e4f5aa822e2456cb999a090fa9fe31b9.ppt
- Количество слайдов: 74
 THE TRANSPLANTATION OF HUMAN ORGANS ACT (1994) Issues, Challenges and Possible Solutions Dr. VIPIN KOUSHAL ASSISTANT PROFESSOR PGIMER Chandigarh AASASS Assisted by Dr. Navin Pandey
THE TRANSPLANTATION OF HUMAN ORGANS ACT (1994) Issues, Challenges and Possible Solutions Dr. VIPIN KOUSHAL ASSISTANT PROFESSOR PGIMER Chandigarh AASASS Assisted by Dr. Navin Pandey
 Transplantation is the future of medicine THOA EImproved technology EBetter medicines Prosecution EIncreased awareness EIncreasing waiting list Legal & Ethical issues Illegal trade Exploitation
Transplantation is the future of medicine THOA EImproved technology EBetter medicines Prosecution EIncreased awareness EIncreasing waiting list Legal & Ethical issues Illegal trade Exploitation
 Need for the Act E Patients requiring transplantation increasing. E No corresponding increase in organ donation E Lead to black marketing & organ trading E Huge susceptible population that can be exploited Contd. .
Need for the Act E Patients requiring transplantation increasing. E No corresponding increase in organ donation E Lead to black marketing & organ trading E Huge susceptible population that can be exploited Contd. .
 THOA E Provides for the regulation of : P Removal P Storage P Transplantation E Of human organs & tissues for therapeutic purposes, and E For the prevention of commercial dealings in human organs
THOA E Provides for the regulation of : P Removal P Storage P Transplantation E Of human organs & tissues for therapeutic purposes, and E For the prevention of commercial dealings in human organs
 THOA (Amendment) Act 2011 E Includes donation of tissues. E Organ swapping legalised. E Penalties enhanced. E Grandparents and Grandchildren included in the list of near relatives.
THOA (Amendment) Act 2011 E Includes donation of tissues. E Organ swapping legalised. E Penalties enhanced. E Grandparents and Grandchildren included in the list of near relatives.
 THOA (Amendment) Act 2011 E In the absence of a neurologist or neurosurgeon : P An independent surgeon or physician P An anesthetist or intensivist P Maybe nominated for brain death declaration E Makes it mandatory for a doctor in an ICU to ascertain if a family wants to donate organs E No organs or tissues shall be removed from a mentally challenged person before his death.
THOA (Amendment) Act 2011 E In the absence of a neurologist or neurosurgeon : P An independent surgeon or physician P An anesthetist or intensivist P Maybe nominated for brain death declaration E Makes it mandatory for a doctor in an ICU to ascertain if a family wants to donate organs E No organs or tissues shall be removed from a mentally challenged person before his death.
 THOA (Amendment) Act 2011 E Transplantation involving a foreign national, even if near relatives requires approval by AC. E National registry of donors and recipients. E Cornea, can be retrieved by a certified eye technician
THOA (Amendment) Act 2011 E Transplantation involving a foreign national, even if near relatives requires approval by AC. E National registry of donors and recipients. E Cornea, can be retrieved by a certified eye technician
 THOA (Amendment) Act 2011 E NGOs registered specially to work on human organ transplantation would be allowed. E Mandatory to appoint a transplant coordinator in registered hospitals
THOA (Amendment) Act 2011 E NGOs registered specially to work on human organ transplantation would be allowed. E Mandatory to appoint a transplant coordinator in registered hospitals
 The Authorities Two authorities have been formed under the Act: E Appropriate Authority (AA) and E Authorization Committee (AC)
The Authorities Two authorities have been formed under the Act: E Appropriate Authority (AA) and E Authorization Committee (AC)
 Constitution of AA The Central and State Governments shall appoint, by notification, one or more officers as Appropriate Authorities for purposes of this Act.
Constitution of AA The Central and State Governments shall appoint, by notification, one or more officers as Appropriate Authorities for purposes of this Act.
 Role of AA E To grant registration to a hospital E To suspend or cancel such registration. E To enforce standards of registered hospitals E To investigate any complaint or breach of any provision of the Act (Contd. . )
Role of AA E To grant registration to a hospital E To suspend or cancel such registration. E To enforce standards of registered hospitals E To investigate any complaint or breach of any provision of the Act (Contd. . )
 Role of AA E AA has the power to: P Summon any person P Seek production of a document P Issue a warrant for the search of any place E Suspected to be indulging in unauthorized transactions in human organs.
