9b382fca35a45149e7e3f65a3944df78.ppt
- Количество слайдов: 41
 Preoperative Assessment Risk assessment and management G. L. Bryson, MD, FRCPC, MSc Department of Anesthesiology The Ottawa Hospital – Civic Campus
Preoperative Assessment Risk assessment and management G. L. Bryson, MD, FRCPC, MSc Department of Anesthesiology The Ottawa Hospital – Civic Campus
 Objectives • Perioperative morbidity and mortality • You can’t avoid what you can’t anticipate • Preoperative testing • Less than you’d expect • NPO guidelines • Problems Department of Anesthesiology Civic Campus
Objectives • Perioperative morbidity and mortality • You can’t avoid what you can’t anticipate • Preoperative testing • Less than you’d expect • NPO guidelines • Problems Department of Anesthesiology Civic Campus
 Preoperative assessment • Just like the rest of medicine… • History • Physical • Laboratory Department of Anesthesiology Civic Campus
Preoperative assessment • Just like the rest of medicine… • History • Physical • Laboratory Department of Anesthesiology Civic Campus
 An approach to preoperative evaluation • • • What’s wrong with the patient? Is the patient is good as they can get? If not, does it have to be better pre-op? Getting to the OR is less than half the job. Anticipate postoperative problems, then plan. Department of Anesthesiology Civic Campus
An approach to preoperative evaluation • • • What’s wrong with the patient? Is the patient is good as they can get? If not, does it have to be better pre-op? Getting to the OR is less than half the job. Anticipate postoperative problems, then plan. Department of Anesthesiology Civic Campus
 Anesthesia is bad for you • Unable to protect airway • Aspiration • Obstruction • Altered control of ventilation • Diminished response to CO 2 and O 2 • Altered respiratory mechanics • • • FRC, restrictive chest wall defect Myocardial depression Decreased conductivity Vasodilatation Immune suppression Department of Anesthesiology Civic Campus
Anesthesia is bad for you • Unable to protect airway • Aspiration • Obstruction • Altered control of ventilation • Diminished response to CO 2 and O 2 • Altered respiratory mechanics • • • FRC, restrictive chest wall defect Myocardial depression Decreased conductivity Vasodilatation Immune suppression Department of Anesthesiology Civic Campus
 The Killing Fields • Getting patients out of the OR is easy • Getting patients home is another matter • Postoperative course complicated by: • • Increased O 2 demand Myocardial ischemia/infarction Respiratory depression / VQ mismatching Hemorrhage Fluid and electrolyte shifts Hypercoagulable Protein catabolism Department of Anesthesiology Civic Campus
The Killing Fields • Getting patients out of the OR is easy • Getting patients home is another matter • Postoperative course complicated by: • • Increased O 2 demand Myocardial ischemia/infarction Respiratory depression / VQ mismatching Hemorrhage Fluid and electrolyte shifts Hypercoagulable Protein catabolism Department of Anesthesiology Civic Campus
