e45d6c6589a376e04b6d218eb11d2a12.ppt
- Количество слайдов: 58
 Team Form & Functions: From Multi-Disciplinary to Interprofessional Collaborative Geriatric Teams. Assessment & Educational Models Debra Fromm Faria Marla Berg-Weger V. Associate Professor, Social Work Professor, School of Social Work Co-Director Center for Excellence in Gerontological Social Work College at Brockport, State University of New York dffaria@brockport. edu Executive Director, Geriatric Education Center Saint Louis University bergwm@slu. edu Webinar October 23, 2012 The Presenters also wish to acknowledge a collaborative input for some of the health care slides by Assistant Professor Thomas Caprio, MD, MPH, FACP, University of Rochester Medical Center , School of Medicine, Division of Geriatrics
Team Form & Functions: From Multi-Disciplinary to Interprofessional Collaborative Geriatric Teams. Assessment & Educational Models Debra Fromm Faria Marla Berg-Weger V. Associate Professor, Social Work Professor, School of Social Work Co-Director Center for Excellence in Gerontological Social Work College at Brockport, State University of New York dffaria@brockport. edu Executive Director, Geriatric Education Center Saint Louis University bergwm@slu. edu Webinar October 23, 2012 The Presenters also wish to acknowledge a collaborative input for some of the health care slides by Assistant Professor Thomas Caprio, MD, MPH, FACP, University of Rochester Medical Center , School of Medicine, Division of Geriatrics
 Objectives 1. Define 2. 3. 4. Understand the roles of interprofessional team members 5. Provide resources for future use types of teams Multidisciplinary Interprofessional Transprofessional Describe the value of interprofessional geriatric assessment Introduce model of using interprofessional education in clinical settings and courses to prepare the next generation of interprofessional team members 2
Objectives 1. Define 2. 3. 4. Understand the roles of interprofessional team members 5. Provide resources for future use types of teams Multidisciplinary Interprofessional Transprofessional Describe the value of interprofessional geriatric assessment Introduce model of using interprofessional education in clinical settings and courses to prepare the next generation of interprofessional team members 2
 What are the differences and similarities with types of teams? The terms multidisciplinary, interprofessional and transdisciplinary often are used interchangeably. It is useful to understand definitions, and assess how our teams are functioning www. asha. org/uploaded. Files/aud/Team. Approac hes. pdf
What are the differences and similarities with types of teams? The terms multidisciplinary, interprofessional and transdisciplinary often are used interchangeably. It is useful to understand definitions, and assess how our teams are functioning www. asha. org/uploaded. Files/aud/Team. Approac hes. pdf
 Multidisciplinary Team Approach Professional Silos are common “A multidisciplinary approach to service delivery means that persons from several disciplines are involved in the delivery of services. The approach, however, is discipline-oriented with each team member responsible only for the activities related to his or her own discipline (Melvin, 1989; Rothberg, 1981). One team member is affected very little by the efforts of the other team members. . ” Melvin, J. L. (1989, April). Status report on interdisciplinary medical education. Archives of Physical Medicine and Rehabilitation, 70, 273– 276. Rothberg, J. (1981, August). The rehabilitation team: Future direction. Archives of Physical Medicine and Rehabilitation, 62, 407– 410. as cited in Catlett, C. & Halper, A. (1992, Summer). Team Approaches: Working Together to Improve Quality ASHA Quality Improvement Digest. http: //www. asha. org/uploaded. Files/aud/Team. Approaches. pdf
Multidisciplinary Team Approach Professional Silos are common “A multidisciplinary approach to service delivery means that persons from several disciplines are involved in the delivery of services. The approach, however, is discipline-oriented with each team member responsible only for the activities related to his or her own discipline (Melvin, 1989; Rothberg, 1981). One team member is affected very little by the efforts of the other team members. . ” Melvin, J. L. (1989, April). Status report on interdisciplinary medical education. Archives of Physical Medicine and Rehabilitation, 70, 273– 276. Rothberg, J. (1981, August). The rehabilitation team: Future direction. Archives of Physical Medicine and Rehabilitation, 62, 407– 410. as cited in Catlett, C. & Halper, A. (1992, Summer). Team Approaches: Working Together to Improve Quality ASHA Quality Improvement Digest. http: //www. asha. org/uploaded. Files/aud/Team. Approaches. pdf
 Interdisciplinary Team An interdisciplinary approach to service delivery requires Interaction among the disciplines. Not only are individuals from several disciplines working toward a common goal, but the team members have the additional responsibility of the group effort (Rothberg, 1981). Effective communication is required among those involved (Melvin, 1989). The team includes the patient/client and his/her family Melvin, J. L. (1989, April). Status report on interdisciplinary medical education. Archives of Physical Medicine and Rehabilitation, 70, 273– 276. Rothberg, J. (1981, August). The rehabilitation team: Future direction. Archives of Physical Medicine and Rehabilitation, 62, 407– 410. as cited in Catlett, C. & Halper, A. (1992, Summer). Team Approaches: Working Together to Improve Quality ASHA Quality Improvement Digest. http: //www. asha. org/uploaded. Files/aud/Team. Approaches. pdf
Interdisciplinary Team An interdisciplinary approach to service delivery requires Interaction among the disciplines. Not only are individuals from several disciplines working toward a common goal, but the team members have the additional responsibility of the group effort (Rothberg, 1981). Effective communication is required among those involved (Melvin, 1989). The team includes the patient/client and his/her family Melvin, J. L. (1989, April). Status report on interdisciplinary medical education. Archives of Physical Medicine and Rehabilitation, 70, 273– 276. Rothberg, J. (1981, August). The rehabilitation team: Future direction. Archives of Physical Medicine and Rehabilitation, 62, 407– 410. as cited in Catlett, C. & Halper, A. (1992, Summer). Team Approaches: Working Together to Improve Quality ASHA Quality Improvement Digest. http: //www. asha. org/uploaded. Files/aud/Team. Approaches. pdf