Role of AA E AA has the power to: P Summon any person P Seek production of a document P Issue a warrant for the search of any place E Suspected to be indulging in unauthorized transactions in human organs.
 Constitution of AC EThe composition of the AC is such as may be prescribed by the Central Government. EThe State Government and the Union territories shall constitute, EOne or more ACs EConsisting of members nominated by the State Governments and the UTs.
Constitution of AC EThe composition of the AC is such as may be prescribed by the Central Government. EThe State Government and the Union territories shall constitute, EOne or more ACs EConsisting of members nominated by the State Governments and the UTs.
 EA senior person officiating as a Director or MS or CMO E 2 senior medical practitioners from same hospital who are not part of the team. E 2 members being persons of high integrity, social standing & credibility ESecretary health or nominee& DGHS or nominee E 2 senior medical practitioners who are residing in the state but not part of transplant team. E 2 senior citizens of nonmedical background.
EA senior person officiating as a Director or MS or CMO E 2 senior medical practitioners from same hospital who are not part of the team. E 2 members being persons of high integrity, social standing & credibility ESecretary health or nominee& DGHS or nominee E 2 senior medical practitioners who are residing in the state but not part of transplant team. E 2 senior citizens of nonmedical background.
 Role of AC E Approve transplants between unrelated donors and recipients E NOC from their respective country’s embassy if the donor or recipient is a foreign national E NOC from respective domicile states, if donor or recipient are from different states.
Role of AC E Approve transplants between unrelated donors and recipients E NOC from their respective country’s embassy if the donor or recipient is a foreign national E NOC from respective domicile states, if donor or recipient are from different states.
 Punishment For violation of act by medical professionals EImprisonment of 10 years EFine of Rs. 5 lacs ERemoval from the medical council roll for two years for the first offence and permanently for any subsequent offence. Commercial dealings will invite an EImprisonment ranging from 5 -10 years EFine between 20 lakh to 1 crore
Punishment For violation of act by medical professionals EImprisonment of 10 years EFine of Rs. 5 lacs ERemoval from the medical council roll for two years for the first offence and permanently for any subsequent offence. Commercial dealings will invite an EImprisonment ranging from 5 -10 years EFine between 20 lakh to 1 crore
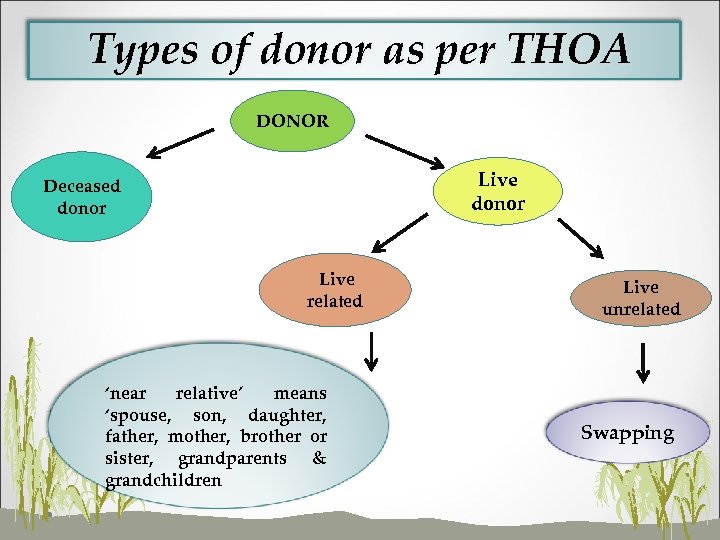 Types of donor as per THOA DONOR Live donor Deceased donor Live related ‘near relative’ means ‘spouse, son, daughter, father, mother, brother or sister, grandparents & grandchildren Live unrelated Swapping
Types of donor as per THOA DONOR Live donor Deceased donor Live related ‘near relative’ means ‘spouse, son, daughter, father, mother, brother or sister, grandparents & grandchildren Live unrelated Swapping
 Live related donor E Medical practitioner certifies that the donor is in a proper state of health and is fit to donate E Donor has to give his authorization in appropriate Form 1(A) or 1(B) E Donor has to submit an application in (Form 10) jointly with the recipient. E Necessary medical tests to determine the factum of near relationship.
