5f55f539711de620a44edd68ab907924.ppt
- Количество слайдов: 40

September 21, 2017 Sepsis is a Medical Emergency… Are You Ready? Amy L. Sprague DNP, RN, ACNS-BC, CCRN Patient Safety Manager

When a Shirt Says it all….

Objectives • Distinguish between SIRS, Sepsis, Severe Sepsis, and Septic Shock and compare these to the new definitions for sepsis. • Review the pathophysiology of Sepsis. • Examine the bundle for treating sepsis. • Recognize Sepsis as a Medical Emergency……as important as Stroke or MI Care. • Discuss SOFA and q. SOFA. • Review the CMS measures.

Sepsis Statistics • 1. 6 million patients in the US develop sepsis each year. • Sepsis kills more people than prostrate cancer, breast cancer, and AIDS combined. • Estimates put sepsis world wide at 19 million. • Severe Sepsis has a mortality rate of 30%-35% • Septic Shock has a mortality rate of 50%.

More Facts • Severe Sepsis occurs most often from pneumonia followed by intra-abdominal infections and urinary tract infections. • Severe Sepsis occurs as a result of community acquired infections and health care associated infections.

What keeps me up at night?

Numerator Definition SEVERE SEPSIS SEPTIC SHOCK Exclusion: Patients receiving IV antibiotics for more than 24 hours prior to presentation of severe sepsis

Denominator CMS Baseline data begins 10/1/15 INCLUDED POPULATIONS: • Discharges age 18 and over with an ICD-10 -CM Principal or Other Diagnosis Code of Sepsis, Severe Sepsis, or Septic Shock EXCLUDED POPULATIONS: • • Directive for Comfort Care within 3 hours of presentation of severe sepsis Directive for Comfort Care within 6 hours of presentation of septic shock Administrative contraindication to care (documented and witnessed) Length of Stay >120 days Transfer in from another acute care facility Patients with severe sepsis who expire within 3 hours of presentation Patients with septic shock who expire within 6 hours of presentation

Sepsis Time Zero • Will always be when the chart annotation suggests signs and symptoms are all present • May be from nursing charting, lab flow sheets, physician documentation, anything with a time stamp • Will = ED triage time if all signs and symptoms are present at triage • Positive Sepsis diagnosis must be documented in MD/APN/PA notes, whereas • Time zero is identified when all criteria are met from other source documentation; SIRS screening can be pulled into MD/APN/PA notes

September 1 TO BE COMPLETED WITHIN 3 HOURS OF TIME OF PRESENTATION † : ü Measure lactate level ü Obtain blood cultures prior to administration of antibiotics ü Administer broad spectrum antibiotics ü Administer 30 ml/kg crystalloid for hypotension or lactate ≥ 4 mmol/L † “time of presentation” (time zero) is defined as the time of earliest chart annotation consistent with all elements severe sepsis or septic shock ascertained through chart review .

September 1 TO BE COMPLETED WITHIN 6 HOURS OF TIME OF PRESENTATION: ü Apply vasopressors (for hypotension that does not respond to initial fluid resuscitation) to maintain a mean arterial pressure (MAP) ≥ 65 mm. Hg. ü In the event of persistent hypotension after initial fluid administration (MAP < 65 mm Hg) or if initial lactate was ≥ 4 mmol/L, re-assess volume status and tissue perfusion and document findings according to table 1. ü Re-measure lactate if initial lactate elevated.

Document re-assessment of volume status & tissue perfusion EITHER • Repeat focused exam (after initial fluid resuscitation) by licensed independent practitioner including vital signs, cardiopulmonary, capillary refill, pulse and skin findings OR TWO OF THE FOLLOWING: • • • Esophageal Doppler Measure CVP Measure Scv. O 2 Bedside cardiovascular ultrasound Dynamic assessment of fluid responsiveness with passive leg raise or fluid challenge CMS wants to see the provider do these and document them.

What comes next? • Sepsis will probably follow the same path that the SCIP measures followed: • We supplied data for about 1 year without penalty. • After about 1 year of data submission the measures became “pay for performance” measures.

