93e79900508390ce9160f5e6a2c154b0.ppt
- Количество слайдов: 69

RE-DISCOVERING PATIENTS: Evidence-based Improvement Dr Pat Straw, Head of Patient & Public Partnership NHS Lothian University Hospitals Division, Edinburgh E-mail pat. straw@luht. scot. nhs. uk Copenhagen 2007

Re-discovering patients? • Engage with patients in different and better ways • Systematic and robust methods to obtain information on clinical care to complement clinical conversations • Place these daily exchanges in a broader and more powerful context Copenhagen 2007

Presentation 1. Introduction 2. Background – rigorous surveys 3. Summary of results 4. Dissemination and publicity 5. Patient Information 6. Pain Management 7. Questions Copenhagen 2007

Introduction Copenhagen 2007

Edinburgh, Scotland Copenhagen 2007

Edinburgh, Scotland Copenhagen 2007

NHS Lothian – University Hospitals Division 9 hospitals on 8 sites, including the Royal Infirmary of Edinburgh, the Western General Hospital, St John’s, and the Royal Hospital for Sick Children. One of the largest teaching organisations in the UK, employing around 16, 000 staff, and with almost a million patient episodes per year. Copenhagen 2007

Royal Infirmary Copenhagen 2007

Background Copenhagen 2007

Patients, clients and parents are experts Copenhagen 2007

A great deal of expert knowledge Copenhagen 2007

Feedback overview Poor surveys - methodologically flawed, untrained staff, badly resourced, few (if any) improvements Over reliance on unrepresentative information: Complaints = 0. 1% Patient groups – anecdote and participants self-selected Copenhagen 2007

External Partners Patient Perspective, Oxford * recognised leaders in the field * independent * rapid turnaround time * better value for money than in-house Copenhagen 2007

Survey and Change Management Programme - Essentials • Using aggregated data from large representative samples of patients/clients/parents to make a difference to individual patients/parents in a ward or in a clinic • Providing information to clinicians and managers about patient priorities that is immediately useful (so although methodologically rigorous, programme is not mainly an academic exercise) Copenhagen 2007

Methodology 1 - Components of the Study All adult in-patients (9 broad groups) Coronary Heart Disease (national priority area) Medicine of the Elderly Paediatric Services Maternity Services Copenhagen 2007

Methodology 2 - Development of Questionnaires Focus groups in local library Independent, professional moderator Tape-recorded, transcribed, report Draft questionnaire Cognitive interviews to test questionnaire Final questionnaire Pilot postal survey - analysis & report Copenhagen 2007

Patients tell us what’s important to them. . . 8 Dimensions of Care – Respect for values, preferences and expressed needs – Access to care – Co-ordination of care – Information, communication and education – Pain management – Emotional support – Involvement of family and friends – Transition and continuity Copenhagen 2007
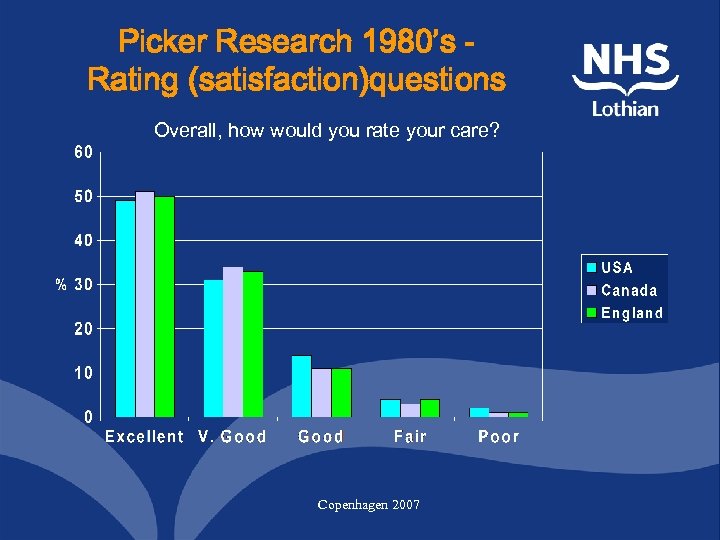
Picker Research 1980’s Rating (satisfaction)questions Overall, how would you rate your care? Copenhagen 2007

