fca957d42f2064de0c7bf202be8086e7.ppt
- Количество слайдов: 68

Researching Venous Thromboembolism in vulnerable adult populations Professor DA Fitzmaurice Department of Primary Care & General Practice University of Birmingham

Conclusions 1 • Risk factors for venous thromboembolism (VTE) are common and widespread (and not just in hospital) • VTE is a common disease • VTE is a major cause of death • The majority of VTE-associated deaths are sudden PE or following undiagnosed and untreated VTE • Therefore VTE must be managed by prevention

Conclusions 2 • Many of these events and deaths are preventable with available effective prophylaxis • We know this is true for hospital inpatients, lack of research outside medical/surgical environments

VTE • Comprises DVT and PE • 3 rd leading cause of cardiovascular mortality • 25 -60, 000 deaths per year in UK • 900, 000 across Europe • 50% may be due to hospital stay • 1/20 lifetime incidence

THE SIZE OF THE VTE PROBLEM • An estimated 60, 000 deaths due to VTE in the UK • 2/3 due to hospital admission of which 25, 000 are preventable • Hospital acquired VTE causes more deaths than hospital acquired infection (MRSA & C difficile, peaked at 10, 000) • Autopsy data suggests reported incidences are markedly underestimated. Baglin J Clin Path 1997; 50: 609 -10 • Registered deaths in England in 2007 -19, 000 - but underdiagnosed…(House of Commons Question summer 2009)

Hospital Preventive Strategies "Making Health Care Safer: a Critical Analysis. . . " A systematic review ranked 79 safety interventions • Based on the strength of evidence • The highest ranked safety practice was the "appropriate use of prophylaxis to prevent VTE. . " • Based on overwhelming evidence that thromboprophylaxis reduces adverse patient outcomes and decreasing overall costs Shojania KG. Agency for Healthcare Research and Quality 2001; 20 July. Available at www. ahrq. gov/clinic/ptsafety.

VTE prevention in SURGICAL patients
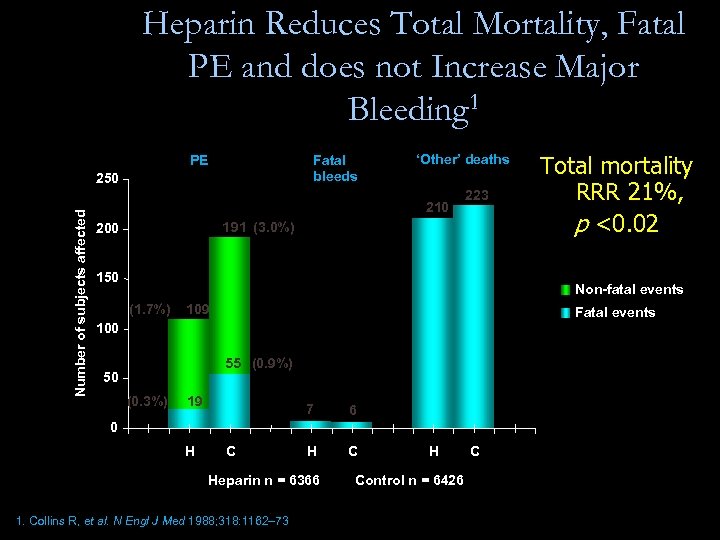
Heparin Reduces Total Mortality, Fatal PE and does not Increase Major Bleeding 1 Fatal bleeds PE Number of subjects affected 250 ‘Other’ deaths 210 223 191 (3. 0%) 200 150 Total mortality RRR 21%, p <0. 02 Non-fatal events (1. 7%) 109 Fatal events 100 55 (0. 9%) 50 (0. 3%) 19 7 6 H C 0 H C Heparin n = 6366 1. Collins R, et al. N Engl J Med 1988; 318: 1162– 73 H Control n = 6426 C

VTE prevention in MEDICAL patients
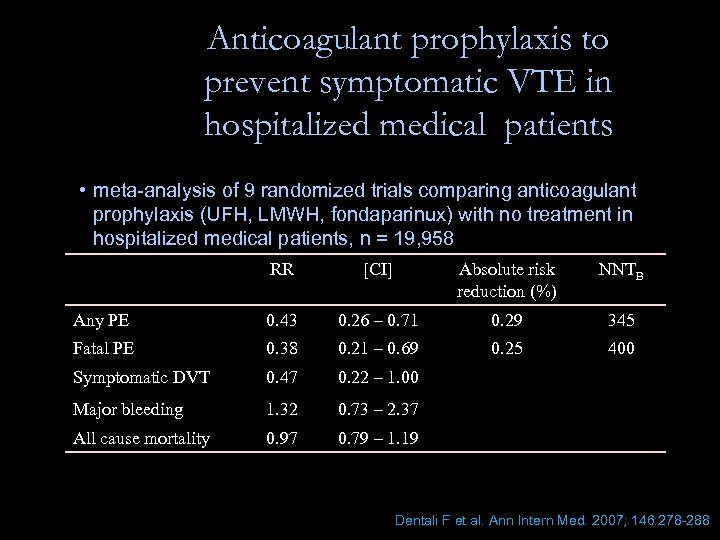
Anticoagulant prophylaxis to prevent symptomatic VTE in hospitalized medical patients • meta-analysis of 9 randomized trials comparing anticoagulant prophylaxis (UFH, LMWH, fondaparinux) with no treatment in hospitalized medical patients, n = 19, 958 RR [CI] Absolute risk reduction (%) NNTB Any PE 0. 43 0. 26 – 0. 71 0. 29 345 Fatal PE 0. 38 0. 21 – 0. 69 0. 25 400 Symptomatic DVT 0. 47 0. 22 – 1. 00 Major bleeding 1. 32 0. 73 – 2. 37 All cause mortality 0. 97 0. 79 – 1. 19 Dentali F et al. Ann Intern Med. 2007; 146: 278 -288

