d9022d456bc49259be39c9a87a64e06a.ppt
- Количество слайдов: 60
 The Science of Effective Pediatric Inpatient Nutrition 2005 Kevin M. Creamer M. D. , FAAP Medical Director, PICU WRAMC Chief, Pediatric Nutrition Support Team
The Science of Effective Pediatric Inpatient Nutrition 2005 Kevin M. Creamer M. D. , FAAP Medical Director, PICU WRAMC Chief, Pediatric Nutrition Support Team
 A hypothetical case u Starvin Marvin is a 2 y. o. who presents with a 2 -3 week Hx of fevers, weight loss, pallor, decreased energy, appetite and activity u PE reveals Wt 13 kg , down 1. 5 kg, pallor, petechia, + HSM u Labs reveal WBC 26 K with 50% blasts, anemia and thrombocytopenia
A hypothetical case u Starvin Marvin is a 2 y. o. who presents with a 2 -3 week Hx of fevers, weight loss, pallor, decreased energy, appetite and activity u PE reveals Wt 13 kg , down 1. 5 kg, pallor, petechia, + HSM u Labs reveal WBC 26 K with 50% blasts, anemia and thrombocytopenia
 Hospital Course u Day 1 - NPO, IVFs, labs, Xrays u Day 2 – NPO for BM and LP, as well as Hickman u Day 3 - Chemo, picky PO u Day 4 -6 - continued poor PO, with emesis occasionally u Day 7 -10 – emesis resolves, PO inadequate u Day 12 – pancytopenia, sepsis with GNR
Hospital Course u Day 1 - NPO, IVFs, labs, Xrays u Day 2 – NPO for BM and LP, as well as Hickman u Day 3 - Chemo, picky PO u Day 4 -6 - continued poor PO, with emesis occasionally u Day 7 -10 – emesis resolves, PO inadequate u Day 12 – pancytopenia, sepsis with GNR
 Teaching points u. Nutritionally-at-risk from the word GO • Debilitated Ortho spine patient • Recurrent bowel obstruction patient u. No nutrition plan, No monitoring, No intervention u. Hope is not a method u. Could sepsis event been avoided? ?
Teaching points u. Nutritionally-at-risk from the word GO • Debilitated Ortho spine patient • Recurrent bowel obstruction patient u. No nutrition plan, No monitoring, No intervention u. Hope is not a method u. Could sepsis event been avoided? ?
 Inpatient Nutrition Goals Think about nutritional status on every patient Outline the dynamic between illness, nutritional state and secondary morbidity Recognize need to estimate/calculate goals calories in order to reach the goal u u u • u Individualized goals for time course, and disease process Institute effective nutrition support with the help of Pediatric nutritionist
Inpatient Nutrition Goals Think about nutritional status on every patient Outline the dynamic between illness, nutritional state and secondary morbidity Recognize need to estimate/calculate goals calories in order to reach the goal u u u • u Individualized goals for time course, and disease process Institute effective nutrition support with the help of Pediatric nutritionist
 Acute Stress
Acute Stress
 The 5 W’s of Inpatient Nutrition Why, Who, When, Where, What ?
The 5 W’s of Inpatient Nutrition Why, Who, When, Where, What ?
 Acute Stress u Major Surgery, Sepsis, Burns, Trauma • Result in massive outpouring of catechols, ACTH, GH, ADH, glucagon, somatomedins – Insulin inhibition, elevation of glucose and free fatty acids • ↑ Inflammatory Cytokines: TNF, IL 1 , IL-6 – PMN release and degranulation Mucosal permeability u Stress hormones and mediators ↑ release of c. AMP which down-regulate lymphoid immune activity
