904818bec19706e74b88b1aad403c90d.ppt
- Количество слайдов: 44
 The Comatose Patient Hans House, MD, FACEP Professor Department of Emergency Medicine University of Iowa
The Comatose Patient Hans House, MD, FACEP Professor Department of Emergency Medicine University of Iowa
 Objective § Outline the general approach to the patient with stupor or coma, including the use of clinical, laboratory, and imaging investigations
Objective § Outline the general approach to the patient with stupor or coma, including the use of clinical, laboratory, and imaging investigations
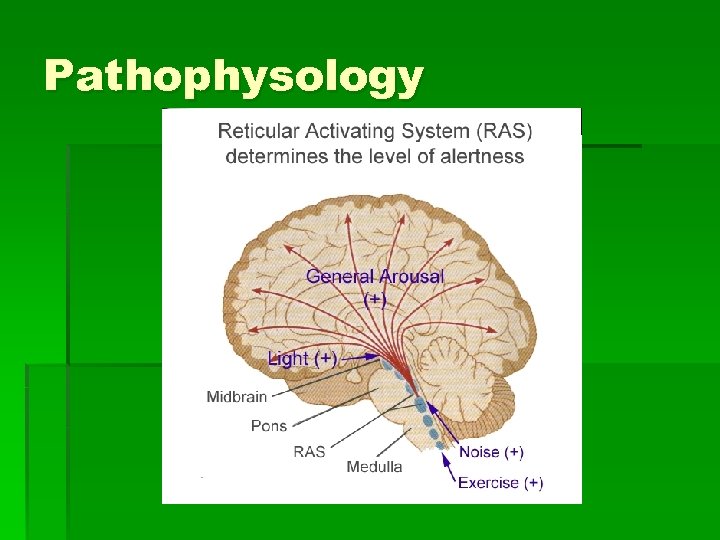 Pathophysology
Pathophysology
 Initial Management § § A: Airway control if needed B: Assist ventilations, 100% O 2 C: Volume if hypotensive D: Dextrose § Consider: glucose, thiamine, nalaxone
Initial Management § § A: Airway control if needed B: Assist ventilations, 100% O 2 C: Volume if hypotensive D: Dextrose § Consider: glucose, thiamine, nalaxone
 Differential Diagnosis § § § A - alcohol, anoxia E - epilepsy I - insulin (diabetes) O - overdose U - uremia, underdose T- trauma I - infection P - psychiatric S – stroke / sub-arachnoid
Differential Diagnosis § § § A - alcohol, anoxia E - epilepsy I - insulin (diabetes) O - overdose U - uremia, underdose T- trauma I - infection P - psychiatric S – stroke / sub-arachnoid
 Differential Diagnosis Most common ED diagnosis: § Trauma § CVA § Intoxications § Metabolic § Post- ictal state § Post- cardiopulmonary arrest
Differential Diagnosis Most common ED diagnosis: § Trauma § CVA § Intoxications § Metabolic § Post- ictal state § Post- cardiopulmonary arrest
 Differential Diagnosis 1) Cerebral Anemia 2) Mechanical injury 3) Convulsive attacks 4) CVA 5) Poisons, endogenous and exogenous 6) Infection Young GS. Can Med Assoc J. 1934; 31(4): 381– 385.
Differential Diagnosis 1) Cerebral Anemia 2) Mechanical injury 3) Convulsive attacks 4) CVA 5) Poisons, endogenous and exogenous 6) Infection Young GS. Can Med Assoc J. 1934; 31(4): 381– 385.
