5fe0b773c11b115920825cc3cea1ae8a.ppt
- Количество слайдов: 48
 Practical Evaluation of a Pharmacoeconomic Paper Dr J Miot Wits University May 2011
Practical Evaluation of a Pharmacoeconomic Paper Dr J Miot Wits University May 2011
 What is “Health”? World Health Organisation: Health is a “state of complete physical, mental and social well-being” Everyone wants it! HEA PTP: M 207 Health Economics
What is “Health”? World Health Organisation: Health is a “state of complete physical, mental and social well-being” Everyone wants it! HEA PTP: M 207 Health Economics
 Why do we need Health Economics? “All effective health technologies should be free” l Archie Cochrane But l l The introduction of new effective technology is faster than the increase in our ability to pay for them Uncertainty about both effects and resource use for new technologies
Why do we need Health Economics? “All effective health technologies should be free” l Archie Cochrane But l l The introduction of new effective technology is faster than the increase in our ability to pay for them Uncertainty about both effects and resource use for new technologies
 Economic Drivers of Healthcare Costs • • Increasing population Changing population Increase in pace and price of new technology Patient choice and expectation Economies of scale (pvt vs public) Tensions between different fund options Lack of legislative bodies to control price and quality of new health treatments Role of country’s economic well being
Economic Drivers of Healthcare Costs • • Increasing population Changing population Increase in pace and price of new technology Patient choice and expectation Economies of scale (pvt vs public) Tensions between different fund options Lack of legislative bodies to control price and quality of new health treatments Role of country’s economic well being
 Its all about choices Resources are scarce What we “want” is unlimited Therefore involves “choice” How do we choose? HEA PTP: M 207 Health Economics
Its all about choices Resources are scarce What we “want” is unlimited Therefore involves “choice” How do we choose? HEA PTP: M 207 Health Economics
 Balancing Uncertainty and Access Unrestricted Access l Spending scarce healthcare resources on technologies that provide little if any benefit or may even harm Restricted Access l Delaying benefits which could be accrued whilst generating further evidence on effectiveness Need to explore ways to take into account uncertainty while also offering chance for earlier/increased access to novel treatments Trueman P. ISPOR SA 3 rd Annual Conference 2010
Balancing Uncertainty and Access Unrestricted Access l Spending scarce healthcare resources on technologies that provide little if any benefit or may even harm Restricted Access l Delaying benefits which could be accrued whilst generating further evidence on effectiveness Need to explore ways to take into account uncertainty while also offering chance for earlier/increased access to novel treatments Trueman P. ISPOR SA 3 rd Annual Conference 2010
 Health Economics and Choices “Assessment of the overall value of a healthcare intervention for the allocation of resources in a given environment” • Maximise the benefits from available resources • Provides tools to make consistent decisions • Provides value for money based on cost-effectiveness and not on the basis of cost alone
Health Economics and Choices “Assessment of the overall value of a healthcare intervention for the allocation of resources in a given environment” • Maximise the benefits from available resources • Provides tools to make consistent decisions • Provides value for money based on cost-effectiveness and not on the basis of cost alone
 Uses of Health Economics Studies Submission for Re-imbursement Submission for Regulatory approval Academic and Educational Publication for information National Guidance Policy Determination Cost-Benefit Analysis
Uses of Health Economics Studies Submission for Re-imbursement Submission for Regulatory approval Academic and Educational Publication for information National Guidance Policy Determination Cost-Benefit Analysis
 Lets start with an example. . This workshop is giving you a headache! You need treatment for immediate relief. Your treatment options are: Treatment Dose Paracetamol 1000 mg Ibuprofen 400 mg Tramadol 50 mg Lavender essence 1 drop Which is the most cost-effective option?
Lets start with an example. . This workshop is giving you a headache! You need treatment for immediate relief. Your treatment options are: Treatment Dose Paracetamol 1000 mg Ibuprofen 400 mg Tramadol 50 mg Lavender essence 1 drop Which is the most cost-effective option?
 Which is the most cost-effective option? What do you look at first? Clinical Evidence! • Which products have proven clinical benefits? • • Are they all the same or are there differences in outcome? Paracetamol = ibuprofen > tramadol Now look at the costs Which is the most cost-effective option? Sachs C. Oral analgesics for acute non-specific pain. Am Fam Physician 2005; 71: 913 -18.
Which is the most cost-effective option? What do you look at first? Clinical Evidence! • Which products have proven clinical benefits? • • Are they all the same or are there differences in outcome? Paracetamol = ibuprofen > tramadol Now look at the costs Which is the most cost-effective option? Sachs C. Oral analgesics for acute non-specific pain. Am Fam Physician 2005; 71: 913 -18.
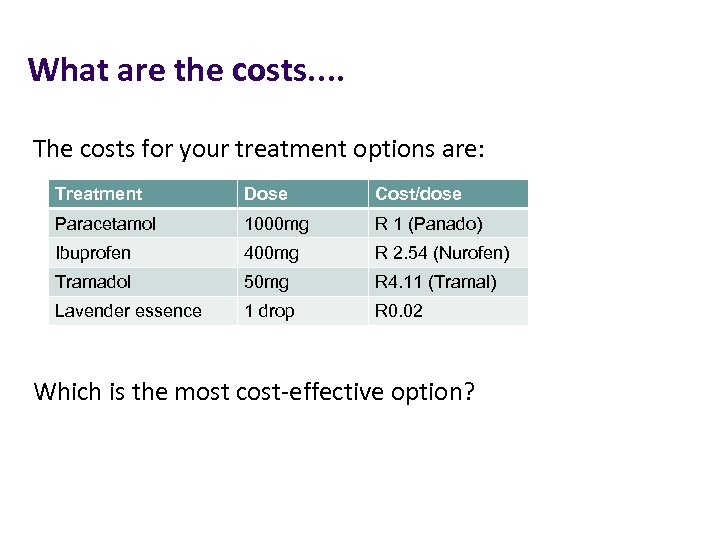 What are the costs. . The costs for your treatment options are: Treatment Dose Cost/dose Paracetamol 1000 mg R 1 (Panado) Ibuprofen 400 mg R 2. 54 (Nurofen) Tramadol 50 mg R 4. 11 (Tramal) Lavender essence 1 drop R 0. 02 Which is the most cost-effective option?