Acute Stress u Major Surgery, Sepsis, Burns, Trauma • Result in massive outpouring of catechols, ACTH, GH, ADH, glucagon, somatomedins – Insulin inhibition, elevation of glucose and free fatty acids • ↑ Inflammatory Cytokines: TNF, IL 1 , IL-6 – PMN release and degranulation Mucosal permeability u Stress hormones and mediators ↑ release of c. AMP which down-regulate lymphoid immune activity
 Acute Stress u NPO state starves gut mucosa • Gut mass 50% in 7 days of fasting • Gut contains 80% of body’s immune tissue – “GALT and MALT” • Intestinal s. Ig. A ↓ in 5 days • ↑ Th 1 pro-inflammatory lymphocytes u Major stress doubles protein turnover • Skeletal muscle cannibalized for fuel for enterocytes (glutamine) Stechmiller JK, Am J Crit Care, 1997
Acute Stress u NPO state starves gut mucosa • Gut mass 50% in 7 days of fasting • Gut contains 80% of body’s immune tissue – “GALT and MALT” • Intestinal s. Ig. A ↓ in 5 days • ↑ Th 1 pro-inflammatory lymphocytes u Major stress doubles protein turnover • Skeletal muscle cannibalized for fuel for enterocytes (glutamine) Stechmiller JK, Am J Crit Care, 1997
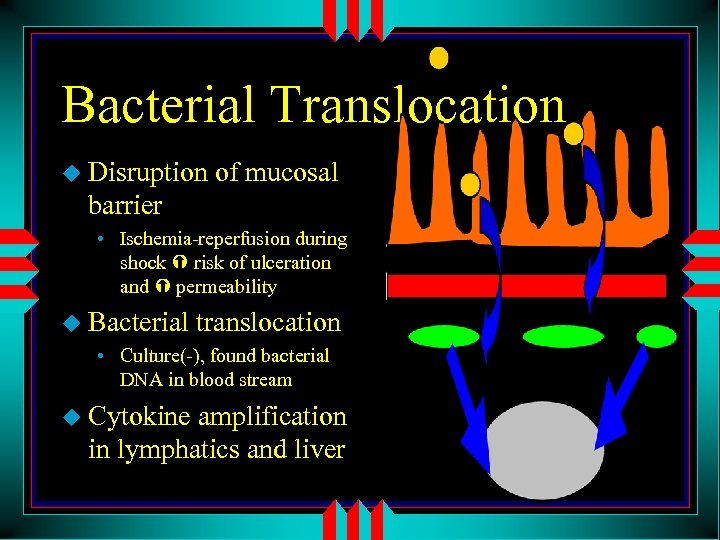 Bacterial Translocation u Disruption of mucosal barrier • Ischemia-reperfusion during shock risk of ulceration and permeability u Bacterial translocation • Culture(-), found bacterial DNA in blood stream u Cytokine amplification in lymphatics and liver
Bacterial Translocation u Disruption of mucosal barrier • Ischemia-reperfusion during shock risk of ulceration and permeability u Bacterial translocation • Culture(-), found bacterial DNA in blood stream u Cytokine amplification in lymphatics and liver
 Bacterial Translocation u Enteral nutrition can prevent translocation • Trophic feeds stimulate gut hormones and nourish mucosa, increase blood flow, re-energize tight junctions, improve brush border • Enteral vs. Parenteral feeds - postop septic related complications u Enteral feeds stimulate Th 2 lymphocytes which PMN adhesion in lung Deitch EA, Ann Surg, 1987, 1990; Border JR, Ann. Surg, 1987; Carrico CJ, Arch Surg, 1986; Alverdy JC, Surgery, 1988; Moore J, JPEN, 1991, Kudsk, Am J Surg, 2002
Bacterial Translocation u Enteral nutrition can prevent translocation • Trophic feeds stimulate gut hormones and nourish mucosa, increase blood flow, re-energize tight junctions, improve brush border • Enteral vs. Parenteral feeds - postop septic related complications u Enteral feeds stimulate Th 2 lymphocytes which PMN adhesion in lung Deitch EA, Ann Surg, 1987, 1990; Border JR, Ann. Surg, 1987; Carrico CJ, Arch Surg, 1986; Alverdy JC, Surgery, 1988; Moore J, JPEN, 1991, Kudsk, Am J Surg, 2002
 WHY ? Is nutrition such a big deal? Malnutrition Prevalence Nutrition Status and Outcomes Gut Bacterial Translocation
WHY ? Is nutrition such a big deal? Malnutrition Prevalence Nutrition Status and Outcomes Gut Bacterial Translocation
 Malnutrition Prevalence u 15 to 50 % of hospitalized pediatric inpatients are malnourished on presentation (down from 35 -65%) • 15 to 20 % of critically ill patients • 33% patients with congenital heart disease • 39% awaiting elective surgery Parsons, AJCN, 1980; Mize, Nutr Supt Ser, 1984; Merritt, Am J Clin Nutr, 1979, Huddleston KC, CC Clin of NA, 1993, Cameron, Arch Ped 1995, Cooper, J Ped Surg 1981
