468f0644242e01d9bb1c756fffa94e45.ppt
- Количество слайдов: 35

Teenage Pregnancy EBM Club 23. 2. 2009 Damian Wood

Learning Objectives Identify current trends in teenage conceptions and births in the UK in an international context List factors that increase the risk of, or protect against, teenage pregnancy and young parenthood Describe the health outcomes of young parenthood for both the child and the parents Identify issues relating to working with young people when they become parents during adolescence

Pre-Test 1. Teenage conception rates in the UK are now lower than they were 20 years ago 2. Young mothers are no more likely to give birth to small gestational age (SGA) babies than older mothers 3. A young person from a black Caribbean background has a heightened risk of becoming a young parent 4. The UK still has the highest teenage pregnancy rate in Western Europe 5. Health professionals can help reduce the cycle of disadvantage typically seen in this group

Pre Test 6. Teenagers who have been in care more likely to become young parents 7. Young women are less likely to become pregnant if they have just had a pregnancy or termination 8. Having been conceived to a teenage mother increases the likelihood of a young man becoming a young father 9. Young people from a Chinese or Jewish background are at lower risk of becoming young parents than other young people 10. Adolescents whose fathers are from a background of low socio-economic status (SES) are more likely to become young parents

Introduction Different ages are used to define teenage mothers in different contexts. Teenage Pregnancy Strategy under 18 s; Every Child Matters Programme under 19 s Breastfeeding and smoking rates from the Infant Feeding Survey under 20 s Maternity services for teenagers use various age cut off levels
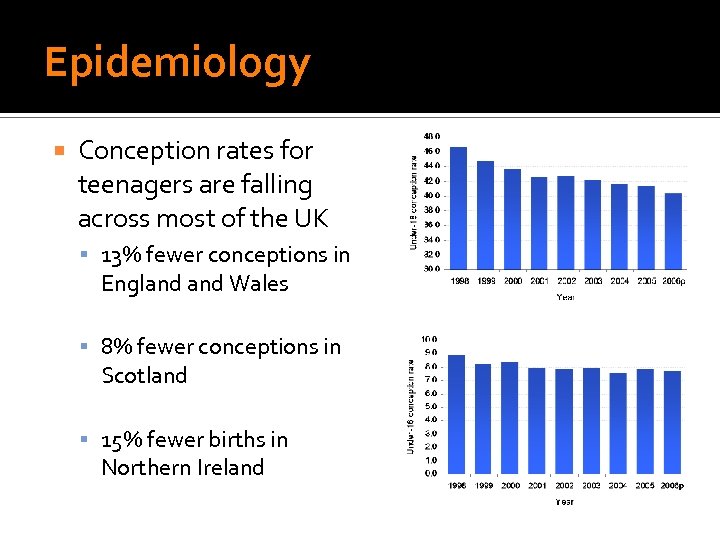
Epidemiology Conception rates for teenagers are falling across most of the UK 13% fewer conceptions in England Wales 8% fewer conceptions in Scotland 15% fewer births in Northern Ireland

Epidemiology Highest rate in Western Europe Multifactorial Comparisons with Sweden and Netherlands

Regional Data Large variation between regions, and between local authority areas within regions Range from 48. 3 per 1000 in the North East 32. 9 per 1000 in the South East and South West.
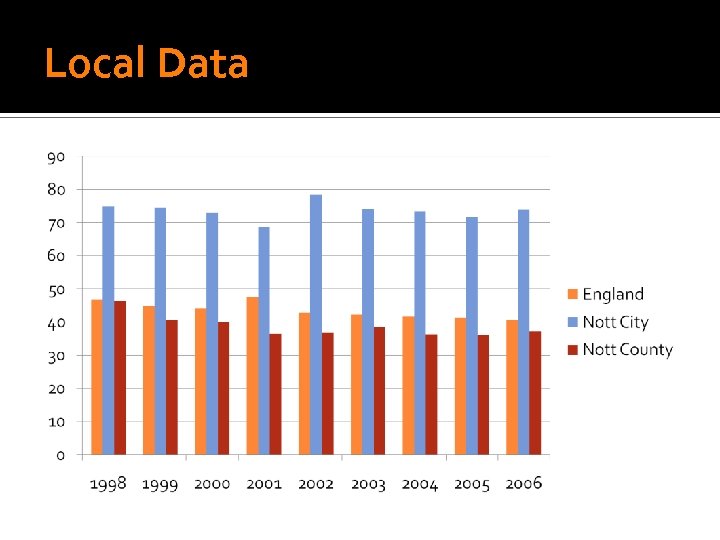
Local Data

