b7f797bd8409bfd1ae43d931241bcf51.ppt
- Количество слайдов: 63
 The Management of Cervical , Vulvar and Vaginal Cancers Kerry J. Rodabaugh, M. D. Division of Gynecologic Oncology University of Nebraska Medical Center
The Management of Cervical , Vulvar and Vaginal Cancers Kerry J. Rodabaugh, M. D. Division of Gynecologic Oncology University of Nebraska Medical Center
 Incidence: global public health issue 450, 000 – 500, 000 women diagnosed each year worldwide In developing countries, it is the most common cause of cancer death 340, 000 deaths in 1985
Incidence: global public health issue 450, 000 – 500, 000 women diagnosed each year worldwide In developing countries, it is the most common cause of cancer death 340, 000 deaths in 1985
 United States Incidence 15, 000 women diagnosed annually 4, 800 annual deaths
United States Incidence 15, 000 women diagnosed annually 4, 800 annual deaths
 Mortality Rates • <2/100, 000: Finland, France, Greece, Israel, Japan, Korea, Spain, Thailand • 2. 7/100, 000: USA • 12 -15. 9/100, 000: Chile, Costa Rica, Mexico
Mortality Rates • <2/100, 000: Finland, France, Greece, Israel, Japan, Korea, Spain, Thailand • 2. 7/100, 000: USA • 12 -15. 9/100, 000: Chile, Costa Rica, Mexico
 Lifetime risk of developing cervical cancer 5% - South America 0. 7% - USA
Lifetime risk of developing cervical cancer 5% - South America 0. 7% - USA
 Cervical CA Risk Factors • • Early age of intercourse Number of sexual partners Smoking Lower socioeconomic status High-risk male partner Other sexually transmitted diseases Up to 70% of the U. S. population is infected with HPV
Cervical CA Risk Factors • • Early age of intercourse Number of sexual partners Smoking Lower socioeconomic status High-risk male partner Other sexually transmitted diseases Up to 70% of the U. S. population is infected with HPV
 Screening Guidelines for the Early Detection of Cervical Cancer, American Cancer Society 2003 • Screening should begin approximately three years after a women begins having vaginal intercourse, but no later than 21 years of age. • Screening should be done every year with regular Pap tests or every two years using liquid-based tests. • At or after age 30, women who have had three normal test results in a row may get screened every 2 -3 years. However, doctors may suggest a woman get screened more if she has certain risk factors, such as HIV infection or a weakened immune system. • Women 70 and older who have had three or more consecutive Pap tests in the last ten years may choose to stop cervical cancer screening. • Screening after a total hysterectomy (with removal of the cervix) is not necessary unless the surgery was done as a treatment for cervical cancer. American Cancer Society. Cancer Facts & Figures. 2004. Atlanta, GA; 2005
Screening Guidelines for the Early Detection of Cervical Cancer, American Cancer Society 2003 • Screening should begin approximately three years after a women begins having vaginal intercourse, but no later than 21 years of age. • Screening should be done every year with regular Pap tests or every two years using liquid-based tests. • At or after age 30, women who have had three normal test results in a row may get screened every 2 -3 years. However, doctors may suggest a woman get screened more if she has certain risk factors, such as HIV infection or a weakened immune system. • Women 70 and older who have had three or more consecutive Pap tests in the last ten years may choose to stop cervical cancer screening. • Screening after a total hysterectomy (with removal of the cervix) is not necessary unless the surgery was done as a treatment for cervical cancer. American Cancer Society. Cancer Facts & Figures. 2004. Atlanta, GA; 2005
 Pap Smear • Single Pap false negative rate is 20%. • The latency period from dysplasia to cancer of the cervix is variable. • 50% of women with cervical cancer have never had a Pap smear. • 25% of cases and 41% of deaths occur in women 65 years of age or older.
Pap Smear • Single Pap false negative rate is 20%. • The latency period from dysplasia to cancer of the cervix is variable. • 50% of women with cervical cancer have never had a Pap smear. • 25% of cases and 41% of deaths occur in women 65 years of age or older.