Live related donor E Medical practitioner certifies that the donor is in a proper state of health and is fit to donate E Donor has to give his authorization in appropriate Form 1(A) or 1(B) E Donor has to submit an application in (Form 10) jointly with the recipient. E Necessary medical tests to determine the factum of near relationship.
 Spousal donor Rule 4 -A(2) EJoint application by donor & recipient with certificate of proof. EApproval by the authorization committee.
Spousal donor Rule 4 -A(2) EJoint application by donor & recipient with certificate of proof. EApproval by the authorization committee.
 Live unrelated donor EThe AC ensures that there is no commercial transaction or middle man / tout involved EFinancial status of the donor and the recipient ENext of the kin of the proposed unrelated donor is interviewed ESeeks an explanation of : Elink between the donor and recipient. EDocumentary evidence of the link (Contd. . )
Live unrelated donor EThe AC ensures that there is no commercial transaction or middle man / tout involved EFinancial status of the donor and the recipient ENext of the kin of the proposed unrelated donor is interviewed ESeeks an explanation of : Elink between the donor and recipient. EDocumentary evidence of the link (Contd. . )
 Deceased donation E Authorised medical board has to certify that patient is brain dead. E A medical board comprises of: P Hospital Administrator, P A neurologist or neurosurgeon (an independent surgeon or physician, and an anesthetist or intensivist. ) P And the patient’s treating doctor.
Deceased donation E Authorised medical board has to certify that patient is brain dead. E A medical board comprises of: P Hospital Administrator, P A neurologist or neurosurgeon (an independent surgeon or physician, and an anesthetist or intensivist. ) P And the patient’s treating doctor.

 CASE STUDY 1 ORGAN TRANSPLANT IN PGIMER
CASE STUDY 1 ORGAN TRANSPLANT IN PGIMER
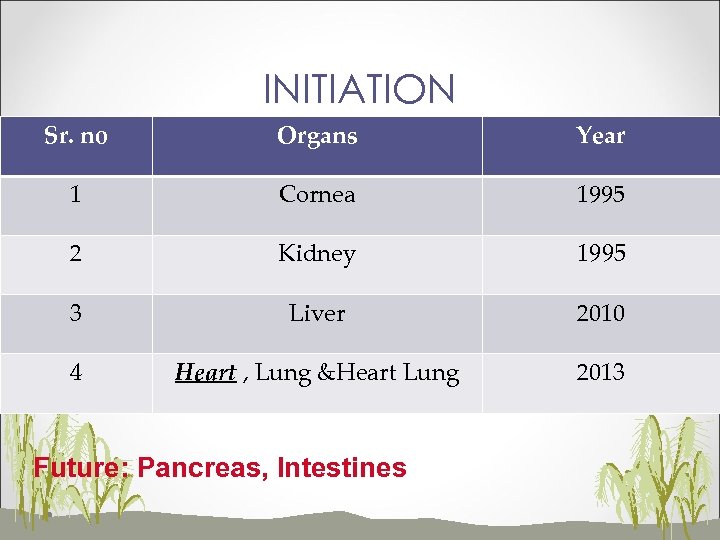 INITIATION Sr. no Organs Year 1 Cornea 1995 2 Kidney 1995 3 Liver 2010 4 Heart , Lung &Heart Lung 2013 Future: Pancreas, Intestines
INITIATION Sr. no Organs Year 1 Cornea 1995 2 Kidney 1995 3 Liver 2010 4 Heart , Lung &Heart Lung 2013 Future: Pancreas, Intestines
 Authorization Committee Prof. A. K. Gupta, MS-cum-Head, Deptt of Hospital Administration, PGIMER, Chd Secretary Health Director Health Services Dr. (Mrs. )Saroj Sharma, Prof Rajinder Singh Prof. Deepak Bhasin Prof. (Retd) KN Pathak Mr. P. C. Dogra, U. T Admn or his nominee Prof Medical Microbiology HOD, Surgery, PGIMER. Deptt of Gastro, PGIMER Vice Chancellor, Punjab University DGP (Retd. )
Authorization Committee Prof. A. K. Gupta, MS-cum-Head, Deptt of Hospital Administration, PGIMER, Chd Secretary Health Director Health Services Dr. (Mrs. )Saroj Sharma, Prof Rajinder Singh Prof. Deepak Bhasin Prof. (Retd) KN Pathak Mr. P. C. Dogra, U. T Admn or his nominee Prof Medical Microbiology HOD, Surgery, PGIMER. Deptt of Gastro, PGIMER Vice Chancellor, Punjab University DGP (Retd. )
 ISSUE Initiating the Heart Transplant Program in PGIMER
ISSUE Initiating the Heart Transplant Program in PGIMER
 CHALLENGES E INFRASTRUCTURE E TRAINED & QUALIFIED MANPOWER E REGISTRATION E ORGAN DONOR E ORGAN RECEIPIENT E CHALLENGES FOR MANAGEMENT
CHALLENGES E INFRASTRUCTURE E TRAINED & QUALIFIED MANPOWER E REGISTRATION E ORGAN DONOR E ORGAN RECEIPIENT E CHALLENGES FOR MANAGEMENT
 Solution EApplication in Form 11 justifying the ü Infrastructure ü Manpower. EInspection by team from DGHS ERegistration granted.
