cae2e442a74ea1083b873b0f4a29e8ac.ppt
- Количество слайдов: 44
 Social and Familial Influences on Chronic Disease Management among African Americans Carmen D. Samuel-Hodge, Ph. D, MS, RD April 2, 2007
Social and Familial Influences on Chronic Disease Management among African Americans Carmen D. Samuel-Hodge, Ph. D, MS, RD April 2, 2007
 Today’s Presentation n n Context – Focus on type 2 diabetes Social and Familial Factors Social Relationships n Family Interactions n Social Stressors n n Implications for Self-Management Interventions
Today’s Presentation n n Context – Focus on type 2 diabetes Social and Familial Factors Social Relationships n Family Interactions n Social Stressors n n Implications for Self-Management Interventions
 Wicked Problems that are illusive or difficult to pin down and influenced by a constellation of complex social and political factors Source: Rittel HJ, Webber MM: dilemmas in a general theory of planning. Policy Sci 4: 155 -169, 1973 Cited in: Kreuter MW et al. , Health Educ Behav 2004; 31(4): 441 -454
Wicked Problems that are illusive or difficult to pin down and influenced by a constellation of complex social and political factors Source: Rittel HJ, Webber MM: dilemmas in a general theory of planning. Policy Sci 4: 155 -169, 1973 Cited in: Kreuter MW et al. , Health Educ Behav 2004; 31(4): 441 -454
 Who’s Living with Diabetes? n 20. 8 million people – 7. 0% of the US population (all ages) n n n Age > 20 years: 9. 6% Age 60 and older: 20. 9% Diagnosed – 14. 6 million Undiagnosed 6. 2 million Incidence (new cases/year): 1. 5 million people > 20 years Source: American Diabetes Association, 2005 estimates
Who’s Living with Diabetes? n 20. 8 million people – 7. 0% of the US population (all ages) n n n Age > 20 years: 9. 6% Age 60 and older: 20. 9% Diagnosed – 14. 6 million Undiagnosed 6. 2 million Incidence (new cases/year): 1. 5 million people > 20 years Source: American Diabetes Association, 2005 estimates
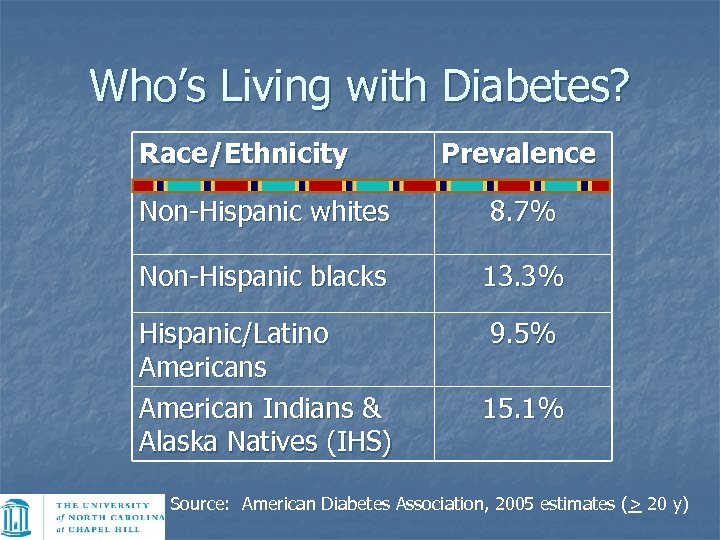 Who’s Living with Diabetes? Race/Ethnicity Prevalence Non-Hispanic whites 8. 7% Non-Hispanic blacks 13. 3% Hispanic/Latino Americans American Indians & Alaska Natives (IHS) 9. 5% 15. 1% Source: American Diabetes Association, 2005 estimates (> 20 y)
Who’s Living with Diabetes? Race/Ethnicity Prevalence Non-Hispanic whites 8. 7% Non-Hispanic blacks 13. 3% Hispanic/Latino Americans American Indians & Alaska Natives (IHS) 9. 5% 15. 1% Source: American Diabetes Association, 2005 estimates (> 20 y)
