c2b03a336b4d2f15a1571f8279398a23.ppt
- Количество слайдов: 81

Rebecca L. Johnson, MD Chair, Pathology & Clinical Labs Berkshire Health Systems President, American Board of Pathology

MOC MAINTENANCE OF CERTIFICATION WHY SHOULD I CARE?

History of Board Certification n 1908 Derrick Vail, MD n Presidential address to the American Academy of Ophthalmology & Otolaryngology n “I hope to see the time…. let him then be permitted and licensed to practice ophthalmology. ”

American Board Of Ophthalmology Am. Ophthalmologic Society, AMA, Academy of Ophthalmology n 1915—Defined requirements n 1917—ABO established n

Early Boards n n n n 1924—Am Board of Otolaryngology 1930—Am Board of Obstetrics & Gynecology 1932—Am Board of Derm & Syphilology 1933—Am Board of Pediatrics 1934—Psychiatry & Neurology, Radiology, Orthopedic Surgery 1935—Colon & Rectal Surgery, Urology 1936—Internal Medicine, PATHOLOGY

Advisory Board For Medical Specialties Est. 1933 n Uniformity in MD certification n Increase public awareness n Education, training, and certification n

Advisory Board For Medical Specialties n Four first specialty boards n AHA, AAMC, FSMB, AMA Council on Med Ed & Hospitals, NBME n 1970 - American Board of Medical Specialties (ABMS)

ABMS Purpose Discuss common issues n Advise Boards n Coordinate work n Jurisdiction over policies as delegated n Autonomy of any Board n Stimulate improvements in med ed n

ABMS n 24 Boards 37 Primary specialties n 94 Subspecialties n 2005 ~89% licensed US MDs n Evanston, IL n Kevin Weiss, MD, EVP n www. abms. org n

ABMS MISSION n Improve quality of medical care n n Professional and educational standards for certification Assurance to the public n Certification has meaning and required components

ABMS & Member Boards n Assess n n Education, Training, Licensure, Ethical and professional requirements Initial examination Construction-fair, objective n Psychometrically reliable and valid n Assess knowledge & clinical skills n

Limits of Board Certification Assesses only medical knowledge n Snapshot n SOLUTION? Recertification n Time limited certification n Maintenance of Certification (MOC) n
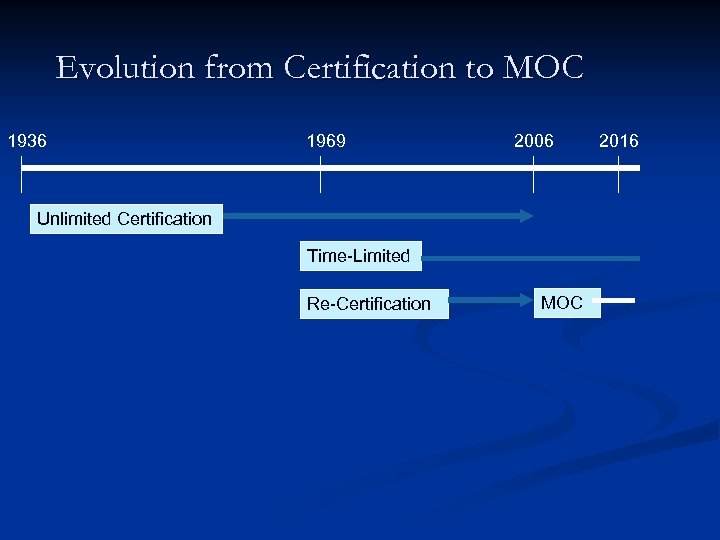
Evolution from Certification to MOC 1936 1969 2006 Unlimited Certification Time-Limited Re-Certification MOC 2016

ABMS n 1993 Member Boards agree to Recertification n 1997/98 ABPath Voluntary Recertification

1998 ABMS Task Force on Competency Mission statement—Diplomates are competent n Define competence n Research and assessment, validation n Template to assess competence n Peer review of certification n Collaborative methods of assessment n

GOALS MOC Relevant • Accountability for competence • Accountability for practice quality • Reshape Continuing Medical Education MOC is Essential; Tied to: • Hospital Credentialing • Maintenance of Licensure • Pay for Performance

