a8c9e3bc8003e1e2bd649aea232c33fa.ppt
- Количество слайдов: 36
 SYRINGE DRIVERS Coranne Rice. Clinical Nurse Specialist in Palliative Care Beaumont Hospital. 23 rd Sept 2010
SYRINGE DRIVERS Coranne Rice. Clinical Nurse Specialist in Palliative Care Beaumont Hospital. 23 rd Sept 2010
 Definition. n A portable battery operated pump, which delivers a continuous subcutaneous infusion over a specified period of time. Dickman et al 2005
Definition. n A portable battery operated pump, which delivers a continuous subcutaneous infusion over a specified period of time. Dickman et al 2005
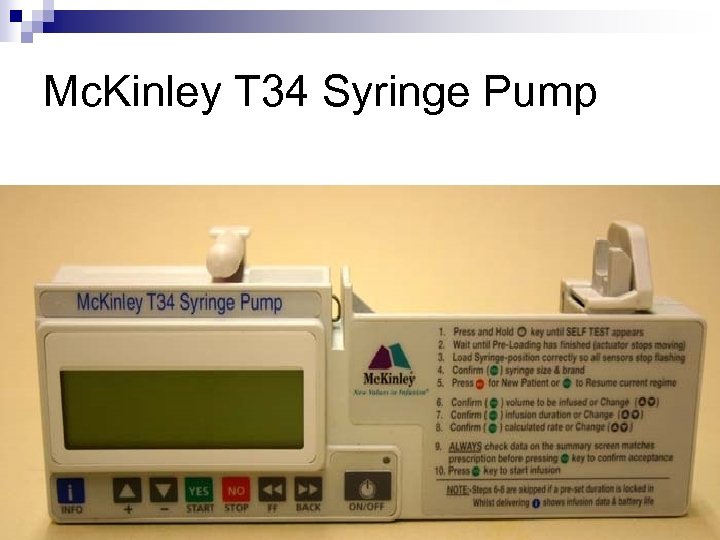 Mc. Kinley T 34 Syringe Pump
Mc. Kinley T 34 Syringe Pump
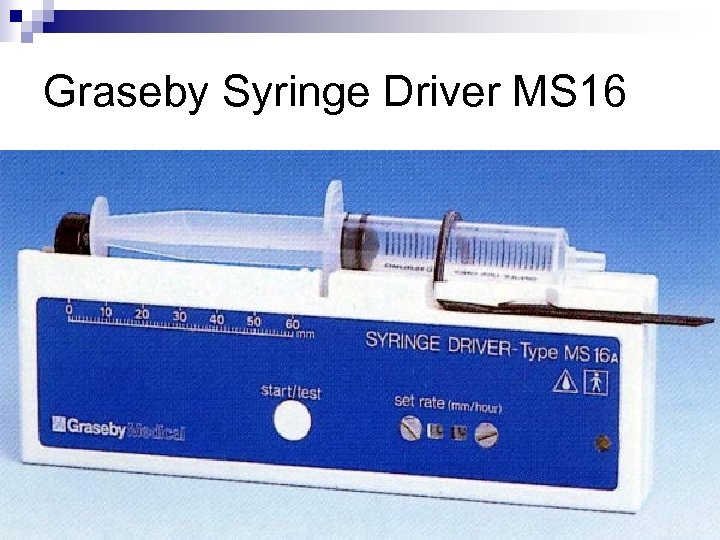 Graseby Syringe Driver MS 16
Graseby Syringe Driver MS 16
 Aims. Delivers a continuous infusion of drugs via subcutaneous route. n Ensures a stable plasma level of drugs. n Eliminates the need for repeated injections. n Used when oral medications are no longer appropriate for a number of reasons. n
Aims. Delivers a continuous infusion of drugs via subcutaneous route. n Ensures a stable plasma level of drugs. n Eliminates the need for repeated injections. n Used when oral medications are no longer appropriate for a number of reasons. n
 Indications For Use n n n Persistent nausea and vomiting Inability to swallow oral medications. Severe mucositis Poor alimentary absorption (intestinal obstruction/ mal-absorption) Intractable pain not controlled by oral medications Rectal route not appropriate.
Indications For Use n n n Persistent nausea and vomiting Inability to swallow oral medications. Severe mucositis Poor alimentary absorption (intestinal obstruction/ mal-absorption) Intractable pain not controlled by oral medications Rectal route not appropriate.
