3839652a0e3d6173b09214a582c63884.ppt
- Количество слайдов: 34
 State of the Art in Nocturia Jeffrey P. Weiss, MD, FACS Professor and Chair Department of Urology SUNY Downstate College of Medicine Brooklyn, NY
State of the Art in Nocturia Jeffrey P. Weiss, MD, FACS Professor and Chair Department of Urology SUNY Downstate College of Medicine Brooklyn, NY
 Agenda • • • Evolution Recent reviews/guidelines Definitions, related issues and prevalence Consequences Causes, diagnosis and treatment 2
Agenda • • • Evolution Recent reviews/guidelines Definitions, related issues and prevalence Consequences Causes, diagnosis and treatment 2
 Evolution of nocturia: nocturia in 2000 - Not a distinct condition but rather part of an array of symptoms associated with other diseases such as OAB or BPH - A normal factor of aging - Only important for the male population - No standardized definition and terminology of nocturia Important studies during the last decade ICS standardization of terminology (2002) TAMUS study (1994 -1999) Japan mortality study (2009 -2011) Population based study in Finland (FINNO) (2003 / 2004) Epi. LUTS study (2009) NERI analysis of nocturia and mortality (2010 / 2011) based on NHANES III results The Krimpen study (starting 1995) 3
Evolution of nocturia: nocturia in 2000 - Not a distinct condition but rather part of an array of symptoms associated with other diseases such as OAB or BPH - A normal factor of aging - Only important for the male population - No standardized definition and terminology of nocturia Important studies during the last decade ICS standardization of terminology (2002) TAMUS study (1994 -1999) Japan mortality study (2009 -2011) Population based study in Finland (FINNO) (2003 / 2004) Epi. LUTS study (2009) NERI analysis of nocturia and mortality (2010 / 2011) based on NHANES III results The Krimpen study (starting 1995) 3
 Evolution of nocturia: nocturia in 2012 - Nocturia Think Tank established under ICI-RS - Understanding of nocturia as a distinct medical condition, rather than as a symptom of BPH, OAB or other diseases - Nocturnal polyuria a common finding in all nocturia patients - Clearly correlated with age, but problem seems larger for younger patients - Not only a male disease but also similarly prevalent among females - Better understanding of quality of life effects of nocturia: ØDecreased daytime productivity due to sleep disruption ØHigher associated mortality and morbidity - Preliminary suggestions for treatment and diagnostic algorithms are available - Better perspective on ineffectiveness of some treatments (especially in primary nocturia) such as anti-muscarinics and alpha blockers 4
Evolution of nocturia: nocturia in 2012 - Nocturia Think Tank established under ICI-RS - Understanding of nocturia as a distinct medical condition, rather than as a symptom of BPH, OAB or other diseases - Nocturnal polyuria a common finding in all nocturia patients - Clearly correlated with age, but problem seems larger for younger patients - Not only a male disease but also similarly prevalent among females - Better understanding of quality of life effects of nocturia: ØDecreased daytime productivity due to sleep disruption ØHigher associated mortality and morbidity - Preliminary suggestions for treatment and diagnostic algorithms are available - Better perspective on ineffectiveness of some treatments (especially in primary nocturia) such as anti-muscarinics and alpha blockers 4
 Most recent publications summarising nocturia state of the art 5
Most recent publications summarising nocturia state of the art 5
 Many guidelines address nocturia 6
Many guidelines address nocturia 6
 Definition and related issues • Definition: voiding during (nocturnal) sleep time – Preceded and followed by sleep (ICS guidelines) • • Normal: nocturia <1 x 1 Scientific problems: – How to define sleep time – Is patient awakened by the need to void? or – Do patients void because they’re awake? 1. van Kerrebroeck et al Neurourol and Urodyn 2002; 21: 179 -83 7