 Transdisciplinary Team Model “A transdisciplinary model includes the following components: • one person can perform professionals’ roles by providing services to the patient/client under the supervision of the individuals from the other disciplines involved. • Disciplines work together in the initial evaluation and care plan, but only one or two members actually provide the services. • Professionals are still accountable for areas related to their specific discipline and for training the team member delivering the service” (e. g. , ACT). Bailey, D. B. , & Wolery, M. (1989). Assessing Infants and Preschooler With Handicaps. Columbus, OH: Merrill Publishing Co. Connor, F. P. , Williamson, G. G. , & Stepp, J. M. (1978). Program Guide for Infants and Toddlers With Neuromotor and Other Developmental Disabilities. New York: Teachers College Press. as cited in Catlett, C. & Halper, A. (1992, Summer). Team Approaches: Working Together to Improve Quality ASHA Quality Improvement Digest. http: //www. asha. org/uploaded. Files/aud/Team. Approaches. pdf
Transdisciplinary Team Model “A transdisciplinary model includes the following components: • one person can perform professionals’ roles by providing services to the patient/client under the supervision of the individuals from the other disciplines involved. • Disciplines work together in the initial evaluation and care plan, but only one or two members actually provide the services. • Professionals are still accountable for areas related to their specific discipline and for training the team member delivering the service” (e. g. , ACT). Bailey, D. B. , & Wolery, M. (1989). Assessing Infants and Preschooler With Handicaps. Columbus, OH: Merrill Publishing Co. Connor, F. P. , Williamson, G. G. , & Stepp, J. M. (1978). Program Guide for Infants and Toddlers With Neuromotor and Other Developmental Disabilities. New York: Teachers College Press. as cited in Catlett, C. & Halper, A. (1992, Summer). Team Approaches: Working Together to Improve Quality ASHA Quality Improvement Digest. http: //www. asha. org/uploaded. Files/aud/Team. Approaches. pdf
 Example of Transdisciplinary Team in Behavioral Health Assertive Community Team (ACT) Evidence–Based Practice Model designed to provide treatment, rehabilitation and support services to individuals diagnosed with a severe mental illness whose needs have not been met with traditional mental health services ACT team: psychiatry, nursing, psychology, social work, substance abuse & vocational rehabilitation. Based on respective areas of expertise, team members collaborate to deliver integrated services of the recipients' choice, assist in making progress towards goals, adjust services over time to meet recipients' changing needs and goals. NYS Office of Mental Health, Assertive Community Treatment http: //bi. omh. ny. gov/act/index www. socialworkleadership. org
Example of Transdisciplinary Team in Behavioral Health Assertive Community Team (ACT) Evidence–Based Practice Model designed to provide treatment, rehabilitation and support services to individuals diagnosed with a severe mental illness whose needs have not been met with traditional mental health services ACT team: psychiatry, nursing, psychology, social work, substance abuse & vocational rehabilitation. Based on respective areas of expertise, team members collaborate to deliver integrated services of the recipients' choice, assist in making progress towards goals, adjust services over time to meet recipients' changing needs and goals. NYS Office of Mental Health, Assertive Community Treatment http: //bi. omh. ny. gov/act/index www. socialworkleadership. org
 Definition of Interprofessional Team Collaboration “ Interprofessional collaboration is a ‘partnership’ between a team of health providers and a client in a participatory collaborative and coordinated approach to shared decision making around health and social issues. ” Canadian Interprofessional Health Collaborative. A national interprofessional competency framework. February 2010. Available from: http: //www. cihc. ca/files/CIHC_IPCompetencies_Feb 1210. pdf
Definition of Interprofessional Team Collaboration “ Interprofessional collaboration is a ‘partnership’ between a team of health providers and a client in a participatory collaborative and coordinated approach to shared decision making around health and social issues. ” Canadian Interprofessional Health Collaborative. A national interprofessional competency framework. February 2010. Available from: http: //www. cihc. ca/files/CIHC_IPCompetencies_Feb 1210. pdf
 Interprofessional Collaborative Practice Principles A process by which professionals: Reflect on and develop ways of practicing that provides an integrated and cohesive answer to the needs of the client/family/population. Involves continuous interaction and knowledge sharing between professionals. Organized to solve or explore care and social issues while seeking to optimize the patient’s participation. Sources: Core Competencies for Interprofessional Collaborative Practice. Report of an Expert Panel, May 2011, Sponsored by the Interprofessional Education Consortium, p 8. http: //www. aacn. nche. edu/education-resources/ipecreport. pdf Morrison S. Working together: why bother with collaboration? Work Bas Learn Prim Care. 2007; 5: 65– 70.
Interprofessional Collaborative Practice Principles A process by which professionals: Reflect on and develop ways of practicing that provides an integrated and cohesive answer to the needs of the client/family/population. Involves continuous interaction and knowledge sharing between professionals. Organized to solve or explore care and social issues while seeking to optimize the patient’s participation. Sources: Core Competencies for Interprofessional Collaborative Practice. Report of an Expert Panel, May 2011, Sponsored by the Interprofessional Education Consortium, p 8. http: //www. aacn. nche. edu/education-resources/ipecreport. pdf Morrison S. Working together: why bother with collaboration? Work Bas Learn Prim Care. 2007; 5: 65– 70.
 Benefits of an Interprofessional Team Approach Interprofessional approaches to health and social care linked to improved clinical services and enhanced problem-solving (Mitchell, Parker& White, 2010) 10
Benefits of an Interprofessional Team Approach Interprofessional approaches to health and social care linked to improved clinical services and enhanced problem-solving (Mitchell, Parker& White, 2010) 10
 Characteristics of Effective Collaborative Interprofessional Teams Belief that the team is important to the outcome Open communication Equality of resources Respect Shared decision making All members feel valued
Characteristics of Effective Collaborative Interprofessional Teams Belief that the team is important to the outcome Open communication Equality of resources Respect Shared decision making All members feel valued
 Meet Mrs. C.
Meet Mrs. C.
