88ef06a3cbf69006681bc8730e341f79.ppt
- Количество слайдов: 37
 Quality Colloquium August 22, 2005 REDUCTION OF ADVERSE DRUG EVENTS Kathy Haig Director Quality Resource Management Risk Manager/Patient Safety Officer
Quality Colloquium August 22, 2005 REDUCTION OF ADVERSE DRUG EVENTS Kathy Haig Director Quality Resource Management Risk Manager/Patient Safety Officer
 OBJECTIVES Introduce process changes that contribute to reduction of adverse drug events Discuss the impact of culture on medication event reduction efforts Review tools used in process improvement collaborative Learn about Medication Reconciliation
OBJECTIVES Introduce process changes that contribute to reduction of adverse drug events Discuss the impact of culture on medication event reduction efforts Review tools used in process improvement collaborative Learn about Medication Reconciliation
 OSF ST. JOSEPH MEDICAL CENTER Located in Bloomington, Illinois Serves a community of 100, 500 people Licensed for 157 beds Provides Open Heart Surgery Services Started “Beating Heart” Program in 1999 5 Hospital-Owned Physician Office Practices Urgent Care Center Licensed as a Level II Trauma Center
OSF ST. JOSEPH MEDICAL CENTER Located in Bloomington, Illinois Serves a community of 100, 500 people Licensed for 157 beds Provides Open Heart Surgery Services Started “Beating Heart” Program in 1999 5 Hospital-Owned Physician Office Practices Urgent Care Center Licensed as a Level II Trauma Center
 GOALS Maintain a cultural survey score above 4 Involve patients with safety Conduct 3 phases of med reconciliation Decrease the Dispensing and Ordering FMEA Promote Dosing Service for Anticoagulants Deploy Pharmacy Based Order Sets Comply with JCAHO Patient Safety Goals Safety tool kit (RCA, FMEA, Human Factors, CAS, TRM)
GOALS Maintain a cultural survey score above 4 Involve patients with safety Conduct 3 phases of med reconciliation Decrease the Dispensing and Ordering FMEA Promote Dosing Service for Anticoagulants Deploy Pharmacy Based Order Sets Comply with JCAHO Patient Safety Goals Safety tool kit (RCA, FMEA, Human Factors, CAS, TRM)
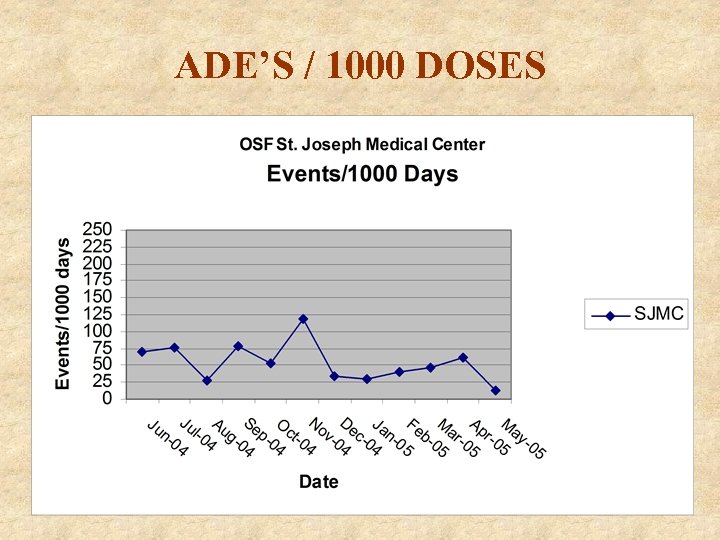 ADE’S / 1000 DOSES
ADE’S / 1000 DOSES
 Idealized Design of the Medication System Key Areas of Focus ØCulture ØReconciliation ØDispensing ØOrdering ØHigh Risk Medications
Idealized Design of the Medication System Key Areas of Focus ØCulture ØReconciliation ØDispensing ØOrdering ØHigh Risk Medications
 Cultural Transformation Improve Safety Climate or culture ØCultural survey or safety climate score Focus on harm, not errors ØMeaningful, avoids blame game Focus on process and system ØPoor processes; not “bad people” Focus on communication and teamwork
Cultural Transformation Improve Safety Climate or culture ØCultural survey or safety climate score Focus on harm, not errors ØMeaningful, avoids blame game Focus on process and system ØPoor processes; not “bad people” Focus on communication and teamwork
 High Reliability t en i at P In vo lve Medication System me nt Safer Core Processes • R CA Co llab • FM ora EA tion • Simulation . System thinkin g rs acto nf • CRM • CAS uma • H nge used on Cha Foc e c den i Ev Leadership Driven Culture of Safety
High Reliability t en i at P In vo lve Medication System me nt Safer Core Processes • R CA Co llab • FM ora EA tion • Simulation . System thinkin g rs acto nf • CRM • CAS uma • H nge used on Cha Foc e c den i Ev Leadership Driven Culture of Safety
 High Reliability Characteristics Preoccupation with failure ØIs 80% good enough? Deference to expertise ØMost knowledgeable takes charge regardless of role Ask yourself: ØWhat have I missed today? ØWhat should I have seen that I didn’t?