 Clinical Presentation • • • CIN/CIS/ACIS – asymptomatic Irregular vaginal bleeding Vaginal discharge Pelvic pain Leg edema Bowel/bladder symptoms
Clinical Presentation • • • CIN/CIS/ACIS – asymptomatic Irregular vaginal bleeding Vaginal discharge Pelvic pain Leg edema Bowel/bladder symptoms
 Physical Findings • Exophytic, cauliflower like mass • Cervical ulcer, friable or necrotic • Firm “barrel-shaped” cervix • Hydronephrosis • Anemia • Weight loss
Physical Findings • Exophytic, cauliflower like mass • Cervical ulcer, friable or necrotic • Firm “barrel-shaped” cervix • Hydronephrosis • Anemia • Weight loss
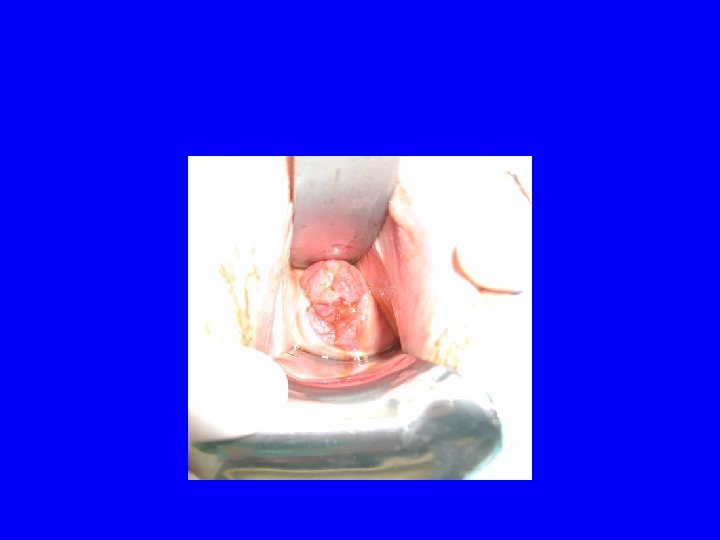
 Histology Squamous 85 -90% Adenocarcinoma 10 -15% Lymphoma Neuroendocrine/small cell Melanoma
Histology Squamous 85 -90% Adenocarcinoma 10 -15% Lymphoma Neuroendocrine/small cell Melanoma
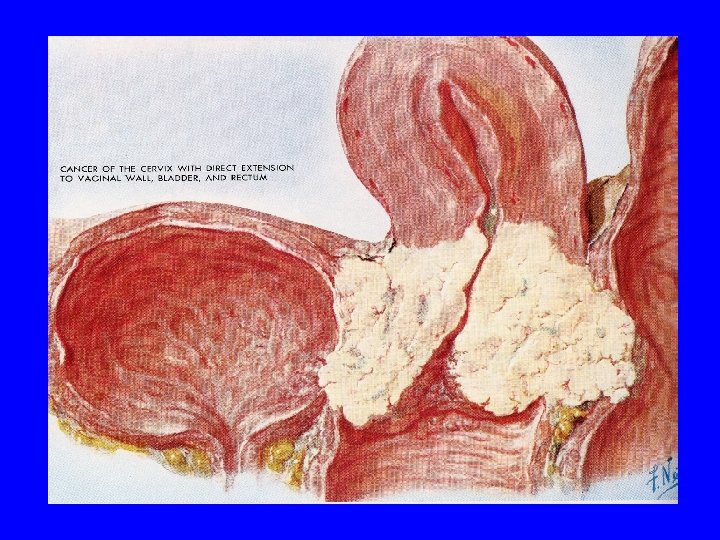
 Route of Spread Cervical cancer spreads by direct invasion or by lymphatic spread Vascular spread is rare
Route of Spread Cervical cancer spreads by direct invasion or by lymphatic spread Vascular spread is rare
 Staging • • • Physical exam Cervical biopsies Chest x-ray IVP (Ct scan) Barium enema, cystoscopy, proctoscopy Surgical staging
