047147c2704975761e18ab6770c4652f.ppt
- Количество слайдов: 192
 #teachproject Good Morning! Welcome to DAY 3 #teachproject 1
#teachproject Good Morning! Welcome to DAY 3 #teachproject 1
 Were you able to complete the Values Check #2 exercise last night? a. b. c. #teachproject Yes No I meant to, but was busy doing other things. 2
Were you able to complete the Values Check #2 exercise last night? a. b. c. #teachproject Yes No I meant to, but was busy doing other things. 2
 Values Exercise # 2 Choose the answer closest to yours : “Women smoke because _______”? a. b. c. d. e. #teachproject They think it’s feminine They want to control their weight They love to smoke It helps their stress levels Other 4
Values Exercise # 2 Choose the answer closest to yours : “Women smoke because _______”? a. b. c. d. e. #teachproject They think it’s feminine They want to control their weight They love to smoke It helps their stress levels Other 4
 Values Exercise # 2 Choose the answer closest to yours : “Tobacco manufacturers are _______”? a. b. c. d. e. #teachproject Too powerful Gazillionaires Killing millions of people every year Coercing children and youth to smoke through their advertising campaigns Other 6
Values Exercise # 2 Choose the answer closest to yours : “Tobacco manufacturers are _______”? a. b. c. d. e. #teachproject Too powerful Gazillionaires Killing millions of people every year Coercing children and youth to smoke through their advertising campaigns Other 6
 Specific Populations and Tobacco Use #teachproject 7
Specific Populations and Tobacco Use #teachproject 7
 Learning Objectives • • #teachproject Increased salient factors in different populations. Enhanced skills at applying effective cessation. 8
Learning Objectives • • #teachproject Increased salient factors in different populations. Enhanced skills at applying effective cessation. 8
 Introduction (1): Defining Special Populations • Defined as having 1 or more of: – T: Lack of prospective, longitudinal treatment trials. – A: Less access to treatments, and/or – D: Disproportionate tobacco-related health disparities, and/or – V: Increased vulnerability to addiction, and/or – P: >10% higher smoking prevalence than the general population of smokers, and/or Adapted from: Borrelli B. (2010). Journal of Consulting and Clinical Psychology, 78(1), 1– 12 #teachproject
Introduction (1): Defining Special Populations • Defined as having 1 or more of: – T: Lack of prospective, longitudinal treatment trials. – A: Less access to treatments, and/or – D: Disproportionate tobacco-related health disparities, and/or – V: Increased vulnerability to addiction, and/or – P: >10% higher smoking prevalence than the general population of smokers, and/or Adapted from: Borrelli B. (2010). Journal of Consulting and Clinical Psychology, 78(1), 1– 12 #teachproject
 Introduction (2) • Historically neglected • Multiple barriers exist • Complex associations, yet: – Robust, – Reproducible, – Clinically significant Els & Kunyk (2008). Smoking Cessation Rounds, 2(2). #teachproject
Introduction (2) • Historically neglected • Multiple barriers exist • Complex associations, yet: – Robust, – Reproducible, – Clinically significant Els & Kunyk (2008). Smoking Cessation Rounds, 2(2). #teachproject
 Why Focus on Specific Populations? • • • Mental health issues Medical issues Addictions Gambling disorders People who are homeless or underhoused • Older Adults #teachproject • • LGBTTTIQQ persons Youth Pregnant women Incarcerated individuals • Military recruits • Ethno-cultural groups • Aboriginal Persons 11
Why Focus on Specific Populations? • • • Mental health issues Medical issues Addictions Gambling disorders People who are homeless or underhoused • Older Adults #teachproject • • LGBTTTIQQ persons Youth Pregnant women Incarcerated individuals • Military recruits • Ethno-cultural groups • Aboriginal Persons 11
 Brief Focus on Selected Populations (1) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Indigenous Peoples
Brief Focus on Selected Populations (1) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Indigenous Peoples
 In which type of disorder would we see the highest rate of smoking prevalence? a. Anxiety disorder b. Major depression c. Bi-polar disorder d. Schizophrenia e. Personality disorders #teachproject 13
In which type of disorder would we see the highest rate of smoking prevalence? a. Anxiety disorder b. Major depression c. Bi-polar disorder d. Schizophrenia e. Personality disorders #teachproject 13
 Tobacco and Mental Illness (1) • Mental illnesses associated with higher rates: • Schizophrenia • Major mood disorders – Depression – Mania / Bipolar illness • Alcohol use • Other substance-related disorders • Anxiety disorders • Personality disorders Lasser et al. (2000). JAMA, 284(20): 2606 -10. Kalman et al. (2005) Am J Addict 14(2): 106 -23. #teachproject 14
Tobacco and Mental Illness (1) • Mental illnesses associated with higher rates: • Schizophrenia • Major mood disorders – Depression – Mania / Bipolar illness • Alcohol use • Other substance-related disorders • Anxiety disorders • Personality disorders Lasser et al. (2000). JAMA, 284(20): 2606 -10. Kalman et al. (2005) Am J Addict 14(2): 106 -23. #teachproject 14
 Tobacco and Mental Illness (2) • • High prevalence and high consumption. Unique topography and variables. Increased morbidity and mortality. Treatment guidelines available Mc. Clave et al. (2010). Am J Public Health, 100: 2464 -72. #teachproject
Tobacco and Mental Illness (2) • • High prevalence and high consumption. Unique topography and variables. Increased morbidity and mortality. Treatment guidelines available Mc. Clave et al. (2010). Am J Public Health, 100: 2464 -72. #teachproject
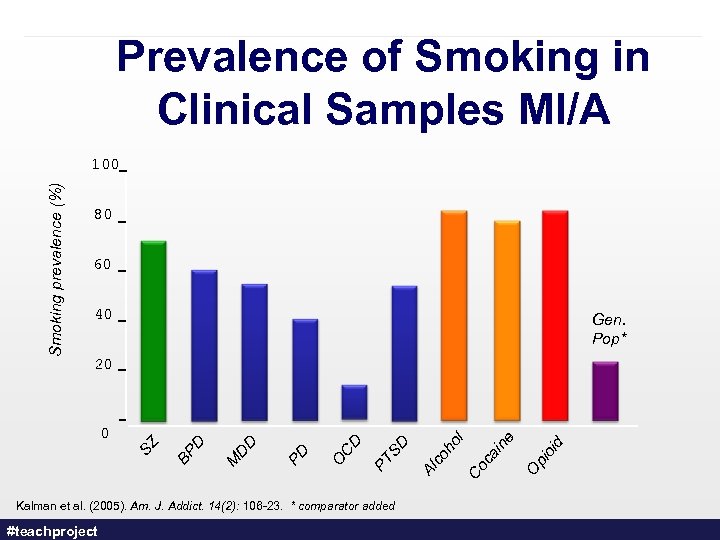 Prevalence of Smoking in Clinical Samples MI/A 80 60 40 Gen. Pop* Kalman et al. (2005). Am. J. Addict. 14(2): 106 -23. * comparator added #teachproject id pi o O l Co ca in e Al co ho SD PT CD O PD DD M BP 0 D 20 SZ Smoking prevalence (%) 100
Prevalence of Smoking in Clinical Samples MI/A 80 60 40 Gen. Pop* Kalman et al. (2005). Am. J. Addict. 14(2): 106 -23. * comparator added #teachproject id pi o O l Co ca in e Al co ho SD PT CD O PD DD M BP 0 D 20 SZ Smoking prevalence (%) 100
 I have, or my organization has, cessation services available for specific populations: a. We are structured to be accessible to a range of populations. b. We are accessible to a few specific populations on an as-needed basis. c. I am not sure what is available. d. Limited cessation services are available for specific populations. e. No services available #teachproject 17
I have, or my organization has, cessation services available for specific populations: a. We are structured to be accessible to a range of populations. b. We are accessible to a few specific populations on an as-needed basis. c. I am not sure what is available. d. Limited cessation services are available for specific populations. e. No services available #teachproject 17
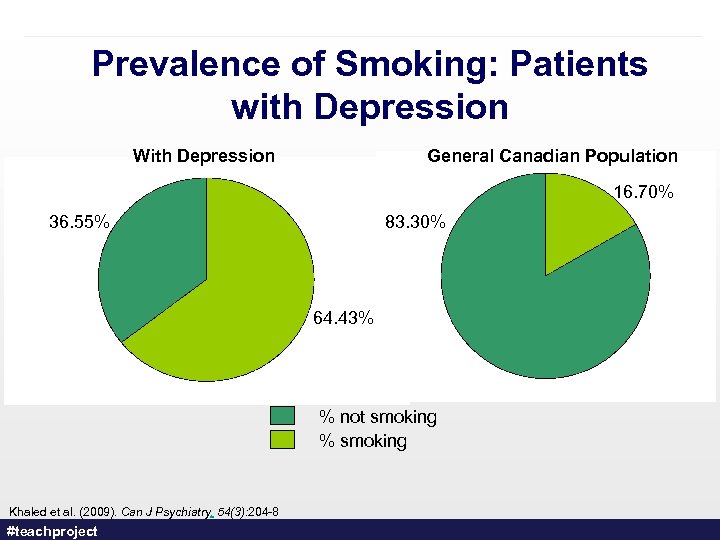 Prevalence of Smoking: Patients with Depression With Depression General Canadian Population 16. 70% 36. 55% 83. 30% 64. 43% % not smoking % smoking Khaled et al. (2009). Can J Psychiatry. 54(3): 204 -8 #teachproject 18
Prevalence of Smoking: Patients with Depression With Depression General Canadian Population 16. 70% 36. 55% 83. 30% 64. 43% % not smoking % smoking Khaled et al. (2009). Can J Psychiatry. 54(3): 204 -8 #teachproject 18
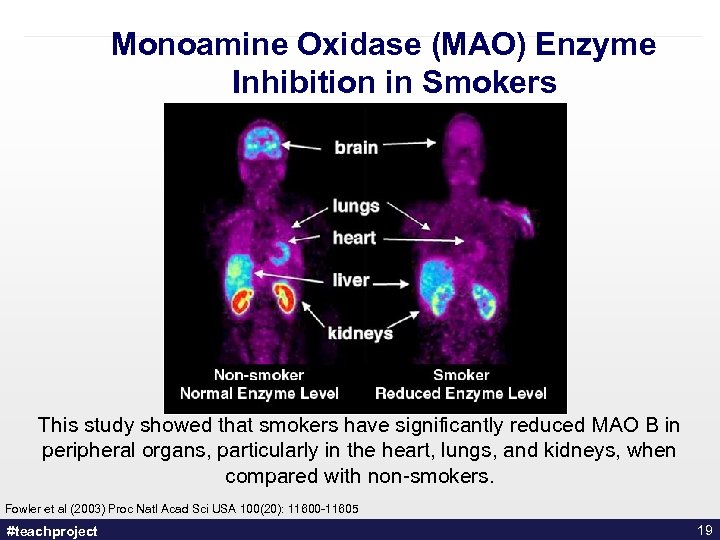 Monoamine Oxidase (MAO) Enzyme Inhibition in Smokers This study showed that smokers have significantly reduced MAO B in peripheral organs, particularly in the heart, lungs, and kidneys, when compared with non-smokers. Fowler et al (2003) Proc Natl Acad Sci USA 100(20): 11600 -11605 #teachproject 19
Monoamine Oxidase (MAO) Enzyme Inhibition in Smokers This study showed that smokers have significantly reduced MAO B in peripheral organs, particularly in the heart, lungs, and kidneys, when compared with non-smokers. Fowler et al (2003) Proc Natl Acad Sci USA 100(20): 11600 -11605 #teachproject 19
 Smoking and Depression Tobacco smoke exposure is associated with a marked reduction in brain MAO A, which suggests that MAO A inhibition needs to be considered as a potential contributing variable in the high rate of smoking in depression. Fowler et al. (1996). Proc Natl Acad Sci USA 93: 14065 -14069 #teachproject 20
Smoking and Depression Tobacco smoke exposure is associated with a marked reduction in brain MAO A, which suggests that MAO A inhibition needs to be considered as a potential contributing variable in the high rate of smoking in depression. Fowler et al. (1996). Proc Natl Acad Sci USA 93: 14065 -14069 #teachproject 20
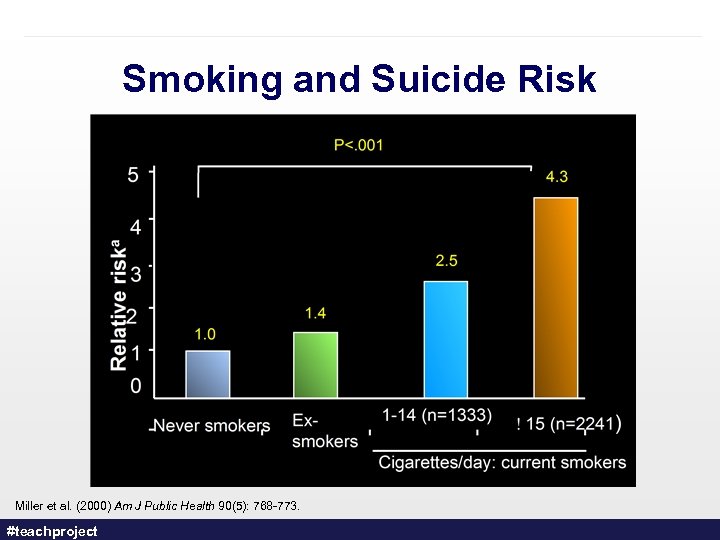 Smoking and Suicide Risk Miller et al. (2000) Am J Public Health 90(5): 768 -773. #teachproject
Smoking and Suicide Risk Miller et al. (2000) Am J Public Health 90(5): 768 -773. #teachproject
 Smoking and Mood Disorders – Etiological explanations vary: 1. MAO 2. Nicotine withdrawal 3. Caffeine 4. Pre-existing psychopathology – Suicide risk – Treatment Mackay J. et al. , (2006). The Tobacco Atlas 2 nd ed. Tonstad S & Els C. (2010). Clinical Medical Insights Therapeutics, 2: 681 -695. #teachproject
Smoking and Mood Disorders – Etiological explanations vary: 1. MAO 2. Nicotine withdrawal 3. Caffeine 4. Pre-existing psychopathology – Suicide risk – Treatment Mackay J. et al. , (2006). The Tobacco Atlas 2 nd ed. Tonstad S & Els C. (2010). Clinical Medical Insights Therapeutics, 2: 681 -695. #teachproject
 Treatment Implications • • 1) 2) 3) NRT 1 Bupropion 2 Atypical antipsychotics 1 Varenicline 3 George, Ziedonis, et al. (2000). Am J Psychiatry, 157 (11): 1835 -42. George, Vessicchio, et al. (2002). Biological Psychiatry, 52(1): 53 – 61. Smith, Lindenmayer, Davis, et al. (2009). Schizophrenia Research, 110: 149 -155. #teachproject 23
Treatment Implications • • 1) 2) 3) NRT 1 Bupropion 2 Atypical antipsychotics 1 Varenicline 3 George, Ziedonis, et al. (2000). Am J Psychiatry, 157 (11): 1835 -42. George, Vessicchio, et al. (2002). Biological Psychiatry, 52(1): 53 – 61. Smith, Lindenmayer, Davis, et al. (2009). Schizophrenia Research, 110: 149 -155. #teachproject 23
 Safety Considerations • History of Depression: • • High prevalence of depressed mood when quitting Need aggressive monitoring and treatment Vigilance for up to 6 months after quitting Beck Depression Inventory, consultation with psychiatrist • Depression is a predictor of relapse Wilhelm, Wedgwood et al. (2005). Drug and Alcohol Review, 25, 97 – 107. #teachproject 24
Safety Considerations • History of Depression: • • High prevalence of depressed mood when quitting Need aggressive monitoring and treatment Vigilance for up to 6 months after quitting Beck Depression Inventory, consultation with psychiatrist • Depression is a predictor of relapse Wilhelm, Wedgwood et al. (2005). Drug and Alcohol Review, 25, 97 – 107. #teachproject 24
 Anxiety • Rates of smoking 2 x greater then general population • Range 19. 2 – 56% • Panic Disorder 40% • PTSD 63% • Nicotine is anxiogenic • Lower anxiety within 2 weeks of quitting Kalman et al. (2005). Am. J. Addict. 14(2): 106 -23. * comparator added #teachproject 25
Anxiety • Rates of smoking 2 x greater then general population • Range 19. 2 – 56% • Panic Disorder 40% • PTSD 63% • Nicotine is anxiogenic • Lower anxiety within 2 weeks of quitting Kalman et al. (2005). Am. J. Addict. 14(2): 106 -23. * comparator added #teachproject 25
 Gambling • Strong association • 45% tobacco prevalence in Ontario among problem gamblers 1 • Limited empirical evidence • Systemic approaches, e. g. bans, have little impact on monetary profits 2 1. Ontario Tobacco Research Unit (2010). Monitoring and Evaluation Series, Vol. 14/15(2). 2. Glantz & Wilson-Loots (2003). Tob Control, 12(4): 411 -3. #teachproject
Gambling • Strong association • 45% tobacco prevalence in Ontario among problem gamblers 1 • Limited empirical evidence • Systemic approaches, e. g. bans, have little impact on monetary profits 2 1. Ontario Tobacco Research Unit (2010). Monitoring and Evaluation Series, Vol. 14/15(2). 2. Glantz & Wilson-Loots (2003). Tob Control, 12(4): 411 -3. #teachproject
 Smoking and Schizophrenia – Impact on MSE – Impact on Medication – Cessation interventions Ferron, Alterman, et al. (2009). Mental Health and Substance Use, 2(1), 64 -79 #teachproject
Smoking and Schizophrenia – Impact on MSE – Impact on Medication – Cessation interventions Ferron, Alterman, et al. (2009). Mental Health and Substance Use, 2(1), 64 -79 #teachproject
 Smoking and Schizophrenia • • Prevalence rates of 72. 5% (up to 90%) More likely to smoke and less likely to quit Biological variables Quitting smoking may impact on symptoms of schizophrenia: • Positive symptoms • Negative symptoms • Cognitive symptoms Baker, Lubman, et al. (2010) Primary Psychiatry, 17(1): 49 -54. #teachproject 28
