6c6a1e412187b2da1c5e2a5f23be7d52.ppt
- Количество слайдов: 84

Sunnybrook/TSRCC Breast Program Strategic Planning Retreat April 23, 2007

Breast Cancer: State of the Union • What has changed? • What will change ? 2

Breast Cancer in Canada • Most common malignancy affecting women in 2002 in Canada § 20, 500 diagnosed § 5, 400 died • Incidence rates have leveled over last 10 years • Mortality rates have dropped by 25% in last 20 years 3

Preventive Oncology: Key changes in the last 5 years • Increased demand for and utilization of genetic services for assessment of hereditary predisposition • Increased evidence to support risk reduction interventions in patients with hereditary predisposition to breast cancer • Chemoprevention of breast cancer § ? Research vs. standard of care • Clarification of Breast Cancer Risk Factors § e. g. HRT • Development of a provincial cancer prevention strategy § “Cancer 2020” 4

Preventive Oncology: What can we expect in the next 5 years? • More complex genetic assessment § More genes, more sophisticated testing • More prevention studies • More accountability re: provincial targets/CSQI • More cancer • NOT more funding • MRI screening 5

MRI Screening in Canada • Currently being performed in a few large centres and a few private clinics • National Hereditary Taskforce Guidelines (Jan/07): Annual mammography should be supplemented by MRI where it is available. • Ontario PEBC Guideline in final stages. Like ACS but: § 25% lifetime risk § Includes some patients with LCIS / atypia • Aim to bring MRI screening under umbrella of OBSP to ensure: § Minimum standards are met by all centres § Access for all women who might benefit § Outcome analysis and CQI 6

Imaging: Key changes in the last 5 years • Increasing volume § US & MRI • Increasing interventions § Core & vacuum assisted biopsies – expense • Digital mammography • Choice of residents for teaching • Clinical research – CAD § DMIST § ACRIN 6666 Screening Ultrasound § MRI high risk screening § CEDM & DBT 7

Imaging: What can we expect in the next 5 years? • • Screening & increasing diagnostic volume & interventions OBSP – screening & assessment centre Conversion to all digital imaging Timely diagnosis Research – MRI Contrast –enhanced digital mammography Digital Breast Tomosynthesis CE DBT 8

Surgical Oncology: Key changes in the last 5 years • More emphasis on “minimally invasive” surgery • Importance of breast imaging for surgical decision-making • Importance of multidisciplinary care • Critical mass of breast surgeons at TSRCC 9

Surgical Oncology: What can we expect in the next 5 years? • • • Increased emphasis on neoadjuvant treatments Greater reliance on imaging (MRI as standard? ) Greater multidisciplinary care § More resources/patient § Better coordination of services/streamlining of appts needed • • Consumer demand for patient-focused services The challenge of maintaining referral base § Patient navigation § Admin support § Efficient triage and follow-up services 10

Pathology: Key changes in the last 5 years • screen detected breast lesions § Difficult to assess borderline lesions • # of non-palpable breast lesions § More volume to process • Development of new biological markers and their adoption as standard of care § Impact on HR, pathology & lab budget • Pathology has become an integral part of clinical multidisciplinary teams (HR) • Pathology is a key player in breast cancer research (HR) 11

Pathology : What can we expect in the next 5 years? • volume • discovery of new biological markers, both as prognostic and predictive markers • New molecular / genetic classification • Molecular finger printing of breast cancer • Increased use of image analysis for marker assessment • Identification of stem cell markers 12

Radiation Oncology: Key changes in the last 5 years Infiltrating Ductal Carcinoma • The Expanding Role of XRT § Increasing use of Locoregional XRT • Improved Techniques of XRT § Intensity-Modulated Radiation Therapy § Boost for women < 50 years old § Partial breast radiation (Brachytherapy) less toxicity • Reducing the Toxicity of XRT § Cardiac toxicity § IMRT leads to less scatter Ductal Carcinoma in Situ • Increasing incidence • Increasing evidence of benefit of XRT • Increasing concerns of under treatment and potential over treatment 13

Radiation Oncology : What can we expect in the next 5 years? • Early Stage Breast Cancer § Partial breast irradiation (external beam/brachytherapy/IORT) § Image guidance and Adaptive Radiotherapy § Is bolus necessary? • • Locally Advanced Breast Cancer § § § Combined modality therapy Increased intensity of treatment with reduced treatment time Imaging for the evaluation of treatment response (US, PET, MRI) DCIS § Identify factors predictive of invasive recurrence § Improved Risk Stratification o Lumpectomy /Lumpectomy + XRT / Mastectomy § Improve XRT Techniques o o 14 Partial breast irradiation Role of boost for young women

Medical Oncology: Key changes in the last 5 years • Expanded indications for adjuvant chemotherapy § Node negative, HER 2 positive • Dose-dense chemo § Use of G-CSRF, erythropoetin • Use of adjuvant taxanes • Increased use of neo-adjuvant therapy • AI’s in adjuvant therapy § Length of adjuvant endocrine therapy • Wide use of bisphonates • Use of biologics Herception – met//adjuvant § Lapatinib § 15

Medical Oncology: What can we expect in the next 5 years? • New tests for prediction § Oncotype DX § Other molecular signatures • Use of biologics in adjuvant therapy • Use of adjuvant chemotherapy • Drugs for metastatic disease • Fewer patients with metastatic disease 16