Malnutrition Prevalence u 15 to 50 % of hospitalized pediatric inpatients are malnourished on presentation (down from 35 -65%) • 15 to 20 % of critically ill patients • 33% patients with congenital heart disease • 39% awaiting elective surgery Parsons, AJCN, 1980; Mize, Nutr Supt Ser, 1984; Merritt, Am J Clin Nutr, 1979, Huddleston KC, CC Clin of NA, 1993, Cameron, Arch Ped 1995, Cooper, J Ped Surg 1981
 Malnutrition Snapshot u Inpatient population of Boston Children’s Hospital was surveyed Sept 24, 1992 • 268 children ages 0 -18 years u Using Waterlow criteria: • 25% were acutely malnourished, 27% were chronically malnourished u Of 17 ICU patients, 4 (24%) were classified with severe PEM Hendricks, Arch Ped Adol Med, 1995
Malnutrition Snapshot u Inpatient population of Boston Children’s Hospital was surveyed Sept 24, 1992 • 268 children ages 0 -18 years u Using Waterlow criteria: • 25% were acutely malnourished, 27% were chronically malnourished u Of 17 ICU patients, 4 (24%) were classified with severe PEM Hendricks, Arch Ped Adol Med, 1995
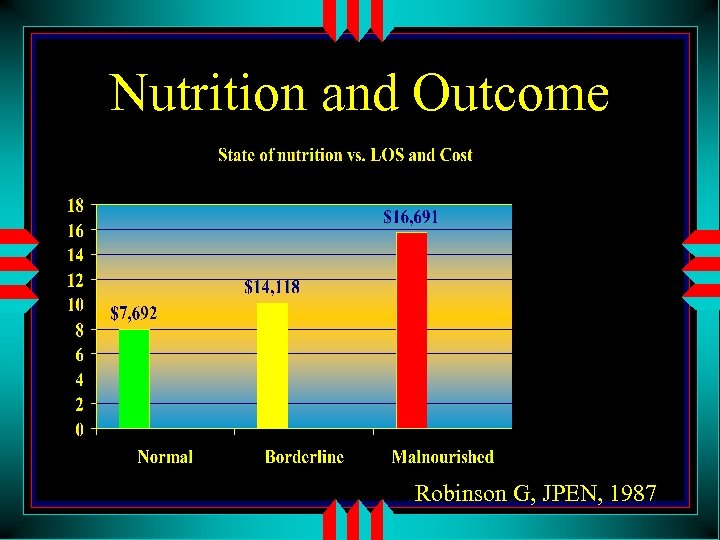 Nutrition and Outcome Robinson G, JPEN, 1987
Nutrition and Outcome Robinson G, JPEN, 1987
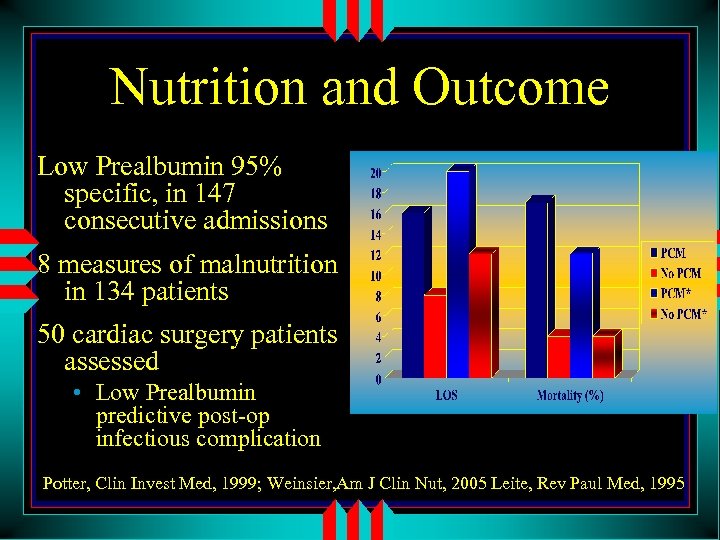 Nutrition and Outcome Low Prealbumin 95% specific, in 147 consecutive admissions 8 measures of malnutrition in 134 patients 50 cardiac surgery patients assessed • Low Prealbumin predictive post-op infectious complication Potter, Clin Invest Med, 1999; Weinsier, Am J Clin Nut, 2005 Leite, Rev Paul Med, 1995
Nutrition and Outcome Low Prealbumin 95% specific, in 147 consecutive admissions 8 measures of malnutrition in 134 patients 50 cardiac surgery patients assessed • Low Prealbumin predictive post-op infectious complication Potter, Clin Invest Med, 1999; Weinsier, Am J Clin Nut, 2005 Leite, Rev Paul Med, 1995
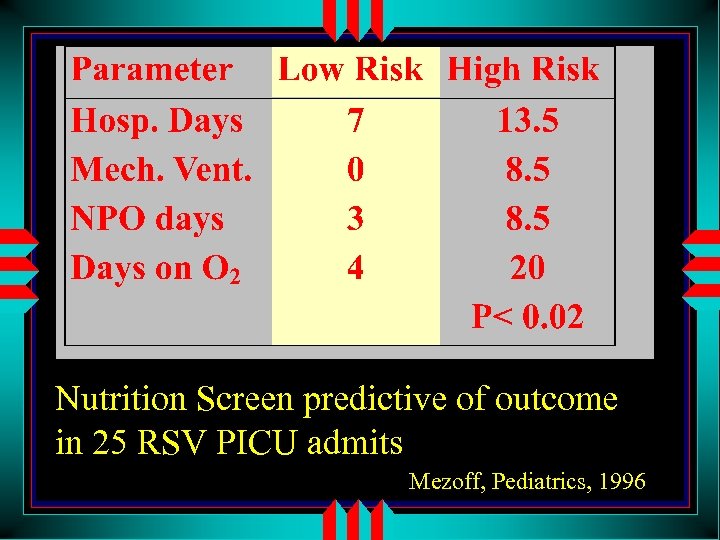 Nutrition Screen predictive of outcome in 25 RSV PICU admits Mezoff, Pediatrics, 1996
Nutrition Screen predictive of outcome in 25 RSV PICU admits Mezoff, Pediatrics, 1996
 Nutrition and Outcome u 60 PICU patients had nutrition status evaluated, with PSI, and TISS applied u Acute PEM associated (P<0. 01) with physiologic instability, mortality and quantity of care u Malnutrition can result in delayed wound healing, respiratory failure, increased potential for infection, death Pollack MM, JPEN, 1985
Nutrition and Outcome u 60 PICU patients had nutrition status evaluated, with PSI, and TISS applied u Acute PEM associated (P<0. 01) with physiologic instability, mortality and quantity of care u Malnutrition can result in delayed wound healing, respiratory failure, increased potential for infection, death Pollack MM, JPEN, 1985
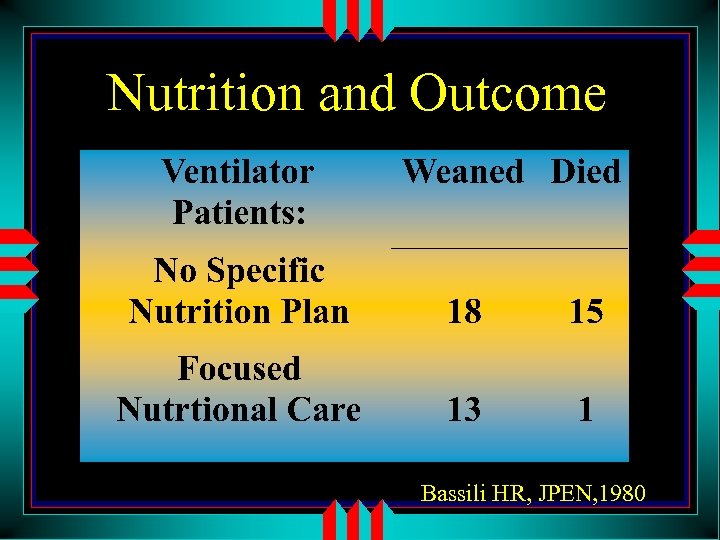 Nutrition and Outcome Bassili HR, JPEN, 1980
Nutrition and Outcome Bassili HR, JPEN, 1980
 Nutrition and Outcome u. PICU Outcomes in 323 patients after Nutrition support team instituted • Use of Enteral nutrition (EN) in medical patients increased 25% to 67% u. Mortality risk decreased 83% for those receiving EN >50% of LOS • EN independent predictor of survival in multiple regression analysis. Gurgueira, JPEN, 2005
Nutrition and Outcome u. PICU Outcomes in 323 patients after Nutrition support team instituted • Use of Enteral nutrition (EN) in medical patients increased 25% to 67% u. Mortality risk decreased 83% for those receiving EN >50% of LOS • EN independent predictor of survival in multiple regression analysis. Gurgueira, JPEN, 2005
 WHO ? Needs to know? Gets assessed? ALL Physicians! ALL Patients!
