f69c78149fddcee86ecf115f22f84ab4.ppt
- Количество слайдов: 41

Resistance is futile ? – antibiotic resistance in Scottish pneumococci Andrew Smith Professor of Clinical Bacteriology

Acknowledgements Ben Cooke Mathew Diggle Karen Lamb Christopher Robertson Donald Inverarity Johanna Jefferies Giles Edwards Stuart Clarke Jim Mc. Menamin Tim Mitchell All staff at SHLMPRL Prof T Mitchell Pneumococcal Research Group
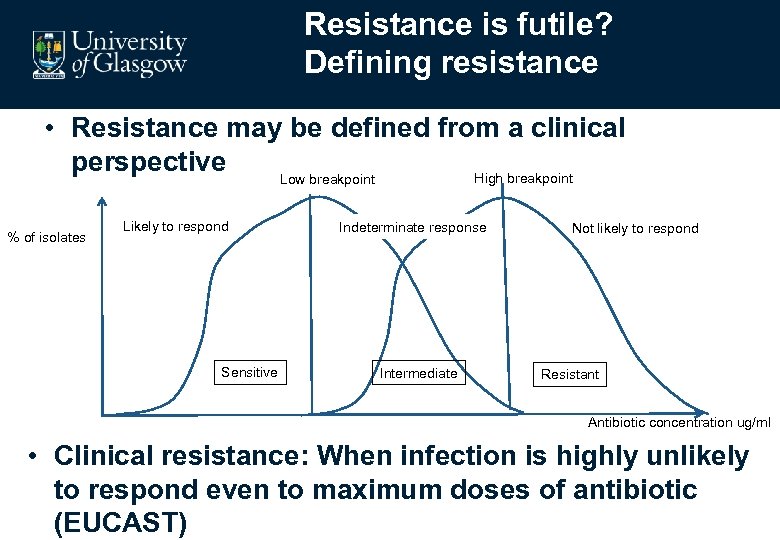
Resistance is futile? Defining resistance • Resistance may be defined from a clinical perspective High breakpoint Low breakpoint % of isolates Likely to respond Sensitive Indeterminate response Intermediate Not likely to respond Resistant Antibiotic concentration ug/ml • Clinical resistance: When infection is highly unlikely to respond even to maximum doses of antibiotic (EUCAST)

Defining resistance • Resistance may be defined from a biological perspective – National variations in breakpoints • Resistance definitions usually based on in-vitro quantitative testing of bacterial suspensions to antibacterial agents Minimum inhibitory concentration
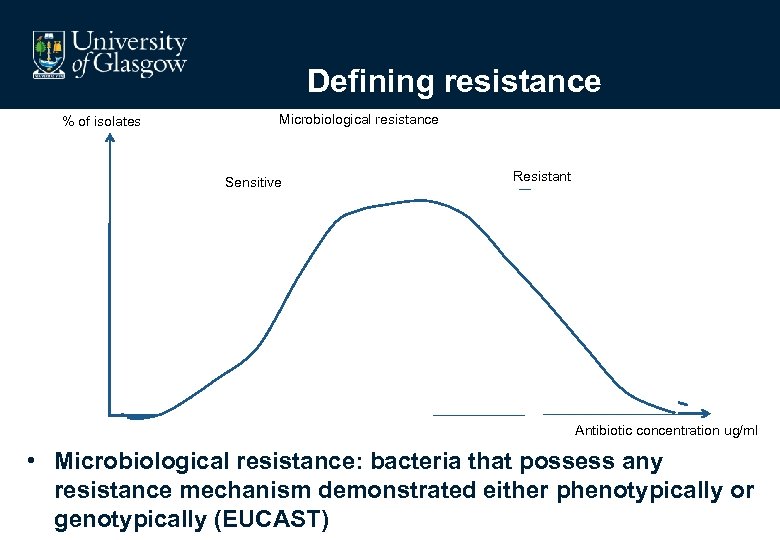
Defining resistance % of isolates Microbiological resistance Resistant Sensitive Breakpoint Antibiotic concentration ug/ml • Microbiological resistance: bacteria that possess any resistance mechanism demonstrated either phenotypically or genotypically (EUCAST)

Confounding variables • Laboratory – Inoculum size, growth phase, planktonic, p. H, atmosphere… • Clinical – Co-morbidities, pus collections, foreign bodies, site of infection ………. . – Pharmacokinetics – Pharmacodynamics