Survivorship: What has changed in the last 5 years? • Awareness of survivorship issues • Length of endocrine adjuvant therapy • More survivors for longer • Issues of QOL § Exercise, body and weight § Other lifestyle issues § 17

Survivorship : What will change in the next 5 years? • Extended endocrine adjuvant therapy • Focus on lifestyle issues • Biologics and their long term effects 18

Palliative Care: Key changes in the last 5 years • Expanding role in the care of patients prior to end-of-life • Clinical expertise in the management of symptoms associated with breast cancer: lymphedema, brachial plexopathy, complex neuropathic/bony mets pain syndromes 19

Palliative Care: What can we expect in the next 5 years? • As the research base within the field of palliative medicine expands, greater body of evidence for targeted and individualized pain and symptom management interventions • Expanding role for interventional pain management procedures: nerve blocks • Ongoing source of care and support for patients with disease progression 20

Care Delivery Models: Key changes in the last 5 years • • 21 Screening Programs (OBSP) Diagnostic Assessment Units Multidisciplinary Programs Survivorship Programs

Diagnostic Assessment Units • Completing diagnostic evaluation in a streamlined, comprehensive and timely manner • Principles § Patient-focused § Multidisciplinary § Timely • Components § § 22 Triage mechanism Breast imaging: mammography, US, biopsy, MRI Clinical assessment Patient Navigator

Diagnostic Assessment Unit : What might it look like? • Triage referrals § Imaging o Screening or diagnostic § Clinic o • Surgical or nonsurgical Streamlined diagnostic imaging § All diagnostic studies (except MRI) same day § MRI and MRI-generated FU studies same day • • • Rapid turnaround of pathology Prompt clinic appt after diagnostic evaluation Patient navigation/nursing support 23

Breast cancer : Summary of Key changes in the last 5 years • • • Improved and expanded screening and early diagnosis Reduced mortality rates Reduced or stable incidence rates Increased use of imaging Use of sentinel node More breast conserving surgery New radiation approaches Improved adjuvant endocrine therapy New adjuvant chemotherapy Biologics 24

Breast Cancer : Key changes in the next 5 years • New approaches to surgery § Image-guidance • New approaches to radiation § Image-guidance • New approaches to systemic therapy § Especially biologics • Lifestyle approaches for survivors • More survivors for longer 25

What Do Women Want? In-depth interviews with: • • Health care providers Former patients Informal caregivers Telephone survey of 800 women without cancer • Cancer professionals 26

Executive Summary The Problem • Lack of coordination of care • Gaps in communication between health care providers • Lack of psycho-social support with the shock of the diagnosis • Lack of information: Feeling “numb and dumb” at time of critical treatment decisionmaking • Provider knowledge § “Many participants expressed disappointment with the breast cancer knowledge of their primary care providers” 27
Executive Summary The Problem The Potential Solution • Lack of coordination of care Navigator ? • Gaps in communication between health care providers Multidisciplinary care ? • Lack of psycho-social support with the shock of the diagnosis • Lack of information: Feeling “numb and dumb” at time of critical treatment decisionmaking • Provider knowledge § “Many participants expressed disappointment with the breast cancer knowledge of their primary care providers” 28 Increased Psychosocial support Educational websites? Brochures? DVDs? Well follow-up clinics?

What Could Make Treatment for Breast Cancer a “Wonderful Experience? ” • Informed Participation • Emotional Support • Timeliness 29

Breast Cancer at TSRCC/Sunnybrook

Breast Cancer at TSRCC • • • One of 2 largest breast programs in Canada One of 6 or 8 largest breast programs in North America Primary nursing model Multidisciplinary care Interdisciplinary care Strong emphasis on research/teaching • Volumes Surgery volumes Radiation volumes Medical Oncology volumes See handout in package for breast activity at TSRCC 31

Breast Site Group at TSRCC • • • 32 17 Medical Oncologists 16 Radiation Oncologists 4 Surgeons 3 (4) Specialist pathologists 2 (3) Specialist diagnostic imagers 15 RNs Social workers Dietitians Pharmacists Physicists Radiation therapists Genetic counselors

Accomplishments

Honors and Awards • Prominent Role in NCIC/CTG – Breast Group • Prominent Role in OCOG Breast Group • Fellowship Program § § Campbell Endowed Fellowship Industry Fellowships CAMO Fellows CBCF Fellows • CFI Awards § 11. 2 x 106$ for Breast Centre • Breast Centre – 27 million dollars • As a primary fundraising target SHSC 34

Honours and Awards (cont’d) 1. Grants: o o Dr. Eileen Rakovitch – largest CBCRA grant 2007, 5 years Dr. Arun Seth – CBCRA 2005 -2010 Metastatic “Breast Cancer Genome Anatomy” $ 610, 000 – CBCRA (Grant Core Component) 2005 -2010 “New Approaches to Metastatic Disease in Breast Cancer (METS)” $ 969, 067 – NIH, USA 2007 -2012 The. BCA 2 Ubiquitin. E 3 Ligase as a Target in Breast Cancer $1, 759, 000 USD 35

Honours and Awards (cont’d) • Grants: Dr. Greg Czarnota – 2 OICR grants ~$300, 000 – CBCF $428, 000 o Drs. Yaffe/Plewes – Terry Fox Grant o Dr. Claire Holloway and others – OCRN grant ~ $300, 000 o • Plenary Session at ASTRO – Dr. Jean-Philippe Pignol • O. H. Warwick Award - Dr. Kathleen I. Pritchard, 2005 36

