073b3804c6a6ac57a14a3a8dd09b0894.ppt
- Количество слайдов: 47
 The Poisoned Patient Core Clerkship in Emergency Medicine University of Colorado at Denver Health Sciences Center
The Poisoned Patient Core Clerkship in Emergency Medicine University of Colorado at Denver Health Sciences Center
 Objectives Apply general emergency medicine management principles to the poisoned patient n Review basic pharmacology and toxicology of common poisons n Utilize clues from the history, physical exam, and diagnostics to identify the poisons involved n
Objectives Apply general emergency medicine management principles to the poisoned patient n Review basic pharmacology and toxicology of common poisons n Utilize clues from the history, physical exam, and diagnostics to identify the poisons involved n
 First principle in poisoning management Sick or not sick? n Poisoned patients can present with a broad spectrum of illness n If sick, start treatment n Resuscitation is always the first stepremember your ABCs n
First principle in poisoning management Sick or not sick? n Poisoned patients can present with a broad spectrum of illness n If sick, start treatment n Resuscitation is always the first stepremember your ABCs n
 General principles of emergency management Resuscitation/Stabilization n Evaluation n Rule out the life-threats n Identify what you can n n Symptomatic care/monitoring Prevention of deterioration n Treat symptoms n Antidotes n
General principles of emergency management Resuscitation/Stabilization n Evaluation n Rule out the life-threats n Identify what you can n n Symptomatic care/monitoring Prevention of deterioration n Treat symptoms n Antidotes n
 Case – Altered Mental Status
Case – Altered Mental Status
 EMS Report n n n “This is a 57 yo male. We were called to his house by his son, who found him confused. The son is on the way here. “On our arrival, we found a somnolent male who is not able to answer questions, is mildly diaphoretic, and had BP 135/75, HR 100, RR 32, and oxygen sat of 99% on room air. We have a 16 gauge IV in the left AC. Dstick was 95. “Any questions for us before we leave? ”
EMS Report n n n “This is a 57 yo male. We were called to his house by his son, who found him confused. The son is on the way here. “On our arrival, we found a somnolent male who is not able to answer questions, is mildly diaphoretic, and had BP 135/75, HR 100, RR 32, and oxygen sat of 99% on room air. We have a 16 gauge IV in the left AC. Dstick was 95. “Any questions for us before we leave? ”
 EMS Report House was clean, no signs of an assault, etc. n No drug paraphernalia around n No medicalert bracelet or necklace n No open pill bottles near patient n Patient was found 5 ft from the bottom of a staircase n
EMS Report House was clean, no signs of an assault, etc. n No drug paraphernalia around n No medicalert bracelet or necklace n No open pill bottles near patient n Patient was found 5 ft from the bottom of a staircase n
 The patient’s son arrives… What would you like to ask his son?
The patient’s son arrives… What would you like to ask his son?
 His son tells you… He talked to his dad yesterday, seemed normal n No significant PMH n PSHX: gallbladder taken out about 10 years ago n No medications except for something he occasionally takes for a “stomach flu bug” n SH: smoker : 40 pack/year hx, occasional social drinker n Wife died of cancer about a month ago—dad took her death “very hard” n
His son tells you… He talked to his dad yesterday, seemed normal n No significant PMH n PSHX: gallbladder taken out about 10 years ago n No medications except for something he occasionally takes for a “stomach flu bug” n SH: smoker : 40 pack/year hx, occasional social drinker n Wife died of cancer about a month ago—dad took her death “very hard” n
 Physical Exam n n n n n Vitals – T 38. 2; BP 134/78; Pulse 102; RR 30; Sa. O 2 98% on RA Gen: Confused, drowsy Skin: moist and flushed, no lesions, no cyanosis Pupils: mid position (not constricted or dilated) and reactive CV: tachy RR, no murmur/rubs/gallops Lungs: CTA bilaterally Bowel sounds: present No evidence of trauma, neck is not stiff Neuro: otherwise nonfocal
Physical Exam n n n n n Vitals – T 38. 2; BP 134/78; Pulse 102; RR 30; Sa. O 2 98% on RA Gen: Confused, drowsy Skin: moist and flushed, no lesions, no cyanosis Pupils: mid position (not constricted or dilated) and reactive CV: tachy RR, no murmur/rubs/gallops Lungs: CTA bilaterally Bowel sounds: present No evidence of trauma, neck is not stiff Neuro: otherwise nonfocal
 Sick or not sick?