Mechanisms of resistance in pneumococci • Penicillin resistance: Pencillin binding proteins (PBPs) • 6 PBP’s described in the pneumococcus • Alterations in PBP’s = resistance • Resistance= mosiacism in PBP 2 b, 2 x and 1 a
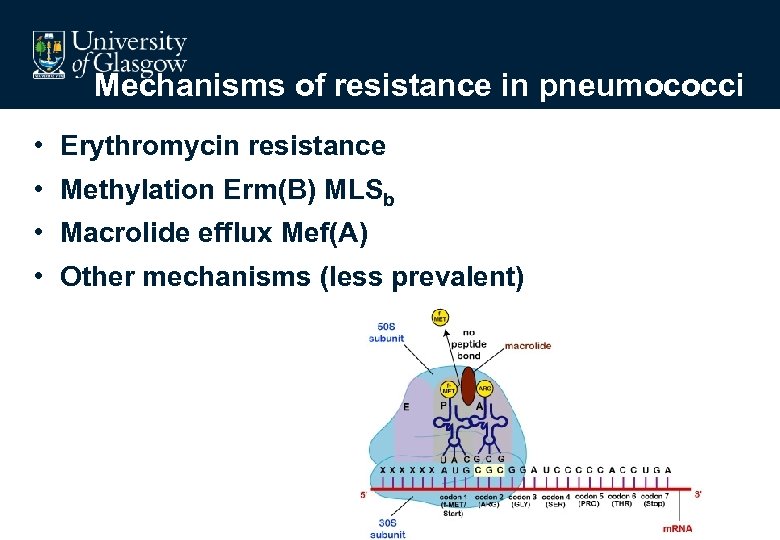
Mechanisms of resistance in pneumococci • Erythromycin resistance • Methylation Erm(B) MLSb • Macrolide efflux Mef(A) • Other mechanisms (less prevalent)

Penicillin resistance in pneumococcus 1 st Reported in 1967 (Hansman & Bullen 1967) Serotype 23 Pen MIC = 0. 6 ug/ml Subsequent reports from Papua New Guinea 1974 12% - 1980 30% resistant 1974 -1984 Foci with >10% include New Guinea, Israel, Spain, Poland, South Africa & USA (states) Klugman Clin Micro Rev 1990 171

Penicillin resistance in pneumococcus (1990’s) Rates 5 -80% (Forward Sem Resp Infect 1999 243 -254, Thornberg et al AAC 199943: 2612; Song et al CID 1999 28: 1206) USA 2/3 of PRP’s have MICs of 2 ug/ml & others = 4 ug/ml (Doern et al EID 1999; 5: 757) MIC values of 8 ug/ml reported from Spain (Baquero et al AAC 1999; 43: 357) & USA (Doern et al AAC 1996; 40: 1208) MIC of 16 ug/ml reported from Eastern Europe & USA (Applebaum CID 1992; 15: 77; Gross et al AAC 1996; 39: 116668)

Prevalence of penicillin non-susceptible pneumococcus in Europe (EARS 2008) • 1 -5% UK, Germany , Austria, Norway & Sweden • 10 -25% Portugal, Ireland, Finland & Turkey • 25 -50% Spain, France, Greece & Israel
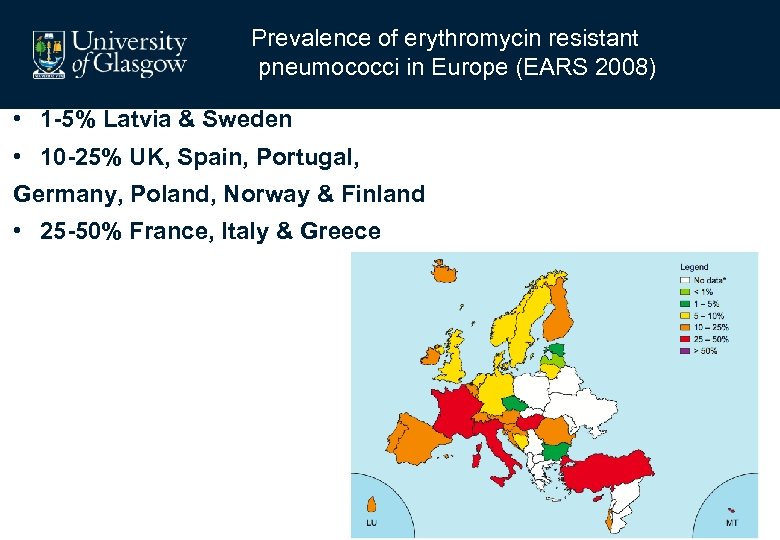
Prevalence of erythromycin resistant pneumococci in Europe (EARS 2008) • 1 -5% Latvia & Sweden • 10 -25% UK, Spain, Portugal, Germany, Poland, Norway & Finland • 25 -50% France, Italy & Greece

Aims • Identify susceptibility profiles (1999 -2007) to • Penicillin & erythromycin • Establish contribution that different serogroups and sequence types make to the burden of antibiotic resistance. • Explore extent to which internationally recognised PMEN (Pneumococcal molecular epidemiology Network) clones are seen in Scotland

