c6e2b8690065257f3012a9c1d8592e2a.ppt
- Количество слайдов: 23
 Strategies to support change in your facility Susanne Salem-Schatz, Sc. D. Program Director, MA Coalition for the Prevention of Medical Errors Health. Care Quality Initiatives sss@HCQI. com 1
Strategies to support change in your facility Susanne Salem-Schatz, Sc. D. Program Director, MA Coalition for the Prevention of Medical Errors Health. Care Quality Initiatives sss@HCQI. com 1
 So far you have heard § § § Why it is important not to use antibioitics unless absolutely necessary; How the high prevalence of asymptomatic bacteriuria in the elderly can lead to unnecessary antibiotic use; Expert recommendations for when to test and when to treat a suspected UTI; 2
So far you have heard § § § Why it is important not to use antibioitics unless absolutely necessary; How the high prevalence of asymptomatic bacteriuria in the elderly can lead to unnecessary antibiotic use; Expert recommendations for when to test and when to treat a suspected UTI; 2
 I’m convinced… § § § Much of what we heard is not widely understood; Long standing and habitual practices can actually harm the people we are trying to help. Changing practices about urine testing and treatment of the elderly is a very reasonable thing to do. 3
I’m convinced… § § § Much of what we heard is not widely understood; Long standing and habitual practices can actually harm the people we are trying to help. Changing practices about urine testing and treatment of the elderly is a very reasonable thing to do. 3
 Time for change § Should be easy § § We know the right thing to do We intend to make a change We are sure others will follow suit when we share what we have learned. Not so fast § § Change is hard Intention is not enough 4
Time for change § Should be easy § § We know the right thing to do We intend to make a change We are sure others will follow suit when we share what we have learned. Not so fast § § Change is hard Intention is not enough 4
 Good news: we can help 1. Tools and strategies to support practice change (after lunch) 2. Proven organizational approaches to practice improvement § § Engagement strategies: from buy-in to ownership A quality improvement framework. 5
Good news: we can help 1. Tools and strategies to support practice change (after lunch) 2. Proven organizational approaches to practice improvement § § Engagement strategies: from buy-in to ownership A quality improvement framework. 5
 Some facts § § § Knowing is not enough. Evidence of non-clinical influences on clinical decision-making* It’s not just what you know, it’s who you know. *Salem-Schatz SR, Avorn J, Soumerai SB. Influence of knowledge and attitudes on the quality of physicians‘ transfusion practice. Medical Care, 1993; 31: 868 -878. 6
Some facts § § § Knowing is not enough. Evidence of non-clinical influences on clinical decision-making* It’s not just what you know, it’s who you know. *Salem-Schatz SR, Avorn J, Soumerai SB. Influence of knowledge and attitudes on the quality of physicians‘ transfusion practice. Medical Care, 1993; 31: 868 -878. 6
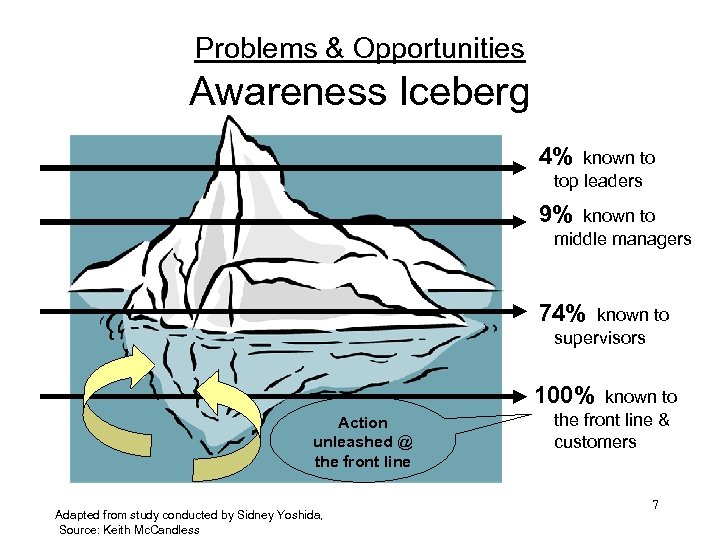 Problems & Opportunities Awareness Iceberg 4% known to top leaders 9% known to middle managers 74% known to supervisors 100% Action unleashed @ the front line Adapted from study conducted by Sidney Yoshida, Source: Keith Mc. Candless known to the front line & customers 7
Problems & Opportunities Awareness Iceberg 4% known to top leaders 9% known to middle managers 74% known to supervisors 100% Action unleashed @ the front line Adapted from study conducted by Sidney Yoshida, Source: Keith Mc. Candless known to the front line & customers 7
 Including front line staff: § § Engages the very people “whose behavior needs to change to solve the problem” to identify existing solutions from within Front line engagement & ownership can: elicit good ideas that account for day to day realities suppress the “immune rejection response” 8
Including front line staff: § § Engages the very people “whose behavior needs to change to solve the problem” to identify existing solutions from within Front line engagement & ownership can: elicit good ideas that account for day to day realities suppress the “immune rejection response” 8
 Jasper Palmer to remo discovered a b ve gow ns and etter way gloves Over and over we discovered staff who had better practices. And staff helped develop even better ideas….