 Mrs. C. Social History Data 92 -year-old woman lives alone Widowed 14 years ago; daughter lives locally and son lives in Arizona Worked for 15 years as an executive secretary at a local company Active in her faith community all her life Volunteers in a children’s reading program at the local library 13
Mrs. C. Social History Data 92 -year-old woman lives alone Widowed 14 years ago; daughter lives locally and son lives in Arizona Worked for 15 years as an executive secretary at a local company Active in her faith community all her life Volunteers in a children’s reading program at the local library 13
 Case Presentation - Mrs. C. Health History Multiple chronic health problems (Cardiac, Pulmonary, Diabetes, Arthritis) Hospitalized for shortness of breath and chest pain twice in the last 3 months 14
Case Presentation - Mrs. C. Health History Multiple chronic health problems (Cardiac, Pulmonary, Diabetes, Arthritis) Hospitalized for shortness of breath and chest pain twice in the last 3 months 14
 Acute Incident Falls at home paramedics arrive and find her with right leg pain and unable to walk Taken by ambulance to the hospital
Acute Incident Falls at home paramedics arrive and find her with right leg pain and unable to walk Taken by ambulance to the hospital
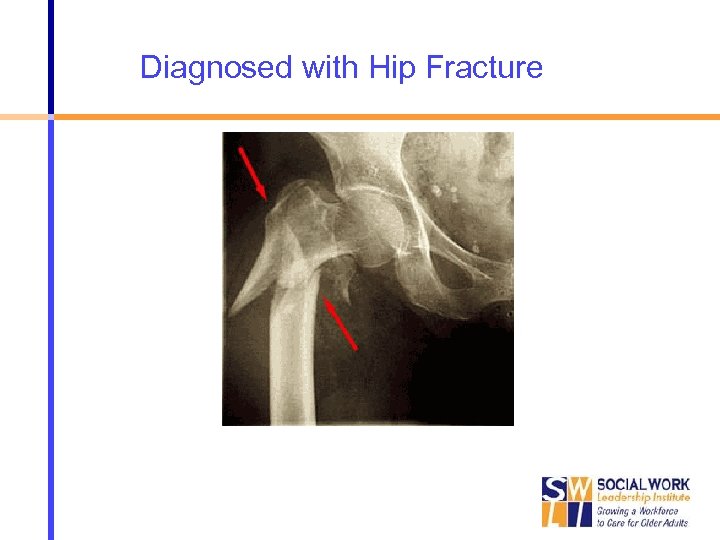 Diagnosed with Hip Fracture
Diagnosed with Hip Fracture
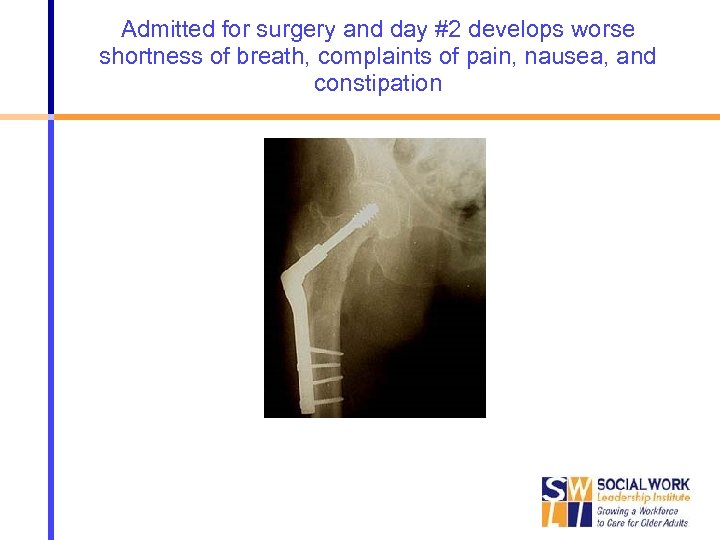 Admitted for surgery and day #2 develops worse shortness of breath, complaints of pain, nausea, and constipation
Admitted for surgery and day #2 develops worse shortness of breath, complaints of pain, nausea, and constipation
 Mrs. C. - Discharge Planning Fearful of falling, hard time using walker Discharged to a skilled nursing facility for rehabilitation 18
Mrs. C. - Discharge Planning Fearful of falling, hard time using walker Discharged to a skilled nursing facility for rehabilitation 18
 Mrs. C. - Rehab Update 4 weeks of rehabilitation: family is concerned about her returning home alone They report Mrs C. has a history of several falls at home without injury Family is concerned she is “taking her medications wrong” sometimes they notice “she is wearing clothes that have stains and appear dirty” 19
Mrs. C. - Rehab Update 4 weeks of rehabilitation: family is concerned about her returning home alone They report Mrs C. has a history of several falls at home without injury Family is concerned she is “taking her medications wrong” sometimes they notice “she is wearing clothes that have stains and appear dirty” 19
 Mrs. C. - Rehab Discharge Outcome Discharged back home after 6 weeks Plan includes: Home Care Aids 4 hours per day Weekly nursing visits Referral to outpatient PT Daughter plans on shopping weekly and setting up mediset
Mrs. C. - Rehab Discharge Outcome Discharged back home after 6 weeks Plan includes: Home Care Aids 4 hours per day Weekly nursing visits Referral to outpatient PT Daughter plans on shopping weekly and setting up mediset
 Mrs. C. - Five days later…. . Family brings Mrs C back to hospital Emergency Department Increased confusion, not eating/drinking Found on the floor where it appeared she had been for many hours after aide left in morning and daughter visited at night Admitted to the hospital with pneumonia, dehydration, and “failure to thrive” 21
Mrs. C. - Five days later…. . Family brings Mrs C back to hospital Emergency Department Increased confusion, not eating/drinking Found on the floor where it appeared she had been for many hours after aide left in morning and daughter visited at night Admitted to the hospital with pneumonia, dehydration, and “failure to thrive” 21
 With which health care teams did Mrs. C. interface? Hospital: Multi-Disciplinary? discipline-oriented with each team member responsible only for the activities related to his or her own discipline. Communicate with one another through chart documentation and unit reports. Rehabilitation Nursing Home Stay? Likely interdiscplinary / perhaps interprofessional Discharge Home? Multi-Disciplinary PCP for medical Care Home Care agency Outpatient PT clinic Family
With which health care teams did Mrs. C. interface? Hospital: Multi-Disciplinary? discipline-oriented with each team member responsible only for the activities related to his or her own discipline. Communicate with one another through chart documentation and unit reports. Rehabilitation Nursing Home Stay? Likely interdiscplinary / perhaps interprofessional Discharge Home? Multi-Disciplinary PCP for medical Care Home Care agency Outpatient PT clinic Family
 Mrs. C. ’s Story: Important to Assess how team function can improve across service sectors Next steps in management? How could this have been prevented? How can the team think about? Prior level of function at home Hospital management Rehabilitation course in nursing home Home Care Plan and safeguards What about: Cognitive & psychosocial strengths and challenges Family caregiving & interface with the formal care system Functional & Environmental Factors 23
Mrs. C. ’s Story: Important to Assess how team function can improve across service sectors Next steps in management? How could this have been prevented? How can the team think about? Prior level of function at home Hospital management Rehabilitation course in nursing home Home Care Plan and safeguards What about: Cognitive & psychosocial strengths and challenges Family caregiving & interface with the formal care system Functional & Environmental Factors 23
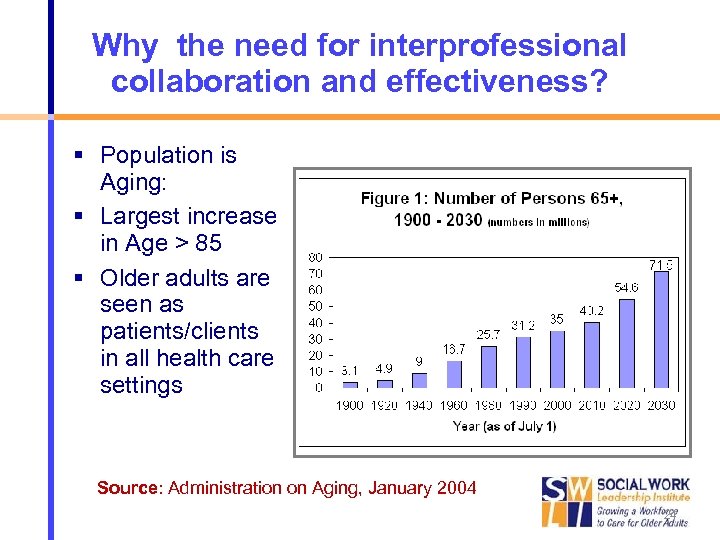 Why the need for interprofessional collaboration and effectiveness? Population is Aging: Largest increase in Age > 85 Older adults are seen as patients/clients in all health care settings Source: Administration on Aging, January 2004 24
Why the need for interprofessional collaboration and effectiveness? Population is Aging: Largest increase in Age > 85 Older adults are seen as patients/clients in all health care settings Source: Administration on Aging, January 2004 24
