eece57fe23114575c0cfcfd9ce0181b2.ppt
- Количество слайдов: 69
 Sterling Education Services A Practical Guide to Workers’ Compensation – Friday January 17, 2014, Rochester, New York 1
Sterling Education Services A Practical Guide to Workers’ Compensation – Friday January 17, 2014, Rochester, New York 1
 A Practical Guide to Workers’ Compensation III. LWEC – Recent Developments IV. Valuing and Negotiating Claims for Settlement V. Legislative and Case Law Update VI. The Board’s Treatment of Labor Market Attachment Post-Zamora Presented by Melissa A. Day, Esq. and James B. Cousins, Esq. The Law Offices of Melissa A. Day, PLLC Friday, January 17, 2014 2
A Practical Guide to Workers’ Compensation III. LWEC – Recent Developments IV. Valuing and Negotiating Claims for Settlement V. Legislative and Case Law Update VI. The Board’s Treatment of Labor Market Attachment Post-Zamora Presented by Melissa A. Day, Esq. and James B. Cousins, Esq. The Law Offices of Melissa A. Day, PLLC Friday, January 17, 2014 2
 III. LWEC – Recent Developments 3
III. LWEC – Recent Developments 3
 LWEC/PPD Classifications Review 4
LWEC/PPD Classifications Review 4
 Maximum Medical Improvement 5
Maximum Medical Improvement 5
 6
6
 Maximum Medical Improvement n The starting point for determining both schedule and non-schedule permanent disabilities is the finding by a medical professional that the injured worker has reached maximum medical improvement (MMI) and has a causally related permanent impairment. 7
Maximum Medical Improvement n The starting point for determining both schedule and non-schedule permanent disabilities is the finding by a medical professional that the injured worker has reached maximum medical improvement (MMI) and has a causally related permanent impairment. 7
 Three Steps to LWEC 8
Three Steps to LWEC 8
 9
9
 Three Steps to LWEC 1. A medical determination of permanent medical impairment; 2. A medical assessment of functional abilities/limitations; and, 3. A judicial (legal) determination of LWEC using the impairment, functional, and vocational (nonmedical) evidence. 10
Three Steps to LWEC 1. A medical determination of permanent medical impairment; 2. A medical assessment of functional abilities/limitations; and, 3. A judicial (legal) determination of LWEC using the impairment, functional, and vocational (nonmedical) evidence. 10
 Non-Schedule Permanent Disabilities n Under Buffalo Auto Recovery Services, 2010 N. Y. Wrk. Comp. 80703905, LWEC is determined based upon the preponderance of the evidence concerning the nature and degree of the work-related permanent impairment, work restrictions, claimant's age, and any other relevant factors, with wage earning capacity as its inverse. n Longley Jones Management Corp. , 2012 N. Y. Wrk. Comp. 6070 4882 (February 8, 2012) decision overrules part of Buffalo Auto Recovery. RTW wages are just one of the factors taken into account in determining LWEC. n While the impairment rating may coincidentally be the same percentage as the ultimate finding of loss of wage-earning capacity, the medical impairment rating is not to be used as a direct translation to loss of wageearning capacity (see e. g. Matter of Patchogue-Medford School Dist. , 2011 NY Wrk Comp 40803044). 11
Non-Schedule Permanent Disabilities n Under Buffalo Auto Recovery Services, 2010 N. Y. Wrk. Comp. 80703905, LWEC is determined based upon the preponderance of the evidence concerning the nature and degree of the work-related permanent impairment, work restrictions, claimant's age, and any other relevant factors, with wage earning capacity as its inverse. n Longley Jones Management Corp. , 2012 N. Y. Wrk. Comp. 6070 4882 (February 8, 2012) decision overrules part of Buffalo Auto Recovery. RTW wages are just one of the factors taken into account in determining LWEC. n While the impairment rating may coincidentally be the same percentage as the ultimate finding of loss of wage-earning capacity, the medical impairment rating is not to be used as a direct translation to loss of wageearning capacity (see e. g. Matter of Patchogue-Medford School Dist. , 2011 NY Wrk Comp 40803044). 11
 Cameron v. Crooked Lake House, 106 A. D. 3 d 1416 (3 rd Dept. 2013) n The Appellate Division considered Claimant’s appeal after a finding that he had a 75% LWEC and affirmed finding: ¨ Inasmuch as claimant has not worked since sustaining his partial disability, the Board is authorized to "fix such wage earning capacity as shall be reasonable. . . having due regard to the nature of his injury and his physical impairment" (Workers' Compensation Law § 15 [5 -a]; see Matter of Mc. Cann v Mc. Cormack's Garage, Inc. , 203 App Div 387, 388 -389, 197 N. Y. S. 19 [1922]). In fixing that capacity, the Board relies upon various factors, including "the nature and degree of the work-related permanent physical and/or mental impairment, work restrictions, [and] claimant's age" (Employer: Buffalo Auto Recovery Serv. , 2009 NY Wrk Comp LEXIS 15501, *27, 2009 WL 5177881, *10 [WCB No. 8070 3905, Nov. 12, 2009]). Here, in addition to the medical evidence documenting claimant's degree of impairment, the Board considered claimant's testimony in this regard, as well as his age and his efforts to train for or seek other work within his limitations. Deferring to the Board's assessments of credibility, substantial evidence supports its decision that claimant's established, partial disability has deprived him of 75% of his wage-earning capacity (see generally Matter of Haibel v C. G. Haibel, Inc. , 101 AD 2 d 678, 679, 475 N. Y. S. 2 d 576 [1984]). 12
Cameron v. Crooked Lake House, 106 A. D. 3 d 1416 (3 rd Dept. 2013) n The Appellate Division considered Claimant’s appeal after a finding that he had a 75% LWEC and affirmed finding: ¨ Inasmuch as claimant has not worked since sustaining his partial disability, the Board is authorized to "fix such wage earning capacity as shall be reasonable. . . having due regard to the nature of his injury and his physical impairment" (Workers' Compensation Law § 15 [5 -a]; see Matter of Mc. Cann v Mc. Cormack's Garage, Inc. , 203 App Div 387, 388 -389, 197 N. Y. S. 19 [1922]). In fixing that capacity, the Board relies upon various factors, including "the nature and degree of the work-related permanent physical and/or mental impairment, work restrictions, [and] claimant's age" (Employer: Buffalo Auto Recovery Serv. , 2009 NY Wrk Comp LEXIS 15501, *27, 2009 WL 5177881, *10 [WCB No. 8070 3905, Nov. 12, 2009]). Here, in addition to the medical evidence documenting claimant's degree of impairment, the Board considered claimant's testimony in this regard, as well as his age and his efforts to train for or seek other work within his limitations. Deferring to the Board's assessments of credibility, substantial evidence supports its decision that claimant's established, partial disability has deprived him of 75% of his wage-earning capacity (see generally Matter of Haibel v C. G. Haibel, Inc. , 101 AD 2 d 678, 679, 475 N. Y. S. 2 d 576 [1984]). 12
 PPD Caps 13
PPD Caps 13
 PPD Caps n The date that the caps begins to run is the date of the decision classifying the claimant. See Target, 2012 N. Y. Wrk. Comp. G 005 9924. n If classification and LWEC are bifurcated, the caps begin to run on the date of classification. See Grandma’s Candy Cottage, 2013 NY Wrk. Comp. 2080 0327, 2013 NY Wrk. Comp. LEXIS 11562: ¨ Here, the evidence shows that the claimant was classified with a permanent partial disability to a 50% degree via the WCLJ reserved decision of April 5, 2012. Since classification took place on that date, the date on which the cap weeks should properly begin to run is April 5, 2012; not the subsequent date when the finding of loss of wage earning capacity was made. 14
