4311045e40cff7e0f89f6cb62ed79397.ppt
- Количество слайдов: 114

The Management of the children with spastic Cerebral Palsy: Adjuncts to Physiotherapy Intervention Robyn Smith Department of Physiotherapy UFS 2012

Spasticity : a complex problem • Spasticity is a complex problem and can have a significant influence on: – a child’s quality of life, – negatively impact the rehabilitation process, – achievement of functional goals • In some cases however a child may use spasticity for function

What is spasticity? • Spasticity is a physiological consequence of damage to the central nervous system or spinal cord • Overactive stretch reflex

How to we measure spasticity objectively • Objective Scales available: – – Ashworth scale Modified Ashworth (Scale 1 -5) Tardieu (includes some neurological aspects, speed of PM) PENN spasm scale: self report on f, severity ? Reliable and valid ? Effect of velocity on spasticity Scales do not look at the effect of spasticity on function

Ineffective management of spasticity The impact of spasticity can be devastating if not managed early and appropriately it can result in: – – – muscle contractures, severe postural and/or limb deformities , pressure sores which may even, make basic nursing care a challenge, Pain resulting from spasticity is also a significant concern.

Aggravation of spasticity • Spasticity may be aggravated by factors such as: – emotional distress – illness – hypothermia – poor positioning – Pressure sores

The effective management of spasticity is fundamental in the successful management of neurological disabilities and the prevention of secondary complications.

Physiotherapy remains the most common first line treatment option for patients with spasticity

Physiotherapy in the management of spasticty Physiotherapists make use of : • • physical activities tone influencing techniques and/or positions, passive movements, muscle stretching, orthotics and serial casting, therapeutic standing, hydrotherapy, electrotherapeutic modalities such as (TENS) and Functional Electrical Stimualtion (FESS)

Dealing with severe spasticity in a child with neurological dysfunction a huge problem especially when it limits functional abilities.

? If physiotherapy is not in itself effective enough to manage/ influence the child’s tone, What alternative therapies are available?

Alternative Management strategies for spasticity Pharmacological treatments Intramuscular agents • BOTOX (Bo. NT) • Intrathecal Baclofen • Oral agents e. g. benzodiazepines and baclofen Injectable agents/nerve blocks • Phenol Neuro. Surgical intervention • Selective Dorsal Rhizotomy (SDR) • Orthopaedic surgery • Tendon transfer • Osteotomy

Pharmaceutical Agents

Oral medications

Oral Baclofen • • • Muscle relaxant and antispasmodic agent Can also be used Not always available in public sector Not specific Results in a general decrease in muscle tone

Valium /Diazepam (Benzodiazepine) • Can also be used as a last resort to relieve spasticity • Antipsychotic agent with muscle relaxation properties • Not a drug of choice to manage spasticity • CNS suppression –resulting in drowsiness, over-sedation, respiratory function impairment. • Cannot then continue with therapy as child is often non responsive and drowsy

Intrathecal Baclofen
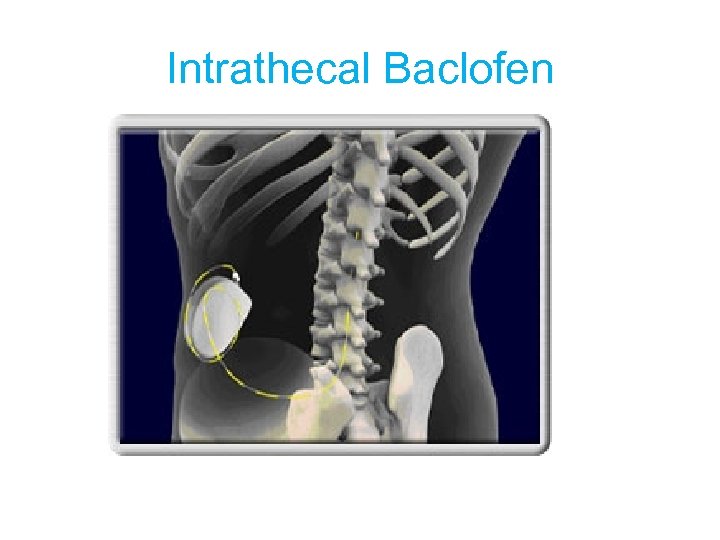
Intrathecal Baclofen

Intrathecal Baclofen • Use of implantable, programmable pump • To deliver precise amounts of Baclofen directly to the site of action at the spinal cord via the CSF • Precise action of Baclofen as a muscle relaxant and antispasmodic agent is not fully understood. • Baclofen inhibits both monosynaptic and polysynaptic reflexes at the spinal level.

Negative aspects of using a intrathecal Baclofen pump • Side effects – Dislodging – mechanical malfunctioning of the pump – Infection • Should not suddenly be discontinued as the patient will go into withdrawal.