 Where are older adults interfacing with service providers? Home (independent in the community) Home (with Home Care Services) Independent or Senior Housing Assisted Living Facilities Adult Day Care Programs Long-Term Care Facilities (Nursing Homes) Rehabilitation Centers Hospitals Community Retail Providers (Pharmacy ) 25
Where are older adults interfacing with service providers? Home (independent in the community) Home (with Home Care Services) Independent or Senior Housing Assisted Living Facilities Adult Day Care Programs Long-Term Care Facilities (Nursing Homes) Rehabilitation Centers Hospitals Community Retail Providers (Pharmacy ) 25
 What challenges do older adults experience as they age? Disability (loss of function) Comorbidity (chronic medical conditions) Frailty (vulnerability) Multiple Losses (compounding effect) 26
What challenges do older adults experience as they age? Disability (loss of function) Comorbidity (chronic medical conditions) Frailty (vulnerability) Multiple Losses (compounding effect) 26
 Why is assessment important? Goal: decrease disability and dependence Identify “pre-clinical” disability Majority older adults live independently 50% Lifetime Risk of nursing home placement 27
Why is assessment important? Goal: decrease disability and dependence Identify “pre-clinical” disability Majority older adults live independently 50% Lifetime Risk of nursing home placement 27
 Geriatric Syndromes Broad categories of signs and symptoms common in the geriatric population Ø Ø Ø Vision impairment Hearing loss Incontinence Falls/Mobility Depression Memory disorders HELP! 28
Geriatric Syndromes Broad categories of signs and symptoms common in the geriatric population Ø Ø Ø Vision impairment Hearing loss Incontinence Falls/Mobility Depression Memory disorders HELP! 28
 What is geriatric assessment? Method to identify problems/challenges early Goal to maintain or improve FUNCTION Screen for common problems of aging (geriatric syndromes) Identifies the strengths/resilience of the individual and family system Performed by interdisciplinary/interprofessional team Focus on chronic disease management and effective resource utilization to enhance quality of life 29 *
What is geriatric assessment? Method to identify problems/challenges early Goal to maintain or improve FUNCTION Screen for common problems of aging (geriatric syndromes) Identifies the strengths/resilience of the individual and family system Performed by interdisciplinary/interprofessional team Focus on chronic disease management and effective resource utilization to enhance quality of life 29 *
 Geriatric Assessment: Interprofessional Team Interface Comprehensive assessment is performed by an interdisciplinary/interprofessional team Each team member’s professional domain knowledge is recognized. Collaborative team practices are central to the model. Allowing for contextual understanding of complex issues. Geriatricians Social Workers Patient/Family Neuropsychologists Nurses Pharmacists 30
Geriatric Assessment: Interprofessional Team Interface Comprehensive assessment is performed by an interdisciplinary/interprofessional team Each team member’s professional domain knowledge is recognized. Collaborative team practices are central to the model. Allowing for contextual understanding of complex issues. Geriatricians Social Workers Patient/Family Neuropsychologists Nurses Pharmacists 30
 Addressing Complexities Through an Interprofessional Approach Medicine Nursing Social Work Association of American Medical Colleges / John A. Hartford Foundation, Inc. July 2007 Consensus Conference on Competencies in Geriatrics Education Academic Medicine. 84(5): 604 -10, May 2009. John A. Hartford Foundation Institute for Geriatric Nursing, 2002 Geriatric Social Work Competency Scale II with Life-long Learning in Relationship to Leadership Skills Demonstrate within care plan appropriate intervention to promote function in response to change in ADLS and IADLS Conduct a comprehensive biopsychosocialspiritual assessment identifying older adults strengths and problems, social supports, social functioning, ADL and IADLs Interface of Geriatric Assess & describe Competencies baseline and current functional abilities in an older patient Functional (ADLs/IADLS) by Assessment collecting historical data and performing a confirmatory physical exam http: //www. pogoe. org/sites/defa ult/files/Minimum%20 Geri%2 0 Competencies%202. 0%20 w% 20 narr%20 Academ. Med%2039 -09_0. pdf http: //hartfordign. org/uplo ads/File/competencies. p df http: //www. pcssprimarycare. org/nsw/com petencies/competencies. php# 31
Addressing Complexities Through an Interprofessional Approach Medicine Nursing Social Work Association of American Medical Colleges / John A. Hartford Foundation, Inc. July 2007 Consensus Conference on Competencies in Geriatrics Education Academic Medicine. 84(5): 604 -10, May 2009. John A. Hartford Foundation Institute for Geriatric Nursing, 2002 Geriatric Social Work Competency Scale II with Life-long Learning in Relationship to Leadership Skills Demonstrate within care plan appropriate intervention to promote function in response to change in ADLS and IADLS Conduct a comprehensive biopsychosocialspiritual assessment identifying older adults strengths and problems, social supports, social functioning, ADL and IADLs Interface of Geriatric Assess & describe Competencies baseline and current functional abilities in an older patient Functional (ADLs/IADLS) by Assessment collecting historical data and performing a confirmatory physical exam http: //www. pogoe. org/sites/defa ult/files/Minimum%20 Geri%2 0 Competencies%202. 0%20 w% 20 narr%20 Academ. Med%2039 -09_0. pdf http: //hartfordign. org/uplo ads/File/competencies. p df http: //www. pcssprimarycare. org/nsw/com petencies/competencies. php# 31