Definition and related issues • Definition: voiding during (nocturnal) sleep time – Preceded and followed by sleep (ICS guidelines) • • Normal: nocturia <1 x 1 Scientific problems: – How to define sleep time – Is patient awakened by the need to void? or – Do patients void because they’re awake? 1. van Kerrebroeck et al Neurourol and Urodyn 2002; 21: 179 -83 7
 What triggers nocturia? • 50 men and women – Mean number of nocturia events = 2. 6 • Nocturia awakenings attributed to urge or not? 1 – 78% nocturic voids were preceded by urge to void – In the remainder, the patient awakened for some other reason, then voided out of habit or convenience before going back to sleep The aetiology and treatment of these two groups is likely to be different 1. Blaivas JG, Amirian M, Weiss JP et al: SUFU abstract 2010 8
What triggers nocturia? • 50 men and women – Mean number of nocturia events = 2. 6 • Nocturia awakenings attributed to urge or not? 1 – 78% nocturic voids were preceded by urge to void – In the remainder, the patient awakened for some other reason, then voided out of habit or convenience before going back to sleep The aetiology and treatment of these two groups is likely to be different 1. Blaivas JG, Amirian M, Weiss JP et al: SUFU abstract 2010 8
 What degree of nocturia is important? • Results from multiple studies of mortality, fractures and Qo. L all show ≥ 2 voids/night is a ‘threshold’ for significant negative impact from nocturia • One void/night is less likely to have serious consequences • Impact zone If treatment can reduce nocturia frequency to <2 voids/night on average, risks Comfort zone and bother to patients may be significantly reduced 9
What degree of nocturia is important? • Results from multiple studies of mortality, fractures and Qo. L all show ≥ 2 voids/night is a ‘threshold’ for significant negative impact from nocturia • One void/night is less likely to have serious consequences • Impact zone If treatment can reduce nocturia frequency to <2 voids/night on average, risks Comfort zone and bother to patients may be significantly reduced 9
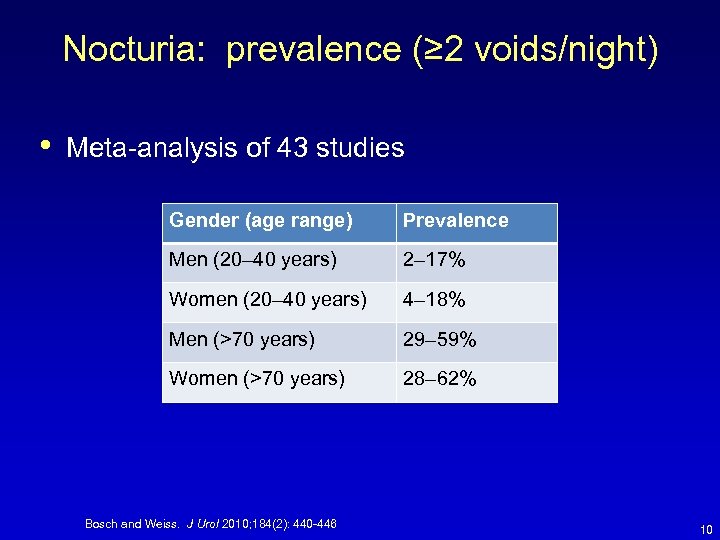 Nocturia: prevalence (≥ 2 voids/night) • Meta-analysis of 43 studies Gender (age range) Prevalence Men (20– 40 years) 2– 17% Women (20– 40 years) 4– 18% Men (>70 years) 29– 59% Women (>70 years) 28– 62% Bosch and Weiss. J Urol 2010; 184(2): 440 -446 10
Nocturia: prevalence (≥ 2 voids/night) • Meta-analysis of 43 studies Gender (age range) Prevalence Men (20– 40 years) 2– 17% Women (20– 40 years) 4– 18% Men (>70 years) 29– 59% Women (>70 years) 28– 62% Bosch and Weiss. J Urol 2010; 184(2): 440 -446 10
 Nocturia: consequences Mediated by sleep deprivation 12
Nocturia: consequences Mediated by sleep deprivation 12
 Nocturia disrupts sleep • • Nocturia is the major cause of disrupted sleep • Reduced slow wave sleep (SWS) and sleep efficiency, and short/long sleep duration may: – Increase mortality – Reduce health (including hypertension, glucose homeostasis, immunity) – Reduce Qo. L and productivity • Night-time urology must take sleep and the impact of its disruption into account Sleep is crucial for well-being, health, vitality and essential biological rhythms. Disrupted sleep impairs all of these 13
Nocturia disrupts sleep • • Nocturia is the major cause of disrupted sleep • Reduced slow wave sleep (SWS) and sleep efficiency, and short/long sleep duration may: – Increase mortality – Reduce health (including hypertension, glucose homeostasis, immunity) – Reduce Qo. L and productivity • Night-time urology must take sleep and the impact of its disruption into account Sleep is crucial for well-being, health, vitality and essential biological rhythms. Disrupted sleep impairs all of these 13
