57d39f6f90ec28bc0f57a774ebf1915a.ppt
- Количество слайдов: 26


Selecting Patients Best Suited for CEA Nick Hopkins MD Mandy Binning MD Elad Levy MD Adnan Siddiqui MD, Ph. D Dept of Neurosurgery SUNY Buffalo

DISCLOSURES L. Nelson Hopkins, MD Consulting Fees – Abbott Vascular, Bard Peripheral Vascular, Boston Scientific Corporation, Micrus Endovascular Cordis, a Johnson & Johnson company Grants/Contracted Research – Cordis, a Johnson & Johnson company, Boston Scientific Corporation, Micrus Endovascular Honoraria – Access. Closure, Inc. , Bard Peripheral Vascular, Boston Scientific Corporation, Cordis, a Johnson & Johnson company, market. Rx, Inc. , Micrus Endovascular, Medsn Ownership Interest (Stocks, Stock Options or Other Ownership Interest) – APW Holding, Inc. , Boston Scientific Corporation, Magellan Spine Tech, Inc. , Med. Focus Accelerator Fund, Micrus Endovascular
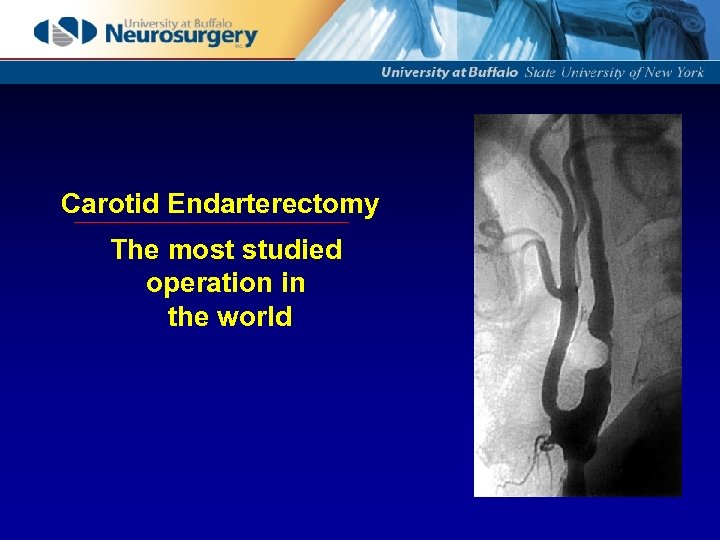
Carotid Endarterectomy The most studied operation in the world

CEA • CEA is effective in reducing risk of stroke in carefully selected patients with symptomatic carotid stenosis ≥ 50% or asymptomatic carotid stenosis ≥ 70% • Many variations on CEA technique are in use, but none have been proven to be superior • Certain subgroups are at higher risk of complications with CEA

Symptomatic Carotid Stenosis • NASCET − 70 -99% stenosis: 17% (26 to 9%)ARR (65% RRR) / 2 yrs − 50 -69% stenosis: 6. 5% ARR (29% RRR) / 5 yrs − <50% stenosis: no benefit − Favors CEA for 50 -99% symptomatic stenosis − 13. 1% vs. 2. 5% with CEA for major ipsilat. CVA • ECST (reanalysis by NASCET criteria, Lancet 2003; 34: 514) − 3, 024 pts w/ TIA, retinal infarction, or non-disabling stroke within 6 months − 70 -99% stenosis: 21. 2% ARR / 5 yrs − 50 -69% stenosis: 5. 7% ARR / 5 yrs − <50% stenosis: no benefit (harm if <30% stenosis)

Outcome after CEA depends on risk for perioperative complications • NASCET: 30 -day rate of disabling stroke and death was 2. 9% • ECST 30 -day rates − disabling stroke: 2. 5% − death: 1. 0%

Asymptomatic RCT’s: Best Med Tx ± CEA ACAS (JAMA 1995; 273: 1421) 1, 662 pts w/ angio or validated doppler > 60% 5. 9% ARR (53% RRR) / 5 yrs required low surgical M&M (1. 5%) no stat. sig. benefit for women ACST (Lancet 2004; 363: 1491) 3120 pts w/ doppler > 60% stenosis 5. 4% ARR (11. 8→ 6. 4% risk) / 5 yrs results more robust than ACAS surgical M&M (3. 0%)

AHA Recommendations • CEA in symptomatic patients should be undertaken by surgeons whose surgical morbidity and mortality rate is <6% Moore et al. , Stroke 26: 188 -201, 1995

− High-Risk features for CEA − Anatomical − C 2 and higher lesion − Contralateral carotid occlusion / stenosis (is relative) − Severe ulceration − Tandem intracranial stenosis − Functional − Age > 80 (some say 75) − Active coronary artery disease (before intervention) − Recent major stroke in reference vascular territory

AHA Recommendations • CEA in asymptomatic patients should be undertaken by surgeons whose surgical morbidity and mortality rate is <3% Moore et al. , Stroke 26: 188 -201, 1995

Patient Evaluation • CEA is most effective when patients are selected appropriately • NASCET, ECST, VACS: patient eligibility was based on angiographic criteria • Furthermore, CEA in asymptomatic patients carries a narrow risk-benefit ratio, making accurate patient selection essential

