8c05eb23b0e62cb20bcd59f38cca81f4.ppt
- Количество слайдов: 20
 Reverse Remodeling and the Risk of Ventricular Tachyarrhythmias in MADITCRT Alon Barsheshet, MD 1, Paul J. Wang, MD 2, Arthur J. Moss, MD 1, Scott D. Solomon, MD 3, Amin Al-Ahmad, MD 2, Scott Mc. Nitt, MS 1, Elyse Foster, MD 4, David T. Huang, MD 1, Helmut U. Klein, MD 1, Wojciech Zareba, MD, Ph. D 1, Michael Eldar, MD 5, Ilan Goldenberg, MD 1 1 Cardiology Division, University of Rochester Medical Center, Rochester, NY; 2 Cardiology Division, Stanford University, Stanford, CA; 3 Cardiovascular Division, Brigham and Women's Hospital, Harvard Medical School, Boston, MA; 4 Department of Medicine, University of California at San Francisco, CA; 5 Heart Institute, Sheba Medical Center, Tel Hashomer, Israel
Reverse Remodeling and the Risk of Ventricular Tachyarrhythmias in MADITCRT Alon Barsheshet, MD 1, Paul J. Wang, MD 2, Arthur J. Moss, MD 1, Scott D. Solomon, MD 3, Amin Al-Ahmad, MD 2, Scott Mc. Nitt, MS 1, Elyse Foster, MD 4, David T. Huang, MD 1, Helmut U. Klein, MD 1, Wojciech Zareba, MD, Ph. D 1, Michael Eldar, MD 5, Ilan Goldenberg, MD 1 1 Cardiology Division, University of Rochester Medical Center, Rochester, NY; 2 Cardiology Division, Stanford University, Stanford, CA; 3 Cardiovascular Division, Brigham and Women's Hospital, Harvard Medical School, Boston, MA; 4 Department of Medicine, University of California at San Francisco, CA; 5 Heart Institute, Sheba Medical Center, Tel Hashomer, Israel
 Background • The effect of CRT on the risk of ventricular tachyarrhythmias (VTA) is controversial • Reverse remodeling • LV epicardial pacing • VTA and ICD shocks are associated with reduction in quality of life and with poor prognosis
