 14%.
HIV prevalence varied considerably by race/ethnicity. With the exception of Asian/Pacific Islanders, non-Whites had the highest HIV prevalence. Consistent with data from other seroprevalence studies conducted in recent years by HIV Epidemiology Program, the seroprevalence is highest among Blacks, followed by Latinos and Whites. HIV prevalence for Asian/Pacific Islanders is 7%, Blacks 16%, Latinos 11%, Whites 9% and Other 14%.
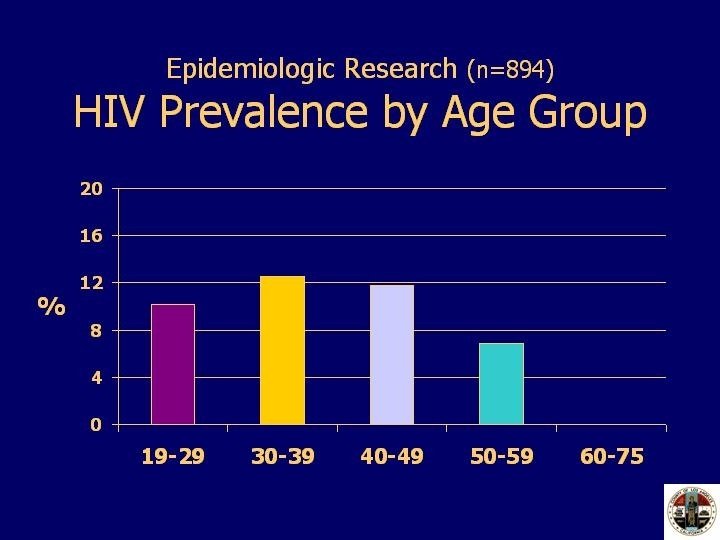
 The highest prevalence was among participants between the ages of 30 to 49. HIV prevalence was 13% in the 30 to 39 age group and 12% in the 40 to 49 age group. HIV prevalence in the younger age group, 19 to 29 was 10% followed by those age 50 to 59 at 7%. None of the participants in the 60 to 75 year age group tested positive for HIV.
The highest prevalence was among participants between the ages of 30 to 49. HIV prevalence was 13% in the 30 to 39 age group and 12% in the 40 to 49 age group. HIV prevalence in the younger age group, 19 to 29 was 10% followed by those age 50 to 59 at 7%. None of the participants in the 60 to 75 year age group tested positive for HIV.

 Only forty-one of 102 (40%) of those testing HIV positive received their test results and post-test counseling. Five-hundred-twelve of 808 HIV negative results (63%) were given to study participants. These percentages are far too low and reflects a significant problem with conducting traditional serum-based HIV testing in these venues. Shortly after the study began, it was obvious that return rates were low and within X months a protocol was initiated whereby participants could elect to telephone the researchers for results. This increased the number of persons receiving their results. Nonetheless, many of those who tested positive for HIV who chose to receive results over the phone, did not call for their results. For all tests (HIV, syphilis, gonorrhea, and chlamydia) 61% of participants received their results. These findings suggest that Rapid HIV Testing (where results are available within 20 minutes) is better suited for venues such as bathhouses.
Only forty-one of 102 (40%) of those testing HIV positive received their test results and post-test counseling. Five-hundred-twelve of 808 HIV negative results (63%) were given to study participants. These percentages are far too low and reflects a significant problem with conducting traditional serum-based HIV testing in these venues. Shortly after the study began, it was obvious that return rates were low and within X months a protocol was initiated whereby participants could elect to telephone the researchers for results. This increased the number of persons receiving their results. Nonetheless, many of those who tested positive for HIV who chose to receive results over the phone, did not call for their results. For all tests (HIV, syphilis, gonorrhea, and chlamydia) 61% of participants received their results. These findings suggest that Rapid HIV Testing (where results are available within 20 minutes) is better suited for venues such as bathhouses.