VTE prevention in PRACTICE
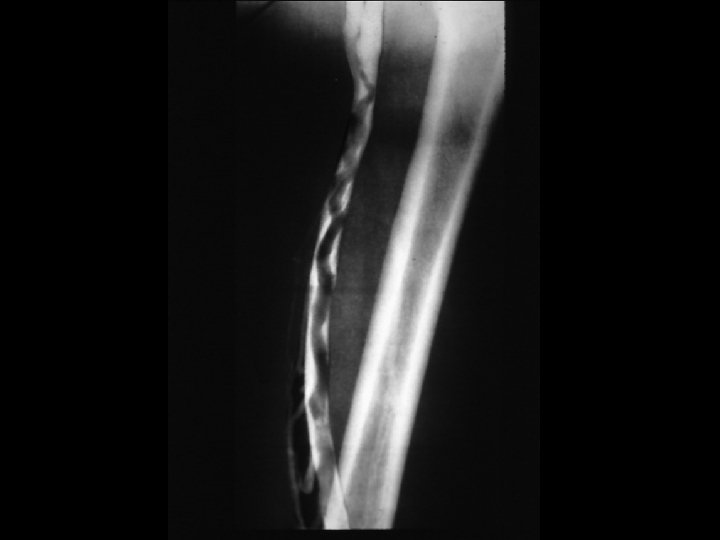
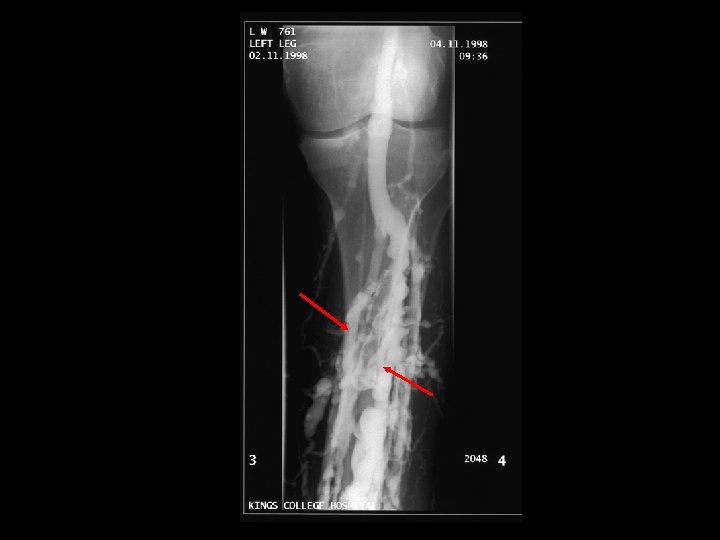
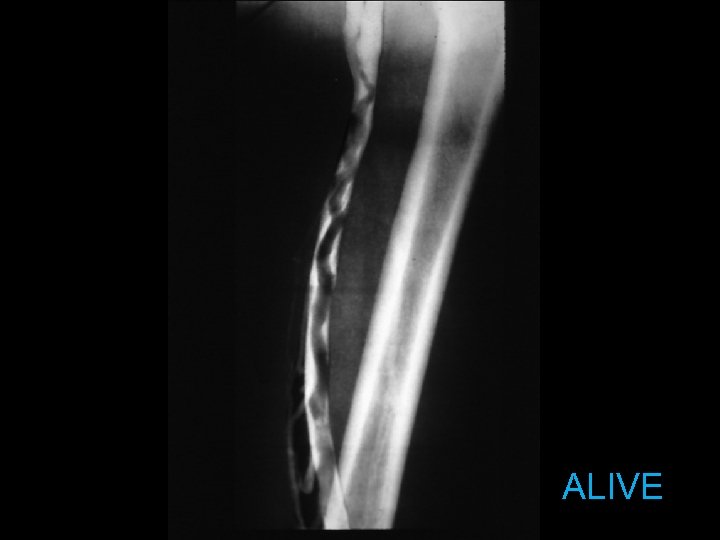
ALIVE
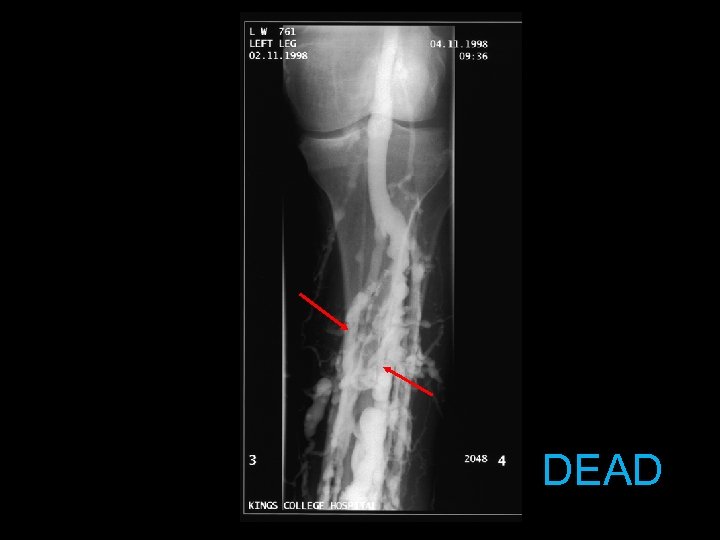
DEAD
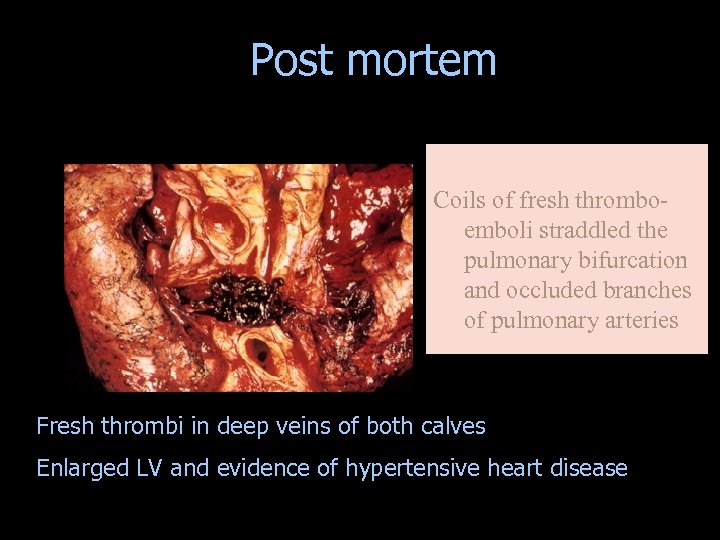
Post mortem Coils of fresh thromboemboli straddled the pulmonary bifurcation and occluded branches of pulmonary arteries Fresh thrombi in deep veins of both calves Enlarged LV and evidence of hypertensive heart disease

