8b4740d98e2db237bcba9865eb9ce2d1.ppt
- Количество слайдов: 36
 Schizophrenia Professor Sari Gilman Aronson Professor William Greenough Medical Behavioral Sciences
Schizophrenia Professor Sari Gilman Aronson Professor William Greenough Medical Behavioral Sciences
 A Few Historical Tidbits 1952 Chlorpromazine noted to ameliorate psychosis late 1950 s Widespread clinical use of chlorpromazine 1967 Haloperidol released in the United States 1975 CT scan technology in clinical use (EMI scan) 1985 MRI scan technology in clinical use 1990 s “Atypical” antipsychotics released
A Few Historical Tidbits 1952 Chlorpromazine noted to ameliorate psychosis late 1950 s Widespread clinical use of chlorpromazine 1967 Haloperidol released in the United States 1975 CT scan technology in clinical use (EMI scan) 1985 MRI scan technology in clinical use 1990 s “Atypical” antipsychotics released
 PSYCHOACTIVE DRUGS Drugs have revolutionized psychiatric treatment since the 1950's. Most psychoactive drugs act stereospecifically on receptors, enzymes, or other active protein elements of the nerve cell (e. g. , ion channnels, blocked by local anesthetics). Existence of a drug can lead to discovery of a mechanism (e. g. , opiates, salicylates, chlorpromazine). The majority of psychoactive drugs affect synaptic transmission. Drugs can have synergystic (combinatorial) interactions with other drugs. (Some may be good, many are bad) Many drugs have side effects (We will talk about tardive dyskinesia, a side effect of long term treatment with antipsychotic drugs).
PSYCHOACTIVE DRUGS Drugs have revolutionized psychiatric treatment since the 1950's. Most psychoactive drugs act stereospecifically on receptors, enzymes, or other active protein elements of the nerve cell (e. g. , ion channnels, blocked by local anesthetics). Existence of a drug can lead to discovery of a mechanism (e. g. , opiates, salicylates, chlorpromazine). The majority of psychoactive drugs affect synaptic transmission. Drugs can have synergystic (combinatorial) interactions with other drugs. (Some may be good, many are bad) Many drugs have side effects (We will talk about tardive dyskinesia, a side effect of long term treatment with antipsychotic drugs).
 1. The Natural History of Schizophrenia • Generally an insidious onset. • Possible history of complications during pregnancy and birth. • History in early adolescence of excessive shyness, social awkwardness, withdrawal from social relationships, inability to form friendships, sometimes academic difficulties. • Onset of acute psychosis in late adolescence or early adulthood. Symptoms may be brief or vague. Infrequent onset after age 40. • Variable course among patients. Episodes of acute psychosis superimposed on baseline functioning. Baseline function may show residual symptoms or patient may be in remission. .
1. The Natural History of Schizophrenia • Generally an insidious onset. • Possible history of complications during pregnancy and birth. • History in early adolescence of excessive shyness, social awkwardness, withdrawal from social relationships, inability to form friendships, sometimes academic difficulties. • Onset of acute psychosis in late adolescence or early adulthood. Symptoms may be brief or vague. Infrequent onset after age 40. • Variable course among patients. Episodes of acute psychosis superimposed on baseline functioning. Baseline function may show residual symptoms or patient may be in remission. .
 2. The Natural History of Schizophrenia • Good prognosis associated with: · acute onset · past high functioning and excellent interpersonal adjustment · good response to antipsychotic medications · absence of negative symptoms · absence of a secondary affective disorder (depression or mania) • In a sample of 200 patients followed after 30 years of disease · 20% asymptomatic · 25% moderate symptoms · 55% severe symptoms
2. The Natural History of Schizophrenia • Good prognosis associated with: · acute onset · past high functioning and excellent interpersonal adjustment · good response to antipsychotic medications · absence of negative symptoms · absence of a secondary affective disorder (depression or mania) • In a sample of 200 patients followed after 30 years of disease · 20% asymptomatic · 25% moderate symptoms · 55% severe symptoms
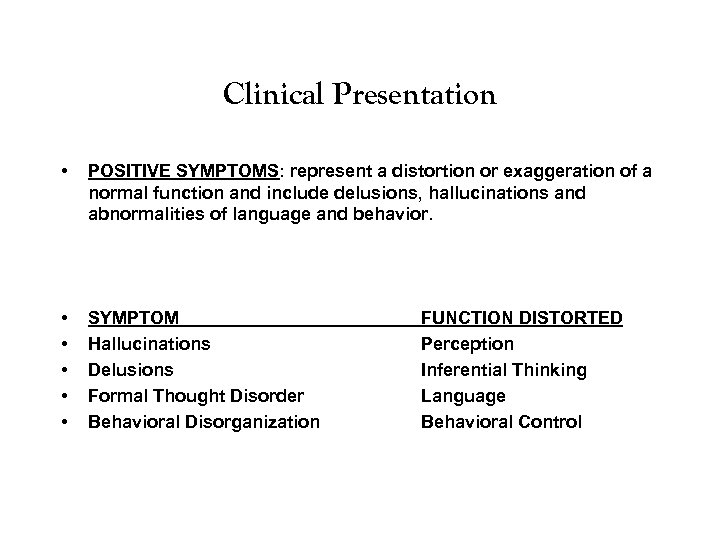 Clinical Presentation • POSITIVE SYMPTOMS: represent a distortion or exaggeration of a normal function and include delusions, hallucinations and abnormalities of language and behavior. • • • SYMPTOM Hallucinations Delusions Formal Thought Disorder Behavioral Disorganization FUNCTION DISTORTED Perception Inferential Thinking Language Behavioral Control
Clinical Presentation • POSITIVE SYMPTOMS: represent a distortion or exaggeration of a normal function and include delusions, hallucinations and abnormalities of language and behavior. • • • SYMPTOM Hallucinations Delusions Formal Thought Disorder Behavioral Disorganization FUNCTION DISTORTED Perception Inferential Thinking Language Behavioral Control
 Clinical Presentation • NEGATIVE SYMPTOMS: represent a diminution or loss of function including poverty of speech and content of speech (alogia), affective blunting, asociality, anhedonia, and avolition. • • • SYMPTOM Alogia Affective Blunting Avolition-Asociality Anhedonia Attentional Impairment FUNCTION LOST Fluency of speech Emotional Expression Volition and drive Hedonic capacity Attention
Clinical Presentation • NEGATIVE SYMPTOMS: represent a diminution or loss of function including poverty of speech and content of speech (alogia), affective blunting, asociality, anhedonia, and avolition. • • • SYMPTOM Alogia Affective Blunting Avolition-Asociality Anhedonia Attentional Impairment FUNCTION LOST Fluency of speech Emotional Expression Volition and drive Hedonic capacity Attention
 Diagnosis of Schizophrenia (1) DSM-IV Diagnostic Criteria (Abbreviated) • Characteristic symptoms: Two or more of the following, each present for a significant portion of the time during a 1 month period (or less if successfully treated): – delusions – hallucinations – disorganized speech (e. g. frequent derailment or incoherence) – grossly disorganized or catatonic behavior – negative symptoms, i. e. , affective flattening, alogia, or avolition • Social/occupational dysfunction: For a significant portion of the time since the onset of the disturbance, one or more major areas of functioning such as work, interpersonal relations, or self-care markedly below the level achieved prior to the onset (or when the onset is in childhood or adolescence, failure to achieve expected level of interpersonal, academic, or occupational achievement).