What are the costs. . The costs for your treatment options are: Treatment Dose Cost/dose Paracetamol 1000 mg R 1 (Panado) Ibuprofen 400 mg R 2. 54 (Nurofen) Tramadol 50 mg R 4. 11 (Tramal) Lavender essence 1 drop R 0. 02 Which is the most cost-effective option?
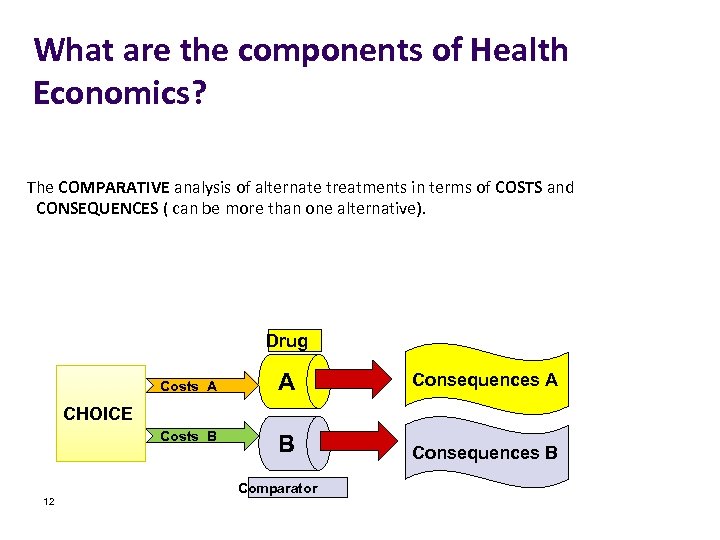 What are the components of Health Economics? The COMPARATIVE analysis of alternate treatments in terms of COSTS and CONSEQUENCES ( can be more than one alternative). Drug Costs A A Consequences A B Consequences B CHOICE Costs B Comparator 12
What are the components of Health Economics? The COMPARATIVE analysis of alternate treatments in terms of COSTS and CONSEQUENCES ( can be more than one alternative). Drug Costs A A Consequences A B Consequences B CHOICE Costs B Comparator 12
 Incremental benefits and costs Generally going to spend more money so have to ask “Is the increased benefit worth the increased cost? ” Incremental Cost Effectiveness Ratio ICER = (Costs B – Costs A) (Effects B- Effects A)
Incremental benefits and costs Generally going to spend more money so have to ask “Is the increased benefit worth the increased cost? ” Incremental Cost Effectiveness Ratio ICER = (Costs B – Costs A) (Effects B- Effects A)
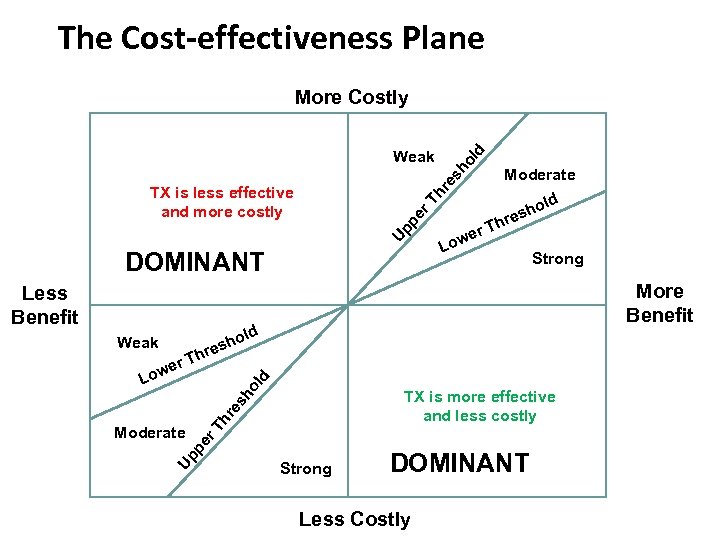 The Cost-effectiveness Plane More Costly ol d Weak Th re sh Moderate Up pe r TX is less effective and more costly DOMINANT Less Benefit Weak o esh r ld h r. T we Lo Strong More Benefit ld h r. T we ho l d Lo Up hr es r. T pe Moderate TX is more effective and less costly Strong DOMINANT Less Costly
The Cost-effectiveness Plane More Costly ol d Weak Th re sh Moderate Up pe r TX is less effective and more costly DOMINANT Less Benefit Weak o esh r ld h r. T we Lo Strong More Benefit ld h r. T we ho l d Lo Up hr es r. T pe Moderate TX is more effective and less costly Strong DOMINANT Less Costly
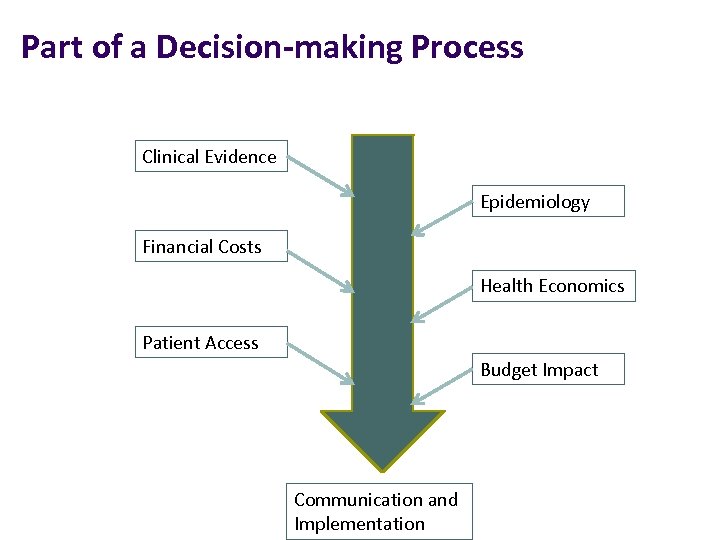 Part of a Decision-making Process Clinical Evidence Epidemiology Financial Costs Health Economics Patient Access Budget Impact Communication and Implementation
Part of a Decision-making Process Clinical Evidence Epidemiology Financial Costs Health Economics Patient Access Budget Impact Communication and Implementation