Background • The effect of CRT on the risk of ventricular tachyarrhythmias (VTA) is controversial • Reverse remodeling • LV epicardial pacing • VTA and ICD shocks are associated with reduction in quality of life and with poor prognosis
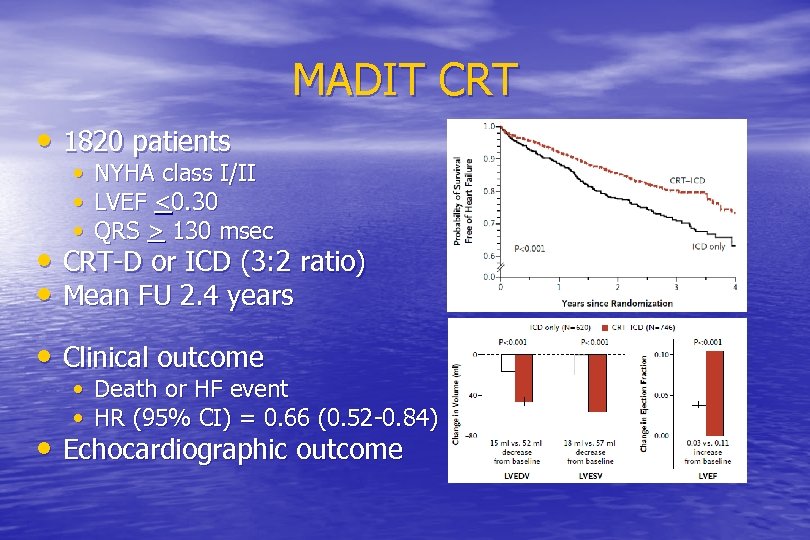 MADIT CRT • 1820 patients • NYHA class I/II • LVEF <0. 30 • QRS > 130 msec • CRT-D or ICD (3: 2 ratio) • Mean FU 2. 4 years • Clinical outcome • Death or HF event • HR (95% CI) = 0. 66 (0. 52 -0. 84) • Echocardiographic outcome
MADIT CRT • 1820 patients • NYHA class I/II • LVEF <0. 30 • QRS > 130 msec • CRT-D or ICD (3: 2 ratio) • Mean FU 2. 4 years • Clinical outcome • Death or HF event • HR (95% CI) = 0. 66 (0. 52 -0. 84) • Echocardiographic outcome
 Objective • To explore the association between the magnitude of echocardiographic response to CRT and subsequent risk for VTA in MADIT-CRT
Objective • To explore the association between the magnitude of echocardiographic response to CRT and subsequent risk for VTA in MADIT-CRT
 Methods
Methods
 Study Population • 1372 patients • Patients were categorized into 3 groups – CRT-D high echo responders (≥ 25% reduction in LVESV at 1 -year) – CRT-D low echo responders – ICD-only patients
Study Population • 1372 patients • Patients were categorized into 3 groups – CRT-D high echo responders (≥ 25% reduction in LVESV at 1 -year) – CRT-D low echo responders – ICD-only patients
 Definitions • ΔVolume/ baseline volume = (1 year volume- baseline volume)/ baseline volume • VT: ≤ 250 bpm • VF: > 250 bpm with disorganized EGMs • Vflutter: > 250 bpm and monomorphic
Definitions • ΔVolume/ baseline volume = (1 year volume- baseline volume)/ baseline volume • VT: ≤ 250 bpm • VF: > 250 bpm with disorganized EGMs • Vflutter: > 250 bpm and monomorphic