Smoking and Schizophrenia • • Prevalence rates of 72. 5% (up to 90%) More likely to smoke and less likely to quit Biological variables Quitting smoking may impact on symptoms of schizophrenia: • Positive symptoms • Negative symptoms • Cognitive symptoms Baker, Lubman, et al. (2010) Primary Psychiatry, 17(1): 49 -54. #teachproject 28
 Psychotropic Drug Interactions Impacted: • Clozapine • Olanzapine • Haloperidol • Chlorpromazine • Caffeine Not Impacted: • Risperidone • Ziprasidone • Aripiprazole • Quetiapine • Bupropion De. Leon (2004). Psychopharmacology, 55(5): 491 -493. Desai, Seabolt, et al. (2001). CNS Drugs, 15(6): 469 -494. #teachproject 29
Psychotropic Drug Interactions Impacted: • Clozapine • Olanzapine • Haloperidol • Chlorpromazine • Caffeine Not Impacted: • Risperidone • Ziprasidone • Aripiprazole • Quetiapine • Bupropion De. Leon (2004). Psychopharmacology, 55(5): 491 -493. Desai, Seabolt, et al. (2001). CNS Drugs, 15(6): 469 -494. #teachproject 29
 Psychotropic Drug Interaction Example: Clozapine • Smoking cessation leads to increased clozapine plasma levels of up to 50%, which could lead to adverse events and toxicity 1 • Increase could persist to up to 4 weeks • Plasma levels should be monitored frequently 2 • Dose may require lowering of 30 -40% of original dose 3 • Warning signs that medication dose needs adjusting 3 Worsening psychiatric symptoms – Excessive fatigue or sleepiness – Extrapyrimidal effects (i. e. tremor, slurred speech, dystonia) – Seizures 1) Cormac, Brown, et al. (2010). Acta Psychiatr Scand 2010: 121: 393– 397 2) De. Leon (2004). Psychopharmacology, 55(5): 491 -493. 3) Lowe & Ackman (2010). Ann Pharmacother. 44(4): 727 -32 #teachproject 30
Psychotropic Drug Interaction Example: Clozapine • Smoking cessation leads to increased clozapine plasma levels of up to 50%, which could lead to adverse events and toxicity 1 • Increase could persist to up to 4 weeks • Plasma levels should be monitored frequently 2 • Dose may require lowering of 30 -40% of original dose 3 • Warning signs that medication dose needs adjusting 3 Worsening psychiatric symptoms – Excessive fatigue or sleepiness – Extrapyrimidal effects (i. e. tremor, slurred speech, dystonia) – Seizures 1) Cormac, Brown, et al. (2010). Acta Psychiatr Scand 2010: 121: 393– 397 2) De. Leon (2004). Psychopharmacology, 55(5): 491 -493. 3) Lowe & Ackman (2010). Ann Pharmacother. 44(4): 727 -32 #teachproject 30
 When is the “best” time for a person with substance use problems to quit smoking? a. Before they enter addiction treatment b. Concurrently with their other treatment c. After they have been treated #teachproject 31
When is the “best” time for a person with substance use problems to quit smoking? a. Before they enter addiction treatment b. Concurrently with their other treatment c. After they have been treated #teachproject 31
 Concurrent Treatment of Tobacco and Other Substances • 25% of clients in addiction treatment want to quit all substances 1 • Relapse rates lower if all substances are addressed concurrently 2 • Need to address therapists’ misconceptions of concurrent substance use treatment – Concurrent tobacco dependence treatment does not jeopardize alcohol and non-nicotine drug outcomes 3 1. Schroeder & Morris (2010) Annual Review of Public Health, 31: 297 -314. 2. Kohn, Tsoh et al. (2003). Drug and Alcohol Dependence, 69(1): 61 -71. 3. Kalman, Kim, et al. (2010 ). Clinical Psychology Review, 30: 12 -24. #teachproject 32
Concurrent Treatment of Tobacco and Other Substances • 25% of clients in addiction treatment want to quit all substances 1 • Relapse rates lower if all substances are addressed concurrently 2 • Need to address therapists’ misconceptions of concurrent substance use treatment – Concurrent tobacco dependence treatment does not jeopardize alcohol and non-nicotine drug outcomes 3 1. Schroeder & Morris (2010) Annual Review of Public Health, 31: 297 -314. 2. Kohn, Tsoh et al. (2003). Drug and Alcohol Dependence, 69(1): 61 -71. 3. Kalman, Kim, et al. (2010 ). Clinical Psychology Review, 30: 12 -24. #teachproject 32
 Concurrent Treatment: A Standardof-Care and a Duty-of-Practice “A court could have sufficient basis to find that the failure to adequately treat the main cause of preventable disease and death qualifies as a violation of the legal duty that healthcare practitioners owe to patients habituated to tobacco use and dependence…” Torrijos & Glantz (2006). Tob Control 2006; 15: 447 -451 #teachproject 33
Concurrent Treatment: A Standardof-Care and a Duty-of-Practice “A court could have sufficient basis to find that the failure to adequately treat the main cause of preventable disease and death qualifies as a violation of the legal duty that healthcare practitioners owe to patients habituated to tobacco use and dependence…” Torrijos & Glantz (2006). Tob Control 2006; 15: 447 -451 #teachproject 33
 Alcohol and Tobacco • • Strong correlation Dose-dependent Mortality rates increased Possible gateway hypothesis? Selby & Els (2004). Alcohol & Drug Problems: A Practical Guide for Counsellors (pp. 709– 731). #teachproject 34
Alcohol and Tobacco • • Strong correlation Dose-dependent Mortality rates increased Possible gateway hypothesis? Selby & Els (2004). Alcohol & Drug Problems: A Practical Guide for Counsellors (pp. 709– 731). #teachproject 34
 Smoking and Substance-Related Disorders – Significant co-occurrence epidemiologically – Increased mortality – Biological and Sociological interface – Optimal sequencing of treatment – Treatment Kalman et al. (2005). Am. J. Addict. 14(2): 106 -23. #teachproject
Smoking and Substance-Related Disorders – Significant co-occurrence epidemiologically – Increased mortality – Biological and Sociological interface – Optimal sequencing of treatment – Treatment Kalman et al. (2005). Am. J. Addict. 14(2): 106 -23. #teachproject
 Summary Statement #1 Health care providers should screen persons with mental illness and/or addictions for tobacco use. GRADE: 1 A Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
Summary Statement #1 Health care providers should screen persons with mental illness and/or addictions for tobacco use. GRADE: 1 A Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
 Summary Statement #2 Health care providers should offer counseling and pharmacotherapy treatment to persons who smoke and who have a mental illness and/or addiction to other substances. GRADE: 1 A Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
Summary Statement #2 Health care providers should offer counseling and pharmacotherapy treatment to persons who smoke and who have a mental illness and/or addiction to other substances. GRADE: 1 A Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
 Summary Statement #3 While reducing smoking or abstaining (quitting), health care providers should monitor the patient’s/client’s psychiatric condition(s). Medication dosage should be monitored and adjusted as necessary. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject GRADE: 1 A
Summary Statement #3 While reducing smoking or abstaining (quitting), health care providers should monitor the patient’s/client’s psychiatric condition(s). Medication dosage should be monitored and adjusted as necessary. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject GRADE: 1 A
 Clinical Considerations cont’d • Offer pharmacotherapy/counselling q It should be noted that no (cessation) pharmacotherapy has been contraindicated in persons with mental illness unless medically contraindicated. q Recognize that involuntary abstinence from tobacco requires management with an agonist at sufficient doses. q The withdrawal/anxiety experienced by persons abstaining from smoking should be recognized and addressed; especially in acute care facilities. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
Clinical Considerations cont’d • Offer pharmacotherapy/counselling q It should be noted that no (cessation) pharmacotherapy has been contraindicated in persons with mental illness unless medically contraindicated. q Recognize that involuntary abstinence from tobacco requires management with an agonist at sufficient doses. q The withdrawal/anxiety experienced by persons abstaining from smoking should be recognized and addressed; especially in acute care facilities. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
 Clinical Considerations cont’d • Offer pharmacotherapy/counselling • It should be noted that no (cessation) pharmacotherapy has been contraindicated in persons with mental illness unless medically contraindicated. • Recognize that involuntary abstinence from tobacco requires management with an agonist at sufficient doses. • The withdrawal/anxiety experienced by persons abstaining from smoking should be recognized and addressed; especially in acute care facilities. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
Clinical Considerations cont’d • Offer pharmacotherapy/counselling • It should be noted that no (cessation) pharmacotherapy has been contraindicated in persons with mental illness unless medically contraindicated. • Recognize that involuntary abstinence from tobacco requires management with an agonist at sufficient doses. • The withdrawal/anxiety experienced by persons abstaining from smoking should be recognized and addressed; especially in acute care facilities. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
 Clinical Considerations cont’d Monitor • Consider that persons with mental illness and/or addiction(s) who smoke might need higher doses of NRT or combination therapies and for a longer duration. • Assess for interactions with medications used for co- morbid conditions. • Caffeine should be considered a compound to be monitored. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
Clinical Considerations cont’d Monitor • Consider that persons with mental illness and/or addiction(s) who smoke might need higher doses of NRT or combination therapies and for a longer duration. • Assess for interactions with medications used for co- morbid conditions. • Caffeine should be considered a compound to be monitored. Slide Source: CAN-ADAPTT http: //www. can-adaptt. net/ #teachproject
 Clinical Considerations cont’d • Monitor q Consider that persons with mental illness and/or addiction(s) who smoke might need higher doses of NRT or combination therapies and for a longer duration. q Assess for interactions with medications used for co- morbid conditions. q Caffeine should be considered a compound to be monitored. #teachproject
Clinical Considerations cont’d • Monitor q Consider that persons with mental illness and/or addiction(s) who smoke might need higher doses of NRT or combination therapies and for a longer duration. q Assess for interactions with medications used for co- morbid conditions. q Caffeine should be considered a compound to be monitored. #teachproject
 Brief Focus on Selected Populations (2) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
Brief Focus on Selected Populations (2) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
 People who are homeless or underhoused • Difficult research population • 70 -80 % tobacco prevalence 1 • Master Settlement Agreement revealed industry marketing 2 • No peer-reviewed smoking cessation programs • Interest likely exists in quitting 1. Tsai, J. , & Rosenheck, R. A. (2012). Psychiatric Services in Advance. 2. Apollonio & Malone (2005). Tob Control; 14: 409 -415 #teachproject 44
People who are homeless or underhoused • Difficult research population • 70 -80 % tobacco prevalence 1 • Master Settlement Agreement revealed industry marketing 2 • No peer-reviewed smoking cessation programs • Interest likely exists in quitting 1. Tsai, J. , & Rosenheck, R. A. (2012). Psychiatric Services in Advance. 2. Apollonio & Malone (2005). Tob Control; 14: 409 -415 #teachproject 44
 Brief Focus on Selected Populations (3) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
Brief Focus on Selected Populations (3) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
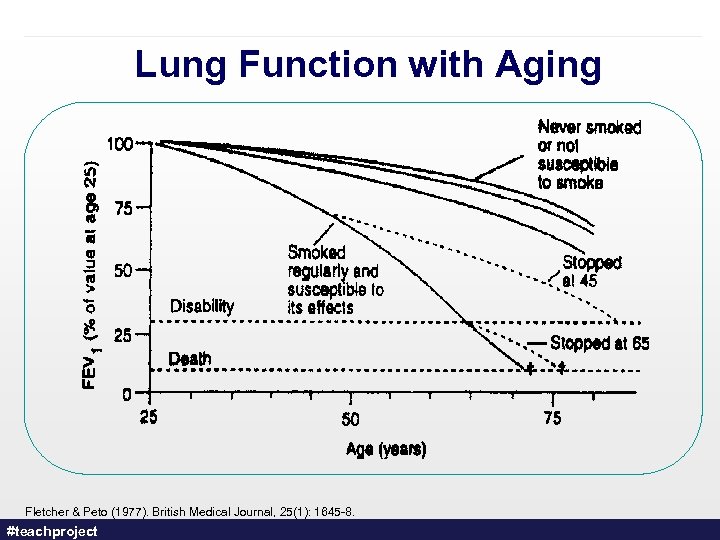 Lung Function with Aging Fletcher & Peto (1977). British Medical Journal, 25(1): 1645 -8. #teachproject
Lung Function with Aging Fletcher & Peto (1977). British Medical Journal, 25(1): 1645 -8. #teachproject
 Smoking in Elderly Persons • Prevalence 10% • Obstacles to smoking cessation • Interventions Tuppo, E. E. (2008). Smoking and the Older Person. Clinical Geriatrics #teachproject
Smoking in Elderly Persons • Prevalence 10% • Obstacles to smoking cessation • Interventions Tuppo, E. E. (2008). Smoking and the Older Person. Clinical Geriatrics #teachproject
 Brief Focus on Selected Populations (4) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
Brief Focus on Selected Populations (4) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
 LGBTTTIQ* Population • • Limited studies & almost no Canadian data Demographics vary & methodological flaws Reasons for high smoking rates? Treatment on small scale with limited evidence * L = Lesbian; G = Gay; B = Bisexual; T= Transsexual; T = Transgendered; T = Two-Spirited; I = Intersex; Q = Queer/Questioning Greenwood et al (2005). Am J Public Health, 95(1): 145 -51. #teachproject 49
