12c0bbab89b07fc003f53cada7c2eb9d.ppt
- Количество слайдов: 21
 The Scope of PHI Claims Leakage & “Fraud” – Definitions, Measures, Counting, Success AHIA Claims Leakage & Fraud Forum Hunter Valley Gardens 29 -31 August 2007 Michael Douman Manager, Business & Clinical Analysis
The Scope of PHI Claims Leakage & “Fraud” – Definitions, Measures, Counting, Success AHIA Claims Leakage & Fraud Forum Hunter Valley Gardens 29 -31 August 2007 Michael Douman Manager, Business & Clinical Analysis
 Why is this issue important ? [ It underpins much of what we will be talking about through this conference and canvasses issues we need to resolve as an industry [ We don’t all: [ define terms the same way and it would be helpful if we did [ analyse issues the same way [ analyse hospital, medical and ancillary to the same extent eg some Funds have a predominantly ancillary focus [ measure success the same way [ As a consequence there will be: [ some consistency across the industry when we talk about these issues [ the ability to speak in a more informed way about fraud and related issues and be better able to quantify fraud and claims leakage [ a more professional image of the industry
Why is this issue important ? [ It underpins much of what we will be talking about through this conference and canvasses issues we need to resolve as an industry [ We don’t all: [ define terms the same way and it would be helpful if we did [ analyse issues the same way [ analyse hospital, medical and ancillary to the same extent eg some Funds have a predominantly ancillary focus [ measure success the same way [ As a consequence there will be: [ some consistency across the industry when we talk about these issues [ the ability to speak in a more informed way about fraud and related issues and be better able to quantify fraud and claims leakage [ a more professional image of the industry
 What do we mean ? “When I use a word, " Humpty Dumpty said in rather a scornful tone, "It means just what I choose it to mean - neither more or less. " "The question is, " said Alice, "whether you can make words mean so many different things. " "The question is, " said Humpty Dumpty, "which is to be master - that's all. " Lewis Carroll
What do we mean ? “When I use a word, " Humpty Dumpty said in rather a scornful tone, "It means just what I choose it to mean - neither more or less. " "The question is, " said Alice, "whether you can make words mean so many different things. " "The question is, " said Humpty Dumpty, "which is to be master - that's all. " Lewis Carroll
 What’s it all about - Alfie ?
What’s it all about - Alfie ?
 Defining PHI “Fraud” – Australia [ If we are all defining the term differently then we get different answers - to state the obvious [ There are definitional ambiguities between: [ [ [ [ fraud abuse waste errors incompetence differences of medical opinion, eg over servicing (your over servicing is my medical caring), members and/or providers exploiting product weaknesses, eg “use it or lose it” campaigns, splitting service years, etc [ And then there is the complicating factor of proving intent [ For all the above reasons, MBF prefers to use the term Claims Leakage
Defining PHI “Fraud” – Australia [ If we are all defining the term differently then we get different answers - to state the obvious [ There are definitional ambiguities between: [ [ [ [ fraud abuse waste errors incompetence differences of medical opinion, eg over servicing (your over servicing is my medical caring), members and/or providers exploiting product weaknesses, eg “use it or lose it” campaigns, splitting service years, etc [ And then there is the complicating factor of proving intent [ For all the above reasons, MBF prefers to use the term Claims Leakage
 Claims Leakage Defined [ We can overcome the definitional issues if we use the term Claims Leakage which encompasses anything from fraud at the extreme end to any inappropriate benefit payment however caused [ Claims leakage can encompass the over payment of a claim as a result of any of the following: [ Provider incorrect billing for whatever reason e. g. over servicing, no service provided, service upcoding [ Member submitting incorrect claim [ Fund assessing staff perpetrating fraud [ Assessor errors with subsequent recovery [ Incorrect advice by staff to members re benefits payable [ System controls not working and subsequently rectified [ Clinical or business rules not working and subsequently rectified [ Pricing tables or contract rates incorrect in the system [ Failure to recover from reinsurers or co-insurers e. g. PHIAC [ Indemnity refunds from third party payors e. g. workers compensation, motor vehicle accident, public liability
Claims Leakage Defined [ We can overcome the definitional issues if we use the term Claims Leakage which encompasses anything from fraud at the extreme end to any inappropriate benefit payment however caused [ Claims leakage can encompass the over payment of a claim as a result of any of the following: [ Provider incorrect billing for whatever reason e. g. over servicing, no service provided, service upcoding [ Member submitting incorrect claim [ Fund assessing staff perpetrating fraud [ Assessor errors with subsequent recovery [ Incorrect advice by staff to members re benefits payable [ System controls not working and subsequently rectified [ Clinical or business rules not working and subsequently rectified [ Pricing tables or contract rates incorrect in the system [ Failure to recover from reinsurers or co-insurers e. g. PHIAC [ Indemnity refunds from third party payors e. g. workers compensation, motor vehicle accident, public liability