 Outcome measures • Primary end point – Appropriate ICD therapy for VTA after the assessment of echocardiographic response • Secondary endpoints – Appropriate ICD therapy for • VTA or death • VT • VF • Vflutter
Outcome measures • Primary end point – Appropriate ICD therapy for VTA after the assessment of echocardiographic response • Secondary endpoints – Appropriate ICD therapy for • VTA or death • VT • VF • Vflutter
 Statistical analysis • Effect of echocardiographic response to CRT-D on outcome • Categorical variable • Continuous measure • Cox proportional hazards model and a landmark analysis
Statistical analysis • Effect of echocardiographic response to CRT-D on outcome • Categorical variable • Continuous measure • Cox proportional hazards model and a landmark analysis
 Results
Results
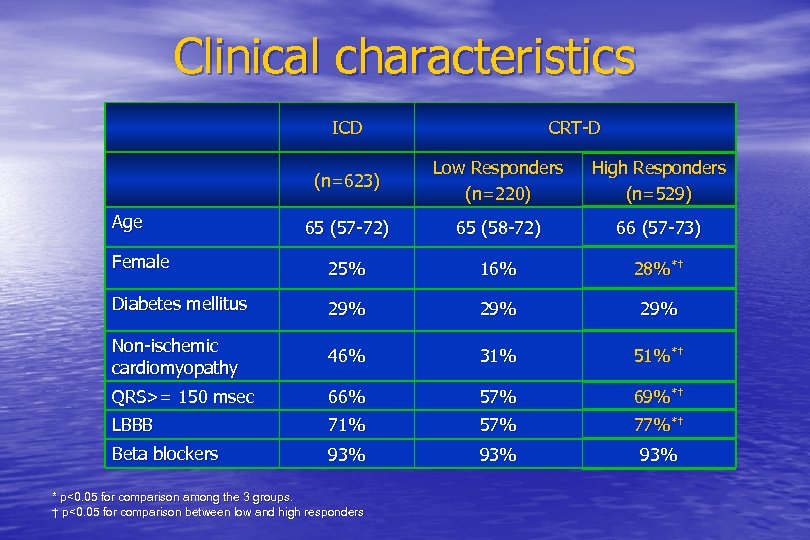 Clinical characteristics ICD CRT-D (n=623) Low Responders (n=220) High Responders (n=529) 65 (57 -72) 65 (58 -72) 66 (57 -73) Female 25% 16% 28%*† Diabetes mellitus 29% 29% Non-ischemic cardiomyopathy 46% 31% 51%*† QRS>= 150 msec 66% 57% 69%*† LBBB 71% 57% 77%*† Beta blockers 93% 93% Age * p<0. 05 for comparison among the 3 groups. † p<0. 05 for comparison between low and high responders
Clinical characteristics ICD CRT-D (n=623) Low Responders (n=220) High Responders (n=529) 65 (57 -72) 65 (58 -72) 66 (57 -73) Female 25% 16% 28%*† Diabetes mellitus 29% 29% Non-ischemic cardiomyopathy 46% 31% 51%*† QRS>= 150 msec 66% 57% 69%*† LBBB 71% 57% 77%*† Beta blockers 93% 93% Age * p<0. 05 for comparison among the 3 groups. † p<0. 05 for comparison between low and high responders