Risk Factors The five factors which most significantly affect the likelihood of becoming a teenage mother or young father are: Own mother being a teenage mother Father coming from a socio-economic status of iv. or v. Having conduct disorder at the age of 10 Being in social housing at the age of 10 Having a poor reading ability at the age of 10 Most teenage parents express the view that they received less than satisfactory sex education at school and at home.
More risk and protective factors INCREASED RISK Black African and Caribbean, Bangladeshi, Pakistani, Muslim or traveller community (within or outside marriage) Having just had a baby or termination Deprived neighbourhood Being a looked-after child Family with low educational aspirations for their children Disliking school and/or low school attendance Mother having no educational qualifications Poor mental health Learning difficulties Domestic abuse and/or school bullying Being victims/witnesses of violence in the home Involvement in crime DECREASED RISK Chinese, Indian or Jewish community Good, and early, SRE in schools, and parents open to discussions about sex and relationships Youth-friendly sexual health advice service and youth service High educational aspirations and enjoyment in school Educational qualifications An adult in their life whom they trust

Warning Majority of cases teenage pregnancies are unplanned Over half of teenage pregnancies end in termination ‘Unplanned’ does not necessarily mean ‘unwanted’ Numerous young people conceive intentionally Many avoid the adverse outcomes to be discussed

Consequences for the Mother In pairs think of five outcomes for young mothers. Choose at least one from the following headings: Physical Psychological Social/financial

Consequences for the mother Majority of studies compare a young 16– 19 year-old age group with an older group Comparisons do not allow for differences in physical or psychological maturity over the range of the teenage years Retrospective/database studies Control for variety of confounding factors
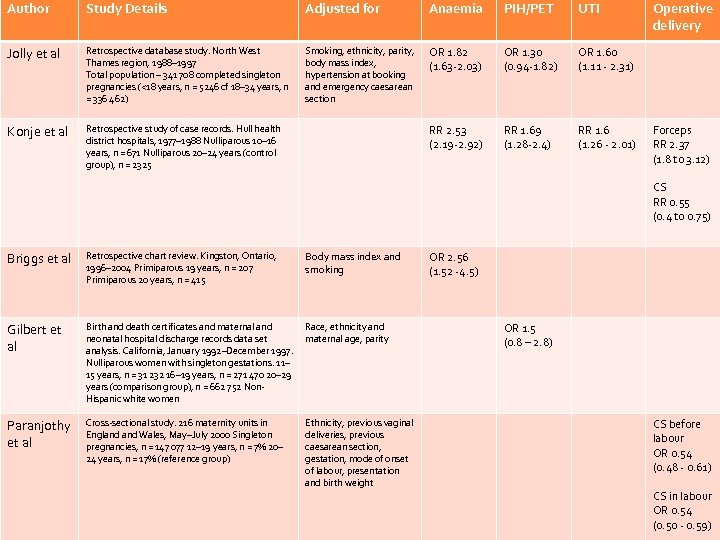
Author Study Details Adjusted for Anaemia PIH/PET UTI Jolly et al Retrospective database study. North West Thames region, 1988– 1997 Total population – 341 708 completed singleton pregnancies (<18 years, n = 5246 cf 18– 34 years, n = 336 462) Smoking, ethnicity, parity, body mass index, hypertension at booking and emergency caesarean section OR 1. 82 (1. 63 -2. 03) OR 1. 30 (0. 94 -1. 82) OR 1. 60 (1. 11 - 2. 31) Konje et al Retrospective study of case records. Hull health district hospitals, 1977– 1988 Nulliparous 10– 16 years, n = 671 Nulliparous 20– 24 years (control group), n = 2325 RR 2. 53 (2. 19 -2. 92) RR 1. 69 (1. 28 -2. 4) RR 1. 6 (1. 26 - 2. 01) Operative delivery Forceps RR 2. 37 (1. 8 to 3. 12) CS RR 0. 55 (0. 4 to 0. 75) Briggs et al Retrospective chart review. Kingston, Ontario, 1996– 2004 Primiparous 19 years, n = 207 Primiparous 20 years, n = 415 Body mass index and smoking Gilbert et al Birth and death certificates and maternal and neonatal hospital discharge records data set analysis. California, January 1992–December 1997. Nulliparous women with singleton gestations. 11– 15 years, n = 31 232 16– 19 years, n = 271 470 20– 29 years (comparison group), n = 662 752 Non. Hispanic white women Race, ethnicity and maternal age, parity Paranjothy et al Cross-sectional study. 216 maternity units in England Wales, May–July 2000 Singleton pregnancies, n = 147 077 12– 19 years, n = 7% 20– 24 years, n = 17% (reference group) Ethnicity, previous vaginal deliveries, previous caesarean section, gestation, mode of onset of labour, presentation and birth weight OR 2. 56 (1. 52 -4. 5) OR 1. 5 (0. 8 – 2. 8) CS before labour OR 0. 54 (0. 48 - 0. 61) CS in labour OR 0. 54 (0. 50 - 0. 59)
Obstetric Complications Increased risk of anaemia No increased risk of PIH/PET Lower CS rate but increased risk of instrumental delivery