Methods • Isolates obtained from SHLMPRL • Received from diagnostic labs in Scotland from all invasive isolates • Typing & antimicrobial testing as part of Electronic Communication of Surveillance in Scotland (ECOSS) • 4, 727 isolates available covering 1999 - 2007
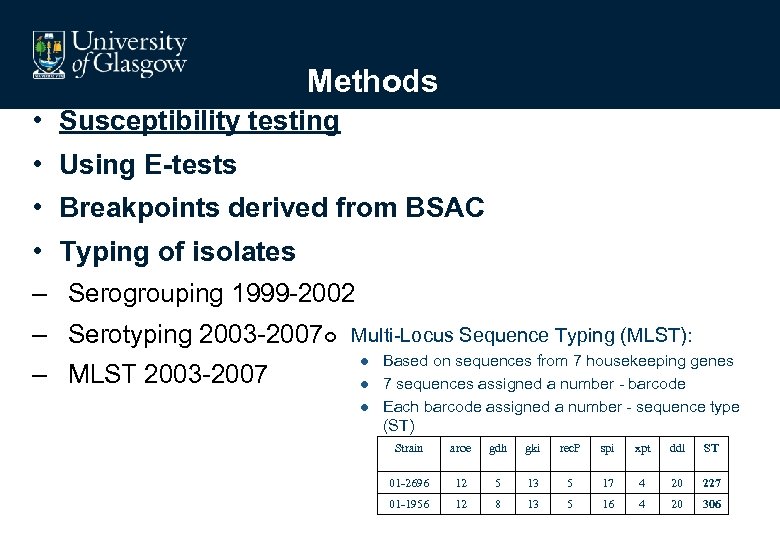