LGBTTTIQ* Population • • Limited studies & almost no Canadian data Demographics vary & methodological flaws Reasons for high smoking rates? Treatment on small scale with limited evidence * L = Lesbian; G = Gay; B = Bisexual; T= Transsexual; T = Transgendered; T = Two-Spirited; I = Intersex; Q = Queer/Questioning Greenwood et al (2005). Am J Public Health, 95(1): 145 -51. #teachproject 49
 Statistics in LGBTTTIQ Community • Some US studies estimate 48% of LGBTTTIQ population smoke • Association between smoking and bacterial pneumonia, hairy leukoplakia, oral candidiasis and AIDS-related dementia Forsythe, (2010). Healthy People: Lesbian, Gay, Bisexual and Transgender Health. Chapter on Tobacco Use. #teachproject 50
Statistics in LGBTTTIQ Community • Some US studies estimate 48% of LGBTTTIQ population smoke • Association between smoking and bacterial pneumonia, hairy leukoplakia, oral candidiasis and AIDS-related dementia Forsythe, (2010). Healthy People: Lesbian, Gay, Bisexual and Transgender Health. Chapter on Tobacco Use. #teachproject 50
 Brief Focus on Selected Populations (5) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
Brief Focus on Selected Populations (5) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
 Youth & Smoking: There is no significant difference between the number of teenage males and teenage females who smoke a. b. c. #teachproject True False – Significantly more teenage females smoke False – Significantly more teenage males smoke 52
Youth & Smoking: There is no significant difference between the number of teenage males and teenage females who smoke a. b. c. #teachproject True False – Significantly more teenage females smoke False – Significantly more teenage males smoke 52
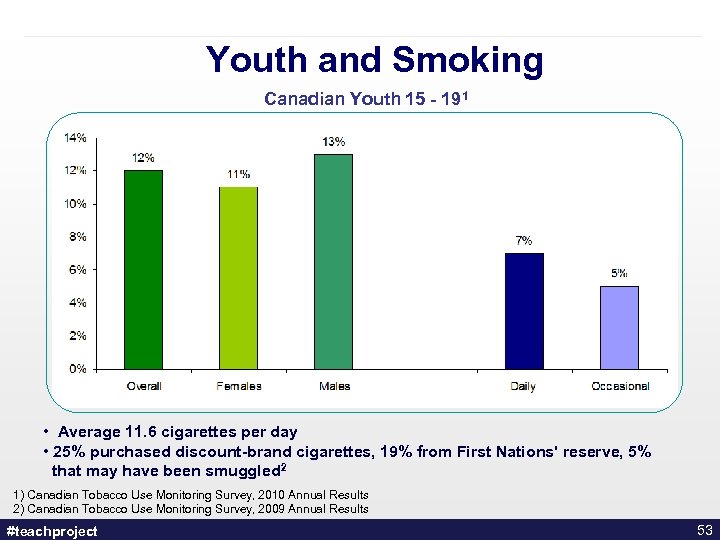 Youth and Smoking Canadian Youth 15 - 191 • Average 11. 6 cigarettes per day • 25% purchased discount-brand cigarettes, 19% from First Nations' reserve, 5% that may have been smuggled 2 1) Canadian Tobacco Use Monitoring Survey, 2010 Annual Results 2) Canadian Tobacco Use Monitoring Survey, 2009 Annual Results #teachproject 53
Youth and Smoking Canadian Youth 15 - 191 • Average 11. 6 cigarettes per day • 25% purchased discount-brand cigarettes, 19% from First Nations' reserve, 5% that may have been smuggled 2 1) Canadian Tobacco Use Monitoring Survey, 2010 Annual Results 2) Canadian Tobacco Use Monitoring Survey, 2009 Annual Results #teachproject 53
 Young Adult Male Smoking: 20 -24 Years of Age • 24% are Current Smokers § has consumed 100 cigarettes in his/her life and has smoked within the last 30 days • 16. 4% are Daily Smokers § has consumed 100 cigarettes in his/her life and has smoked daily for the last 30 days • 8. 5% are Former Smokers § Someone who has not smoked in the last 30 days • 67. 5% are Non Smokers § Someone who has never smoked 100 cigarettes or more in his life Canadian Tobacco Use Monitoring Survey, 2010 Annual Results #teachproject 54
Young Adult Male Smoking: 20 -24 Years of Age • 24% are Current Smokers § has consumed 100 cigarettes in his/her life and has smoked within the last 30 days • 16. 4% are Daily Smokers § has consumed 100 cigarettes in his/her life and has smoked daily for the last 30 days • 8. 5% are Former Smokers § Someone who has not smoked in the last 30 days • 67. 5% are Non Smokers § Someone who has never smoked 100 cigarettes or more in his life Canadian Tobacco Use Monitoring Survey, 2010 Annual Results #teachproject 54
 Other Associations in Youth • Sexual and physical abuse/trauma 1, 2 • Other psychiatric disorders – Eating disorders 4 – Depressive disorders 7 – Suicide attempts 5 – Substance abuse 5 – ADHD 6 • Impoverished and dysfunctional households 3 1. 2. 3. 4. 5. 6. De Von Figueroa-Moseley, Landrine, Klonoff. (2004). Addictive Behaviors, 29: 245 -251 Dube, Felitti, et al. (2003). Pediatrics, 111(3): 564 -72 Potter, Peterson, et al. (2004). Nicotine & Tobacco Research, 6(3): 397 -425. Cornelius, Sallorum, et al. (2001). Annals of the New York Academy of Sciences, 932: 78 -90. Mäkikyrö, Hakko, Timonen, et al. (2004). Journal of Adolescent Health, 34(3): 250 -253 Milberger, Biederman, Faraone, et al. (1997). Journal of the American Academy of Child and Adolescent Psychiatry, 36(1): 37 -44. #teachproject 55
Other Associations in Youth • Sexual and physical abuse/trauma 1, 2 • Other psychiatric disorders – Eating disorders 4 – Depressive disorders 7 – Suicide attempts 5 – Substance abuse 5 – ADHD 6 • Impoverished and dysfunctional households 3 1. 2. 3. 4. 5. 6. De Von Figueroa-Moseley, Landrine, Klonoff. (2004). Addictive Behaviors, 29: 245 -251 Dube, Felitti, et al. (2003). Pediatrics, 111(3): 564 -72 Potter, Peterson, et al. (2004). Nicotine & Tobacco Research, 6(3): 397 -425. Cornelius, Sallorum, et al. (2001). Annals of the New York Academy of Sciences, 932: 78 -90. Mäkikyrö, Hakko, Timonen, et al. (2004). Journal of Adolescent Health, 34(3): 250 -253 Milberger, Biederman, Faraone, et al. (1997). Journal of the American Academy of Child and Adolescent Psychiatry, 36(1): 37 -44. #teachproject 55
 Brief Focus on Selected Populations (6) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
Brief Focus on Selected Populations (6) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
 Women and Pregnancy Why do women smoke? • • • Controlling weight / fear of weight gain Addiction Concurrent mental health problems Coping with emotions, stress “Fitting in” Fashion, style and marketing Risks decrease with quitting: • • • #teachproject Vaginal bleeding, premature delivery, abruptio placenta and placenta previa Spontaneous abortion Perinatal mortality Better chance of having a healthier birth weight Easier time with breastfeeding 57
Women and Pregnancy Why do women smoke? • • • Controlling weight / fear of weight gain Addiction Concurrent mental health problems Coping with emotions, stress “Fitting in” Fashion, style and marketing Risks decrease with quitting: • • • #teachproject Vaginal bleeding, premature delivery, abruptio placenta and placenta previa Spontaneous abortion Perinatal mortality Better chance of having a healthier birth weight Easier time with breastfeeding 57
 Evidence-Based Interventions • Maximum quit rate about 20% despite best intervention • Self-help materials tend to have good quit rates • Telephone quit lines are a cost-effective way to reach smokers with some efficacy • Counselling doubled abstinence rates • Seven quit-line counselling sessions • Brief treatment often no different than intensive counselling • Consider NRT if behavioural interventions do not work Lumley, Chamerlain, et al. (2009). Interventions for promoting smoking cessation during pregnancy. Cochrane Database of Systematic Reviews #teachproject 58
Evidence-Based Interventions • Maximum quit rate about 20% despite best intervention • Self-help materials tend to have good quit rates • Telephone quit lines are a cost-effective way to reach smokers with some efficacy • Counselling doubled abstinence rates • Seven quit-line counselling sessions • Brief treatment often no different than intensive counselling • Consider NRT if behavioural interventions do not work Lumley, Chamerlain, et al. (2009). Interventions for promoting smoking cessation during pregnancy. Cochrane Database of Systematic Reviews #teachproject 58
 Brief Focus on Selected Populations (7) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
Brief Focus on Selected Populations (7) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
 Incarcerated Individuals • Extremely high smoking prevalence: – Up to 91%2 – Nearly 50% report other substance abuse and mental health issues 3 – 75 -100% relapse rate upon release 3 • Limited treatment or programs available – 1 RCT to date; outcome indicates a combination of CBT + pharmacotherapy is effective (quit rate of 14% at 6 -month follow -up)1 • Smoking bans will contribute to a healthier environment, better air quality; but should be coupled with cessation interventions for sustained quit – Forced abstinence through bans leads to short-term cessation only 1. Cropsley et al. (2008). American Journal of Public Health, 98, 1894– 1901 2. Donahue (2009). Journal of Offender Rehabilitation, 48: 7, 589 — 604 3. Diamond et al. (2009). Adm Policy Ment Health, 29: 21– 40 #teachproject 60
Incarcerated Individuals • Extremely high smoking prevalence: – Up to 91%2 – Nearly 50% report other substance abuse and mental health issues 3 – 75 -100% relapse rate upon release 3 • Limited treatment or programs available – 1 RCT to date; outcome indicates a combination of CBT + pharmacotherapy is effective (quit rate of 14% at 6 -month follow -up)1 • Smoking bans will contribute to a healthier environment, better air quality; but should be coupled with cessation interventions for sustained quit – Forced abstinence through bans leads to short-term cessation only 1. Cropsley et al. (2008). American Journal of Public Health, 98, 1894– 1901 2. Donahue (2009). Journal of Offender Rehabilitation, 48: 7, 589 — 604 3. Diamond et al. (2009). Adm Policy Ment Health, 29: 21– 40 #teachproject 60
 Brief Focus on Selected Populations (7) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
Brief Focus on Selected Populations (7) • • People with MI/A Homeless persons Older Adults LGBTTTIQQ persons #teachproject • • Youth Pregnancy Incarcerated persons Ethno-cultural groups
 Are you aware of the differences between non-traditional and traditional tobacco use in First Nations? a. b. c. #teachproject Yes, I am sensitive to this in my practice. Yes but I don’t know how to approach it with my Aboriginal clients. No, this is something I need more information about. 62
Are you aware of the differences between non-traditional and traditional tobacco use in First Nations? a. b. c. #teachproject Yes, I am sensitive to this in my practice. Yes but I don’t know how to approach it with my Aboriginal clients. No, this is something I need more information about. 62
 Indigenous Populations • What is traditional use of tobacco? • Smoking rates higher • Lower age groups overrepresented *Although the tobacco plant is sacred among some First Nations, it is not revered by all groups or by the Inuit Health Canada, 2004. Baseline Study Among First Nations On-reserve and Inuit in the North. http: //www. hcsc. gc. ca/fniah-spnia/substan/tobac-tabac/index-eng. php #teachproject 63
Indigenous Populations • What is traditional use of tobacco? • Smoking rates higher • Lower age groups overrepresented *Although the tobacco plant is sacred among some First Nations, it is not revered by all groups or by the Inuit Health Canada, 2004. Baseline Study Among First Nations On-reserve and Inuit in the North. http: //www. hcsc. gc. ca/fniah-spnia/substan/tobac-tabac/index-eng. php #teachproject 63
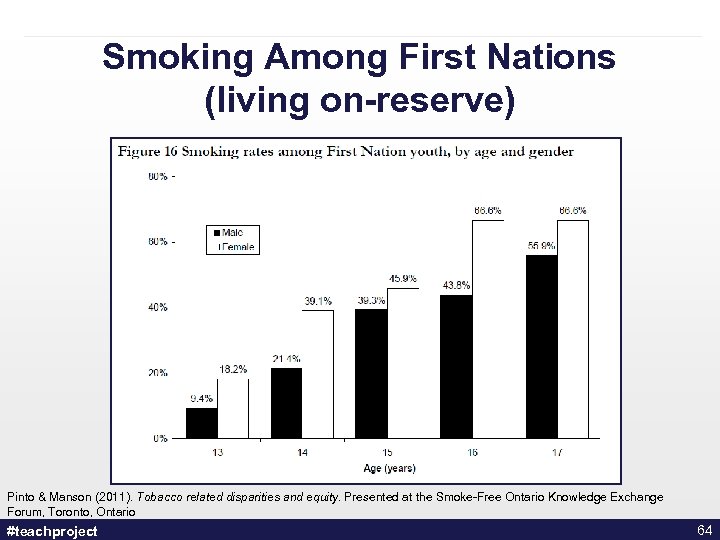 Smoking Among First Nations (living on-reserve) Pinto & Manson (2011). Tobacco related disparities and equity. Presented at the Smoke-Free Ontario Knowledge Exchange Forum, Toronto, Ontario #teachproject 64
Smoking Among First Nations (living on-reserve) Pinto & Manson (2011). Tobacco related disparities and equity. Presented at the Smoke-Free Ontario Knowledge Exchange Forum, Toronto, Ontario #teachproject 64
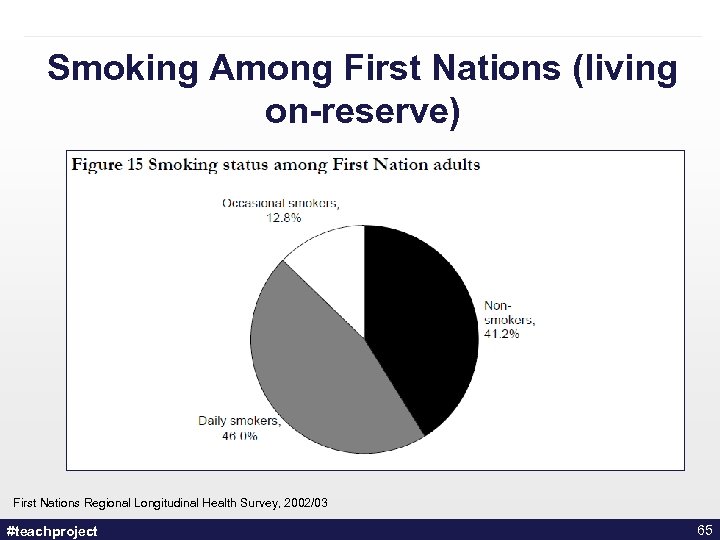 Smoking Among First Nations (living on-reserve) First Nations Regional Longitudinal Health Survey, 2002/03 #teachproject 65
Smoking Among First Nations (living on-reserve) First Nations Regional Longitudinal Health Survey, 2002/03 #teachproject 65
 Small Group Discussion • At your tables, please share your experiences providing cessation services to specific populations…. . • What are some key considerations? • What questions to do you have? #teachproject 66
Small Group Discussion • At your tables, please share your experiences providing cessation services to specific populations…. . • What are some key considerations? • What questions to do you have? #teachproject 66
 Factors to Consider • • • Diversity among Indigenous Populations Access to healthcare resources Traditional approaches to healing/recovery Geographical location Intergenerational trauma Economic incentives from tobacco sales/production in some communities #teachproject 67
Factors to Consider • • • Diversity among Indigenous Populations Access to healthcare resources Traditional approaches to healing/recovery Geographical location Intergenerational trauma Economic incentives from tobacco sales/production in some communities #teachproject 67
 Focus on Special Populations: Implications for Tobacco Control • • • High prevalence & high risk Smoking impacts disproportionately Rates overrepresented in subgroups Mentally ill youth at greater risk of uptake Often not addressed by mainstream tobacco control approaches #teachproject 68