 African Americans n n n 1. 8 times more likely to have diabetes than non-Hispanic whites African American and other minority women have 2 -4 times higher prevalence Compared to non-Hispanic whites, African Americans suffer disproportionately: n n n Diabetes-related blindness (2 times more likely) Lower limb amputations (1. 5 -2. 5 times) Kidney failure (2. 6 -5. 6 times)
African Americans n n n 1. 8 times more likely to have diabetes than non-Hispanic whites African American and other minority women have 2 -4 times higher prevalence Compared to non-Hispanic whites, African Americans suffer disproportionately: n n n Diabetes-related blindness (2 times more likely) Lower limb amputations (1. 5 -2. 5 times) Kidney failure (2. 6 -5. 6 times)
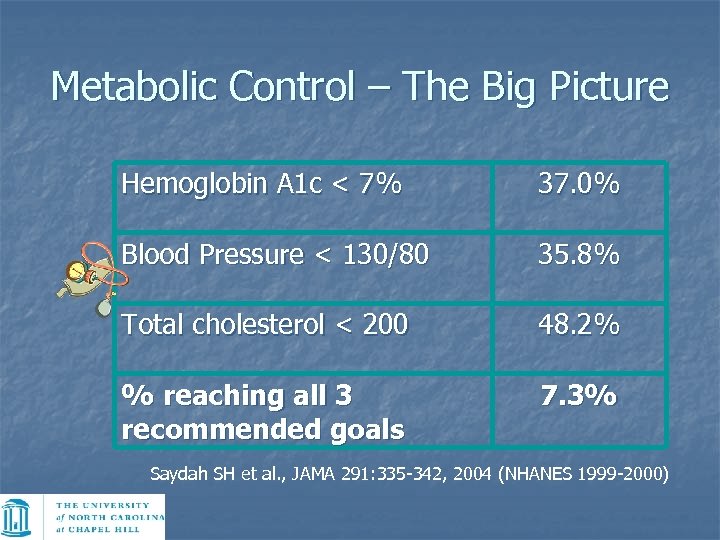 Metabolic Control – The Big Picture Hemoglobin A 1 c < 7% 37. 0% Blood Pressure < 130/80 35. 8% Total cholesterol < 200 48. 2% % reaching all 3 recommended goals 7. 3% Saydah SH et al. , JAMA 291: 335 -342, 2004 (NHANES 1999 -2000)
Metabolic Control – The Big Picture Hemoglobin A 1 c < 7% 37. 0% Blood Pressure < 130/80 35. 8% Total cholesterol < 200 48. 2% % reaching all 3 recommended goals 7. 3% Saydah SH et al. , JAMA 291: 335 -342, 2004 (NHANES 1999 -2000)
 Lifestyle Behaviors Physical Activity n Recommended – > 5 episodes/week n n About 70% do not meet recommended levels of activity associated with income and education Dietary Behavior n Almost 2/3 consumed >30% daily calories from fat; > 10% saturated fat n 62% ate < 5 servings of fruits/ vegetables per day Nelson KM, et al. , Diabetes Care 25: 1722 -1728, 2002
Lifestyle Behaviors Physical Activity n Recommended – > 5 episodes/week n n About 70% do not meet recommended levels of activity associated with income and education Dietary Behavior n Almost 2/3 consumed >30% daily calories from fat; > 10% saturated fat n 62% ate < 5 servings of fruits/ vegetables per day Nelson KM, et al. , Diabetes Care 25: 1722 -1728, 2002
 Wickedness of the Problem n Factors associated with disease management n Access to care n Quality of care n Knowledge/skill deficits n Beliefs about diabetes (Psychological factors) n Socio-cultural factors n Self-management behaviors – diet, physical activity, blood glucose monitoring, foot care, etc.
Wickedness of the Problem n Factors associated with disease management n Access to care n Quality of care n Knowledge/skill deficits n Beliefs about diabetes (Psychological factors) n Socio-cultural factors n Self-management behaviors – diet, physical activity, blood glucose monitoring, foot care, etc.