Reports not Rating Facts not Satisfaction Questions that: • elicit reports about specific care experiences that reflect quality of care, not amenities • are less subjective and less influenced by patient characteristics and expectations (eliminate bias) • are more interpretable and point to specific areas for improvement Copenhagen 2007

NO to Patient/Client/Parent Satisfaction! Asking patients/clients/parents to report on what happened NOT Asking patients/clients/parents to rate their satisfaction Copenhagen 2007

Methodology 3 - The Surveys Mailing of questionnaires, 3 weeks after stay/visit, to randomly samples Mailing of 2 reminders to non-responders Freepost envelope for patients to return questionnaires Freephone telephone for queries Response rate of around 70% = margin of error 3% Copenhagen 2007

Methodology 3 - The Survey New method 2006/07! Copenhagen 2007

Summary Results Copenhagen 2007

OP Programme Essentials • Majority of patients do not stay overnight; outpatients outnumber inpatients by a ratio of 5: 1. • Contact time between patients and staff in OP setting more limited and circumscribed than IP context so quality of experience highly significant. Copenhagen 2007

How would you rate the care you received? Adult outpatients: What percentage of our patients were ‘very satisfied’? Copenhagen 2007

86% of our patients were ‘very satisfied’ Copenhagen 2007

Did you feel involved enough in decisions about your care? What percentage of the SAME patients did not feel involved in decisions about their care? Copenhagen 2007

Reporting Questions Orthopaedics, ENT, Dermatology 44% (Ortho. ), 37% (ENT), 41% (Derm. ) wanted to be more involved in decisions about their care Didn’t always see same doctor Didn’t know names of staff Not told what would happen at appointment Not told who appointment was with Not enough chance to discuss problem with dr. How surgery/treatment went not explained well Risks & benefits of operation not discussed Not told what to do if symptoms got worse Copenhagen 2007 70 64 46 51 39 36 35 35 % 63 60 65 55 30 32 28 34 49 60 54 32 33 29 29 34

Reporting Questions % No understandable explanation of test results 29 37 Reason for appointment not dealt with 26 31 Dr. didn’t know enough about medical history 24 23 22 Not told side effects of medication 23 22 Staff contradicted each other 22 11 Didn’t get answers to questions from doctors 18 11 Spent < 5 minutes with doctor 36 3 No written information 18 16 Clinic not well organised 42 27 Copenhagen 2007 46 27 19 13 17 19 18 26

Improving the Patient’s Journey: Outpatient Clinics • Patient Information • Staff communication within/between departments • Appointments • Numbers of patients • Junior doctors’ roles • Role of nurse practitioners • Culture Copenhagen 2007

How would you rate the care you received? Adult inpatients: What percentage of our patients were ‘very satisfied’? Copenhagen 2007

90%, 89% , 92% of our patients were ‘very satisfied’ Copenhagen 2007

Did you feel involved enough in decisions about your care? What percentage of the SAME patients did not feel involved in decisions about their care? Copenhagen 2007
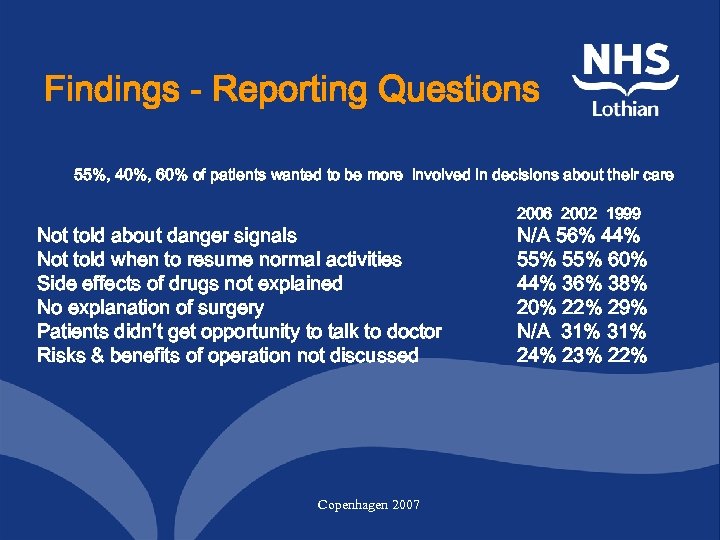
Findings - Reporting Questions 55%, 40%, 60% of patients wanted to be more involved in decisions about their care Not told about danger signals Not told when to resume normal activities Side effects of drugs not explained No explanation of surgery Patients didn’t get opportunity to talk to doctor Risks & benefits of operation not discussed Copenhagen 2007 2006 2002 1999 N/A 56% 44% 55% 60% 44% 36% 38% 20% 22% 29% N/A 31% 24% 23% 22%

