0ebdd4c6244124ec015e7592f614ae58.ppt
- Количество слайдов: 33
 Presentation to the Health Portfolio Committee Sagie Pillay CEO STRATEGY 2010 - 2015 May 5, 2010
Presentation to the Health Portfolio Committee Sagie Pillay CEO STRATEGY 2010 - 2015 May 5, 2010
 STRATEGY 2010 -2015: 1. Mission & Purpose 2. Guiding Principles: “NHLS Credo” 3. Strategic Dialogue 4. Key Strategic Issues 5. Strategic Dilemmas: “Themes” 6. Strategic Dream: “Vision” 7. Strategic Drivers: “ 10 -point Plan” 8. Strategic Deliverables: “Strategic Objectives” 5 yr 9. Strategic Deliverables: “Balanced Score-card” 1 yr 2
STRATEGY 2010 -2015: 1. Mission & Purpose 2. Guiding Principles: “NHLS Credo” 3. Strategic Dialogue 4. Key Strategic Issues 5. Strategic Dilemmas: “Themes” 6. Strategic Dream: “Vision” 7. Strategic Drivers: “ 10 -point Plan” 8. Strategic Deliverables: “Strategic Objectives” 5 yr 9. Strategic Deliverables: “Balanced Score-card” 1 yr 2
 OUR PURPOSE & MISSION To provide quality, affordable and sustainable health laboratory and related public health services, To train for health science education, and To promote and undertake health research In support of National & Provincial Departments of Health In their delivery of health care to the nation 3
OUR PURPOSE & MISSION To provide quality, affordable and sustainable health laboratory and related public health services, To train for health science education, and To promote and undertake health research In support of National & Provincial Departments of Health In their delivery of health care to the nation 3
 THE NHLS CREDO: “OUR GUIDING PRINCIPLES” Our first responsibility is to our customers whom we desire to serve with passion and commitment, and strive to provide with an effortless quality yet affordable experience We are accountable to our employees, respect their dignity employees and recognise their value. We value a disciplined organisation culture that promotes loyalty, trust, accountability and collaborative effort to mutual benefit, with employees who seek to contribute to the pursuit of NHLS’s purpose We endeavour to maintain exceptional standards and improve our offering through continuous learning and innovation appropriate to our environment We strive to contribute to and make a difference to the Communities in which we live and work, ultimately influencing the improvement in our Nation’s health 4
THE NHLS CREDO: “OUR GUIDING PRINCIPLES” Our first responsibility is to our customers whom we desire to serve with passion and commitment, and strive to provide with an effortless quality yet affordable experience We are accountable to our employees, respect their dignity employees and recognise their value. We value a disciplined organisation culture that promotes loyalty, trust, accountability and collaborative effort to mutual benefit, with employees who seek to contribute to the pursuit of NHLS’s purpose We endeavour to maintain exceptional standards and improve our offering through continuous learning and innovation appropriate to our environment We strive to contribute to and make a difference to the Communities in which we live and work, ultimately influencing the improvement in our Nation’s health 4
 STRATEGIC DIALOGUE STAKEHOLDER INPUT For the first time in NHLS history, Key Stakeholders were invited to engage in a national Strategic discussion to provide insight and guide the strategic thrust of the next 5 year period. The following documents were used to inform the strategic discussion: The Maputo Declaration on the Strengthening of Laboratory Systems, WHO, 2008 Government’s Programme of Action 2009 – Human Development Cluster: Health NDOH 10 point plan NHLS Strategy 2007 -2010 (February 2009 Review) NHLS Annual Report 2008/2009 Invitees included*: Key Customers on Service Delivery: DDG: Strategic Health Programmes, CD: Communicable Disease, CD: Non-Communicable Diseases (from National Department of Health), all 9 Provincial Heads of Health, Key Stakeholders in Research and Teaching: Department Science and Technology, all 9 Deans of University Faculties of Health Sciences, all 9 Heads of Schools of Pathology (or equivalent), Key representatives from Universities of Technology Internal Stakeholders: Chairpersons of NHLS Board and its Subcommittees, in addition to the NHLS Executive Management Team *Full list of Attendees, and their Strategic Input (in the form of Powerpoint presentations) are attached as Appendices 5
STRATEGIC DIALOGUE STAKEHOLDER INPUT For the first time in NHLS history, Key Stakeholders were invited to engage in a national Strategic discussion to provide insight and guide the strategic thrust of the next 5 year period. The following documents were used to inform the strategic discussion: The Maputo Declaration on the Strengthening of Laboratory Systems, WHO, 2008 Government’s Programme of Action 2009 – Human Development Cluster: Health NDOH 10 point plan NHLS Strategy 2007 -2010 (February 2009 Review) NHLS Annual Report 2008/2009 Invitees included*: Key Customers on Service Delivery: DDG: Strategic Health Programmes, CD: Communicable Disease, CD: Non-Communicable Diseases (from National Department of Health), all 9 Provincial Heads of Health, Key Stakeholders in Research and Teaching: Department Science and Technology, all 9 Deans of University Faculties of Health Sciences, all 9 Heads of Schools of Pathology (or equivalent), Key representatives from Universities of Technology Internal Stakeholders: Chairpersons of NHLS Board and its Subcommittees, in addition to the NHLS Executive Management Team *Full list of Attendees, and their Strategic Input (in the form of Powerpoint presentations) are attached as Appendices 5
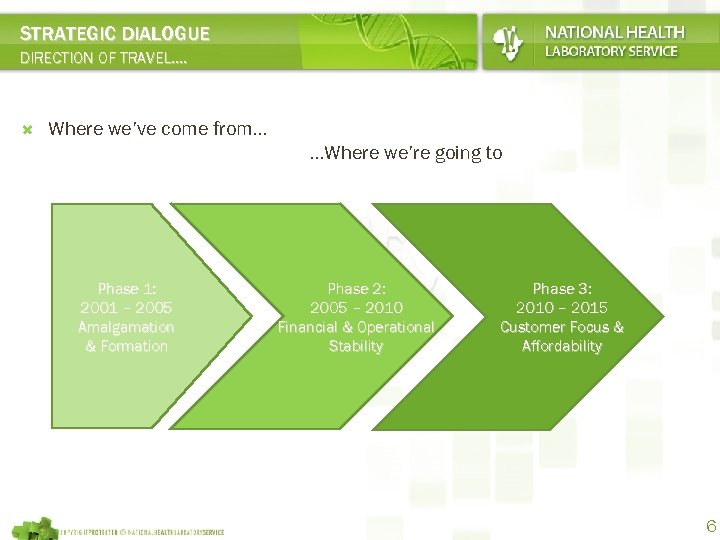 STRATEGIC DIALOGUE DIRECTION OF TRAVEL. . Where we’ve come from. . . Where we’re going to Phase 1: 2001 – 2005 Amalgamation & Formation Phase 2: 2005 – 2010 Financial & Operational Stability Phase 3: 2010 – 2015 Customer Focus & Affordability 6
STRATEGIC DIALOGUE DIRECTION OF TRAVEL. . Where we’ve come from. . . Where we’re going to Phase 1: 2001 – 2005 Amalgamation & Formation Phase 2: 2005 – 2010 Financial & Operational Stability Phase 3: 2010 – 2015 Customer Focus & Affordability 6
 STRATEGIC DIALOGUE KEY STRATEGIC ISSUES IDENTIFIED Strategic Issues related to SERVICE DELIVERY: The NHLS and the DOH need to weigh up the affordability of the current fee-for-service model, which results in invoices that exceed DOH’s budget, against the cost of accessibility of NHLS services, particularly in relation to the expectation by the DOH that laboratories be available at the most local level. The NHLS must seek clarity on who is/should be responsible for containing DOH costs through “gatekeeping” the volumes & types of tests requested in relation to the established guidelines. The NHLS must establish a costing model and correlate this to its key cost drivers, namely: Human Resources, Technology and Physical Infrastructure (whilst maintaining Quality Assurance). The NHLS must establish a funding model that will generate a meaningful tariff. The options to weigh up are the current fee-for-service model, Lump Sum estimates, Conditional Grant, or combination. Given the recent Strategic Alignment of NHLS with Government’s Programme of Action, especially the Accelerated Programme for Development, the NHLS must ensure its capacity in terms of Human Resources, Technology and Infrastructure, to respond to help address the emerging Burden of Disease. The NHLS realises that it is under-utilising its vast potential to provide Information to DOH which should assist with decision-making that informs policy and practice. The potential is currently diminished by the lack of a unique patient identifier, as well as a common IT platform within DOH , & between DOH & NHLS. The lack of an over-arching framework – such as a National Policy for Laboratory Services – to inform Guidelines (e. g. Point Of Care Testing), Quality Assurance, Training, Monitoring & Evaluation is not ideal and must be addressed. 7
STRATEGIC DIALOGUE KEY STRATEGIC ISSUES IDENTIFIED Strategic Issues related to SERVICE DELIVERY: The NHLS and the DOH need to weigh up the affordability of the current fee-for-service model, which results in invoices that exceed DOH’s budget, against the cost of accessibility of NHLS services, particularly in relation to the expectation by the DOH that laboratories be available at the most local level. The NHLS must seek clarity on who is/should be responsible for containing DOH costs through “gatekeeping” the volumes & types of tests requested in relation to the established guidelines. The NHLS must establish a costing model and correlate this to its key cost drivers, namely: Human Resources, Technology and Physical Infrastructure (whilst maintaining Quality Assurance). The NHLS must establish a funding model that will generate a meaningful tariff. The options to weigh up are the current fee-for-service model, Lump Sum estimates, Conditional Grant, or combination. Given the recent Strategic Alignment of NHLS with Government’s Programme of Action, especially the Accelerated Programme for Development, the NHLS must ensure its capacity in terms of Human Resources, Technology and Infrastructure, to respond to help address the emerging Burden of Disease. The NHLS realises that it is under-utilising its vast potential to provide Information to DOH which should assist with decision-making that informs policy and practice. The potential is currently diminished by the lack of a unique patient identifier, as well as a common IT platform within DOH , & between DOH & NHLS. The lack of an over-arching framework – such as a National Policy for Laboratory Services – to inform Guidelines (e. g. Point Of Care Testing), Quality Assurance, Training, Monitoring & Evaluation is not ideal and must be addressed. 7