Intrathecal Baclofen • • Expensive Central nervous system effects Used with good success in Europe Not currently available as a treatment option in in SA

Intramuscular agents: BOTOX

BOTOX

BOTOX • = Bo. NT • Botilium type A toxin (BOTOX) is a poison that is injected in small amounts locally • into a specific spastic muscle • used to reduce spasticity • No benefit if muscle is already contractured • Not licensed to be used in children under 2 years. • Has been used very successfully in hemiplegic, and diplegic children

BOTOX • • • Effect is temporary and lasts for 3 -4 months Expensive (R 2000 -4000/injection) Repeated administration is often required Not available on code for public sector patients Safety ? FDA has it under investigation has resulted in deaths in adults when used in high doses causing inability to swallow and respiratory failure • Needs to be administered by an experienced paediatrician/neurologist
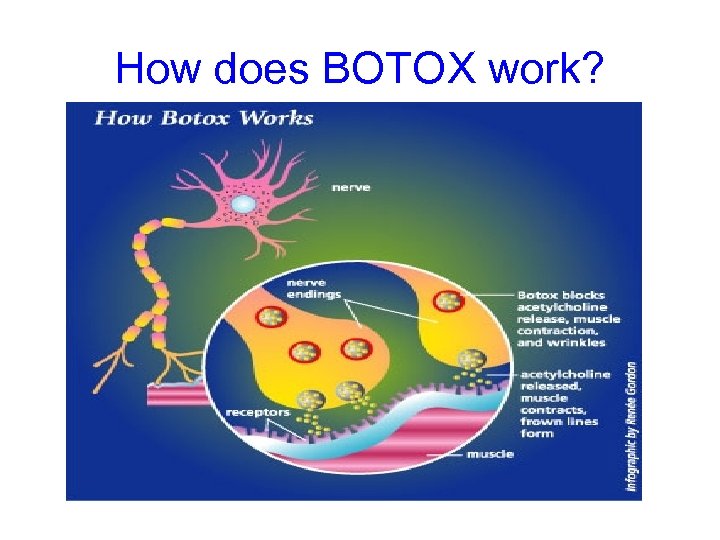
How does BOTOX work?

Benefit of using BOTOX (Bo. NT) • Effect temporary/reversible • Can be used before something more permanent such as surgery is considered • Injections however need to be followed up with intensive physiotherapy and appropriate orthoses

Surgical Intervention: Selective Dorsal Rhizotomy

Selective dorsal rhizotomy (SDR) What is SDR? • “Myelonotomy” • Is a neurosurgical procedure where the dorsal nerve roots are severed • Used management of spasticity • Mainly in case spastic diplegic child • Permanent effect or relief of spasticity
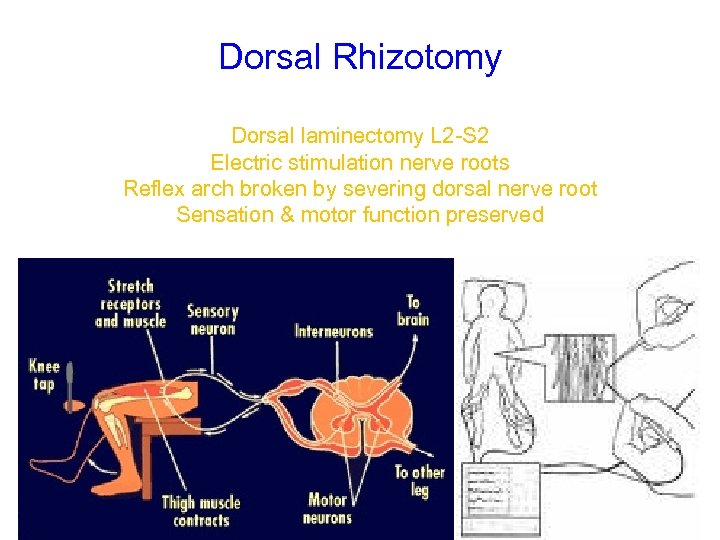
Dorsal Rhizotomy Dorsal laminectomy L 2 -S 2 Electric stimulation nerve roots Reflex arch broken by severing dorsal nerve root Sensation & motor function preserved

Important to assess if the child spasticity useful or harmful? • Harmful : impedes function • Useful: aids in antigravity movement and functioning Consideration is that if spasticity is useful removing the child’s spasticity via a SDR may result in deterioration of function

Considerations before doing SDR: • Main problem must be spasticity • Adequate underlying muscle strength (lower limbs, pelvis and trunk) • Child must have received intensive surgery for at least 2 years prior to the surgery • Family and child must be motivated • Cognitive ability of the child to participate actively in intensive rehabilitation programme Surgery best between 6 -8 years of age (but no age limit)

