e5902c7b77d1a4a8345862580e1af41f.ppt
- Количество слайдов: 39
 Psychiatry in Older Adults - the primary care perspective Dr Pramod Prabhakaran Consultant Psychiatrist, CNWL NHS Foundation Trust Hon. Sr. Lecturer and Jt. Course Leader, Imperial College pramodp@doctors. org. uk 02084247717, 07838254672
Psychiatry in Older Adults - the primary care perspective Dr Pramod Prabhakaran Consultant Psychiatrist, CNWL NHS Foundation Trust Hon. Sr. Lecturer and Jt. Course Leader, Imperial College pramodp@doctors. org. uk 02084247717, 07838254672
 Topics Clinical – – Dementia - workup, diagnostic process Acute Confusional State Suicide in Elderly Li. Toxicity, NMS, Serotonin syndrome, Metabolic syndrome MCA and DOLS Dementia Strategy Discussion/ Questions
Topics Clinical – – Dementia - workup, diagnostic process Acute Confusional State Suicide in Elderly Li. Toxicity, NMS, Serotonin syndrome, Metabolic syndrome MCA and DOLS Dementia Strategy Discussion/ Questions

 Case Example Mrs P • • • Anne, aged 76 living alone, housing association flat Three children, Good social support home help daily
Case Example Mrs P • • • Anne, aged 76 living alone, housing association flat Three children, Good social support home help daily
 History • patient unaware of any problems • First referred two years ago – – Forgetting to pay bills Food out-of-date Forgot grandchild’s birthday Initial MMSE 20/30 • Non-smoker, previously healthy • living alone and coping well
History • patient unaware of any problems • First referred two years ago – – Forgetting to pay bills Food out-of-date Forgot grandchild’s birthday Initial MMSE 20/30 • Non-smoker, previously healthy • living alone and coping well
 History increasingly forgetful since first presentation Now • wandering at night • Forgetting to eat • Lets strangers into flat
History increasingly forgetful since first presentation Now • wandering at night • Forgetting to eat • Lets strangers into flat
 Examination • • • Not depressed MMSE 11/30 Disheveled Thin Vague and defensive
Examination • • • Not depressed MMSE 11/30 Disheveled Thin Vague and defensive
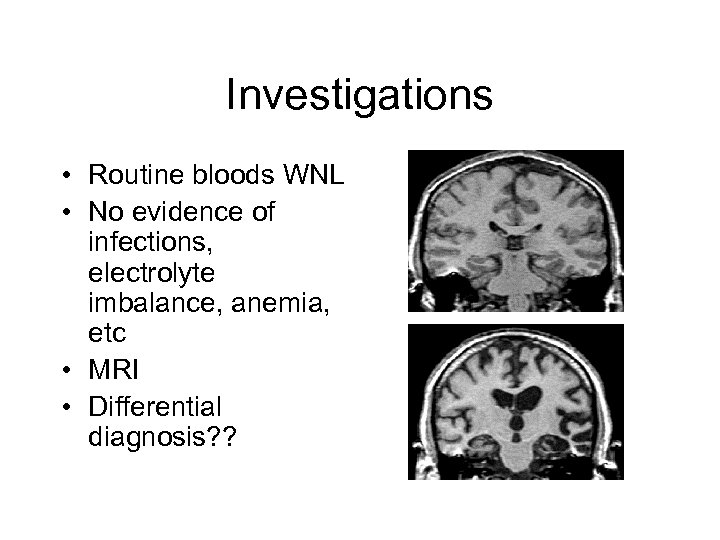 Investigations • Routine bloods WNL • No evidence of infections, electrolyte imbalance, anemia, etc • MRI • Differential diagnosis? ?
Investigations • Routine bloods WNL • No evidence of infections, electrolyte imbalance, anemia, etc • MRI • Differential diagnosis? ?