 Measuring PHI Claims Leakage – Australia [ [ [ What should you include ? [ Only what you stop [ Deterrent or Hawthorn effect beyond those matters you are auditing [ Indemnity refunds How should you count it – Timing ? [ 12 months from point of intervention and then stop [ Cumulatively How should you count it – Multivariate analysis ? [ Double counting [ How do you discount movements due to others actions rather than your own eg membership movements, product changes, sales promotions, etc How should you count it – Cause or coincidence ? [ Is your action causal or simply a correlation What measure (s)/KPIs should you use ? [ Dollars saved ? [ Percentage of benefits paid [ Multiple of operating costs
Measuring PHI Claims Leakage – Australia [ [ [ What should you include ? [ Only what you stop [ Deterrent or Hawthorn effect beyond those matters you are auditing [ Indemnity refunds How should you count it – Timing ? [ 12 months from point of intervention and then stop [ Cumulatively How should you count it – Multivariate analysis ? [ Double counting [ How do you discount movements due to others actions rather than your own eg membership movements, product changes, sales promotions, etc How should you count it – Cause or coincidence ? [ Is your action causal or simply a correlation What measure (s)/KPIs should you use ? [ Dollars saved ? [ Percentage of benefits paid [ Multiple of operating costs
 What is Success in PHI Claims Leakage & Where should you Focus ? [ Does more always signify success ? [ Or is it the case that the less effective your existing controls are the more you can save. [ Is that good fraud prevention or poor systems controls ? [ Are you better off concentrating on reviewing only ancillary claims rather than hospital and medical because: [ [ [ ancillary providers are more prone to “fraud” ? large organisations like hospitals would not do this ? medical providers would not do this, and in any case Medicare is a sufficient guarantee ?
What is Success in PHI Claims Leakage & Where should you Focus ? [ Does more always signify success ? [ Or is it the case that the less effective your existing controls are the more you can save. [ Is that good fraud prevention or poor systems controls ? [ Are you better off concentrating on reviewing only ancillary claims rather than hospital and medical because: [ [ [ ancillary providers are more prone to “fraud” ? large organisations like hospitals would not do this ? medical providers would not do this, and in any case Medicare is a sufficient guarantee ?
 Quantifying U. S. Health “Fraud” Levels [ Prof Malcolm Sparrow, a Harvard academic, says in his Book “Licence to Steal” (2000), that health fraud in the U. S. could be as high as $300 billion to $500 billion out of a total health expenditure of $1, 300 billion or 23% to 38% of all payments (p. vii, 4648). [ A range of 10% to 40% is also quoted by Sparrow (Sparrow, p. 71) [ An OIG study in 1997 says it is 14% of Medicare payments, in 1998 the figure reduced to 11%, and in 1999 it reduced further to 7. 1% and in March 2000 it increases to 7. 97%. This was based on a desk audit and only picks up lack of medical documentation to support claims [ Illinois OIG says “payment inaccuracy” is 4. 7% [ Only Illinois and Texas have seriously attempted to measure the losses due to fraud, abuse and errors in their Medicaid programs [ IRS compliance study in the U. S. (1995) showed that on a conservative definition of fraud 19% of claims were fraudulent. 39% were inflated or unmerited (Sparrow, p. 151) [ Confusion in the U. S. between utilisation review with 2% outlier concerns, with fraud which can be more difficult to detect and is at a higher level (Sparrow, p. 42) [ More than 50% of whistle blower fraud in U. S. relates to health care and more than half health care fraud comes as a result of whistle blowers
Quantifying U. S. Health “Fraud” Levels [ Prof Malcolm Sparrow, a Harvard academic, says in his Book “Licence to Steal” (2000), that health fraud in the U. S. could be as high as $300 billion to $500 billion out of a total health expenditure of $1, 300 billion or 23% to 38% of all payments (p. vii, 4648). [ A range of 10% to 40% is also quoted by Sparrow (Sparrow, p. 71) [ An OIG study in 1997 says it is 14% of Medicare payments, in 1998 the figure reduced to 11%, and in 1999 it reduced further to 7. 1% and in March 2000 it increases to 7. 97%. This was based on a desk audit and only picks up lack of medical documentation to support claims [ Illinois OIG says “payment inaccuracy” is 4. 7% [ Only Illinois and Texas have seriously attempted to measure the losses due to fraud, abuse and errors in their Medicaid programs [ IRS compliance study in the U. S. (1995) showed that on a conservative definition of fraud 19% of claims were fraudulent. 39% were inflated or unmerited (Sparrow, p. 151) [ Confusion in the U. S. between utilisation review with 2% outlier concerns, with fraud which can be more difficult to detect and is at a higher level (Sparrow, p. 42) [ More than 50% of whistle blower fraud in U. S. relates to health care and more than half health care fraud comes as a result of whistle blowers
 Quantifying “Fraud” Overseas [ A comparative international study of insurance fraud in 1990 stated that: “there is no evidence that any insurer has undertaken research to establish the real extent of fraud in any given area of risk” (Sparrow, p. 145) [ Visa card says that its confirmed fraud rate is 0. 1%. This is the rate that it aspires to achieve, and can live with.