Diagnosis of Schizophrenia (1) DSM-IV Diagnostic Criteria (Abbreviated) • Characteristic symptoms: Two or more of the following, each present for a significant portion of the time during a 1 month period (or less if successfully treated): – delusions – hallucinations – disorganized speech (e. g. frequent derailment or incoherence) – grossly disorganized or catatonic behavior – negative symptoms, i. e. , affective flattening, alogia, or avolition • Social/occupational dysfunction: For a significant portion of the time since the onset of the disturbance, one or more major areas of functioning such as work, interpersonal relations, or self-care markedly below the level achieved prior to the onset (or when the onset is in childhood or adolescence, failure to achieve expected level of interpersonal, academic, or occupational achievement).
 Diagnosis of Schizophrenia (2) DSM-IV Diagnostic Criteria (Abbreviated) • Continuous signs of the disturbance for at least 6 months. This 6 month period must include at least 1 month of symptoms (or less if successfully treated) that meet Criterion A, and may include prodromal or residual symptoms (Criterion A symptoms manifested in attenuated form or negative symptoms present). • Symptoms not due to Schizoaffective Disorder or a Mood Disorder. • Symptoms not due to a general medical condition.
Diagnosis of Schizophrenia (2) DSM-IV Diagnostic Criteria (Abbreviated) • Continuous signs of the disturbance for at least 6 months. This 6 month period must include at least 1 month of symptoms (or less if successfully treated) that meet Criterion A, and may include prodromal or residual symptoms (Criterion A symptoms manifested in attenuated form or negative symptoms present). • Symptoms not due to Schizoaffective Disorder or a Mood Disorder. • Symptoms not due to a general medical condition.
 Subtypes of Schizophrenia (1) • Paranoid Type · preoccupation with one or more delusions or frequent auditory hallucinations · no disorganized speech, disorganized or catatonic behavior, or flat or inappropriate affect • Disorganized Type · Prominent disorganized speech, disorganized behavior, flat or inappropriate behavior · does not meet criteria for Catatonic Type • • Catatonic Type clinical picture dominated by at least 2 of the following: · motoric immobility as evidenced by catalepsy (body remains in one position) or stupor · excessive motor activity that is apparently purposeless and not influenced by external stimuli · extreme negativism (apparently motiveless resistance to all instructions or maintenance of rigid posture against attempts to be moved) or mutism · peculiarities of voluntary movement as evidenced by posturing (voluntary assumption of inappropriate or bizarre postures), stereotyped movements, prominent mannerisms, or prominent grimacing · echolalia or echopraxia
Subtypes of Schizophrenia (1) • Paranoid Type · preoccupation with one or more delusions or frequent auditory hallucinations · no disorganized speech, disorganized or catatonic behavior, or flat or inappropriate affect • Disorganized Type · Prominent disorganized speech, disorganized behavior, flat or inappropriate behavior · does not meet criteria for Catatonic Type • • Catatonic Type clinical picture dominated by at least 2 of the following: · motoric immobility as evidenced by catalepsy (body remains in one position) or stupor · excessive motor activity that is apparently purposeless and not influenced by external stimuli · extreme negativism (apparently motiveless resistance to all instructions or maintenance of rigid posture against attempts to be moved) or mutism · peculiarities of voluntary movement as evidenced by posturing (voluntary assumption of inappropriate or bizarre postures), stereotyped movements, prominent mannerisms, or prominent grimacing · echolalia or echopraxia
 Subtypes of Schizophrenia (2) • • Undifferentiated Type Symptoms are met for Criterion A, but criteria are not met for Paranoid, Disorganized or Catatonic Types • Residual Type · Absence of prominent delusions, hallucinations, disorganized speech and grossly disorganized or catatonic behavior · Continuing evidence of disturbance as indicated by presence of negative symptoms or 2 or more Criterion A symptoms present in an attenuated form (odd beliefs, unusual perceptual experiences).
Subtypes of Schizophrenia (2) • • Undifferentiated Type Symptoms are met for Criterion A, but criteria are not met for Paranoid, Disorganized or Catatonic Types • Residual Type · Absence of prominent delusions, hallucinations, disorganized speech and grossly disorganized or catatonic behavior · Continuing evidence of disturbance as indicated by presence of negative symptoms or 2 or more Criterion A symptoms present in an attenuated form (odd beliefs, unusual perceptual experiences).
