ea6d8a6ce414a2f36ed751fafea975cb.ppt
- Количество слайдов: 23

Resuscitation Teams

Code Blue Teams Who • Physicians from Anesthesia Medicine (on call MICU and cardiology teams) Surgery • Nursing House supervisor ACLS trained nurse from CCU/CTICU ED nurse for specific areas All neuroscience floors except 6 NSH All diagnostic areas (Radiology, labs, Clinics) All non-patient care areas • • Pharmacy Respiratory therapy Pastoral care Patient transportation (responds if in a non-patient care area)

Code Blue Where • All codes within UNC Hospitals • Within the following external boundaries: Base of Cardinal, Dogwood and Neurosciences parking deck ramps ED parking area visible from doorway of ED

Code Team Once you get there: • Physician team leader must identify self • ACLS trained nurse from CCU/CTICU provides nursing support ICU nurse must remain with the patient until the patient is transferred to the appropriate level of care • Primary nurse remains present for the duration of the code • Pharmacist assists with medication preparation • Respiratory therapy provides respiratory support • Nursing supervisor Provides assistance with crowd control Facilitates patient transfer to appropriate level of care All team members should identify themselves and their roles upon arrival

Code Blue documentation A resuscitation record must be kept by a documentation nurse The physician team leader signs the record and completes a summary section

Rapid Response Teams Background • 80% of codes are preceded by a prolonged period of physiologic instability • Introduced at UNC in 2006 • Purpose: To quickly and appropriately respond to inpatients with early signs of physiologic deterioration, and thus: Decrease the number of Code Blues Ideally improve survival to hospital discharge
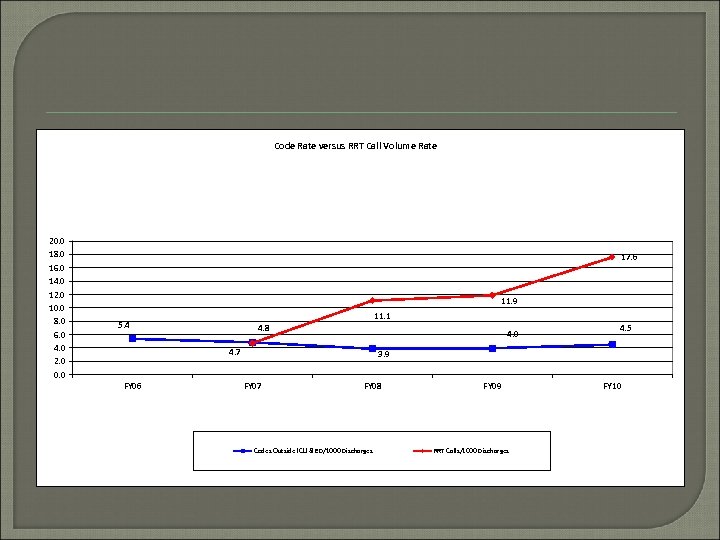
Code Rate versus RRT Call Volume Rate 20. 0 18. 0 16. 0 14. 0 12. 0 10. 0 8. 0 6. 0 4. 0 2. 0 0. 0 17. 6 11. 9 11. 1 5. 4 4. 8 4. 0 4. 7 FY 06 4. 5 3. 9 FY 07 FY 08 Codes Outside ICU & ED/1000 Discharges FY 09 RRT Calls/1000 Discharges FY 10
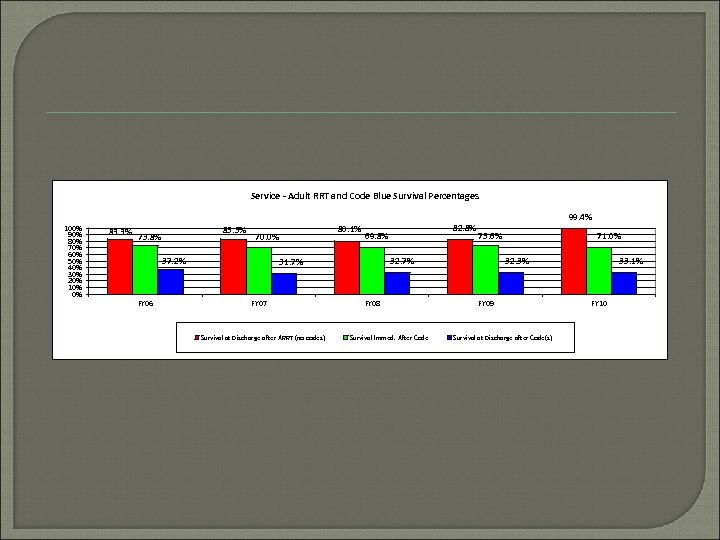
Service - Adult RRT and Code Blue Survival Percentages 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 83. 3% 73. 8% 70. 0% 37. 2% FY 06 80. 1% 69. 8% Survival at Discharge after ARRT (no codes) 99. 4% FY 08 Survival Immed. After Code 71. 0% 73. 6% 32. 7% 31. 7% FY 07 82. 8% 33. 1% 32. 3% FY 09 Survival at Discharge after Code(s) FY 10