High Reliability Characteristics Preoccupation with failure ØIs 80% good enough? Deference to expertise ØMost knowledgeable takes charge regardless of role Ask yourself: ØWhat have I missed today? ØWhat should I have seen that I didn’t?
 STARTING THE JOURNEY CULTURE ØSystem Thinking § Influenced by patient condition, tasks, staff, environment, teamwork, management ØCollaboration § Friendly competition; accomplish more, faster ØCommitment to Change § New, better ways; test ideas ØEvidence Based § Order Sets; Protocols
STARTING THE JOURNEY CULTURE ØSystem Thinking § Influenced by patient condition, tasks, staff, environment, teamwork, management ØCollaboration § Friendly competition; accomplish more, faster ØCommitment to Change § New, better ways; test ideas ØEvidence Based § Order Sets; Protocols
 CULTURE STAFF INVOLVEMENT Non-Punitive Reporting Policy Systems Thinking ØFocus on harm and processes; not the care provider Safety Briefings with Employee Feedback Unit Councils ØStaff identify and address unit safety concerns ØInvolves staff in development of processes
CULTURE STAFF INVOLVEMENT Non-Punitive Reporting Policy Systems Thinking ØFocus on harm and processes; not the care provider Safety Briefings with Employee Feedback Unit Councils ØStaff identify and address unit safety concerns ØInvolves staff in development of processes
 CULTURE PHYSICIAN ENGAGEMENT Patient Safety is a standing agenda item Safety Briefings and Feedback is provided Monthly updates of PI projects are provided Root Causes Analyses include physician input Human Factors included in the Peer Review Expectations and goals of the organization are shared Efforts made to obtain input while being mindful of the physician’s time
CULTURE PHYSICIAN ENGAGEMENT Patient Safety is a standing agenda item Safety Briefings and Feedback is provided Monthly updates of PI projects are provided Root Causes Analyses include physician input Human Factors included in the Peer Review Expectations and goals of the organization are shared Efforts made to obtain input while being mindful of the physician’s time
 PHYSICIAN INPUT Ad Hoc team developed process and protocol for Peri-operative Beta Blockade Anesthesiologists developed Epidural Protocol Pediatricians requested child Med Safety Brochure for their offices Internists and CV Surgeons assisted in development of IV Insulin Infusion Protocol
PHYSICIAN INPUT Ad Hoc team developed process and protocol for Peri-operative Beta Blockade Anesthesiologists developed Epidural Protocol Pediatricians requested child Med Safety Brochure for their offices Internists and CV Surgeons assisted in development of IV Insulin Infusion Protocol
 CULTURE PATIENT INVOLVEMENT Satisfaction survey questions for safety Medication Safety Brochure given to all new admissions; distributed by physician offices Community resource collaboration to encourage patient to keep updated med list Patient education channel is available 24/7 with information about disease Community Board serves a dual role as the Patient Advisory Council
CULTURE PATIENT INVOLVEMENT Satisfaction survey questions for safety Medication Safety Brochure given to all new admissions; distributed by physician offices Community resource collaboration to encourage patient to keep updated med list Patient education channel is available 24/7 with information about disease Community Board serves a dual role as the Patient Advisory Council
 PATIENT SAFETY POSTER ALSO AVAILABLE IN SPANISH Be Involved in Your Care Make sure the nurse checks your armband before giving your medicine. Ask the nurse about medication that is unfamiliar to you BEFORE you take it. Make sure the staff and physician washes their hands before / after providing care to you
PATIENT SAFETY POSTER ALSO AVAILABLE IN SPANISH Be Involved in Your Care Make sure the nurse checks your armband before giving your medicine. Ask the nurse about medication that is unfamiliar to you BEFORE you take it. Make sure the staff and physician washes their hands before / after providing care to you
 MEDICATION RECONCILIATION Definition A process of identifying the most accurate list of all medications a patient is taking and using this list to provide care in any setting It requires comparing the patient’s list of current medications against the physician’s admission, transfer and discharge orders.