Strategic & Local Action Plans Pain Management Patient involvement in decision-making Who’s in charge of care? Discharge Planning Informed consent and info. about surgery No. of nurses on the ward/in clinic Clinical Improvement Teams (directorates) Copenhagen 2007

Dissemination & publicity Copenhagen 2007
Copenhagen 2007
Copenhagen 2007
Copenhagen 2007
Copenhagen 2007

Copenhagen 2007

Copenhagen 2007

Copenhagen 2007

Managed Patient Information Copenhagen 2007

Information is Power Individual Patients making informed decisions and choices about their treatment and care Members of the public exerting informed influence on service planning and delivery. Copenhagen 2007

Copenhagen 2007

Genesis of Project § Patient feedback … Copenhagen 2007
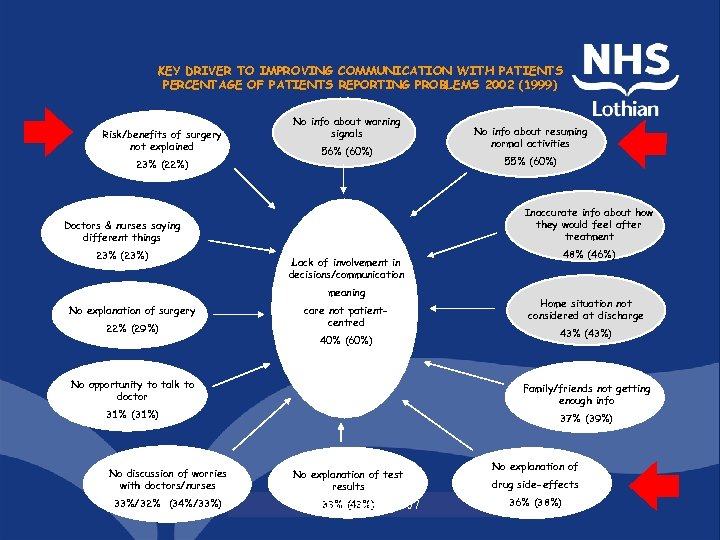
KEY DRIVER TO IMPROVING COMMUNICATION WITH PATIENTS PERCENTAGE OF PATIENTS REPORTING PROBLEMS 2002 (1999) Risk/benefits of surgery not explained 23% (22%) No info about warning signals 56% (60%) 22% (29%) 48% (46%) Lack of involvement in decisions/communication meaning No explanation of surgery 55% (60%) Inaccurate info about how they would feel after treatment Doctors & nurses saying different things 23% (23%) No info about resuming normal activities care not patientcentred 40% (60%) Home situation not considered at discharge 43% (43%) No opportunity to talk to doctor Family/friends not getting enough info 31% (31%) 37% (39%) No discussion of worries with doctors/nurses 33%/32% (34%/33%) No explanation of test results 33% (43%) Copenhagen 2007 No explanation of drug side-effects 36% (38%)

Genesis of Project §To make it easy for staff to ‘get it right’ - give the right sort of information, the right amount of information, at the right time, in the right place, in the right format Copenhagen 2007

Web-based System (but much more than a web-site) § Modules (text and graphics) of health information to make leaflets, folders or booklets, as well as everything related to system administration § Information for hospital staff and GPs to view or print, and share with patients, relatives and carers + direct access for people via home, school or library PCs, kiosks and bedside terminals. § Audit trails of creation, approval, updating and reapproval; what’s been updated and when (and what hasn’t); archive and date the content modules and leaflets at each update Copenhagen 2007
Copenhagen 2007
Copenhagen 2007
Copenhagen 2007