 STRATEGIC DIALOGUE KEY STRATEGIC ISSUES IDENTIFIED Strategic Issues related to OPERATIONAL PROCESSES: PROCESSES Skills shortages and the inequitable geographic distribution of talent is a major challenge. In fact the NHLS has an absolute shortage in four key professional groupings which demand long lead times to fill. The NHLS should consider the option of training mid-level laboratory workers to fill the gap. The NHLS must investigate the cost-benefit of in-sourcing key Auxillary Services which have a massive impact on service delivery - e. g. Transport & Logistics, and Health Care Waste Removal – against the current option of outsourcing alone. The NHLS must drive Standardisation of Technology to reduce cost and wastage, and improve quality. Customer-related concerns such as the following must be addressed: 1. Turn Around Time (TAT) issues such as the inability to measure & account for Total TAT, as well as key priorities e. g. TB Culture 2. The DOH’s need to eliminate duplicate test requests 3. Interpretation Issues w. r. t. Billing, Programme Data and Customer Satisfaction Survey results : confusion with regards to non-coterminous boundaries between NHLS Branches and Provinces, and between Business Units and Districts 3. Training required on Thusano and www. Disa 4. Training required on clinical specimen collection (e. g. dry spot collection) and request form completion) 5. Poor Communication between Stakeholders contributes to unmet expectations. 6. Space requirements of NHLS that are not met by DOH compromise the ability to get the job done, and to meet expectations. 7. The NHLS should consider Task-shifting, such as Phlebotomists at high volume hospital The NHLS has major Cash Flow challenges due to significant outstanding debtors. The users’ poor awareness of NHLS, lack of single identity and poor customer perceptions does not bode well for the organisation. Poor Staff morale and entropic organisational culture compromise stability and skills retention. 7
STRATEGIC DIALOGUE KEY STRATEGIC ISSUES IDENTIFIED Strategic Issues related to OPERATIONAL PROCESSES: PROCESSES Skills shortages and the inequitable geographic distribution of talent is a major challenge. In fact the NHLS has an absolute shortage in four key professional groupings which demand long lead times to fill. The NHLS should consider the option of training mid-level laboratory workers to fill the gap. The NHLS must investigate the cost-benefit of in-sourcing key Auxillary Services which have a massive impact on service delivery - e. g. Transport & Logistics, and Health Care Waste Removal – against the current option of outsourcing alone. The NHLS must drive Standardisation of Technology to reduce cost and wastage, and improve quality. Customer-related concerns such as the following must be addressed: 1. Turn Around Time (TAT) issues such as the inability to measure & account for Total TAT, as well as key priorities e. g. TB Culture 2. The DOH’s need to eliminate duplicate test requests 3. Interpretation Issues w. r. t. Billing, Programme Data and Customer Satisfaction Survey results : confusion with regards to non-coterminous boundaries between NHLS Branches and Provinces, and between Business Units and Districts 3. Training required on Thusano and www. Disa 4. Training required on clinical specimen collection (e. g. dry spot collection) and request form completion) 5. Poor Communication between Stakeholders contributes to unmet expectations. 6. Space requirements of NHLS that are not met by DOH compromise the ability to get the job done, and to meet expectations. 7. The NHLS should consider Task-shifting, such as Phlebotomists at high volume hospital The NHLS has major Cash Flow challenges due to significant outstanding debtors. The users’ poor awareness of NHLS, lack of single identity and poor customer perceptions does not bode well for the organisation. Poor Staff morale and entropic organisational culture compromise stability and skills retention. 7
 STRATEGIC DIALOGUE KEY ISSUES IDENTIFIED Strategic Issues related to RESEARCH & DEVELOPMENT: DEVELOPMENT This was a previously under-emphasised mandate within NHLS, whereas it is a Cabinet imperative, which has resulted in a missed opportunity for synergy around a National perspective vs. individual University perspectives alone. This must be rectified. Under-collaboration with the Department of Science and Technology has been a missed potential opportunity. The Funding Model for research, which currently entails cross-subsidisation from Service Income and externally-funded Grants, must be interrogated. NHLS needs to even consider shifting to a Conditional Grant model or investigate other alternatives. Currently research is an “unfunded mandate” with the resultant impact being poor retention ability of talented & skilled researchers. The challenge between alignment with National Research Priorities against funder interests & expectations, and even against individual researcher interests, may limit opportunity for “leap-frog” innovation if the NHLS introduces a complete limitation on “blue-sky” research. Research should be translational i. e. lead to and/or impact changes to policy and practice. The footprints of the National Institutes for Communicable Diseases and Occupational Health (NICD & NIOH) are too localised, and the NHLS must aim towards extending these nationally. 8
STRATEGIC DIALOGUE KEY ISSUES IDENTIFIED Strategic Issues related to RESEARCH & DEVELOPMENT: DEVELOPMENT This was a previously under-emphasised mandate within NHLS, whereas it is a Cabinet imperative, which has resulted in a missed opportunity for synergy around a National perspective vs. individual University perspectives alone. This must be rectified. Under-collaboration with the Department of Science and Technology has been a missed potential opportunity. The Funding Model for research, which currently entails cross-subsidisation from Service Income and externally-funded Grants, must be interrogated. NHLS needs to even consider shifting to a Conditional Grant model or investigate other alternatives. Currently research is an “unfunded mandate” with the resultant impact being poor retention ability of talented & skilled researchers. The challenge between alignment with National Research Priorities against funder interests & expectations, and even against individual researcher interests, may limit opportunity for “leap-frog” innovation if the NHLS introduces a complete limitation on “blue-sky” research. Research should be translational i. e. lead to and/or impact changes to policy and practice. The footprints of the National Institutes for Communicable Diseases and Occupational Health (NICD & NIOH) are too localised, and the NHLS must aim towards extending these nationally. 8
 STRATEGIC DIALOGUE KEY ISSUES IDENTIFIED Strategic Issues related to TEACHING & HUMAN RESOURCE PIPELINE: PIPELINE Unlike the DOH, the NHLS does not have a 10 -year Human Resource Plan for its Core Professionals of Pathologists, Scientists, Medical Technologists and Technicians. The NHLS is not fully leveraging its relationships with Universities & the Universities of Technology to ensure the sustainability of laboratory services. The NHLS must recognise that the role of academic institutions is far greater than merely teaching & research; it includes Academic Leadership to optimise technology. Recruitment for the four core professionals is very difficult. The failure rates of Medical Technologists is concerning; especially with reduced capacity in NHLS to supervise students. With the reduction in applications into Clinical Pathology as a discipline, academic institutions are questioning the profitability of providing this specialisation. The NHLS must consider the potential implications should universities decide to cease teaching Clinical Pathology. The NHLS should consider playing a greater role in undergraduate teaching, thereby also improving current diluted exposure & education in pathology. In addition, the NHLS needs to clarify its teaching role at the Universities of Technology. There are opportunities for partnering with academic institutions to extend teaching into Africa. There is a challenge with finding the balance for professional workforce between service : teaching : research Opportunities for New Professionals exist, e. g. BTech; but experience with conversion courses is problematic. The current Funding model – which entails Cross-subsidisation from Service Income – needs to be interrogated and perhaps even consider shifting to a Conditional Grant or other alternatives. 9
