3cbb6b283ede3a9e708dde30532b6780.ppt
- Количество слайдов: 91
 Sepsis markers Dr. Natalie Leung 6 th January 2012 ICU, Pamela Youde Nethersole Eastern Hospital, Hong Kong
Sepsis markers Dr. Natalie Leung 6 th January 2012 ICU, Pamela Youde Nethersole Eastern Hospital, Hong Kong
 Introduction • Sepsis can occur suddenly and deteriorate rapidly • Timely diagnosis of sepsis is the key of success
Introduction • Sepsis can occur suddenly and deteriorate rapidly • Timely diagnosis of sepsis is the key of success
 However…… can sometimes be challenging
However…… can sometimes be challenging
 How to improve the outcome of sepsis? • Early diagnosis and treatment • Surviving Sepsis Campaign – reduction in mortality rate of severe sepsis.
How to improve the outcome of sepsis? • Early diagnosis and treatment • Surviving Sepsis Campaign – reduction in mortality rate of severe sepsis.
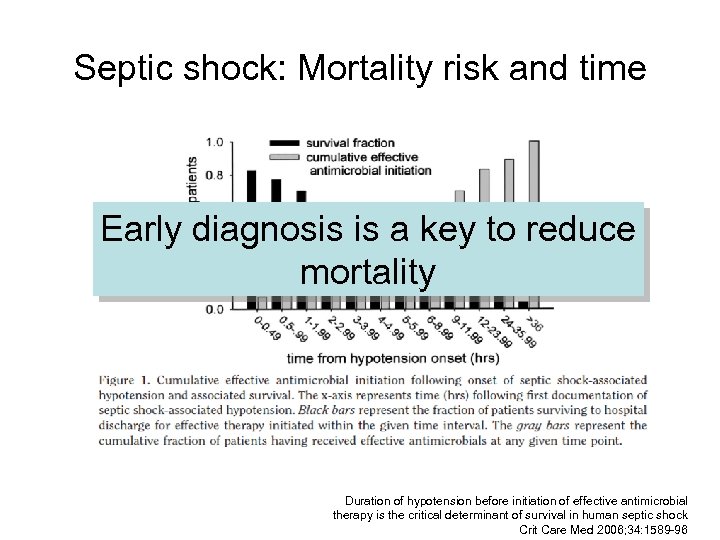 Septic shock: Mortality risk and time Early diagnosis is a key to reduce mortality Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock Crit Care Med 2006; 34: 1589 -96
Septic shock: Mortality risk and time Early diagnosis is a key to reduce mortality Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock Crit Care Med 2006; 34: 1589 -96
 Sepsis markers • Diagnostic – Useful for identifying or ruling out sepsis – Identifying patients who may benefit from specific therapies • Assessing the response to therapy • Prognostic
Sepsis markers • Diagnostic – Useful for identifying or ruling out sepsis – Identifying patients who may benefit from specific therapies • Assessing the response to therapy • Prognostic
 Ideal sepsis markers • High sensitivity (increase pathologically in the presence of disease) • High specificity (does not increase in the absence of disease) • Related to the disease burden and extent • Changes in accordance with the clinical evolution • Anticipates clinical changes before it happens
Ideal sepsis markers • High sensitivity (increase pathologically in the presence of disease) • High specificity (does not increase in the absence of disease) • Related to the disease burden and extent • Changes in accordance with the clinical evolution • Anticipates clinical changes before it happens
 Ideal sepsis markers • Adds independent information about the risk or prognosis • Reproducible • Easy and cheap
Ideal sepsis markers • Adds independent information about the risk or prognosis • Reproducible • Easy and cheap
 What do we have now? • WCC • Lactate – Tissue perfusion variables • Biomarkers – C-reactive protein (CRP) – Procalcitonin (PCT) – Cytokines – New markers
What do we have now? • WCC • Lactate – Tissue perfusion variables • Biomarkers – C-reactive protein (CRP) – Procalcitonin (PCT) – Cytokines – New markers
 What do we have now? • A review of sepsis biomarkers – 178 different biomarkers – Most of them had been tested clinically • Primiarily as prognostic markers • Relatively few have been used for diagnosis Sepsis biomarkers: a review. Critical Care. 2010; 14(1): R 15
What do we have now? • A review of sepsis biomarkers – 178 different biomarkers – Most of them had been tested clinically • Primiarily as prognostic markers • Relatively few have been used for diagnosis Sepsis biomarkers: a review. Critical Care. 2010; 14(1): R 15
 What do we have now? • Large numbers of markers – Cytokines – Receptors biomarkers – Coagulation biomarkers – Biomarkers related to vascular endothelial damage – Markers related to organ dysfunction – Acute phase protein biomarkers – others Sepsis biomarkers: a review Crit Care. 2010; 14(1): R 15
What do we have now? • Large numbers of markers – Cytokines – Receptors biomarkers – Coagulation biomarkers – Biomarkers related to vascular endothelial damage – Markers related to organ dysfunction – Acute phase protein biomarkers – others Sepsis biomarkers: a review Crit Care. 2010; 14(1): R 15