Staging • • • Physical exam Cervical biopsies Chest x-ray IVP (Ct scan) Barium enema, cystoscopy, proctoscopy Surgical staging
 Staging Stage I – confined to the cervix IA 1 – <3 mm depth of invasion IA 2 – stromal invasion 3 -5 mm in depth or <7 mm in width IB 1 - tumor < 4 cm IB 2 - tumor > 4 cm in diameter Stage II – extension beyond cervix IIA – upper 2/3 of vagina IIB – Parametrial involvement
Staging Stage I – confined to the cervix IA 1 – <3 mm depth of invasion IA 2 – stromal invasion 3 -5 mm in depth or <7 mm in width IB 1 - tumor < 4 cm IB 2 - tumor > 4 cm in diameter Stage II – extension beyond cervix IIA – upper 2/3 of vagina IIB – Parametrial involvement
 Staging Stage IIIA – lower 1/3 of vagina IIIB – extension to pelvic sidewall or hydronephrosis Stage IV IVA – bladder or rectal mucosa IVB – distant metastases
Staging Stage IIIA – lower 1/3 of vagina IIIB – extension to pelvic sidewall or hydronephrosis Stage IV IVA – bladder or rectal mucosa IVB – distant metastases
 5 year survival rates Stage IA Stage IB Stage III Stage IV 90 -100% 70 -90% 50 -60% 30 -40% 5%
5 year survival rates Stage IA Stage IB Stage III Stage IV 90 -100% 70 -90% 50 -60% 30 -40% 5%
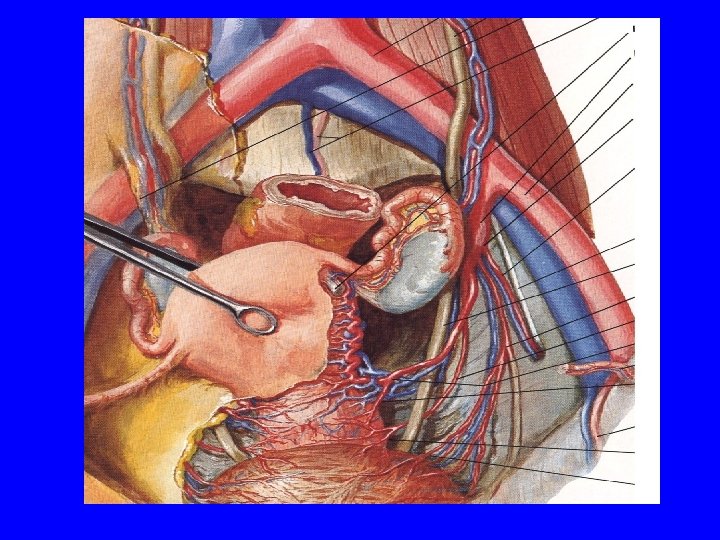
 Therapy Cervical conization Simple hysterectomy Radical hysterectomy Radiation therapy with chemosensitization