Landmark Papers • Warner E. et al. Surveillance of BRCA 1 and BRCA 2 Mutation Carriers With Magnetic Resonance Imaging, Ultrasound, Mammography, and Clinical Breast Examination. JAMA. 2004; 292: 1317 -1325 • Yaffe, M. et al. Diagnostic Performance of Digital versus Film Mammography for Breast-Cancer Screening. New England Journal of Medicine, Volume 353: 1773 -1783 October 27, 2005 Number 17 • Pritchard, K. I. et al. HER 2 and Responsiveness of Breast Cancer to Adjuvant Chemotherapy. New England Journal of Medicine, Volume 354: 2103 -11, May 18, 2006 Number 26 • Seth, A. K. et al. A Novel RING-Type Ubiquitin Ligase Breast Cancer-Associated Gene 2 Correlates with Outcome in Invasive Breast Cancer. American Association for Cancer Research. 37

Prevention: Accomplishments • Comprehensive assessment of genetic and cancer risk • Accrual to chemoprevention studies • Follow-up of high risk women • Participation in collaborative research • Education/training • Regional role 38

Surgery: Accomplishments • Establishment of an academic program in breast surgery § Fellowship training program § Critical mass of academic surgeons o Standardized multi- and interdisciplinary care § Integrated research program o Multidisciplinary o Partnerships with U of T, ICES, CCO § Surgical representation at provincial, national organizations • Grants § Imaging and histopathology correlation after neo-adjuvant chemotherapy (CBCF) § Radioimmunoguided surgery (OCRN) § Evaluating the quality of sentinel lymph node biopsy quality in Ontario (CBCF) § Patterns of breast cancer surgery in Ontario (CCO) 39

Pathology : Accomplishments • Sign-out of breast cases by dedicated specialized pathologists • Adoption of synoptic reporting • Testing for ER/PR and Her 2/neu on all patients at the time of diagnosis • Improving TAT. In general, only 10% of cases are >10 days for the whole department (all specimen types) • Leader for setting provincial and national Her 2 testing guidelines and QA program • Established TMA facility 40

Pathology : Accomplishments Academic achievements: a) Grants b) CME activities c) Tumour Boards d) Regular clinicopathological rounds weekly e) Member of expert panel and publication of CAP/ASCO guidelines (Wolff AC, Hammond EH, Schwartz JN. Guideline Recommendations for Human Epidermal Growth Factor Receptor 2 Testing in Breast Cancer. J Clin Oncol 2007; 25(1): 1 -28. ) f) Tumour Banking initiative (old & new) 41

Radiation Oncology: Accomplishments • Prevention / Screening § Population-based assessments of screening • Treatment § Development of a Permanent Breast Seed implant § PI of randomized clinical trial on Breast IMRT o Plenary Session at ASTRO § Development of international bone metastases module to accompany the EORTC QLQ-C 30 for patients with bone metastases. § PI on International RCT of Single versus Multiple Fractions for Re. Irradiation of Painful Bony Metastases – NCIC SC 20 § Chemoradiation for LABC § Novel imaging of LABC to determine response to treatment • Outcomes § Establishment of population-based provincial cohort of DCIS, LCIS (Pathology) § Population-based assessment of cardiac toxicity following XRT for breast cancer 42
Medical Oncology : Accomplishments • Strong contribution to new international standards for adjuvant endocrine, biologic and chemotherapy via NCIC CTG (MA. 5, MA. 17 R, MA. 21, MA. 27) • Strong phase II program: § NCIC CTG § PMH Consortium • Strong Correlation phase I-IV programs § MA. 22 § MA. 29 • Chemo radiation • LABC programs • BLISS programs 43

Specialty Clinical Components • • • Primary Nursing Model LABC Brachytherapy Lymphedema clinic Breast prosthesis BLISS 44

LABC Program Mission • To provide consistent, high quality, multidisciplinary care in a patient-centered or needs-led format. Objectives • Increase understanding of long-term clinical outcomes. • Design program of excellence. • Continue national preceptorship program for health care professionals. 45
Ongoing Clinical Trials Imaging: Neoadjuvant Therapy: MRI Study (Wright) MRI Technique (Czarnota) Spectroscopy (Czarnota) MA. 22 (Trudeau) ATSEA (Clemons/Holloway/Verma) Chemorads (Spayne/Holloway) Psychosocial: Risk Perception Delayed Presentation Male Partner’s Role 46 (Fergus/Fitzgerald)