Solution EApplication in Form 11 justifying the ü Infrastructure ü Manpower. EInspection by team from DGHS ERegistration granted.
 Solution : Organ recipient EWaiting list prepared E 5 patients put on the waiting list
Solution : Organ recipient EWaiting list prepared E 5 patients put on the waiting list
 Solution : Donor ERoad traffic accident victim in PGIMER on 30 th JULY 2013 EPotential brain dead donor EInformation from the treating doctor about potential brain death status of patient EHospital SOP activated
Solution : Donor ERoad traffic accident victim in PGIMER on 30 th JULY 2013 EPotential brain dead donor EInformation from the treating doctor about potential brain death status of patient EHospital SOP activated
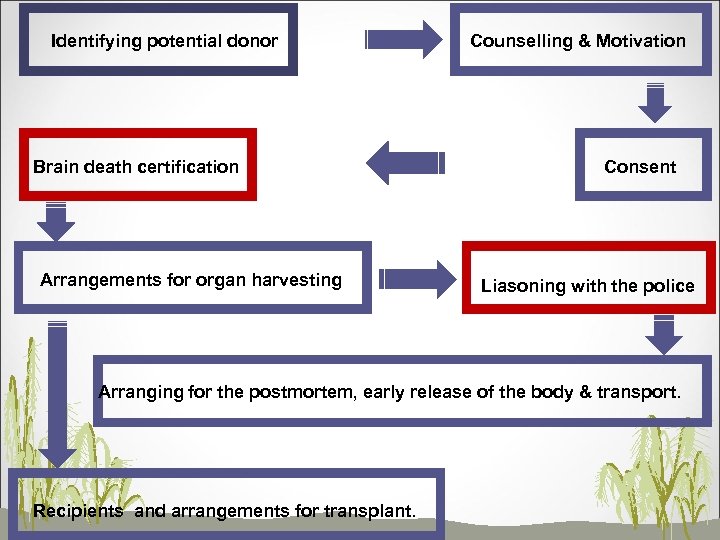 Identifying potential donor Brain death certification Arrangements for organ harvesting Counselling & Motivation Consent Liasoning with the police Arranging for the postmortem, early release of the body & transport. Recipients and arrangements for transplant.
Identifying potential donor Brain death certification Arrangements for organ harvesting Counselling & Motivation Consent Liasoning with the police Arranging for the postmortem, early release of the body & transport. Recipients and arrangements for transplant.
 Solution First successful heart transplant at PGIMER on 4 th august 2013
Solution First successful heart transplant at PGIMER on 4 th august 2013

 Case Study 2 ORGAN TRANSLANT & ALLEGATION AGAINST AN INSTITUTE
Case Study 2 ORGAN TRANSLANT & ALLEGATION AGAINST AN INSTITUTE
 ISSUE EX complained to NHRC that Y who was well known to him took him to PGIMER, Chandigarh. EY threatened X to donate his kidney for Y’s wife. EDoctors at PGIMER were also involved in this.
ISSUE EX complained to NHRC that Y who was well known to him took him to PGIMER, Chandigarh. EY threatened X to donate his kidney for Y’s wife. EDoctors at PGIMER were also involved in this.
 FACTS Report sent to NHRC with the following explanation: E The centre strictly performs kidney transplantation from related donors only as per the provisions of THOA. E The transplant was carried out after approval by the AC of Bihar state.
FACTS Report sent to NHRC with the following explanation: E The centre strictly performs kidney transplantation from related donors only as per the provisions of THOA. E The transplant was carried out after approval by the AC of Bihar state.