Jasper Palmer to remo discovered a b ve gow ns and etter way gloves Over and over we discovered staff who had better practices. And staff helped develop even better ideas….
 “…when a group of individuals becomes a ‘we’, a harmonious whole, they have reached as high as humans can reach. ” ~ Albert Einstein, 1954
“…when a group of individuals becomes a ‘we’, a harmonious whole, they have reached as high as humans can reach. ” ~ Albert Einstein, 1954
 Harrington staff step up the fight against hospital acquired infections 11
Harrington staff step up the fight against hospital acquired infections 11
 What you can do § § § Expand the circle of your conversation Don’t rely solely on train-the-trainer ASK about their experience § § What do they know about the problem? What would they like to know? What keeps them doing the right thing 100% of the time? What ideas do they have that might help? 12
What you can do § § § Expand the circle of your conversation Don’t rely solely on train-the-trainer ASK about their experience § § What do they know about the problem? What would they like to know? What keeps them doing the right thing 100% of the time? What ideas do they have that might help? 12
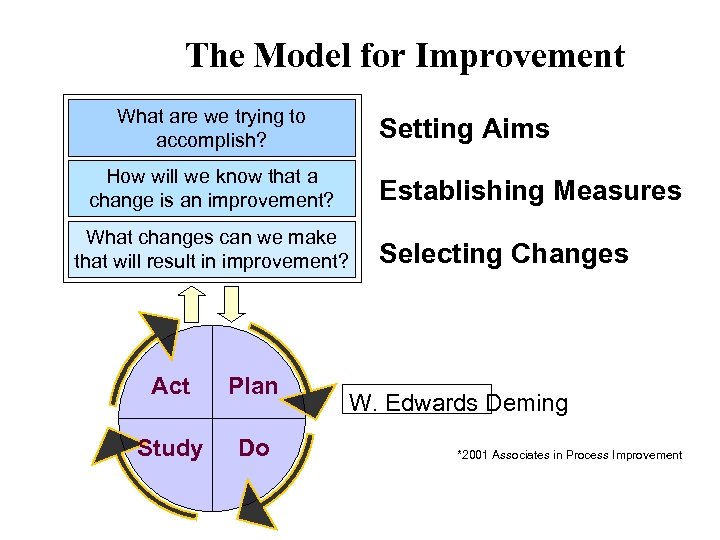 The Model for Improvement What are we trying to accomplish? How will we know that a change is an improvement? What changes can we make that will result in improvement? Act Plan Study Do Setting Aims Establishing Measures Selecting Changes W. Edwards Deming *2001 Associates in Process Improvement
The Model for Improvement What are we trying to accomplish? How will we know that a change is an improvement? What changes can we make that will result in improvement? Act Plan Study Do Setting Aims Establishing Measures Selecting Changes W. Edwards Deming *2001 Associates in Process Improvement
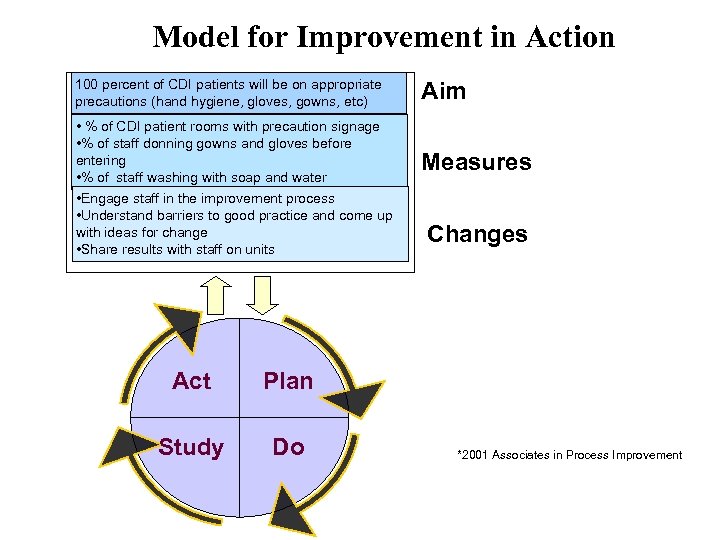 Model for Improvement in Action 100 percent of CDI patients will be on appropriate precautions (hand hygiene, gloves, gowns, etc) • % of CDI patient rooms with precaution signage • % of staff donning gowns and gloves before entering • % of staff washing with soap and water • Engage staff in the improvement process • Understand barriers to good practice and come up with ideas for change • Share results with staff on units Act Do Measures Changes Plan Study Aim *2001 Associates in Process Improvement
Model for Improvement in Action 100 percent of CDI patients will be on appropriate precautions (hand hygiene, gloves, gowns, etc) • % of CDI patient rooms with precaution signage • % of staff donning gowns and gloves before entering • % of staff washing with soap and water • Engage staff in the improvement process • Understand barriers to good practice and come up with ideas for change • Share results with staff on units Act Do Measures Changes Plan Study Aim *2001 Associates in Process Improvement