STRATEGIC DIALOGUE KEY ISSUES IDENTIFIED Strategic Issues related to TEACHING & HUMAN RESOURCE PIPELINE: PIPELINE Unlike the DOH, the NHLS does not have a 10 -year Human Resource Plan for its Core Professionals of Pathologists, Scientists, Medical Technologists and Technicians. The NHLS is not fully leveraging its relationships with Universities & the Universities of Technology to ensure the sustainability of laboratory services. The NHLS must recognise that the role of academic institutions is far greater than merely teaching & research; it includes Academic Leadership to optimise technology. Recruitment for the four core professionals is very difficult. The failure rates of Medical Technologists is concerning; especially with reduced capacity in NHLS to supervise students. With the reduction in applications into Clinical Pathology as a discipline, academic institutions are questioning the profitability of providing this specialisation. The NHLS must consider the potential implications should universities decide to cease teaching Clinical Pathology. The NHLS should consider playing a greater role in undergraduate teaching, thereby also improving current diluted exposure & education in pathology. In addition, the NHLS needs to clarify its teaching role at the Universities of Technology. There are opportunities for partnering with academic institutions to extend teaching into Africa. There is a challenge with finding the balance for professional workforce between service : teaching : research Opportunities for New Professionals exist, e. g. BTech; but experience with conversion courses is problematic. The current Funding model – which entails Cross-subsidisation from Service Income – needs to be interrogated and perhaps even consider shifting to a Conditional Grant or other alternatives. 9
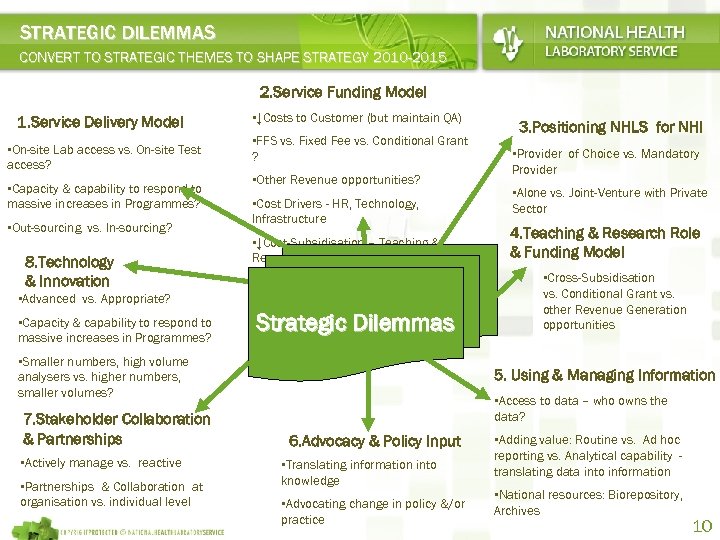 STRATEGIC DILEMMAS CONVERT TO STRATEGIC THEMES TO SHAPE STRATEGY 2010 -2015 2. Service Funding Model 1. Service Delivery Model • On-site Lab access vs. On-site Test access? • Capacity & capability to respond to massive increases in Programmes? • Out-sourcing vs. In-sourcing? 8. Technology & Innovation • ↓Costs to Customer (but maintain QA) • FFS vs. Fixed Fee vs. Conditional Grant ? • Other Revenue opportunities? • Cost Drivers - HR, Technology, Infrastructure • ↓Cost-Subsidisation – Teaching & Research • Advanced vs. Appropriate? • Capacity & capability to respond to massive increases in Programmes? Strategic Dilemmas • Smaller numbers, high volume analysers vs. higher numbers, smaller volumes? 7. Stakeholder Collaboration & Partnerships • Actively manage vs. reactive • Partnerships & Collaboration at organisation vs. individual level 3. Positioning NHLS for NHI • Provider of Choice vs. Mandatory Provider • Alone vs. Joint-Venture with Private Sector 4. Teaching & Research Role & Funding Model • Cross-Subsidisation vs. Conditional Grant vs. other Revenue Generation opportunities 5. Using & Managing Information • Access to data – who owns the data? 6. Advocacy & Policy Input • Translating information into knowledge • Advocating change in policy &/or practice • Adding value: Routine vs. Ad hoc reporting vs. Analytical capability translating data into information • National resources: Biorepository, Archives 10
STRATEGIC DILEMMAS CONVERT TO STRATEGIC THEMES TO SHAPE STRATEGY 2010 -2015 2. Service Funding Model 1. Service Delivery Model • On-site Lab access vs. On-site Test access? • Capacity & capability to respond to massive increases in Programmes? • Out-sourcing vs. In-sourcing? 8. Technology & Innovation • ↓Costs to Customer (but maintain QA) • FFS vs. Fixed Fee vs. Conditional Grant ? • Other Revenue opportunities? • Cost Drivers - HR, Technology, Infrastructure • ↓Cost-Subsidisation – Teaching & Research • Advanced vs. Appropriate? • Capacity & capability to respond to massive increases in Programmes? Strategic Dilemmas • Smaller numbers, high volume analysers vs. higher numbers, smaller volumes? 7. Stakeholder Collaboration & Partnerships • Actively manage vs. reactive • Partnerships & Collaboration at organisation vs. individual level 3. Positioning NHLS for NHI • Provider of Choice vs. Mandatory Provider • Alone vs. Joint-Venture with Private Sector 4. Teaching & Research Role & Funding Model • Cross-Subsidisation vs. Conditional Grant vs. other Revenue Generation opportunities 5. Using & Managing Information • Access to data – who owns the data? 6. Advocacy & Policy Input • Translating information into knowledge • Advocating change in policy &/or practice • Adding value: Routine vs. Ad hoc reporting vs. Analytical capability translating data into information • National resources: Biorepository, Archives 10
 STRATEGIC DILEMMAS FOR THE NHLS 1. SERVICE DELIVERY MODEL Current Service Delivery Model: Extended “footprint” of numerous physical laboratories country-wide close to periphery However, challenges are: Potentially inefficient test repertoires Costly to run Difficult to staff with Skills shortage Difficult to upscale capacity rapidly Potential options for the service delivery model Large capacity laboratories with less diverse “footprint”, equipped with bulk analysers and ramped-up logistics to ensure acceptable TAT standards Hybrid model as a combination of smaller “footprint” and Point-of-Care-Testing (POCT) However: Is a hybrid model that involves POCT sites which are not managed by a nurse, but by a travelling lab technologist in areas where there is no high throughput possible and financially feasible? Should the role of the NHLS, NICD particularly, be expanded beyond surveillance alone to that of support to all DOH services? 11
STRATEGIC DILEMMAS FOR THE NHLS 1. SERVICE DELIVERY MODEL Current Service Delivery Model: Extended “footprint” of numerous physical laboratories country-wide close to periphery However, challenges are: Potentially inefficient test repertoires Costly to run Difficult to staff with Skills shortage Difficult to upscale capacity rapidly Potential options for the service delivery model Large capacity laboratories with less diverse “footprint”, equipped with bulk analysers and ramped-up logistics to ensure acceptable TAT standards Hybrid model as a combination of smaller “footprint” and Point-of-Care-Testing (POCT) However: Is a hybrid model that involves POCT sites which are not managed by a nurse, but by a travelling lab technologist in areas where there is no high throughput possible and financially feasible? Should the role of the NHLS, NICD particularly, be expanded beyond surveillance alone to that of support to all DOH services? 11
 STRATEGIC DILEMMAS FOR THE NHLS 2. SERVICE FUNDING MODEL Current Service Funding Model: Fee-for-Service with Cross-subsidisation of Teaching & Research Mandates However, challenges are: Unaffordable for Provinces Does not encourage Efficiency and Waste reduction (for customer or NHLS) NHLS should investigate and pursue alternative Funding model options such as: Conditional grant funding for Research & Teaching + FFS without cross-subsidisation Fixed Costs, trading volume for margin Increasing surveillance grants Other revenue generation opportunities Key Cost Drivers are Human Resources, Technology, Infrastructure Explore the modification of Service grant reporting to reflect Income vs. Outputs The NHLS must convince the DOH about the additional value that it provides for the cost of “lab services” 12
STRATEGIC DILEMMAS FOR THE NHLS 2. SERVICE FUNDING MODEL Current Service Funding Model: Fee-for-Service with Cross-subsidisation of Teaching & Research Mandates However, challenges are: Unaffordable for Provinces Does not encourage Efficiency and Waste reduction (for customer or NHLS) NHLS should investigate and pursue alternative Funding model options such as: Conditional grant funding for Research & Teaching + FFS without cross-subsidisation Fixed Costs, trading volume for margin Increasing surveillance grants Other revenue generation opportunities Key Cost Drivers are Human Resources, Technology, Infrastructure Explore the modification of Service grant reporting to reflect Income vs. Outputs The NHLS must convince the DOH about the additional value that it provides for the cost of “lab services” 12