Maternal Mortality In developing countries, complications from pregnancy and childbirth are the leading cause of death among teenagers. In the UK, maternal mortality is rare (14 per 100 000 maternities) 9. 9 per 100 000 maternities in <20 yrs Highly associated with deprivation maternal mortality is 46% higher in most compared to least deprived areas unemployment is associated with a sevenfold increased risk of maternal death Young maternal age is not a itself an identified risk factor for maternal mortality in the UK Deprivation is a risk factor for teenage pregnancy and maternal mortality

Maternal Morbidity Swedish population based cohort study using record linkage of census data with at least 30 years’ follow-up Compared with mothers aged 20– 24 years at first birth 70% increase in the risk of premature death for mothers aged 17 years or under at first birth 50% increase for those aged 18– 19 years Major causes of death associated with a previous teenage birth: Cervical cancer Ischaemic heart disease Suicide Death following violence, assault and homicide

Maternal Psychosocial Morbidity more deprivation more mental health difficulties lower levels of educational attainment more emotional and behavioural problems three times more likely to be living in poverty compared with mothers in their thirties less likely to complete their education and training restricted job opportunities, potentially reinforcing the cycle of deprivation and teenage pregnancy

Harm to the Baby? Risk factor for pre-term delivery low birth weight small for gestational age neonatal and infant mortality But confounding factors tobacco, alcohol or recreational drug use poor nutrition poor antenatal care attendance
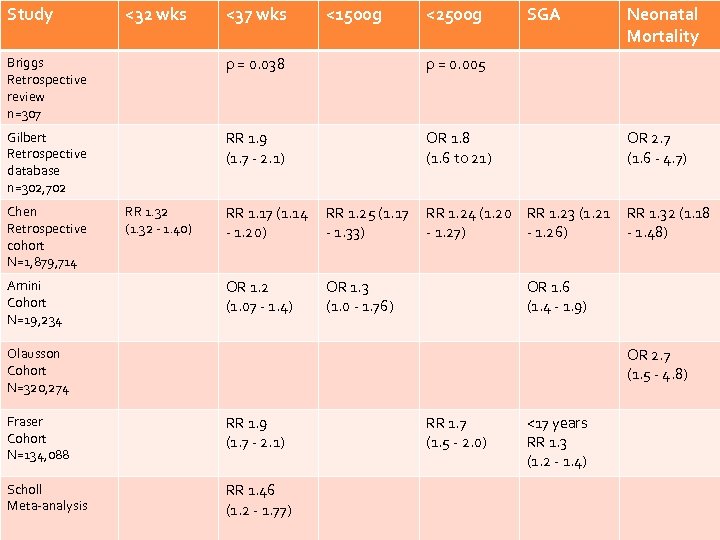
Study <32 wks <37 wks <1500 g <2500 g SGA Neonatal Mortality Briggs Retrospective review n=307 p = 0. 038 p = 0. 005 Gilbert Retrospective database n=302, 702 RR 1. 9 (1. 7 - 2. 1) OR 1. 8 (1. 6 to 21) OR 2. 7 (1. 6 - 4. 7) RR 1. 24 (1. 20 RR 1. 23 (1. 21 - 1. 27) - 1. 26) RR 1. 32 (1. 18 - 1. 48) Chen Retrospective cohort N=1, 879, 714 Amini Cohort N=19, 234 RR 1. 32 (1. 32 - 1. 40) RR 1. 17 (1. 14 - 1. 20) RR 1. 25 (1. 17 - 1. 33) OR 1. 2 (1. 07 - 1. 4) OR 1. 3 (1. 0 - 1. 76) OR 1. 6 (1. 4 - 1. 9) OR 2. 7 (1. 5 - 4. 8) Olausson Cohort N=320, 274 Fraser Cohort N=134, 088 RR 1. 9 (1. 7 - 2. 1) Scholl Meta-analysis RR 1. 46 (1. 2 - 1. 77) RR 1. 7 (1. 5 - 2. 0) <17 years RR 1. 3 (1. 2 - 1. 4)