PPD Caps n The date that the caps begins to run is the date of the decision classifying the claimant. See Target, 2012 N. Y. Wrk. Comp. G 005 9924. n If classification and LWEC are bifurcated, the caps begin to run on the date of classification. See Grandma’s Candy Cottage, 2013 NY Wrk. Comp. 2080 0327, 2013 NY Wrk. Comp. LEXIS 11562: ¨ Here, the evidence shows that the claimant was classified with a permanent partial disability to a 50% degree via the WCLJ reserved decision of April 5, 2012. Since classification took place on that date, the date on which the cap weeks should properly begin to run is April 5, 2012; not the subsequent date when the finding of loss of wage earning capacity was made. 14
 Hearing Process PPD Claims 15
Hearing Process PPD Claims 15
 LWEC Hearing Process 1. Maximum Medical Improvement a) When one opinion received, Board issues EC-81. 8 to other party to respond and claimant directed to complete VDF-1 form. b) If there is a dispute, litigate MMI with decision in 45 days. c) If no MMI, process ends (for now). 16
LWEC Hearing Process 1. Maximum Medical Improvement a) When one opinion received, Board issues EC-81. 8 to other party to respond and claimant directed to complete VDF-1 form. b) If there is a dispute, litigate MMI with decision in 45 days. c) If no MMI, process ends (for now). 16
 Proof of MMI Medical Opinions from Both Parties Agree or Parties Stipulate to Medical: If the Board receives medical opinions from both parties that agree on MMI, impairment and function or if the parties stipulate to medical facts (by submitting the C 300. 5 Stipulation Agreement), the Board will schedule a hearing, or parties may use the Walk-in Stipulation Calendar process. At the hearing, the parties can develop the record on vocational factors and the WC Law Judge will issue a decision on loss of wage earning capacity. One Medical Opinion Received: If the Board receives only one medical opinion on MMI/Non-schedule Permanency, it will send the other party a letter that advises the party that it can: (1) accept the original medical opinion or (2) submit conflicting medical evidence on any of the issues. The Board will also schedule a hearing for medical development/scheduling of testimony.
Proof of MMI Medical Opinions from Both Parties Agree or Parties Stipulate to Medical: If the Board receives medical opinions from both parties that agree on MMI, impairment and function or if the parties stipulate to medical facts (by submitting the C 300. 5 Stipulation Agreement), the Board will schedule a hearing, or parties may use the Walk-in Stipulation Calendar process. At the hearing, the parties can develop the record on vocational factors and the WC Law Judge will issue a decision on loss of wage earning capacity. One Medical Opinion Received: If the Board receives only one medical opinion on MMI/Non-schedule Permanency, it will send the other party a letter that advises the party that it can: (1) accept the original medical opinion or (2) submit conflicting medical evidence on any of the issues. The Board will also schedule a hearing for medical development/scheduling of testimony.
 Resolving Medical Conflicts Initial Hearing: If the Board receives conflicting medical opinions on MMI and/or Non-schedule Permanency, the Board will calendar an initial hearing for medical development/scheduling of testimony. At this initial hearing, the WC Law Judge will review the classification process, make findings as appropriate and direct medical development as necessary. If medical development is necessary and the claimant is unrepresented, the WC Law Judge will schedule a subsequent hearing with live medical testimony in lieu of directing depositions. Note: Deposition transcripts should address the relevant outstanding issues which may include whether or not the claimant has reached maximum medical improvement, classification as a non-schedule permanent partial disability, the severity rating of the claimant's medical impairment, and the claimant's functional capabilities/exertional abilities as provided by the 2012 Guidelines for Determining Impairment and Loss of Wage Earning Capacity. The deposition transcripts should be submitted by the date designated in the Notice of Decision.
Resolving Medical Conflicts Initial Hearing: If the Board receives conflicting medical opinions on MMI and/or Non-schedule Permanency, the Board will calendar an initial hearing for medical development/scheduling of testimony. At this initial hearing, the WC Law Judge will review the classification process, make findings as appropriate and direct medical development as necessary. If medical development is necessary and the claimant is unrepresented, the WC Law Judge will schedule a subsequent hearing with live medical testimony in lieu of directing depositions. Note: Deposition transcripts should address the relevant outstanding issues which may include whether or not the claimant has reached maximum medical improvement, classification as a non-schedule permanent partial disability, the severity rating of the claimant's medical impairment, and the claimant's functional capabilities/exertional abilities as provided by the 2012 Guidelines for Determining Impairment and Loss of Wage Earning Capacity. The deposition transcripts should be submitted by the date designated in the Notice of Decision.
 Determining Loss of Wage Earning Capacity The WC Law Judge will schedule the Permanency/Classification hearing (with medical evidence and lay testimony regarding vocational factors) approximately 90 days from the date of the initial hearing to allow time for the submission of deposition transcripts, as well as to ensure that the WC Law Judge has time to review the deposition transcripts off calendar and in advance of the hearing. Permanency/Classification Hearing: The WC Law Judge will review the medical depositions prior to the hearing. At the hearing, the WC Law Judge will take live lay testimony on vocational factors and hear summations. After considering all the medical and non-medical evidence, the judge will issue a decision on loss of wage earning capacity. Note: If at any point the parties reach agreement or stipulate to the medical evidence, the parties should submit a C-300. 5 Stipulation Agreement. The Board will schedule a hearing and the WC Law Judge conducting the hearing will issue a decision on loss of wage earning capacity.
Determining Loss of Wage Earning Capacity The WC Law Judge will schedule the Permanency/Classification hearing (with medical evidence and lay testimony regarding vocational factors) approximately 90 days from the date of the initial hearing to allow time for the submission of deposition transcripts, as well as to ensure that the WC Law Judge has time to review the deposition transcripts off calendar and in advance of the hearing. Permanency/Classification Hearing: The WC Law Judge will review the medical depositions prior to the hearing. At the hearing, the WC Law Judge will take live lay testimony on vocational factors and hear summations. After considering all the medical and non-medical evidence, the judge will issue a decision on loss of wage earning capacity. Note: If at any point the parties reach agreement or stipulate to the medical evidence, the parties should submit a C-300. 5 Stipulation Agreement. The Board will schedule a hearing and the WC Law Judge conducting the hearing will issue a decision on loss of wage earning capacity.