Methods • Susceptibility testing • Using E-tests • Breakpoints derived from BSAC • Typing of isolates – Serogrouping 1999 -2002 – Serotyping 2003 -2007¢ – MLST 2003 -2007 Multi-Locus Sequence Typing (MLST): l l l Based on sequences from 7 housekeeping genes 7 sequences assigned a number - barcode Each barcode assigned a number - sequence type (ST) Strain aroe gdh gki rec. P spi xpt ddl ST 01 -2696 12 5 13 5 17 4 20 227 01 -1956 12 8 13 5 16 4 20 306
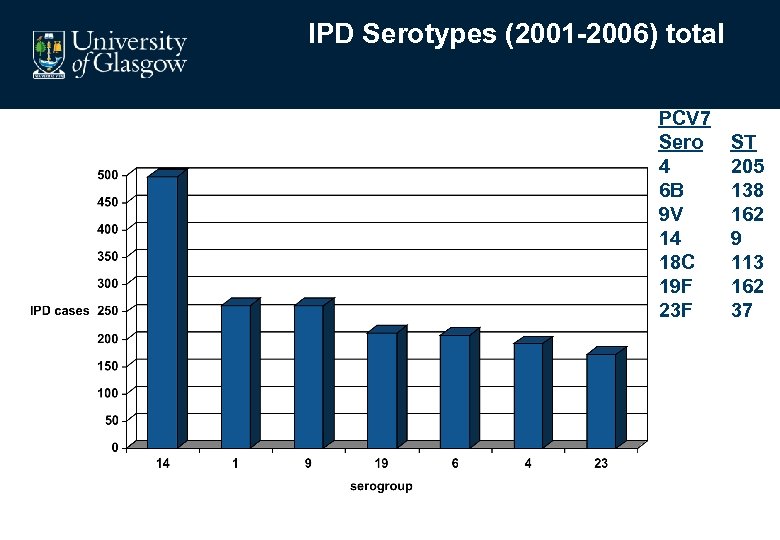
IPD Serotypes (2001 -2006) total PCV 7 Sero 4 6 B 9 V 14 18 C 19 F 23 F ST 205 138 162 9 113 162 37
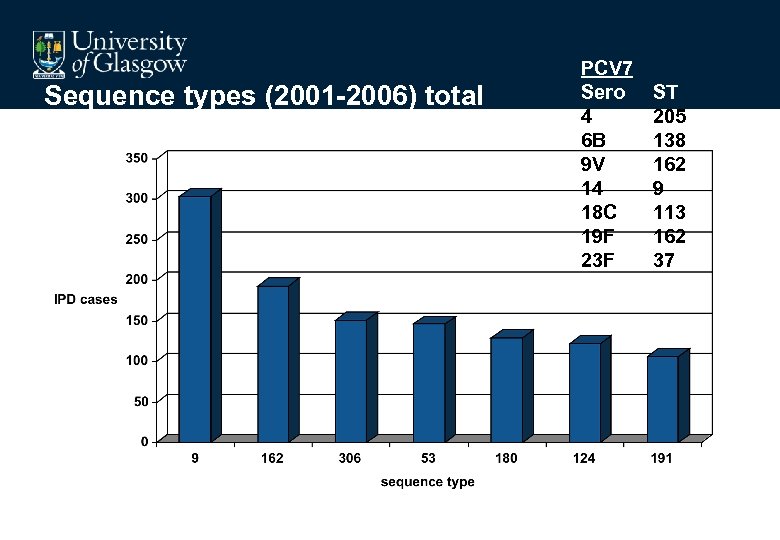
Sequence types (2001 -2006) total PCV 7 Sero 4 6 B 9 V 14 18 C 19 F 23 F ST 205 138 162 9 113 162 37
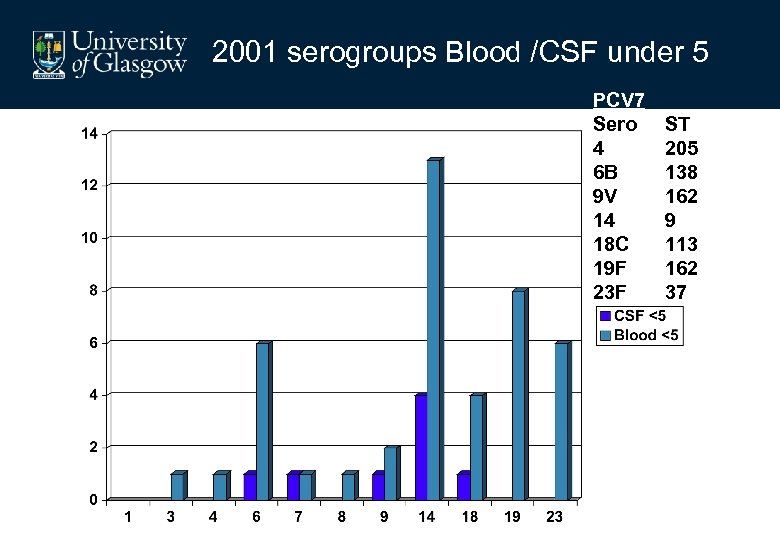
2001 serogroups Blood /CSF under 5 PCV 7 Sero 4 6 B 9 V 14 18 C 19 F 23 F ST 205 138 162 9 113 162 37
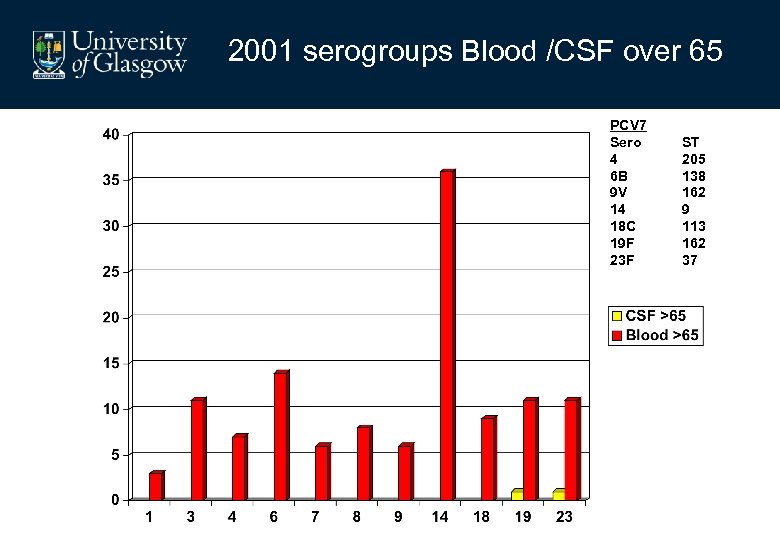
2001 serogroups Blood /CSF over 65 PCV 7 Sero 4 6 B 9 V 14 18 C 19 F 23 F ST 205 138 162 9 113 162 37
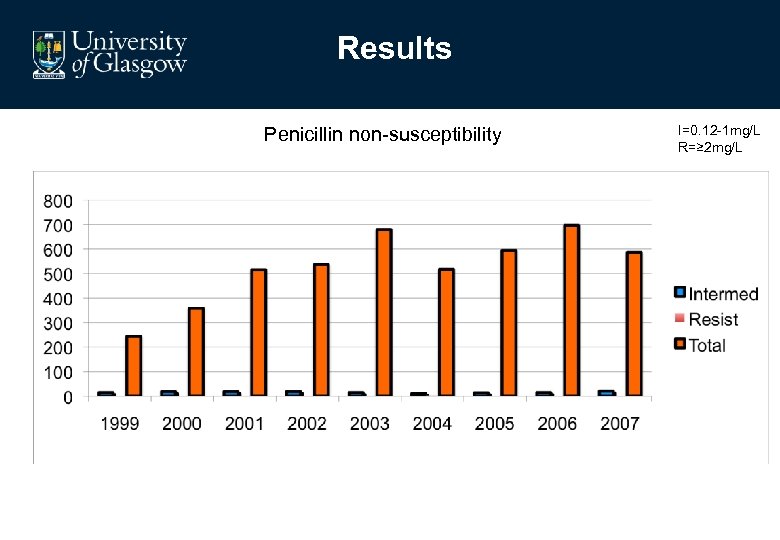
Results Penicillin non-susceptibility I=0. 12 -1 mg/L R=≥ 2 mg/L
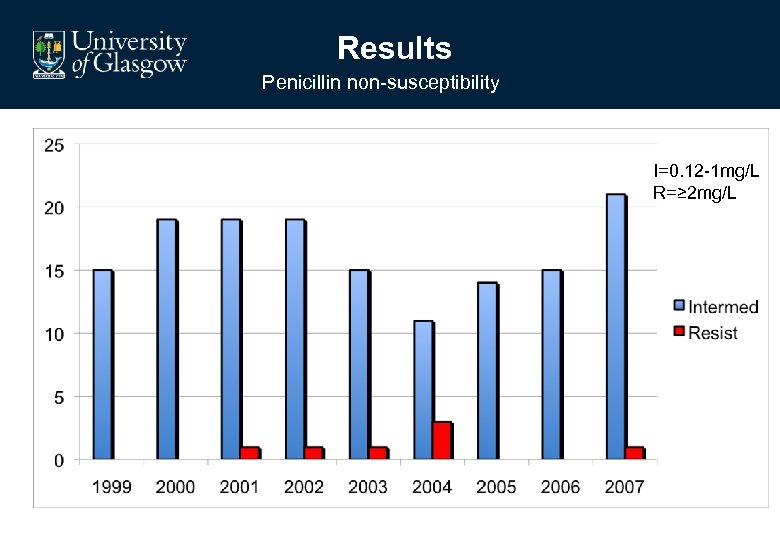
Results Penicillin non-susceptibility I=0. 12 -1 mg/L R=≥ 2 mg/L