Overview • The problem • Risk factors • Prophylaxis in medical patients • Therapeutic options • New studies


Public / Media perception - travel

Travelling in cramped conditions

Other media perceptions: Gamerelated / Office Workers?


VTE Hospital Trends
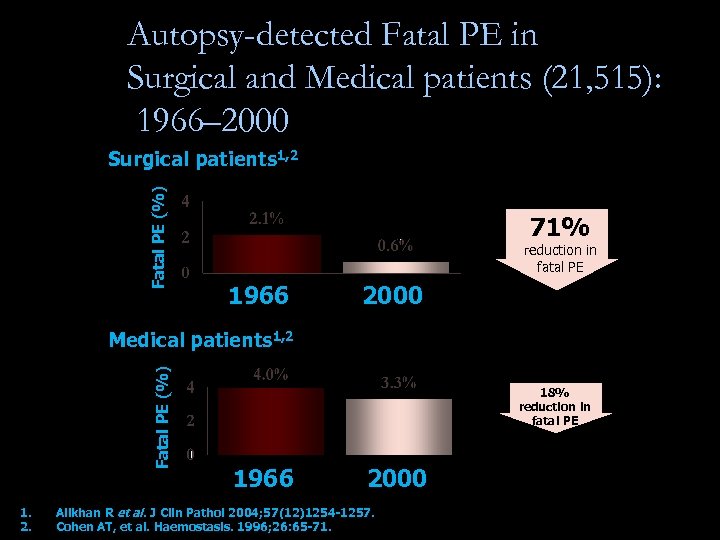
Autopsy-detected Fatal PE in Surgical and Medical patients (21, 515): 1966– 2000 Fatal PE (%) Surgical patients 1, 2 71% reduction in fatal PE 1966 2000 Fatal PE (%) Medical patients 1, 2 1. 2. 18% reduction in fatal PE 1966 2000 Alikhan R et al. J Clin Pathol 2004; 57(12)1254 -1257. Cohen AT, et al. Haemostasis. 1996; 26: 65 -71.

Autopsy Proven Fatal PE % in Medical Patients • Incidence of fatal PE • Studies from Scandinavia, USA and UK • 59% to 83% Nielsen et al. Acta Med Scand 1981; 209: 351 -5 Hauch et al. Acta Chir Scand 1990; 156: 747 -9 Sperry et al. Hum Pathol 1990; 21: 159 -65 Cohen et al. Haemostasis 1996; 26: 65 -71
Medical Inpatients 60% of admissions 75% of PE deaths 10% of consensus statements Cohen et al. Haemostasis 1996; 26: 65 -71