Three Trends Make MOC Relevant n Public wants accountability for performance n n Purchaser decision about quality Quality can be measured n n n Patient’s perceptions and health status Guideline adherence and achieving outcomes Quality can be improved n Health care results from system n Change system processes improves care

Relevance of MOC For A Composite Measure of Physician Quality n Customers Healthcare purchasers & patients n Health plans, medical staffs, group practices n n Competitors National Committee for Quality Assessment n Center for Medicare and Medicaid Services n Doctor Quality web sites n n Collaborators JCAHO n State Medical Boards/FSMB n

Changing View of Professionalism Autonomy Collaboration Authority Evidence Assertion Measurement Control Transparency

Accountability n Develop evidence of achieving best results for patient care n Communicate results regularly and widely to those to whom accountability is owed Profession Public

ABMS & ACGME Lifetime Competencies MEDICAL KNOWLEDGE n PATIENT CARE n INTERPERSONAL & COMMUNICATION SKILLS n PROFESSIONALISM n PRACTICE BASED LEARNING & IMPROVEMENT n SYSTEMS BASED PRACTICE n

MOC – A Composite Measure of Competence and Quality Safe Timely Efficient Effective Equitable Patient Centered Competencies IOM Quality Aims

Evolution of MOC 1936 --Certification 2006 - Maintenance of Certification ØTraining Ø Certification after training Ø Competence/Practice Ø Milestone evidence of competence I. Professional standing II. Lifelong learning & selfassessment Ø CME III. Cognitive expertise Ø License & privileges IV. Practice performance & improvement Ø Examination 1998 Voluntary Recertification Ø Examination (optional) Ø Can apply to all certificates Ø Single credential o Board Certification o Maintenance of License o Hospital Privileges o Public accountability


American Board of Pathology 1936 Michigan n Primary Certification n AP/CP, AP, CP Subspecialty certification 10 n ACGME approved fellowship n n Change in training requirements

AMERICAN BOARD OF PATHOLOGY n PRIMARY CERTIFICATION ANATOMIC & CLINICAL PATHOLOGY n ANATOMIC PATHOLOGY n CLINICAL PATHOLOGY n

AMERICAN BOARD OF PATHOLOGY- SUBSPECIALTY n n n n n Blood Banking/Transfusion Medicine Chemical Pathology Cytopathology Dermatopathology* Forensic Pathology Hematology Medical Microbiology Molecular Genetic Pathology* Neuropathology Pediatric Pathology

ABP Cooperating Societies n n n n ACLPS ADASP AMA Pathology Section Council APC ASCP ASIP CAP USCAP

Maintenance of Certification n ABMS initiative n All 24 specialty boards n 2006 -Time-limited (10 year) primary and subspecialty certificates n Participation in MOC process required n Completed within 8 -10 years
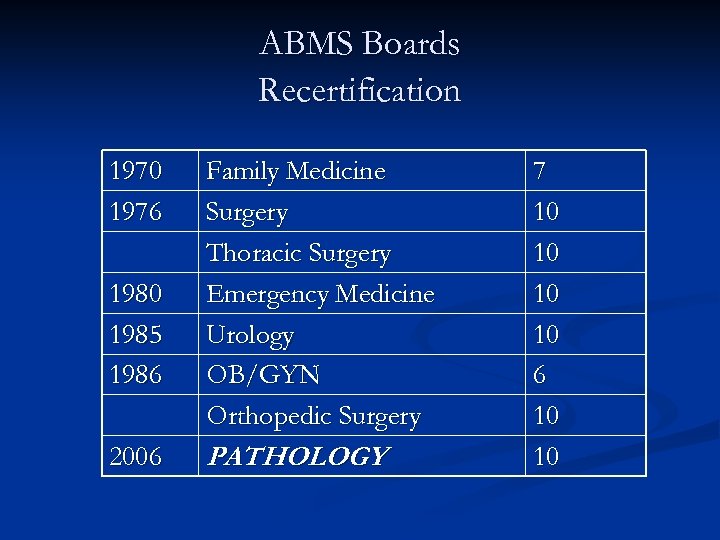
ABMS Boards Recertification 1970 1976 1980 1985 1986 2006 Family Medicine Surgery Thoracic Surgery Emergency Medicine Urology OB/GYN Orthopedic Surgery PATHOLOGY 7 10 10 6 10 10