 Nocturia reduces Qo. L and improvement in nocturia improves Qo. L • Reduced Qo. L (based on HR-Qo. L) is specifically associated with nocturia in LUTS patients 1, 2 • Burden of nocturia increases with severity (based on N-Qo. L 3) • Nocturia is associated with significant decreases in 14/15 dimensions of HR-Qo. L 4 (all except eating) • Nocturia’s impact on sleep and Qo. L is more pronounced in younger compared with older patients 5, 6, 7 • Qo. L (based on N-Qo. L) increases significantly with each void reduced (~5 points) and with each hour gained in the first period of undisturbed sleep (~4 points)8 1. Hernández et al. Curr Med Res Opin 2008; 24: 1033– 1038. 2. Van Dijk et al. BJU Int 2010; 105: 1141 – 1146. 3. Yu et al. Urology 2006; 67: 713– 718. 4. Tikkinen et al. Eur Urol 2010; 57: 488– 496. 5. Asplund & Aberg. Maturitas 1996; 24: 73– 81 6. Hunskaar. BJU Int 2005; 96(suppl 1): 4– 7 7. Irwin et al. Eur Urol 2006; 50: 1306– 1314 8. Daneshgari et al. Abstract 212 at ICS/IUGA 2010 14
Nocturia reduces Qo. L and improvement in nocturia improves Qo. L • Reduced Qo. L (based on HR-Qo. L) is specifically associated with nocturia in LUTS patients 1, 2 • Burden of nocturia increases with severity (based on N-Qo. L 3) • Nocturia is associated with significant decreases in 14/15 dimensions of HR-Qo. L 4 (all except eating) • Nocturia’s impact on sleep and Qo. L is more pronounced in younger compared with older patients 5, 6, 7 • Qo. L (based on N-Qo. L) increases significantly with each void reduced (~5 points) and with each hour gained in the first period of undisturbed sleep (~4 points)8 1. Hernández et al. Curr Med Res Opin 2008; 24: 1033– 1038. 2. Van Dijk et al. BJU Int 2010; 105: 1141 – 1146. 3. Yu et al. Urology 2006; 67: 713– 718. 4. Tikkinen et al. Eur Urol 2010; 57: 488– 496. 5. Asplund & Aberg. Maturitas 1996; 24: 73– 81 6. Hunskaar. BJU Int 2005; 96(suppl 1): 4– 7 7. Irwin et al. Eur Urol 2006; 50: 1306– 1314 8. Daneshgari et al. Abstract 212 at ICS/IUGA 2010 14
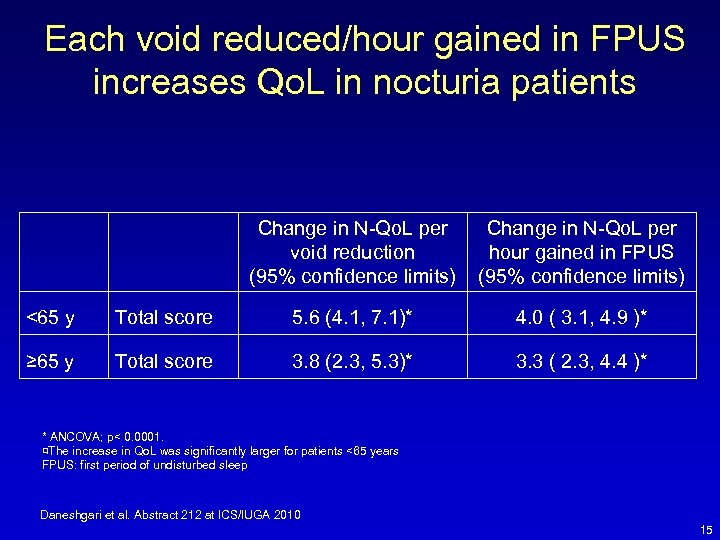 Each void reduced/hour gained in FPUS increases Qo. L in nocturia patients Change in N-Qo. L per void reduction (95% confidence limits) Change in N-Qo. L per hour gained in FPUS (95% confidence limits) <65 y Total score 5. 6 (4. 1, 7. 1)* 4. 0 ( 3. 1, 4. 9 )* ≥ 65 y Total score 3. 8 (2. 3, 5. 3)* 3. 3 ( 2. 3, 4. 4 )* * ANCOVA; p< 0. 0001. ¤The increase in Qo. L was significantly larger for patients <65 years FPUS: first period of undisturbed sleep Daneshgari et al. Abstract 212 at ICS/IUGA 2010 15
Each void reduced/hour gained in FPUS increases Qo. L in nocturia patients Change in N-Qo. L per void reduction (95% confidence limits) Change in N-Qo. L per hour gained in FPUS (95% confidence limits) <65 y Total score 5. 6 (4. 1, 7. 1)* 4. 0 ( 3. 1, 4. 9 )* ≥ 65 y Total score 3. 8 (2. 3, 5. 3)* 3. 3 ( 2. 3, 4. 4 )* * ANCOVA; p< 0. 0001. ¤The increase in Qo. L was significantly larger for patients <65 years FPUS: first period of undisturbed sleep Daneshgari et al. Abstract 212 at ICS/IUGA 2010 15
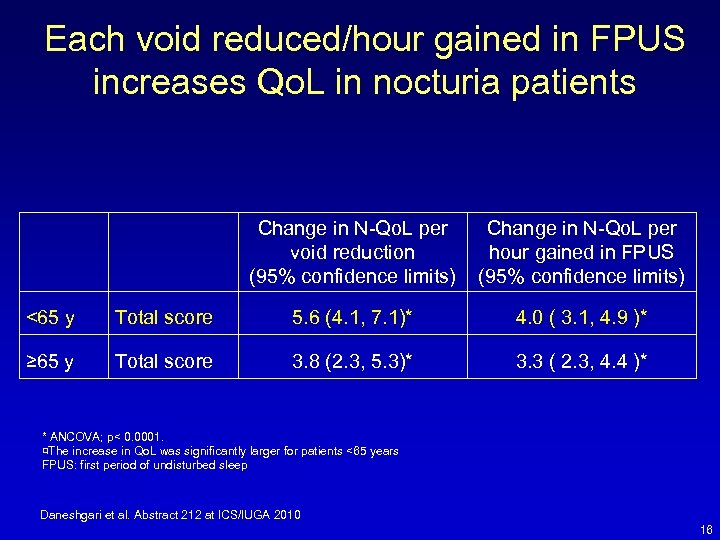 Each void reduced/hour gained in FPUS increases Qo. L in nocturia patients Change in N-Qo. L per void reduction (95% confidence limits) Change in N-Qo. L per hour gained in FPUS (95% confidence limits) <65 y Total score 5. 6 (4. 1, 7. 1)* 4. 0 ( 3. 1, 4. 9 )* ≥ 65 y Total score 3. 8 (2. 3, 5. 3)* 3. 3 ( 2. 3, 4. 4 )* * ANCOVA; p< 0. 0001. ¤The increase in Qo. L was significantly larger for patients <65 years FPUS: first period of undisturbed sleep Daneshgari et al. Abstract 212 at ICS/IUGA 2010 16
Each void reduced/hour gained in FPUS increases Qo. L in nocturia patients Change in N-Qo. L per void reduction (95% confidence limits) Change in N-Qo. L per hour gained in FPUS (95% confidence limits) <65 y Total score 5. 6 (4. 1, 7. 1)* 4. 0 ( 3. 1, 4. 9 )* ≥ 65 y Total score 3. 8 (2. 3, 5. 3)* 3. 3 ( 2. 3, 4. 4 )* * ANCOVA; p< 0. 0001. ¤The increase in Qo. L was significantly larger for patients <65 years FPUS: first period of undisturbed sleep Daneshgari et al. Abstract 212 at ICS/IUGA 2010 16
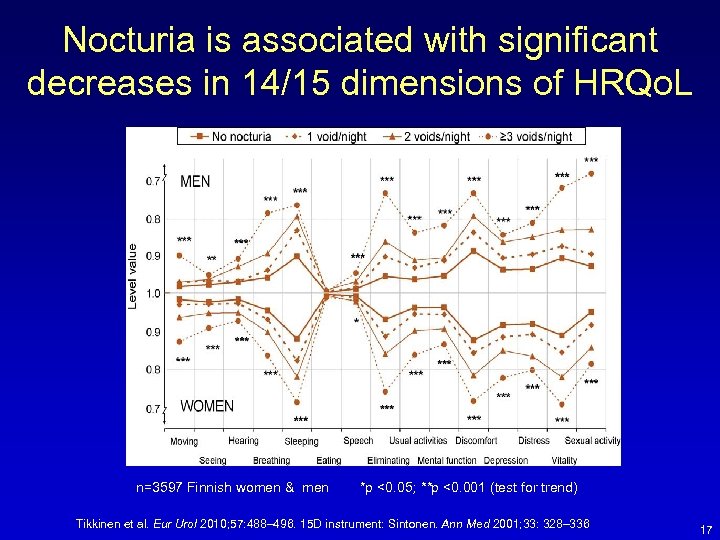 Nocturia is associated with significant decreases in 14/15 dimensions of HRQo. L n=3597 Finnish women & men *p <0. 05; **p <0. 001 (test for trend) Tikkinen et al. Eur Urol 2010; 57: 488– 496. 15 D instrument: Sintonen. Ann Med 2001; 33: 328– 336 17
Nocturia is associated with significant decreases in 14/15 dimensions of HRQo. L n=3597 Finnish women & men *p <0. 05; **p <0. 001 (test for trend) Tikkinen et al. Eur Urol 2010; 57: 488– 496. 15 D instrument: Sintonen. Ann Med 2001; 33: 328– 336 17