Focus on Special Populations: Implications for Tobacco Control • • • High prevalence & high risk Smoking impacts disproportionately Rates overrepresented in subgroups Mentally ill youth at greater risk of uptake Often not addressed by mainstream tobacco control approaches #teachproject 68
 Contingency Management • Incentive based programming • Despite demonstrated efficacy in addictions limited use in smoking cessation • Barriers include people’s attitude towards incentives in treatment. Ledgerwood (2008). Current Drug Abuse Reviews 1(3): 340 -9 #teachproject 69
Contingency Management • Incentive based programming • Despite demonstrated efficacy in addictions limited use in smoking cessation • Barriers include people’s attitude towards incentives in treatment. Ledgerwood (2008). Current Drug Abuse Reviews 1(3): 340 -9 #teachproject 69
 Suggestions for Tobacco Control • Identify high-risk youth • Identify hard-to-reach populations • Offer counselling/medications in criminal justice settings • Parity of coverage #teachproject 70
Suggestions for Tobacco Control • Identify high-risk youth • Identify hard-to-reach populations • Offer counselling/medications in criminal justice settings • Parity of coverage #teachproject 70
 Conclusions • Evidence emerging • Supporting cessation is crucial for health promotion • Needed: – More comprehensive and tailored supports – Further research – Advocacy #teachproject 71
Conclusions • Evidence emerging • Supporting cessation is crucial for health promotion • Needed: – More comprehensive and tailored supports – Further research – Advocacy #teachproject 71
 Case Discussion • Kevin is a 45 -year-old male who is living with schizophrenia who reports regular smoking since age 14. • He is on clozapine, which he takes regularly as prescribed, and was referred to the tobacco clinic by his community support worker. • His support worker noticed that even though Kevin smokes contraband cigarettes, the financial impact of his smoking affects his overall quality of life and ability to “make ends meet” between receiving government disability cheques. • Kevin states that he smokes approximately 76 cigarettes per day, and says that he has been wanting to quit for a long time. • His CO levels are 25 ppm. In his assessment, Kevin states, “I heard you people can make quitting easy – that’s what I need. • This is it! I am walking out of here a non-smoker. ” #teachproject 72
Case Discussion • Kevin is a 45 -year-old male who is living with schizophrenia who reports regular smoking since age 14. • He is on clozapine, which he takes regularly as prescribed, and was referred to the tobacco clinic by his community support worker. • His support worker noticed that even though Kevin smokes contraband cigarettes, the financial impact of his smoking affects his overall quality of life and ability to “make ends meet” between receiving government disability cheques. • Kevin states that he smokes approximately 76 cigarettes per day, and says that he has been wanting to quit for a long time. • His CO levels are 25 ppm. In his assessment, Kevin states, “I heard you people can make quitting easy – that’s what I need. • This is it! I am walking out of here a non-smoker. ” #teachproject 72
 Discussion Questions 1. In addition to the financial impact and # of cigarettes per day, what other areas would you want to assess (and address) with respect to Kevin’s tobacco use? 2. What do you think of Kevin’s decision to quit immediately? How would you respond? 3. If you were recommending a nicotine patch, what level would you recommend he start with? 4. What psychosocial intervention(s) might be helpful in this case? #teachproject 73
Discussion Questions 1. In addition to the financial impact and # of cigarettes per day, what other areas would you want to assess (and address) with respect to Kevin’s tobacco use? 2. What do you think of Kevin’s decision to quit immediately? How would you respond? 3. If you were recommending a nicotine patch, what level would you recommend he start with? 4. What psychosocial intervention(s) might be helpful in this case? #teachproject 73
 Break Time: 15 Minutes #teachproject 74
Break Time: 15 Minutes #teachproject 74
 Tobacco Industry Denormalization Michael Perley: Director, Ontario Campaign for Action on Tobacco Based on research and presentations from the Non-Smokers’ Rights Association #teachproject 75
Tobacco Industry Denormalization Michael Perley: Director, Ontario Campaign for Action on Tobacco Based on research and presentations from the Non-Smokers’ Rights Association #teachproject 75
 Learning Objective Contextualize tobacco use within a broader tobacco control policy framework #teachproject 76
Learning Objective Contextualize tobacco use within a broader tobacco control policy framework #teachproject 76
 What is Tobacco Industry Denormalization (TID)? • Telling the public the truth about the tobacco industry’s role in the perpetuation of the tobacco epidemic in appropriate language • Show the public why the tobacco industry falls outside the boundaries of normal business behaviour • Reverse the industry’s decades-long effort to normalize itself #teachproject 77
What is Tobacco Industry Denormalization (TID)? • Telling the public the truth about the tobacco industry’s role in the perpetuation of the tobacco epidemic in appropriate language • Show the public why the tobacco industry falls outside the boundaries of normal business behaviour • Reverse the industry’s decades-long effort to normalize itself #teachproject 77
 What Tobacco Industry Denormalization Is Not • Messages or programs that do not refer to the tobacco industry and its role in the epidemic, such as those referring to “smoking” or “smokers” as their main subjects #teachproject 78
What Tobacco Industry Denormalization Is Not • Messages or programs that do not refer to the tobacco industry and its role in the epidemic, such as those referring to “smoking” or “smokers” as their main subjects #teachproject 78
 From this list, select one statement with which you agree the most strongly. a. Cigarettes are too dangerous to be sold at all; b. The tobacco industry rarely/never tells the truth about health effects of smoking; c. The tobacco industry is mostly/completely responsible for health problems smokers have because of their smoking; d. The Ontario government should sue tobacco companies for health care costs caused by tobacco products; e. The tobacco industry should be fined by government for money earned from tobacco sales to minors. #teachproject 79
From this list, select one statement with which you agree the most strongly. a. Cigarettes are too dangerous to be sold at all; b. The tobacco industry rarely/never tells the truth about health effects of smoking; c. The tobacco industry is mostly/completely responsible for health problems smokers have because of their smoking; d. The Ontario government should sue tobacco companies for health care costs caused by tobacco products; e. The tobacco industry should be fined by government for money earned from tobacco sales to minors. #teachproject 79
 Tobacco Industry Behaviour 1950 s-60 s • First linkage of tobacco-lung cancer in medical literature; industry PR firm suggests counter-attack against scientists to reduce public worry • The TIRC plan: spend massively to block scientists and public health officials from warning people of potential health hazards • Industry researchers find numerous carcinogens in tobacco smoke: research hidden #teachproject 80
Tobacco Industry Behaviour 1950 s-60 s • First linkage of tobacco-lung cancer in medical literature; industry PR firm suggests counter-attack against scientists to reduce public worry • The TIRC plan: spend massively to block scientists and public health officials from warning people of potential health hazards • Industry researchers find numerous carcinogens in tobacco smoke: research hidden #teachproject 80
 #teachproject 81
#teachproject 81
 Tobacco Industry Behaviour (2) • In 1962, the Chairman of British American Tobacco asked: “If we make safer brands, how to justify continuing the sale of other brands? It would be admitting that some of (our) products already on the market might be harmful. ” (A Mc. Cormick, British American Tobacco, 1962) 1970 s • “Safer” cigarettes designed and tested, but companies could no longer afford to offer safer cigarettes to smokers #teachproject 82
Tobacco Industry Behaviour (2) • In 1962, the Chairman of British American Tobacco asked: “If we make safer brands, how to justify continuing the sale of other brands? It would be admitting that some of (our) products already on the market might be harmful. ” (A Mc. Cormick, British American Tobacco, 1962) 1970 s • “Safer” cigarettes designed and tested, but companies could no longer afford to offer safer cigarettes to smokers #teachproject 82
 #teachproject 83
#teachproject 83
 Tobacco Industry Behaviour (3) • The 1977 Bath Summit (BAT, PM, ITL, RBH, RJR): agreed to deny known health effects of tobacco and conceal known toxicity of tar, nicotine and other chemicals in tobacco 1980 s • Company scientific labs shut down, medical findings hidden or destroyed #teachproject 84
Tobacco Industry Behaviour (3) • The 1977 Bath Summit (BAT, PM, ITL, RBH, RJR): agreed to deny known health effects of tobacco and conceal known toxicity of tar, nicotine and other chemicals in tobacco 1980 s • Company scientific labs shut down, medical findings hidden or destroyed #teachproject 84
 The Industry’s Behaviour Today “Cigarette makers destroyed research on health risks, court hears” - The Montreal Gazette, 2 April 2012 “A former tobacco executive has admitted he helped to destroy research documents in the 1990 s, when he was Vice-President of Legal Affairs at Imperial Tobacco and a member of the firm’s management committee. ” “This all happened 20 -some-odd years ago, and I have no memory of it” - Roger Ackman #teachproject 85
The Industry’s Behaviour Today “Cigarette makers destroyed research on health risks, court hears” - The Montreal Gazette, 2 April 2012 “A former tobacco executive has admitted he helped to destroy research documents in the 1990 s, when he was Vice-President of Legal Affairs at Imperial Tobacco and a member of the firm’s management committee. ” “This all happened 20 -some-odd years ago, and I have no memory of it” - Roger Ackman #teachproject 85
 The Industry’s Behaviour Today (2) “Documents show Imperial sought to discredit scientific evidence against tobacco, trial hears” - The Montreal Gazette, 15 March 2012 “When Alcan Aluminum Ltd became one of the first companies to institute a workplace ban on smoking in 1980, Imperial Tobacco launched a campaign to convince the manufacturer to reverse its ban, according to evidence before the Quebec class action lawsuit against Canada’s three largest tobacco companies. ” #teachproject 86
The Industry’s Behaviour Today (2) “Documents show Imperial sought to discredit scientific evidence against tobacco, trial hears” - The Montreal Gazette, 15 March 2012 “When Alcan Aluminum Ltd became one of the first companies to institute a workplace ban on smoking in 1980, Imperial Tobacco launched a campaign to convince the manufacturer to reverse its ban, according to evidence before the Quebec class action lawsuit against Canada’s three largest tobacco companies. ” #teachproject 86
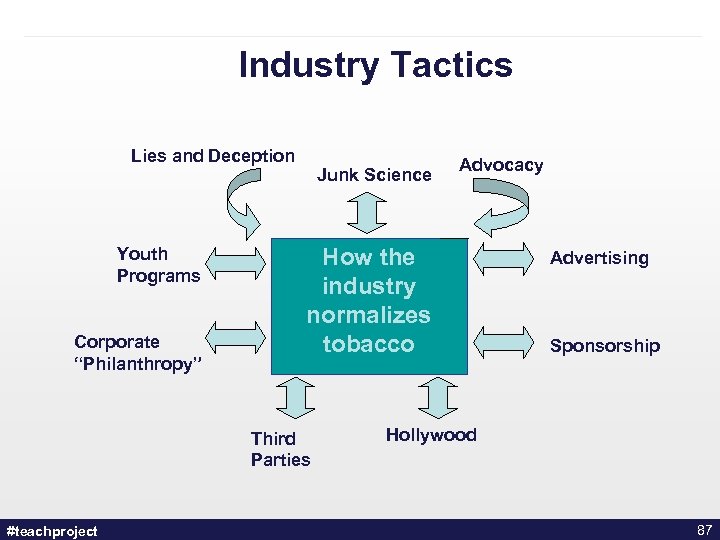 Industry Tactics Lies and Deception Youth Programs Corporate “Philanthropy” Junk Science How the industry normalizes tobacco Third Parties #teachproject Advocacy Advertising Sponsorship Hollywood 87
Industry Tactics Lies and Deception Youth Programs Corporate “Philanthropy” Junk Science How the industry normalizes tobacco Third Parties #teachproject Advocacy Advertising Sponsorship Hollywood 87
 What the Industry Really Thinks “In order to make further inroads into the younger segment, we must continue to project an image that is consistent with the needs and values of today’s younger smokers. ” (RJR, 1989) “Although the key 15 -19 age group is a must for RBH there are other bigger volume groups that we cannot ignore. ” (RBH, 1997) #teachproject 88
What the Industry Really Thinks “In order to make further inroads into the younger segment, we must continue to project an image that is consistent with the needs and values of today’s younger smokers. ” (RJR, 1989) “Although the key 15 -19 age group is a must for RBH there are other bigger volume groups that we cannot ignore. ” (RBH, 1997) #teachproject 88
 What the Industry Really Does “The 1988 tracking study is the second of a planned series of research studies into the lifestyles and value systems of young men and women in the 13 -24 age range. ” (ITL, 1988) #teachproject 89
What the Industry Really Does “The 1988 tracking study is the second of a planned series of research studies into the lifestyles and value systems of young men and women in the 13 -24 age range. ” (ITL, 1988) #teachproject 89
 Operation ID: The Tobacco Industry’s Youth-Friendly Face #teachproject 90
Operation ID: The Tobacco Industry’s Youth-Friendly Face #teachproject 90
 Concerned About Children Smoking? We Are, Too! #teachproject 91