MOC Components n n Professional Standing Lifelong Learning & Self. Assessment Cognitive Expertise (the EXAM!) Evaluation of Performance in Practice

Part I Professional Standing n Maintenance of a full and unrestricted license in at least one U. S. jurisdiction, territory, or Canada n Documentation of medical staff membership and privileges or, if not applicable, scope of practice n Documentation of licensure and medical staff privileges at 4 th and 8 th year

Part II Life Long Learning- Self-Assessment n 70 Category 1 CME credits / 2 year cycle n 20 CME credits / 2 yr cycle must be SAMs n 80% CME related to individual’s practice n Updated electronic record of activities every 2 years n A fellowship fulfills Part II requirements for 2 year period n Incomplete fellowships prorated

Part II Life Long Learning and Self-Assessment n Content specifications n Important advancements, key concepts n Basis for CME and self-assessment n Prep for MOC exam. n Direct MOC test question development n Practical “need to know” information, used in daily practice, required for competence n Cover all disciplines of pathology

Part II Life Long Learning-Self-Assessment AP and CP Content Committees’ “Content Outlines” on line, updated annually n Fundamental information for daily practice; important, validated new knowledge n Outlines are not templates for exam or endorsements of authors n

Self-Assessment Modules (SAMs) n Elements of SAMs n Educational product n Self-administered exam n Minimum performance level n Feedback n n SAM requirement for 2006 -09 period waived because of insufficient offerings Certificates issued by societies should reflect regular CME versus CME / SAM

Part III--Cognitive Expertise n Examination is mandatory n “Secure” and closed book n At least once per year n Taken 8 -10 years after initial certification n Potential 3 year period of qualification

Part III - Cognitive Expertise Modular exams related to practice n Exams will include: n Fundamental knowledge n Current practice-related knowledge n Emphasis on information new to field n Practice environment knowledge n

Part III Cognitive Expertise n AP/CP certified individuals may chose to maintain their certification in AP/CP, AP only or CP only n Individuals with subspecialty certification may choose to maintain only their subspecialty certification

Part III Cognitive Expertise MOC exam: n “tailor” exam to practice by selecting modules. n Menu of multiple modules n At least one general module of AP or CP must be selected by AP/CP examinees

Part III - Cognitive Expertise MOC EXAM n 6 modules of 25 questions (150 total questions) n 80% practical (virtual microscopy, case-based questions etc); 20% written n Modules graded as one exam

AP/CP MOC Exam Option 1 + Option 2 + Option 3 + + 4 add. = total 6 + 3 add. = 6 total CP General module AP Specialty module
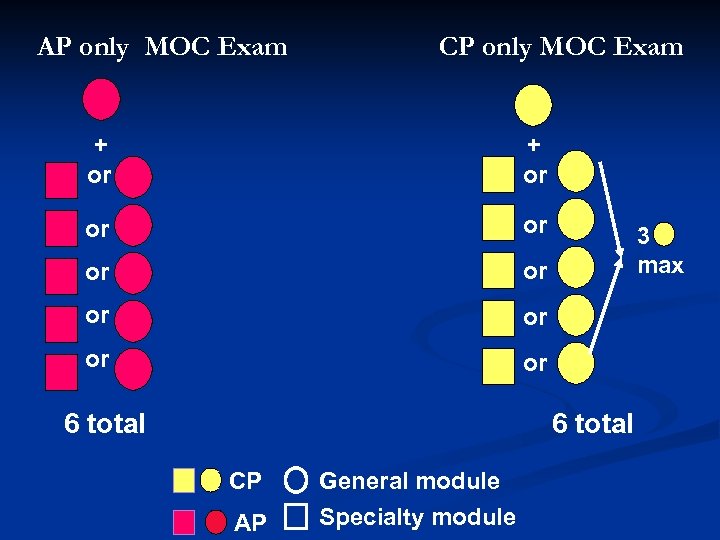
AP only MOC Exam CP only MOC Exam + or or or 6 total 3 max 6 total CP AP General module Specialty module

Modules Clinical Pathology General CP I, III, IV Hematology I, II Blood Bank I, II Immunopathology Blood Bank-Coagulation Microbiology I, II Coagulation Chemistry I, II