Therapy Cervical conization Simple hysterectomy Radical hysterectomy Radiation therapy with chemosensitization
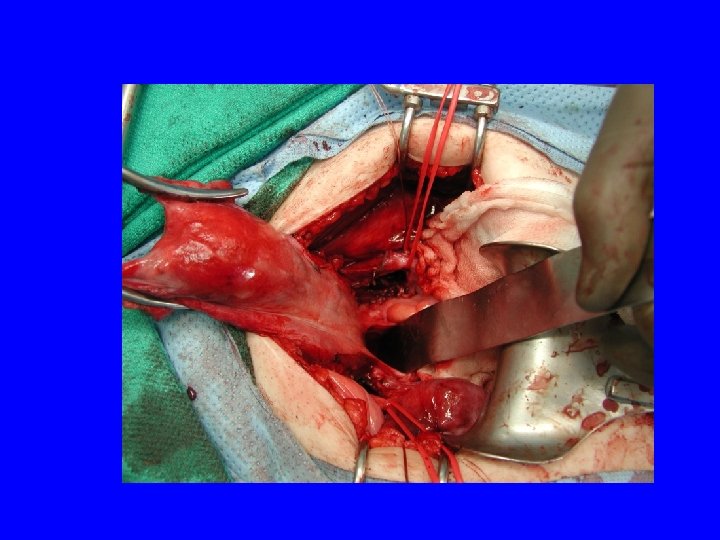
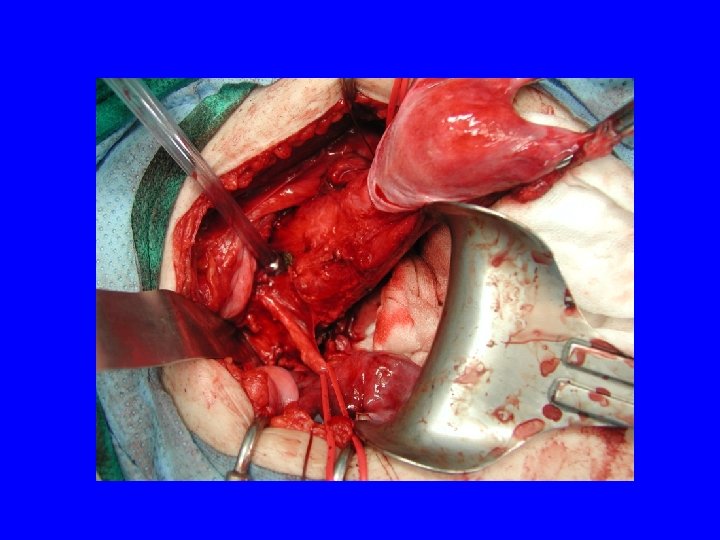
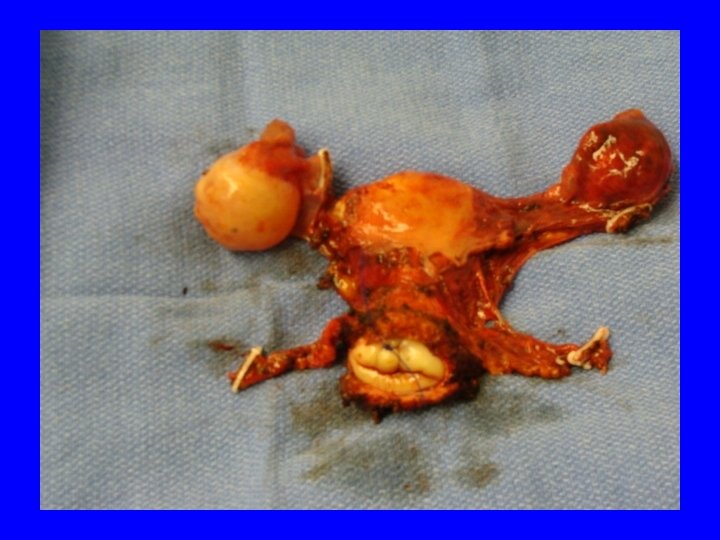 5 year Survival • • Stage III Stage IV 70% 51% 33% 17%
5 year Survival • • Stage III Stage IV 70% 51% 33% 17%
 Pros and Cons Surgery Bladder dysfunction Vesico/uretero fistula Bowel obstruction Ovarian preservation Vaginal preservation Radiation Sigmoiditis Rectovaginal fistula Bowel obstruction Vesico/uretero fistula Ovarian failure
Pros and Cons Surgery Bladder dysfunction Vesico/uretero fistula Bowel obstruction Ovarian preservation Vaginal preservation Radiation Sigmoiditis Rectovaginal fistula Bowel obstruction Vesico/uretero fistula Ovarian failure
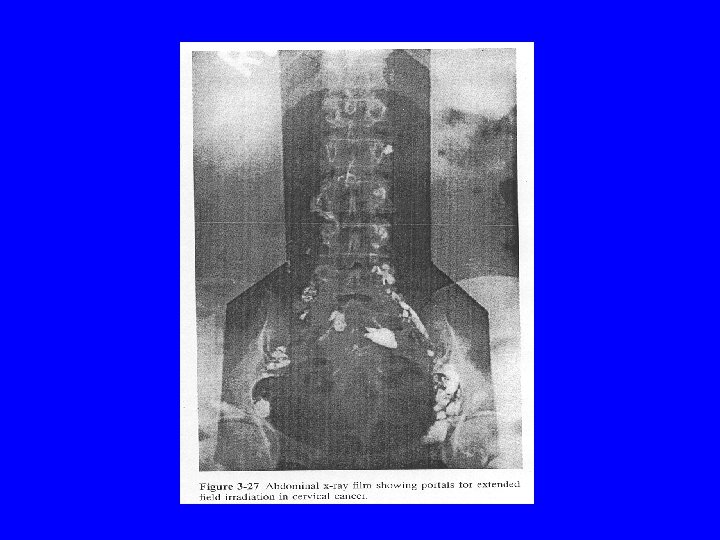
 Radiation Therapy External Beam Whole pelvis or para-aortic window 4000 -6000 c. Gy Over 4 -5 weeks Brachytherapy Intracavitary or interstitial 2000 -3000 c. Gy Over 2 implants
Radiation Therapy External Beam Whole pelvis or para-aortic window 4000 -6000 c. Gy Over 4 -5 weeks Brachytherapy Intracavitary or interstitial 2000 -3000 c. Gy Over 2 implants
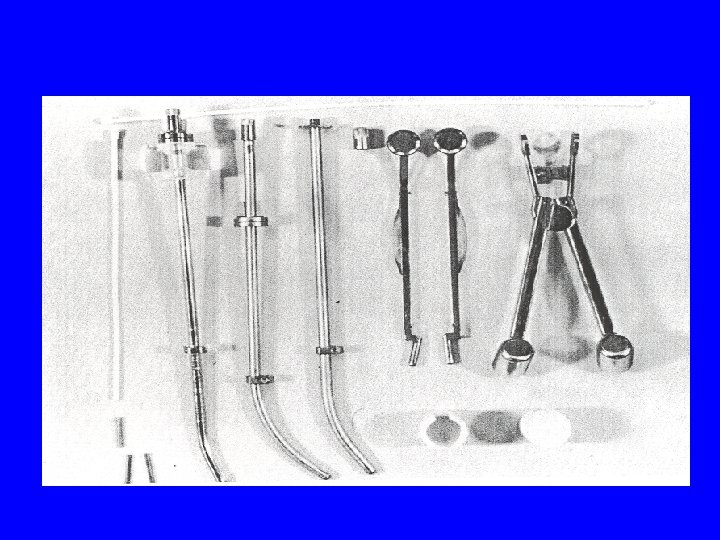
