68f1ff1eefefae0e7639bc21509d9757.ppt
- Количество слайдов: 23

Promoting rational use of medicines: a global perspective Hans V. Hogerzeil, MD Ph. D FRCP Edin Director, Medicines Policy and Standards World Health Organization www. who. int/medicines WHO/PSM

The problem • Increasing antimicrobial resistance – 70 -90% resistance to original 1 st line antibiotics for dysentery (shigella), pneumonia (pneumococcal), gonorrhoea, and hospital infections (staph. aureus) – Driven by over-use and inappropriate use of antimicrobials and poor infection control • Over-use & incorrect use medicines – Over half of all prescriptions are inappropriate or incorrect – Over half of all medicines are not taken correctly by patients – One-third of the world's population does not have regular access to essential medicines WHO/PSM
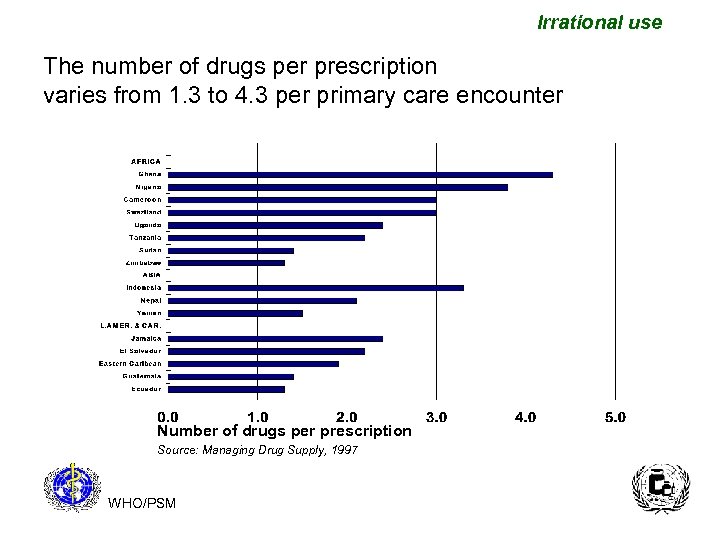
Irrational use The number of drugs per prescription varies from 1. 3 to 4. 3 per primary care encounter Number of drugs per prescription Source: Managing Drug Supply, 1997 WHO/PSM
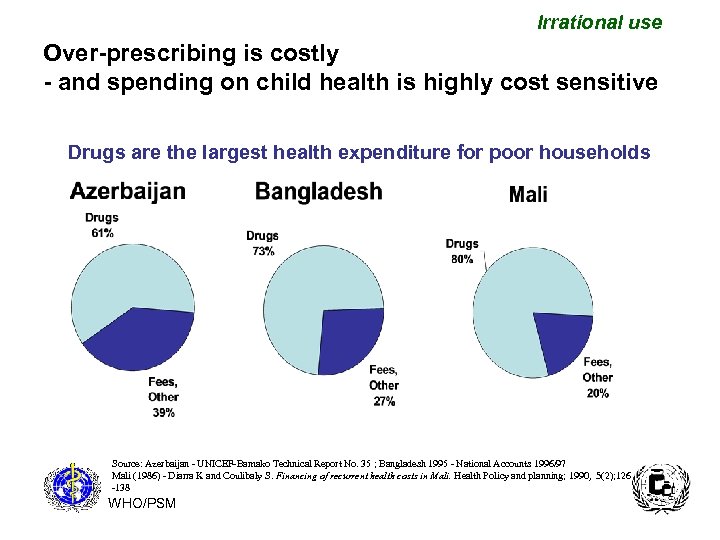
Irrational use Over-prescribing is costly - and spending on child health is highly cost sensitive Drugs are the largest health expenditure for poor households Source: Azerbaijan - UNICEF-Bamako Technical Report No. 35 ; Bangladesh 1995 - National Accounts 1996/97 Mali (1986) - Diarra K and Coulibaly S. Financing of recurrent health costs in Mali. Health Policy and planning; 1990, 5(2); 126 -138 WHO/PSM