 Nocturia increases the risk of falls and fractures • Falls: – Parsons et al. 20091: Nocturia is the LUTS most strongly associated with falls and the risk increases with number of voids/night • Fractures: – Temml et al. 20092: Nocturia (≥ 2 voids/night) is an ageindependent risk factor for hip fractures – Nakagawa et al. 20103: In elderly patients (70– 97 yrs), nocturia (≥ 2 voids/night) HR for fall-related fractures was 2. 20 (1. 04– 4. 68) 1. Parsons et al. BJU Int 2009; 104: 63– 68; 2. Temml et al. Neurourol Urodyn 2009; 28: 949– 95; 3. Nakagawa et al. J Urol 2010; 184: 1414 -1418 18
Nocturia increases the risk of falls and fractures • Falls: – Parsons et al. 20091: Nocturia is the LUTS most strongly associated with falls and the risk increases with number of voids/night • Fractures: – Temml et al. 20092: Nocturia (≥ 2 voids/night) is an ageindependent risk factor for hip fractures – Nakagawa et al. 20103: In elderly patients (70– 97 yrs), nocturia (≥ 2 voids/night) HR for fall-related fractures was 2. 20 (1. 04– 4. 68) 1. Parsons et al. BJU Int 2009; 104: 63– 68; 2. Temml et al. Neurourol Urodyn 2009; 28: 949– 95; 3. Nakagawa et al. J Urol 2010; 184: 1414 -1418 18
 Nocturia is associated with increased mortality • Summary of three recent key studies: – Nakagawa et al. 1 (788 men and women, aged 70– 97 years): significantly increased mortality risk in elderly patients with 2, 3, and 4 vs. 1 voids/night – Kupelian et al. 2 (15, 988 men and women, aged ≥ 20 years): significantly increased mortality risk with ≥ 2 vs. <2 voids/night • Magnitude of the nocturia and mortality association was greater in those aged <65 years and in those without baseline comorbidities – Lightner et al. 3 (2, 447 men, aged 40– 79 years): significantly increased mortality risk and CHD risk in younger patients (40– 59 years) with ≥ 3 voids/night 1. Nakagawa et al. J Urol 2010; 184: 1413 -1418; 2. Kupelian et al. J Urol 2011; 185, 571 -577; 3. Lightner et al. BJU Int 2012; Jan (epub/early view) 19
Nocturia is associated with increased mortality • Summary of three recent key studies: – Nakagawa et al. 1 (788 men and women, aged 70– 97 years): significantly increased mortality risk in elderly patients with 2, 3, and 4 vs. 1 voids/night – Kupelian et al. 2 (15, 988 men and women, aged ≥ 20 years): significantly increased mortality risk with ≥ 2 vs. <2 voids/night • Magnitude of the nocturia and mortality association was greater in those aged <65 years and in those without baseline comorbidities – Lightner et al. 3 (2, 447 men, aged 40– 79 years): significantly increased mortality risk and CHD risk in younger patients (40– 59 years) with ≥ 3 voids/night 1. Nakagawa et al. J Urol 2010; 184: 1413 -1418; 2. Kupelian et al. J Urol 2011; 185, 571 -577; 3. Lightner et al. BJU Int 2012; Jan (epub/early view) 19
 Nocturia is a socio-economic burden • US analysis (based on 2008 wages and ≥ 2 voids/night)1 – Economic value of productivity lost estimated at $61 billion/year – Estimated medical cost of nocturia-associated falls estimated at $1. 5 billion/year • European analysis (based on 2007 wages in EU-15 and ≥ 3 voids/night)2 – Economic value of productivity lost estimated at € 29 billion/year – Estimated medical cost of nocturia-associated hip fractures estimated at € 1 billion/year 1. 2. Holm-Larsen et al. J Urol 2010; 183: e 1. Van Kerrebroeck et al. Abstract 373 at ICS/IUGA 2010 21
Nocturia is a socio-economic burden • US analysis (based on 2008 wages and ≥ 2 voids/night)1 – Economic value of productivity lost estimated at $61 billion/year – Estimated medical cost of nocturia-associated falls estimated at $1. 5 billion/year • European analysis (based on 2007 wages in EU-15 and ≥ 3 voids/night)2 – Economic value of productivity lost estimated at € 29 billion/year – Estimated medical cost of nocturia-associated hip fractures estimated at € 1 billion/year 1. 2. Holm-Larsen et al. J Urol 2010; 183: e 1. Van Kerrebroeck et al. Abstract 373 at ICS/IUGA 2010 21