MEDICATION RECONCILIATION Definition A process of identifying the most accurate list of all medications a patient is taking and using this list to provide care in any setting It requires comparing the patient’s list of current medications against the physician’s admission, transfer and discharge orders.
 WHY DO THIS? Provides the ability to accurately compare home meds to meds ordered during hospitalization Detects medication errors before they happen Promotes continuity of care between different levels of care Wrong dose, route or frequency may be prescribed Important meds may be omitted
WHY DO THIS? Provides the ability to accurately compare home meds to meds ordered during hospitalization Detects medication errors before they happen Promotes continuity of care between different levels of care Wrong dose, route or frequency may be prescribed Important meds may be omitted
 RECONCILIATION PROCESS Med history is completed Med history is compared with admission medication orders Transfer reconciliation is conducted when the patient moves to a different level of care Discharge reconciliation compares the meds ordered during hospitalization with those ordered to be taken at home Variances between med history and admission orders is clarified with the physician What is included? Ø Current home meds, OTC, Herbals Ø Includes dose, route, frequency, time of last dose
RECONCILIATION PROCESS Med history is completed Med history is compared with admission medication orders Transfer reconciliation is conducted when the patient moves to a different level of care Discharge reconciliation compares the meds ordered during hospitalization with those ordered to be taken at home Variances between med history and admission orders is clarified with the physician What is included? Ø Current home meds, OTC, Herbals Ø Includes dose, route, frequency, time of last dose
 WHERE TO GET INFORMATION Patient or family Patient’s pharmacy Previous medical records Primary care physician’s office Patient’s medication bottles
WHERE TO GET INFORMATION Patient or family Patient’s pharmacy Previous medical records Primary care physician’s office Patient’s medication bottles
 BARRIERS Bureaucracy Complexity of communication--interruptions Accountability—staff too busy Lack of teamwork—office does not have updated list or nursing home list is confusing Patient brings in incorrect list Patient does not take what is marked on the bottle Patient does not know names of meds Patient is unable to tell you