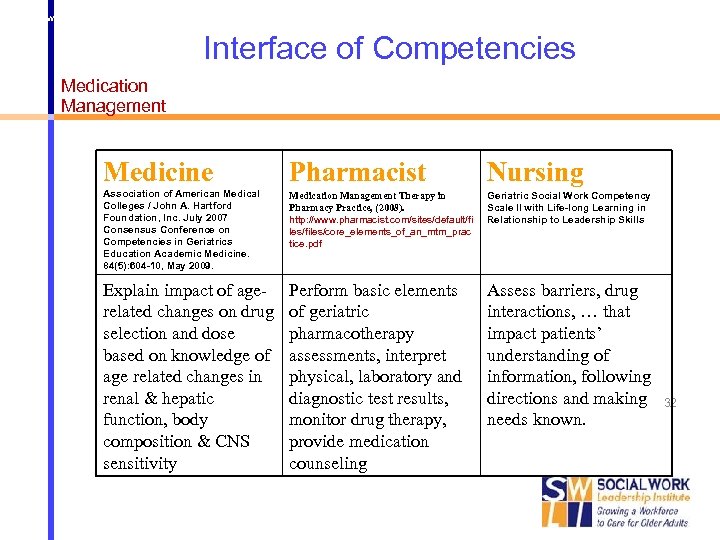 http: //www. pharmacist. com/sites/default/files/core_elements_of_an_mtm_practice. pdf Interface of Competencies Medication Management Medicine Pharmacist Nursing Association of American Medical Colleges / John A. Hartford Foundation, Inc. July 2007 Consensus Conference on Competencies in Geriatrics Education Academic Medicine. 84(5): 604 -10, May 2009. Medication Management Therapy in Pharmacy Practice, (2008). http: //www. pharmacist. com/sites/default/fi les/files/core_elements_of_an_mtm_prac tice. pdf Geriatric Social Work Competency Scale II with Life-long Learning in Relationship to Leadership Skills Explain impact of agerelated changes on drug selection and dose based on knowledge of age related changes in renal & hepatic function, body composition & CNS sensitivity Perform basic elements of geriatric pharmacotherapy assessments, interpret physical, laboratory and diagnostic test results, monitor drug therapy, provide medication counseling Assess barriers, drug interactions, … that impact patients’ understanding of information, following directions and making needs known. 32
http: //www. pharmacist. com/sites/default/files/core_elements_of_an_mtm_practice. pdf Interface of Competencies Medication Management Medicine Pharmacist Nursing Association of American Medical Colleges / John A. Hartford Foundation, Inc. July 2007 Consensus Conference on Competencies in Geriatrics Education Academic Medicine. 84(5): 604 -10, May 2009. Medication Management Therapy in Pharmacy Practice, (2008). http: //www. pharmacist. com/sites/default/fi les/files/core_elements_of_an_mtm_prac tice. pdf Geriatric Social Work Competency Scale II with Life-long Learning in Relationship to Leadership Skills Explain impact of agerelated changes on drug selection and dose based on knowledge of age related changes in renal & hepatic function, body composition & CNS sensitivity Perform basic elements of geriatric pharmacotherapy assessments, interpret physical, laboratory and diagnostic test results, monitor drug therapy, provide medication counseling Assess barriers, drug interactions, … that impact patients’ understanding of information, following directions and making needs known. 32
 Components of Geriatric Assessment Medical Functional Psychological Cognitive Social Economic Family Dynamics 33
Components of Geriatric Assessment Medical Functional Psychological Cognitive Social Economic Family Dynamics 33
 Dimensions of Geriatric Assessment: Medical Assessment Geriatric Syndromes: Past Medical and Surgical Histories Vision & Hearing Family History Incontinence Falls/Mobility Physical Exam Memory/Mood Review Medications: Nutrition Polypharmacy Pain “Bad Drugs” 34 *
Dimensions of Geriatric Assessment: Medical Assessment Geriatric Syndromes: Past Medical and Surgical Histories Vision & Hearing Family History Incontinence Falls/Mobility Physical Exam Memory/Mood Review Medications: Nutrition Polypharmacy Pain “Bad Drugs” 34 *
 Medication Review: Medicine, Nurse Practitioners and Pharmacy While Social Workers are not the primary profession dealing with medication review, observations from home assessments, knowledge of environmental issues such as finances can inform the interprofessional team Drug distribution and metabolism altered with aging Adverse Drug Reactions & Drug-Drug Interactions Number of medications OTC and herbal/dietary “Inappropriate” Meds: falls, urinary problems, delirium, hospitalizations 35
Medication Review: Medicine, Nurse Practitioners and Pharmacy While Social Workers are not the primary profession dealing with medication review, observations from home assessments, knowledge of environmental issues such as finances can inform the interprofessional team Drug distribution and metabolism altered with aging Adverse Drug Reactions & Drug-Drug Interactions Number of medications OTC and herbal/dietary “Inappropriate” Meds: falls, urinary problems, delirium, hospitalizations 35
 Functional Assessment: Activities of Daily Living (ADL) Dressing Toileting (+/- continence) Eating Bathing/Hygiene Mobility Ambulating (personal care) Transferring 36
Functional Assessment: Activities of Daily Living (ADL) Dressing Toileting (+/- continence) Eating Bathing/Hygiene Mobility Ambulating (personal care) Transferring 36
 Instrumental Activities of Daily Living (IADLs) Shopping Housekeeping (cleaning, laundry) Finances Cooking Using telephone Medications Transportation (driving, buses, etc. ) 37
Instrumental Activities of Daily Living (IADLs) Shopping Housekeeping (cleaning, laundry) Finances Cooking Using telephone Medications Transportation (driving, buses, etc. ) 37
 Psycho-Social * Social History Contextual understanding of who the patient is Presenting Challenges & Goals Patient perspective Family perspective Mental Health Assessment Coping skills, stressors, risk factors, depression screen 38 Social Functioning Assessment Social skills, social activity level, social supports Caregiver Needs/Levels of Stress
Psycho-Social * Social History Contextual understanding of who the patient is Presenting Challenges & Goals Patient perspective Family perspective Mental Health Assessment Coping skills, stressors, risk factors, depression screen 38 Social Functioning Assessment Social skills, social activity level, social supports Caregiver Needs/Levels of Stress
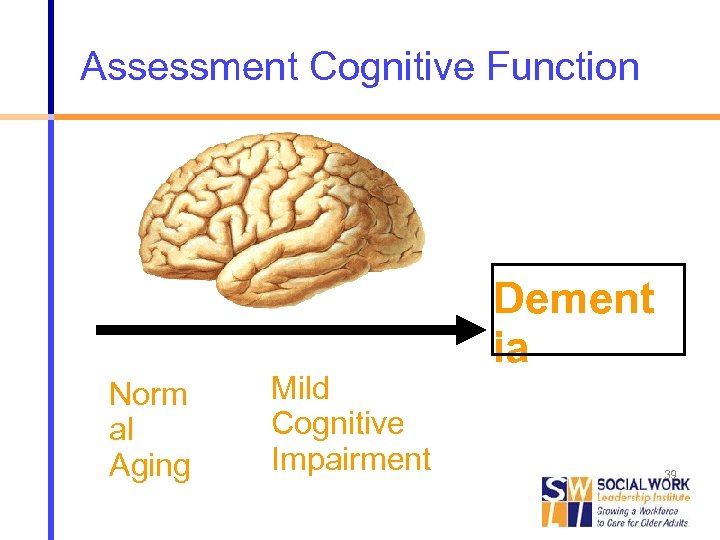 Assessment Cognitive Function Norm al Aging Mild Cognitive Impairment Dement ia Alzheimer ’s Disease 39
Assessment Cognitive Function Norm al Aging Mild Cognitive Impairment Dement ia Alzheimer ’s Disease 39
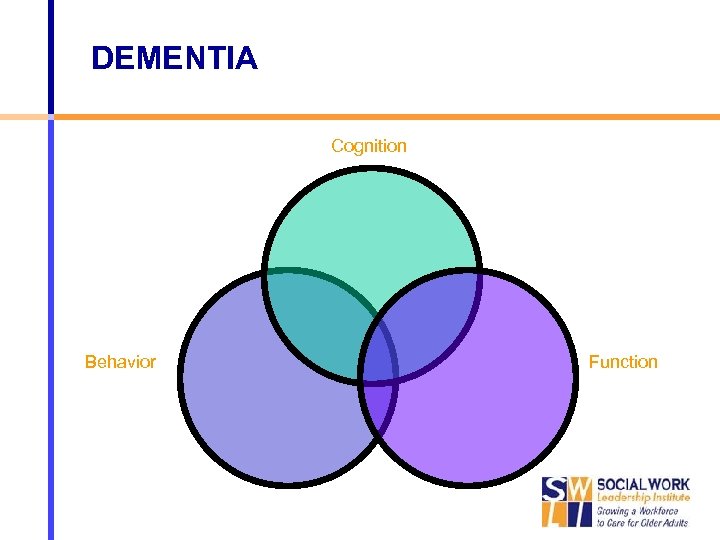 DEMENTIA Cognition Behavior Function
DEMENTIA Cognition Behavior Function