Considerations before doing SDR: • Will not prevent hip dislocations due to poor biomechanics Need to reconsider in the following cases: • Previous orthopaedic surgery. Usually decide to do SDR. Orthopaedic surgery then only done afterwards if indicated to correct remaining shortenings or deformities. • Contractures or spinal deformities present ? Orthopaedic surgery first

Physiotherapy Assessment before SDR • NB!!! • Evaluate child’s underlying muscle strength in trunk and legs • Evaluate functional activities – – sitting up from supine standing up from chair Walking running. • Functional abilities and potential • Computerised/video gait analysis widely now used to measure before and after changes (objective measure)
Complications SDR Early: • Dysasthesia (loss sensation) • CSF leak (severe spinal headache) • Neurogenic bladder Late: • Back pain • Spondilolisthesis Complications in the case of a competent neurosurgeon are however very rare

Post operative management • Strict bed rest 5 days Precautionary measures: • • No passive or active trunk rotation 4/52 No lumber flexion 4 -6/52 70 ◦ degrees hip flexion 4 -6/52 Intensive physiotherapy essential after surgery once child can mobilize more freely

Otherapy intervention for motor problems related to neurological pathology and spasticity • Orthopaedic surgery • Hyperbaric Oxygen Therapy (HBOT) • Constraint Induced Therapy (CIT) • Compression Suit therapy • Static weight bearing therapy • Strength training • Orthoses and assistive devices • Hippotherapy • Virtual Reality Training (VRT) :

Other Management Approaches

Orthopaedic Surgery

Why consult an Orthopaedic surgeon? SPASTICITY • Often severe spasticity, poor biomechanics and muscle imbalances lead to contracturing of the soft tissue and muscles • Can also lead to postural and joint deformities. • Contractures can and do limit function • Especially limiting in terms of mobility in diplegic and hemiplegic patients.

Why consult an Orthopaedic surgeon? • Severe spastic quadruplegic patients adductor muscle contracturing can make nursing care difficult e. g. bathing, dressing, changing diaper • Muscles most often effected in the LL are: – m. iliopsoas – m. Hamstrings – m. adductors – m. Gastrognemius and souleus (TA)

Why consult an Orthopaedic surgeon? • Muscles most often effected in the UL are: – m. biceps brachii – m. long flexors over the wrist and fingers – m. flexor pollicis brevis, longus and opponens pollicis at the thumb

Soft Tissue Releases

Soft Tissue Releases • Before sending child for surgery: – Evaluate underlying muscle length (shortening vs. contracture) and which specific joints are affected – Evaluate underlying muscle strength carefully – Evaluate how tone influences function – Evaluate the child’s functional abilities and potential • Physiotherapists input essential prior to surgery to ensure optimal functional outcome post operatively

• Z-plasty for lengthening of shortened/contractured muscle • “Full house” release is when in the LL they release: – – m. iliopsoas, M. adductors magnus Hamstrings TA • ? ? ? Often too aggressive and results in “over-releasing with subsequent: – Loss of function – Joint hyper-mobility – Loss muscle tone

Soft Tissue Releases • Usually only done after 5 years of age – Make sure that procedure does not have to be repeated over and over again at short intervals • Releases of arm contractures not often done and not very successful • Post operative intensive physiotherapy must be available

Physiotherapy after Soft Tissue Releases • POP spika with cross bar for 6/52 • S Therapeutic standing commenced from day 2 • Stretch m. iliopsoas in standing/prone lying • Positioning: – no pillow under legs – Lie in prone least 30 min. /day – No extended periods sitting • Keep POP dry and clean • Daily therapeutic standing until POP removed
Physiotherapy after Soft Tissue Releases Once the POP removed 6 weeks: • KAFO(knee and ankle foot orthosis)/AFO (ankle foot orthosis) worn 3 months full time • Intensive physiotherapy (remove KAFO/AFO if needed during therapy) • Sleep with KAFO/AFO 6 months to prevent shortening of the lengthened muscles • Include a ROM and stretching programme
Rehabilitation following Soft tissue surgery

Muscle or Tendon Transfers

Muscle or Tendon Transfers • Careful selection for procedure • Tendon or muscle transfers can be done in cases where it may result in improved function • UL and LL transfers are done • Followed up by intensive physiotherapy, reeducate the muscles new function
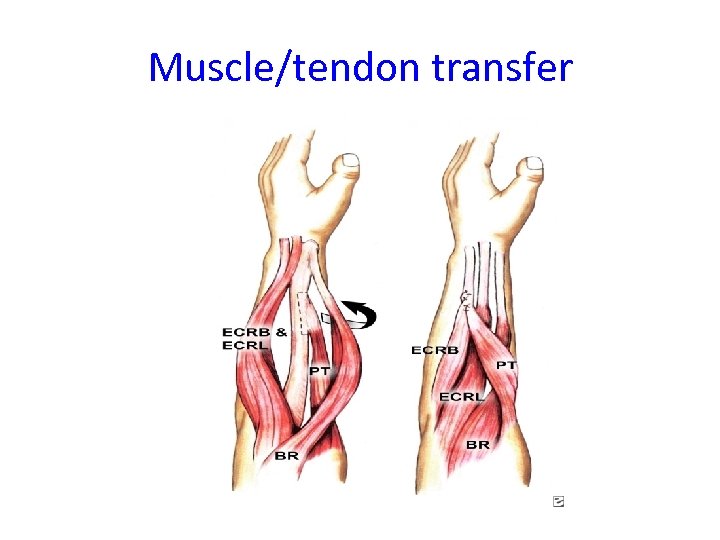
Muscle/tendon transfer