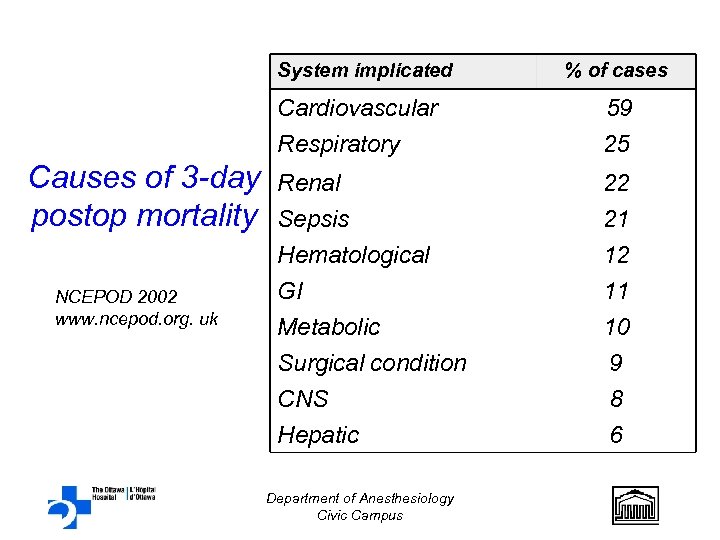 System implicated % of cases Cardiovascular Respiratory Causes of 3 -day postop mortality NCEPOD 2002 www. ncepod. org. uk 59 25 Renal 22 Sepsis Hematological GI Metabolic Surgical condition CNS Hepatic 21 12 11 10 9 8 6 Department of Anesthesiology Civic Campus
System implicated % of cases Cardiovascular Respiratory Causes of 3 -day postop mortality NCEPOD 2002 www. ncepod. org. uk 59 25 Renal 22 Sepsis Hematological GI Metabolic Surgical condition CNS Hepatic 21 12 11 10 9 8 6 Department of Anesthesiology Civic Campus
 Functional capacity predicts outcome • Postoperative cardiac deaths confined to those with VO 2 Max < 3 METS Older P. Chest 1999; 116: 355 -62 • Inability to climb 2 flights of stairs 82% PPV (97% specific) for postoperative CV/RS complications Girish M. Chest 2001; 120: 1147 -51 • Self-reported exercise tolerance < 2 flights of stairs doubled risk of complications following non-cardiac surgery (20% v 10%) Reilly DF. Arch Intern Med 1999; 159(18): 2185 -92 Department of Anesthesiology Civic Campus
Functional capacity predicts outcome • Postoperative cardiac deaths confined to those with VO 2 Max < 3 METS Older P. Chest 1999; 116: 355 -62 • Inability to climb 2 flights of stairs 82% PPV (97% specific) for postoperative CV/RS complications Girish M. Chest 2001; 120: 1147 -51 • Self-reported exercise tolerance < 2 flights of stairs doubled risk of complications following non-cardiac surgery (20% v 10%) Reilly DF. Arch Intern Med 1999; 159(18): 2185 -92 Department of Anesthesiology Civic Campus
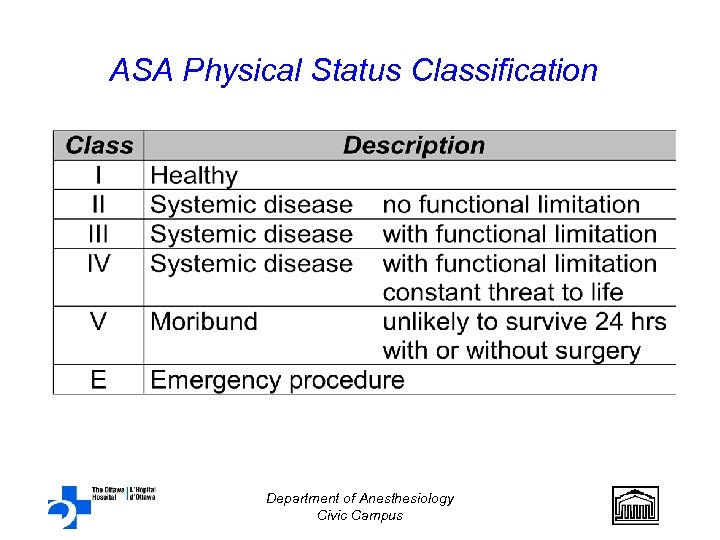 ASA Physical Status Classification Department of Anesthesiology Civic Campus
ASA Physical Status Classification Department of Anesthesiology Civic Campus
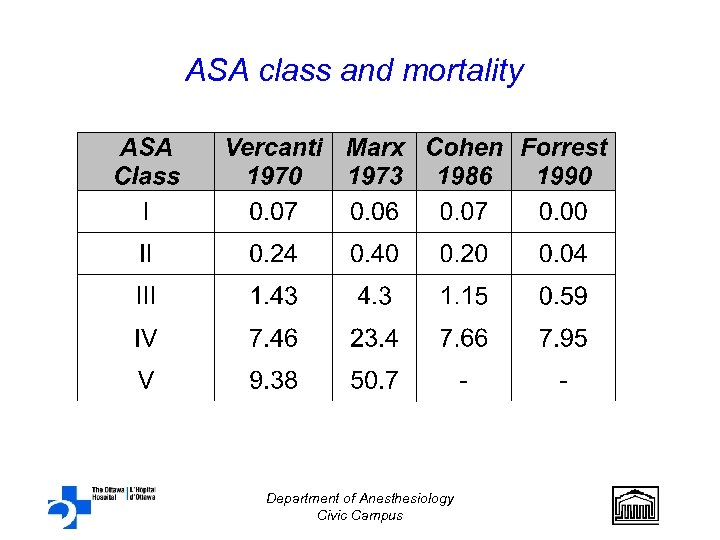 ASA class and mortality Department of Anesthesiology Civic Campus
ASA class and mortality Department of Anesthesiology Civic Campus
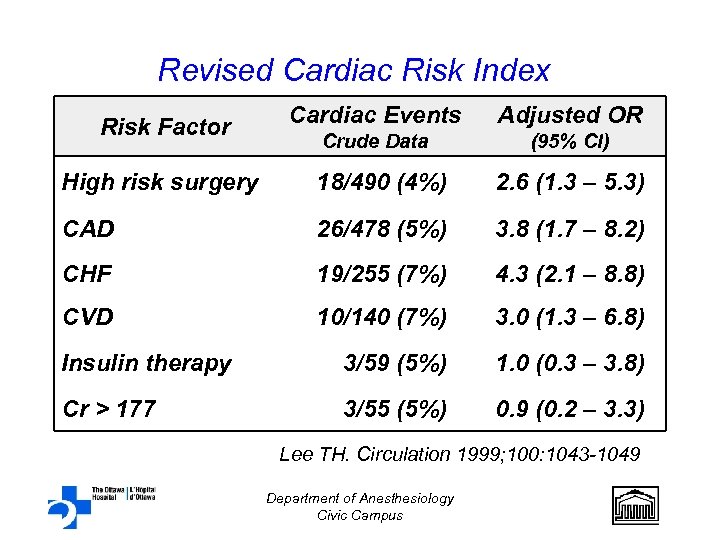 Revised Cardiac Risk Index Risk Factor Cardiac Events Adjusted OR Crude Data (95% CI) High risk surgery 18/490 (4%) 2. 6 (1. 3 – 5. 3) CAD 26/478 (5%) 3. 8 (1. 7 – 8. 2) CHF 19/255 (7%) 4. 3 (2. 1 – 8. 8) CVD 10/140 (7%) 3. 0 (1. 3 – 6. 8) Insulin therapy 3/59 (5%) 1. 0 (0. 3 – 3. 8) Cr > 177 3/55 (5%) 0. 9 (0. 2 – 3. 3) Lee TH. Circulation 1999; 100: 1043 -1049 Department of Anesthesiology Civic Campus
Revised Cardiac Risk Index Risk Factor Cardiac Events Adjusted OR Crude Data (95% CI) High risk surgery 18/490 (4%) 2. 6 (1. 3 – 5. 3) CAD 26/478 (5%) 3. 8 (1. 7 – 8. 2) CHF 19/255 (7%) 4. 3 (2. 1 – 8. 8) CVD 10/140 (7%) 3. 0 (1. 3 – 6. 8) Insulin therapy 3/59 (5%) 1. 0 (0. 3 – 3. 8) Cr > 177 3/55 (5%) 0. 9 (0. 2 – 3. 3) Lee TH. Circulation 1999; 100: 1043 -1049 Department of Anesthesiology Civic Campus
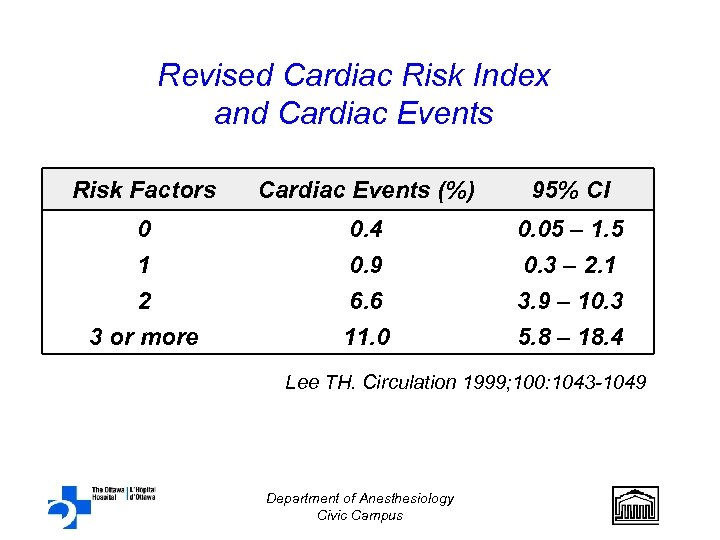 Revised Cardiac Risk Index and Cardiac Events Risk Factors Cardiac Events (%) 95% CI 0 0. 4 0. 05 – 1. 5 1 0. 9 0. 3 – 2. 1 2 6. 6 3. 9 – 10. 3 3 or more 11. 0 5. 8 – 18. 4 Lee TH. Circulation 1999; 100: 1043 -1049 Department of Anesthesiology Civic Campus
Revised Cardiac Risk Index and Cardiac Events Risk Factors Cardiac Events (%) 95% CI 0 0. 4 0. 05 – 1. 5 1 0. 9 0. 3 – 2. 1 2 6. 6 3. 9 – 10. 3 3 or more 11. 0 5. 8 – 18. 4 Lee TH. Circulation 1999; 100: 1043 -1049 Department of Anesthesiology Civic Campus