Equality and Diversity (psychosocial-prescribing) § It enables staff to be educationally, socially, spiritually and culturally competent via: §Minimising Barriers Checklists (instant access to barriers service users themselves have identified) §Service Contact Lists (25 data bases, e. g. homelessness, learning disabilities, alcohol/drugs) §Helplines Contact List (phone based services, local and national) §Signposting Briefing Sheets (e. g. smoking, careers, benefits, adult learning, exercise) Copenhagen 2007

Pain Management Copenhagen 2007
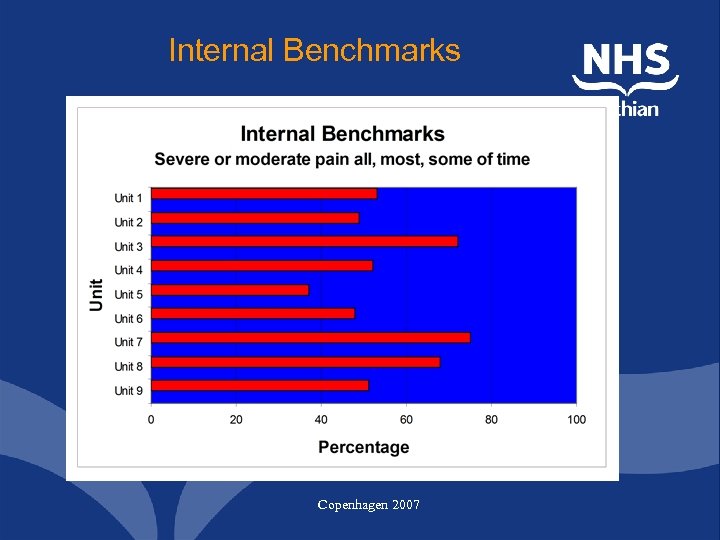
Internal Benchmarks Copenhagen 2007
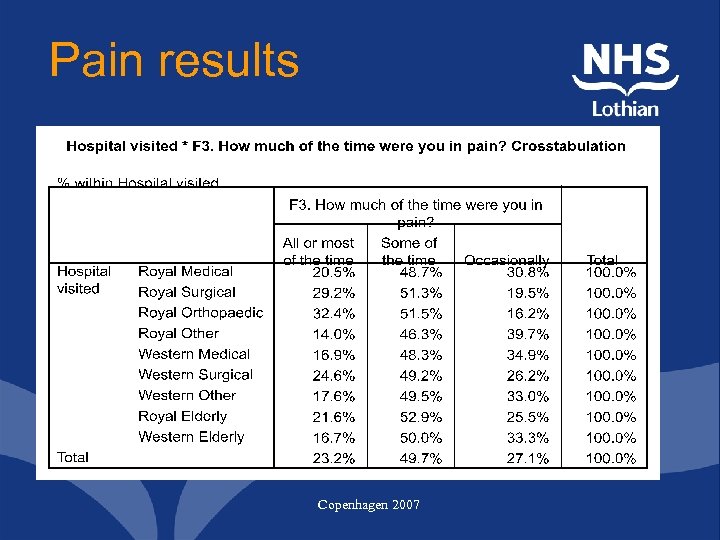
Pain results Copenhagen 2007

Who experiences more severe pain ? • • • Younger people Emergency admissions Patient’s feeling less involved in their care Patients having tests Patients who reported the doctors and nurses working poorly together NOT • Patients having surgery • Patients able to give themselves pain medicine Copenhagen 2007

Who experienced pain all or most of the time? • Younger people • Patient’s feeling less involved in their care • Patients not able to give themselves pain medicine NOT • Patients having surgery • Patients having tests • Emergency admissions • Patients who reported the doctors and nurses working poorly together Copenhagen 2007

Pain Management - Issues • Research and science sophisticated v. routine practice primitive • Pain fundamental - vital sign - surely should be monitored like blood pressure, heart rate, etc. • Related to morbidity and mortality • Training • Equipment Copenhagen 2007

