8b4f5e452e6d482f48f1803192b84c91.ppt
- Количество слайдов: 26

SURGICAL MANAGEMENT OF TUBERCULOSIS Paul Bolanowski, MD Associate Professor of Surgery Division of Cardiothoracic Surgery UMDNJ-NJ Medical School

HISTORY OF TUBERCULOSIS • Scourge Of Early Humanity – Hippocrates – Phthisis • Disease characterized by progressive weight loss and wasting – Romans – Consumption • Consumed its victims – Schonlein - Tuberculosis • First to use term based on autopsy findings

SURGICAL HISTORY • 1821 - Carson - collapse therapy – 1925 - Alexander • 1869 - Simon - thoracoplasty – 1920 - Sauerbruch & Alexander • 1882 - Block - first resection • 1891 - Tuffier – first partial resection • 1934 - Freelander – first lobectomy

COLLAPSE THERAPY • Pneumothorax • Phrenic nerve crush • Pneumoperitoneum • Extrapleural pneumolysis – Plombage thoracoplasty – Extraperiosteal • Thoracoplasty

EFFICACY OF COLLAPSE THERAPY • 1880 - 300 deaths/100, 000 • 1935 - 69 deaths /100, 000 • Plombage thoracoplasty – Sputum negative - 30 -60% • Thoracoplasty – Closure of cavity in 80% – Mortality 10%

SURGICAL INDICATIONS - 1 • Failure of medical treatment – Cavity with persistently positive sputum • Resistant strains – MDR-TB – XDR-TB • Atypical organisms – M. kansasii - surgery infrequent – M. avium - localized – lobectomy • Solitary nodule – Lung carcinoma vs. tuberculoma

SURGICAL INDICATIONS - 2 • Massive or recurrent hemoptysis – Etiology • Bronchial collateral circulation – Rasmussin aneurysm – Aspergilloma – Bronchiectasis – Treatment • Embolization • Surgery

MASSIVE HEMOPTYSIS - 1 • Definition – Based on amount and duration • MASSIVE 600 ml WITHIN 16 hrs • 200 ml, >300 ml, >500 ml, >600 ml / 24 -48 hrs – Based on threat to life • Acute airway obstruction • Shock • Persistent hemoptysis despite good medical management

MASSIVE HEMOPTYSIS - 2 • Position patient • Chest x-ray • Bronchoscopy – Localize site – Intubation • Bronchial arteriography • Surgery – Resection – Videoendoscopic thoracoscopy
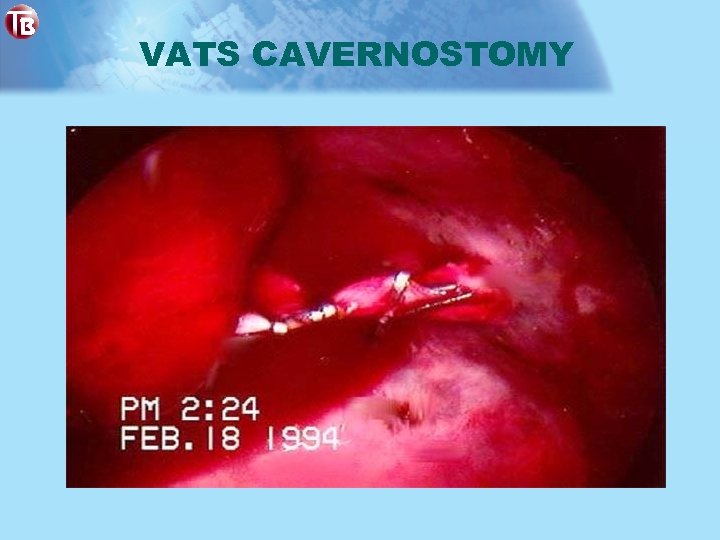
VATS CAVERNOSTOMY