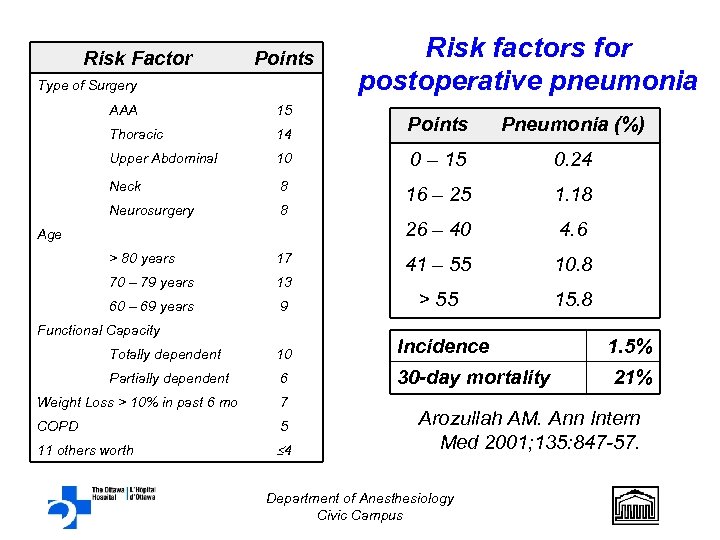 Risk Factor Points Type of Surgery AAA 15 Thoracic 14 Upper Abdominal Risk factors for postoperative pneumonia Points Pneumonia (%) 10 0 – 15 0. 24 Neck 8 Neurosurgery 8 16 – 25 1. 18 26 – 40 4. 6 > 80 years 17 70 – 79 years 13 41 – 55 10. 8 60 – 69 years 9 > 55 15. 8 Age Functional Capacity Totally dependent 10 Incidence 1. 5% Partially dependent 6 30 -day mortality 21% Weight Loss > 10% in past 6 mo 7 COPD 5 11 others worth 4 Arozullah AM. Ann Intern Med 2001; 135: 847 -57. Department of Anesthesiology Civic Campus
Risk Factor Points Type of Surgery AAA 15 Thoracic 14 Upper Abdominal Risk factors for postoperative pneumonia Points Pneumonia (%) 10 0 – 15 0. 24 Neck 8 Neurosurgery 8 16 – 25 1. 18 26 – 40 4. 6 > 80 years 17 70 – 79 years 13 41 – 55 10. 8 60 – 69 years 9 > 55 15. 8 Age Functional Capacity Totally dependent 10 Incidence 1. 5% Partially dependent 6 30 -day mortality 21% Weight Loss > 10% in past 6 mo 7 COPD 5 11 others worth 4 Arozullah AM. Ann Intern Med 2001; 135: 847 -57. Department of Anesthesiology Civic Campus
 Preoperative testing • Routine preoperative testing isn’t helpful Munro J. Health Technology Assessment 1997; 1(12) • Testing should “follow” history and physical • Like most testing, it’s most helpful when you don’t know what the answer is. • OMA-GAC statement • http: //gacguidelines. ca/pdfs/tools/Ontario%20 Preoperative%20 Testing %20 Grid. pdf • Elective versus emergency patient Department of Anesthesiology Civic Campus
Preoperative testing • Routine preoperative testing isn’t helpful Munro J. Health Technology Assessment 1997; 1(12) • Testing should “follow” history and physical • Like most testing, it’s most helpful when you don’t know what the answer is. • OMA-GAC statement • http: //gacguidelines. ca/pdfs/tools/Ontario%20 Preoperative%20 Testing %20 Grid. pdf • Elective versus emergency patient Department of Anesthesiology Civic Campus
 OMA-GAC recommendations http: //gacguidelines. ca/pdfs/tools/ Ontario%20 Preoperative%20 Tes ting%20 Grid. pdf Department of Anesthesiology Civic Campus
OMA-GAC recommendations http: //gacguidelines. ca/pdfs/tools/ Ontario%20 Preoperative%20 Tes ting%20 Grid. pdf Department of Anesthesiology Civic Campus
 TOH fasting guidelines • For elective surgery: • NPO solids at 2400 • Unlimited water until 3 hours preop • For urgent surgery: • NPO solids a minimum of 6 hours • NPO clear fluids 3 hours • Modified by urgency of surgery • All usual medications given, except • Anticoagulants, oral hypoglycemics, MAOIs • Insulin and glucose require physician order Department of Anesthesiology Civic Campus
TOH fasting guidelines • For elective surgery: • NPO solids at 2400 • Unlimited water until 3 hours preop • For urgent surgery: • NPO solids a minimum of 6 hours • NPO clear fluids 3 hours • Modified by urgency of surgery • All usual medications given, except • Anticoagulants, oral hypoglycemics, MAOIs • Insulin and glucose require physician order Department of Anesthesiology Civic Campus