 Dementia - definition “global impairment of higher mental function in clear consciousness”
Dementia - definition “global impairment of higher mental function in clear consciousness”
 Dementia ICD-10 • Decline in: – memory – other cognitive abilities • planning • organising • problem solving – absence of clouding of consciousness – change in emotion, personality or behaviour
Dementia ICD-10 • Decline in: – memory – other cognitive abilities • planning • organising • problem solving – absence of clouding of consciousness – change in emotion, personality or behaviour
 Dementia - Epidemiology • • • 5% in individuals over 65 20% in over 80’s 700, 000 cases in the UK In 2000, 0. 4 million men and 0. 9 million women over 85. Projected to be 1. 4 and 2. 4 million respectively by 2050 67. 2/100000 in 30 - 60 age group • • Lobo et al 2001 Alzheimer’s society
Dementia - Epidemiology • • • 5% in individuals over 65 20% in over 80’s 700, 000 cases in the UK In 2000, 0. 4 million men and 0. 9 million women over 85. Projected to be 1. 4 and 2. 4 million respectively by 2050 67. 2/100000 in 30 - 60 age group • • Lobo et al 2001 Alzheimer’s society
 Dementia types • • • Alzheimers - 55% Vascular - 20% Dementia with Lewy Bodies - 15% Fronto-temporal dementia - 5% Other - 5%
Dementia types • • • Alzheimers - 55% Vascular - 20% Dementia with Lewy Bodies - 15% Fronto-temporal dementia - 5% Other - 5%
 Dementia types • “common, ” rare dementias (<5% of cases) – Fronto-temporal dementia – Picks disease – Huntington’s disease – alcohol dementia – metabolic disorders
Dementia types • “common, ” rare dementias (<5% of cases) – Fronto-temporal dementia – Picks disease – Huntington’s disease – alcohol dementia – metabolic disorders
 Dementia types • Some “treatable” dementias (very rare) – vitamin deficiency (B 1, B 12) – syphilis – normal pressure hydrocephalus – hypothyroidism – cerebral tumours (especially meningiomas) – subdural haematoma
Dementia types • Some “treatable” dementias (very rare) – vitamin deficiency (B 1, B 12) – syphilis – normal pressure hydrocephalus – hypothyroidism – cerebral tumours (especially meningiomas) – subdural haematoma
 Dementia - Differential diagnosis • mild cognitive impairment – (age-associated memory impairment) • • depression delirium dysphasia learning disability
Dementia - Differential diagnosis • mild cognitive impairment – (age-associated memory impairment) • • depression delirium dysphasia learning disability
 Alzheimer’s disease • Most common type • Genetics - presenilin 1, 2, APP • Pathology - Beta amyloid plaques and NFT’s • Risk factors - Old age, Downs, Head injury, Vascular, premorbid intelligence
Alzheimer’s disease • Most common type • Genetics - presenilin 1, 2, APP • Pathology - Beta amyloid plaques and NFT’s • Risk factors - Old age, Downs, Head injury, Vascular, premorbid intelligence
 Alzheimer’s disease characteristics • Insidious onset • Gradual progression • Typical cognitive profile - temporal disorientation, impaired short term memory, new learning affected, 4 A’s - amnesia, agnosia, apraxia and aphasia • Impaired insight • Behavioural symptoms common - depression, psychosis in about 1/3 to 1/2 • Ch. I’s useful
Alzheimer’s disease characteristics • Insidious onset • Gradual progression • Typical cognitive profile - temporal disorientation, impaired short term memory, new learning affected, 4 A’s - amnesia, agnosia, apraxia and aphasia • Impaired insight • Behavioural symptoms common - depression, psychosis in about 1/3 to 1/2 • Ch. I’s useful
 Vascular Dementia • single strategic stroke – thalamus • • • multiple large vessel infarcts multiple subcortical (lacunar) infarcts extensive white matter disease hypoxic brain damage vasculitis
Vascular Dementia • single strategic stroke – thalamus • • • multiple large vessel infarcts multiple subcortical (lacunar) infarcts extensive white matter disease hypoxic brain damage vasculitis
 Vascular Dementia characteristics • • • abrupt onset stepwise deterioration fluctuating course vascular risk factors focal neurological signs patchy deficits Insight better Depression more common Fluctuations more common
Vascular Dementia characteristics • • • abrupt onset stepwise deterioration fluctuating course vascular risk factors focal neurological signs patchy deficits Insight better Depression more common Fluctuations more common
 Case example • 75 male Italian, married, living at home. • 1 year history of memory problems, mainly short term, and disorientation to time and place • 3/12 - seeing several strangers in the house, house restaurant with excellent food and wine, which wife disputes. Not distressed by this. Sometimes says that he is seeing things. • Differential diagnosis? ?
Case example • 75 male Italian, married, living at home. • 1 year history of memory problems, mainly short term, and disorientation to time and place • 3/12 - seeing several strangers in the house, house restaurant with excellent food and wine, which wife disputes. Not distressed by this. Sometimes says that he is seeing things. • Differential diagnosis? ?
 Case example • 89 year female in NH • Multiple medical problems including severe osteoarthritis • ? Dementia of several years duration • Now acutely psychotic - very agitated, accused staff of trying to rape her, said she saw them in her room at night • Was better when reviewed next morning • Differential diagnosis? ?