 Case Daniel is an 18 year old white middle class male brought to the hospital emergency room by his parents. His parents were concerned that Daniel had been acting strangely lately, although Daniel denied any problem saying, "I've seen the light. " Daniel lives with his parents and is a sophomore at a local college. He has always been a good student, but his grades fell significantly one month ago. He has always been a rather quiet child, but seemed to socialize well with other children until about age 12. At that time, he began to withdraw from friends and family, choosing to spend alot of time alone in his room. He enjoyed reading and playing guitar. He told the examiner that he liked to read fantasy novels and that he thought highly of John Lennon. His parents said that Daniel never dated and in fact seemed intimidated by girls. Daniel stated, "females are the right hand of the devil" but he would not elaborate on that thought. His parents began to feel more concern 8 months ago during the first semester of his freshman year in college as he seemed even more withdrawn from them than usual. He also began talking about John Lennon more frequently, telling his parents that John "knew the way" and that he needed to "find his meaning in this meaningless world". Within the past two months, Daniel seemed even more preoccupied with concerns of life and death and has stopped going to class. His parents became alarmed when he told them this morning that he believes that he can communicate with John Lennon by getting John’s “karma in my mind”. In addition, he told them that “I am becoming the walrus…I can use my tusks to read the waters of life. ” Daniel has not slept or eaten for the past two days. Daniel and his parents stated that he had never used drugs or alcohol. Daniel is the eldest of 3 children with siblings age 15 and 11. He has never been seriously ill and has no history of head injury, seizures, fever, or toxic exposure. His development as an infant and young child was unremarkable except for the problems noted previously. His family denies a family history of psychiatric disorder, but remembered a maternal cousin who was unusual and spent much of his later life living alone. There was a family story about how this man used to collect thousands of magazines and lock himself in his house for months.
Case Daniel is an 18 year old white middle class male brought to the hospital emergency room by his parents. His parents were concerned that Daniel had been acting strangely lately, although Daniel denied any problem saying, "I've seen the light. " Daniel lives with his parents and is a sophomore at a local college. He has always been a good student, but his grades fell significantly one month ago. He has always been a rather quiet child, but seemed to socialize well with other children until about age 12. At that time, he began to withdraw from friends and family, choosing to spend alot of time alone in his room. He enjoyed reading and playing guitar. He told the examiner that he liked to read fantasy novels and that he thought highly of John Lennon. His parents said that Daniel never dated and in fact seemed intimidated by girls. Daniel stated, "females are the right hand of the devil" but he would not elaborate on that thought. His parents began to feel more concern 8 months ago during the first semester of his freshman year in college as he seemed even more withdrawn from them than usual. He also began talking about John Lennon more frequently, telling his parents that John "knew the way" and that he needed to "find his meaning in this meaningless world". Within the past two months, Daniel seemed even more preoccupied with concerns of life and death and has stopped going to class. His parents became alarmed when he told them this morning that he believes that he can communicate with John Lennon by getting John’s “karma in my mind”. In addition, he told them that “I am becoming the walrus…I can use my tusks to read the waters of life. ” Daniel has not slept or eaten for the past two days. Daniel and his parents stated that he had never used drugs or alcohol. Daniel is the eldest of 3 children with siblings age 15 and 11. He has never been seriously ill and has no history of head injury, seizures, fever, or toxic exposure. His development as an infant and young child was unremarkable except for the problems noted previously. His family denies a family history of psychiatric disorder, but remembered a maternal cousin who was unusual and spent much of his later life living alone. There was a family story about how this man used to collect thousands of magazines and lock himself in his house for months.
 Mental Status Evaluation The Mental Status Evaluation (MSE) is an assessment of a patient’s appearance, behavior, speech, mood, affect, thought content, thought process, orientation, memory and other cognitive functioning, judgement and insight at one point in time. A MSE can change quickly if the patient’s functioning is fluctuating, such as when a patient is delirious. The MSE will be covered in detail in the second year psychiatry course. Daniel’s MSE is presented to clarify his symptoms. Daniel was dressed in tattered blue jeans, a V-neck sweater without a shirt and loafers without socks. He was unshaven and looked tired although he remained alert throughout the interview. He did not want to sit down in a chair but preferred to stand near the door, often turning his head towards it when there was some noise in the hallway. He was distant and made poor eye contact with the examiner. Daniel looked at his watch or at a book about John Lennon which he had brought with him. His speech was somewhat slowed and quiet. He seemed mildly agitated, standing still then pacing for a few minutes. Daniel did not want to describe his mood. His affect was blunted and he expressed little emotion. He denied depression and suicidal thoughts. Daniel was reluctant to discuss his thoughts. He did talk about his interest in Lennon's life as a "guide" for him, but denied thinking about dying or joining John. On one occasion, he said that he was worried that he might be killed by someone who "fought the principles of God and Lennon". Daniel had thought blocking on several occasions and had loose associations. Daniel was very guarded and suspicious and seemed to be attending to internal stimuli. At one point during the interview, he mumbled something softly but would not discuss it with the examiner. He was alert and oriented with no fluctuations in consciousness. His attention was poor as a result of his preoccupation with himself. He knew the names of 6 past presidents, was familiar with current events, and did not seem to be impaired intellectually. Daniel did not want to perform any tests of memory saying, "that's stupid- there is nothing wrong with my memory". He had little insight into his problem and showed poor judgement, i. e. "it really doesn't matter if I eat as God will provide sustenance for me".