 Expedited Permanency Process Part 29 Even cases which do not have medical evidence that the Claimant is at MMI can be put on the calendar on the issue of permanency pursuant to the Chair’s recent efforts “To promote permanency classifications” (Board Subject # 146 -548). Thus cases which are: (1) at least two years old; (2) had ongoing indemnity benefits and a continuing payment order; (3) was established for readily classifiable injuries to the head, neck or back; (4) had been marked “NFA” at the last hearing; May also be scheduled for a hearing on permanency.
Expedited Permanency Process Part 29 Even cases which do not have medical evidence that the Claimant is at MMI can be put on the calendar on the issue of permanency pursuant to the Chair’s recent efforts “To promote permanency classifications” (Board Subject # 146 -548). Thus cases which are: (1) at least two years old; (2) had ongoing indemnity benefits and a continuing payment order; (3) was established for readily classifiable injuries to the head, neck or back; (4) had been marked “NFA” at the last hearing; May also be scheduled for a hearing on permanency.
 The Medical Direction Hearing n At this hearing, both parties will be directed to produce evidence of MMI and permanency within 60 days by a valid IME-4 and a properly completed C-4. 3.
The Medical Direction Hearing n At this hearing, both parties will be directed to produce evidence of MMI and permanency within 60 days by a valid IME-4 and a properly completed C-4. 3.
 22
22
 The Medical Production Hearing Schedule Litigation. 60 Days sixty days to produce deposition transcripts (medical testimony) Case continued 90 days for the testimony of the claimant on loss of wage earning capacity. If a party fails to produce the directed evidence of MMI, that party will be precluded from producing such evidence on the issue. If neither party produces evidence of MMI, the case will be continued again for another 60 days for production of that evidence. Neither party will be precluded, but the carrier will be penalized under WCL § 114 -a(3)(ii) for causing undue delay and an unnecessary continuance. No penalty will be levied against a carrier if they can show “good cause” for the failure to produce the directed medical evidence. In lieu of such a penalty against a claimant, it may instead be levied against his/her counsel.
The Medical Production Hearing Schedule Litigation. 60 Days sixty days to produce deposition transcripts (medical testimony) Case continued 90 days for the testimony of the claimant on loss of wage earning capacity. If a party fails to produce the directed evidence of MMI, that party will be precluded from producing such evidence on the issue. If neither party produces evidence of MMI, the case will be continued again for another 60 days for production of that evidence. Neither party will be precluded, but the carrier will be penalized under WCL § 114 -a(3)(ii) for causing undue delay and an unnecessary continuance. No penalty will be levied against a carrier if they can show “good cause” for the failure to produce the directed medical evidence. In lieu of such a penalty against a claimant, it may instead be levied against his/her counsel.
 The Loss of Wage Earning Capacity Hearing Parties depose the conflicting medical experts and produce transcripts 60 days after the “Medical Production Hearing. ” At this hearing, the WCLJ will hear the claimant’s testimony on LWEC as well as arguments from counsel and issue a bench ruling on MMI, Impairment and Loss of Wage Earning Capacity. If the record is complex, or complicated, an opportunity to brief the case may be permitted. If depositions were unable to be timely completed, the WCLJ may permit the parties to brief the case simply to keep the process moving forward and permit the claimant to testify about LWEC without forcing a continuance.
The Loss of Wage Earning Capacity Hearing Parties depose the conflicting medical experts and produce transcripts 60 days after the “Medical Production Hearing. ” At this hearing, the WCLJ will hear the claimant’s testimony on LWEC as well as arguments from counsel and issue a bench ruling on MMI, Impairment and Loss of Wage Earning Capacity. If the record is complex, or complicated, an opportunity to brief the case may be permitted. If depositions were unable to be timely completed, the WCLJ may permit the parties to brief the case simply to keep the process moving forward and permit the claimant to testify about LWEC without forcing a continuance.
 Removing a Case from the Expedited Permanency Part 1. Seek a finding of “No MMI. ” 2. Produce Proof of a Section 32 Agreement. 3. Produce proof that CMS approval of a settlement is required, and that an effort to obtain CMS approval is underway. 4. Obtain a ruling of MMI without Permanency.
Removing a Case from the Expedited Permanency Part 1. Seek a finding of “No MMI. ” 2. Produce Proof of a Section 32 Agreement. 3. Produce proof that CMS approval of a settlement is required, and that an effort to obtain CMS approval is underway. 4. Obtain a ruling of MMI without Permanency.
 Request Review by an Impartial Specialist n The Board recently announced improvements to its Impartial Specialist program, which allow the parties to agree to use an Impartial Specialist and to select the specific physician. Parties are encouraged to utilize Impartial Specialists or other jointly selected authorized physicians to perform a single permanency evaluation rather than engaging competing medical experts.
Request Review by an Impartial Specialist n The Board recently announced improvements to its Impartial Specialist program, which allow the parties to agree to use an Impartial Specialist and to select the specific physician. Parties are encouraged to utilize Impartial Specialists or other jointly selected authorized physicians to perform a single permanency evaluation rather than engaging competing medical experts.
 Improved Process for IS A referral to an Impartial Specialist may be: ordered by a judge, a Board panel, or the full Board during an administrative appeal, or may be agreed to by the parties in a claim. The referral may be for a full examination or a review of records. Parties have 10 days ten days to submit any medical evidence that is not currently in the Board’s electronic file. During that time, the parties have the opportunity to agree on a particular Impartial Specialist; if they do not, the Board will assign one from the panel based on the relevant specialty, geographic area, and the physician’s availability. Under exceptional circumstances, such as when there is no designated Impartial Specialist with the relevant specialty training within a reasonable geographic area who is available to evaluate the claimant, the Chair may designate a physician to conduct a particular Impartial Specialist examination or review of records. If the Impartial Specialist is required to perform a physical examination, the Board will arrange the appointment with the Impartial Specialist and notify the claimant of the location, date and time. The Board will provide the Impartial Specialist with an electronic (or paper) copy of the medical records contained in the Board’s e-case file in advance. The Impartial Specialist must submit his or her report to the Board using the Form IS-4, Report of Impartial Specialist Examination or Record Review, within 20 days of the examination or 25 days of receiving the records, if no exam is performed. The parties will have the option of cross-examining the Impartial Specialist, either by deposition if the claimant is represented or at a hearing if not. If testimony is taken by deposition, the carrier must arrange for the transcript to be submitted to the Board within 45 days.