WHO ? Needs to know? Gets assessed? ALL Physicians! ALL Patients!
 Nutrition Dichotomy u 79 FP residents • Nutrition Interest (72. 2%) vs. Perceived Knowledge – Parenteral and enteral nutrition 34. 2%, Infant nutrition 27. 5 %, Nutrition assessment 17. 7% u 3416 Primary Care physicians • < 40% practiced what they preached Lasswell AB, J of Med Ed, 1984, Levine BS, Am J Clin Nut, 1993
Nutrition Dichotomy u 79 FP residents • Nutrition Interest (72. 2%) vs. Perceived Knowledge – Parenteral and enteral nutrition 34. 2%, Infant nutrition 27. 5 %, Nutrition assessment 17. 7% u 3416 Primary Care physicians • < 40% practiced what they preached Lasswell AB, J of Med Ed, 1984, Levine BS, Am J Clin Nut, 1993
 Nutrition Practice: Uphill battle u. Adult ICU group found their patients only received 52% of goal calories • Reasons included physician under ordering, frequent cessations, and slow advancement u. Designed a protocol but only 58% went on it Spain, JPEN, 1999
Nutrition Practice: Uphill battle u. Adult ICU group found their patients only received 52% of goal calories • Reasons included physician under ordering, frequent cessations, and slow advancement u. Designed a protocol but only 58% went on it Spain, JPEN, 1999
 I wonder if I’m missing out on some critical piece of information
I wonder if I’m missing out on some critical piece of information
 Nutrition Screen u. Should be completed within 24 hours of admission u. High risk surgical patients should be screened weeks to months ahead of planned surgery In your continuity clinic • Multidisciplinary team • Supplement , reassess, or reschedule
Nutrition Screen u. Should be completed within 24 hours of admission u. High risk surgical patients should be screened weeks to months ahead of planned surgery In your continuity clinic • Multidisciplinary team • Supplement , reassess, or reschedule
 Nutritionally-at-risk u Weight for age < 10 th % tile u Weight for Height < 10 th % tile u Acute weight loss > 5% over 1 month or >10% total u Birth weight < 2 SD below mean for gestational age u Increased metabolic requirements 2 chronic disease u Impaired ability to ingest or tolerate oral feeds u Weight % tile crossing 2 contour lines over time (FTT)
Nutritionally-at-risk u Weight for age < 10 th % tile u Weight for Height < 10 th % tile u Acute weight loss > 5% over 1 month or >10% total u Birth weight < 2 SD below mean for gestational age u Increased metabolic requirements 2 chronic disease u Impaired ability to ingest or tolerate oral feeds u Weight % tile crossing 2 contour lines over time (FTT)
 Prealbumin u. Transthyretin albumin has nothing to do with • Small body pool and half life of 2 days makes prealbumin an reasonable monitor of visceral protein homeostasis u. Drops during the first 3 -5 days of stress it should rise thereafter u Daily rise of 1 mg/dl indicates anabolism
Prealbumin u. Transthyretin albumin has nothing to do with • Small body pool and half life of 2 days makes prealbumin an reasonable monitor of visceral protein homeostasis u. Drops during the first 3 -5 days of stress it should rise thereafter u Daily rise of 1 mg/dl indicates anabolism
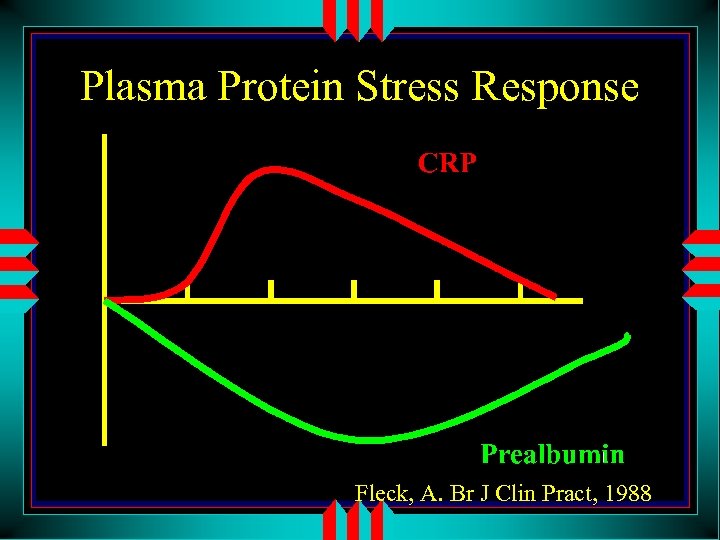 Plasma Protein Stress Response Fleck, A. Br J Clin Pract, 1988
Plasma Protein Stress Response Fleck, A. Br J Clin Pract, 1988
 Prealbumin as a predictor u Surgically stressed Infants • Prolonged ↑ CRP with ↓ Prealbumin had ↑ mortality – Strongest predictor POD#5 prealbumin depression u Prealbumin ideal nutrition screen for: • 50 children with solid tumors – before and during chemo • 86 Adult post-op patients requiring TPN Chwals WJ, Surg Clin NA, 1992, Elhasid, Cancer, 1999, Erstad, Pharmaco, 1994
Prealbumin as a predictor u Surgically stressed Infants • Prolonged ↑ CRP with ↓ Prealbumin had ↑ mortality – Strongest predictor POD#5 prealbumin depression u Prealbumin ideal nutrition screen for: • 50 children with solid tumors – before and during chemo • 86 Adult post-op patients requiring TPN Chwals WJ, Surg Clin NA, 1992, Elhasid, Cancer, 1999, Erstad, Pharmaco, 1994