BRONCHIAL ARTERIOGRAPHY • Advantages – – – Localize site Control bleeding by embolization Prevent contamination of normal lung Buy time to improve pulmonary function Less blood loss during surgery • Disadvantages – Spinal cord paralysis – Temporary • Acute control - 75% effective • Rebleed rate - 43%
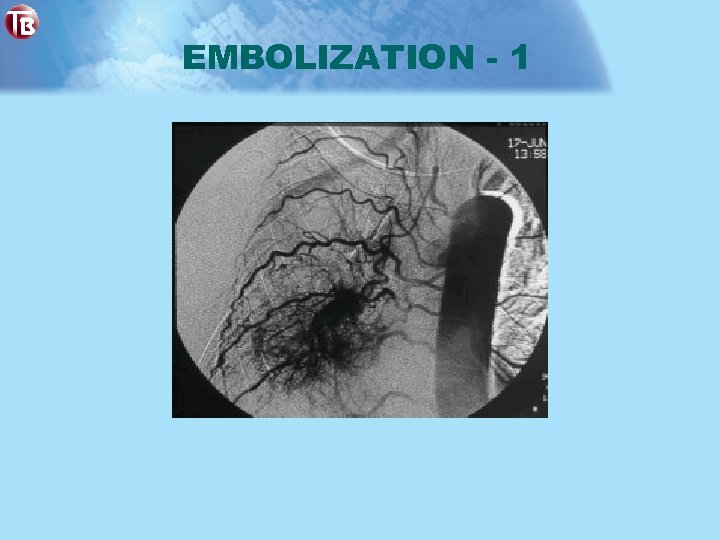
EMBOLIZATION - 1
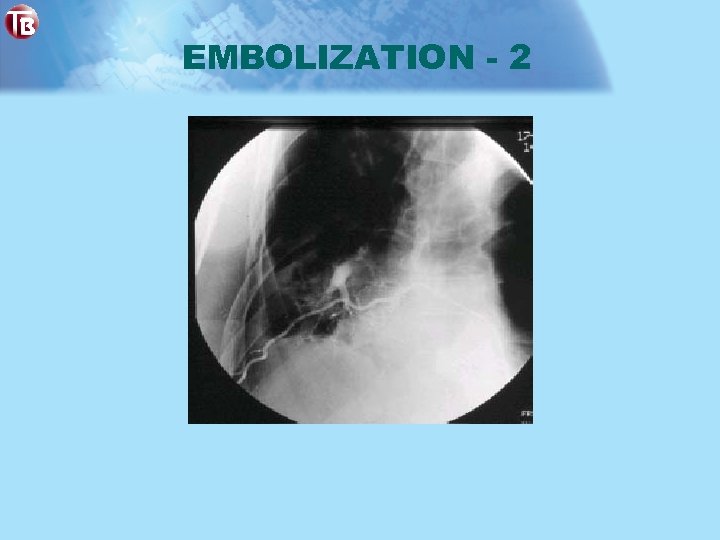
EMBOLIZATION - 2
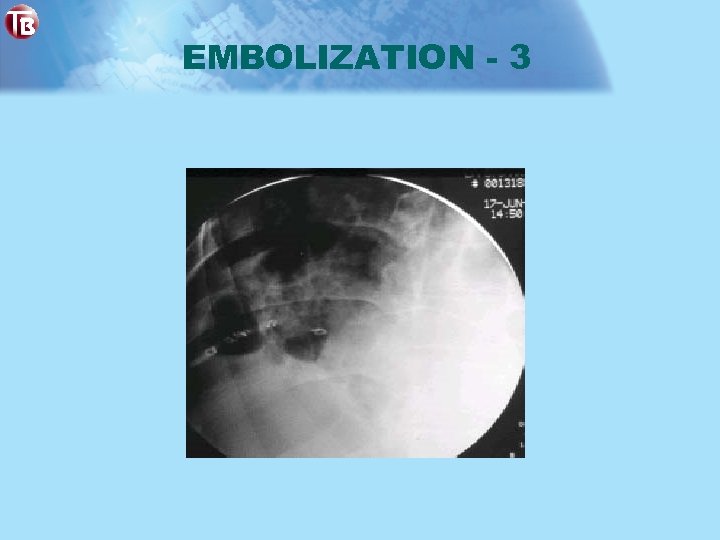
EMBOLIZATION - 3