Sick or not sick?
 Sick or not sick Sick but stable n No immediate airway, breathing or circulation interventions required n But altered mental status may be due to a lifethreatening condition that requires prompt intervention n
Sick or not sick Sick but stable n No immediate airway, breathing or circulation interventions required n But altered mental status may be due to a lifethreatening condition that requires prompt intervention n
 What’s our differential diagnosis for this patient?
What’s our differential diagnosis for this patient?
 Broad Differential Diagnoses Neurologic n Malignant n Endocrine n Infection n Trauma n Toxicologic n
Broad Differential Diagnoses Neurologic n Malignant n Endocrine n Infection n Trauma n Toxicologic n
 Altered Mental Status n Four life-threatening causes that require immediate treatment Hypoxia (ruled out by normal pulse ox) n Hypotension/severe hypertension (ruled out by normal BP) n Herniation of the brainstem (ruled out by non-focal neurological exam) n Hypoglycemia (needs to be evaluated in every patient with altered mental status) n
Altered Mental Status n Four life-threatening causes that require immediate treatment Hypoxia (ruled out by normal pulse ox) n Hypotension/severe hypertension (ruled out by normal BP) n Herniation of the brainstem (ruled out by non-focal neurological exam) n Hypoglycemia (needs to be evaluated in every patient with altered mental status) n
 Get the best history possible Often unreliable or unobtainable from patient n Rely on EMS, bystanders, family members and other physicians n Psychiatric files n Obtain bottles/medications from home n n Any missing pills, amount, time of ingestion Environmental setting n Check pockets, bags, belongings n
Get the best history possible Often unreliable or unobtainable from patient n Rely on EMS, bystanders, family members and other physicians n Psychiatric files n Obtain bottles/medications from home n n Any missing pills, amount, time of ingestion Environmental setting n Check pockets, bags, belongings n
 Physical Exam n Thorough exam looking for clues: Toxidromes- constellation of signs and symptoms of a particular poison n In the ED we always look for the “classic” presentation n n Also look for signs of non-toxicologic causes: n Evidence of trauma, infection, metabolic or neurological causes, etc.
Physical Exam n Thorough exam looking for clues: Toxidromes- constellation of signs and symptoms of a particular poison n In the ED we always look for the “classic” presentation n n Also look for signs of non-toxicologic causes: n Evidence of trauma, infection, metabolic or neurological causes, etc.
 Common Toxidromes Sympathomimetics n Anti-cholinergics n Cholinergics n Sedatives n Opiates n
Common Toxidromes Sympathomimetics n Anti-cholinergics n Cholinergics n Sedatives n Opiates n
 Sympathomimetics n Cocaine, Amphetamines, PCP Hypertension n Tachycardia n Diaphoresis n Mydriasis n Agitation n n Does this sound like our guy?
Sympathomimetics n Cocaine, Amphetamines, PCP Hypertension n Tachycardia n Diaphoresis n Mydriasis n Agitation n n Does this sound like our guy?
 Anticholinergics n Antihistamines, some plants, side effect of many drugs n n n n n Tachycardia Hyperthermia Dry skin Mydriasis Decreased bowel sounds Urinary retention Delirium, agitation Hot as a hare, Dry as a bone, Red as a beet, Mad as a hatter, Blind as a bat. Does this sound like our guy?
Anticholinergics n Antihistamines, some plants, side effect of many drugs n n n n n Tachycardia Hyperthermia Dry skin Mydriasis Decreased bowel sounds Urinary retention Delirium, agitation Hot as a hare, Dry as a bone, Red as a beet, Mad as a hatter, Blind as a bat. Does this sound like our guy?
 Cholinergics n Organophosphates, Carbamates, Nerve agents n Effects both muscarinic and nicotinic receptors Muscarinic effects n n n n S- SALIVATION, SEIZURE L- LACRIMATION U- URINATION G- GI DISTRESS (diarrhea & vomiting) B- BRONCHORRHEA A- ABDOMINAL CRAMPS M- MIOSIS
Cholinergics n Organophosphates, Carbamates, Nerve agents n Effects both muscarinic and nicotinic receptors Muscarinic effects n n n n S- SALIVATION, SEIZURE L- LACRIMATION U- URINATION G- GI DISTRESS (diarrhea & vomiting) B- BRONCHORRHEA A- ABDOMINAL CRAMPS M- MIOSIS
 Cholinergics n Nicotinic effects - MTWTh. F M-Mydriasis n T-Tachycardia n W-Weakness n TH-Hyperthermia n F-Fasciculations n n Does this sound like our guy?