 Prealbumin u. Measure twice weekly u. Once 65% of needs met expect levels to rise 1 mg/dl a day u If weekly rise is less than 4 mg/dl • check N 2 balance and CRP to determine if cause is nutritional inadequacy or ongoing SIRS Expert roundtable, 10 th World Congress of Gastroenterolgy
Prealbumin u. Measure twice weekly u. Once 65% of needs met expect levels to rise 1 mg/dl a day u If weekly rise is less than 4 mg/dl • check N 2 balance and CRP to determine if cause is nutritional inadequacy or ongoing SIRS Expert roundtable, 10 th World Congress of Gastroenterolgy
 WHEN? Should I start? Early Enteral vs Standard timing
WHEN? Should I start? Early Enteral vs Standard timing
 Enteral Contraindications Intubation/extubation planned within 4° u Hemodynamic instability requiring escalation in therapy u Intestinal obstruction u Massive UGI bleed u Gut ischemia u I’m nervous about this kid u
Enteral Contraindications Intubation/extubation planned within 4° u Hemodynamic instability requiring escalation in therapy u Intestinal obstruction u Massive UGI bleed u Gut ischemia u I’m nervous about this kid u
 Early feeds vs. Standard u. Adults with gut malignancies and neurotrauma has shorter LOS and fewer infections when fed early u 19 controlled studies (24° vs 3 -5 days) • 16/19 studies showed improved outcome • Improved healing, complications and LOS • Recommended for critically ill surgical pts Braga, CCM, 2001 Grahm T, Neurosurgery, 1989 Taylor, CCM 1999 Heyland DK, CC Clin of NA, 1998 Zaloga. CCM 1999
Early feeds vs. Standard u. Adults with gut malignancies and neurotrauma has shorter LOS and fewer infections when fed early u 19 controlled studies (24° vs 3 -5 days) • 16/19 studies showed improved outcome • Improved healing, complications and LOS • Recommended for critically ill surgical pts Braga, CCM, 2001 Grahm T, Neurosurgery, 1989 Taylor, CCM 1999 Heyland DK, CC Clin of NA, 1998 Zaloga. CCM 1999
 Early feeds: Pediatrics u Tolerated pediatric burn patients u 42 ventilated children (76% on vasoactive meds) • Transpyloric feeding tubes placed at bedside • 74% of patients reached full feeds within 24 hrs, rest within 48 hrs – No complications Chellis MJ, JPEN, 1996, Trocki, Burns, 1995
Early feeds: Pediatrics u Tolerated pediatric burn patients u 42 ventilated children (76% on vasoactive meds) • Transpyloric feeding tubes placed at bedside • 74% of patients reached full feeds within 24 hrs, rest within 48 hrs – No complications Chellis MJ, JPEN, 1996, Trocki, Burns, 1995
 All is Not Rosy u All Mechanical Ventilated patients u. Group exclusions Lots of Early (75) Late (75) VAP 49. 3% 30. 7% C diff 13. 3% 4. 0% ICU stay 13. 6± 14. 2 9. 8 ± 7. 4 Mortality 20% 26. 7% p. 02. 043. 334 Ibraham, JPEN, 2002
All is Not Rosy u All Mechanical Ventilated patients u. Group exclusions Lots of Early (75) Late (75) VAP 49. 3% 30. 7% C diff 13. 3% 4. 0% ICU stay 13. 6± 14. 2 9. 8 ± 7. 4 Mortality 20% 26. 7% p. 02. 043. 334 Ibraham, JPEN, 2002
 WHERE? In the gut do I put the food? Oral vs. Tube feeding Gastric vs. Transpyloric feeds
WHERE? In the gut do I put the food? Oral vs. Tube feeding Gastric vs. Transpyloric feeds
 Tube Feeding Considerations Nutritionally-at-risk with inadequate oral intake for the past 3 -5 days. u Meeting <50% estimated needs orally for previous 7 -10 days. u • Shorten to 3 -5 days if traumatized or severely catabolic u. Disease state preventing adequate P. O. intake for >5 days
Tube Feeding Considerations Nutritionally-at-risk with inadequate oral intake for the past 3 -5 days. u Meeting <50% estimated needs orally for previous 7 -10 days. u • Shorten to 3 -5 days if traumatized or severely catabolic u. Disease state preventing adequate P. O. intake for >5 days
 Gastric vs. Transpyloric u No aspiration difference in 54 patients receiving gastric vs transpyloric radiolabeled feeds u 33 mechanicaly ventilated Micro-aspiration 7. 5 >> 3. 9% in NJ fed patients u 80 adult trauma victims • Duodenally fed patients reached goal calories 34 vs. 44 hours with had less pneumonia 27% vs 42%* u 80 ventilated adults randomized • gastric feeds + E-mycin 200 mg q 8 (55% / 74%) • Transpyloric feeds (44% / 67%) Esparza, Intens C Med, 2001, Kortbeek, J Trauma, 1999, Heyland, CCM, 2001, Boivin, CCM, 2001