 General Approach: History “Further history limited to patient’s medical condition”
General Approach: History “Further history limited to patient’s medical condition”
 General Approach: History Ask family, EMS, chart: § Time course of onset § Duration of symptoms § Focal signs § Past Medical History § Medications § Alcohol or drug use
General Approach: History Ask family, EMS, chart: § Time course of onset § Duration of symptoms § Focal signs § Past Medical History § Medications § Alcohol or drug use
 General Approach: Physical § § § PE normal in 85% of all patients Vital signs are vital! Elevated or lowered temp may be helpful Need a core temp! Ventilatory patterns not helpful
General Approach: Physical § § § PE normal in 85% of all patients Vital signs are vital! Elevated or lowered temp may be helpful Need a core temp! Ventilatory patterns not helpful
 General Approach: Physical § After nervous, skin is the most useful system to examine § Trauma § Infection § Toxidromes § Jaundice § Seizure trauma § Rhinnorrhea
General Approach: Physical § After nervous, skin is the most useful system to examine § Trauma § Infection § Toxidromes § Jaundice § Seizure trauma § Rhinnorrhea
 General Approach: Physical § § § Nervous System Assess and document level of arousal Useful for prognosis, not diagnosis Use GCS “Less than eight, in-tu-bate!”
General Approach: Physical § § § Nervous System Assess and document level of arousal Useful for prognosis, not diagnosis Use GCS “Less than eight, in-tu-bate!”
 General Approach: Physical § Assessing level of arousal § Shouting, sternal rub, pinching trapezius, nailbed pressure § Supraorbital pressure? Smelling Salts?
General Approach: Physical § Assessing level of arousal § Shouting, sternal rub, pinching trapezius, nailbed pressure § Supraorbital pressure? Smelling Salts?
 General Approach: Physical § § Motor function Unable to do routine oppositional force Use reflexes Look for asymmerty
General Approach: Physical § § Motor function Unable to do routine oppositional force Use reflexes Look for asymmerty
 General Approach: physical Cranial nerves: Pupils § Supertentorial mass/ hemorrhage or primary brainstem lesion § Disruption of 3 rd CN or brainstem nuclei § Transtentorial herniation: § First dilation/ loss of light reflex § Later, midrange (4 -5 mm) and fixed § May be mimicked in severe sedative O/D
General Approach: physical Cranial nerves: Pupils § Supertentorial mass/ hemorrhage or primary brainstem lesion § Disruption of 3 rd CN or brainstem nuclei § Transtentorial herniation: § First dilation/ loss of light reflex § Later, midrange (4 -5 mm) and fixed § May be mimicked in severe sedative O/D
 General Approach: physical Cranial nerves: Pupils § 20% of population have 1 mm difference in pupil size § Try looking at Driver’s License for previous doc. of anisicoria § Huge: anticholinergic § Tiny: pontine, opiate
General Approach: physical Cranial nerves: Pupils § 20% of population have 1 mm difference in pupil size § Try looking at Driver’s License for previous doc. of anisicoria § Huge: anticholinergic § Tiny: pontine, opiate
 General Approach: Physical Cranial Nerves: eye movements § Large cerebral mass lesions cause deviation toward side of lesion § Seizure focus (irritable inflammation or blood) causes deviation away from lesion § Vestibuloocular reflexes § Oculocephalic (doll’s eyes) § Oculovestibular (caloric testing)
General Approach: Physical Cranial Nerves: eye movements § Large cerebral mass lesions cause deviation toward side of lesion § Seizure focus (irritable inflammation or blood) causes deviation away from lesion § Vestibuloocular reflexes § Oculocephalic (doll’s eyes) § Oculovestibular (caloric testing)
 General Approach: Physical Oculocephalic Reflex § Normal is for the eyes to turn opposite to head movement to keep focused on a fixed point § Do not perform in trauma patient! § Positive Doll’s Eyes?
General Approach: Physical Oculocephalic Reflex § Normal is for the eyes to turn opposite to head movement to keep focused on a fixed point § Do not perform in trauma patient! § Positive Doll’s Eyes?