 STRATEGIC DILEMMAS FOR THE NHLS 3. POSITIONING FOR NHI The NHLS must maintain competitiveness in an NHI environment Price will be an issue – particularly in a climate where new entrants could partner with Indian companies. Thus NHLS should: Explore Optimising partnerships for logistics to bring down costs Explore Partnering with new entrants through a JV system Leverage on current standing - as service provider (with extended test repertoire), training next generation and conducting research. Improve billing, systems, etc, as this will be even more pertinent than currently. Improve & upscale skills and technical capacity Remain alert to the potential risks (losing public sector work) vs. potential return (gaining additional private sector work) Worst case scenario: The NHLS will have to BID to be the preferred provider – the NHLS Act is unlikely to be “protective”. The NHLS must get involved on technical committee to be set up by the Minister to understand influence policy formulation. 13
STRATEGIC DILEMMAS FOR THE NHLS 3. POSITIONING FOR NHI The NHLS must maintain competitiveness in an NHI environment Price will be an issue – particularly in a climate where new entrants could partner with Indian companies. Thus NHLS should: Explore Optimising partnerships for logistics to bring down costs Explore Partnering with new entrants through a JV system Leverage on current standing - as service provider (with extended test repertoire), training next generation and conducting research. Improve billing, systems, etc, as this will be even more pertinent than currently. Improve & upscale skills and technical capacity Remain alert to the potential risks (losing public sector work) vs. potential return (gaining additional private sector work) Worst case scenario: The NHLS will have to BID to be the preferred provider – the NHLS Act is unlikely to be “protective”. The NHLS must get involved on technical committee to be set up by the Minister to understand influence policy formulation. 13
 STRATEGIC DILEMMAS FOR THE NHLS 4. MODEL FOR TEACHING AND RESEARCH Current Teaching & Research Funding Model: Cross-subsidisation of Teaching & Research Mandates from Fee-for-Service Tariffs NHLS should investigate and pursue alternative Funding model options for its Teaching Mandate Note: NHLS not registered as a higher education institution. NHLS must gain understanding of the implications of a Conditional Grant vs. Fee-for-service on: budgeting the NHLS’ ability to deliver on the mandates of training and research sustainably ability to attract and retain cutting edge talent Risk with Conditional Grant: NHLS could eventually viewed as merely “a laboratory service” from which to cherry-pick, and lose the ability to attract core professionals, such as Pathologists and Medical technologists to be the best in the world. Important to keep the currently structured NHLS intact – such as the HPA model. The NHLS should: Explore internal mechanism to create teaching platform budgeting mechanism. In reporting, reflect ‘service’ provided by NICD & NIOH against grant by NDo. H. Explore additional grant / bridging finance for research to ensure continuity of research/ innovation and fulltime employment of scientists beyond the lifespan of funded Grant. Leverage convening power of NHLS to engage with other agencies/departments. 14
STRATEGIC DILEMMAS FOR THE NHLS 4. MODEL FOR TEACHING AND RESEARCH Current Teaching & Research Funding Model: Cross-subsidisation of Teaching & Research Mandates from Fee-for-Service Tariffs NHLS should investigate and pursue alternative Funding model options for its Teaching Mandate Note: NHLS not registered as a higher education institution. NHLS must gain understanding of the implications of a Conditional Grant vs. Fee-for-service on: budgeting the NHLS’ ability to deliver on the mandates of training and research sustainably ability to attract and retain cutting edge talent Risk with Conditional Grant: NHLS could eventually viewed as merely “a laboratory service” from which to cherry-pick, and lose the ability to attract core professionals, such as Pathologists and Medical technologists to be the best in the world. Important to keep the currently structured NHLS intact – such as the HPA model. The NHLS should: Explore internal mechanism to create teaching platform budgeting mechanism. In reporting, reflect ‘service’ provided by NICD & NIOH against grant by NDo. H. Explore additional grant / bridging finance for research to ensure continuity of research/ innovation and fulltime employment of scientists beyond the lifespan of funded Grant. Leverage convening power of NHLS to engage with other agencies/departments. 14
 STRATEGIC DILEMMAS FOR THE NHLS 5. USING & MANAGING INFORMATION The NHLS must provide Enabling Health Information The NHLS must develop and expand the immense value of the extensive Health data (for which its acts as Custodian) into useful Information, through: Developing Stakeholder Accessibility to NHLS Information Systems Thereby enabling improved Monitoring & Evaluation of passive surveillance programs & NCR Improving Stakeholder Information Accessibility to Active Surveillance Programs Improving Stakeholder Information Accessibility to utilisation trends to enable effective management 15
STRATEGIC DILEMMAS FOR THE NHLS 5. USING & MANAGING INFORMATION The NHLS must provide Enabling Health Information The NHLS must develop and expand the immense value of the extensive Health data (for which its acts as Custodian) into useful Information, through: Developing Stakeholder Accessibility to NHLS Information Systems Thereby enabling improved Monitoring & Evaluation of passive surveillance programs & NCR Improving Stakeholder Information Accessibility to Active Surveillance Programs Improving Stakeholder Information Accessibility to utilisation trends to enable effective management 15
 STRATEGIC DILEMMAS FOR THE NHLS 6. ADVOCACY & POLICY FORMULATION Key value-add of NHLS: Translating information into knowledge (adding expert analysis and interpretation) NHLS needs to take this step further: Advocating change in policy &/or practice Key Policy initiatives to engage in and drive: 1. National Laboratory Policy • 2. Point Of Care (POC) Testing • • 3. NHLS to take lead in driving this crucial process Requires extensive discussion and investigation Clarity required as to interpretation of POCT (5000 clinics or 265 labs? ). NHLS should conduct internal analysis to determine feasibility and value-add to health delivery of POCT; however, POC is not an alternative to a centralised service. Also important to investigate consequences of POCT on teaching and research NHLS must take the lead in informing policy around the issue of POCT. NHLS must deal with misperceptions around POC. Current reality: International agencies are pushing POCT and the Department of Science and Technology (DST) is informing NDOH that it can work. Should NHLS disagree , must be able to show empirical evidence that POCT not viable option. Gate-keeping / monitoring use of tests § § Should the NHLS be the “gate-keeper” for the Do. H in terms of declining test requests to limit over-utilisation or over-servicing? Or should NHLS rather provide protocols and formularies, as well as provide management information to empower hospitals to deal with “guilty doctors” who over-utilise. 16
STRATEGIC DILEMMAS FOR THE NHLS 6. ADVOCACY & POLICY FORMULATION Key value-add of NHLS: Translating information into knowledge (adding expert analysis and interpretation) NHLS needs to take this step further: Advocating change in policy &/or practice Key Policy initiatives to engage in and drive: 1. National Laboratory Policy • 2. Point Of Care (POC) Testing • • 3. NHLS to take lead in driving this crucial process Requires extensive discussion and investigation Clarity required as to interpretation of POCT (5000 clinics or 265 labs? ). NHLS should conduct internal analysis to determine feasibility and value-add to health delivery of POCT; however, POC is not an alternative to a centralised service. Also important to investigate consequences of POCT on teaching and research NHLS must take the lead in informing policy around the issue of POCT. NHLS must deal with misperceptions around POC. Current reality: International agencies are pushing POCT and the Department of Science and Technology (DST) is informing NDOH that it can work. Should NHLS disagree , must be able to show empirical evidence that POCT not viable option. Gate-keeping / monitoring use of tests § § Should the NHLS be the “gate-keeper” for the Do. H in terms of declining test requests to limit over-utilisation or over-servicing? Or should NHLS rather provide protocols and formularies, as well as provide management information to empower hospitals to deal with “guilty doctors” who over-utilise. 16