LABC: The Future • Maintain high quality, multidisciplinary care for our patients • Re-institute RN lead program • Improve public awareness • Maintain LABC database • Improve outcomes for women with LABC 47
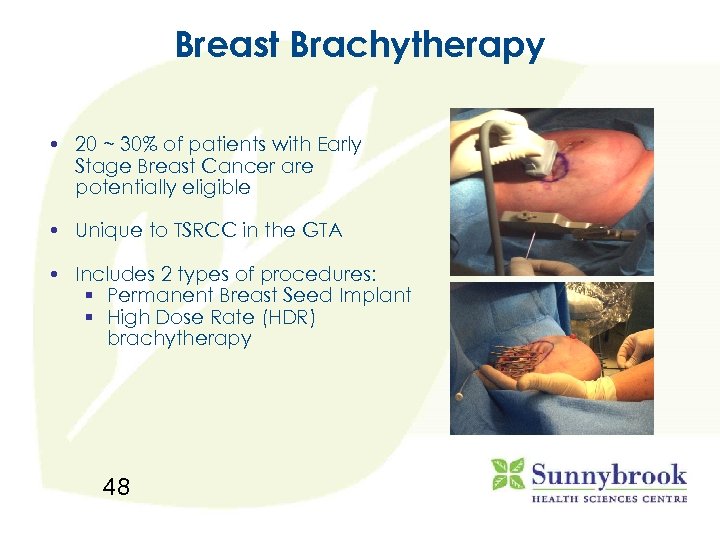
Breast Brachytherapy • 20 ~ 30% of patients with Early Stage Breast Cancer are potentially eligible • Unique to TSRCC in the GTA • Includes 2 types of procedures: § Permanent Breast Seed Implant § High Dose Rate (HDR) brachytherapy 48
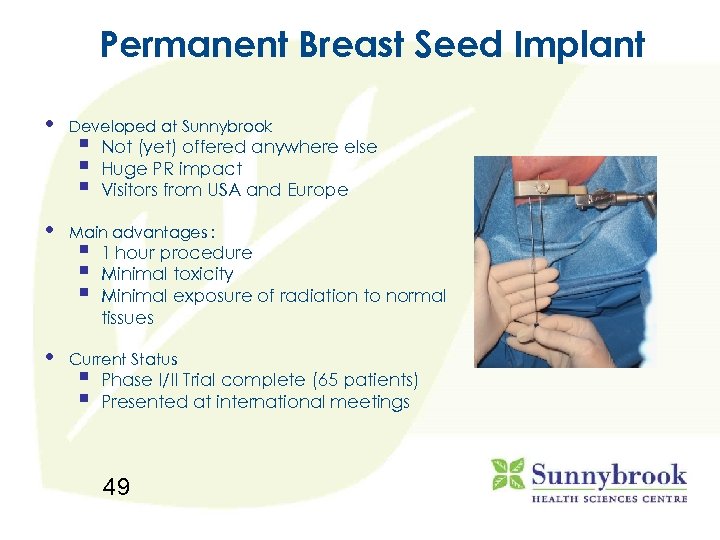
Permanent Breast Seed Implant • Developed at Sunnybrook • Main advantages : • Current Status § § § § Not (yet) offered anywhere else Huge PR impact Visitors from USA and Europe 1 hour procedure Minimal toxicity Minimal exposure of radiation to normal tissues Phase I/II Trial complete (65 patients) Presented at international meetings 49
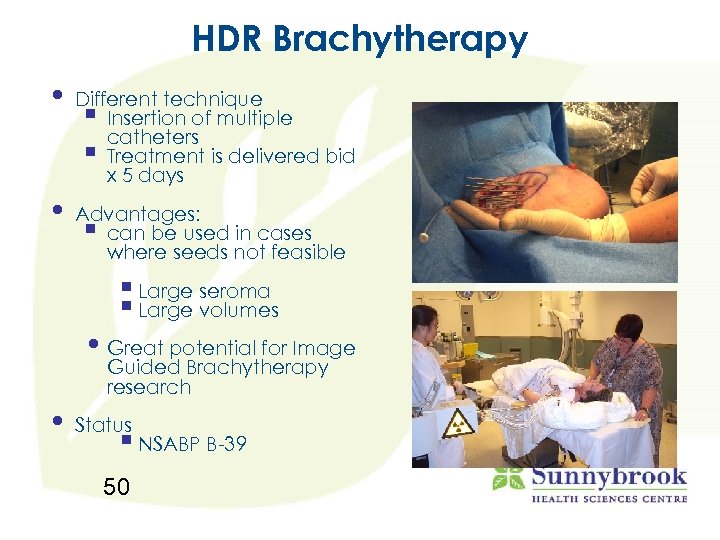
HDR Brachytherapy • Different technique § Insertion of multiple catheters § Treatment is delivered bid x 5 days • Advantages: § can be used in cases where seeds not feasible § Large seroma § Large volumes • Great potential for Image Guided Brachytherapy research • Status § NSABP B-39 50
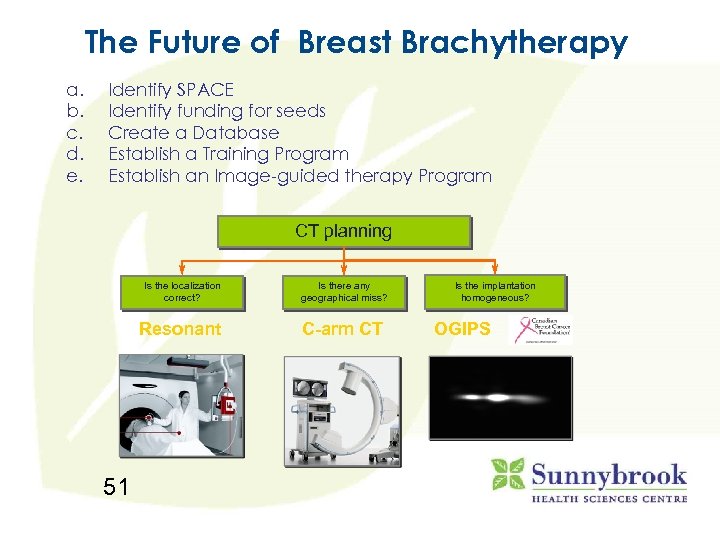
The Future of Breast Brachytherapy a. b. c. d. e. Identify SPACE Identify funding for seeds Create a Database Establish a Training Program Establish an Image-guided therapy Program CT planning Is the localization correct? Resonant 51 Is there any geographical miss? C-arm CT Is the implantation homogeneous? OGIPS

