a9c4d524587dd03c60ce631eac4ed1c4.ppt
- Количество слайдов: 32
 THE DIVISION OF WORKERS’ COMPENSATION MEDICAL DATA TRAINING WCIS Medical Data Collection 1
THE DIVISION OF WORKERS’ COMPENSATION MEDICAL DATA TRAINING WCIS Medical Data Collection 1
 Workers’ Compensation Information System Division of Workers’ Compensation 2
Workers’ Compensation Information System Division of Workers’ Compensation 2
 www. dir. ca. gov Workers’ Compensation Information System (WCIS) California EDI Implementation Guide for Medical Bill Payment Records Version 1. 0 December 2005 3
www. dir. ca. gov Workers’ Compensation Information System (WCIS) California EDI Implementation Guide for Medical Bill Payment Records Version 1. 0 December 2005 3
 California Implementation Guide Table of Contents • EDI service providers • Events that trigger required medical EDI reports • Required medical data elements üData edits üSystem specifications üIAIABC information • Code lists and state license numbers • Medical EDI glossary and acronyms • Standard medical forms Page 3 4
California Implementation Guide Table of Contents • EDI service providers • Events that trigger required medical EDI reports • Required medical data elements üData edits üSystem specifications üIAIABC information • Code lists and state license numbers • Medical EDI glossary and acronyms • Standard medical forms Page 3 4
 Section M Data edits Page 81 5
Section M Data edits Page 81 5
 IAIABC Detailed Data Edits Mandatory field not present Must be numeric (0 -9) Must be a valid date (CCYYMMDD) Must be A-Z, 0 -9, or spaces Must be a valid time (HHMMSS) Must be <= date of injury Must be >= date of injury No match on database All digits cannot be the same Must be <= current date Duplicate transmission/transaction Code/ID invalid Event table criteria not met Invalid event sequence/relationship Invalid data relationship Must be>= date payer received bill Must be >= from date of service Must be <= thru service date Pages 82 -87 6
IAIABC Detailed Data Edits Mandatory field not present Must be numeric (0 -9) Must be a valid date (CCYYMMDD) Must be A-Z, 0 -9, or spaces Must be a valid time (HHMMSS) Must be <= date of injury Must be >= date of injury No match on database All digits cannot be the same Must be <= current date Duplicate transmission/transaction Code/ID invalid Event table criteria not met Invalid event sequence/relationship Invalid data relationship Must be>= date payer received bill Must be >= from date of service Must be <= thru service date Pages 82 -87 6
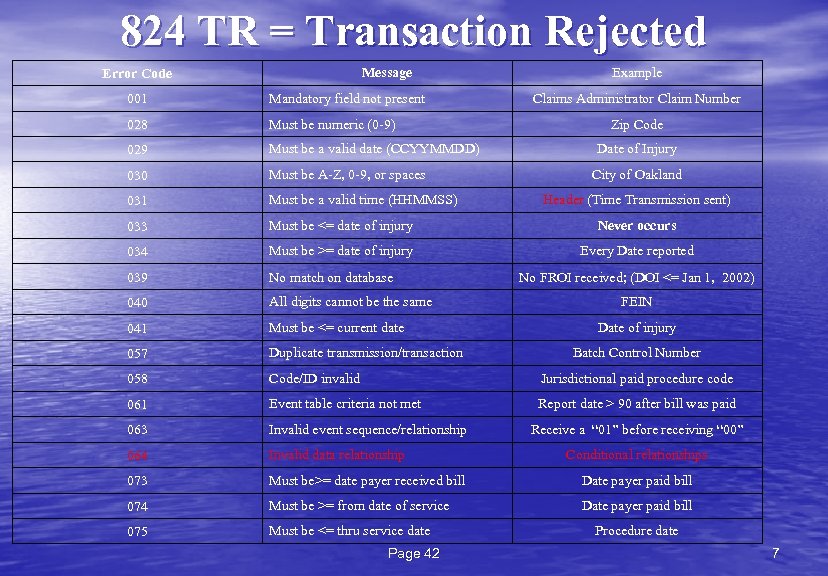 824 TR = Transaction Rejected Message Error Code Example 001 Mandatory field not present 028 Must be numeric (0 -9) 029 Must be a valid date (CCYYMMDD) 030 Must be A-Z, 0 -9, or spaces 031 Must be a valid time (HHMMSS) 033 Must be <= date of injury Never occurs 034 Must be >= date of injury Every Date reported 039 No match on database 040 All digits cannot be the same 041 Must be <= current date 057 Duplicate transmission/transaction 058 Code/ID invalid Jurisdictional paid procedure code 061 Event table criteria not met Report date > 90 after bill was paid 063 Invalid event sequence/relationship 064 Invalid data relationship 073 Must be>= date payer received bill Date payer paid bill 074 Must be >= from date of service Date payer paid bill 075 Must be <= thru service date Page 42 Claims Administrator Claim Number Zip Code Date of Injury City of Oakland Header (Time Transmission sent) No FROI received; (DOI <= Jan 1, 2002) FEIN Date of injury Batch Control Number Receive a “ 01” before receiving “ 00” Conditional relationships Procedure date 7