 Recurrent Cervical Cancer 10 -20% of patients treated with radical hysterectomy Recurrence has an 85% mortality 83% are diagnosed within the first two years of post-treatment surveillance
Recurrent Cervical Cancer 10 -20% of patients treated with radical hysterectomy Recurrence has an 85% mortality 83% are diagnosed within the first two years of post-treatment surveillance
 Recurrent Cervical Cancer Radiation Pelvic exenteration Palliative chemotherapy
Recurrent Cervical Cancer Radiation Pelvic exenteration Palliative chemotherapy
 Vulvar Cancer • 3870 new cases 2005 • 870 deaths • Approximately 5% of Gynecologic Cancers American Cancer Society. Cancer Facts & Figures. 2004. Atlanta, GA; 2005
Vulvar Cancer • 3870 new cases 2005 • 870 deaths • Approximately 5% of Gynecologic Cancers American Cancer Society. Cancer Facts & Figures. 2004. Atlanta, GA; 2005
 Vulvar Cancer • • 85% Squamous Cell Carcinoma 5% Melanoma 2% Sarcoma 8% Others
Vulvar Cancer • • 85% Squamous Cell Carcinoma 5% Melanoma 2% Sarcoma 8% Others
 Vulvar Cancer • Biphasic Distribution • Average Age 70 years • 20% in patients UNDER 40 and appears to be increasing
Vulvar Cancer • Biphasic Distribution • Average Age 70 years • 20% in patients UNDER 40 and appears to be increasing
