b822d3715594d22d3ac52b02b7eadcfd.ppt
- Количество слайдов: 65
 QUALITY AND EFFICIENCY IN HEALTHCARE: SOME EXPERIENCES IN THE U. S. Kenneth W. Kizer, M. D. , M. P. H. President and CEO National Quality Forum March 2, 2004 1
QUALITY AND EFFICIENCY IN HEALTHCARE: SOME EXPERIENCES IN THE U. S. Kenneth W. Kizer, M. D. , M. P. H. President and CEO National Quality Forum March 2, 2004 1
 Presentation Overview Ø Transformation of the VA Health Care System Ø System overview Ø Problems with VA health care in 1994 Ø VA’s reengineering strategy and implementation logistics Ø Results Ø Some Ø at 5 -7 years lessons learned The National Quality Forum 2
Presentation Overview Ø Transformation of the VA Health Care System Ø System overview Ø Problems with VA health care in 1994 Ø VA’s reengineering strategy and implementation logistics Ø Results Ø Some Ø at 5 -7 years lessons learned The National Quality Forum 2
 The VA Health Care System 3
The VA Health Care System 3
 VA Health Care-Core Missions Ø Medical care Ø Health professional training Ø Research Ø Emergency management Ø Homelessness 4
VA Health Care-Core Missions Ø Medical care Ø Health professional training Ø Research Ø Emergency management Ø Homelessness 4
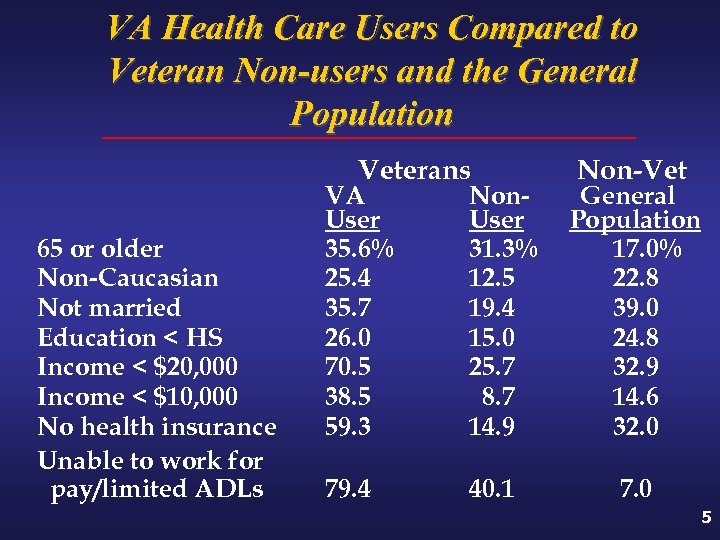 VA Health Care Users Compared to Veteran Non-users and the General Population Veterans 65 or older Non-Caucasian Not married Education < HS Income < $20, 000 Income < $10, 000 No health insurance Unable to work for pay/limited ADLs VA User 35. 6% 25. 4 35. 7 26. 0 70. 5 38. 5 59. 3 Non. User 31. 3% 12. 5 19. 4 15. 0 25. 7 8. 7 14. 9 79. 4 40. 1 Non-Vet General Population 17. 0% 22. 8 39. 0 24. 8 32. 9 14. 6 32. 0 7. 0 5
VA Health Care Users Compared to Veteran Non-users and the General Population Veterans 65 or older Non-Caucasian Not married Education < HS Income < $20, 000 Income < $10, 000 No health insurance Unable to work for pay/limited ADLs VA User 35. 6% 25. 4 35. 7 26. 0 70. 5 38. 5 59. 3 Non. User 31. 3% 12. 5 19. 4 15. 0 25. 7 8. 7 14. 9 79. 4 40. 1 Non-Vet General Population 17. 0% 22. 8 39. 0 24. 8 32. 9 14. 6 32. 0 7. 0 5
 VA Health Care – Assets (1999) 172 hospitals Ø >600 ambulatory care and communitybased outpatient clinics Ø 131 nursing homes Ø 40 residential care facilities Ø 73 primary care at home programs Ø 206 counseling centers Ø 6
VA Health Care – Assets (1999) 172 hospitals Ø >600 ambulatory care and communitybased outpatient clinics Ø 131 nursing homes Ø 40 residential care facilities Ø 73 primary care at home programs Ø 206 counseling centers Ø 6
 VA Health Care – Assets (1999) Many telemedicine programs Ø Contract and fee-basis care Ø 94 state veterans homes Ø >1, 200 sharing agreements (DOD, universities, private providers) Ø 75 laundries Ø 29 fire departments Ø VCS, historic buildings, other Ø 7
VA Health Care – Assets (1999) Many telemedicine programs Ø Contract and fee-basis care Ø 94 state veterans homes Ø >1, 200 sharing agreements (DOD, universities, private providers) Ø 75 laundries Ø 29 fire departments Ø VCS, historic buildings, other Ø 7
 VA Health Care – Problems (1994) Ø Hospital-focused, specialist-based, episodic treatment of illness Ø Independent, centers Ø Too competing medical much inter-facility variation Ø Care too difficult to access Ø Staff demoralized 8
VA Health Care – Problems (1994) Ø Hospital-focused, specialist-based, episodic treatment of illness Ø Independent, centers Ø Too competing medical much inter-facility variation Ø Care too difficult to access Ø Staff demoralized 8
 VA Healthcare – Problems (1994) Ø Centralized, hierarchical, top-down micro-management Ø Reams of rigid policies and procedures Ø Capital investment decisions too political Ø Organization too inwardly focused Ø Inadequate funding (? ? ) 9