 General Approach § § Oculovestibular Reflex Torso inclined 30º 50 ml cold water into ear COWS: § Cold water causes nystagmus toward contralateral ear § Warm water causes nystagmus to ipsilateral § Conscious patients may vomit § Test both sides: may be asymmetrical
General Approach § § Oculovestibular Reflex Torso inclined 30º 50 ml cold water into ear COWS: § Cold water causes nystagmus toward contralateral ear § Warm water causes nystagmus to ipsilateral § Conscious patients may vomit § Test both sides: may be asymmetrical
 General Approach: Physical Cranial Nerves: Corneal reflexes § Indicative of depth of metabolic coma § Absent 24 hours after trauma / cardiac arrest indicates poor prognosis § May be diminished in conscious elderly, diabetic, or optho patients due to loss of sensation of cornea
General Approach: Physical Cranial Nerves: Corneal reflexes § Indicative of depth of metabolic coma § Absent 24 hours after trauma / cardiac arrest indicates poor prognosis § May be diminished in conscious elderly, diabetic, or optho patients due to loss of sensation of cornea
 Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
 Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
 Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
 Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
 Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
Toxidromes § Pinpoint pupils, decreased respiratory effort and rate, hypothermia, AC scars § Widely dilated pupils, moderate tachycardia (120’s), flushed skin, dry skin § Hyperthermia, tachycardia, tremor, myoclonus, rigidity § Miosis, salivation, lacrimation, urination, defecation, emesis, bradycardia
 Laboratory Testing § § Serum labs Radiography (Head CT) Lumbar Puncture EEG
Laboratory Testing § § Serum labs Radiography (Head CT) Lumbar Puncture EEG
 Laboratory Testing: Serum § Accu-check is part of the ABCD’s! § Electrolytes essential to r/o metabolic § Na, BUN/Cr, anion gap § Consider § UA, urine and blood cultures § TSH § Carboxyhemoglobin § Drug Screen and Et. OH level