Epidemiology of VTE • Mortality
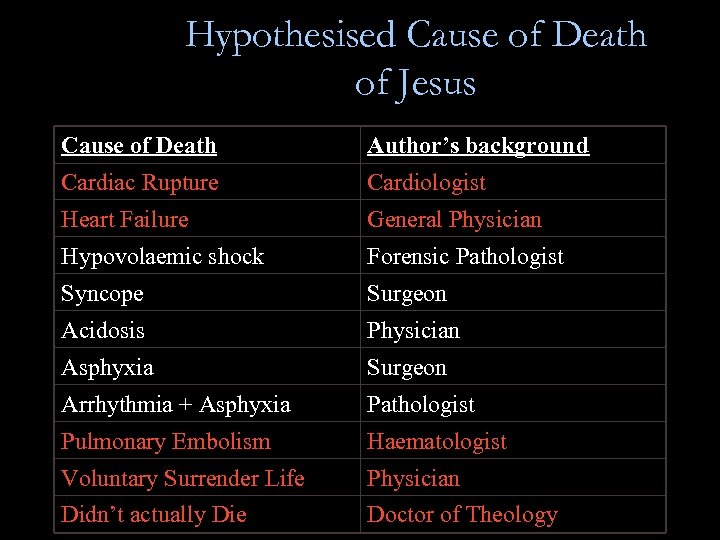

Hypothesised Cause of Death of Jesus Cause of Death Author’s background Cardiac Rupture Cardiologist Heart Failure General Physician Hypovolaemic shock Forensic Pathologist Syncope Surgeon Acidosis Physician Asphyxia Surgeon Arrhythmia + Asphyxia Pathologist Pulmonary Embolism Haematologist Voluntary Surrender Life Physician Didn’t actually Die Doctor of Theology
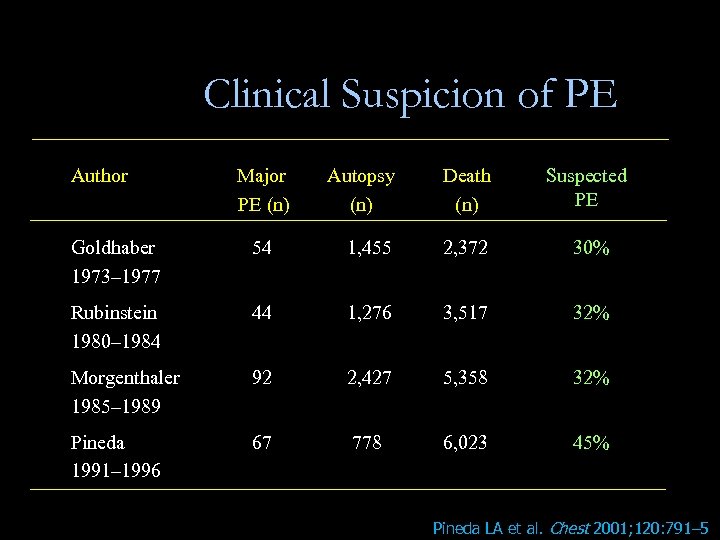
Clinical Suspicion of PE Author Major PE (n) Autopsy (n) Death (n) Suspected PE Goldhaber 1973– 1977 54 1, 455 2, 372 30% Rubinstein 1980– 1984 44 1, 276 3, 517 32% Morgenthaler 1985– 1989 92 2, 427 5, 358 32% Pineda 1991– 1996 67 778 6, 023 45% Pineda LA et al. Chest 2001; 120: 791– 5

Overview • The problem • Risk factors • Prophylaxis in medical patients • New studies

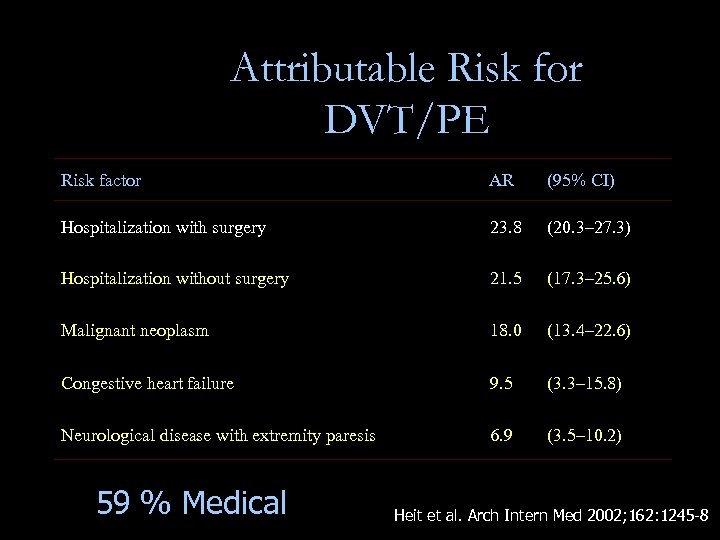
Attributable Risk for DVT/PE Risk factor AR (95% CI) Hospitalization with surgery 23. 8 (20. 3– 27. 3) Hospitalization without surgery 21. 5 (17. 3– 25. 6) Malignant neoplasm 18. 0 (13. 4– 22. 6) Congestive heart failure 9. 5 (3. 3– 15. 8) Neurological disease with extremity paresis 6. 9 (3. 5– 10. 2) 59 % Medical Heit et al. Arch Intern Med 2002; 162: 1245 -8

Overview • The problem • Risk factors • Prophylaxis in medical patients • New studies • Therapeutic options

H e p a r i n s Here is Darla being kissed by Chuck Ford, Senior Director of Clinical Operations for the Emergency Department of the IU Burn Center at Wishar w o r k
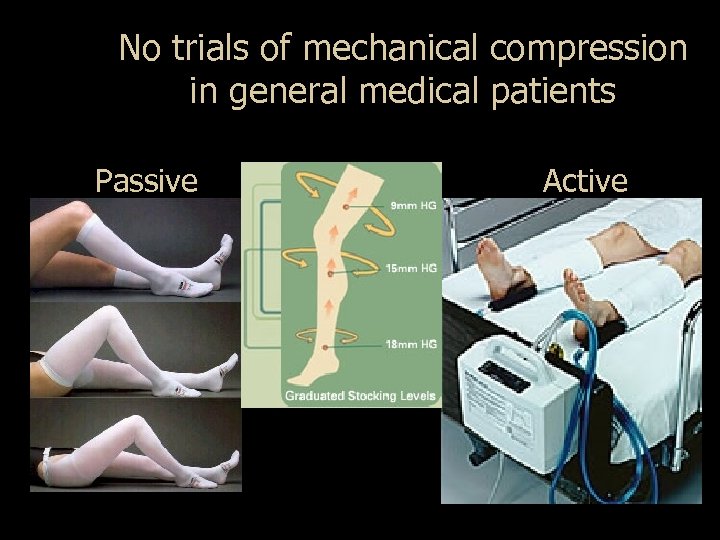
No trials of mechanical compression in general medical patients Passive Active