VA Healthcare – Problems (1994) Ø Centralized, hierarchical, top-down micro-management Ø Reams of rigid policies and procedures Ø Capital investment decisions too political Ø Organization too inwardly focused Ø Inadequate funding (? ? ) 9
 RE-ENGINEERING VA HEALTH CARE 10
RE-ENGINEERING VA HEALTH CARE 10
 VA Transformation… Critical Strategic Goals (Vision) 1. Create a seamless continuum of care 2. Make superior quality consistent and predictable 3. Demonstrate good value 11
VA Transformation… Critical Strategic Goals (Vision) 1. Create a seamless continuum of care 2. Make superior quality consistent and predictable 3. Demonstrate good value 11
 VA Transformation… Key Strategic Objectives Improve and standardize quality management Ø Improve access Ø Standardize services Ø Improve service satisfaction Ø Ø Reduce operating costs Ø Allocate resources fairly and equitably 12
VA Transformation… Key Strategic Objectives Improve and standardize quality management Ø Improve access Ø Standardize services Ø Improve service satisfaction Ø Ø Reduce operating costs Ø Allocate resources fairly and equitably 12
 VA Transformation. . . Essential Enabling Actions Ø Ø Ø Ø Ø Reengineer operational structure Decentralize operational decision making Streamline processes Improve information management Systematize “best practices” Reform eligibility rules Expand contractual authority Diversity funding base Increase partnerships and alliances Change the culture 13
VA Transformation. . . Essential Enabling Actions Ø Ø Ø Ø Ø Reengineer operational structure Decentralize operational decision making Streamline processes Improve information management Systematize “best practices” Reform eligibility rules Expand contractual authority Diversity funding base Increase partnerships and alliances Change the culture 13
 VA Transformation. . . Key Structural & Process Changes 1. New organizational model - VISNs 2. Statutory changes 3. New capitation-based resource allocation system (VERA) 4. Enhanced information management 5. New performance management system 14
VA Transformation. . . Key Structural & Process Changes 1. New organizational model - VISNs 2. Statutory changes 3. New capitation-based resource allocation system (VERA) 4. Enhanced information management 5. New performance management system 14
 VA Transformation. . . Operational Restructuring Veterans Integrated Service Networks (VISNs) 15
VA Transformation. . . Operational Restructuring Veterans Integrated Service Networks (VISNs) 15
 VA Transformation… Integrated Service Network: Definition An organized set of treatment facilities, caregivers and support services having a collective goal of delivering services to a defined population in a coordinated and collaborative manner that maximizes the healthcare value of the services. 16
VA Transformation… Integrated Service Network: Definition An organized set of treatment facilities, caregivers and support services having a collective goal of delivering services to a defined population in a coordinated and collaborative manner that maximizes the healthcare value of the services. 16
 VA Transformation… Integrated Service Network: Typical Assets Ø 7 -10 Hospitals Ø 25 -30 Ambulatory care clinics Ø 5 -7 Nursing homes Ø 1 -2 Residential care facilities Ø 10 -15 Counseling centers 17
VA Transformation… Integrated Service Network: Typical Assets Ø 7 -10 Hospitals Ø 25 -30 Ambulatory care clinics Ø 5 -7 Nursing homes Ø 1 -2 Residential care facilities Ø 10 -15 Counseling centers 17
 22 Veterans Integrated Service Networks 18
22 Veterans Integrated Service Networks 18
 What is Healthcare Value? Ø Ø Ø V = Value C = Cost/price A = Accessibility TQ = Technical quality FS = Functional status SS = Service satisfaction V = A+TQ + FS + SS C 19
What is Healthcare Value? Ø Ø Ø V = Value C = Cost/price A = Accessibility TQ = Technical quality FS = Functional status SS = Service satisfaction V = A+TQ + FS + SS C 19