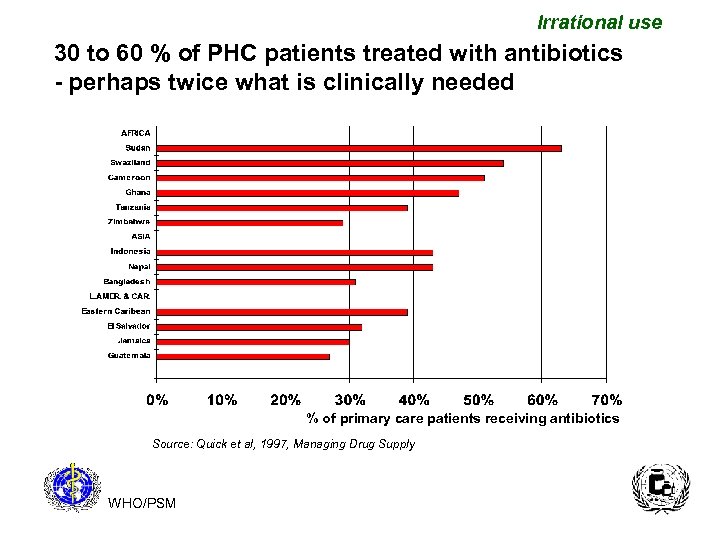
Irrational use 30 to 60 % of PHC patients treated with antibiotics - perhaps twice what is clinically needed % of primary care patients receiving antibiotics Source: Quick et al, 1997, Managing Drug Supply WHO/PSM
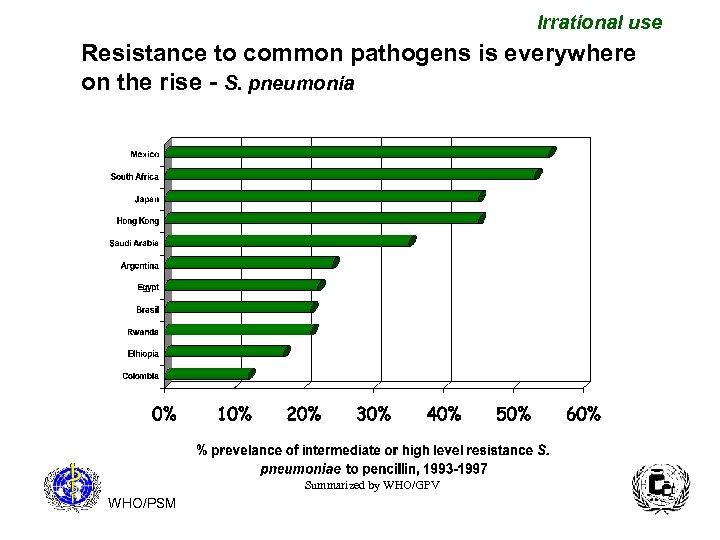
Irrational use Resistance to common pathogens is everywhere on the rise - S. pneumonia Summarized by WHO/GPV WHO/PSM
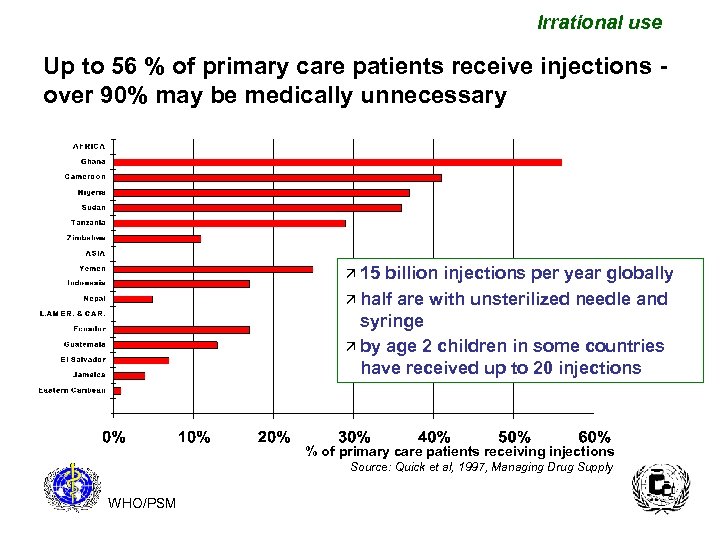
Irrational use Up to 56 % of primary care patients receive injections over 90% may be medically unnecessary ä 15 billion injections per year globally ä half are with unsterilized needle and syringe ä by age 2 children in some countries have received up to 20 injections % of primary care patients receiving injections Source: Quick et al, 1997, Managing Drug Supply WHO/PSM
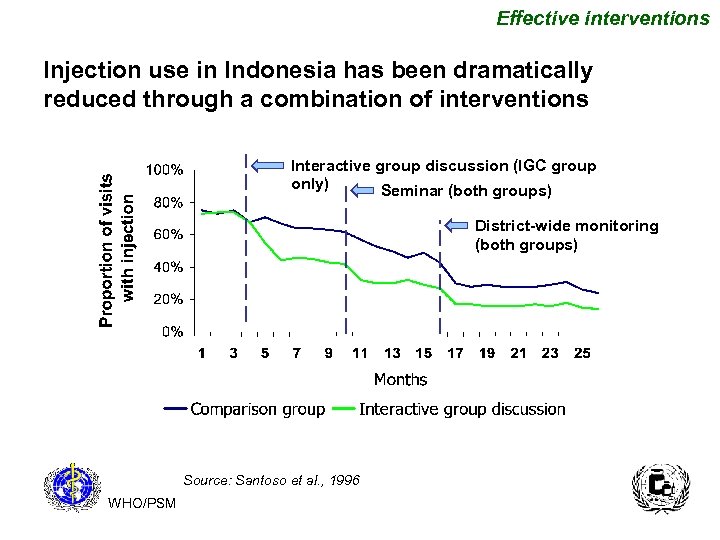
Effective interventions Injection use in Indonesia has been dramatically reduced through a combination of interventions Interactive group discussion (IGC group only) Seminar (both groups) District-wide monitoring (both groups) Source: Santoso et al. , 1996 WHO/PSM
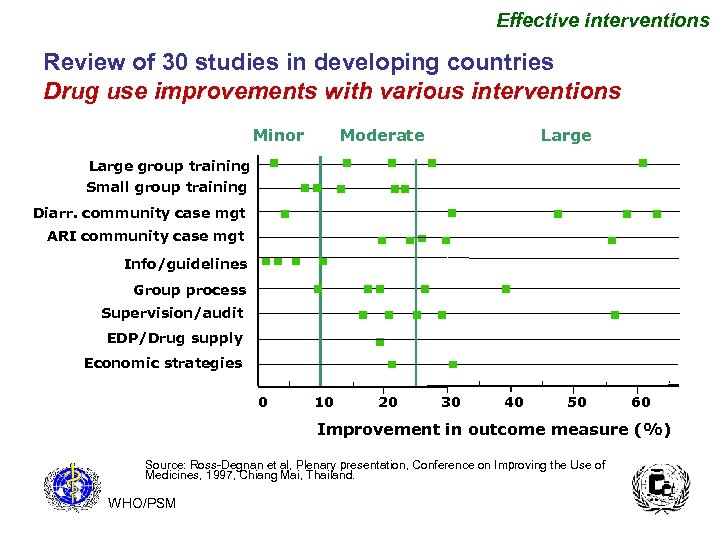