Quantifying “Fraud” Overseas [ A comparative international study of insurance fraud in 1990 stated that: “there is no evidence that any insurer has undertaken research to establish the real extent of fraud in any given area of risk” (Sparrow, p. 145) [ Visa card says that its confirmed fraud rate is 0. 1%. This is the rate that it aspires to achieve, and can live with.
 Quantifying PHI “Fraud” – Australia (1) [ You cannot use U. S. health figures which we have just seen, as the sectors are structured differently, and have different players at different levels eg billing agents etc. [ Fraud differs between industry sectors and countries [ You cannot just use a KPMG/Ernst & Young annual surveys of all industries in Australia and say it applies to PHI [ There a range of percentages quoted by consultants from 5% upwards
Quantifying PHI “Fraud” – Australia (1) [ You cannot use U. S. health figures which we have just seen, as the sectors are structured differently, and have different players at different levels eg billing agents etc. [ Fraud differs between industry sectors and countries [ You cannot just use a KPMG/Ernst & Young annual surveys of all industries in Australia and say it applies to PHI [ There a range of percentages quoted by consultants from 5% upwards
 Quantifying PHI “Fraud” – Australia (2) [ Senator Benardi, in Parliament in Oct 2006, claimed that health insurance fraud “could be costing up to $800 million dollars every year” which, if true, would mean that fraud was 9. 6% of all benefits paid. I do not accept that figure. [ Senator Bernardi also stated that “One recent audit of a major capital city hospital identified nearly $1. 5 million worth of fraudulent claims. There are over 1, 000 hospitals in Australia…” [ This statement could lead people to believe that fraud was $1. 5 million*1000 or $1. 5 billion which is 24. 6% of all hospital, medical and prostheses benefits paid. This is assuming the initial figure of $1. 5 million at the unnamed hospital is correct and provable. I don’t believe this is plausible. [ Some of the preceding is based on use of overseas data or an attempt to drum up business by consultants [ There is an old Medicare Australia quoted figure of some years ago that it is in a range of 1. 3% to 2. 3% of benefits paid, but no one honestly knows [ No one I know is making savings at the high end of the order cited by Medicare across the total hospital, medical, and ancillary services
Quantifying PHI “Fraud” – Australia (2) [ Senator Benardi, in Parliament in Oct 2006, claimed that health insurance fraud “could be costing up to $800 million dollars every year” which, if true, would mean that fraud was 9. 6% of all benefits paid. I do not accept that figure. [ Senator Bernardi also stated that “One recent audit of a major capital city hospital identified nearly $1. 5 million worth of fraudulent claims. There are over 1, 000 hospitals in Australia…” [ This statement could lead people to believe that fraud was $1. 5 million*1000 or $1. 5 billion which is 24. 6% of all hospital, medical and prostheses benefits paid. This is assuming the initial figure of $1. 5 million at the unnamed hospital is correct and provable. I don’t believe this is plausible. [ Some of the preceding is based on use of overseas data or an attempt to drum up business by consultants [ There is an old Medicare Australia quoted figure of some years ago that it is in a range of 1. 3% to 2. 3% of benefits paid, but no one honestly knows [ No one I know is making savings at the high end of the order cited by Medicare across the total hospital, medical, and ancillary services
 PHI Industry Benefits Paid & Possible “Claims Leakage” costs - Australia [ $8. 4 billion in hospital and ancillary claims paid in FY 06 split [ [ [ Hospital, Medical, Prostheses - $6. 1 billion Ancillary - $2. 3 billion Claims Disaggregation [ [ Hospital - $4. 3 billion Prostheses - $837. 9 million Medical - $957. 2 million Ancillary - $2. 3 billion (dental, optical, physio, chiro, pharmacy, podiatry the top modalities by benefits paid) (Source PHIAC Annual Financial statements 2006, latest report available) [ Depending on: [ [ [ what percentage you wish to apply whether that percentage varies by sub group above, or is the same across all areas Health insurance “Claims Leakage” in Australia could be in a mid range of $83 million (1%) or any multiple up or down from that