Modules Anatomic Pathology Gen AP I, II Breast Gen Surg Path I, II Cardiovascular General Cytology I, II Dermatology I, II Cytology, Gyn Endocrine Cytology, Non Gyn GI-Liver-Biliary Bone-Soft Tissue Autopsy Revised 11/08

Modules Revised 11/08 Anatomic Pathology cont’d Genitourinary Pediatric Pathology Gynecologic Pulmonary/Mediastinal Head-Neck Transplant pathology Medical Renal Forensic Pathology Neuropathology

Common Modules* Revised 11/08 Anatomic and Clinical Pathology General Hemepath I (Lymph node-Spleen) Flow Cytometry General Hemepath II (Bone Marrow) Molecular Pathology Molecular-Cytogenetics Lab Man / Informatics * May be used to fulfill AP or CP specialty modules

Part III—Exam & MOC Myths High stakes—Low failure rate n Irrelevant—Modular n Not useful—Improves MK, Pt. Care n Time consuming—Payoff- meet pt and regulatory expectations for quality, accountability, self-regulation n

Part IV. Evaluation of Performance in Practice n Demo to pts, public, profession n Safe, effective, pt centered, timely, efficient, equitable health care Improve quality of PC n CI of practice performance n Evaluate n n Individual physician performance

Part IV. Evaluation of Performance in Practice - ABMS Principles n n n Phase-in; evaluate effectiveness; improve Reflect activities of diplomate Assessment based on n EBM/guidelines Expert consensus Normative peer comparisons

Part IV. Evaluation of Performance in Practice- ABMS Principles n Compare diplomate to standards • n n n Baseline, plan to improve, measure Assess all 6 competencies during cycle Key disease or clinical processes Collaborative/shared databases Proven educational & assessment methods MOC for inactive and no PC MDs

Part IV. Evaluation of Performance in Practice - ABMS Principles Provide feedback to improve PC, workflow, efficiency n Not be duplicative-P 4 P n Collaborate with specialty societies n Begin assessment during residency n

Part IV Performance in Practice n n Four personal attestations (4 th and 8 th year) Lab accreditation (4 th and 8 th year) except forensic labs Laboratory participation in inter-laboratory PI programs (2 yrs) Individual participation at least 1 laboratory PIQA program/yr. (2 yrs)

Part IV Performance in Practice Society-sponsored programs or created by departments/institutions n On-line application for Part IV programs n Programs must be ABP-approved n

Part IV. Evaluation of Performance in Practice n Attestations as to: n Interpersonal and communication skills n Professionalism n Ethics n Effectiveness in systems-based practice

Part IV. Evaluation of Performance in Practice – Interpersonal & Communication Skills n n 4 th year after certification and at application for exam Attestations from: n ABP-certified pathologist n Credentials Com or equivalent (e. g. CMO) n Board-certified physician in another specialty n Technologist or physician’s assistant (360)

Part IV. Evaluation of Performance in Practice Laboratory Accreditation n Timeline: 8 th-10 th year with exam application n Document accreditation status of laboratory

Part IV. Evaluation of Performance in Practice Laboratory Improvement n Every 2 years after certification n Documentation to ABP of successful participation in inter-laboratory improvement and quality assurance programs relevant to the practice

Part IV. Evaluation of Performance in Practice Individual Improvement & QA Activity Every 2 years after certification n Documents individual participation in at least one QA program/year relevant to professional activities, or n Document use of appropriate protocols, outcome measures, & practice guidelines to improve practice n
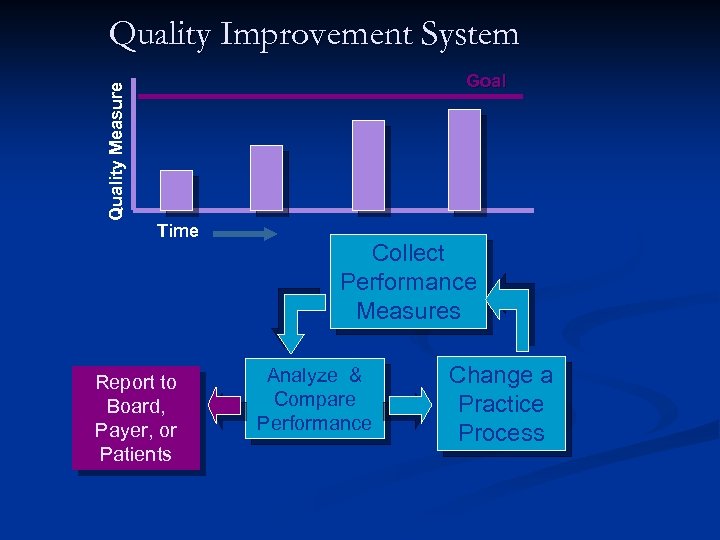
Quality Improvement System Quality Measure Goal Time Report to Board, Payer, or Patients Collect Performance Measures Analyze & Compare Performance Change a Practice Process

