6c0e5d01feaccc96ed9e6a2ad9457b59.ppt
- Количество слайдов: 57
 The Queen’s Medical Center – Honolulu, Hawaii © SBAR What Every Nurse Needs to Know ! Liane Fujita, APRN, MS, CCRN Jean Henderson, APRN, MS, CCRN 1
The Queen’s Medical Center – Honolulu, Hawaii © SBAR What Every Nurse Needs to Know ! Liane Fujita, APRN, MS, CCRN Jean Henderson, APRN, MS, CCRN 1
 © Program Objectives 1. Explain how SBAR evolved as an important communication tool. 2. State the impact of SBAR on patient safety. 3. Describe the 4 components of SBAR. 4. State 3 “Tips for Talking” before calling a physician. 5. Apply SBAR format when relaying critical patient information. 2
© Program Objectives 1. Explain how SBAR evolved as an important communication tool. 2. State the impact of SBAR on patient safety. 3. Describe the 4 components of SBAR. 4. State 3 “Tips for Talking” before calling a physician. 5. Apply SBAR format when relaying critical patient information. 2
 © History Of SBAR • SBAR was developed by our United States Navy. • Submariners use this communication tool. • Works well in their stressful, time-critical, emergency situations. 3
© History Of SBAR • SBAR was developed by our United States Navy. • Submariners use this communication tool. • Works well in their stressful, time-critical, emergency situations. 3
 © History Of SBAR In many ways we have similar stressful working environments! Saving our patients Saving our country 4
© History Of SBAR In many ways we have similar stressful working environments! Saving our patients Saving our country 4
 © SBAR Stands For: • • Situation Background Assessment Recommendation • Helps you identify most important points of a situation • Organizes relevant information • Helps you present it to others in a quick but coherent way 5
© SBAR Stands For: • • Situation Background Assessment Recommendation • Helps you identify most important points of a situation • Organizes relevant information • Helps you present it to others in a quick but coherent way 5
 New Requirement for Patient Safety • Facilities must implement a standardized approach to hand-off communication. • This needs to include an opportunity to ask and respond to questions. • The Queen’s Medical Center in Honolulu has selected SBAR. • Without a shared communication model among all healthcare providers (RN, MD, Pharmacist, Lab, RT, OT, PT, Dietary etc) tragic patient outcomes can and do occur. 6
New Requirement for Patient Safety • Facilities must implement a standardized approach to hand-off communication. • This needs to include an opportunity to ask and respond to questions. • The Queen’s Medical Center in Honolulu has selected SBAR. • Without a shared communication model among all healthcare providers (RN, MD, Pharmacist, Lab, RT, OT, PT, Dietary etc) tragic patient outcomes can and do occur. 6
 Why Is Using SBAR Important? • Effective communication between healthcare providers is critical to patient safety. • JCAHO reports that approximately 65% of the sentinel events in 2006 were due to problems with communication (shown in next slide). • SBAR has proven to be effective in many healthcare organizations in improving communication. 7
Why Is Using SBAR Important? • Effective communication between healthcare providers is critical to patient safety. • JCAHO reports that approximately 65% of the sentinel events in 2006 were due to problems with communication (shown in next slide). • SBAR has proven to be effective in many healthcare organizations in improving communication. 7
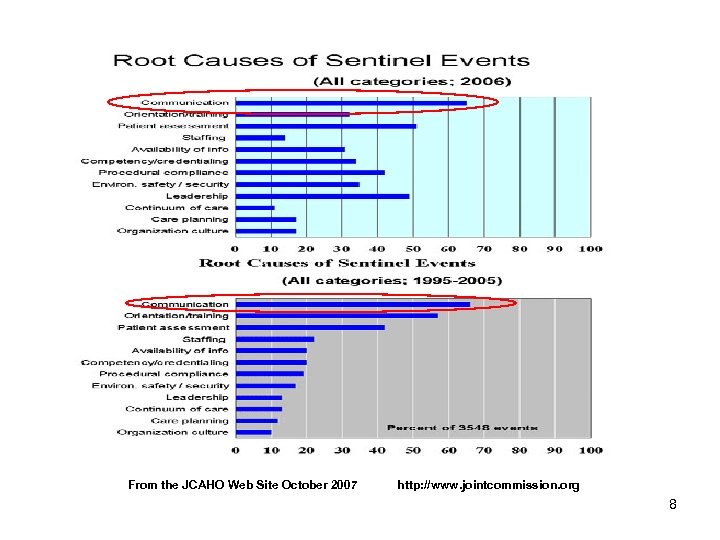 From the JCAHO Web Site October 2007 http: //www. jointcommission. org 8
From the JCAHO Web Site October 2007 http: //www. jointcommission. org 8
 © Question # 1 Why is SBAR important? 1. It has proven to save lives in the aviation arena only. 2. Communication issues continues to be the most predominant cause of sentinel events. 3. For the primary reason that it helps create respectful working relationships. 4. It is an enjoyable game people like to play. 9
© Question # 1 Why is SBAR important? 1. It has proven to save lives in the aviation arena only. 2. Communication issues continues to be the most predominant cause of sentinel events. 3. For the primary reason that it helps create respectful working relationships. 4. It is an enjoyable game people like to play. 9
 Communication Styles Venus or Mars? • Training approaches differ between nurses and physicians – Nurses tend to be descriptive and narrative/ trained not to make “diagnoses”. – Physicians would rather just “have the facts”/trained as problem solvers. • Frustration on both ends – Physicians keep waiting for the punch line. – nurses feel interrupted, not listened to. • This frustration while attempting to communicate important clinical information can and does lead to near misses and sentinel events. 10
Communication Styles Venus or Mars? • Training approaches differ between nurses and physicians – Nurses tend to be descriptive and narrative/ trained not to make “diagnoses”. – Physicians would rather just “have the facts”/trained as problem solvers. • Frustration on both ends – Physicians keep waiting for the punch line. – nurses feel interrupted, not listened to. • This frustration while attempting to communicate important clinical information can and does lead to near misses and sentinel events. 10