Major Gynae. Surgery – Improvements in 9 months • LOS reduced from 7 to 4 days = Shorter waiting times • Severe pain on movement 68% down to 12% • 81. 3 % use of prophylactic antiemetics now • 100% prescription of oral analgesia Copenhagen 2007

Major Gynaecological Surgery Where did system breakdown? • In theatre - under-dosing • In recovery - no staff trained to give intravenous drugs • In ward - PCA discontinued too soon • Oral analgesia not prescribed • Antiemetics not prescribed • PCA Bolus too small • Prescribed oral analgesia not given • Prophylactic antiemetics not used • Prescribed antiemetics not given Copenhagen 2007

What did we do? • Fedback results • Training in intravenous drug administration • Production of guidelines • Introduction & training in use of guideline • Pre-printed drug charts Copenhagen 2007

Standards set • No severe pain • 100% use of prophylactic antiemetics • 100% prescription of oral analgesia & rescue antiemetics • Better morphine - loading, bolusing, duration of use • Crossover from morphine to oral analgesia Copenhagen 2007
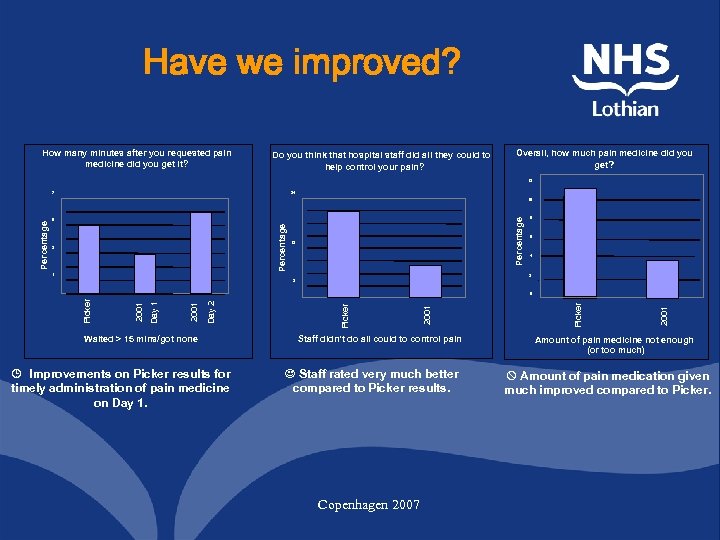
Have we improved? How many minutes after you requested pain medicine did you get it? Do you think that hospital staff did all they could to help control your pain? Overall, how much pain medicine did you get? 12 7 24 Percentage 5 Percentage 10 3 12 1 8 6 4 2 3 Waited > 15 mins/got none ¹ Improvements on Picker results for timely administration of pain medicine on Day 1. Staff didn't do all could to control pain J Staff rated very much better compared to Picker results. Copenhagen 2007 2001 Picker Day 2 2001 Day 1 2001 Picker 0 Amount of pain medicine not enough (or too much) W Amount of pain medication given much improved compared to Picker.

What more can we do? • Increase use of oral opioids? Oxycodone? • Increase use of regional techniques - epidurals • Other co-treatments? Drugs used in chronic pain? Amitryptiline? • Ensure 100% antiemetic prophylaxis - increase PCA bolus to 2 mgs morphine, increase guideline compliance • At least maintain improvements Copenhagen 2007

Pain Management - Issues • Staff expertise - many doctors and nurses have had little training on pain management (sometimes the pharmacists are the only experts) • Co-ordination - who is in charge of pain management; at admission, on the ward(s), before surgery, during surgery, after surgery, back on the ward(s), at discharge • The surgical patients see the acute pain team and have their pain well controlled post-operatively - what about after “postoperative” and what about non-surgical patients? • Patients are often under dosed or dosed at the lower end of a suggested range • Concerns over addiction still exist Copenhagen 2007

Improving the Patient’s Journey: Pain Management • Division strategy - standards, time scales, responsibilities • Expert team at strategic level • Best practice • Education • Equipment • Improved patient care & savings Copenhagen 2007

Any Questions? Copenhagen 2007
93e79900508390ce9160f5e6a2c154b0.ppt