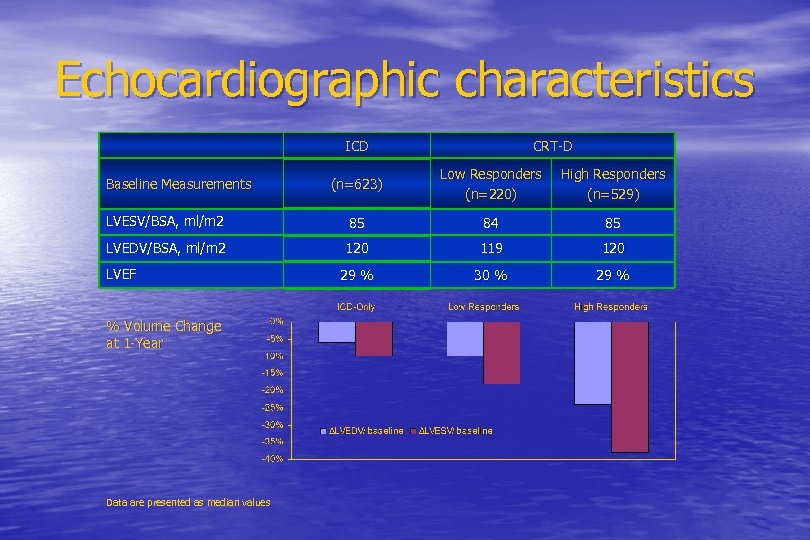 Echocardiographic characteristics ICD CRT-D (n=623) Low Responders (n=220) High Responders (n=529) LVESV/BSA, ml/m 2 85 84 85 LVEDV/BSA, ml/m 2 120 119 120 29 % 30 % 29 % Baseline Measurements LVEF % Volume Change at 1 -Year Data are presented as median values
Echocardiographic characteristics ICD CRT-D (n=623) Low Responders (n=220) High Responders (n=529) LVESV/BSA, ml/m 2 85 84 85 LVEDV/BSA, ml/m 2 120 119 120 29 % 30 % 29 % Baseline Measurements LVEF % Volume Change at 1 -Year Data are presented as median values
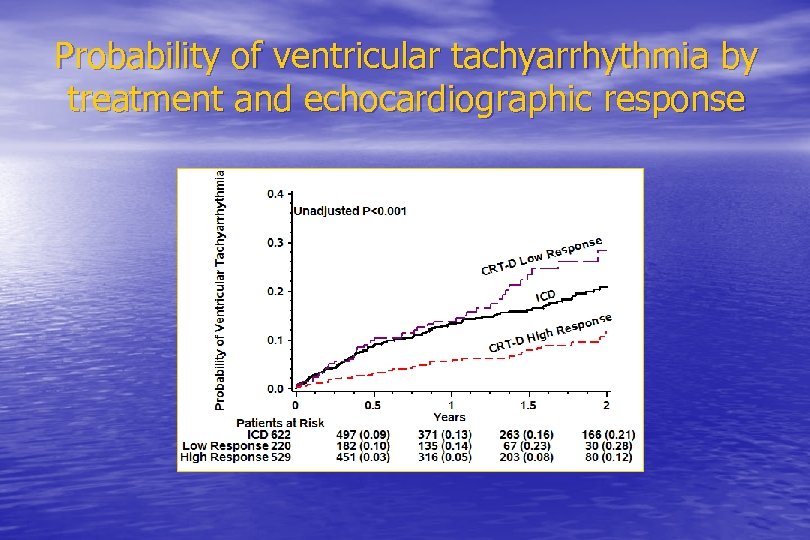 Probability of ventricular tachyarrhythmia by treatment and echocardiographic response
Probability of ventricular tachyarrhythmia by treatment and echocardiographic response
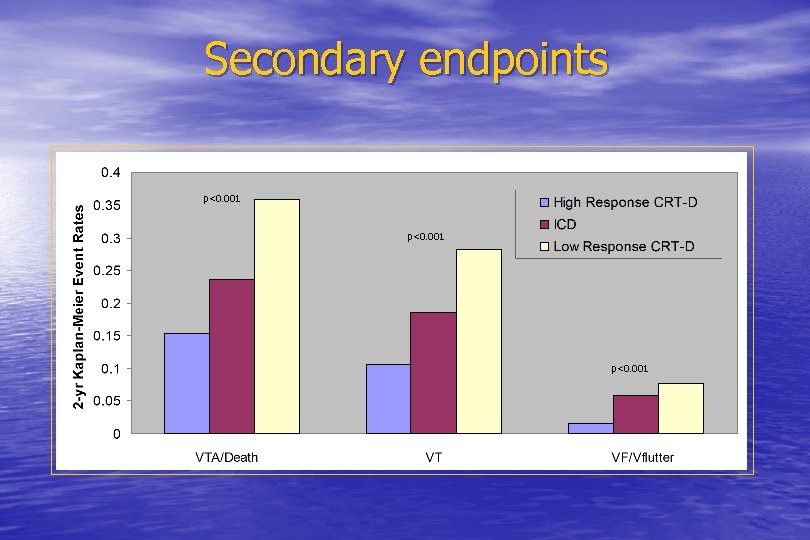 Secondary endpoints p<0. 001
Secondary endpoints p<0. 001
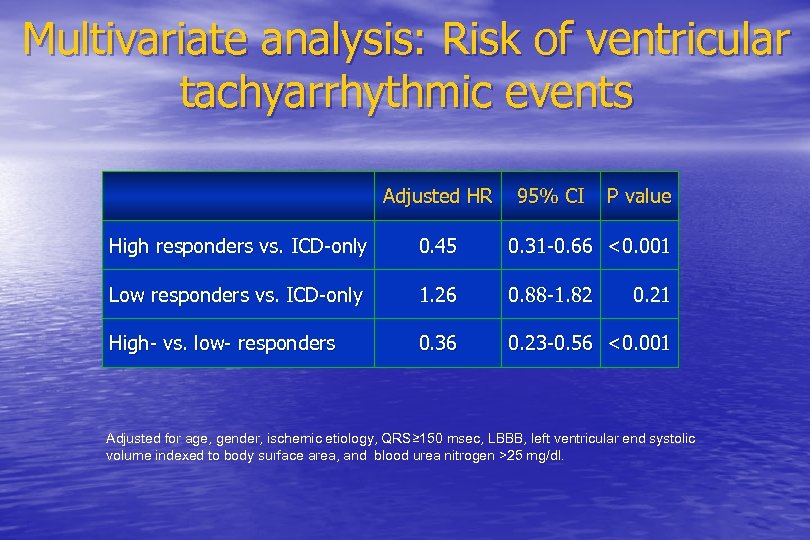 Multivariate analysis: Risk of ventricular tachyarrhythmic events Adjusted HR 95% CI P value High responders vs. ICD-only 0. 45 0. 31 -0. 66 <0. 001 Low responders vs. ICD-only 1. 26 0. 88 -1. 82 High- vs. low- responders 0. 36 0. 23 -0. 56 <0. 001 0. 21 Adjusted for age, gender, ischemic etiology, QRS≥ 150 msec, LBBB, left ventricular end systolic volume indexed to body surface area, and blood urea nitrogen >25 mg/dl.
Multivariate analysis: Risk of ventricular tachyarrhythmic events Adjusted HR 95% CI P value High responders vs. ICD-only 0. 45 0. 31 -0. 66 <0. 001 Low responders vs. ICD-only 1. 26 0. 88 -1. 82 High- vs. low- responders 0. 36 0. 23 -0. 56 <0. 001 0. 21 Adjusted for age, gender, ischemic etiology, QRS≥ 150 msec, LBBB, left ventricular end systolic volume indexed to body surface area, and blood urea nitrogen >25 mg/dl.