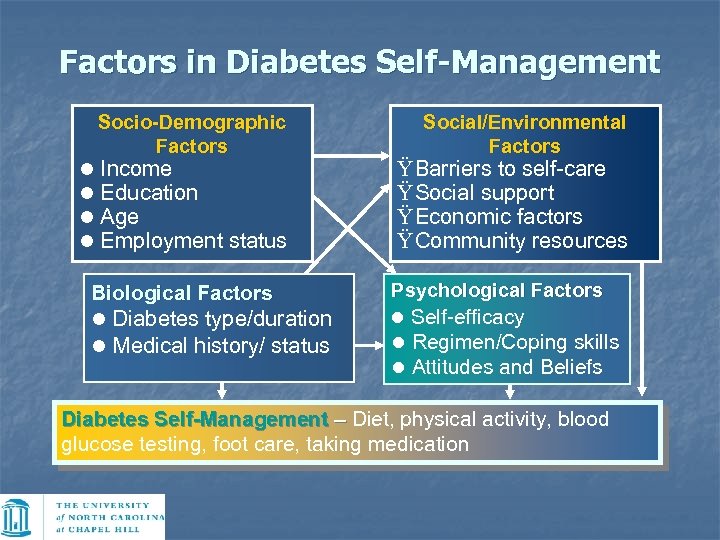 Factors in Diabetes Self-Management Socio-Demographic Factors l l Income Education Age Employment status Biological Factors l Diabetes type/duration l Medical history/ status Social/Environmental Factors Ÿ Barriers to self-care Ÿ Social support Ÿ Economic factors Ÿ Community resources Psychological Factors l Self-efficacy l Regimen/Coping skills l Attitudes and Beliefs Diabetes Self-Management – Diet, physical activity, blood glucose testing, foot care, taking medication
Factors in Diabetes Self-Management Socio-Demographic Factors l l Income Education Age Employment status Biological Factors l Diabetes type/duration l Medical history/ status Social/Environmental Factors Ÿ Barriers to self-care Ÿ Social support Ÿ Economic factors Ÿ Community resources Psychological Factors l Self-efficacy l Regimen/Coping skills l Attitudes and Beliefs Diabetes Self-Management – Diet, physical activity, blood glucose testing, foot care, taking medication
 Ecological Model of Health Behavior Community & Policy Culture, System, Group Family, Friends, Small Group Individual Biological Psychological Fisher EB et al. , Diabetes Care 25: 599 -600, 2002
Ecological Model of Health Behavior Community & Policy Culture, System, Group Family, Friends, Small Group Individual Biological Psychological Fisher EB et al. , Diabetes Care 25: 599 -600, 2002
 Social and Familial Influences
Social and Familial Influences
 Living with Diabetes… (What People Say)
Living with Diabetes… (What People Say)
 Qualitative Research Influences on day-to-day selfmanagement of type 2 diabetes among African American women* *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
Qualitative Research Influences on day-to-day selfmanagement of type 2 diabetes among African American women* *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
 Qualitative Findings Dominant Theme 1 n Spirituality as an important factor in general health, disease adjustment, and coping “I’ve had 3 heart attacks. I just ask God to give me the strength to do the things that I have to do. Sometimes I think if I would stop and sit down long enough, I would die. But I’m thankful for having God on my side. ” *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
Qualitative Findings Dominant Theme 1 n Spirituality as an important factor in general health, disease adjustment, and coping “I’ve had 3 heart attacks. I just ask God to give me the strength to do the things that I have to do. Sometimes I think if I would stop and sit down long enough, I would die. But I’m thankful for having God on my side. ” *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
 Qualitative Findings Dominant Theme 2 n General life stress and multi-caregiving responsibilities interfering with disease management “What causes me a lot of problem, gets my nerves out of shape and cause my diabetes to flare up [is that] I live around family. And they come to my house, you know …when they get off the school bus, here they come. When they get out from work, here they come. ” *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
