247af13b1153e8fc5c8e23038be2e4f7.ppt
- Количество слайдов: 69
 Stroke Management Chemeketa Community College Peggy Andrews
Stroke Management Chemeketa Community College Peggy Andrews
A Look at Current Stroke" src="https://present5.com/presentation/247af13b1153e8fc5c8e23038be2e4f7/image-2.jpg" alt="The "Golden Hour" of Acute Ischemic Stroke § > A Look at Current Stroke" />
The "Golden Hour" of Acute Ischemic Stroke § > A Look at Current Stroke Treatment What's Changed in 2000? “EMS systems should implement a prehospital stroke protocol to evaluate and rapidly identify patients who may benefit from fibrinolytic therapy, similar to the protocol for chest pain patients” (Class IIb). “Patients who may be candidates for fibrinolytic therapy should be transported to hospitals identified as capable of providing acute stroke care, including 24 -hours availability of CT scan and interpretation. ” (Class IIb). “Stroke presenting with 3 hours should be triaged on an emergent basis with urgency similar to acute ST-elevation myocardial infarction. ” 2
 Acute Stroke Where are we today? § Public poorly informed § Response time too slow § Presentation too late § Hospitals ill prepared 3
Acute Stroke Where are we today? § Public poorly informed § Response time too slow § Presentation too late § Hospitals ill prepared 3
 Models for the "Golden Hour" Trauma § Times studied/defined § Centralized trauma center system § Mortality Low AMI § Similar door-drug/groin benchmarks for reperfusion § Decentralized system § Treatment data strongly supports 4
Models for the "Golden Hour" Trauma § Times studied/defined § Centralized trauma center system § Mortality Low AMI § Similar door-drug/groin benchmarks for reperfusion § Decentralized system § Treatment data strongly supports 4
 AMI - example The paradigm has shifted § Chest pain - patients know to call 911 § Rapid access to EMS – Early recognition § ECG § S/S § Rapid Transport § Team, protocols, drugs in the ED § “Door to Drug” in 30 Minutes 5
AMI - example The paradigm has shifted § Chest pain - patients know to call 911 § Rapid access to EMS – Early recognition § ECG § S/S § Rapid Transport § Team, protocols, drugs in the ED § “Door to Drug” in 30 Minutes 5
 Why Care? Impact of Stroke § § § 3 rd leading cause of death in U. S. Leading cause of adult disability 750, 000 new cases/year in U. S. – 150, 000 deaths/year – 1/3 Under age 65 6
Why Care? Impact of Stroke § § § 3 rd leading cause of death in U. S. Leading cause of adult disability 750, 000 new cases/year in U. S. – 150, 000 deaths/year – 1/3 Under age 65 6
 Forces of Change 1. Public expectations – Aware of “Draino for the Braino” 2. Medical - legal pressures 3. Managed care cost concerns - Long term vs Short Term 4. New/better treatments 5. Physicians‘ willing/able to treat - Evidenced based medicine 7
Forces of Change 1. Public expectations – Aware of “Draino for the Braino” 2. Medical - legal pressures 3. Managed care cost concerns - Long term vs Short Term 4. New/better treatments 5. Physicians‘ willing/able to treat - Evidenced based medicine 7
 Organized Stroke Care Saves Lives § 21% reduction in early mortality § 18% reduction in 12 month mortality § Decreased length of hospital stay § Decreased need for institutional care Source: Jorgenson, Stroke, 1994 8