Cholinergics n Nicotinic effects - MTWTh. F M-Mydriasis n T-Tachycardia n W-Weakness n TH-Hyperthermia n F-Fasciculations n n Does this sound like our guy?
 Opiates, Clonidine Miosis n Hypotension n Bradypnea n Bradycardia n Hypothermia n CNS Depression n Does this look like our guy?
Opiates, Clonidine Miosis n Hypotension n Bradypnea n Bradycardia n Hypothermia n CNS Depression n Does this look like our guy?
 Sedatives Benzodiazepines, GHB “Coma with normal vital signs” CNS Depression n Normotensive n Mild bradypnea or normal RR n n Does this look like our guy?
Sedatives Benzodiazepines, GHB “Coma with normal vital signs” CNS Depression n Normotensive n Mild bradypnea or normal RR n n Does this look like our guy?
 Toxins and Vital Signs n n n n Hyperthermia - aspirin, cocaine, anticholinergics Hypothermia - opioids, sedatives Hypertension - stimulants, tricyclics, antihistamines Hypotension - blood pressure medications, opioids Tachycardia - stimulants, vasodilators, anticholinergics Bradycardia - beta-blockers, Ca Ch blockers, clonidine, digoxin Tachypnea- aspirin, amphetamines, CO Bradypnea- narcotics, clonidine, ETOH
Toxins and Vital Signs n n n n Hyperthermia - aspirin, cocaine, anticholinergics Hypothermia - opioids, sedatives Hypertension - stimulants, tricyclics, antihistamines Hypotension - blood pressure medications, opioids Tachycardia - stimulants, vasodilators, anticholinergics Bradycardia - beta-blockers, Ca Ch blockers, clonidine, digoxin Tachypnea- aspirin, amphetamines, CO Bradypnea- narcotics, clonidine, ETOH
 Assessment The history suggests an overdose, but we don’t know what n The physical exam is non-specific n No common toxidrome to suggest a diagnosis n Nothing to strongly suggest another cause n n Time to gather more data….
Assessment The history suggests an overdose, but we don’t know what n The physical exam is non-specific n No common toxidrome to suggest a diagnosis n Nothing to strongly suggest another cause n n Time to gather more data….
 Diagnostic Testing What diagnostics might be helpful in this case?
Diagnostic Testing What diagnostics might be helpful in this case?
 Diagnostics n General lab testing Serum chemistry, blood gas to identify metabolic abnormalities n CBC, UA, CSF analysis to identify infection n Drug/alcohol screen to identify common drugs of abuse n n Specific lab testing n Some poisons require specific testing
Diagnostics n General lab testing Serum chemistry, blood gas to identify metabolic abnormalities n CBC, UA, CSF analysis to identify infection n Drug/alcohol screen to identify common drugs of abuse n n Specific lab testing n Some poisons require specific testing
 Labs Na 135 K 3. 5 Cl 100 HCO 3 15 Glucose 120 BUN 25 Cr 1. 0 n ABG 7. 50/15/90/16/-12 n Et. OH undetectable n Urine drug screen negative for drugs of abuse n ECG – sinus tachycardia n Head CT – negative n CXR - normal n
Labs Na 135 K 3. 5 Cl 100 HCO 3 15 Glucose 120 BUN 25 Cr 1. 0 n ABG 7. 50/15/90/16/-12 n Et. OH undetectable n Urine drug screen negative for drugs of abuse n ECG – sinus tachycardia n Head CT – negative n CXR - normal n
 What is your assessment now? What is the acid/base disturbance? n What is the differential for this acid/base disturbance? n Is this consistent with a common overdose? n How can we assess this problem? n Was the ECG, head CT, and CXR helpful? n