Lymphedema Clinic • • 1990 N. P. 2 per week, 2007 6 N. P. per wk. Growth 2006, 300 N. P. F. U 700 from all sites Now 2 Nurses Clinics expanded to 2 ½ days per week 52

Lymphedema Highlights • • Patient information booklet in progress Education booklet in progress Visiting Therapists Palliative Care Physicians rotate through clinic Inpatient consults XRT Student Research Staff inservice and staff orientation Delta Study participation 53

Breast Prosthesis • Craniofacial Prosthetic Unit • Trial currently underway comparing artistic custom breast prostheses against current standard prostheses • Assessing patient demand, patient preference, business model, and technical methods • Early results extremely encouraging • Objective is to integrate custom breast prostheses into breast site care path 54
BLISS: A Program for Young Women With Breast Cancer Breast cancer before 40 Life after cancer Innovative treatments Scientific research Support for women and their families 55
BLISS Executive Summary • 5% of breast cancers occur in women < age 40 at diagnosis (10% of TSRCC patients) • Disproportionately represent ‘breast cancer burden’ of excess morbidity, mortality, and loss to society. • Women have special clinical needs which are currently not being met • Large research gaps exist • CLINICAL AND RESEARCH CHALLENGE BLISS • Interdisciplinary treatment and research program • Opportunity to: § Create a new model of care § Improve outcomes of all young women with breast cancer 56

Research

External funding has more than tripled… 58
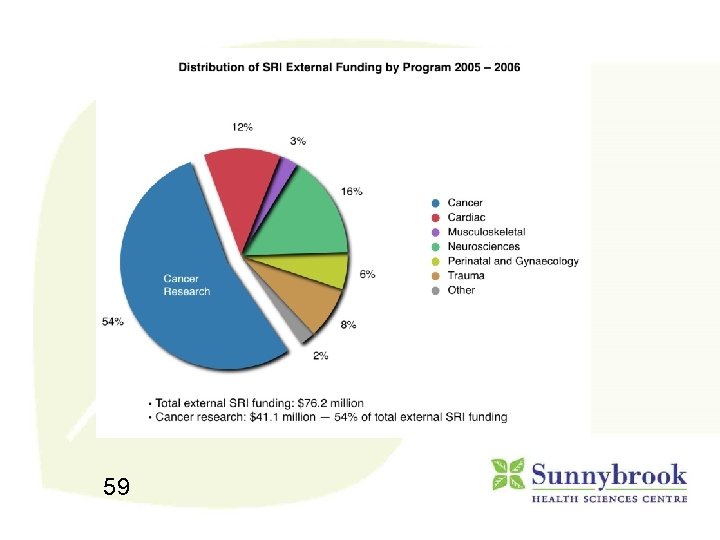
59

Our Research Directions • Improved detection § Developments in breast MRI, tomosynthesis § Population-based assessments of screening • More accurate diagnosis § 3 D pathology, high field MRI • Efficient and accurate localization for biopsy/therapy § MRI, US • More precise, less invasive surgical treatment § Image-guided surgical intervention (Intraoperative US, specialized surgical instruments) • New radiation techniques § Brachytherapy § Image-guided radiation therapy 60

Our Research Directions • Phase II/III trials § With major correlational components • Monitoring response to therapy § High and mid freq ultrasound • Patient-specific treatment § Molecular profiling, correlative studies(tumour/tissue/image data warehouse), and mid/high frequency US and MRI • Better understanding of disease processes § High field MRI, molecular pathology, 3 D pathology § Identifying tumour signatures leads to improved detection, diagnostic and therapeutic techniques, preventive measures 61

Our Research Directions • Palliative research • Psychosocial research § Psychosocial and Behavioral Research Unit (790 Bay Street) § Community Research Initiative (survivorship issues, health disparities, participatory research expertise) § Ontario Breast Cancer Information Exchange Partnership (needs assessment, dissemination expertise) • Outcomes Research § Ongoing independent research projects evaluating breast cancer outcomes: o DCIS, LABC, young women, BRCA, Henrietta Banting Database § No formal organization or co-ordination of projects or resources § CFI funded data server for patient data and imaging (hardware in H wing) 62