Concerned About Children Smoking? We Are, Too! #teachproject 91
 Three on Three Hockey #teachproject 92
Three on Three Hockey #teachproject 92
 Lanny Mc. Donald #teachproject 93
Lanny Mc. Donald #teachproject 93
 Guy Carbonneau #teachproject 94
Guy Carbonneau #teachproject 94
 In 2002, the Ontario Medical Association drew the following conclusions about Operation ID: • “Tobacco industry documents make clear that their youth access programs have little or nothing to do with reducing youth smoking”. • “The failure of these programs is inevitable because they are voluntary”. • “Youth access and educational programs target the wrong outcome, access, rather than consumption”. Perley, M. , (2002). More Smoke and Mirrors: Tobacco Industry-Sponsored Youth Prevention Programs in the Context of Comprehensive Tobacco Control Programs in Canada. Ontario Medical Association. #teachproject 95
In 2002, the Ontario Medical Association drew the following conclusions about Operation ID: • “Tobacco industry documents make clear that their youth access programs have little or nothing to do with reducing youth smoking”. • “The failure of these programs is inevitable because they are voluntary”. • “Youth access and educational programs target the wrong outcome, access, rather than consumption”. Perley, M. , (2002). More Smoke and Mirrors: Tobacco Industry-Sponsored Youth Prevention Programs in the Context of Comprehensive Tobacco Control Programs in Canada. Ontario Medical Association. #teachproject 95
 Key Industry Tactics/Messages A risky – but legal – product • “We don’t market to children” • Light and mild • Questionable research (attacks on the risks of secondhand smoke) • Cigarette smuggling uncontrollable • Rights and freedoms: the “nanny state” • Economic fallout • Front groups (mychoice. ca [now defunded by ITL], FAAC, hospitality) #teachproject 96
Key Industry Tactics/Messages A risky – but legal – product • “We don’t market to children” • Light and mild • Questionable research (attacks on the risks of secondhand smoke) • Cigarette smuggling uncontrollable • Rights and freedoms: the “nanny state” • Economic fallout • Front groups (mychoice. ca [now defunded by ITL], FAAC, hospitality) #teachproject 96
 Industry Tactics: Advertising and Promotion • • • Power walls (banned in most provinces, including Ontario) Point-of-sale signage and displays (as above) Branding Movies Grey areas (bar promotions) #teachproject 97
Industry Tactics: Advertising and Promotion • • • Power walls (banned in most provinces, including Ontario) Point-of-sale signage and displays (as above) Branding Movies Grey areas (bar promotions) #teachproject 97
 Industry Sponsored Tobacco Promotions http: //www. tobaccofreekids. org/ adgallery/display. php 3? ID=204 #teachproject 98
Industry Sponsored Tobacco Promotions http: //www. tobaccofreekids. org/ adgallery/display. php 3? ID=204 #teachproject 98
 Benson and Hedges Cigarette Girls for a 2003 promotion aimed at Young Adults #teachproject 99
Benson and Hedges Cigarette Girls for a 2003 promotion aimed at Young Adults #teachproject 99
 The Industry’s Behaviour Today #teachproject 100
The Industry’s Behaviour Today #teachproject 100
 The Industry’s Behaviour Today #teachproject 101
The Industry’s Behaviour Today #teachproject 101
 The Industry’s Behaviour Today Post Bill C-32 and Ontario Bill 124, cigarillos have simply become small cigars without filters, but with the same attractive flavours such as cherry, strawberry and peach. #teachproject 102
The Industry’s Behaviour Today Post Bill C-32 and Ontario Bill 124, cigarillos have simply become small cigars without filters, but with the same attractive flavours such as cherry, strawberry and peach. #teachproject 102
 #teachproject 103
#teachproject 103
 Flavoured Tobacco Products The above products were purchased by TEACH staff months after the bill banning flavoured tobacco was passed #teachproject 104
Flavoured Tobacco Products The above products were purchased by TEACH staff months after the bill banning flavoured tobacco was passed #teachproject 104
 An Ontario Response to Flavoured Products • NDP MPP France Gélinas introduces a Private Member’s Bill to ban all flavoured products, and new tobacco products such as sticks, strips and orbs now being tested in the U. S. , across Ontario (April 17, 2012) #teachproject 105
An Ontario Response to Flavoured Products • NDP MPP France Gélinas introduces a Private Member’s Bill to ban all flavoured products, and new tobacco products such as sticks, strips and orbs now being tested in the U. S. , across Ontario (April 17, 2012) #teachproject 105
 Tobacco Industry Denormalization Strategies Objective: Expose the Industry • Combat myths about tobacco products • Draw attention to nature, extent, impact of tobacco industry advertising/promotional activities • Draw attention to role of other organizations in supporting promotion and sale of tobacco #teachproject 106
Tobacco Industry Denormalization Strategies Objective: Expose the Industry • Combat myths about tobacco products • Draw attention to nature, extent, impact of tobacco industry advertising/promotional activities • Draw attention to role of other organizations in supporting promotion and sale of tobacco #teachproject 106
 Tobacco Industry Denormalization Strategies (2) • Paid media (CA, Mass. , other US states) • Earned media (NSRA exposure of St. Michael’s University acceptance of ITL corporate ethics funding; CCS/NSRA protest chief tobacco lobbyist’s presence on WCH board; U of Sask. SU rejects $250, 000 grant from ITL) • Research/lobbying/advocacy #teachproject 107
Tobacco Industry Denormalization Strategies (2) • Paid media (CA, Mass. , other US states) • Earned media (NSRA exposure of St. Michael’s University acceptance of ITL corporate ethics funding; CCS/NSRA protest chief tobacco lobbyist’s presence on WCH board; U of Sask. SU rejects $250, 000 grant from ITL) • Research/lobbying/advocacy #teachproject 107
 Unsweetened Truth #teachproject 108
Unsweetened Truth #teachproject 108
 Do You Have What it Takes…? #teachproject 109
Do You Have What it Takes…? #teachproject 109
 Smokenders #teachproject 110
Smokenders #teachproject 110
 Smoking Dog #teachproject 111
Smoking Dog #teachproject 111
 Demon Awards #teachproject 112
Demon Awards #teachproject 112
 Contraband #teachproject 113
Contraband #teachproject 113
 Contraband What does this word mean to you? With a partner, discuss this for a few minutes. #teachproject 114
Contraband What does this word mean to you? With a partner, discuss this for a few minutes. #teachproject 114
 Are some cigarettes more harmful than others? A. No- all have the same level of danger to health, no matter where the cigarettes are manufactured B. Yes- unregulated cigarettes are more harmful C. Maybe- I need some more information to make a decision #teachproject 115
Are some cigarettes more harmful than others? A. No- all have the same level of danger to health, no matter where the cigarettes are manufactured B. Yes- unregulated cigarettes are more harmful C. Maybe- I need some more information to make a decision #teachproject 115
 The 1990 s Smuggling Crisis • Tobacco industry-driven: tax-free main-brand industry products exported to bonded warehouses in New York State, smuggled back into Ontario/Quebec • Result: Federal and several provincial governments cut tobacco taxes by 50% in 1994 • Impact: Up to 40, 000 excess deaths as a result of increased youth smoking (Health Canada draft) #teachproject 116
The 1990 s Smuggling Crisis • Tobacco industry-driven: tax-free main-brand industry products exported to bonded warehouses in New York State, smuggled back into Ontario/Quebec • Result: Federal and several provincial governments cut tobacco taxes by 50% in 1994 • Impact: Up to 40, 000 excess deaths as a result of increased youth smoking (Health Canada draft) #teachproject 116
 Smuggling/Contraband Today • The product: 200 -cigarette “baggies” manufactured on 4 -5 U. S. /Ontario/Quebec reserves (contrast: 190+ reserves in Ontario alone) • Involvement of non-FN organized crime elements: contraband tobacco trade funds smuggling of drugs/guns/people #teachproject 117
Smuggling/Contraband Today • The product: 200 -cigarette “baggies” manufactured on 4 -5 U. S. /Ontario/Quebec reserves (contrast: 190+ reserves in Ontario alone) • Involvement of non-FN organized crime elements: contraband tobacco trade funds smuggling of drugs/guns/people #teachproject 117
 Smuggling/Contraband Today (2) • A problem for all communities: $810/baggie cigarettes vs. $50 -70+ discount/main brands help lead to 1) FN community smoking rate of 59%; 2) flattening/reversal of non-FN prevalence declines • Sources: on-reserve smoke shacks (some southern Ontario/ Quebec reserves), off-reserve non-FN supply chains #teachproject 118
Smuggling/Contraband Today (2) • A problem for all communities: $810/baggie cigarettes vs. $50 -70+ discount/main brands help lead to 1) FN community smoking rate of 59%; 2) flattening/reversal of non-FN prevalence declines • Sources: on-reserve smoke shacks (some southern Ontario/ Quebec reserves), off-reserve non-FN supply chains #teachproject 118
 #teachproject 119
#teachproject 119
 #teachproject 120
#teachproject 120
 #teachproject 121
#teachproject 121
 Solutions • Nation-to-nation negotiations/trade and other economic agreements • Off-reserve enforcement esp. re: organized crime #teachproject 122
Solutions • Nation-to-nation negotiations/trade and other economic agreements • Off-reserve enforcement esp. re: organized crime #teachproject 122
 Ontario’s Bill 186 • • • Tobacco leaf management system Fine cut tobacco marking system New fine structure Seizure “in plain view” Arrangements and agreements with First Nations #teachproject 123
Ontario’s Bill 186 • • • Tobacco leaf management system Fine cut tobacco marking system New fine structure Seizure “in plain view” Arrangements and agreements with First Nations #teachproject 123
 The 2012 Ontario Budget • Promises to double enforcement efforts – annual enforcement costs to increase by $34 million by 2014 -15. • Numerous measures promised including increased fine, POA Part 1 tickets, vehicle impoundment, other best practices. #teachproject 124
The 2012 Ontario Budget • Promises to double enforcement efforts – annual enforcement costs to increase by $34 million by 2014 -15. • Numerous measures promised including increased fine, POA Part 1 tickets, vehicle impoundment, other best practices. #teachproject 124
 Questions? #teachproject 125
Questions? #teachproject 125
 Lunch! 30 Minutes #teachproject 126
Lunch! 30 Minutes #teachproject 126
 Ask the Expert! Q & A Session Dr. Peter Selby Dr. Charl Els Dr. Marilyn Herie Alexandra Andric #teachproject 127
Ask the Expert! Q & A Session Dr. Peter Selby Dr. Charl Els Dr. Marilyn Herie Alexandra Andric #teachproject 127
 Break Time: 15 Minutes #teachproject 128
Break Time: 15 Minutes #teachproject 128
 Harm Reduction #teachproject 129
Harm Reduction #teachproject 129
 Learning Objective Apply harm reduction strategies with clients who are not ready to quit smoking #teachproject 130
Learning Objective Apply harm reduction strategies with clients who are not ready to quit smoking #teachproject 130
 What is your perspective on harm reduction and tobacco use? a. There is no such thing – all tobacco use is harmful b. I can see that might be necessary with some populations c. I believe in using a harm reduction approach d. I’m not sure - I need more information #teachproject 131
What is your perspective on harm reduction and tobacco use? a. There is no such thing – all tobacco use is harmful b. I can see that might be necessary with some populations c. I believe in using a harm reduction approach d. I’m not sure - I need more information #teachproject 131
 Discussion What is one thing you want to take away about harm reduction? #teachproject 132
Discussion What is one thing you want to take away about harm reduction? #teachproject 132
 “ Don’t give up the ship in a storm because you cannot hold back the winds. You must not deliver strange and out of the way speeches to people with whom they will carry no weight because they are firmly persuaded the other way. Instead, by an indirect approach, you must strive and struggle as best you can to handle everything tactfully – and thus what you cannot turn to good, you must at least make as little bad as you can. ” St. Thomas More 1478 -1535, Utopia, CWM, v. 4, pp. 99, 101 #teachproject 133
“ Don’t give up the ship in a storm because you cannot hold back the winds. You must not deliver strange and out of the way speeches to people with whom they will carry no weight because they are firmly persuaded the other way. Instead, by an indirect approach, you must strive and struggle as best you can to handle everything tactfully – and thus what you cannot turn to good, you must at least make as little bad as you can. ” St. Thomas More 1478 -1535, Utopia, CWM, v. 4, pp. 99, 101 #teachproject 133
