a06c5f688f9f6f62a062a343d64b1ea3.ppt
- Количество слайдов: 34

The Challenges of Health Informatics BCS Glasgow – 4 February 2008 Woodcote Consulting

Introductions • Dr Ian Mc. Nicoll - Ian. Mc. Nicoll@oceaninformatics. com – Clydebank GP until 2001 – Developer and Director of leading UK GP accounting system until 2007 – Consultant Health Informatician • Currently working with Ocean Informatics on NHS Clinical models project • Ewan Davis – ewan@woodcote-consulting. com – Immediate Past Chairman of BCS PHCSG – Past Chairman of Intellect Healthcare Group – Founder and CEO of GP system supplier AAH Meditel until 1999 – Consultant Health Informatician

Background • Changing demographics – Aging population increasing numbers needing care fewer people to deliver and pay for it • Increasingly capable medical technologies – Medicines – Genomics – Medical devices – New techniques and procedures • Greater citizen expectations – Quality – Convenience

UK Government Response • Stick to NHS founding principles • Double UK Health Expenditure bringing it closer to European Norm • Seek greater involvement of private and third sector in the provision and commissioning of NHS services • Seek greater engagement of patients and informal carers in delivering health care • Look to technology and particularly information technology to enable transformational change

Government Perspective on NHS IT • IT not achieving transformational change as in other sectors • Existing systems not delivering anything much useful • Existing suppliers lacking capability and scale • Professional vested interests blocking progress • Recognition of inadequate and fragmented investment

The Vision for NHS IT • To provide secure and timely access to all those concerned with the delivery of health and social care to an individual to relevant parts of that individual’s care records where and when needed irrespective of organisational boundaries. • To provide workflow management and decision support tools to manage the patient’s journey along the most appropriate clinical pathway within and across organisational boundaries in a way that delivers quality care, convenient service and makes the best use of NHS resources.

Government Response on IT • To raise NHS IT spend to 4% of NHS revenue by 2008 (from a base of 1. 7%) • To launch major programmes in each of the home countries • To seek involvement of major global IT players in NHS IT (England only!!)

Approach • England – Deliver national infrastructure via two major contracts – Deliver two monolithic systems via four global IT suppliers • Wales and NI – At early stage, hopefully learning from English failures – More incremental approach

Scotland : Delivering for Health 2005 “. . . procure as soon as possible, and by 2008 at the latest, a single information technology system with the following key features: – An electronic health record available to all those who require it to provide patient care across the whole NHS – Patient access to the record and the facility to update it – Picture Archiving and Communications (PACS) – Electronic prescribing – Electronic booking – Tele-health and tele-care.

Progress • England – Some national infrastructure and peripheral services delivered – Two major suppliers departed and third with high profile problems – Disruption to progress with existing systems – No real progress in hospital sector or with detailed care record – Summary Care Record in initial pilot

Progress • Scotland – “In recognition that there is, as yet, no one single electronic patient record system available within the commercial sector, the framework for the national Software Applications is based on a convergence strategy over the period to 2011. . . • Emergency Care Summary (95% popn. ) – Palliative Care summary • Electronic Prescription Service • PACS/RIS Radiology systems (PACS/RIS) • SCI Gateway Comms infrastructure • SCI Diabetes Shared Care • National A&E system • GP systems GP 2 GP + Scanned document transfer

Progress • Scotland’s EHR – Applications • Generic Clinical System : Hospital system “gap filler” • IPACC Integrated GP Community services • SCI Store(s) – multiple, integration stores per HB • Multiagency Store Social work systems • The independent Republic of Tayside – Standards • Messaging : SCI-XML (not HL 7 as in England) • Clinical knowledge : NCDDP National clinical datasets • Terminology : SNOMED-CT • Information Model: NONE

Current Perspectives • Growing recognition that approach based on a small number of monolithic has failed and was fundamentally flawed • Need to develop solutions that: – Allows interworking of a large number of heterogeneous systems – Address privacy and confidentiality concerns – Shares that which is usefully shared – Allows incremental and agile development able to respond to unpredictable and changing needs – Exploit emerging web 2. 0 and SOA technologies

Why is Health Different • Healthcare is large and very complex – The NHS is a large supply chain or eco-system – Not an organisation or federation – Health records are probably the most complex entity informatics has ever tried to address (certainly the most complex with potentially ubiquitous, large scale applicability) • Health is high profile – Raises fundamental economic and moral issues – High Political and public profile – Has “Life and Death” consequence that effect us all • Requirement are poorly defined and continually changing

Challenges • Electronic Care Records – Coded and structured text using large and complex terminologies – Sophisticated narrative text – Large number of numeric values – Drawings, still and moving images and sounds – Much information represented by context of and relationships between record items – Conception to grave, spanning many organisations and jurisdictions • Workflow management (Integrated Care Pathways) – Many actors including patients, carers and professionals across many organisations in public, private and third sector • Decision Support – Passive – Context appropriate access to very large knowledgebase – Active – Prompts and alerts supporting, not interfering with, the clinical process