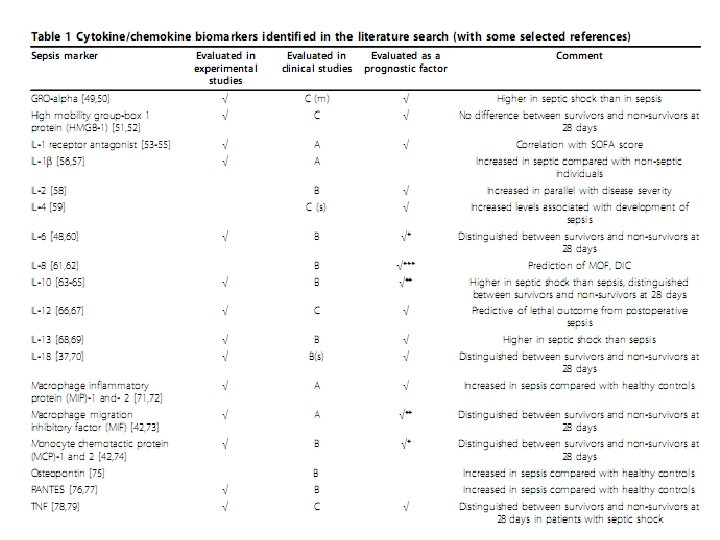
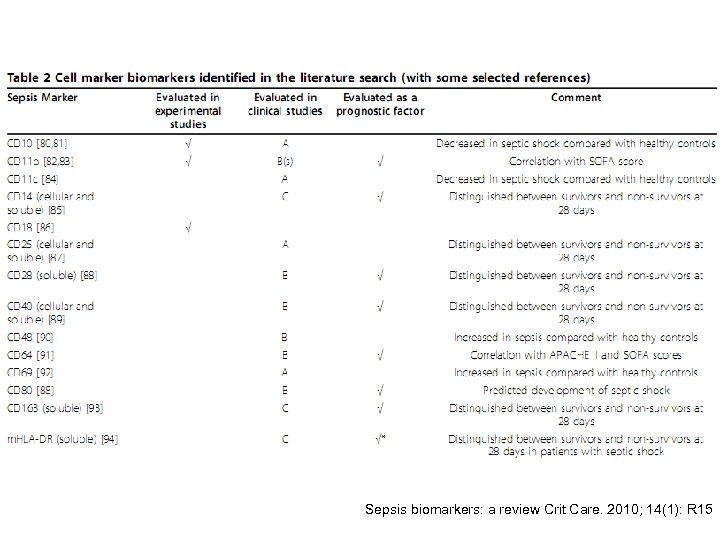 Sepsis biomarkers: a review Crit Care. 2010; 14(1): R 15
Sepsis biomarkers: a review Crit Care. 2010; 14(1): R 15
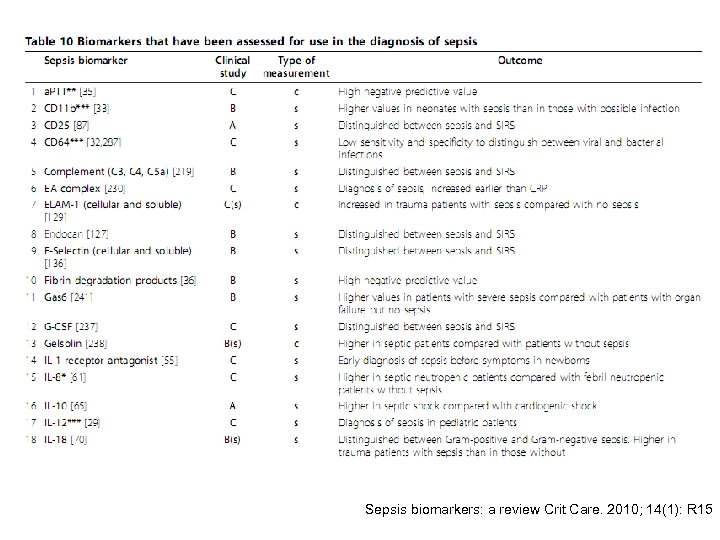 Sepsis biomarkers: a review Crit Care. 2010; 14(1): R 15
Sepsis biomarkers: a review Crit Care. 2010; 14(1): R 15
 Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
 Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
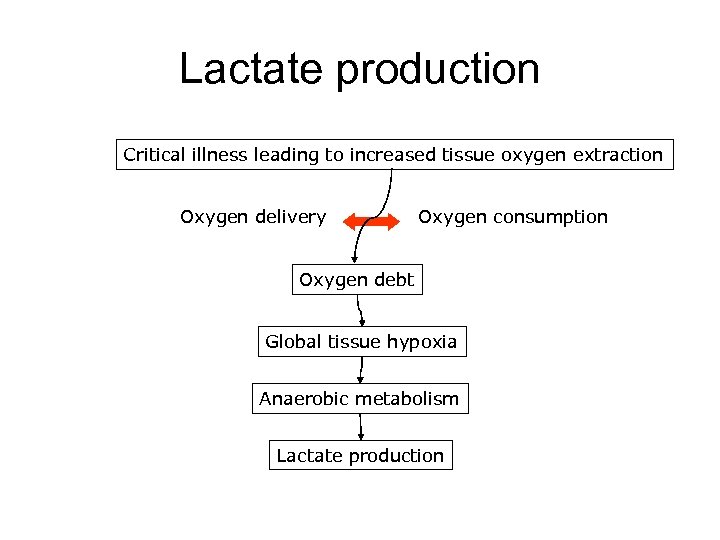 Lactate production Critical illness leading to increased tissue oxygen extraction Oxygen delivery Oxygen consumption Oxygen debt Global tissue hypoxia Anaerobic metabolism Lactate production
Lactate production Critical illness leading to increased tissue oxygen extraction Oxygen delivery Oxygen consumption Oxygen debt Global tissue hypoxia Anaerobic metabolism Lactate production
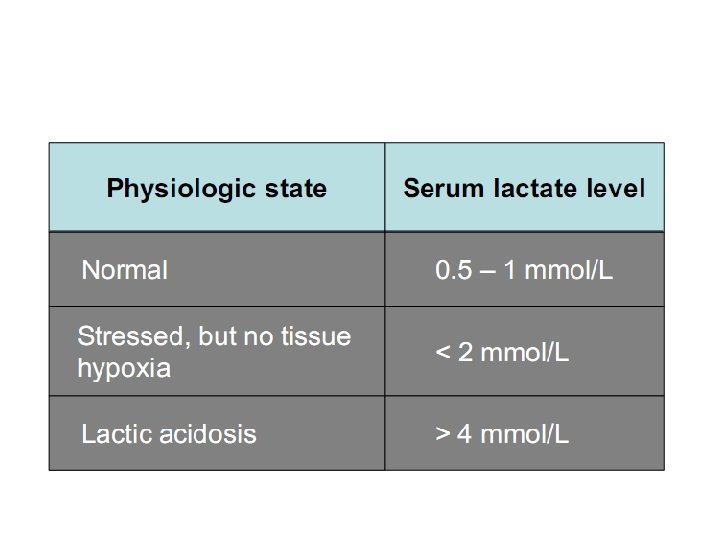
 Lactate • Raised in severe sepsis and septic shock – Hypoperfusion (secondary to anaerobic metabolism) – Cellular metabolic failure – Decrease clearance by the liver
Lactate • Raised in severe sepsis and septic shock – Hypoperfusion (secondary to anaerobic metabolism) – Cellular metabolic failure – Decrease clearance by the liver
 • Numerous studies have established that lactate is a good marker of global hypoxia in circulatory shock
• Numerous studies have established that lactate is a good marker of global hypoxia in circulatory shock
 Use of lactate as a sepsis marker • Diagnosis • Prognostic and predict mortality
Use of lactate as a sepsis marker • Diagnosis • Prognostic and predict mortality
 Diagnosis • Limited role in diagnostic • Surviving Sepsis Campaign guidelines 2008 – “begin resuscitation immediately in patients with hypotension/ elevated serum lactate >=4 mmol/l”
Diagnosis • Limited role in diagnostic • Surviving Sepsis Campaign guidelines 2008 – “begin resuscitation immediately in patients with hypotension/ elevated serum lactate >=4 mmol/l”
 Prognostic and predict mortality • It can be used as … – Monitoring response of septic patients to resuscitation – Stratification and prognosis • Serial lactate level monitoring is recommended – High lactate clearance: • less required vasopressors therapy, greater improvements in APACHE II scores and decreased mortality rates
Prognostic and predict mortality • It can be used as … – Monitoring response of septic patients to resuscitation – Stratification and prognosis • Serial lactate level monitoring is recommended – High lactate clearance: • less required vasopressors therapy, greater improvements in APACHE II scores and decreased mortality rates
 Lactate clearance • In patients with septic shock – Survivors vs non-survivors • Initial lactate level did not differ much • Survivors had a significant decrease in lactate levels and less “lactate clearance time” Low exogenous lactate clearance as an early predictor of mortality in normolactatemic critically ill septic patients. Crit Care Med. 2003; 31(3): 705 -710.
Lactate clearance • In patients with septic shock – Survivors vs non-survivors • Initial lactate level did not differ much • Survivors had a significant decrease in lactate levels and less “lactate clearance time” Low exogenous lactate clearance as an early predictor of mortality in normolactatemic critically ill septic patients. Crit Care Med. 2003; 31(3): 705 -710.
 Lactate clearance • 111 ED and ICU patients with severe sepsis and septic shock • Lactate clearance – The percentage lactate decrease over the initial 6 hr ED evaluation and treatment period Low exogenous lactate clearance as an early predictor of mortality in normolactatemic critically ill septic patients. Crit Care Med. 2003; 31(3): 705 -710.