Case example • 89 year female in NH • Multiple medical problems including severe osteoarthritis • ? Dementia of several years duration • Now acutely psychotic - very agitated, accused staff of trying to rape her, said she saw them in her room at night • Was better when reviewed next morning • Differential diagnosis? ?
 Lewy Body disease • Progressive cognitive decline of insidious onset and gradual progression • Fluctuations often marked • Hallucinations, esp. visual and secondary delusions • REM sleep behaviour disorder • Parkinsonian symptoms • Falls • Hallucinators respond better to Ch. I’s
Lewy Body disease • Progressive cognitive decline of insidious onset and gradual progression • Fluctuations often marked • Hallucinations, esp. visual and secondary delusions • REM sleep behaviour disorder • Parkinsonian symptoms • Falls • Hallucinators respond better to Ch. I’s
 Acute Confusional State • • Rapid onset May have pre-existing dementia Intrusive abnormalities of perception or affect Fluctuating confusion and agitation – Often worse at night • Hypoactive, hyperactive or mixed (usually)
Acute Confusional State • • Rapid onset May have pre-existing dementia Intrusive abnormalities of perception or affect Fluctuating confusion and agitation – Often worse at night • Hypoactive, hyperactive or mixed (usually)
 Delirium - causes I WATCH DEATH • • • Infectious Withdrawal Acute metabolic Trauma CNS Pathology Hypoxia Deficiencies Endocrinopathies Acute vascular Toxins/drugs Heavy Metals • Note that prescribed medicines may cause delirium
Delirium - causes I WATCH DEATH • • • Infectious Withdrawal Acute metabolic Trauma CNS Pathology Hypoxia Deficiencies Endocrinopathies Acute vascular Toxins/drugs Heavy Metals • Note that prescribed medicines may cause delirium
 Suicide in the Elderly • Suicide rates highest in males > 75 • UK - approx 19/100, 000/year • Methods: Men - hanging, women - OD. – CNWL - jumping • Depression in 60 - 90% • Conwell et al 1996 - 60% major depression, non affective psychosis rare, addiction less common, late onset depression the rule. • However, parasuicide less common, hence necessary to refer to 2 care. Rates decreasing.
Suicide in the Elderly • Suicide rates highest in males > 75 • UK - approx 19/100, 000/year • Methods: Men - hanging, women - OD. – CNWL - jumping • Depression in 60 - 90% • Conwell et al 1996 - 60% major depression, non affective psychosis rare, addiction less common, late onset depression the rule. • However, parasuicide less common, hence necessary to refer to 2 care. Rates decreasing.
 SAD PERSONS S ex (male) A ge (elderly or adolescent) D epression P revious attempts E thanol abuse R ational thinking loss (psychosis) S ocial supports lacking O rganised plan to commit suicide N o spouse (divorced > widowed > single) S ickness (physical illness)
SAD PERSONS S ex (male) A ge (elderly or adolescent) D epression P revious attempts E thanol abuse R ational thinking loss (psychosis) S ocial supports lacking O rganised plan to commit suicide N o spouse (divorced > widowed > single) S ickness (physical illness)
 Lithium toxicity • Commonly used for MDD, BAD - high risk group • Narrow therapeutic index ( adults 0. 6 to 1, elderly 0. 4 - 0. 8) • Half life 12 - 27 hours, increased with chronic use and in the elderly • Other medications esp loop diuretics and ACE inhibitors • Medical comorbidity • Commonest cause for litigation in psychiatry
Lithium toxicity • Commonly used for MDD, BAD - high risk group • Narrow therapeutic index ( adults 0. 6 to 1, elderly 0. 4 - 0. 8) • Half life 12 - 27 hours, increased with chronic use and in the elderly • Other medications esp loop diuretics and ACE inhibitors • Medical comorbidity • Commonest cause for litigation in psychiatry
 Lithium toxicity • Symptoms – Nausea and vomiting – Diarrhoea – Weakness and fatigue – Lethargy and confusion – Tremor – Seizure
Lithium toxicity • Symptoms – Nausea and vomiting – Diarrhoea – Weakness and fatigue – Lethargy and confusion – Tremor – Seizure
 Li toxicity - physical • Mild to moderate toxicity – Generalised weakness, fine resting tremor, mild confusion • Moderate to severe toxicity – Severe tremor, fasciculations, hyperreflexia, stupor, coma, seizures, shock.
Li toxicity - physical • Mild to moderate toxicity – Generalised weakness, fine resting tremor, mild confusion • Moderate to severe toxicity – Severe tremor, fasciculations, hyperreflexia, stupor, coma, seizures, shock.
