e23335d24ad608dc5c09489ac3341137.ppt
- Количество слайдов: 60
 Taking a sexual history Dr Kate Armitage June 2016 SHA conference, Leeds
Taking a sexual history Dr Kate Armitage June 2016 SHA conference, Leeds
 Biography • GP at Leeds Student Medical Practice since 2008 -Partner since November 2014 • Staff grade in GUM before becoming a GP in 2007 • Honorary Secretary, Faculty of Sexual and Reproductive Health since June 2015
Biography • GP at Leeds Student Medical Practice since 2008 -Partner since November 2014 • Staff grade in GUM before becoming a GP in 2007 • Honorary Secretary, Faculty of Sexual and Reproductive Health since June 2015
 Disclosure of interests • Bayer since 2010 • Investigator sponsor study/speaker fees/attending conferences • MSD since 2010 • Investigator sponsor study/speaker fees • Pfizer 2013 • Speaker fees • Hon Sec role at FSRH in education and training
Disclosure of interests • Bayer since 2010 • Investigator sponsor study/speaker fees/attending conferences • MSD since 2010 • Investigator sponsor study/speaker fees • Pfizer 2013 • Speaker fees • Hon Sec role at FSRH in education and training
 And you? . . • Who in the room is a • GP? • Nurse? • Any other staff group?
And you? . . • Who in the room is a • GP? • Nurse? • Any other staff group?
 Some sobering thoughts… • Sexual health of the UK population is in decline • UK has highest teen pregnancy rate in Western Europe • TOP rates have increased over recent years • Anecdotal evidence that many women not offered a range of contraceptive options especially LARC
Some sobering thoughts… • Sexual health of the UK population is in decline • UK has highest teen pregnancy rate in Western Europe • TOP rates have increased over recent years • Anecdotal evidence that many women not offered a range of contraceptive options especially LARC
 And there is more… • Rates of STIs are increasing • Burden in under 25 s, urban areas
And there is more… • Rates of STIs are increasing • Burden in under 25 s, urban areas
 HIV in the UK-situation report 2015 • • 2015 approx 103, 000 people living with HIV 1. 9 per 1000 adults ( over 15) Approx 18, 100 of these unaware of status (17%) Men who have sex with men (MSM) age 15 -44: 1 in 20 living with HIV • 2014: 69% of eligible GUM attendees tested for HIV • Document advocates ‘ask your GP for a HIV test’ • Home testing for HIV www. freetesting. hiv
HIV in the UK-situation report 2015 • • 2015 approx 103, 000 people living with HIV 1. 9 per 1000 adults ( over 15) Approx 18, 100 of these unaware of status (17%) Men who have sex with men (MSM) age 15 -44: 1 in 20 living with HIV • 2014: 69% of eligible GUM attendees tested for HIV • Document advocates ‘ask your GP for a HIV test’ • Home testing for HIV www. freetesting. hiv
 Nat. SAL • National survey of sexual attitudes and lifestyles • 1990 • 2000 • 2010
Nat. SAL • National survey of sexual attitudes and lifestyles • 1990 • 2000 • 2010
 Nat. SAL-1 • 2000 -over 11, 000 respondents • 16 -24 yr olds had highest rates of new partners • 1/3 rd men and 1/10 th women had at least 10 lifetime partners • 4. 3% men have paid for sex • 5. 4% men and 4. 9% women had same sex contacts