Challenges • Human factors – Patient access to records – Information sharing and privacy – Diverse health beliefs and values – Patient mobility – Individual vs population health • Semantic interoperability between diverse systems – Maintaining human meaning – Maintaining computability • Handling change – – In underpinning science and technology In health policy and organisation

Addressing the challenge • Collaborative working – Open standards – Open IPR • Agile methodologies

Standards/Open. Source Activity • ISO 215 CEN 251 • SNOMED SDO • HL 7 • Open. EHR • Vist. A • Healthcare Services Specification Project • Open Health Tools • Integrating the Health Enterprise - IHE • Open Source Health Care Alliance - OSHCA

Interoperability = making ‘meaning’ • . . . and the problem of making ‘meaning’ is that like "making babies" it takes time; One can't do it by oneself - someone else has to make a contribution; It doesn't happen all at once and once born, it changes, grows and develops Terry Burridge, Primary Care Complexity Group

Shifting sands. . . • “Medical knowledge is currently doubling every eight years. . . ” • Paradigm shifts • Genomics • Patient access to records • Political / managerial change – “Choice!!” – “Government!!”

Terminologies • Labels of clinical concepts + relationships between those concepts – SNOMED CT, dm+d • By necessity ‘static’ – internationalised, complex, inflexible – limited extensibility, flexibility • Models of real-world entities – Do not model clinical records

Terminology limitations • Issues of context – Differential Diagnosis -“Myocardial Infarction” – Discharge Diagnosis – “Myocardial Infarction” – “Risk of arson Y/N” • History of risk • Assessed risk • Possible future risk • Atomic worldview with limited structure – The “clinical statement” is often not a simple label: • SNOMED : Blood pressure finding -. . . (finding) – 392570002 • BP 120/94, Sitting, Cuff Large for age

Record of BP 120/94, Sitting, large cuff § SNOMED CT Concepts § Blood pressure finding -. . . (finding) – 392570002 • Sitting blood pressure -. . . (observable entity) – 163035008 • Blood pressure -. . . (observable entity) – 75367002 • Blood pressure taking -. . . (procedure) – 46973005

Forms and Fragments • ‘Clinical Forms’ – Nursing assessments – Elderly shared assessments – Gold Standards Palliative care forms • made up of ‘Clinical Fragments’ – Blood pressure – Waterlow venous ulcer scales – Carer details – Lifestyle – smoking, alcohol

Information Model • “provide formalism to the description of a problem domain without constraining how that description is mapped to an actual implementation in software” • In health systems, mostly closely integrated with application and underlying storage designs – Hard coded forms/ dialogs – End user Form builders • Progress with messaging between applications – SCI-XML in Scotland – HL 7 (NHS England GP to GP) – ? Not scalable to EHR modelling
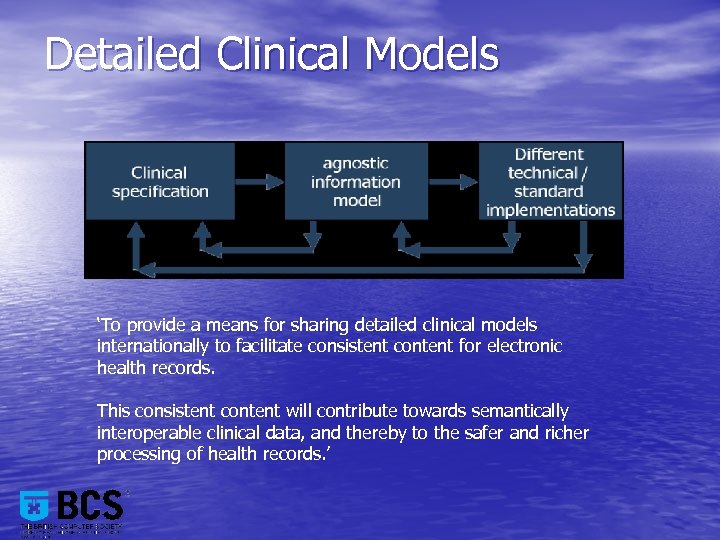
Detailed Clinical Models ‘To provide a means for sharing detailed clinical models internationally to facilitate consistent content for electronic health records. This consistent content will contribute towards semantically interoperable clinical data, and thereby to the safer and richer processing of health records. ’
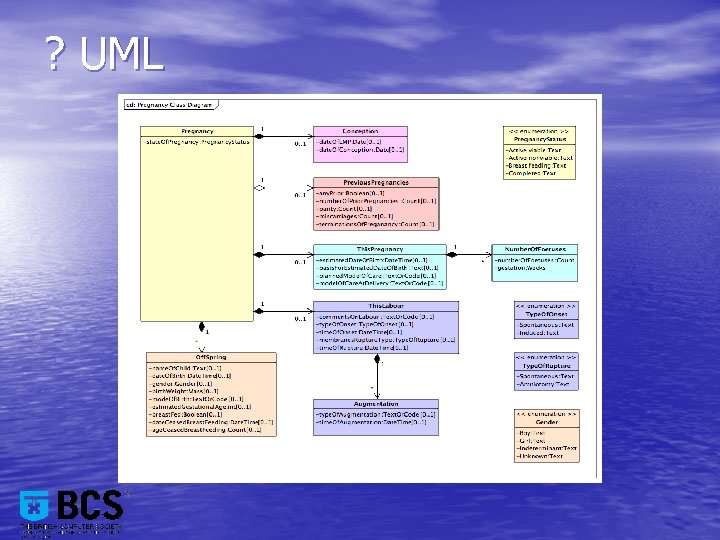
? UML
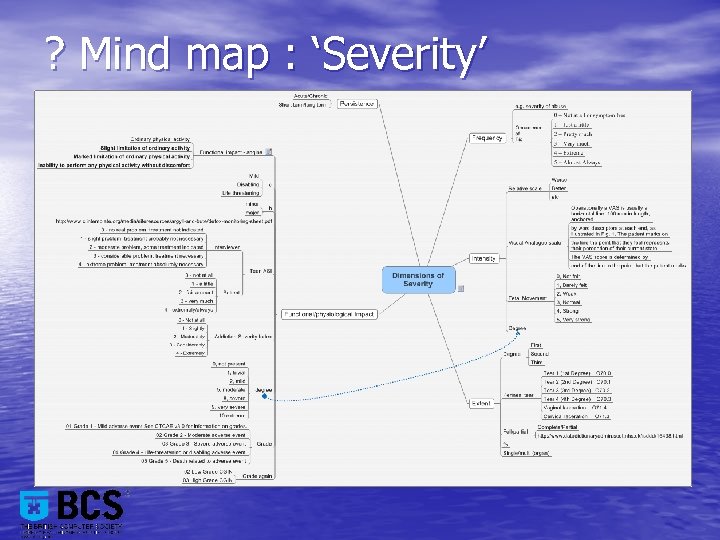
? Mind map : ‘Severity’