 SOLUTION : FACTS E X voluntarily registered as the patient’s younger brother and was a willing kidney donor. E The recipient and the donor were evaluated in the Deptt. of Nephrology for medical fitness and establishment of relationship between the donor and the recipient after approval by AC.
SOLUTION : FACTS E X voluntarily registered as the patient’s younger brother and was a willing kidney donor. E The recipient and the donor were evaluated in the Deptt. of Nephrology for medical fitness and establishment of relationship between the donor and the recipient after approval by AC.
 SOLUTION : FACTS E The complainant had obtained a travelling concession form for Chandigarh with a fake name. E A number of doctors, nurses, technicians, paramedical staff interacted with the donor and not once did he complain.
SOLUTION : FACTS E The complainant had obtained a travelling concession form for Chandigarh with a fake name. E A number of doctors, nurses, technicians, paramedical staff interacted with the donor and not once did he complain.
 Solution ENHRC dismissed the case. EProper documentation saved the day for PGIMER.
Solution ENHRC dismissed the case. EProper documentation saved the day for PGIMER.
 CASE STUDY 3 ORGAN TRANSPLANT LIVE AND CADAVERIC
CASE STUDY 3 ORGAN TRANSPLANT LIVE AND CADAVERIC
 ISSUE E Patient with attempted suicide was admitted at a reputed Corporate Hospital (CH), in Mohali E Patient had a head injury, put on ventilator, poor prognosis explained to family E Family motivated to donate the organs of their young patient. E Transplant team of the institute informed of the family’s decision.
ISSUE E Patient with attempted suicide was admitted at a reputed Corporate Hospital (CH), in Mohali E Patient had a head injury, put on ventilator, poor prognosis explained to family E Family motivated to donate the organs of their young patient. E Transplant team of the institute informed of the family’s decision.
 Challenge E CH was conducting only living donor transplants. E CH did not have a Brainstem Death Certification Committee approved by the AA
Challenge E CH was conducting only living donor transplants. E CH did not have a Brainstem Death Certification Committee approved by the AA
 CHALLENGE E There was no forensic expert available at the Hospital. E The forensic expert had to be deputed by the AA (civil Surgeon)- this process was time consuming and involved a legal clearance from the government.
CHALLENGE E There was no forensic expert available at the Hospital. E The forensic expert had to be deputed by the AA (civil Surgeon)- this process was time consuming and involved a legal clearance from the government.
 Solution E Patient shifted to PGIMER on request and the process for organ donation started E CH informs the institute that one kidney & liver were required for patients on their waiting list.
Solution E Patient shifted to PGIMER on request and the process for organ donation started E CH informs the institute that one kidney & liver were required for patients on their waiting list.
 SOLUTION EPGIMER not in position to do the liver transplant as recipient not available EThe patient’s family decided to donate only kidneys.
SOLUTION EPGIMER not in position to do the liver transplant as recipient not available EThe patient’s family decided to donate only kidneys.
 SOLUTION EAny hospital having live organ transplant program should be prepared for cadaver organ transplant. E Brain stem death certifying committee should be identified and approved by the AA. EFormalities for conducting autopsy should be available as most of brain dead cases are MLC cases.
SOLUTION EAny hospital having live organ transplant program should be prepared for cadaver organ transplant. E Brain stem death certifying committee should be identified and approved by the AA. EFormalities for conducting autopsy should be available as most of brain dead cases are MLC cases.
 SOLUTION ECollaboration with national level NGOs. ETransplant team has to be in a state of alert with a ready updated recipients list.
SOLUTION ECollaboration with national level NGOs. ETransplant team has to be in a state of alert with a ready updated recipients list.
 Case Study - 4 ORGAN TRANSPLANT & DOMICILE OF DONOR/RECIPIENT Dolma Bhuti & another. . . . . Petitioners Vs PGIMER, Chandigarh &others. . . Respondents CASE NO : Appeal (Civil) 11977 of 2012 DATE OF JUDGMENT: March 28 th , 2008
Case Study - 4 ORGAN TRANSPLANT & DOMICILE OF DONOR/RECIPIENT Dolma Bhuti & another. . . . . Petitioners Vs PGIMER, Chandigarh &others. . . Respondents CASE NO : Appeal (Civil) 11977 of 2012 DATE OF JUDGMENT: March 28 th , 2008
 ISSUE E Petitioner No. 1 (resident of Tibet) - studying in Tibetan Children Village School at Dharamshala. E Developed CRF due to Nephrotic Syndrome E Petitioner No. 2 – A Buddhist monk (resident of HP) decided to donate his one kidney out of compassion to save Petitioner 1’s life.