Sequential Organ Failure Assessment (SOFA) score and Quick SOFA • Respiratory system ~ • • • Fi 02/Pao 2 mm. Hg Nervous system ~ Glasgow Coma Score Cardiovascular system ~ Mean Arterial Pressure OR administration of vasopressors required Liver ~ Bilirubin (mg/dl) [μmol/L] Coagulation ~ Platelets× 103/µl Renal ~ Creatinine (mg/dl) [μmol/L] (or urine output) • q. SOFA • An alteration in mental status. • A decrease in systolic blood • pressure of less than 100 mm. Hg. A respiratory rate greater than 22 breaths/min.
Sepsis Definitions “Old” • Sepsis is 2 SIRS Criteria and a known, new, suspected, or presumed infection. • Severe Sepsis is SIRS PLUS one organ involved. • Septic Shock is a lactate >4 OR hypotension that is not corrected with fluid volume resuscitation. “New” • Removed the SIRS criteria. • Sepsis is a life threatening organ dysfunction due to a dysregulated host response to infection. • Septic shock is a subset of sepsis in which particularly profound circulatory, cellular, and metabolic abnormalities substantially increase mortality.

SIRS stands for Systemic Inflammatory Response Syndrome • • Fever >38. 3°C (100. 9°F) Hypothermia < 36°C (96. 8°F) Heart rate >90 beats per minute Respiratory rate of more than 20 breaths per minute or arterial carbon dioxide tension (Pa. CO 2) of less than 32 mm Hg • Abnormal white blood cell count (>12, 000/µL or < 4, 000/µL or >10% immature [band] forms) ADDITIONAL CRITERIA • Mental status altered from baseline • Hyperglycemia > 140 mg/dl in absence of diabetes • Significant edema or positive fluid balance > 20 ml/kg over 24 hours

Systemic Inflammatory Response Syndrome (SIRS) • A serious inflammatory state throughout the entire body. • The most common etiology of SIRS is an infection. • Non-infectious processes can also cause the response. – complications of surgery – adrenal insufficiency – pulmonary embolism – cardiac tamponade – anaphylaxis – drug overdose – pancreatitis

Sepsis New, known, presumed, or worsening infection and at least 2 SIRS criteria.
Severe Sepsis associated with organ dysfunction, hypotension, or hypoperfusion abnormalities including: • Skin mottling or capillary refill time >3 seconds • Urine output < 0. 5 ml/kg for at least 1 h or patient requiring renal replacement therapy • Serum lactate >2 mmol/L • Acute alteration of mentation or encephalopathic changes on electroencephalogram • Disseminated intravascular coagulation or platelets <100 K cells/m. L • Acute lung injury or acute respiratory distress syndrome • Lactate of 2 or >
Septic Shock • Septic Shock is Severe Sepsis PLUS • Hypotension despite adequate fluid resuscitation OR • Serum Lactate > 4 mmol/L

Stroke and MI Care STROKE CARE • Note time of system onset…. . ”last time well” • NIH stroke scale • CBC, chem 7, PT/PTT and INR labs drawn prior to head CT. • Head CT non-contrast within 45 minutes of Code Stroke or ED arrival. • MRI-later • Oxygen • IV • NPO • Thrombolytic if they qualify • R/O hypoglycemia, seizure, migraine, and drug OD MI CARE • ASA 325 mg • Oxygen • Stat EKG • Nitro SL (Do not give if taken meds for ED. ) • IV • Morphine • Cardiac Enzymes • Cardiologist
Follow the Sepsis 3 Hour Bundle • Measure lactate level stat • Obtain blood cultures prior to • • administration of antibiotics Administer broad spectrum antibiotic Administer 30 ml/kg crystalloid (Normal Saline) for hypotension or lactate > 4 mmol/L

Fluid Resuscitation • • What it is not……it is not 999 on the pump. It is fast…. . over 20 minutes or less. Use a pressure bag or the rapid infuser. If patient improves 10% (B/P or MAP) then give more fluid. ETC……keep giving the fluid with each 10% improvement.