824 TR = Transaction Rejected Message Error Code Example 001 Mandatory field not present 028 Must be numeric (0 -9) 029 Must be a valid date (CCYYMMDD) 030 Must be A-Z, 0 -9, or spaces 031 Must be a valid time (HHMMSS) 033 Must be <= date of injury Never occurs 034 Must be >= date of injury Every Date reported 039 No match on database 040 All digits cannot be the same 041 Must be <= current date 057 Duplicate transmission/transaction 058 Code/ID invalid Jurisdictional paid procedure code 061 Event table criteria not met Report date > 90 after bill was paid 063 Invalid event sequence/relationship 064 Invalid data relationship 073 Must be>= date payer received bill Date payer paid bill 074 Must be >= from date of service Date payer paid bill 075 Must be <= thru service date Page 42 Claims Administrator Claim Number Zip Code Date of Injury City of Oakland Header (Time Transmission sent) No FROI received; (DOI <= Jan 1, 2002) FEIN Date of injury Batch Control Number Receive a “ 01” before receiving “ 00” Conditional relationships Procedure date 7
 824 with an Error ISA*00**ZZ*943160882*ZZ*450483908 *051122*1202*U*00401*000000045*0*P*~ GS*01*943160882*450483908*20051122*1202*68*X*004010~ ST*824*0015~ BGN*11*MED 01*20051122*1202~ N 1*10**FI*943160882~ N 4***946121413~ N 1*40**FI*450483908~ N 4***239640040~ OTI*TR*55*00001***20051109*1627***837~ DTM*009*20051121*153124~ LM*IB~ LQ*FZ*040~ RED~. . RED~ SE*11*0015~ GE*1*68~ IEA*1*000000045~ 8
824 with an Error ISA*00**ZZ*943160882*ZZ*450483908 *051122*1202*U*00401*000000045*0*P*~ GS*01*943160882*450483908*20051122*1202*68*X*004010~ ST*824*0015~ BGN*11*MED 01*20051122*1202~ N 1*10**FI*943160882~ N 4***946121413~ N 1*40**FI*450483908~ N 4***239640040~ OTI*TR*55*00001***20051109*1627***837~ DTM*009*20051121*153124~ LM*IB~ LQ*FZ*040~ RED~. . RED~ SE*11*0015~ GE*1*68~ IEA*1*000000045~ 8
 California Specific Data Edits • Must be numeric (error code = 028) • DWC specifies an more exact numerical value • Postal Codes • Units (days, minutes, number of pills etc) • Social security number • Lines numbers • Code/ID invalid (error code = 058) • DWC specifies exact IAIABC values in a lookup table • Bill Submission Reason Code (00 or 01 or 05) • Billing Format Code ( A or B) • Billing Type Code ( DM or MO or RX) • Diagnosis Pointer (1 or 2 or 3 or 4) • Service Adjustment Group Code ( CO or MA or OA or PI or PR) Page 88 9
California Specific Data Edits • Must be numeric (error code = 028) • DWC specifies an more exact numerical value • Postal Codes • Units (days, minutes, number of pills etc) • Social security number • Lines numbers • Code/ID invalid (error code = 058) • DWC specifies exact IAIABC values in a lookup table • Bill Submission Reason Code (00 or 01 or 05) • Billing Format Code ( A or B) • Billing Type Code ( DM or MO or RX) • Diagnosis Pointer (1 or 2 or 3 or 4) • Service Adjustment Group Code ( CO or MA or OA or PI or PR) Page 88 9