Organized Stroke Care Saves Lives § 21% reduction in early mortality § 18% reduction in 12 month mortality § Decreased length of hospital stay § Decreased need for institutional care Source: Jorgenson, Stroke, 1994 8
 What are we talking about here? § Ischemic Stroke (84%) § Hemorrhagic Stroke (16%) – These have very different needs – Philosophy in treatment takes a different direction § Traumatic Brain Injury (TBI) – Not talking about today – PHTLS 9
What are we talking about here? § Ischemic Stroke (84%) § Hemorrhagic Stroke (16%) – These have very different needs – Philosophy in treatment takes a different direction § Traumatic Brain Injury (TBI) – Not talking about today – PHTLS 9
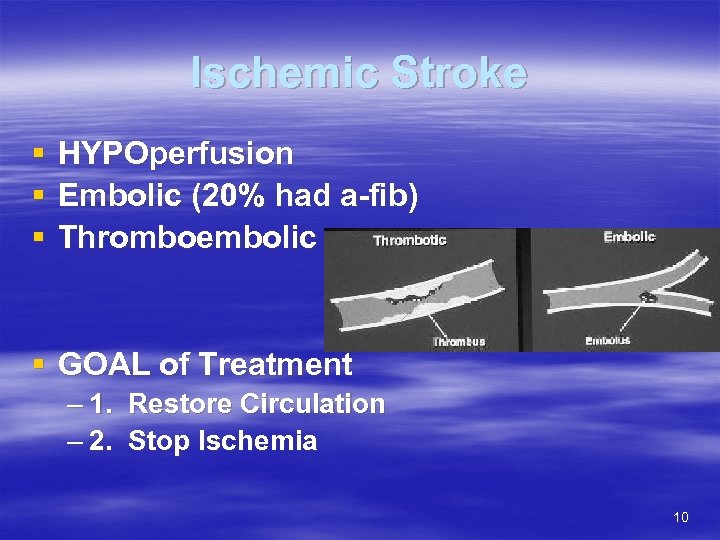 Ischemic Stroke § § § HYPOperfusion Embolic (20% had a-fib) Thromboembolic § GOAL of Treatment – 1. Restore Circulation – 2. Stop Ischemia 10
Ischemic Stroke § § § HYPOperfusion Embolic (20% had a-fib) Thromboembolic § GOAL of Treatment – 1. Restore Circulation – 2. Stop Ischemia 10
 What is this rt-PA § Recombinant Tissue Plasminogen Activator § Review of clotting cascade – Collagen Exposed § § Vessel injury Damage Long term wear Embolus – Clotting factors aggregate – Fibrin Repair (Bond-O) – FIBRINOLYSIS 11
What is this rt-PA § Recombinant Tissue Plasminogen Activator § Review of clotting cascade – Collagen Exposed § § Vessel injury Damage Long term wear Embolus – Clotting factors aggregate – Fibrin Repair (Bond-O) – FIBRINOLYSIS 11
 Intra-venous fibrinolysis for acute ISCHEMIC stroke § Class I IV - t-PA within 3 hours of onset § Class Indeterminate IV - t-PA between 3 and 6 hours of onset 12
Intra-venous fibrinolysis for acute ISCHEMIC stroke § Class I IV - t-PA within 3 hours of onset § Class Indeterminate IV - t-PA between 3 and 6 hours of onset 12
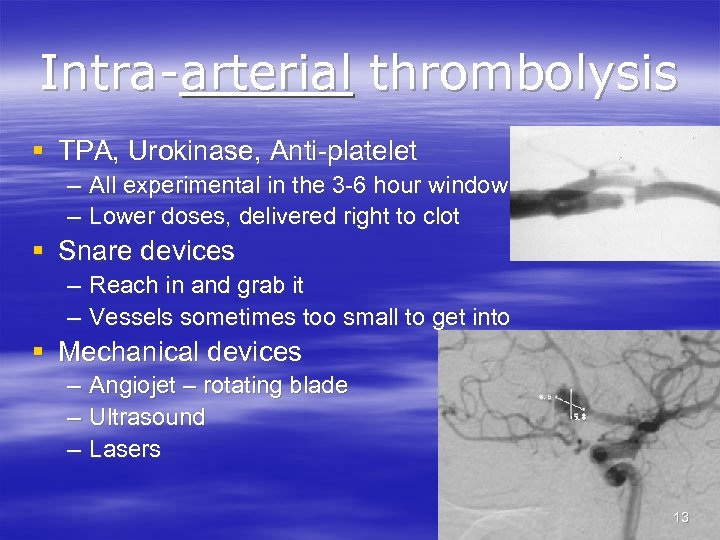 Intra-arterial thrombolysis § TPA, Urokinase, Anti-platelet – All experimental in the 3 -6 hour window – Lower doses, delivered right to clot § Snare devices – Reach in and grab it – Vessels sometimes too small to get into § Mechanical devices – Angiojet – rotating blade – Ultrasound – Lasers 13
Intra-arterial thrombolysis § TPA, Urokinase, Anti-platelet – All experimental in the 3 -6 hour window – Lower doses, delivered right to clot § Snare devices – Reach in and grab it – Vessels sometimes too small to get into § Mechanical devices – Angiojet – rotating blade – Ultrasound – Lasers 13
 With rt-PA, considering 1, 000 eligible patients: § Hospitalization costs = $1. 7 million more § Rehabilitation costs = $1. 4 million less § Nursing home costs = $4. 8 million less § 564 quality-adjusted life-years saved Source: Fagan, Neurology 1998 14
With rt-PA, considering 1, 000 eligible patients: § Hospitalization costs = $1. 7 million more § Rehabilitation costs = $1. 4 million less § Nursing home costs = $4. 8 million less § 564 quality-adjusted life-years saved Source: Fagan, Neurology 1998 14
 NIH National Symposium Recommendations § § § Door-to-MD: > 10 minutes Door-to-Neurologic Expertise: > 15 minutes Door-to-CT scan: > 25 minutes Door-to-CT Interpretation: > 45 minutes Door-to-Drug: (80% compliance) > 60 minutes Door-to-Admission: > 3 hours 15