Chen 2007 US study of births to women aged under 25 years of age After adjustment for confounding factors Teenage pregnancy was independently associated with the increased risks of state of birth maternal race marital status tobacco smoking alcohol use during pregnancy prenatal care status very pre-term delivery + pre-term delivery low birth weight + small for gestational age neonatal mortality Did not adequately control for employment status or occupation recreational drugs psychological and emotional stress during pregnancy

Other Morbidity 60 % higher rate of infant mortality Less likely to be breastfed Increased risk of poor nutrition Twice as likely to be hospitalised due to accidental injuries up to the age of five Teenage mothers x 5 more likely to smoke in pregnancy More likely to suffer from smoking-related illnesses Higher rates of maternal STIs

Harm to the Father? Young fathers have low socio-economic status backgrounds low levels of education and low earning potential By the age of 30, half of young fathers are no longer living with their first child and one fifth have never lived with their children. High levels of paternal engagement have positive effects on child development with reported lower levels of delinquency, higher IQ scores and fewer behavioural problems. Feel excluded from healthcare and professionals often know little about them

Harm to Society? Move away from family value based to sexualised society Teenage childbirth increasingly deviant from norm as age at first child increases Teenage mothers are often NEET Children with absent fathers in early childhood are more likely to be sexually active at a younger age and have a teenage pregnancy, therefore perpetuating the cycle Estimated cost to the NHS alone of pregnancy among under 18 year olds was over £ 63 million per year in 2002

Teenage Pregnancy Strategy UK government to set targets to halve the under-18 conception rate in England by 2010 from the 1998 rate of 46. 6 per 1000 Target not going to be met Most deprived areas have seen smallest gains

Interventions RCT showed reduction in preterm birth with teenage specific antenatal clinic Health visiting interventions shown to: Reduced CS rates Increased breast feeding Reduced smoking Fewer pregnancies Better developmental outcome

Supporting Teenage Parents Encourage early booking and attendance at AN clinics Healthy Start form, discuss the importance of eating well during pregnancy and ensure access to Healthy Start vitamins Future contraception method Refer young parents to appropriate mental health or social services, including groups to provide help with parenting, and youth-specific services in your local area Facilitate and encourage young fathers to be involved in antenatal care. Discuss postnatal depression with expectant young mothers and fathers Screening for anaemia Identify high risk behaviours that may influence their health Smoking Sexual health