Nat. SAL-1 • 2000 -over 11, 000 respondents • 16 -24 yr olds had highest rates of new partners • 1/3 rd men and 1/10 th women had at least 10 lifetime partners • 4. 3% men have paid for sex • 5. 4% men and 4. 9% women had same sex contacts
 Nat. SAL-1 and -2 • Comparing 2000 to 1990 figures • • • Earlier age of first sexual intercourse Increased number of lifetime partners Decline in marriage, growth in cohabitation Increased partner change Decreased condom use
Nat. SAL-1 and -2 • Comparing 2000 to 1990 figures • • • Earlier age of first sexual intercourse Increased number of lifetime partners Decline in marriage, growth in cohabitation Increased partner change Decreased condom use
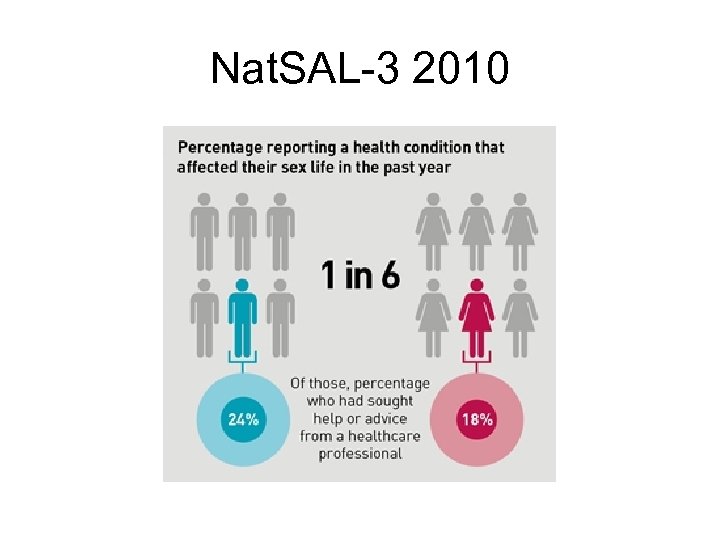 Nat. SAL-3 2010
Nat. SAL-3 2010
 Taking a sexual history
Taking a sexual history
 Sexual health care • Includes • Risk assessment • Prevention, diagnosis and treatment of STIs • Contraception • Management of unplanned pregnancy
Sexual health care • Includes • Risk assessment • Prevention, diagnosis and treatment of STIs • Contraception • Management of unplanned pregnancy
 Barriers to delivery of sexual health care in general practice ? • • • Time Other priorities Confidence Knowledge and skills Technical issues ( access to tests/labs etc) • Confidentiality/anonymity • Partner notification • Conflict between public health and that of individual
Barriers to delivery of sexual health care in general practice ? • • • Time Other priorities Confidence Knowledge and skills Technical issues ( access to tests/labs etc) • Confidentiality/anonymity • Partner notification • Conflict between public health and that of individual
 Remember… • Most STIs are asymptomatic • Risk assessment is the key to management • History taking is the key to risk management
Remember… • Most STIs are asymptomatic • Risk assessment is the key to management • History taking is the key to risk management
 So-before you start. . • Consider • Physical environment • Privacy • Confidentiality
So-before you start. . • Consider • Physical environment • Privacy • Confidentiality
 Communication • Clinic literature- advertising the need for sexual history taking-this may improve acceptability • Communication skills of clinician including attitudes and beliefs-use non judgemental inclusive language • Communication issues for patient such as access to interpreters
Communication • Clinic literature- advertising the need for sexual history taking-this may improve acceptability • Communication skills of clinician including attitudes and beliefs-use non judgemental inclusive language • Communication issues for patient such as access to interpreters
 What do you think is the most difficult question to ask/subject to raise during sexual history taking? A moment to give it some thought and write it on a post it note. You can discuss with your neighbour if you wish!
What do you think is the most difficult question to ask/subject to raise during sexual history taking? A moment to give it some thought and write it on a post it note. You can discuss with your neighbour if you wish!