 Geriatric Assessments depend on context and location: Hospital – discharge planning Clinic/office – comprehensive assessment Nursing Home – improve or maintenance Home – mobility and safety Rehabilitation – improve function 41
Geriatric Assessments depend on context and location: Hospital – discharge planning Clinic/office – comprehensive assessment Nursing Home – improve or maintenance Home – mobility and safety Rehabilitation – improve function 41
 Core Areas Functional assessment (observations) Areas of concern (mobility impairment, weakness, ROM, falls, etc. ) Medical Conditions (dementia, CHF, etc. ) Rehabilitation tolerance and potential Psycho/Social Assessment 42
Core Areas Functional assessment (observations) Areas of concern (mobility impairment, weakness, ROM, falls, etc. ) Medical Conditions (dementia, CHF, etc. ) Rehabilitation tolerance and potential Psycho/Social Assessment 42
 Establishing Goals with Older Adults Individualized and person-centered Maintain independence longer Reduce stress or burden on caregivers Gradual or stepwise loss of function common in patients Some older adults’ function may “plateau” after an illness or injury Small improvements in physical function go a 43 long way (high “investment payoff”) *
Establishing Goals with Older Adults Individualized and person-centered Maintain independence longer Reduce stress or burden on caregivers Gradual or stepwise loss of function common in patients Some older adults’ function may “plateau” after an illness or injury Small improvements in physical function go a 43 long way (high “investment payoff”) *
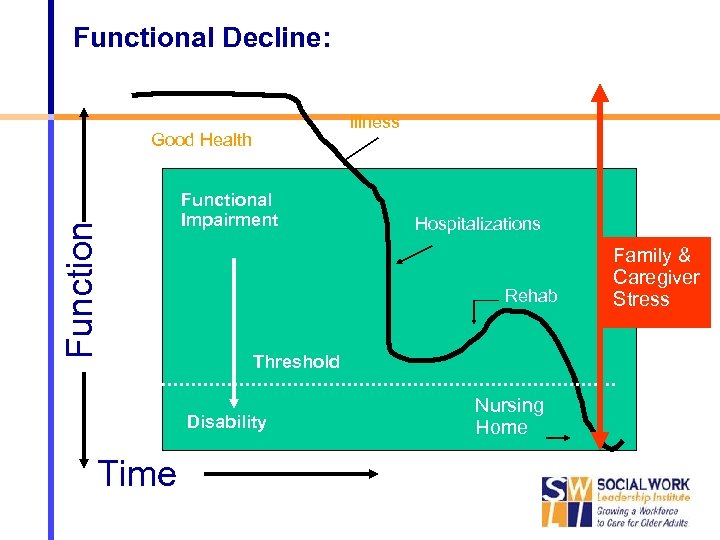 Functional Decline: Illness Function Good Health Functional Impairment Rehab Threshold Disability Time Hospitalizations Nursing Home Family & Caregiver Stress
Functional Decline: Illness Function Good Health Functional Impairment Rehab Threshold Disability Time Hospitalizations Nursing Home Family & Caregiver Stress
 Summary Interprofessional team collaboration improves communication and patient/client outcomes Geriatric assessment emphasizes functional status and the goal of maximizing independence and quality of life Loss of function is common but small improvements go a long way Person-Centered Approach 45
Summary Interprofessional team collaboration improves communication and patient/client outcomes Geriatric assessment emphasizes functional status and the goal of maximizing independence and quality of life Loss of function is common but small improvements go a long way Person-Centered Approach 45
 Next Steps: Workforce Preparation through Interprofessional Educational Models Interprofessional educational models Engaging students across professional disciplines Source: Core Competencies for Interprofessional Collaborative Practice. Report of an Expert Panel, May 2011, Sponsored by the Interprofessional Education Consortium, cover page picture. www. socialworkleadership. org
Next Steps: Workforce Preparation through Interprofessional Educational Models Interprofessional educational models Engaging students across professional disciplines Source: Core Competencies for Interprofessional Collaborative Practice. Report of an Expert Panel, May 2011, Sponsored by the Interprofessional Education Consortium, cover page picture. www. socialworkleadership. org
 What is Interprofessional Education? When “students” from two or more professional learn about, from, and with each other to enable effective collaboration and to improve health outcomes Framework for Action on Interprofessional Education & Collaborative Practice, World Health Organization, 2010 www. socialworkleadership. org
What is Interprofessional Education? When “students” from two or more professional learn about, from, and with each other to enable effective collaboration and to improve health outcomes Framework for Action on Interprofessional Education & Collaborative Practice, World Health Organization, 2010 www. socialworkleadership. org
 Educational Models to Prepare Competent Interprofessional Practitioners “The transformation envisioned would enable opportunities for health professions students to engage in interactive learning with those outside their profession as a routine part of their education” Source: Core Competencies for Interprofessional Collaborative Practice. Report of an Expert Panel, May 2011, Sponsored by the Interprofessional Education Consortium, p 3. http: //www. aacn. nche. edu/education-resources/ipecreport. pdf
Educational Models to Prepare Competent Interprofessional Practitioners “The transformation envisioned would enable opportunities for health professions students to engage in interactive learning with those outside their profession as a routine part of their education” Source: Core Competencies for Interprofessional Collaborative Practice. Report of an Expert Panel, May 2011, Sponsored by the Interprofessional Education Consortium, p 3. http: //www. aacn. nche. edu/education-resources/ipecreport. pdf
 Educational Strategies in Fostering Interprofessional Collaborative Practice Patient/family centered Community/population oriented Relationship focused Process oriented Linked to learning activities, educational strategies, and behavioral assessments that are developmentally appropriate for the learner Able to be integrated across the learning continuum Sensitive to the systems context/applicable across practice settings Applicable across professions Stated in language common and meaningful across the professions Source: Core Competencies for Interprofessional collaborative Outcome driven Practiceof an Expert Panel, May 2011, Sponsored by the Report Interprofessional Education Consortium http: //www. aacn. nche. edu/education-resources/ipecreport. pdf