 © Question # 2 Communication styles differ between nurses and physicians because… 1. 2. 3. 4. Physicians are taught the Hippocratic communication style. Nurses are taught short, bullet type communication style. Nurses and physicians are trained in different communication styles. Physicians prefer long and lengthy narrative type communication. 11
© Question # 2 Communication styles differ between nurses and physicians because… 1. 2. 3. 4. Physicians are taught the Hippocratic communication style. Nurses are taught short, bullet type communication style. Nurses and physicians are trained in different communication styles. Physicians prefer long and lengthy narrative type communication. 11
 © What Goes Wrong? • Concern is expressed but gets lost in the story. • Problem is stated but often not clearly (the hint and hope syndrome). 12
© What Goes Wrong? • Concern is expressed but gets lost in the story. • Problem is stated but often not clearly (the hint and hope syndrome). 12
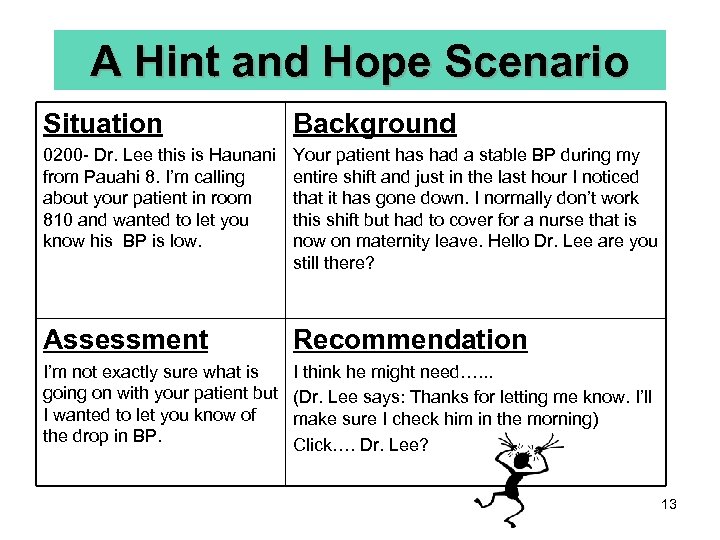 A Hint and Hope Scenario Situation Background 0200 - Dr. Lee this is Haunani from Pauahi 8. I’m calling about your patient in room 810 and wanted to let you know his BP is low. Your patient has had a stable BP during my entire shift and just in the last hour I noticed that it has gone down. I normally don’t work this shift but had to cover for a nurse that is now on maternity leave. Hello Dr. Lee are you still there? Assessment Recommendation I’m not exactly sure what is going on with your patient but I wanted to let you know of the drop in BP. I think he might need…. . . (Dr. Lee says: Thanks for letting me know. I’ll make sure I check him in the morning) Click…. Dr. Lee? 13
A Hint and Hope Scenario Situation Background 0200 - Dr. Lee this is Haunani from Pauahi 8. I’m calling about your patient in room 810 and wanted to let you know his BP is low. Your patient has had a stable BP during my entire shift and just in the last hour I noticed that it has gone down. I normally don’t work this shift but had to cover for a nurse that is now on maternity leave. Hello Dr. Lee are you still there? Assessment Recommendation I’m not exactly sure what is going on with your patient but I wanted to let you know of the drop in BP. I think he might need…. . . (Dr. Lee says: Thanks for letting me know. I’ll make sure I check him in the morning) Click…. Dr. Lee? 13
 © What Goes Wrong? – con’t • Individual not prepared with the pertinent information. • Outcome not achieved. • Both parties are frustrated by the interaction. 14
© What Goes Wrong? – con’t • Individual not prepared with the pertinent information. • Outcome not achieved. • Both parties are frustrated by the interaction. 14
 © How Does SBAR Help? • Provides a framework for organizing information. • Bridges gap in communication styles. • Calls for you to share your assessment & recommendation. 15
© How Does SBAR Help? • Provides a framework for organizing information. • Bridges gap in communication styles. • Calls for you to share your assessment & recommendation. 15
 © How Does SBAR Help? • Concludes with you being clear about what you need (no more hint and hope). • Provides a “common” framework for everyone to utilize and makes it acceptable to remind each other of missing components. • Can prevent delay in treatment. 16
© How Does SBAR Help? • Concludes with you being clear about what you need (no more hint and hope). • Provides a “common” framework for everyone to utilize and makes it acceptable to remind each other of missing components. • Can prevent delay in treatment. 16
 © Question # 3 Due to differences in communication styles, SBAR helps by… 1. 2. 3. 4. 5. Avoiding the hint and hope syndrome. Achieving outcomes contributing to both parties being satisfied. Having individuals be organized and prepared with the pertinent information. Having you not share your assessment of the situation. Expressing your concern using a common framework understood by both parties. a. b. c. d. 1, 3, 4 4 only All of the above 1, 2, 3, 5 17
© Question # 3 Due to differences in communication styles, SBAR helps by… 1. 2. 3. 4. 5. Avoiding the hint and hope syndrome. Achieving outcomes contributing to both parties being satisfied. Having individuals be organized and prepared with the pertinent information. Having you not share your assessment of the situation. Expressing your concern using a common framework understood by both parties. a. b. c. d. 1, 3, 4 4 only All of the above 1, 2, 3, 5 17
 Tips Before Talking Before calling a physician be ready with the following Information…. . • • • Check to make sure you are calling the right physician! Know the admitting diagnosis. Assess the patient and have recent VS, lab work, test results. Know the I&O status, allergies, medications and IV fluids. Read the most recent progress notes and prior shift nursing assessment & notes. 18
Tips Before Talking Before calling a physician be ready with the following Information…. . • • • Check to make sure you are calling the right physician! Know the admitting diagnosis. Assess the patient and have recent VS, lab work, test results. Know the I&O status, allergies, medications and IV fluids. Read the most recent progress notes and prior shift nursing assessment & notes. 18
 Physician’s Have 3 Main Questions • What is the problem? • What do you need me to do? • When do I have to respond? (Is this just an update or does this need immediate attention? ) 19
Physician’s Have 3 Main Questions • What is the problem? • What do you need me to do? • When do I have to respond? (Is this just an update or does this need immediate attention? ) 19