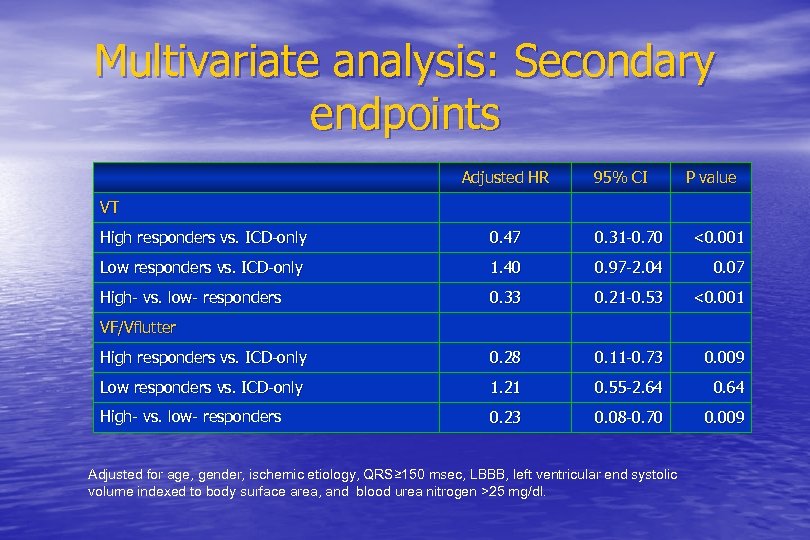 Multivariate analysis: Secondary endpoints Adjusted HR 95% CI P value VT High responders vs. ICD-only 0. 47 0. 31 -0. 70 <0. 001 Low responders vs. ICD-only 1. 40 0. 97 -2. 04 0. 07 High- vs. low- responders 0. 33 0. 21 -0. 53 <0. 001 High responders vs. ICD-only 0. 28 0. 11 -0. 73 0. 009 Low responders vs. ICD-only 1. 21 0. 55 -2. 64 0. 64 High- vs. low- responders 0. 23 0. 08 -0. 70 0. 009 VF/Vflutter Adjusted for age, gender, ischemic etiology, QRS≥ 150 msec, LBBB, left ventricular end systolic volume indexed to body surface area, and blood urea nitrogen >25 mg/dl.
Multivariate analysis: Secondary endpoints Adjusted HR 95% CI P value VT High responders vs. ICD-only 0. 47 0. 31 -0. 70 <0. 001 Low responders vs. ICD-only 1. 40 0. 97 -2. 04 0. 07 High- vs. low- responders 0. 33 0. 21 -0. 53 <0. 001 High responders vs. ICD-only 0. 28 0. 11 -0. 73 0. 009 Low responders vs. ICD-only 1. 21 0. 55 -2. 64 0. 64 High- vs. low- responders 0. 23 0. 08 -0. 70 0. 009 VF/Vflutter Adjusted for age, gender, ischemic etiology, QRS≥ 150 msec, LBBB, left ventricular end systolic volume indexed to body surface area, and blood urea nitrogen >25 mg/dl.