Mental Status Evaluation The Mental Status Evaluation (MSE) is an assessment of a patient’s appearance, behavior, speech, mood, affect, thought content, thought process, orientation, memory and other cognitive functioning, judgement and insight at one point in time. A MSE can change quickly if the patient’s functioning is fluctuating, such as when a patient is delirious. The MSE will be covered in detail in the second year psychiatry course. Daniel’s MSE is presented to clarify his symptoms. Daniel was dressed in tattered blue jeans, a V-neck sweater without a shirt and loafers without socks. He was unshaven and looked tired although he remained alert throughout the interview. He did not want to sit down in a chair but preferred to stand near the door, often turning his head towards it when there was some noise in the hallway. He was distant and made poor eye contact with the examiner. Daniel looked at his watch or at a book about John Lennon which he had brought with him. His speech was somewhat slowed and quiet. He seemed mildly agitated, standing still then pacing for a few minutes. Daniel did not want to describe his mood. His affect was blunted and he expressed little emotion. He denied depression and suicidal thoughts. Daniel was reluctant to discuss his thoughts. He did talk about his interest in Lennon's life as a "guide" for him, but denied thinking about dying or joining John. On one occasion, he said that he was worried that he might be killed by someone who "fought the principles of God and Lennon". Daniel had thought blocking on several occasions and had loose associations. Daniel was very guarded and suspicious and seemed to be attending to internal stimuli. At one point during the interview, he mumbled something softly but would not discuss it with the examiner. He was alert and oriented with no fluctuations in consciousness. His attention was poor as a result of his preoccupation with himself. He knew the names of 6 past presidents, was familiar with current events, and did not seem to be impaired intellectually. Daniel did not want to perform any tests of memory saying, "that's stupid- there is nothing wrong with my memory". He had little insight into his problem and showed poor judgement, i. e. "it really doesn't matter if I eat as God will provide sustenance for me".
 Questions And Discussion Points • What psychiatric problem is Daniel experiencing? • . Schizophrenia, probably paranoid • . Key Diagnostic Features of Schizophrenia –At least 2 psychotic features present for at least a month » . Hallucinations » . Delusions » . Disorganized speech: incoherence, frequent derailment » . Grossly disorganized or catatonic behavior » . Negative symptoms: affective blunting, anhedonia, lack of motivation –Impairment in social or occupational functioning or self-care –Duration for at least 6 months with 1 month of active symptoms (unless treated) –Symptoms not due to a mood disorder or schizoaffective disorder –Symptoms not due to a medical, neurological or substance use disorder » (Schizoaffective disorder usually diagnosed when manic or depressive symptoms are prominent and consistent part of patient’s long term psychotic illness) • . Diagnostic Subtypes of Schizophrenia –The diagnosis of schizophrenia also contains the related issue of subtypes of schizophrenia. The purpose of defining subtypes is to improve predictive validity and subsequent treatment. Subtypes identified in DSM- IV include: » . Catatonic: motor abnormalities such as rigidity and posturing » . Disorganized: disorganized speech and behavior, flat affect » . Paranoid: paranoid symptoms in the absence of catatonic or disorganized features » . Undifferentiated: some combination of the above
Questions And Discussion Points • What psychiatric problem is Daniel experiencing? • . Schizophrenia, probably paranoid • . Key Diagnostic Features of Schizophrenia –At least 2 psychotic features present for at least a month » . Hallucinations » . Delusions » . Disorganized speech: incoherence, frequent derailment » . Grossly disorganized or catatonic behavior » . Negative symptoms: affective blunting, anhedonia, lack of motivation –Impairment in social or occupational functioning or self-care –Duration for at least 6 months with 1 month of active symptoms (unless treated) –Symptoms not due to a mood disorder or schizoaffective disorder –Symptoms not due to a medical, neurological or substance use disorder » (Schizoaffective disorder usually diagnosed when manic or depressive symptoms are prominent and consistent part of patient’s long term psychotic illness) • . Diagnostic Subtypes of Schizophrenia –The diagnosis of schizophrenia also contains the related issue of subtypes of schizophrenia. The purpose of defining subtypes is to improve predictive validity and subsequent treatment. Subtypes identified in DSM- IV include: » . Catatonic: motor abnormalities such as rigidity and posturing » . Disorganized: disorganized speech and behavior, flat affect » . Paranoid: paranoid symptoms in the absence of catatonic or disorganized features » . Undifferentiated: some combination of the above
 List the symptoms that Daniel is experiencing • delusions • probable hallucinations • social withdrawal • decreased sleep and appetite • impairment in functioning in school • agitation • blunted affect • thought blocking • loose associations • little insight and poor judgement
List the symptoms that Daniel is experiencing • delusions • probable hallucinations • social withdrawal • decreased sleep and appetite • impairment in functioning in school • agitation • blunted affect • thought blocking • loose associations • little insight and poor judgement
 Treatment Daniel was offered hospitalization which he initially refused, but decided to accept after some discussion. He said, “I’ll come in to be sure that no one shoot me like they did John…he warned me that something bad might happen. ” His medical work-up showed a healthy 18 year old male. He was started on haloperidol 5 mg at bedtime and discharged in 5 days to his parents home. He was seen weekly by a psychiatrist in the outpatient clinic. Within 5 days of starting medication, he was sleeping better and gaining weight. After 2 weeks, he seemed calmer, but still talked about his connection to John Lennon. His haloperidol was held at this dose for 2 more weeks as research has shown that low dose treatment takes longer to work, but is easier for patients to tolerate. Within a month, he no longer seemed to be hallucinating and was more interactive. His delusions had “softened” and he seemed less fearful of being hurt. After 4 months of treatment, Daniel stated, “I don’t think about John Lennon much anymore. He is still important to me, but my mind took off on its own”. He was much improved, but still was socially withdrawn and had a blunted affect.
Treatment Daniel was offered hospitalization which he initially refused, but decided to accept after some discussion. He said, “I’ll come in to be sure that no one shoot me like they did John…he warned me that something bad might happen. ” His medical work-up showed a healthy 18 year old male. He was started on haloperidol 5 mg at bedtime and discharged in 5 days to his parents home. He was seen weekly by a psychiatrist in the outpatient clinic. Within 5 days of starting medication, he was sleeping better and gaining weight. After 2 weeks, he seemed calmer, but still talked about his connection to John Lennon. His haloperidol was held at this dose for 2 more weeks as research has shown that low dose treatment takes longer to work, but is easier for patients to tolerate. Within a month, he no longer seemed to be hallucinating and was more interactive. His delusions had “softened” and he seemed less fearful of being hurt. After 4 months of treatment, Daniel stated, “I don’t think about John Lennon much anymore. He is still important to me, but my mind took off on its own”. He was much improved, but still was socially withdrawn and had a blunted affect.