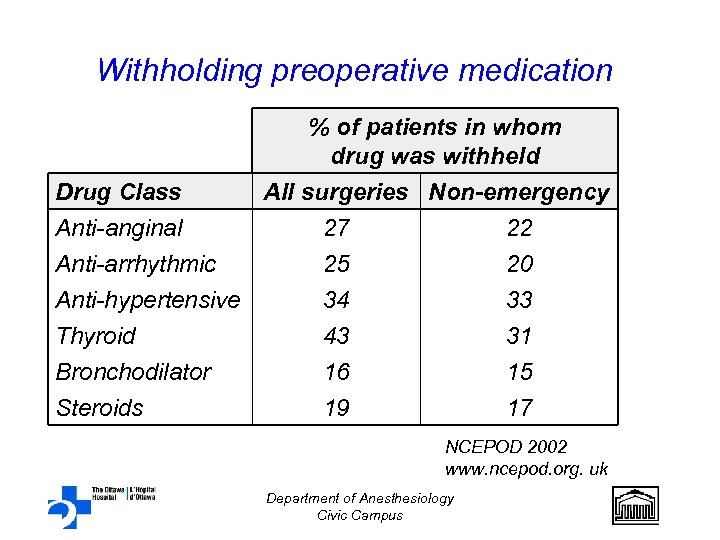 Withholding preoperative medication Drug Class Anti-anginal Anti-arrhythmic Anti-hypertensive Thyroid Bronchodilator Steroids % of patients in whom drug was withheld All surgeries Non-emergency 27 22 25 34 43 16 19 20 33 31 15 17 NCEPOD 2002 www. ncepod. org. uk Department of Anesthesiology Civic Campus
Withholding preoperative medication Drug Class Anti-anginal Anti-arrhythmic Anti-hypertensive Thyroid Bronchodilator Steroids % of patients in whom drug was withheld All surgeries Non-emergency 27 22 25 34 43 16 19 20 33 31 15 17 NCEPOD 2002 www. ncepod. org. uk Department of Anesthesiology Civic Campus
 Valvular or congenital heart disease • Stenotic lesions intolerant of changes in preload/afterload • R L shunts aggravated by hypoxia & SVR • Important to understand the plumbing • Preoperative echocardiogram helpful • Anticoagulation issues • SBE prophylaxis • www. americanheart. org/Scientific/statements/1997/079701. html Department of Anesthesiology Civic Campus
Valvular or congenital heart disease • Stenotic lesions intolerant of changes in preload/afterload • R L shunts aggravated by hypoxia & SVR • Important to understand the plumbing • Preoperative echocardiogram helpful • Anticoagulation issues • SBE prophylaxis • www. americanheart. org/Scientific/statements/1997/079701. html Department of Anesthesiology Civic Campus
 Subacute bacterial endocarditits • Oral / dental surgery • Ampicillin 2000 mg (50 mg/kg) IV 60 min pre-op • Cefazolin 1000 mg (25 mg/kg) IV 60 min pre-op • Clindamycin 600 mg (20 mg/kg) IV 60 min pre-op • Gastrointestinal, genitourinary • As above, plus • Gentamicin 1. 5 mg/kg IV 60 minutes pre-op • Vancomycin 1000 mg (20 mg/kg) IV 60 minutes pre-op, if penicillin-sensitive • Repeat Ampicillin 6 hours post-op if high-risk pathology http: //circ. ahajournals. org/cgi/content/full/96/1/358 Department of Anesthesiology Civic Campus
Subacute bacterial endocarditits • Oral / dental surgery • Ampicillin 2000 mg (50 mg/kg) IV 60 min pre-op • Cefazolin 1000 mg (25 mg/kg) IV 60 min pre-op • Clindamycin 600 mg (20 mg/kg) IV 60 min pre-op • Gastrointestinal, genitourinary • As above, plus • Gentamicin 1. 5 mg/kg IV 60 minutes pre-op • Vancomycin 1000 mg (20 mg/kg) IV 60 minutes pre-op, if penicillin-sensitive • Repeat Ampicillin 6 hours post-op if high-risk pathology http: //circ. ahajournals. org/cgi/content/full/96/1/358 Department of Anesthesiology Civic Campus
 Pacemakers and AICDs • Pacemakers • • • Should be evaluated preoperatively If pacemaker dependent, reprogram to VOO Rate adaptive functions may need to be disabled Use bipolar cautery, if possible Short bursts if monopolar required • AICDs • Must be turned off preoperatively • in monitored environment Department of Anesthesiology Civic Campus
Pacemakers and AICDs • Pacemakers • • • Should be evaluated preoperatively If pacemaker dependent, reprogram to VOO Rate adaptive functions may need to be disabled Use bipolar cautery, if possible Short bursts if monopolar required • AICDs • Must be turned off preoperatively • in monitored environment Department of Anesthesiology Civic Campus