 VA Transformation. . . Operational Restructuring ØNew operational model üuniversal ücare primary care management üstandardized ütelephone üshift benefits linked care to outpatient care 20
VA Transformation. . . Operational Restructuring ØNew operational model üuniversal ücare primary care management üstandardized ütelephone üshift benefits linked care to outpatient care 20
 VA Transformation. . . Key Structural & Process Changes Ø Statutory changes ü eligibility reform ü contractual authority ü enrollment 21
VA Transformation. . . Key Structural & Process Changes Ø Statutory changes ü eligibility reform ü contractual authority ü enrollment 21
 VA Transformation. . . Key Structural & Process Changes Veterans Equitable Resource Allocation (VERA) – a capitation-based resource allocation system. Funds allocated to the VISNs according to the number of patients who were provided care (averaged over the prior 3 years) and adjusted according to acuity and certain other factors. 22
VA Transformation. . . Key Structural & Process Changes Veterans Equitable Resource Allocation (VERA) – a capitation-based resource allocation system. Funds allocated to the VISNs according to the number of patients who were provided care (averaged over the prior 3 years) and adjusted according to acuity and certain other factors. 22
 VA Transformation… Resource Allocation Veterans Equitable Resource Allocation (VERA) Methodology - FY 1999 W Basic Care - $2, 857 (PMPM - $238) • 96% patients • 62% funds W Complex Care - $36, 955 (PMPM - $3080) • 4% patients • 38% funds 23
VA Transformation… Resource Allocation Veterans Equitable Resource Allocation (VERA) Methodology - FY 1999 W Basic Care - $2, 857 (PMPM - $238) • 96% patients • 62% funds W Complex Care - $36, 955 (PMPM - $3080) • 4% patients • 38% funds 23
 VA Transformation. . . Key Structural & Process Changes Ø Enhanced information management ü Implemented electronic health record systemwide ü Standardized information systems systemwide 24
VA Transformation. . . Key Structural & Process Changes Ø Enhanced information management ü Implemented electronic health record systemwide ü Standardized information systems systemwide 24
 RESULTS AT FIVE YEARS 25
RESULTS AT FIVE YEARS 25
 VA Transformation… Selected Results: FY 1995 -1999 Ø Implemented universal primary care Ø Closed 55% (28, 886) of acute care hospital beds Ø Reduced BDOC per 1000 patients by 68% Ø Increased patients treated by >24% (700, 000) Ø ~350, 000 (36%) fewer admissions per year Ø 48% increase (25 to 37 million) in ambulatory care visits Ø Decreased staffing by 12% (25, 867 FTEEs) 26
VA Transformation… Selected Results: FY 1995 -1999 Ø Implemented universal primary care Ø Closed 55% (28, 886) of acute care hospital beds Ø Reduced BDOC per 1000 patients by 68% Ø Increased patients treated by >24% (700, 000) Ø ~350, 000 (36%) fewer admissions per year Ø 48% increase (25 to 37 million) in ambulatory care visits Ø Decreased staffing by 12% (25, 867 FTEEs) 26
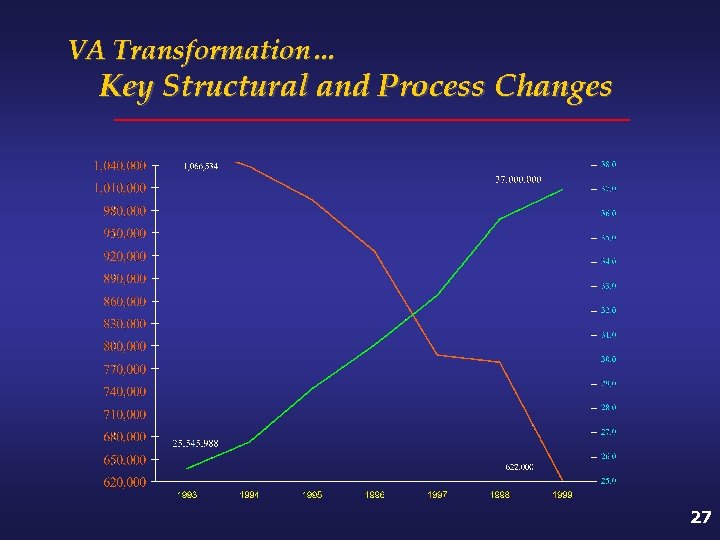 VA Transformation… Key Structural and Process Changes 27
VA Transformation… Key Structural and Process Changes 27
 VA Transformation… Selected Results: FY 1995 -1999 Ø Ø Ø Increased ambulatory surgery from 35% to >75% of all surgeries Established 302 new community-based outpatient clinics Merged the management and operations of 52 hospitals into 25 locally integrated systems Eliminated 72% (2, 793) of all forms and automated the rest Universal access and identification card 25% decrease in per patient costs (constant dollars) 28
VA Transformation… Selected Results: FY 1995 -1999 Ø Ø Ø Increased ambulatory surgery from 35% to >75% of all surgeries Established 302 new community-based outpatient clinics Merged the management and operations of 52 hospitals into 25 locally integrated systems Eliminated 72% (2, 793) of all forms and automated the rest Universal access and identification card 25% decrease in per patient costs (constant dollars) 28