PHI Industry Benefits Paid & Possible “Claims Leakage” costs - Australia [ $8. 4 billion in hospital and ancillary claims paid in FY 06 split [ [ [ Hospital, Medical, Prostheses - $6. 1 billion Ancillary - $2. 3 billion Claims Disaggregation [ [ Hospital - $4. 3 billion Prostheses - $837. 9 million Medical - $957. 2 million Ancillary - $2. 3 billion (dental, optical, physio, chiro, pharmacy, podiatry the top modalities by benefits paid) (Source PHIAC Annual Financial statements 2006, latest report available) [ Depending on: [ [ [ what percentage you wish to apply whether that percentage varies by sub group above, or is the same across all areas Health insurance “Claims Leakage” in Australia could be in a mid range of $83 million (1%) or any multiple up or down from that
 How effective are Australian Health Funds in “Claims Leakage” Prevention Savings (1) ? [ There are differing views of what individual Funds save either in total dollars, as a percentage of benefits paid, or as a multiple of operating costs. [ We know that some Funds can’t embed rules in their mainframe systems, due to the limitations of those systems. [ Some Funds don’t have body parts data capture in ancillary claims eg tooth ID, as mandatory in their mainframe systems so they cannot use rules to limit benefits paid, and some who may be able to insert them haven’t for marketing or other reasons [ The less effective your existing controls are the more you can save. Is that good fraud prevention or poor systems controls ? [ Further, like all statistics it depends on how you define fraud and how you count and measure it (inclusions and exclusions) as discussed earlier in this paper
How effective are Australian Health Funds in “Claims Leakage” Prevention Savings (1) ? [ There are differing views of what individual Funds save either in total dollars, as a percentage of benefits paid, or as a multiple of operating costs. [ We know that some Funds can’t embed rules in their mainframe systems, due to the limitations of those systems. [ Some Funds don’t have body parts data capture in ancillary claims eg tooth ID, as mandatory in their mainframe systems so they cannot use rules to limit benefits paid, and some who may be able to insert them haven’t for marketing or other reasons [ The less effective your existing controls are the more you can save. Is that good fraud prevention or poor systems controls ? [ Further, like all statistics it depends on how you define fraud and how you count and measure it (inclusions and exclusions) as discussed earlier in this paper
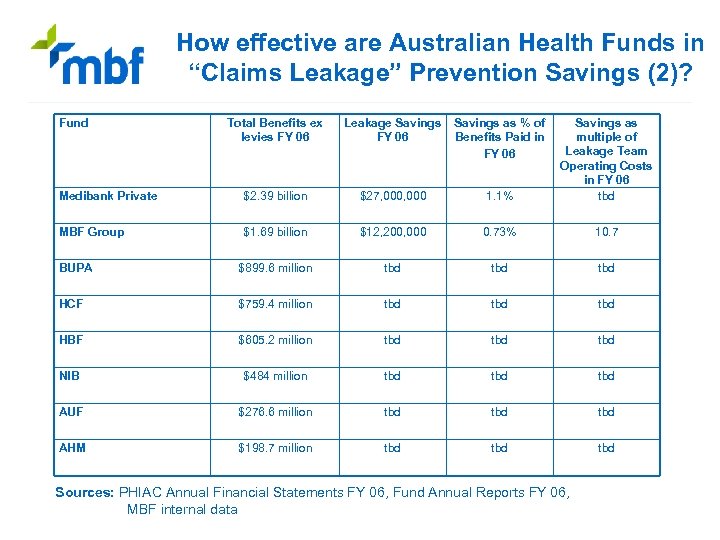 How effective are Australian Health Funds in “Claims Leakage” Prevention Savings (2)? Fund Total Benefits ex levies FY 06 Leakage Savings FY 06 Savings as % of Benefits Paid in FY 06 Medibank Private $2. 39 billion $27, 000 1. 1% Savings as multiple of Leakage Team Operating Costs in FY 06 tbd MBF Group $1. 69 billion $12, 200, 000 0. 73% 10. 7 BUPA $899. 6 million tbd tbd HCF $759. 4 million tbd tbd HBF $605. 2 million tbd tbd NIB $484 million tbd tbd AUF $276. 6 million tbd tbd AHM $198. 7 million tbd tbd Sources: PHIAC Annual Financial Statements FY 06, Fund Annual Reports FY 06, MBF internal data
How effective are Australian Health Funds in “Claims Leakage” Prevention Savings (2)? Fund Total Benefits ex levies FY 06 Leakage Savings FY 06 Savings as % of Benefits Paid in FY 06 Medibank Private $2. 39 billion $27, 000 1. 1% Savings as multiple of Leakage Team Operating Costs in FY 06 tbd MBF Group $1. 69 billion $12, 200, 000 0. 73% 10. 7 BUPA $899. 6 million tbd tbd HCF $759. 4 million tbd tbd HBF $605. 2 million tbd tbd NIB $484 million tbd tbd AUF $276. 6 million tbd tbd AHM $198. 7 million tbd tbd Sources: PHIAC Annual Financial Statements FY 06, Fund Annual Reports FY 06, MBF internal data