RRT Calling Criteria Staff or family have concerns Acute change in HR Acute change in systolic BP Acute change in respiratory rate Acute change in oxygen saturation Acute change in urine output Acute mental status change New or prolonged seizure Patient with difficult to control pain or agitation

RRT Call Protocol Activation of RRT by calling 6 -4111 Page primary resident

RRT: Who depends on • Medicine floors: location 3 W/HD, 3 BT (CRU), MPCU, 4 ADU, 6 BT, 6 W, 7 BT, 8 BT, 3, 4, 5 Neuro; 4 BM and 4 ONC, 5 And South (Jail) NOT cafeteria, radiology, GI suite – Call a code MICU nurse MICU fellow (when in-house) Hospitalist on call (after 7 pm) MICU resident (recommended)

RRT: Who? • Cardiology floors: CCU nurse Cardiology team (Resident) • Surgery floors: SICU team and nurse • Primary team physician (or cross-cover) must show up as well

RRT: Once you get there Physician team leader identifies self and coordinates assessment and care with the primary physician RRT nurse from ICU provides nursing support and coordinate with primary nurse Respiratory therapy assists with maintenance of airway and ventilation

RRT: Documentation of Adult Rapid Response Activation must be completed by the responding care providers Debriefing following the event with the RRT and primary care team (including nurse!) should take place

Brain Attack Team (BAT) Introduced March 2010 Purpose: • To provide inpatients with acute stroke the same care they would obtain if they presented to the ED: Rapid head imaging Rapid evaluation by neurology Early administration of fibrinolytic therapy if indicated

BAT team Composition • Neurology resident • Neurology/neurosurgery ICU nurse • Patient transport