 © Question # 4 When calling a physician which statement is incorrect? 1. 2. 3. 4. 5. Do check to make sure you are calling the right MD. Assess the patient prior to calling. Read off all lab and test results in the last 24 hours. Provide only pertinent lab values to this patient’s situation. Review progress and nursing notes prior to call. 20
© Question # 4 When calling a physician which statement is incorrect? 1. 2. 3. 4. 5. Do check to make sure you are calling the right MD. Assess the patient prior to calling. Read off all lab and test results in the last 24 hours. Provide only pertinent lab values to this patient’s situation. Review progress and nursing notes prior to call. 20
 Situations When SBAR Can Make a Difference ! • RN – MD communication • RN – RN communication o o o RN – Crisis RN Intra-shift hand-offs (when going on a break) Inter-shift hand-offs Patient transfer hand-offs to another unit Patient transfer hand-offs to another area for procedures • RN – other departments o o o Lab Pharmacy Rehabilitation Services Respiratory Therapy Imaging Services 21
Situations When SBAR Can Make a Difference ! • RN – MD communication • RN – RN communication o o o RN – Crisis RN Intra-shift hand-offs (when going on a break) Inter-shift hand-offs Patient transfer hand-offs to another unit Patient transfer hand-offs to another area for procedures • RN – other departments o o o Lab Pharmacy Rehabilitation Services Respiratory Therapy Imaging Services 21
 Components Of “SBAR” • What does SBAR stand for? © o Situation o Background o Assessmemt o Recommendation 22
Components Of “SBAR” • What does SBAR stand for? © o Situation o Background o Assessmemt o Recommendation 22
 © Situation • The situation is described by stating the problem. • It is a to-the-point punch-line done in 5 -10 seconds to get the attention of the receiver. • Included are: o Identification of yourself – your name and unit o Patient’s name, physician, and room number o Brief and to-the-point statement of your concern 23
© Situation • The situation is described by stating the problem. • It is a to-the-point punch-line done in 5 -10 seconds to get the attention of the receiver. • Included are: o Identification of yourself – your name and unit o Patient’s name, physician, and room number o Brief and to-the-point statement of your concern 23
 “Situation” Example Harry Green (patient) • “Dr. Smith, this is Jenny from QET 9 Ewa. I am calling in regards to Harry Green, Dr. Bond’s patient in room 947. His heart rate has increased to the 150’s and it is irregular. He does admit to feeling a little dizzy, short of breath and complains of palpitations. ” 24
“Situation” Example Harry Green (patient) • “Dr. Smith, this is Jenny from QET 9 Ewa. I am calling in regards to Harry Green, Dr. Bond’s patient in room 947. His heart rate has increased to the 150’s and it is irregular. He does admit to feeling a little dizzy, short of breath and complains of palpitations. ” 24
 Background • A brief history of the situation is provided to further describe the problem. • The background information may include: o Admission diagnosis and date of admission o Pertinent medical history o Brief summary of the treatment to date o Clinical assessment (include vital signs) o Recent interventions given and effectiveness o Abnormal lab or imaging tests 25
Background • A brief history of the situation is provided to further describe the problem. • The background information may include: o Admission diagnosis and date of admission o Pertinent medical history o Brief summary of the treatment to date o Clinical assessment (include vital signs) o Recent interventions given and effectiveness o Abnormal lab or imaging tests 25
 “Background” Example • “He walked for the first time since returning from PEG placement this morning. His PEG site looks fine. Prior to the walk, his pulse was in the 90’s at rest with blood pressure of 110/70. After applying O 2 at 2 liters nasal cannula, his O 2 sat increased to 96% from 94%. ” 26
“Background” Example • “He walked for the first time since returning from PEG placement this morning. His PEG site looks fine. Prior to the walk, his pulse was in the 90’s at rest with blood pressure of 110/70. After applying O 2 at 2 liters nasal cannula, his O 2 sat increased to 96% from 94%. ” 26
 “Background” Tips • Prior to speaking with the other person: * * * Anticipate what information the receiving person needs. Have all the relevant information in front of you. Have the medical record / electronic record open to that patient. Using SBAR notepad, write down all information. Practice conversation if uncomfortable with the situation. 27
“Background” Tips • Prior to speaking with the other person: * * * Anticipate what information the receiving person needs. Have all the relevant information in front of you. Have the medical record / electronic record open to that patient. Using SBAR notepad, write down all information. Practice conversation if uncomfortable with the situation. 27
 Assessment • An assessment of the situation is made. o What you think is going on with the patient. o What you think the problem is. • At times, you may not be able to make an interpretation of the problem…. If so, it is OK to report this. For example: o “I am not sure what the problem is, but the patient is deteriorating”. o “The patient seems to be unstable and may get worse, I think we need to do something”. 28