 Do you drive a car with anti-lock brakes? a. Yes b. No c. Do bikes count? #teachproject 134
Do you drive a car with anti-lock brakes? a. Yes b. No c. Do bikes count? #teachproject 134
 Which type of vehicle allows you to stop faster? a. Cars with anti-lock brakes b. Cars without anti-lock brakes c. No difference #teachproject 135
Which type of vehicle allows you to stop faster? a. Cars with anti-lock brakes b. Cars without anti-lock brakes c. No difference #teachproject 135
 Tobacco Harm Reduction TOTAL HARM Harmfulness Danger Intensity Prevalence National Research Council. "Front Matter. " Clearing the Smoke: Assessing the Science Base for Tobacco Harm Reduction. Washington, DC: The National Academies Press, 2001 #teachproject 136
Tobacco Harm Reduction TOTAL HARM Harmfulness Danger Intensity Prevalence National Research Council. "Front Matter. " Clearing the Smoke: Assessing the Science Base for Tobacco Harm Reduction. Washington, DC: The National Academies Press, 2001 #teachproject 136
 Issue: The Precautionary Principle – Can science of nicotine help? • The precautionary principle: – "When an activity raises threats of harm to human health or the environment, precautionary measures should be taken even if some cause and effect relationships are not fully established scientifically. In this context the proponent of an activity, rather than the public, should bear the burden of proof. " • A key issue in advocating a tobacco control harm reduction strategy involving the use of less harmful forms of nicotine delivery, is the evidence of safety of nicotine per se. Kurland (2002). The Heart of the Precautionary Principle in Democracy. Public Health Reports, December. #teachproject 137
Issue: The Precautionary Principle – Can science of nicotine help? • The precautionary principle: – "When an activity raises threats of harm to human health or the environment, precautionary measures should be taken even if some cause and effect relationships are not fully established scientifically. In this context the proponent of an activity, rather than the public, should bear the burden of proof. " • A key issue in advocating a tobacco control harm reduction strategy involving the use of less harmful forms of nicotine delivery, is the evidence of safety of nicotine per se. Kurland (2002). The Heart of the Precautionary Principle in Democracy. Public Health Reports, December. #teachproject 137
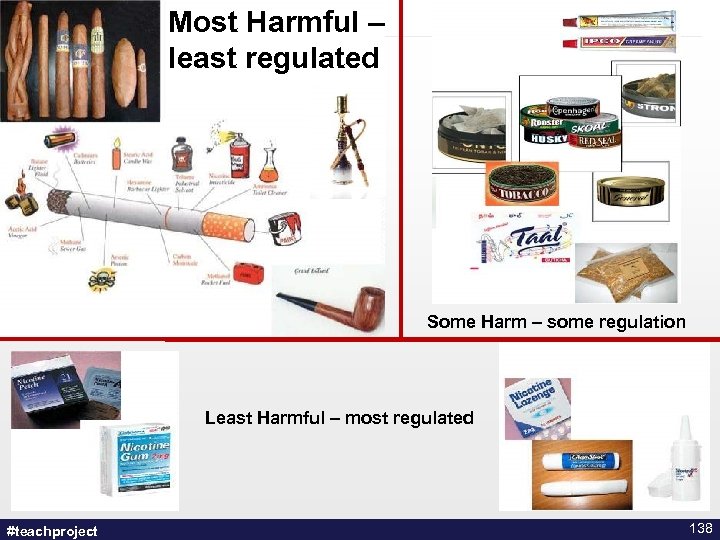 Most Harmful – least regulated Some Harm – some regulation Least Harmful – most regulated #teachproject 138
Most Harmful – least regulated Some Harm – some regulation Least Harmful – most regulated #teachproject 138
 A Controversial Topic? • Tobacco control has always taken a harm reduction perspective – Smoke free policies, taxation, etc. • There is support for harm reduction – CAMH, OMA • What do we mean by harm reduction? #teachproject 139
A Controversial Topic? • Tobacco control has always taken a harm reduction perspective – Smoke free policies, taxation, etc. • There is support for harm reduction – CAMH, OMA • What do we mean by harm reduction? #teachproject 139
 General View on Harm Reduction • Aims to reduce the adverse health, social, and economic consequences of drug use without requiring abstinence • Abstinence is healthiest choice • Focuses on the most immediate and achievable changes • Public health alternative to the moral/criminal and disease models of drug use • Non-judgmental, non-coercive #teachproject 140
General View on Harm Reduction • Aims to reduce the adverse health, social, and economic consequences of drug use without requiring abstinence • Abstinence is healthiest choice • Focuses on the most immediate and achievable changes • Public health alternative to the moral/criminal and disease models of drug use • Non-judgmental, non-coercive #teachproject 140
 General Principles of Harm Reduction • End users should have a voice in the creation of programs and policies designed to serve them (clientcentered care) • Values patient autonomy and provider patience • Culturally sensitive • Although abstinence from tobacco is recommended, many smokers are unable or not ready to quit #teachproject 141
General Principles of Harm Reduction • End users should have a voice in the creation of programs and policies designed to serve them (clientcentered care) • Values patient autonomy and provider patience • Culturally sensitive • Although abstinence from tobacco is recommended, many smokers are unable or not ready to quit #teachproject 141
 Benefits of Harm Reduction Approach (1) Daily use Reduction Abstinence Continuum • Engages • Increases confidence • Changes behavioural patterns #teachproject 142
Benefits of Harm Reduction Approach (1) Daily use Reduction Abstinence Continuum • Engages • Increases confidence • Changes behavioural patterns #teachproject 142
 • • “Quit or die” is irresponsible, unethical and unrealistic Millions are highly addicted and have low cessation rates • Appears deeply rooted in some communities (i. e. : those with mental health issues, aboriginal) • Creates a market incentive for ever-better products to replace cigarettes #teachproject 143
• • “Quit or die” is irresponsible, unethical and unrealistic Millions are highly addicted and have low cessation rates • Appears deeply rooted in some communities (i. e. : those with mental health issues, aboriginal) • Creates a market incentive for ever-better products to replace cigarettes #teachproject 143
 Cautions against Harm Reduction • Distraction from quitting – Need more resources devoted to quitting • Premature admission of defeat • Extra harm to people that would have otherwise quit completely • Potential for young people to start with products they believe it to be safe • Ex-smokers may use products as an option causing relapse #teachproject 144
Cautions against Harm Reduction • Distraction from quitting – Need more resources devoted to quitting • Premature admission of defeat • Extra harm to people that would have otherwise quit completely • Potential for young people to start with products they believe it to be safe • Ex-smokers may use products as an option causing relapse #teachproject 144
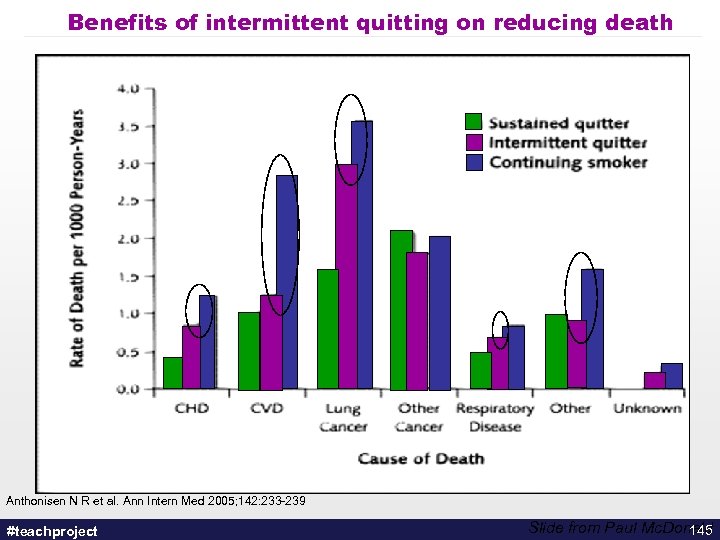 Benefits of intermittent quitting on reducing death Anthonisen N R et al. Ann Intern Med 2005; 142: 233 -239 #teachproject Slide from Paul Mc. Donald 145
Benefits of intermittent quitting on reducing death Anthonisen N R et al. Ann Intern Med 2005; 142: 233 -239 #teachproject Slide from Paul Mc. Donald 145
 Effective Harm Reduction Strategies • Product regulation – warnings on packages, making cigarettes taste bad, anti-counterfeiting • Changing nature of products containing nicotine – Low nitrosamine cigarettes only cut out 1 carcinogen • Taxation - increasing the amount of taxes on cigarettes decreases consumption especially with 18 -24 year olds • Limiting access / visibility – retail displays being removed. “Out of sight out of mind” • NRT, bupropion and other approved cessation medications • Eliminating provincial sales tax in Ontario on nicotine replacement products`` #teachproject 146
Effective Harm Reduction Strategies • Product regulation – warnings on packages, making cigarettes taste bad, anti-counterfeiting • Changing nature of products containing nicotine – Low nitrosamine cigarettes only cut out 1 carcinogen • Taxation - increasing the amount of taxes on cigarettes decreases consumption especially with 18 -24 year olds • Limiting access / visibility – retail displays being removed. “Out of sight out of mind” • NRT, bupropion and other approved cessation medications • Eliminating provincial sales tax in Ontario on nicotine replacement products`` #teachproject 146
 NRT and Reduction • Cleaner, safer delivery system of nicotine • Separates addictive behaviour from harm • Prevents use of tobacco products to help withdrawal • Increases familiarity with cessation products • Combined with other treatment (behavioral, emotional triggers) • New literature = start NRT two weeks before quit date Nicotine Assisted Reduction to Stop (NARS), Action on Smoking Health (2005). #teachproject 147
NRT and Reduction • Cleaner, safer delivery system of nicotine • Separates addictive behaviour from harm • Prevents use of tobacco products to help withdrawal • Increases familiarity with cessation products • Combined with other treatment (behavioral, emotional triggers) • New literature = start NRT two weeks before quit date Nicotine Assisted Reduction to Stop (NARS), Action on Smoking Health (2005). #teachproject 147
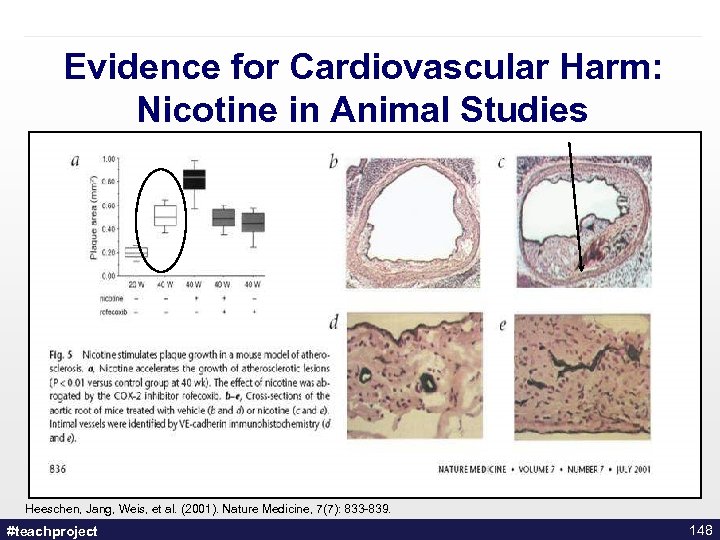 Evidence for Cardiovascular Harm: Nicotine in Animal Studies Heeschen, Jang, Weis, et al. (2001). Nature Medicine, 7(7): 833 -839. #teachproject 148
Evidence for Cardiovascular Harm: Nicotine in Animal Studies Heeschen, Jang, Weis, et al. (2001). Nature Medicine, 7(7): 833 -839. #teachproject 148
 Evidence for Cardiovascular Harm – Humans • Blood pressure: older studies, higher resting BP, newer studies, no effect. • Heart rate: mild increase but not significant • Waist-hip: nil/variable • BMI: variable • Max workload capacity: no difference • Insulin resistance higher risk both in long term NRT users. Variable in smokeless users. Asplund (2003). Progress in Cardiovascular Diseases, 45: 383 -394. #teachproject 149
Evidence for Cardiovascular Harm – Humans • Blood pressure: older studies, higher resting BP, newer studies, no effect. • Heart rate: mild increase but not significant • Waist-hip: nil/variable • BMI: variable • Max workload capacity: no difference • Insulin resistance higher risk both in long term NRT users. Variable in smokeless users. Asplund (2003). Progress in Cardiovascular Diseases, 45: 383 -394. #teachproject 149
 Conclusion • Nicotine may have increased cardiovascular effects that are associated with increased morbidity and mortality mainly in smokers. • However, compared to smoked tobacco, other forms have less risk and at times are similar to that of non-smokers. • In Sweden, many males switch to smokeless as a means to quit smoking. • NRT appears to be safe. However long-term use only examined in the Lung Health Study (1996). #teachproject 150
Conclusion • Nicotine may have increased cardiovascular effects that are associated with increased morbidity and mortality mainly in smokers. • However, compared to smoked tobacco, other forms have less risk and at times are similar to that of non-smokers. • In Sweden, many males switch to smokeless as a means to quit smoking. • NRT appears to be safe. However long-term use only examined in the Lung Health Study (1996). #teachproject 150
 Evidence of Harm in Pregnancy • Nicotine is a neuroteratogen • However, CO and Thiocyanates also play a role • Smoking is associated with cleft lip, low birth weight, SIDS • Downstream psychiatric symptoms in children • However, most pregnant women continue to smoke while pregnant even with the best available intervention. • Fetocentric versus woman-centred approach Slotkin, Seider, et al. , (2005). Neuropsychopharmacology, 30(1): 129 -44. #teachproject 151
Evidence of Harm in Pregnancy • Nicotine is a neuroteratogen • However, CO and Thiocyanates also play a role • Smoking is associated with cleft lip, low birth weight, SIDS • Downstream psychiatric symptoms in children • However, most pregnant women continue to smoke while pregnant even with the best available intervention. • Fetocentric versus woman-centred approach Slotkin, Seider, et al. , (2005). Neuropsychopharmacology, 30(1): 129 -44. #teachproject 151
 NRT in pregnancy • Try behavioural interventions first • When cannot quit, try intermittent forms of NRT starting with lowest dose • If using patch, remove at bedtime • Continue behavioural support Benowitz, Dempsey (2004). Nicotine and Tobacco Research, 6(Suppl 2): S 189 -S 202. #teachproject 152
NRT in pregnancy • Try behavioural interventions first • When cannot quit, try intermittent forms of NRT starting with lowest dose • If using patch, remove at bedtime • Continue behavioural support Benowitz, Dempsey (2004). Nicotine and Tobacco Research, 6(Suppl 2): S 189 -S 202. #teachproject 152
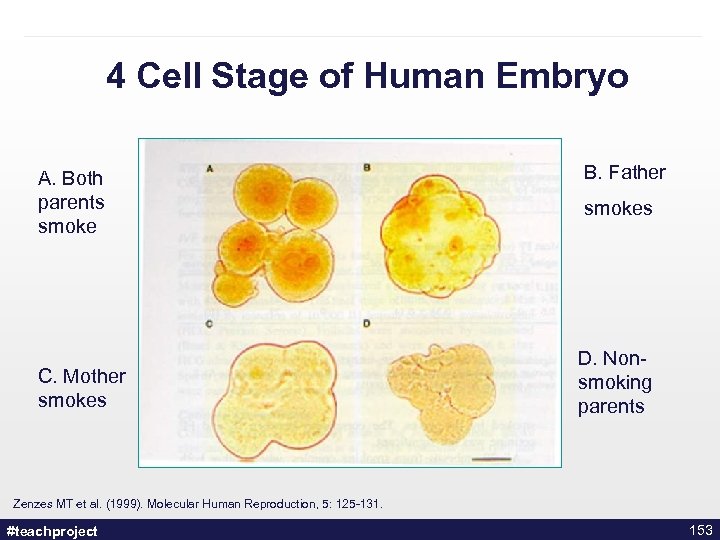 4 Cell Stage of Human Embryo A. Both parents smoke C. Mother smokes B. Father smokes D. Nonsmoking parents Zenzes MT et al. (1999). Molecular Human Reproduction, 5: 125 -131. #teachproject 153
4 Cell Stage of Human Embryo A. Both parents smoke C. Mother smokes B. Father smokes D. Nonsmoking parents Zenzes MT et al. (1999). Molecular Human Reproduction, 5: 125 -131. #teachproject 153
 Cigarettes and Reproduction • Women who smoke undergo menopause 1 to 4 years earlier than non-smokers. • Zenzes et al have shown that smoking causes benzo(a)pyrene diol epoxide DNA (BPDE-DNA) adduct formation in human sperm • Similar proportions of BPDE-DNA adducts in embryos where both parents smoke, compared to where only the father smoked, suggested that contribution of DNA adducts is mainly from sperm Zenzes MT et al. (1999). Molecular Human Reproduction, 5: 125 -131. #teachproject 154