Gastric vs. Transpyloric u No aspiration difference in 54 patients receiving gastric vs transpyloric radiolabeled feeds u 33 mechanicaly ventilated Micro-aspiration 7. 5 >> 3. 9% in NJ fed patients u 80 adult trauma victims • Duodenally fed patients reached goal calories 34 vs. 44 hours with had less pneumonia 27% vs 42%* u 80 ventilated adults randomized • gastric feeds + E-mycin 200 mg q 8 (55% / 74%) • Transpyloric feeds (44% / 67%) Esparza, Intens C Med, 2001, Kortbeek, J Trauma, 1999, Heyland, CCM, 2001, Boivin, CCM, 2001
 Transpyloric u 59 ventilated children randomized to receive continuous or interrupted transpyloric feeds during the day before and of extubation • Continuous group got >90% goal calories both day vs 73% and 46% • No aspiration events or difference in adverse events Lyons, JPEN, 2002
Transpyloric u 59 ventilated children randomized to receive continuous or interrupted transpyloric feeds during the day before and of extubation • Continuous group got >90% goal calories both day vs 73% and 46% • No aspiration events or difference in adverse events Lyons, JPEN, 2002
 Neuromuscular blockade and ECMO? u May decreased REE by 10 -15 % u Primary Neurotransmitter in Gut is VIP not acetylcholine • Neuromuscular blockade work via Ac. H receptors u By what mechanism do neuromuscularly blocked patients become intolerant of enteral feeds? • Gastric atony 2° Benzodiazepines and narcotics u Enteral feeds for Pediatric ECMO patients is safe with trends toward improved survival Pettignano, CCM, 1998
Neuromuscular blockade and ECMO? u May decreased REE by 10 -15 % u Primary Neurotransmitter in Gut is VIP not acetylcholine • Neuromuscular blockade work via Ac. H receptors u By what mechanism do neuromuscularly blocked patients become intolerant of enteral feeds? • Gastric atony 2° Benzodiazepines and narcotics u Enteral feeds for Pediatric ECMO patients is safe with trends toward improved survival Pettignano, CCM, 1998
 Enteral Pitfalls u 2 adult studies with 95 ICU pts, had 66%-78% of goal feeds prescribed, 52%- 71% delivered • Gastric Intolerance (Residuals #1) – BZD and Narcs effect stomach > intestine • Airway management – 22/26 PICU pts had feeds held for extubation that only 5 got • Diagnostic procedures – Some ventilated patients fed right up to OR Mc. Clave SA, CCM, 1999, De. Jonghe, CCM, 2001, Fry-Brower +Mc. Cunn, CCM(a), 2002,
Enteral Pitfalls u 2 adult studies with 95 ICU pts, had 66%-78% of goal feeds prescribed, 52%- 71% delivered • Gastric Intolerance (Residuals #1) – BZD and Narcs effect stomach > intestine • Airway management – 22/26 PICU pts had feeds held for extubation that only 5 got • Diagnostic procedures – Some ventilated patients fed right up to OR Mc. Clave SA, CCM, 1999, De. Jonghe, CCM, 2001, Fry-Brower +Mc. Cunn, CCM(a), 2002,
 WHAT? Amount of calories do I Feed Them? How much to feed Trophic feeds Enteral vs. Parenteral Lipid phobia
WHAT? Amount of calories do I Feed Them? How much to feed Trophic feeds Enteral vs. Parenteral Lipid phobia
 Caloric Goals? u. Brazilian PICU reviewed 37 charts u. Only 3 had an assessment done in 425 days u. No Patient had caloric goals set • Only 29. 7% met goals • 80. 5 % fed Parenterally Leite, Rev Assoc Med Bras, 1996
Caloric Goals? u. Brazilian PICU reviewed 37 charts u. Only 3 had an assessment done in 425 days u. No Patient had caloric goals set • Only 29. 7% met goals • 80. 5 % fed Parenterally Leite, Rev Assoc Med Bras, 1996
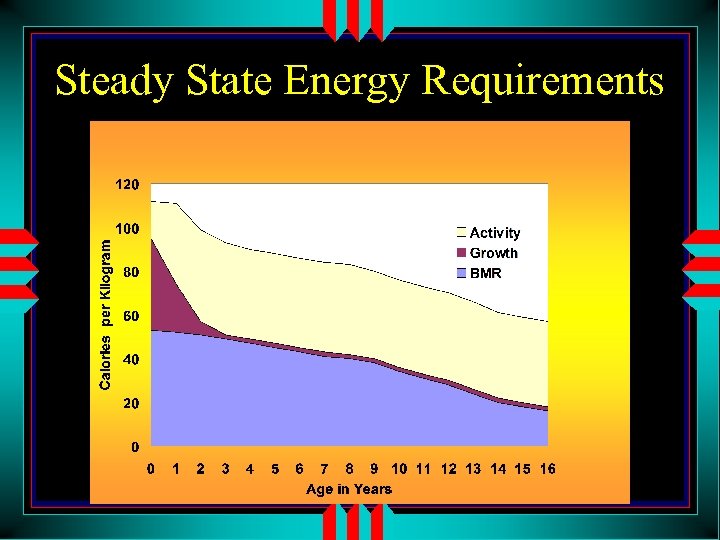 Steady State Energy Requirements
Steady State Energy Requirements
 Energy Requirements u Calorie needs change during the course of the hospitalization. • Hemodynamically unstable? • Ventilated vs Extubated u Ebb phase (Hypometabolic): obligate (–) nitrogen balance during acute critical illness • No need for growth calories (BMR may suffice? ) • Watch out for overfeeding – Steatosis, Hyperglycemia, Hypertriglyceridemia
Energy Requirements u Calorie needs change during the course of the hospitalization. • Hemodynamically unstable? • Ventilated vs Extubated u Ebb phase (Hypometabolic): obligate (–) nitrogen balance during acute critical illness • No need for growth calories (BMR may suffice? ) • Watch out for overfeeding – Steatosis, Hyperglycemia, Hypertriglyceridemia