Assessment • An assessment of the situation is made. o What you think is going on with the patient. o What you think the problem is. • At times, you may not be able to make an interpretation of the problem…. If so, it is OK to report this. For example: o “I am not sure what the problem is, but the patient is deteriorating”. o “The patient seems to be unstable and may get worse, I think we need to do something”. 28
 “Assessment” example • “I think this change in heart rate is causing him to be symptomatic. ” 29
“Assessment” example • “I think this change in heart rate is causing him to be symptomatic. ” 29
 Recommendation • Based on the situation, background assessment of the case, state what you think needs to be done. • Some staff find this step of SBAR intimidating as they feel they are not qualified to make a recommendation or worry that their recommendation is incorrect. 30
Recommendation • Based on the situation, background assessment of the case, state what you think needs to be done. • Some staff find this step of SBAR intimidating as they feel they are not qualified to make a recommendation or worry that their recommendation is incorrect. 30
 Recommendation – con’t • It is important to remember that you are not making the final decision. • The purpose of the recommendation is to outline your thoughts. • If you are not sure what needs to be done, simply stating, “It is important for you to check on the patient now” is an appropriate recommendation. 31
Recommendation – con’t • It is important to remember that you are not making the final decision. • The purpose of the recommendation is to outline your thoughts. • If you are not sure what needs to be done, simply stating, “It is important for you to check on the patient now” is an appropriate recommendation. 31
 “Recommendation” Example • “I would like you to see Mr. Green now. In the meantime, would you like a 12 -lead EKG done? ” 32
“Recommendation” Example • “I would like you to see Mr. Green now. In the meantime, would you like a 12 -lead EKG done? ” 32
 “Recommendation” Tips • Using “critical” words can increase the intensity of your message – it conveys a sense of urgency. • Examples: o “The patient needs medication now. ” o “I need you to check on the patient immediately. ” “Critical” words: • Now • Must • Need • Immediately • Critical • Priority • Important • Quickly • Requires • At once • Instantly/this instant • Acute • Imperative • Vital • Crucial • Urgent • Essential 33
“Recommendation” Tips • Using “critical” words can increase the intensity of your message – it conveys a sense of urgency. • Examples: o “The patient needs medication now. ” o “I need you to check on the patient immediately. ” “Critical” words: • Now • Must • Need • Immediately • Critical • Priority • Important • Quickly • Requires • At once • Instantly/this instant • Acute • Imperative • Vital • Crucial • Urgent • Essential 33
 © Question # 5 Which statement is incorrect? 1. 2. 3. 4. In the first step, Situation, it is crucial to get the attention of the receiver by concisely stating the problem in 5 -10 seconds. Before making a call, always have relevant information available which the receiver is likely to ask or want to know. Before making a call, you must know what the specific problem is with your patient to make a definitive assessment of the situation. Using one of the “critical” words can help to convey the sense of urgency requiring attention. 34
© Question # 5 Which statement is incorrect? 1. 2. 3. 4. In the first step, Situation, it is crucial to get the attention of the receiver by concisely stating the problem in 5 -10 seconds. Before making a call, always have relevant information available which the receiver is likely to ask or want to know. Before making a call, you must know what the specific problem is with your patient to make a definitive assessment of the situation. Using one of the “critical” words can help to convey the sense of urgency requiring attention. 34
 © Question # 6 Which word is not considered a “critical” word because it doesn’t convey a sense of urgency? 1. 2. 3. 4. Now Important Crucial Perhaps 35
© Question # 6 Which word is not considered a “critical” word because it doesn’t convey a sense of urgency? 1. 2. 3. 4. Now Important Crucial Perhaps 35
 © C. U. S. An assertion tool to help formulate your recommendation. Utilize C. U. S. statements in your SBAR briefing. v “I am Concerned for my patient’s condition. ” v “I am Uncomfortable with my patient’s condition. ” v “The Safety of my patient is at risk. ” 36
© C. U. S. An assertion tool to help formulate your recommendation. Utilize C. U. S. statements in your SBAR briefing. v “I am Concerned for my patient’s condition. ” v “I am Uncomfortable with my patient’s condition. ” v “The Safety of my patient is at risk. ” 36
 What to do if you are not getting what you need…. Escalate and use your “Chain of Command” to make certain the patient gets the care they deserve and need. 37
What to do if you are not getting what you need…. Escalate and use your “Chain of Command” to make certain the patient gets the care they deserve and need. 37
 © Question # 7 What Do You Do if SBAR Isn’t Working? 1. 2. 3. 4. Wait until change of shift and ask the oncoming nurse to follow up with the problem. Assume that no follow up is needed since the physician is not concerned. Curse at the physician hoping for some action. Use the C. U. S. tool in your discussion with the physician and if that fails use your chain of command. 38