Carotid Duplex Ultrasonography: Limitations • Significant proportion of CEAs are performed in centers without designated, accredited vascular labs Goldstein Stroke 26: 1607 -1615, 1995 • Even accredited, high-volume vascular labs may report false-positive results for carotid stenosis in 20 -41% of cases Qureshi Stroke 32: 2287 -2291, 2001 • Duplex scanning cannot accurately distinguish preocclusive disease from total occlusion Dawson J Vasc Surg 18: 673 -683, 1993 • Duplex scanning does not indicate whether the lesion is relatively high in the cervical region, which is information that is important for surgical planning • Duplex scanning does not image the intracranial vasculature

Radiographic Evaluation • Doppler alone is NOT enough • MRA or CTA + Doppler ok if congruent • Angio still gold standard for anatomy and collateral circulation
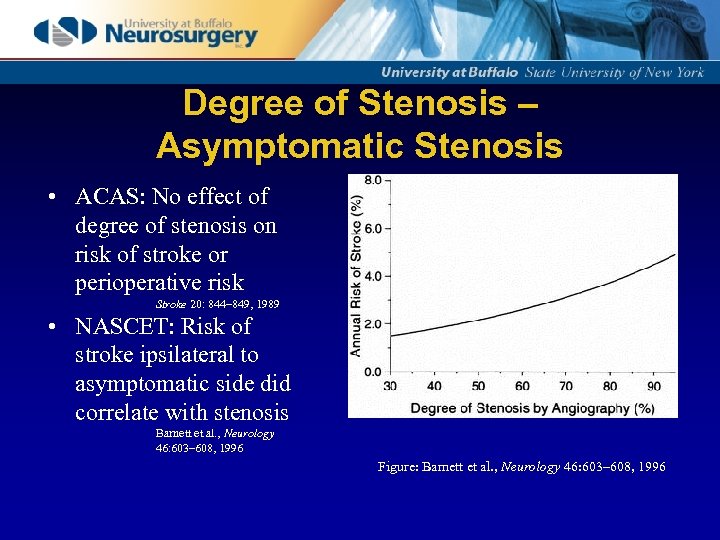
Degree of Stenosis – Asymptomatic Stenosis • ACAS: No effect of degree of stenosis on risk of stroke or perioperative risk Stroke 20: 844– 849, 1989 • NASCET: Risk of stroke ipsilateral to asymptomatic side did correlate with stenosis Barnett et al. , Neurology 46: 603– 608, 1996 Figure: Barnett et al. , Neurology 46: 603– 608, 1996

Multicenter Review of Preoperative Risk Factors for CEA in Patients with Symptomatic Stenosis • • • 1, 160 CEAs performed at 12 academic medical centers 697 patients with ipsilateral symptoms 8. 5% had either stroke, MI, or died during the postoperative period of hospitalization. Those >75 yo had a greater risk of MI (6. 6% vs 2. 3%, P=. 024) but not of stroke or death (P>. 10) Variables with >90% probability of being associated with adverse outcomes − age ≥ 75 years − angiographic evidence of − ipsilateral carotid occlusion − stenosis in the region of the carotid siphon − intraluminal thrombus Goldstein et al. , Stroke 25: 2096 -2097, 1994

Endarterectomy in the Elderly • 11, 973 CEAs • No significant difference in stroke rate in patients aged < or > 75 yo • Mortality 2. 14% in >75 yo vs 0. 88% in <75 yo (P =. 0001) Maxwell et al. , Am J Surg 1997; 174: 655 -660

Heart Disease • Patients with coronary artery disease are also at an elevated risk of perioperative stroke and death, with an incidence as high as 40% Ferguson et al. , Stroke 24: 1285 -1291, 1993

Subgroup Analysis: Ulcerated Plaque • NASCET: Risk of perioperative stroke or death was 1. 5 times higher in the presence of an ipsilateral ulcerated plaque Ferguson et al. , Stroke 30: 1751 -1758, 1999

Intracranial Stenosis • ACAS: Presence of contralateral carotid siphon stenosis was associated with a significantly higher risk of perioperative stroke after CEA Young et al. Stroke 27: 2216 -2224, 1996

Contralateral Occlusion • NASCET: Perioperative risk of stroke and death is increased in the presence of contralateral carotid occlusion (14. 3% vs. 4. 0%) Gasecki et al. J Neurosurg 83: 778 -782, 1995
Absence of Collateral Circulation • NASCET: Risk of perioperative stroke in patients with an absence of collaterals on angiography is increased by a factor of 4 (4. 9% vs. 1. 1%) Henderson et al. Stroke 31: 128 -132, 2000

Intraluminal Thrombus • NASCET: 30 -day stroke risk for CEA in patients with an intraluminal thrombus was 12. 0% Villareal et al. , Stroke 29: 276, 1998

CAS Risk Factors CEA a Better Alternative than CAS + Filter 1. Sx (hot) lesion… 2. Elderly pts… ? ? 3. Low GSM… 4. Multiple stents… 5. Duration Filter… 6. Pre dil without EP … 7. Tortuousity- severe… 8. Concentric calcium… 9. Aortic Arch disease… 10. Renal Failure. . .

Conclusions • • CEA: a good operation CEA: great alternative for most high risk CAS pts Acceptable risk: 3% Asx and 6% Sx CEA Risk factors/pts to avoid CEA − Body habitus, high & low lesions − Medical comorbitities: cardiac, resp − Hostile neck − Severe intracranial ds/poor collateral circulation − Neurologic instability

Thank you
57d39f6f90ec28bc0f57a774ebf1915a.ppt