Cigarettes and Reproduction • Women who smoke undergo menopause 1 to 4 years earlier than non-smokers. • Zenzes et al have shown that smoking causes benzo(a)pyrene diol epoxide DNA (BPDE-DNA) adduct formation in human sperm • Similar proportions of BPDE-DNA adducts in embryos where both parents smoke, compared to where only the father smoked, suggested that contribution of DNA adducts is mainly from sperm Zenzes MT et al. (1999). Molecular Human Reproduction, 5: 125 -131. #teachproject 154
 Implications • Understanding the role of nicotine in the harm caused by smoking is important if smokers are to be encouraged to use less harmful nicotine delivery devices and will help to identify where a cautious approach might be necessary as well as gaps for further research. #teachproject 155
Implications • Understanding the role of nicotine in the harm caused by smoking is important if smokers are to be encouraged to use less harmful nicotine delivery devices and will help to identify where a cautious approach might be necessary as well as gaps for further research. #teachproject 155
 When does a person’s risk of developing lung cancer become high? ( > 10 times the risk of a non-smoker) a. b. c. d. e. #teachproject Up to 10 cigarettes per day Between 10 -19 cigarettes per day 20 cigarettes per day Between 21 -31 cigarettes per day More than 31 cigarettes per day 156
When does a person’s risk of developing lung cancer become high? ( > 10 times the risk of a non-smoker) a. b. c. d. e. #teachproject Up to 10 cigarettes per day Between 10 -19 cigarettes per day 20 cigarettes per day Between 21 -31 cigarettes per day More than 31 cigarettes per day 156
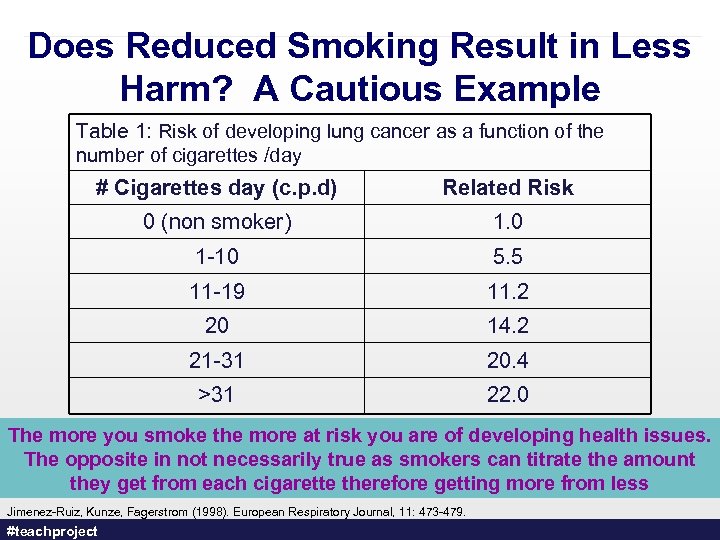 Does Reduced Smoking Result in Less Harm? A Cautious Example Table 1: Risk of developing lung cancer as a function of the number of cigarettes /day # Cigarettes day (c. p. d) Related Risk 0 (non smoker) 1. 0 1 -10 5. 5 11 -19 11. 2 20 14. 2 21 -31 20. 4 >31 22. 0 The more you smoke the more at risk you are of developing health issues. The opposite in not necessarily true as smokers can titrate the amount they get from each cigarette therefore getting more from less Jimenez-Ruiz, Kunze, Fagerstrom (1998). European Respiratory Journal, 11: 473 -479. #teachproject
Does Reduced Smoking Result in Less Harm? A Cautious Example Table 1: Risk of developing lung cancer as a function of the number of cigarettes /day # Cigarettes day (c. p. d) Related Risk 0 (non smoker) 1. 0 1 -10 5. 5 11 -19 11. 2 20 14. 2 21 -31 20. 4 >31 22. 0 The more you smoke the more at risk you are of developing health issues. The opposite in not necessarily true as smokers can titrate the amount they get from each cigarette therefore getting more from less Jimenez-Ruiz, Kunze, Fagerstrom (1998). European Respiratory Journal, 11: 473 -479. #teachproject
 What about………. One can contains 4 x the nicotine in a pack of cigarettes Tobacco or tobacco blends that are chewed or sucked on. A person who uses eight to 10 dips or chews a day receives the same amount of nicotine as a heavy smoker who smokes 30 to 40 cigarettes a day World Health Organization International Agency for Research on Cancer (2007). IARC Monographs on the Evaluation of Carcinogenic Risks to Humans, Volume 89. #teachproject 158
What about………. One can contains 4 x the nicotine in a pack of cigarettes Tobacco or tobacco blends that are chewed or sucked on. A person who uses eight to 10 dips or chews a day receives the same amount of nicotine as a heavy smoker who smokes 30 to 40 cigarettes a day World Health Organization International Agency for Research on Cancer (2007). IARC Monographs on the Evaluation of Carcinogenic Risks to Humans, Volume 89. #teachproject 158
 Snuff, Chews and Plugs…… Snuff – Fermented, ground -up moist tobacco usually placed between the bottom lip and gum. This is also referred to as "dipping“ (Swedish form is Snus – lower risk). Mayo Clinic (2011). Chewing tobacco: Not a safe alternative to cigarettes: http: //www. mayoclinic. com/health/chewing-tobacco/CA 00019 #teachproject 159
Snuff, Chews and Plugs…… Snuff – Fermented, ground -up moist tobacco usually placed between the bottom lip and gum. This is also referred to as "dipping“ (Swedish form is Snus – lower risk). Mayo Clinic (2011). Chewing tobacco: Not a safe alternative to cigarettes: http: //www. mayoclinic. com/health/chewing-tobacco/CA 00019 #teachproject 159
 Chew – shredded tobacco leaves placed between the cheek and gum. This is also referred to as "a wad". Plug – shredded tobacco leaves which are pressed into a hard block and placed between the cheek and gum Mayo Clinic (2011). Chewing tobacco: Not a safe alternative to cigarettes: http: //www. mayoclinic. com/health/chewing-tobacco/CA 00019 #teachproject 160
Chew – shredded tobacco leaves placed between the cheek and gum. This is also referred to as "a wad". Plug – shredded tobacco leaves which are pressed into a hard block and placed between the cheek and gum Mayo Clinic (2011). Chewing tobacco: Not a safe alternative to cigarettes: http: //www. mayoclinic. com/health/chewing-tobacco/CA 00019 #teachproject 160
 Ingredients in Smokeless Tobacco • Nicotine: poisonous and highly addictive drug • Carcinogens: many cancer-producing chemicals have been identified in smokeless (spit) tobacco. • Sweeteners: tobacco has an unpleasant taste, some brands of smokeless tobacco are heavily sweetened with sugars, which promote tooth decay. • Abrasives: scratch the soft tissues in the mouth, allowing the nicotine and other chemicals to get directly into the blood system. • Salt: Flavouring salts found to contribute to abnormal blood pressure and kidney disease. • Other Chemicals: Hundreds of other chemicals can be found in tobacco which contribute to many health problems. National Institute of Dental and Craniofacial Research (2010). Smokeless Tobacco: A Guide for Quitting http: //www. nidcr. nih. gov/Oral. Health/Topics/Spit. Tobacco. AGuidefor. Quitting. htm #teachproject 161
Ingredients in Smokeless Tobacco • Nicotine: poisonous and highly addictive drug • Carcinogens: many cancer-producing chemicals have been identified in smokeless (spit) tobacco. • Sweeteners: tobacco has an unpleasant taste, some brands of smokeless tobacco are heavily sweetened with sugars, which promote tooth decay. • Abrasives: scratch the soft tissues in the mouth, allowing the nicotine and other chemicals to get directly into the blood system. • Salt: Flavouring salts found to contribute to abnormal blood pressure and kidney disease. • Other Chemicals: Hundreds of other chemicals can be found in tobacco which contribute to many health problems. National Institute of Dental and Craniofacial Research (2010). Smokeless Tobacco: A Guide for Quitting http: //www. nidcr. nih. gov/Oral. Health/Topics/Spit. Tobacco. AGuidefor. Quitting. htm #teachproject 161
 Health Risks of Smokeless Tobacco (1) • • • Mouth Cancer – cancer of the cheeks, gums, lips and tongue. Smokeless (spit) tobacco users have a 50% higher chance of getting oral cancer than non-users. Throat Cancer – cancer of the voice box and cancer of the esophagus. Heart disease – heart attacks, strokes and high blood pressure. http: //www. health. gov. sk. ca/rr_smokeless_tobacco. html #teachproject 162
Health Risks of Smokeless Tobacco (1) • • • Mouth Cancer – cancer of the cheeks, gums, lips and tongue. Smokeless (spit) tobacco users have a 50% higher chance of getting oral cancer than non-users. Throat Cancer – cancer of the voice box and cancer of the esophagus. Heart disease – heart attacks, strokes and high blood pressure. http: //www. health. gov. sk. ca/rr_smokeless_tobacco. html #teachproject 162
 Health Risks of Smokeless Tobacco (2) • Dental diseases – stained teeth, tooth decay, receding gums, gum disease, bad breath and black hairy tongue. • Stomach problems – ulcers, stomach upset, increased bowel activity and stomach cancer. • Loss of taste and smell – causes loss of appetite which results in poor nutrition and poor health. • Physical changes – fatigue, muscle weakness, dizziness and decreased physical performance, dermatologic changes http: //www. health. gov. sk. ca/rr_smokeless_tobacco. html #teachproject 163
Health Risks of Smokeless Tobacco (2) • Dental diseases – stained teeth, tooth decay, receding gums, gum disease, bad breath and black hairy tongue. • Stomach problems – ulcers, stomach upset, increased bowel activity and stomach cancer. • Loss of taste and smell – causes loss of appetite which results in poor nutrition and poor health. • Physical changes – fatigue, muscle weakness, dizziness and decreased physical performance, dermatologic changes http: //www. health. gov. sk. ca/rr_smokeless_tobacco. html #teachproject 163
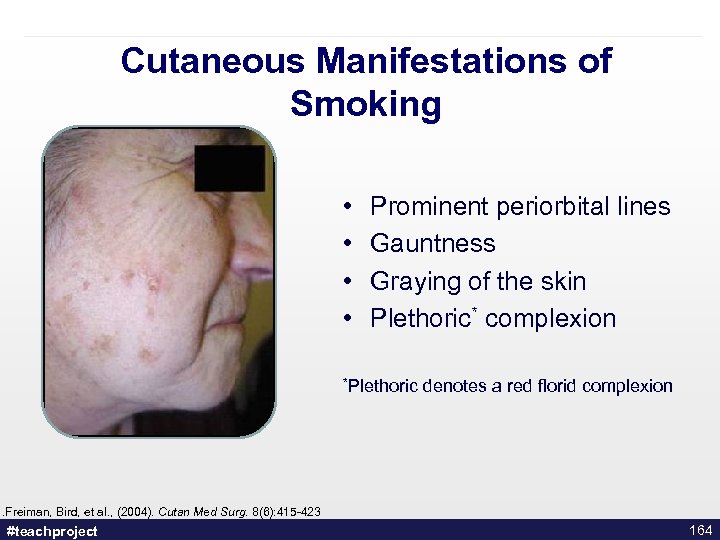 Cutaneous Manifestations of Smoking • • Prominent periorbital lines Gauntness Graying of the skin Plethoric* complexion *Plethoric denotes a red florid complexion . Freiman, Bird, et al. , (2004). Cutan Med Surg. 8(6): 415 -423 #teachproject 164
Cutaneous Manifestations of Smoking • • Prominent periorbital lines Gauntness Graying of the skin Plethoric* complexion *Plethoric denotes a red florid complexion . Freiman, Bird, et al. , (2004). Cutan Med Surg. 8(6): 415 -423 #teachproject 164
 Signs of Smoking Clinical Signs Harlequin nail Synonyms Quitter’s nail Description Demarcation line in the nail Smoker’s comedones Smoker’s face Large comedones with furrows and nodules a) Lines or wrinkles b) Gauntness c) Graying of the skin d) Plethoric complexion Smoker’s melanosis Smoker’s moustache Smoker’s nail Pigmentation of the gingiva Smoker’s palate Moustache discoloration Nicotine sign Nicotine stomatitis, leukokeratosis nicotina palati Smoker’s tongue Leukokeratosis nicotina glossi. Freiman, Bird, et al. , (2004). Cutan Med Surg. 8(6): 415 -423 Snuff Smokeless tobacco #teachproject dipper’s Nail discoloration Coloration of the palatal mucosa Pink-coloured depressions White lesion in the oral cavity 165
Signs of Smoking Clinical Signs Harlequin nail Synonyms Quitter’s nail Description Demarcation line in the nail Smoker’s comedones Smoker’s face Large comedones with furrows and nodules a) Lines or wrinkles b) Gauntness c) Graying of the skin d) Plethoric complexion Smoker’s melanosis Smoker’s moustache Smoker’s nail Pigmentation of the gingiva Smoker’s palate Moustache discoloration Nicotine sign Nicotine stomatitis, leukokeratosis nicotina palati Smoker’s tongue Leukokeratosis nicotina glossi. Freiman, Bird, et al. , (2004). Cutan Med Surg. 8(6): 415 -423 Snuff Smokeless tobacco #teachproject dipper’s Nail discoloration Coloration of the palatal mucosa Pink-coloured depressions White lesion in the oral cavity 165
 Smoking-Attributable Periodontitis • Smoking is a major risk factor for periodontitis • Current smokers are approximately 4 times as likely as persons who have never smoked to have periodontitis • Periodontal disease is one of the main causes of tooth loss worldwide Tomar, & Asma (2000). J Periodontol. 71(5): 743 -751 #teachproject 166
Smoking-Attributable Periodontitis • Smoking is a major risk factor for periodontitis • Current smokers are approximately 4 times as likely as persons who have never smoked to have periodontitis • Periodontal disease is one of the main causes of tooth loss worldwide Tomar, & Asma (2000). J Periodontol. 71(5): 743 -751 #teachproject 166
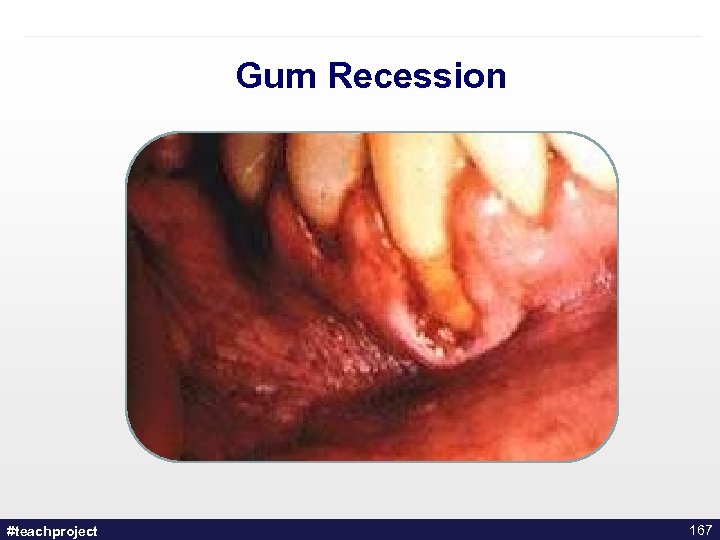 Gum Recession #teachproject 167
Gum Recession #teachproject 167
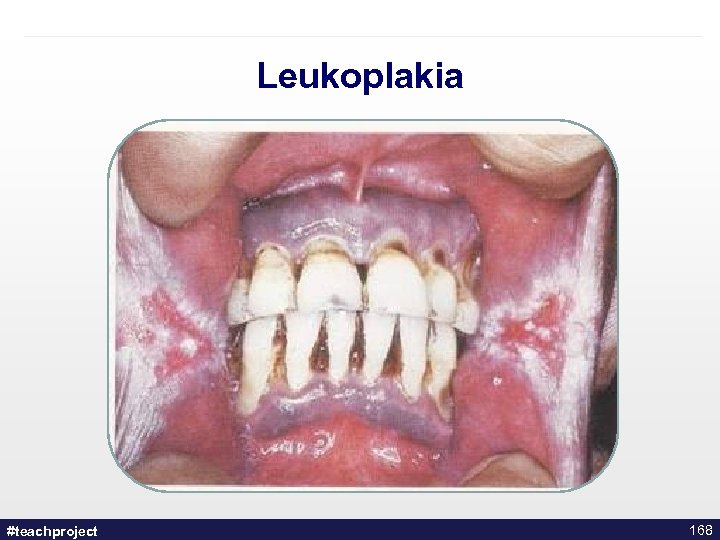 Leukoplakia #teachproject 168
Leukoplakia #teachproject 168
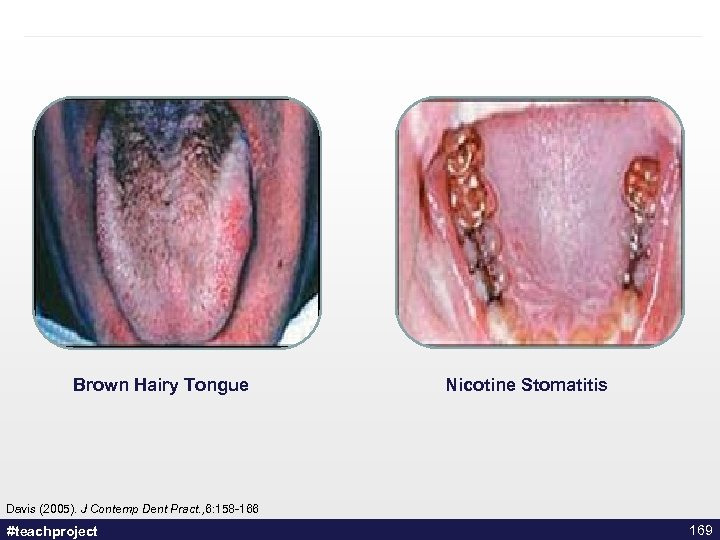 Brown Hairy Tongue Nicotine Stomatitis Davis (2005). J Contemp Dent Pract. , 6: 158 -166 #teachproject 169
Brown Hairy Tongue Nicotine Stomatitis Davis (2005). J Contemp Dent Pract. , 6: 158 -166 #teachproject 169
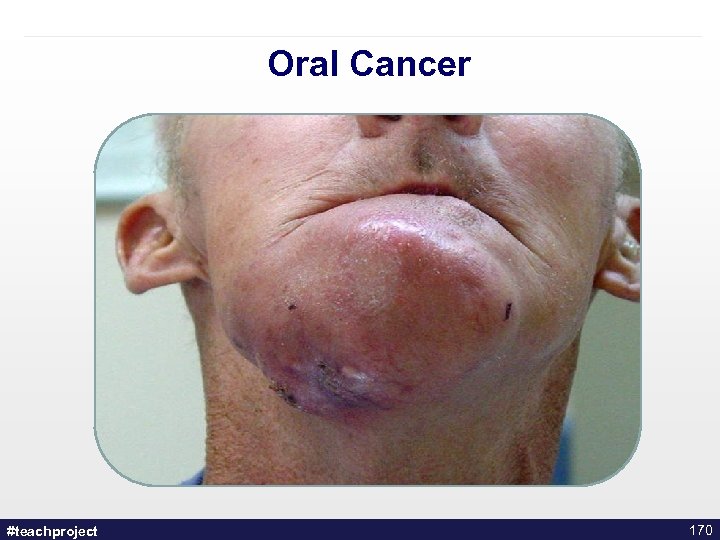 Oral Cancer #teachproject 170
Oral Cancer #teachproject 170
 Smokeless Tobacco Prevention Websites • http: //mylastdip. com/ - Web-based intervention that is designed to help young chewing tobacco users quit. • http: //www. chewfree. com/ - Website created to help people quit their use of chewing tobacco or snuff. #teachproject 171
Smokeless Tobacco Prevention Websites • http: //mylastdip. com/ - Web-based intervention that is designed to help young chewing tobacco users quit. • http: //www. chewfree. com/ - Website created to help people quit their use of chewing tobacco or snuff. #teachproject 171