 STARHS is the acronym for the Serologic Testing Algorithm for Recent HIV Seroconversion. This testing method is designed to distinguish recent (acute) HIV infections from longstanding (chronic) HIV infections. Of all testers, there were 102 HIV positive specimens. Of those, 60 consented to storage of remnant sera for “future” HIV tests. Fifty of the sixty were serum specimens. The of the 50 HIV positive serum specimens, 40 were tested using the STARHS method. Unfortunately, the laboratory mistakenly discarded 10 of the 50 serum specimens. Of the 40 specimens tested using the STARHS methodology, 11 were “recent” infections.
STARHS is the acronym for the Serologic Testing Algorithm for Recent HIV Seroconversion. This testing method is designed to distinguish recent (acute) HIV infections from longstanding (chronic) HIV infections. Of all testers, there were 102 HIV positive specimens. Of those, 60 consented to storage of remnant sera for “future” HIV tests. Fifty of the sixty were serum specimens. The of the 50 HIV positive serum specimens, 40 were tested using the STARHS method. Unfortunately, the laboratory mistakenly discarded 10 of the 50 serum specimens. Of the 40 specimens tested using the STARHS methodology, 11 were “recent” infections.
 27. 5% of HIV positive participants showed evidence of recent infection with an HIV incidence rate of 7. 2 new infections per 100 person years.
27. 5% of HIV positive participants showed evidence of recent infection with an HIV incidence rate of 7. 2 new infections per 100 person years.
 Forty-eight percent of testers believed that fellow patrons knew their own HIV status. An interesting finding of this study is that perception of the HIV status of other bathhouse patrons depended considerably on the HIV status of the patron. Testers, all of whom believed themselves to be HIV negative at the time of testing, presumed that 38% of bathhouse patrons are HIV positive. An Exit Survey was conducted in the summer of 2002 to get information from bathhouse patrons who did not access the in-house testing clinic and therefore did not participate in the quantitative study. Exit survey participants were also asked their perception of the HIV prevalence of fellow bathhouse patrons. On average, the HIV positive Exit Survey participants believed that 65% of bathhouse patrons were HIV positive. These disparate perceptions of HIVserostatus may have important implications for risk-taking behaviors. HIV positive patrons may be less likely to engage in safe sex practices if they make assumptions that their anonymous sex partners are also HIV positive. Additionally, HIV negative partners may be more apt to take risks if they underestimate the likelihood of having sex with an HIV positive partner.
Forty-eight percent of testers believed that fellow patrons knew their own HIV status. An interesting finding of this study is that perception of the HIV status of other bathhouse patrons depended considerably on the HIV status of the patron. Testers, all of whom believed themselves to be HIV negative at the time of testing, presumed that 38% of bathhouse patrons are HIV positive. An Exit Survey was conducted in the summer of 2002 to get information from bathhouse patrons who did not access the in-house testing clinic and therefore did not participate in the quantitative study. Exit survey participants were also asked their perception of the HIV prevalence of fellow bathhouse patrons. On average, the HIV positive Exit Survey participants believed that 65% of bathhouse patrons were HIV positive. These disparate perceptions of HIVserostatus may have important implications for risk-taking behaviors. HIV positive patrons may be less likely to engage in safe sex practices if they make assumptions that their anonymous sex partners are also HIV positive. Additionally, HIV negative partners may be more apt to take risks if they underestimate the likelihood of having sex with an HIV positive partner.

 Some of the limitations of the findings are as follows: First, finding are limited due to sampling bias. This was a convenience sample, participants were not systematically selected in any way. All patrons interested in participation who believed themselves to be HIV negative were offered HIV testing and interview. Secondly, all findings regarding behaviors are based on the selfreport of participants. Some participants may not have provided entirely accurate responses to all questions. Findings from STARHS testing may be limited due to the fact that many participants declined the option to allow storing sera for STARHS testing.
Some of the limitations of the findings are as follows: First, finding are limited due to sampling bias. This was a convenience sample, participants were not systematically selected in any way. All patrons interested in participation who believed themselves to be HIV negative were offered HIV testing and interview. Secondly, all findings regarding behaviors are based on the selfreport of participants. Some participants may not have provided entirely accurate responses to all questions. Findings from STARHS testing may be limited due to the fact that many participants declined the option to allow storing sera for STARHS testing.

 This slide includes some thought for future intervention and prevention in commercial sex venues. First, at a minimum, the option to receive test results via phone should be available. Many patrons may not wish to receive their results on-site. The option to call in for results will appeal to many who do not wish to receive their results on-site. Secondly, use of rapid oral testing for HIV should substantially increase the proportion of testers who receive their results and post-test counseling. Third, recruitment for testing should be an active process. In this study, research staff were not permitted to move freely through the bathhouse to recruit participants. Testing clinic staff had to remain in the clinic and wait for patrons to enter the testing clinic. Fourth, patrons perceptions of the HIV status of other patrons should be challenged.
This slide includes some thought for future intervention and prevention in commercial sex venues. First, at a minimum, the option to receive test results via phone should be available. Many patrons may not wish to receive their results on-site. The option to call in for results will appeal to many who do not wish to receive their results on-site. Secondly, use of rapid oral testing for HIV should substantially increase the proportion of testers who receive their results and post-test counseling. Third, recruitment for testing should be an active process. In this study, research staff were not permitted to move freely through the bathhouse to recruit participants. Testing clinic staff had to remain in the clinic and wait for patrons to enter the testing clinic. Fourth, patrons perceptions of the HIV status of other patrons should be challenged.