 Type of HE Study Design: Cost Minimisation Analysis (CMA) Cost Effectiveness Analysis (CEA) • Same outcome, different costs • e. g. antibiotics, generics • “the cheapest option” • Cost Utility Analysis (CUA) Cost Benefit Analysis (CBA) Multiple outcomes, different costs • ‘soft’ measures - pain, suffering and disability • ‘hard’ measures - years of reduced life, restenosis • Combined into a single outcome measure: Quality Adjusted Life Year (QALY) • e. g. biologics in Rheumatoid Arthritis • • Different outcome, different costs • Usually measured in events prevented, lives saved • e. g. Open vs. laparoscopic surgery Similar to CUA but the output measure expressed in monetary units. • Measured in terms of “Willingness to pay” • e. g. cost of diabetic counselling 16
Type of HE Study Design: Cost Minimisation Analysis (CMA) Cost Effectiveness Analysis (CEA) • Same outcome, different costs • e. g. antibiotics, generics • “the cheapest option” • Cost Utility Analysis (CUA) Cost Benefit Analysis (CBA) Multiple outcomes, different costs • ‘soft’ measures - pain, suffering and disability • ‘hard’ measures - years of reduced life, restenosis • Combined into a single outcome measure: Quality Adjusted Life Year (QALY) • e. g. biologics in Rheumatoid Arthritis • • Different outcome, different costs • Usually measured in events prevented, lives saved • e. g. Open vs. laparoscopic surgery Similar to CUA but the output measure expressed in monetary units. • Measured in terms of “Willingness to pay” • e. g. cost of diabetic counselling 16
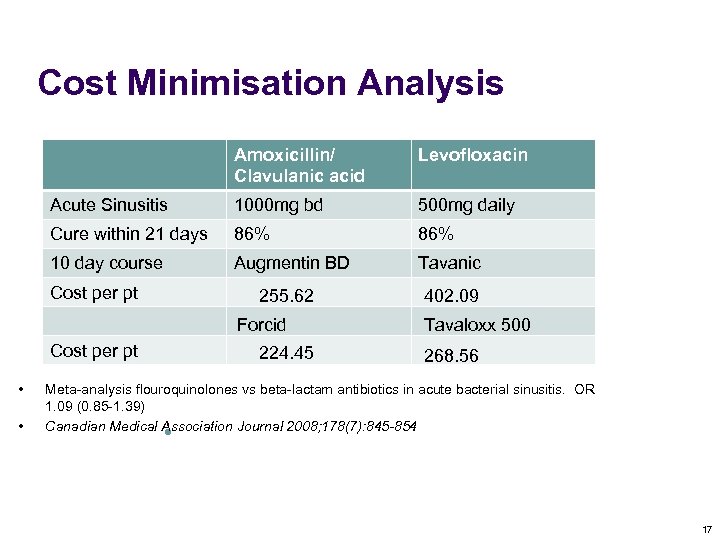 Cost Minimisation Analysis Amoxicillin/ Clavulanic acid Levofloxacin Acute Sinusitis 1000 mg bd 500 mg daily Cure within 21 days 86% 10 day course Augmentin BD Tavanic 255. 62 402. 09 Cost per pt Forcid Cost per pt • • 224. 45 Tavaloxx 500 268. 56 Meta-analysis flouroquinolones vs beta-lactam antibiotics in acute bacterial sinusitis. OR 1. 09 (0. 85 -1. 39) Canadian Medical Association Journal 2008; 178(7): 845 -854 l. Bradley J et al. NEJM, 1991; 325(2): 87 -91 17
Cost Minimisation Analysis Amoxicillin/ Clavulanic acid Levofloxacin Acute Sinusitis 1000 mg bd 500 mg daily Cure within 21 days 86% 10 day course Augmentin BD Tavanic 255. 62 402. 09 Cost per pt Forcid Cost per pt • • 224. 45 Tavaloxx 500 268. 56 Meta-analysis flouroquinolones vs beta-lactam antibiotics in acute bacterial sinusitis. OR 1. 09 (0. 85 -1. 39) Canadian Medical Association Journal 2008; 178(7): 845 -854 l. Bradley J et al. NEJM, 1991; 325(2): 87 -91 17
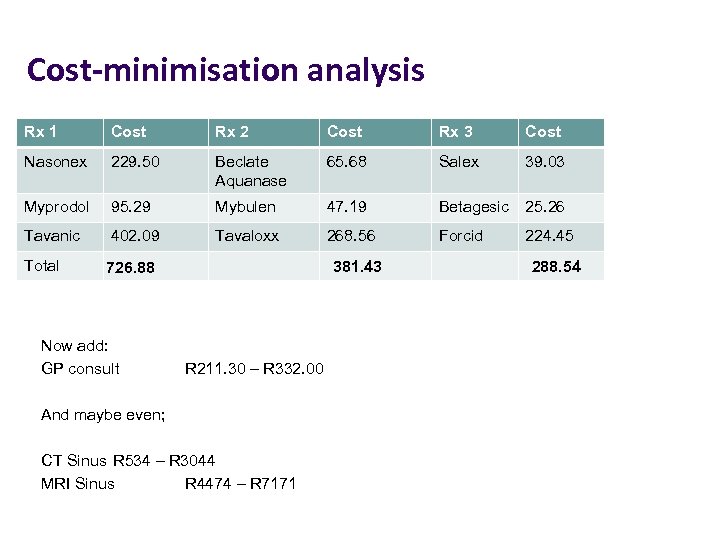 Cost-minimisation analysis Rx 1 Cost Rx 2 Cost Rx 3 Cost Nasonex 229. 50 Beclate Aquanase 65. 68 Salex 39. 03 Myprodol 95. 29 Mybulen 47. 19 Betagesic 25. 26 Tavanic 402. 09 Tavaloxx 268. 56 Forcid 224. 45 Total 726. 88 Now add: GP consult 381. 43 R 211. 30 – R 332. 00 And maybe even; CT Sinus R 534 – R 3044 MRI Sinus R 4474 – R 7171 288. 54