1980’s LMWH
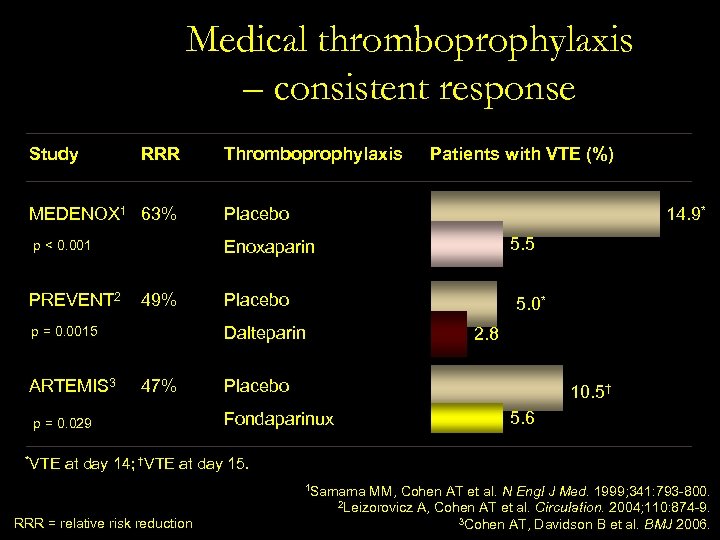
Medical thromboprophylaxis – consistent response Study RRR Thromboprophylaxis MEDENOX 1 63% Placebo p < 0. 001 Patients with VTE (%) Enoxaparin PREVENT 2 49% 47% p = 0. 029 *VTE 5. 5 Placebo 5. 0* Dalteparin p = 0. 0015 ARTEMIS 3 14. 9* 2. 8 Placebo 10. 5† 5. 6 Fondaparinux at day 14; †VTE at day 15. 1 Samama RRR = relative risk reduction MM, Cohen AT et al. N Engl J Med. 1999; 341: 793 -800. 2 Leizorovicz A, Cohen AT et al. Circulation. 2004; 110: 874 -9. 3 Cohen AT, Davidson B et al. BMJ 2006.
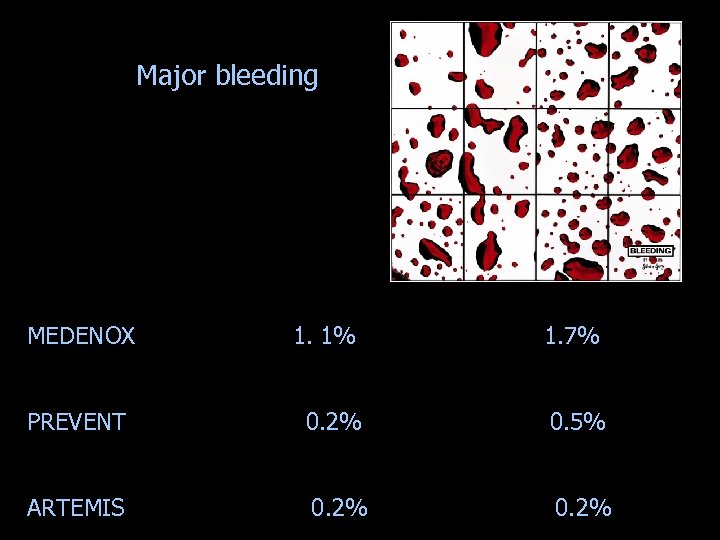
Major bleeding MEDENOX 1. 1% 1. 7% PREVENT 0. 2% 0. 5% ARTEMIS 0. 2%

Overview • The problem • Risk factors • Prophylaxis in medical patients • New studies – based on ACCP recommendations

American College of Chest Physicians recommendations Are the gold standard Are not just American but are written by experts from all over the globe ACCP

New Studies VITAE – Epidemiology PREVAIL Study – Stroke ENDORSE study – Survey EXCLAIM study – Medical