Qualitative Findings Dominant Theme 2 n General life stress and multi-caregiving responsibilities interfering with disease management “What causes me a lot of problem, gets my nerves out of shape and cause my diabetes to flare up [is that] I live around family. And they come to my house, you know …when they get off the school bus, here they come. When they get out from work, here they come. ” *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
 Qualitative Findings Dominant Theme 3 n Impact of diabetes manifested in feelings of dietary deprivation, physical and emotional “tiredness”, “worry”, and fear of complications” “When I think about the people that … already have diabetes and they lose their limbs, you know. Sometimes I get kind of numb – my legs. And I’m worried am I next. It bears on your mind a lot. ” *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
Qualitative Findings Dominant Theme 3 n Impact of diabetes manifested in feelings of dietary deprivation, physical and emotional “tiredness”, “worry”, and fear of complications” “When I think about the people that … already have diabetes and they lose their limbs, you know. Sometimes I get kind of numb – my legs. And I’m worried am I next. It bears on your mind a lot. ” *Samuel-Hodge et al. , Diabetes Care 23: 928 -933, 2000
 Similar Views From Other Populations of Color n Native Americans “I just want to say that diabetes is a real emotional issue. My dad was diabetic, his brother was, his sister was and she had an amputation. As a result, we carry a lot of pain. ” Struthers R et al. , Qualitative Health Res 13: 1094 -1115, 2003
Similar Views From Other Populations of Color n Native Americans “I just want to say that diabetes is a real emotional issue. My dad was diabetic, his brother was, his sister was and she had an amputation. As a result, we carry a lot of pain. ” Struthers R et al. , Qualitative Health Res 13: 1094 -1115, 2003
 Similar Views From Other Populations of Color n Native Americans (on ‘diabetes prevention’) “Some workers from IHS tell us all you have to do is exercise and eat right. Eat fresh fruits and vegetables … Where do they think they are? You know it is totally unrealistic because our reservation living conditions are sad, our families are pitiful … It makes me angry to know they can say that to us in English, and you try to tell that to the person that has 12 kids to take care of, probably no vehicle, limited income … we have all these challenges that we face every day. So I’m thinking, ‘Get real here’. ” Struthers R et al. , Qualitative Health Res 13: 1094 -1115, 2003