Improved Process for IS A referral to an Impartial Specialist may be: ordered by a judge, a Board panel, or the full Board during an administrative appeal, or may be agreed to by the parties in a claim. The referral may be for a full examination or a review of records. Parties have 10 days ten days to submit any medical evidence that is not currently in the Board’s electronic file. During that time, the parties have the opportunity to agree on a particular Impartial Specialist; if they do not, the Board will assign one from the panel based on the relevant specialty, geographic area, and the physician’s availability. Under exceptional circumstances, such as when there is no designated Impartial Specialist with the relevant specialty training within a reasonable geographic area who is available to evaluate the claimant, the Chair may designate a physician to conduct a particular Impartial Specialist examination or review of records. If the Impartial Specialist is required to perform a physical examination, the Board will arrange the appointment with the Impartial Specialist and notify the claimant of the location, date and time. The Board will provide the Impartial Specialist with an electronic (or paper) copy of the medical records contained in the Board’s e-case file in advance. The Impartial Specialist must submit his or her report to the Board using the Form IS-4, Report of Impartial Specialist Examination or Record Review, within 20 days of the examination or 25 days of receiving the records, if no exam is performed. The parties will have the option of cross-examining the Impartial Specialist, either by deposition if the claimant is represented or at a hearing if not. If testimony is taken by deposition, the carrier must arrange for the transcript to be submitted to the Board within 45 days.
 Board Appoints Impartial Specialist Sua Sponte n Widely, or wildly, divergent opinions between the AP and IME may lead the Board to have the claimant reviewed by an impartial specialist. See Broadalbin. Perth Central, 2013 NY Wrk. Comp. 5070 7906, 2013 NY Wrk. Comp. LEXIS 9597. n Parties are given 10 days to agree on the IS or the Board will appoint one and then meds must be submitted within 10 days of appointment if they are not in e. Case.
Board Appoints Impartial Specialist Sua Sponte n Widely, or wildly, divergent opinions between the AP and IME may lead the Board to have the claimant reviewed by an impartial specialist. See Broadalbin. Perth Central, 2013 NY Wrk. Comp. 5070 7906, 2013 NY Wrk. Comp. LEXIS 9597. n Parties are given 10 days to agree on the IS or the Board will appoint one and then meds must be submitted within 10 days of appointment if they are not in e. Case.
 Medical Impairment 29
Medical Impairment 29
 Medical Impairment n Although the PILWECG do not envision evaluating claimants by assessing their degree of disability (the evaluation is supposed to assess severity of the impairment and functional capabilities), in Mc. Donalds, 2013 NY Wrk. Comp. G 032 8068, 2013 NY Wrk. Comp. LEXIS 12004, the Board upheld a LWEC finding which was based in part on a finding that the claimant had a: ¨ 62. 50% impairment, based on the testimony of the claimant's physician, Dr. Zhou, and the carrier's consultant, Dr. Totero. The Board Panel finds that a finding of a moderate-tomarked disability is consistent with the medical record and the Board Medical Guidelines. ”
Medical Impairment n Although the PILWECG do not envision evaluating claimants by assessing their degree of disability (the evaluation is supposed to assess severity of the impairment and functional capabilities), in Mc. Donalds, 2013 NY Wrk. Comp. G 032 8068, 2013 NY Wrk. Comp. LEXIS 12004, the Board upheld a LWEC finding which was based in part on a finding that the claimant had a: ¨ 62. 50% impairment, based on the testimony of the claimant's physician, Dr. Zhou, and the carrier's consultant, Dr. Totero. The Board Panel finds that a finding of a moderate-tomarked disability is consistent with the medical record and the Board Medical Guidelines. ”
 Medical Impairment + Voc Factors = LWEC ¨ In Hannibal Central School District, 2013 NY Wrk. Comp. G 014 8455, 2013 NY Wrk. Comp. LEXIS 9544, the WCLJ found that the Claimant had a 50% disability and given “the claimant's vocational history and education, as well as his age and retirement status, I do find an additional 25% loss in addition to the 50% physical impairment for an overall 75% loss of wage earning capacity. “ The Board affirmed.
Medical Impairment + Voc Factors = LWEC ¨ In Hannibal Central School District, 2013 NY Wrk. Comp. G 014 8455, 2013 NY Wrk. Comp. LEXIS 9544, the WCLJ found that the Claimant had a 50% disability and given “the claimant's vocational history and education, as well as his age and retirement status, I do find an additional 25% loss in addition to the 50% physical impairment for an overall 75% loss of wage earning capacity. “ The Board affirmed.
 Severity of the Impairment n In Town of Southold, 2013 NY Wrk. Comp. 4080 0339, 2013 NY Wrk. Comp. LEXIS 10602, the judge fashioned his own severity ranking after neither the AP or the IME provided one and the Board Panel found: ¨ “Thus, although both medical opinions on permanency were filed after January 1, 2012, neither medical opinion followed the 2012 Guidelines. Nonetheless, the WCLJ apparently agreed with Dr. Morrissey that the claimant's back injury had resolved, as he limited his findings to the neck, and then attempted to convert the two medical opinions regarding the claimant's neck injury by finding a severity rating of M under both Table 11. 1 and Table 11. 2, findings that were not expressly made by either physician. No explanation was provided for the WCLJ's severity findings either on the record at the September 13, 2012 hearing or in his decision. As a result, the Board Panel is unable to undertake any intelligent review of the WCLJ's reasoning, and since the Board may not fashion its own medical opinion, the WCLJ's decision must be rescinded. (Citations omitted). ”
Severity of the Impairment n In Town of Southold, 2013 NY Wrk. Comp. 4080 0339, 2013 NY Wrk. Comp. LEXIS 10602, the judge fashioned his own severity ranking after neither the AP or the IME provided one and the Board Panel found: ¨ “Thus, although both medical opinions on permanency were filed after January 1, 2012, neither medical opinion followed the 2012 Guidelines. Nonetheless, the WCLJ apparently agreed with Dr. Morrissey that the claimant's back injury had resolved, as he limited his findings to the neck, and then attempted to convert the two medical opinions regarding the claimant's neck injury by finding a severity rating of M under both Table 11. 1 and Table 11. 2, findings that were not expressly made by either physician. No explanation was provided for the WCLJ's severity findings either on the record at the September 13, 2012 hearing or in his decision. As a result, the Board Panel is unable to undertake any intelligent review of the WCLJ's reasoning, and since the Board may not fashion its own medical opinion, the WCLJ's decision must be rescinded. (Citations omitted). ”
 However…. n In New York Tent Company, Inc. , 2013 NY Wrk. Comp. G 044 1054, 2013 NY Wrk. Comp. LEXIS 10239, the Board rescinded the WCLJ’s finding that the claimant had a moderate disability: ¨ Here, both physicians testified to a moderate permanent partial disability. However, the work restrictions imposed by the carrier's orthopedic consultant (i. e. , no pushing, pulling, or lifting over five pounds; and no standing over 10 minutes without the opportunity to sit) are indicative of a percentage of medical impairment greater than a straight 50%. As a result, the Board Panel finds that the claimant has a 55% causally related medical impairment based on the credible testimony of Dr. Song and Dr. Toriello and the significant work restrictions placed on the claimant.