Other orthopaedic surgery

Hip Dislocations

Why consult an Orthopaedic surgeon? HIP DISLOCATION: • Severe spasticity/hypotonicity and constant abnormal biomechanics do result in dislocations • Posterior dislocation more common, anterior dislocation can also occur • Important to remember that the acetabulum does not develop its normal shape and depth in children that do not weightbear – contributing further to the risk of dislocation

Why consult an Orthopaedic surgeon? HIP DISLOCATION: • Common in severe spastic quadruplegia – posterior dislocation due to spastic pattern • Can contribute to o severe postural deformities as well

Orthopaedic management of hip dislocations • Femoral osteotomy is done to: – relieve pain – and to aid nursing care – improve posture – Improve function • At times arthroplasty may also be done.
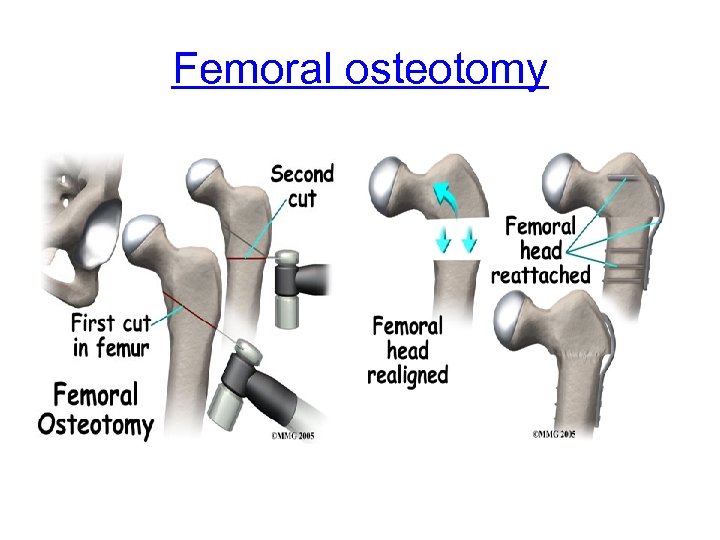
Femoral osteotomy
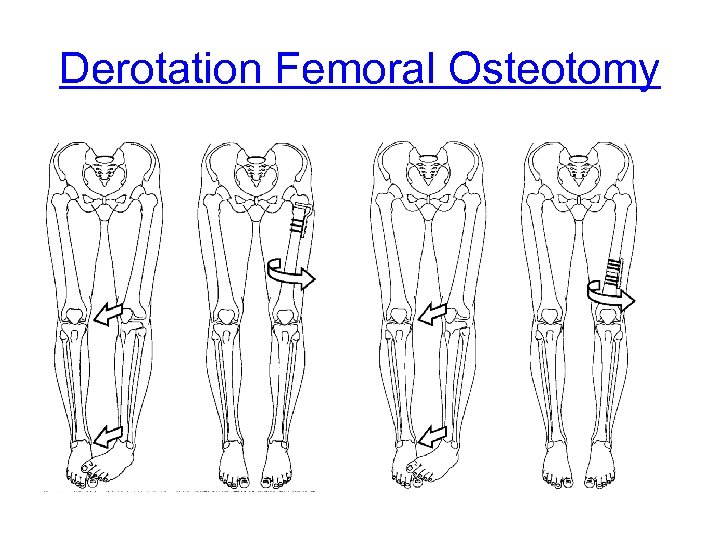
Derotation Femoral Osteotomy

Physiotherapy following a femoral osteotomy • Rehabilitation commences on day 2 • May be in a spika (same STR) • Mobilisation for ROM • Can start weightbearing mobilisation as pain allows • Arthoplasty of the hip NWB for up to 6 weeks