 Section N System Specifications Page 69 10
Section N System Specifications Page 69 10
 Bill Submission Sequencing • Bill submission reason codes (BSRC) • 00 Original • 01 Cancellation • 05 Replace • 00 must be used with the initial medical bill payment report sent. • 01 must be preceded by the initial (00) medical bill payment report. • 05 must be preceded by the initial (00) medical bill payment report. Page 90 11
Bill Submission Sequencing • Bill submission reason codes (BSRC) • 00 Original • 01 Cancellation • 05 Replace • 00 must be used with the initial medical bill payment report sent. • 01 must be preceded by the initial (00) medical bill payment report. • 05 must be preceded by the initial (00) medical bill payment report. Page 90 11
 Application Acknowledgment Codes • 824 detailed acknowledgment • inform the Trading partner of the accepted or rejected status of each 837 transmission – TA • Transaction accepted – No Errors – TR • Transaction rejected – At least one error – TE • Transaction accepted with errors – No Claim Administrator Claim Number in the WCIS Database Page 91 12
Application Acknowledgment Codes • 824 detailed acknowledgment • inform the Trading partner of the accepted or rejected status of each 837 transmission – TA • Transaction accepted – No Errors – TR • Transaction rejected – At least one error – TE • Transaction accepted with errors – No Claim Administrator Claim Number in the WCIS Database Page 91 12
 DWC Automated Processes • Corrected data element • (BSRC=00)(ACC=TR) • Corrected medical bill • (BSRC=01)(ACC=TA) • Replacement of a claims administrator claim number • (BSRC=05)(ACC=TA) 13
DWC Automated Processes • Corrected data element • (BSRC=00)(ACC=TR) • Corrected medical bill • (BSRC=01)(ACC=TA) • Replacement of a claims administrator claim number • (BSRC=05)(ACC=TA) 13
 Corrected data element process (BSRC=00)(ACC=TR) 1. Sender transmits original bill, including all lines, 2. 3. 4. 5. utilizing a BSRC "00". DWC sends a “TR” 824 acknowledgement with errors to sender. Sender corrects errors in the original bill. Sender transmits the corrected bill, including all lines, as an original BSRC "00". DWC sends a 997 and a “TA” 824 acknowledgement to sender. Page 91 14
Corrected data element process (BSRC=00)(ACC=TR) 1. Sender transmits original bill, including all lines, 2. 3. 4. 5. utilizing a BSRC "00". DWC sends a “TR” 824 acknowledgement with errors to sender. Sender corrects errors in the original bill. Sender transmits the corrected bill, including all lines, as an original BSRC "00". DWC sends a 997 and a “TA” 824 acknowledgement to sender. Page 91 14
 Corrected medical bill process (BSRC=01)(ACC=TA) 1. Sender transmits original bill, including all lines, utilizing a BSRC "00". 2. 3. 4. 5. 6. DWC sends a 997 and a “TA” 824 acknowledgement to sender. Sender changes the value of data elements on the original bill. Sender cancels incorrect original bill by transmitting a BSRC "01". DWC sends a 997 and a “TA” 824 acknowledgement to sender. Sender transmits the updated bill, including all lines, as a BSRC "00". 7. DWC sends a 997 and “TA” 824 acknowledgement to sender. Page 91 15