However…. n In New York Tent Company, Inc. , 2013 NY Wrk. Comp. G 044 1054, 2013 NY Wrk. Comp. LEXIS 10239, the Board rescinded the WCLJ’s finding that the claimant had a moderate disability: ¨ Here, both physicians testified to a moderate permanent partial disability. However, the work restrictions imposed by the carrier's orthopedic consultant (i. e. , no pushing, pulling, or lifting over five pounds; and no standing over 10 minutes without the opportunity to sit) are indicative of a percentage of medical impairment greater than a straight 50%. As a result, the Board Panel finds that the claimant has a 55% causally related medical impairment based on the credible testimony of Dr. Song and Dr. Toriello and the significant work restrictions placed on the claimant.
 Multiple Claims or Conditions 34
Multiple Claims or Conditions 34
 Multiple Claims or Conditions n Not uncommon for an injured worker to have a permanent impairment of more than one body part or system. n PILWECG do not provide for a mathematical combination of medical impairments. n The impact of each impairment on function and wage earning capacity to determine their cumulative effect. 35
Multiple Claims or Conditions n Not uncommon for an injured worker to have a permanent impairment of more than one body part or system. n PILWECG do not provide for a mathematical combination of medical impairments. n The impact of each impairment on function and wage earning capacity to determine their cumulative effect. 35
 Adesa Corporation, 2013 NY Wrk. Comp 8060 0263, 2013 NY Wrk. Comp. Lexis 8492 n Where a Claimant has multiple workers’ compensation claims which both contribute to his overall disability, there must be a determination as to what percent of the disability is related to a claim where LWEC is determined. n The Board remanded the claim for permanency opinions which provided the claimant’s overall disability, the extent to which the claimant’s disability was caused by both claims. n The prior claim was an SLU and there is no indication that the SLU claim should be reopened. 36
Adesa Corporation, 2013 NY Wrk. Comp 8060 0263, 2013 NY Wrk. Comp. Lexis 8492 n Where a Claimant has multiple workers’ compensation claims which both contribute to his overall disability, there must be a determination as to what percent of the disability is related to a claim where LWEC is determined. n The Board remanded the claim for permanency opinions which provided the claimant’s overall disability, the extent to which the claimant’s disability was caused by both claims. n The prior claim was an SLU and there is no indication that the SLU claim should be reopened. 36
 Fresh Direct Holdings, Inc. , 2013 NY Wrk. Comp G 032 3859, 2013 NY Wrk. Comp. Lexis 11430 n Claimant evaluated and found to have medical impairments with a severity ranking of 4 G at two levels: in his cervical spine and his lumbar spine. ¨ “Utilizing the guidelines crosswalk, a 4 G impairment rating for either the lumbar or cervical spine translates to a moderate or 50% permanent partial disability. While the guidelines do not specifically address the situation where, as here, the claimant has been assessed with a 4 G rating at two levels of the spine, the Board Panel deems it appropriate to take this factor into consideration in assessing the overall level of impairment for all compensable injuries. Based upon the credible medical findings of Dr. Schwartz, and pursuant to the reference to the Board's impairment guidelines, the Board Panel finds that the claimant is properly assessed with a 66 -2/3% medical impairment when taking into consideration the claimant's disability pertaining to both the cervical and lumbar spines. 37
Fresh Direct Holdings, Inc. , 2013 NY Wrk. Comp G 032 3859, 2013 NY Wrk. Comp. Lexis 11430 n Claimant evaluated and found to have medical impairments with a severity ranking of 4 G at two levels: in his cervical spine and his lumbar spine. ¨ “Utilizing the guidelines crosswalk, a 4 G impairment rating for either the lumbar or cervical spine translates to a moderate or 50% permanent partial disability. While the guidelines do not specifically address the situation where, as here, the claimant has been assessed with a 4 G rating at two levels of the spine, the Board Panel deems it appropriate to take this factor into consideration in assessing the overall level of impairment for all compensable injuries. Based upon the credible medical findings of Dr. Schwartz, and pursuant to the reference to the Board's impairment guidelines, the Board Panel finds that the claimant is properly assessed with a 66 -2/3% medical impairment when taking into consideration the claimant's disability pertaining to both the cervical and lumbar spines. 37
 38
38
 Use, but don’t use, the Crosswalk n In Price Chopper, 2013 NY Wrk. Comp. G 026 0095, 2013 NY Wrk. Comp. LEXIS 9492, the Board discusses how the new severity ratings can be translated into the old system: ¨ “Taking this finding and applying the Medical Impairment Severity Crosswalk (id. at 120) which creates a range of 0 - 6, (0 representing no medical impairment, 1 representing 25% medical impairment, 2 representing 33. 33% medical impairment, 3 representing 50% medical impairment, 4 representing 66. 66% medical impairment and 5 representing 75% medical impairment and 6 representing total medical impairment), the Board Panel finds the claimant has a marked permanent partial medical impairment (75%) as a brain injury severity rating Q - S drawn from Table 15. 1 falls within relative severity class 5 on the Medical Impairment Severity Crosswalk. ” 39
Use, but don’t use, the Crosswalk n In Price Chopper, 2013 NY Wrk. Comp. G 026 0095, 2013 NY Wrk. Comp. LEXIS 9492, the Board discusses how the new severity ratings can be translated into the old system: ¨ “Taking this finding and applying the Medical Impairment Severity Crosswalk (id. at 120) which creates a range of 0 - 6, (0 representing no medical impairment, 1 representing 25% medical impairment, 2 representing 33. 33% medical impairment, 3 representing 50% medical impairment, 4 representing 66. 66% medical impairment and 5 representing 75% medical impairment and 6 representing total medical impairment), the Board Panel finds the claimant has a marked permanent partial medical impairment (75%) as a brain injury severity rating Q - S drawn from Table 15. 1 falls within relative severity class 5 on the Medical Impairment Severity Crosswalk. ” 39