Foot Abnormalities

Club-foot Deformities
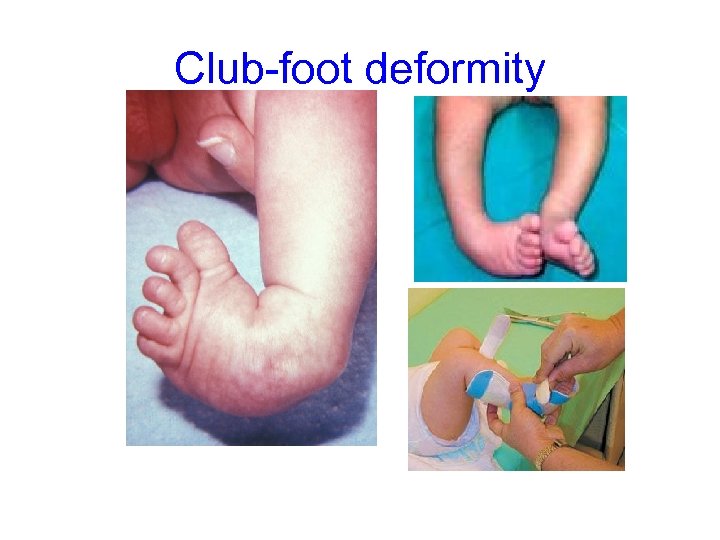
Club-foot deformity

Club-foot deformity • “Tallipes equinovarus” • Causes often unknown • Club foot causes may be iodiopathic or arise in conjunction with other neuromuscular deformities. • Deformity is structural and is fixed or rigid requires may require surgery depending on degree. • A positional clubfoot occurs when an otherwise normal foot is held in a deformed position in utero.

Management of a Club–foot deformity Positional Clubfoot Management commences 2 -3 days after birth • POP –repeat weekly • Strapping/ splinting –every few days • Until correct positioning attained • Orthoses may be useful

Management of a Club–foot deformity Structural Clubfoot • Management started as soon as is possible. • Ponseti method – manipulation funder anaesthesia, followed by POP – Dennis Brown boots to be worn 6 -12 months. – Careful not cause Rocker-bottom foot (mid foot fracture).

Dennis Brown Boot

Management of a Club–foot deformity • When conservative management fails The club foot will require surgical management: – Child Younger 5 years only soft tissue surgery. Best results at 3 -4 months of age. – Older 5 years also often also involves bony reconstruction of the foo • Surgery followed by POP 6 weeks • FWB mobilization in POP/boot • Orthotics once POP removed • 25 % chance of reoccurrence

Management of a other common foot deformities
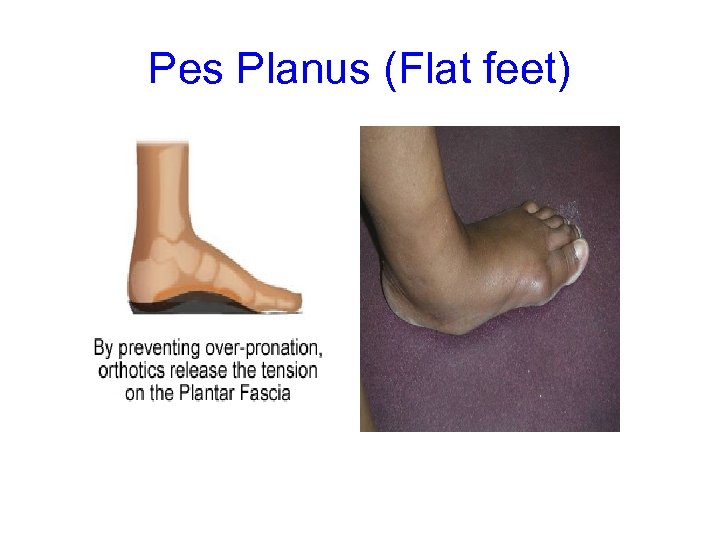
Pes Planus (Flat feet)

Pes Planus (Flat feet) • All babies' feet look flat because an arch hasn't formed yet. – Arches only start to form once the child is weight bearing; – and the intrinsic foot muscles are activated. – Foot arches should form by the time child is 2 or 3 years old. • In CP children flat feet may be caused by: – hypotonia, – spastic everters – biomechanical issues of the LL
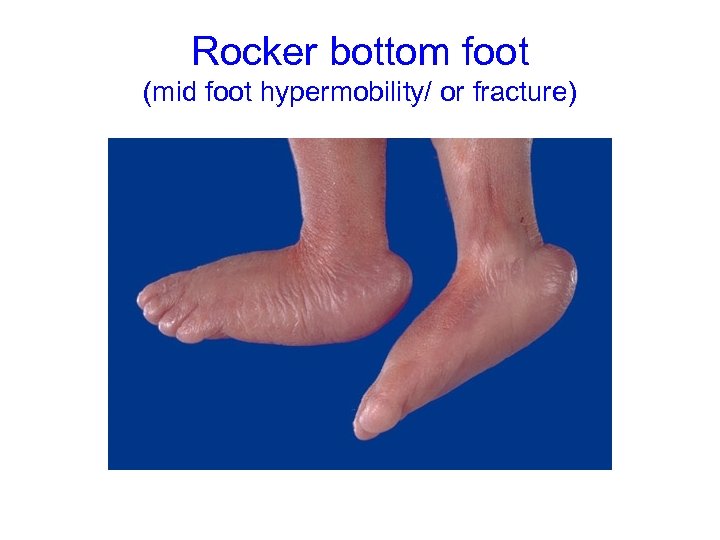
Rocker bottom foot (mid foot hypermobility/ or fracture)