 Theories on the Mechanism(s) of Schizophrenia What brain abnormalities might underlie such a potentially devastating disorder? Daniel’s case was relatively mild. Genetic Vulnerability: MZ (identical) twin concordance >4 X more likely than DZ (sibling) twins; MZ twins average 50% discordance rate suggesting environmental influences Experience-based Vulnerability: More frequent in lower socioeconomic classes; stress may precipitate relapse; social network an important buffering influence (often disrupted by schizophrenic’s own behavior)
Theories on the Mechanism(s) of Schizophrenia What brain abnormalities might underlie such a potentially devastating disorder? Daniel’s case was relatively mild. Genetic Vulnerability: MZ (identical) twin concordance >4 X more likely than DZ (sibling) twins; MZ twins average 50% discordance rate suggesting environmental influences Experience-based Vulnerability: More frequent in lower socioeconomic classes; stress may precipitate relapse; social network an important buffering influence (often disrupted by schizophrenic’s own behavior)
 Brain structure-based theories implicate frontal and medial temporal lobes * Ventricular enlargement: In effect this means that tissue adjacent to the ventricles shrinks--temporal lobe, hippocampus *Several reports of shrinkage of frontal lobes, fewer synapses per neuron, reduced dendritic field size in prefrontal brain regions *f. MRI and PET (blood flow/metabolism) studies indicate “hypofrontality, ” decreased activity of frontal lobes
Brain structure-based theories implicate frontal and medial temporal lobes * Ventricular enlargement: In effect this means that tissue adjacent to the ventricles shrinks--temporal lobe, hippocampus *Several reports of shrinkage of frontal lobes, fewer synapses per neuron, reduced dendritic field size in prefrontal brain regions *f. MRI and PET (blood flow/metabolism) studies indicate “hypofrontality, ” decreased activity of frontal lobes
 Pharmacological treatment-based theories *From Chlorpromazine in the 1950 s to the recent past, “typical” neuroleptic drugs, effective in schizophrenia had in common the blockage of the D 2 Dopamine receptor. (They differ in therapeutic and negative side effects. ) * The Dopamine systems of the brainstem project to limbic (“mesolimbic”) and frontal cortical (“mesocortical”) brain regions. Both may be involved in Schizophrenia. *The Serotonin system projects to all regions of the brain from its origin in the raphe nuclei of the brainstem. *We won’t detail receptor actions because there will probably be more receptors when you’re MDs.
Pharmacological treatment-based theories *From Chlorpromazine in the 1950 s to the recent past, “typical” neuroleptic drugs, effective in schizophrenia had in common the blockage of the D 2 Dopamine receptor. (They differ in therapeutic and negative side effects. ) * The Dopamine systems of the brainstem project to limbic (“mesolimbic”) and frontal cortical (“mesocortical”) brain regions. Both may be involved in Schizophrenia. *The Serotonin system projects to all regions of the brain from its origin in the raphe nuclei of the brainstem. *We won’t detail receptor actions because there will probably be more receptors when you’re MDs.
 What do these drugs do? They largely act at synapses. Can we discern, from their effects at synapses, what the basis of schizophrenia might be?
What do these drugs do? They largely act at synapses. Can we discern, from their effects at synapses, what the basis of schizophrenia might be?
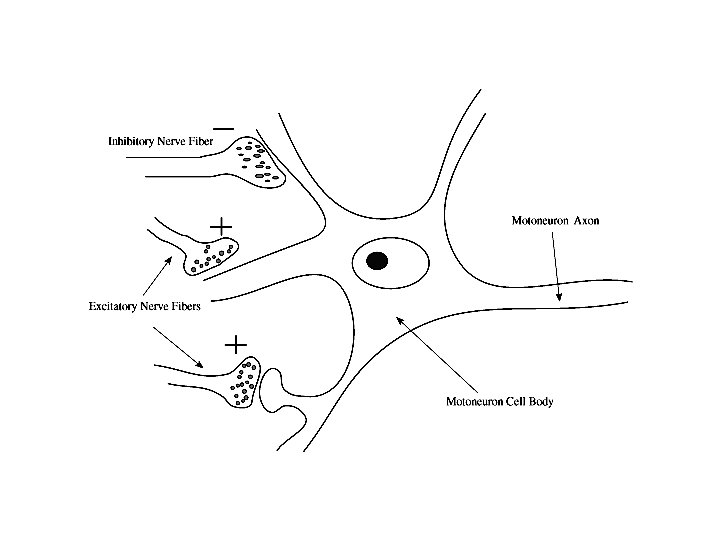
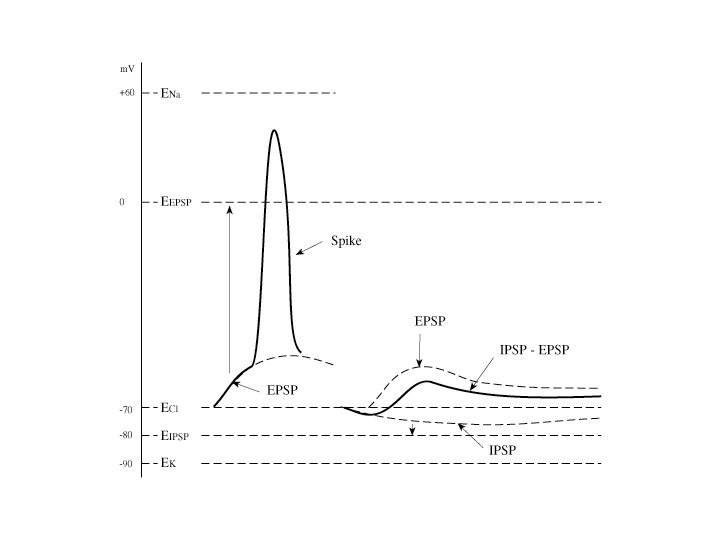
 There are Two Classes of Neurotransmitter Receptors: Ionotropic Receptors, when activated by neurotransmitter, allow ions to cross the cell membrane via channels Metabotropic Receptors, when activated by neurotransmitter, trigger enzymatic activity The same neurotransmitter, e. g. , glutamate or serotonin, can activate both ionotropic and metabotropic receptors Ionotropic receptors will be used for illustration of the way drugs work.