Clinical Outcomes Unit: Future • COU planning group (ER, LP, MLQ) meeting bimonthly to shape the initial vision of the COU • Collaborate with existing provincial resources to determine the elements of the TSRCC Outcomes Unit • Develop a comprehensive provincial population-based patient database • Acquisition of complete data on treatment and outcomes • Develop research priorities 63
Breast Cancer Research at SHSC Increased Convenience Lower morbidity Higher cure rates Improving the QOL of women with Breast Cancer 64 Greater support Survivor
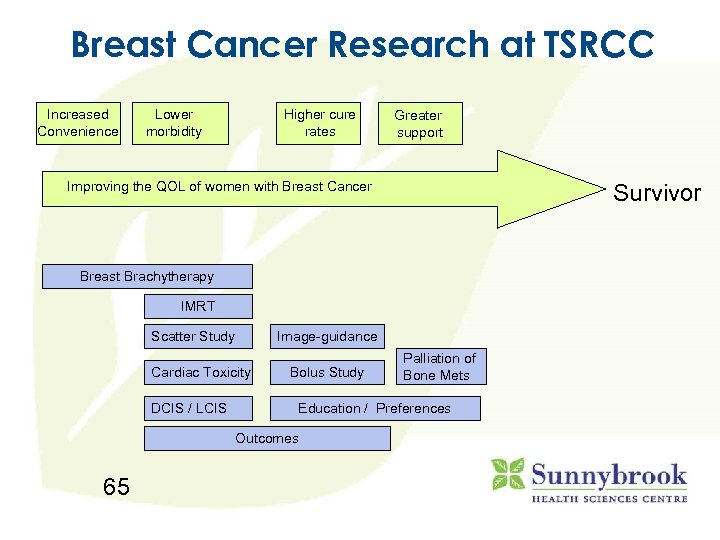
Breast Cancer Research at TSRCC Increased Convenience Lower morbidity Higher cure rates Greater support Improving the QOL of women with Breast Cancer Survivor Breast Brachytherapy IMRT Scatter Study Cardiac Toxicity DCIS / LCIS Image-guidance Bolus Study Education / Preferences Outcomes 65 Palliation of Bone Mets
Breast Cancer Research at TSRCC Increased Convenience Lower morbidity Higher cure rates Greater support Improving the QOL of women with Breast Cancer Survivor Hot Flash Therapy Trials Adjuvant Chemotherapy Endocrine, Biologics Studies of Cognitive Change on Chemotherapy Phase II Breast Brachytherapy IMRT Scatter Study Cardiac Toxicity DCIS / LCIS 66 Image-guidance Bolus Study Palliation of Bone Mets Education / Preferences Outcomes
Breast Cancer Research at TSRCC Increased Convenience Lower morbidity Higher cure rates Greater support Improving the QOL of women with Breast Cancer Survivor Hot Flash Therapy Trials Adjuvant Chemotherapy Endocrine, Biologics Studies of Cognitive Change on Chemotherapy Phase II Breast Brachytherapy Chemoradiation IMRT Cardiac Toxicity 67 LABC clinic BLISS clinic Scatter Study DCIS / LCIS Survivorship Program Image-guidance Bolus Study Palliation of Bone Mets Education / Preferences Outcomes
Breast Cancer Research at TSRCC Increased Convenience Lower morbidity Higher cure rates Greater support Improving the QOL of women with Breast Cancer Survivor Hot Flash Therapy Trials Adjuvant Chemotherapy Endocrine, Biologics Studies of Cognitive Change on Chemotherapy Phase II Survivorship Program Experimental OR Breast Brachytherapy Chemoradiation IMRT BLISS clinic Scatter Study Cardiac Toxicity 68 DCIS / LCIS LABC clinic Image-guidance Bolus Study Palliation of Bone Mets Education / Preferences Outcomes
Breast Cancer Research at TSRCC Increased Convenience Lower morbidity Higher cure rates Greater support Improving the QOL of women with Breast Cancer Survivor Hot Flash Therapy Trials Adjuvant Chemotherapy Endocrine, Biologics Studies of Cognitive Change on Chemotherapy Phase II Survivorship Program Image-guided surgery Breast Brachytherapy Chemoradiation IMRT BLISS clinic Scatter Study Cardiac Toxicity 69 DCIS / LCIS LABC clinic Image-guidance Bolus Study Palliation of Bone Mets Education / Preferences Outcomes

Education

Health Care Education Activities • Undergraduate • Postgraduate § Residents § Fellows • Other health care professionals § Oncologists o Regional Cancer Centers § Family Physicians § Nurses and Pharmacists § Allied health care workers 71

Health Care Education Activities • Current Key Education Activities § Local o Breast Cancer Rounds o Breast Cancer Visiting Professorship o Toronto Breast Cancer Guidelines o Fellowship Program • Current Key Education Activities § National and International o Breast Cancer Fellowship Program o www. oncologyeducation. ca o Toronto Breast Cancer Symposia 72

Patient Education • Patient Education Program – strategic priority for TSRCC • Providing Patients with the right information, at the right time, in the right way, by the right people • Breast Site including Breast Centre has identified commitment to patient education throughout draft functional program 73

Patient Education Initiatives • Breast Cancer Patient Portal • Breast site patient education package § Development of Internal Breast Resources (lumpectomy, mastectomy, lymphedema booklet) • Patient Education and Learning Resource Centre (PEARL) • Patient Education Satellite Site (Breast Centre) 74