 Act Plan Study PDSA: Small Tests of Change Do Plan: • • • 1 small change to test Predict what will happen Decide on what data to evaluate test Do: • • • Study Run the test Document problems and observations Organize your data • • • Analyze your data Compare results t your predictions Summarize what you have learned Act • Decide what to do next • More testing? • Try something else? • Finalize the change?
Act Plan Study PDSA: Small Tests of Change Do Plan: • • • 1 small change to test Predict what will happen Decide on what data to evaluate test Do: • • • Study Run the test Document problems and observations Organize your data • • • Analyze your data Compare results t your predictions Summarize what you have learned Act • Decide what to do next • More testing? • Try something else? • Finalize the change?
 Some tips for testing § § Small tests of change Rule of 1 § § Test over a short period of time § § § 1 patient/resident – 1 staff person – 1 day If they say weeks, think days If they say days, think hours PDSA Worksheet to plan your test § Call for help! 16
Some tips for testing § § Small tests of change Rule of 1 § § Test over a short period of time § § § 1 patient/resident – 1 staff person – 1 day If they say weeks, think days If they say days, think hours PDSA Worksheet to plan your test § Call for help! 16
 Planning your Changes (in your handouts)
Planning your Changes (in your handouts)
 Using the model for improvement to prevent transmission of CDI: How Franciscan Hospital for Children makes it work. 18
Using the model for improvement to prevent transmission of CDI: How Franciscan Hospital for Children makes it work. 18
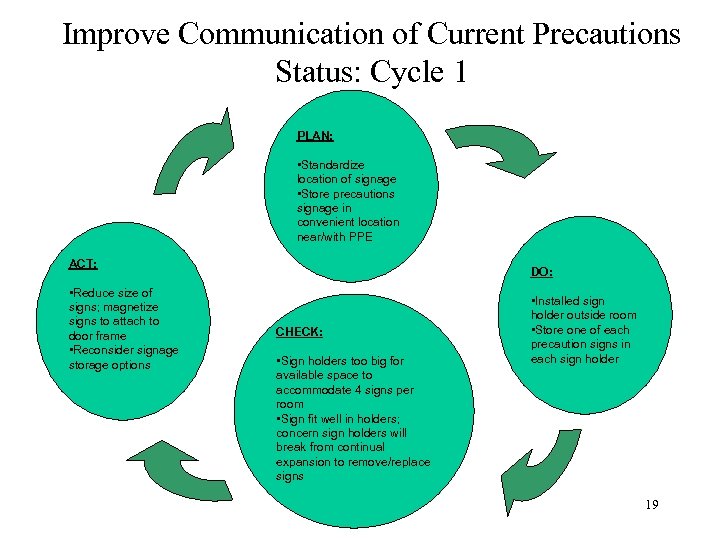 Improve Communication of Current Precautions Status: Cycle 1 PLAN: • Standardize location of signage • Store precautions signage in convenient location near/with PPE ACT: • Reduce size of signs; magnetize signs to attach to door frame • Reconsider signage storage options DO: CHECK: • Sign holders too big for available space to accommodate 4 signs per room • Sign fit well in holders; concern sign holders will break from continual expansion to remove/replace signs • Installed sign holder outside room • Store one of each precaution signs in each sign holder 19
Improve Communication of Current Precautions Status: Cycle 1 PLAN: • Standardize location of signage • Store precautions signage in convenient location near/with PPE ACT: • Reduce size of signs; magnetize signs to attach to door frame • Reconsider signage storage options DO: CHECK: • Sign holders too big for available space to accommodate 4 signs per room • Sign fit well in holders; concern sign holders will break from continual expansion to remove/replace signs • Installed sign holder outside room • Store one of each precaution signs in each sign holder 19