There are Two Classes of Neurotransmitter Receptors: Ionotropic Receptors, when activated by neurotransmitter, allow ions to cross the cell membrane via channels Metabotropic Receptors, when activated by neurotransmitter, trigger enzymatic activity The same neurotransmitter, e. g. , glutamate or serotonin, can activate both ionotropic and metabotropic receptors Ionotropic receptors will be used for illustration of the way drugs work.
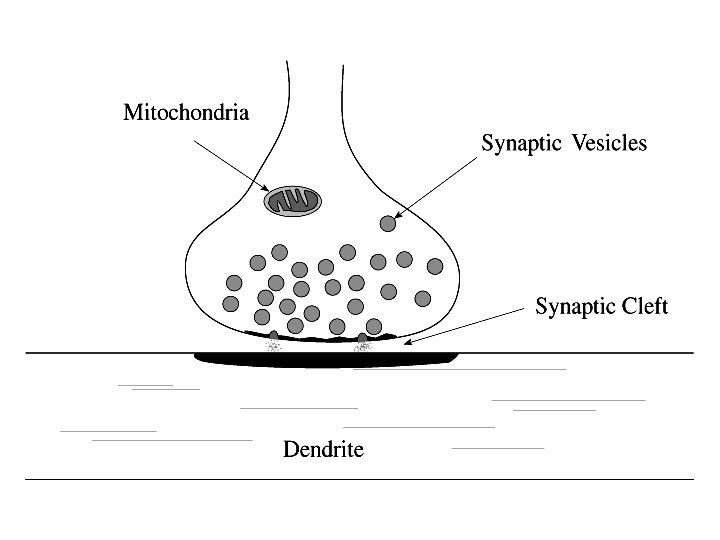
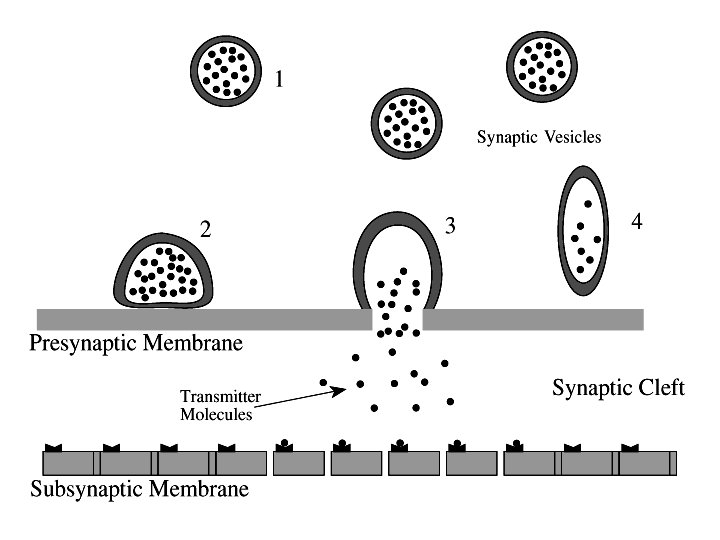
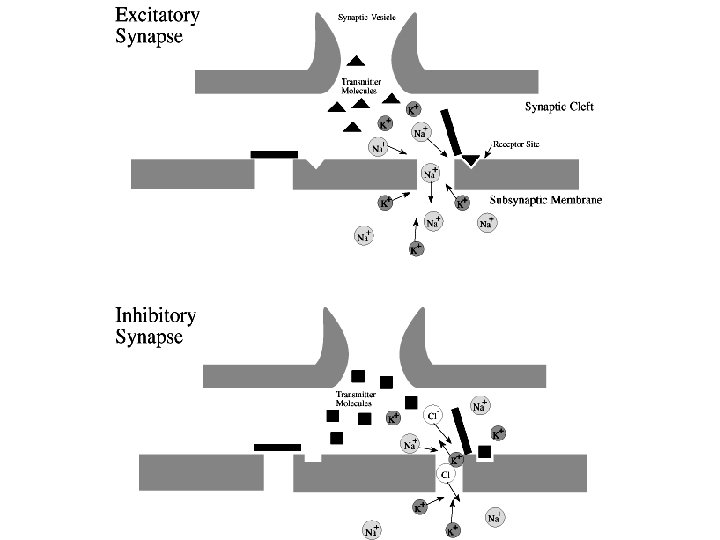
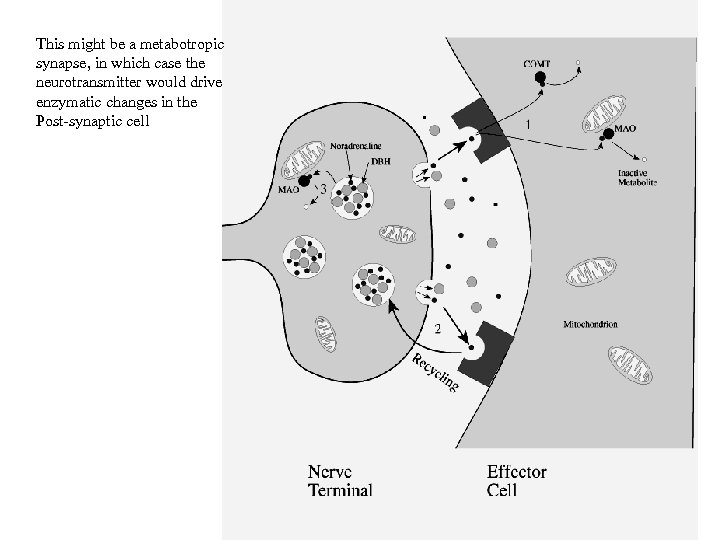 This might be a metabotropic synapse, in which case the neurotransmitter would drive enzymatic changes in the Post-synaptic cell
This might be a metabotropic synapse, in which case the neurotransmitter would drive enzymatic changes in the Post-synaptic cell
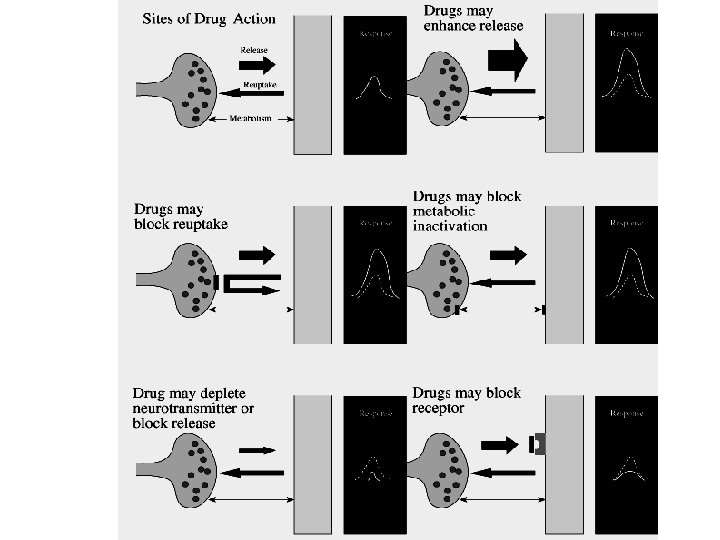
 “Atypical” Antipsychotic Drugs: Affect both Dopamine and (especially) Serotonin Systems * These drugs appear to do better at controlling both positive and negative symptoms of schizophrenia * Some “atypicals” (e. g. clozapine) have high affinity for newly discovered D 4 Dopamine receptors * Atypicals appear Not to cause Tardive Dyskinesia
“Atypical” Antipsychotic Drugs: Affect both Dopamine and (especially) Serotonin Systems * These drugs appear to do better at controlling both positive and negative symptoms of schizophrenia * Some “atypicals” (e. g. clozapine) have high affinity for newly discovered D 4 Dopamine receptors * Atypicals appear Not to cause Tardive Dyskinesia
 Drug Therapy for Schizophrenia: Medication alone is never the treatment for a patient Medications may be important components of a larger overall treatment plan
Drug Therapy for Schizophrenia: Medication alone is never the treatment for a patient Medications may be important components of a larger overall treatment plan
 What are some of the side effects of antipsychotics? • Imbalance of dopaminergic (nigrostriatal) and cholinergic systems leading to extrapyramidal side effects (acute dystonic reaction; parkinsonian side effects such as tremor, rigidity, and bradykinesia; akathisia). • Nigrostriatal dopamine receptor supersensitivity leading to tardive dyskinesia. • Anticholinergic side effects such as dry mouth, sedation, difficulty with urination, blurry vision, orthostatic hypotension. • Weight gain. • Elevation of prolactin leading to sexual dysfunction, altered/lowered mood, loss of menses in female patients, inability to become pregnant, weight gain.
What are some of the side effects of antipsychotics? • Imbalance of dopaminergic (nigrostriatal) and cholinergic systems leading to extrapyramidal side effects (acute dystonic reaction; parkinsonian side effects such as tremor, rigidity, and bradykinesia; akathisia). • Nigrostriatal dopamine receptor supersensitivity leading to tardive dyskinesia. • Anticholinergic side effects such as dry mouth, sedation, difficulty with urination, blurry vision, orthostatic hypotension. • Weight gain. • Elevation of prolactin leading to sexual dysfunction, altered/lowered mood, loss of menses in female patients, inability to become pregnant, weight gain.