 Drugs used in Syringe Drivers Analgesics. n Anti emetics. n Sedatives. n Drying agents. n
Drugs used in Syringe Drivers Analgesics. n Anti emetics. n Sedatives. n Drying agents. n
 Analgesics Morphine Sulphate. n Oxycodone. n Hydromorphone. n Fentanyl. n Diclofenac. n
Analgesics Morphine Sulphate. n Oxycodone. n Hydromorphone. n Fentanyl. n Diclofenac. n
 Morphine Sulphate Opioid of choice. n Most commonly used. n Controlled drug. n Preparations – 10, 15, 30, 60 100 mg/ml vials. n
Morphine Sulphate Opioid of choice. n Most commonly used. n Controlled drug. n Preparations – 10, 15, 30, 60 100 mg/ml vials. n
 Oxycodone. Twice as strong as Morphine Sulphate eg. Morphine Sulphate 60 mgs = Oxycodone 30 mgs. n Controlled drug. n Used in patients with renal failure. n Caution when mixed with Cyclizine. n Preparation - 10 mg/ml vial n
Oxycodone. Twice as strong as Morphine Sulphate eg. Morphine Sulphate 60 mgs = Oxycodone 30 mgs. n Controlled drug. n Used in patients with renal failure. n Caution when mixed with Cyclizine. n Preparation - 10 mg/ml vial n
 Hydromorphone Six times stronger than Morphine Sulphate eg. Morphine Sulphate 60 mgs = Hydromorphone 10 mgs. n Controlled drug. n Used in patients with renal failure. n Preparation - 20 mg/ml vial. n
Hydromorphone Six times stronger than Morphine Sulphate eg. Morphine Sulphate 60 mgs = Hydromorphone 10 mgs. n Controlled drug. n Used in patients with renal failure. n Preparation - 20 mg/ml vial. n
 Fentanyl Used under the advice of Specialist Palliative Care. n Opioid. n Controlled drug. n Used in patients with renal failure n
Fentanyl Used under the advice of Specialist Palliative Care. n Opioid. n Controlled drug. n Used in patients with renal failure n
 Diclofenac. Difene. n Non steroidal anti-inflammatory drug (NSAID). n Total dose in 24 hrs -150 mgs. n Caution in patients with renal failure and peptic ulcer disease. n Mix with Na. Cl in a 20 ml syringe. n Use a separate syringe driver. n
Diclofenac. Difene. n Non steroidal anti-inflammatory drug (NSAID). n Total dose in 24 hrs -150 mgs. n Caution in patients with renal failure and peptic ulcer disease. n Mix with Na. Cl in a 20 ml syringe. n Use a separate syringe driver. n
 Anti Emetics Cyclizine. n Metoclopramide. n Haloperidol. n Methotrimeprazine. n Ondansetron. n
Anti Emetics Cyclizine. n Metoclopramide. n Haloperidol. n Methotrimeprazine. n Ondansetron. n
 Cyclizine Valoid. n Nausea/Vomiting caused by stimulation of the vomiting centre or vagus nerve eg. raised intracranial pressure, radiotherapy to head/ neck, bowel obstruction and movement. n Preparation - 50 mg/ml vial. n Total dose in 24 hrs – 150 mgs. n Incompatible with Buscopan and used with caution with Oxycodone. n
Cyclizine Valoid. n Nausea/Vomiting caused by stimulation of the vomiting centre or vagus nerve eg. raised intracranial pressure, radiotherapy to head/ neck, bowel obstruction and movement. n Preparation - 50 mg/ml vial. n Total dose in 24 hrs – 150 mgs. n Incompatible with Buscopan and used with caution with Oxycodone. n
 Metoclopramide Maxalon. n Nausea/Vomiting caused by drugs, gastric stasis, partial obstruction, constipation. n Preparation - 20 mg/2 ml vial. n Total dose in 24 hrs - 120 mgs n Caution when used with Cyclizine. n
Metoclopramide Maxalon. n Nausea/Vomiting caused by drugs, gastric stasis, partial obstruction, constipation. n Preparation - 20 mg/2 ml vial. n Total dose in 24 hrs - 120 mgs n Caution when used with Cyclizine. n
 Haloperidol Serenace. n Nausea/Vomiting caused by stimulation of the chemoreceptor trigger zone eg. Drugs (especially opioids), intestinal obstruction, hypercalcaemia. n Preparation - 5 mg/ml vial. n Can be used for the treatment of Delirium. n