NIH National Symposium Recommendations § § § Door-to-MD: > 10 minutes Door-to-Neurologic Expertise: > 15 minutes Door-to-CT scan: > 25 minutes Door-to-CT Interpretation: > 45 minutes Door-to-Drug: (80% compliance) > 60 minutes Door-to-Admission: > 3 hours 15
 Stroke Chain of Survival & Recovery § Detection: Early recognition § Dispatch: Early EMS activation § Delivery: Transport & management § Door: ED triage § Data: ED evaluation & management § Decision: Specific therapies § Drug: Thrombolytic & future agents 16
Stroke Chain of Survival & Recovery § Detection: Early recognition § Dispatch: Early EMS activation § Delivery: Transport & management § Door: ED triage § Data: ED evaluation & management § Decision: Specific therapies § Drug: Thrombolytic & future agents 16
 Dispatch & Delivery: Transport & Management § § § § ABC’s Stroke recognition Establish time of onset Perform neurological evaluation Check glucose Early hospital notification Rapid transport 17
Dispatch & Delivery: Transport & Management § § § § ABC’s Stroke recognition Establish time of onset Perform neurological evaluation Check glucose Early hospital notification Rapid transport 17
 Cincinnati Pre-Hospital Stroke Scale Facial Droop § Normal: Both sides of face move equally § Abnormal: One side of face does not move at all 18
Cincinnati Pre-Hospital Stroke Scale Facial Droop § Normal: Both sides of face move equally § Abnormal: One side of face does not move at all 18
 Cincinnati Pre-Hospital Stroke Scale Arm Drift § Normal: Both arms move equally or not at all § Abnormal: One arm drifts compared to the other 19
Cincinnati Pre-Hospital Stroke Scale Arm Drift § Normal: Both arms move equally or not at all § Abnormal: One arm drifts compared to the other 19
 Cincinnati Pre-Hospital Stroke Scale Speech § Normal: Patient uses correct words without slurring § Abnormal: Slurred or inappropriate words or mute 20
Cincinnati Pre-Hospital Stroke Scale Speech § Normal: Patient uses correct words without slurring § Abnormal: Slurred or inappropriate words or mute 20
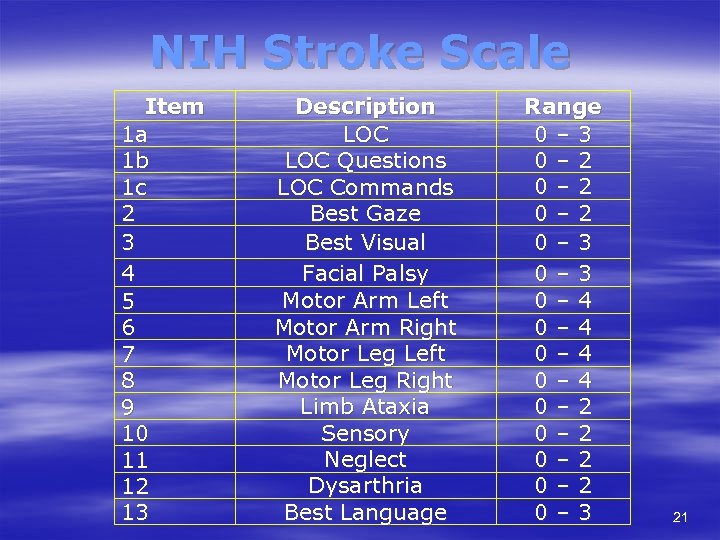 NIH Stroke Scale Item 1 a 1 b 1 c 2 3 4 5 6 7 8 9 10 11 12 13 Description LOC Questions LOC Commands Best Gaze Best Visual Facial Palsy Motor Arm Left Motor Arm Right Motor Leg Left Motor Leg Right Limb Ataxia Sensory Neglect Dysarthria Best Language Range 0 – 3 0 – 2 0 – 3 0 – 4 0 – 2 0 – 3 21
NIH Stroke Scale Item 1 a 1 b 1 c 2 3 4 5 6 7 8 9 10 11 12 13 Description LOC Questions LOC Commands Best Gaze Best Visual Facial Palsy Motor Arm Left Motor Arm Right Motor Leg Left Motor Leg Right Limb Ataxia Sensory Neglect Dysarthria Best Language Range 0 – 3 0 – 2 0 – 3 0 – 4 0 – 2 0 – 3 21
 12 cranial nerves check § § § I smell II vision III pupil constriction, eye movement IV downward gaze V facial sensation VI lateral eye movement § VII taste, frown, smile § VIII hearing, balance § IX taste, gag, swallowing § X voice § XI shoulder shrug § XII tongue 22 movement
12 cranial nerves check § § § I smell II vision III pupil constriction, eye movement IV downward gaze V facial sensation VI lateral eye movement § VII taste, frown, smile § VIII hearing, balance § IX taste, gag, swallowing § X voice § XI shoulder shrug § XII tongue 22 movement