 MBF’s Measurement and Tracking of Claims Leakage Effectiveness (1) Hospital Items Counted [ Recoveries received irrespective of the method used or area of focus eg type 3 B refunds, prostheses failures covered under warranty, incorrect assessment by MBF, incorrect invoice by hospital [ Decrease in benefits payable as a result of: [ automated rule changes programmed into the mainframe system eg item reference tables [ auditing (DRG coding or chart to bill) [ product changes that we instigate [ contract changes that we instigate [ changes to errors in pricing tables [ corrections to Do. HA schedules eg prostheses [ changes to mainframe system controls Medical Items Counted [ [ [ Recoveries as above Automated rule changes programmed into the mainframe system eg Gap item reference tables Decrease in benefits as above
MBF’s Measurement and Tracking of Claims Leakage Effectiveness (1) Hospital Items Counted [ Recoveries received irrespective of the method used or area of focus eg type 3 B refunds, prostheses failures covered under warranty, incorrect assessment by MBF, incorrect invoice by hospital [ Decrease in benefits payable as a result of: [ automated rule changes programmed into the mainframe system eg item reference tables [ auditing (DRG coding or chart to bill) [ product changes that we instigate [ contract changes that we instigate [ changes to errors in pricing tables [ corrections to Do. HA schedules eg prostheses [ changes to mainframe system controls Medical Items Counted [ [ [ Recoveries as above Automated rule changes programmed into the mainframe system eg Gap item reference tables Decrease in benefits as above
 MBF’s Measurement and Tracking of Claims Leakage Effectiveness (2) Ancillary Items Counted [ Recoveries received irrespective of the method used or area of focus eg refunds from provider counselling [ Decrease in benefits payable as a result of: [ [ [ proactive automated rule changes programmed into the mainframe system eg tooth id auditing of providers, members or staff product changes that we instigate provider deregistration provider de-recognition provider, member or staff member prosecution member or staff termination preferred provider contract changes that we instigate changes to errors in pricing tables corrections to ancillary schedules changes to mainframe system controls
MBF’s Measurement and Tracking of Claims Leakage Effectiveness (2) Ancillary Items Counted [ Recoveries received irrespective of the method used or area of focus eg refunds from provider counselling [ Decrease in benefits payable as a result of: [ [ [ proactive automated rule changes programmed into the mainframe system eg tooth id auditing of providers, members or staff product changes that we instigate provider deregistration provider de-recognition provider, member or staff member prosecution member or staff termination preferred provider contract changes that we instigate changes to errors in pricing tables corrections to ancillary schedules changes to mainframe system controls
 MBF’s Proposed approach to Measuring and Tracking Claims Leakage Savings (3) Calculating Savings – Hospital [ [ [ Determining our impact is confirmed by a multivariate analysis so that for example a decrease in benefits which may result from a declining membership, or patient base for a provider, is not wrongly attributed to our actions, or the actions of others in the Fund are not claimed by my team Recoveries are counted at 100% Rules or system changes introduction at 100% linked to a claiming patient ratio Schedule changes at 100% eg prostheses linked to a claiming patient ratio Audited items at 100% of reduced billings linked to a claiming patient ratio Contract changes at 100% linked to a claiming patient ratio Calculating Savings – Medical [ [ Similar to above Type C, B recoveries at 100% with billing decreases linked to a claiming patient ratio Gap recoveries at 100% with billing decreases linked to a claiming patient ratio EDI system rules review at 100% linked to a claiming patient ratio
MBF’s Proposed approach to Measuring and Tracking Claims Leakage Savings (3) Calculating Savings – Hospital [ [ [ Determining our impact is confirmed by a multivariate analysis so that for example a decrease in benefits which may result from a declining membership, or patient base for a provider, is not wrongly attributed to our actions, or the actions of others in the Fund are not claimed by my team Recoveries are counted at 100% Rules or system changes introduction at 100% linked to a claiming patient ratio Schedule changes at 100% eg prostheses linked to a claiming patient ratio Audited items at 100% of reduced billings linked to a claiming patient ratio Contract changes at 100% linked to a claiming patient ratio Calculating Savings – Medical [ [ Similar to above Type C, B recoveries at 100% with billing decreases linked to a claiming patient ratio Gap recoveries at 100% with billing decreases linked to a claiming patient ratio EDI system rules review at 100% linked to a claiming patient ratio