 What are some of the problems that patients face when deciding to take medication? • Lack of acceptance of mental disorders as diseases- the perception that mental illness is willful and psychologically driven. • Inability to face the illness or a desire to run away and pretend that the illness will go away on its own. • Lack of support from important others like family or mate. • Realistic problems like job loss and social rejection. • General fear of mind-altering medications (which may be quite irrational as the individual may not fear the use of alcohol, cigarettes, marijuana, or cocaine). • The disease itself leads to fear of treatment (e. g. paranoid hallucinations telling the patient to not trust anyone or that the medication is really poison). • Unhappiness with side effects of medication. • Fear of tardive dyskinesia. • Discomfort with the physician or other members of the treatment team.
What are some of the problems that patients face when deciding to take medication? • Lack of acceptance of mental disorders as diseases- the perception that mental illness is willful and psychologically driven. • Inability to face the illness or a desire to run away and pretend that the illness will go away on its own. • Lack of support from important others like family or mate. • Realistic problems like job loss and social rejection. • General fear of mind-altering medications (which may be quite irrational as the individual may not fear the use of alcohol, cigarettes, marijuana, or cocaine). • The disease itself leads to fear of treatment (e. g. paranoid hallucinations telling the patient to not trust anyone or that the medication is really poison). • Unhappiness with side effects of medication. • Fear of tardive dyskinesia. • Discomfort with the physician or other members of the treatment team.
 How can these problems be minimized? • Education of the patient about his/her disease; the probable course and risks if untreated, and the probable course and benefits/risks if medication is used. • Develop an understanding of the patient’s point of view about his/her disease, symptoms, hopes for the future, fears. • Identify the patient’s strengths and help the patient mobilize all his/her individual and social resources. Involve the family when this is helpful. • Acknowledge the possible risks of medication treatment and assure the patient that he/she will be followed carefully. • Encourage open communication between patient and physician.
How can these problems be minimized? • Education of the patient about his/her disease; the probable course and risks if untreated, and the probable course and benefits/risks if medication is used. • Develop an understanding of the patient’s point of view about his/her disease, symptoms, hopes for the future, fears. • Identify the patient’s strengths and help the patient mobilize all his/her individual and social resources. Involve the family when this is helpful. • Acknowledge the possible risks of medication treatment and assure the patient that he/she will be followed carefully. • Encourage open communication between patient and physician.