 VA Transformation… Key Structural and Process Changes PERFORMANCE MANAGEMENT 29
VA Transformation… Key Structural and Process Changes PERFORMANCE MANAGEMENT 29
 VA Transformation… Performance Management Strategy Ø Align vision and mission with quantifiable strategic goals Ø Identify performance indicators for strategic goals Ø Hold managers accountable for achieving results 30
VA Transformation… Performance Management Strategy Ø Align vision and mission with quantifiable strategic goals Ø Identify performance indicators for strategic goals Ø Hold managers accountable for achieving results 30
 VA Transformation… Surgical Mortality and Morbidity Rates Ø Overall 30 -day mortality and morbidity rates dropped 9% and 30%, respectively, from 1994 to 1997 with no change in patient risk profile Ø Mortality rates lowest or equal to U. S. lowest for • Colectomy • Abdominal aortic aneurysm repair • Carotid endarterectomy • Cholecystectomy • Hip replacement 31
VA Transformation… Surgical Mortality and Morbidity Rates Ø Overall 30 -day mortality and morbidity rates dropped 9% and 30%, respectively, from 1994 to 1997 with no change in patient risk profile Ø Mortality rates lowest or equal to U. S. lowest for • Colectomy • Abdominal aortic aneurysm repair • Carotid endarterectomy • Cholecystectomy • Hip replacement 31
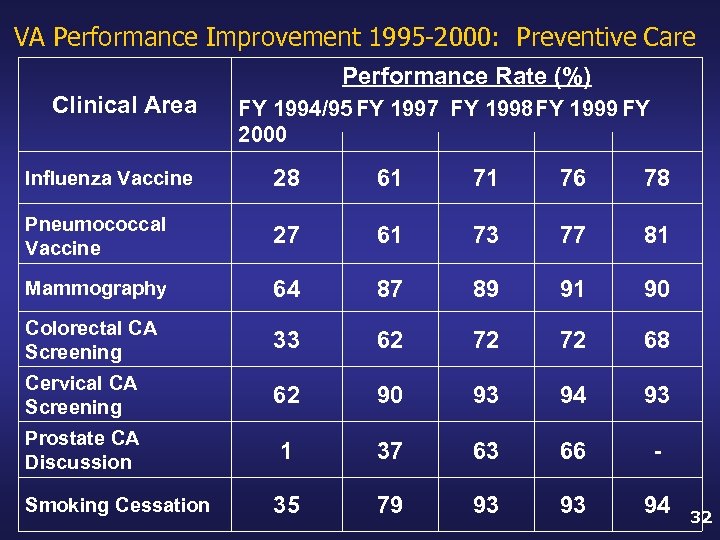 VA Performance Improvement 1995 -2000: Preventive Care Performance Rate (%) Clinical Area FY 1994/95 FY 1997 FY 1998 FY 1999 FY 2000 Influenza Vaccine 28 61 71 76 78 Pneumococcal Vaccine 27 61 73 77 81 Mammography 64 87 89 91 90 Colorectal CA Screening 33 62 72 72 68 Cervical CA Screening 62 90 93 94 93 Prostate CA Discussion 1 37 63 66 - 35 79 93 93 94 Smoking Cessation 32
VA Performance Improvement 1995 -2000: Preventive Care Performance Rate (%) Clinical Area FY 1994/95 FY 1997 FY 1998 FY 1999 FY 2000 Influenza Vaccine 28 61 71 76 78 Pneumococcal Vaccine 27 61 73 77 81 Mammography 64 87 89 91 90 Colorectal CA Screening 33 62 72 72 68 Cervical CA Screening 62 90 93 94 93 Prostate CA Discussion 1 37 63 66 - 35 79 93 93 94 Smoking Cessation 32
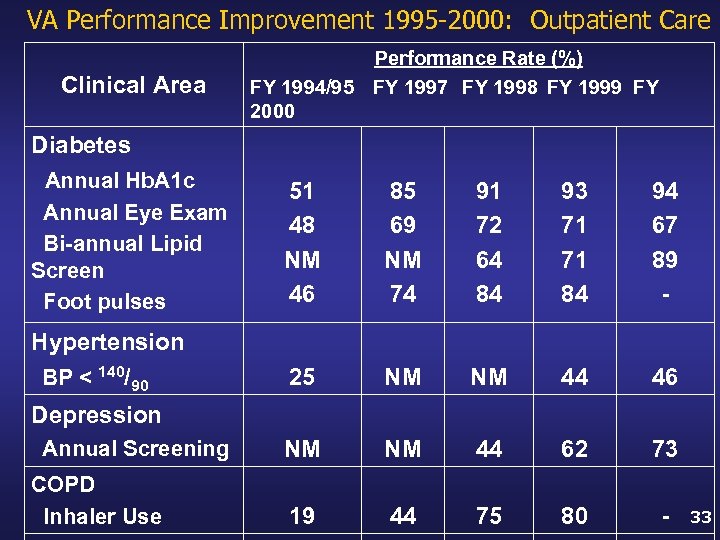 VA Performance Improvement 1995 -2000: Outpatient Care Clinical Area Performance Rate (%) FY 1994/95 FY 1997 FY 1998 FY 1999 FY 2000 Diabetes Annual Hb. A 1 c Annual Eye Exam Bi-annual Lipid Screen Foot pulses 51 48 NM 46 85 69 NM 74 91 72 64 84 93 71 71 84 94 67 89 - Hypertension BP < 140/90 25 NM NM 44 46 NM NM 44 62 73 19 44 75 80 - Depression Annual Screening COPD Inhaler Use 33
VA Performance Improvement 1995 -2000: Outpatient Care Clinical Area Performance Rate (%) FY 1994/95 FY 1997 FY 1998 FY 1999 FY 2000 Diabetes Annual Hb. A 1 c Annual Eye Exam Bi-annual Lipid Screen Foot pulses 51 48 NM 46 85 69 NM 74 91 72 64 84 93 71 71 84 94 67 89 - Hypertension BP < 140/90 25 NM NM 44 46 NM NM 44 62 73 19 44 75 80 - Depression Annual Screening COPD Inhaler Use 33
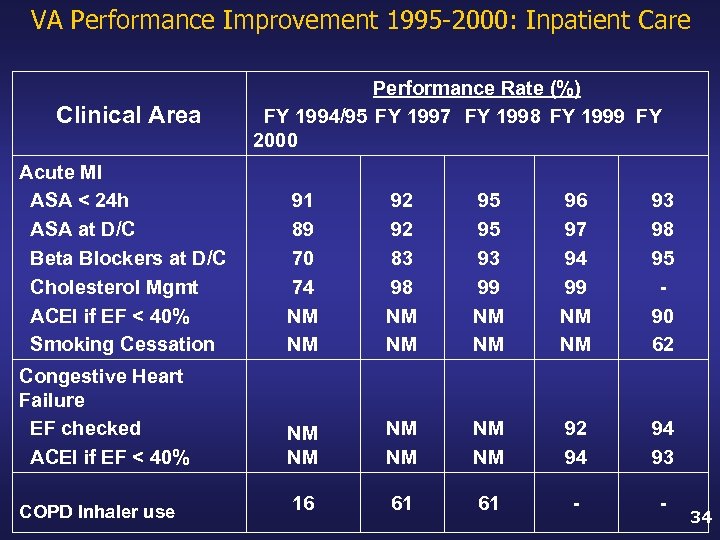 VA Performance Improvement 1995 -2000: Inpatient Care Clinical Area Performance Rate (%) FY 1994/95 FY 1997 FY 1998 FY 1999 FY 2000 Acute MI ASA < 24 h ASA at D/C Beta Blockers at D/C Cholesterol Mgmt ACEI if EF < 40% Smoking Cessation 91 89 70 74 NM NM 92 92 83 98 NM NM 95 95 93 99 NM NM 96 97 94 99 NM NM 93 98 95 90 62 Congestive Heart Failure EF checked ACEI if EF < 40% NM NM NM 92 94 94 93 COPD Inhaler use 16 61 61 - - 34
VA Performance Improvement 1995 -2000: Inpatient Care Clinical Area Performance Rate (%) FY 1994/95 FY 1997 FY 1998 FY 1999 FY 2000 Acute MI ASA < 24 h ASA at D/C Beta Blockers at D/C Cholesterol Mgmt ACEI if EF < 40% Smoking Cessation 91 89 70 74 NM NM 92 92 83 98 NM NM 95 95 93 99 NM NM 96 97 94 99 NM NM 93 98 95 90 62 Congestive Heart Failure EF checked ACEI if EF < 40% NM NM NM 92 94 94 93 COPD Inhaler use 16 61 61 - - 34