Corrected medical bill process (BSRC=01)(ACC=TA) 1. Sender transmits original bill, including all lines, utilizing a BSRC "00". 2. 3. 4. 5. 6. DWC sends a 997 and a “TA” 824 acknowledgement to sender. Sender changes the value of data elements on the original bill. Sender cancels incorrect original bill by transmitting a BSRC "01". DWC sends a 997 and a “TA” 824 acknowledgement to sender. Sender transmits the updated bill, including all lines, as a BSRC "00". 7. DWC sends a 997 and “TA” 824 acknowledgement to sender. Page 91 15
 Replacement of a claims administrator claim number process (BSRC=05)(ACC=TA) 1. Sender transmits original bill, including all lines, utilizing a 2. 3. 4. BSRC "00". DWC sends a 997 and a “TA” 824 acknowledgement to sender. Sender changes the claims administrator claim number on the original bill. Sender notifies the DWCWCIS of the new claims administrator claim number by transmitting a BSRC "05" with the old and new claims administrator claim number. Page 92 16
Replacement of a claims administrator claim number process (BSRC=05)(ACC=TA) 1. Sender transmits original bill, including all lines, utilizing a 2. 3. 4. BSRC "00". DWC sends a 997 and a “TA” 824 acknowledgement to sender. Sender changes the claims administrator claim number on the original bill. Sender notifies the DWCWCIS of the new claims administrator claim number by transmitting a BSRC "05" with the old and new claims administrator claim number. Page 92 16
 Duplicate transmissions, transactions, and medical bills • Transmission duplicates • ISA or GE functional groups contain the same key header information • Transaction duplicates • ST-SE transaction sets contain the same header information (DN 532) • Bill duplicates • ST-SE transaction sets from the same sender, contain the same information on the claim administrator FEIN, claim administrator claim number, and unique bill identification number. Page 92 17
Duplicate transmissions, transactions, and medical bills • Transmission duplicates • ISA or GE functional groups contain the same key header information • Transaction duplicates • ST-SE transaction sets contain the same header information (DN 532) • Bill duplicates • ST-SE transaction sets from the same sender, contain the same information on the claim administrator FEIN, claim administrator claim number, and unique bill identification number. Page 92 17
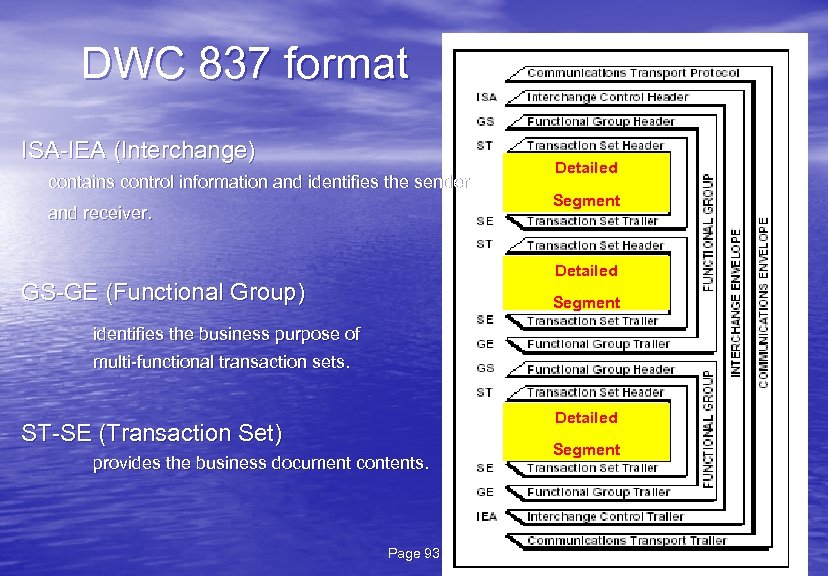 DWC 837 format ISA-IEA (Interchange) contains control information and identifies the sender and receiver. Detailed Segment Detailed GS-GE (Functional Group) Segment identifies the business purpose of multi-functional transaction sets. Detailed ST-SE (Transaction Set) provides the business document contents. Page 93 Segment 18
DWC 837 format ISA-IEA (Interchange) contains control information and identifies the sender and receiver. Detailed Segment Detailed GS-GE (Functional Group) Segment identifies the business purpose of multi-functional transaction sets. Detailed ST-SE (Transaction Set) provides the business document contents. Page 93 Segment 18