Laboratory Testing: Serum § Accu-check is part of the ABCD’s! § Electrolytes essential to r/o metabolic § Na, BUN/Cr, anion gap § Consider § UA, urine and blood cultures § TSH § Carboxyhemoglobin § Drug Screen and Et. OH level
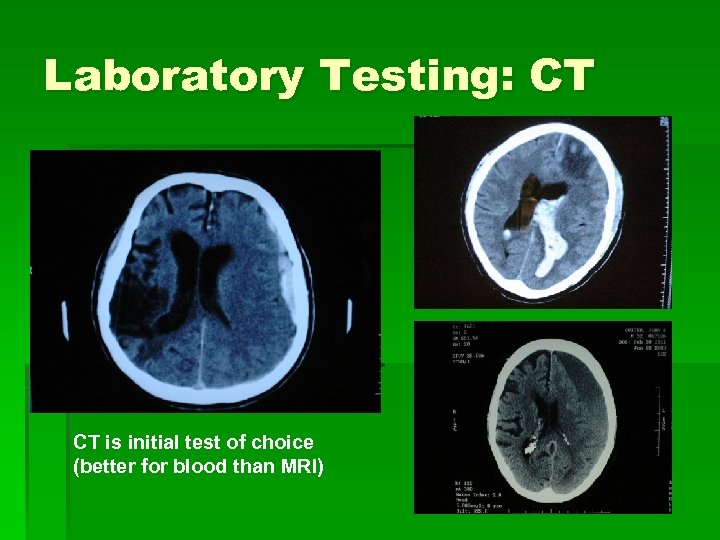 Laboratory Testing: CT CT is initial test of choice (better for blood than MRI)
Laboratory Testing: CT CT is initial test of choice (better for blood than MRI)
 Laboratory Testing: LP § Head CT before LP recommended for possible mass lesions § DO NOT DELAY ANTIBIOTICS/ STEROIDS! (you have the blood cultures. . . ) § LP after CT if SAH suspected
Laboratory Testing: LP § Head CT before LP recommended for possible mass lesions § DO NOT DELAY ANTIBIOTICS/ STEROIDS! (you have the blood cultures. . . ) § LP after CT if SAH suspected
 Laboratory Testing: EEG § Indications: § Status epilepticus (SE) with paralysis § Suspected non-convulsive SE (NCSE) § Aid in diagnosis of unknown case § 8 of 236 patients without overt seziure activity in coma had NCSE § Pattern may indicate cause of coma (metabolic, structural, seizure, anoxic)
Laboratory Testing: EEG § Indications: § Status epilepticus (SE) with paralysis § Suspected non-convulsive SE (NCSE) § Aid in diagnosis of unknown case § 8 of 236 patients without overt seziure activity in coma had NCSE § Pattern may indicate cause of coma (metabolic, structural, seizure, anoxic)
 Case #1 § 78 yo male BIB RA from SNF for fever and altered mental status § Temp 40º, HR 110, BP 95/60, R 20 § PE: dry mucous membranes, poor tugor § Minimally responsive, groans when neck flexed, hot to touch § UA normal
Case #1 § 78 yo male BIB RA from SNF for fever and altered mental status § Temp 40º, HR 110, BP 95/60, R 20 § PE: dry mucous membranes, poor tugor § Minimally responsive, groans when neck flexed, hot to touch § UA normal
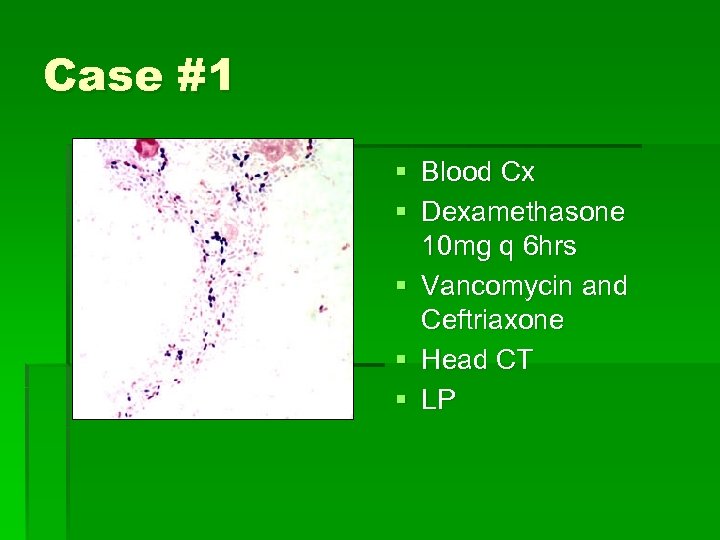 Case #1 § Blood Cx § Dexamethasone 10 mg q 6 hrs § Vancomycin and Ceftriaxone § Head CT § LP
Case #1 § Blood Cx § Dexamethasone 10 mg q 6 hrs § Vancomycin and Ceftriaxone § Head CT § LP
 Case #2 § 42 yo male of “no fixed abode” BIB police after found down in street § Pt is “well known to service” § Vitals normal except mild hypothermia § GCS 9 (withdraws and moans to pain) § Odor of Et. OH on breath