 Preparation Know your stroke team before you need them § Check glucose § Two large IV lines § Oxygen as needed § Cardiac monitor § Continuous pulse-ox § Stat non-contrast CT scan § ECG § CXR § Get rt-PA > Prepare to mix > Have pharmacy alerted § Discuss options with patient and family § Contact primary care provider 23
Preparation Know your stroke team before you need them § Check glucose § Two large IV lines § Oxygen as needed § Cardiac monitor § Continuous pulse-ox § Stat non-contrast CT scan § ECG § CXR § Get rt-PA > Prepare to mix > Have pharmacy alerted § Discuss options with patient and family § Contact primary care provider 23
 American Heart Association Recommendations Oxygen § Use to correct hypoxia § Suggestion that supernormal levels may hurt > one year survival 69% 3 L NC vs 73% control Glucose § Maintain euglycemia § Treat glucose > 300 mg/dl with insulin 24 Source: Rønning, Stroke 1999
American Heart Association Recommendations Oxygen § Use to correct hypoxia § Suggestion that supernormal levels may hurt > one year survival 69% 3 L NC vs 73% control Glucose § Maintain euglycemia § Treat glucose > 300 mg/dl with insulin 24 Source: Rønning, Stroke 1999
 True Time of Onset How normal were they? § What are they like at baseline? § Who saw them last? § Clearly no symptoms? Times of reference § Television § The time the basketball game started 25
True Time of Onset How normal were they? § What are they like at baseline? § Who saw them last? § Clearly no symptoms? Times of reference § Television § The time the basketball game started 25
 Stroke Risk Factors Modifiable risk factors Non-modifiable risk factors § High blood pressure § Cigarette smoking § Transient ischemic attacks § Heart disease § Diabetes mellitus § Hypercoagulopathy § Carotid stenosis § § § Age Gender Race Prior stroke Heredity – Bruits § Other 26
Stroke Risk Factors Modifiable risk factors Non-modifiable risk factors § High blood pressure § Cigarette smoking § Transient ischemic attacks § Heart disease § Diabetes mellitus § Hypercoagulopathy § Carotid stenosis § § § Age Gender Race Prior stroke Heredity – Bruits § Other 26
 Differential Diagnosis Intracerebral hemorrhage Hypoglycemia / Hyperglycemia Seizure Migraine headache Hypertensive crisis Epidural / Subdural Meningitis / Encephalitis / Brain abscess § Tumor § § § § 27
Differential Diagnosis Intracerebral hemorrhage Hypoglycemia / Hyperglycemia Seizure Migraine headache Hypertensive crisis Epidural / Subdural Meningitis / Encephalitis / Brain abscess § Tumor § § § § 27
 What are the Options? No thrombolytics § Nothing § Aspirin § Heparin Intravenous rt-PA Other § Intra-arterial thrombolytics § Investigative procedure 28
What are the Options? No thrombolytics § Nothing § Aspirin § Heparin Intravenous rt-PA Other § Intra-arterial thrombolytics § Investigative procedure 28
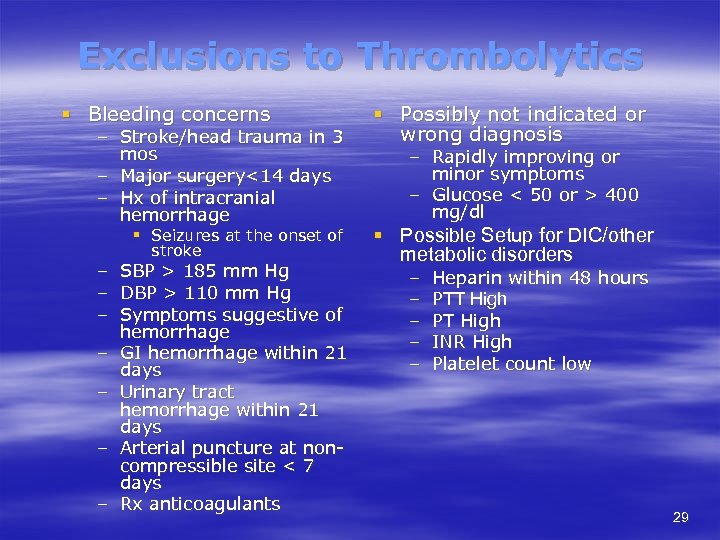 Exclusions to Thrombolytics § Bleeding concerns – Stroke/head trauma in 3 mos – Major surgery<14 days – Hx of intracranial hemorrhage § Seizures at the onset of stroke – SBP > 185 mm Hg – DBP > 110 mm Hg – Symptoms suggestive of hemorrhage – GI hemorrhage within 21 days – Urinary tract hemorrhage within 21 days – Arterial puncture at noncompressible site < 7 days – Rx anticoagulants § Possibly not indicated or wrong diagnosis – Rapidly improving or minor symptoms – Glucose < 50 or > 400 mg/dl § Possible Setup for DIC/other metabolic disorders – – – Heparin within 48 hours PTT High PT High INR High Platelet count low 29