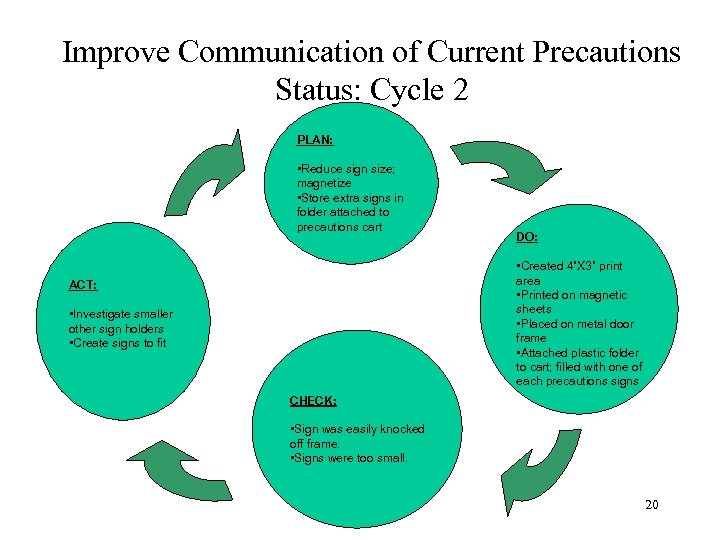 Improve Communication of Current Precautions Status: Cycle 2 PLAN: • Reduce sign size; magnetize • Store extra signs in folder attached to precautions cart DO: • Created 4”X 3” print area • Printed on magnetic sheets • Placed on metal door frame • Attached plastic folder to cart; filled with one of each precautions signs ACT: • Investigate smaller other sign holders • Create signs to fit CHECK: • Sign was easily knocked off frame. • Signs were too small. 20
Improve Communication of Current Precautions Status: Cycle 2 PLAN: • Reduce sign size; magnetize • Store extra signs in folder attached to precautions cart DO: • Created 4”X 3” print area • Printed on magnetic sheets • Placed on metal door frame • Attached plastic folder to cart; filled with one of each precautions signs ACT: • Investigate smaller other sign holders • Create signs to fit CHECK: • Sign was easily knocked off frame. • Signs were too small. 20
 Aim: Improve Communication of Current Precautions Status TA A D AP SD Delays in precautions implementation A S P D DS PA AP SD DS PA Improved adherence to current precautions Cycle 1 E: Implement sign holders for all rooms Cycle 1 D: Educate clinical, ancillary, and support staff on new signage Cycle 1 C: Increase size, post in plastic sign holder, test on one room get feedback Cycle 1 B: Reduce size, magnetize for doorframe placement. Test on one room get feedback. Cycle 1 A: Standardize precautions signage location, test on one room, and get feedback. 21
Aim: Improve Communication of Current Precautions Status TA A D AP SD Delays in precautions implementation A S P D DS PA AP SD DS PA Improved adherence to current precautions Cycle 1 E: Implement sign holders for all rooms Cycle 1 D: Educate clinical, ancillary, and support staff on new signage Cycle 1 C: Increase size, post in plastic sign holder, test on one room get feedback Cycle 1 B: Reduce size, magnetize for doorframe placement. Test on one room get feedback. Cycle 1 A: Standardize precautions signage location, test on one room, and get feedback. 21
 22
22
 Questions? § We are always available for your questions § § Listserve Email Next? § § § Lunch Tools and tips for training and practice change Program measurement 23
Questions? § We are always available for your questions § § Listserve Email Next? § § § Lunch Tools and tips for training and practice change Program measurement 23