 Vulvar Cancer Etiology • Chronic inflammatory conditions and vulvar dystrophies are implicated in older patients • Syphilis and lymphogranuloma venereum and granuloma inguinal • HPV in younger patients • Tobacco
Vulvar Cancer Etiology • Chronic inflammatory conditions and vulvar dystrophies are implicated in older patients • Syphilis and lymphogranuloma venereum and granuloma inguinal • HPV in younger patients • Tobacco
 Vulvar Cancer • Paget’s Disease of Vulva – 10% will be invasive – 4 -8% association with underlying Adenocarcinoma of the vulva
Vulvar Cancer • Paget’s Disease of Vulva – 10% will be invasive – 4 -8% association with underlying Adenocarcinoma of the vulva
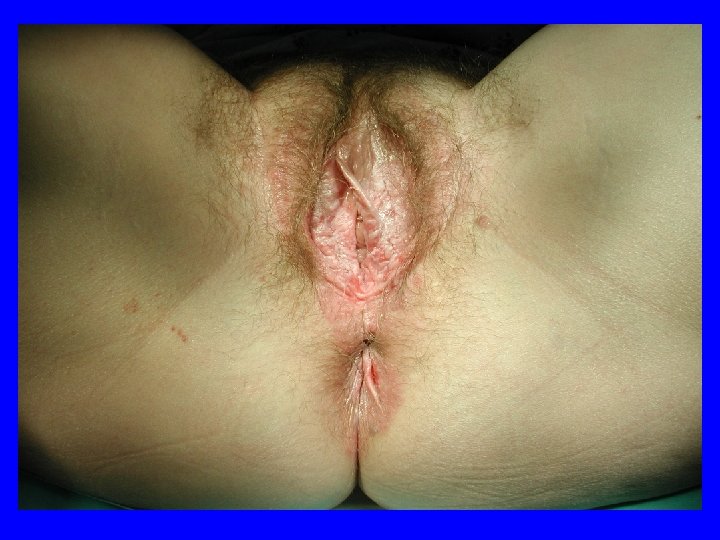
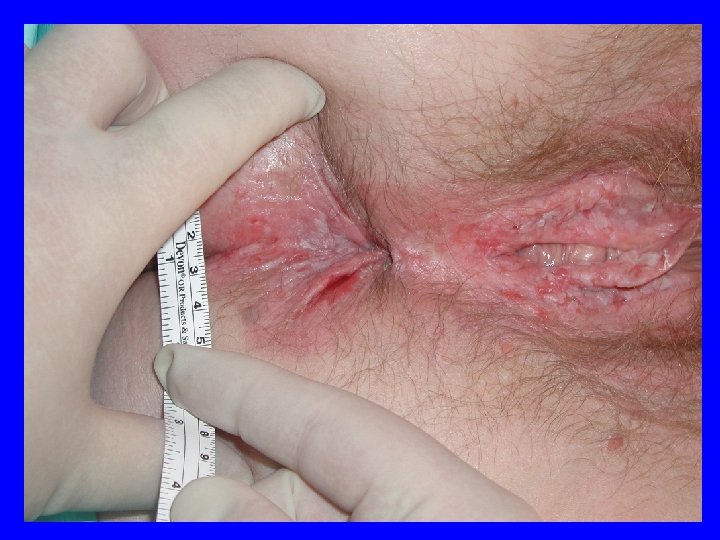
 Symptoms • Most patients are treated for “other” conditions • 12 month or greater time from symptoms to diagnosis
Symptoms • Most patients are treated for “other” conditions • 12 month or greater time from symptoms to diagnosis
 Symptoms • • Pruritus Mass Pain Bleeding Ulceration Dysuria Discharge Groin Mass
Symptoms • • Pruritus Mass Pain Bleeding Ulceration Dysuria Discharge Groin Mass
 Symptoms • May look like: – Raised – Erythematous – Ulcerated – Condylomatous – Nodular
Symptoms • May look like: – Raised – Erythematous – Ulcerated – Condylomatous – Nodular
 Vulvar Cancer • IF IT LOOKS ABNORMAL ON THE VULVA • BIOPSY!