Types of foot deformities common in children with CP? • Equinous foot (downwards) • Equinovarus foot (down and in) • Equinovalgus foot (down and out)

When to refer to orthopaedic surgeon? • Earliest age possible !!! • As soon as abnormalities are observed, severe spasticity is noted and shortening has started so that the orthopaedic surgeon can follow up the child regularly at his clinic until surgery is deemed necessary • Usually do not operate before 3 -4 years of age • Must give corrective foot wear and orthotics on e. g. inner soles, AFO, orthopaedic boots to limit deformities as far as soon as is possible
Physiotherapy after foot surgery Mobilisation post-operatively: • Child to mobilize FWB with below knee POP cast 6/52 • Foot surgery often combined with TA lengthening • Appropriate orthotics • Continued rehabilitation

The Toolbox. . alternative therapy approaches

Hyperbaric Oxygen Therapy

Hyperbaric Oxygen Therapy (HBOT) What is HBOT? • 100% Oxygen administered at a controlled pressure using a hyperbaric chamber • The use is HBOT remains controversial • Has been used in management of children with CP, traumatic and anoxic brain injuries

Hyperbaric Oxygen Chambers

Suggested benefits HBOT • • Hyper-oxygenation Neurovascularization Vasoconstriction Antibacterial activity

How is HBOT supposed to work ? • Brain injuries result in neuronal death • Also forms “ idling” neurons suggesting recoverable brain tissue • HBOT postulated to re-activate “idling” neurons • Suggest more beneficial when done shortly after neuronal injury (CP? ? ? vs. hypoxic or traumatic brain injury)

What do I tell a parent who wants to try it ? • Current research about HBOT efficacy in the management of neuronal injury is inconclusive Research studies results are very contradictive. • Not widely used any more as adjunct to therapy. Not as fashionable any more. • Expensive (R 150 - 350/per session, and several sessions in a course).

Constraint Induced Therapy
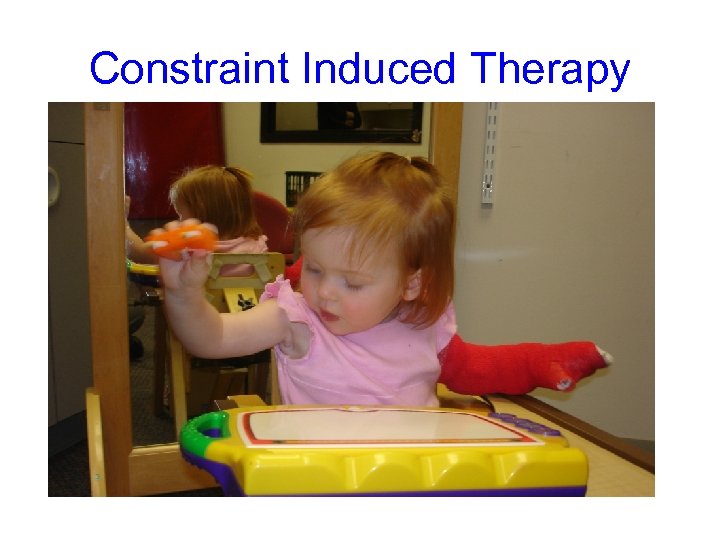
Constraint Induced Therapy

Constraint induced therapy (CIT) • Used in hemiplegia and assymetircal diplegia • Involves the physical constraint of the unaffected upper limb • Aim is to improve awareness of , and the physical activity and function of the affected arm and hand • Based on the learn- not use concept • Combined with intensive PT/OT

What do I tell a parent who wants to try it ? • Definitely give it a try ! • Use a bandage/immobi-sling/neoprene splint • Labour intensive for parent/therapist got to be followed up with task or goal directed activity for hand • Have been some controlled clinical trial done on CIT • Research results have been promising – research has shown improved use of the arm and hand to lesser extent • More clinical trial research indicated • Concerns : Often difficult to implement with a child with little active use of arm or even in cases severe hemineglect. Use your clinical judgement here.