• Pneumococcal penicillin resistance is rare • MIC ≥ 2 mgl-1 • Highest MIC found = 2 mgl-1 • N=7 (0. 15%) • Mainly represented by serogroup 14

• Pneumococcal penicillin intermediate sensitivity • MIC 0. 12 -1 mgl-1 • N=148 (3%) • Mainly represented by serogroup 14
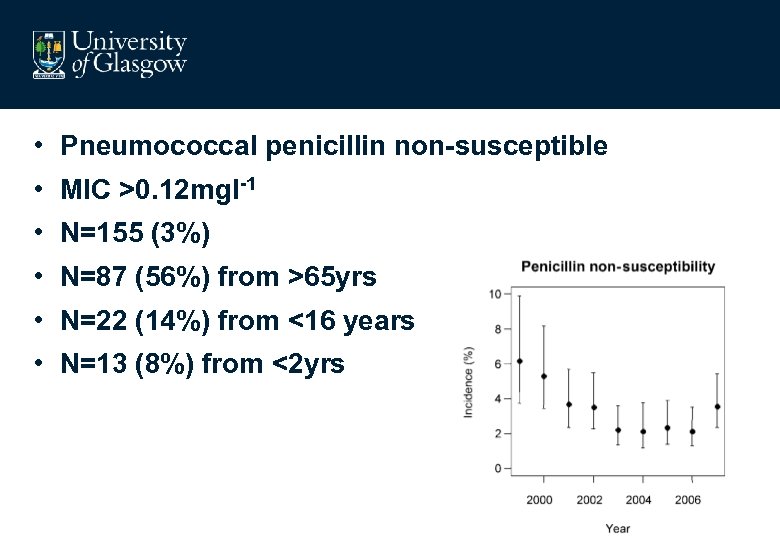
• Pneumococcal penicillin non-susceptible • MIC >0. 12 mgl-1 • N=155 (3%) • N=87 (56%) from >65 yrs • N=22 (14%) from <16 years • N=13 (8%) from <2 yrs

• Pneumococcal penicillin non-susceptible • MIC >0. 12 mgl-1 • Varied with age (P=0. 01) • 4. 1 % >65 yrs (95% CI 3. 3 -5. 0%) • 2. 4% 16 -64 yrs (95% CI 1. 8 -3. 2%) • 3. 1% <16 yrs (95% CI 2. 1 -4. 7%)