Case #2 § 42 yo male of “no fixed abode” BIB police after found down in street § Pt is “well known to service” § Vitals normal except mild hypothermia § GCS 9 (withdraws and moans to pain) § Odor of Et. OH on breath
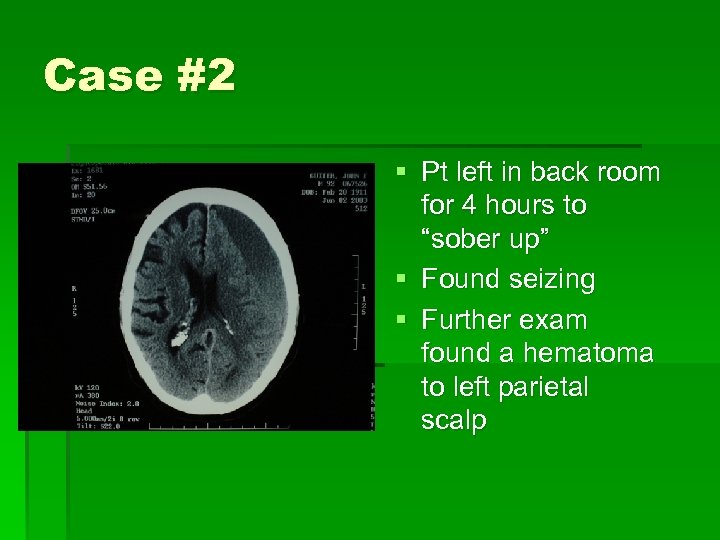 Case #2 § Pt left in back room for 4 hours to “sober up” § Found seizing § Further exam found a hematoma to left parietal scalp
Case #2 § Pt left in back room for 4 hours to “sober up” § Found seizing § Further exam found a hematoma to left parietal scalp
 Case #3 § 46 yo male alcoholic BIB family for decreased consciousness § He moans in response to stimulation, withdraws from pain, eye remain shut § Skin is jaundiced, sclera icteric § Foul breath (fetor hepaticus) § Abdomen: swollen, caput medusae
Case #3 § 46 yo male alcoholic BIB family for decreased consciousness § He moans in response to stimulation, withdraws from pain, eye remain shut § Skin is jaundiced, sclera icteric § Foul breath (fetor hepaticus) § Abdomen: swollen, caput medusae
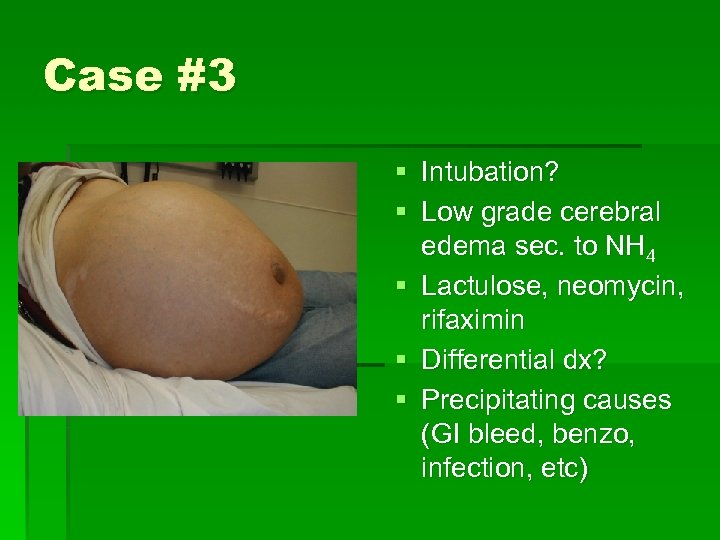 Case #3 § Intubation? § Low grade cerebral edema sec. to NH 4 § Lactulose, neomycin, rifaximin § Differential dx? § Precipitating causes (GI bleed, benzo, infection, etc)
Case #3 § Intubation? § Low grade cerebral edema sec. to NH 4 § Lactulose, neomycin, rifaximin § Differential dx? § Precipitating causes (GI bleed, benzo, infection, etc)
 Case #4 § § § 22 yo male BIB police for odd behavior He was found in the street yelling Agitated, combative, anxious BP 184/97, HR 140, R 22, T 38 Eyes open to pain, moves all 4’s, incomprehensible sounds § Eyes have rotatory nystagmus
Case #4 § § § 22 yo male BIB police for odd behavior He was found in the street yelling Agitated, combative, anxious BP 184/97, HR 140, R 22, T 38 Eyes open to pain, moves all 4’s, incomprehensible sounds § Eyes have rotatory nystagmus
 Case #4 § Used PCP § Essentially adrenergic toxidrome § Hallucinogen § Causes all forms of nystagmus
Case #4 § Used PCP § Essentially adrenergic toxidrome § Hallucinogen § Causes all forms of nystagmus