CBC • Leukocytosis (WBC count > 12, 000) • Leukopenia (WBC count <4, 000) • Normal WBC count with greater than 10% immature bands
Serum Lactate • • Is a marker of malprofusion. Lactate > 2 mmol/L Severe Sepsis Lactate > 4 mmol/L Septic Shock Not everyone with sepsis will have an elevated lactate level. • Look for other characteristics of poor profusion: • Mean Arterial Pressure (MAP) < 65 mm. Hg • Urine Output < 0. 5 ml/kg/hr

Procalcitonin • Is a peptide precursor of the • • • hormone calcitonin. It is secreted from the Thyroid gland in response to a bacterial infection. Helpful to tell the difference between a bacterial infection and a viral infection. PCT rises in 3 -6 hours of a bacterial infection. Very helpful when the bacterial infection is a pneumonia.
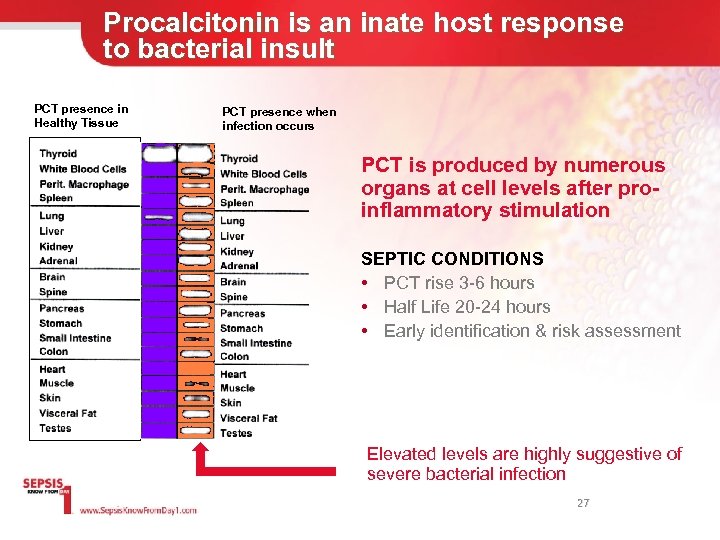
Procalcitonin is an inate host response to bacterial insult PCT presence in Healthy Tissue PCT presence when infection occurs PCT is produced by numerous organs at cell levels after proinflammatory