 Anticoagulation • Normal coagulation expected preoperatively • Neuraxial hematoma & surgical hemorrhage • • • Coumadin held for 5 days INR less than 1. 4 LMWH held for 24 hours UFH held for 6 hours Fancy antiplatelet drugs withdrawn (7 days) ASA is OK for most procedures • Vitamin K needs a day • Don’t drown folks with FFP Department of Anesthesiology Civic Campus
Anticoagulation • Normal coagulation expected preoperatively • Neuraxial hematoma & surgical hemorrhage • • • Coumadin held for 5 days INR less than 1. 4 LMWH held for 24 hours UFH held for 6 hours Fancy antiplatelet drugs withdrawn (7 days) ASA is OK for most procedures • Vitamin K needs a day • Don’t drown folks with FFP Department of Anesthesiology Civic Campus
 I think that’s a blood thinner • Clopidogrel (Plavix) • Abciximab (Rheo. Pro) • Eptifibatide (Integrilin) • Low molecular weight heparins • • Dalteparin (Fragmin) Enoxaparin (Lovenox) Nadroparin (Fraxiparin) Tinzaparin (Innohep) • Fondaparinux (Arixtra) • Ximelagatran (Exanta) Department of Anesthesiology Civic Campus
I think that’s a blood thinner • Clopidogrel (Plavix) • Abciximab (Rheo. Pro) • Eptifibatide (Integrilin) • Low molecular weight heparins • • Dalteparin (Fragmin) Enoxaparin (Lovenox) Nadroparin (Fraxiparin) Tinzaparin (Innohep) • Fondaparinux (Arixtra) • Ximelagatran (Exanta) Department of Anesthesiology Civic Campus
 Summary • Preoperative assessment must identify and anticipate perioperative problems • Getting to the OR is the easy part • Communication is essential • Fasting should not exclude hydration or medication • Laboratory testing should be individualized Department of Anesthesiology Civic Campus
Summary • Preoperative assessment must identify and anticipate perioperative problems • Getting to the OR is the easy part • Communication is essential • Fasting should not exclude hydration or medication • Laboratory testing should be individualized Department of Anesthesiology Civic Campus
 Questions? ? The surgeon is a carnivorous beast. It’s happy only when there is fresh meat on the table. Ross Kerridge MD, FRCA Newcastle, Australia At WCA Montreal 2000 Department of Anesthesiology Civic Campus
Questions? ? The surgeon is a carnivorous beast. It’s happy only when there is fresh meat on the table. Ross Kerridge MD, FRCA Newcastle, Australia At WCA Montreal 2000 Department of Anesthesiology Civic Campus
 Case 1 • 64 yr old male scheduled for hemicolectomy for colon ca. Past history includes: • • Diabetes x 15 years (on insulin) CVA 3 years ago Stable CCS 3 angina He takes diltiazem, hctz, and plavix • What is his risk of cardiovascular event? • What preoperative tests would you order? • What preop instructions would you give? Department of Anesthesiology Civic Campus
Case 1 • 64 yr old male scheduled for hemicolectomy for colon ca. Past history includes: • • Diabetes x 15 years (on insulin) CVA 3 years ago Stable CCS 3 angina He takes diltiazem, hctz, and plavix • What is his risk of cardiovascular event? • What preoperative tests would you order? • What preop instructions would you give? Department of Anesthesiology Civic Campus