Cost-minimisation analysis Rx 1 Cost Rx 2 Cost Rx 3 Cost Nasonex 229. 50 Beclate Aquanase 65. 68 Salex 39. 03 Myprodol 95. 29 Mybulen 47. 19 Betagesic 25. 26 Tavanic 402. 09 Tavaloxx 268. 56 Forcid 224. 45 Total 726. 88 Now add: GP consult 381. 43 R 211. 30 – R 332. 00 And maybe even; CT Sinus R 534 – R 3044 MRI Sinus R 4474 – R 7171 288. 54
 Type of HE Study Design: Cost Minimisation Analysis (CMA) Cost Effectiveness Analysis (CEA) Different outcome, different costs • Usually measured in events prevented, lives saved • e. g. Open vs. laparoscopic surgery • Cost Utility Analysis (CUA) Cost Benefit Analysis (CBA) 19
Type of HE Study Design: Cost Minimisation Analysis (CMA) Cost Effectiveness Analysis (CEA) Different outcome, different costs • Usually measured in events prevented, lives saved • e. g. Open vs. laparoscopic surgery • Cost Utility Analysis (CUA) Cost Benefit Analysis (CBA) 19
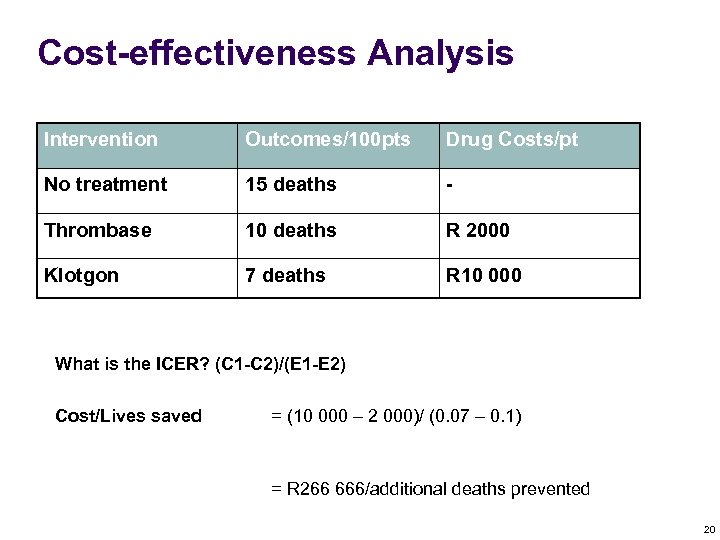 Cost-effectiveness Analysis Intervention Outcomes/100 pts Drug Costs/pt No treatment 15 deaths - Thrombase 10 deaths R 2000 Klotgon 7 deaths R 10 000 What is the ICER? (C 1 -C 2)/(E 1 -E 2) Cost/Lives saved = (10 000 – 2 000)/ (0. 07 – 0. 1) = R 266 666/additional deaths prevented 20
Cost-effectiveness Analysis Intervention Outcomes/100 pts Drug Costs/pt No treatment 15 deaths - Thrombase 10 deaths R 2000 Klotgon 7 deaths R 10 000 What is the ICER? (C 1 -C 2)/(E 1 -E 2) Cost/Lives saved = (10 000 – 2 000)/ (0. 07 – 0. 1) = R 266 666/additional deaths prevented 20
 Type of HE Study Design: Cost Minimisation Analysis (CMA) Cost Effectiveness Analysis (CEA) Cost Utility Analysis (CUA) Cost Benefit Analysis (CBA) Multiple outcomes, different costs • ‘soft’ measures - pain, suffering and disability • ‘hard’ measures - years of reduced life, restenosis • Combined into a single outcome measure: Quality Adjusted Life Year (QALY) • e. g. biologics in Rheumatoid Arthritis • 21
Type of HE Study Design: Cost Minimisation Analysis (CMA) Cost Effectiveness Analysis (CEA) Cost Utility Analysis (CUA) Cost Benefit Analysis (CBA) Multiple outcomes, different costs • ‘soft’ measures - pain, suffering and disability • ‘hard’ measures - years of reduced life, restenosis • Combined into a single outcome measure: Quality Adjusted Life Year (QALY) • e. g. biologics in Rheumatoid Arthritis • 21