 More Crosswalk Claims n In Community Memorial Hospital, 2013 NY Wrk. Comp. G 026 3055, 2013 NY Wrk. Comp. LEXIS 9493, the Board again uses the crosswalk to translate a severity rating into the old system: ¨ Here, the Board Panel finds Dr. Hausmann credibly found the claimant has a class 3 low back medical impairment, with a severity ranking B, given the claimant has a soft tissue lumbar injury with persistent pain and mobility symptoms and given the May 20, 2011 MRI showed annular bulges and stenosis at several levels of the claimant lumbar spine. A review of the record showed the claimant was not treated surgically and did not have radicular symptoms…Taking this finding and applying the Medical Impairment Severity Crosswalk (id. at 120) which creates a range of 0 - 6, (0 representing no medical impairment, 1 representing 25% medical impairment, 2 representing 33. 33% medical impairment, 3 representing 50% medical impairment, 4 representing 66. 66% medical impairment and 5 representing 75% medical impairment and 6 representing total medical impairment), the Board Panel finds the claimant has a mild permanent partial medical impairment (25%) as a lumbar spine injury severity rating B drawn from Table 11. 1 falls within relative severity class 1 on the Medical Impairment Severity Crosswalk, as the claimant does not have radicular symptoms. 40
More Crosswalk Claims n In Community Memorial Hospital, 2013 NY Wrk. Comp. G 026 3055, 2013 NY Wrk. Comp. LEXIS 9493, the Board again uses the crosswalk to translate a severity rating into the old system: ¨ Here, the Board Panel finds Dr. Hausmann credibly found the claimant has a class 3 low back medical impairment, with a severity ranking B, given the claimant has a soft tissue lumbar injury with persistent pain and mobility symptoms and given the May 20, 2011 MRI showed annular bulges and stenosis at several levels of the claimant lumbar spine. A review of the record showed the claimant was not treated surgically and did not have radicular symptoms…Taking this finding and applying the Medical Impairment Severity Crosswalk (id. at 120) which creates a range of 0 - 6, (0 representing no medical impairment, 1 representing 25% medical impairment, 2 representing 33. 33% medical impairment, 3 representing 50% medical impairment, 4 representing 66. 66% medical impairment and 5 representing 75% medical impairment and 6 representing total medical impairment), the Board Panel finds the claimant has a mild permanent partial medical impairment (25%) as a lumbar spine injury severity rating B drawn from Table 11. 1 falls within relative severity class 1 on the Medical Impairment Severity Crosswalk, as the claimant does not have radicular symptoms. 40
 Non Causally Related Conditions 41
Non Causally Related Conditions 41
 Non-Causally Related Conditions n Guidelines are completely silent on the effect of non-occupational medical conditions which may affect earning capacity. n The language related to medical impairment and functional loss evaluations and findings are limited to the occupational conditions and affected injury sites. 42
Non-Causally Related Conditions n Guidelines are completely silent on the effect of non-occupational medical conditions which may affect earning capacity. n The language related to medical impairment and functional loss evaluations and findings are limited to the occupational conditions and affected injury sites. 42
 “Fuzzy” Factors n Any other factor which may impact the injured worker’s ability to perform paid employment. n Guidelines do not give non -occupational conditions as an example 43
“Fuzzy” Factors n Any other factor which may impact the injured worker’s ability to perform paid employment. n Guidelines do not give non -occupational conditions as an example 43
 Co-Morbidities’ Effect on LWEC n In Town of Riverhead, 2013 NY Wrk. Comp. G 002 4531, 2013 NY Wrk. Comp. LEXIS 9677, the Board discounted the opinion of a voc expert, because her, “report disregards the claimant's causally related psychological disability and the claimant's list of co-morbidities that impact his wage earning capacity. ” 44
Co-Morbidities’ Effect on LWEC n In Town of Riverhead, 2013 NY Wrk. Comp. G 002 4531, 2013 NY Wrk. Comp. LEXIS 9677, the Board discounted the opinion of a voc expert, because her, “report disregards the claimant's causally related psychological disability and the claimant's list of co-morbidities that impact his wage earning capacity. ” 44
 Co-Morbidities’ Effect on LWEC n In Price Chopper, 2013 NY Wrk. Comp. G 026 0095, 2013 NY Wrk. Comp. LEXIS 9492, the Board affirmed a finding that the Claimant had an “aggregate loss of wage earning capacity to a PTD” considering the claimant’s impairment and “pre-existing conditions, such as diabetes and a serious heart condition. ” 45
Co-Morbidities’ Effect on LWEC n In Price Chopper, 2013 NY Wrk. Comp. G 026 0095, 2013 NY Wrk. Comp. LEXIS 9492, the Board affirmed a finding that the Claimant had an “aggregate loss of wage earning capacity to a PTD” considering the claimant’s impairment and “pre-existing conditions, such as diabetes and a serious heart condition. ” 45
 Literacy and Language Proficiency 46
Literacy and Language Proficiency 46
 47
47
 Literacy and Language Proficiency n In Cooperative Home Care, 2013 NY Wrk. Comp. 0081 7463, 2013 NY Wrk. Comp. LEXIS 11860, the Board upheld a 60% LWEC of a Spanish only speaking claimant with a moderate disability: ¨ “The WCLJ noted that the claimant's reliance upon Spanish for communication was not as great an impediment as the claimant's attorney argues, considering the claimant's geographical location within New York State. ” 48
Literacy and Language Proficiency n In Cooperative Home Care, 2013 NY Wrk. Comp. 0081 7463, 2013 NY Wrk. Comp. LEXIS 11860, the Board upheld a 60% LWEC of a Spanish only speaking claimant with a moderate disability: ¨ “The WCLJ noted that the claimant's reliance upon Spanish for communication was not as great an impediment as the claimant's attorney argues, considering the claimant's geographical location within New York State. ” 48
 Claimant Returns to Work 49
Claimant Returns to Work 49
 Claimant RTW Earning in Excess of AWW n In more than one Board Panel Decision, including Wegmans, 2012 NY Wrk. Comp. G 003 2313 and Great Meadow Correctional, 2012 NY Wrk. Comp. , G 011 4439, the Board found that a Claimant who has returned to work earning in excess of their established weekly wage has a 0% loss of wage earning capacity but is still entitled to 225 weeks of capped PPD benefits in the event that they are wages fall below their former AWW. 50