© Question # 7 What Do You Do if SBAR Isn’t Working? 1. 2. 3. 4. Wait until change of shift and ask the oncoming nurse to follow up with the problem. Assume that no follow up is needed since the physician is not concerned. Curse at the physician hoping for some action. Use the C. U. S. tool in your discussion with the physician and if that fails use your chain of command. 38
 Sample SBAR Quick Reference (next 3 screens) 39
Sample SBAR Quick Reference (next 3 screens) 39
 Sample SBAR Quick Reference • SBAR report about a critical situation: Situation I am calling about (patient name and location). The patient’s code status is (code status). The problem I am calling about is. I have just assessed the patient personally: • Vital signs are: blood pressure ___/___, pulse ___, respiration ___, and temperature ___. • I am concerned about the patient’s • blood pressure because it is over 200 or less than 100 or 30 mm. Hg below usual • pulse because it is > 140 or < 50 • respiration because it is < 8 or > 30 • temperature because it is < 96 or > 103 40
Sample SBAR Quick Reference • SBAR report about a critical situation: Situation I am calling about (patient name and location). The patient’s code status is (code status). The problem I am calling about is. I have just assessed the patient personally: • Vital signs are: blood pressure ___/___, pulse ___, respiration ___, and temperature ___. • I am concerned about the patient’s • blood pressure because it is over 200 or less than 100 or 30 mm. Hg below usual • pulse because it is > 140 or < 50 • respiration because it is < 8 or > 30 • temperature because it is < 96 or > 103 40
 Sample SBAR Quick Reference Background The patient’s mental status is: • Alert and oriented to person, place, and time • Confused and cooperative or non-cooperative • Agitated or combative • Lethargic but conversant and able to swallow • Stuporous, not talking clearly, and possibly unable to swallow • Comatose, eyes closed, and not responding to stimulation The skin is: • warm and dry / diaphoretic / mottled • pale / extremities are cold / extremities are warm The patient is not or is on oxygen. • The patient has been on _____(liters/min. ) or _____ (%) oxygen for _____ minutes (hours) • The oximeter reads _____% • The oximeter does not detect a good pulse and is giving erratic readings 41
Sample SBAR Quick Reference Background The patient’s mental status is: • Alert and oriented to person, place, and time • Confused and cooperative or non-cooperative • Agitated or combative • Lethargic but conversant and able to swallow • Stuporous, not talking clearly, and possibly unable to swallow • Comatose, eyes closed, and not responding to stimulation The skin is: • warm and dry / diaphoretic / mottled • pale / extremities are cold / extremities are warm The patient is not or is on oxygen. • The patient has been on _____(liters/min. ) or _____ (%) oxygen for _____ minutes (hours) • The oximeter reads _____% • The oximeter does not detect a good pulse and is giving erratic readings 41
 Sample SBAR Quick Reference Assessment I think the problem is (say what you think is the problem). • The problem seems to be cardiac/infection/neurologic/respiratory. • I am not sure what the problem is, but the patient is deteriorating. • The patient seems to be unstable and may get worse. We need to do something. Recommendation I suggest or request that you (say what you would like to see done) • Transfer the patient to critical care. • Come and see the patient at this time. • Talk to the patient or family about code status. • Ask the on-call family practice resident to see the patient now. • Ask for a consultant to see the patient now. Are any tests needed? • Do you need any tests done (e. g. CXR, ABG, EKG, CBC)? • Others? If a change in treatment is ordered, ask: • How often do you want vital signs? • How long do you expect this problem will last? • If the patient does not get better, when would you want us to call again? . 42
Sample SBAR Quick Reference Assessment I think the problem is (say what you think is the problem). • The problem seems to be cardiac/infection/neurologic/respiratory. • I am not sure what the problem is, but the patient is deteriorating. • The patient seems to be unstable and may get worse. We need to do something. Recommendation I suggest or request that you (say what you would like to see done) • Transfer the patient to critical care. • Come and see the patient at this time. • Talk to the patient or family about code status. • Ask the on-call family practice resident to see the patient now. • Ask for a consultant to see the patient now. Are any tests needed? • Do you need any tests done (e. g. CXR, ABG, EKG, CBC)? • Others? If a change in treatment is ordered, ask: • How often do you want vital signs? • How long do you expect this problem will last? • If the patient does not get better, when would you want us to call again? . 42
 Impact of SBAR to the Profession of Nursing Empowers staff with the knowledge that they have influence over decisions that affect their work life Job Satisfaction Magnet Force 9: Autonomy 43
Impact of SBAR to the Profession of Nursing Empowers staff with the knowledge that they have influence over decisions that affect their work life Job Satisfaction Magnet Force 9: Autonomy 43
 4 SBAR Examples © 44
4 SBAR Examples © 44