Lactate clearance • 111 ED and ICU patients with severe sepsis and septic shock • Lactate clearance – The percentage lactate decrease over the initial 6 hr ED evaluation and treatment period Low exogenous lactate clearance as an early predictor of mortality in normolactatemic critically ill septic patients. Crit Care Med. 2003; 31(3): 705 -710.
 Lactate clearance • All patients were followed for 72 hrs and received a protocol-driver EGDT • Results – The higher the lactate clearance, the lower the mortality Low exogenous lactate clearance as an early predictor of mortality in normolactatemic critically ill septic patients. Crit Care Med. 2003; 31(3): 705 -710.
Lactate clearance • All patients were followed for 72 hrs and received a protocol-driver EGDT • Results – The higher the lactate clearance, the lower the mortality Low exogenous lactate clearance as an early predictor of mortality in normolactatemic critically ill septic patients. Crit Care Med. 2003; 31(3): 705 -710.
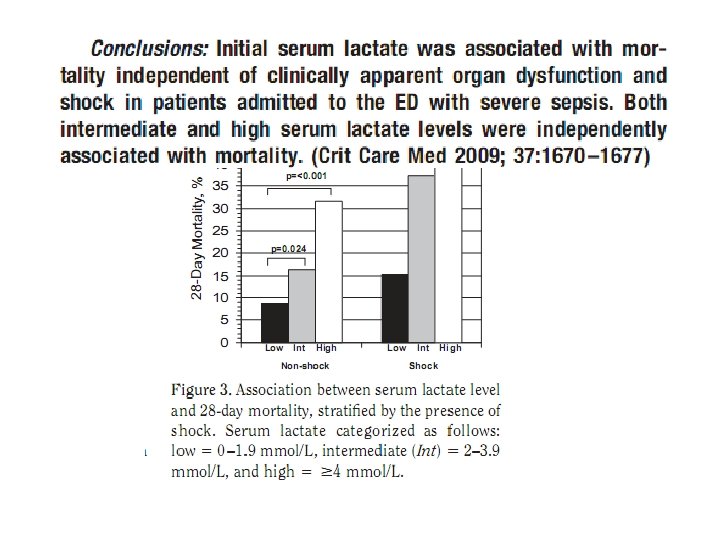
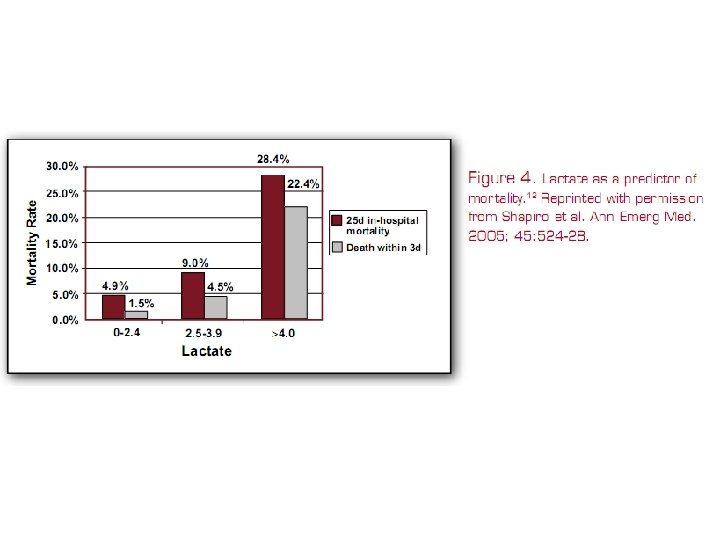
 • Single-center cohort study • 830 patients • Test the association between initial serum lactate level and mortality in patients presenting to AED with severe sepsis is independent of organ dysfunction and shock
• Single-center cohort study • 830 patients • Test the association between initial serum lactate level and mortality in patients presenting to AED with severe sepsis is independent of organ dysfunction and shock
 Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
 CRP • Acute phase protein • Synthesized in liver • IL-6 (and IL-1 and TNFα) stimulate synthesis • Binds bacterial polysaccharide/ chromatin – Activates the classical complement pathway – Increase the immune inflammatory response • Esp. in bacteria infection (vs viral)
CRP • Acute phase protein • Synthesized in liver • IL-6 (and IL-1 and TNFα) stimulate synthesis • Binds bacterial polysaccharide/ chromatin – Activates the classical complement pathway – Increase the immune inflammatory response • Esp. in bacteria infection (vs viral)
 CRP • Level of CRP begins within 4 -6 hrs after stimulus • Doubles every 8 hrs • Peaks at 36 -50 hrs • Half-life 19 hrs
CRP • Level of CRP begins within 4 -6 hrs after stimulus • Doubles every 8 hrs • Peaks at 36 -50 hrs • Half-life 19 hrs
 CRP • A sensitive marker of inflammation and tissue damage • Other conditions result in raised in CRP – Rheumatological disease • • SLE Systemic sclerosis Dermatomyositis Sjogren’s disease – Inflammatory bowel disease – Haematological disease • E. g. leukaemia – Graft-versus-host disease
CRP • A sensitive marker of inflammation and tissue damage • Other conditions result in raised in CRP – Rheumatological disease • • SLE Systemic sclerosis Dermatomyositis Sjogren’s disease – Inflammatory bowel disease – Haematological disease • E. g. leukaemia – Graft-versus-host disease
 CRP
CRP
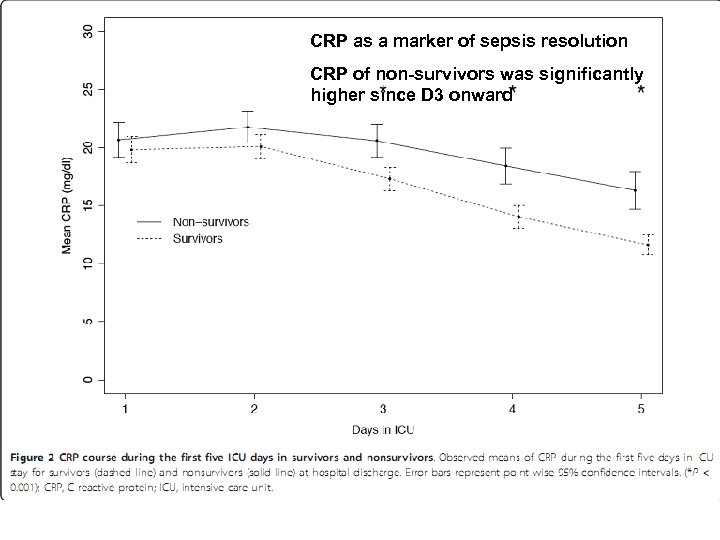 CRP as a marker of sepsis resolution CRP of non-survivors was significantly higher since D 3 onward
CRP as a marker of sepsis resolution CRP of non-survivors was significantly higher since D 3 onward