Vulvar Cancer • IF IT LOOKS ABNORMAL ON THE VULVA • BIOPSY!
 Tumor Spread • Very Specific nodal spread pattern • Direct Spread • Hematogenous
Tumor Spread • Very Specific nodal spread pattern • Direct Spread • Hematogenous
 Staging • Based on TNM Surgical Staging – Tumor size – Node Status – Metastatic Disease
Staging • Based on TNM Surgical Staging – Tumor size – Node Status – Metastatic Disease
 Staging • Stage I T 1 N 0 M 0 – Tumor ≤ 2 cm – IA – IB ≤ 1 mm depth of Invasion 1 mm or more depth of invasion
Staging • Stage I T 1 N 0 M 0 – Tumor ≤ 2 cm – IA – IB ≤ 1 mm depth of Invasion 1 mm or more depth of invasion
 Staging • Stage II T 2 N 0 M 0 – Tumor >2 cm – Confined to Vulva or Perineum
Staging • Stage II T 2 N 0 M 0 – Tumor >2 cm – Confined to Vulva or Perineum
 Staging • Stage III – T 3 N 0 M 0 – T 3 N 1 M 0 – T 1 N 1 M 0 – T 2 N 1 M 0 • Tumor any size involving lower urethra, vagina, anus OR unilateral positive nodes
Staging • Stage III – T 3 N 0 M 0 – T 3 N 1 M 0 – T 1 N 1 M 0 – T 2 N 1 M 0 • Tumor any size involving lower urethra, vagina, anus OR unilateral positive nodes
 Staging • Stage IVA – T 1 N 2 M 0 – T 2 N 2 M 0 – T 3 N 2 M 0 – T 4 N any M 0 • Tumor invading upper urethra, bladder, rectum, pelvic bone or bilateral nodes
Staging • Stage IVA – T 1 N 2 M 0 – T 2 N 2 M 0 – T 3 N 2 M 0 – T 4 N any M 0 • Tumor invading upper urethra, bladder, rectum, pelvic bone or bilateral nodes
 Staging • Stage IVB – Any T Any N M 1 • Any distal mets including pelvic nodes
Staging • Stage IVB – Any T Any N M 1 • Any distal mets including pelvic nodes
 Treatment • Primarily Surgical – Wide Local Excision – Radical Vulvectomy with Inguinal Node Dissection • Unilateral • Bilateral • Possible Node Mapping, still investigational
Treatment • Primarily Surgical – Wide Local Excision – Radical Vulvectomy with Inguinal Node Dissection • Unilateral • Bilateral • Possible Node Mapping, still investigational
 Treatment • Local advanced may be treated with Radiation plus Chemosensitizer • Positive Nodal Status – 1 or 2 microscopic nodes < 5 mm can be observed – 3 or more or >5 mm post op radiation
Treatment • Local advanced may be treated with Radiation plus Chemosensitizer • Positive Nodal Status – 1 or 2 microscopic nodes < 5 mm can be observed – 3 or more or >5 mm post op radiation
 Treatment • Special Tumor – Verrucous Carcinoma • Indolent tumor with local disease, rare mets UNLESS given radiation, becomes Highly malignant and aggressive • Excision or Vulvectomy ONLY
Treatment • Special Tumor – Verrucous Carcinoma • Indolent tumor with local disease, rare mets UNLESS given radiation, becomes Highly malignant and aggressive • Excision or Vulvectomy ONLY
 Vulva 5 year survival • • Stage III Stage IV 90 77 51 18 Hacker and Berek, Practical Gynecologic Oncology 4 th Edition, 2005
Vulva 5 year survival • • Stage III Stage IV 90 77 51 18 Hacker and Berek, Practical Gynecologic Oncology 4 th Edition, 2005
 Recurrence • Local Recurrence in Vulva – Reexcision or radiation and good prognosis if not in original site of tumor – Poor prognosis if in original site