Exclusions to Thrombolytics § Bleeding concerns – Stroke/head trauma in 3 mos – Major surgery<14 days – Hx of intracranial hemorrhage § Seizures at the onset of stroke – SBP > 185 mm Hg – DBP > 110 mm Hg – Symptoms suggestive of hemorrhage – GI hemorrhage within 21 days – Urinary tract hemorrhage within 21 days – Arterial puncture at noncompressible site < 7 days – Rx anticoagulants § Possibly not indicated or wrong diagnosis – Rapidly improving or minor symptoms – Glucose < 50 or > 400 mg/dl § Possible Setup for DIC/other metabolic disorders – – – Heparin within 48 hours PTT High PT High INR High Platelet count low 29
 Let’s talk about blood pressure § MAP – Mean Arterial Pressure (70 -90 Normal) § ICP – Intracranial Pressure – – Normally about 0 -15 mm. Hg >20 = Bad § CPP – Cerebral Perfusion Pressure – – CPP=MAP-ICP CPP must be above 70 mm. Hg for cerebral perfusion § You do the math 30
Let’s talk about blood pressure § MAP – Mean Arterial Pressure (70 -90 Normal) § ICP – Intracranial Pressure – – Normally about 0 -15 mm. Hg >20 = Bad § CPP – Cerebral Perfusion Pressure – – CPP=MAP-ICP CPP must be above 70 mm. Hg for cerebral perfusion § You do the math 30
 IF CPP=MAP-ICP § And we know that the body autoregulates pressures to preserve itself – 80 -90% of ischemic strokes present with elevated BP – ICP may have risen because of Edema 31
IF CPP=MAP-ICP § And we know that the body autoregulates pressures to preserve itself – 80 -90% of ischemic strokes present with elevated BP – ICP may have risen because of Edema 31
 Studied: – Multicenter Study – 372 patients – Compared Neuro outcome vs BP changes in first 24 hours – If Diastolic BP decreased by >25% (even once) § Poorer outcomes regardless of baseline diastolic BP levels, Stroke location or use of HTN agents – NO EVIDENCE THAT LOWERING BP HELPS § Remember we’re still talking about ischemic strokes – FAIR Evidence that it harms 32
Studied: – Multicenter Study – 372 patients – Compared Neuro outcome vs BP changes in first 24 hours – If Diastolic BP decreased by >25% (even once) § Poorer outcomes regardless of baseline diastolic BP levels, Stroke location or use of HTN agents – NO EVIDENCE THAT LOWERING BP HELPS § Remember we’re still talking about ischemic strokes – FAIR Evidence that it harms 32
 BP Treated in extreme cases “Gentle” management if thrombolytic candidate: § SBP > 180 mm Hg § DBP > 110 mm Hg Choices: § Labetalol § Enalapril § Nitropaste 33
BP Treated in extreme cases “Gentle” management if thrombolytic candidate: § SBP > 180 mm Hg § DBP > 110 mm Hg Choices: § Labetalol § Enalapril § Nitropaste 33
 Treatment Considerations: Who will benefit from rt-PA? § Patient age § Co-morbid factors – Medical history § Risks of treatment – Odds of Presenting § Benefits of Treatment – Odds of surviving 34
Treatment Considerations: Who will benefit from rt-PA? § Patient age § Co-morbid factors – Medical history § Risks of treatment – Odds of Presenting § Benefits of Treatment – Odds of surviving 34