• Pneumococcal blood culture isolates • N=4531 (96%) • N= 143 (3%) were pen non-susceptible (MIC >0. 12 mgl 1) • Pneumococcal CSF isolates • N=171 (4%) • N=6 were pen non-susceptible (MIC >0. 12 mgl-1)
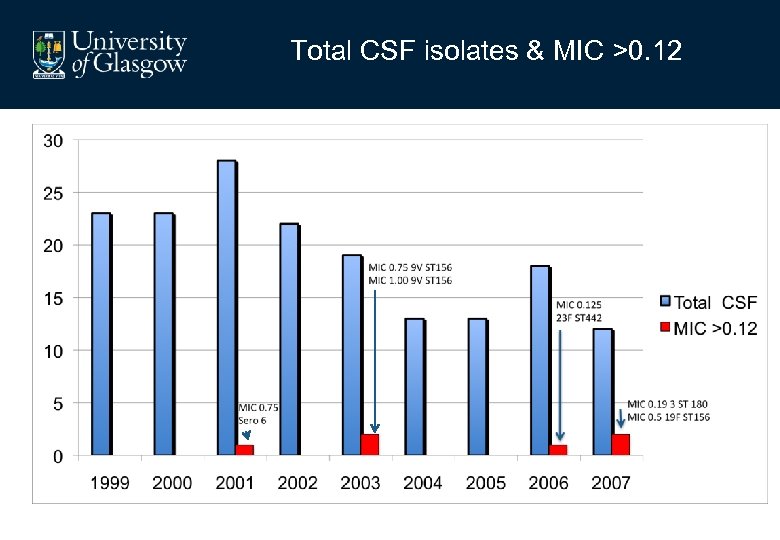
Total CSF isolates & MIC >0. 12
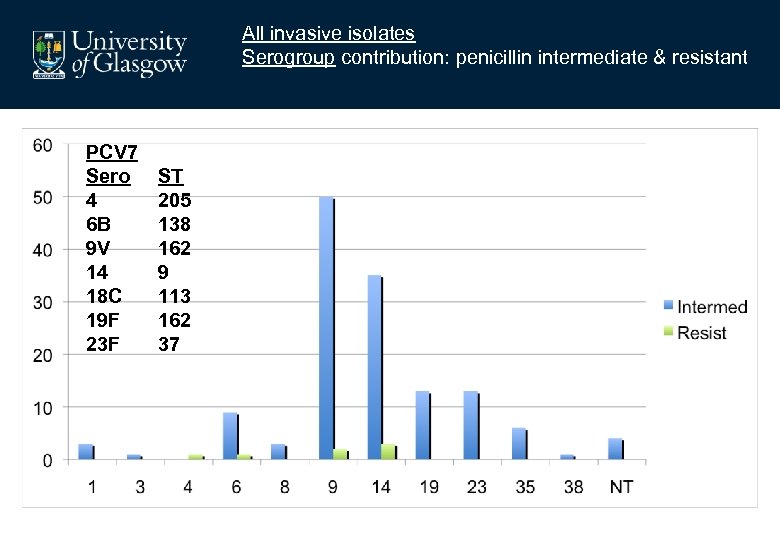
All invasive isolates Serogroup contribution: penicillin intermediate & resistant PCV 7 Sero 4 6 B 9 V 14 18 C 19 F 23 F ST 205 138 162 9 113 162 37