MASSIVE HEMOPTYSIS • Surgical results • Massive • • 600 ml in < 16 hrs 18% MORTALITY Conservative management • Massive 600 ml or more in 16 hrs – 75% MORTALITY • 600 ml or more in 48 hrs – 54% MORTALITY • • Embolization + surgery Acute control in 75% • Mortality 7 -9% •

SURGICAL INDICATIONS - 1 • Bronchopleural fistula – Complication of disease • Treatment – Lobectomy or pneumonectomy – Complication of surgery • Treatment – Immediate chest tube » Pneumonectomy – Thoracotomy with closure using intercostal muscle flap

SURGICAL INDICATIONS - 2 • Empyema – Acute • No chest tube unless respiration compromised – Chronic • Decortication – Trapped lung – Muscle transposition
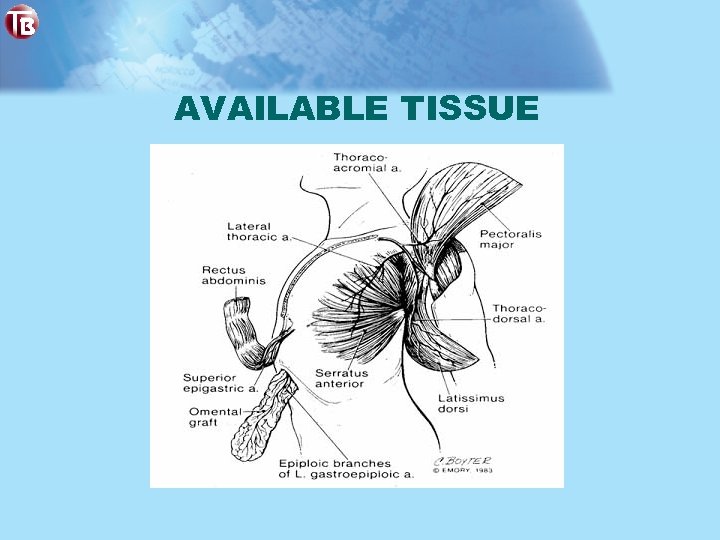
AVAILABLE TISSUE

SURGICAL INDICATIONS - 3 • Destroyed lung or lobe – Surgical resection • Pott’s abscess – Drainage – Spine reconstruction • Mycetoma (aspirgeloma) – Recurrent hemoptysis • Resection

SURGICAL INDICATIONS - 4 • Pericarditis – Acute • With or without tamponade – Pericardial window – Chronic • Constrictive pericarditis – Total pericardioectomy » Cardiopulmonary bypass – Lymphadenitis • Cervical (scrofula) • Mediastinal – Drainage

SURGICAL INDICATIONS - 5 • Destroyed lung or lobe – Surgical resection • Pott’s abscess – Drainage – Spine reconstruction • Mycetoma (aspirgeloma) – Recurrent hemoptysis • Resection

SURGICAL INDICATIONS - 6 • Pericarditis – Acute • With or without tamponade – Pericardial window – Chronic • Constrictive pericarditis – Total pericardioectomy » Cardiopulmonary bypass – Lymphadenitis • Cervical (scrofula) • Mediastinal – Drainage

PRE-OP MANAGEMENT - 1 • Medical management – Nutrition – Atypical mycobacterium • M. avium – Perioperatively – ethambutol, rifabutin, biaxan, and amikacin – Operate when sputum converts to negative • M. abscessus – Pre-op – imipenem & amakacin for 2 months – Post-op – same drugs for 4 months • M. kansasii – surgery infrequent

PRE-OP MANAGEMENT - 2 • Multi-drug resistant tuberculosis – Pre-op • 2 -3 months of 3 or 4 drugs they have never received – Post-op • 18 to 24 months of therapy – These patients must be followed diligently post-op for recurrence

PRE-OP MANAGEMENT - 3 • PET-CT scan – Determine extent of disease • Bronchoscopy – Determine if line of transection is disease free • Arteriography – To control bleeding pre-operatively – To decrease blood loss at time of surgery

POST-OP MANAGEMENT • Immediate – Intensive care unit • Isolation • Room with air exchange • Ventilator • Collaborative medical management – Anti-tuberculous drugs • Length of stay • Long term
8b4f5e452e6d482f48f1803192b84c91.ppt