 WCIS matching rules Primary: 1. Jurisdiction claim number Secondary match for medical bill payment reports to the FROI: 2 a. Claim administrator claim number Insurer FEIN (match on insurer FEIN if provided, otherwise match on claim administrator FEIN) 2 b. Employee social security number 2 c. Date of injury Employee last name Employee middle name Employee first name Page 93 19
WCIS matching rules Primary: 1. Jurisdiction claim number Secondary match for medical bill payment reports to the FROI: 2 a. Claim administrator claim number Insurer FEIN (match on insurer FEIN if provided, otherwise match on claim administrator FEIN) 2 b. Employee social security number 2 c. Date of injury Employee last name Employee middle name Employee first name Page 93 19
 Unmatched Transactions (BSRC=00)(ACC=TE) 1. The DWC retains the transmission and continuously searches for a match (FROI). 2. If no match (FROI) or BSRC = 01 the DWC sends an 824 acknowledgment indicating transaction accepted with errors (TE). The error code will be 039_nomatch on database. 3. The DWC continues to retain the transmission and searches for a match (FROI). 4. The DWC plans to produce data quality reports within 30 days to send to all trading partners. Page 93 - 94 20
Unmatched Transactions (BSRC=00)(ACC=TE) 1. The DWC retains the transmission and continuously searches for a match (FROI). 2. If no match (FROI) or BSRC = 01 the DWC sends an 824 acknowledgment indicating transaction accepted with errors (TE). The error code will be 039_nomatch on database. 3. The DWC continues to retain the transmission and searches for a match (FROI). 4. The DWC plans to produce data quality reports within 30 days to send to all trading partners. Page 93 - 94 20
 Section O IAIABC Information Page 95 21
Section O IAIABC Information Page 95 21
 IAIABC Information • Introduction • History of the IAIABC and EDI • What is EDI? • Standards • Software • Communications Pages 95 - 99 22
IAIABC Information • Introduction • History of the IAIABC and EDI • What is EDI? • Standards • Software • Communications Pages 95 - 99 22
 Section P Code lists and State license numbers Page 99 23
Section P Code lists and State license numbers Page 99 23
 Standard Code Sets • Facility/Place of Service Codes (page 102) • IAIABC • Place of Service Bill/Line Codes (page 103) • IAIABC • Revenue Billed/Paid Codes (page 104) • IAIABC • Claim Adjustment Group Codes (page 116) • IAIABC • Claim Adjustment Reason Codes (11. 25 -11. 43) • IAIABC • California Medical License Numbers (page 116) • California Department of Consumer Affairs • California Medical Facility License Numbers • California Department of Health Services 24
Standard Code Sets • Facility/Place of Service Codes (page 102) • IAIABC • Place of Service Bill/Line Codes (page 103) • IAIABC • Revenue Billed/Paid Codes (page 104) • IAIABC • Claim Adjustment Group Codes (page 116) • IAIABC • Claim Adjustment Reason Codes (11. 25 -11. 43) • IAIABC • California Medical License Numbers (page 116) • California Department of Consumer Affairs • California Medical Facility License Numbers • California Department of Health Services 24