 Components of a sexual history • • Symptoms-to guide examination and tests Exposure history Contraception use/pregnancy risk Other sexual health issues ( including psychosexual issues) • HIV/ Hep. B/Hep. C risk assessment for testing and prevention • Assessment of risk behaviours, leading to partner notification and sexual health promotion
Components of a sexual history • • Symptoms-to guide examination and tests Exposure history Contraception use/pregnancy risk Other sexual health issues ( including psychosexual issues) • HIV/ Hep. B/Hep. C risk assessment for testing and prevention • Assessment of risk behaviours, leading to partner notification and sexual health promotion
 Reason for attendance • Symptoms • No symptoms-why today? • Contact? • Response to media article? Etc etc
Reason for attendance • Symptoms • No symptoms-why today? • Contact? • Response to media article? Etc etc
 Symptoms • Women • Men • • • Change to discharge Change to bleeding Dysuria Abdominal pain Pain with sex Genital skin problems Urethral discharge Dysuria Testicular pain Genital skin problems • Perianal/anal symptoms
Symptoms • Women • Men • • • Change to discharge Change to bleeding Dysuria Abdominal pain Pain with sex Genital skin problems Urethral discharge Dysuria Testicular pain Genital skin problems • Perianal/anal symptoms
 Core component of sexual history • • • Last sexual intercourse (LSI) Partner gender/sites of exposure*/condom use Previous sexual partner (PSP) as for LSI Women: LMP/contraception/cytology HIV risk history Hep B and C risk assessment Any child protection concerns? Access to results * most practitioners worry about asking this
Core component of sexual history • • • Last sexual intercourse (LSI) Partner gender/sites of exposure*/condom use Previous sexual partner (PSP) as for LSI Women: LMP/contraception/cytology HIV risk history Hep B and C risk assessment Any child protection concerns? Access to results * most practitioners worry about asking this
 How to ask…. • May use ‘warning shot’ • ‘I am going to ask you some personal questions, these are all for a reason, and they are all confidential-is that ok with you? ’ • Don’t apologise…
How to ask…. • May use ‘warning shot’ • ‘I am going to ask you some personal questions, these are all for a reason, and they are all confidential-is that ok with you? ’ • Don’t apologise…
 How to ask…. . • ‘when did you last have sex/sexual contact? ’ • ‘was that with a regular or a one-off partner? ’ ‘ was it someone you know or didn’t know? ’ • ‘was that a male or female partner? ’ • What kind of sex was it? Was it vaginal/oral/anal sex’ • ‘Did you use condoms? Do you use condoms always, sometimes or never? ’ • ‘does that person have any symptoms? ’
How to ask…. . • ‘when did you last have sex/sexual contact? ’ • ‘was that with a regular or a one-off partner? ’ ‘ was it someone you know or didn’t know? ’ • ‘was that a male or female partner? ’ • What kind of sex was it? Was it vaginal/oral/anal sex’ • ‘Did you use condoms? Do you use condoms always, sometimes or never? ’ • ‘does that person have any symptoms? ’
 How to ask… ‘When was the last time you had sex with somebody different? ’ ……as for last sexual intercourse
How to ask… ‘When was the last time you had sex with somebody different? ’ ……as for last sexual intercourse
 How not to ask. . • • • No closed questions to start ‘Are you married? ’ ‘Are you in a stable relationship? ’ ‘Are you sexually active? ’ ‘are you homosexual? ’ Want questions that are precise and useful without being blunt, that are understood by both patient and clinician
How not to ask. . • • • No closed questions to start ‘Are you married? ’ ‘Are you in a stable relationship? ’ ‘Are you sexually active? ’ ‘are you homosexual? ’ Want questions that are precise and useful without being blunt, that are understood by both patient and clinician
 Sexual history • Should include all partners within past three months as rough guide • ‘How many sexual partners have you had in the past three months? ’ • If not already established with male patients, ‘have you ever had sex with another man? ’
Sexual history • Should include all partners within past three months as rough guide • ‘How many sexual partners have you had in the past three months? ’ • If not already established with male patients, ‘have you ever had sex with another man? ’
 Also relevant. . • Past history of STIs including details of treatment and compliance/follow up • Past medical and surgical history • Drug history/allergies • Contraceptive and reproductive health history • Asking men what contraception their female partner is using?
Also relevant. . • Past history of STIs including details of treatment and compliance/follow up • Past medical and surgical history • Drug history/allergies • Contraceptive and reproductive health history • Asking men what contraception their female partner is using?