 Quality Adjusted Life Years (QALYs) QALYs are generally considered the standard unit of comparison for measuring quality of life outcomes in health economic evaluations QALYs = time (years) x quality (utilities) e. g after amputation above the knee – LE is 40 years but utility is 0. 875 40 x 0. 875 = 35 QALYs
Quality Adjusted Life Years (QALYs) QALYs are generally considered the standard unit of comparison for measuring quality of life outcomes in health economic evaluations QALYs = time (years) x quality (utilities) e. g after amputation above the knee – LE is 40 years but utility is 0. 875 40 x 0. 875 = 35 QALYs
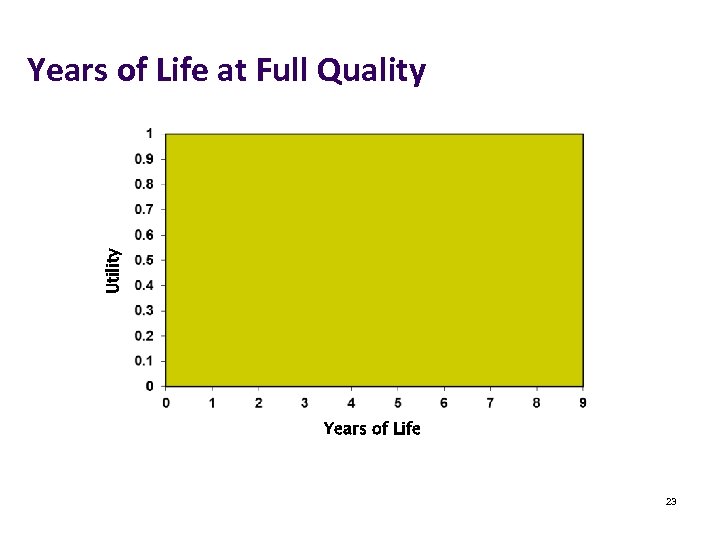 Utility Years of Life at Full Quality Years of Life 23
Utility Years of Life at Full Quality Years of Life 23
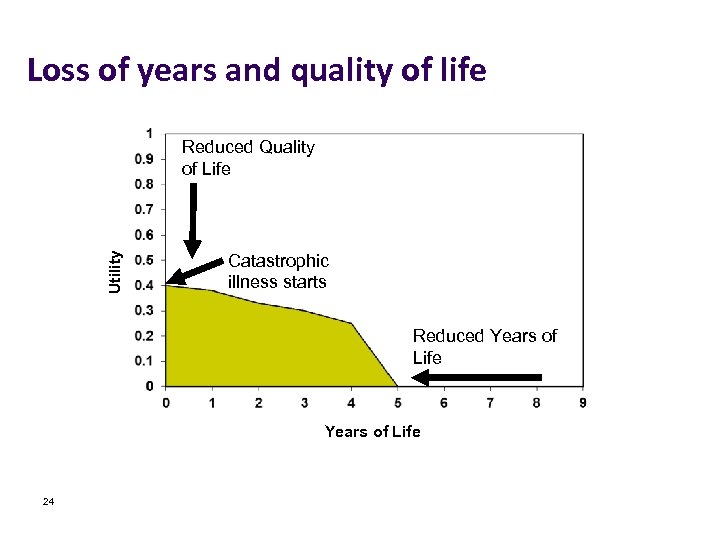 Loss of years and quality of life Utility Reduced Quality of Life Catastrophic illness starts Reduced Years of Life 24
Loss of years and quality of life Utility Reduced Quality of Life Catastrophic illness starts Reduced Years of Life 24
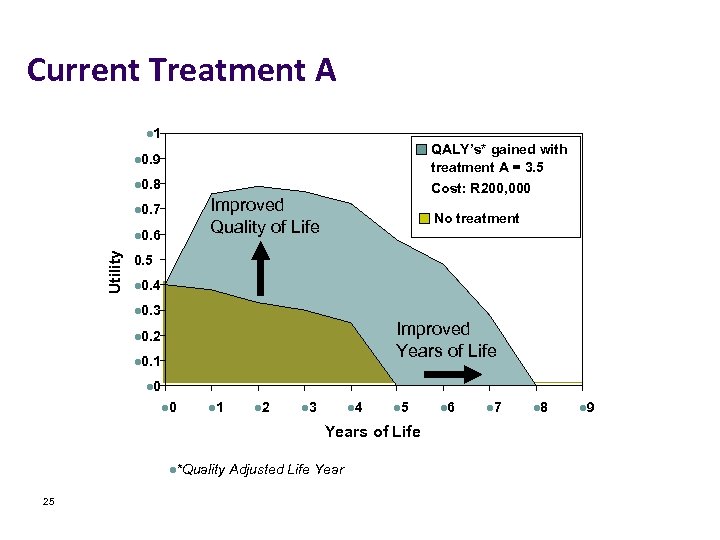 Current Treatment A l 1 QALY’s* gained with treatment A = 3. 5 Cost: R 200, 000 l 0. 9 l 0. 8 Improved l. Improve Quality of Life l 0. 7 Utility l 0. 6 No treatment d Quality of Life 0. 5 l 0. 4 l 0. 3 Improved l. Improv Years of Life l 0. 2 ed Years l 0. 1 l 0 l 1 l 2 l 3 l 4 l 5 Years of Life l*Quality 25 Adjusted Life Year l 6 l 7 l 8 l 9
Current Treatment A l 1 QALY’s* gained with treatment A = 3. 5 Cost: R 200, 000 l 0. 9 l 0. 8 Improved l. Improve Quality of Life l 0. 7 Utility l 0. 6 No treatment d Quality of Life 0. 5 l 0. 4 l 0. 3 Improved l. Improv Years of Life l 0. 2 ed Years l 0. 1 l 0 l 1 l 2 l 3 l 4 l 5 Years of Life l*Quality 25 Adjusted Life Year l 6 l 7 l 8 l 9
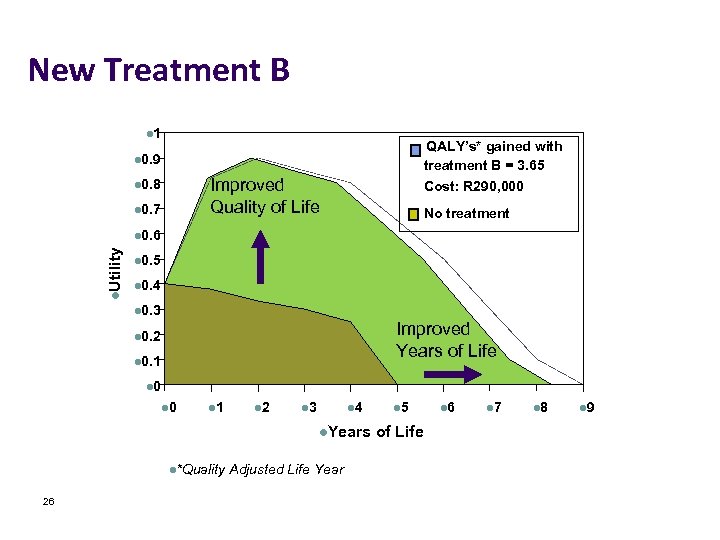 New Treatment B l 1 QALY’s* gained with treatment B = 3. 65 Cost: R 290, 000 l 0. 9 Improved Quality of Life l 0. 8 l 0. 7 No treatment l. Utility l 0. 6 l 0. 5 l 0. 4 l 0. 3 Improved Years of Life l 0. 2 l 0. 1 l 0 l 1 l 2 l 3 l 4 l. Years l*Quality 26 Adjusted Life Year l 5 of Life l 6 l 7 l 8 l 9
New Treatment B l 1 QALY’s* gained with treatment B = 3. 65 Cost: R 290, 000 l 0. 9 Improved Quality of Life l 0. 8 l 0. 7 No treatment l. Utility l 0. 6 l 0. 5 l 0. 4 l 0. 3 Improved Years of Life l 0. 2 l 0. 1 l 0 l 1 l 2 l 3 l 4 l. Years l*Quality 26 Adjusted Life Year l 5 of Life l 6 l 7 l 8 l 9