The Burden – VITAE Study
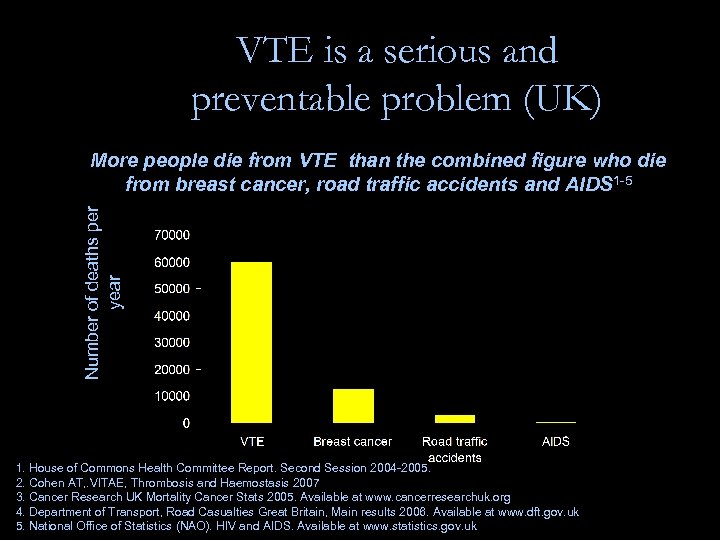
VTE is a serious and preventable problem (UK) Number of deaths per year More people die from VTE than the combined figure who die from breast cancer, road traffic accidents and AIDS 1 -5 1. House of Commons Health Committee Report. Second Session 2004 -2005. 2. Cohen AT, . VITAE, Thrombosis and Haemostasis 2007 3. Cancer Research UK Mortality Cancer Stats 2005. Available at www. cancerresearchuk. org 4. Department of Transport, Road Casualties Great Britain, Main results 2006. Available at www. dft. gov. uk 5. National Office of Statistics (NAO). HIV and AIDS. Available at www. statistics. gov. uk
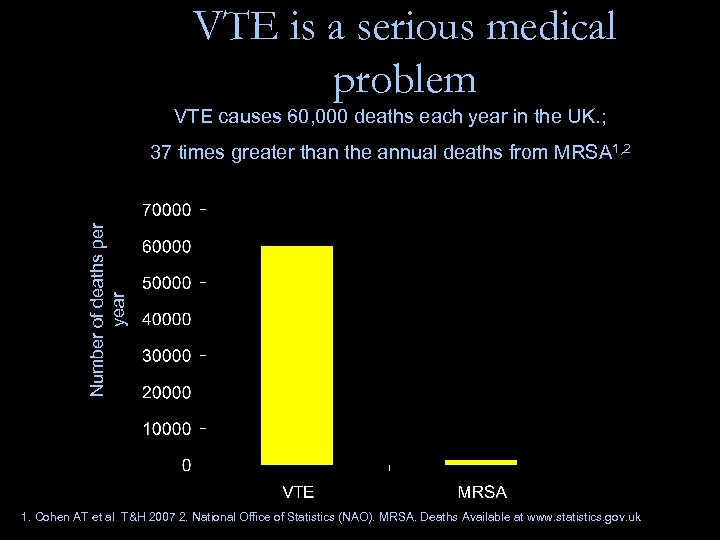
VTE is a serious medical problem VTE causes 60, 000 deaths each year in the UK. ; Number of deaths per year 37 times greater than the annual deaths from MRSA 1, 2 1. Cohen AT et al T&H 2007 2. National Office of Statistics (NAO). MRSA. Deaths Available at www. statistics. gov. uk
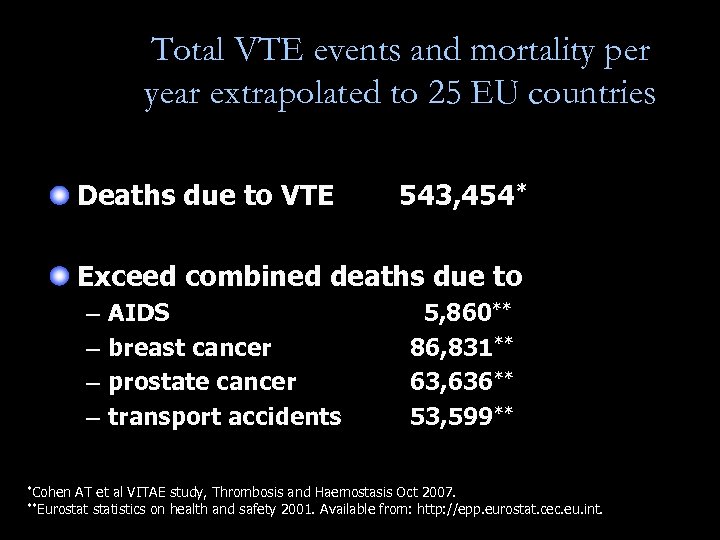
Total VTE events and mortality per year extrapolated to 25 EU countries Deaths due to VTE 543, 454* Exceed combined deaths due to – – *Cohen AIDS breast cancer prostate cancer transport accidents 5, 860** 86, 831** 63, 636** 53, 599** AT et al VITAE study, Thrombosis and Haemostasis Oct 2007. statistics on health and safety 2001. Available from: http: //epp. eurostat. cec. eu. int. **Eurostat


Design and hospital characteristics • Multinational, cross-sectional survey • Hospitals randomly selected from authoritative national lists of all acute care hospitals • Hospitals with greater than 50 beds for – Acute medical illnesses – Elective major surgery

All hospital wards were included in this survey except • Psychiatric • Pediatric • Palliative care • Maternity/obstetrics • Neonatal • Burn units • Eye, ear, nose and throat units • Dermatological/ophthalmologic wards • Rehabilitation units/wards • Emergency units • Long-term care units