 In summary: nocturia (≥ 2 voids/night) is a very common condition and associated with multiple negative outcomes Consequently, underlying causes should be diagnosed and treated appropriately 22
In summary: nocturia (≥ 2 voids/night) is a very common condition and associated with multiple negative outcomes Consequently, underlying causes should be diagnosed and treated appropriately 22
 CAUSES AND TREATMENT OF NOCTURIA
CAUSES AND TREATMENT OF NOCTURIA
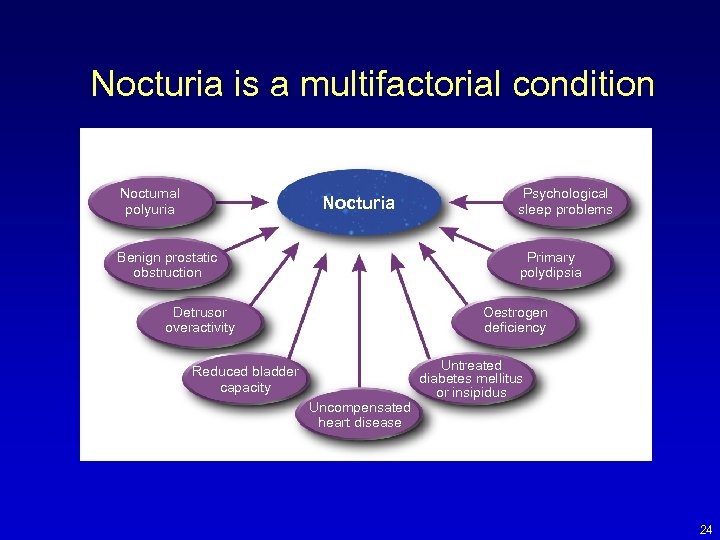 Nocturia is a multifactorial condition Nocturnal polyuria Nocturia Benign prostatic obstruction Psychological sleep problems Primary polydipsia Detrusor overactivity Oestrogen deficiency Reduced bladder capacity Uncompensated heart disease Untreated diabetes mellitus or insipidus 24
Nocturia is a multifactorial condition Nocturnal polyuria Nocturia Benign prostatic obstruction Psychological sleep problems Primary polydipsia Detrusor overactivity Oestrogen deficiency Reduced bladder capacity Uncompensated heart disease Untreated diabetes mellitus or insipidus 24
 Potential factors underlying nocturia Urological evaluation reveals: Nocturnal polyuria Definition: Nocturnal urine volume >20– 30% of total 24 -hour urinary volume (dependent on age) Urine production within normal limits; increased frequency, small voided volumes 24 -hour urinary output exceeding 40 m. L/kg body weight Possible causes: • Impaired circadian rhythm of AVP secretion • Congestive heart failure • Renal insufficiency • Excessive evening fluid/caffeine intake • Diuretic medication • Oestrogen deficiency • Sleep apnoea • Venous insufficiency • Oedema • Hypoalbuminemia • Overactive bladder • Bladder outlet obstruction (including benign prostatic enlargement) • Infection • Interstitial cystitis • Bladder hypersensitivity • Calculi • Cancer • Neurogenic detrusor overactivity (e. g. multiple sclerosis) • Poorly-controlled diabetes mellitus (type 1 or type 2) • Diabetes insipidus • Polydipsia Van Kerrebroeck P. Curr Opin Obstet Gynecol 2011; 23(5): 376 -85. Reduced nocturnal bladder capacity 24 -hour polyuria 25
Potential factors underlying nocturia Urological evaluation reveals: Nocturnal polyuria Definition: Nocturnal urine volume >20– 30% of total 24 -hour urinary volume (dependent on age) Urine production within normal limits; increased frequency, small voided volumes 24 -hour urinary output exceeding 40 m. L/kg body weight Possible causes: • Impaired circadian rhythm of AVP secretion • Congestive heart failure • Renal insufficiency • Excessive evening fluid/caffeine intake • Diuretic medication • Oestrogen deficiency • Sleep apnoea • Venous insufficiency • Oedema • Hypoalbuminemia • Overactive bladder • Bladder outlet obstruction (including benign prostatic enlargement) • Infection • Interstitial cystitis • Bladder hypersensitivity • Calculi • Cancer • Neurogenic detrusor overactivity (e. g. multiple sclerosis) • Poorly-controlled diabetes mellitus (type 1 or type 2) • Diabetes insipidus • Polydipsia Van Kerrebroeck P. Curr Opin Obstet Gynecol 2011; 23(5): 376 -85. Reduced nocturnal bladder capacity 24 -hour polyuria 25
 Nocturia: classification/aetiology by frequency–volume charts (FVC) • FVC/voiding diaries provide invaluable guidance. DDx: 1. NP (NUV >33% by ICS guideline criterion) • Krimpen study: proposes NUV cutpoint >90 ml/hr sleep 2. Decreased bladder capacity (global/night – distinction difficult) 3. Mixed (1+2) 4. Global polyuria (24 -hour output >40 ml/kg) 26
Nocturia: classification/aetiology by frequency–volume charts (FVC) • FVC/voiding diaries provide invaluable guidance. DDx: 1. NP (NUV >33% by ICS guideline criterion) • Krimpen study: proposes NUV cutpoint >90 ml/hr sleep 2. Decreased bladder capacity (global/night – distinction difficult) 3. Mixed (1+2) 4. Global polyuria (24 -hour output >40 ml/kg) 26
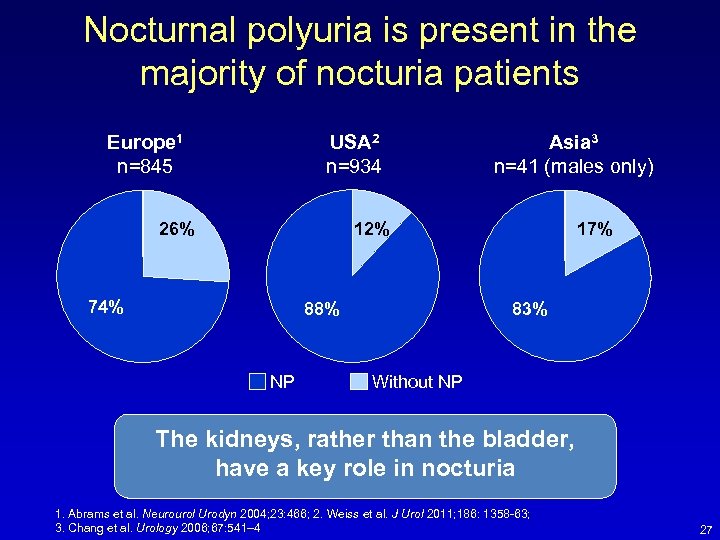 Nocturnal polyuria is present in the majority of nocturia patients USA 2 n=934 Europe 1 n=845 26% Asia 3 n=41 (males only) 12% 74% 88% NP 17% 83% Without NP The kidneys, rather than the bladder, have a key role in nocturia 1. Abrams et al. Neurourol Urodyn 2004; 23: 466; 2. Weiss et al. J Urol 2011; 186: 1358 -63; 3. Chang et al. Urology 2006; 67: 541– 4 27