 Example #1 RN to Crisis RN • It is 20: 10 on a med-surg floor and you are caring for a 85 -year old female in room 980 admitted yesterday for anorexia and pneumonia. • She has a history of Alzheimer's disease, stroke, and is on home peritoneal dialysis (PD). • She was started on NG tube feedings at 30 cc/hour 3 hours ago. • As you prepare to start her PD, you note that she appears more lethargic from her baseline with intermittent periods of restlessness. BP 122/74, HR 110 and slightly irregular, RR 30, and O 2 sat 90% on 4 liters nasal cannula. • You place her on O 2 6 L N/C and stat page RT. O 2 sat remains ~90% so RT applies a 100% non-rebreather mask and O 2 sat increases to 92%. You call the Crisis Nurse/ Rapid Response Team to get assistance. Using SBAR, how would you report the condition of this patient and state your needs? 45
Example #1 RN to Crisis RN • It is 20: 10 on a med-surg floor and you are caring for a 85 -year old female in room 980 admitted yesterday for anorexia and pneumonia. • She has a history of Alzheimer's disease, stroke, and is on home peritoneal dialysis (PD). • She was started on NG tube feedings at 30 cc/hour 3 hours ago. • As you prepare to start her PD, you note that she appears more lethargic from her baseline with intermittent periods of restlessness. BP 122/74, HR 110 and slightly irregular, RR 30, and O 2 sat 90% on 4 liters nasal cannula. • You place her on O 2 6 L N/C and stat page RT. O 2 sat remains ~90% so RT applies a 100% non-rebreather mask and O 2 sat increases to 92%. You call the Crisis Nurse/ Rapid Response Team to get assistance. Using SBAR, how would you report the condition of this patient and state your needs? 45
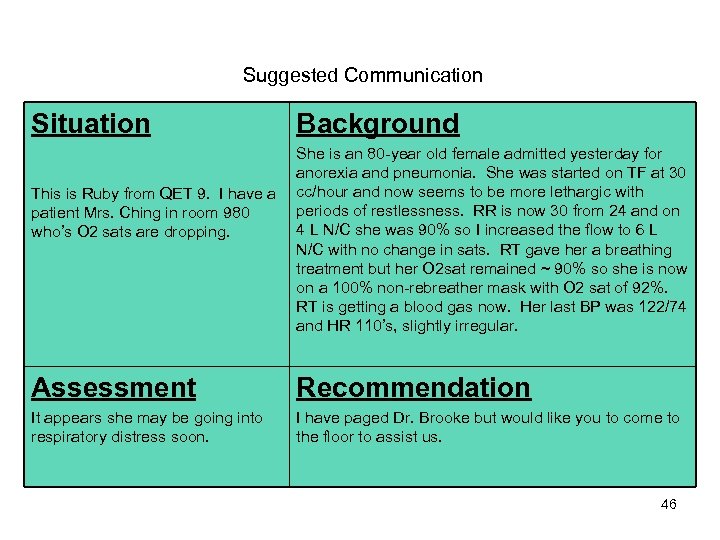 Suggested Communication Situation This is Ruby from QET 9. I have a patient Mrs. Ching in room 980 who’s O 2 sats are dropping. Background She is an 80 -year old female admitted yesterday for anorexia and pneumonia. She was started on TF at 30 cc/hour and now seems to be more lethargic with periods of restlessness. RR is now 30 from 24 and on 4 L N/C she was 90% so I increased the flow to 6 L N/C with no change in sats. RT gave her a breathing treatment but her O 2 sat remained ~ 90% so she is now on a 100% non-rebreather mask with O 2 sat of 92%. RT is getting a blood gas now. Her last BP was 122/74 and HR 110’s, slightly irregular. Assessment Recommendation It appears she may be going into respiratory distress soon. I have paged Dr. Brooke but would like you to come to the floor to assist us. 46
Suggested Communication Situation This is Ruby from QET 9. I have a patient Mrs. Ching in room 980 who’s O 2 sats are dropping. Background She is an 80 -year old female admitted yesterday for anorexia and pneumonia. She was started on TF at 30 cc/hour and now seems to be more lethargic with periods of restlessness. RR is now 30 from 24 and on 4 L N/C she was 90% so I increased the flow to 6 L N/C with no change in sats. RT gave her a breathing treatment but her O 2 sat remained ~ 90% so she is now on a 100% non-rebreather mask with O 2 sat of 92%. RT is getting a blood gas now. Her last BP was 122/74 and HR 110’s, slightly irregular. Assessment Recommendation It appears she may be going into respiratory distress soon. I have paged Dr. Brooke but would like you to come to the floor to assist us. 46
 Example #2 RN to RN Patient Transfer • • • It is 14: 50 on a orthopedic med-surg floor and you are caring for a 64 -year old male admitted 2 days ago for acute pancreatitis with a hx of HTN, diabetes, and alcoholism. He is NPO with a NG tube in place. The plan is to transfer him to a medical floor because there are orthopedic patients in PACU waiting to be transferred to your unit as they need the room to accommodate patients coming out of OR. You recognize it is shift change but also know you need the bed asap. You called the unit twice but they were not able to receive Mr. Ching then. You call the medical floor and ask to speak to the nurse receiving this patient. Using SBAR, how would you approach this situation? 47
Example #2 RN to RN Patient Transfer • • • It is 14: 50 on a orthopedic med-surg floor and you are caring for a 64 -year old male admitted 2 days ago for acute pancreatitis with a hx of HTN, diabetes, and alcoholism. He is NPO with a NG tube in place. The plan is to transfer him to a medical floor because there are orthopedic patients in PACU waiting to be transferred to your unit as they need the room to accommodate patients coming out of OR. You recognize it is shift change but also know you need the bed asap. You called the unit twice but they were not able to receive Mr. Ching then. You call the medical floor and ask to speak to the nurse receiving this patient. Using SBAR, how would you approach this situation? 47
 Suggested Communication Situation Background This is Abe from QET 8. I recognize it is shift change but it is urgent that we transfer our patient to you. Mr. Ching is being transferred to your unit as we need to accommodate orthopedic patients ready to be discharged from PACU needs the beds soon to receive patients coming out of OR. Assessment Recommendation I recognize your unit has been busy as well but we all need to do the best possible to help accommodate all patients. I need to transfer Mr. Ching to your unit now. By the time I prepare to transfer him, if the oncoming shift RN is available, I could give him/her report if that would help you. 48
Suggested Communication Situation Background This is Abe from QET 8. I recognize it is shift change but it is urgent that we transfer our patient to you. Mr. Ching is being transferred to your unit as we need to accommodate orthopedic patients ready to be discharged from PACU needs the beds soon to receive patients coming out of OR. Assessment Recommendation I recognize your unit has been busy as well but we all need to do the best possible to help accommodate all patients. I need to transfer Mr. Ching to your unit now. By the time I prepare to transfer him, if the oncoming shift RN is available, I could give him/her report if that would help you. 48