? Archetypes : Open. EHR • International group led by CHIME UCL and Ocean Informatics (www. openehr. org) • Open specifications, open source software and tools producing re-usable clinical models of content and process – 3 layer representation • Reference model – e. g. Quantity, Text, Coded_Text, Section • Archetypes – Maximal dataset of a well-defined clinical concept – Pregnancy “Archetype” • Templates – Aggregation and constraint on archetypes for particular use case – NHS England Clinical Models project – Scottish NHS NCDDP • Evaluating as a replacement for current clinical data standards representation

Open. EHR: NHS England Clinical Models • Currently ‘production line’ approach – Business analysts • Clinical domain “Learning disability team” • Paper forms to spreadsheet – Clinical modellers • Spreadsheet to Open. EHR archetypes and templates – Terminologists • Bind clinical models to Snomed CT – HTML output of Open. EHR templates • Not easy for end-users – User interface design • “Out of scope” but impacts on modelling process

RAD : Requirements gathering and prototyping tool • Single web based modelling environment • Early involvement of all designers/ modellers • Web based communications between users/ designers • Iterative development including limited user interface prototyping to aid end user verification of design and capture form-level workflow • A vendor/technology independent “prescription” of reusable, computable clinical content for a specific setting

Summary • The challenge is too big and too important for a fragmented approach – Need to develop collaborative approaches • Combining generic skills with domain expertise • Combining commercial IT capabilities with health provider • and academic knowledge Develop an open ecosystems in which commercial players can both cooperate and compete – Need to apply agile Methodologies • Able to be applied on large scale projects

Links • BCS PHCSG – www. phcsg. org • UK drugs and medical devices datbase -dm+d - www. dmd. nhs. uk • SNOMED SDO – www. snomed. org • • HL 7 UK- www. hl 7. org. uk • • Veterans Health Information Systems and Technology Architecture - Vist. A - www. va. gov/vista_monograph • • Open Health Tools - www. openhealthtools. org • • Scottish Care Information – SCI - www. sci. scot. nhs. uk • • NHS Cf. H – www. cfh. nhs. uk • • CEN Healthcare - http: //tinyurl. com/242 mgt • • International Medical Informatics Association – IMIA - www. imia. org Open. EHR - www. openehr. org Healthcare Services Specification Project – www. hssp. wikispaces. com Integrating the Healthcare Enterprise - IHE - www. ihe. net SCIMP - www. scimp. scot. nhs. uk ISO 215 - http: //tinyurl. com/2 m 8 qxk Open Source Health Care Alliance – OSHCA - www. oshca. org e. Health Insider – www. e-health-insider. com

The Challenges of Health Informatics BCS Glasgow – 4 February 2008 Woodcote Consulting
a06c5f688f9f6f62a062a343d64b1ea3.ppt