Nocturnal polyuria is present in the majority of nocturia patients USA 2 n=934 Europe 1 n=845 26% Asia 3 n=41 (males only) 12% 74% 88% NP 17% 83% Without NP The kidneys, rather than the bladder, have a key role in nocturia 1. Abrams et al. Neurourol Urodyn 2004; 23: 466; 2. Weiss et al. J Urol 2011; 186: 1358 -63; 3. Chang et al. Urology 2006; 67: 541– 4 27
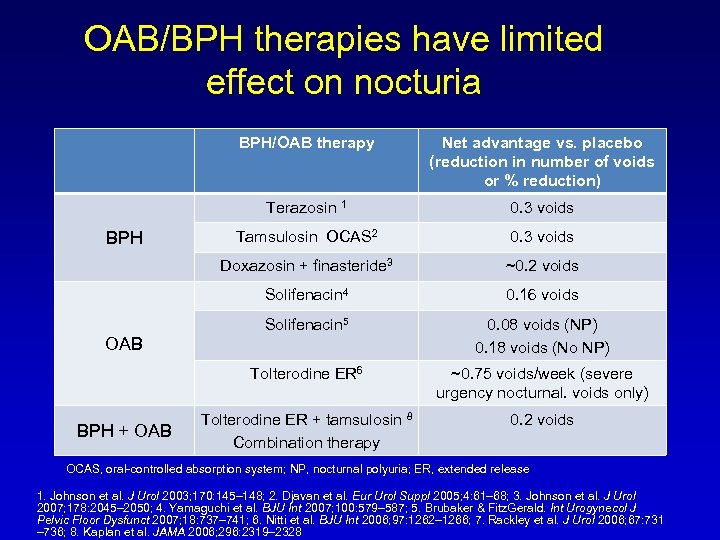 OAB/BPH therapies have limited effect on nocturia BPH/OAB therapy Terazosin 1 0. 3 voids Tamsulosin OCAS 2 0. 3 voids Doxazosin + finasteride 3 ~0. 2 voids Solifenacin 4 0. 16 voids Solifenacin 5 0. 08 voids (NP) 0. 18 voids (No NP) Tolterodine ER 6 BPH Net advantage vs. placebo (reduction in number of voids or % reduction) ~0. 75 voids/week (severe urgency nocturnal. voids only) Tolterodine ER + tamsulosin 8 Combination therapy 0. 2 voids OAB BPH + OAB OCAS, oral-controlled absorption system; NP, nocturnal polyuria; ER, extended release 1. Johnson et al. J Urol 2003; 170: 145– 148; 2. Djavan et al. Eur Urol Suppl 2005; 4: 61– 68; 3. Johnson et al. J Urol 2007; 178: 2045– 2050; 4. Yamaguchi et al. BJU Int 2007; 100: 579– 587; 5. Brubaker & Fitz. Gerald. Int Urogynecol J Pelvic Floor Dysfunct 2007; 18: 737– 741; 6. Nitti et al. BJU Int 2006; 97: 1262– 1266; 7. Rackley et al. J Urol 2006; 67: 731 – 736; 8. Kaplan et al. JAMA 2006; 296: 2319– 2328
OAB/BPH therapies have limited effect on nocturia BPH/OAB therapy Terazosin 1 0. 3 voids Tamsulosin OCAS 2 0. 3 voids Doxazosin + finasteride 3 ~0. 2 voids Solifenacin 4 0. 16 voids Solifenacin 5 0. 08 voids (NP) 0. 18 voids (No NP) Tolterodine ER 6 BPH Net advantage vs. placebo (reduction in number of voids or % reduction) ~0. 75 voids/week (severe urgency nocturnal. voids only) Tolterodine ER + tamsulosin 8 Combination therapy 0. 2 voids OAB BPH + OAB OCAS, oral-controlled absorption system; NP, nocturnal polyuria; ER, extended release 1. Johnson et al. J Urol 2003; 170: 145– 148; 2. Djavan et al. Eur Urol Suppl 2005; 4: 61– 68; 3. Johnson et al. J Urol 2007; 178: 2045– 2050; 4. Yamaguchi et al. BJU Int 2007; 100: 579– 587; 5. Brubaker & Fitz. Gerald. Int Urogynecol J Pelvic Floor Dysfunct 2007; 18: 737– 741; 6. Nitti et al. BJU Int 2006; 97: 1262– 1266; 7. Rackley et al. J Urol 2006; 67: 731 – 736; 8. Kaplan et al. JAMA 2006; 296: 2319– 2328
 Desmopressin: mechanism of action • Desmopressin is a selective V 2 -receptor agonist: – Retains the antidiuretic properties of vasopressin 1 – Lacks the unwanted pressor activity of vasopressin • When bound to V 2 -receptors in the kidney, it: – Increases tubular water permeability – Enhances water reabsorption – Extracellular fluid becomes more dilute – Urine becomes more concentrated 2 1. Vilhardt H. Drug Investigation 1990; 2(Suppl. 5): 2– 8; 2. Hammer M & Vilhardt H. J Pharmacol Exp Ther 1985; 234: 754– 60. 29
Desmopressin: mechanism of action • Desmopressin is a selective V 2 -receptor agonist: – Retains the antidiuretic properties of vasopressin 1 – Lacks the unwanted pressor activity of vasopressin • When bound to V 2 -receptors in the kidney, it: – Increases tubular water permeability – Enhances water reabsorption – Extracellular fluid becomes more dilute – Urine becomes more concentrated 2 1. Vilhardt H. Drug Investigation 1990; 2(Suppl. 5): 2– 8; 2. Hammer M & Vilhardt H. J Pharmacol Exp Ther 1985; 234: 754– 60. 29
 Desmopressin: key recommendations • • ICI: Grade A (level 1)1, 2 EAU: Grade A (level 1 b)3, 4, 5. 1. In Abrams et al. (eds) Incontinence; 4 th International Consultation on Incontinence. Paris: Health Publication Ltd, 2009. Available at: p: //www. icsoffice. org/Publications/ICI_4/files-book/Comite-8. pdf 2. Abrams et al. Neurourol Urodyn 2010 ; 29 : 213– 40 3. Schröder et al. Guidelines on Urinary Incontinence. © European Association of Urology 2010. Available at: http: //www. uroweb. org/gls/pdf/16_Urinary_Incontinence%202010. pdf 4. Thüroff et al. EAU Guidelines on Urinary Incontinence. Eur Urol 2011; 59: 387 -400 5. Oelke et al. Guidelines on the Treatment of Non-neurogenic Male LUTS. © European Association of Urology 2011. Available at: http: //www. uroweb. org/gls/pdf/12_Male_LUTS. pdf 30