 Case #5 § § § 39 yo female found down by husband Had complained of a headache earlier PMH: Htn FHx: polycystic kidney disease BP 150/90, HR 65, T 37 Eyes closed, withdraws to pain, no verbal
Case #5 § § § 39 yo female found down by husband Had complained of a headache earlier PMH: Htn FHx: polycystic kidney disease BP 150/90, HR 65, T 37 Eyes closed, withdraws to pain, no verbal
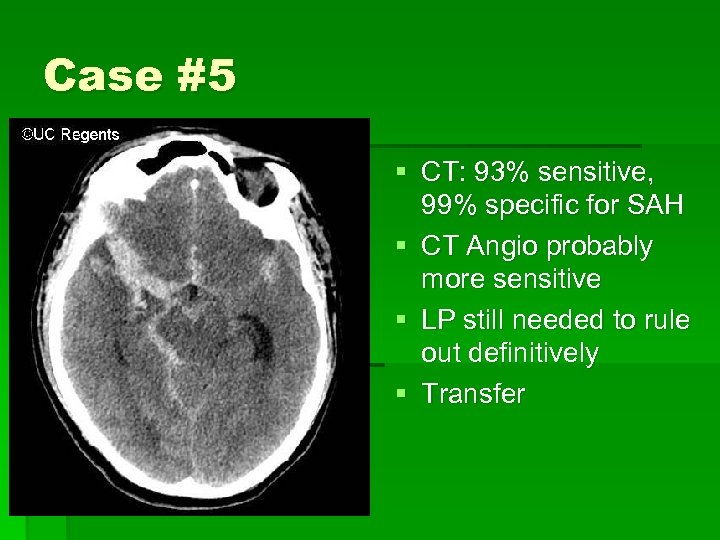 Case #5 § CT: 93% sensitive, 99% specific for SAH § CT Angio probably more sensitive § LP still needed to rule out definitively § Transfer
Case #5 § CT: 93% sensitive, 99% specific for SAH § CT Angio probably more sensitive § LP still needed to rule out definitively § Transfer
 Case #6 § § § 27 yo female BIB family for odd behavior Previous history of bipolar d/o Now not responsive No signs of trauma or intoxication Exam normal except for intermittent nystagmus and eye deviation § All labs, including head CT and drug screen WNL
Case #6 § § § 27 yo female BIB family for odd behavior Previous history of bipolar d/o Now not responsive No signs of trauma or intoxication Exam normal except for intermittent nystagmus and eye deviation § All labs, including head CT and drug screen WNL
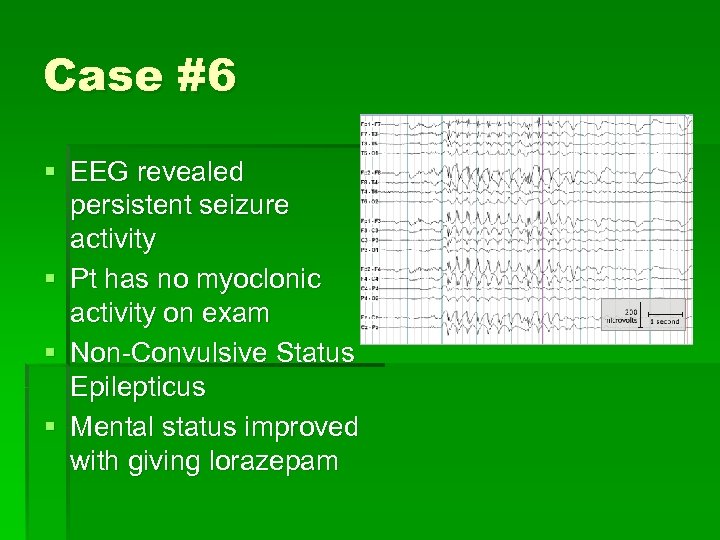 Case #6 § EEG revealed persistent seizure activity § Pt has no myoclonic activity on exam § Non-Convulsive Status Epilepticus § Mental status improved with giving lorazepam
Case #6 § EEG revealed persistent seizure activity § Pt has no myoclonic activity on exam § Non-Convulsive Status Epilepticus § Mental status improved with giving lorazepam
 Conclusions § ABC-D (D is for Dextrose) § If elevated or low Temp would change your management, get a core temp § Less than 8, in-tu-bate! § For meningitis: IV, then blood cultures, then steroids, then Abx, then CT, then LP § Beware of occult trauma in the intoxicated
Conclusions § ABC-D (D is for Dextrose) § If elevated or low Temp would change your management, get a core temp § Less than 8, in-tu-bate! § For meningitis: IV, then blood cultures, then steroids, then Abx, then CT, then LP § Beware of occult trauma in the intoxicated
 Any Questions?
Any Questions?