stimulation SEPTIC CONDITIONS • PCT rise 3 -6 hours • Half Life 20 -24 hours • Early identification & risk assessment Elevated levels are highly suggestive of severe bacterial infection Muller B, et al. J Clin Endocrinol Metab 2001 Jan; 86(1): 396 -404. 27
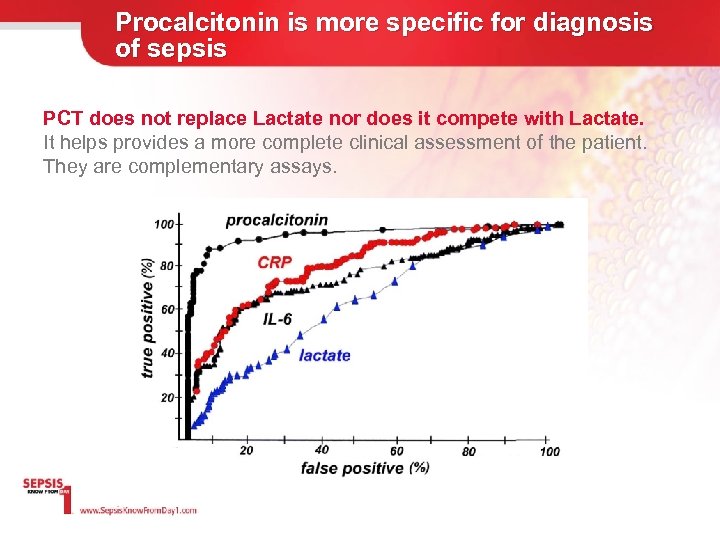
Procalcitonin is more specific for diagnosis of sepsis PCT does not replace Lactate nor does it compete with Lactate. It helps provides a more complete clinical assessment of the patient. They are complementary assays.
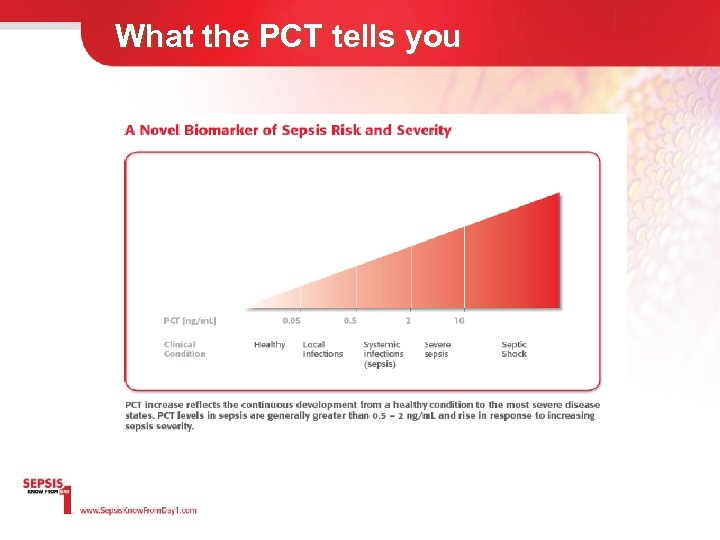
What the PCT tells you
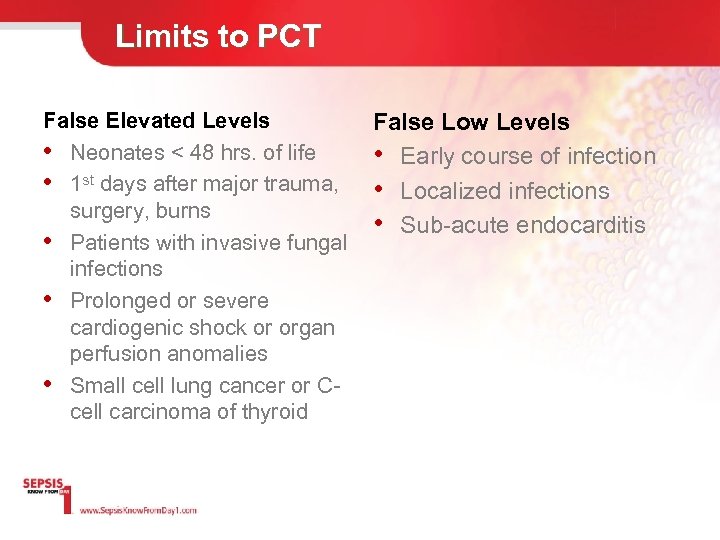
Limits to PCT False Elevated Levels False Low Levels • Neonates < 48 hrs. of life • Early course of infection • 1 st days after major trauma, • Localized infections surgery, burns • Sub-acute endocarditis • Patients with invasive fungal infections • Prolonged or severe cardiogenic shock or organ perfusion anomalies • Small cell lung cancer or Ccell carcinoma of thyroid