 STRATEGIC DILEMMAS FOR THE NHLS 7. STAKEHOLDER MANAGEMENT & PARTNERSHIPS Given that there are many more stakeholders in health than NDOH, the NHLS should endevour to ensure synergy of efforts and elimination of duplication & overlap in funding and service & research efforts NHLS therefore needs to engage the following stakeholders: Public Sector: DST, DTI, DOE, DOL, DPSA, Dept Public Enterprises, Treasury Private Sector: other Pathology providers, suppliers, logistics & supply chain management International: WHO, ILO, etc The NHLS must actively manage vs. reactively respond to these stakeholder relationships, given that NHLS has significant convening power. NHLS must ensure that partnerships and collaboration occurs at an organisational vs. individual level, so as to live beyond the individual. Every overseas visit should be seen as networking and exploratory collaborative opportunity 17
STRATEGIC DILEMMAS FOR THE NHLS 7. STAKEHOLDER MANAGEMENT & PARTNERSHIPS Given that there are many more stakeholders in health than NDOH, the NHLS should endevour to ensure synergy of efforts and elimination of duplication & overlap in funding and service & research efforts NHLS therefore needs to engage the following stakeholders: Public Sector: DST, DTI, DOE, DOL, DPSA, Dept Public Enterprises, Treasury Private Sector: other Pathology providers, suppliers, logistics & supply chain management International: WHO, ILO, etc The NHLS must actively manage vs. reactively respond to these stakeholder relationships, given that NHLS has significant convening power. NHLS must ensure that partnerships and collaboration occurs at an organisational vs. individual level, so as to live beyond the individual. Every overseas visit should be seen as networking and exploratory collaborative opportunity 17
 STRATEGIC DILEMMAS FOR THE NHLS 8. TECHNOLOGY & INNOVATION NHLS must ensure Technology is appropriate yet innovative The NHLS must find the balance between acquiring and utilising highly Advanced “cutting-edge” technology” vs. technology appropriate to resource-limited settings NHLS must balance the needs and the consequences of affordability vs. future opportunity and possible “leap-frog” innovation created through “cutting-edge” research and retention of committed skilled professionals The NHLS must ensure technological capacity & capability to respond to massive and rapid upscaling in Priority Health Programmes, as well as consequent large and rapid downscaling with policy changes NHLS must ensure technology is appropriate to the Service Delivery Framework, Platform and Model, such as: Smaller numbers of high volume analysers for extended “footprint” of tests vs. larger numbers of small volume analysers for extended “footprint” of labs NHLS must explore other Innovative ways to deliver Laboratory services in resourcelimited settings, and in in remote settings. 18
STRATEGIC DILEMMAS FOR THE NHLS 8. TECHNOLOGY & INNOVATION NHLS must ensure Technology is appropriate yet innovative The NHLS must find the balance between acquiring and utilising highly Advanced “cutting-edge” technology” vs. technology appropriate to resource-limited settings NHLS must balance the needs and the consequences of affordability vs. future opportunity and possible “leap-frog” innovation created through “cutting-edge” research and retention of committed skilled professionals The NHLS must ensure technological capacity & capability to respond to massive and rapid upscaling in Priority Health Programmes, as well as consequent large and rapid downscaling with policy changes NHLS must ensure technology is appropriate to the Service Delivery Framework, Platform and Model, such as: Smaller numbers of high volume analysers for extended “footprint” of tests vs. larger numbers of small volume analysers for extended “footprint” of labs NHLS must explore other Innovative ways to deliver Laboratory services in resourcelimited settings, and in in remote settings. 18
 5 -YEAR STRATEGIC DREAM THE DESTINATION… 2015 The NHLS will be: “Household” name in health – with a SINGLE identity Laboratory services provider of choice African leader in laboratory services Provider of Quality and cost-efficient services through Lab standardisation The provider of WHO African surveillance Primary reference point for promoting worker health sub-Saharan Africa SA health information powerhouse A key player in Health Policy formulation Top employer of real talent – Laboratory services “employer of choice” Protector of our environment through Resource and Energy efficiency 19
5 -YEAR STRATEGIC DREAM THE DESTINATION… 2015 The NHLS will be: “Household” name in health – with a SINGLE identity Laboratory services provider of choice African leader in laboratory services Provider of Quality and cost-efficient services through Lab standardisation The provider of WHO African surveillance Primary reference point for promoting worker health sub-Saharan Africa SA health information powerhouse A key player in Health Policy formulation Top employer of real talent – Laboratory services “employer of choice” Protector of our environment through Resource and Energy efficiency 19
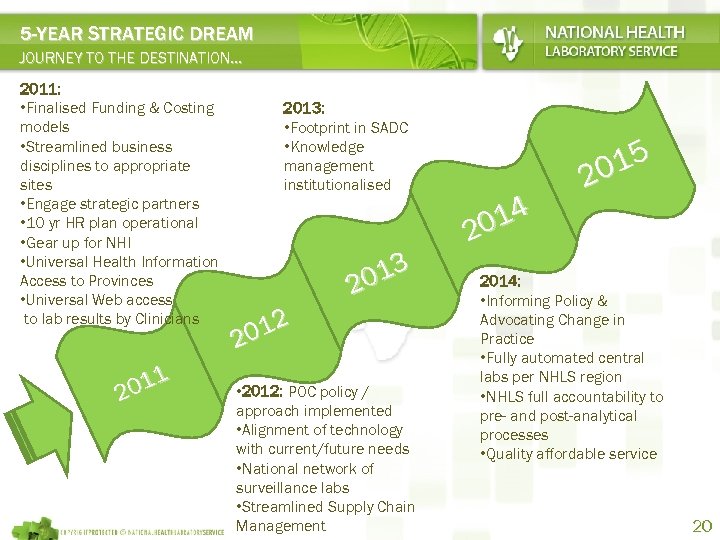 5 -YEAR STRATEGIC DREAM JOURNEY TO THE DESTINATION… 2011: • Finalised Funding & Costing models • Streamlined business disciplines to appropriate sites • Engage strategic partners • 10 yr HR plan operational • Gear up for NHI • Universal Health Information Access to Provinces • Universal Web access to lab results by Clinicians 011 2 2013: • Footprint in SADC • Knowledge management institutionalised 13 20 012 2 • 2012: POC policy / approach implemented • Alignment of technology with current/future needs • National network of surveillance labs • Streamlined Supply Chain Management 14 20 15 20 2014: • Informing Policy & Advocating Change in Practice • Fully automated central labs per NHLS region • NHLS full accountability to pre- and post-analytical processes • Quality affordable service 20
5 -YEAR STRATEGIC DREAM JOURNEY TO THE DESTINATION… 2011: • Finalised Funding & Costing models • Streamlined business disciplines to appropriate sites • Engage strategic partners • 10 yr HR plan operational • Gear up for NHI • Universal Health Information Access to Provinces • Universal Web access to lab results by Clinicians 011 2 2013: • Footprint in SADC • Knowledge management institutionalised 13 20 012 2 • 2012: POC policy / approach implemented • Alignment of technology with current/future needs • National network of surveillance labs • Streamlined Supply Chain Management 14 20 15 20 2014: • Informing Policy & Advocating Change in Practice • Fully automated central labs per NHLS region • NHLS full accountability to pre- and post-analytical processes • Quality affordable service 20
 5 -YEAR STRATEGIC DRIVERS 10 -POINT PLAN 1. Deliver affordable service to Public Sector d) Find alternative Funding models for Research & Teaching Determine Transparent pricing model Ensure guaranteed Funding for Surveillance Services – NICD + NIOH Explore other Revenue-generating opportunities a) Implement the 10 -year Human Resource Pipeline Plan a) b) c) 2. 3. 4. NDOH Point 2. 7 Accelerate implementation of HIV/AIDS & Determine “best-fit” Service Delivery Model STI’s, & increase focus on TB STI’s, a) Ensure Capability & Capacity to rapidly upscale for Health Priority programmes – HIV/AIDS, STI’s, TB b) Choose and implement On-site Laboratory Access (with tiered laboratory model) vs. on-site Test Access (with tiered test repertoire supported by massive logistics platform) c) Determine Point-of-Care Testing Policy and Implementation d) Determine most appropriate standardised technology – automated, centralised vs. decentralised e) Fulfill Statutory Functions – NIOH, NICD, NCR, expanded to include Forensic Toxicology Deliver Quality, Customer-focused Service NDOH Point 2. 3 Improving Quality of Health Services a) Improve Customer perceptions of service delivery to the bench-mark score of 75% b) Ensure retention of international quality standards to ISO 15189 Accredit ALL reference, academic and regional labs with SANAS Develop and maintain internal accreditation system for peripheral labs in line with ISO 15189 Expand accredited EQA programmes throughout Africa NDOH Point 2. 6 Revitalisation Align Resources, Support Services & Infrastructural Development for Service Delivery of Infrastructure b) c) d) Implement the 10 -year Infrastructural Plan Enhance Supply Chain Management Align ICT systems to optimise service delivery Rollout LIS country-wide Develop and utilise Health Technology Assessment Unit Become Laboratory Services “Employer of Choice” vs. “Employer of last resort” a) Recruit & retain key talent – both in core professional groups, as well as support services b) Strengthen leadership & management capacity – implement NHLS Leadership Academy c) Drive disciplined, accountable, collaborative, purpose-filled Organisational Culture e) 5. Partner with Academic Institutions to align teaching and training of core professionals for fulfilment of planned pipeline Investigate mid-level workers NDOH Point 2. 5 Improved HR Planning, Devt and Management NDOH Point 2. 4 Overhauling Health Care System & Improve its Management 21