Effective interventions Review of 30 studies in developing countries Drug use improvements with various interventions Minor Moderate Large group training Small group training Diarr. community case mgt ARI community case mgt Info/guidelines Group process Supervision/audit EDP/Drug supply Economic strategies 0 10 20 30 40 50 60 Improvement in outcome measure (%) Source: Ross-Degnan et al, Plenary presentation, Conference on Improving the Use of Medicines, 1997, Chiang Mai, Thailand. WHO/PSM
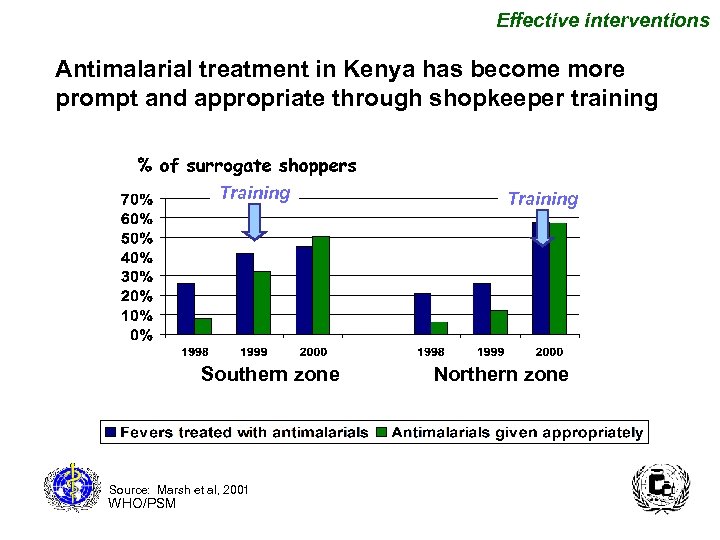
Effective interventions Antimalarial treatment in Kenya has become more prompt and appropriate through shopkeeper training Training Southern zone Source: Marsh et al, 2001 WHO/PSM Training Northern zone

Effective interventions Actions to improve use of medicines: consider effectiveness and feasibility • Recommended approaches – Standard treatment guidelines – Essential drugs list based on treatments of choice – Hospital pharmacy and therapeutics committees – Problem-based pharmacotherapy training – Problem-based in-service and continuing education • Promising approaches – Interactive group process among providers and consumers – Pharmacist and drug seller training – Consumer involvement in public education Source: Laing, Hogerzeil and Ross-Degnanl, Health Policy and Planning, 2001 WHO/PSM