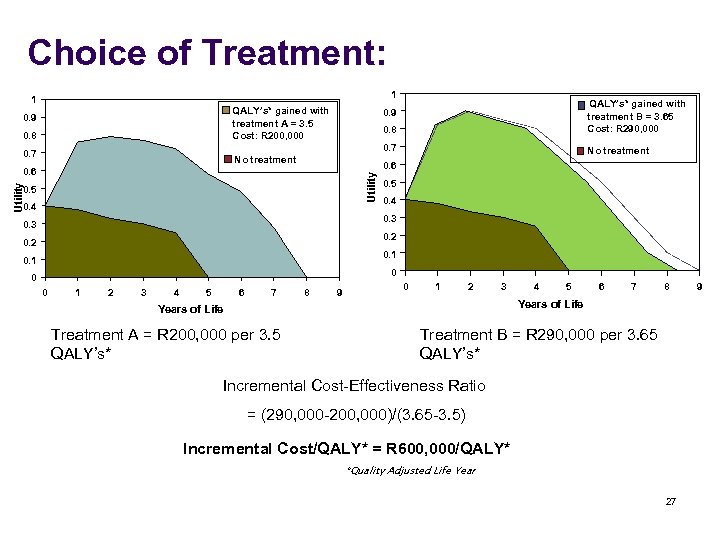 Choice of Treatment: 1 1 0. 8 0. 9 0. 8 Improved Quality of Life No treatment 0. 6 Utility 0. 6 No treatment 0. 9 Utility 0. 7 QALY’s* gained with treatment B = 3. 65 Cost: R 290, 000 0. 7 QALY’s* gained with treatment A = 3. 5 Cost: R 200, 000 0. 5 0. 4 0. 3 0. 2 Improved Years of Life 0. 2 0. 1 0 0 0 1 2 3 4 5 6 7 8 9 0 1 2 3 5 6 7 8 Years of Life Treatment A = R 200, 000 per 3. 5 QALY’s* 4 Treatment B = R 290, 000 per 3. 65 QALY’s* Incremental Cost-Effectiveness Ratio = (290, 000 -200, 000)/(3. 65 -3. 5) Incremental Cost/QALY* = R 600, 000/QALY* *Quality Adjusted Life Year 27 9
Choice of Treatment: 1 1 0. 8 0. 9 0. 8 Improved Quality of Life No treatment 0. 6 Utility 0. 6 No treatment 0. 9 Utility 0. 7 QALY’s* gained with treatment B = 3. 65 Cost: R 290, 000 0. 7 QALY’s* gained with treatment A = 3. 5 Cost: R 200, 000 0. 5 0. 4 0. 3 0. 2 Improved Years of Life 0. 2 0. 1 0 0 0 1 2 3 4 5 6 7 8 9 0 1 2 3 5 6 7 8 Years of Life Treatment A = R 200, 000 per 3. 5 QALY’s* 4 Treatment B = R 290, 000 per 3. 65 QALY’s* Incremental Cost-Effectiveness Ratio = (290, 000 -200, 000)/(3. 65 -3. 5) Incremental Cost/QALY* = R 600, 000/QALY* *Quality Adjusted Life Year 27 9
 Is it a health economics study? l. M. No No Examines only consequences Yes Examines only costs PARTIAL EVALUATION Outcome description alternatives? l. Comparison of two or more Are both costs and consequences examined? Yes PARTIAL EVALUATION Cost-outcome description PARTIAL EVALUATION FULL ECONOMIC EVALUATION Efficacy or effectiveness evaluation Cost -minimisation Cost-effectiveness Cost-utility Cost-benefit Cost analysis Drummond et al, Methods for Economic Evaluation of Health Care Programmes. 2 nd Ed. 1997
Is it a health economics study? l. M. No No Examines only consequences Yes Examines only costs PARTIAL EVALUATION Outcome description alternatives? l. Comparison of two or more Are both costs and consequences examined? Yes PARTIAL EVALUATION Cost-outcome description PARTIAL EVALUATION FULL ECONOMIC EVALUATION Efficacy or effectiveness evaluation Cost -minimisation Cost-effectiveness Cost-utility Cost-benefit Cost analysis Drummond et al, Methods for Economic Evaluation of Health Care Programmes. 2 nd Ed. 1997
 Steps to Evaluating Health Economics 1. What is the question being answered? Was a well-defined question posed in answerable form Look in the introduction and methodology for this info Drummond et al, 1996. Methods for the Economic Evaluation of Health Care Programmes. Chap 3.