Protocols for the bedside nurse: • Labs: Draw 2 sets of blood cultures drawn before antibiotics initiated. If you have antibiotics ordered GIVE THEM, do not wait to obtain the blood cultures beyond 1 attempt to draw them. • Lactate, if not already completed. Repeat the lactate in 5 hours. • CBC, if not already completed above, with MANUAL DIFF (This change is due to not seeing the bands with the automated diff. ) • • • BMP Procalcitonin UA stat with reflex to culture. IF respiratory symptoms order portable Chest x-ray. IF Diarrhea send for CDiff toxin/antigen.

Our Sepsis Protocols: • We added PCT to our sepsis protocols for nurses. • We did a collaborative with the Surviving Sepsis Campaign on our Geriatrics unit. We included PCT as a lab to be completed with the CBC and the lactate.
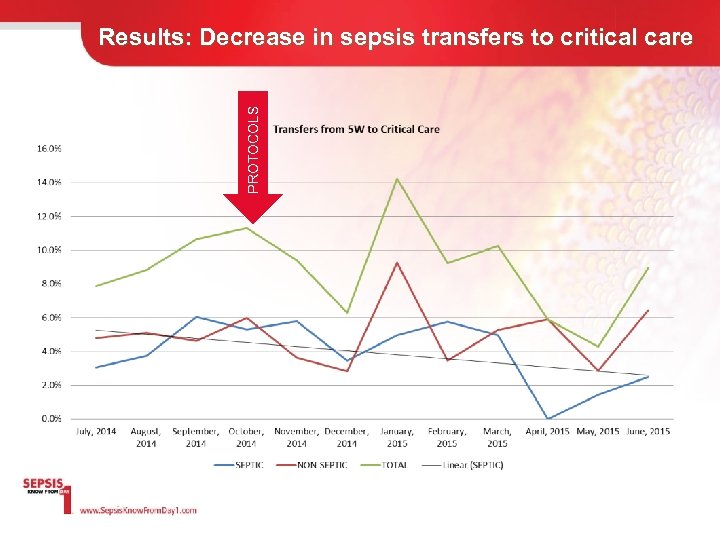
PROTOCOLS Results: Decrease in sepsis transfers to critical care
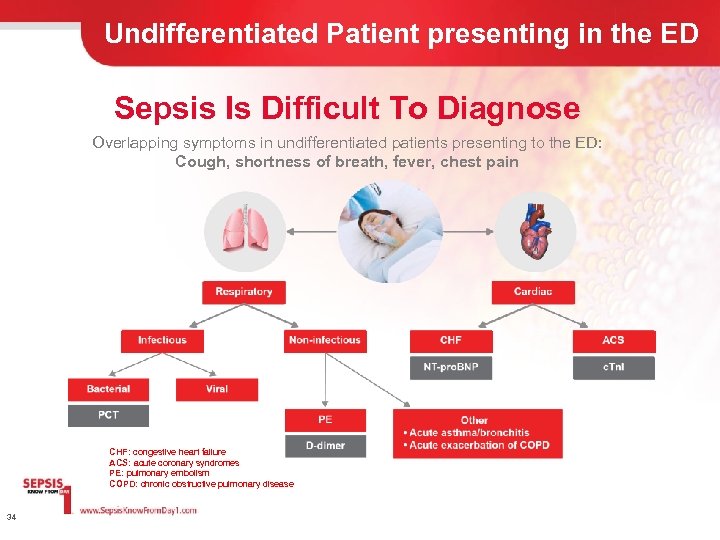
Undifferentiated Patient presenting in the ED Sepsis Is Difficult To Diagnose Overlapping symptoms in undifferentiated patients presenting to the ED: Cough, shortness of breath, fever, chest pain CHF: congestive heart failure ACS: acute coronary syndromes PE: pulmonary embolism COPD: chronic obstructive pulmonary disease 34
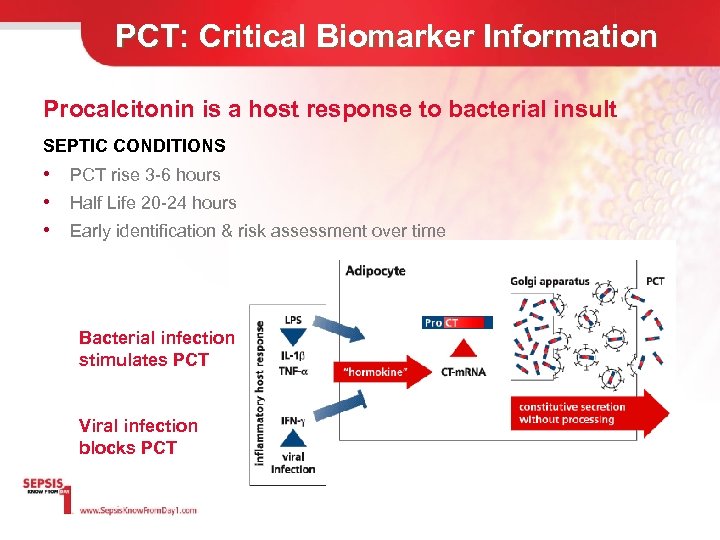
PCT: Critical Biomarker Information Procalcitonin is a host response to bacterial insult SEPTIC CONDITIONS • PCT rise 3 -6 hours • Half Life 20 -24 hours • Early identification & risk assessment over time Bacterial infection stimulates PCT Viral infection blocks PCT