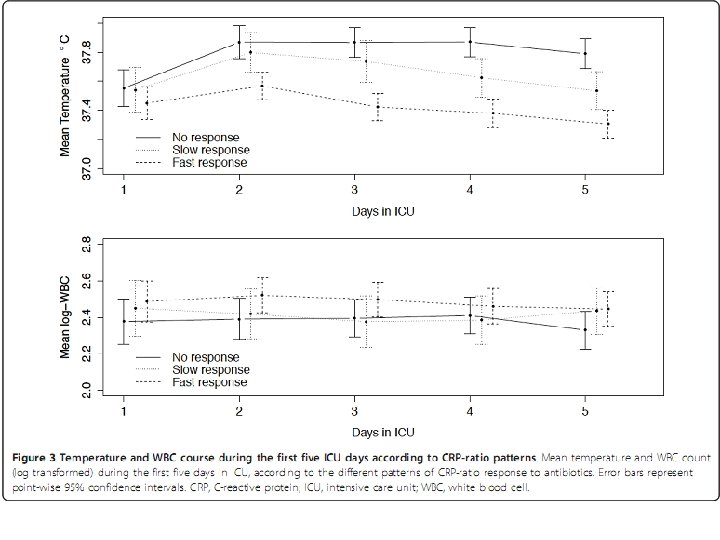

 Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
 Procalcitonin • A peptide precursor of calcitonin • Produced by – parafollicular cells of the thyroid – neuroendocrine cells of the lung and the intestine (extrathyroidal) • It raises in a response to a proinflammatory stimulus – Esp of bacterial origin (mainly from the cells of lung and the intestine)
Procalcitonin • A peptide precursor of calcitonin • Produced by – parafollicular cells of the thyroid – neuroendocrine cells of the lung and the intestine (extrathyroidal) • It raises in a response to a proinflammatory stimulus – Esp of bacterial origin (mainly from the cells of lung and the intestine)
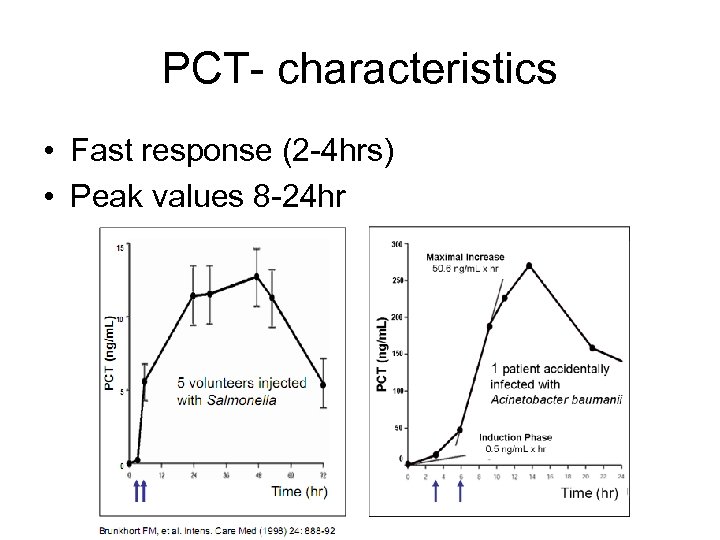 PCT- characteristics • Fast response (2 -4 hrs) • Peak values 8 -24 hr
PCT- characteristics • Fast response (2 -4 hrs) • Peak values 8 -24 hr
 PCT- characteristics • Short half-life (~24 hrs) independent of renal function • Easy to measure in serum and plasma (stable in vivo and in vitro) • Plasma concentration ~ <0. 05 -1000 ng/ml
PCT- characteristics • Short half-life (~24 hrs) independent of renal function • Easy to measure in serum and plasma (stable in vivo and in vitro) • Plasma concentration ~ <0. 05 -1000 ng/ml
 • In systemic inflammation or in infection – Persists as long as inflammatory process continues • Mechanical trauma – Increase within 2 -4 hrs – Peak in 1 st or 2 nd day then diminish
• In systemic inflammation or in infection – Persists as long as inflammatory process continues • Mechanical trauma – Increase within 2 -4 hrs – Peak in 1 st or 2 nd day then diminish
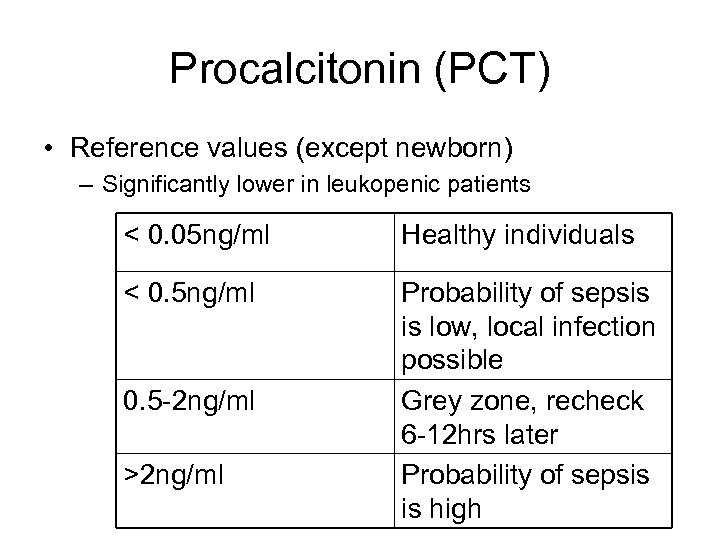 Procalcitonin (PCT) • Reference values (except newborn) – Significantly lower in leukopenic patients < 0. 05 ng/ml Healthy individuals < 0. 5 ng/ml Probability of sepsis is low, local infection possible Grey zone, recheck 6 -12 hrs later Probability of sepsis is high 0. 5 -2 ng/ml >2 ng/ml
Procalcitonin (PCT) • Reference values (except newborn) – Significantly lower in leukopenic patients < 0. 05 ng/ml Healthy individuals < 0. 5 ng/ml Probability of sepsis is low, local infection possible Grey zone, recheck 6 -12 hrs later Probability of sepsis is high 0. 5 -2 ng/ml >2 ng/ml
 Use of PCT • Sepsis diagnosis • Antibiotic guidance • Patient prognosis
Use of PCT • Sepsis diagnosis • Antibiotic guidance • Patient prognosis
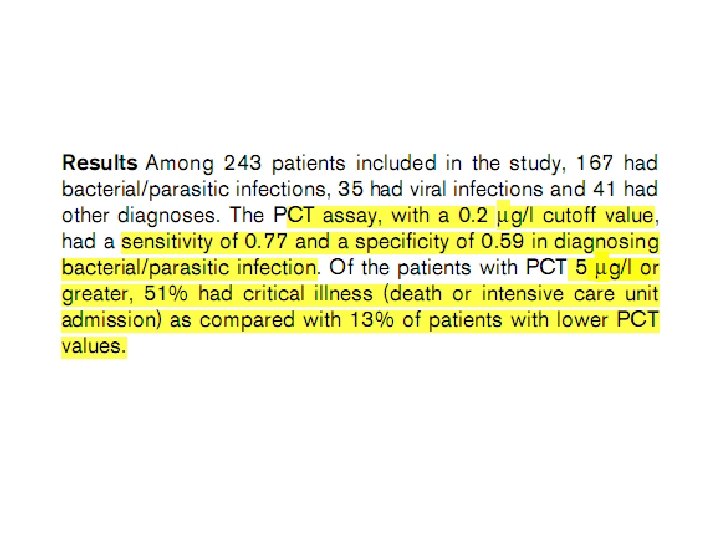
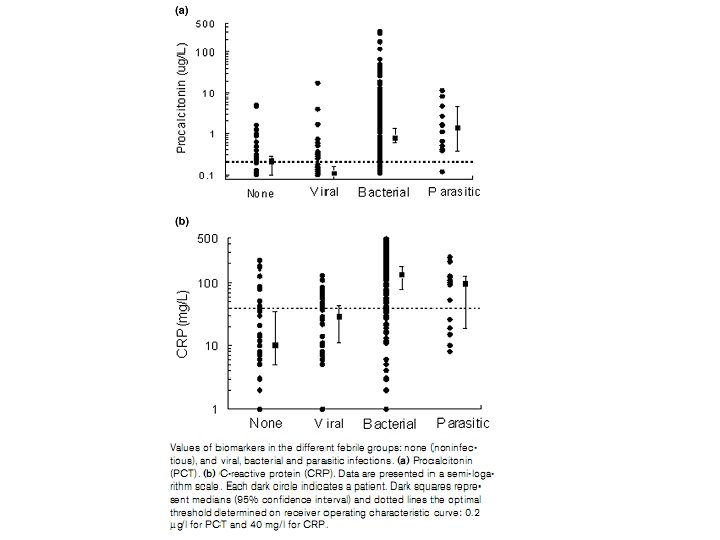
 Sepsis diagnosis • Prospective single centre, noninterventional study • Patients > 38 C Bruno Riou et al. Critical Care 2007; 11: R 60
Sepsis diagnosis • Prospective single centre, noninterventional study • Patients > 38 C Bruno Riou et al. Critical Care 2007; 11: R 60
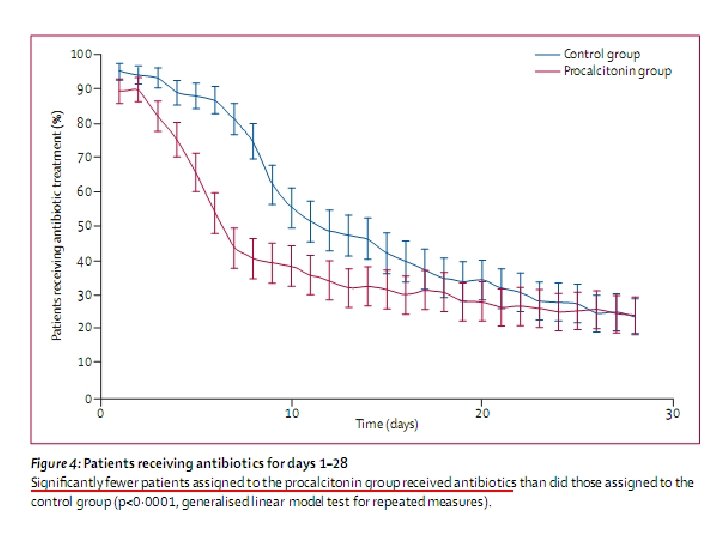
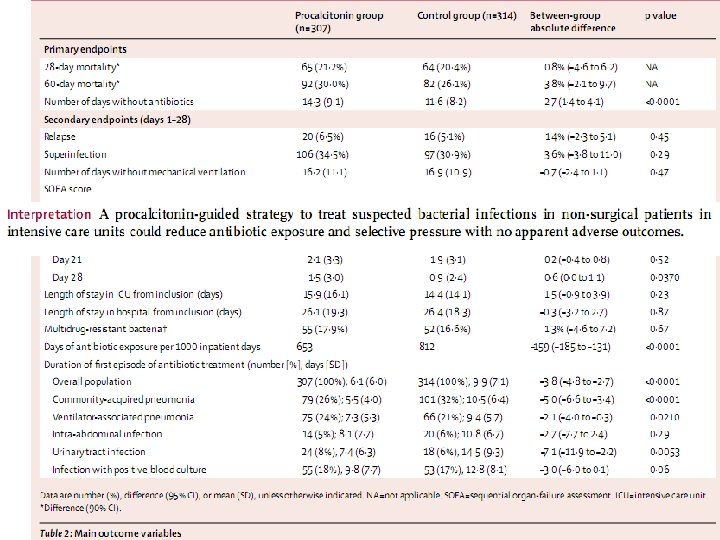
 Antibiotic therapy • Multicentre, prospective, parallel-group, open-label trial • 1: 1 ratio of procalcitonin (n=311) and control group (n=319)
Antibiotic therapy • Multicentre, prospective, parallel-group, open-label trial • 1: 1 ratio of procalcitonin (n=311) and control group (n=319)