5 -YEAR STRATEGIC DRIVERS 10 -POINT PLAN 1. Deliver affordable service to Public Sector d) Find alternative Funding models for Research & Teaching Determine Transparent pricing model Ensure guaranteed Funding for Surveillance Services – NICD + NIOH Explore other Revenue-generating opportunities a) Implement the 10 -year Human Resource Pipeline Plan a) b) c) 2. 3. 4. NDOH Point 2. 7 Accelerate implementation of HIV/AIDS & Determine “best-fit” Service Delivery Model STI’s, & increase focus on TB STI’s, a) Ensure Capability & Capacity to rapidly upscale for Health Priority programmes – HIV/AIDS, STI’s, TB b) Choose and implement On-site Laboratory Access (with tiered laboratory model) vs. on-site Test Access (with tiered test repertoire supported by massive logistics platform) c) Determine Point-of-Care Testing Policy and Implementation d) Determine most appropriate standardised technology – automated, centralised vs. decentralised e) Fulfill Statutory Functions – NIOH, NICD, NCR, expanded to include Forensic Toxicology Deliver Quality, Customer-focused Service NDOH Point 2. 3 Improving Quality of Health Services a) Improve Customer perceptions of service delivery to the bench-mark score of 75% b) Ensure retention of international quality standards to ISO 15189 Accredit ALL reference, academic and regional labs with SANAS Develop and maintain internal accreditation system for peripheral labs in line with ISO 15189 Expand accredited EQA programmes throughout Africa NDOH Point 2. 6 Revitalisation Align Resources, Support Services & Infrastructural Development for Service Delivery of Infrastructure b) c) d) Implement the 10 -year Infrastructural Plan Enhance Supply Chain Management Align ICT systems to optimise service delivery Rollout LIS country-wide Develop and utilise Health Technology Assessment Unit Become Laboratory Services “Employer of Choice” vs. “Employer of last resort” a) Recruit & retain key talent – both in core professional groups, as well as support services b) Strengthen leadership & management capacity – implement NHLS Leadership Academy c) Drive disciplined, accountable, collaborative, purpose-filled Organisational Culture e) 5. Partner with Academic Institutions to align teaching and training of core professionals for fulfilment of planned pipeline Investigate mid-level workers NDOH Point 2. 5 Improved HR Planning, Devt and Management NDOH Point 2. 4 Overhauling Health Care System & Improve its Management 21
 5 -YEAR STRATEGIC DRIVERS 10 -POINT PLAN 6. Position NHLS as the Provider of Choice for NHI a) b) 7. b) c) 8. Investigate Joint-Ventures with other providers / suppliers Deliver Quality, Customer-focused Service to build credibility and Trust in NHLS Prioritise Innovation & Research a) c) d) e) 9. Establish Biorepository – specimens for teaching & research Build Institutional Archives – recording pioneering ventures & historical “firsts”, retaining knowledge capital for posterity Expand monitoring & evaluation of programme & health outcomes beyond Surveillance Avail Health System Information to decision-makers (using coterminous health boundaries) Provide information to manage the organisation & promote Accountability culture Convert information to knowledge to advocate Policy and change Practice Drive Stakeholder Collaboration a) Ensure integrated and unified plans of action amongst cross-sector stakeholders 10. NDOH Point 2. 3 Improving Quality of Health Services Safeguard national assets b) NDOH Point 2. 10 Strengthen Research & Development Develop new diagnostic tools applicable to resource-limited settings Encourage research into solutions (applicable to resource-limited settings) for priority diseases Innovate in systems and processes to improve laboratory and health service delivery Become the Health Information Powerhouse a) NDOH Point 2. 2 Implementation of NHI To manage priority diseases To improve worker health To strengthen Health system delivery NDOH Point 2. 1 Creation of Social Compact for better health outcomes Protect our Community & Environment a) b) c) Become energy & resource efficient Dispose waste and assets in environmentally-friendly manner Strive for paperless organisation 22
5 -YEAR STRATEGIC DRIVERS 10 -POINT PLAN 6. Position NHLS as the Provider of Choice for NHI a) b) 7. b) c) 8. Investigate Joint-Ventures with other providers / suppliers Deliver Quality, Customer-focused Service to build credibility and Trust in NHLS Prioritise Innovation & Research a) c) d) e) 9. Establish Biorepository – specimens for teaching & research Build Institutional Archives – recording pioneering ventures & historical “firsts”, retaining knowledge capital for posterity Expand monitoring & evaluation of programme & health outcomes beyond Surveillance Avail Health System Information to decision-makers (using coterminous health boundaries) Provide information to manage the organisation & promote Accountability culture Convert information to knowledge to advocate Policy and change Practice Drive Stakeholder Collaboration a) Ensure integrated and unified plans of action amongst cross-sector stakeholders 10. NDOH Point 2. 3 Improving Quality of Health Services Safeguard national assets b) NDOH Point 2. 10 Strengthen Research & Development Develop new diagnostic tools applicable to resource-limited settings Encourage research into solutions (applicable to resource-limited settings) for priority diseases Innovate in systems and processes to improve laboratory and health service delivery Become the Health Information Powerhouse a) NDOH Point 2. 2 Implementation of NHI To manage priority diseases To improve worker health To strengthen Health system delivery NDOH Point 2. 1 Creation of Social Compact for better health outcomes Protect our Community & Environment a) b) c) Become energy & resource efficient Dispose waste and assets in environmentally-friendly manner Strive for paperless organisation 22
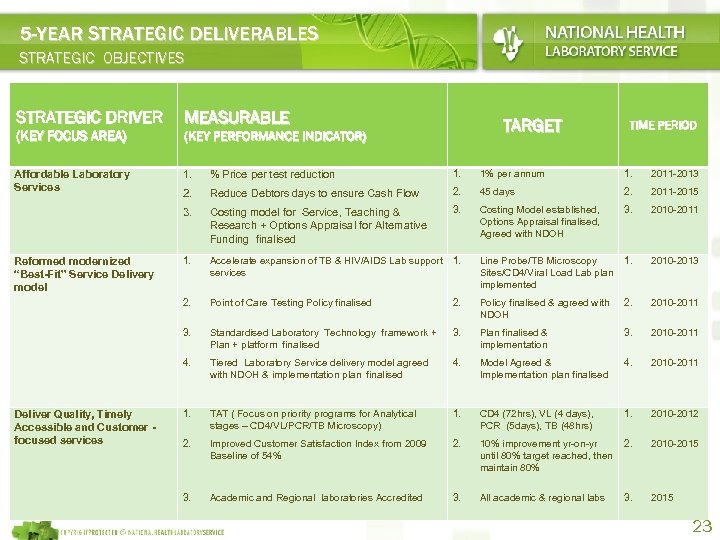 5 -YEAR STRATEGIC DELIVERABLES STRATEGIC OBJECTIVES STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) TIME PERIOD 1. 1% per annum 1. 2011 -2013 2. Reduce Debtors days to ensure Cash Flow 2. 45 days 2. 2011 -2015 Costing model for Service, Teaching & Research + Options Appraisal for Alternative Funding finalised 3. Costing Model established, Options Appraisal finalised, Agreed with NDOH 3. 2010 -2011 1. Accelerate expansion of TB & HIV/AIDS Lab support services 1. Line Probe/TB Microscopy Sites/CD 4/Viral Load Lab plan implemented 1. 2010 -2013 Point of Care Testing Policy finalised 2. Policy finalised & agreed with NDOH 2. 2010 -2011 3. Standardised Laboratory Technology framework + Plan + platform finalised 3. Plan finalised & implementation 3. 2010 -2011 4. Deliver Quality, Timely Accessible and Customer focused services % Price per test reduction 2. Reformed modernized “Best-Fit” Service Delivery model 1. 3. Affordable Laboratory Services Tiered Laboratory Service delivery model agreed with NDOH & implementation plan finalised 4. Model Agreed & Implementation plan finalised 4. 2010 -2011 1. TAT ( Focus on priority programs for Analytical stages – CD 4/VL/PCR/TB Microscopy) 1. CD 4 (72 hrs), VL (4 days), PCR (5 days), TB (48 hrs) 1. 2010 -2012 2. Improved Customer Satisfaction Index from 2009 Baseline of 54% 2. 10% improvement yr-on-yr until 80% target reached, then maintain 80% 2. 2010 -2015 3. Academic and Regional laboratories Accredited 3. All academic & regional labs 3. 2015 23
5 -YEAR STRATEGIC DELIVERABLES STRATEGIC OBJECTIVES STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) TIME PERIOD 1. 1% per annum 1. 2011 -2013 2. Reduce Debtors days to ensure Cash Flow 2. 45 days 2. 2011 -2015 Costing model for Service, Teaching & Research + Options Appraisal for Alternative Funding finalised 3. Costing Model established, Options Appraisal finalised, Agreed with NDOH 3. 2010 -2011 1. Accelerate expansion of TB & HIV/AIDS Lab support services 1. Line Probe/TB Microscopy Sites/CD 4/Viral Load Lab plan implemented 1. 2010 -2013 Point of Care Testing Policy finalised 2. Policy finalised & agreed with NDOH 2. 2010 -2011 3. Standardised Laboratory Technology framework + Plan + platform finalised 3. Plan finalised & implementation 3. 2010 -2011 4. Deliver Quality, Timely Accessible and Customer focused services % Price per test reduction 2. Reformed modernized “Best-Fit” Service Delivery model 1. 3. Affordable Laboratory Services Tiered Laboratory Service delivery model agreed with NDOH & implementation plan finalised 4. Model Agreed & Implementation plan finalised 4. 2010 -2011 1. TAT ( Focus on priority programs for Analytical stages – CD 4/VL/PCR/TB Microscopy) 1. CD 4 (72 hrs), VL (4 days), PCR (5 days), TB (48 hrs) 1. 2010 -2012 2. Improved Customer Satisfaction Index from 2009 Baseline of 54% 2. 10% improvement yr-on-yr until 80% target reached, then maintain 80% 2. 2010 -2015 3. Academic and Regional laboratories Accredited 3. All academic & regional labs 3. 2015 23