 Neuroleptic Malignant Syndrome • Reaction to D 2 antagonist medication, such as antipsychotics, phenergan, metoclopramide, etc • Rare, idiosyncratic • Clinical signs - fever, rigidity, tremor, diaphoresis, tachycardia, hypertension or hypotension, altered mental state. • Elderly - organic conditions, other medications predispose. • Complication - rhabdomyolysis and Acute renal failure. • Inv - CK levels + others
Neuroleptic Malignant Syndrome • Reaction to D 2 antagonist medication, such as antipsychotics, phenergan, metoclopramide, etc • Rare, idiosyncratic • Clinical signs - fever, rigidity, tremor, diaphoresis, tachycardia, hypertension or hypotension, altered mental state. • Elderly - organic conditions, other medications predispose. • Complication - rhabdomyolysis and Acute renal failure. • Inv - CK levels + others
 Serotonin syndrome • Potentially life threatening syndrome related to use of serotonergic medication. • Clinical presentation - similar to NMS, differences - acute onset, myoclonus > rigidity, rhabdomyolysis rare, Rx supportive.
Serotonin syndrome • Potentially life threatening syndrome related to use of serotonergic medication. • Clinical presentation - similar to NMS, differences - acute onset, myoclonus > rigidity, rhabdomyolysis rare, Rx supportive.
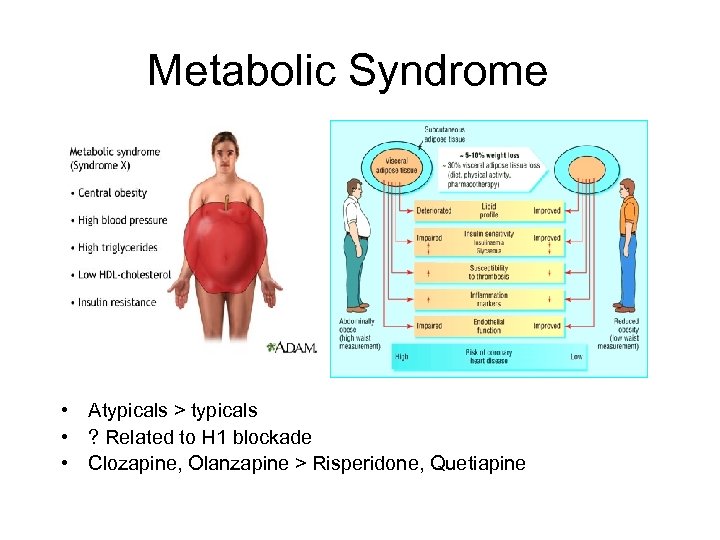 Metabolic Syndrome • Atypicals > typicals • ? Related to H 1 blockade • Clozapine, Olanzapine > Risperidone, Quetiapine
Metabolic Syndrome • Atypicals > typicals • ? Related to H 1 blockade • Clozapine, Olanzapine > Risperidone, Quetiapine
 Mental Capacity Act 2005 key principles • A presumption of capacity • Individuals must be supported in making their own decisions • Individuals with capacity retain the right to make what might appear to be unwise decisions • Best interests • Least restrictive option
Mental Capacity Act 2005 key principles • A presumption of capacity • Individuals must be supported in making their own decisions • Individuals with capacity retain the right to make what might appear to be unwise decisions • Best interests • Least restrictive option
 MCA 2005 definition of capacity • Patient lacks capacity if because of an impairment of, or a disturbance in the functioning of, the brain or mind (which can be permanent or temporary), he is unable to: – – understand information relevant to the decision retain that information use or weigh the information, or communicate a decision
MCA 2005 definition of capacity • Patient lacks capacity if because of an impairment of, or a disturbance in the functioning of, the brain or mind (which can be permanent or temporary), he is unable to: – – understand information relevant to the decision retain that information use or weigh the information, or communicate a decision
 Deprivation Of Liberty Safeguards • Introduced into Mental Capacity Act 2005 (MCA) through the Mental Health Act 2007 • Will prevent arbitrary decisions that deprive vulnerable people of their liberty • Safeguards are to protect service users and if they do need to be deprived of their liberty give them representatives, rights of appeal and for the “deprivation” to be reviewed and monitored. • Safeguards cover people in hospital and care homes registered under the Care Standards Act 2000 • Statutory obligation in April 2009
Deprivation Of Liberty Safeguards • Introduced into Mental Capacity Act 2005 (MCA) through the Mental Health Act 2007 • Will prevent arbitrary decisions that deprive vulnerable people of their liberty • Safeguards are to protect service users and if they do need to be deprived of their liberty give them representatives, rights of appeal and for the “deprivation” to be reviewed and monitored. • Safeguards cover people in hospital and care homes registered under the Care Standards Act 2000 • Statutory obligation in April 2009