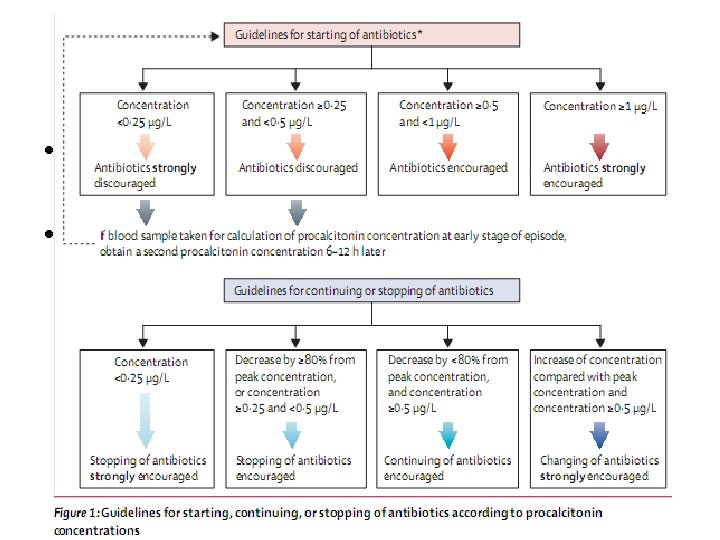 • Antibiotics were started/ stopped based on a predefined cut-off ranges of PCT value • Primary end point – 28 and 60 days mortality – No. of days without antibiotics
• Antibiotics were started/ stopped based on a predefined cut-off ranges of PCT value • Primary end point – 28 and 60 days mortality – No. of days without antibiotics
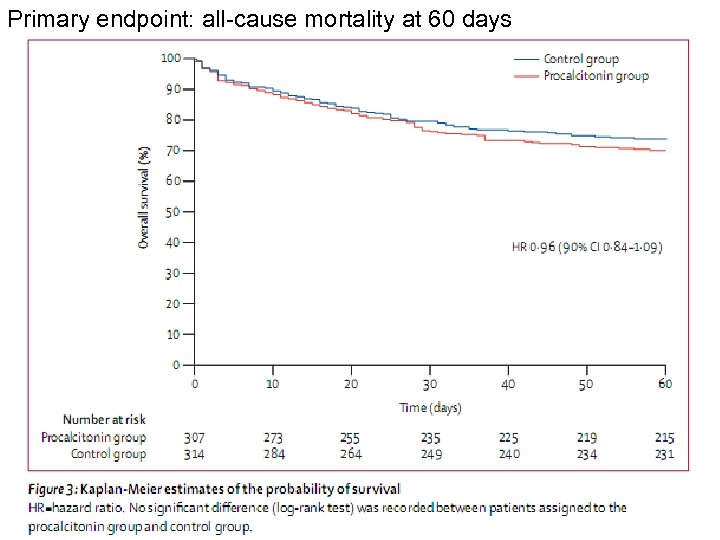 Primary endpoint: all-cause mortality at 60 days
Primary endpoint: all-cause mortality at 60 days
 Antibiotic therapy and prognosis Charles PE, et al. Critical Care 2009: 13; 16 -20 • 180 patients • PCT levels were obtained at the onset of clinical sepsis (Day 1) and at least twice more within next 3 days • Monitor change in PCT levels to assess effectiveness of antibiotic treatment
Antibiotic therapy and prognosis Charles PE, et al. Critical Care 2009: 13; 16 -20 • 180 patients • PCT levels were obtained at the onset of clinical sepsis (Day 1) and at least twice more within next 3 days • Monitor change in PCT levels to assess effectiveness of antibiotic treatment
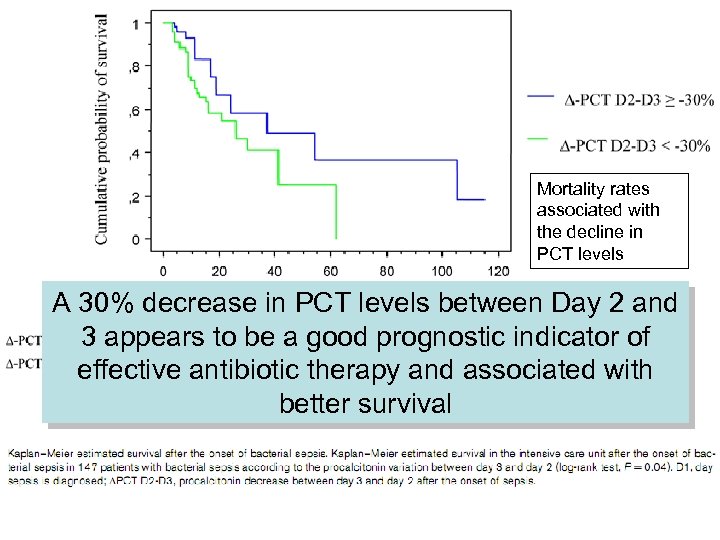 Mortality rates associated with the decline in PCT levels A 30% decrease in PCT levels between Day 2 and 3 appears to be a good prognostic indicator of effective antibiotic therapy and associated with better survival
Mortality rates associated with the decline in PCT levels A 30% decrease in PCT levels between Day 2 and 3 appears to be a good prognostic indicator of effective antibiotic therapy and associated with better survival
 • PCT is also associated with other conditions – VAP – Severe acute pancreatitis – Acute exacerbation of COPD
• PCT is also associated with other conditions – VAP – Severe acute pancreatitis – Acute exacerbation of COPD
 Nonbacterial infection: Viruses, Fungi, Parasites • PCT tend to be low in viral infection – However, in systemic viral infection, PCT value can as high as 16 ng/ml • A low serum PCT cannot be used to exclude bacterial from viral infections but that a combination of PCT, CRP, white blood cell count, and clinical illness scoring might be more useful
Nonbacterial infection: Viruses, Fungi, Parasites • PCT tend to be low in viral infection – However, in systemic viral infection, PCT value can as high as 16 ng/ml • A low serum PCT cannot be used to exclude bacterial from viral infections but that a combination of PCT, CRP, white blood cell count, and clinical illness scoring might be more useful
 Nonbacterial infection: Viruses, Fungi, Parasites • In patients with fungal infections, results have been variable • Infection with the malaria parasite often leads to very high levels of serum, as high as 662 ng/m. L
Nonbacterial infection: Viruses, Fungi, Parasites • In patients with fungal infections, results have been variable • Infection with the malaria parasite often leads to very high levels of serum, as high as 662 ng/m. L
 Sepsis and PCT: The Pediatric Experience • Complicated by a physiological rise in both term and preterm, healthy infants, which peaks at approximately 24 h and returns to normal by day 3