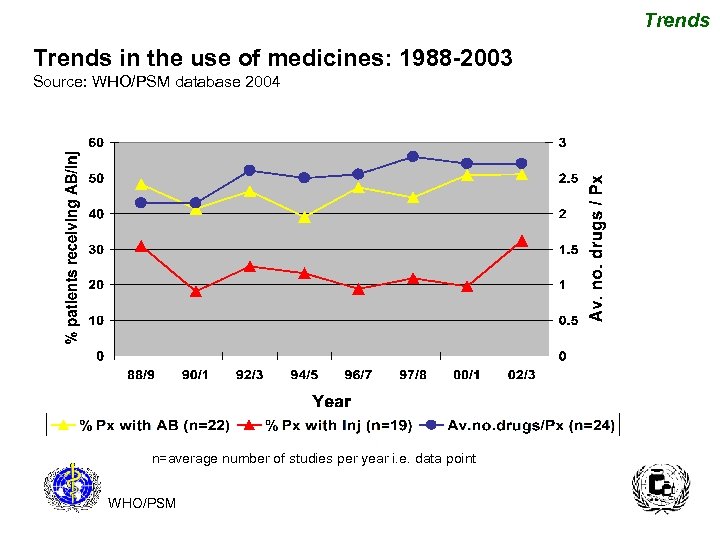
Trends in the use of medicines: 1988 -2003 Source: WHO/PSM database 2004 n=average number of studies per year i. e. data point WHO/PSM
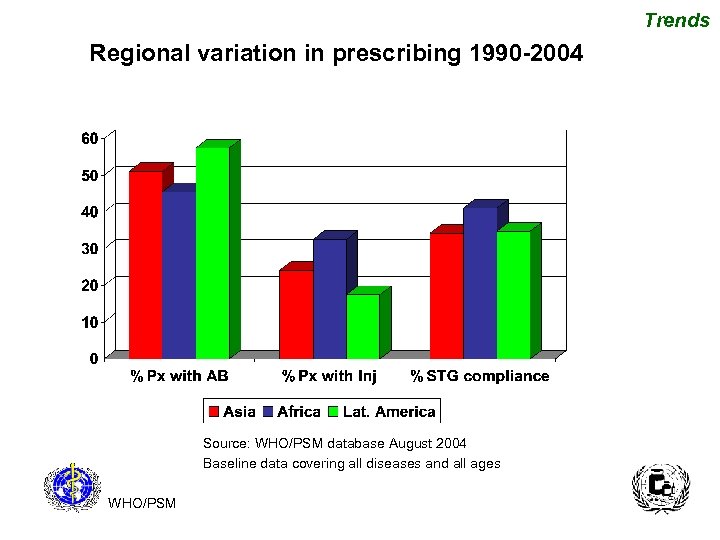
Trends Regional variation in prescribing 1990 -2004 Source: WHO/PSM database August 2004 Baseline data covering all diseases and all ages WHO/PSM
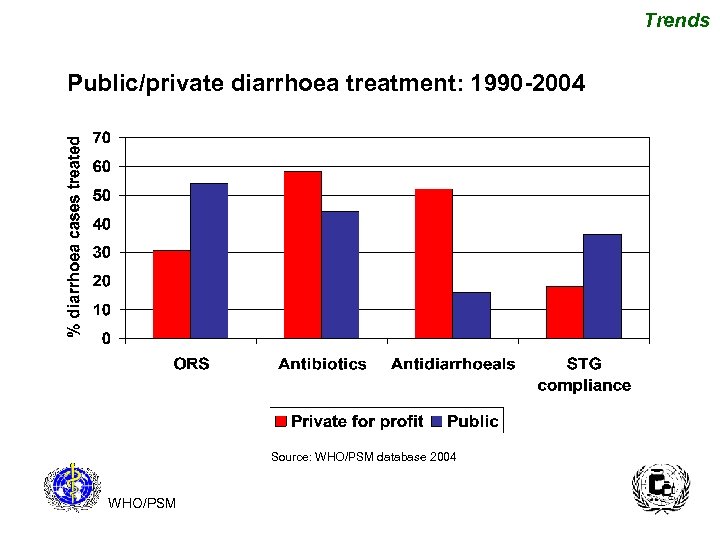
Trends Public/private diarrhoea treatment: 1990 -2004 Source: WHO/PSM database 2004 WHO/PSM
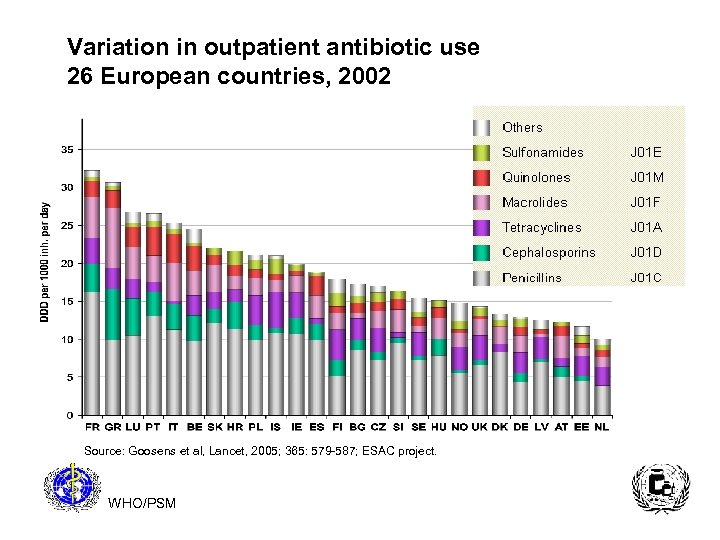
Variation in outpatient antibiotic use 26 European countries, 2002 Source: Goosens et al, Lancet, 2005; 365: 579 -587; ESAC project. WHO/PSM
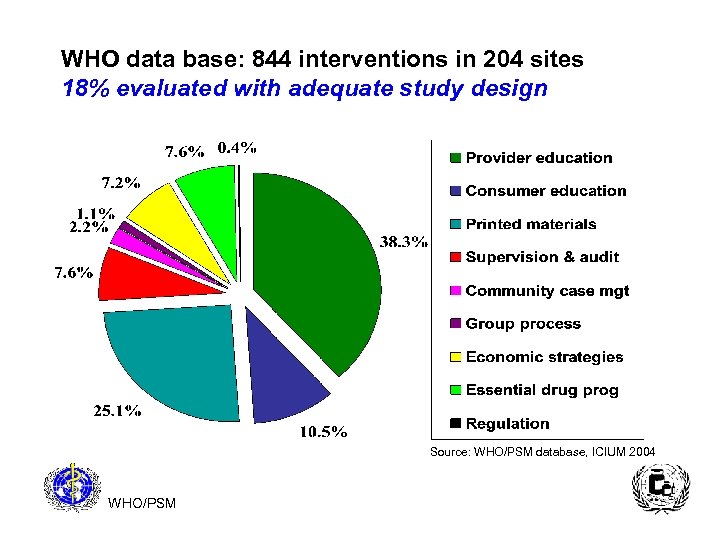
WHO data base: 844 interventions in 204 sites 18% evaluated with adequate study design Source: WHO/PSM database, ICIUM 2004 WHO/PSM

2 nd International Conference for Improving Use of Medicines http: //www. icium. org Chiang Mai, Thailand, 2004, 472 participants from 70 countries. Recommendations for countries to: • Implement national medicines programmes to improve medicines use in private and public sectors – Long term with in-built monitoring system • Scale up successful interventions – Coordinated multi-faceted rather than single interventions • Implement interventions to address community drug use – School programs, and regulation of pharmaceutical promotion WHO/PSM