Ontario Breast Screening Program
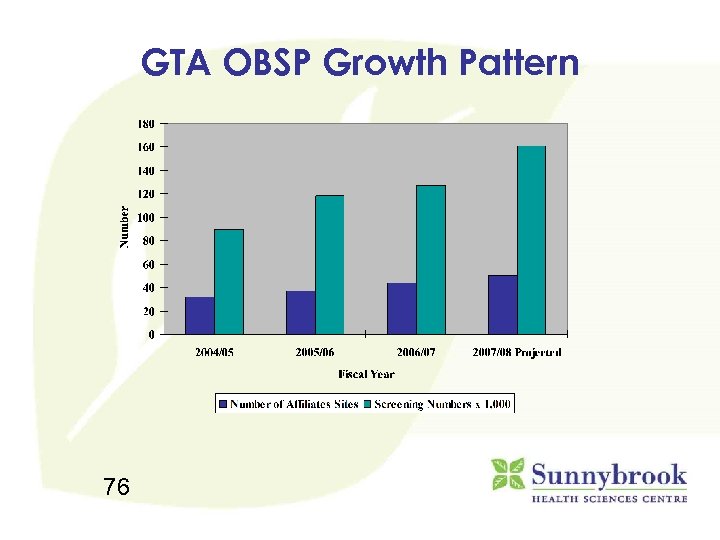
GTA OBSP Growth Pattern 76
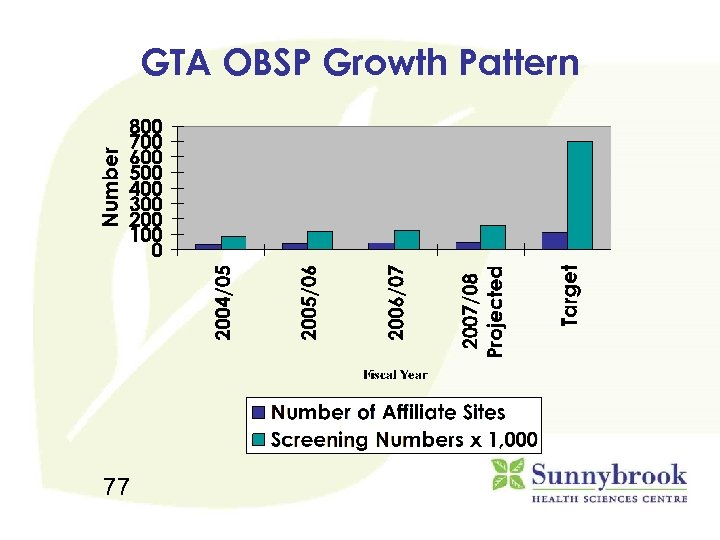
GTA OBSP Growth Pattern 77
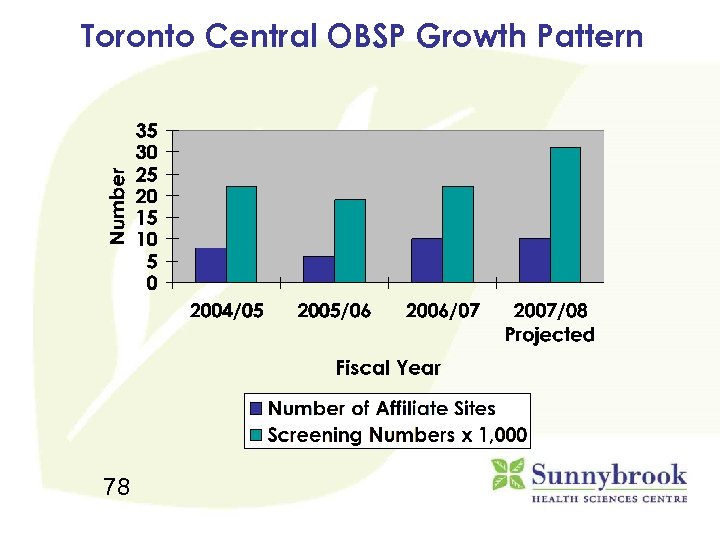
Toronto Central OBSP Growth Pattern 78
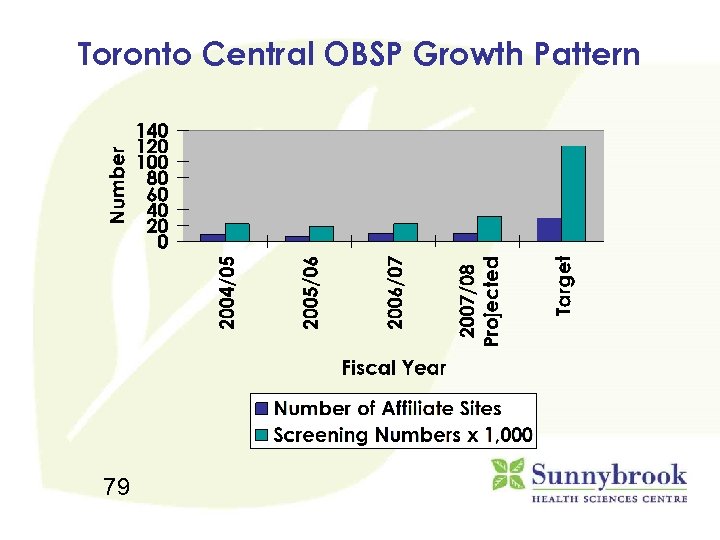
Toronto Central OBSP Growth Pattern 79