ISSUE E Petitioner No. 1 (resident of Tibet) - studying in Tibetan Children Village School at Dharamshala. E Developed CRF due to Nephrotic Syndrome E Petitioner No. 2 – A Buddhist monk (resident of HP) decided to donate his one kidney out of compassion to save Petitioner 1’s life.
 ISSUE EThe patient had reached a stage where she required daily dialysis at PGIMER. EOnly solution was urgent transplant surgery EPGIMER seeks clearance by AC of HP as the petitioners were residents of HP.
ISSUE EThe patient had reached a stage where she required daily dialysis at PGIMER. EOnly solution was urgent transplant surgery EPGIMER seeks clearance by AC of HP as the petitioners were residents of HP.
 Challenge E Is PGIMER under legal obligation to carry out the kidney transplantation of petitioner no. 1 keeping in view her critical condition? ECan the AC of PGIMER permit the transplantation considering that both were residing in HP?
Challenge E Is PGIMER under legal obligation to carry out the kidney transplantation of petitioner no. 1 keeping in view her critical condition? ECan the AC of PGIMER permit the transplantation considering that both were residing in HP?
 SOLUTION E The petitioners filed a case in the High court. E Court stated that since P the patient is very critical and P transplant is life saving for her, E Taking permission from HP AC will take time. E PGI to examine and clear the case in its AC ( UTAC) and carry out the transplant as soon as possible.
SOLUTION E The petitioners filed a case in the High court. E Court stated that since P the patient is very critical and P transplant is life saving for her, E Taking permission from HP AC will take time. E PGI to examine and clear the case in its AC ( UTAC) and carry out the transplant as soon as possible.
 SOLUTION Case was cleared by the AC of PGIMER and transplantation was carried out at PGIMER.
SOLUTION Case was cleared by the AC of PGIMER and transplantation was carried out at PGIMER.
 Case study 5 Organ Sharing
Case study 5 Organ Sharing
 ISSUE A potential brain dead donor in GMCH 32, Chd Family wished to donate organs Patient shifted to PGIMER, Chd
ISSUE A potential brain dead donor in GMCH 32, Chd Family wished to donate organs Patient shifted to PGIMER, Chd
 CHALLENGE No EHeart transplant program not started ENo recipient for liver ERecipient for kidney & cornea present Explore possibility of organ sharing EShould heart & liver be allowed to go unutilised ?