Educational Strategies in Fostering Interprofessional Collaborative Practice Patient/family centered Community/population oriented Relationship focused Process oriented Linked to learning activities, educational strategies, and behavioral assessments that are developmentally appropriate for the learner Able to be integrated across the learning continuum Sensitive to the systems context/applicable across practice settings Applicable across professions Stated in language common and meaningful across the professions Source: Core Competencies for Interprofessional collaborative Outcome driven Practiceof an Expert Panel, May 2011, Sponsored by the Report Interprofessional Education Consortium http: //www. aacn. nche. edu/education-resources/ipecreport. pdf
 Competencies in the Care of Older Adults at the Completion of the Entry-level Health Profession Partnership for Health in Aging (PHA) Representing 10 Health Care Professions Developed broad competencies in six domains to provide a baseline for geriatrics and gerontology training To Access competencies: http: //www. americangeriatrics. org/files/docu ments/health_care_pros/PHA_Multidisc_Co mpetencies. pdf www. socialworkleadership. org Dentistry Medicine Nursing Nutrition Occupational Therapy Pharmacy Physical Therapy Physician Assistants Psychology Social Work
Competencies in the Care of Older Adults at the Completion of the Entry-level Health Profession Partnership for Health in Aging (PHA) Representing 10 Health Care Professions Developed broad competencies in six domains to provide a baseline for geriatrics and gerontology training To Access competencies: http: //www. americangeriatrics. org/files/docu ments/health_care_pros/PHA_Multidisc_Co mpetencies. pdf www. socialworkleadership. org Dentistry Medicine Nursing Nutrition Occupational Therapy Pharmacy Physical Therapy Physician Assistants Psychology Social Work
 Competencies in the Care of Older Adults at the Completion of the Entry-level Health Profession Domains: 1. Health Promotion and Safety 2. Evaluation and Assessment 3. Care Planning and Coordination Across the Care Spectrum 4. Interdisciplinary and Team Care 5. Caregiver Support 51 6. Healthcare Systems and Benefits Source: Partnership for Health in Aging Workgroup on Multidisciplinary Competencies in Geriatrics http: //www. americangeriatrics. org/files/documents/health_care_pros/P HA_Multidisc_Competencies. pdf
Competencies in the Care of Older Adults at the Completion of the Entry-level Health Profession Domains: 1. Health Promotion and Safety 2. Evaluation and Assessment 3. Care Planning and Coordination Across the Care Spectrum 4. Interdisciplinary and Team Care 5. Caregiver Support 51 6. Healthcare Systems and Benefits Source: Partnership for Health in Aging Workgroup on Multidisciplinary Competencies in Geriatrics http: //www. americangeriatrics. org/files/documents/health_care_pros/P HA_Multidisc_Competencies. pdf
 Endorsements Competencies in the Care of Older Adults at the Completion of the Entry-level Health Profession Alliance for Aging Research American Academy of Nursing – Expert Panel on Aging* Association of Directors of Geriatric Academic Programs Association for Gerontology in Higher Education American Academy of Physician Assistants Council on Social Work Education American Assisted Living Nurses Association* American Association of Colleges of Pharmacy Gerontological Advanced Practice Nurses Association* American Association for Geriatric Psychiatry Gerontological Society of American Association for Long Term Care Nursing* The Hartford Institute for Geriatric Nursing* American Association of Nurse Assessment Coordinators* National Association for Geriatric Education National Association of Geriatric Education Centers American College of Clinical Pharmacy American Dental Association National Association of Directors of Nursing Administration in Long Term Care* American Dietetic Association National Association of Professional Geriatric Care Managers American Geriatrics Society National Gerontological Nursing Association* American Occupational Therapy Association American Pharmacists Association New York Academy of Medicine/Social Work Leadership Institute American Physical Therapy Association PHI – Quality Care through Quality Jobs American Society on Aging American Society of Consultant Pharmacists www. socialworkleadership. org
Endorsements Competencies in the Care of Older Adults at the Completion of the Entry-level Health Profession Alliance for Aging Research American Academy of Nursing – Expert Panel on Aging* Association of Directors of Geriatric Academic Programs Association for Gerontology in Higher Education American Academy of Physician Assistants Council on Social Work Education American Assisted Living Nurses Association* American Association of Colleges of Pharmacy Gerontological Advanced Practice Nurses Association* American Association for Geriatric Psychiatry Gerontological Society of American Association for Long Term Care Nursing* The Hartford Institute for Geriatric Nursing* American Association of Nurse Assessment Coordinators* National Association for Geriatric Education National Association of Geriatric Education Centers American College of Clinical Pharmacy American Dental Association National Association of Directors of Nursing Administration in Long Term Care* American Dietetic Association National Association of Professional Geriatric Care Managers American Geriatrics Society National Gerontological Nursing Association* American Occupational Therapy Association American Pharmacists Association New York Academy of Medicine/Social Work Leadership Institute American Physical Therapy Association PHI – Quality Care through Quality Jobs American Society on Aging American Society of Consultant Pharmacists www. socialworkleadership. org
 Lessons Learned…. Social workers are experts on interprofessional collaboration so should be at the forefront Review the Core Competencies for Interprofessional Collaborative Practice http: //www. aacn. nche. edu/education-resources/ipecreport. pdf Utilize the Partnership for Health and Aging (PHA) Core Competencies to establish dialogue with other professions in exploring interprofessional educational opportunities Remember: Interprofessional Education as a model is a long term “process” Seek funding www. socialworkleadership. org