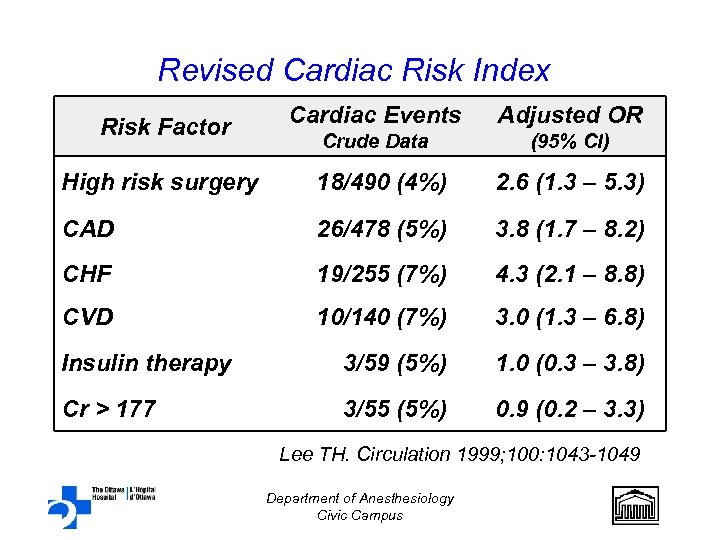 Revised Cardiac Risk Index Risk Factor Cardiac Events Adjusted OR Crude Data (95% CI) High risk surgery 18/490 (4%) 2. 6 (1. 3 – 5. 3) CAD 26/478 (5%) 3. 8 (1. 7 – 8. 2) CHF 19/255 (7%) 4. 3 (2. 1 – 8. 8) CVD 10/140 (7%) 3. 0 (1. 3 – 6. 8) Insulin therapy 3/59 (5%) 1. 0 (0. 3 – 3. 8) Cr > 177 3/55 (5%) 0. 9 (0. 2 – 3. 3) Lee TH. Circulation 1999; 100: 1043 -1049 Department of Anesthesiology Civic Campus
Revised Cardiac Risk Index Risk Factor Cardiac Events Adjusted OR Crude Data (95% CI) High risk surgery 18/490 (4%) 2. 6 (1. 3 – 5. 3) CAD 26/478 (5%) 3. 8 (1. 7 – 8. 2) CHF 19/255 (7%) 4. 3 (2. 1 – 8. 8) CVD 10/140 (7%) 3. 0 (1. 3 – 6. 8) Insulin therapy 3/59 (5%) 1. 0 (0. 3 – 3. 8) Cr > 177 3/55 (5%) 0. 9 (0. 2 – 3. 3) Lee TH. Circulation 1999; 100: 1043 -1049 Department of Anesthesiology Civic Campus
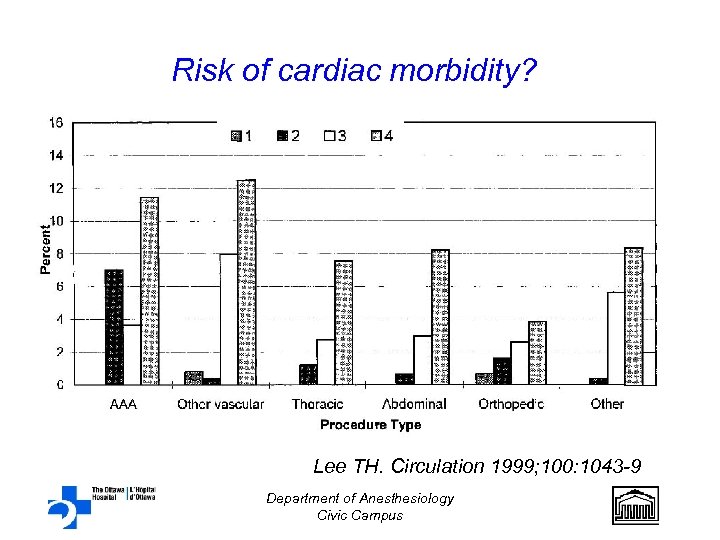 Risk of cardiac morbidity? Lee TH. Circulation 1999; 100: 1043 -9 Department of Anesthesiology Civic Campus
Risk of cardiac morbidity? Lee TH. Circulation 1999; 100: 1043 -9 Department of Anesthesiology Civic Campus
 AHA ACC guidelines for cardiac evaluation prior to noncardiac surgery Department of Anesthesiology Civic Campus
AHA ACC guidelines for cardiac evaluation prior to noncardiac surgery Department of Anesthesiology Civic Campus
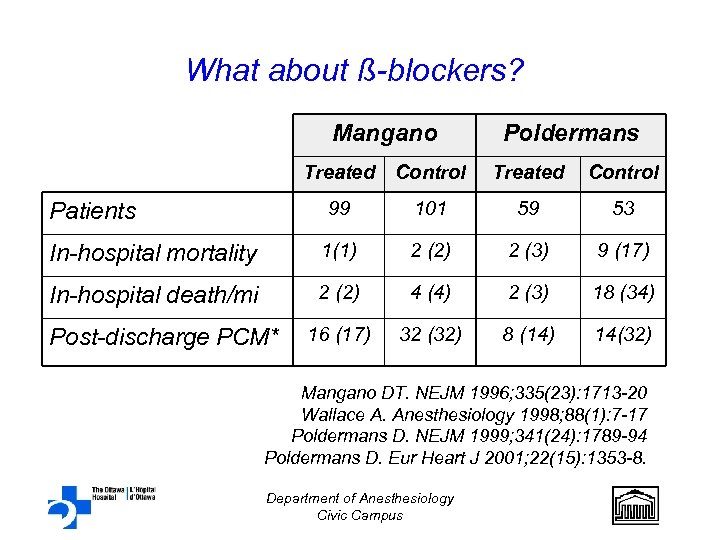 What about ß-blockers? Mangano Poldermans Treated Control 99 101 59 53 In-hospital mortality 1(1) 2 (2) 2 (3) 9 (17) In-hospital death/mi 2 (2) 4 (4) 2 (3) 18 (34) 16 (17) 32 (32) 8 (14) 14(32) Patients Post-discharge PCM* Mangano DT. NEJM 1996; 335(23): 1713 -20 Wallace A. Anesthesiology 1998; 88(1): 7 -17 Poldermans D. NEJM 1999; 341(24): 1789 -94 Poldermans D. Eur Heart J 2001; 22(15): 1353 -8. Department of Anesthesiology Civic Campus
What about ß-blockers? Mangano Poldermans Treated Control 99 101 59 53 In-hospital mortality 1(1) 2 (2) 2 (3) 9 (17) In-hospital death/mi 2 (2) 4 (4) 2 (3) 18 (34) 16 (17) 32 (32) 8 (14) 14(32) Patients Post-discharge PCM* Mangano DT. NEJM 1996; 335(23): 1713 -20 Wallace A. Anesthesiology 1998; 88(1): 7 -17 Poldermans D. NEJM 1999; 341(24): 1789 -94 Poldermans D. Eur Heart J 2001; 22(15): 1353 -8. Department of Anesthesiology Civic Campus
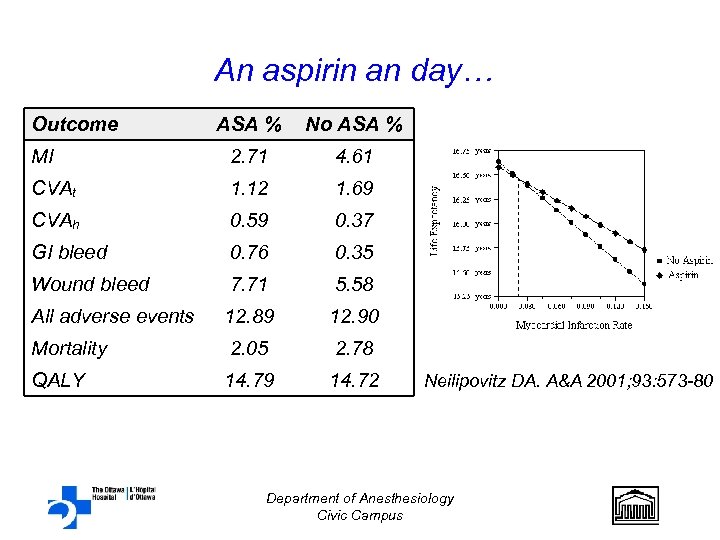 An aspirin an day… Outcome ASA % No ASA % MI 2. 71 4. 61 CVAt 1. 12 1. 69 CVAh 0. 59 0. 37 GI bleed 0. 76 0. 35 Wound bleed 7. 71 5. 58 All adverse events 12. 89 12. 90 Mortality 2. 05 2. 78 QALY 14. 79 14. 72 Neilipovitz DA. A&A 2001; 93: 573 -80 Department of Anesthesiology Civic Campus
An aspirin an day… Outcome ASA % No ASA % MI 2. 71 4. 61 CVAt 1. 12 1. 69 CVAh 0. 59 0. 37 GI bleed 0. 76 0. 35 Wound bleed 7. 71 5. 58 All adverse events 12. 89 12. 90 Mortality 2. 05 2. 78 QALY 14. 79 14. 72 Neilipovitz DA. A&A 2001; 93: 573 -80 Department of Anesthesiology Civic Campus
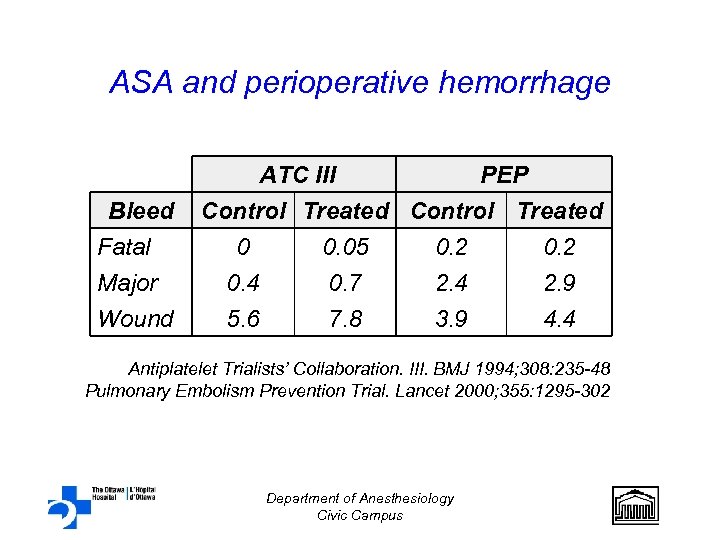 ASA and perioperative hemorrhage Bleed Fatal Major Wound ATC III PEP Control Treated 0 0. 05 0. 2 0. 4 0. 7 2. 4 2. 9 5. 6 7. 8 3. 9 4. 4 Antiplatelet Trialists’ Collaboration. III. BMJ 1994; 308: 235 -48 Pulmonary Embolism Prevention Trial. Lancet 2000; 355: 1295 -302 Department of Anesthesiology Civic Campus