CHALLENGE No EHeart transplant program not started ENo recipient for liver ERecipient for kidney & cornea present Explore possibility of organ sharing EShould heart & liver be allowed to go unutilised ?
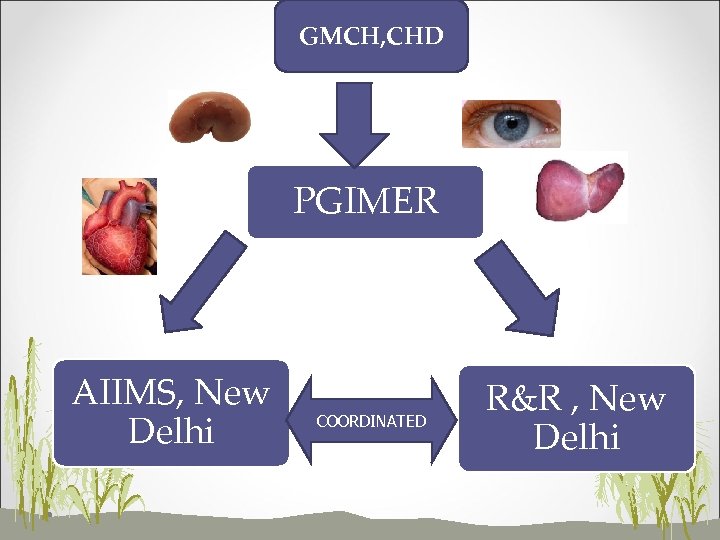 GMCH, CHD PGIMER AIIMS, New Delhi COORDINATED R&R , New Delhi
GMCH, CHD PGIMER AIIMS, New Delhi COORDINATED R&R , New Delhi
 Solution ENational registry of waiting recipients ELogistic support to transport organs ECoordination among different hospitals
Solution ENational registry of waiting recipients ELogistic support to transport organs ECoordination among different hospitals
 Case study 6 Promoting organ donation
Case study 6 Promoting organ donation
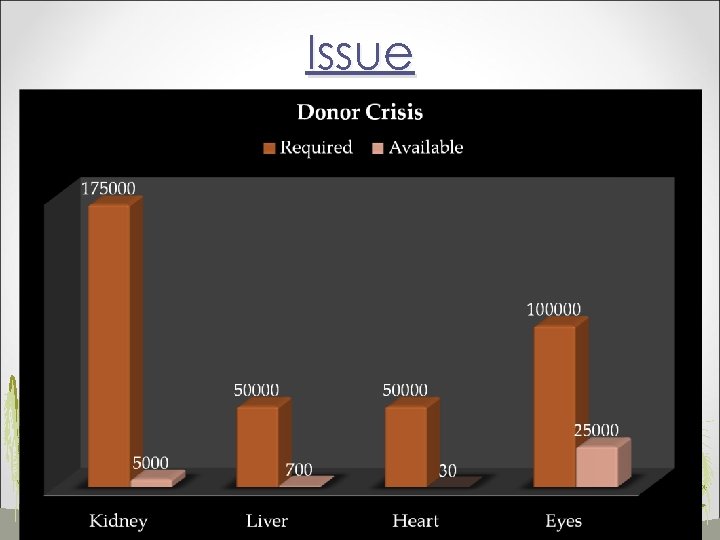 Issue
Issue
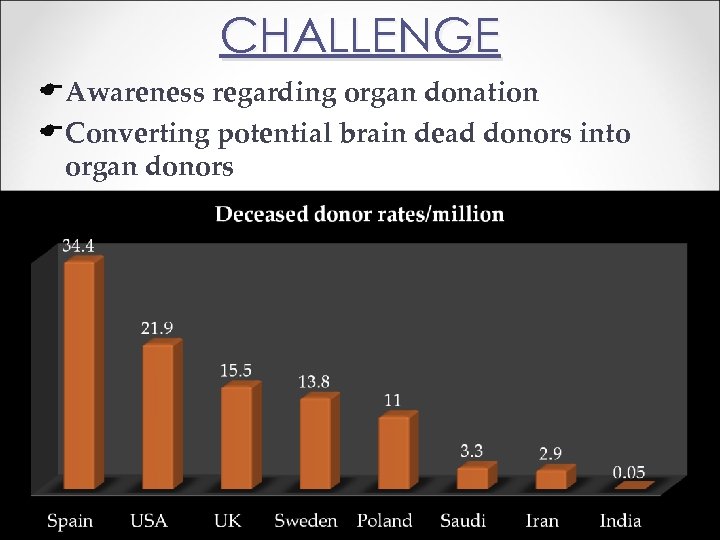 CHALLENGE EAwareness regarding organ donation EConverting potential brain dead donors into organ donors
CHALLENGE EAwareness regarding organ donation EConverting potential brain dead donors into organ donors
 SOLUTION Awareness regarding organ donation P IEC P Mass media P Public forums P Religious heads P NGOs ü Donor card ü Helpline numbers ü Website
SOLUTION Awareness regarding organ donation P IEC P Mass media P Public forums P Religious heads P NGOs ü Donor card ü Helpline numbers ü Website
 Solution To increase the conversion rate ü Identification of brain dead potential donors ü Role of transplant coordinators ü Modification of death certificate for promoting eye donation ü Maintenance of brain dead potential donors ü Inter and intra departmental liason ü Modification of driving license ü Support to the donor family ü Taking care of myths & misconceptions
Solution To increase the conversion rate ü Identification of brain dead potential donors ü Role of transplant coordinators ü Modification of death certificate for promoting eye donation ü Maintenance of brain dead potential donors ü Inter and intra departmental liason ü Modification of driving license ü Support to the donor family ü Taking care of myths & misconceptions
 INITIATVES BY PGIMER
INITIATVES BY PGIMER
 Initiative by PGIMER
Initiative by PGIMER

 www. lampoflife. com
www. lampoflife. com





 Our little effort will make a big change & give life to someone
Our little effort will make a big change & give life to someone
 THANK YOU Thank You
THANK YOU Thank You