Flexible and stabilising orthotics: Compression Suit Therapy
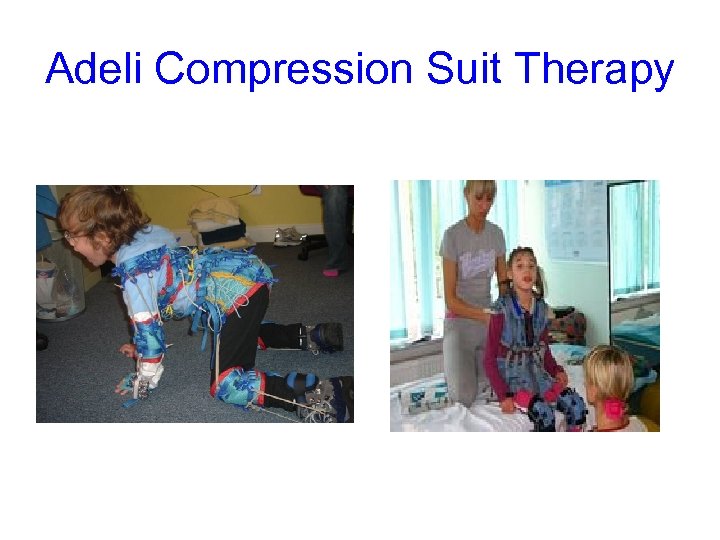
Adeli Compression Suit Therapy

Adeli compression Suit Therapy • “Wearable therapy clothes” = Adeli suit • Originated in Poland being used worldwide • Compression and support orthotics used in attempt to improve muscular and motor control, as well as resistance to some movement in individuals suffering from neurological dysfunctions • ? ? ? Use in cases low tone, ataxia • Cases where you feel you do not “have enough hands’’during therapy • Increased sensory feedback and bodily awareness

Electrical Stimulation
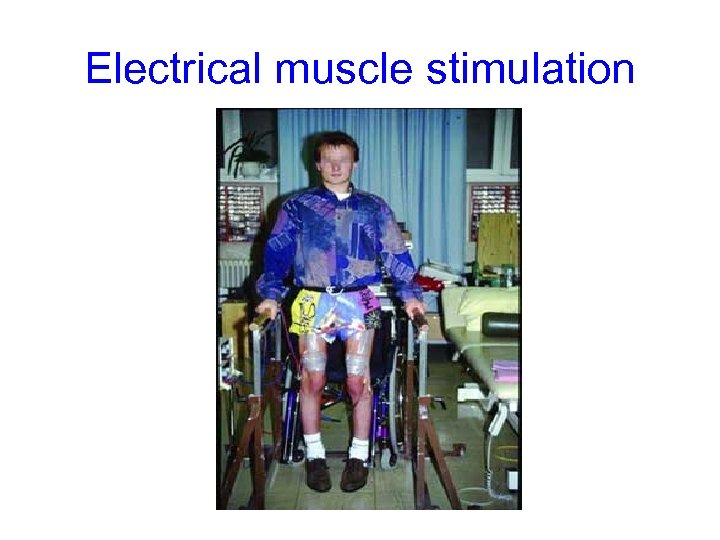
Electrical muscle stimulation

Electrical Stimulation (FES) • ? ? ? Use in muscle specific re-education & strengthening programs • Used in strengthening quadriceps in ambulant diplegic children who find resisted exercises' difficult • Lack of scientific evidence at this therapy • Use remains controversial • Not widely implemented

Static Weight bearing Exercises

Static Weight bearing

Static Weight bearing Exercises • “therapeutic standing” • Widely used e. g. standing frame or tilting table • Used to – – – stimulate antigravity muscle strength, prevent hip dislocations, improve bone density, reduce spasticity and improve bowel and bladder function • ? ? ? Little scientific evidence to support its use • Deemed to be motivating to child and family

Strength Training

Strengthening exercises

Strength Training • Increase the power and strength of muscles – very important in neurological re-education • Treadmill training. Partial body weight supported walking on a treadmill. Initial studies show benefits e. g. walking speed, endurance and strength • General strength training “ functional strengthening” also improves child’s functional abilities in the long run • Scientific evidence to support its use widespread

Virtual Reality Training (VRT)

Virtual Reality Training (VRT)

Virtual Reality Training (VRT)

Orthotics & Assistive Devices
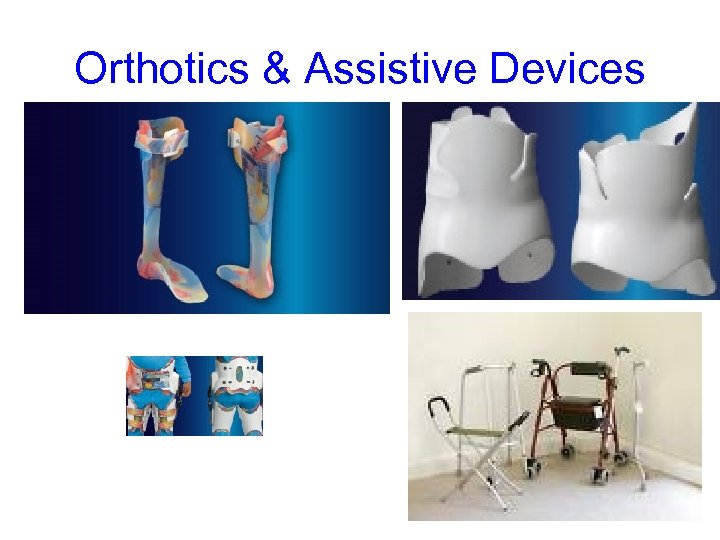
Orthotics & Assistive Devices