 Treatment considerations (cont’d) § § § Time from onset (Remember 3 hours) Stroke severity Stroke subtype – Data driven here too § CT findings – Assymetry = Bad – Density image – Tissue/fluid ratio § § Charcoal=Normal Dark = Higher density (more tissue than fluid) – Ischemia § Light = Lower density (More fluid than tissue) – Hemorrhage – Tumor 35
Treatment considerations (cont’d) § § § Time from onset (Remember 3 hours) Stroke severity Stroke subtype – Data driven here too § CT findings – Assymetry = Bad – Density image – Tissue/fluid ratio § § Charcoal=Normal Dark = Higher density (more tissue than fluid) – Ischemia § Light = Lower density (More fluid than tissue) – Hemorrhage – Tumor 35
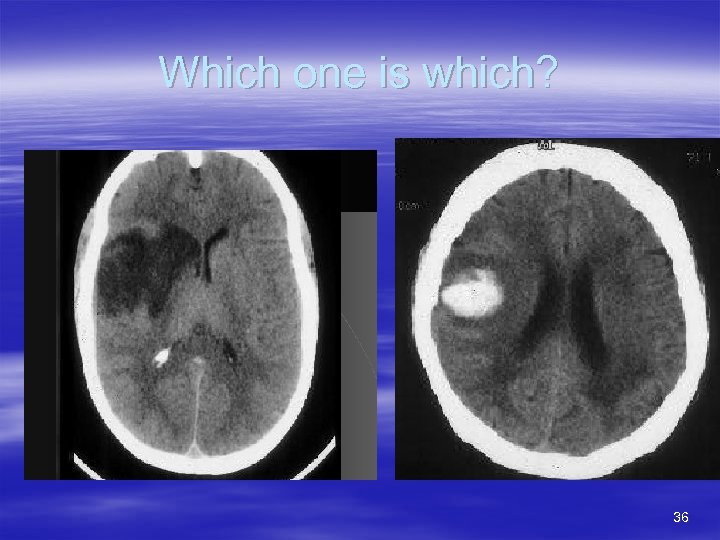 Which one is which? 36
Which one is which? 36
 Factors Associated with Increased Risk of ICH § § § Treatment initiated > 3 hours Increased thrombolytic dose Elevated blood pressure NIHSS > 20 * Acute hypodensity or mass effect * * Even though increased r/o ICH, still with benefit vs. placebo 37
Factors Associated with Increased Risk of ICH § § § Treatment initiated > 3 hours Increased thrombolytic dose Elevated blood pressure NIHSS > 20 * Acute hypodensity or mass effect * * Even though increased r/o ICH, still with benefit vs. placebo 37
 Stroke Treatment – Aspirin § Two important trials: > International Stroke Trial > Chinese Acute Stroke Trial § Combined analysis (n=40, 090) § Death / nonfatal strokes reduced 11% § Don’t forget to check swallowing § Local protocol driven 38
Stroke Treatment – Aspirin § Two important trials: > International Stroke Trial > Chinese Acute Stroke Trial § Combined analysis (n=40, 090) § Death / nonfatal strokes reduced 11% § Don’t forget to check swallowing § Local protocol driven 38
 Stroke Treatment – Heparinoids § Decreased recurrent ischemic strokes § Increased hemorrhagic events § No net stroke benefit 39
Stroke Treatment – Heparinoids § Decreased recurrent ischemic strokes § Increased hemorrhagic events § No net stroke benefit 39
Case Study § History: § A" src="https://present5.com/presentation/247af13b1153e8fc5c8e23038be2e4f7/image-40.jpg" alt="The "Golden Hour" of Acute Ischemic Stroke > Case Study § History: § A" />
The "Golden Hour" of Acute Ischemic Stroke > Case Study § History: § A 61 year old male, with acute aphasia, right facial droop, and right sided weakness. 40
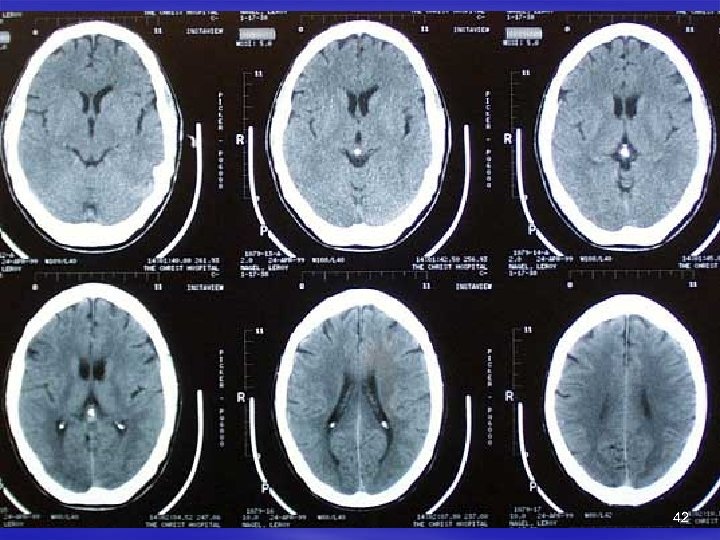
 12: 30 Sudden onset while working in yard. 12: 45 Family calls 911. 13: 05 Advanced squad evaluates neurologic deficits and glucose. 13: 15 Squad notifies receiving hospital of possible stroke patient 13: 30 ED arrival. Initial evaluation by E. D. physician. 13: 45 Stroke Team arrives. NIHSS 18. 14: 00 CT scan performed. 14: 15 Discuss with family and PMD. 14: 20 Labs back: gluc 97. BP remains 150/70’s. 14: 20 CT reading back. No hemorrhage or early signs of ischemia 41
12: 30 Sudden onset while working in yard. 12: 45 Family calls 911. 13: 05 Advanced squad evaluates neurologic deficits and glucose. 13: 15 Squad notifies receiving hospital of possible stroke patient 13: 30 ED arrival. Initial evaluation by E. D. physician. 13: 45 Stroke Team arrives. NIHSS 18. 14: 00 CT scan performed. 14: 15 Discuss with family and PMD. 14: 20 Labs back: gluc 97. BP remains 150/70’s. 14: 20 CT reading back. No hemorrhage or early signs of ischemia 41