Haloperidol Serenace. n Nausea/Vomiting caused by stimulation of the chemoreceptor trigger zone eg. Drugs (especially opioids), intestinal obstruction, hypercalcaemia. n Preparation - 5 mg/ml vial. n Can be used for the treatment of Delirium. n
 Methotrimeprazine. Nozinan. n Broad acting anti emetic. n Acts on main receptor sites involved in the vomiting pathway n Strong sedative effect. n Preparation – 25 mg/ml vial. n Can be used in the treatment of agitation. n
Methotrimeprazine. Nozinan. n Broad acting anti emetic. n Acts on main receptor sites involved in the vomiting pathway n Strong sedative effect. n Preparation – 25 mg/ml vial. n Can be used in the treatment of agitation. n
 Ondansetron Zofran n Nausea/Vomiting caused by chemotherapy and radiotherapy. n Total dose in 24 hrs – 32 mgs. n Caution - causes constipation. n
Ondansetron Zofran n Nausea/Vomiting caused by chemotherapy and radiotherapy. n Total dose in 24 hrs – 32 mgs. n Caution - causes constipation. n
 Sedatives Midazolam n Haloperidol (Serenace) n Methotrimeprazine (Nozinan) n Clonazepam n
Sedatives Midazolam n Haloperidol (Serenace) n Methotrimeprazine (Nozinan) n Clonazepam n
 Midazolam. Short acting benzodiazepine n Used in the treatment of agitation, anxiety, seizures, myoclonus n Preparation 10 mg/2 ml vial n Can use up to 60 mgs in 24 hrs. n
Midazolam. Short acting benzodiazepine n Used in the treatment of agitation, anxiety, seizures, myoclonus n Preparation 10 mg/2 ml vial n Can use up to 60 mgs in 24 hrs. n
 Clonazepam Used under the advice of Specialist Palliative Care. n Benzodiazepine. n Used in the treatment of neuropathic pain, agitation, anxiety, seizures and myoclonus. n Preparation – 1 mg/ml vial. n
Clonazepam Used under the advice of Specialist Palliative Care. n Benzodiazepine. n Used in the treatment of neuropathic pain, agitation, anxiety, seizures and myoclonus. n Preparation – 1 mg/ml vial. n
 Drying Agents n Hyoscine Butylbromide (Buscopan) n Glycopyrronium (Robinul) n Hyoscine Hydrobromide (Hyoscine)
Drying Agents n Hyoscine Butylbromide (Buscopan) n Glycopyrronium (Robinul) n Hyoscine Hydrobromide (Hyoscine)
 Hyoscine Butylbromide Buscopan. n 1 st drug of choice. n Non sedating. n Doesn’t cross the blood brain barrier. n Incompatible with Cyclizine. n Preparation - 20 mg/ml vial. n Maximum dose in 24 hrs -120 mgs. n
Hyoscine Butylbromide Buscopan. n 1 st drug of choice. n Non sedating. n Doesn’t cross the blood brain barrier. n Incompatible with Cyclizine. n Preparation - 20 mg/ml vial. n Maximum dose in 24 hrs -120 mgs. n
 Glycopyrronium Robinul. n Non sedating. n Doesn’t cross the blood brain barrier. n Preparation 200 mcg/ml vial. n Maximum dose in 24 hrs – 2. 4 mgs. n
Glycopyrronium Robinul. n Non sedating. n Doesn’t cross the blood brain barrier. n Preparation 200 mcg/ml vial. n Maximum dose in 24 hrs – 2. 4 mgs. n
 Hyoscine Hydrobromide Hyoscine. n Crosses the blood brain barrier. n Can cause agitation and delirium n Preparation – 400, 600 mcg/ml vials n Maximum dose in 24 hrs – 2. 4 mgs. n Not recommended in Palliative Care. n
Hyoscine Hydrobromide Hyoscine. n Crosses the blood brain barrier. n Can cause agitation and delirium n Preparation – 400, 600 mcg/ml vials n Maximum dose in 24 hrs – 2. 4 mgs. n Not recommended in Palliative Care. n
 Other Drugs occasionally used Octreotide n Phenobarbitone n Ketamine n Methadone n Dexamethasone n
Other Drugs occasionally used Octreotide n Phenobarbitone n Ketamine n Methadone n Dexamethasone n
 Octreotide Used under the advice of Specialist Palliative Care. n Reduction of intestinal secretions n Used in the treatment of excessive diarrhoea or large volume vomiting. n Preparation 100, 500 mcg vials. n Can use up to 2, 000 mcg in 24 hrs. n