What is your assessment now? What is the acid/base disturbance? n What is the differential for this acid/base disturbance? n Is this consistent with a common overdose? n How can we assess this problem? n Was the ECG, head CT, and CXR helpful? n
 Salicylism (Aspirin Poisoning) n Respiratory alkalosis n Direct stimulation of respiratory centers n Tachypnea n Metabolic acidosis Aspirin is salicylic acid n Causes lactic acidosis by uncoupling oxidative phosphorylation n Causes ketosis by stimulating lipid metabolism n n Confusion/cerebral edema
Salicylism (Aspirin Poisoning) n Respiratory alkalosis n Direct stimulation of respiratory centers n Tachypnea n Metabolic acidosis Aspirin is salicylic acid n Causes lactic acidosis by uncoupling oxidative phosphorylation n Causes ketosis by stimulating lipid metabolism n n Confusion/cerebral edema
 Evaluation In most poisonings, symptoms do not correlate well with serum drug levels, so levels are not useful n Acute salicylate ingestion is one case where symptoms DO correlate with levels n Therapeutic is up to 30 mg/dl n This patient’s level was 75 mg/dl n
Evaluation In most poisonings, symptoms do not correlate well with serum drug levels, so levels are not useful n Acute salicylate ingestion is one case where symptoms DO correlate with levels n Therapeutic is up to 30 mg/dl n This patient’s level was 75 mg/dl n
 Poisoning Management n Supportive and symptomatic care required for all poisonings
Poisoning Management n Supportive and symptomatic care required for all poisonings
 Treating Common Poisoning Symptoms Symptom Treatment None Observation Hypoglycemia Glucose Somnolence/coma Intubation Agitation/seizures Sedatives (benzodiazepines) Hypotension Fluids/adrenergic pressors Cardiac arrhythmia Sodium bicarbonate, calcium, anti-dysrhythmics, pacing Vomiting Anti-emetics, IVF
Treating Common Poisoning Symptoms Symptom Treatment None Observation Hypoglycemia Glucose Somnolence/coma Intubation Agitation/seizures Sedatives (benzodiazepines) Hypotension Fluids/adrenergic pressors Cardiac arrhythmia Sodium bicarbonate, calcium, anti-dysrhythmics, pacing Vomiting Anti-emetics, IVF
 Poisoning Management Antidotal therapies are needed for only a few poisons. (Consult your EM book for detailed listings. ) n Consider GI decontamination n n Removal of drug or decrease absorption from GI tract
Poisoning Management Antidotal therapies are needed for only a few poisons. (Consult your EM book for detailed listings. ) n Consider GI decontamination n n Removal of drug or decrease absorption from GI tract
 GI Decontamination n Ipecac syrup n n No longer recommended for poisonings Activated charcoal Binds to most medications and potentially decreases GI absorption n Potentially useful within 1 hour of ingestion but no evidence of improved clinical outcomes n Aspiration is uncommon unless given by an NG tube or in patient with altered mental status n
GI Decontamination n Ipecac syrup n n No longer recommended for poisonings Activated charcoal Binds to most medications and potentially decreases GI absorption n Potentially useful within 1 hour of ingestion but no evidence of improved clinical outcomes n Aspiration is uncommon unless given by an NG tube or in patient with altered mental status n