Similar Views From Other Populations of Color n Native Americans (on ‘diabetes prevention’) “Some workers from IHS tell us all you have to do is exercise and eat right. Eat fresh fruits and vegetables … Where do they think they are? You know it is totally unrealistic because our reservation living conditions are sad, our families are pitiful … It makes me angry to know they can say that to us in English, and you try to tell that to the person that has 12 kids to take care of, probably no vehicle, limited income … we have all these challenges that we face every day. So I’m thinking, ‘Get real here’. ” Struthers R et al. , Qualitative Health Res 13: 1094 -1115, 2003
 How Do We Quantify These Views?
How Do We Quantify These Views?
 Measurement Instruments n n Strong Ties/Close Contacts Social Barriers Perceived Diabetes & Dietary Competence (PDDC) Multi-Caregiver Role (Family)
Measurement Instruments n n Strong Ties/Close Contacts Social Barriers Perceived Diabetes & Dietary Competence (PDDC) Multi-Caregiver Role (Family)
 Social Contact / Strong Ties 4 items; 4 -point frequency responses 1. How often are you bothered by not having a close companion? 2. How often are you bothered by not seeing enough of people you feel close to? 3. How often are you bothered by not having enough close friends? 4. How often are you bothered by not having someone who shows you love and affection? n How many relatives do you have that you feel close to? Dean AE and Lin N, J Nervous Mental Dis 165: 403 -417, 1977
Social Contact / Strong Ties 4 items; 4 -point frequency responses 1. How often are you bothered by not having a close companion? 2. How often are you bothered by not seeing enough of people you feel close to? 3. How often are you bothered by not having enough close friends? 4. How often are you bothered by not having someone who shows you love and affection? n How many relatives do you have that you feel close to? Dean AE and Lin N, J Nervous Mental Dis 165: 403 -417, 1977
 Social Support for Diabetes n n Diabetes Family Behavior Checklist II – adapted Frequency of 12 behaviors (praise, nag, help, etc. ) Helpfulness of behaviors Score = Cross product (frequency X helpfulness) Mc. Caul et al. , Med Care 25: 868 -881, 1987
Social Support for Diabetes n n Diabetes Family Behavior Checklist II – adapted Frequency of 12 behaviors (praise, nag, help, etc. ) Helpfulness of behaviors Score = Cross product (frequency X helpfulness) Mc. Caul et al. , Med Care 25: 868 -881, 1987
 Social Barriers n n 5 items ; 4 -point Likert scale responses Measure problems related to Money (finances) n Street crime n Housing n Family care-giving responsibilities n * Hill-Briggs F. et al. , J Gen Intern Med 2002; 17: 412 -19
Social Barriers n n 5 items ; 4 -point Likert scale responses Measure problems related to Money (finances) n Street crime n Housing n Family care-giving responsibilities n * Hill-Briggs F. et al. , J Gen Intern Med 2002; 17: 412 -19
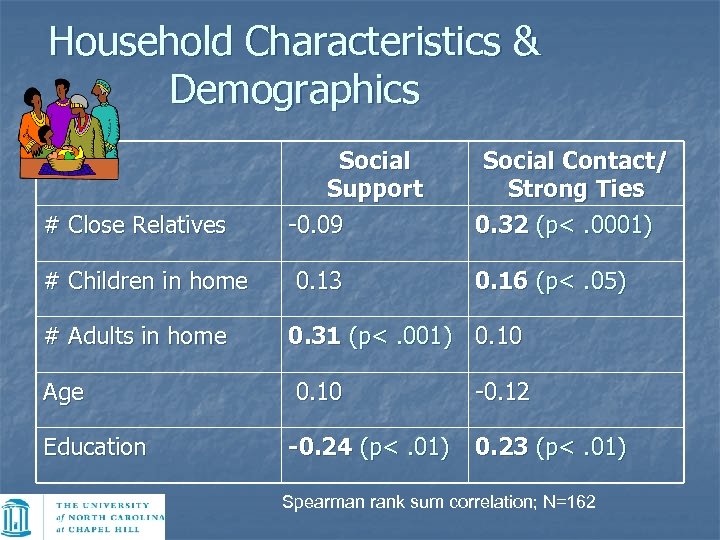 Household Characteristics & Demographics # Close Relatives # Children in home # Adults in home Age Education Social Support -0. 09 0. 13 Social Contact/ Strong Ties 0. 32 (p<. 0001) 0. 16 (p<. 05) 0. 31 (p<. 001) 0. 10 -0. 24 (p<. 01) -0. 12 0. 23 (p<. 01) Spearman rank sum correlation; N=162