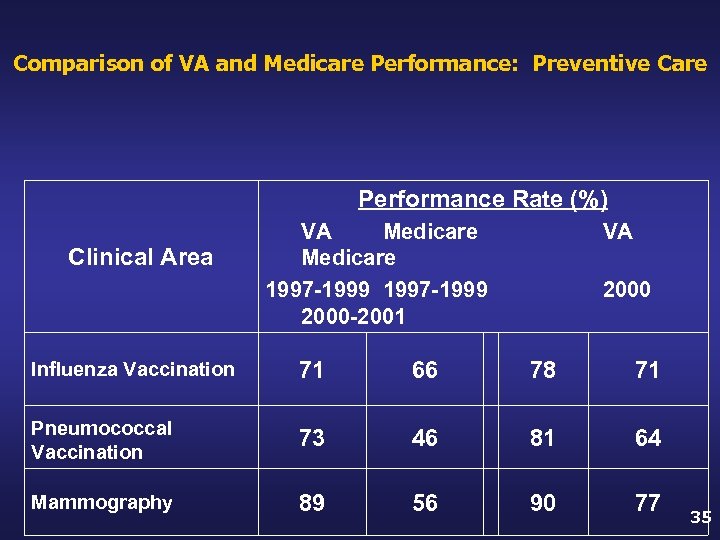 Comparison of VA and Medicare Performance: Preventive Care Performance Rate (%) Clinical Area VA Medicare 1997 -1999 2000 -2001 VA 2000 Influenza Vaccination 71 66 78 71 Pneumococcal Vaccination 73 46 81 64 Mammography 89 56 90 77 35
Comparison of VA and Medicare Performance: Preventive Care Performance Rate (%) Clinical Area VA Medicare 1997 -1999 2000 -2001 VA 2000 Influenza Vaccination 71 66 78 71 Pneumococcal Vaccination 73 46 81 64 Mammography 89 56 90 77 35
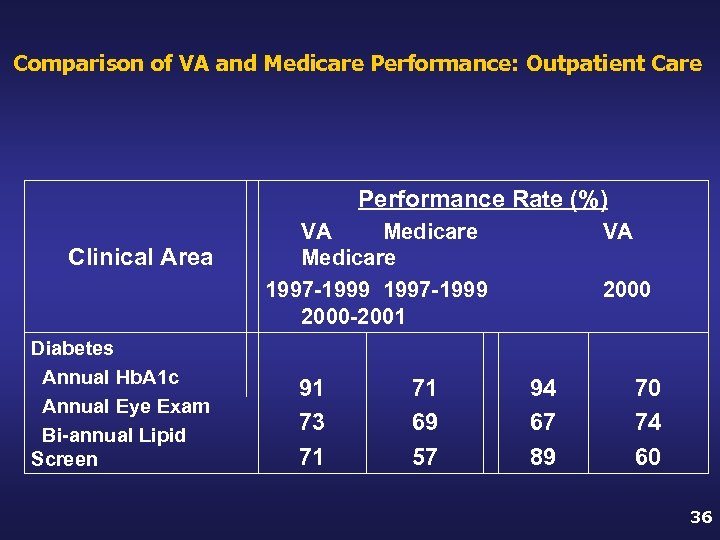 Comparison of VA and Medicare Performance: Outpatient Care Performance Rate (%) Clinical Area Diabetes Annual Hb. A 1 c Annual Eye Exam Bi-annual Lipid Screen VA Medicare 1997 -1999 2000 -2001 91 73 71 71 69 57 VA 2000 94 67 89 70 74 60 36
Comparison of VA and Medicare Performance: Outpatient Care Performance Rate (%) Clinical Area Diabetes Annual Hb. A 1 c Annual Eye Exam Bi-annual Lipid Screen VA Medicare 1997 -1999 2000 -2001 91 73 71 71 69 57 VA 2000 94 67 89 70 74 60 36
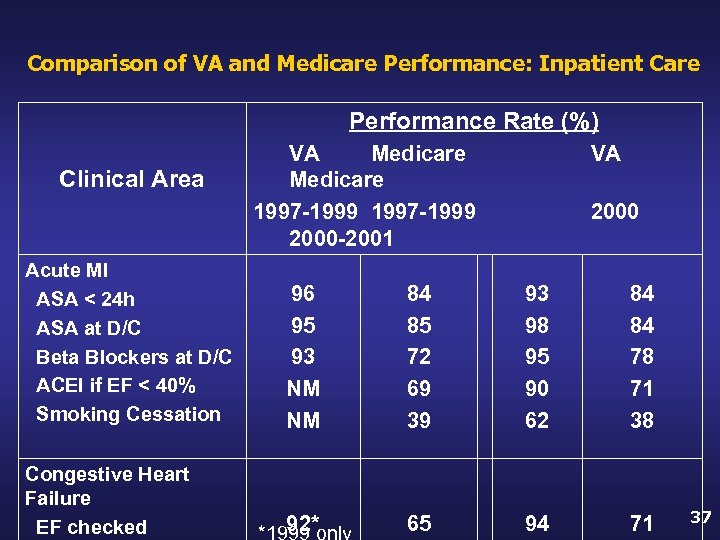 Comparison of VA and Medicare Performance: Inpatient Care Performance Rate (%) Clinical Area Acute MI ASA < 24 h ASA at D/C Beta Blockers at D/C ACEI if EF < 40% Smoking Cessation Congestive Heart Failure EF checked VA Medicare 1997 -1999 2000 -2001 VA 2000 96 95 93 NM NM 84 85 72 69 39 93 98 95 90 62 84 84 78 71 38 92* *1999 only 65 94 71 37
Comparison of VA and Medicare Performance: Inpatient Care Performance Rate (%) Clinical Area Acute MI ASA < 24 h ASA at D/C Beta Blockers at D/C ACEI if EF < 40% Smoking Cessation Congestive Heart Failure EF checked VA Medicare 1997 -1999 2000 -2001 VA 2000 96 95 93 NM NM 84 85 72 69 39 93 98 95 90 62 84 84 78 71 38 92* *1999 only 65 94 71 37
 VA Transformation… One Year Survival Rates for Selected High Volume Conditions 38
VA Transformation… One Year Survival Rates for Selected High Volume Conditions 38
 VA Transformation… American Customer Satisfaction Index Ø 80 percent of VHA users experience more satisfied now than two years ago. Ø VHA’s score on the index is 79 (the score for private hospitals is 70). 39
VA Transformation… American Customer Satisfaction Index Ø 80 percent of VHA users experience more satisfied now than two years ago. Ø VHA’s score on the index is 79 (the score for private hospitals is 70). 39
 VA Transformation… SOME LESSONS LEARNED 40
VA Transformation… SOME LESSONS LEARNED 40
 VA Transformation… LESSONS LEARNED Ø Rapid improvement is possible in a large, politically sensitive, financially stressed, publicly administered healthcare system. 41
VA Transformation… LESSONS LEARNED Ø Rapid improvement is possible in a large, politically sensitive, financially stressed, publicly administered healthcare system. 41
 VA Transformation… LESSONS LEARNED Ø Improved quality, better service and reduced cost can all be achieved at the same time. 42
VA Transformation… LESSONS LEARNED Ø Improved quality, better service and reduced cost can all be achieved at the same time. 42
 VA Transformation… LESSONS LEARNED ØHow you conceptualize your business is critically important. 43
VA Transformation… LESSONS LEARNED ØHow you conceptualize your business is critically important. 43
 VA Transformation… LESSONS LEARNED Ø Decentralization of operational decision making must be coupled with a full understanding of mission critical functions or activities, clear delineation of responsibility, and careful planning and monitoring of performance so that systemwide coordination and accountability. 44