ASA and perioperative hemorrhage Bleed Fatal Major Wound ATC III PEP Control Treated 0 0. 05 0. 2 0. 4 0. 7 2. 4 2. 9 5. 6 7. 8 3. 9 4. 4 Antiplatelet Trialists’ Collaboration. III. BMJ 1994; 308: 235 -48 Pulmonary Embolism Prevention Trial. Lancet 2000; 355: 1295 -302 Department of Anesthesiology Civic Campus
 Case 2 • A 45 yr old male is scheduled for TURP. • He has hypertension, atrial fibrillation, and had a mechanical aortic valve placed 4 years ago. • He takes metoprolol and coumadin. • What investigations? • What instructions? Department of Anesthesiology Civic Campus
Case 2 • A 45 yr old male is scheduled for TURP. • He has hypertension, atrial fibrillation, and had a mechanical aortic valve placed 4 years ago. • He takes metoprolol and coumadin. • What investigations? • What instructions? Department of Anesthesiology Civic Campus
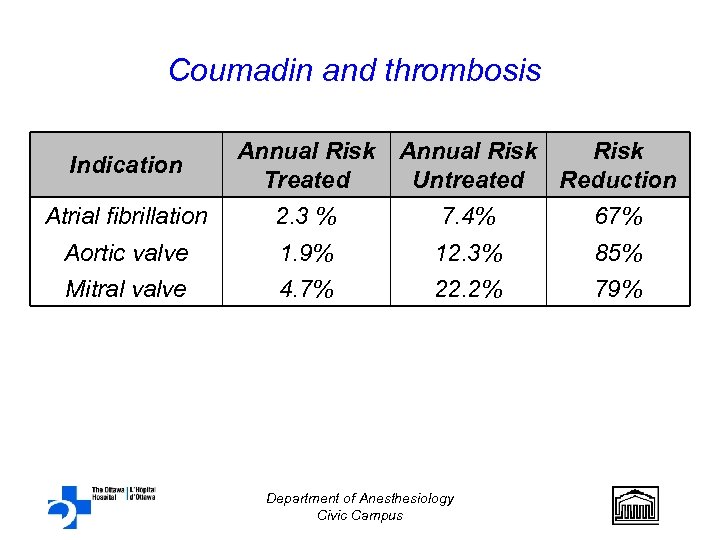 Coumadin and thrombosis Indication Annual Risk Treated Untreated Reduction Atrial fibrillation 2. 3 % 7. 4% 67% Aortic valve Mitral valve 1. 9% 4. 7% 12. 3% 22. 2% 85% 79% Department of Anesthesiology Civic Campus
Coumadin and thrombosis Indication Annual Risk Treated Untreated Reduction Atrial fibrillation 2. 3 % 7. 4% 67% Aortic valve Mitral valve 1. 9% 4. 7% 12. 3% 22. 2% 85% 79% Department of Anesthesiology Civic Campus
 Who needs special care with coumadin? • • DVT < 3 months ago History of recurrent DVT Arterial thromboembolism < 3 months ago Mechanical prosthetic heart valves Tissue prosthetic heart valves + embolism Thrombophilia (lupus ac, Factor V - L, C&S) Atrial fibrillation + embolism Department of Anesthesiology Civic Campus
Who needs special care with coumadin? • • DVT < 3 months ago History of recurrent DVT Arterial thromboembolism < 3 months ago Mechanical prosthetic heart valves Tissue prosthetic heart valves + embolism Thrombophilia (lupus ac, Factor V - L, C&S) Atrial fibrillation + embolism Department of Anesthesiology Civic Campus
 Coumadin withdrawal plan • • • Day -5. Day -3. Day -2. Day -1. Day 0. Day +1. Stop coumadin. Dalteparin 200 u·kg-1 sc. Dalteparin 100 u·kg-1 sc. Check INR pre-op Is surgical blood loss controlled? Restart coumadin Dalteparin 200 u·kg-1 until INR >2. 0 Department of Anesthesiology Civic Campus
Coumadin withdrawal plan • • • Day -5. Day -3. Day -2. Day -1. Day 0. Day +1. Stop coumadin. Dalteparin 200 u·kg-1 sc. Dalteparin 100 u·kg-1 sc. Check INR pre-op Is surgical blood loss controlled? Restart coumadin Dalteparin 200 u·kg-1 until INR >2. 0 Department of Anesthesiology Civic Campus
 Subacute bacterial endocarditits • Oral / dental surgery • Ampicillin 2000 mg (50 mg/kg) IV 60 min pre-op • Cefazolin 1000 mg (25 mg/kg) IV 60 min pre-op • Clindamycin 600 mg (20 mg/kg) IV 60 min pre-op • Gastrointestinal, genitourinary • As above, plus • Gentamicin 1. 5 mg/kg IV 60 minutes pre-op • Vancomycin 1000 mg (20 mg/kg) IV 60 minutes pre-op, if penicillin-sensitive • Repeat Ampicillin 6 hours post-op if high-risk pathology http: //circ. ahajournals. org/cgi/content/full/96/1/358 Department of Anesthesiology Civic Campus