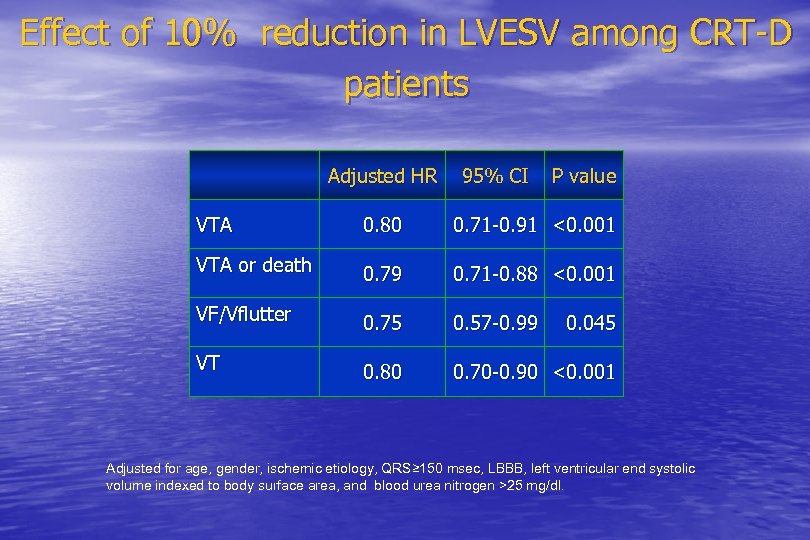 Effect of 10% reduction in LVESV among CRT-D patients Adjusted HR 95% CI P value VTA 0. 80 0. 71 -0. 91 <0. 001 VTA or death 0. 79 0. 71 -0. 88 <0. 001 VF/Vflutter 0. 75 0. 57 -0. 99 VT 0. 80 0. 70 -0. 90 <0. 001 0. 045 Adjusted for age, gender, ischemic etiology, QRS≥ 150 msec, LBBB, left ventricular end systolic volume indexed to body surface area, and blood urea nitrogen >25 mg/dl.
Effect of 10% reduction in LVESV among CRT-D patients Adjusted HR 95% CI P value VTA 0. 80 0. 71 -0. 91 <0. 001 VTA or death 0. 79 0. 71 -0. 88 <0. 001 VF/Vflutter 0. 75 0. 57 -0. 99 VT 0. 80 0. 70 -0. 90 <0. 001 0. 045 Adjusted for age, gender, ischemic etiology, QRS≥ 150 msec, LBBB, left ventricular end systolic volume indexed to body surface area, and blood urea nitrogen >25 mg/dl.
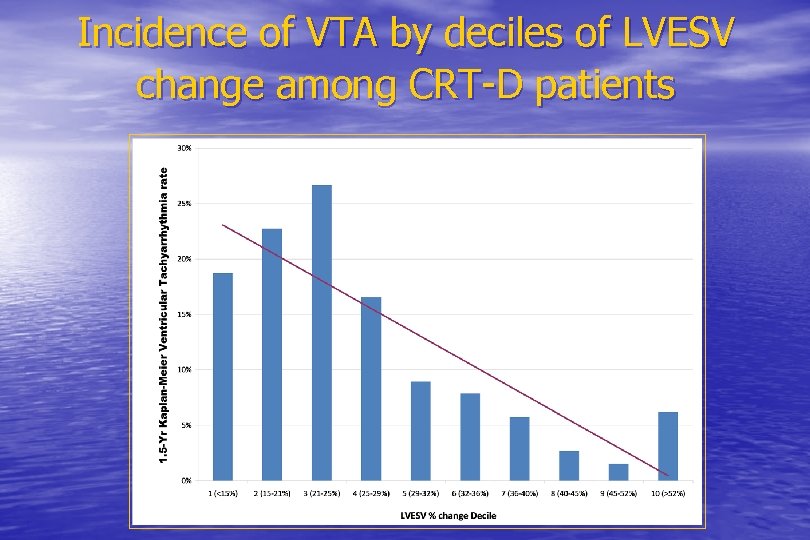 Incidence of VTA by deciles of LVESV change among CRT-D patients
Incidence of VTA by deciles of LVESV change among CRT-D patients
 Conclusions 1. Patients with high echocardiographic 2. response to CRT-D (≥ 25% reduction in LVESV) exhibit a significant reduction in the risk of VTA events. The magnitude of reverse remodeling is inversely related to VTA risk: 10% reduction in LVESV → 20 % reduction in the risk of VTA.
Conclusions 1. Patients with high echocardiographic 2. response to CRT-D (≥ 25% reduction in LVESV) exhibit a significant reduction in the risk of VTA events. The magnitude of reverse remodeling is inversely related to VTA risk: 10% reduction in LVESV → 20 % reduction in the risk of VTA.
 Conclusions 3. The process of reverse remodeling induced by CRT leads to a lower risk of both HF and arrhythmic events.
Conclusions 3. The process of reverse remodeling induced by CRT leads to a lower risk of both HF and arrhythmic events.