VA Transformation… LESSONS LEARNED Ø Decentralization of operational decision making must be coupled with a full understanding of mission critical functions or activities, clear delineation of responsibility, and careful planning and monitoring of performance so that systemwide coordination and accountability. 44
 VA Transformation… LESSONS LEARNED Ø Focus on organizational performance, not on individuals. 45
VA Transformation… LESSONS LEARNED Ø Focus on organizational performance, not on individuals. 45
 VA Transformation… LESSONS LEARNED Ø Measuring and publicly reporting quality data is a powerful change strategy 46
VA Transformation… LESSONS LEARNED Ø Measuring and publicly reporting quality data is a powerful change strategy 46
 VA Transformation… LESSONS LEARNED ØA coordinated system of healthcare can be achieved by both vertical and virtual integration 47
VA Transformation… LESSONS LEARNED ØA coordinated system of healthcare can be achieved by both vertical and virtual integration 47
 VA Transformation… LESSONS LEARNED Ø Information is the basic currency of healthcare, and automated information management is critical to healthcare success today 48
VA Transformation… LESSONS LEARNED Ø Information is the basic currency of healthcare, and automated information management is critical to healthcare success today 48
 VA Transformation… LESSONS LEARNED Ø The information management system is the glue that holds an integrated system together 49
VA Transformation… LESSONS LEARNED Ø The information management system is the glue that holds an integrated system together 49
 VA Transformation… LESSONS LEARNED Ø Training and education must be included as an integral component of the change process so managers/staff prepared to function in the new way 50
VA Transformation… LESSONS LEARNED Ø Training and education must be included as an integral component of the change process so managers/staff prepared to function in the new way 50
 VA Transformation… LESSONS LEARNED Ø You cannot communicate too much; conventional communication strategies may not work well enough to keep front-line employees informed 51
VA Transformation… LESSONS LEARNED Ø You cannot communicate too much; conventional communication strategies may not work well enough to keep front-line employees informed 51
 VA Transformation… LESSONS LEARNED Ø Creation of a clear vision of the new future with a coherent transformation plan having concrete and concise goals and performance measures are essential 52
VA Transformation… LESSONS LEARNED Ø Creation of a clear vision of the new future with a coherent transformation plan having concrete and concise goals and performance measures are essential 52
 VA Transformation. . . Selected Principles The future is not what it used to be! 53
VA Transformation. . . Selected Principles The future is not what it used to be! 53
 NATIONAL QUALITY FORUM 54
NATIONAL QUALITY FORUM 54
 WHAT IS THE NQF? The National Quality Forum is a private, non-profit voluntary consensus standards setting organization. 55
WHAT IS THE NQF? The National Quality Forum is a private, non-profit voluntary consensus standards setting organization. 55
 HISTORY Ø Presidential Advisory Commission on Consumer Protection and Quality in the Health Care Industry established (1996) Ø Commission recommended the creation of a private sector entity (“Quality Forum”) that would bring healthcare stakeholder sectors together to standardize health care performance measures and standards (1998) Ø Quality Forum Planning Committee convened by White House (1998) Ø NQF incorporated in District of Columbia (1999) Ø NQF operational (2000) 56
HISTORY Ø Presidential Advisory Commission on Consumer Protection and Quality in the Health Care Industry established (1996) Ø Commission recommended the creation of a private sector entity (“Quality Forum”) that would bring healthcare stakeholder sectors together to standardize health care performance measures and standards (1998) Ø Quality Forum Planning Committee convened by White House (1998) Ø NQF incorporated in District of Columbia (1999) Ø NQF operational (2000) 56