Sepsis and PCT: The Pediatric Experience • Complicated by a physiological rise in both term and preterm, healthy infants, which peaks at approximately 24 h and returns to normal by day 3
 Sepsis and PCT: The Pediatric Experience • Variable in sensitivity and specificity • Some authors recommended against the use of PCT in routine diagnosis of bacterial sepsis in neonates, because of more complicated PCT measurement and its expense in comparison with CRP.
Sepsis and PCT: The Pediatric Experience • Variable in sensitivity and specificity • Some authors recommended against the use of PCT in routine diagnosis of bacterial sepsis in neonates, because of more complicated PCT measurement and its expense in comparison with CRP.
 Different features of CRP and PCT • CRP levels may not further increase during more severe stages of sepsis. • PCT rises the diagnosticto the severity of in proportion capacity of PCT is Therefore, sepsis andto that of CRP due to the close superior reaches its highest levels in septic shock. between PCT levels and the correlation severity of sepsis and outcome.
Different features of CRP and PCT • CRP levels may not further increase during more severe stages of sepsis. • PCT rises the diagnosticto the severity of in proportion capacity of PCT is Therefore, sepsis andto that of CRP due to the close superior reaches its highest levels in septic shock. between PCT levels and the correlation severity of sepsis and outcome.
 Different features of CRP and PCT • PCT reacted more quickly than CRP • PCT concentrations had their maximum Allows anticipation levels prior to those of CRP of a diagnosis of sepsis 24 -48 hours before the CRP level would Procalcitonin and C-reactive protein during systemic inflammatory response syndrome, sepsis and organ dysfunction Crit Care. 2004; 8(4): 234– 42.
Different features of CRP and PCT • PCT reacted more quickly than CRP • PCT concentrations had their maximum Allows anticipation levels prior to those of CRP of a diagnosis of sepsis 24 -48 hours before the CRP level would Procalcitonin and C-reactive protein during systemic inflammatory response syndrome, sepsis and organ dysfunction Crit Care. 2004; 8(4): 234– 42.

 Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
Sepsis markers • • Lactate C-reactive protein (CRP) Procalcitonin (PCT) Newer sepsis markers
 New sepsis markers • Soluble CD 14 subtype (Generic name. Presepsin) • Heparin-Binding protein • Others
New sepsis markers • Soluble CD 14 subtype (Generic name. Presepsin) • Heparin-Binding protein • Others
 Soluble CD 14 subtype
Soluble CD 14 subtype
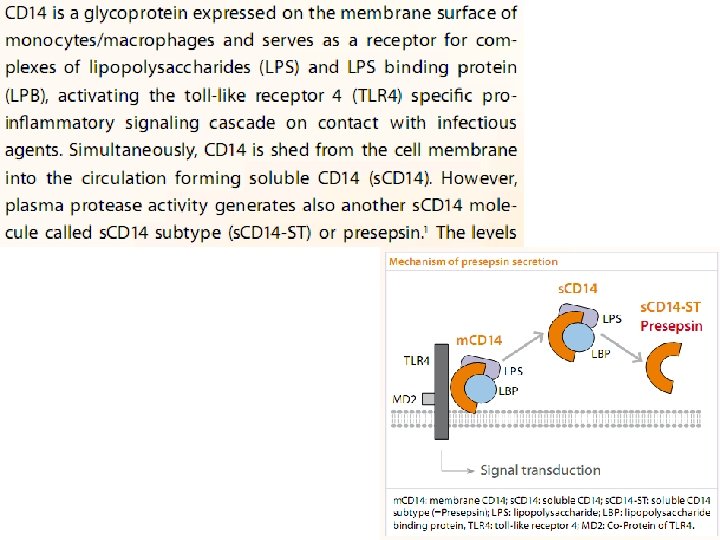
 Early diagnosis and prognosis
Early diagnosis and prognosis
 Early diagnosis and prognosis
Early diagnosis and prognosis
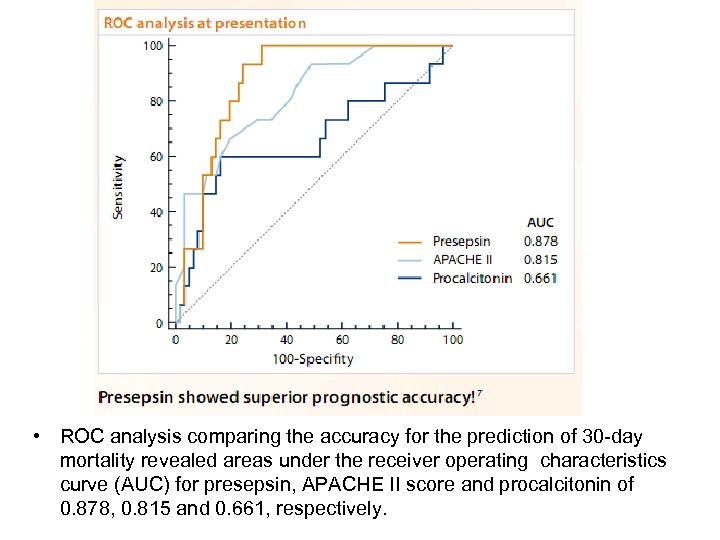 • ROC analysis comparing the accuracy for the prediction of 30 -day mortality revealed areas under the receiver operating characteristics curve (AUC) for presepsin, APACHE II score and procalcitonin of 0. 878, 0. 815 and 0. 661, respectively.