 Example #3 RN to MD • Situation: Dr. Aloha, this is Lani Chun on T 9 DH. I am calling about your patient Millie Flowers in room 636. Millie is complaining of shortness of breath and pain in her right chest area when she breathes. She is a full code. Her BP is up from 118/74 to 154/92 and her heart rate is 112 , up from 72. Her temp is 97. 7 and her respiratory rate is 28. I am concerned about her pain and respiratory status. • Background: Millie had been stable since her admission this morning for pneumonia. She is a long time smoker and her oxygen sat on 2 L nasal cannula that had been 94% is now 85%. Her last chest x-ray this am showed LLL pneumonia. She has a non productive cough and is now short of breath. All labs were in normal range this am. I’m also not hearing any breath sounds on her right and rhonchi on her left. • Assessment: Millie’s condition is deteriorating and I’m very worried about her respiratory status. 49
Example #3 RN to MD • Situation: Dr. Aloha, this is Lani Chun on T 9 DH. I am calling about your patient Millie Flowers in room 636. Millie is complaining of shortness of breath and pain in her right chest area when she breathes. She is a full code. Her BP is up from 118/74 to 154/92 and her heart rate is 112 , up from 72. Her temp is 97. 7 and her respiratory rate is 28. I am concerned about her pain and respiratory status. • Background: Millie had been stable since her admission this morning for pneumonia. She is a long time smoker and her oxygen sat on 2 L nasal cannula that had been 94% is now 85%. Her last chest x-ray this am showed LLL pneumonia. She has a non productive cough and is now short of breath. All labs were in normal range this am. I’m also not hearing any breath sounds on her right and rhonchi on her left. • Assessment: Millie’s condition is deteriorating and I’m very worried about her respiratory status. 49
 © Question # 8 What Would be the Most Appropriate Recommendation? 1. 2. 3. 4. I’m not sure what is going on with Millie, what do you want to do? I’m not sure what is going on with Millie but I suggest she be seen by you or the resident when you get a chance. Be silent and wait to hear what Dr. Aloha recommends first. I’m not sure what is going on with Millie but I suggest she be seen by you or the resident now. Do you need any tests/labs done? 50
© Question # 8 What Would be the Most Appropriate Recommendation? 1. 2. 3. 4. I’m not sure what is going on with Millie, what do you want to do? I’m not sure what is going on with Millie but I suggest she be seen by you or the resident when you get a chance. Be silent and wait to hear what Dr. Aloha recommends first. I’m not sure what is going on with Millie but I suggest she be seen by you or the resident now. Do you need any tests/labs done? 50
 © Question # 9 Dr. Aloha tells you he is in his office seeing patients and feels it can wait until he sees his last patient (within the next hour or so). What would be your next 2 actions? 1. 2. 3. 4. Agree with him and tell the next shift Dr. Aloha will be in to see the patient after his office hours. Tell Dr. Aloha you are concerned for his patient and share that the patient may stop breathing soon. Inform him that you will be calling the resident to come stat. Comfort the patient, call RT and have them increase Millie’s O 2 flow to 6 liters nasal cannula. Obtain an ABG and order a stat portable Chest X-ray per our emergency protocol. 51
© Question # 9 Dr. Aloha tells you he is in his office seeing patients and feels it can wait until he sees his last patient (within the next hour or so). What would be your next 2 actions? 1. 2. 3. 4. Agree with him and tell the next shift Dr. Aloha will be in to see the patient after his office hours. Tell Dr. Aloha you are concerned for his patient and share that the patient may stop breathing soon. Inform him that you will be calling the resident to come stat. Comfort the patient, call RT and have them increase Millie’s O 2 flow to 6 liters nasal cannula. Obtain an ABG and order a stat portable Chest X-ray per our emergency protocol. 51
 Example # 4 RN to RN Handoff • Situation: I’d like to give you report on my patients so I can go to lunch. I plan to take only 20 minutes so I won’t give you all the details of each patient. • Background: I have 5 patients. Rooms 32, 33, 34, 35 and 36. • Assessment: All of them are “stable” and eating their lunch now. There is really nothing that can’t wait until I get back. Here’s my phone. Thanks. 15 Minutes after taking that “brief” report the CNA comes running down the hallway yelling that the patient in room 33 is blue and not breathing. You immediately call a code blue, get the code cart and start bagging the patient. The CRNA has intubated and the code team is there. Your break buddy, returning from lunch comes running into the room yelling “This patient is a full DNAR and specifically did not want to be intubated!” 52