 HIV risk assessment • Current/past use of injecting drugs, personal history or that of partners • SI with anyone from abroad • SI with men/bisexual partner • Medical treatment abroad • SI with HIV positive partner • Sex work • History of HIV testing
HIV risk assessment • Current/past use of injecting drugs, personal history or that of partners • SI with anyone from abroad • SI with men/bisexual partner • Medical treatment abroad • SI with HIV positive partner • Sex work • History of HIV testing
 HIV risk assessment • ‘Have you ever injected drugs? Or had sex with anyone who injected drugs? ’ • ‘Have you had sex with someone born outside the UK? ’ (Country/dates) • ‘Have you had any operations or blood transfusions abroad? ’ • ‘Have you ever had sex with another man? ’ • ‘Have you had sex with a man who had sex with men? ’
HIV risk assessment • ‘Have you ever injected drugs? Or had sex with anyone who injected drugs? ’ • ‘Have you had sex with someone born outside the UK? ’ (Country/dates) • ‘Have you had any operations or blood transfusions abroad? ’ • ‘Have you ever had sex with another man? ’ • ‘Have you had sex with a man who had sex with men? ’
 HIV risk assessment (2) • ‘have you had sex with anyone you knew to have HIV? ’ • ‘Have you ever paid for sex, or been paid for sex? ’ • If the answer is yes to any of the above, they are in a higher risk group • ‘Have you ever had a test for HIV? When/where/what was result? ’
HIV risk assessment (2) • ‘have you had sex with anyone you knew to have HIV? ’ • ‘Have you ever paid for sex, or been paid for sex? ’ • If the answer is yes to any of the above, they are in a higher risk group • ‘Have you ever had a test for HIV? When/where/what was result? ’
 HIV testing discussion • Compare your objective risk assessment as clinician with subjective risk assessment of patient • Further discussion if patient is high risk • Discussion may also occur if mismatch in risk assessments
HIV testing discussion • Compare your objective risk assessment as clinician with subjective risk assessment of patient • Further discussion if patient is high risk • Discussion may also occur if mismatch in risk assessments
 HIV testing discussion • What do you think the result will be? ’ • ‘Have you given any thought to how you may feel if the result is positive? ’ ‘Who will you tell/what support have you got if the result is positive? ’ • Discuss what would happen in event of positive result-repeat testing/HIV care under GUM • Arranging to give result -in person if high risk
HIV testing discussion • What do you think the result will be? ’ • ‘Have you given any thought to how you may feel if the result is positive? ’ ‘Who will you tell/what support have you got if the result is positive? ’ • Discuss what would happen in event of positive result-repeat testing/HIV care under GUM • Arranging to give result -in person if high risk
 Blood borne viruses (BBV) • Hepatitis B and C • Risk assessment broadly similar to HIV • In high risk groups • Consider Hep B vaccination history +/starting vax course • Consider Hep B and C testing
Blood borne viruses (BBV) • Hepatitis B and C • Risk assessment broadly similar to HIV • In high risk groups • Consider Hep B vaccination history +/starting vax course • Consider Hep B and C testing
 Other risks • Alcohol and drugs • Useful to ask as can give idea of patients approach to risk taking behaviour, or whether they are taking risks with sex when under the influence • Though can be distractors from focus when taking sexual history, taking time to discuss but may not influence management on this occasion ( revisit at later consults)
Other risks • Alcohol and drugs • Useful to ask as can give idea of patients approach to risk taking behaviour, or whether they are taking risks with sex when under the influence • Though can be distractors from focus when taking sexual history, taking time to discuss but may not influence management on this occasion ( revisit at later consults)
 Other risks • Mental health issues • Mania • Disinhibition • Hypersexuality
Other risks • Mental health issues • Mania • Disinhibition • Hypersexuality
 Access to results • • Important to clarify with patient at time of testing In person? Phone message for patient note? Phone call with clinician? • Many different approaches taken in GUM services, for example • Text • ‘No news is good news’? What do you think of this approach?
Access to results • • Important to clarify with patient at time of testing In person? Phone message for patient note? Phone call with clinician? • Many different approaches taken in GUM services, for example • Text • ‘No news is good news’? What do you think of this approach?