Recurrence • Local Recurrence in Vulva – Reexcision or radiation and good prognosis if not in original site of tumor – Poor prognosis if in original site
 Recurrence • Distal or Metastatic – Very poor prognosis, active agents include Cisplatin, mitomycin C, bleomycin, methotrexate and cyclophosphamide
Recurrence • Distal or Metastatic – Very poor prognosis, active agents include Cisplatin, mitomycin C, bleomycin, methotrexate and cyclophosphamide
 Melanoma • 5% of Vulvar Cancers • Not UV related • Commonly periclitoral or labia minora
Melanoma • 5% of Vulvar Cancers • Not UV related • Commonly periclitoral or labia minora
 Melanoma • Microstaged by one of 3 criteria – Clark’s Level – Chung’s Level – Breslow
Melanoma • Microstaged by one of 3 criteria – Clark’s Level – Chung’s Level – Breslow
 Melanoma Treatment • Wide local or Wide Radical excision with bilateral groin dissection • Interferon Alpha 2 -b
Melanoma Treatment • Wide local or Wide Radical excision with bilateral groin dissection • Interferon Alpha 2 -b
 Vaginal Carcinoma • 2140 new cases projected 2005 • 810 deaths projected 2005 • Represents 2 -3% of Pelvic Cancers American Cancer Society. Cancer Facts & Figures. 2004. Atlanta, GA; 2005
Vaginal Carcinoma • 2140 new cases projected 2005 • 810 deaths projected 2005 • Represents 2 -3% of Pelvic Cancers American Cancer Society. Cancer Facts & Figures. 2004. Atlanta, GA; 2005
 Vaginal Cancer • 84% of cancers in vaginal area are secondary – Cervical – Uterine – Colorectal – Ovary – Vagina Fu YS, Pathology of the Uterine Cervix, Vagina and nd
Vaginal Cancer • 84% of cancers in vaginal area are secondary – Cervical – Uterine – Colorectal – Ovary – Vagina Fu YS, Pathology of the Uterine Cervix, Vagina and nd
 Vaginal Carcinoma • • Squamous Cell Clear Cell Sarcoma Melanoma 80 -85% 10% 3 -4% 2 -3%
Vaginal Carcinoma • • Squamous Cell Clear Cell Sarcoma Melanoma 80 -85% 10% 3 -4% 2 -3%
 Clear Cell Carcinoma • Associated with DES Exposure In Utero – DES used as anti abortifcant from 1949 -1971 – 500+ cases confirmed by DES Registry – Usually occurred late teens
Clear Cell Carcinoma • Associated with DES Exposure In Utero – DES used as anti abortifcant from 1949 -1971 – 500+ cases confirmed by DES Registry – Usually occurred late teens
 Vaginal Cancer Etiology • Mimics Cervical Carcinoma – HPV 16 and 18
Vaginal Cancer Etiology • Mimics Cervical Carcinoma – HPV 16 and 18
 Staging • Stage II Confined to Vaginal Wall Subvaginal tissue but not to pelvic sidewall • Stage III Extended to pelvic sidewall • Stage IVA Bowel or Bladder • Stage IVB Distant mets
Staging • Stage II Confined to Vaginal Wall Subvaginal tissue but not to pelvic sidewall • Stage III Extended to pelvic sidewall • Stage IVA Bowel or Bladder • Stage IVB Distant mets
 Treatment • Surgery with Radical Hysterectomy and pelvic lymph dissection in selected stage I tumors high in Vagina • All others treated with radiation with chemosensitization
Treatment • Surgery with Radical Hysterectomy and pelvic lymph dissection in selected stage I tumors high in Vagina • All others treated with radiation with chemosensitization