Six Core Competencies In Medical Practice n Medical knowledge n Patient care n Interpersonal and communication skills n Professionalism n Practice-based learning and improvement n Systems-based practice

Involvement of Specialty Societies in MOC ABP --standard setting organization n Cooperating Societies: n CME n Self-assessment tools n Programs for evaluation of practice performance n Verification of satisfactory performance n Remedial education programs n Content n

MOC Cost to Diplomates Fee for electronic database n $50/year n CME n Self-assessment modules n Cognitive exam n Currently $2200 n

Requirements For MOC Parts I-IV Part I: Professional Standing Part II: Life-Long Learning and Self-Assessment Part III: Cognitive Expertise Part IV: Evaluation of Performance in Practice


Failure to meet MOC Requirements n Must participate and demonstrate satisfactory performance in all 4 parts of MOC n Performance below expectations requires an implementation plan to improve performance n Failure to satisfy performance criteria results in loss of certification December 31 st of 10 year anniversary of initial certification

Transition to MOC n Holders of life-time certificates: Voluntary recertification n Participate in MOC n Original certificate NOT jeopardized n n Holders of time-limited certificates: n n Must participate in MOC Candidates for initial certification: n Must participate in MOC after certification

Voluntary Recertification and MOC

Voluntary Recertification 1998 ABMS initiative n Assessment of individual credentials n Measure quality of professional practice n Evaluate basic parameters of practice n

Voluntary Recertification Diplomates of ABP with non-time-limited certificate n Recertification certificate dated January 1 of the year following completion of process n Valid for 10 years n Expiration--no effect on original certificate n

Voluntary Recertification Requirements n n n Possess lifetime primary certificate Current valid, full, and unrestricted license to practice medicine or osteopathy in US, its territories, or Canada Provide a written statement attesting physically and mentally ability to practice pathology

Voluntary Recertification Requirements n 150 CME credits during the 3 years prior to application n 100/150 hours must be Category 1 n 80/100 Category 1 hours must be directly related to practice n Verify that primary laboratory or work environment is accredited

Voluntary Recertification Requirements Written statement documenting medical staff standing n References from the head of the department or section chief and from chief of the medical staff n Demonstrate membership in appropriate professional organizations n

Recertification Examination n Optional secure examination n Computer based, ABP test center n May be mandatory if candidate does not fully meet the other requirements

Voluntary Recertification vs MOC n Requirements differ in degree n CME n VR – 150 hours in 3 years prior to application; 100 Category 1 n MOC - 25 hours/yr, all Category 1 AND 1 SAM /yr for 10 years n 80% of CME related to practice

Voluntary Recertification vs MOC n Practice evaluation VR – licensure, references, laboratory accreditation, medical staff standing, quality of practice assessed by references n MOC – licensure, references, laboratory accreditation, inter-laboratory improvement and QA programs, individual improvement and QA programs n

Voluntary Recertification vs MOC n Examination VR – voluntary, (now) secure, combined AP and CP questions n MOC – mandatory, secure, closed-book exam, modular n

Voluntary Recertification vs MOC n Consequences VR – failure to meet requirements or decision not to recertify subsequently has no effect on original certification status n MOC – failure to meet requirements results in loss of certification n

MOC-Special Circumstance Physicians n Not in active practice n Must complete MOC Parts I, III n Will not need to complete Part IV

MOC Unanswered Questions n MOL n Hospital Credentialling n Health Plan Credentialling

AMERICAN BOARD OF PATHOLOGY <www. abpath. org>
c2b03a336b4d2f15a1571f8279398a23.ppt