PCT: New Indication SHORT VERSION “…determine the change in PCT level over time…” FULL VERSION VIDAS® B·R·A·H·M·S PCT™ (PCT) is also intended for use to determine the change in PCT level over time as an aid in assessing the cumulative 28 -day risk of all-cause mortality in conjunction with other laboratory findings and clinical assessments for patients diagnosed with severe sepsis or septic shock in the ICU or when obtained in the emergency department or other medical wards prior to ICU admission.
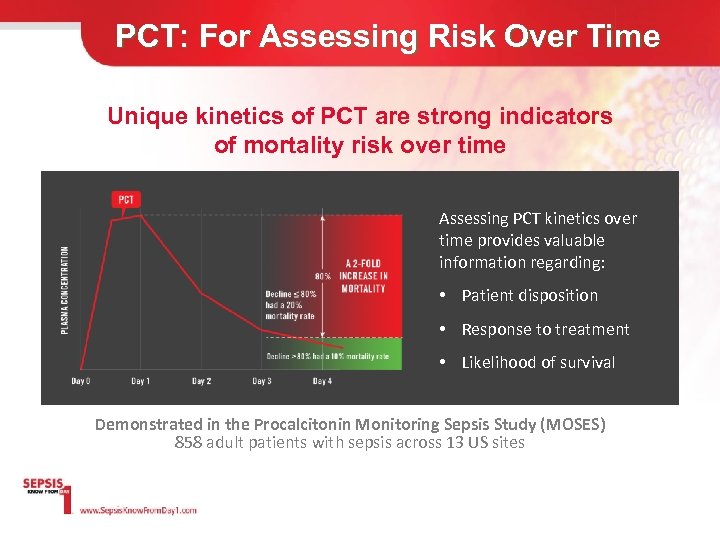
PCT: For Assessing Risk Over Time Unique kinetics of PCT are strong indicators of mortality risk over time Assessing PCT kinetics over time provides valuable information regarding: • Patient disposition • Response to treatment • Likelihood of survival Demonstrated in the Procalcitonin Monitoring Sepsis Study (MOSES) 858 adult patients with sepsis across 13 US sites
Join the Conversations www. survivingsepsis. org

References • Elixhauser A et al: Septicemia in US Hospitals 2009 , statistical brief #122 Rockville , MD: Agency for Healthcare Research and Quality ; 2001 • Dellinger, R. P. , Levy, M. , Rhodes, A. , Annane, D. , Gerlach, H. , Opal, S. , . . . Surviving Sepsis Campaign Guidelines Committee. (2013). Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012. ritical Care Medicine, C 41(2), 580 -637. • El Solh, A. , Akinnusi, M, Alsawalha, L, Pineda, L. (2008). Outcome of septic shock in older adults after implementation of the sepsis “bundle”. Journal of the American Geriatrics Society, 56(2), 272 -278. • Evans, E. , Therriault, M. , & Townsend, S. R. (2015). Early Management Bundle, Severe Sepsis/Septic Shock. New York: Centers for Medicare & Medicaid Services. Retrieved June 22, 2015, from http: //www. qualityreportingcenter. com/inpatient/iqr/events/ • Kumar, A. , Roberts, D. , Wood, K. , Light, B. , Parrillo, J. , Sharma, S. , . . . Cheang, M. (2006). Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Critical Care Medicine, 1589 -1596. • Levy MM, Dellinger RP, Townsend S, et al. The Surviving Sepsis Campaign: results of an international guideline-based performance improvement program targeting severe sepsis. Crit Care Med. 2010; 38(2): 367– 374 • Specifications Manual for National Hospital Inpatient Quality Measures, Discharges 10 -01 -15 through 06 -30 -16, Version 5. 0 a. (See www. qualitynet. org) • Singer M, et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3) • Shankar-Hari M, et al. Developing a New Definition and Assessing New Clinical Criteria for Septic Shock: For the Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3) • Seymour CW, et al. Assessment of Clinical Criteria for Sepsis: For the Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3) 39

Questions THANK YOU! Amy. sprague@va. gov 317. 988. 3547 PRN: 16 -0237 -00/MK
5f55f539711de620a44edd68ab907924.ppt