Objectives • Primary – To identify patients at risk for venous thromboembolism (VTE) hospitalized in representative hospitals throughout the world – To determine the proportion of patients who receive effective VTE prophylaxis • Secondary – To define the above globally by acute illness (in medical and surgical populations)
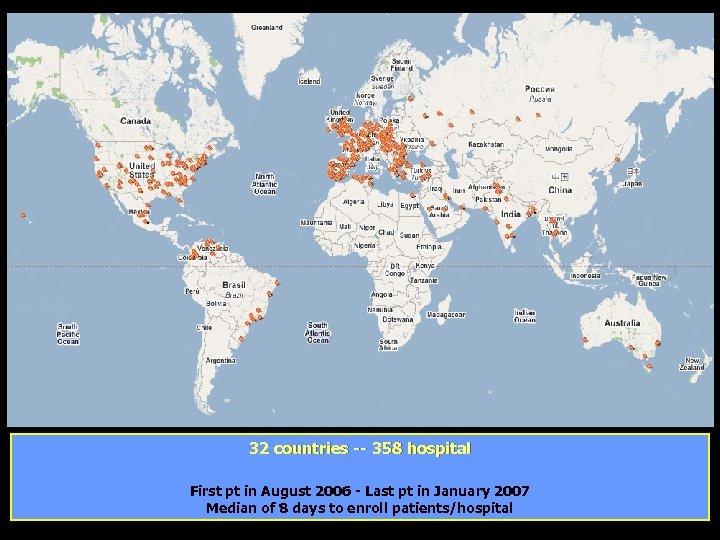
32 countries -- 358 hospital First pt in August 2006 - Last pt in January 2007 Median of 8 days to enroll patients/hospital
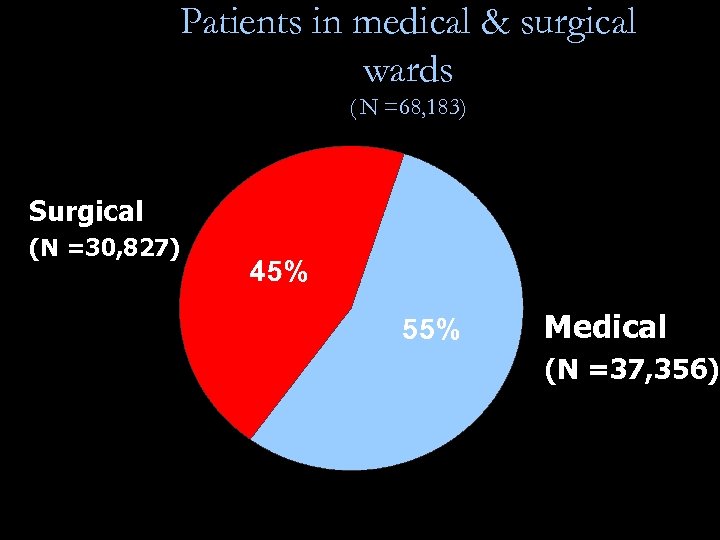
Patients in medical & surgical wards ( N =68, 183) Surgical (N =30, 827) Medical (N =37, 356)
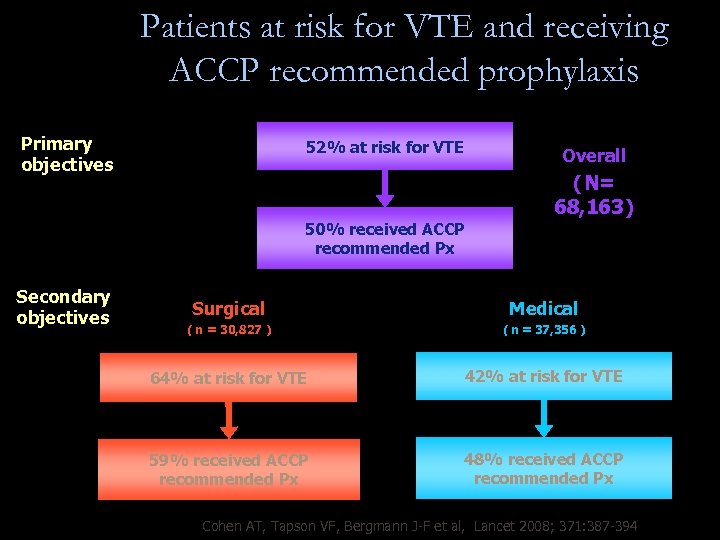
Patients at risk for VTE and receiving ACCP recommended prophylaxis Primary objectives 52% at risk for VTE Overall ( N= 68, 163 ) 50% received ACCP recommended Px Secondary objectives Surgical Medical ( n = 30, 827 ) ( n = 37, 356 ) 64% at risk for VTE 42% at risk for VTE 59% received ACCP recommended Px 48% received ACCP recommended Px Cohen AT, Tapson VF, Bergmann J-F et al, Lancet 2008; 371: 387 -394
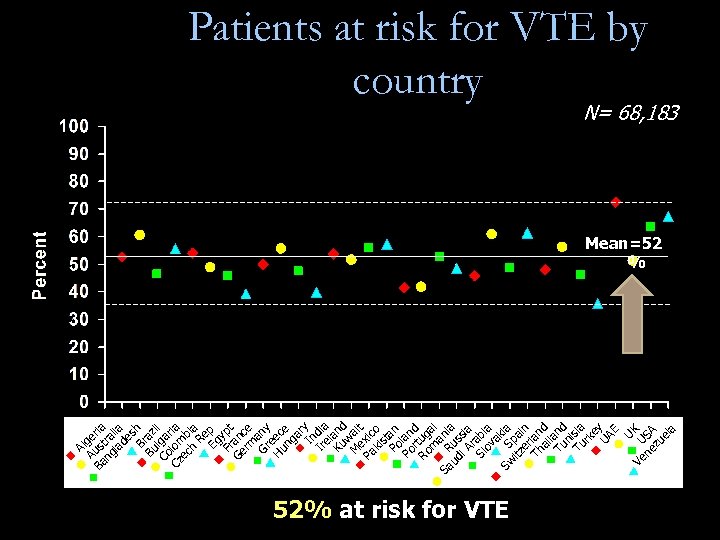
U Ve U K ne SA zu el a A Au lger Ba s ia ng tra la lia de s Br h Bu az i Co lga l ria Cz lom ec b h ia Re Eg p Fr ypt Ge an rm ce Gr any e Hu ec ng e ar In y Ir dia el Ku and w M ait ex Pa ic ki o st Po an Po lan r d Ro tug m al Sa R ani ud us a i A sia r Sl abi ov a a Sw S kia itz pa er in Th lan ai d l Tu and n Tu isia rk e UA y E Patients at risk for VTE by country N= 68, 183 Mean=52 % 52% at risk for VTE
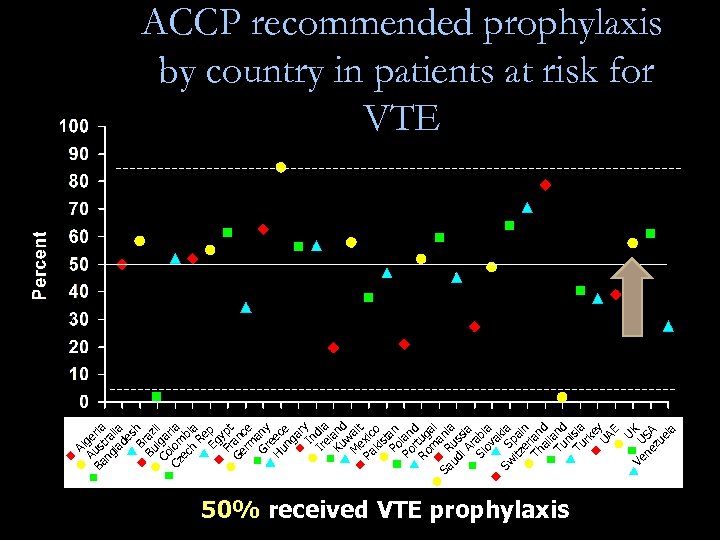
U Ve U K ne SA zu el a A Au lger Ba s ia ng tra la lia de s Br h Bu az i Co lga l ria Cz lom ec b h ia Re Eg p Fr ypt Ge an rm ce Gr any e Hu ec ng e ar In y Ir dia el Ku and w M ait ex Pa ic ki o st Po an Po lan r d Ro tug m al Sa R ani ud us a i A sia r Sl abi ov a a Sw S kia itz pa er in Th lan ai d l Tu and n Tu isia rk e UA y E ACCP recommended prophylaxis by country in patients at risk for VTE 50% received VTE prophylaxis