 Therapeutic window u 187 critically ill adults >96º in ICU • Tertiles of % ACCP recommended caloric intake u Patients receiving 33 -65% goal Vs. <33% (18 kcal/kg) • OR survival 1. 22, discharge without sepsis 1. 2, without vent 1. 8 • Patients > 65% goal OR 0. 82, 0. 75, 0. 69 u Sickest patients (SAPS>50) • Did worse when they received >33% goal Krishnan, Chest, 2003
Therapeutic window u 187 critically ill adults >96º in ICU • Tertiles of % ACCP recommended caloric intake u Patients receiving 33 -65% goal Vs. <33% (18 kcal/kg) • OR survival 1. 22, discharge without sepsis 1. 2, without vent 1. 8 • Patients > 65% goal OR 0. 82, 0. 75, 0. 69 u Sickest patients (SAPS>50) • Did worse when they received >33% goal Krishnan, Chest, 2003
 Energy Requirements u Flow phase (Hypermetabolic) • As the child improves and becomes anabolic, calorie needs for growth and activity must be included u. Underestimating needs can increase risk for infection, poor wound healing, poor growth, and overall poor outcome
Energy Requirements u Flow phase (Hypermetabolic) • As the child improves and becomes anabolic, calorie needs for growth and activity must be included u. Underestimating needs can increase risk for infection, poor wound healing, poor growth, and overall poor outcome
 Energy Requirements u 12 Septic and 12 Traumatized patients • Total energy expenditure and REE measured for 2 separate 5 -day periods • TEE Sepsis 25 kcal/kg >>> 47 kcal/kg • TEE Trauma 31 kcal/kg >>> 59 kcal/kg u. Second week TEE: indirect calorimetry X 1. 8 u. TEE remained elevated for weeks Uehara, CCM, 1999
Energy Requirements u 12 Septic and 12 Traumatized patients • Total energy expenditure and REE measured for 2 separate 5 -day periods • TEE Sepsis 25 kcal/kg >>> 47 kcal/kg • TEE Trauma 31 kcal/kg >>> 59 kcal/kg u. Second week TEE: indirect calorimetry X 1. 8 u. TEE remained elevated for weeks Uehara, CCM, 1999
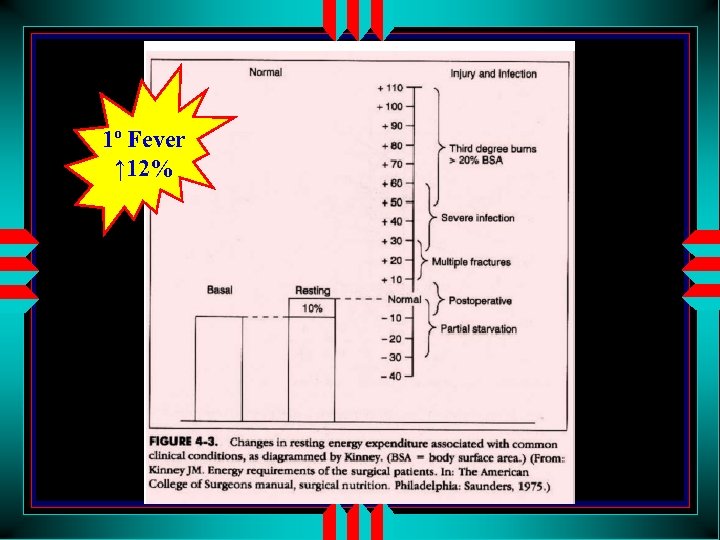 1º Fever ↑ 12%
1º Fever ↑ 12%
 Trophic Feeds fed 15% calories enterally had permeability and bacterial translocation u 10 post-op infants fed trophically (21 cal/kg/d) had improved Staph killing vs TPN alone u Rats • 37% vs. 52% vs. 65% (Controls) – Related to production of TNFα u> 6 kcal/kg (>25% ACCP cal goals) in 138 adult MICU patients reduced BSI (relative hazard 0. 24) Omura, Ann Surg, 2000, Okada, J Ped Surg, Robinson, CCM, 2004
Trophic Feeds fed 15% calories enterally had permeability and bacterial translocation u 10 post-op infants fed trophically (21 cal/kg/d) had improved Staph killing vs TPN alone u Rats • 37% vs. 52% vs. 65% (Controls) – Related to production of TNFα u> 6 kcal/kg (>25% ACCP cal goals) in 138 adult MICU patients reduced BSI (relative hazard 0. 24) Omura, Ann Surg, 2000, Okada, J Ped Surg, Robinson, CCM, 2004
 Trophic feeds Feed type # Patients Mortality SMR Enteral 167 25% . 71 Parenteral 26 54% 1. 4 Parenteral + Trickle 24 38% . 9 Trophic feeds are stress ulcer and antibiotic prophylaxis rolled into one Marik, CCM(a), 2002
Trophic feeds Feed type # Patients Mortality SMR Enteral 167 25% . 71 Parenteral 26 54% 1. 4 Parenteral + Trickle 24 38% . 9 Trophic feeds are stress ulcer and antibiotic prophylaxis rolled into one Marik, CCM(a), 2002
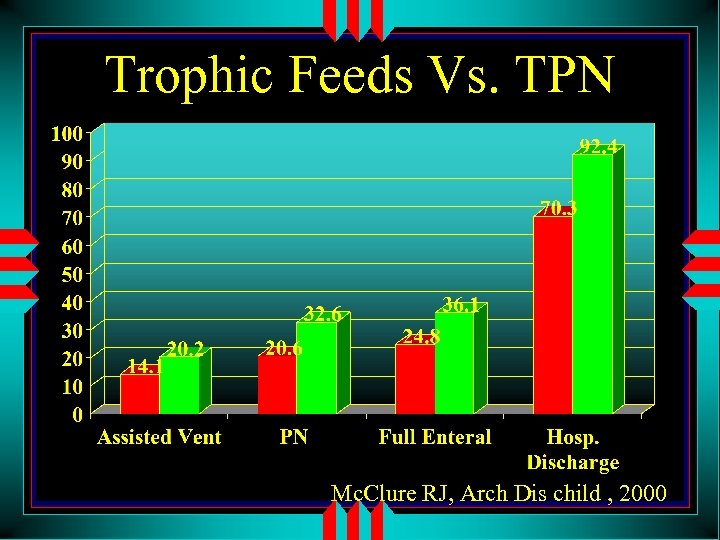 Trophic Feeds Vs. TPN Mc. Clure RJ, Arch Dis child , 2000
Trophic Feeds Vs. TPN Mc. Clure RJ, Arch Dis child , 2000
 Enteral Feeds vs. TPN u. Enteral feeds in Critically ill population • improve wound healing, mucosal permeability u> 10 studies show enteral feeds are safe, feasible and cheaper than TPN u. Meta analysis adult ICU patients Enteral feeds vs. TPN RR infection 0. 66 Schroeder D, JPEN, 1991, Hadfield R, Am J Resp Crit Care Med, 1995 Robert Dimand, UC Davis, Peds CC Update 2002, Gramlich, Nutrition, 2004