Supporting Teenage Fathers Include them! Discuss his role in supporting his partner During labour and birth In choosing to breastfeed and give up smoking To avoid and cope with postnatal depression Youth-friendly appointment times Be aware of language: i. e. 'child's father’, not ‘husband’ or ‘partner’ unless status is known Encourage joint birth registration, leading to parental responsibility Let them know they can ask questions, however basic Ensure any correspondence is sent to both parents, and that two copies of any resources are available (books/leaflets etc. )

Supporting Child’s Development Join a local library to borrow books/attend events for free Visit websites that promote positive parenting such as the Parenting and Child Health site or the National Literacy Trust’s ‘Talk To Your Baby’ site (see links in the resources section) Visit the local children’s centre and join local parenting/play groups Talk to, play, dance and sing with their child as much as possible

Improving Financial Well-being Local Connexions services and Targeted Youth Support Benefits advice e. g. citizens advice, job centres Sure Start Children’s Centres Children’s Information Services The Healthy Start Programme (vouchers for milk, fruit and vegetables to families with children under four years old and/or pregnant women)
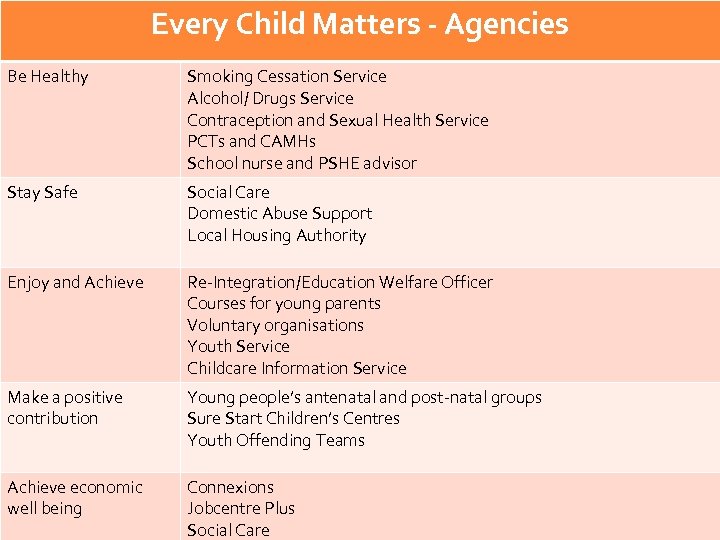
Every Child Matters - Agencies Be Healthy Smoking Cessation Service Alcohol/ Drugs Service Contraception and Sexual Health Service PCTs and CAMHs School nurse and PSHE advisor Stay Safe Social Care Domestic Abuse Support Local Housing Authority Enjoy and Achieve Re-Integration/Education Welfare Officer Courses for young parents Voluntary organisations Youth Service Childcare Information Service Make a positive contribution Young people’s antenatal and post-natal groups Sure Start Children’s Centres Youth Offending Teams Achieve economic well being Connexions Jobcentre Plus Social Care

Antenatal Care 83 % of pregnant teenagers did not attend antenatal classes and many had limited understanding of the progress of their pregnancies. Reasons may include: Taking time to come to terms with the pregnancy Chaotic lifestyles and frequent changes in address Timing and location of clinics/classes when young people are employed or in education Feeling out of place amongst older parents or in a group setting Fear of being judged or treated disrespectfully Prioritising other crisis issues (money, housing, relationships)

Final Task List six things that paediatricians can do to improve the health outcomes of young parents and their children

Summary UK teenage pregnancy rate is falling but not quickly enough to meet government target Many risk and protective factors but deprivation is main association Affects health of mother, child and father Teenage specific services, health visiting and other interventions show promise
468f0644242e01d9bb1c756fffa94e45.ppt