Steps to Evaluating Health Economics 1. What is the question being answered? Was a well-defined question posed in answerable form Look in the introduction and methodology for this info Drummond et al, 1996. Methods for the Economic Evaluation of Health Care Programmes. Chap 3.
 2. Are these results useful to me in my setting? • Only if methodology is appropriate and results • • are valid Not every study will answer every question Will reveal weaknesses and strengths of the study
2. Are these results useful to me in my setting? • Only if methodology is appropriate and results • • are valid Not every study will answer every question Will reveal weaknesses and strengths of the study
 Study Perspective Societal : all costs and outcomes Third party payer : public or private Health care provider : hospital Benefits manager in private industry : direct medical costs to employees, productivity of employee Patients : out of pocket expenses, travel and waiting time
Study Perspective Societal : all costs and outcomes Third party payer : public or private Health care provider : hospital Benefits manager in private industry : direct medical costs to employees, productivity of employee Patients : out of pocket expenses, travel and waiting time
 Time horizon Depends on the intervention and the associated harm or benefit Days Weeks Months Years Lifetime 32
Time horizon Depends on the intervention and the associated harm or benefit Days Weeks Months Years Lifetime 32
 3. What are the Clinical Comparators? • Are they properly described? • Were any important alternatives omitted? • Was (should) a do-nothing alternative be considered? • Was an appropriate alternative chosen?
3. What are the Clinical Comparators? • Are they properly described? • Were any important alternatives omitted? • Was (should) a do-nothing alternative be considered? • Was an appropriate alternative chosen?
 4. Is there evidence of effectiveness? • Is it from randomized clinical trials, meta-analysis or • • • expert opinion? Is it effective in clinical practice? Were observational data or assumptions used to establish effectiveness? What about potential biases? Is the appropriate patient population being evaluated? If the treatment is not safe or effective – don’t go any further!
4. Is there evidence of effectiveness? • Is it from randomized clinical trials, meta-analysis or • • • expert opinion? Is it effective in clinical practice? Were observational data or assumptions used to establish effectiveness? What about potential biases? Is the appropriate patient population being evaluated? If the treatment is not safe or effective – don’t go any further!
 5. What are the Clinical Measures? • Hard endpoints – survival, events, cures • Surrogate markers – BP, TC, Viral load etc • Are they relevant and appropriate? • How are they presented? OR, RRR, AR etc
5. What are the Clinical Measures? • Hard endpoints – survival, events, cures • Surrogate markers – BP, TC, Viral load etc • Are they relevant and appropriate? • How are they presented? OR, RRR, AR etc
 6. What costs were measured? • Depends on Perspective • Direct medical costs: drug acquisition costs, pharmacy dispensing costs, lab costs, physician visits for monitoring, treatment of sideeffects etc • Indirect cost: decreased productivity, absenteeism, income lost, forgone leisure time, time spent by pt seeking medical services, time spent by family and friends attending the pt • Intangible cost: psychosocial costs, apprehension, anxiety, grief, loss of well-being, social isolation, family conflict, pain, changes in social functioning and activities of daily living
6. What costs were measured? • Depends on Perspective • Direct medical costs: drug acquisition costs, pharmacy dispensing costs, lab costs, physician visits for monitoring, treatment of sideeffects etc • Indirect cost: decreased productivity, absenteeism, income lost, forgone leisure time, time spent by pt seeking medical services, time spent by family and friends attending the pt • Intangible cost: psychosocial costs, apprehension, anxiety, grief, loss of well-being, social isolation, family conflict, pain, changes in social functioning and activities of daily living
 What costs were measured? Cost = price x utilisation • Were the costs measured correctly in appropriate • • • physical units What measures were used? Were they appropriate? What was omitted from measurement – why? Any special circumstances that make measurement difficult?
What costs were measured? Cost = price x utilisation • Were the costs measured correctly in appropriate • • • physical units What measures were used? Were they appropriate? What was omitted from measurement – why? Any special circumstances that make measurement difficult?
 Were the costs and consequences adjusted for differential timing • Were costs and outcomes occurring in the future • “discounted” to present value Was there any justification of discount rate used? • Were all cost brought to a fixed time period?
Were the costs and consequences adjusted for differential timing • Were costs and outcomes occurring in the future • “discounted” to present value Was there any justification of discount rate used? • Were all cost brought to a fixed time period?

 7. What are the Health Economic Measures? Was an incremental analysis performed? Incremental Cost/Life year gained (LYG) Incremental Cost/QALY Incremental Cost/event prevented Incremental Cost/procedure
7. What are the Health Economic Measures? Was an incremental analysis performed? Incremental Cost/Life year gained (LYG) Incremental Cost/QALY Incremental Cost/event prevented Incremental Cost/procedure
 8. How confident are you that this is a valid outcome? • Was a sensitivity analysis performed? • Was justification provided for the range of values? • Which parameters were sensitive to change and reasons • given for why? Has a statistical analysis been done?
8. How confident are you that this is a valid outcome? • Was a sensitivity analysis performed? • Was justification provided for the range of values? • Which parameters were sensitive to change and reasons • given for why? Has a statistical analysis been done?
 9. Presentation and Discussion • Did the presentation and discussion of study results include all • • • issues of concern to users? Interpreted intelligently or mechanistically? Results compared with other similar studies? What were differences/similarities Discussion on generalisability of results to other settings or pt groups? Account for other important factors? Discuss impact and feasibility of implementation? Conflict of Interests?