Clinical significance of intermediate sensitivity? • Non-meningeal pneumococcal infections • Doubtful (Choi & Lee 1998) • Drug levels usually >MIC (Heiber & Nelson 1977) • Pharmacodynamics: T>40% MIC • Meningeal pneumococcal infections • Impact of blood brain barrier • Lower levels of resistance associated with failure (Friedland 1992) • Increased failure of monotherapy if MIC>1
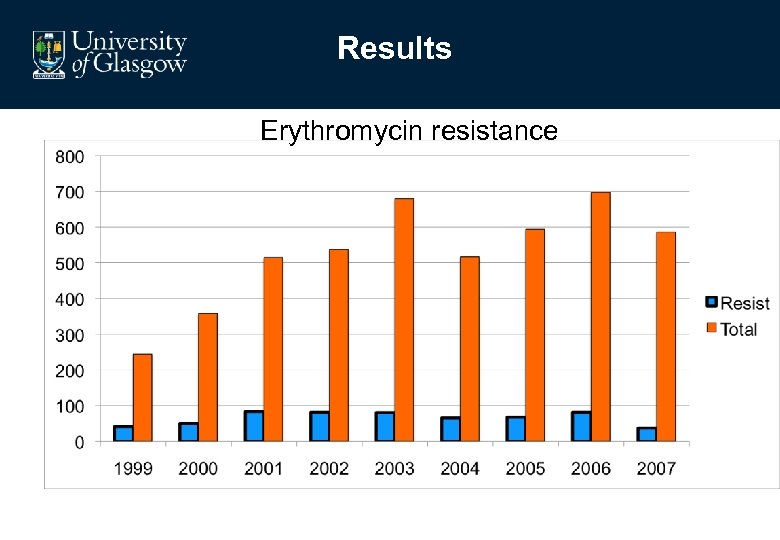
Results Erythromycin resistance
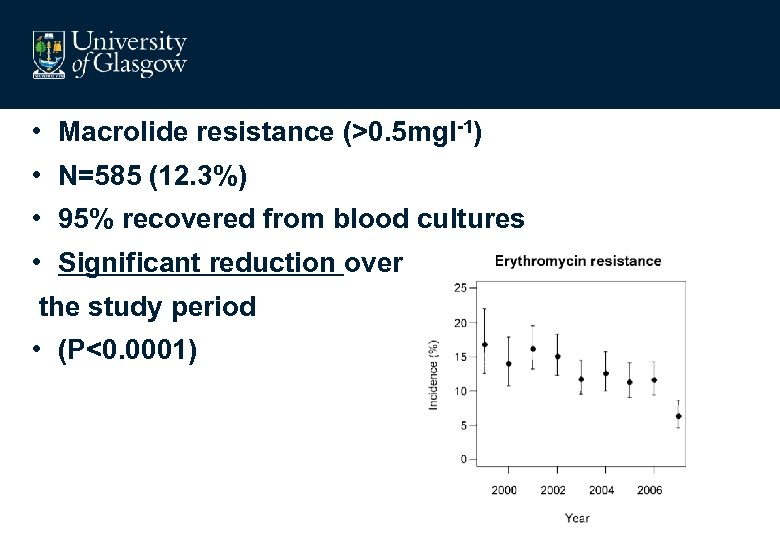
• Macrolide resistance (>0. 5 mgl-1) • N=585 (12. 3%) • 95% recovered from blood cultures • Significant reduction over the study period • (P<0. 0001)
• Macrolide resistance & serogroup • 22 different serogroups • Serotype 14 = 467 (80%)

PMEN clones identified in Scottish invasive pneumococcal isolates (2003 -2007) • PMEN clones • Internationally distributed clones identified by serotype and MLST • should have wide geographic distribution (isolated on at least 2 continents) • Can be resistant to one or more antibiotics that are in wide clinical use; or a global susceptible clone known to be important in disease http: //www. sph. emory. edu/PMEN/pmen_ww_spread_clones. html
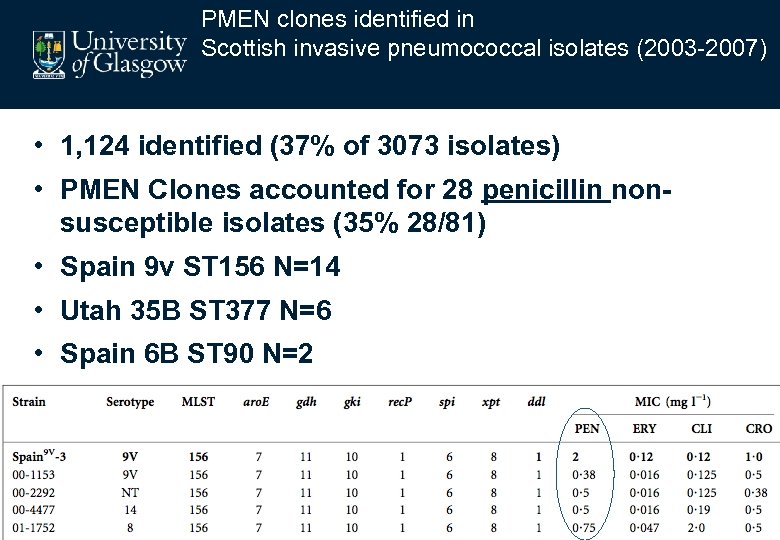
PMEN clones identified in Scottish invasive pneumococcal isolates (2003 -2007) • 1, 124 identified (37% of 3073 isolates) • PMEN Clones accounted for 28 penicillin nonsusceptible isolates (35% 28/81) • Spain 9 v ST 156 N=14 • Utah 35 B ST 377 N=6 • Spain 6 B ST 90 N=2

PMEN clones identified in Scottish invasive pneumococcal isolates (2003 -2007) • 1, 124 identified (37% of 3073 isolates) • PMEN Clones accounted for 248 of the macrolide resistant isolates (75% 248/330) • England 14 ST 9 N=230