Breast Activity at TSRCC
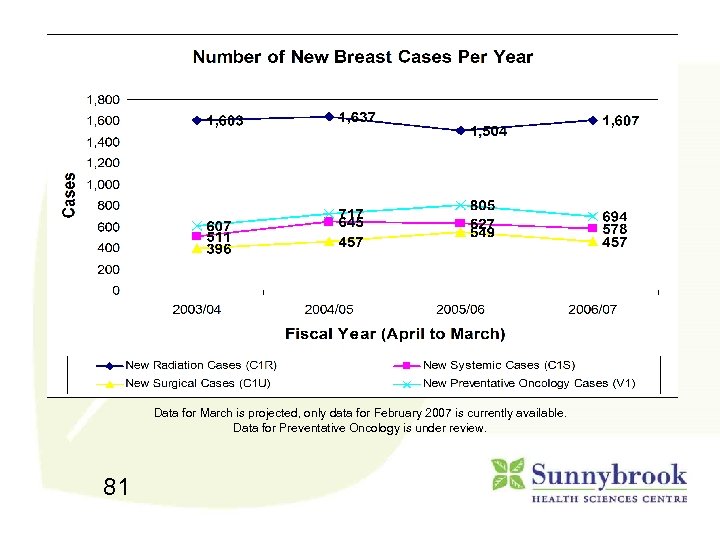
Data for March is projected, only data for February 2007 is currently available. Data for Preventative Oncology is under review. 81
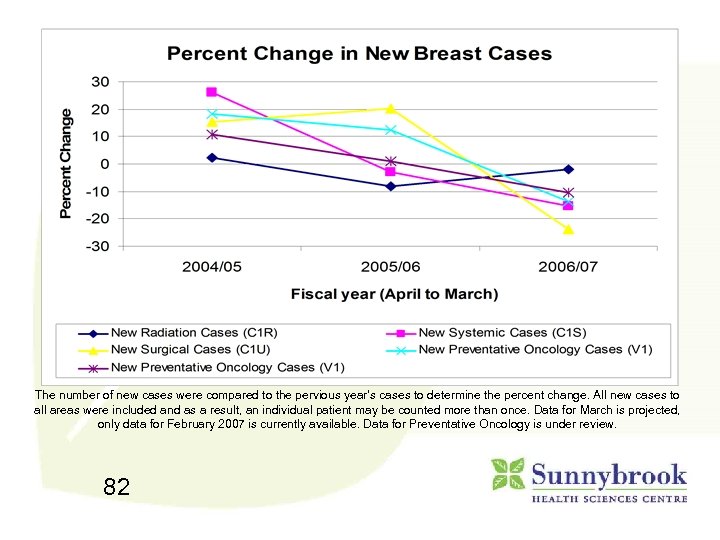
The number of new cases were compared to the pervious year’s cases to determine the percent change. All new cases to all areas were included and as a result, an individual patient may be counted more than once. Data for March is projected, only data for February 2007 is currently available. Data for Preventative Oncology is under review. 82
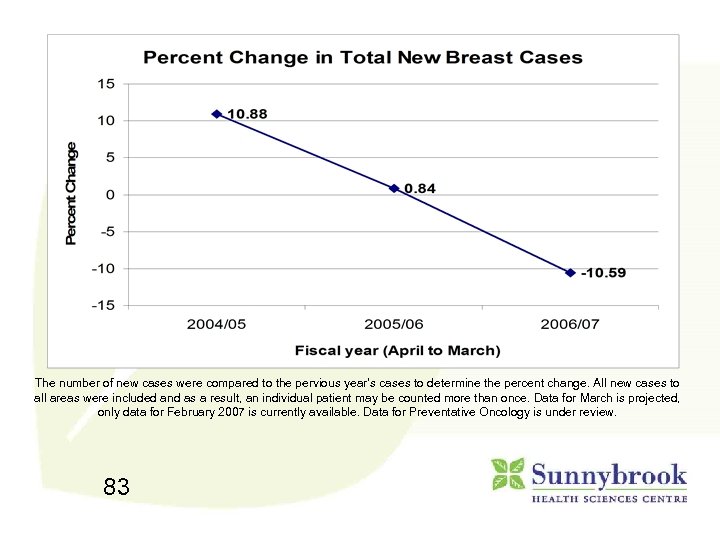
The number of new cases were compared to the pervious year’s cases to determine the percent change. All new cases to all areas were included and as a result, an individual patient may be counted more than once. Data for March is projected, only data for February 2007 is currently available. Data for Preventative Oncology is under review. 83
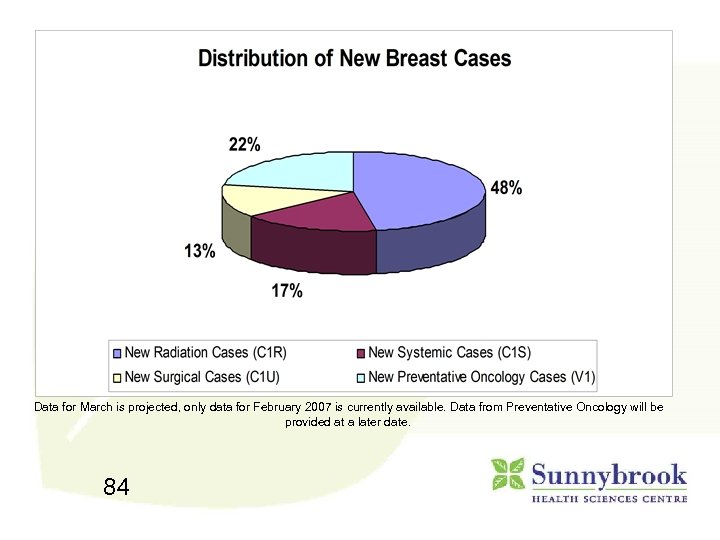
Data for March is projected, only data for February 2007 is currently available. Data from Preventative Oncology will be provided at a later date. 84
6c6a1e412187b2da1c5e2a5f23be7d52.ppt