Example # 4 RN to RN Handoff • Situation: I’d like to give you report on my patients so I can go to lunch. I plan to take only 20 minutes so I won’t give you all the details of each patient. • Background: I have 5 patients. Rooms 32, 33, 34, 35 and 36. • Assessment: All of them are “stable” and eating their lunch now. There is really nothing that can’t wait until I get back. Here’s my phone. Thanks. 15 Minutes after taking that “brief” report the CNA comes running down the hallway yelling that the patient in room 33 is blue and not breathing. You immediately call a code blue, get the code cart and start bagging the patient. The CRNA has intubated and the code team is there. Your break buddy, returning from lunch comes running into the room yelling “This patient is a full DNAR and specifically did not want to be intubated!” 52
 © Question # 10 SBAR was used in this unfortunate situation, what reasons lead to its failure? 1. 2. 3. 4. Not enough time was allocated to communicate important information. No time was allowed for the covering nurse to ask questions. Limitation of the exchange of info lead to unsafe patient care. Information such as patient status, diagnoses, medications, treatment and advanced directives was not passed along. a. b. c. d. 1, 3, 4 4 only All of the above 1, 2, 3 53
© Question # 10 SBAR was used in this unfortunate situation, what reasons lead to its failure? 1. 2. 3. 4. Not enough time was allocated to communicate important information. No time was allowed for the covering nurse to ask questions. Limitation of the exchange of info lead to unsafe patient care. Information such as patient status, diagnoses, medications, treatment and advanced directives was not passed along. a. b. c. d. 1, 3, 4 4 only All of the above 1, 2, 3 53
 54
54
 © References • Crum, Brenda S. (Dec 2006). Standardizing Hand-off Processes. AORNJ. 84 (6). AORN , Inc. • Haig, K. M. , Sutton, S. , & Whittington, J. (March 2006). SBAR: A Shared Mental Model for Improving Communication Between Clinicians. Joint Commission Journal of Quality and Patient Safety, 32(3). Retrieved October 3, 2007 from http: //www. jcipatientsafety. org/fpdf/psp/SBAR. pdf • Nagamine, J. , & Leonard, M. (July 2007). SBAR: The Role of Structured Communication in Preventing Harm. Web. Ex Conference sponsored by MPQH. July 23, 2007. • Pothier, D. ( November 2005) Pilot Study to Show the Loss of Important Data in Nursing Handover. British Journal of Nursing, 14, 1090 -1093. • Quality Insights of Penn, Contracted with CMS. SBAR: An opportunity to Improve Communication Within the Home Health Arena. HHQIOSC. • The Healthcare Compliance Company. (2007). SBAR Situation, Background, Assessment, Recommendation A Communication Handbook for All Staff. Marblehead, M. A. : HCPro. • The Joint Commission. (May 2007). Communication During Patient Hand-Overs. Patient Safety Solutions, 1 (3). Geneva, Switzerland 55
© References • Crum, Brenda S. (Dec 2006). Standardizing Hand-off Processes. AORNJ. 84 (6). AORN , Inc. • Haig, K. M. , Sutton, S. , & Whittington, J. (March 2006). SBAR: A Shared Mental Model for Improving Communication Between Clinicians. Joint Commission Journal of Quality and Patient Safety, 32(3). Retrieved October 3, 2007 from http: //www. jcipatientsafety. org/fpdf/psp/SBAR. pdf • Nagamine, J. , & Leonard, M. (July 2007). SBAR: The Role of Structured Communication in Preventing Harm. Web. Ex Conference sponsored by MPQH. July 23, 2007. • Pothier, D. ( November 2005) Pilot Study to Show the Loss of Important Data in Nursing Handover. British Journal of Nursing, 14, 1090 -1093. • Quality Insights of Penn, Contracted with CMS. SBAR: An opportunity to Improve Communication Within the Home Health Arena. HHQIOSC. • The Healthcare Compliance Company. (2007). SBAR Situation, Background, Assessment, Recommendation A Communication Handbook for All Staff. Marblehead, M. A. : HCPro. • The Joint Commission. (May 2007). Communication During Patient Hand-Overs. Patient Safety Solutions, 1 (3). Geneva, Switzerland 55
 © • • • Answers to Questions Question 1 Question 2 Question 3 Question 4 Question 5 Question 6 Question 7 Question 8 Question 9 Question 10 # # # # # 2 3 d 3 3 4 4 4 2, 4 c 56
© • • • Answers to Questions Question 1 Question 2 Question 3 Question 4 Question 5 Question 6 Question 7 Question 8 Question 9 Question 10 # # # # # 2 3 d 3 3 4 4 4 2, 4 c 56
 We hope you have enjoyed this learning module and wish that it has brought you to a better understanding of SBAR use in the acute clinical setting. We encourage you to share this with other nurses and personally use this format in all of your communications in the hope that patient safety will be enhanced. We would also like to acknowledge Mountain-Pacific Quality Health, the Quality Improvement Organization for Hawaii and the Pacific Territories for their assistance and information in their SBAR Communication Package. We only ask that you in some way give credit to The Queen’s Medical Center when you use this learning tool. © The Queen’s Medical Center 1301 Punchbowl Street Honolulu, HI 96813 57
We hope you have enjoyed this learning module and wish that it has brought you to a better understanding of SBAR use in the acute clinical setting. We encourage you to share this with other nurses and personally use this format in all of your communications in the hope that patient safety will be enhanced. We would also like to acknowledge Mountain-Pacific Quality Health, the Quality Improvement Organization for Hawaii and the Pacific Territories for their assistance and information in their SBAR Communication Package. We only ask that you in some way give credit to The Queen’s Medical Center when you use this learning tool. © The Queen’s Medical Center 1301 Punchbowl Street Honolulu, HI 96813 57