9. Presentation and Discussion • Did the presentation and discussion of study results include all • • • issues of concern to users? Interpreted intelligently or mechanistically? Results compared with other similar studies? What were differences/similarities Discussion on generalisability of results to other settings or pt groups? Account for other important factors? Discuss impact and feasibility of implementation? Conflict of Interests?
 What is your perspective? Pessimist: bottle ½ empty Optimist: bottle ½ full Economist: bottle ½ wasted inefficient! HEA PTP: M 207 Health Economics
What is your perspective? Pessimist: bottle ½ empty Optimist: bottle ½ full Economist: bottle ½ wasted inefficient! HEA PTP: M 207 Health Economics
 Challenges in HE Analysis Lack of direct comparisons to relevant alternative l l Head-to-head trials often not available Comparator in trials may not be relevant in our setting Measuring relevant costs and benefits l l Vary from country to country ( transferability) Value of surrogate endpoints Lack of long-term follow-up – extrapolation beyond clinical trials l l l Especially important in chronic disease Some modelling is required Decision needed now - can’t wait until long-term data is available Relevance to local settings – adapting from other settings l Local costs and resource utilisation Reducing uncertainty to improve confidence in outcome l l Sensitivity analysis Cost-effectiveness acceptability curves plotted from probabilistic models
Challenges in HE Analysis Lack of direct comparisons to relevant alternative l l Head-to-head trials often not available Comparator in trials may not be relevant in our setting Measuring relevant costs and benefits l l Vary from country to country ( transferability) Value of surrogate endpoints Lack of long-term follow-up – extrapolation beyond clinical trials l l l Especially important in chronic disease Some modelling is required Decision needed now - can’t wait until long-term data is available Relevance to local settings – adapting from other settings l Local costs and resource utilisation Reducing uncertainty to improve confidence in outcome l l Sensitivity analysis Cost-effectiveness acceptability curves plotted from probabilistic models
 Challenges are Opportunities • Using EBM and Health Economics leads to; • Better clinical outcomes • More efficient use of resources • Reduce over-utilisation • Reduce perverse incentives • Improved re-imbursement structures • Improved training and skills
Challenges are Opportunities • Using EBM and Health Economics leads to; • Better clinical outcomes • More efficient use of resources • Reduce over-utilisation • Reduce perverse incentives • Improved re-imbursement structures • Improved training and skills
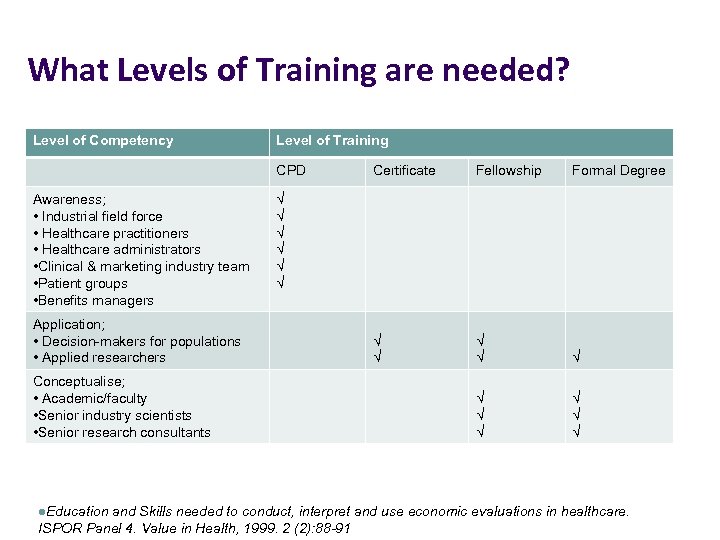 What Levels of Training are needed? Level of Competency Level of Training CPD Awareness; • Industrial field force • Healthcare practitioners • Healthcare administrators • Clinical & marketing industry team • Patient groups • Benefits managers Application; • Decision-makers for populations • Applied researchers Conceptualise; • Academic/faculty • Senior industry scientists • Senior research consultants l. Education Certificate Fellowship Formal Degree √ √ √ √ √ and Skills needed to conduct, interpret and use economic evaluations in healthcare. ISPOR Panel 4. Value in Health, 1999. 2 (2): 88 -91
What Levels of Training are needed? Level of Competency Level of Training CPD Awareness; • Industrial field force • Healthcare practitioners • Healthcare administrators • Clinical & marketing industry team • Patient groups • Benefits managers Application; • Decision-makers for populations • Applied researchers Conceptualise; • Academic/faculty • Senior industry scientists • Senior research consultants l. Education Certificate Fellowship Formal Degree √ √ √ √ √ and Skills needed to conduct, interpret and use economic evaluations in healthcare. ISPOR Panel 4. Value in Health, 1999. 2 (2): 88 -91
 Websites and other useful info ISPOR www. ispor. org NICE www. nice. org. uk Cochrane Database http: //www. healtheconomics. com/ Guidelines for authors and peer reviewers of economic submissions to the BMJ. Drummond M and Jefferson TO. BMJ, 1996: 313: 275 -283 - Notes in file Challenges in systematic reviews of economic analyses. Pignone et al. Ann Intern Med, 2005: 142: 1073 -1079 Methods for Economic Evaluation of Health Care Programmes. Second Edition. Drummond et al. Oxford Medical Publications
Websites and other useful info ISPOR www. ispor. org NICE www. nice. org. uk Cochrane Database http: //www. healtheconomics. com/ Guidelines for authors and peer reviewers of economic submissions to the BMJ. Drummond M and Jefferson TO. BMJ, 1996: 313: 275 -283 - Notes in file Challenges in systematic reviews of economic analyses. Pignone et al. Ann Intern Med, 2005: 142: 1073 -1079 Methods for Economic Evaluation of Health Care Programmes. Second Edition. Drummond et al. Oxford Medical Publications
 Questions?
Questions?