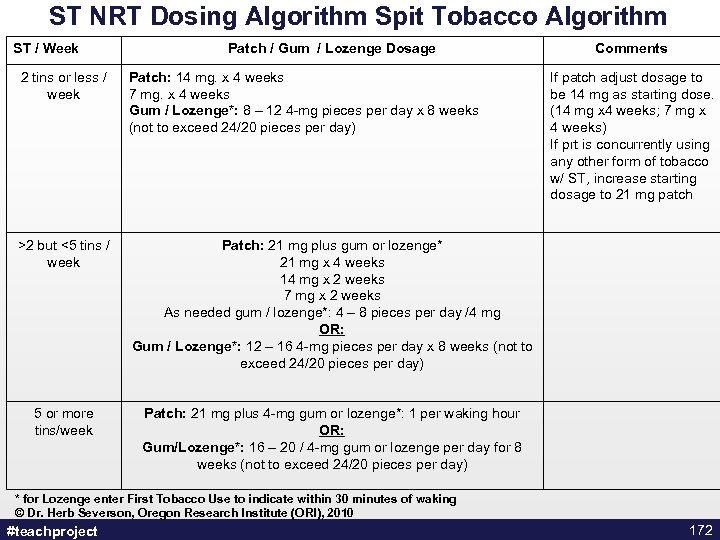 ST NRT Dosing Algorithm Spit Tobacco Algorithm ST / Week Patch / Gum / Lozenge Dosage 2 tins or less / week Patch: 14 mg. x 4 weeks 7 mg. x 4 weeks Gum / Lozenge*: 8 – 12 4 -mg pieces per day x 8 weeks (not to exceed 24/20 pieces per day) >2 but <5 tins / week Patch: 21 mg plus gum or lozenge* 21 mg x 4 weeks 14 mg x 2 weeks 7 mg x 2 weeks As needed gum / lozenge*: 4 – 8 pieces per day /4 mg OR: Gum / Lozenge*: 12 – 16 4 -mg pieces per day x 8 weeks (not to exceed 24/20 pieces per day) 5 or more tins/week Comments If patch adjust dosage to be 14 mg as starting dose. (14 mg x 4 weeks; 7 mg x 4 weeks) If prt is concurrently using any other form of tobacco w/ ST, increase starting dosage to 21 mg patch Patch: 21 mg plus 4 -mg gum or lozenge*: 1 per waking hour OR: Gum/Lozenge*: 16 – 20 / 4 -mg gum or lozenge per day for 8 weeks (not to exceed 24/20 pieces per day) * for Lozenge enter First Tobacco Use to indicate within 30 minutes of waking © Dr. Herb Severson, Oregon Research Institute (ORI), 2010 #teachproject 172
ST NRT Dosing Algorithm Spit Tobacco Algorithm ST / Week Patch / Gum / Lozenge Dosage 2 tins or less / week Patch: 14 mg. x 4 weeks 7 mg. x 4 weeks Gum / Lozenge*: 8 – 12 4 -mg pieces per day x 8 weeks (not to exceed 24/20 pieces per day) >2 but <5 tins / week Patch: 21 mg plus gum or lozenge* 21 mg x 4 weeks 14 mg x 2 weeks 7 mg x 2 weeks As needed gum / lozenge*: 4 – 8 pieces per day /4 mg OR: Gum / Lozenge*: 12 – 16 4 -mg pieces per day x 8 weeks (not to exceed 24/20 pieces per day) 5 or more tins/week Comments If patch adjust dosage to be 14 mg as starting dose. (14 mg x 4 weeks; 7 mg x 4 weeks) If prt is concurrently using any other form of tobacco w/ ST, increase starting dosage to 21 mg patch Patch: 21 mg plus 4 -mg gum or lozenge*: 1 per waking hour OR: Gum/Lozenge*: 16 – 20 / 4 -mg gum or lozenge per day for 8 weeks (not to exceed 24/20 pieces per day) * for Lozenge enter First Tobacco Use to indicate within 30 minutes of waking © Dr. Herb Severson, Oregon Research Institute (ORI), 2010 #teachproject 172
 Snus • Moist smokeless tobacco, snuff • Although used worldwide, the highest consumption of snus is in Sweden • Associated with an increased risk of pancreatic cancer (RR 2. 0; 95% CI, 1. 2 -3. 3 a) a. The probability of an event (developing a disease) occurring in exposed people compared with the probability of the event in nonexposed people. Luo, Zendehdel et al. , (2007) Lancet, 370: 2015 -2020. #teachproject
Snus • Moist smokeless tobacco, snuff • Although used worldwide, the highest consumption of snus is in Sweden • Associated with an increased risk of pancreatic cancer (RR 2. 0; 95% CI, 1. 2 -3. 3 a) a. The probability of an event (developing a disease) occurring in exposed people compared with the probability of the event in nonexposed people. Luo, Zendehdel et al. , (2007) Lancet, 370: 2015 -2020. #teachproject
 Snus • Different from other chew tobacco – it is sterilized, decreasing the number of nitrosamines (cancer-causing agents) • Reduced risk of lung cancer • No emphysema • 2 x risk of pancreatic cancer (down from 3 x risk with smoking) #teachproject 174
Snus • Different from other chew tobacco – it is sterilized, decreasing the number of nitrosamines (cancer-causing agents) • Reduced risk of lung cancer • No emphysema • 2 x risk of pancreatic cancer (down from 3 x risk with smoking) #teachproject 174
 Snus Study • International researchers followed 279, 897 male Swedish construction workers from 1978 to 1992. About 26 percent were snus users, 37 percent were smokers and the rest never used tobacco. • For smokers, the incidence rate of pancreatic cancer was 13 cases per 100, 000 versus 8. 8 cases per 100, 000 for snus users. • Among those who did not use tobacco, the rate was 3. 9 cases per 100, 000. Luo, Zendehdel et al. , (2007) Lancet, 370: 2015 -2020. #teachproject 175
Snus Study • International researchers followed 279, 897 male Swedish construction workers from 1978 to 1992. About 26 percent were snus users, 37 percent were smokers and the rest never used tobacco. • For smokers, the incidence rate of pancreatic cancer was 13 cases per 100, 000 versus 8. 8 cases per 100, 000 for snus users. • Among those who did not use tobacco, the rate was 3. 9 cases per 100, 000. Luo, Zendehdel et al. , (2007) Lancet, 370: 2015 -2020. #teachproject 175
 Hookah: Waterpipe Tobacco Smoking • Shisha, a mixture of tobacco, molasses, and fruit flavors used in the hookah • Water in the hookah does not diminish tobacco toxicity • A 1 -hour session of hookah smoking exposes the user to 100 - 200 times the volume of smoke inhaled from a single cigarette 1 • Smoke produced contains high levels of carbon monoxide, heavy metals, and other carcinogens • Delivers significant levels of nicotine • Use has been significantly associated with lung cancer, respiratory illness, low birth weight, and periodontal disease 2 1. World Health Organization, 2005. Waterpipe tobacco smoking: building the evidence base. 2. Akl, Gaddam, et al. (2010). International Journal of Epidemiology, 39: 834 -857. #teachproject 176
Hookah: Waterpipe Tobacco Smoking • Shisha, a mixture of tobacco, molasses, and fruit flavors used in the hookah • Water in the hookah does not diminish tobacco toxicity • A 1 -hour session of hookah smoking exposes the user to 100 - 200 times the volume of smoke inhaled from a single cigarette 1 • Smoke produced contains high levels of carbon monoxide, heavy metals, and other carcinogens • Delivers significant levels of nicotine • Use has been significantly associated with lung cancer, respiratory illness, low birth weight, and periodontal disease 2 1. World Health Organization, 2005. Waterpipe tobacco smoking: building the evidence base. 2. Akl, Gaddam, et al. (2010). International Journal of Epidemiology, 39: 834 -857. #teachproject 176
 #teachproject 177
#teachproject 177
 #teachproject 178
#teachproject 178
 Smokeless Tobacco as Harm Reduction? (1) • As dependence-forming as cigarettes • Users develop cravings and nicotine withdrawal when abstaining • Does not produce second-hand-smoke BUT people who dip or chew spread their germs when they spit. This increases the risk of passing an infection to others. Benowitz (2011). Clinical Pharmacology & Therapeutics 90, 491 -493 American Cancer Society (2011). Quitting Smokeless Tobacco. #teachproject 179
Smokeless Tobacco as Harm Reduction? (1) • As dependence-forming as cigarettes • Users develop cravings and nicotine withdrawal when abstaining • Does not produce second-hand-smoke BUT people who dip or chew spread their germs when they spit. This increases the risk of passing an infection to others. Benowitz (2011). Clinical Pharmacology & Therapeutics 90, 491 -493 American Cancer Society (2011). Quitting Smokeless Tobacco. #teachproject 179
 Smokeless Tobacco as Harm Reduction? (2) • Most smokeless tobacco users are regular users before age 18 • Almost all users are male • High co-use of cigarettes (est. 10 -20%) • 38% of users develop oral lesions within 3 years Benowitz (2011). Clinical Pharmacology & Therapeutics 90, 491 -493 American Cancer Society (2011). Quitting Smokeless Tobacco. #teachproject 180
Smokeless Tobacco as Harm Reduction? (2) • Most smokeless tobacco users are regular users before age 18 • Almost all users are male • High co-use of cigarettes (est. 10 -20%) • 38% of users develop oral lesions within 3 years Benowitz (2011). Clinical Pharmacology & Therapeutics 90, 491 -493 American Cancer Society (2011). Quitting Smokeless Tobacco. #teachproject 180
 Smokeless Tobacco Cessation • Nicotine lozenge appears to be the most preferred cessation aid • Varenicline and behavioural interventions can assist cessation • Presence of lesions is an opportunity to motivate behaviour change • 2 week rule: If lesions do not heal within 2 weeks, recommend a biopsy Ebbert, Montori et al. (2011). Interventions for smokeless tobacco use cessation. Cochrane Database of Systematic Reviews (2). #teachproject 181
Smokeless Tobacco Cessation • Nicotine lozenge appears to be the most preferred cessation aid • Varenicline and behavioural interventions can assist cessation • Presence of lesions is an opportunity to motivate behaviour change • 2 week rule: If lesions do not heal within 2 weeks, recommend a biopsy Ebbert, Montori et al. (2011). Interventions for smokeless tobacco use cessation. Cochrane Database of Systematic Reviews (2). #teachproject 181
 New Smokeless Cessation Aid. Mint Snuff • Non tobacco product, edible and made with real mint • Safe to swallow/eat • Available in 4 flavours • Mint Snuff Pouches are miniature teabags filled with Mint and Mint Oil Crystals. • 1 -800 -EAT-MINT www. mintsnuff. com #teachproject 182
New Smokeless Cessation Aid. Mint Snuff • Non tobacco product, edible and made with real mint • Safe to swallow/eat • Available in 4 flavours • Mint Snuff Pouches are miniature teabags filled with Mint and Mint Oil Crystals. • 1 -800 -EAT-MINT www. mintsnuff. com #teachproject 182
 Bottom Line on Harm Reduction Using fewer tobacco products may have little to no effect on reducing morbidity and mortality BUT Reducing consumption may increase likelihood of future cessation #teachproject 183
Bottom Line on Harm Reduction Using fewer tobacco products may have little to no effect on reducing morbidity and mortality BUT Reducing consumption may increase likelihood of future cessation #teachproject 183
 What is your perspective on harm reduction and tobacco use? a. There is no such thing – all tobacco use is harmful b. I can see it that might be necessary with some populations c. I believe in using a harm reduction approach d. I’m not sure - I need more information #teachproject 184
What is your perspective on harm reduction and tobacco use? a. There is no such thing – all tobacco use is harmful b. I can see it that might be necessary with some populations c. I believe in using a harm reduction approach d. I’m not sure - I need more information #teachproject 184
 Evaluation and Wrap Up #teachproject 185
Evaluation and Wrap Up #teachproject 185
 Learning Objective Access additional clinical tools and resources to use in clinical practice and continuing professional development #teachproject 186
Learning Objective Access additional clinical tools and resources to use in clinical practice and continuing professional development #teachproject 186
 TEACH Community of Practice & Listserv As a graduate of this course, you are eligible to join the TEACH Community of Practice Listserv! Our TEACH COP Listserv is configured so that you need to self-register, which quick and easy to do. To “subscribe” to the Listserv, please send an email to: teach-request@info 2. camh. net and write: “subscribe teach” in the subject line of your email. You will then receive a message confirming your subscription to the List, as well as instructions on how to post or unsubscribe. #teachproject 187
TEACH Community of Practice & Listserv As a graduate of this course, you are eligible to join the TEACH Community of Practice Listserv! Our TEACH COP Listserv is configured so that you need to self-register, which quick and easy to do. To “subscribe” to the Listserv, please send an email to: teach-request@info 2. camh. net and write: “subscribe teach” in the subject line of your email. You will then receive a message confirming your subscription to the List, as well as instructions on how to post or unsubscribe. #teachproject 187
 Course Evaluation: 3 Things to Remember 1. Please complete the Evaluation Form before you leave. 2. Log on to the TEACH Website to make sure you’ve completed Learning Assessments # 1 & #2 (you must complete both in order to receive the CAMH Letter of Completion and U of T Certificate). 3. Online follow-up survey in three and six months – TEACH will send you a reminder ! #teachproject 188
Course Evaluation: 3 Things to Remember 1. Please complete the Evaluation Form before you leave. 2. Log on to the TEACH Website to make sure you’ve completed Learning Assessments # 1 & #2 (you must complete both in order to receive the CAMH Letter of Completion and U of T Certificate). 3. Online follow-up survey in three and six months – TEACH will send you a reminder ! #teachproject 188
 Are you interested in becoming a Tobacco Cessation Practice Leader? An Opportunity to…. Possible Roles…. . • Develop your skills - Clinical Consultation • Network - Conference Speaker • Attend TEACH courses - In –Service Trainer • Achieve credit units - Media Interviews - Resource Link Questions? Email: teach@camh. net #teachproject 189
Are you interested in becoming a Tobacco Cessation Practice Leader? An Opportunity to…. Possible Roles…. . • Develop your skills - Clinical Consultation • Network - Conference Speaker • Attend TEACH courses - In –Service Trainer • Achieve credit units - Media Interviews - Resource Link Questions? Email: teach@camh. net #teachproject 189
 How would you rate this course? a. Excellent b. Very good c. Good d. Fair e. Poor #teachproject 190
How would you rate this course? a. Excellent b. Very good c. Good d. Fair e. Poor #teachproject 190
 Quick Break See you in 10 minutes! #teachproject 191
Quick Break See you in 10 minutes! #teachproject 191
 TEACH Exam #teachproject 192
TEACH Exam #teachproject 192
 Please remember to leave your i-clicker on your table, Thanks. #teachproject 193
Please remember to leave your i-clicker on your table, Thanks. #teachproject 193
 #teachproject 194
#teachproject 194