 42
42
 14: 25 Checklist done. No exclusion criteria met. 14: 30 Decision time. 14: 35 IV rt-PA given. 0. 9 mg/kg total > 10% bolus - 9 mg > 90% over 1 hr - 81 mg 15: 45 Patient goes to ICU. Report personally given to ICU staff. 15: 50 Pathway actions begin (HOB, BP parameters, aspiration precautions). 43
14: 25 Checklist done. No exclusion criteria met. 14: 30 Decision time. 14: 35 IV rt-PA given. 0. 9 mg/kg total > 10% bolus - 9 mg > 90% over 1 hr - 81 mg 15: 45 Patient goes to ICU. Report personally given to ICU staff. 15: 50 Pathway actions begin (HOB, BP parameters, aspiration precautions). 43
 24 Hour Follow-up § A 61 year old male, with acute stroke, treated with rt-PA. § Repeat NIHSS = 3: § VF intact § No gaze palsy § Mild facial palsy § Mild right arm drift § Mild dysarthria 44
24 Hour Follow-up § A 61 year old male, with acute stroke, treated with rt-PA. § Repeat NIHSS = 3: § VF intact § No gaze palsy § Mild facial palsy § Mild right arm drift § Mild dysarthria 44
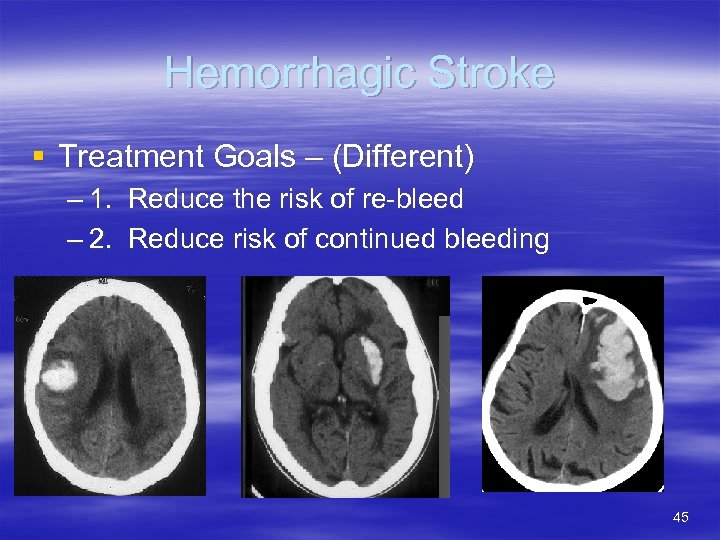 Hemorrhagic Stroke § Treatment Goals – (Different) – 1. Reduce the risk of re-bleed – 2. Reduce risk of continued bleeding 45
Hemorrhagic Stroke § Treatment Goals – (Different) – 1. Reduce the risk of re-bleed – 2. Reduce risk of continued bleeding 45
 Hemorrhagic Stroke (16%) § Bleeding into or surrounding the brain § Intracerebral Hemorrhage (ICH) – HTN – Tumor/Lesions – Venous sinus thrombosis § Drains from the dura mater – Amyloid angiopathy § Starch-like deposits on vessel walls- precursor 46
Hemorrhagic Stroke (16%) § Bleeding into or surrounding the brain § Intracerebral Hemorrhage (ICH) – HTN – Tumor/Lesions – Venous sinus thrombosis § Drains from the dura mater – Amyloid angiopathy § Starch-like deposits on vessel walls- precursor 46
 Hemorrhagic Stroke (16%) § Bleeding into or surrounding the brain § Sub-arachnoid hemorrhage (SAH) – Blood in arachnoid space, basal cisterns & often intraventricular § § § Aneurysm rupture Trauma Arteriovenous malformation (AVM) 47
Hemorrhagic Stroke (16%) § Bleeding into or surrounding the brain § Sub-arachnoid hemorrhage (SAH) – Blood in arachnoid space, basal cisterns & often intraventricular § § § Aneurysm rupture Trauma Arteriovenous malformation (AVM) 47
 Some Skull Ground Rules § Monroe-Kellie Hypothesis – Intracranial space/volume constant – Three components = ICP § CSF – 100 m. L – Production/absorption is pressure driven § Blood – 150 m. L – Here lies the problem § Brain – 1250 m. L (or grams) – Relatively constant (IS H 2 O minimally displaceable) 48
Some Skull Ground Rules § Monroe-Kellie Hypothesis – Intracranial space/volume constant – Three components = ICP § CSF – 100 m. L – Production/absorption is pressure driven § Blood – 150 m. L – Here lies the problem § Brain – 1250 m. L (or grams) – Relatively constant (IS H 2 O minimally displaceable) 48
 Head Bleeds § § § Still assuming a closed system (non-trauma) ICP will rise BP will rise – Remember autoregulation (compensatory) § If SBP>230 & DBP > 120 – Sodium Nitroprusside 0. 5 mcg/kg/min § If SBP>180 & DBP >105 – Labetolol 10 mg/1 -2 min – Double q 10 to 300 mg § If Hypertensive, but not extremely high – LEAVE IT ALONE 49