 Mission The mission of the NQF is to improve American healthcare through endorsement of consensus-based standards for measurement and public reporting of healthcare performance data that provides meaningful information about whether care is patient-entered, safe, timely, beneficial, equitable and efficient. 57
Mission The mission of the NQF is to improve American healthcare through endorsement of consensus-based standards for measurement and public reporting of healthcare performance data that provides meaningful information about whether care is patient-entered, safe, timely, beneficial, equitable and efficient. 57
 Strategic Vision 1) NQF-endorsed standards will become the primary standards used to measure the quality of health care in the United States 2) The NQF will be the principal body that endorses national healthcare performance measures, quality indicators and/or quality of care standards; 3) The NQF will increase the demand for high quality healthcare; and 4) The NQF will be recognized as a major driving force for and facilitator of continuous improvement of American healthcare quality. 58
Strategic Vision 1) NQF-endorsed standards will become the primary standards used to measure the quality of health care in the United States 2) The NQF will be the principal body that endorses national healthcare performance measures, quality indicators and/or quality of care standards; 3) The NQF will increase the demand for high quality healthcare; and 4) The NQF will be recognized as a major driving force for and facilitator of continuous improvement of American healthcare quality. 58
 Board of Directors Ø 23 voting members ü The CEOs of 3 federal agencies (CMS, OPM and AHRQ) ü Representatives of state health officers and Medicaid ü Private sector representatives Ø 6 liaison members (JCAHO, NCQA, IOM, NIH, FACCT and PCPI-AMA) Ø Consumers and purchasers a majority 59
Board of Directors Ø 23 voting members ü The CEOs of 3 federal agencies (CMS, OPM and AHRQ) ü Representatives of state health officers and Medicaid ü Private sector representatives Ø 6 liaison members (JCAHO, NCQA, IOM, NIH, FACCT and PCPI-AMA) Ø Consumers and purchasers a majority 59
 UNIQUE FEATURES Ø Ø Ø Open membership Public and private sector representation on governing board Equitable status of stakeholder sectors (member councils) Attention to overall strategy for measuring and reporting healthcare quality, including establishing national goals Focus is on the entire continuum of healthcare Formal consensus process (“voluntary consensus standards”) 60
UNIQUE FEATURES Ø Ø Ø Open membership Public and private sector representation on governing board Equitable status of stakeholder sectors (member councils) Attention to overall strategy for measuring and reporting healthcare quality, including establishing national goals Focus is on the entire continuum of healthcare Formal consensus process (“voluntary consensus standards”) 60
 National Technology and Transfer Advancement of Act of 1995 (NTTAA) Ø Defines the 5 key attributes of a “voluntary consensus standards body” (i. e. , openness, balance of interest, due process, consensus, and an appeals process) Ø Obligates federal government to adopt voluntary consensus standards (when the government is adopting standards) Ø Encourages federal government to participate in setting voluntary consensus standards 61
National Technology and Transfer Advancement of Act of 1995 (NTTAA) Ø Defines the 5 key attributes of a “voluntary consensus standards body” (i. e. , openness, balance of interest, due process, consensus, and an appeals process) Ø Obligates federal government to adopt voluntary consensus standards (when the government is adopting standards) Ø Encourages federal government to participate in setting voluntary consensus standards 61