 Standard Code Sets • Zip Codes (page 100) • US Postal Service • HCPCS (page 100) • Centers for Medicare & Medicaid Services • ICD_9 (page 100) • Centers for Medicare & Medicaid Services • CPT (page 101) • American Medical Association • NDC (page 101) • First databank • DRG (101) • US Government printing Office • Medical Provider Codes (page 102) • Washington Publishing Company 25
Standard Code Sets • Zip Codes (page 100) • US Postal Service • HCPCS (page 100) • Centers for Medicare & Medicaid Services • ICD_9 (page 100) • Centers for Medicare & Medicaid Services • CPT (page 101) • American Medical Association • NDC (page 101) • First databank • DRG (101) • US Government printing Office • Medical Provider Codes (page 102) • Washington Publishing Company 25
 California DWC Code Sets Chapter 4. 5 Division of Workers' Compensation Subchapter 1 Administrative Director-Administrative Rules Ø Article 5. 3__Official Medical Fee Schedule ا 9789. 10 through § 9789. 111 Ø Article 5. 5__Application of Official Medical Fee Schedule ا 9790. through § 9792. 15 Ø Article 5. 6__Medical-legal Expenses and Comprehensive Medical-Legal Evaluations ا 9793. through § 9795 Ø Article 5. 7__Fees for Interpreter Services ا 9795. 1 through § 9795. 4 26
California DWC Code Sets Chapter 4. 5 Division of Workers' Compensation Subchapter 1 Administrative Director-Administrative Rules Ø Article 5. 3__Official Medical Fee Schedule ا 9789. 10 through § 9789. 111 Ø Article 5. 5__Application of Official Medical Fee Schedule ا 9790. through § 9792. 15 Ø Article 5. 6__Medical-legal Expenses and Comprehensive Medical-Legal Evaluations ا 9793. through § 9795 Ø Article 5. 7__Fees for Interpreter Services ا 9795. 1 through § 9795. 4 26
 California DWC Code Sets • Official Medical Fee Schedule – Evaluation and Management 99201 -- 99499 – Anesthesiology 00100 -- 01999 99100 – 99140 – Surgery 10040 – 69979 – Radiology 70010 – 79999 – Pathology and Laboratory 80002 – 89399 – Medicine 90701 -- 99199 • Official Hospital Fee Schedule – § 9789. 24 • Pharmacy – § 9789. 40 • Durable Medical Equipment – § 9789. 60 27
California DWC Code Sets • Official Medical Fee Schedule – Evaluation and Management 99201 -- 99499 – Anesthesiology 00100 -- 01999 99100 – 99140 – Surgery 10040 – 69979 – Radiology 70010 – 79999 – Pathology and Laboratory 80002 – 89399 – Medicine 90701 -- 99199 • Official Hospital Fee Schedule – § 9789. 24 • Pharmacy – § 9789. 40 • Durable Medical Equipment – § 9789. 60 27
 DWC/WCIS Medical Code Contact David Henderson WCIS Research Unit Research Program Specialist II (Medical Data) Division of Workers' Compensation 1515 Clay Street, 18 th floor Oakland, CA 94612 Tel: 916 -263 -0942 Fax: 916 -263 -0971 e-mail: dhenderson@dir. ca. gov 28
DWC/WCIS Medical Code Contact David Henderson WCIS Research Unit Research Program Specialist II (Medical Data) Division of Workers' Compensation 1515 Clay Street, 18 th floor Oakland, CA 94612 Tel: 916 -263 -0942 Fax: 916 -263 -0971 e-mail: dhenderson@dir. ca. gov 28
 Form HCFA-1500 or CMS-1500 29
Form HCFA-1500 or CMS-1500 29
 Form HCFA-1450 or UB-92 30
Form HCFA-1450 or UB-92 30
 American Dental Association Claim Form 31
American Dental Association Claim Form 31
 NCDPD Universal Claim Form 32
NCDPD Universal Claim Form 32