• ROC analysis comparing the accuracy for the prediction of 30 -day mortality revealed areas under the receiver operating characteristics curve (AUC) for presepsin, APACHE II score and procalcitonin of 0. 878, 0. 815 and 0. 661, respectively.

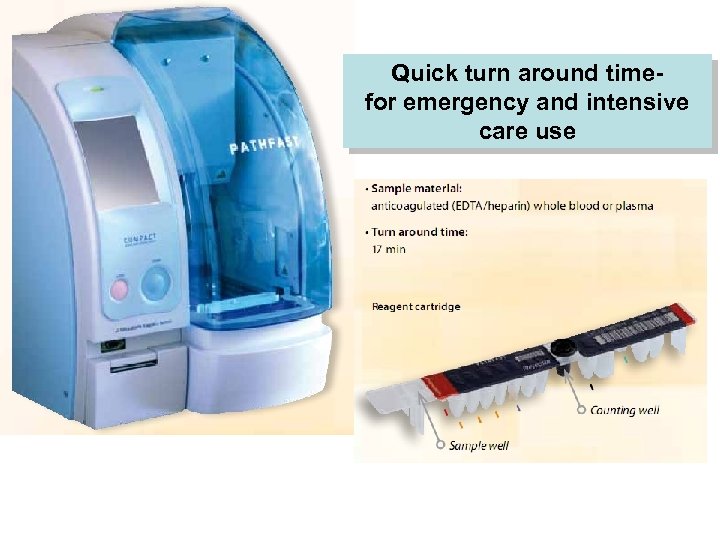 Quick turn around timefor emergency and intensive care use
Quick turn around timefor emergency and intensive care use
 Heparin-binding protein • An early marker of circulatory failure in sepsis • Release from activated neutrophils – A potent inducer of vascular leakage – Resulted in extravasation of plasma and WBC to the focus of infection
Heparin-binding protein • An early marker of circulatory failure in sepsis • Release from activated neutrophils – A potent inducer of vascular leakage – Resulted in extravasation of plasma and WBC to the focus of infection
 Clinical Infectious Diseases 2009; 49: 1044 -50
Clinical Infectious Diseases 2009; 49: 1044 -50
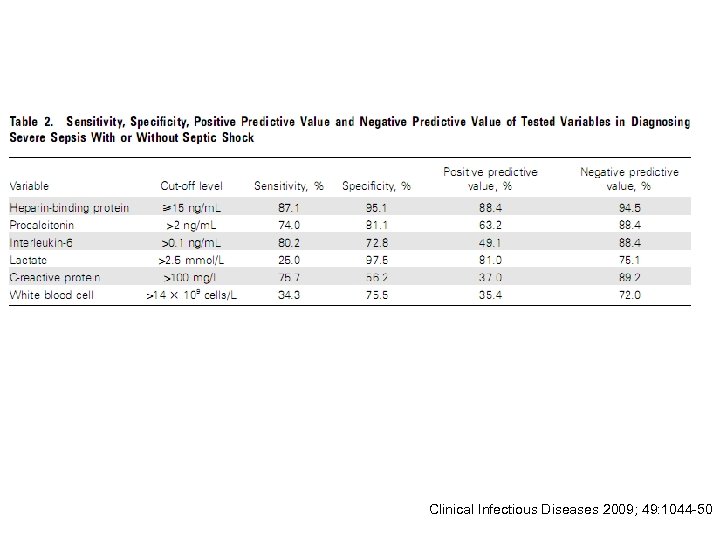 Clinical Infectious Diseases 2009; 49: 1044 -50
Clinical Infectious Diseases 2009; 49: 1044 -50
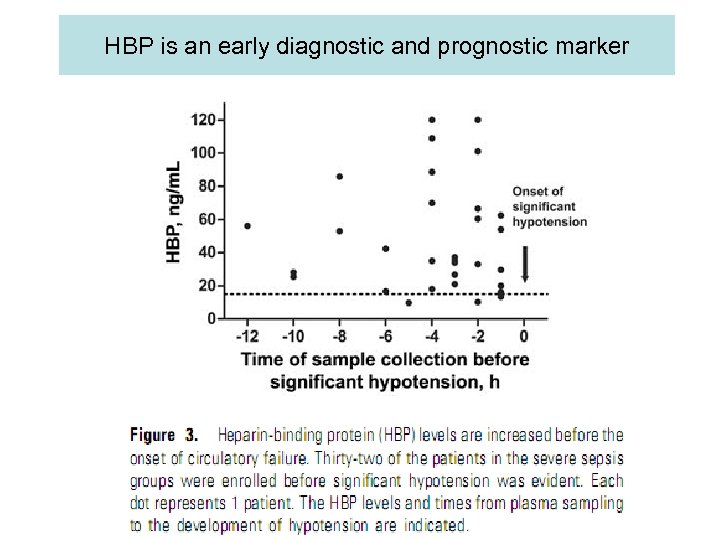 HBP is an early diagnostic and prognostic marker
HBP is an early diagnostic and prognostic marker
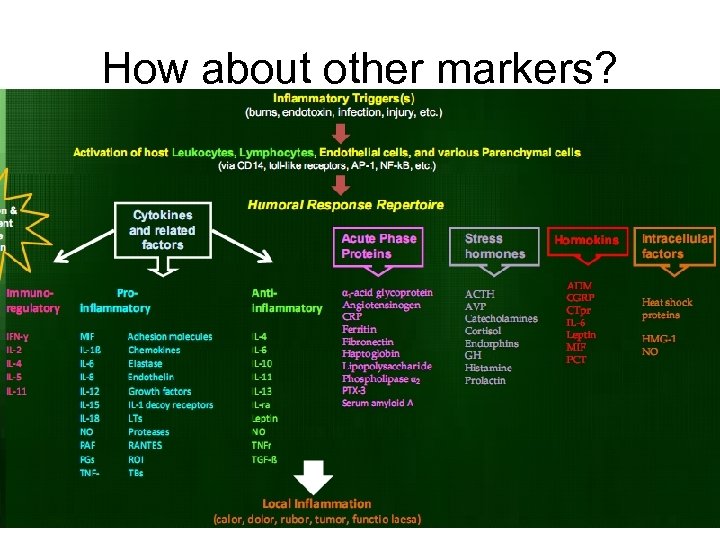 How about other markers?