AMR recommendations from ICIUM 1. Develop standard surveillance methodology for anti-microbial use and resistance, for community and hospitals 2. Develop, implement, evaluate targeted multi-component interventions, adapted to health care system and regulation 3. Focus on high priority areas to contain AMR such as – – – Infection control, surgical prophylaxis, use by drug sellers Regulatory approaches to restrict use of some antimicrobials Incentives to prescribers and consumers Inclusion of AMR in graduate curricula and CME improved quality control of laboratories for AMR surveillance 4. Develop surveillance systems and regulation to control nonhuman antimicrobial use WHO/PSM
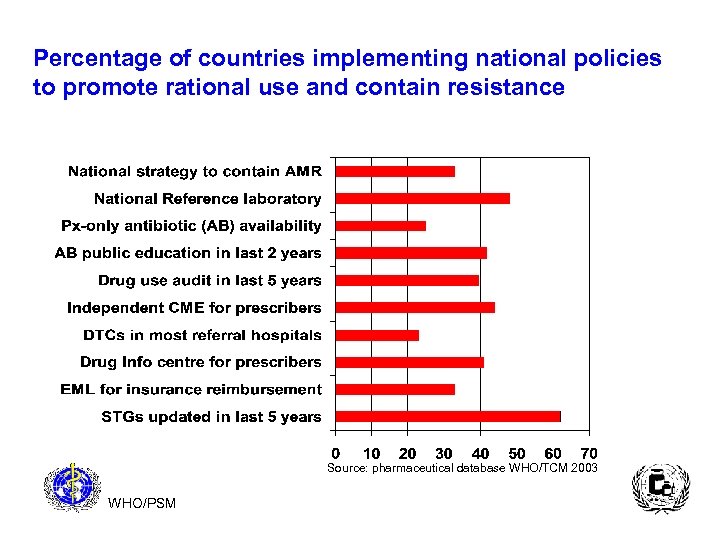
Percentage of countries implementing national policies to promote rational use and contain resistance Source: pharmaceutical database WHO/TCM 2003 WHO/PSM

What is WHO doing to promote rational use? • Advocacy for the rational use of medicines (RUM) – Essential Drug Monitor, effective drug info, meetings, ICIUM • Model Formulary process – Model List of Essential Medicines, Essential Medicines Library, WHO Model Formulary (five languages) • Training programmes - about 250 