 To recap……. Components of a sexual history • • Symptoms-to guide examination and tests Exposure history Contraception use/pregnancy risk Other sexual health issues ( including psychosexual issues) • HIV/ Hep. B/Hep. C risk assessment for testing and prevention • Assessment of risk behaviours, leading to partner notification and sexual health promotion
To recap……. Components of a sexual history • • Symptoms-to guide examination and tests Exposure history Contraception use/pregnancy risk Other sexual health issues ( including psychosexual issues) • HIV/ Hep. B/Hep. C risk assessment for testing and prevention • Assessment of risk behaviours, leading to partner notification and sexual health promotion
 Child protection issues • Under 16 s • Some laws relevant to under 18 s such as grooming/exploitation and sex work • Assessing competency to consent to history taking and examination, documenting this • Fraser guidelines
Child protection issues • Under 16 s • Some laws relevant to under 18 s such as grooming/exploitation and sex work • Assessing competency to consent to history taking and examination, documenting this • Fraser guidelines
 Child protection issues • • • Relevant to establish & document include Age of partner/s Age at sexual debut Parents/carer awareness of sexual activity Parents/carer awareness of clinic attendance Coercion Transactional sex Educational venue/attendance Vulnerability
Child protection issues • • • Relevant to establish & document include Age of partner/s Age at sexual debut Parents/carer awareness of sexual activity Parents/carer awareness of clinic attendance Coercion Transactional sex Educational venue/attendance Vulnerability
 Child protection issues • Discuss with colleagues • Child protection training • Local child protection leads/named GP and nurse
Child protection issues • Discuss with colleagues • Child protection training • Local child protection leads/named GP and nurse
 After taking a history • Access to results (see previous slide) • Explaining examination, investigation and management • Documentation of history (proformas/templates? )
After taking a history • Access to results (see previous slide) • Explaining examination, investigation and management • Documentation of history (proformas/templates? )
 Follow up • Sexual histories are dynamic and can change within days • Low threshold for retaking history and reexamining
Follow up • Sexual histories are dynamic and can change within days • Low threshold for retaking history and reexamining
 Scenarios 4 to consider Spend a minute thinking what you would ask this patient/discuss with your neighbour before I reveal the relevant details
Scenarios 4 to consider Spend a minute thinking what you would ask this patient/discuss with your neighbour before I reveal the relevant details
 Scenario 1 • Amit • Age 22 • Pain passing urine • What do you ask?
Scenario 1 • Amit • Age 22 • Pain passing urine • What do you ask?
 Would you have established that. . • Amit was born in India, been in the UK 4 months • He has had pain passing urine for 2 weeks • He has regular female partner of 4 years ( his wife) and does not use condoms • He has never had any other lifetime partners
Would you have established that. . • Amit was born in India, been in the UK 4 months • He has had pain passing urine for 2 weeks • He has regular female partner of 4 years ( his wife) and does not use condoms • He has never had any other lifetime partners
 Scenario 2 • Amit • Age 22 • Pain passing urine • What do you ask?
Scenario 2 • Amit • Age 22 • Pain passing urine • What do you ask?
 Would you have established that. . • Amit was born in Bradford • Amit has had pain passing urine for 7 days • He last had sex a week ago with his regular female partner of 7 months, intermittent condom use for VI, no OI • He last had sex with someone different on holiday in Tenerife a month ago, she was from UK, no condoms used
Would you have established that. . • Amit was born in Bradford • Amit has had pain passing urine for 7 days • He last had sex a week ago with his regular female partner of 7 months, intermittent condom use for VI, no OI • He last had sex with someone different on holiday in Tenerife a month ago, she was from UK, no condoms used
 Scenario 3 • Amit • Age 22 • Pain passing urine • What do you ask?
Scenario 3 • Amit • Age 22 • Pain passing urine • What do you ask?