How about other markers?
 • TNF-a – The initiating factor in the activation of host response and subsequent cytokine release during infection – Concentration increase 24 times after LPS challenge during in vivo experimental endotoxemia
• TNF-a – The initiating factor in the activation of host response and subsequent cytokine release during infection – Concentration increase 24 times after LPS challenge during in vivo experimental endotoxemia
 However, the diagnostic utility of TNF is insufficient for distinguishing infectious inflammation Why? • Short half-life of 17 min – Short-term concentration in response to bacterial challenge
However, the diagnostic utility of TNF is insufficient for distinguishing infectious inflammation Why? • Short half-life of 17 min – Short-term concentration in response to bacterial challenge
 • Interleukin-6 – – – Increased concentrations correlating to infection Activation time: very short Half-life time ~ 1 hr Sensitive early diagnosis of neonatal sepsis Adult values • Sepsis 300 -2700 ng/L • SIRS 100 ng/L – Usefulness in adult diagnosis has not well established. Interleukin-6 concentrations in neonatal sepsis. Lancet 353; 9148: 239 -40
• Interleukin-6 – – – Increased concentrations correlating to infection Activation time: very short Half-life time ~ 1 hr Sensitive early diagnosis of neonatal sepsis Adult values • Sepsis 300 -2700 ng/L • SIRS 100 ng/L – Usefulness in adult diagnosis has not well established. Interleukin-6 concentrations in neonatal sepsis. Lancet 353; 9148: 239 -40
 Conclusion • Sepsis is associated with significant mortality and morbidity • Sepsis markers can aid in the diagnosis of sepsis • It may provide prognostic value • Many new sepsis markers are under investigation
Conclusion • Sepsis is associated with significant mortality and morbidity • Sepsis markers can aid in the diagnosis of sepsis • It may provide prognostic value • Many new sepsis markers are under investigation
 • Procalcitonin is a well-established biomarker of sepsis that fulfills several criteria of clinical needs – it responds both to infection and severity of infection – antibiotic treatment can also be guided by PCT – Prognostic value
• Procalcitonin is a well-established biomarker of sepsis that fulfills several criteria of clinical needs – it responds both to infection and severity of infection – antibiotic treatment can also be guided by PCT – Prognostic value
 Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock: 2008. Critical Care Medicine 2008; 36: 269 -327
Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock: 2008. Critical Care Medicine 2008; 36: 269 -327
 The End Thank you
The End Thank you


 Different features of CRP and PCT • CRP concentrations were high already during the less severe stages of organ dysfunction and systemic inflammation – values useful much further increased during the CRP less were not in distinguishing evolution of more severe stages of disease. sepsis in severe sepsis and septic shock • PCT levels correlates with the stages of disease (especially increased in patients with organ dysfunction, severe sepsis or septic shock. ) Procalcitonin and C-reactive protein during systemic inflammatory response syndrome, sepsis and organ dysfunction Crit Care. 2004; 8(4): 234– 42.
Different features of CRP and PCT • CRP concentrations were high already during the less severe stages of organ dysfunction and systemic inflammation – values useful much further increased during the CRP less were not in distinguishing evolution of more severe stages of disease. sepsis in severe sepsis and septic shock • PCT levels correlates with the stages of disease (especially increased in patients with organ dysfunction, severe sepsis or septic shock. ) Procalcitonin and C-reactive protein during systemic inflammatory response syndrome, sepsis and organ dysfunction Crit Care. 2004; 8(4): 234– 42.
 Different features of CRP and PCT • PCT concentrations more rapidly declined as compared with CRP remained high even in the late stage of disease Procalcitonin and C-reactive protein during systemic inflammatory response syndrome, sepsis and organ dysfunction Crit Care. 2004; 8(4): 234– 42.
Different features of CRP and PCT • PCT concentrations more rapidly declined as compared with CRP remained high even in the late stage of disease Procalcitonin and C-reactive protein during systemic inflammatory response syndrome, sepsis and organ dysfunction Crit Care. 2004; 8(4): 234– 42.
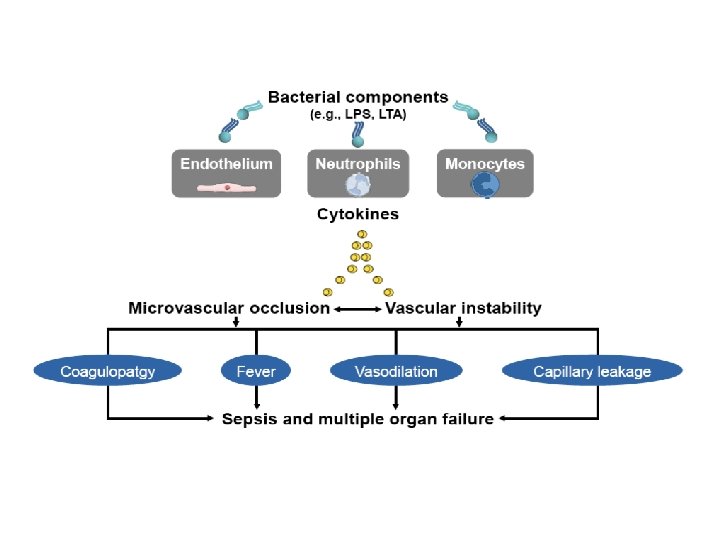
 Prognosis • PCT levels were significantly associated with – – admission to a special care unit duration of intravenous antibiotic use total duration of antibiotic treatment length of hospital stay, whereas CRP was related only to the latter two variables. • These data suggest that PCT may be a valuable addition to currently used markers of infection for diagnosis of infection and prognosis in patients with fever at the AED Critical Care Med 2010; 38: 457– 463
Prognosis • PCT levels were significantly associated with – – admission to a special care unit duration of intravenous antibiotic use total duration of antibiotic treatment length of hospital stay, whereas CRP was related only to the latter two variables. • These data suggest that PCT may be a valuable addition to currently used markers of infection for diagnosis of infection and prognosis in patients with fever at the AED Critical Care Med 2010; 38: 457– 463
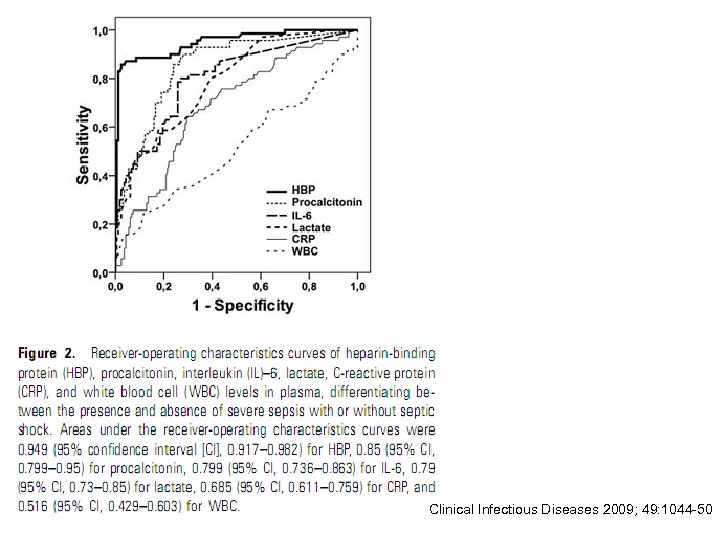 Clinical Infectious Diseases 2009; 49: 1044 -50
Clinical Infectious Diseases 2009; 49: 1044 -50