 GI Decontamination n Gastric Lavage Insertion of large orogastric tube into the stomach and lavaging with several liters of fluid n Potentially useful in life threatening ingestions < 1 hour n Aspiration occurs in around 5% of patients n
GI Decontamination n Gastric Lavage Insertion of large orogastric tube into the stomach and lavaging with several liters of fluid n Potentially useful in life threatening ingestions < 1 hour n Aspiration occurs in around 5% of patients n
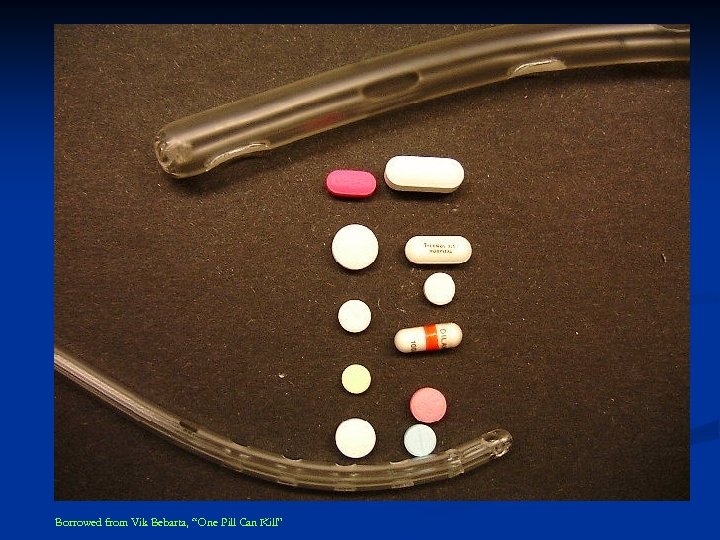 Borrowed from Vik Bebarta, “One Pill Can Kill”
Borrowed from Vik Bebarta, “One Pill Can Kill”
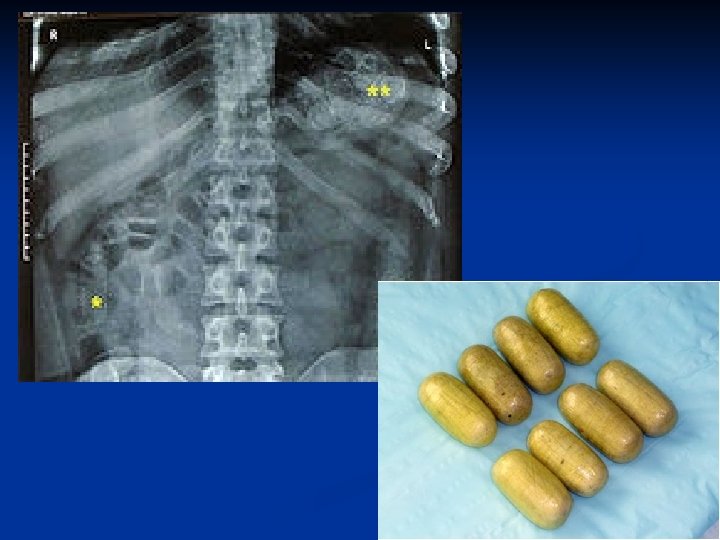
 GI Decontamination n Whole Bowel Irrigation Decreases GI transit time using PEG n Useful in life threatening ingestions when other methods not helpful n
GI Decontamination n Whole Bowel Irrigation Decreases GI transit time using PEG n Useful in life threatening ingestions when other methods not helpful n
 GI Decontamination Would GI decontamination be useful in this patient? n Do you think that this patient has more drug in the GI tract? n
GI Decontamination Would GI decontamination be useful in this patient? n Do you think that this patient has more drug in the GI tract? n
 GI Decontamination He has a high salicylate level n He has been “confused for a couple of hours” n Probably not much drug left in the GI tract n
GI Decontamination He has a high salicylate level n He has been “confused for a couple of hours” n Probably not much drug left in the GI tract n
 Specific Treatments Very few poisons require specific treatments such as: Dialysis n Diuresis n Chelation n Cardiac pacing n
Specific Treatments Very few poisons require specific treatments such as: Dialysis n Diuresis n Chelation n Cardiac pacing n
 Salicylism - Treatment n Salicylate poisoning has a specific treatment n Alkaline diuresis – increase in urine p. H favors movement of salicylate ion into urine n Dialysis for severe cases Is this patient sick enough to get dialysis?
Salicylism - Treatment n Salicylate poisoning has a specific treatment n Alkaline diuresis – increase in urine p. H favors movement of salicylate ion into urine n Dialysis for severe cases Is this patient sick enough to get dialysis?
 Non-Toxic Ingestions (Small amounts) n n n n Household bleach Cigarettes (<3) Cosmetics Glues/paste Hydrogen peroxide (medicinal) Matches Paint (indoor, latex) n n n n Shampoos, lotions Rat poison Detergents Chalk Laxatives Ink Antibiotics Antacids
Non-Toxic Ingestions (Small amounts) n n n n Household bleach Cigarettes (<3) Cosmetics Glues/paste Hydrogen peroxide (medicinal) Matches Paint (indoor, latex) n n n n Shampoos, lotions Rat poison Detergents Chalk Laxatives Ink Antibiotics Antacids
 Summary Always start with the ABCs n Target your history and physical for clues to the diagnosis n Labs and other testing may be useful n Most poisons only require supportive care n If you have questions call the Rocky Mountain Poison Center n
Summary Always start with the ABCs n Target your history and physical for clues to the diagnosis n Labs and other testing may be useful n Most poisons only require supportive care n If you have questions call the Rocky Mountain Poison Center n