 Would you have established that. . • • Amit is from Kenya, studying in the UK He has had pain passing urine for 7 days He has been in the UK for 6 months His last sexual contact was when he paid for oral sex 2 weeks ago in London
Would you have established that. . • • Amit is from Kenya, studying in the UK He has had pain passing urine for 7 days He has been in the UK for 6 months His last sexual contact was when he paid for oral sex 2 weeks ago in London
 Scenario 4 • Amit • Age 22 • Pain passing urine • What do you ask?
Scenario 4 • Amit • Age 22 • Pain passing urine • What do you ask?
 Would you have established that. . • Amit is a first generation Ghanaian Indian, who has been in the UK since October 2010 • He has had pain passing urine for the past 7 days • He has had 10 male partners in the past three months, he has had anal sex without condoms • He last had sex with a woman 4 months ago
Would you have established that. . • Amit is a first generation Ghanaian Indian, who has been in the UK since October 2010 • He has had pain passing urine for the past 7 days • He has had 10 male partners in the past three months, he has had anal sex without condoms • He last had sex with a woman 4 months ago
 Key points Risk assessment is the key to management History taking is the key to risk assessment Don’t apologise for asking Don’t make assumptions
Key points Risk assessment is the key to management History taking is the key to risk assessment Don’t apologise for asking Don’t make assumptions
 Role play If we have time!
Role play If we have time!
 Role play • Tim • Age 24 • Registered today • Jane • Age 20 • Registered today
Role play • Tim • Age 24 • Registered today • Jane • Age 20 • Registered today
 Role play • • • Tim age 24 Dysuria 5 days Some testicular pain One off SI with FP on holiday in Ibiza 2 FP on holiday-5 partners in 3 months No condoms, drinks 30 units a week No SI with men Concerned is ‘thrush’, never had any tests Low risk for HIV on questioning
Role play • • • Tim age 24 Dysuria 5 days Some testicular pain One off SI with FP on holiday in Ibiza 2 FP on holiday-5 partners in 3 months No condoms, drinks 30 units a week No SI with men Concerned is ‘thrush’, never had any tests Low risk for HIV on questioning
 Role play • • Jane age 20 Vaginal discharge 2 wks, not itchy Small sore on vulva today, painful Last SI 3 wk ago with reg MP one year Previous SI 4 wk ago with one off MP Implant one year, no condoms Never had STI testing Low risk for HIV on direct questioning
Role play • • Jane age 20 Vaginal discharge 2 wks, not itchy Small sore on vulva today, painful Last SI 3 wk ago with reg MP one year Previous SI 4 wk ago with one off MP Implant one year, no condoms Never had STI testing Low risk for HIV on direct questioning
 Further reading • http: //www. bashh. org/documents/Sexual% 20 History%20 Taking%20 guideline%20201 3. pdf • 2013 UK national guideline for consultations requiring sexual history taking • BASHH-British Association for Sexual Health and HIV
Further reading • http: //www. bashh. org/documents/Sexual% 20 History%20 Taking%20 guideline%20201 3. pdf • 2013 UK national guideline for consultations requiring sexual history taking • BASHH-British Association for Sexual Health and HIV
 Further training in Sexual and Reproductive Health • RCGP Introductory Certificate in Sexual Health • http: //www. rcgp. org. uk/substance_misuse/sex__drugs_and_hiv_group/i ntro_cert_in_sexual_health. aspx • FSRH- Diploma/DFSRH • New course-SRH essentials for Practice Nurses • BASHH- STIF training • ‘Core’ and ‘plus’ course • Clinical competencies assessments
Further training in Sexual and Reproductive Health • RCGP Introductory Certificate in Sexual Health • http: //www. rcgp. org. uk/substance_misuse/sex__drugs_and_hiv_group/i ntro_cert_in_sexual_health. aspx • FSRH- Diploma/DFSRH • New course-SRH essentials for Practice Nurses • BASHH- STIF training • ‘Core’ and ‘plus’ course • Clinical competencies assessments
 Thank you Any questions? Catherine. armitage@nhs. net
Thank you Any questions? Catherine. armitage@nhs. net