Desmopressin: key recommendations • • ICI: Grade A (level 1)1, 2 EAU: Grade A (level 1 b)3, 4, 5. 1. In Abrams et al. (eds) Incontinence; 4 th International Consultation on Incontinence. Paris: Health Publication Ltd, 2009. Available at: p: //www. icsoffice. org/Publications/ICI_4/files-book/Comite-8. pdf 2. Abrams et al. Neurourol Urodyn 2010 ; 29 : 213– 40 3. Schröder et al. Guidelines on Urinary Incontinence. © European Association of Urology 2010. Available at: http: //www. uroweb. org/gls/pdf/16_Urinary_Incontinence%202010. pdf 4. Thüroff et al. EAU Guidelines on Urinary Incontinence. Eur Urol 2011; 59: 387 -400 5. Oelke et al. Guidelines on the Treatment of Non-neurogenic Male LUTS. © European Association of Urology 2011. Available at: http: //www. uroweb. org/gls/pdf/12_Male_LUTS. pdf 30
 Summary of key desmopressin data • • • Nocturia patients experience significant and clinically meaningful reduction in night-time voiding and prolongation of initial sleep period with short- and long-term desmopressin treatment 1– 5 Desmopressin is well tolerated in the short- and long-term; cessation causes nocturia severity to revert to baseline at 1 year 1– 5 Both patient Qo. L and productivity at work improve with desmopressin treatment 4, 6 Data is available for conventional tablets and the newer melt formulation, which has higher bioavailability and can be taken without water Gender-specific and lower dosing with the new formulation (especially in women) may further reduce the low but important risk of hyponatremia without reducing efficacy 7 1. Lose et al. Am J Obstet Gynecol 2003; 189: 1106– 1113; 2. Mattiasson et al. BJU Int 2002; 89: 855– 862; 3. Lose et al. J Urol 2004; 172: 1021– 1025; 4. van Kerrebroeck et al. Eur Urol 2007; 52: 221– 229; 5. Weiss et al. Abstract 198/ ICS 2010. 6. Daneshgari et al. Abstract 212/ ICS 2010. 7. Juul et al. Am J Physiol Renal Physiol 2011; 300(5): F 1116 -22 31
Summary of key desmopressin data • • • Nocturia patients experience significant and clinically meaningful reduction in night-time voiding and prolongation of initial sleep period with short- and long-term desmopressin treatment 1– 5 Desmopressin is well tolerated in the short- and long-term; cessation causes nocturia severity to revert to baseline at 1 year 1– 5 Both patient Qo. L and productivity at work improve with desmopressin treatment 4, 6 Data is available for conventional tablets and the newer melt formulation, which has higher bioavailability and can be taken without water Gender-specific and lower dosing with the new formulation (especially in women) may further reduce the low but important risk of hyponatremia without reducing efficacy 7 1. Lose et al. Am J Obstet Gynecol 2003; 189: 1106– 1113; 2. Mattiasson et al. BJU Int 2002; 89: 855– 862; 3. Lose et al. J Urol 2004; 172: 1021– 1025; 4. van Kerrebroeck et al. Eur Urol 2007; 52: 221– 229; 5. Weiss et al. Abstract 198/ ICS 2010. 6. Daneshgari et al. Abstract 212/ ICS 2010. 7. Juul et al. Am J Physiol Renal Physiol 2011; 300(5): F 1116 -22 31
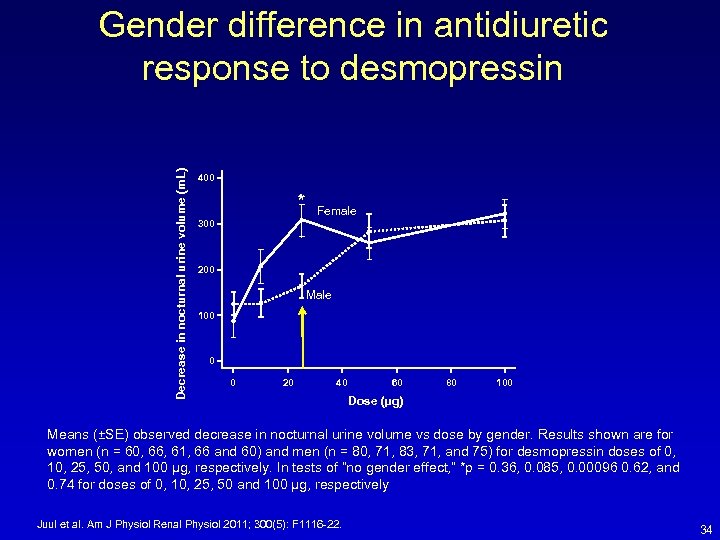 Decrease in nocturnal urine volume (m. L) Gender difference in antidiuretic response to desmopressin 400 * Female 300 200 Male 100 0 0 20 40 60 80 100 Dose (µg) Means (±SE) observed decrease in nocturnal urine volume vs dose by gender. Results shown are for women (n = 60, 66, 61, 66 and 60) and men (n = 80, 71, 83, 71, and 75) for desmopressin doses of 0, 10, 25, 50, and 100 µg, respectively. In tests of “no gender effect, ” *p = 0. 36, 0. 085, 0. 00096 0. 62, and 0. 74 for doses of 0, 10, 25, 50 and 100 µg, respectively Juul et al. Am J Physiol Renal Physiol 2011; 300(5): F 1116 -22. 34