BARRIERS Bureaucracy Complexity of communication--interruptions Accountability—staff too busy Lack of teamwork—office does not have updated list or nursing home list is confusing Patient brings in incorrect list Patient does not take what is marked on the bottle Patient does not know names of meds Patient is unable to tell you
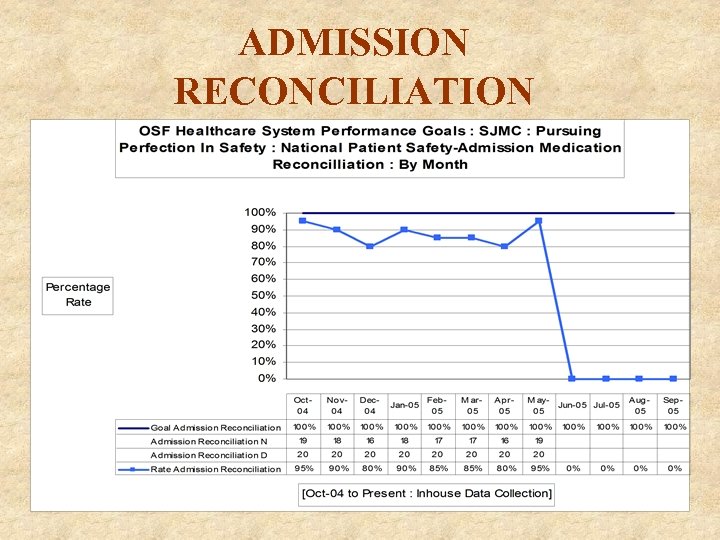 ADMISSION RECONCILIATION
ADMISSION RECONCILIATION
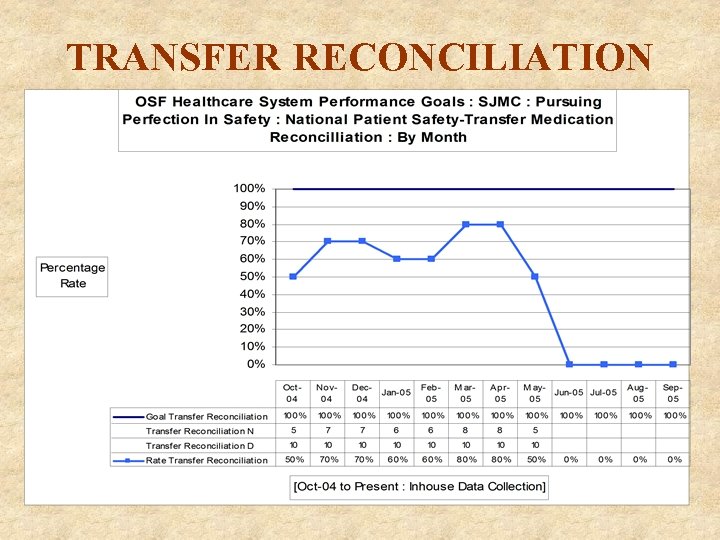 TRANSFER RECONCILIATION
TRANSFER RECONCILIATION
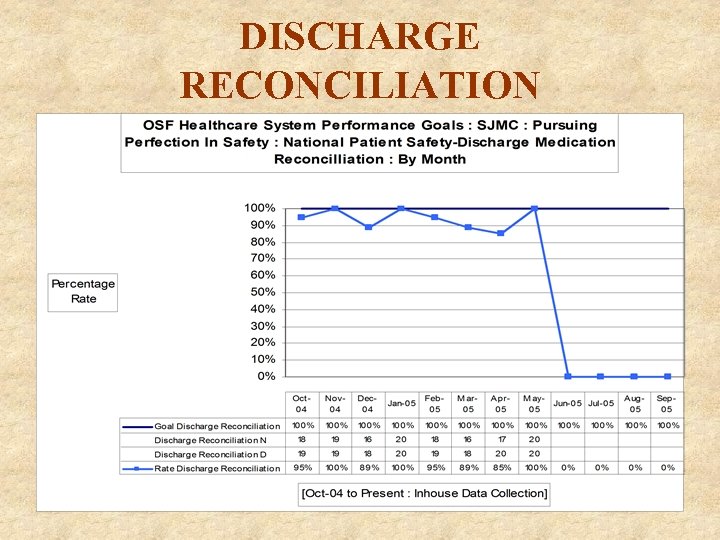 DISCHARGE RECONCILIATION
DISCHARGE RECONCILIATION
 FMEA—DISPENSING The Dispensing FMEA has been reduced 66% Pharmacy reduced/standardized unit stock meds Pharmacy prepares all non-standard doses Labels on all IV pumps encourage caution when stopping the pump to make rate or dose changes IV Drug Administration Reference matrix directs dosages, guidelines, monitoring information An automated dispensing system was installed Renovation of nursing and pharmacy workspaces to improve process flow and efficiency
FMEA—DISPENSING The Dispensing FMEA has been reduced 66% Pharmacy reduced/standardized unit stock meds Pharmacy prepares all non-standard doses Labels on all IV pumps encourage caution when stopping the pump to make rate or dose changes IV Drug Administration Reference matrix directs dosages, guidelines, monitoring information An automated dispensing system was installed Renovation of nursing and pharmacy workspaces to improve process flow and efficiency
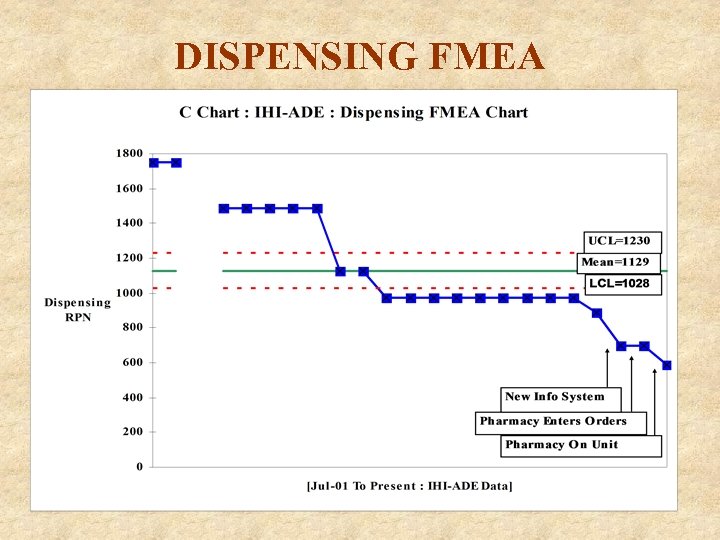 DISPENSING FMEA
DISPENSING FMEA
 FMEA-ORDERING Hazard Vulnerability Score has been reduced 34% A Periop-Beta Blocker Protocol was initiated 1/03 Surgical Prophylaxis Antibiotic Protocol developed Pharmacists assigned to a nursing unit/enter orders Renal dosing review based on creatinine clearance Abbreviations ØUnapproved abbreviations are on orders sheets Illegibility ØPharmacists call with any question of the order Read-Backs ØNurses read back 95% of all telephone orders and sign with “TORB”
FMEA-ORDERING Hazard Vulnerability Score has been reduced 34% A Periop-Beta Blocker Protocol was initiated 1/03 Surgical Prophylaxis Antibiotic Protocol developed Pharmacists assigned to a nursing unit/enter orders Renal dosing review based on creatinine clearance Abbreviations ØUnapproved abbreviations are on orders sheets Illegibility ØPharmacists call with any question of the order Read-Backs ØNurses read back 95% of all telephone orders and sign with “TORB”