Household Characteristics & Demographics # Close Relatives # Children in home # Adults in home Age Education Social Support -0. 09 0. 13 Social Contact/ Strong Ties 0. 32 (p<. 0001) 0. 16 (p<. 05) 0. 31 (p<. 001) 0. 10 -0. 24 (p<. 01) -0. 12 0. 23 (p<. 01) Spearman rank sum correlation; N=162
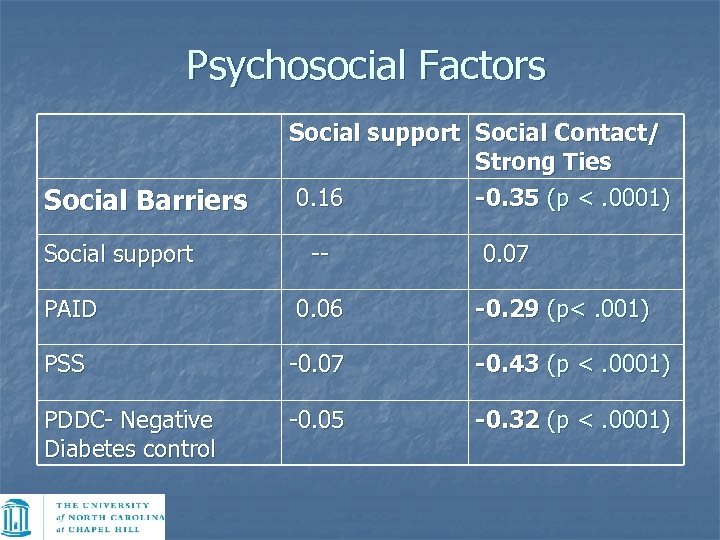 Psychosocial Factors Social Barriers Social support Social Contact/ Strong Ties 0. 16 -0. 35 (p <. 0001) -- 0. 07 PAID 0. 06 -0. 29 (p<. 001) PSS -0. 07 -0. 43 (p <. 0001) PDDC- Negative Diabetes control -0. 05 -0. 32 (p <. 0001)
Psychosocial Factors Social Barriers Social support Social Contact/ Strong Ties 0. 16 -0. 35 (p <. 0001) -- 0. 07 PAID 0. 06 -0. 29 (p<. 001) PSS -0. 07 -0. 43 (p <. 0001) PDDC- Negative Diabetes control -0. 05 -0. 32 (p <. 0001)
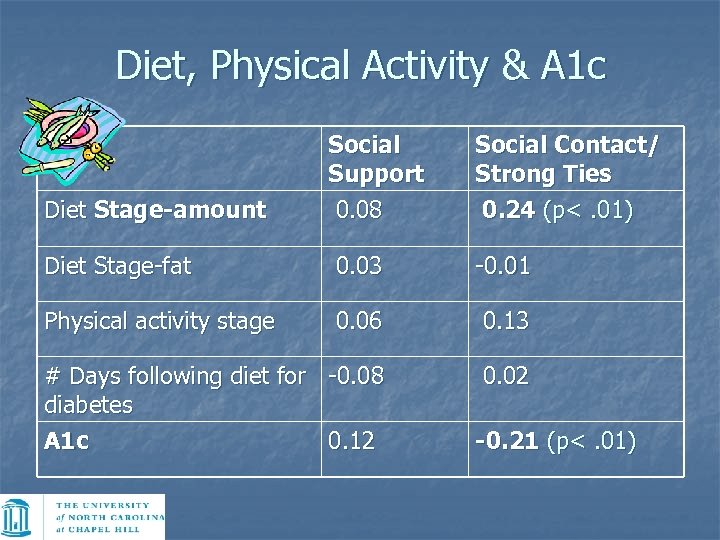 Diet, Physical Activity & A 1 c Diet Stage-amount Social Support 0. 08 Social Contact/ Strong Ties 0. 24 (p<. 01) Diet Stage-fat 0. 03 -0. 01 Physical activity stage 0. 06 0. 13 # Days following diet for -0. 08 diabetes A 1 c 0. 12 0. 02 -0. 21 (p<. 01)
Diet, Physical Activity & A 1 c Diet Stage-amount Social Support 0. 08 Social Contact/ Strong Ties 0. 24 (p<. 01) Diet Stage-fat 0. 03 -0. 01 Physical activity stage 0. 06 0. 13 # Days following diet for -0. 08 diabetes A 1 c 0. 12 0. 02 -0. 21 (p<. 01)
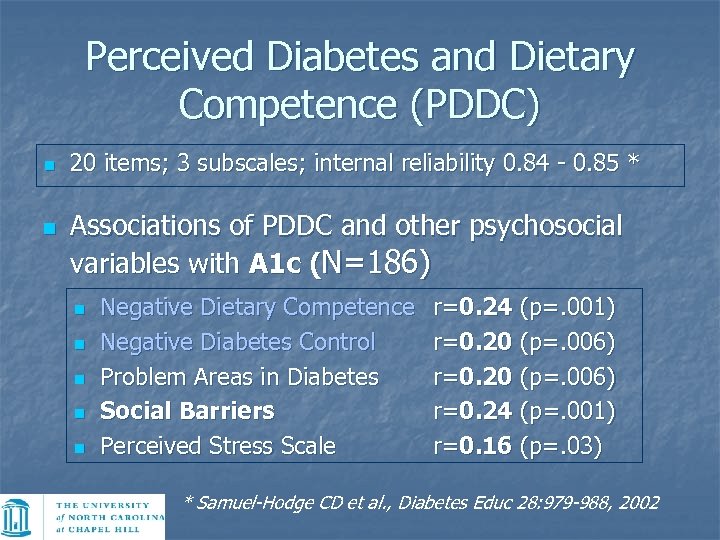 Perceived Diabetes and Dietary Competence (PDDC) n n 20 items; 3 subscales; internal reliability 0. 84 - 0. 85 * Associations of PDDC and other psychosocial variables with A 1 c (N=186) n n n Negative Dietary Competence Negative Diabetes Control Problem Areas in Diabetes Social Barriers Perceived Stress Scale r=0. 24 (p=. 001) r=0. 20 (p=. 006) r=0. 24 (p=. 001) r=0. 16 (p=. 03) * Samuel-Hodge CD et al. , Diabetes Educ 28: 979 -988, 2002
Perceived Diabetes and Dietary Competence (PDDC) n n 20 items; 3 subscales; internal reliability 0. 84 - 0. 85 * Associations of PDDC and other psychosocial variables with A 1 c (N=186) n n n Negative Dietary Competence Negative Diabetes Control Problem Areas in Diabetes Social Barriers Perceived Stress Scale r=0. 24 (p=. 001) r=0. 20 (p=. 006) r=0. 24 (p=. 001) r=0. 16 (p=. 03) * Samuel-Hodge CD et al. , Diabetes Educ 28: 979 -988, 2002
 In Summary… n n n Social barriers were associated with measures of metabolic control (A 1 c) and quality of social relationships (and HRQOL) Strong ties / social contacts relate to A 1 c and dietary behaviors; no relationship with social support The relationship between social relationships and disease management is complex.
In Summary… n n n Social barriers were associated with measures of metabolic control (A 1 c) and quality of social relationships (and HRQOL) Strong ties / social contacts relate to A 1 c and dietary behaviors; no relationship with social support The relationship between social relationships and disease management is complex.