Octreotide Used under the advice of Specialist Palliative Care. n Reduction of intestinal secretions n Used in the treatment of excessive diarrhoea or large volume vomiting. n Preparation 100, 500 mcg vials. n Can use up to 2, 000 mcg in 24 hrs. n
 Phenobarbitone Used under the advice of Specialist Palliative Care. n Long acting barbiturate. n Anti epileptic. n Controlled drug n Preparation -200 mg/ml vial. n Can use up to 1, 200 mgs in 24 hrs. n Used in terminal restlessness/agitation n Used in separate syringe driver n
Phenobarbitone Used under the advice of Specialist Palliative Care. n Long acting barbiturate. n Anti epileptic. n Controlled drug n Preparation -200 mg/ml vial. n Can use up to 1, 200 mgs in 24 hrs. n Used in terminal restlessness/agitation n Used in separate syringe driver n
 Drugs never used in Syringe Drivers Diazepam n Chlorpromazine (Largactil) n Prochlorperazine (Stemetil) n
Drugs never used in Syringe Drivers Diazepam n Chlorpromazine (Largactil) n Prochlorperazine (Stemetil) n
 Mixing Medications in a Syringe Driver. n n n Care should be taken when mixing two or more drugs in a syringe driver. Ensure that the drugs used are compatible with each other. Ensure that the diluent used is compatible with the drugs used. At least 2 -3 mls of diluent should be added to all syringes. Observe for crystallisation of drugs in syringe driver. Change drugs in syringe driver every 24 hrs.
Mixing Medications in a Syringe Driver. n n n Care should be taken when mixing two or more drugs in a syringe driver. Ensure that the drugs used are compatible with each other. Ensure that the diluent used is compatible with the drugs used. At least 2 -3 mls of diluent should be added to all syringes. Observe for crystallisation of drugs in syringe driver. Change drugs in syringe driver every 24 hrs.

 “Kill Two Birds with the One Stone” n n n n Morphine Sulphate: Pain, Dyspnoea. Midazolam: Agitation, Dyspnoea. Haloperidol: Antiemetic, Agitation, Delirium. Metoclopramide: Antiemetic, Constipation. Hyoscine Butylbromide: Drying secretions, Crampy abdominal pain. Methotrimeprazine: Antiemetic, Agitation. Phenobarbitone: Anti-Epileptic, Agitation
“Kill Two Birds with the One Stone” n n n n Morphine Sulphate: Pain, Dyspnoea. Midazolam: Agitation, Dyspnoea. Haloperidol: Antiemetic, Agitation, Delirium. Metoclopramide: Antiemetic, Constipation. Hyoscine Butylbromide: Drying secretions, Crampy abdominal pain. Methotrimeprazine: Antiemetic, Agitation. Phenobarbitone: Anti-Epileptic, Agitation
 The “Box”
The “Box”
 Information n n n The Syringe Driver- Continuous subcutaneous infusions in palliative care. Policy/Procedure/Guidelines for the safe and appropriate use of the Mc. Kinley T 34 Syringe Pump Observation Sheet. Careplan - Comfort measures for palliative care patients. Analgesic Conversion Guidelines in Palliative Care. Drug Combinations as Subcutaneous Infusions (in Syringe Driver) for Palliative Care
Information n n n The Syringe Driver- Continuous subcutaneous infusions in palliative care. Policy/Procedure/Guidelines for the safe and appropriate use of the Mc. Kinley T 34 Syringe Pump Observation Sheet. Careplan - Comfort measures for palliative care patients. Analgesic Conversion Guidelines in Palliative Care. Drug Combinations as Subcutaneous Infusions (in Syringe Driver) for Palliative Care
 References n Dickman A. Schneider J. Varga J. (2005) Continuous Subcutaneous Infusions in Palliative Care. 2 nded Oxford University Press.
References n Dickman A. Schneider J. Varga J. (2005) Continuous Subcutaneous Infusions in Palliative Care. 2 nded Oxford University Press.