 MBF’s Proposed approach to Measuring and Tracking Claims Leakage Savings (4) Calculating Savings – Ancillary [ [ [ Determining our impact is confirmed by a multivariate analysis so that for example a decrease in benefits which may result from a declining membership or patient base for a provider is not wrongly attributed to our actions, or the actions of others in the Fund are not claimed by my team Recoveries counted at 100% Rules introduction at 100% linked to a claiming patient ratio Audited providers at 100% of reduced billings linked to a claiming patient ratio Withdrawn HICAPS providers at 100% of reduced billings linked to a claiming patient ratio Deregistered or de-recognised provider savings are calculated as the difference between the State average benefit per patient and the average benefit previously paid to the provider's patients. The full benefit paid is not claimed, because, unless the patients are bogus, it is assumed that they will be treated by another provider at the State average
MBF’s Proposed approach to Measuring and Tracking Claims Leakage Savings (4) Calculating Savings – Ancillary [ [ [ Determining our impact is confirmed by a multivariate analysis so that for example a decrease in benefits which may result from a declining membership or patient base for a provider is not wrongly attributed to our actions, or the actions of others in the Fund are not claimed by my team Recoveries counted at 100% Rules introduction at 100% linked to a claiming patient ratio Audited providers at 100% of reduced billings linked to a claiming patient ratio Withdrawn HICAPS providers at 100% of reduced billings linked to a claiming patient ratio Deregistered or de-recognised provider savings are calculated as the difference between the State average benefit per patient and the average benefit previously paid to the provider's patients. The full benefit paid is not claimed, because, unless the patients are bogus, it is assumed that they will be treated by another provider at the State average
 MBF’s Proposed approach to Measuring and Tracking Claims Leakage Savings (5) Members & Fund Staff [ Separate from what has gone before, terminated members and staff savings are calculated at the rate at which they were abusing the system, which would have continued but for the intervention Savings claiming period [ [ Rules and audit changes which lead to behaviour change are claimed for a period of 12 months from point of intervention and then cease as a new benchmark has been set Funds recalled are simply claimed in the month the funds are actually received What we don’t count [ [ We do not claim any benefits for any preventative/deterrent impact (Hawthorn effect) on providers, members or staff who we have not been involved with, as we believe that it is difficult to verify We do not count Indemnity refunds in leakage savings. They are recorded separately as they are seen as a debt recovery exercise
MBF’s Proposed approach to Measuring and Tracking Claims Leakage Savings (5) Members & Fund Staff [ Separate from what has gone before, terminated members and staff savings are calculated at the rate at which they were abusing the system, which would have continued but for the intervention Savings claiming period [ [ Rules and audit changes which lead to behaviour change are claimed for a period of 12 months from point of intervention and then cease as a new benchmark has been set Funds recalled are simply claimed in the month the funds are actually received What we don’t count [ [ We do not claim any benefits for any preventative/deterrent impact (Hawthorn effect) on providers, members or staff who we have not been involved with, as we believe that it is difficult to verify We do not count Indemnity refunds in leakage savings. They are recorded separately as they are seen as a debt recovery exercise
 THE END QUESTIONS/COMMENTS
THE END QUESTIONS/COMMENTS