participants/year – Promoting rational use of drugs at primary health care, community levels and hospital levels (Drugs and Therapeutic Committees) • WHO Global Strategy on antimicrobial resistance – Operational research, advocacy for implementation • Intervention research to promote RUM – Identifying cost-effectiveness of interventions and policies – Database to monitor trends in use and impact of interventions WHO/PSM
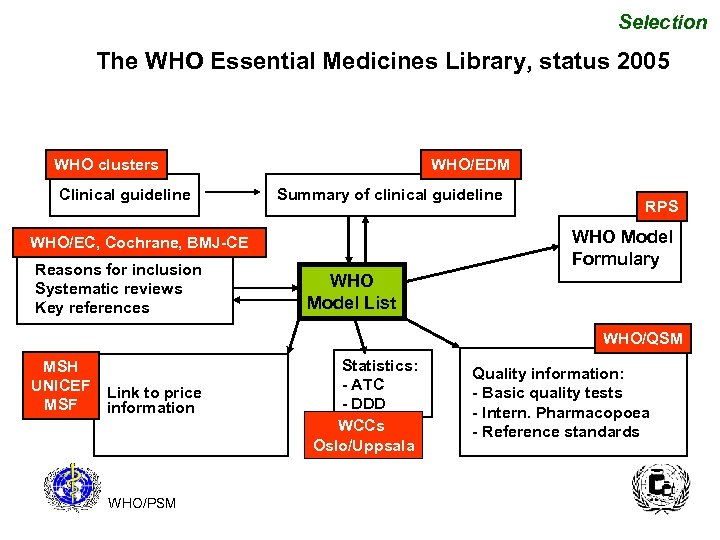
Selection The WHO Essential Medicines Library, status 2005 WHO clusters Clinical guideline WHO/EDM Summary of clinical guideline WHO Model Formulary WHO/EC, Cochrane, BMJ-CE Reasons for inclusion Systematic reviews Key references RPS WHO Model List WHO/QSM MSH UNICEF MSF Link to price information WHO/PSM Statistics: - ATC - DDD WCCs Oslo/Uppsala Quality information: - Basic quality tests - Intern. Pharmacopoea - Reference standards
WHO/PSM

Conclusions • AMR and irrational use of antimicrobials is a very serious global public health problem • Much is known about how to improve rational use of medicines but much more policy implementation is needed at the national level • Rational use could be greatly improved and resistance contained if a fraction of the resources spent on medicines were spent on improving use WHO/PSM
68f1ff1eefefae0e7639bc21509d9757.ppt