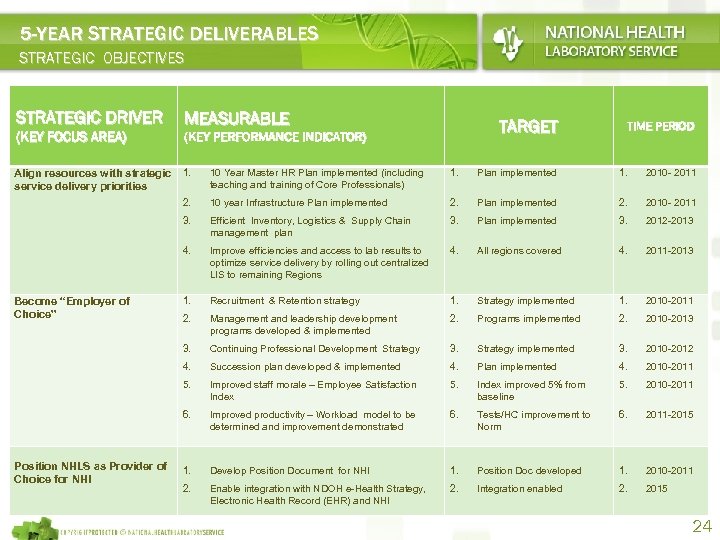 5 -YEAR STRATEGIC DELIVERABLES STRATEGIC OBJECTIVES STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) TIME PERIOD 1. Plan implemented 1. 2010 - 2011 10 year Infrastructure Plan implemented 2. 2010 - 2011 Efficient Inventory, Logistics & Supply Chain management plan 3. Plan implemented 3. 2012 -2013 4. Improve efficiencies and access to lab results to optimize service delivery by rolling out centralized LIS to remaining Regions 4. All regions covered 4. 2011 -2013 1. Recruitment & Retention strategy 1. Strategy implemented 1. 2010 -2011 2. Management and leadership development programs developed & implemented 2. Programs implemented 2. 2010 -2013 3. Continuing Professional Development Strategy 3. Strategy implemented 3. 2010 -2012 4. Succession plan developed & implemented 4. Plan implemented 4. 2010 -2011 5. Improved staff morale – Employee Satisfaction Index 5. Index improved 5% from baseline 5. 2010 -2011 6. Position NHLS as Provider of Choice for NHI 10 Year Master HR Plan implemented (including teaching and training of Core Professionals) 3. Become “Employer of Choice” 1. 2. Align resources with strategic service delivery priorities Improved productivity – Workload model to be determined and improvement demonstrated 6. Tests/HC improvement to Norm 6. 2011 -2015 1. Develop Position Document for NHI 1. Position Doc developed 1. 2010 -2011 2. Enable integration with NDOH e-Health Strategy, Electronic Health Record (EHR) and NHI 2. Integration enabled 2. 2015 24
5 -YEAR STRATEGIC DELIVERABLES STRATEGIC OBJECTIVES STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) TIME PERIOD 1. Plan implemented 1. 2010 - 2011 10 year Infrastructure Plan implemented 2. 2010 - 2011 Efficient Inventory, Logistics & Supply Chain management plan 3. Plan implemented 3. 2012 -2013 4. Improve efficiencies and access to lab results to optimize service delivery by rolling out centralized LIS to remaining Regions 4. All regions covered 4. 2011 -2013 1. Recruitment & Retention strategy 1. Strategy implemented 1. 2010 -2011 2. Management and leadership development programs developed & implemented 2. Programs implemented 2. 2010 -2013 3. Continuing Professional Development Strategy 3. Strategy implemented 3. 2010 -2012 4. Succession plan developed & implemented 4. Plan implemented 4. 2010 -2011 5. Improved staff morale – Employee Satisfaction Index 5. Index improved 5% from baseline 5. 2010 -2011 6. Position NHLS as Provider of Choice for NHI 10 Year Master HR Plan implemented (including teaching and training of Core Professionals) 3. Become “Employer of Choice” 1. 2. Align resources with strategic service delivery priorities Improved productivity – Workload model to be determined and improvement demonstrated 6. Tests/HC improvement to Norm 6. 2011 -2015 1. Develop Position Document for NHI 1. Position Doc developed 1. 2010 -2011 2. Enable integration with NDOH e-Health Strategy, Electronic Health Record (EHR) and NHI 2. Integration enabled 2. 2015 24
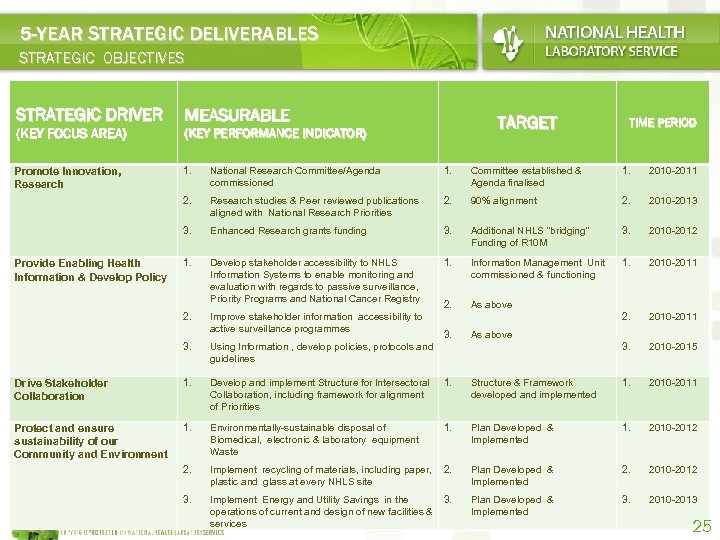 5 -YEAR STRATEGIC DELIVERABLES STRATEGIC OBJECTIVES STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) TIME PERIOD 1. National Research Committee/Agenda commissioned 1. Committee established & Agenda finalised 1. 2010 -2011 2. Research studies & Peer reviewed publications aligned with National Research Priorities 2. 90% alignment 2. 2010 -2013 3. Enhanced Research grants funding 3. Additional NHLS “bridging” Funding of R 10 M 3. 2010 -2012 1. Develop stakeholder accessibility to NHLS Information Systems to enable monitoring and evaluation with regards to passive surveillance, Priority Programs and National Cancer Registry 1. Information Management Unit commissioned & functioning 1. 2010 -2011 2. As above 2. Improve stakeholder information accessibility to active surveillance programmes 2. 2010 -2011 3. Using Information , develop policies, protocols and guidelines 3. 2010 -2015 Drive Stakeholder Collaboration 1. Develop and implement Structure for Intersectoral Collaboration, including framework for alignment of Priorities 1. Structure & Framework developed and implemented 1. 2010 -2011 Protect and ensure sustainability of our Community and Environment 1. Environmentally-sustainable disposal of Biomedical, electronic & laboratory equipment Waste 1. Plan Developed & Implemented 1. 2010 -2012 2. Implement recycling of materials, including paper, plastic and glass at every NHLS site 2. Plan Developed & Implemented 2. 2010 -2012 3. Implement Energy and Utility Savings in the operations of current and design of new facilities & services 3. Plan Developed & Implemented 3. 2010 -2013 Promote Innovation, Research Provide Enabling Health Information & Develop Policy 3. As above 25
5 -YEAR STRATEGIC DELIVERABLES STRATEGIC OBJECTIVES STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) TIME PERIOD 1. National Research Committee/Agenda commissioned 1. Committee established & Agenda finalised 1. 2010 -2011 2. Research studies & Peer reviewed publications aligned with National Research Priorities 2. 90% alignment 2. 2010 -2013 3. Enhanced Research grants funding 3. Additional NHLS “bridging” Funding of R 10 M 3. 2010 -2012 1. Develop stakeholder accessibility to NHLS Information Systems to enable monitoring and evaluation with regards to passive surveillance, Priority Programs and National Cancer Registry 1. Information Management Unit commissioned & functioning 1. 2010 -2011 2. As above 2. Improve stakeholder information accessibility to active surveillance programmes 2. 2010 -2011 3. Using Information , develop policies, protocols and guidelines 3. 2010 -2015 Drive Stakeholder Collaboration 1. Develop and implement Structure for Intersectoral Collaboration, including framework for alignment of Priorities 1. Structure & Framework developed and implemented 1. 2010 -2011 Protect and ensure sustainability of our Community and Environment 1. Environmentally-sustainable disposal of Biomedical, electronic & laboratory equipment Waste 1. Plan Developed & Implemented 1. 2010 -2012 2. Implement recycling of materials, including paper, plastic and glass at every NHLS site 2. Plan Developed & Implemented 2. 2010 -2012 3. Implement Energy and Utility Savings in the operations of current and design of new facilities & services 3. Plan Developed & Implemented 3. 2010 -2013 Promote Innovation, Research Provide Enabling Health Information & Develop Policy 3. As above 25
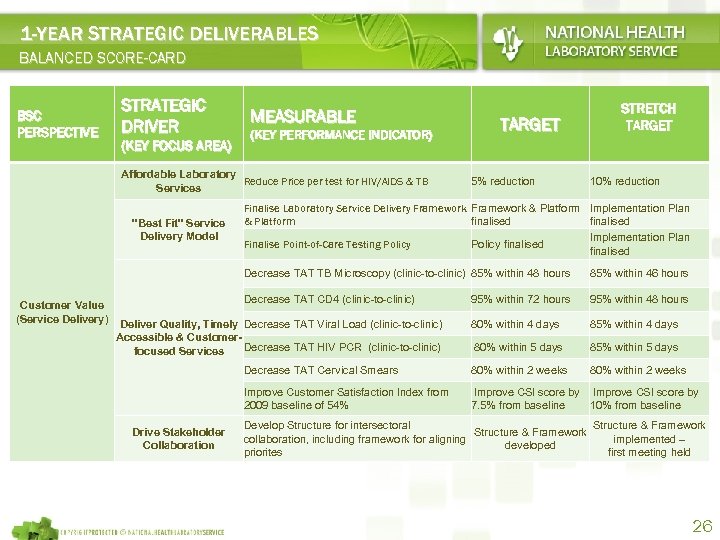 1 -YEAR STRATEGIC DELIVERABLES BALANCED SCORE-CARD BSC PERSPECTIVE STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE (KEY PERFORMANCE INDICATOR) Affordable Laboratory Reduce Price per test for HIV/AIDS & TB Services "Best Fit" Service Delivery Model TARGET 5% reduction STRETCH TARGET 10% reduction Finalise Laboratory Service Delivery Framework & Platform Implementation Plan & Platform finalised Finalise Point-of-Care Testing Policy finalised Implementation Plan finalised Decrease TAT TB Microscopy (clinic-to-clinic) 85% within 48 hours Customer Value (Service Delivery) 85% within 46 hours Decrease TAT CD 4 (clinic-to-clinic) 95% within 72 hours 95% within 48 hours 80% within 4 days 85% within 4 days 80% within 5 days 85% within 5 days Decrease TAT Cervical Smears 80% within 2 weeks Improve Customer Satisfaction Index from 2009 baseline of 54% Improve CSI score by 7. 5% from baseline 10% from baseline Deliver Quality, Timely Decrease TAT Viral Load (clinic-to-clinic) Accessible & Customer. Decrease TAT HIV PCR (clinic-to-clinic) focused Services Drive Stakeholder Collaboration Develop Structure for intersectoral Structure & Framework collaboration, including framework for aligning implemented – developed priorites first meeting held 26
1 -YEAR STRATEGIC DELIVERABLES BALANCED SCORE-CARD BSC PERSPECTIVE STRATEGIC DRIVER (KEY FOCUS AREA) MEASURABLE (KEY PERFORMANCE INDICATOR) Affordable Laboratory Reduce Price per test for HIV/AIDS & TB Services "Best Fit" Service Delivery Model TARGET 5% reduction STRETCH TARGET 10% reduction Finalise Laboratory Service Delivery Framework & Platform Implementation Plan & Platform finalised Finalise Point-of-Care Testing Policy finalised Implementation Plan finalised Decrease TAT TB Microscopy (clinic-to-clinic) 85% within 48 hours Customer Value (Service Delivery) 85% within 46 hours Decrease TAT CD 4 (clinic-to-clinic) 95% within 72 hours 95% within 48 hours 80% within 4 days 85% within 4 days 80% within 5 days 85% within 5 days Decrease TAT Cervical Smears 80% within 2 weeks Improve Customer Satisfaction Index from 2009 baseline of 54% Improve CSI score by 7. 5% from baseline 10% from baseline Deliver Quality, Timely Decrease TAT Viral Load (clinic-to-clinic) Accessible & Customer. Decrease TAT HIV PCR (clinic-to-clinic) focused Services Drive Stakeholder Collaboration Develop Structure for intersectoral Structure & Framework collaboration, including framework for aligning implemented – developed priorites first meeting held 26