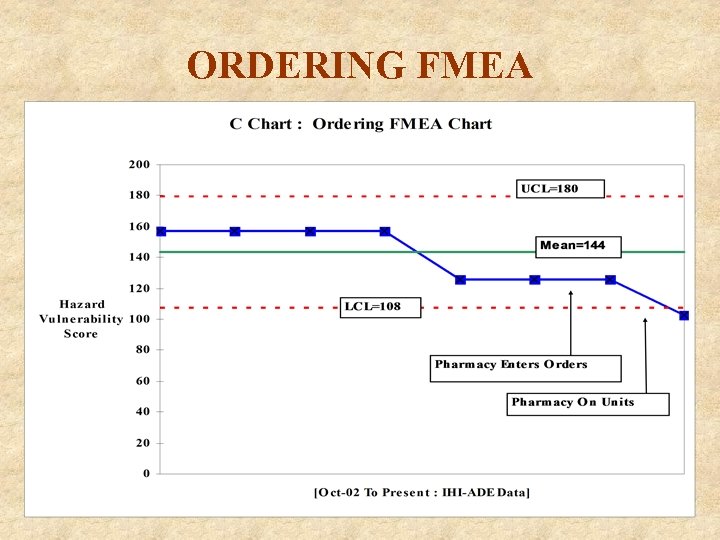 ORDERING FMEA
ORDERING FMEA
 HIGH RISK MEDICATIONS Heparin Nomogram PCA Protocol with default orders TPN Protocol IV Insulin Infusion Protocol Chemotherapy Order Set Coumadin dosing service DVT Protocol Review of all INR’s above 4 to identify opportunities in dosing regimens
HIGH RISK MEDICATIONS Heparin Nomogram PCA Protocol with default orders TPN Protocol IV Insulin Infusion Protocol Chemotherapy Order Set Coumadin dosing service DVT Protocol Review of all INR’s above 4 to identify opportunities in dosing regimens
 SIMULATION “Sim Man” purchased Simulation lab created Simulation used for Clinical Orientation for RN/LPN/US/CNA Simulation used for annual skills validation Simulation used for Root Cause Analysis
SIMULATION “Sim Man” purchased Simulation lab created Simulation used for Clinical Orientation for RN/LPN/US/CNA Simulation used for annual skills validation Simulation used for Root Cause Analysis
 ROOT CAUSE ANALYSIS Human Factor Triage Questions incorporated into RCA—approved and applauded by JCAHO One RCA resulted in improvements that prevented care issues in a subsequent trauma (ED/difficult intubation boxes) Success of RCA’s spreading—being used independently by other areas such as OR and EMS Services to evaluate a “near miss”
ROOT CAUSE ANALYSIS Human Factor Triage Questions incorporated into RCA—approved and applauded by JCAHO One RCA resulted in improvements that prevented care issues in a subsequent trauma (ED/difficult intubation boxes) Success of RCA’s spreading—being used independently by other areas such as OR and EMS Services to evaluate a “near miss”
 SBAR Acronym-Situation, Background, Assessment and Recommendation Laminated pocket cards including the acronym have been distributed to all nurses Posters explaining SBAR have been posted in clinical areas and stickers have been placed on phones Use of SBAR spreading to all areas for any issue Medical Staff are encouraged to ask staff to use SBAR
SBAR Acronym-Situation, Background, Assessment and Recommendation Laminated pocket cards including the acronym have been distributed to all nurses Posters explaining SBAR have been posted in clinical areas and stickers have been placed on phones Use of SBAR spreading to all areas for any issue Medical Staff are encouraged to ask staff to use SBAR
 SBAR POCKET CARD In the interest of Patient Safety and to ensure we are giving complete, accurate information to the physician, please use the following acronym to direct the information we provide: S (the current Situation or problem) B (a little about the patient’s Background) A (your Assessment of the patient) R (your Recommendation of what is needed from the physician)