Head Bleeds § § § Still assuming a closed system (non-trauma) ICP will rise BP will rise – Remember autoregulation (compensatory) § If SBP>230 & DBP > 120 – Sodium Nitroprusside 0. 5 mcg/kg/min § If SBP>180 & DBP >105 – Labetolol 10 mg/1 -2 min – Double q 10 to 300 mg § If Hypertensive, but not extremely high – LEAVE IT ALONE 49
 Benefits of playing with BP § § § Decrease Edema Limit size of damaged area Limit further vascular damage § Might actually need a fluid bolus – 1 Hypotensive episode-mortality 30+ % 50
Benefits of playing with BP § § § Decrease Edema Limit size of damaged area Limit further vascular damage § Might actually need a fluid bolus – 1 Hypotensive episode-mortality 30+ % 50
 Risks of playing with BP § TOO MUCH § TOO FAST – Can extend stroke by eliminating tamponade – Expose patients to medication reactions § Goal – SBP < 160 – DBP < 100 § Sometimes use a 20% of original rule 51
Risks of playing with BP § TOO MUCH § TOO FAST – Can extend stroke by eliminating tamponade – Expose patients to medication reactions § Goal – SBP < 160 – DBP < 100 § Sometimes use a 20% of original rule 51
 Respiratory Management § Intubate patients with GCS < 8 § Paralyze & Heavily Sedate – 11 th commandment § Causes of Increased ICP – – Gagging Puking Stress Respiratory distress § Cause increased intra-thoracic pressure § Decreases cerebral drainage 52
Respiratory Management § Intubate patients with GCS < 8 § Paralyze & Heavily Sedate – 11 th commandment § Causes of Increased ICP – – Gagging Puking Stress Respiratory distress § Cause increased intra-thoracic pressure § Decreases cerebral drainage 52
 Respiratory Management § Post-intubation – Use LA paralytic § Watch BP Carefully for hypotension 53
Respiratory Management § Post-intubation – Use LA paralytic § Watch BP Carefully for hypotension 53
 Respiratory Management § Hyper-oxygenate § DO NOT hyperventilate – CO 2 is POTENT vasodilator – Hypocarbia causes cerebral vasoconstriction § Vasoconstriction causes edema § ICP’s may rise § CPP will drop § Loss of autoregulation … Brain death 54
Respiratory Management § Hyper-oxygenate § DO NOT hyperventilate – CO 2 is POTENT vasodilator – Hypocarbia causes cerebral vasoconstriction § Vasoconstriction causes edema § ICP’s may rise § CPP will drop § Loss of autoregulation … Brain death 54
 Adjuncts § Sp. O 2 Monitoring (Volume) – Bag to keep sat’s at 95 -100% – (This might be VERY slow) – 5 -7 m. L/kg § CO 2 Monitoring (Rate) – Bag slow enough to keep Et. CO 2 § 28 -32 § (40 ish is normal) 55
Adjuncts § Sp. O 2 Monitoring (Volume) – Bag to keep sat’s at 95 -100% – (This might be VERY slow) – 5 -7 m. L/kg § CO 2 Monitoring (Rate) – Bag slow enough to keep Et. CO 2 § 28 -32 § (40 ish is normal) 55
 Other treatments considered § Osmotic Diuretics – Mannitol (comes in and out of favor) § Anticonvulsant’s – Prevent seizures § Anti-emetics § May operate on bleeders – Often too late by the time it is diagnosed 56
Other treatments considered § Osmotic Diuretics – Mannitol (comes in and out of favor) § Anticonvulsant’s – Prevent seizures § Anti-emetics § May operate on bleeders – Often too late by the time it is diagnosed 56
 Questions 57
Questions 57
 Some pictures, Just for fun 58
Some pictures, Just for fun 58
 59
59
 60
60
 61
61
 62
62
 63
63
 64
64
 65
65
 66
66
 67
67
 68
68
 69
69