 1 -YEAR STRATEGIC DELIVERABLES BALANCED SCORE-CARD STRATEGIC DRIVER BSC PERSPECTIVE (KEY FOCUS AREA) MEASURABLE (KEY PERFORMANCE INDICATOR) Promote Innovation & Commission National Research Committee & Research Agenda Customer Value (Service Delivery) Provide Enabling Health Develop Stakeholder accessibility to Information & Develop information through Information Management Policy Unit (IMU) 30% TARGET STRETCH TARGET Committee established Research Agenda & Research Agenda established with Action finalised Plan Develop list and reporting framework (routine & ad hoc) for Management Information to Stakeholders Determine & Implement Standardised Framework developed Laboratory Technology Framework, Plan and by June 2010 & Plan Platform implemented Situation Analysis complete and Align Resources with Determine & Implement 10 year Infrastructure Plan Strategic Service Plan Operational developed (aligned with Delivery Priorities Efficiency (Internal DOH) Review Trak. Care Lab LIS Rollout Operations) Reviewed Plan finalised Implementation Plan (aligned to Service & Implement for Current Delivery Framework & Platform) & Implement Year Plan Current Year Deliver Quality, Timely Increase % of Academic & Regional Labs 1 more lab than Accessible & Customer 100% of scheduled accredited scheduled focused Services 25% 27
1 -YEAR STRATEGIC DELIVERABLES BALANCED SCORE-CARD STRATEGIC DRIVER BSC PERSPECTIVE (KEY FOCUS AREA) MEASURABLE (KEY PERFORMANCE INDICATOR) Promote Innovation & Commission National Research Committee & Research Agenda Customer Value (Service Delivery) Provide Enabling Health Develop Stakeholder accessibility to Information & Develop information through Information Management Policy Unit (IMU) 30% TARGET STRETCH TARGET Committee established Research Agenda & Research Agenda established with Action finalised Plan Develop list and reporting framework (routine & ad hoc) for Management Information to Stakeholders Determine & Implement Standardised Framework developed Laboratory Technology Framework, Plan and by June 2010 & Plan Platform implemented Situation Analysis complete and Align Resources with Determine & Implement 10 year Infrastructure Plan Strategic Service Plan Operational developed (aligned with Delivery Priorities Efficiency (Internal DOH) Review Trak. Care Lab LIS Rollout Operations) Reviewed Plan finalised Implementation Plan (aligned to Service & Implement for Current Delivery Framework & Platform) & Implement Year Plan Current Year Deliver Quality, Timely Increase % of Academic & Regional Labs 1 more lab than Accessible & Customer 100% of scheduled accredited scheduled focused Services 25% 27
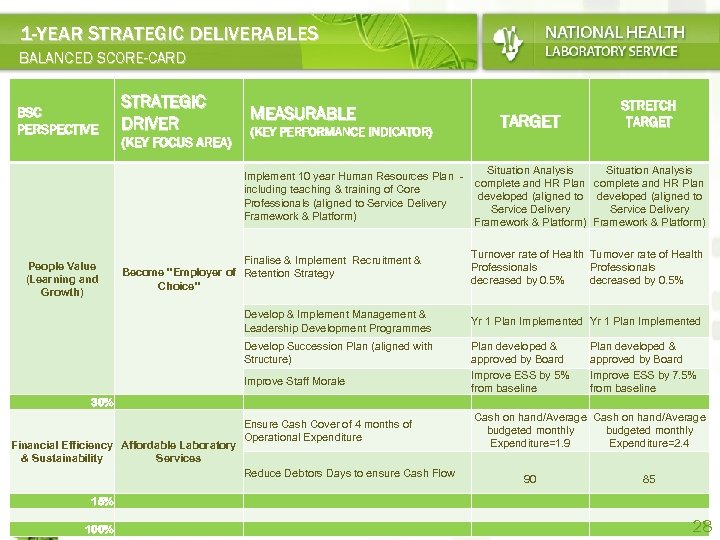 1 -YEAR STRATEGIC DELIVERABLES BALANCED SCORE-CARD BSC PERSPECTIVE STRATEGIC DRIVER MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) (KEY FOCUS AREA) Situation Analysis complete and HR Plan developed (aligned to Service Delivery Framework & Platform) Implement 10 year Human Resources Plan including teaching & training of Core Professionals (aligned to Service Delivery Framework & Platform) People Value (Learning and Growth) Finalise & Implement Recruitment & Become "Employer of Retention Strategy Choice" Develop & Implement Management & Leadership Development Programmes Develop Succession Plan (aligned with Structure) Improve Staff Morale 30% Financial Efficiency Affordable Laboratory & Sustainability Services Ensure Cash Cover of 4 months of Operational Expenditure STRETCH TARGET Turnover rate of Health Professionals decreased by 0. 5% Yr 1 Plan Implemented Plan developed & approved by Board Improve ESS by 5% Improve ESS by 7. 5% from baseline Cash on hand/Average budgeted monthly Expenditure=1. 9 Expenditure=2. 4 Reduce Debtors Days to ensure Cash Flow 90 85 15% 100% 28
1 -YEAR STRATEGIC DELIVERABLES BALANCED SCORE-CARD BSC PERSPECTIVE STRATEGIC DRIVER MEASURABLE TARGET (KEY PERFORMANCE INDICATOR) (KEY FOCUS AREA) Situation Analysis complete and HR Plan developed (aligned to Service Delivery Framework & Platform) Implement 10 year Human Resources Plan including teaching & training of Core Professionals (aligned to Service Delivery Framework & Platform) People Value (Learning and Growth) Finalise & Implement Recruitment & Become "Employer of Retention Strategy Choice" Develop & Implement Management & Leadership Development Programmes Develop Succession Plan (aligned with Structure) Improve Staff Morale 30% Financial Efficiency Affordable Laboratory & Sustainability Services Ensure Cash Cover of 4 months of Operational Expenditure STRETCH TARGET Turnover rate of Health Professionals decreased by 0. 5% Yr 1 Plan Implemented Plan developed & approved by Board Improve ESS by 5% Improve ESS by 7. 5% from baseline Cash on hand/Average budgeted monthly Expenditure=1. 9 Expenditure=2. 4 Reduce Debtors Days to ensure Cash Flow 90 85 15% 100% 28
 www. nhls. ac. za 2010 -11 BUDGET HIGHLIGHTS Financial Objectives: 1. Reduce HIV and TB tests by an average of 10% 2. Generate adequate cashflow R 30 m - R 50 m Cost and Volume assumptions Refer to following slide. Critical dependency in achieving financial objectives In order to achieve the financial objectives set out above, it is imperative that KZN moves from a cost recovery billing model to a Fee for Service model from 1 April 2010. Recommendation ASSUMING that KZN Fee for Service commences 1 April 2010, the following price changes are recommended to achieve a 1. 2% overall effective price reduction over all tests. 1. HIV + TB --> 10% price reduction 2. Other tests --> 1% price increase This would generate the following: - Accounting Surplus - Cash --> R 114 m --> R 30 m Slide 35
www. nhls. ac. za 2010 -11 BUDGET HIGHLIGHTS Financial Objectives: 1. Reduce HIV and TB tests by an average of 10% 2. Generate adequate cashflow R 30 m - R 50 m Cost and Volume assumptions Refer to following slide. Critical dependency in achieving financial objectives In order to achieve the financial objectives set out above, it is imperative that KZN moves from a cost recovery billing model to a Fee for Service model from 1 April 2010. Recommendation ASSUMING that KZN Fee for Service commences 1 April 2010, the following price changes are recommended to achieve a 1. 2% overall effective price reduction over all tests. 1. HIV + TB --> 10% price reduction 2. Other tests --> 1% price increase This would generate the following: - Accounting Surplus - Cash --> R 114 m --> R 30 m Slide 35
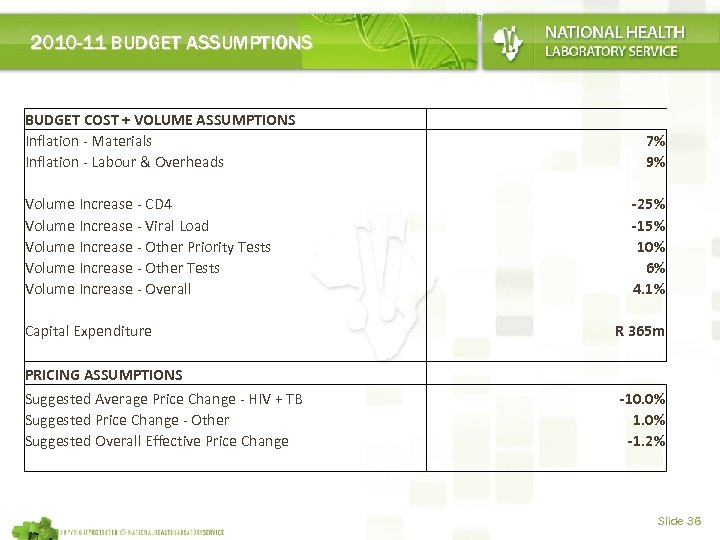 www. nhls. ac. za 2010 -11 BUDGET ASSUMPTIONS BUDGET COST + VOLUME ASSUMPTIONS Inflation - Materials Inflation - Labour & Overheads Volume Increase - CD 4 Volume Increase - Viral Load Volume Increase - Other Priority Tests Volume Increase - Other Tests Volume Increase - Overall Capital Expenditure PRICING ASSUMPTIONS Suggested Average Price Change - HIV + TB Suggested Price Change - Other Suggested Overall Effective Price Change 7% 9% -25% -15% 10% 6% 4. 1% R 365 m -10. 0% 1. 0% -1. 2% Slide 36
www. nhls. ac. za 2010 -11 BUDGET ASSUMPTIONS BUDGET COST + VOLUME ASSUMPTIONS Inflation - Materials Inflation - Labour & Overheads Volume Increase - CD 4 Volume Increase - Viral Load Volume Increase - Other Priority Tests Volume Increase - Other Tests Volume Increase - Overall Capital Expenditure PRICING ASSUMPTIONS Suggested Average Price Change - HIV + TB Suggested Price Change - Other Suggested Overall Effective Price Change 7% 9% -25% -15% 10% 6% 4. 1% R 365 m -10. 0% 1. 0% -1. 2% Slide 36
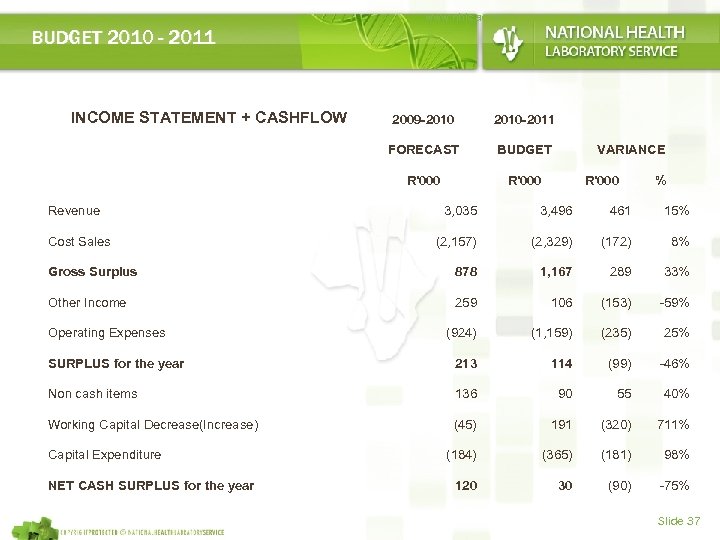 www. nhls. ac. za BUDGET 2010 - 2011 INCOME STATEMENT + CASHFLOW 2010 -2011 FORECAST BUDGET R'000 Revenue 2009 -2010 R'000 VARIANCE R'000 % 3, 035 3, 496 461 15% (2, 157) (2, 329) (172) 8% Gross Surplus 878 1, 167 289 33% Other Income 259 106 (153) -59% (924) (1, 159) (235) 25% SURPLUS for the year 213 114 (99) -46% Non cash items 136 90 55 40% Working Capital Decrease(Increase) (45) 191 (320) 711% (184) (365) (181) 98% 120 30 (90) -75% Cost Sales Operating Expenses Capital Expenditure NET CASH SURPLUS for the year Slide 37
www. nhls. ac. za BUDGET 2010 - 2011 INCOME STATEMENT + CASHFLOW 2010 -2011 FORECAST BUDGET R'000 Revenue 2009 -2010 R'000 VARIANCE R'000 % 3, 035 3, 496 461 15% (2, 157) (2, 329) (172) 8% Gross Surplus 878 1, 167 289 33% Other Income 259 106 (153) -59% (924) (1, 159) (235) 25% SURPLUS for the year 213 114 (99) -46% Non cash items 136 90 55 40% Working Capital Decrease(Increase) (45) 191 (320) 711% (184) (365) (181) 98% 120 30 (90) -75% Cost Sales Operating Expenses Capital Expenditure NET CASH SURPLUS for the year Slide 37
 CONCLUSION Our appreciation to the honourable Chair and members for this opportunity. Questions
CONCLUSION Our appreciation to the honourable Chair and members for this opportunity. Questions