 Familial Multiple Care-giving Roles n 12 items; 2 subscales; internal reliability 0. 72 -0. 76 n Sample items: n n n Taking care of family and friends interferes with caring for myself. Being available for family and friends is important to me. It’s hard to say “no” when friends and family come to me for help. Samuel-Hodge CD, et al. , Ethn Dis 2005; 15: 436 -443
Familial Multiple Care-giving Roles n 12 items; 2 subscales; internal reliability 0. 72 -0. 76 n Sample items: n n n Taking care of family and friends interferes with caring for myself. Being available for family and friends is important to me. It’s hard to say “no” when friends and family come to me for help. Samuel-Hodge CD, et al. , Ethn Dis 2005; 15: 436 -443
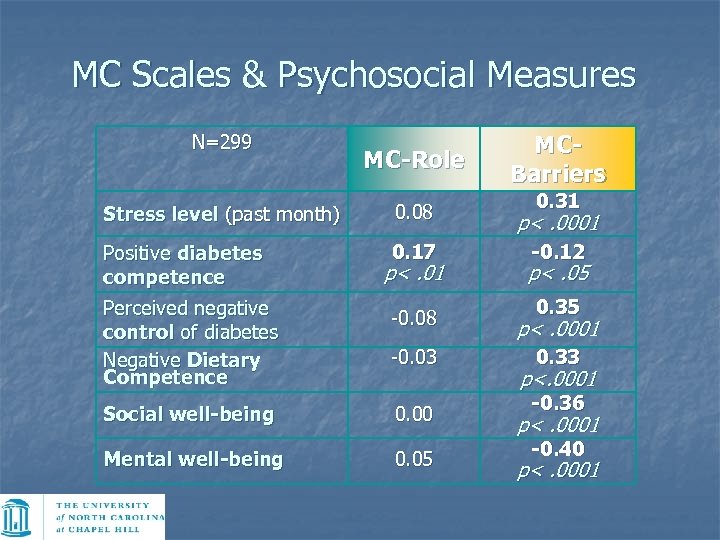 MC Scales & Psychosocial Measures N=299 MC-Role MCBarriers 0. 31 Stress level (past month) 0. 08 p<. 0001 Positive diabetes competence 0. 17 -0. 12 p<. 01 p<. 05 0. 35 Perceived negative control of diabetes Negative Dietary Competence -0. 08 p<. 0001 -0. 03 0. 33 Social well-being 0. 00 Mental well-being 0. 05 p<. 0001 -0. 36 p<. 0001 -0. 40 p<. 0001
MC Scales & Psychosocial Measures N=299 MC-Role MCBarriers 0. 31 Stress level (past month) 0. 08 p<. 0001 Positive diabetes competence 0. 17 -0. 12 p<. 01 p<. 05 0. 35 Perceived negative control of diabetes Negative Dietary Competence -0. 08 p<. 0001 -0. 03 0. 33 Social well-being 0. 00 Mental well-being 0. 05 p<. 0001 -0. 36 p<. 0001 -0. 40 p<. 0001
 Relationship with Self-Care Behaviors Comparison of means* (n=298) n n Women who reported they were not following a diet for diabetes also reported more people who regularly depend on them for help/support (p<. 05) No other significant findings with diet or PA
Relationship with Self-Care Behaviors Comparison of means* (n=298) n n Women who reported they were not following a diet for diabetes also reported more people who regularly depend on them for help/support (p<. 05) No other significant findings with diet or PA
 Multiple Care-giving and Family In summary … n Multiple care-giving role barriers were positively associated with: n n Number of children in the home Number of adults in the home No association between care-giving barriers and the number of people who are regularly provided with help or support Barriers associated with dietary behaviors
Multiple Care-giving and Family In summary … n Multiple care-giving role barriers were positively associated with: n n Number of children in the home Number of adults in the home No association between care-giving barriers and the number of people who are regularly provided with help or support Barriers associated with dietary behaviors
 In Summary… Is there more stress/strain when the number of people who are provided with help/support increases? n While the number of people helped/supported was not associated with MC-barriers, it was associated with stress level, and negative perceptions of dietary competence and diabetes control
In Summary… Is there more stress/strain when the number of people who are provided with help/support increases? n While the number of people helped/supported was not associated with MC-barriers, it was associated with stress level, and negative perceptions of dietary competence and diabetes control
 In Summary… Difficulty saying ‘no’ to family and friends seems to be related to many negative psychosocial outcomes n n Difficulty saying ‘no’ was associated with: n Higher stress n Higher perceived self-care barriers n A reduced sense of well-being (mental and social) Same relationships found with care-giving barriers
In Summary… Difficulty saying ‘no’ to family and friends seems to be related to many negative psychosocial outcomes n n Difficulty saying ‘no’ was associated with: n Higher stress n Higher perceived self-care barriers n A reduced sense of well-being (mental and social) Same relationships found with care-giving barriers
 Family as the Behavioral Context n Research among Latinos with type 2 n n n Patients in families that were more cohesive had better diet and exercise habits Family variables accounted for most variance in both depressive affect and anxiety Research among African Americans n Family functioning (conflict, cohesion) was associated with A 1 c
Family as the Behavioral Context n Research among Latinos with type 2 n n n Patients in families that were more cohesive had better diet and exercise habits Family variables accounted for most variance in both depressive affect and anxiety Research among African Americans n Family functioning (conflict, cohesion) was associated with A 1 c
 So … What Now?