Orthoses & Assitive Devices • Devices that by an application of an external force attempt to correct the alignment of a body segment – Help to prevent or correct deformities • Static s. dynamic orthoses avaiable. Decided on in consultation with orthotist. • Plaster of fiberglass or plastic • Serial casting (management of spasticity as well) • Research about use of orthoses is more favourable in terms of LL than UL. Effect however deemed to be short term • Assistive devices including walking frames, rolators
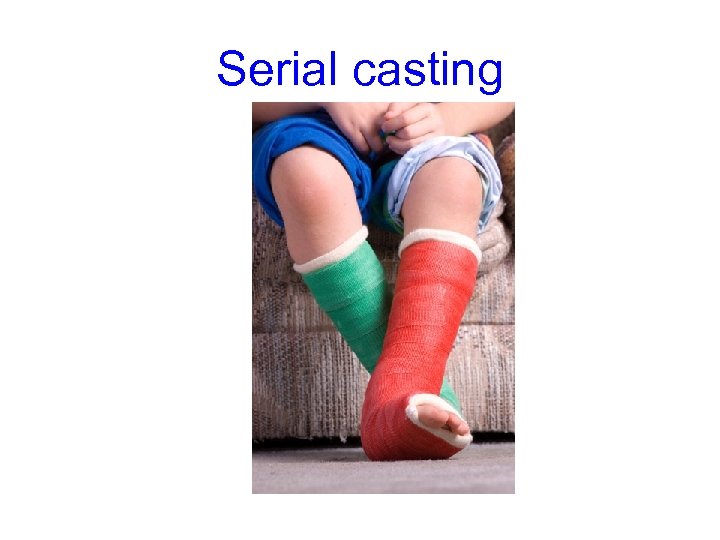
Serial casting

Hippotherapy

Hippotherapy

Hippotherapy • Therapeutic horse-back riding under the supervision of a trained and licensed therapist • Often deemed recreational • Studies have shown therapy to be beneficial in reducing spasticity and improving central control, muscle symmetry in hips and trunk and improving gross motor function • ? ? ? Expensive • ? ? ? Availability • Becoming more popular in SA, more widely used in USA and in Europe

In Conclusion ……. Weighing up available treatment options extremely important in the management of a child with spasticity and motor dysfunction Sometimes need to think outside the NDT box !!!!! In NDT we apply principles of motor learning but also need to include aspects like: – strength and endurance – CVS fitness training

In Conclusion ……. The following needs to be taken into consideration when making decisions regarding therapy and adjuntive modalities: • Clinical picture and diagnosis of the child • Interdisciplinary approach essential – parent/child must be involved in the decision making. • Cost vs. proven effectivness of therapies (evidence based practice) • Treatment must be individualised –there are no recipes

In Conclusion ……. • We also need to make use of appropriate orthotics and assistive devices where indicated • Ultimate aim is improving the child’s functional ability and participation • Need to accurately assess the impact tone and especially spasticty has on a child’s functional abilities

In conclusion …… • Collaborative effort to decide on which approaches and interventions are right for each child considering: • Financial resources of the parent • Availability of quality, intensive physiotherapy treatment • Commitment and parent/caregiver/child participation in therapy • Preference of child and their family. It ultimately remains their choice.

References • Images Courtesy of GOOGLE (2009) • Alternative approaches to managing spasticity (2008) PANDA course provided Prof. Fieggen & Prof. Peter (UCT, Dept. Neurosurgery) • Brown, E. 2001. Neurodevelopmental Therapy (NDT) Course notes. (Unpublished) Bloemfontein. • Coovadia, H. M. & Wittenberg, D. F. 2006. Paediatrics & Child health. A manual for health professionals in developing countires. 5 th ed. Cape Town: Oxford University Press

References • Downie, P. A. 1986. Cash’s Text book of Neurology for Physiotherapists. 4 th ed. London: Faber and Faber • Fieggen, G. 2005. Selective dorsal rhizotomy. Who should be considered for the procedure. . (lecture) University of Cape Town • Stokes, M. 1998. Neurological physiotherapy. London: Mosby International Ltd. • Papavasiliou, A. S. 2008. Management of motor problems in cerebral palsy: a critical update for the clinician
4311045e40cff7e0f89f6cb62ed79397.ppt