Lessons Learned…. Social workers are experts on interprofessional collaboration so should be at the forefront Review the Core Competencies for Interprofessional Collaborative Practice http: //www. aacn. nche. edu/education-resources/ipecreport. pdf Utilize the Partnership for Health and Aging (PHA) Core Competencies to establish dialogue with other professions in exploring interprofessional educational opportunities Remember: Interprofessional Education as a model is a long term “process” Seek funding www. socialworkleadership. org
 Getting Started…. Determine your goals for interprofessional education Gain support from university leadership at all levels Conduct syllabus audit to identify strengths and areas for change related to interprofessional content Document and promote the interprofessional collaboration strengths of the social work profession www. socialworkleadership. org
Getting Started…. Determine your goals for interprofessional education Gain support from university leadership at all levels Conduct syllabus audit to identify strengths and areas for change related to interprofessional content Document and promote the interprofessional collaboration strengths of the social work profession www. socialworkleadership. org
 Getting started… Curricular interventions: Integration into existing courses (including practicum seminar) Cross-listing courses Co-teaching courses Certificate/minor/specialization If your university has no health professions, consider reaching out to the community www. socialworkleadership. org
Getting started… Curricular interventions: Integration into existing courses (including practicum seminar) Cross-listing courses Co-teaching courses Certificate/minor/specialization If your university has no health professions, consider reaching out to the community www. socialworkleadership. org
 Resources: Interprofessional Teams, Assessment & Instruction Tools King, G. , Shaw, L. , Orchard, C. , & Miller, S. (2010). The interprofessional socialization and valuing scale: A tool for evaluating the shift toward collaborative care approaches in health care settings. (35 ed. , pp. 77 -85). IOS Press. Team Fitness Test (GITT) Geriatric Interprofessional Team Tools) available www. gittprogram. org/files/team_fitness_test. doc Models of Care and Inter-Professional Care Related to Complex Care of Older Adults by Sharon Stahl Wexler pdf download available at : hartfordign. org/uploads/File/. . . /gnec_interdisciplinary_care. pdf GITT video on You Tube available: available at http: //www. youtube. com/watch? v=Yrp. Pcgk 99 l 8 Interprofessional Care and Training ( Pharmacy & Medicine) University of Pittsburgh available at http: //www. youtube. com/watch? v=OTq. Jxne. LRt. Q www. socialworkleadership. org
Resources: Interprofessional Teams, Assessment & Instruction Tools King, G. , Shaw, L. , Orchard, C. , & Miller, S. (2010). The interprofessional socialization and valuing scale: A tool for evaluating the shift toward collaborative care approaches in health care settings. (35 ed. , pp. 77 -85). IOS Press. Team Fitness Test (GITT) Geriatric Interprofessional Team Tools) available www. gittprogram. org/files/team_fitness_test. doc Models of Care and Inter-Professional Care Related to Complex Care of Older Adults by Sharon Stahl Wexler pdf download available at : hartfordign. org/uploads/File/. . . /gnec_interdisciplinary_care. pdf GITT video on You Tube available: available at http: //www. youtube. com/watch? v=Yrp. Pcgk 99 l 8 Interprofessional Care and Training ( Pharmacy & Medicine) University of Pittsburgh available at http: //www. youtube. com/watch? v=OTq. Jxne. LRt. Q www. socialworkleadership. org
 Resources: Interprofessional Teams, Assessment & Instruction Tools Online training module on Interprofessional Geriatric Assessment available from the Finger Lakes Geriatric Center (Includes Social Work) http: //www. nptrainingworks. com/flgec The Center for Interprofessional Education and Research, Saint Louis University ipe. slu. edu The National Coordinating Center for Interprofessional Education and Collaborative Practice, University of Minnesota For information on this new project, contact: Barbara F. Brandt; brandt@umn. edu; 612/625 -3972 www. socialworkleadership. org
Resources: Interprofessional Teams, Assessment & Instruction Tools Online training module on Interprofessional Geriatric Assessment available from the Finger Lakes Geriatric Center (Includes Social Work) http: //www. nptrainingworks. com/flgec The Center for Interprofessional Education and Research, Saint Louis University ipe. slu. edu The National Coordinating Center for Interprofessional Education and Collaborative Practice, University of Minnesota For information on this new project, contact: Barbara F. Brandt; brandt@umn. edu; 612/625 -3972 www. socialworkleadership. org
 Resources: Interprofessional Teams, Assessment & Instruction Tools American Association of Colleges of Pharmacy (AACP)* http: //www. aacp. org/resources/education/Pages/IPEC. aspx *See Core Competencies for Interprofessional Education Framework for Action on Interprofessional Education & Collaborative Practice http: //www. who. int/hrh/resources/framework_action/en/ www. socialworkleadership. org
Resources: Interprofessional Teams, Assessment & Instruction Tools American Association of Colleges of Pharmacy (AACP)* http: //www. aacp. org/resources/education/Pages/IPEC. aspx *See Core Competencies for Interprofessional Education Framework for Action on Interprofessional Education & Collaborative Practice http: //www. who. int/hrh/resources/framework_action/en/ www. socialworkleadership. org