Decrease in nocturnal urine volume (m. L) Gender difference in antidiuretic response to desmopressin 400 * Female 300 200 Male 100 0 0 20 40 60 80 100 Dose (µg) Means (±SE) observed decrease in nocturnal urine volume vs dose by gender. Results shown are for women (n = 60, 66, 61, 66 and 60) and men (n = 80, 71, 83, 71, and 75) for desmopressin doses of 0, 10, 25, 50, and 100 µg, respectively. In tests of “no gender effect, ” *p = 0. 36, 0. 085, 0. 00096 0. 62, and 0. 74 for doses of 0, 10, 25, 50 and 100 µg, respectively Juul et al. Am J Physiol Renal Physiol 2011; 300(5): F 1116 -22. 34
 Example of a potential simple algorithm to differentiate night-time urination LUTS / NOCTURIA • Exclude and treat non-urological causes (such as cardiac, OSA) • Lifestyle changes Daytime LUTS (predominantly daytime symptoms) OAB anticholinergic • • BPO Mixed LUTS (mixed daytime and night-time symptoms) Night-time LUTS (predominantly night-time symptoms) BPO and OAB Address daytime symptoms • anticholinergic • a 1 -blocker • combinations a 1 -blocker + a 1 -blocker anticholinergic 5 -a RI combination outlet reducing surgery Persistent night-time symptoms desmopressin LUTS, lower urinary tract symptoms; BPO, benign prostatic obstruction; 5 -a RI, 5 -alpha reductase inhibitor 35
Example of a potential simple algorithm to differentiate night-time urination LUTS / NOCTURIA • Exclude and treat non-urological causes (such as cardiac, OSA) • Lifestyle changes Daytime LUTS (predominantly daytime symptoms) OAB anticholinergic • • BPO Mixed LUTS (mixed daytime and night-time symptoms) Night-time LUTS (predominantly night-time symptoms) BPO and OAB Address daytime symptoms • anticholinergic • a 1 -blocker • combinations a 1 -blocker + a 1 -blocker anticholinergic 5 -a RI combination outlet reducing surgery Persistent night-time symptoms desmopressin LUTS, lower urinary tract symptoms; BPO, benign prostatic obstruction; 5 -a RI, 5 -alpha reductase inhibitor 35
 To take away… • • Nocturia is highly prevalent and a leading cause of sleep disruption • Diagnosis and treatment must be differentiated between dayand night-time LUTS. Nocturia is caused by NP (alone or in combination with OAB/BPO) in a majority of cases; diagnosing NP is simple, and desmopressin the Grade A recommended pharmacologic intervention • • Two episodes of nocturia constitute meaningful nocturia • Left untreated, nocturia affects productivity at work and represents a significant socio-economic burden Many studies have demonstrated a multifactorial aetiology for nocturia Nocturia affects sleep and quality of life and is associated with an increased risk of morbidity and mortality 36
To take away… • • Nocturia is highly prevalent and a leading cause of sleep disruption • Diagnosis and treatment must be differentiated between dayand night-time LUTS. Nocturia is caused by NP (alone or in combination with OAB/BPO) in a majority of cases; diagnosing NP is simple, and desmopressin the Grade A recommended pharmacologic intervention • • Two episodes of nocturia constitute meaningful nocturia • Left untreated, nocturia affects productivity at work and represents a significant socio-economic burden Many studies have demonstrated a multifactorial aetiology for nocturia Nocturia affects sleep and quality of life and is associated with an increased risk of morbidity and mortality 36
 Challenges… • • Epidemiology: the key data are there Causes and targeted therapies: – Differentiating day-time vs. night-time LUTS (diagnosis and treatment) – Differentiating patients? – Treatment irrespective of bother? • Desmopressin – Hyponatraemia: explore risk populations – Doses: clear communication • Education – NP, consequences in younger patients (eg bother and mortality) – Get nocturia/desmopressin into more guidelines (eg. AUA) 37
Challenges… • • Epidemiology: the key data are there Causes and targeted therapies: – Differentiating day-time vs. night-time LUTS (diagnosis and treatment) – Differentiating patients? – Treatment irrespective of bother? • Desmopressin – Hyponatraemia: explore risk populations – Doses: clear communication • Education – NP, consequences in younger patients (eg bother and mortality) – Get nocturia/desmopressin into more guidelines (eg. AUA) 37
 Nocturia: discussion 38
Nocturia: discussion 38