BAT activation If rapid response team or code blue team is worried about a primary CNS event, the team calls the hospital operator to activate the brain attack team
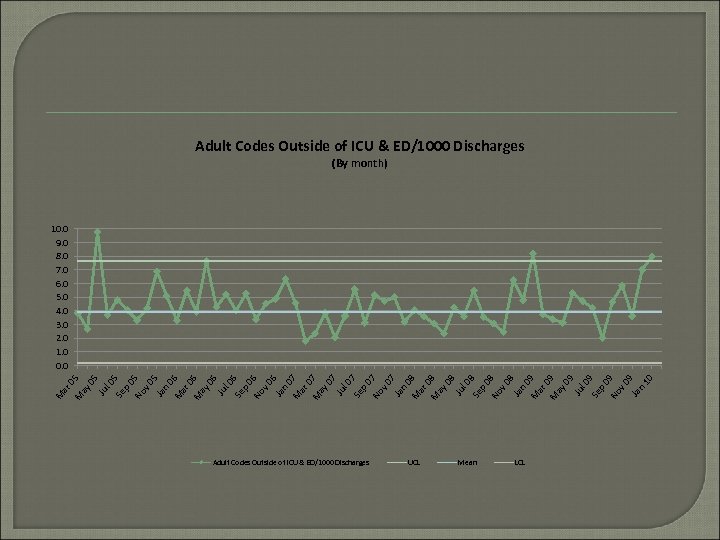
05 p 0 No 5 v 0 5 Ja n 0 M 6 ar 0 M 6 ay 06 Ju l 0 6 Se p 0 No 6 v 0 6 Ja n 0 M 7 ar 0 M 7 ay 07 Ju l 0 7 Se p 0 No 7 v 0 7 Ja n 0 M 8 ar 0 M 8 ay 08 Ju l 0 8 Se p 0 No 8 v 0 8 Ja n 0 M 9 ar 0 M 9 ay 09 Ju l 0 9 Se p 0 No 9 v 0 9 Ja n 1 0 Se Ju l 5 05 ar 0 ay M M Adult Codes Outside of ICU & ED/1000 Discharges (By month) 10. 0 9. 0 8. 0 7. 0 6. 0 5. 0 4. 0 3. 0 2. 0 1. 0 0. 0 Adult Codes Outside of ICU & ED/1000 Discharges UCL Mean LCL

Special Case: Cancer Hospital Med E Resident on call is first responder to all codes/RRT in the Cancer Hospital • This includes clinics! In the aftermath, have a lower threshold to move patient to stepdown level of care Med E patient (and Solid Med H? ) in MPCU managed by MICU team • Do not let this dissuade you from moving patient to stepdown level of care!!!
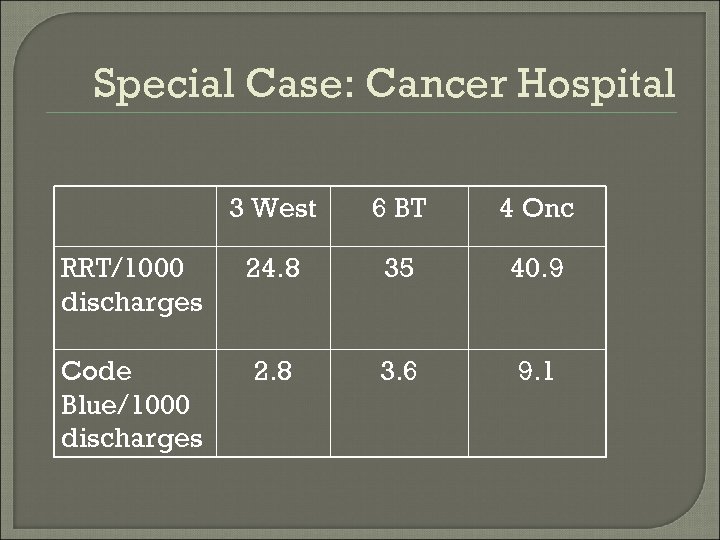
Special Case: Cancer Hospital 3 West 6 BT 4 Onc RRT/1000 discharges 24. 8 35 40. 9 Code Blue/1000 discharges 2. 8 3. 6 9. 1

It’s a land far, far away It gets lonely out there • Med E resident in ED, covering patients elsewhere • Only on floor 30 -40 percent of the time at night Ryan, fix this please Teams are reluctant to transfer patients to stepdown

Stepdown vs Floor This is based primarily on nursing competency, not resident competency If the floor nurses say they cannot manage the patient, then they must go to stepdown Nursing competencies vary by floor

Please Refrain Blocking and Belittling the referring physician or nurse “There are no ICU beds” • RRT nurse stays to help manage the patient • You work with House Supervisor to find or make a bed • Call in the MICU fellow to lend a hand if your team is overrun Call Dr. Carson if you get any push-back
ea6d8a6ce414a2f36ed751fafea975cb.ppt