Claimant RTW Earning in Excess of AWW n In more than one Board Panel Decision, including Wegmans, 2012 NY Wrk. Comp. G 003 2313 and Great Meadow Correctional, 2012 NY Wrk. Comp. , G 011 4439, the Board found that a Claimant who has returned to work earning in excess of their established weekly wage has a 0% loss of wage earning capacity but is still entitled to 225 weeks of capped PPD benefits in the event that they are wages fall below their former AWW. 50
 Claimant RTW Earning in Excess of AWW after Longley Jones n After Longley Jones, a RTW where the claimant is earning in excess of the former AWW does not require a finding that the Claimant has a 0% LWEC. n See, Bravo Solutions, 2013 NY Wrk. Comp. , G 027 7830, 2013 NY Wrk. Comp. LEXIS 85908 and Catskill Regional Medical Ctr. , 2013 NY Wrk. Comp. , G 008 8390, 2013 NY Wrk. Comp. LEXIS 8026 51
Claimant RTW Earning in Excess of AWW after Longley Jones n After Longley Jones, a RTW where the claimant is earning in excess of the former AWW does not require a finding that the Claimant has a 0% LWEC. n See, Bravo Solutions, 2013 NY Wrk. Comp. , G 027 7830, 2013 NY Wrk. Comp. LEXIS 85908 and Catskill Regional Medical Ctr. , 2013 NY Wrk. Comp. , G 008 8390, 2013 NY Wrk. Comp. LEXIS 8026 51
 Claimant RTW with ARE n Although Longley Jones, holds that wages are not the sole basis for determining LWEC: ¨ “This does not mean that a PPD claimant's wages at the time of classification are irrelevant. They are an important factor that must be considered and weighed by the WCLJ in determining a claimant's actual loss of wage earning capacity" (Matter of Longley Jones Management Corp. , 2012 NY Wrk Comp 60704882). ” See, Ametek Thermal System, 2013 NY Wrk. Comp. G 044 0305, 2013 NY Wrk. Comp. LEXIS 8110. 52
Claimant RTW with ARE n Although Longley Jones, holds that wages are not the sole basis for determining LWEC: ¨ “This does not mean that a PPD claimant's wages at the time of classification are irrelevant. They are an important factor that must be considered and weighed by the WCLJ in determining a claimant's actual loss of wage earning capacity" (Matter of Longley Jones Management Corp. , 2012 NY Wrk Comp 60704882). ” See, Ametek Thermal System, 2013 NY Wrk. Comp. G 044 0305, 2013 NY Wrk. Comp. LEXIS 8110. 52
 Other LWEC Issues 53
Other LWEC Issues 53
 Evaluations by a Vocational Expert n Shining Star Services, LLC, April 15, 2013: A Claimant is not required to submit to an evaluation by the carrier’s consultant for a vocational evaluation. n In OCM Boces, 2013 NY Wrk. Comp. 6070 8709, 2013 NY Wrk. Comp. LEXIS 8976: ¨ While the testimony of the SIE's vocational counselor is helpful in identifying potential employment opportunities and suggesting employment types which might match both claimant's restrictions and aptitudes, little credence is given here to her finding of a 015% loss of wage earning capacity where the counselor calculated the loss of wage earning capacity by identifying wages typical to a few potential alternative employments, some of which were unsuitable given the claimant's physical limitations and work experience. Consideration of only a limited field of possible work opportunities currently available (and some positions actually were not currently available) is an overly narrow basis for a final determination. Moreover, it considers only the capacity at the present time, while a determination of loss of wage earning capacity reasonably includes consideration of the impact upon future earnings potential and not just a limited sample of current work opportunities. Thus, the formulation suggested by the SIE's counselor in determining lost wage earnings capacity is not relied upon in this particular claim.
Evaluations by a Vocational Expert n Shining Star Services, LLC, April 15, 2013: A Claimant is not required to submit to an evaluation by the carrier’s consultant for a vocational evaluation. n In OCM Boces, 2013 NY Wrk. Comp. 6070 8709, 2013 NY Wrk. Comp. LEXIS 8976: ¨ While the testimony of the SIE's vocational counselor is helpful in identifying potential employment opportunities and suggesting employment types which might match both claimant's restrictions and aptitudes, little credence is given here to her finding of a 015% loss of wage earning capacity where the counselor calculated the loss of wage earning capacity by identifying wages typical to a few potential alternative employments, some of which were unsuitable given the claimant's physical limitations and work experience. Consideration of only a limited field of possible work opportunities currently available (and some positions actually were not currently available) is an overly narrow basis for a final determination. Moreover, it considers only the capacity at the present time, while a determination of loss of wage earning capacity reasonably includes consideration of the impact upon future earnings potential and not just a limited sample of current work opportunities. Thus, the formulation suggested by the SIE's counselor in determining lost wage earnings capacity is not relied upon in this particular claim.
 Effect of Social Security Determinations n The Board Panel notes that, while not determinative, the findings of the Social Security Administration reflect some evidence as to the degree and extent of the claimant's physical limitations as well as the impact of these upon the claimant's ability to work. While the conclusion that the claimant is unable to perform any type of work is not credited here, the description of the claimant's limitations and employment opportunities as recited in the Social Security Administration Decision reveals a loss of earning capacity in keeping with the claimant's marked physical restrictions. For these reasons, the claimant is held here to have a 75% loss of wage earning capacity. OCM Boces, 2013 NY Wrk. Comp. 6070 8709, 2013 NY Wrk. Comp. LEXIS 8976.
Effect of Social Security Determinations n The Board Panel notes that, while not determinative, the findings of the Social Security Administration reflect some evidence as to the degree and extent of the claimant's physical limitations as well as the impact of these upon the claimant's ability to work. While the conclusion that the claimant is unable to perform any type of work is not credited here, the description of the claimant's limitations and employment opportunities as recited in the Social Security Administration Decision reveals a loss of earning capacity in keeping with the claimant's marked physical restrictions. For these reasons, the claimant is held here to have a 75% loss of wage earning capacity. OCM Boces, 2013 NY Wrk. Comp. 6070 8709, 2013 NY Wrk. Comp. LEXIS 8976.