Enteral Feeds vs. TPN u. Enteral feeds in Critically ill population • improve wound healing, mucosal permeability u> 10 studies show enteral feeds are safe, feasible and cheaper than TPN u. Meta analysis adult ICU patients Enteral feeds vs. TPN RR infection 0. 66 Schroeder D, JPEN, 1991, Hadfield R, Am J Resp Crit Care Med, 1995 Robert Dimand, UC Davis, Peds CC Update 2002, Gramlich, Nutrition, 2004
 TPN vs. Hope u Meta Analysis 26 studies (210 reviewed) • 2211 patients • Trend toward reduced complications in TPN patients (risk ratio 0. 84) u 4 studies used TPN > 3 weeks • Mortality in TPN pts was 6. 8% vs. 12. 4% u Meta Analysis 11 studies • Parenteral nutrition vs. delayed enteral improved mortality • Increased infectious risk (OR 1. 65 CI 1. 1 -2, 5) in PN vs. all enteral Heyland DK, JAMA, 1999, Simpson, Int Care Med, 2005, Doig, CCM(A) 2005
TPN vs. Hope u Meta Analysis 26 studies (210 reviewed) • 2211 patients • Trend toward reduced complications in TPN patients (risk ratio 0. 84) u 4 studies used TPN > 3 weeks • Mortality in TPN pts was 6. 8% vs. 12. 4% u Meta Analysis 11 studies • Parenteral nutrition vs. delayed enteral improved mortality • Increased infectious risk (OR 1. 65 CI 1. 1 -2, 5) in PN vs. all enteral Heyland DK, JAMA, 1999, Simpson, Int Care Med, 2005, Doig, CCM(A) 2005
 Parenteral Considerations u. Nutritionally-at-risk patient with non- functional gut. u. Adequate nutritional status on admission but non-functioning gut 3 -5 days after admission “The major advance in TPN since the 1980’s is that it is not used as much”
Parenteral Considerations u. Nutritionally-at-risk patient with non- functional gut. u. Adequate nutritional status on admission but non-functioning gut 3 -5 days after admission “The major advance in TPN since the 1980’s is that it is not used as much”
 Lipid Phobia? u When infants given TPN without lipids • CHO only TPN resulted in amino acid oxidation, proteolysis, CO 2 production and lipogenesis u Lipid requirements • Essential fatty acid (0. 5 gm/kg/d), Promote Nitrogen sparing, Increased lipid clearance during stress u Balanced approach to fulfilling energy requirements Bresson, Am J Clin Nut 1991, Tilden, AJDC, 1989, Schears, Crit Care Clin, 1997
Lipid Phobia? u When infants given TPN without lipids • CHO only TPN resulted in amino acid oxidation, proteolysis, CO 2 production and lipogenesis u Lipid requirements • Essential fatty acid (0. 5 gm/kg/d), Promote Nitrogen sparing, Increased lipid clearance during stress u Balanced approach to fulfilling energy requirements Bresson, Am J Clin Nut 1991, Tilden, AJDC, 1989, Schears, Crit Care Clin, 1997
 Lipids u Original 10% lipid compounds – Intravenous fat emulsions contain 50 -60% linoleic acid a precursor to arachidonic acid – May disturb balance between thromboxane and prostacyclin production u Modern 20% emulsion cause less Trig • Neonates clear better, less phospholipids • No problems with oxygenation when given as 1824° infusion • No immune problems when Triglycerides <700
Lipids u Original 10% lipid compounds – Intravenous fat emulsions contain 50 -60% linoleic acid a precursor to arachidonic acid – May disturb balance between thromboxane and prostacyclin production u Modern 20% emulsion cause less Trig • Neonates clear better, less phospholipids • No problems with oxygenation when given as 1824° infusion • No immune problems when Triglycerides <700
 Monitor Outcomes u Residuals u Age appropriate weight gain u Diarrhea / Constipation u Medication Compatibility? u Emesis / Aspiration u Proper wound healing u Fluid and electrolyte balance u Euglycemia u Improved N 2 balance and Prealbumin
Monitor Outcomes u Residuals u Age appropriate weight gain u Diarrhea / Constipation u Medication Compatibility? u Emesis / Aspiration u Proper wound healing u Fluid and electrolyte balance u Euglycemia u Improved N 2 balance and Prealbumin
 HOPE IS NOT A METHOD! u. Who? Is you, screening all your patients u. Why? They’ll do worse if you don’t u. When? The sooner the better u. What? Enteral better, even trophic better than TPN alone u. Where? PO>NG>NJ > IV
HOPE IS NOT A METHOD! u. Who? Is you, screening all your patients u. Why? They’ll do worse if you don’t u. When? The sooner the better u. What? Enteral better, even trophic better than TPN alone u. Where? PO>NG>NJ > IV