So … What Now?
 How Can Interventions Be Designed to Fit the Socio. Cultural Context?
How Can Interventions Be Designed to Fit the Socio. Cultural Context?
 Recent Interventions Among Populations of Color n Approaches/Strategies: (secondary prevention) 1. Peer counselors / Lay Advisors/ Community 2. 3. 4. 5. 6. Health Workers Adherence to clinical guidelines/standards Case Management Frequent follow-up contacts (phone, home or clinic visits) Group education/skills training Provision of medications or glucose selfmonitoring supplies
Recent Interventions Among Populations of Color n Approaches/Strategies: (secondary prevention) 1. Peer counselors / Lay Advisors/ Community 2. 3. 4. 5. 6. Health Workers Adherence to clinical guidelines/standards Case Management Frequent follow-up contacts (phone, home or clinic visits) Group education/skills training Provision of medications or glucose selfmonitoring supplies
 What Do We Know? Evidence from RCTs in type 2 diabetes: n In the short-term you can improve … n n n Knowledge, SMBG skills, and self-reported diet Glycemic control more readily than PA and weight Group education is effective for lifestyle interventions Patient interaction/collaboration is more effective than a didactic approach for weight loss, lipid or glycemic control Regular reinforcement is important
What Do We Know? Evidence from RCTs in type 2 diabetes: n In the short-term you can improve … n n n Knowledge, SMBG skills, and self-reported diet Glycemic control more readily than PA and weight Group education is effective for lifestyle interventions Patient interaction/collaboration is more effective than a didactic approach for weight loss, lipid or glycemic control Regular reinforcement is important
 What Don’t We Know? n n n How psychosocial factors influence changes in behaviors, metabolic control and other outcomes How to design the optimal long-term and maintenance interventions – content, frequency of contacts, or method of delivery How to achieve the ideal self-management intervention … n n acceptable to participants feasible in a variety of settings effective in the long-term relatively low cost and cost-effective
What Don’t We Know? n n n How psychosocial factors influence changes in behaviors, metabolic control and other outcomes How to design the optimal long-term and maintenance interventions – content, frequency of contacts, or method of delivery How to achieve the ideal self-management intervention … n n acceptable to participants feasible in a variety of settings effective in the long-term relatively low cost and cost-effective
 Diabetes Cultural Translation Key Factors: n Listen to the words and stories of those affected (qualitative research) n Identify and measure culturally relevant factors that influence diabetes self-care n Develop culturally appropriate behavior change and skill-building strategies n Let community voices (storytelling) enhance behavior change strategies
Diabetes Cultural Translation Key Factors: n Listen to the words and stories of those affected (qualitative research) n Identify and measure culturally relevant factors that influence diabetes self-care n Develop culturally appropriate behavior change and skill-building strategies n Let community voices (storytelling) enhance behavior change strategies
 Diabetes Cultural Translation Key Factors (cont …) n Increase the visibility of positive role models and exemplars n Train Community Diabetes Advocates (linking patients to community resources) n Strengthen informal support systems n Test the effectiveness of family-based interventions for adults
Diabetes Cultural Translation Key Factors (cont …) n Increase the visibility of positive role models and exemplars n Train Community Diabetes Advocates (linking patients to community resources) n Strengthen informal support systems n Test the effectiveness of family-based interventions for adults
 For every human problem, there is a neat, simple solution, and it is always wrong. H. L. Mencken
For every human problem, there is a neat, simple solution, and it is always wrong. H. L. Mencken