 How is tardive dyskinesia treated? • Discontinue the antipsychotic and hope for the best. The patient may become ill again. • Initiate clonidine (a presynaptic alpha agonist that leads to down-regulation of the DA receptors and hypotension). • Initiate reserpine (depletes monoamines and may cause depression). • Obtain tetrabenazine from Canada (depletes monoamines with lower risk of depression).
How is tardive dyskinesia treated? • Discontinue the antipsychotic and hope for the best. The patient may become ill again. • Initiate clonidine (a presynaptic alpha agonist that leads to down-regulation of the DA receptors and hypotension). • Initiate reserpine (depletes monoamines and may cause depression). • Obtain tetrabenazine from Canada (depletes monoamines with lower risk of depression).
 MRI sheds new light on schizophrenia (Early onset Schizophrenia) - Schizophrenia, one of the most debilitating of mental illnesses, is also one of the most mysterious. Though treatment can control the illness in more than half of patients, little is known about what actually causes the disorder -- which affects about one in every 100 persons worldwide -- and how it affects the mind. UCLA researchers may have just unraveled part of the mystery. Using magnetic resonance imaging, or MRI, and a new analysis technique, they have created the first images showing the toll the disease takes on the brain. The results are reported in the Proceedings of the National Academy of Sciences. Throughout the five-year study, the researchers performed brain scans every two years on a group of 34 teenagers. The study population was made up of clinically diagnosed schizophrenics taking antipsychotic medications, another group of patients taking the same medications for mood disorders, and normal teens. The schizophrenic patients were diagnosed with the illness before adolescence, an unusual group that represents about 5 percent of all schizophrenic patients. The images that resulted from the study "stunned" the scientists, according to lead researcher Paul Thompson. Rather than small, gradual changes, Thompson and his colleagues noted a dramatic wave of destruction of the gray matter in brain tissue of schizophrenic patients. Thompson described the wave as moving across the brain "like a forest fire. " While the healthy teens lost an average of 1 percent of gray matter per year, the schizophrenic patients lost up to 5 percent a year, with loss greatest among individuals with the most severe symptoms. Study Important, But No Direct Therapy Yet Additionally, the movement of tissue loss across the brain seemed to be in sync with the appearance of disease symptoms that would originate in those parts of the brain. Starting off in the brain's logic center, the parietal cortex, tissue loss continued at a dramatic rate into the auditory part of the brain and then onto motor areas. Thompson says this sequence corresponds with the typical course of the disease. The first signs include confused or illogical thinking. As the illness progresses, more bizarre symptoms such as psychosis (unusual perceptions) and hallucinations occur. "The study represents another step forward in our understanding of schizophrenia, " says Dr. Steve Lamberti, associate professor of psychiatry at the University of Rochester Medical Center. Lamberti says the strength of the study is the detail on the nature of deterioration and progression of the illness in young people, and the evidence that brain changes were not related to antipsychotic medications but to the disease process itself. Though experts acknowledge the importance of the study's findings, they say it is limited for now. "Though there is no direct therapy application at this point. . . there is a window of hope here. " says Dr. Robert Freedman, Chairman of the Department of Psychiatry and the University of Colorado Health Sciences College. "Most of us thought the damage was done in utero, " says Freedman, but "the study suggests the changes can possibly be observed during adolescence. " Freedman calls the study groundbreaking as it has "opened up a window to a very complicated piece of biology that none of us completely understand. " Yet, he says, "A lot of work still has to be done. "
MRI sheds new light on schizophrenia (Early onset Schizophrenia) - Schizophrenia, one of the most debilitating of mental illnesses, is also one of the most mysterious. Though treatment can control the illness in more than half of patients, little is known about what actually causes the disorder -- which affects about one in every 100 persons worldwide -- and how it affects the mind. UCLA researchers may have just unraveled part of the mystery. Using magnetic resonance imaging, or MRI, and a new analysis technique, they have created the first images showing the toll the disease takes on the brain. The results are reported in the Proceedings of the National Academy of Sciences. Throughout the five-year study, the researchers performed brain scans every two years on a group of 34 teenagers. The study population was made up of clinically diagnosed schizophrenics taking antipsychotic medications, another group of patients taking the same medications for mood disorders, and normal teens. The schizophrenic patients were diagnosed with the illness before adolescence, an unusual group that represents about 5 percent of all schizophrenic patients. The images that resulted from the study "stunned" the scientists, according to lead researcher Paul Thompson. Rather than small, gradual changes, Thompson and his colleagues noted a dramatic wave of destruction of the gray matter in brain tissue of schizophrenic patients. Thompson described the wave as moving across the brain "like a forest fire. " While the healthy teens lost an average of 1 percent of gray matter per year, the schizophrenic patients lost up to 5 percent a year, with loss greatest among individuals with the most severe symptoms. Study Important, But No Direct Therapy Yet Additionally, the movement of tissue loss across the brain seemed to be in sync with the appearance of disease symptoms that would originate in those parts of the brain. Starting off in the brain's logic center, the parietal cortex, tissue loss continued at a dramatic rate into the auditory part of the brain and then onto motor areas. Thompson says this sequence corresponds with the typical course of the disease. The first signs include confused or illogical thinking. As the illness progresses, more bizarre symptoms such as psychosis (unusual perceptions) and hallucinations occur. "The study represents another step forward in our understanding of schizophrenia, " says Dr. Steve Lamberti, associate professor of psychiatry at the University of Rochester Medical Center. Lamberti says the strength of the study is the detail on the nature of deterioration and progression of the illness in young people, and the evidence that brain changes were not related to antipsychotic medications but to the disease process itself. Though experts acknowledge the importance of the study's findings, they say it is limited for now. "Though there is no direct therapy application at this point. . . there is a window of hope here. " says Dr. Robert Freedman, Chairman of the Department of Psychiatry and the University of Colorado Health Sciences College. "Most of us thought the damage was done in utero, " says Freedman, but "the study suggests the changes can possibly be observed during adolescence. " Freedman calls the study groundbreaking as it has "opened up a window to a very complicated piece of biology that none of us completely understand. " Yet, he says, "A lot of work still has to be done. "
 END
END