Conclusions - ENDORSE • First global view of VTE risk and prophylaxis practices • Unprecedented scope: 32 Countries, 358 Hospitals, 68, 183 Patients • Risk for VTE is common (52%) – 64% of surgical patients – 42% of medical patients • Prophylaxis is underutilized (50%) – Surgical patients: Omitted in 41% – Medically ill population: Omitted in 60% Cohen AT, Tapson VF, Bergmann J-F et al, Lancet 2008; 371: 387 -394

These data reinforce the rationale to • Urgently implement hospital-wide strategies • Systematically assess patient risk for VTE • Provide appropriate prophylaxis to prevent VTE Cohen AT, Tapson VF, Bergmann J-F et al, Lancet 2008; 371: 387 -394

Thromboprophylaxis political momentum ew ram g. F tin ra e Op HS N Consistent investment and a coherent strategy leads to Department of Health taking ownership for VTE prevention 2004 2005 2006 2007 2008 lus nc i ork 2009 2010 2 ion 01 1 0/1

Government documents on VTE prevention March 2005 July 2005 April 2007

The role of Primary Care • Ensuring implementation of extended thromboprophylaxis • Education of patients • Risk Assessment? • Commissioning of services?

Research? • Residential homes • Nursing homes • Hospices • Acutely unwell in own home

Issues • • Perception of importance “A good way to go” Measuring incidence/prevalence Use of chemical agents in the community

Proposed study • Nursing home • 1000 residents from 60 homes • Baseline assessment of VTE risk taken, comorbidity, medication, functional ability and VTE prevention strategies and then followed up 3 monthly for 1 year. • Case records will be checked for any change in risk status from baseline.

Proposed study • Outcomes: number of VTE events, associated hospital admissions, deaths and costs in relation to risk assessment and preventive strategies. • Develop a pragmatic risk assessment tool for NH residents, building on the DH risk assessment tool for hospital in-patients

Conclusions 1 • Risk factors for venous thromboembolism (VTE) are common and widespread (and not just in hospital) • VTE is a common disease • VTE is a major cause of death • The majority of VTE-associated deaths are sudden PE or following undiagnosed and untreated VTE • Therefore VTE must be managed by prevention

Conclusions 2 • Many of these events and deaths are preventable with available effective prophylaxis • We know this is true for hospital inpatients, lack of research outside medical/surgical environments

Co-operation and balance are the keys to success

fca957d42f2064de0c7bf202be8086e7.ppt