SBAR POCKET CARD In the interest of Patient Safety and to ensure we are giving complete, accurate information to the physician, please use the following acronym to direct the information we provide: S (the current Situation or problem) B (a little about the patient’s Background) A (your Assessment of the patient) R (your Recommendation of what is needed from the physician)
 TEAM RESOURCE MANAGEMENT Improves team efficiency and effectiveness Includes multiple concepts ØCommunication tools—SBAR ØStaff assertion ØSituational Awareness ØBriefings ØDebriefings ØRed Flags Initial and refresher training was provided to staff and physicians
TEAM RESOURCE MANAGEMENT Improves team efficiency and effectiveness Includes multiple concepts ØCommunication tools—SBAR ØStaff assertion ØSituational Awareness ØBriefings ØDebriefings ØRed Flags Initial and refresher training was provided to staff and physicians
 BARRIERS Limited Resources Lack of organization/leadership support Lack of physician buy-in Resistance to change Starting too big Moving too quick Reluctance to share safety concerns Multiple projects Added work instead of replacement
BARRIERS Limited Resources Lack of organization/leadership support Lack of physician buy-in Resistance to change Starting too big Moving too quick Reluctance to share safety concerns Multiple projects Added work instead of replacement
 LESSONS LEARNED Involve the right people Use rapid cycle tests of change Simplify processes Share successes Don’t recreate the wheel—network with others Communicate
LESSONS LEARNED Involve the right people Use rapid cycle tests of change Simplify processes Share successes Don’t recreate the wheel—network with others Communicate
 KEYS TO SUCCESS Leadership Support Make it a win-win situation Reward and recognize staff Provide ongoing feedback Always make patient safety the priority! Never give up; there is no obstacle that cannot be overcome!!!
KEYS TO SUCCESS Leadership Support Make it a win-win situation Reward and recognize staff Provide ongoing feedback Always make patient safety the priority! Never give up; there is no obstacle that cannot be overcome!!!
 “Safety is like peeling an onion--the more you look, the more you find and each layer makes you cry”.
“Safety is like peeling an onion--the more you look, the more you find and each layer makes you cry”.