 IV. Valuing and Negotiating Claims for Settlement 56
IV. Valuing and Negotiating Claims for Settlement 56
 Do the Math: Running the Numbers 57
Do the Math: Running the Numbers 57
 Pre-Cap of Post-Cap Claim --- WCL § 15 -3(w) or Lifetime Benefits? 03/13/2007 n Post Cap PPD: WEEKS X RATE – 5% = Value? n 5% = Regulation No. 119 adopting 11 NYCRR § 151 -2. 2 n 6 months to make the deposit § 27 -2(1) – A Ticking Clock n ATF Settlements: WCL § 27 -8 n In the case of a claim concerning which the aggregate trust fund enters a waiver agreement pursuant to section thirty-two of this article, the insurance carrier. . . which paid the present value of the award for such claim, shall not be entitled to a refund of any portion of the present value of such award. n Have you seen an ATF settlement offer? Anecdotal: 5. 5 years or 62 cents on the dollar. 58
Pre-Cap of Post-Cap Claim --- WCL § 15 -3(w) or Lifetime Benefits? 03/13/2007 n Post Cap PPD: WEEKS X RATE – 5% = Value? n 5% = Regulation No. 119 adopting 11 NYCRR § 151 -2. 2 n 6 months to make the deposit § 27 -2(1) – A Ticking Clock n ATF Settlements: WCL § 27 -8 n In the case of a claim concerning which the aggregate trust fund enters a waiver agreement pursuant to section thirty-two of this article, the insurance carrier. . . which paid the present value of the award for such claim, shall not be entitled to a refund of any portion of the present value of such award. n Have you seen an ATF settlement offer? Anecdotal: 5. 5 years or 62 cents on the dollar. 58
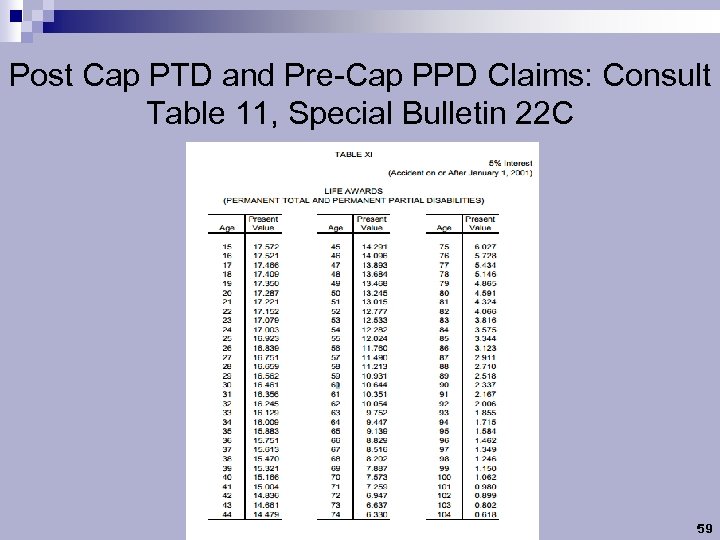 Post Cap PTD and Pre-Cap PPD Claims: Consult Table 11, Special Bulletin 22 C 59
Post Cap PTD and Pre-Cap PPD Claims: Consult Table 11, Special Bulletin 22 C 59
 Post Cap PTD and Pre-Cap PPD Claims: Consult Table 11, Special Bulletin 22 C n Benchmarks: n A 60 year-old claimant gets a 10 year cap. n SIF’s Five-year “Special” is only good for a claimant 78 years old! n Younger claimants benefit less proportionally, but reassessment likelihood probably skyrockets 60
Post Cap PTD and Pre-Cap PPD Claims: Consult Table 11, Special Bulletin 22 C n Benchmarks: n A 60 year-old claimant gets a 10 year cap. n SIF’s Five-year “Special” is only good for a claimant 78 years old! n Younger claimants benefit less proportionally, but reassessment likelihood probably skyrockets 60
 Lawyering: What Numbers Can’t Tell You 61
Lawyering: What Numbers Can’t Tell You 61
 Assessing the Cap n n n Medical Impairment – a Table, a Class and a Severity Ranking Functional Capacity – FCE, Form C-4. 3 Functional Capabilities Assessment Vocational Issues – Form VDF-1 and Independent Vocational Assessments and Claimant Testimony Current earnings are not the sole basis of an LWEC finding. Longley Jones Management Corp. , 2012 NY Wrk Comp 60704882 Factors Considered: Buffalo Auto Recovery Service, 2009 NY Wrk Comp 80703905 and Department of Juvenile Justice, 2011 NY Wrk Comp 00749328 62
Assessing the Cap n n n Medical Impairment – a Table, a Class and a Severity Ranking Functional Capacity – FCE, Form C-4. 3 Functional Capabilities Assessment Vocational Issues – Form VDF-1 and Independent Vocational Assessments and Claimant Testimony Current earnings are not the sole basis of an LWEC finding. Longley Jones Management Corp. , 2012 NY Wrk Comp 60704882 Factors Considered: Buffalo Auto Recovery Service, 2009 NY Wrk Comp 80703905 and Department of Juvenile Justice, 2011 NY Wrk Comp 00749328 62
 Medical Valuation: “Dammit Jim, I’m a lawyer, not a doctor!” 63
Medical Valuation: “Dammit Jim, I’m a lawyer, not a doctor!” 63
 MSA? CMS Approval? n The Medicare Secondary Payer Statute n 42 U. S. C. § 1395 y(b)(2) and 42 C. F. R. § 411. 1, et. seq. n $25, 000 / $250, 000 thresholds for review. n The last two years of medical payouts. n Read the medicals: surgery, pain management, what’s on the horizon? n Carrier: Get a good vendor! n Trust your opponent to CYA. n 64
MSA? CMS Approval? n The Medicare Secondary Payer Statute n 42 U. S. C. § 1395 y(b)(2) and 42 C. F. R. § 411. 1, et. seq. n $25, 000 / $250, 000 thresholds for review. n The last two years of medical payouts. n Read the medicals: surgery, pain management, what’s on the horizon? n Carrier: Get a good vendor! n Trust your opponent to CYA. n 64
 The Intangibles and Fact-Specific Factors n n n n n Claimant’s Age – LWEC, Labor Market Attachment and Willingness Labor Market Attachment – Voluntary Withdrawal, “Compensable Retirement” How strong is the claim for the entire cap? Has LMA been litigated or raised in connection with classification? Know your opponent Has either party shown interest? Has anyone tipped his/her hand? Is an ATF payable? Self-insured, § 15 -8(d), third-party action? WCL § 27 Surveillance and the issues in dispute. Client Expectations – Full and Final vs. Indemnity-Only 65
The Intangibles and Fact-Specific Factors n n n n n Claimant’s Age – LWEC, Labor Market Attachment and Willingness Labor Market Attachment – Voluntary Withdrawal, “Compensable Retirement” How strong is the claim for the entire cap? Has LMA been litigated or raised in connection with classification? Know your opponent Has either party shown interest? Has anyone tipped his/her hand? Is an ATF payable? Self-insured, § 15 -8(d), third-party action? WCL § 27 Surveillance and the issues in dispute. Client Expectations – Full and Final vs. Indemnity-Only 65
 V. Legislative and Case Law Update 66
V. Legislative and Case Law Update 66
 VI. The Board’s Treatment of Labor Market Attachment Post-Zamora 67
VI. The Board’s Treatment of Labor Market Attachment Post-Zamora 67
 QUESTIONS? Contact us! Melissa A. Day, Esq. , James B. Cousins, Esq. The Law Offices of Melissa A. Day, PLLC 2390 North Forest Road Suite 14 Amherst, New York 14068 Phone: (716) 616 -0111 Fax: (855) I GET MAD E-mail: mday@MADWCdefense. com Website: http: //www. MADWCdefense. com 68
QUESTIONS? Contact us! Melissa A. Day, Esq. , James B. Cousins, Esq. The Law Offices of Melissa A. Day, PLLC 2390 North Forest Road Suite 14 Amherst, New York 14068 Phone: (716) 616 -0111 Fax: (855) I GET MAD E-mail: mday@MADWCdefense. com Website: http: //www. MADWCdefense. com 68
 Join the New York Workers’ Compensation Forum 69
Join the New York Workers’ Compensation Forum 69