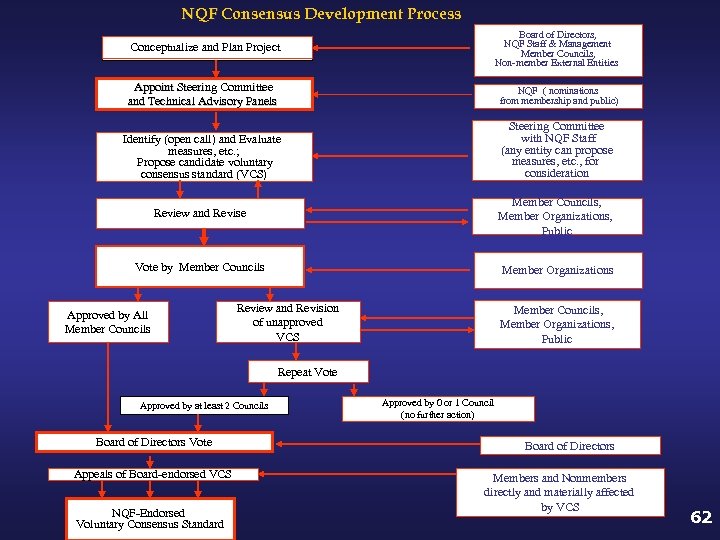 NQF Consensus Development Process Conceptualize and Plan Project Board of Directors, NQF Staff & Management Member Councils, Non-member External Entities Appoint Steering Committee and Technical Advisory Panels NQF ( nominations from membership and public) Identify (open call) and Evaluate measures, etc. ; Propose candidate voluntary consensus standard (VCS) Steering Committee with NQF Staff (any entity can propose measures, etc. , for consideration Review and Revise Member Councils, Member Organizations, Public Vote by Member Councils Member Organizations Approved by All Member Councils Review and Revision of unapproved VCS Member Councils, Member Organizations, Public Repeat Vote Approved by at least 2 Councils Board of Directors Vote Appeals of Board-endorsed VCS NQF-Endorsed Voluntary Consensus Standard Approved by 0 or 1 Council (no further action) Board of Directors Members and Nonmembers directly and materially affected by VCS 62
NQF Consensus Development Process Conceptualize and Plan Project Board of Directors, NQF Staff & Management Member Councils, Non-member External Entities Appoint Steering Committee and Technical Advisory Panels NQF ( nominations from membership and public) Identify (open call) and Evaluate measures, etc. ; Propose candidate voluntary consensus standard (VCS) Steering Committee with NQF Staff (any entity can propose measures, etc. , for consideration Review and Revise Member Councils, Member Organizations, Public Vote by Member Councils Member Organizations Approved by All Member Councils Review and Revision of unapproved VCS Member Councils, Member Organizations, Public Repeat Vote Approved by at least 2 Councils Board of Directors Vote Appeals of Board-endorsed VCS NQF-Endorsed Voluntary Consensus Standard Approved by 0 or 1 Council (no further action) Board of Directors Members and Nonmembers directly and materially affected by VCS 62
 SELECTED PROJECTS Ø Serious Reportable Adverse Events Ø Safe Practices Ø Diabetes Management National Consensus Standards Ø Hospital Care National Performance Measures Ø Nursing Home Care Performance Measures Ø Home Health Care Performance Measures Ø Cancer Care Quality Measures 63
SELECTED PROJECTS Ø Serious Reportable Adverse Events Ø Safe Practices Ø Diabetes Management National Consensus Standards Ø Hospital Care National Performance Measures Ø Nursing Home Care Performance Measures Ø Home Health Care Performance Measures Ø Cancer Care Quality Measures 63
 SELECTED PROJECTS ØMammography ØCardiac Surgery Performance Measures ØNursing Care Performance Measures ØAmbulatory ØChild Standards for Consumers Care Performance Measures Healthcare Performance Measures ØBehavioral ØAcademic Healthcare Performance Measures Health Centers Performance Measures 64
SELECTED PROJECTS ØMammography ØCardiac Surgery Performance Measures ØNursing Care Performance Measures ØAmbulatory ØChild Standards for Consumers Care Performance Measures Healthcare Performance Measures ØBehavioral ØAcademic Healthcare Performance Measures Health Centers Performance Measures 64
 SELECTED PROJECTS ØEnd of Life Care Performance Measures ØPatient Safety Taxonomy ØStandardizing Credentialing ØPatient Safety and Medication Use – Special Emphasis for Limited Proficiency/Low Literacy Populations ØNational Commission for Quality Long Term Care 65
SELECTED PROJECTS ØEnd of Life Care Performance Measures ØPatient Safety Taxonomy ØStandardizing Credentialing ØPatient Safety and Medication Use – Special Emphasis for Limited Proficiency/Low Literacy Populations ØNational Commission for Quality Long Term Care 65