 What is Deprivation of Liberty? • Arises from the “Bournewood” case – a ECt. HR case – Article 5. • HL had been deprived of his liberty unlawfully, because of a lack of a legal procedure which offered sufficient safeguards against arbitrary detention (5(1)) and speedy access to court (5 (4)) • “The distinction between deprivation of and restriction upon liberty is merely one of degree or intensity and not one of nature or substance” • Therefore no definition • Subsequent case law e. g. DE and JE v Surrey County Council • Cases to date have arisen from refusals of requests for “discharge”
What is Deprivation of Liberty? • Arises from the “Bournewood” case – a ECt. HR case – Article 5. • HL had been deprived of his liberty unlawfully, because of a lack of a legal procedure which offered sufficient safeguards against arbitrary detention (5(1)) and speedy access to court (5 (4)) • “The distinction between deprivation of and restriction upon liberty is merely one of degree or intensity and not one of nature or substance” • Therefore no definition • Subsequent case law e. g. DE and JE v Surrey County Council • Cases to date have arisen from refusals of requests for “discharge”
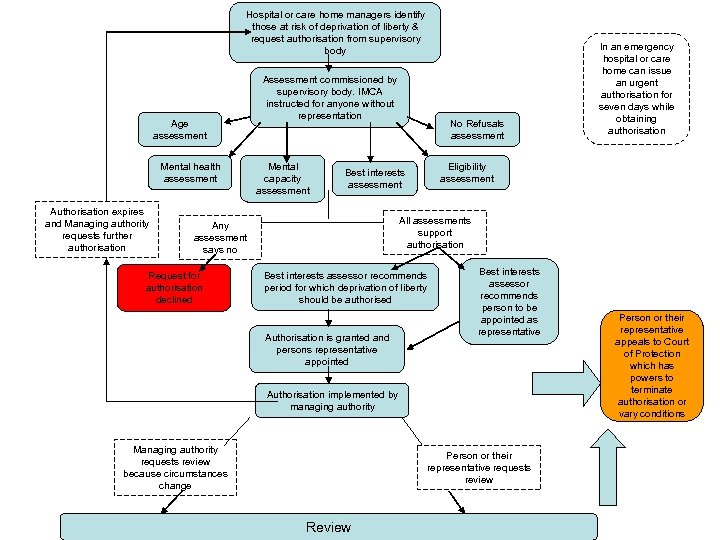 Hospital or care home managers identify those at risk of deprivation of liberty & request authorisation from supervisory body Age assessment Mental health assessment Authorisation expires and Managing authority requests further authorisation Assessment commissioned by supervisory body. IMCA instructed for anyone without representation Mental capacity assessment Eligibility assessment Best interests assessment All assessments support authorisation Any assessment says no Request for authorisation declined No Refusals assessment In an emergency hospital or care home can issue an urgent authorisation for seven days while obtaining authorisation Best interests assessor recommends period for which deprivation of liberty should be authorised Authorisation is granted and persons representative appointed Best interests assessor recommends person to be appointed as representative Authorisation implemented by managing authority Managing authority requests review because circumstances change Person or their representative requests review Review Person or their representative appeals to Court of Protection which has powers to terminate authorisation or vary conditions
Hospital or care home managers identify those at risk of deprivation of liberty & request authorisation from supervisory body Age assessment Mental health assessment Authorisation expires and Managing authority requests further authorisation Assessment commissioned by supervisory body. IMCA instructed for anyone without representation Mental capacity assessment Eligibility assessment Best interests assessment All assessments support authorisation Any assessment says no Request for authorisation declined No Refusals assessment In an emergency hospital or care home can issue an urgent authorisation for seven days while obtaining authorisation Best interests assessor recommends period for which deprivation of liberty should be authorised Authorisation is granted and persons representative appointed Best interests assessor recommends person to be appointed as representative Authorisation implemented by managing authority Managing authority requests review because circumstances change Person or their representative requests review Review Person or their representative appeals to Court of Protection which has powers to terminate authorisation or vary conditions
 Dementia Strategy • 3 main themes – Raising awareness and understanding – Early diagnosis and support – Living well with dementia • 150 million nationally in first 2 years
Dementia Strategy • 3 main themes – Raising awareness and understanding – Early diagnosis and support – Living well with dementia • 150 million nationally in first 2 years
 Discussion/ Questions • Referral process and required information
Discussion/ Questions • Referral process and required information