Subacute bacterial endocarditits • Oral / dental surgery • Ampicillin 2000 mg (50 mg/kg) IV 60 min pre-op • Cefazolin 1000 mg (25 mg/kg) IV 60 min pre-op • Clindamycin 600 mg (20 mg/kg) IV 60 min pre-op • Gastrointestinal, genitourinary • As above, plus • Gentamicin 1. 5 mg/kg IV 60 minutes pre-op • Vancomycin 1000 mg (20 mg/kg) IV 60 minutes pre-op, if penicillin-sensitive • Repeat Ampicillin 6 hours post-op if high-risk pathology http: //circ. ahajournals. org/cgi/content/full/96/1/358 Department of Anesthesiology Civic Campus
 Case 3 • 45 yr old female for lumbar spinal fusion • Uses “some percocets” for pain control • Smokes 1. 5 packs per day Department of Anesthesiology Civic Campus
Case 3 • 45 yr old female for lumbar spinal fusion • Uses “some percocets” for pain control • Smokes 1. 5 packs per day Department of Anesthesiology Civic Campus
 Smoking is bad for you • 6 x increase in pulmonary complications • Need to stop > 4 weeks preop Bluman LG. Chest 1998 Apr; 113(4): 883 -9 • 3 x increase in wound complications following breast surgery Sorensen LT Eur J Surg Oncol 2002 Dec; 28(8): 815 -20 • 2 x increase risk of bony non-union Andersen T. Spine 2001 Dec 1; 26(23): 2623 -8 Department of Anesthesiology Civic Campus
Smoking is bad for you • 6 x increase in pulmonary complications • Need to stop > 4 weeks preop Bluman LG. Chest 1998 Apr; 113(4): 883 -9 • 3 x increase in wound complications following breast surgery Sorensen LT Eur J Surg Oncol 2002 Dec; 28(8): 815 -20 • 2 x increase risk of bony non-union Andersen T. Spine 2001 Dec 1; 26(23): 2623 -8 Department of Anesthesiology Civic Campus
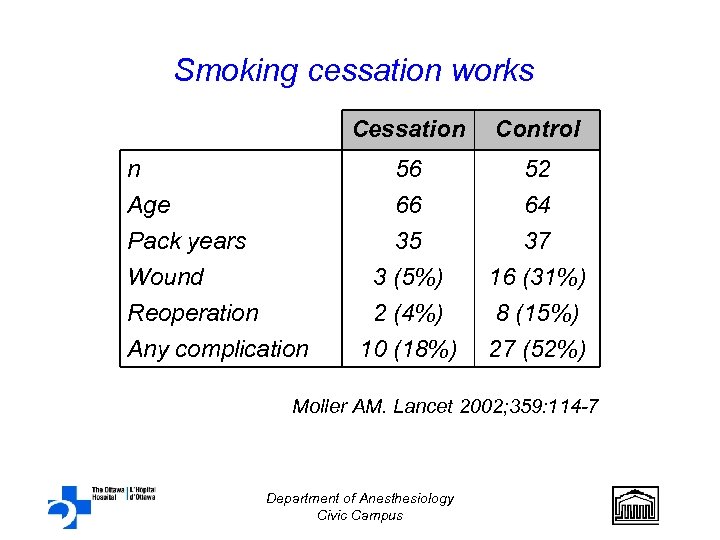 Smoking cessation works Cessation 56 66 35 n Age Pack years Wound Reoperation Any complication Control 52 64 37 3 (5%) 2 (4%) 10 (18%) 16 (31%) 8 (15%) 27 (52%) Moller AM. Lancet 2002; 359: 114 -7 Department of Anesthesiology Civic Campus
Smoking cessation works Cessation 56 66 35 n Age Pack years Wound Reoperation Any complication Control 52 64 37 3 (5%) 2 (4%) 10 (18%) 16 (31%) 8 (15%) 27 (52%) Moller AM. Lancet 2002; 359: 114 -7 Department of Anesthesiology Civic Campus
 Narcotic tolerance • Important to document just how much narcotic patients are taking preoperatively • Previous intake must be accommodated in perioperative care • If patient takes 2 percocets 6 x day • 60 mg oxycodone = 90 mg morphine • 90 mg morphine po = 22. 5 mg morphine IV • Adjust PCA settings accordingly Department of Anesthesiology Civic Campus
Narcotic tolerance • Important to document just how much narcotic patients are taking preoperatively • Previous intake must be accommodated in perioperative care • If patient takes 2 percocets 6 x day • 60 mg oxycodone = 90 mg morphine • 90 mg morphine po = 22. 5 mg morphine IV • Adjust PCA settings accordingly Department of Anesthesiology Civic Campus
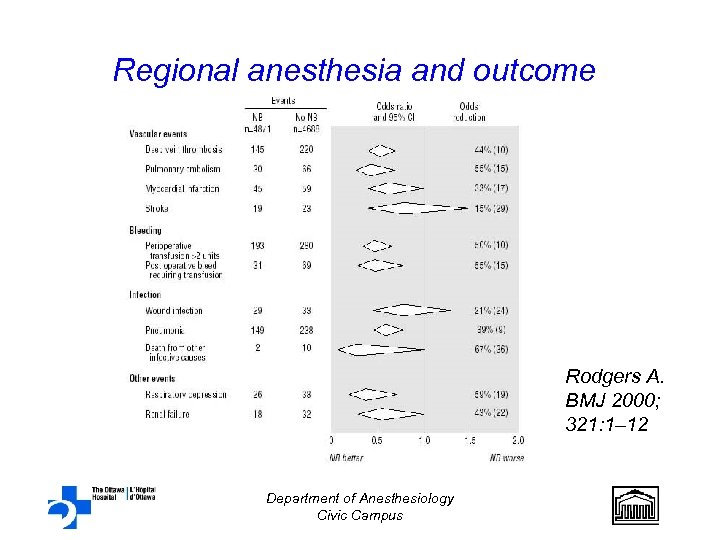 Regional anesthesia and outcome Rodgers A. BMJ 2000; 321: 1– 12 Department of Anesthesiology Civic Campus
Regional anesthesia and outcome Rodgers A. BMJ 2000; 321: 1– 12 Department of Anesthesiology Civic Campus