PMEN clones identified in Scottish invasive pneumococcal isolates (2003 -2007) • Frequency of PMEN clones • England 14 ST 9 n= 239 • Sweden 1 ST 306 = 225 • Netherlands 8 ST 53 = 154 • Netherlands 7 F ST 191 = 136 • Netherlands 3 ST 180 = 126
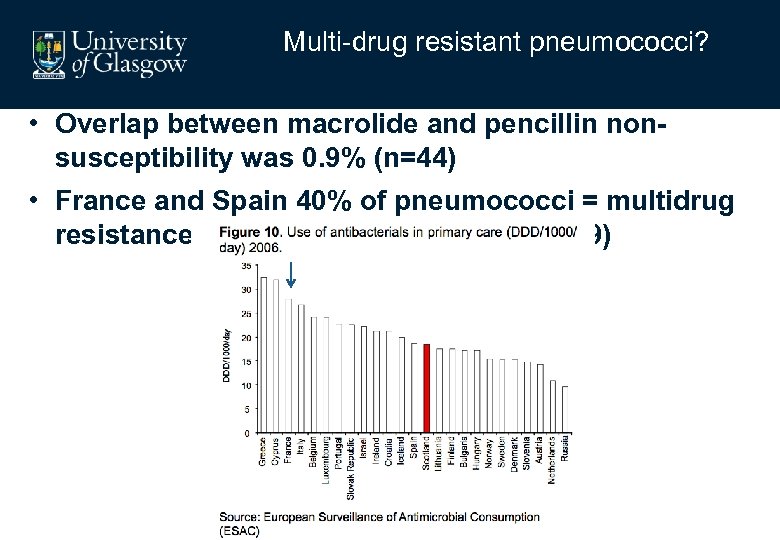
Multi-drug resistant pneumococci? • Overlap between macrolide and pencillin nonsusceptibility was 0. 9% (n=44) • France and Spain 40% of pneumococci = multidrug resistance (Reinert Clin Micro Infect 2009)
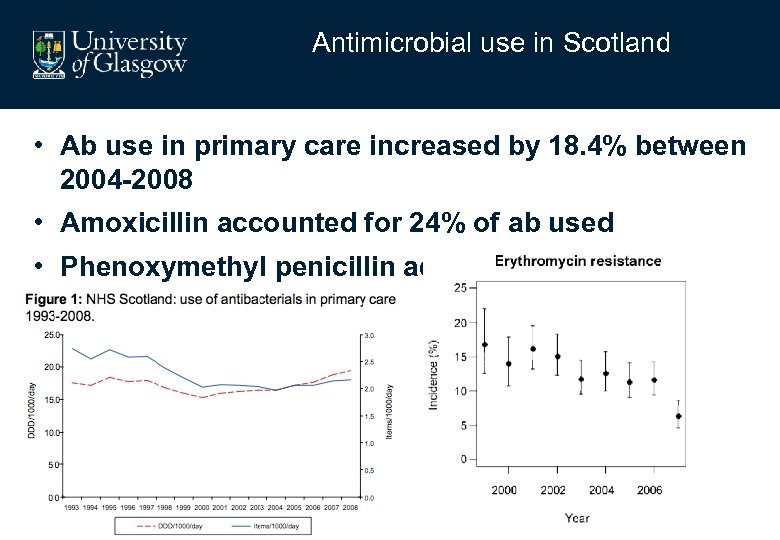
Antimicrobial use in Scotland • Ab use in primary care increased by 18. 4% between 2004 -2008 • Amoxicillin accounted for 24% of ab used • Phenoxymethyl penicillin accounted for 4%

Is Ab resist associated with a fitness cost? • Yes • Adult pneumonia with PRSP = milder clinical manifestations (Einarsson et al SCJID 1998) • ICU admin No sig diff pen MIC>25 vs lower (Moroney et al CID 2001) • Adult pneumococcal pneumonia (10. 5% isolates MIC>1 no signif diff (N=465 adults) (Bedas et al 2001) • In vitro (mice) virulent phenotype was predictive of pen susceptibility (Azoulay-Dupuis et al AAC 2000)

Is Ab resist associated with a fitness cost? • NO (i. e. increased mortality) • Adult pneumonia with PRSP (>4) (Feiken et al AJPH 2000) • Pen MIC>2 independent predictor of mortality (bacteraemia) (Turett et al CID 1999 ) • But • Old age remains biggest predictor of mortality (Mufson et al AJM 1999) • Also chronic renal failure • APACHE II score predict prognosis of bacteraemic disease (Kalin et al 1999)

Conclusions • Relatively low levels of ab resist in invasive pneumococci from Scotland 1999 -2007 • Most common penicillin non-susceptible clone is serogroup 9 MLST 156 clone (PMEN Spain 9 v) • Most common macrolide resistant clone is the serotype 14 MLST 9 clone (PMEN England 14) • Non-susceptibility was rare among non vaccine (PCV 7) serogroups • Pen non-susceptible serotype not covered by PCV 7 or PCV 13 is 35 B ST 377
f69c78149fddcee86ecf115f22f84ab4.ppt